Genipin-Crosslinked Chitosan Gels and Scaffolds for Tissue Engineering and Regeneration of Cartilage and Bone
Abstract
:1. Introduction and Scope
1.1. Characteristic Properties of Genipin
1.2. Characteristic Properties of Chitosans
1.3. Genipin-Crosslinked Chitosan Hydrogels
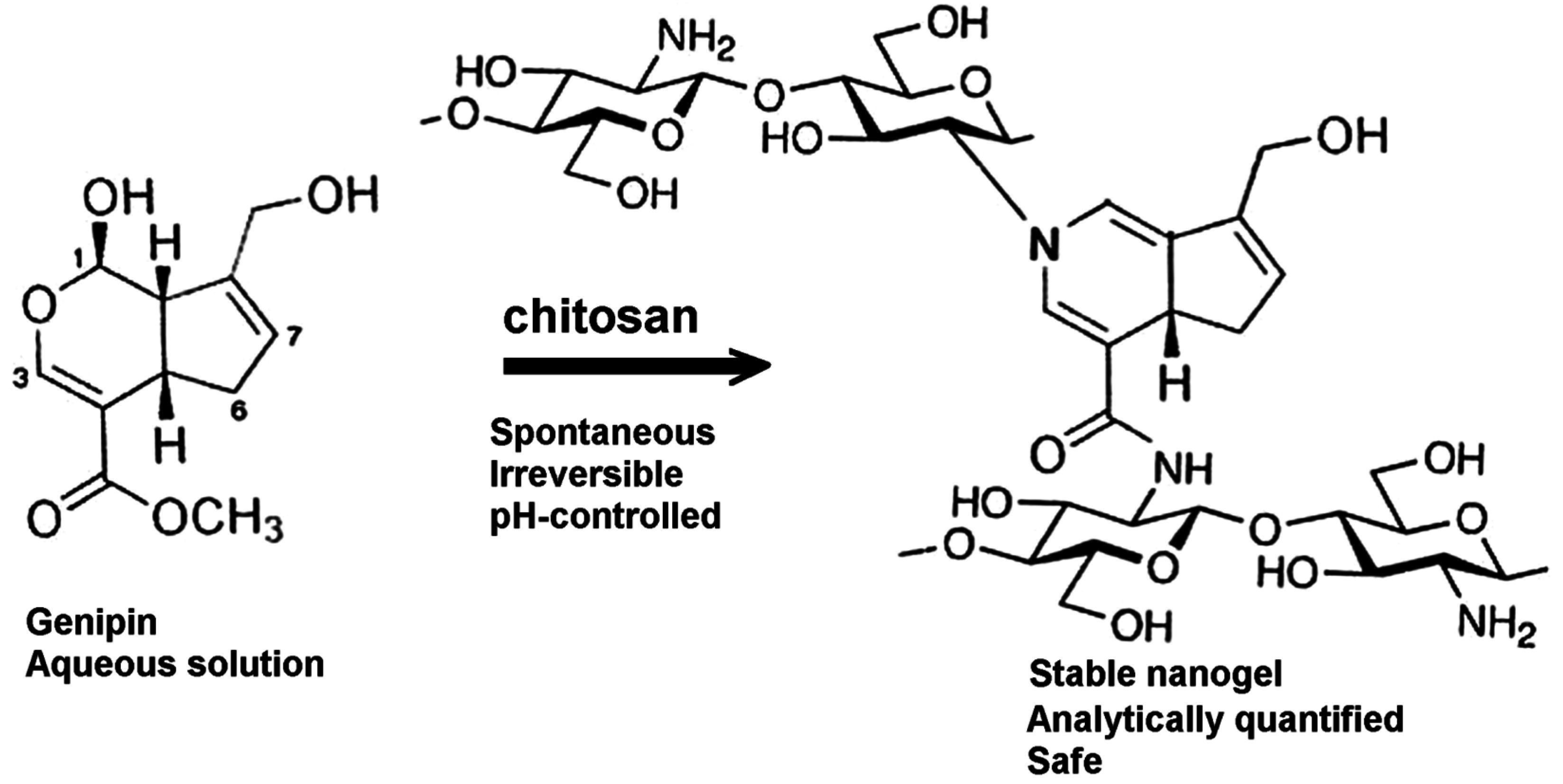

1.4. Scope
2. Therapies Based on the Genipin-Crosslinked Chitosan Alginate Complex
3. Stem Cells in Regenerative Medicine
4. Genipin-Crosslinked Chitosan in Gastric Infections
Further Aspects of Enhanced Antibacterial Efficacy
5. Genipin-Crosslinked Collagen/Gelatin for the Regeneration of the Cartilage
| Genipin Concentration (%, w/w) | Cross-Sectional Area of the Pores (μm2) | Porosity (%) |
|---|---|---|
| 0.0 | 187.9 ± 101.0 | 25.75 ± 1.47 |
| 0.5 | 274.6 ± 123.8 | 33.13 ± 1.30 |
| 1.0 | 533.9 ± 259.8 | 39.95 ± 1.25 |
| 2.0 | 1066.4 ± 396.7 | 44.75 ± 1.50 |

5.1. Fibrin, Poly-l-Lysine, Heparin, Hyaluronan
5.2. Genipin Treatment of Tendon Cells and Matrix
6. Bone Regeneration
6.1. Enhanced Osteogenesis
6.2. Technical Advances, Novel Know-How and Improvements

7. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Muzzarelli, R.A.A. Genipin-crosslinked chitosan hydrogels as biomedical and pharmaceutical aids. Carbohydr. Polym. 2009, 77, 1–9. [Google Scholar] [CrossRef]
- Djerassi, C.; Gray, J.D.; Kinci, F.A. Naturally occurring oxygen heterocycles. IX. Isolation and characterization of genipin. J. Org. Chem. 1960, 25, 2174–2177. [Google Scholar] [CrossRef]
- Djerassi, C.; Nakano, T.; James, A.N.; Zalkow, L.H.; Eisenbraun, E.J.; Shoolery, J.N. Terpenoids. XLVII. The structure of genipin. J. Org. Chem. 1961, 26, 1192–1206. [Google Scholar] [CrossRef]
- Djerassi, C. This man’s Pill: Reflections on the 50th Birthday of the Pill; Oxford University Press: Oxford, UK, 2001. [Google Scholar]
- Zheng, H.Z.; Dong, Z.H.; Yu, J. Modern Research and Application of Chinese Traditional Medicine; Academy Press: Beijing, China, 2000; Volume 4, pp. 3166–3172. [Google Scholar]
- Yu, Y.; Feng, X.L.; Gao, H.; Xie, Z.L.; Dai, Y.; Huang, X.J.; Kurihara, H.; Ye, W.C.; Zhong, Y.; Yao, X.S. Chemical constituents from the fruits of Gardenia jasminoides Ellis. Fitoterapia 2012, 83, 563–567. [Google Scholar] [CrossRef] [PubMed]
- Winotapun, W.; Opanasopit, P.; Ngawhirunpat, T. One enzyme catalyzed simultaneous plant cell disruption and conversion of released glycoside to aglycone combined with in situ product separation as green one-pot production of genipin from Gardenia fruit. Enzym. Microbial Technol. 2013, 53, 92–96. [Google Scholar] [CrossRef] [PubMed]
- Manickam, B.; Sreedharan, R.; Elumalai, M. Genipin the natural water soluble crosslinking agent and its importance in the modified drug delivery systems: An overview. Curr. Drug Deliv. 2014, 11, 139–145. [Google Scholar] [CrossRef] [PubMed]
- Hald, E.S.; Steucke, K.E.; Reeves, J.A.; Win, Z.; Alford, P.W. Long-term vascular contractility assay using genipin-modified muscular thin films. Biofabrication 2014, 6, 045005. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.H.; Cheng, C.Y.; Wang, N.K.; Tan, H.Y.; Tsai, Y.J.; Hsiao, C.H.; Ma, D.H.K.; Yeh, L.K. Characterization of the modified chitosan membrane crosslinked with genipin for the cultured corneal epithelial cells. Colloids Surf. 2015, 126, 237–244. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.K.; Lee, T.C.J.; Sung, H.W. Chemical Modification of Biomedical Materials with Genipin. U.S. Patent 6,608,040, 9 July 2003. [Google Scholar]
- Wu, J.L.; Liao, C.Y.; Wang, Z.; Cheng, W.Z.; Zhou, N.; Wang, S.; Wan, Y. Chitosan-polycaprolactone microspheres as carriers for delivering glial cell line-derived neurotrophic factor. React. Funct. Polym. 2011, 71, 925–932. [Google Scholar] [CrossRef]
- Wu, J.L.; Liao, C.Y.; Zhang, J.; Cheng, W.Z.; Zhou, N.; Wang, S.; Wan, Y. Incorporation of protein-loaded microspheres into chitosan-polycaprolactone scaffolds for controlled release. Carbohydr. Polym. 2011, 86, 1048–1054. [Google Scholar] [CrossRef]
- Yang, Y.M.; Zhao, W.J.; He, J.H.; Zhao, Y.H.; Ding, F.; Gu, X.S. Nerve conduits based on immobilization of nerve growth factor onto modified chitosan by using genipin as a crosslinking agent. Eur. J. Pharm. Biopharm. 2011, 79, 519–525. [Google Scholar] [CrossRef] [PubMed]
- Liu, T.Y.; Lin, Y.L. Novel pH-sensitive chitosan-based hydrogel for encapsulating poorly water-soluble drugs. Acta Biomater. 2010, 6, 1423–1429. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Kim, H.I. Characterization and antibacterial properties of genipin-crosslinked chitosan/poly(ethylene glycol)/ZnO/Ag nanocomposites. Carbohydr. Polym. 2012, 89, 111–116. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.G.; Xie, M.B.; Wang, S.B.; Zheng, Q.Y.; Chen, A.Z.; Deng, Q.J. Facile fabrication of high performances MTX nanocomposites with natural biomembrane bacterial nanoparticles using GP. Mater. Lett. 2013, 100, 248–251. [Google Scholar] [CrossRef]
