Combination of Specific Vascular Lasers and Vascular Intense Pulsed Light Improves Facial Telangiectasias and Redness
Abstract
:1. Introduction
2. Materials and Methods
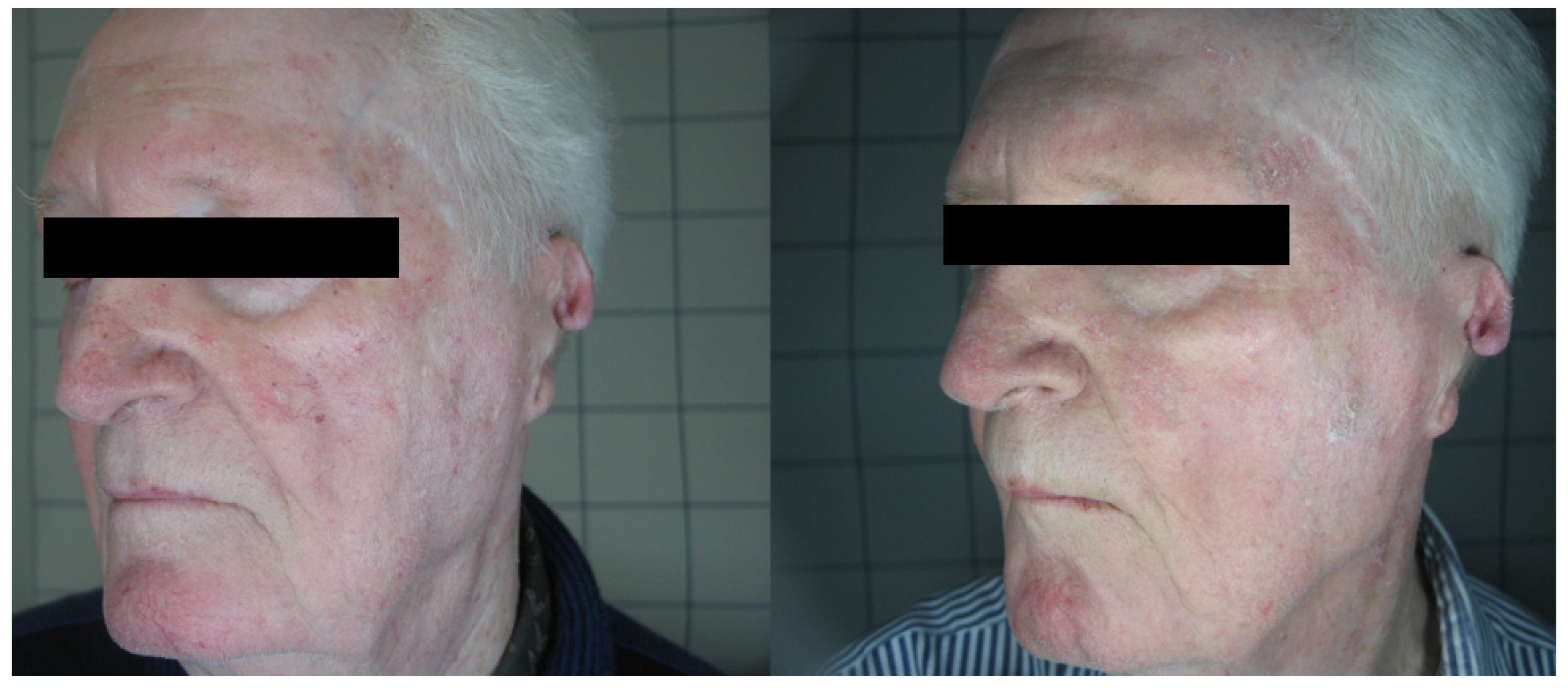
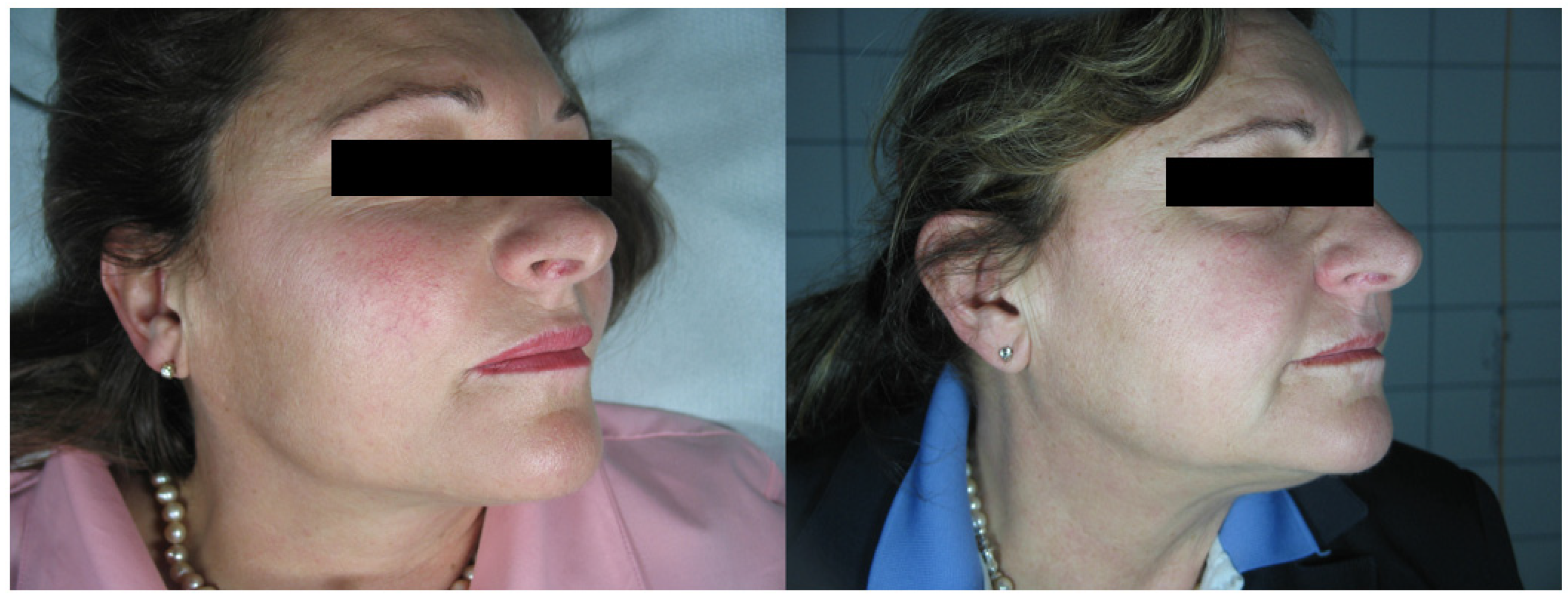
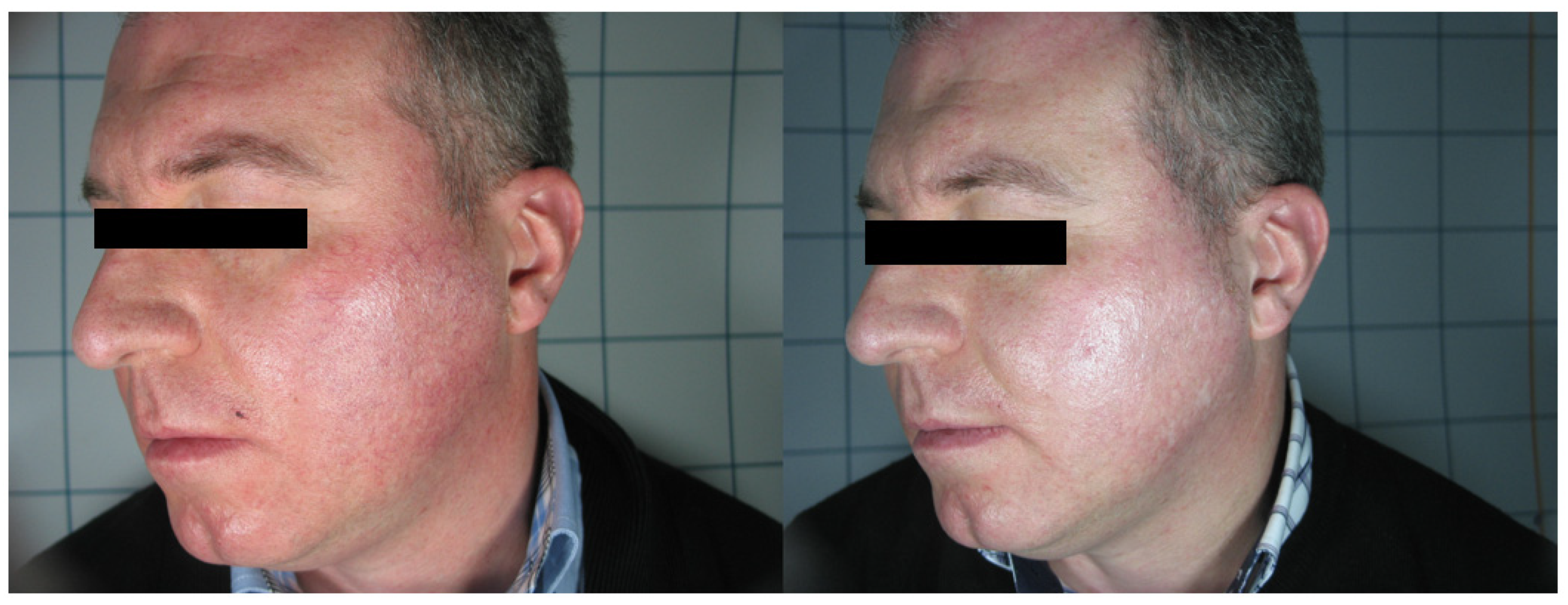
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Mekić, S.; Hamer, M.; Wigmann, C.; Gunn, D.; Kayser, M.; Jacobs, L.; Schikowski, T.; Nijsten, T.; Pardo, L. Epidemiology and determinants of facial telangiectasia: A cross-sectional study. J. Eur. Acad. Dermatol. Venereol. 2020, 34, 821–826. [Google Scholar] [CrossRef] [PubMed]
- Two, A.M.; Wu, W.; Gallo, R.L.; Hata, T.R. Rosacea. J. Am. Acad. Dermatol. 2015, 72, 749–758. [Google Scholar] [CrossRef] [PubMed]
- Katoulis, A.C.; Stavrianeas, N.G.; Georgala, S.; Bozi, E.; Kalogeromitros, D.; Koumantaki, E.; Katsambas, A.D. Poikiloderma of Civatte: A clinical and epidemiological study. J. Eur. Acad. Dermatol. Venereol. 2005, 19, 444–448. [Google Scholar] [CrossRef] [PubMed]
- Vissing, A.-C.E.; Dierickx, C.; Karmisholt, K.E.; Haedersdal, M. Topical brimonidine reduces IPL-induced erythema without affecting efficacy: A randomized controlled trial in patients with facial telangiectasias. Lasers Surg. Med. 2018, 50, 1002–1009. [Google Scholar] [CrossRef] [PubMed]
- Ross, E.V.; Smirnov, M.; Pankratov, M.; Altshuler, G. Intense Pulsed Light and Laser Treatment of Facial Telangiectasias and Dyspigmentation: Some Theoretical and Practical Comparisons. Dermatol. Surg. 2006, 31, 1188–1198. [Google Scholar] [CrossRef] [PubMed]
- McGregor, S.; Miceli, A.; Krishnamurthy, K. Treatment of Facial Telangiectases With Glycerin Sclerotherapy. Dermatol. Surg. 2019, 45, 950–953. [Google Scholar] [CrossRef]
- Yap, F.H.X.; Kumarasinghe, S.P. Brimonidine for treatment of telangiectasia of dermatomyositis. Australas J. Dermatol. 2017, 59, e220–e221. [Google Scholar] [CrossRef]
