Psychological and Social Aspects of Vaccination Hesitancy—Implications for Travel Medicine in the Aftermath of the COVID-19 Crisis: A Narrative Review
Abstract
1. The Content of Vaccine Hesitancy
2. The Effect of the Pandemic
3. Aims—Methods
4. Theoretical Context
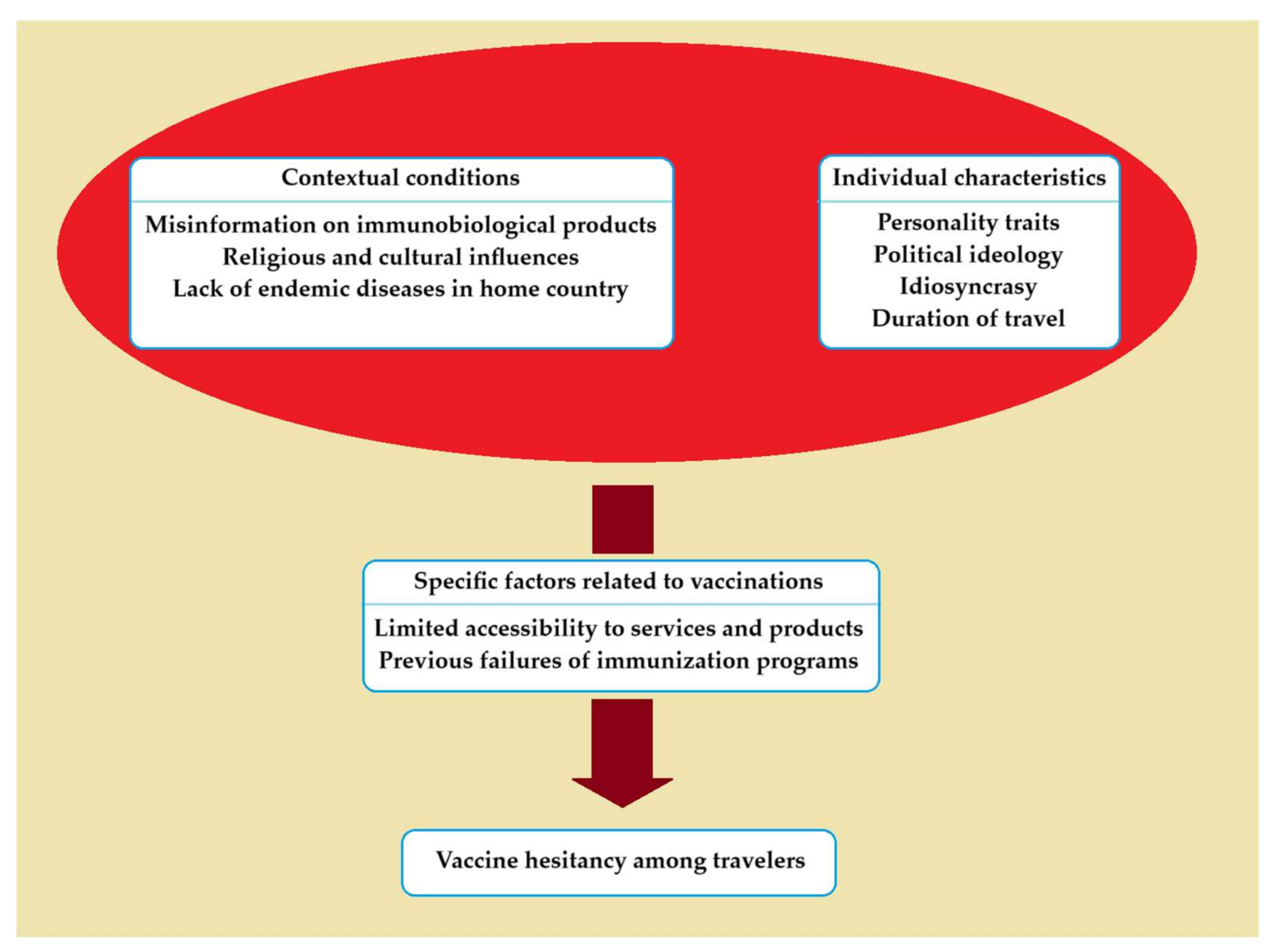
5. Vaccine Hesitancy among Travelers
6. Implications in Clinical Practice
7. Limitations/Caveats
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
References
- Lane, S.; MacDonald, N.E.; Marti, M.; Dumolard, L. Vaccine hesitancy around the globe: Analysis of three years of WHO/UNICEF joint reporting form data-2015–2017. Vaccine 2018, 36, 3861–3867. [Google Scholar] [CrossRef]
- Larson, H.J.; Jarrett, C.; Eckersberger, E.; Smith, D.M.; Paterson, P. Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: A systematic review of published literature, 2007–2012. Vaccine 2014, 32, 2150–2159. [Google Scholar] [CrossRef] [PubMed]
- Broadbent, J.J. Vaccine hesitancy: Misinformation on social media. BMJ 2019, 366, l4457. [Google Scholar] [CrossRef]
- Yaqub, O.; Castle-Clarke, S.; Sevdalis, N.; Chataway, J. Attitudes to vaccination: A critical review. Soc. Sci. Med. 2014, 112, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Tafuri, S.; Gallone, M.S.; Cappelli, M.G.; Martinelli, D.; Prato, R.; Germinario, C. Addressing the anti-vaccination movement and the role of HCWs. Vaccine 2014, 32, 4860–4865. [Google Scholar] [CrossRef] [PubMed]
- Piccirilli, G.; Lazzarotto, T.; Chiereghin, A.; Serra, L.; Gabrielli, L.; Lanari, M. Spotlight on measles in Italy: Why outbreaks of a vaccine-preventable infection continue in the 21st century. Expert. Rev. Anti Infect. Ther. 2015, 13, 355–362. [Google Scholar] [CrossRef] [PubMed]
- Phadke, V.K.; Bednarczyk, R.A.; Salmon, D.A.; Omer, S.B. Association Between Vaccine Refusal and Vaccine-Preventable Diseases in the United States: A Review of Measles and Pertussis. JAMA 2016, 315, 1149–1158. [Google Scholar] [CrossRef]
- Kubin, L. Is There a Resurgence of Vaccine Preventable Diseases in the U.S.? J. Pediatr. Nurs. 2019, 44, 115–118. [Google Scholar] [CrossRef]
- McGovern, M.E.; Canning, D. Vaccination and All-Cause Child Mortality From 1985 to 2011: Global Evidence from the Demographic and Health Surveys. Am. J. Epidemiol. 2015, 182, 791–798. [Google Scholar] [CrossRef]
- Kempe, A.; Daley, M.F.; McCauley, M.M.; Crane, L.A.; Suh, C.A.; Kennedy, A.M.; Basket, M.M.; Stokley, S.K.; Dong, F.; Babbel, C.I.; et al. Prevalence of Parental Concerns About Childhood Vaccines: The Experience of Primary Care Physicians. Am. J. Prev. Med. 2011, 40, 548–555. [Google Scholar] [CrossRef]
