Life after Burn, Part I: Health-Related Quality of Life, Employment and Life Satisfaction
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Endpoints
2.3. Patient Collective, Inclusion and Exclusion Criteria
2.4. Collected Clinical Data
2.5. Questionnaire
2.6. Statistical Analysis
3. Results
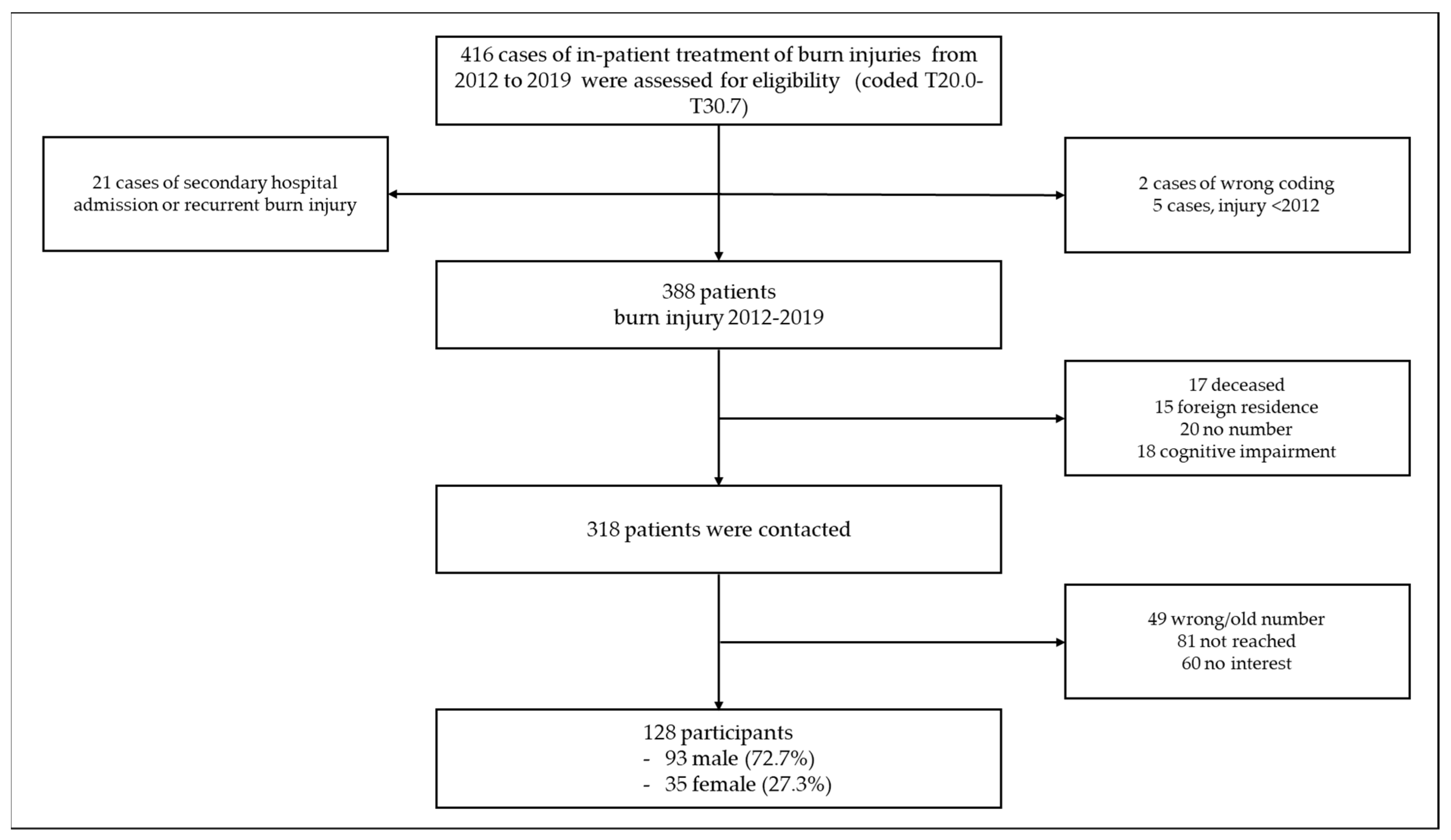
3.1. Included Patients
3.2. Demography
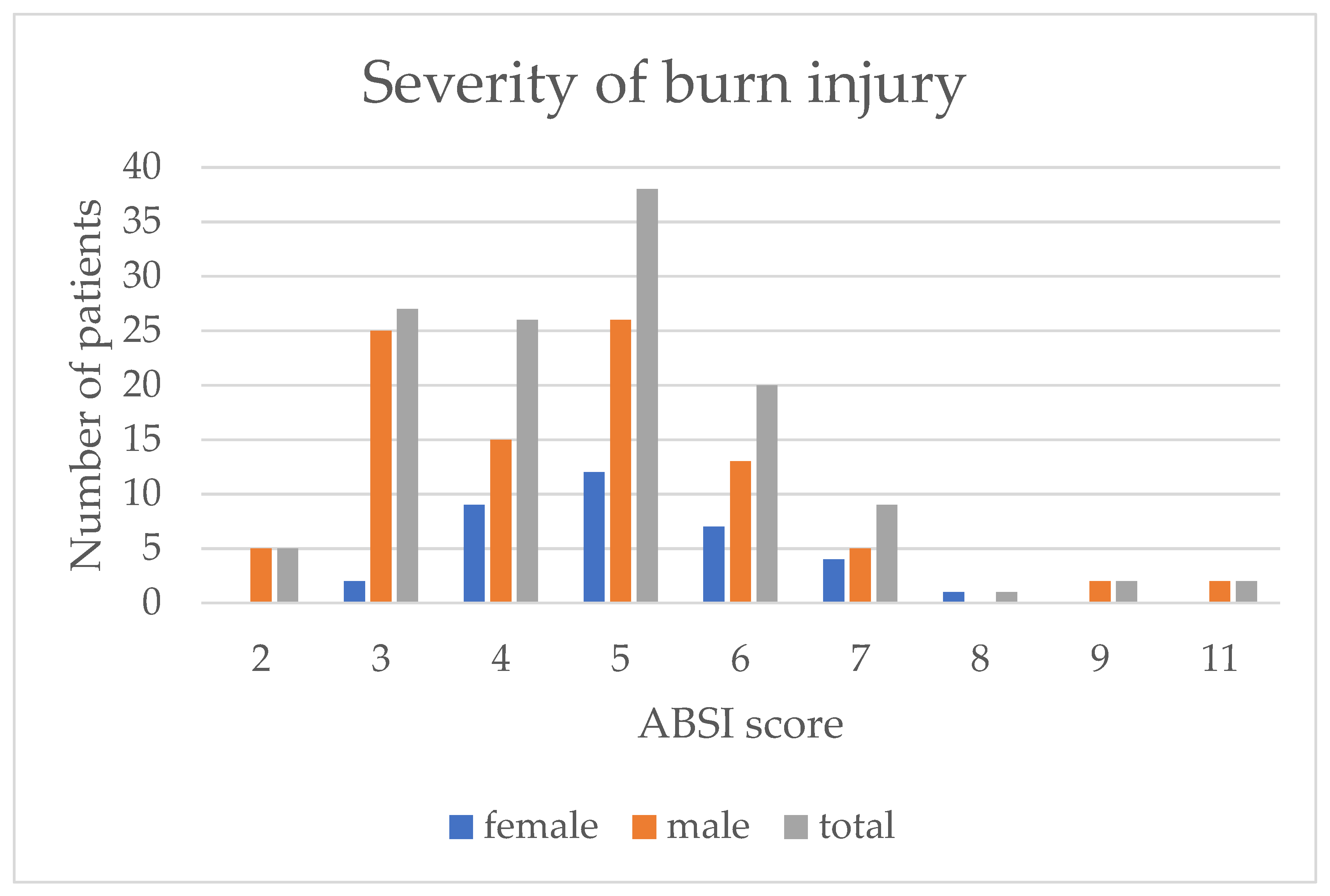
3.3. Injury Characteristics
3.4. Treatment
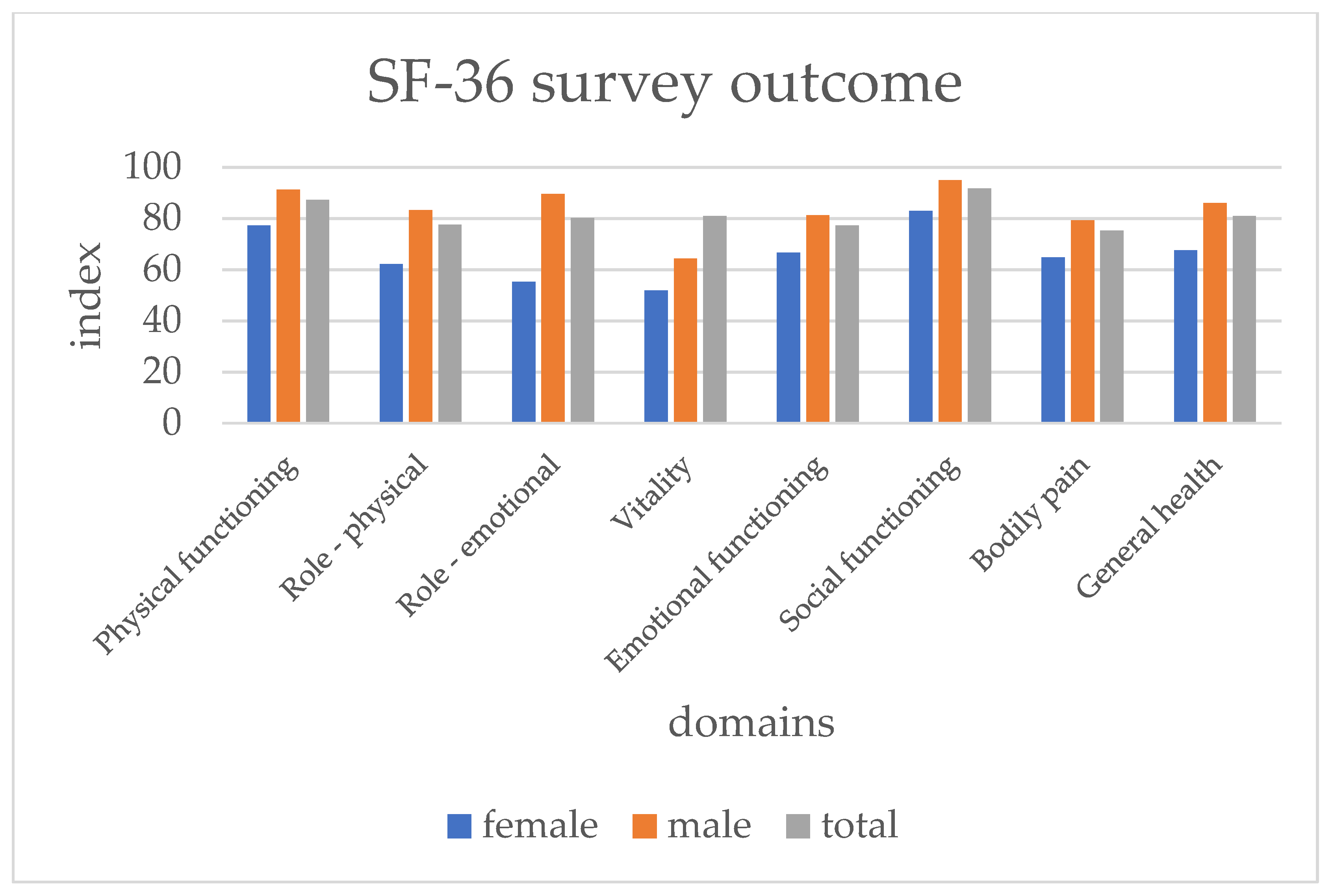
3.5. Health-Related Quality of Life
3.6. Employment Situation
3.7. Life Satisfaction
4. Discussion
4.1. Study Population
4.2. Health-Related Quality of Life
4.3. Employment
4.4. Life Satisfaction
4.5. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Pereira, C.; Murphy, K.; Herndon, D. Outcome measures in burn care: Is mortality dead? Burns 2004, 30, 761–771. [Google Scholar] [CrossRef] [PubMed]
- Jeschke, M.G.; van Baar, M.E.; Choudhry, M.A.; Chung, K.K.; Gibran, N.S.; Logsetty, S. Burn injury. Nat. Rev. Dis. Primers 2020, 6, 11. [Google Scholar] [CrossRef] [PubMed]
- Kamolz, L.P.; Herndon, D.N.; Jeschke, M.G. Verbrennungen: Diagnose, Therapie und Rehabilitation des thermischen Traumas; Springer: Vienna, Austria, 2009; 251p. [Google Scholar]
- Wasiak, J.; Lee, S.J.; Paul, E.; Mahar, P.; Pfitzer, B.; Spinks, A.; Cleland, H.; Gabbe, B. Predictors of health status and health-related quality of life 12 months after severe burn. Burns 2014, 40, 568–574. [Google Scholar] [CrossRef] [PubMed]