- Netto, B.A.S.D.M.; Beiriz, Y.D.R.; Bonatto, A.C.; Maciel, G.S.B.; de Almeida, L.R.; Corassa, J.M. Uso de tartarato de brimonidina para resolução de matting telangiectásico: Relato de caso. J. Vasc. Bras. 2020, 19, e20190159. [Google Scholar] [CrossRef]
- McCoppin, H.H.H.; Goldberg, D.J. Laser Treatment of Facial Telangiectases: An Update. Dermatol. Surg. 2010, 36, 1221–1230. [Google Scholar] [CrossRef]
- Ammirati, C.T.; Carniol, P.J.; Hruza, G.J. Laser Treatment of Facial Vascular Lesions. Facial Plast. Surg. 2001, 17, 193–202. [Google Scholar] [CrossRef]
- Ianosi, G.; Ianosi, S.; Calbureanu-Popescu, M.X.; Tutunaru, C.; Calina, D.; Neagoe, D. Comparative study in leg telangiectasias treatment with Nd:YAG laser and sclerotherapy. Exp. Ther. Med. 2018, 17, 1106–1112. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kim, B.Y.; Moon, H.-R.; Ryu, H.J. Comparative efficacy of short-pulsed intense pulsed light and pulsed dye laser to treat rosacea. J. Cosmet. Laser Ther. 2018, 21, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Deng, Q.; Zhang, S.-P.; Deng, Y.-X.; Liu, F.-F.; Shi, W.; Xie, H.-F.; Xiao, Y.; Huang, Y.-X.; Li, J. Willingness-to-Pay and Benefit–Cost Analysis of IPL for Rosacea Treatment: A Cross-Sectional Study in China. Patient Prefer. Adherence 2020, 14, 1843–1852. [Google Scholar] [CrossRef]
- Nistico, S.P.; Silvestri, M.; Zingoni, T.; Tamburi, F.; Bennardo, L.; Cannarozzo, G. Combination of Fractional CO2 Laser and Rhodamine-Intense Pulsed Light in Facial Rejuvenation: A Randomized Controlled Trial. Photobiomodul. Photomed. Laser Surg. 2021, 39, 113–117. [Google Scholar] [CrossRef] [PubMed]
- Goldman, M.P.; Weiss, R.A.; Brody, H.J.; Coleman, W.P.; Fitzpatrick, R.E. Treatment of Facial Telangiectasia with Sclerotherapy, Laser Surgery, and/or Electrodesiccation: A Review. J. Dermatol. Surg. Oncol. 1993, 19, 899–906. [Google Scholar] [CrossRef]
- Kassir, R.; Kolluru, A.; Kassir, M. Intense pulsed light for the treatment of Rosacea and Telangiectasias. J. Cosmet. Laser Ther. 2011, 13, 216–222. [Google Scholar] [CrossRef]
- Goldberg, D.J. Laser removal of pigmented and vascular lesions. J. Cosmet. Dermatol. 2006, 5, 204–209. [Google Scholar] [CrossRef] [PubMed]