- Leib, S.; Liberatos, P.; Edwards, K. Pediatricians’ Experience with and Response to Parental Vaccine Safety Concerns and Vaccine Refusals: A Survey of Connecticut Pediatricians. Public Health Rep. 2011, 126 (Suppl. 2), 13–23. [Google Scholar] [CrossRef] [PubMed]
- Lo, N.C.; Hotez, P.J. Public Health and Economic Consequences of Vaccine Hesitancy for Measles in the United States. JAMA Pediatr. 2017, 171, 887–892. [Google Scholar] [CrossRef] [PubMed]
- Milionis, C. Provision of healthcare in the context of financial crisis: Approaches to the Greek health system and international implications. Nurs. Philos. 2013, 14, 17–27. [Google Scholar] [CrossRef]
- Nicoli, F.; Appay, V. Immunological considerations regarding parental concerns on pediatric immunizations. Vaccine 2017, 35, 3012–3019. [Google Scholar] [CrossRef]
- Szilagyi, P.G.; Albertin, C.; Gurfinkel, D.; Saville, A.W.; Vangala, S.; Rice, J.; Helmkamp, L.; Zimet, G.D.; Valderrama, R.; Breck, A.; et al. Prevalence and Characteristics of HPV Vaccine Hesitancy Among Parents of Adolescents Across the US. Vaccine 2020, 38, 6027–6037. [Google Scholar] [CrossRef]
- Sestili, C.; Grazina, I.; La Torre, G. HBV vaccine and risk of developing multiple sclerosis: A systematic review and meta-analysis. Hum. Vaccin. Immunother. 2021, 17, 2273–2278. [Google Scholar] [CrossRef]
- Gabis, L.V.; Attia, O.L.; Goldman, M.; Barak, N.; Tefera, P.; Shefer, S.; Shaham, M.; Lerman-Sagie, T. The myth of vaccination and autism spectrum. Eur. J. Paediatr. Neurol. 2022, 36, 151–158. [Google Scholar] [CrossRef]
- Gross, K.; Hartmann, K.; Zemp, E.; Merten, S. ‘I know it has worked for millions of years’: The role of the ‘natural’ in parental reasoning against child immunization in a qualitative study in Switzerland. BMC Public Health 2015, 15, 373. [Google Scholar] [CrossRef][Green Version]
- Dubé, E.; Vivion, M.; Sauvageau, C.; Gagneur, A.; Gagnon, R.; Guay, M. “Nature Does Things Well, Why Should We Interfere?”: Vaccine Hesitancy Among Mothers. Qual. Health Res. 2016, 26, 411–425. [Google Scholar] [CrossRef] [PubMed]
- Ward, P.R.; Attwell, K.; Meyer, S.B.; Rokkas, P.; Leask, J. Understanding the perceived logic of care by vaccine-hesitant and vaccine-refusing parents: A qualitative study in Australia. PLoS ONE 2017, 12, e0185955. [Google Scholar] [CrossRef] [PubMed]
- Goldenberg, M.J. Public Misunderstanding of Science? Reframing the Problem of Vaccine Hesitancy. Perspect. Sci. 2016, 24, 552–581. [Google Scholar] [CrossRef]