- Gauffin, E.; Öster, C.; Sjöberg, F.; Gerdin, B.; Ekselius, L. Health-related quality of life (EQ-5D) early after injury predicts long-term pain after burn. Burns 2016, 42, 1781–1788. [Google Scholar] [CrossRef] [PubMed]
- Dyster-Aas, J.; Kildal, M.; Willebrand, M. Return to work and health-related quality of life after burn injury. J. Rehabil. Med. 2007, 39, 49–55. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Öster, C.; Kildal, M.; Ekselius, L. Return to work after burn injury: Burn-injured individuals’ perception of barriers and facilitators. J. Burn Care Res. 2010, 31, 540–550. [Google Scholar] [CrossRef]
- Orwelius, L.; Willebrand, M.; Gerdin, B.; Ekselius, L.; Fredrikson, M.; Sjöberg, F. Long term health-related quality of life after burns is strongly dependent on pre-existing disease and psychosocial issues and less due to the burn itself. Burns 2013, 39, 229–235. [Google Scholar] [CrossRef] [Green Version]
- Mason, S.T.; Esselman, P.; Fraser, R.; Schomer, K.; Truitt, A.; Johnson, K. Return to work after burn injury: A systematic review. J. Burn Care Res. 2012, 33, 101–109. [Google Scholar] [CrossRef]
- Palmu, R.; Partonen, T.; Suominen, K.; Vuola, J.; Isometsä, E. Return to work six months after burn: A prospective study at the Helsinki Burn Center. Burns 2015, 41, 1152–1160. [Google Scholar] [CrossRef]