- Peng, C.; Zhao, S.Q.; Zhang, J.; Huang, G.Y.; Chen, L.Y.; Zhao, F.Y. Chemical composition, antimicrobial property and microencapsulation of mustard (Sinapis alba) seed essential oil by complex coacervation. Food Chem. 2014, 165, 560–568. [Google Scholar] [CrossRef] [PubMed]
- Song, X.; Wu, H.; Li, S.; Wang, Y.; Ma, X.; Tan, M. Ultrasmall chitosan-genipin nanocarriers fabricated from reverse microemulsion process for tumor photothermal therapy in mice. Biomacromolecules 2015, 16, 2080–2090. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.H.; Wu, S.J.; Wu, J.Y.; Wen, D.Y.; Mi, F.L. Preparation of fucoidan-shelled and genipin-crosslinked chitosan beads for antibacterial application. Carbohydr. Polym. 2015, 126, 97–107. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.Y.; Zhao, B.T.; Huang, X.D.; Chen, B.; Qian, H. A substrate fed-batch biphasic catalysis process for the production of natural cross linking agent genipin with Fusarium solani ACCC 36223. J. Microbiol. Biotechnol. 2015, 25, 814–819. [Google Scholar] [CrossRef] [PubMed]
- Bergonzi, M.C.; Righeschi, C.; Isacchi, B.; Bilia, A.R. Identification and quantification of constituents of Gardenia jasminoides Ellis (Zhizi) by HPLC-DAD-ESI-MS. Food Chem. 2012, 134, 1199–1204. [Google Scholar] [CrossRef] [PubMed]
- Cano, E.V.; Echeverri-Lopez, L.F.; Gil-Romero, J.F.; Correa-Garces, E.A.; Zapata-Porras, S.P. Colorant Compounds Derived from Genipin or Genipin Containing Materials. U.S. Patent Application 2014/0350127 A1, 27 November 2014. [Google Scholar]
- Chen, J.; Wu, H.; Xu, G.B.; Dai, M.M.; Hu, S.L.; Sun, L.L.; Wang, W.; Wang, R.; Li, S.P.; Li, G.Q. Determination of geniposide in adjuvant arthritis rat plasma by ultra-high performance liquid chromatography tandem mass spectrometry and its application to oral bioavailability and plasma protein binding. J. Pharm. Biomed. Anal. 2015, 108, 122–128. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.F.; Fu, G.M.; Wan, Y.; Liu, C.M.; Chai, J.X.; Li, H.G.; Wang, J.T.; Zhang, L.N. Enrichment and purification of gardenia yellow from Gardenia jasminoides var radicans Makino by column chromatography. J. Chromatogr. 2012, 893–894, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y.; Sun, Y.; Wang, Y.; Zhang, J.; Xu, B.; Zhang, H.; Song, D. A practical and rapid method for the simultaneous isolation, purification and quantification of geniposide from the fruit of Gardenia jasminoides Ellis by MSPD extraction and UFLC analysis. Anal. Methods 2013, 5, 4112–4118. [Google Scholar] [CrossRef]
- Lee, S.W.; Lim, J.M.; Bhoo, S.H.; Paik, Y.S.; Hahn, T.R. Colorimetric determination of amino acids using genipin from Gardenia jasminoides. Anal. Chim. Acta 2003, 480, 267–274. [Google Scholar] [CrossRef]
- Ramos-de-la-Pena, A.M.; Renard, C.M.G.C.; Wicker, L.; Montanez, J.C.; García-Cerda, L.A.; Contreras-Esquivel, J.C. Environmental friendly cold-mechanical/sonic enzymatic assisted extraction of genipin from genipap (Genipa americana). Ultrason. Sonochem. 2014, 21, 43–49. [Google Scholar] [CrossRef] [PubMed]
- Ramos-de-la-Pena, A.M.; Renard, C.M.G.C.; Montanez, J.C.; Reyes-Vega, M.; Contreras-Esquivel, J.C. A review through recovery, purification and identification of genipin. Phytochem. Rev. 2014. [Google Scholar] [CrossRef]
- Ramos-Ponce, L.M.; Vega, M.; Saldoval-Fabian, G.C.; Colunga-Urbina, E.; Rodriguez-Gonzalez, F.J.; Contreras-Esquivel, J.C. A simple colorimetric determination of the free amino groups in water soluble chitin derivatives using genipin. Food Sci. Biotechnol. 2010, 19, 683–689. [Google Scholar] [CrossRef]
- Reich, M.S.; Akkus, O. Sporicidal efficacy of genipin: A potential theoretical alternative for biomaterial and tissue graft sterilization. Cell Tissue Bank 2013, 14, 381–393. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Zhang, T.; Yu, S.; Ding, Y.; Zhang, L.; Qiu, C.; Jin, D. Transformation of geniposide into genipin by immobilized β-glucosidase in a two-phase aqueous-organic system. Molecules 2011, 16, 4204–4295. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.S.; Xiang, Y.; Cui, Y.L.; Lin, K.M.; Zhang, X.F. Dietary blue pigments derived from genipin, attenuate inflammation by inhibiting LPS-induced iNOS and COX-2 espression via the NF-κB inactivation. PLoS ONE 2012, 7, e34122. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.W.; Horn, G. Genipin-Rich Material and Its Use. WO Patent 2013/070682 A1, 16 May 2013. [Google Scholar]
