Emergence and Epidemiology of Ciguatera in the Coastal Cities of Southern China
Abstract
:1. Introduction
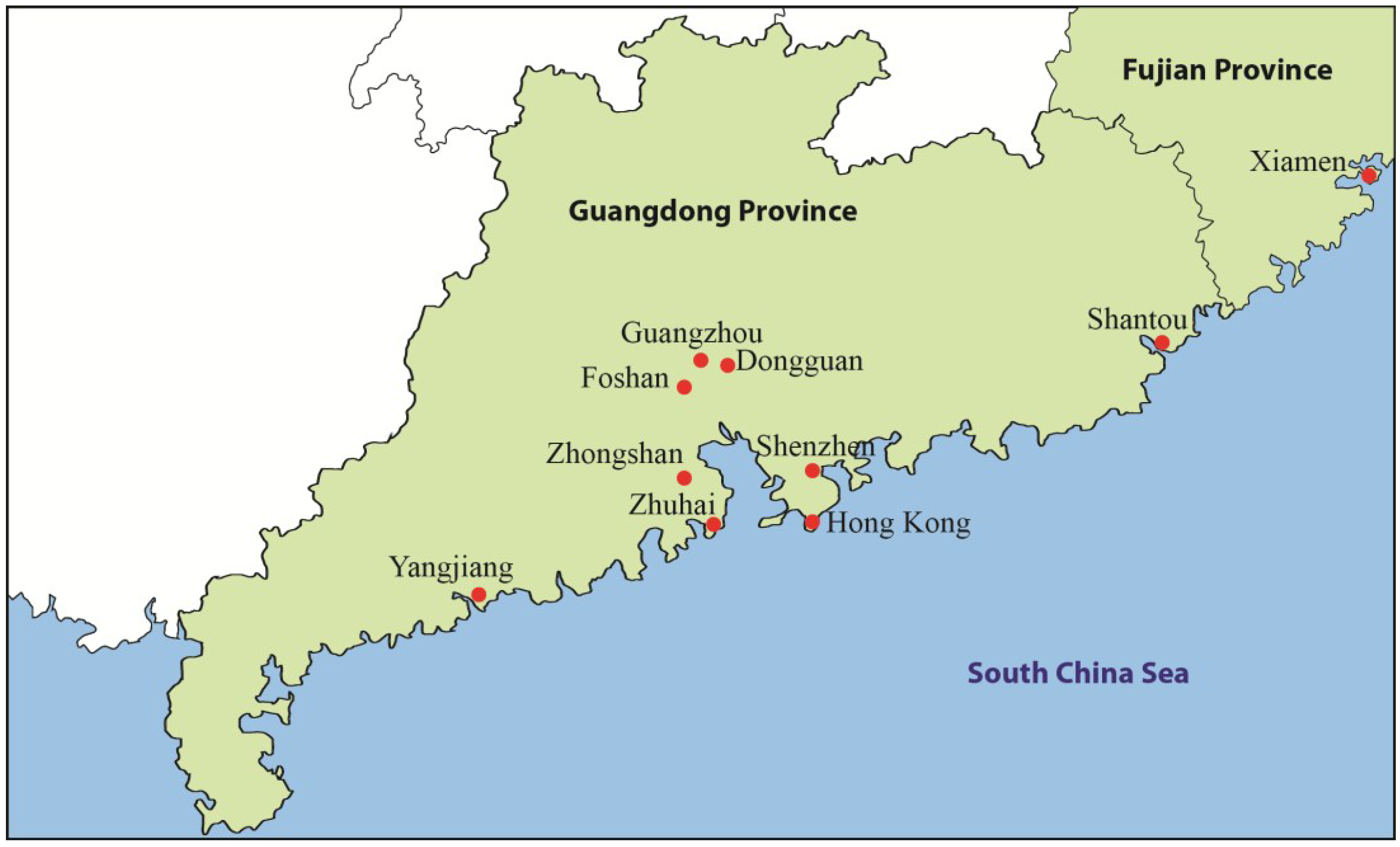
2. Published Case Series of Ciguatera
| City (Reference) | Period | Sex | Age (year) d | Details |
|---|---|---|---|---|
| Xiamen | ||||
| [15] a | 2/2005 | 29M/F c | (9–66) | 3 outbreaks (n = 6–11 in each), after eating portions of large tiger grouper, fish size reflected by the weight of left-over portions (~5 kg), 16 subjects hospitalized |
| Dongguan | ||||
| [16] | 10/2004 | 6M7F | (23–66) | 1 outbreak (n = 14), after sharing a reef fish, 13 subjects admitted to hospital after eating the flesh with skin plus fish head (n = 4), fish belly (n = 8) or fish viscera (n = 4), 1 subject who ate only the flesh had minimal symptoms |
| Foshan | ||||
| [17] | 2004 | 20M/F c | - c | 1 outbreak (n = 20), after sharing a grouper (11.5 kg), 2 subjects hospitalized in cardiac center |
| [18] | 11/2004 | 12M29F | 42(21–92) | 1 outbreak (n = 41), after eating giant grouper, all 41 subjects hospitalized |
| [19] a | 11/2004 | 17M27F | (11–64) | 1 outbreak (n > 100), after eating tiger grouper in a banquet, 44 subjects admitted to this hospital |
| [20] | 11/2004 | 1M1F | (44–47) | 1 outbreak (n > 10), after sharing a grouper, 2 subjects admitted to this hospital |
| [21] | 1/2004–12/2006 | 16M26F | 41(11–60) | 3 outbreaks (n = 42), after eating tiger grouper or leopard coral grouper, all 42 subjects hospitalized |
| Guangzhou | ||||
| [22] | 1–4/1999 | 4M5F | 45(5–80) | 9 subjects hospitalized, after eating moray eel (flesh or viscera) |
| Shantou | ||||
| [23] | 3/1998–4/1999 | 18M7F | (1.4–58) | 6 (4 in 1998, 2 in 1999) outbreaks (n = 3–6 in each), after eating tiger grouper (n = 4) or sea bass (n = 2), 25 subjects hospitalized |
| [24] | 6/2000–12/2004 | 61M21F | (3–68) | 82 subjects hospitalized, after eating humphead wrasse, tiger grouper, flowery grouper, areolated coral grouper, etc. |