- Jacobson, R.M.; St Sauver, J.L.; Griffin, J.M.; MacLaughlin, K.L.; Finney Rutten, L.J. How health care providers should address vaccine hesitancy in the clinical setting: Evidence for presumptive language in making a strong recommendation. Hum. Vaccin. Immunother. 2020, 16, 2131–2135. [Google Scholar] [CrossRef] [PubMed]
- Wheeler, M.; Buttenheim, A.M. Parental vaccine concerns, information source, and choice of alternative immunization schedules. Hum. Vaccin. Immunother. 2013, 9, 1782–1789. [Google Scholar] [CrossRef]
- Hulsey, E.; Bland, T. Immune overload: Parental attitudes toward combination and single antigen vaccines. Vaccine 2015, 33, 2546–2550. [Google Scholar] [CrossRef] [PubMed]
- Reich, J.A. Neoliberal Mothering and Vaccine Refusal: Imagined Gated Communities and the Privilege of Choice. Gend. Soc. 2014, 28, 679–704. [Google Scholar] [CrossRef]
- Kirbiš, A. The Impact of Socioeconomic Status, Perceived Threat and Healthism on Vaccine Hesitancy. Sustainability 2023, 15, 6107. [Google Scholar] [CrossRef]
- Peretti-Watel, P.; Raude, J.; Sagaon-Teyssier, L.; Constant, A.; Verger, P.; Beck, F. Attitudes toward vaccination and the H1N1 vaccine: Poor people’s unfounded fears or legitimate concerns of the elite? Soc. Sci. Med. 2014, 109, 10–18. [Google Scholar] [CrossRef] [PubMed]
- Ali, K.A.; Celentano, L.P. Addressing Vaccine Hesitancy in the ‘Post-Truth’ Era. Eurohealth 2017, 23, 16–20. [Google Scholar]
- Thomson, A.; Robinson, K.; Vallée-Tourangeau, G. The 5As: A practical taxonomy for the determinants of vaccine uptake. Vaccine 2016, 34, 1018–1024. [Google Scholar] [CrossRef] [PubMed]
- Sallam, M. COVID-19 Vaccine Hesitancy Worldwide: A Concise Systematic Review of Vaccine Acceptance Rates. Vaccines 2021, 9, 160. [Google Scholar] [CrossRef]
- Lun, P.; Gao, J.; Tang, B.; Yu, C.C.; Jabbar, K.A.; Low, J.A.; George, P.P. A social ecological approach to identify the barriers and facilitators to COVID-19 vaccination acceptance: A scoping review. PLoS ONE 2022, 17, e0272642. [Google Scholar] [CrossRef]
- Majid, U.; Ahmad, M.; Zain, S.; Akande, A.; Ikhlaq, F. COVID-19 vaccine hesitancy and acceptance: A comprehensive scoping review of global literature. Health Promot. Int. 2022, 37, daac078. [Google Scholar] [CrossRef] [PubMed]
- Troiano, G.; Nardi, A. Vaccine hesitancy in the era of COVID-19. Public Health 2021, 194, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Lazarus, J.V.; Wyka, K.; White, T.M.; Picchio, C.A.; Gostin, L.O.; Larson, H.J.; Rabin, K.; Ratzan, S.C.; Kamarulzaman, A.; El-Mohandes, A. A survey of COVID-19 vaccine acceptance across 23 countries in 2022. Nat. Med. 2023, 29, 366–375. [Google Scholar] [CrossRef] [PubMed]