- Zhang, M.; Ignatova, S.; Hu, P.; Liang, Q.; Wang, Y.; Sutherland, I.; Jun, F.W.; Luo, G. Cost-efficient and process-efficient separation of geniposide from Gardenia jasminoides Ellis by high performance counter-current chromatography. Sep. Purif. Technol. 2012, 89, 193–198. [Google Scholar] [CrossRef]
- Zhou, M.; Zhuo, J.; Wei, W.; Zhu, J.; Ling, X. Simple and effective large-scale preparation of geniposide from fruit of Gardenia jasminoides Ellis using a liquid-liquid two-phase extraction. Fitoterapia 2012, 83, 1558–1561. [Google Scholar] [CrossRef] [PubMed]
- Zhou, T.; Liu, H.; Wen, J.; Fan, G.; Chai, Y.; Wu, Y. Fragmentation study of iridoid glycosides including epimers by liquid chromatography-diode array detection/electrospray ionization mass spectrometry and its application in metabolic fingerprint analysis of Gardenia jasminoides Ellis. Rapid Commun. Mass Spectrom. 2010, 24, 2520–2528. [Google Scholar] [CrossRef] [PubMed]
- Chiono, V.; Pulieri, E.; Vozzi, G.; Ciardelli, G.; Ahluwalia, A.; Giusti, P. Genipin-crosslinked chitosan/gelatin blends for biomedical applications. J. Mater. Sci. Mater. Med. 2008, 19, 889–898. [Google Scholar] [CrossRef] [PubMed]
- Croisier, F.; Jerome, C. Chitosan based biomaterials for tissue engineering. Eur. Polym. J. 2013, 49, 780–792. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A. Chitin; Pergamon Press: Oxford, UK, 1977. [Google Scholar]
- Muzzarelli, R.A.A.; Muzzarelli, C. Chitosan chemistry: Relevance to the biomedical sciences. In Advances in Polymer Science; Heinze, T., Ed.; Springer Verlag: Berlin, Germany, 2005; pp. 151–209. [Google Scholar]
- Muzzarelli, R.A.A. Chitins and chitosans for the repair of wounded skin, nerve, cartilage and bone. Carbohydr. Polym. 2009, 76, 167–182. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A. Chitins and chitosans as immunoadjuvants and non-allergenic drug carriers. Mar. Drugs 2010, 8, 292–312. [Google Scholar] [CrossRef] [PubMed]
- Muzzarelli, R.A.A. Chitin nanostructures in living organisms. In Chitin Formation and Diagenesis; Springer: Dordrecht, The Netherlands, 2011; Volume 34, pp. 1–34. [Google Scholar]
- Muzzarelli, R.A.A. Chemical and technological advances in chitins and chitosans useful for the formulation of biopharmaceuticals. In Chitosan-Based Systems for Biopharmaceuticals; Sarmento, B., DasNeves, J., Eds.; Wiley: New York, NY, USA, 2012; pp. 3–22. [Google Scholar]
- Muzzarelli, R.A.A. Nanochitins and nanochitosans, paving the way to eco-friendly and energy-saving exploitation of marine resources. In Polymer Science: A Comprehensive Reference; Elsevier: Amsterdam, The Netherlands, 2012; Volume 10, pp. 153–164. [Google Scholar]
- Muzzarelli, R.A.A.; Baldassarre, V.; Conti, F.; Gazzanelli, G.; Vasi, V.; Ferrara, P.; Biagini, G. The biological activity of chitosan: An ultrastructural study. Biomaterials 1988, 9, 247–252. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A.; Boudrant, J.; Meyer, D.; Manno, N.; DeMarchis, M.; Paoletti, M.G. A tribute to Henri Braconnot, precursor of the carbohydrate polymers science, on the chitin bicentennial. Carbohydr. Polym. 2012, 87, 995–1012. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A.; El Mehtedi, M.; Mattioli-Belmonte, M. Emerging biomedical applications of nano-chitins and nano-chitosans obtained via advanced eco-friendly technologies from marine resources. Mar. Drugs 2014, 12, 5468–5502. [Google Scholar] [CrossRef] [PubMed]
- Ravi Kumar, M.N.V.; Muzzarelli, R.A.A.; Muzzarelli, C.; Sashiwa, H.; Domb, A.J. Chitosan chemistry and pharmaceutical perspectives. Chem. Rev. 2004, 104, 6017–6084. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.N.; Yang, Y.; Guo, T.Y. Genipin-crosslinked hydrophobical chitosan microspheres and their interactions with bovine serum albumin. Carbohydr. Polym. 2011, 83, 2016–2021. [Google Scholar] [CrossRef]
- Maggi, F.; Ciccarelli, S.; Diociaiuti, M.; Casciardi, S.; Masci, G. Chitosan nanogels by template chemical crosslinking in polyion complex micelle nanoreactors. Biomacromolecules 2011, 12, 3499–3507. [Google Scholar] [CrossRef] [PubMed]
- Pujana, M.A.; Perez-Alvarez, L.; Iturbe, L.C.C.; Katime, I. Biodegradable chitosan nanogels crosslinked with genipin. Carbohydr. Polym. 2013, 94, 836–842. [Google Scholar] [CrossRef] [PubMed]
- Muzzarelli, R.A.A.; Ilari, P.; Xia, W.; Pinotti, M.; Tomasetti, M. Tyrosinase mediated quinone tanning of chitinous materials. Carbohydr. Polym. 1994, 24, 294–300. [Google Scholar] [CrossRef]
- Yao, C.K.; Liao, J.D.; Chung, C.W.; Sung, W.I.; Chang, N.J. Porous chitosan scaffold crosslinked by chemical and natural procedure applied to investigate cell regeneration. Appl. Surf. Sci. 2012, 262, 218–221. [Google Scholar] [CrossRef]
- Bao, D.S.; Chen, M.J.; Wang, H.Y.; Wang, J.F.; Liu, C.F.; Sun, R.C. Preparation and characterization of double crosslinked hydrogel films from carboxymethylchitosan and carboxymethylcellulose. Carbohydr. Polym. 2014, 110, 113–120. [Google Scholar] [CrossRef] [PubMed]