- Goldman, A.; Wollina, U. Komplikationen nach Laserbehandlung vaskulärer Veränderungen des Gesichts. Der Hautarzt 2021, 72, 421–425. [Google Scholar] [CrossRef]
- Coats, J.G.; Maktabi, B.; Abou-Dahech, M.S.; Baki, G. Blue Light Protection, Part I—Effects of blue light on the skin. J. Cosmet. Dermatol. 2020, 20, 714–717. [Google Scholar] [CrossRef]
- Garza, Z.C.F.; Born, M.; Hilbers, P.A.J.; Riel, N.A.W.V.; Liebmann, J. Visible Blue Light Therapy: Molecular Mechanisms and Therapeutic Opportunities. Curr. Med. Chem. 2019, 25, 5564–5577. [Google Scholar] [CrossRef]
- Prohaska, J.; Hohman, M.H. Laser Complications. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2021. [Google Scholar]
- Cannarozzo, G.; Silvestri, M.; Tamburi, F.; Sicilia, C.; Del Duca, E.; Scali, E.; Bennardo, L.; Nisticò, S.P. A new 675-nm laser device in the treatment of acne scars: An observational study. Lasers Med. Sci. 2020, 36, 227–231. [Google Scholar] [CrossRef] [PubMed]
- Nisticò, S.P.; Tolone, M.; Zingoni, T.; Tamburi, F.; Scali, E.; Bennardo, L.; Cannarozzo, G. A New 675 nm Laser Device in the Treatment of Melasma: Results of a Prospective Observational Study. Photobiomodul. Photomed. Laser Surg. 2020, 38, 560–564. [Google Scholar] [CrossRef] [PubMed]
- Bjerring, P.; Christiansen, K.; Troilius, A. Intense pulsed light source for treatment of facial telangiectasias. J. Cutan. Laser Ther. 2001, 3, 169–173. [Google Scholar] [CrossRef] [PubMed]
- Gao, L.; Qu, H.; Gao, N.; Li, K.; Dang, E.; Tan, W.; Wang, G. A retrospective analysis for facial telangiectasia treatment using pulsed dye laser and intense pulsed light configured with different wavelength bands. J. Cosmet. Dermatol. 2019, 19, 88–92. [Google Scholar] [CrossRef]
- Williams, N.M.; Rajabi-Estarabadi, A.; Aigen, A.R. Use of Intense Pulsed Light Versus Pulsed-Dye Laser in the Treatment of Truncal Telangiectasia. Dermatol. Surg. 2020, 47, 862–863. [Google Scholar] [CrossRef]