- Han, X.; Xu, P.; Ye, Q. Analysis of COVID-19 vaccines: Types, thoughts, and application. J. Clin. Lab. Anal. 2021, 35, e23937. [Google Scholar] [CrossRef] [PubMed]
- Leong, C.; Jin, L.; Kim, D.; Kim, J.; Teo, Y.Y.; Ho, T.H. Assessing the impact of novelty and conformity on hesitancy towards COVID-19 vaccines using mRNA technology. Commun. Med. 2022, 2, 61. [Google Scholar] [CrossRef]
- Salerno, L.; Craxì, L.; Amodio, E.; Lo Coco, G. Factors Affecting Hesitancy to mRNA and Viral Vector COVID-19 Vaccines among College Students in Italy. Vaccines 2021, 9, 927. [Google Scholar] [CrossRef] [PubMed]
- Temsah, M.H.; Barry, M.; Aljamaan, F.; Alhuzaimi, A.; Al-Eyadhy, A.; Saddik, B.; Alrabiaah, A.; Alsohime, F.; Alhaboob, A.; Alhasan, K.; et al. Adenovirus and RNA-based COVID-19 vaccines’ perceptions and acceptance among healthcare workers in Saudi Arabia: A national survey. BMJ Open 2021, 11, e048586. [Google Scholar] [CrossRef] [PubMed]
- Ngai, C.S.B.; Singh, R.G.; Yao, L. Impact of COVID-19 Vaccine Misinformation on Social Media Virality: Content Analysis of Message Themes and Writing Strategies. J. Med. Internet Res. 2022, 24, e37806. [Google Scholar] [CrossRef] [PubMed]
- Islam, M.S.; Kamal, A.M.; Kabir, A.; Southern, D.L.; Khan, S.H.; Hasan, S.M.M.; Sarkar, T.; Sharmin, S.; Das, S.; Roy, T.; et al. COVID-19 vaccine rumors and conspiracy theories: The need for cognitive inoculation against misinformation to improve vaccine adherence. PLoS ONE 2021, 16, e0251605. [Google Scholar] [CrossRef]
- Ferrari, R. Writing narrative style literature reviews. Med. Writ. 2015, 24, 230–235. [Google Scholar] [CrossRef]
- Furley, P.; Goldschmied, N. Systematic vs. Narrative Reviews in Sport and Exercise Psychology: Is Either Approach Superior to the Other? Front. Psychol. 2021, 12, 685082. [Google Scholar] [CrossRef] [PubMed]
- Dubé, E.; Laberge, C.; Guay, M.; Bramadat, P.; Roy, R.; Bettinger, J. Vaccine hesitancy: An overview. Hum. Vaccin. Immunother. 2013, 9, 1763–1773. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, N.E.; The SAGE Working Group on Vaccine Hesitancy. Vaccine hesitancy: Definition, scope and determinants. Vaccine 2015, 33, 4161–4164. [Google Scholar] [CrossRef]
- McClure, C.C.; Cataldi, J.R.; O’Leary, S.T. Vaccine hesitancy: Where We Are and Where We Are Going. Clin. Ther. 2017, 39, 1550–1562. [Google Scholar] [CrossRef]
- Leask, J.; Kinnersley, P.; Jackson, C.; Cheater, F.; Bedford, H.; Rowles, G. Communicating with parents about vaccination: A framework for health professionals. BMC Pediatr. 2012, 12, 154. [Google Scholar] [CrossRef] [PubMed]