- Quinn, T.; Wasiak, J.; Cleland, H. An examination of factors that affect return to work following burns: A systematic review of the literature. Burns 2010, 36, 1021–1026. [Google Scholar] [CrossRef]
- Tolentino-Bazán, K.; Chavez-Heres, T.; Morales-García, M.; Macías-Hernández, S.I.; Ramírez-Ramírez, A.C.; Velázquez-Bustamante, A.E.; Rhoades-Torres, G.M.; Velez-Palafox, M. Predictive Factors for Returning to Work in Burn Adult Patients That Were Working Before Their Injury. J. Burn Care Res. 2021, 42, 294–299. [Google Scholar] [CrossRef] [PubMed]
- Öster, C.; Ekselius, L. Return to work after burn-A prospective study. Burns 2011, 37, 1117–1124. [Google Scholar] [CrossRef] [PubMed]
- Esselman, P.C.; Wiechman Askay, S.; Carrougher, G.J.; Lezotte, D.C.; Holavanahalli, R.K.; Magyar-Russell, G.; Fauerbach, J.A.; Engrav, L.H. Barriers to return to work after burn injuries. Arch. Phys. Med. Rehabil. 2007, 88 (Suppl. 2), 50–56. [Google Scholar] [CrossRef] [PubMed]
- Goverman, J.; Mathews, K.; Nadler, D.; Henderson, E.; McMullen, K.; Herndon, D.; Meyer, W.; Fauerbach, J.; Wiechman, S.; Carrougher, G.; et al. Satisfaction with life after burn: A Burn Model System National Database Study. Burns 2016, 42, 1067–1073. [Google Scholar] [CrossRef] [PubMed]
- Amtmann, D.; Bocell, F.D.; McMullen, K.; Bamer, A.M.; Johnson, K.L.; Wiechman, S.A.; Schneider, J.C. Satisfaction With Life Over Time in People With Burn Injury: A National Institute on Disability, Independent Living, and Rehabilitation Research Burn Model System Study. Arch. Phys. Med. Rehabil. 2020, 101, S63–S70. [Google Scholar] [CrossRef] [PubMed]
