Abstract
Background and Objectives: In recent years, the use of radiofrequency diathermy in pelvic floor disorders has grown proportionally to the interest in this specialty. Despite the common use of this therapy among pelvic floor physiotherapists, little is known about its effects and effectiveness in pelvic floor disorders. For this reason, the aim of the present review is to assess the effects of non-invasive 300 kHz–1 MHz radiofrequency diathermy in the treatment of pelvic floor disorders. Materials and Methods: A literature search was performed in PubMed, Scopus and Web of Science, searching for any type of study that included pelvic floor disorder participants and an experimental group treated with non-invasive nor ablative radiofrequency diathermy. Results: There were a total of 578 studies after removing duplicates. The inclusion and exclusion criteria were applied, resulting in a total of 15 studies, which were methodologically assessed with PEDro and the Newcastle and Ottawa scale. Conclusions: Despite the low quality of most of them, the studies showed improvements in urinary incontinence, pelvic pain conditions, pelvic floor muscles strength and sexual function. These findings must be considered with caution until more randomized clinical trials are performed to solve the biases detected.
1. Introduction
Radiofrequency diathermy (RFD) is a non-invasive therapy that consists of the emission of high-frequency electromagnetic waves, which produce deep heat that increases the metabolism of biological tissue [1]. This process promotes tissue repair and influences pain sensitivity [2,3]. Wavelengths of 300 kHz to 1 MHz are commonly used among physiotherapists for pain management and reducing the recovery time of musculoskeletal disorders [4]. Regarding technical aspects, there exist two types of devices regarding energy transmission: capacitive–resistive and dielectric. Moreover, these devices could also be classified according to the number of poles (monopolar or bipolar), the latter including other multipolar devices that are merely a bipolar with more than one output of a pole [5]. Despite the variety of devices and according to our knowledge, there are no studies comparing the effects of different devices on the same pathological condition.
“Pelvic floor disorders” is a term that encompasses any dysfunction related with the pelvic floor: urinary incontinence, dyspareunia, chronic pelvic pain, erectile dysfunction, postpartum symptoms, pre- and postmenstrual syndrome, etc. Physiotherapy has an important role in most of the mentioned disorders, being considered the main therapeutic approach in many of them [6,7]. In this line, the use of RFD as treatment in pelvic floor disorders has grown in recent years due to its metabolic and analgesic effects, which could be helpful in many disorders. Kumaran and Watson defined the deep blood flow changes that appear with the application of RFD, which enhances blood support to soft tissues [1]. Other authors focused their research on the analgesic effects of RFD on musculoskeletal [8,9,10], neuropathic [11], myofascial [12] and post-surgery pain [13]. Nevertheless, Gold et al. [14] reviewed its efficacy in feminine rejuvenation, suggesting improvements in mild to moderate conditions related with vaginal laxity and neocollagenesis proliferation [15], despite the lack of robustness in the quality of the studies found [14]. Although its use is widely accepted, no systematic reviews have been performed to evaluate the existing evidence about the use of RFD in pelvic floor disorders. For this reason, the aim of the present review is to assess the effects of non-invasive 300 kHz–1 MHz RFD in the treatment of pelvic floor disorders.
2. Materials and Methods
2.1. Study Design
A systematic review was carried out in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) (updated version (2020)) guideline [16] and the Cochrane Handbook for Systematic Reviews of Interventions of Higgins and Green (version 2011) [17]. In addition, the PROSPERO register was searched and no prior systematic review of our topic of interest was identified.
2.2. Literature Search
Two researchers independently performed a bibliographic search on PubMed Medline, Scopus and Web of Science databases until December 2021. Additional searches were performed in previously published reviews, books, practice guidelines and gray literature (expert documents and conference proceedings). In order to follow a systematic search strategy, the PICO system was used to develop the bibliographical search chains [17]: Population (patients with pelvic floor disorders), Intervention (radiofrequency diathermy), Comparison (comparison of patients treated with radiofrequency diathermy with sham/placebo therapy or any other treatments) and Outcomes (any related with pelvic floor disorders). The keywords used in this search strategy, according to the Medical Subjects Headings (MeSH), were “radiofrequency therapy”, “hyperthermia induced”, “pelvic floor”, and “pelvic floor disorders”, with its entry terms. Boolean operators “AND”/“OR” were used. In addition, a third researcher with expertise in search strategy took part to resolve any doubts. Table 1 shows the search chains used in each of the databases.