- Chen, R.T.; Rastogi, S.C.; Mullen, J.R.; Hayes, S.W.; Cochi, S.L.; Donlon, J.A.; Wassilak, S.G. The vaccine adverse event reporting system (VAERS). Vaccine 1994, 12, 542–550. [Google Scholar] [CrossRef]
- Janko, M. Vaccination: A Victim of Its Own Success. Virtual Mentor. 2012, 14, 3–4. [Google Scholar] [CrossRef]
- Bednarczyk, R.A. Examining the “Why” of Vaccine Hesitancy. Health Psychol. 2018, 37, 316–317. [Google Scholar] [CrossRef]
- Nyhan, B.; Reifler, J. Does correcting myths about the flu vaccine work? An experimental evaluation of the effects of corrective information. Vaccine 2015, 33, 459–464. [Google Scholar] [CrossRef]
- Nyhan, B.; Reifler, J.; Richey, S.; Freed, G.L. Effective Messages in Vaccine Promotion: A Randomized Trial. Pediatrics 2014, 133, e835–e842. [Google Scholar] [CrossRef] [PubMed]
- Attwell, K.; Smith, D.T. Parenting as politics: Social identity theory and vaccine hesitant communities. Int. J. Health Gov. 2017, 22, 183–198. [Google Scholar] [CrossRef]
- Attwell, K.; Meyer, S.B.; Ward, P.R. The Social Basis of Vaccine Questioning and Refusal: A Qualitative Study Employing Bourdieu’s Concepts of ‘Capitals’ and ‘Habitus’. Int. J. Environ. Res. Public. Health 2018, 15, 1044. [Google Scholar] [CrossRef] [PubMed]
- Sobo, E. Theorizing (Vaccine) Refusal: Through the Looking Glass. Cult. Anthropol. 2016, 31, 342–350. [Google Scholar] [CrossRef]
- Hornsey, M.J.; Harris, E.A.; Fielding, K.S. The psychological roots of anti-vaccination attitudes: A 24-nation investigation. Health Psychol. 2018, 37, 307–315. [Google Scholar] [CrossRef] [PubMed]
- Taddio, A.; MacDonald, N. Addressing vaccine hesitancy in travellers: The CARDTM system. J. Travel Med. 2019, 26, taz056. [Google Scholar] [CrossRef] [PubMed]
- Nicolaï, H.; Verhasselt, Y. Health and tropical geography. Belgeo 2000, 1-2-3-4, 103–114. [Google Scholar] [CrossRef][Green Version]
- Zhu, O.Y.; Grün, B.; Dolnicar, S. Tourism and vaccine hesitancy. Ann. Tour. Res. 2022, 92, 103320. [Google Scholar] [CrossRef] [PubMed]
- Adongo, C.A.; Amenumey, E.K.; Kumi-Kyereme, A.; Dubé, E. Beyond fragmentary: A proposed measure for travel vaccination concerns. Tour. Manag. 2021, 83, 104180. [Google Scholar] [CrossRef]
- Lopes, V.D.S.; Souza, P.C.; Garcia, É.M.; Lima, J.C. Yellow fever vaccine hesitancy and its relationship with contextual, individual, or group influences and vaccine-specific issues: A scoping review. Cien. Saude Colet. 2023, 28, 1717–1727. [Google Scholar] [CrossRef]
- World Tourism Organization (UNWTO). International tourism recovered 63% of pre-pandemic levels in 2022, with Europe and Middle East in the lead. World Tour. Barom. 2023, 21, 1–40. [Google Scholar] [CrossRef]