| [25,26] a | 8/2004 | 48M16F | (4–76) | 1 outbreak (n = 64), after sharing 2 tiger groupers (>7 kg each), all 64 subjects hospitalized, concomitant alcohol consumption (23 out of 59 subjects) increased the risk of bradycardia (78% vs. 19%), hypotension (48% vs. 14%) and altered skin sensation (96% vs. 42%) |
| Shenzhen | ||||
| [11] b | 10/2003–10/2004 | 14M18F | 45(12–68) | 32 subjects hospitalized (n = 2–16 in each outbreak), after eating humphead wrasse |
| [27] | 1–12/2004 | - c | - c | 4 outbreaks, 60 subjects affected, caused by humphead wrasse (n = 3) or leopard coral grouper (n = 1) |
| [28] b | 10/2004 | 18M8F | 46(21–62) | 26 subjects hospitalized, after sharing a humphead wrasse (14.5 kg) |
| [29] b | 10/2004 | 24M15F | (2–78) | 7 outbreaks (n = 3–12 in each), after eating humphead wrasse |
| [30] | 1/2005–12/2006 | - c | - c | 3 outbreaks, 36 subjects affected, caused by humphead wrasse (n = 2) or leopard coral grouper (n = 1) |
| Yangjiang | ||||
| [31] | 4/2005–12/2008 | 10M7F | 30(13–60) | 4 outbreaks, caused by humphead wrasse, leopard coral grouper or tiger grouper, size 2.0–4.3 kg, 17 subjects with cardiovascular features hospitalized |
| Zhongshan | ||||
| [12] | 4/1994–12/2003 | 33M53F | 38(8–87) | 86 out of 358 subjects with cardiovascular features, after eating tiger grouper, leopard coral grouper or sea bass, size 1.5–2.5 kg, concomitant alcohol consumption in 85% of males |
| [32] | 11/2004 | 54M78F | 43 | 1 outbreak, after eating reef fish (tiger grouper e) in a banquet, 132 subjects admitted to this hospital |
| [33] a | 11/2004 | 36M27F | 43(23–70) | 1 outbreak (n > 200), after eating tiger grouper in a banquet, 63 subjects admitted to this hospital |
| Zhuhai | ||||
| [34] | 5–7/2004 | 9M6F | 42(26–73) | 15 subjects hospitalized, after eating flowery grouper (n = 10) or grouper (n = 5) |
| [35] | 6/2005 | 1M1F | (36–41) | 2 subjects hospitalized, after eating humphead wrasse (flesh and viscera) |
3. Discussion