- Tanghetti, E.A. Split-face randomized treatment of facial telangiectasia comparing pulsed dye laser and an intense pulsed light handpiece. Lasers Surg. Med. 2011, 44, 97–102. [Google Scholar] [CrossRef]
- Gan, H.; Yue, B.; Wang, Y.; Lu, Z. Treatment of facial telangiectasia with narrow-band intense pulsed light in Chinese patients. J. Cosmet. Laser Ther. 2018, 20, 442–446. [Google Scholar] [CrossRef]
- Piccolo, D.; Crisman, G.; Kostaki, D.; Cannarozzo, G.; Sannino, M.; Chimenti, S. Rhodamine intense pulsed light versus conventional intense pulsed light for facial telangiectasias. J. Cosmet. Laser Ther. 2016, 18, 80–85. [Google Scholar] [CrossRef]
- Peterson, J.; Friedmann, D.; Abdo, K.; Cahana, Z. Efficacy and Safety of Intense Pulsed Light With a KTP/PDLlike Filter for the Treatment of Facial Telangiectasias. J. Drugs Dermatol. 2020, 19, 844–850. [Google Scholar] [CrossRef]
- Luo, Y.; Luan, X.; Zhang, J.; Wu, L.; Zhou, N. Improved telangiectasia and reduced recurrence rate of rosacea after treatment with 540 nm-wavelength intense pulsed light: A prospective randomized controlled trial with a 2-year follow-up. Exp. Ther. Med. 2020, 19, 3543–3550. [Google Scholar] [CrossRef] [Green Version]
- Chinnadurai, S.; Sathe, N.A.; Surawicz, T. Laser treatment of infantile hemangioma: A systematic review. Lasers Surg. Med. 2015, 48, 221–233. [Google Scholar] [CrossRef] [PubMed]
- Sannino, M.; Ambrosio, A.G.; Lodi, G.; Cannarozzo, G.; Bennardo, L.; Nisticò, S.P. A giant epidermal nevus of the face treated with a CO2 and dye laser combination: A case report and literature review. J. Cosmet. Laser Ther. 2021, 23, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Nisticò, S.P.; Bennardo, L.; Sannino, M.; Negosanti, F.; Tamburi, F.; Del Duca, E.; Giudice, A.; Cannarozzo, G. Combined CO 2 and dye laser technique in the treatment of outcomes due to flap necrosis after surgery for basal cell carcinoma on the nose. Lasers Surg. Med. 2021, 54, 523–529. [Google Scholar] [CrossRef]