- Gao, L.; Gan, H.; Meng, Z.Y.; Gu, R.L.; Wu, Z.N.; Zhang, L.; Zhu, X.X.; Sun, W.Z.; Li, J.; Zheng, Y.; et al. Effects of genipin crosslinking of chitosan hydrogels on cellular adhesion and viability. Colloids Surf. 2014, 117, 398–405. [Google Scholar] [CrossRef] [PubMed]
- Song, W.L.; Oliveira, M.B.; Sher, P.; Gil, S.; Noobrega, J.M.; Mano, J.F. Bioinspired methodology for preparing magnetic responsive chitosan beads to be integrated in a tubular bioreactor for biomedical applications. Biomed. Mater. 2013, 8, 045008. [Google Scholar] [CrossRef] [PubMed]
- Nayak, S.; Dey, S.; Kundu, S.C. Silk sericin-alginate-chitosan microcapsules: Hepatocytes encapsulation for enhanced cellular functions. Int. J. Biol. Macromol. 2014, 65, 258–266. [Google Scholar] [CrossRef] [PubMed]
- Aldana, A.A.; Gonzalez, A.; Strumia, M.C.; Martinelli, M. Preparation and characterization of chitosan/genipin/poly(N-vinyl-2-pyrrolidone) films for controlled release of drugs. Mater. Chem. Phys. 2012, 134, 317–324. [Google Scholar] [CrossRef]
- Glampedaki, P.; Jocic, D.; Warmoeskerken, M.M.C.G. Moisture absorption capacity of polyamide 6,6 fabrics surface functionalised by chitosan-based hydrogel finishes. Prog. Org. Coat. 2011, 72, 562–571. [Google Scholar] [CrossRef]
- Colosi, C.; Costantini, M.; Latini, R.; Ciccarelli, S.; Stampella, A.; Barbetta, A.; Massimi, M.; Devirgiliis, L.C.; Dentini, M. Rapid prototyping of chitosan-coated alginate scaffolds through the use of a 3D fiber deposition technique. J. Mater. Chem. 2014, 2, 6779–6791. [Google Scholar] [CrossRef]
- Silva, J.M.; Duarte, A.R.C.; Caridade, S.G.; Picart, C.; Reis, R.L.; Mano, J.F. Tailored freestanding multi layered membranes based on chitosan and alginate. Biomacromolecules 2014, 15, 3817–3826. [Google Scholar] [CrossRef] [PubMed]
- Silva, J.M.; Duarte, A.R.C.; Custodio, C.A.; Sher, P.; Neto, A.I.; Pinho, A.C.M.; Fonseca, J.; Reis, R.L.; Mano, J.F. Nanostructured hollow tubes based on chitosan and alginate multilayers. Adv. Healthc. Mater. 2014, 3, 433–440. [Google Scholar] [CrossRef] [PubMed]
- Ranganath, S.H.; Tan, A.L.; He, F.; Wang, C.H.; Krantz, W.B. Control and enhancement of permselectivity of membrane-based microcapsules for favorable biomolecular transport and immunoisolation. AIChE J. 2011, 57, 3052–3062. [Google Scholar] [CrossRef]
- Zhang, Z.J.; Zhang, H.; Kang, Y.; Sheng, P.Y.; Ma, Y.C.; Yang, Z.B.; Zhang, Z.Q.; Fu, M.; He, A.S.; Liao, W.M. miRNA expression profile during osteogenic differentiation of human adipose-derived stem cells. J. Cell. Biochem. 2012, 113, 888–898. [Google Scholar] [CrossRef] [PubMed]
- Busilacchi, A.; Gigante, A.; Mattioli-Belmonte, M.; Muzzarelli, R.A.A. Chitosan stabilizes platelet growth factors and modulates stem cell differentiation toward tissue regeneration. Carbohydr. Polym. 2013, 98, 665–676. [Google Scholar] [CrossRef] [PubMed]
- Debnath, T.; Ghosh, S.; Potlapuvu, U.S.; Kona, L.; Kamaraju, S.R.; Sarkar, S.; Gaddam, S.; Chelluri, L.K. Proliferation and differentiation potential of human adipose-derived stem cells grown on chitosan hydrogel. PLoS ONE 2015, 10, e0120803. [Google Scholar] [CrossRef] [PubMed]
- Paul, A.; Chen, G.Y.; Khan, A.; Rao, V.T.S.; Shum-Tim, D.; Prakash, S. Genipin-crosslinked microencapsulated human adipose stem cells augment transplant retention resulting in attenuation of chronically infarcted rat heart fibrosis and cardiac dysfunction. Cell Transplant. 2012, 21, 2735–2751. [Google Scholar] [CrossRef] [PubMed]
- Cheng, N.C.; Estes, B.T.; Young, T.H.; Guilak, F. Engineered cartilage using primary chondrocytes cultured in a porous cartilage-derived matrix. Regen. Med. 2011, 6, 81–93. [Google Scholar] [CrossRef] [PubMed]
- Cheng, N.C.; Estes, B.T.; Young, T.H.; Guilak, F. Genipin-crosslinked cartilage-derived matrix as a scaffold for human adipose-derived stem cell chondrogenesis. Tissue Eng. 2013, 19, 484–496. [Google Scholar] [CrossRef] [PubMed]
- Nogueira, F.; Goncalves, I.C.; Martins, M.C.L. Effect of gastric environment on Helicobacter pylori adhesion to a mucoadhesive polymer. Acta Biomater. 2013, 9, 5208–5215. [Google Scholar] [CrossRef] [PubMed]
- Delmar, K.; Bianco-Peled, H. The dramatic effect of small pH changes on the properties of chitosan hydrogels crosslinked with genipin. Carbohydr. Polym. 2015, 127, 28–37. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.H.; Tsai, S.C.; Lai, C.H.; Lee, C.H.; He, Z.S.; Tseng, G.C. Genipin-crosslinked fucose-chitosan/heparin nanoparticles for the eradication of Helicobacter pylori. Biomaterials 2013, 34, 4466–4479. [Google Scholar] [CrossRef] [PubMed]