| Southern China 1994–2008 | Hong Kong [13] 1989–2008 | |
|---|---|---|
| Incidence/million people (year) | 1.1 (2005/6) a to 7.5 (2004) a | 3.3 to 64.9 (median 10.2) |
| >48.7 (2004) b | 1st peak–64.9 (1998) | |
| >129.9 (2004) c | 2nd peak–35.5 (2004) | |
| Large outbreaks (>100–200 subjects) | 3 | 0 |
| Fish species causing large outbreaks | Tiger grouper | – |
| Important fish species d | Tiger grouper, humphead wrasse, areolated coral grouper | Snappers (until 1996) |
| Groupers (from 1997) d |
4. Conclusions
Acknowledgments
Conflicts of Interests
References
- FAO. Ciguatera Fish Poisoning. In Marine Biotoxins; FAO Food and Nutrition Paper 80; Food and Agriculture Organization of the United Nations: Rome, Italy, 2004; pp. 185–218. [Google Scholar]
- Chan, T.Y.K. Large outbreaks of ciguatera after consumption of brown marbled grouper. Toxins 2014, 6, 2041–2049. [Google Scholar] [CrossRef] [PubMed]
- Chan, T.Y.K. Ciguatera caused by consumption of humphead wrasse. Toxicon 2013, 76, 255–259. [Google Scholar] [CrossRef] [PubMed]
- Litaker, R.W.; Vandersea, M.W.; Faust, M.A.; Kibler, S.R.; Nau, A.W.; Holland, W.C.; Chinain, M.; Holmes, M.J.; Tester, P.A. Global distribution of ciguatera causing dinoflagellates in the genus Gambierdiscus. Toxicon 2010, 56, 711–730. [Google Scholar] [CrossRef] [PubMed]
- Lewis, R.J. Ciguatera: Australian perspectives on a global problem. Toxicon 2006, 48, 799–809. [Google Scholar] [CrossRef] [PubMed]
- Wong, C.K.; Hung, P.; Lo, J.Y. Ciguatera fish poisoning in Hong Kong–a 10-year perspective on the class of ciguatoxins. Toxicon 2014, 86, 96–106. [Google Scholar] [CrossRef] [PubMed]
- Dickey, R.W.; Plakas, S.M. Ciguatera: A public health perspective. Toxicon 2010, 56, 123–136. [Google Scholar] [CrossRef] [PubMed]
- Davis, P.Z.R. The current status of the live reef fish trade for food. Available online: http://www.c-3.org.uk/Multimedia/Reports/Live%20Reef%20Fish%20Trade.pdf (accessed on 12 December 2014).