- Amtmann, D.; Bocell, F.D.; Bamer, A.; Heinemann, A.W.; Hoffman, J.M.; Juengst, S.B.; Rosenberg, M.; Schneider, J.C.; Wiechman, S.; McMullen, K. Psychometric Properties of the Satisfaction With Life Scale in People With Traumatic Brain, Spinal Cord, or Burn Injury: A National Institute on Disability, Independent Living, and Rehabilitation Research Model System Study. Assessment 2019, 26, 695–705. [Google Scholar] [CrossRef] [PubMed]
- Edgar, D.; Dawson, A.; Hankey, G.; Phillips, M.; Wood, F. Demonstration of the validity of the SF-36 for measurement of the temporal recovery of quality of life outcomes in burns survivors. Burns 2010, 36, 1013–1020. [Google Scholar] [CrossRef]
- Bullinger, M.; Kirchberger, I.; Ware, J. Der deutsche SF-36 Health Survey Übersetzung und psychometrische Testung eines krankheitsübergreifenden Instruments zur Erfassung der gesundheitsbezogenen Lebensqualität. Z. Gesundh. 1995, 3, 21–36. [Google Scholar] [CrossRef]
- Morfeld, M.; Bullinger, M. Der SF36 Health Survey zur Erhebung und Dokumentation gesundheitsbezogener Lebensqualität. Phys. Med. Rehabil. Kurortmed. 2008, 18, 250–255. [Google Scholar]
- SF-36 Fragebogen Auswertung und Inhalt (Short Form 36). Heartbeat. Available online: https://heartbeat-med.com/de/wiki/sf-36-fragebogen/# (accessed on 27 July 2021).