- Thakur, A.; Wanchoo, R.K.; Hardeep; Soni, S.K. Chitosan hydrogel beads: A comparative study with glutaraldehyde, epichlorohydrin and genipin as crosslinkers. J. Polym. Mater. 2014, 31, 211–223. [Google Scholar]
- Wang, R.; Neoh, K.G.; Kang, E.T. Integration of antifouling and bactericidal moieties for optimizing the efficacy of antibacterial coatings. J. Colloid Interface Sci. 2015, 438, 138–148. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.K.; Strandman, S.; Zhu, J.X.X.; Barralet, J.; Cerruti, M. Genipin-crosslinked catechol-chitosan mucoadhesive hydrogels for buccal drug delivery. Biomaterials 2015, 37, 395–404. [Google Scholar] [CrossRef] [PubMed]
- Elzoghby, A.O. Gelatin-based nanoparticles as drug and gene delivery systems: Reviewing three decades of research. J. Control. Release 2013, 172, 1075–1091. [Google Scholar] [CrossRef] [PubMed]
- Muzzarelli, R.A.A.; Greco, F.; Busilacchi, A.; Sollazzo, V.; Gigante, A. Chitosan, hyaluronan and chondroitin sulfate in tissue engineering for cartilage regeneration: A review. Carbohydr. Polym. 2012, 89, 723–739. [Google Scholar] [CrossRef] [PubMed]
- Bottegoni, C.; Muzzarelli, R.A.A.; Busilacchi, A.; Giovannini, F.; Gigante, A. Oral chondroprotection with nutraceuticals made of chondroitin sulphate plus glucosamine sulphate in osteoarthritis. Carbohydr. Polym. 2014, 109, 126–138. [Google Scholar] [CrossRef] [PubMed]
- Bi, L.; Cao, Z.; Hu, Y.Y.; Song, Y.; Yu, L.; Yang, B.; Mu, J.H.; Huang, Z.S.; Han, Y.S. Effects of different crosslinking conditions on the properties of genipin-crosslinked chitosan/collagen scaffolds for cartilage tissue engineering. J. Mater. Sci. Mater. Med. 2011, 22, 51–62. [Google Scholar] [CrossRef] [PubMed]
- Yan, L.P.; Wang, Y.J.; Ren, L.; Wu, G.; Caridade, S.G.; Fan, J.B.; Wang, L.Y.; Ji, P.H.; Oliveira, J.M.; Oliveira, J.T.; et al. Genipin-crosslinked collagen/chitosan biomimetic scaffolds for articular cartilage tissue engineering applications. J. Biomed. Mater. Res. 2010, 95, 465–475. [Google Scholar] [CrossRef] [PubMed]
- Kuo, Y.C.; Wang, C.C. Effect of bovine pituitary extract on the formation of neocartilage in chitosan/gelatin scaffolds. J. Taiwan Inst. Chem. Eng. 2010, 41, 150–156. [Google Scholar] [CrossRef]
- Yin, D.K.; Wu, H.; Liu, C.X.; Zhang, J.; Zhou, T.; Wu, J.J.; Wan, Y. Fabrication of composition-graded collagen/chitosan-polylactide scaffolds with gradient architecture and properties. React. Funct. Polym. 2014, 83, 98–106. [Google Scholar] [CrossRef]
- Fernandes-Silva, S.; Moreira-Silva, J.; Silva, T.H.; Perez-Martin, R.; Sotelo, C.G.; Mano, J.F.; Duarte, A.R.C.; Reis, R.L. Porous hydrogels from shark skin collagen crosslinked under dense carbon dioxide atmosphere. Macromol. Biosci. 2013, 13, 1621–1631. [Google Scholar] [CrossRef] [PubMed]
- Wang, P.Y.; Tsai, W.B. Modulation of the proliferation and matrix synthesis of chondrocytes by dynamic compression on genipin-crosslinked chitosan/collagen scaffolds. J. Biomater. Sci. Polym. Ed. 2013, 24, 507–519. [Google Scholar] [CrossRef] [PubMed]
- Kawadkar, J.; Jain, R.; Kishore, R.; Pathak, A.; Chauhan, M.K. Formulation and evaluation of flurbiprofen-loaded genipin crosslinked gelatin microspheres for intra-articular delivery. J. Drug Target. 2013, 21, 200–210. [Google Scholar] [CrossRef] [PubMed]
- Kawadkar, J.; Chauhan, M.K. Intra-articular delivery of genipin crosslinked chitosan microspheres of flurbiprofen: Preparation, characterization, in vitro and in vivo studies. Eur. J. Pharm. Biopharm. 2012, 81, 563–572. [Google Scholar] [CrossRef] [PubMed]
- Sarem, M.; Moztarzadeh, F.; Mozafari, M. How can genipin assist gelatin/carbohydrate chitosan scaffolds to act as replacements of load-bearing soft tissues. Carbohydr. Polym. 2013, 93, 635–643. [Google Scholar] [CrossRef] [PubMed]
- Gorczyca, G.; Tylingo, R.; Szweda, P.; Augustina, E.; Sadowska, M.; Milewski, S. Preparation and characterization of genipin crosslinked porous chitosan-collagen-gelatin scaffolds using chitosan-CO2 solution. Carbohydr. Polym. 2014, 102, 901–911. [Google Scholar] [CrossRef] [PubMed]
- Gamboa-Martinez, T.C.; Cruz, D.M.G.; Carda, C.; Ribelles, J.L.G.; Ferrer, G.G. Fibrin-chitosan composite substrate for in vitro culture of chondrocytes. J. Biomed. Mater. Res. 2013, 101, 404–412. [Google Scholar] [CrossRef] [PubMed]
- Nihn, C.; Iftikhar, A.; Cramer, M.; Bettinger, C.J. Diffusion-reaction models of genipin incorporation into fibrin networks. J. Mater. Chem. B 2015, 3, 4607–4615. [Google Scholar]
- Mekhail, M.; Jahan, K.; Tabrizian, M. Genipin-crosslinked chitosan/poly-l-lysine gels promote fibroblast adhesion and proliferation. Carbohydr. Polym. 2014, 108, 91–98. [Google Scholar] [CrossRef] [PubMed]
- Mathew, A.P.; Oksman, K.; Pierron, D.; Harmand, M.F. Biocompatible fibrous networks of cellulose nanofibres and collagen crosslinked using genipin: Potential as artificial ligament/tendons. Macromol. Biosci. 2013, 13, 289–298. [Google Scholar] [CrossRef] [PubMed]