- Sadovy, Y. Ciguatera hits Hong Kong live reef fish trade. SPC Fish. Newsl. 1997, 83, 26–28. [Google Scholar]
- Chan, T.Y.K.; Wang, A.Y.M. Life-threatening bradycardia and hypotension in a patient with ciguatera fish poisoning. Trans. R. Soc. Trop. Med. Hyg. 1993, 87, 71. [Google Scholar] [CrossRef] [PubMed]
- Li, G.Y.; Ma, X.H. Rescuing and nursing of sumei fish toxicosis patients. Heilongjiang Nurs. J. 2005, 11, 781–782. [Google Scholar]
- Zhong, W.J.; Wu, G.F. Ciguatera poisoning in patients with clinical manifestations of cardiovascular system. New Chin. Med. 2006, 37, 316–317. [Google Scholar]
- Chan, T.Y.K. Epidemiology and clinical features of ciguatera fish poisoning in Hong Kong. Toxins 2014, 6, 2989–2997. [Google Scholar] [CrossRef] [PubMed]
- Ren, Y.B.; Zhang, Y. Diagnosis and treatment of 2 cases of ciguatera poisoning. J. Clin. Emerg. Call 2006, 7, 150. [Google Scholar]
- Luo, H.D.; Bai, Y.Y.; Zhou, N. Study of three ciguatera fish poisoning cases in Xiamen city in 2005. Chin. J. Prev. Med. 2011, 45, 512–515. [Google Scholar]
- Liu, Z.Q.; Hu, S.M. Analysis of 13 cases of ciguatera poisoning. J. Pract. Med. 2005, 21, 622–623. [Google Scholar]
- Liu, H.C.; Yan, J.R.; Xu, N.; Song, H.L.; Hu, X.J. Clinical characteristics and treatment of ciguatera poisoning. Chin. J. Prev. Med. 2005, 39, 295. [Google Scholar]
- Wu, Z.Z. Clinical treatment and nursing of 41 patients with ciguatera fish poisoning. Mod. Clin. Nurs. 2005, 4. [Google Scholar] [CrossRef]
- Wen, Y.M.; Wu, G.Q. Clinical analysis of ciguatera poisoning. China Prac. Med. 2007, 2, 74–75. [Google Scholar]
- Song, B.; Zhang, C.G.; Luo, C.E. Reported 2 cases of ciguatera poisoning with changes of nerve electrophysiological. Chin. J. Neurol. 2005, 38, 321. [Google Scholar]
- Chen, G.H.; Wu, Q.; Sun, Y. Clinical Analysis of 42 Patients with ciguatoxin poisoning. Lingnan J. Emerg. Med. 2008, 13, 121–122. [Google Scholar]
- Lu, X.R.; Xie, P.L. Emergency care of 9 cases of ciguatera poisoning. Guangdong Med. J. 2000, 21, 982. [Google Scholar]
- Liao, Q.G.; Sui, M.S.; Chen, J.P. Clinical analysis of 25 cases of ciguatera poisoning. Chin. J. Pract. Intern. Med. 2001, 21, 87–88. [Google Scholar]
- Sui, M.S.; Liao, Q.G.; Zhang, W.C.; Yan, C.Y. Ciguatoxin affects the electrical activity of the heart after consuming grouper. J. Chin. Physician 2005, 7, 1249–1250. [Google Scholar]
- Chen, S.Z. First aid and nursing for 64 patients with colony ciguatera toxins poisoning. Mod. Hosp. 2005, 5, 78–79. [Google Scholar]
- Liao, Q.G.; Sui, M.S.; Chen, J.P. Outbreak of ciguatoxin poisoning in 59 patients. Chin. J. Emerg. Med. 2005, 14, 663–666. [Google Scholar]
- Zhou, P.; Huang, J.S. Analysis of food poisoning due to ciguatoxin in Shenzhen City in 2004. China Trop. Med. 2006, 6, 1093, 1022. [Google Scholar]