- Iyer, S.; Fitzpatrick, R.E. Long-Pulsed Dye Laser Treatment for Facial Telangiectasias and Erythema. Dermatol. Surg. 2005, 31, 898–903. [Google Scholar] [CrossRef] [PubMed]
- Bennardo, L.; Fasano, G.; Tamburi, F.; Zappia, E.; Rizzuto, F.; Nisticò, S.P.; Cannarozzo, G. Sequential Use of CO2 Laser Prior to Nd:YAG and Dye Laser in the Management of Non-Facial Warts: A Retrospective Study. Medicina 2022, 58, 115. [Google Scholar] [CrossRef] [PubMed]
- Major, A.; Brazzini, B.; Campolmi, P.; Bonan, P.; Mavilia, L.; Ghersetich, I.; Hercogova, J.; Lotti, T. Nd:YAG 1064 nm laser in the treatment of facial and leg telangiectasias. J. Eur. Acad. Dermatol. Venereol. 2001, 15, 559–565. [Google Scholar] [CrossRef]
- Cannarozzo, G.; Negosanti, F.; Sannino, M.; Santoli, M.; Bennardo, L.; Banzola, N.; Negosanti, L.; Nisticò, S.P. Q-switched Nd:YAG laser for cosmetic tattoo removal. Dermatol. Ther. 2019, 32, e13042. [Google Scholar] [CrossRef]
- Cassuto, D.A.; Ancona, D.M.; Emanuelli, G. Treatment of facial telangiectasias with a diode-pumped Nd:YAG laser at 532 nm. J. Cutan. Laser Ther. 2000, 2, 141–146. [Google Scholar] [CrossRef]
- Papaspyrou, G.; Schick, B.; Al Kadah, B. Nd:YAG Laser Treatment for Extranasal Telangiectasias: A Retrospective Analysis of 38 Patients with Hereditary Hemorrhagic Telangiectasia and Review of the Literature. ORL 2016, 78, 245–251. [Google Scholar] [CrossRef]
- Bevin, A.A.; Parlette, E.C.; Domankevitz, Y.; Ross, E.V. Variable-Pulse Nd:YAG Laser in the Treatment of Facial Telangiectasias. Dermatol. Surg. 2008, 32, 7–12. [Google Scholar] [CrossRef]
- Karppinen, T.; Kantola, E.; Karppinen, A.; Rantamäki, A.; Kautiainen, H.; Mordon, S.; Guina, M. Treatment of telangiectasia on the cheeks with a compact yellow (585 nm) semiconductor laser and a green (532 nm) KTP laser: A randomized double-blinded split-face trial. Lasers Surg. Med. 2019, 51, 223–229. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Uebelhoer, N.S.; Bogle, M.A.; Stewart, B.; Arndt, K.A.; Dover, J.S. A Split-Face Comparison Study of Pulsed 532-nm KTP Laser and 595-nm Pulsed Dye Laser in the Treatment of Facial Telangiectasias and Diffuse Telangiectatic Facial Erythema. Dermatol. Surg. 2007, 33, 441–448. [Google Scholar] [CrossRef] [PubMed]