- Kitro, A.; Ngamprasertchai, T.; Srithanaviboonchai, K. Infectious diseases and predominant travel-related syndromes among long-term expatriates living in low-and middle- income countries: A scoping review. Trop. Dis. Travel Med. Vaccines 2022, 8, 11. [Google Scholar] [CrossRef] [PubMed]
- Rapose, A. Travel to Tropical Countries: A Review of Travel-Related Infectious Diseases. Trop. Med. Surg. 2013, 1, 1000128. [Google Scholar] [CrossRef]
- Toovey, S.; Moerman, F.; van Gompel, A. Special Infectious Disease Risks of Expatriates and Long-Term Travelers in Tropical Countries. Part II: Infections Other Than Malaria. J. Travel Med. 2007, 14, 50–60. [Google Scholar] [CrossRef]
- Roupa, Z.; Noula, M.; Farazi, E.; Stylianides, A.; Papaneophytou, C. Vaccination Coverage and Awareness of Hepatitis B Virus Among Healthcare Students at a University in Cyprus. Mater. Sociomed. 2019, 31, 190–196. [Google Scholar] [CrossRef]
- Roupa, Z.; Zikos, D.; Vasilopoulos, A.; Diomidous, M. Common health risks, required precautions of travelers and their customs towards the use of travel medicine services. Mater. Sociomed. 2012, 24, 131–134. [Google Scholar] [CrossRef] [PubMed]
- Wilson, M.E. Travel and the emergence of infectious diseases. Emerg. Infect. Dis. 1995, 1, 39–46. [Google Scholar] [CrossRef] [PubMed]
- Virk, A. Medical Advice for International Travelers. Mayo Clin. Proc. 2001, 76, 831–840. [Google Scholar] [CrossRef]
- Crockett, M.; Keystone, J. “I Hate Needles” and Other Factors Impacting on Travel Vaccine Uptake. J. Travel Med. 2005, 12 (Suppl. 1), S41–S46. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Weinstein, M.C. Should physicians be gatekeepers of medical resources? J. Med. Ethics 2001, 27, 268–274. [Google Scholar] [CrossRef]
- Relman, A.S. Cost Control, Doctors’ Ethics, And Patient Care. Issues Sci. Technol. 1985, 1, 103–111. [Google Scholar]
- Hussain, A.; Ali, S.; Ahmed, M.; Hussain, S. The Anti-vaccination Movement: A Regression in Modern Medicine. Cureus 2018, 10, e2919. [Google Scholar] [CrossRef]
- Bauer, I.L. Travel vaccination examined through the tourism lens. J. Travel Med. 2021, 28, taab142. [Google Scholar] [CrossRef]
- Dubé, E.; Vivion, M.; MacDonald, N.E. Vaccine hesitancy, vaccine refusal and the anti-vaccine movement: Influence, impact and implications. Expert. Rev. Vaccines 2015, 14, 99–117. [Google Scholar] [CrossRef] [PubMed]
- Fatima, K.; Syed, N.I. Dengvaxia controversy: Impact on vaccine hesitancy. J. Glob. Health 2018, 8, 010312. [Google Scholar] [CrossRef] [PubMed]