- Wang, X.; Xie, N.; Huo, L.P. Diagnosis and test method of ciguatoxin poisoning. Shenzhen J. Integr. Tradit. Chin. West. Med. 2007, 17, 105–106, 110. [Google Scholar]
- Wang, W.N.; Yuan, F.Y.; Liu, Q.F.; Liu, Y. Analysis of the feature of 39 patients with ciguatera fish poisoning. Chin. J. Prim. Med. Pharm. 2006, 13, 757–758. [Google Scholar]
- Liao, Q.X.; Yuan, J.H.; Zhao, S.Q.; Liu, J.J.; Zhang, J.Z.; Huang, W. Analysls of food poisoning due to ciguatoxin in Shenzhen in 2004 to 2006. Lingnan J. Emerg. Med. 2007, 12, 218–219. [Google Scholar]
- Mo, B.X.; Su, Y.N.; Yang, J.L. Cardioprotective effect on shenmai injection on ciguatera poisoning. J. Med. Theor. Prac. 2010, 23, 806–807. [Google Scholar]
- Hu, Y.M.; Chen, W.C.; Guan, Q.X.; Li, X. Clinical analysis of 132 cases of ciguatera poisoning. Chin. J. Intern. Med. 2005, 44, 778–779. [Google Scholar]
- Liu, Z.X.; Wei, H.C.; Lin, Z.; Zhang, X.B.; Song, Z.B.; Wu, Y.X.; Meng, J.Y.; Tan, X.H. Clinical analysis of a collective ciguatoxin poisoning accident in a banquet. China Trop. Med. 2006, 6, 1689–1691. [Google Scholar]
- Wei, L.; Li, W.J. Nursing care of 15 cases of ciguatera poisoning. Mod. Clin. Nurs. 2006, 5, 37–38, 41. [Google Scholar]
- Li, X.F.; Wang, Y.; Ma, L.; Guo, H.X. Analysis 2 cases of ciguatera poisoning. Chin. J. Misdiagn. 2007, 7, 1142–1143. [Google Scholar]
- Xu, Y.X.; Wang, A.H.; Hu, R.; Jiang, T.J.; Jiang, T. Ciguatera toxins in coral fishes along the southern coast of China. China Environ. Sci. 2012, 32, 330–336. [Google Scholar]
- Laurent, D.; Yeeting, B.; Labrosse, P.; Gaudechoux, J.P. Ciguatera: Field Reference Guide; Secretariat of the Pacific Community and Institute of Research for Development: Noumea, New Caledonia, 2005. [Google Scholar]
- Centre for Food Safety. Food Safety Foucs (Hong Kong), 12th issue. Natural toxic substances in seafood. Available online: http://www.cfs.gov.hk/english/multimedia/multimedia_pub/files/FSF12%202007–07–18.pdf (accessed on 12 December 2014).
- Chan, T.Y.K.; Chan, A.Y.W.; Sham, J. The clinical features and management of ciguatera fish poisoning. J. Hong Kong Med. Assoc. 1992, 44, 119–121. [Google Scholar]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chan, T.Y.K. Emergence and Epidemiology of Ciguatera in the Coastal Cities of Southern China. Mar. Drugs 2015, 13, 1175-1184. https://doi.org/10.3390/md13031175
Chan TYK. Emergence and Epidemiology of Ciguatera in the Coastal Cities of Southern China. Marine Drugs. 2015; 13(3):1175-1184. https://doi.org/10.3390/md13031175
Chicago/Turabian StyleChan, Thomas Y. K. 2015. "Emergence and Epidemiology of Ciguatera in the Coastal Cities of Southern China" Marine Drugs 13, no. 3: 1175-1184. https://doi.org/10.3390/md13031175
APA StyleChan, T. Y. K. (2015). Emergence and Epidemiology of Ciguatera in the Coastal Cities of Southern China. Marine Drugs, 13(3), 1175-1184. https://doi.org/10.3390/md13031175