- Rose, A.E.; Goldberg, D.J. Successful Treatment of Facial Telangiectasias Using a Micropulse 1,064-nm Neodymium-Doped Yttrium Aluminum Garnet Laser. Dermatol. Surg. 2013, 39, 1062–1066. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Zhou, B.R.; Wu, D.; Xu, Y.; Luo, D. Sequential delivery of intense pulsed light and long-pulse 1.064-nm neodymium-doped yttrium aluminum garnet laser shows better effect in the treatment of facial telangiectasias than using them separately. Ital. J. Dermatol. Venereol. 2016, 152, 1–7. [Google Scholar] [CrossRef]



| Patient Number | Age | Sex | Fitzpatrick Phototype | VAS Score | Researcher Score | Patient Number | Age | Sex | Fitzpatrick Phototype | VAS Score | Researcher Score |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 61 | f | 2 | 8 | 2 | 35 | 49 | m | 1 | 8 | 2 |
| 2 | 43 | m | 3 | 6 | 1 | 36 | 56 | f | 2 | 9 | 3 |
| 3 | 48 | f | 2 | 9 | 3 | 37 | 37 | m | 3 | 8 | 2 |
| 4 | 54 | m | 2 | 9 | 3 | 38 | 52 | f | 3 | 9 | 2 |
| 5 | 58 | f | 3 | 9 | 2 | 39 | 58 | f | 4 | 9 | 3 |
| 6 | 51 | m | 3 | 7 | 2 | 40 | 42 | m | 3 | 8 | 2 |
| 7 | 34 | m | 2 | 8 | 2 | 41 | 51 | m | 2 | 7 | 2 |
| 8 | 27 | f | 1 | 10 | 3 | 42 | 45 | f | 3 | 8 | 2 |
| 9 | 39 | m | 2 | 7 | 2 | 43 | 35 | m | 3 | 8 | 2 |
| 10 | 58 | f | 3 | 8 | 3 | 44 | 38 | m | 2 | 9 | 3 |
| 11 | 52 | m | 4 | 9 | 2 | 45 | 39 | f | 4 | 8 | 2 |
| 12 | 63 | f | 3 | 9 | 3 | 46 | 46 | m | 3 | 8 | 2 |
| 13 | 42 | m | 4 | 6 | 1 | 47 | 73 | f | 4 | 9 | 3 |
| 14 | 49 | f | 4 | 7 | 2 | 48 | 24 | f | 3 | 9 | 2 |
| 15 | 58 | m | 2 | 8 | 2 | 49 | 38 | m | 1 | 10 | 3 |
| 16 | 43 | f | 1 | 9 | 3 | 50 | 46 | m | 4 | 6 | 1 |
| 17 | 38 | m | 2 | 8 | 2 | 51 | 49 | f | 5 | 6 | 0 |
| 18 | 36 | f | 1 | 9 | 3 | 52 | 43 | m | 3 | 7 | 2 |
| 19 | 62 | m | 3 | 8 | 2 | 53 | 38 | f | 4 | 8 | 1 |
| 20 | 56 | f | 2 | 9 | 3 | 54 | 53 | f | 3 | 9 | 2 |
| 21 | 58 | m | 3 | 9 | 3 | 55 | 58 | m | 3 | 8 | 2 |