- Gojowy, D.; Kauke, M.; Ohmann, T.; Homann, H.-H.; Mannil, L. Early and late-recorded predictors of health-related quality of life of burn patients on long-term follow-up. Burns 2019, 45, 1300–1310. [Google Scholar] [CrossRef]
- Ellert, U.; Kurth, B.-M. Methodische Betrachtungen zu den Summenscores des SF-36 anhand der erwachsenen bundesdeutschen Bevölkerung. Bundesgesundheitsblatt-Gesundheitsforschung-Gesundheitsschutz 2004, 47, 1027–1032. [Google Scholar] [CrossRef] [PubMed]
- Smolle, C.; Cambiaso-Daniel, J.; Forbes, A.A.; Wurzer, P.; Hundeshagen, G.; Branski, L.K.; Huss, F.; Kamolz, L. Recent trends in burn epidemiology worldwide: A systematic review. Burns 2017, 43, 249–257. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Peck, M.D. Epidemiology of burns throughout the world. Part I: Distribution and risk factors. Burns 2011, 37, 1087–1100. [Google Scholar] [CrossRef] [PubMed]
- Brusselaers, N.; Monstrey, S.; Vogelaers, D.; Hoste, E.; Blot, S. Severe burn injury in europe: A systematic review of the incidence, etiology, morbidity, and mortality. Crit. Care 2010, 14, R188. [Google Scholar] [CrossRef] [Green Version]
- Dyster-Aas, J.; Willebrand, M.; Wikehult, B.; Gerdin, B.; Ekselius, L. Major Depression and Posttraumatic Stress Disorder Symptoms Following Severe Burn Injury in Relation to Lifetime Psychiatric Morbidity. J. Trauma 2008, 64, 1349–1356. [Google Scholar] [CrossRef]
- Spronk, I.; Legemate, C.M.; Dokter, J.; van Loey, N.E.E.; van Baar, M.E.; Polinder, S. Predictors of health-related quality of life after burn injuries: A systematic review. Crit. Care 2018, 22, 160. [Google Scholar] [CrossRef] [Green Version]
- Spronk, I.; van Loey, N.E.E.; Sewalt, C.; Nieboer, D.; Renneberg, B.; Moi, A.L.; Oster, C.; Orwelius, L.; Van Baar, M.E.; Polinder, S.; et al. Recovery of health-related quality of life after burn injuries: An individual participant data meta-analysis. PLoS ONE 2020, 15, e0226653. [Google Scholar] [CrossRef]
- Palmu, R.; Partonen, T.; Suominen, K.; Saarni, S.I.; Vuola, J.; Isometsä, E. Health-related quality of life 6 months after burns among hospitalized patients: Predictive importance of mental disorders and burn severity. Burns 2015, 41, 742–748. [Google Scholar] [CrossRef]
- Martin, L.; Byrnes, M.; Bulsara, M.K.; McGarry, S.; Rea, S.; Wood, F. Quality of life and posttraumatic growth after adult burn: A prospective, longitudinal study. Burns 2017, 43, 1400–1410. [Google Scholar] [CrossRef]
- Edgar, D.W.; Homer, L.; Phillips, M.; Gurfinkel, R.; Rea, S.; Wood, F.M. The influence of advancing age on quality of life and rate of recovery after treatment for burn. Burns 2013, 39, 1067–1072. [Google Scholar] [CrossRef]
- Renneberg, B.; Ripper, S.; Schulze, J.; Seehausen, A.; Weiler, M.; Wind, G.; Liedl, A. Quality of life and predictors of long-term outcome after severe burn injury. J. Behav. Med. 2014, 37, 967–976. [Google Scholar] [CrossRef] [PubMed]