- Norowski, P.A.; Mishra, S.; Adatrow, P.C.; Haggard, W.O.; Bumgardner, J.D. Suture pullout strength and in vitro fibroblast and RAW 264.7 monocyte biocompatibility of genipin crosslinked nanofibrous chitosan mats for guided tissue regeneration. J. Biomed. Mater. Res. 2012, 100, 2890–2896. [Google Scholar] [CrossRef] [PubMed]
- Tseng, H.J.; Tsou, T.L.; Wang, H.J.; Hsu, S.H. Characterization of chitosan-gelatin scaffolds for dermal tissue engineering. J. Tissue Eng. Regen. Med. 2013, 7, 20–31. [Google Scholar] [CrossRef] [PubMed]
- Skop, N.B.; Calderon, F.; Levison, S.W.; Gandhi, C.D.; Cho, C.H. Heparin crosslinked chitosan microspheres for the delivery of neural stem cells and growth factors for central nervous system repair. Acta Biomater. 2013, 9, 6834–6843. [Google Scholar] [CrossRef] [PubMed]
- Hezaveh, H.; Muhamad, I.I. Controlled drug release via minimization of burst release in pH-response κ-carrageenan/polyvinyl alcohol hydrogels. Chem. Eng. Res. Des. 2013, 91, 508–519. [Google Scholar] [CrossRef]
- Kaihara, S.; Suzuki, Y.; Fujimoto, K. In situ synthesis of polysaccharide nanoparticles via polyion complex of carboxymethyl cellulose and chitosan. Colloids Surf. 2011, 85, 343–348. [Google Scholar] [CrossRef] [PubMed]
- Jalani, G.; Rosenzweig, D.H.; Makhoul, G.; Abdalla, S.; Cecere, R.; Vetrone, F.; Haglund, L.; Cerruti, M. Tough, in situ thermogelling, injectable hydrogels for biomedical applications. Macromol. Biosci. 2015, 15, 473–480. [Google Scholar] [CrossRef] [PubMed]
- Nath, S.D.; Abueva, C.; Kim, B.; Lee, B.T. Chitosan-hyaluronic acid polyelectrolyte complex scaffold crosslinked with genipin for immobilization and controlled release of BMP-2. Carbohydr. Polym. 2015, 115, 160–169. [Google Scholar] [CrossRef] [PubMed]
- Fessel, G.; Cadby, J.; Wunderli, S.; van Weeren, R.; Snedeker, J.G. Dose- and time-dependent effects of genipin crosslinking on cell viability and tissue mechanics: Toward clinical application for tendon repair. Acta Biomater. 2014, 10, 1897–1906. [Google Scholar] [CrossRef] [PubMed]
- Muzzarelli, R.A.A.; Mattioli-Belmonte, M.; Tietz, C.; Biagini, R.; Ferioli, G.; Brunelli, M.A. Stimulatory effect on bone formation exerted by a modified chitosan. Biomaterials 1994, 15, 1075–1081. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A. Chitosan scaffolds for bone regeneration. In Chitin, Chitosan and Their Derivatives: Biological Activities and Applications; Kim, S.K., Ed.; CRC Taylor & Francis: Boca Raton, FL, USA, 2010. [Google Scholar]
- Muzzarelli, R.A.A. Chitosan composites with inorganics, morphogenetic proteins and stem cells, for bone regeneration. Carbohydr. Polym. 2011, 83, 1433–1445. [Google Scholar] [CrossRef]
- Wu, F.; Meng, G.L.; He, J.; Wu, Y.; Wu, F.; Gu, Z.W. Antibiotic-loaded chitosan hydrogel with superior dual functions: Antibacterial efficacy and osteoblastic cell responses. ACS Appl. Mater. Interfaces 2014, 6, 10005–10013. [Google Scholar] [CrossRef] [PubMed]
- Mattioli-Belmonte, M.; Biagini, G.; Muzzarelli, R.A.A.; Castaldini, C.; Gandolfi, M.G.; Krajewski, A.; Ravaglioli, A.; Fini, M.; Giardino, R. Osteoinduction in the presence of chitosan-coated porous hydroxyapatite. J. Bioact. Compat. Polym. 1995, 10, 249–257. [Google Scholar]
- Wang, G.C.; Qiu, J.C.; Zheng, L.; Ren, N.; Li, J.H.; Liu, H.; Miao, J.Y. Sustained delivery of BMP-2 enhanced osteoblastic differentiation of BMSCs based on surface hydroxyapatite nanostructure in chitosan-HAp scaffold. J. Biomater. Sci. Polym. Ed. 2014, 25, 1813–1827. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.C.; Zheng, L.; Zhao, H.S.; Miao, J.Y.; Sun, C.H.; Ren, N.; Wang, J.Y.; Liu, H.; Tao, X.T. In vitro assessment of the differentiation potential of bone marrow-derived mesenchymal stem cells on genipin-chitosan conjugation scaffold with surface hydroxyapatite nanostructure for bone tissue engineering. Tissue Eng. 2011, 17, 1341–1349. [Google Scholar] [CrossRef] [PubMed]
- Li, X.Y.; Nan, K.H.; Shi, S.; Chen, H. Preparation and characterization of nano-hydroxyapatite/chitosan crosslinking composite membrane intended for tissue engineering. Int. J. Biol. Macromol. 2012, 50, 43–49. [Google Scholar] [CrossRef] [PubMed]
- Liu, I.H.; Chang, S.H.; Lin, H.Y. Chitosan-based hydrogel tissue scaffolds made by 3D plotting promotes osteoblast proliferation and mineralization. Biomed. Mater. 2015, 10, 035004. [Google Scholar] [CrossRef] [PubMed]
- Schiffman, J.D.; Schauer, C.L. A review: Electrospinning of biopolymer nanofibers and their applications. Polym. Rev. 2008, 48, 317–352. [Google Scholar] [CrossRef]