| 22 | 43 | m | 3 | 8 | 2 | 56 | 39 | f | 4 | 7 | 2 |
| 23 | 46 | f | 3 | 7 | 2 | 57 | 48 | m | 3 | 9 | 3 |
| 24 | 34 | f | 4 | 7 | 1 | 58 | 53 | f | 3 | 8 | 2 |
| 25 | 49 | f | 3 | 8 | 2 | 59 | 36 | m | 3 | 7 | 1 |
| 26 | 52 | m | 4 | 9 | 3 | 60 | 38 | f | 3 | 8 | 2 |
| 27 | 67 | m | 3 | 8 | 2 | 61 | 48 | m | 2 | 9 | 3 |
| 28 | 52 | f | 4 | 10 | 3 | 62 | 43 | f | 4 | 5 | 0 |
| 29 | 25 | f | 4 | 9 | 2 | 63 | 52 | m | 2 | 10 | 3 |
| 30 | 63 | f | 3 | 9 | 3 | 64 | 58 | f | 3 | 9 | 3 |
| 31 | 64 | m | 3 | 8 | 3 | 65 | 57 | f | 2 | 8 | 2 |
| 32 | 36 | f | 4 | 7 | 2 | 66 | 54 | f | 3 | 7 | 1 |
| 33 | 71 | m | 2 | 8 | 2 | 67 | 52 | m | 3 | 8 | 2 |
| 34 | 48 | f | 3 | 9 | 3 | 68 | 59 | f | 3 | 9 | 3 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bennardo, L.; Patruno, C.; Zappia, E.; Tamburi, F.; Sannino, M.; Negosanti, F.; Nisticò, S.P.; Cannarozzo, G. Combination of Specific Vascular Lasers and Vascular Intense Pulsed Light Improves Facial Telangiectasias and Redness. Medicina 2022, 58, 651. https://doi.org/10.3390/medicina58050651
Bennardo L, Patruno C, Zappia E, Tamburi F, Sannino M, Negosanti F, Nisticò SP, Cannarozzo G. Combination of Specific Vascular Lasers and Vascular Intense Pulsed Light Improves Facial Telangiectasias and Redness. Medicina. 2022; 58(5):651. https://doi.org/10.3390/medicina58050651
Chicago/Turabian StyleBennardo, Luigi, Cataldo Patruno, Elena Zappia, Federica Tamburi, Mario Sannino, Francesca Negosanti, Steven Paul Nisticò, and Giovanni Cannarozzo. 2022. "Combination of Specific Vascular Lasers and Vascular Intense Pulsed Light Improves Facial Telangiectasias and Redness" Medicina 58, no. 5: 651. https://doi.org/10.3390/medicina58050651
APA StyleBennardo, L., Patruno, C., Zappia, E., Tamburi, F., Sannino, M., Negosanti, F., Nisticò, S. P., & Cannarozzo, G. (2022). Combination of Specific Vascular Lasers and Vascular Intense Pulsed Light Improves Facial Telangiectasias and Redness. Medicina, 58(5), 651. https://doi.org/10.3390/medicina58050651