- Moi, A.L.; Haugsmyr, E.; Heisterkamp, H. Long-Term Study Of Health And Quality Of Life After Burn Injury. Ann. Burns Fire Disasters 2016, 29, 295. [Google Scholar] [PubMed]
- Fauerbach, J.A.; Lezotte, D.C.; Hills, R.A.; Cromes, F.G.; Kowalske, K.J.; de Lateur, B.J.; Goodwin, C.W.; Blakeney, P.; Herndon, D.N.; Wiechman, S.A.; et al. Burden of Burn: A Norm-Based Inquiry into the Influence of Burn Size and Distress on Recovery of Physical and Psychosocial Function. J. Burn Care Rehabil. 2005, 26, 21–32. [Google Scholar] [CrossRef] [PubMed]
- Goei, H.; Hop, M.J.; van der Vlies, C.H.; Nieuwenhuis, M.K.; Polinder, S.; Middelkoop, E.; van Baar, M.E. Return to work after specialised burn care: A two-year prospective follow-up study of the prevalence, predictors and related costs. Injury 2016, 47, 1975–1982. [Google Scholar] [CrossRef] [PubMed]
- Spronk, I.; Polinder, S.; Haagsma, J.A.; Nieuwenhuis, M.; Pijpe, A.; van der Vlies, C.; Middelkoop, E.; van Baar, M. Patient-reported scar quality of adults after burn injuries: A five-year multicenter follow-up study. Wound Repair Regen. 2019, 27, 406–414. [Google Scholar] [CrossRef] [Green Version]
- Ware, J.E.; Sherbourne, C.D. The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Med. Care 1992, 30, 473–483. [Google Scholar] [CrossRef]
| Employment, Level of Education and Life Satisfaction | ||
|---|---|---|
| Yes | No | |
| Employment before burn injury | ||
| a Self-employed | 〇 | 〇 |
| b Employee, civil servant | 〇 | 〇 |
| c Worker | 〇 | 〇 |
| d Retiree | 〇 | 〇 |
| e Unemployed | 〇 | 〇 |
| Employment after burn injury | ||
| a Self-employed | 〇 | 〇 |
| b Employee, civil servant | 〇 | 〇 |
| c Worker | 〇 | 〇 |
| d Retiree | 〇 | 〇 |
| e Unemployed | 〇 | 〇 |
| If employed: Change in employment | ||
| a No change (same job and hours) | 〇 | 〇 |
| b Same job and less hours | 〇 | 〇 |
| c Different job and same hours | 〇 | 〇 |
| d Different job and less hours | 〇 | 〇 |
| Highest level of education | ||
| a Middle school | 〇 | 〇 |
| b Apprenticeship | 〇 | 〇 |
| c General qualification for university entrance | 〇 | 〇 |
| d University degree | 〇 | 〇 |
| Description of current life situation | ||
| a Leading an autonomous and self-determined life | 〇 | 〇 |
| b Being needed in everyday life | 〇 | 〇 |
| c Fulfilling work/retirement | 〇 | 〇 |
| d Enjoyable leisure activities | 〇 | 〇 |
| e Desire to change something, if possible | 〇 | 〇 |
| i Appearance (e.g., unsightly scars) | 〇 | 〇 |
| ii Body functionality (e.g., dry skin, mobility) | 〇 | 〇 |
| iii Mental wellbeing (e.g., persisting sleep disorders or anxiety) | 〇 | 〇 |
| Demography of Participants | ||||
|---|---|---|---|---|
| Female | Male | Total | p-Value | |
| Number of patients (%) | 35 (27.3%) | 93 (72.7%) | 128 (100%) | |
| Age at injury | ||||
| Mean (SD) | 41.2 (SD 16.3) | 39.5 (SD 15.6) | 40.0 (SD 15.7) | 0.594 * |
| Age at inquiry | ||||