- Machingaidze, S.; Wiysonge, C.S. Understanding covid-19 vaccine hesitancy. Nat. Med. 2021, 27, 1338–1339. [Google Scholar] [CrossRef]
- Jacobson, R.M.; St Sauver, J.L.; Finney Rutten, L.J. Vaccine Hesitancy. Mayo Clin. Proc. 2015, 90, 1562–1568. [Google Scholar] [CrossRef] [PubMed]
- Rief, W. Fear of Adverse Effects and COVID-19 Vaccine Hesitancy: Recommendations of the Treatment Expectation Expert Group. JAMA Health Forum 2021, 2, e210804. [Google Scholar] [CrossRef]
- De Figueiredo, A.; Simas, C.; Karafillakis, E.; Paterson, P.; Larson, H.J. Mapping global trends in vaccine confidence and investigating barriers to vaccine uptake: A large-scale retrospective temporal modelling study. Lancet 2020, 396, 898–908. [Google Scholar] [CrossRef]
- McGuinness, S.L.; Eades, O.; Seale, H.; Cheng, A.C.; Leder, K. Pre-travel vaccine information needs, attitudes, drivers of uptake and the role for decision aids in travel medicine. J. Travel Med. 2023, 30, taad056. [Google Scholar] [CrossRef]
- Gautret, P.; Botelho-Nevers, E.; Brouqui, P.; Parola, P. The spread of vaccine-preventable diseases by international travellers: A public-health concern. Clin. Microbiol. Infect. 2012, 18 (Suppl. 5), 77–84. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kumar, D.; Chandra, R.; Mathur, M.; Samdariya, S.; Kapoor, N. Vaccine hesitancy: Understanding better to address better. Isr. J. Health Policy Res. 2016, 5, 2. [Google Scholar] [CrossRef] [PubMed]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Milionis, C.; Ilias, I.; Tselebis, A.; Pachi, A. Psychological and Social Aspects of Vaccination Hesitancy—Implications for Travel Medicine in the Aftermath of the COVID-19 Crisis: A Narrative Review. Medicina 2023, 59, 1744. https://doi.org/10.3390/medicina59101744
Milionis C, Ilias I, Tselebis A, Pachi A. Psychological and Social Aspects of Vaccination Hesitancy—Implications for Travel Medicine in the Aftermath of the COVID-19 Crisis: A Narrative Review. Medicina. 2023; 59(10):1744. https://doi.org/10.3390/medicina59101744
Chicago/Turabian StyleMilionis, Charalampos, Ioannis Ilias, Athanasios Tselebis, and Argyro Pachi. 2023. "Psychological and Social Aspects of Vaccination Hesitancy—Implications for Travel Medicine in the Aftermath of the COVID-19 Crisis: A Narrative Review" Medicina 59, no. 10: 1744. https://doi.org/10.3390/medicina59101744
APA StyleMilionis, C., Ilias, I., Tselebis, A., & Pachi, A. (2023). Psychological and Social Aspects of Vaccination Hesitancy—Implications for Travel Medicine in the Aftermath of the COVID-19 Crisis: A Narrative Review. Medicina, 59(10), 1744. https://doi.org/10.3390/medicina59101744