- Li, Q.; Wang, X.; Lou, X.; Yuan, H.; Tu, H.; Li, B.; Zhang, Y. Genipin-crosslinked electrospun chitosan nanofibers: Determination of crosslinking conditions and evaluation of cytocompatibility. Carbohydr. Polym. 2015, 130, 166–174. [Google Scholar] [CrossRef] [PubMed]
- Lelkes, P.I.; Frohbergh, M. Electrospun Mineralized Chitosan Nanofibers Crosslinked with Genipin for Bone Tissue Engineering. U.S. Patent Application 2013/0274892, 17 October 2013. [Google Scholar]
- Frohbergh, M.E.; Katsman, A.; Mondrinos, M.J.; Stabler, C.T.; Hankenson, K.D.; Oristaglio, J.T.; Lelkes, P.I. Osseointegrative properties of electrospun hydroxyapatite-containing nanofibrous chitosan scaffolds. Tissue Eng. 2015, 21, 970–981. [Google Scholar] [CrossRef] [PubMed]
- Frohbergh, M.E.; Katsman, A.; Botta, G.R.; Lazarovici, P.; Schauer, C.L.; Wegst, U.G.K.; Lelkes, P.I. Electrospun hydroxyapatite-containing chitosan nanofibers crosslinked with genipin for bone tissue engineering. Biomaterials 2012, 33, 9167–9178. [Google Scholar] [CrossRef] [PubMed]
- Pu, X.M.; Wei, K.; Zhang, Q.Q. In situ forming chitosan/hydroxyapatite rods reinforced via genipin crosslinking. Mater. Lett. 2013, 94, 169–171. [Google Scholar] [CrossRef]
- Pandit, V.; Zuidema, J.M.; Venuto, K.N.; Macione, J.; Dai, G.H.; Gilbert, R.J.; Kotha, S.P. Evaluation of multifunctional polysaccharide hydrogels with varying stiffness for bone tissue engineering. Tissue Eng. 2013, 19, 2452–2463. [Google Scholar] [CrossRef] [PubMed]
- Ge, S.H.; Zhao, N.; Wang, L.; Yu, M.J.; Liu, H.; Song, A.M.; Huang, J.; Wang, G.C.; Yang, P.S. Bone repair by periodontal ligament stem cell-seeded nanohydroxyapatite-chitosan scaffold. Int. J. Nanomed. 2012, 7, 5405–5414. [Google Scholar] [CrossRef] [PubMed]
- Nwosu, C.J.; Hurst, G.A.; Novakovic, K. Genipin crosslinked chitosan-polyvinylpyrrolidone hydrogels: Influence of composition and postsynthesis treatment on pH responsive behavior. Adv. Mater. Sci. Eng. 2015, 10, 621289. [Google Scholar] [CrossRef]
- Yao, Q.Q.; Li, W.; Yu, S.S.; Ma, L.W.; Jin, D.Y.; Boccaccini, A.R.; Liu, Y. Multifunctional chitosan/polyvinyl pyrrolidone/45S5 Bioglass® scaffolds for MC3T3-E1 cell stimulation and drug. Mater. Sci. Eng. 2015, 56, 473–480. [Google Scholar] [CrossRef] [PubMed]
- Austero, M.S.; Donius, A.E.; Wegst, U.G.K.; Schauer, C.L. New crosslinkers for electrospun chitosan fibre mats. I. Chemical analysis. J. R. Soc. Interface 2012, 9, 2551–2562. [Google Scholar] [CrossRef] [PubMed]
- Donius, A.E.; Kiechel, M.A.; Schauer, C.L.; Wegst, U.G.K. New crosslinkers for electrospun chitosan fibre mats. Part II. Mechanical properties. J. R. Soc. Interface 2012, 10, 20120946. [Google Scholar] [CrossRef] [PubMed]
- Kiechel, M.A.; Beringer, L.T.; Donius, A.E.; Komiya, Y.; Habas, R.; Wegst, U.G.K.; Schauer, C.L. Osteoblast biocompatibility of premineralized, hexamethylene-1,6-diaminocarboxysulfonate crosslinked chitosan fibers. J. Biomed. Mater. Res. 2015, 103, 3201–3211. [Google Scholar] [CrossRef] [PubMed]
- Su, W.T.; Wang, Y.T.; Chou, C.M. Optimal fluid flow enhanced mineralization of MG-63 cells in porous chitosan scaffold. J. Taiwan Inst. Chem. Eng. 2014, 45, 1111–1118. [Google Scholar] [CrossRef]
- Radisic, M.; Marsano, A.; Maidhof, R.; Wang, Y.; Vunjak-Novakovic, G. Cardiac tissue engineering using perfusion bioreactor system. Nat. Protoc. 2008, 3, 719–738. [Google Scholar] [CrossRef] [PubMed]
- Ichinohe, N.; Takamoto, T.; Tabata, Y. Proliferation, osteogenic differentiation, and distribution of rat bone marrow stromal cells in nonwoven fabrics by different culture methods. Tissue Eng. 2008, 14, 107–116. [Google Scholar] [CrossRef]
- Siddiqui, N.; Pramanik, K.; Jabbari, E. Osteogenic differentiation of human mesenchymal stem cells in freeze-gelled chitosan/nano beta-tricalcium phosphate porous scaffolds crosslinked with genipin. Mater. Sci. Eng. 2015, 54, 76–83. [Google Scholar] [CrossRef] [PubMed]
- Norowski, P.A.; Fujiwara, T.; Clem, W.C.; Adatrow, P.C.; Eckstein, E.C.; Haggard, W.O.; Bumgardner, J.D. Novel naturally crosslinked electrospun nanofibrous chitosan mats for guided bone regeneration membranes: Material characterization and cytocompatibility. J. Tissue Eng. Regen. Med. 2015, 9, 577–583. [Google Scholar] [CrossRef] [PubMed]
- Bavariya, A.J.; Norowski, A.; Anderson, K.M.; Adatrow, P.C.; Garcia-Godoy, F.; Stein, S.H.; Bumgardner, J.D. Evaluation of biocompatibility and degradation of chitosan nanofiber membrane crosslinked with genipin. J. Biomed. Mater. Res. 2014, 102, 1084–1092. [Google Scholar] [CrossRef] [PubMed]
- Du, M.C.; Zhu, Y.M.; Yuan, L.H.; Liang, H.; Mou, C.C.; Li, X.R.; Sun, J.; Zhuang, Y.; Zhang, W.; Shi, Q.; et al. Assembled 3D cell niches in chitosan hydrogel network to mimic extracellular matrix. Colloids Surf. 2013, 434, 78–87. [Google Scholar] [CrossRef]