| Mean (SD) | 46.1 (SD 16.4) | 44.7 (SD 16.2) | 45.1 (SD 16.2) | 0.662 * |
| Pre-existing conditions | ||||
| Diabetes mellitus | 1 (2.9%) | 1 (1.1%) | 2 (1.6%) | 0.469 ** |
| Arterial hypertension | 8 (22.9%) | 11 (11.8%) | 19 (14.8%) | 0.118 ** |
| Ischemic heart disease | 3 (8.6%) | 2 (2.2%) | 5 (3.9%) | 0.095 ** |
| Cerebrovascular disease | 1 (2.9%) | 1 (1.1%) | 2 (1.6%) | 0.469 ** |
| Peripheral vascular disease | 1 (2.9%) | 0 | 1 (0.8%) | 0.102 ** |
| Neurologic disease | 3 (8.6%) | 2 (2.2%) | 5 (3.9%) | 0.095 ** |
| History of psychiatric disease | 6 (17.1%) | 2 (2.2%) | 8 (6.3%) | 0.002 ** |
| History of substance abuse | 2 (5.7%) | 0 | 2 (1.6%) | 0.020 ** |
| History of alcohol abuse | 3 (8.6%) | 1 (1.1%) | 4 (3.1%) | 0.030 ** |
| Documented smoker | 3 (8.6%) | 10 (10.8%) | 13 (10.2%) | 0.716 ** |
| Other comorbidities | 2 (5.7%) | 4 (4.3%) | 6 (4.7%) | 0.736 ** |
| Injury Characteristics | ||||
|---|---|---|---|---|
| Female | Male | Total | p-Value | |
| Injury mechanism | 0.292 * | |||
| Flame (%) | 15 (42.9%) | 56 (60.2%) | 71 (55.5%) | |
| Scald (%) | 14 (40.0%) | 26 (28.0%) | 40 (31.3%) | |
| Contact burn (%) | 3 (8.6%) | 4 (4.3%) | 7 (5.5%) | |
| Chemical burn (%) | 3 (8.6%) | 4 (4.3%) | 7 (5.5%) | |
| Electric burn (%) | 0 | 3 (3.2%) | 3 (2.3%) | |
| Circumstances | 0.011 * | |||
| Work-related | 8 (22.9%) | 43 (46.2%) | 51 (39.5%) | |
| Household | 21 (60.0%) | 47 (50.5%) | 68 (53.1%) | |
| Traffic accident | 2 (5.7%) | 3 (3.2%) | 5 (3.9%) | |
| Self-inflicted | 1 (2.9%) | 0 | 1 (0.8%) | |
| Assault | 1 (2.9%) | 0 | 1 (0.8%) | |
| Other | 2 (5.7%) | 0 | 2 (1.6%) | |
| %TBSA | ||||
| Mean (SD) | 5.6 (SD 7.3) | 10.6 (SD 11.8) | 9.2 (SD 11.0) | 0.005 ** |
| No. of patients with third-degree burns (%) | 15 (42.9%) | 51 (54.8%) | 66 (51.6%) | 0.227 * |
| Affected body area | ||||
| Upper extremity | 17 (48.6%) | 65 (69.9%) | 82 (64.1%) | |
| Lower extremity | 23 (65.7%) | 45 (48.4%) | 68 (53.1%) | |
| Back | 4 (11.4%) | 13 (14.0%) | 17 (13.3%) | |
| Ant. thorax/abdomen | 8 (22.9%) | 22 (23.7%) | 30 (23.4%) | |
| Genitals | 1 (2.9%) | 5 (5.4%) | 6 (4.7%) | 0.548 * |
| Hands | 9 (25.7%) | 44 (47.3%) | 53 (41.4%) | 0.024 * |
| Face/neck | 11 (31.4%) | 52 (55.9%) | 63 (49.2%) | 0.014 * |
| Inhalation injury | 0 | 5 (5.4%) | 5 (3.9%) | 0.162 * |
| Survey Outcome | ||||
|---|---|---|---|---|
| Female | Male | Total | p-Value * | |
| Months since injury (mean, SD) | 58.9 (SD 26.5) | 62.0 (SD 25.1) | 61.1 (SD 25.4) | 0.538 |
| SF-36 scale scores (mean, SD) | ||||
| Physical functioning | 77.3 (SD 29.0) | 91.2 (SD 16.3) | 87.3 (SD 21.4) | 0.010 |
| Role—physical | 62.1 (SD 47.5) | 83.3 (SD 35.09) | 77.5 (SD 40.0) | 0.020 |
| Role—emotional | 55.2 (SD 49.8) | 89.6 (SD 30.3) | 80.2 (SD 40.0) | 0.000 |
| Vitality | 51.9 (SD 21.0) | 64.3 (SD 18.1) | 80.9 (SD 19.7) | 0.003 |
| Mental health | 66.6 (SD 21.9) | 81.3 (SD 13.7) | 77.3 (SD 17.5) | 0.001 |
| Social functioning | 82.9 (SD 33.9) | 95.0 (SD 17.9) | 91.7 (SD 23.9) | 0.050 |
| Bodily Pain | 64.8 (SD 40.3) | 79.2 (SD 30.3) | 75.2 (SD 33.8) | 0.061 |
| General health | 67.6 (SD 29.8) | 86.0 (SD 20.8) | 81.0 (SD 24.9) | 0.002 |
| Employment | ||||
|---|---|---|---|---|
| Female | Male | Total | ||
| Pre-burn * | Self-employed | 2 (5.7%) | 10 (10.8%) | 12 (9.4%) |
| Employee/civil servant | 12 (34.3%) | 35 (37.6%) | 47 (36.7%) | |
| Worker | 4 (11.4%) | 32 (34.4%) | 36 (28.1%) | |
| Retiree | 9 (25.7%) | 11 (11.8%) | 20 (15.6%) | |
| Unemployed | 8 (22.9%) | 5 (5.4%) | 13 (10.2%) | |
| Post-burn ** | Self-employed | 2 (5.7%) | 11 (11.8%) | 13 (10.2%) |
| Employee/civil servant | 14 (40%) | 34 (36.6%) | 48 (37.5%) | |
| Worker | 2 (5.7%) | 25 (26.9%) | 27 (21.1%) | |
| Retiree | 13 (37.1%) | 19 (20.4%) | 32 (25.0%) | |
| Unemployed | 4 (11.4%) | 4 (4.3%) | 8 (6.3%) | |
| Change in employment | Same job and hours *** | 20 (57.1%) | 67 (72.0%) | 87 (68.0%) |
| Change in job *** | 1 (2.9%) | 7 (7.5%) | 8 (6.3%) | |
| Change in hours *** | 0 | 2 (2.2%) | 2 (1.6%) | |
| Change in job and hours *** | 1 (2.9%) | 4 (4.3%) | 5 (3.9%) | |
| Got a job | 6 (17.1%) | 2 (2.2%) | 8 (6.3%) | |
| Retired | 4 (11.4%) | 8 (8.6%) | 12 (9.4%) | |
| Lost job | 2 (5.7%) | 1 (1.1%) | 3 (2.3%) | |
| Still unemployed | 1 (2.9%) | 2 (2.2.%) | 3 (2.3%) | |
| Social Reintegration | ||||
|---|---|---|---|---|
| Female | Male | Total | p-Value * | |
| Autonomous, self-determined life | 33 (94.3%) | 91 (97.8%) | 124 (96.9%) | 0.302 |
| Being needed in everyday life | 33 (94.3%) | 89 (95.7%) | 122 (95.3%) | 0.736 |
| Fulfilling job/retirement | 27 (77.1%) | 84 (90.3%) | 111 (86.7%) | 0.050 |
| Enjoyable leisure activities | 30 (85.7%) | 88 (94.6%) | 118 (92.2%) | 0.094 |
| Would change aesthetics | 11 (31.4%) | 20 (21.5%) | 31 (24.2%) | 0.243 |
| Would change body functionality | 14 (40.0%) | 29 (31.2%) | 43 (33.6%) | 0.347 |
| Would change mental wellbeing | 11 (31.4%) | 12 (12.9%) | 23 (18.0%) | 0.015 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hutter, M.F.; Smolle, C.; Kamolz, L.-P. Life after Burn, Part I: Health-Related Quality of Life, Employment and Life Satisfaction. Medicina 2022, 58, 599. https://doi.org/10.3390/medicina58050599
Hutter MF, Smolle C, Kamolz L-P. Life after Burn, Part I: Health-Related Quality of Life, Employment and Life Satisfaction. Medicina. 2022; 58(5):599. https://doi.org/10.3390/medicina58050599
Chicago/Turabian StyleHutter, Maria Fernanda, Christian Smolle, and Lars-Peter Kamolz. 2022. "Life after Burn, Part I: Health-Related Quality of Life, Employment and Life Satisfaction" Medicina 58, no. 5: 599. https://doi.org/10.3390/medicina58050599
APA StyleHutter, M. F., Smolle, C., & Kamolz, L.-P. (2022). Life after Burn, Part I: Health-Related Quality of Life, Employment and Life Satisfaction. Medicina, 58(5), 599. https://doi.org/10.3390/medicina58050599