- Dimida, S.; Demitri, C.; De Benedictis, V.M.; Scalera, F.; Gervaso, F.; Sannino, A. Genipin-cross-linked chitosan-based hydrogels: Reaction kinetics and structure-related characteristics. J. Appl. Polym. Sci. 2015, 132. [Google Scholar] [CrossRef]
- Reves, B.T.; Bumgardner, J.D.; Haggard, W.O. Fabrication of crosslinked carboxymethylchitosan microspheres and their incorporation into composite scaffolds for enhanced bone regeneration. J. Biomed. Mater. Res. 2013, 101, 630–639. [Google Scholar] [CrossRef] [PubMed]
- Gaudiere, F.; Morin-Grognet, S.; Bidault, L.; Lembre, P.; Pauthe, E.; Vannier, J.P.; Atmani, H.; Ladam, G.; Labat, B. Genipin-crosslinked layer-by-layer assemblies: Biocompatible microenvironments to direct bone cell fate. Biomacromolecules 2014, 15, 1602–1611. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.J.; Yang, S.R.; Chu, I.M.; Brey, E.M.; Hsiao, H.Y.; Cheng, M.H. A comparative study of the chondrogenic potential between synthetic and natural scaffolds in an in vivo bioreactor. Sci. Technol. Adv. Mater. 2013, 14, 054403. [Google Scholar] [CrossRef]
- Jayakumar, R.; Chennazhi, K.P.; Muzzarelli, R.A.A.; Tamura, H.; Nair, S.V.; Selvamurugan, N. Chitosan conjugated DNA nanoparticles in gene therapy. Carbohydr. Polym. 2010, 79, 1–8. [Google Scholar] [CrossRef]
- Muzzarelli, R.A.A. Biomedical exploitation of chitin and chitosan via mechano-chemical disassembly, electrospinning, dissolution in imidazolium ionic liquids, and supercritical drying. Mar. Drugs 2011, 9, 1510–1533. [Google Scholar] [CrossRef] [PubMed]
- Muzzarelli, R.A.A. New techniques for optimization of surface area and porosity in nanochitins and nanochitosans. In Advances in Polymer Science: Chitosan for Biomaterials; Jayakumar, R., Prabaharan, A., Muzzarelli, R.A.A., Eds.; Springer Verlag: Berlin, Germany, 2011; Volume 2, pp. 167–186. [Google Scholar]
- Hurst, G.A.; Novakovic, K. A facile in situ morphological characterization of smart genipin-crosslinked chitosan-poly(vinyl pyrrolidone) hydrogels. J. Mater. Res. 2013, 28, 2401–2408. [Google Scholar] [CrossRef]
- Moura, M.J.; Martins, S.P.; Duarte, B.P.M. Production of chitosan microparticles cross-linked with genipin: Identification of factors influencing size and shape properties. Biochem. Eng. J. 2015, 104, 82–90. [Google Scholar] [CrossRef]
- Mi, F.L.; Tan, Y.C.; Liang, H.C.; Huang, R.N.; Sung, H.W. In vitro evaluation of a chitosan membrane cross-linked with genipin. J. Biomater. Sci. Polym. Ed. 2001, 12, 835–850. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.C.; Wu, Y.C.; Mi, F.L.; Lin, Y.H.; Yu, L.C.; Sung, H.W. A novel pH-sensitive hydrogel composed of N,O-carboxymethyl chitosan and alginate cross-linked by genipin for protein drug delivery. J. Control. Release 2004, 96, 285–300. [Google Scholar] [CrossRef] [PubMed]
- Butler, M.F.; Ng, Y.F.; Pudney, P.D.A. Mechanism and kinetics of the crosslinking reaction between biopolymers containing primary amine groups and genipin. J. Polym. Sci. 2003, 41, 3941–3953. [Google Scholar] [CrossRef]
- Mi, F.L.; Sung, H.W.; Shyu, S.S. Synthesis and characterization of a novel chitosan-based network prepared using naturally occurring crosslinker. J. Polym. Sci. Polym. Chem. 2000, 38, 2804–2814. [Google Scholar] [CrossRef]
- Mi, F.L.; Sung, H.W.; Shyu, S.S. Drug release from chitosan-alginate complex beads reinforced by a naturally occurring cross-linking agent. Carbohydr. Polym. 2002, 48, 61–72. [Google Scholar] [CrossRef]
- Mi, F.L.; Tan, Y.C.; Liang, H.F.; Sung, H.W. In vivo biocompatibility and degradability of novel injectable chitosan-based implant. Biomaterials 2002, 23, 181–191. [Google Scholar] [CrossRef]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Muzzarelli, R.A.A.; El Mehtedi, M.; Bottegoni, C.; Aquili, A.; Gigante, A. Genipin-Crosslinked Chitosan Gels and Scaffolds for Tissue Engineering and Regeneration of Cartilage and Bone. Mar. Drugs 2015, 13, 7314-7338. https://doi.org/10.3390/md13127068
Muzzarelli RAA, El Mehtedi M, Bottegoni C, Aquili A, Gigante A. Genipin-Crosslinked Chitosan Gels and Scaffolds for Tissue Engineering and Regeneration of Cartilage and Bone. Marine Drugs. 2015; 13(12):7314-7338. https://doi.org/10.3390/md13127068
Chicago/Turabian StyleMuzzarelli, Riccardo A. A., Mohamad El Mehtedi, Carlo Bottegoni, Alberto Aquili, and Antonio Gigante. 2015. "Genipin-Crosslinked Chitosan Gels and Scaffolds for Tissue Engineering and Regeneration of Cartilage and Bone" Marine Drugs 13, no. 12: 7314-7338. https://doi.org/10.3390/md13127068
APA StyleMuzzarelli, R. A. A., El Mehtedi, M., Bottegoni, C., Aquili, A., & Gigante, A. (2015). Genipin-Crosslinked Chitosan Gels and Scaffolds for Tissue Engineering and Regeneration of Cartilage and Bone. Marine Drugs, 13(12), 7314-7338. https://doi.org/10.3390/md13127068