Table 1.
Bibliographic search strategy used in each database.
2.3. Study Selection
This stage was performed by two authors that independently screened the retrieved articles of each database by title and abstract. If one author considered an article as a possible study to be included in the systematic review, it was examined in detail. A third author was consulted to solve any disputes. A study was included in the review if it met all the following inclusion criteria: (1) trials or cases studies using RFD (from 300 kHz to 1 MHz) as main treatment or part of it; (2) with a sample comprising participants diagnosed with pelvic floor disorders; (3) all studies included, almost must to have an intervention group that perform RFD.; (4) the results of the study must report data concerning pelvic floor function; and (5) studies must have been published in the last 10 years. Otherwise, studies were excluded that: (1) were duplicated; (2) exclusively analyzed outcomes related with pelvic floor rejuvenation or aesthetics; (3) did not report results related with pelvic floor health; (4) used interventional or minimally invasive radiofrequency.
2.4. Data Extraction
Two authors performed data extraction independently, with any discrepancy being resolved by a third researcher. Data included pelvic floor disorders, outcomes, therapy groups, sample size, participants per group, year of publishing, authors, age, sex, adverse effects registered and type of RFD application. Finally, results were also considered to assess the efficacy of the treatment.
2.5. Outcomes
Due to the aim of this systematic review, the main outcomes considered were perceived pain in any part of the pelvic floor, gender interference, sexual satisfaction, urinary incontinence, menopausal symptoms and pelvic floor muscles’ strength. Secondary outcomes included: erectile dysfunction, time of orgasm, allodynia, hyperalgesia and quality of life.
2.6. Methodological Quality Assessment
The PEDro scale was the tool used to assess the methodological quality of studies that were designed as randomized clinical trials [18]. Case series or simple trials were evaluated with the Newcastle–Ottawa Scale (NOS) [19]. The PEDro scale consists of 11 items, each counting as one point with the exception of the first one, which is related to external validity, so the scale scores from 0 to 10. A score of 9–10 indicates excellent methodological quality studies, 6–8 for good-high quality ones, 4–5 for moderate quality and under 4 in the case of low quality [18]. For assessing other non-randomized studies, the NOS allows for analysis of the quality of selection methods, comparability among groups and exposure to interventions [19]. Two researchers independently assessed the methodological quality of the studies included in the review and a third researcher was consulted to resolve the discrepancies that arose.
3. Results
3.1. Study Selection
The PRISMA flow chart (Figure 1) shows the study selection process. Six-hundred-nineteen studies were found among PubMed, Scopus and Web of Science, which were added to another three found by references. From those, 44 were discarded as duplicates. The title and abstract of the remaining 578 were screened and 463 were excluded due to the selection criteria. In the end, 100 more studies were excluded after reading the whole text, obtaining 15 studies that met the inclusion criteria [20,21,22,23,24,25,26,27,28,29,30,31,32,33,34].
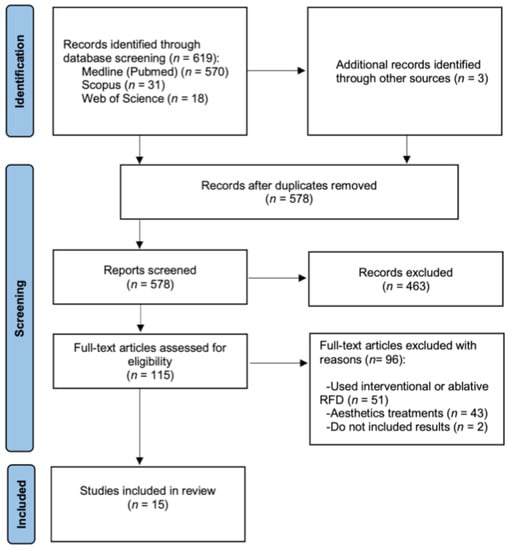
Figure 1.
Flow diagram of the study search.
3.2. Characteristics of the Studies Included in the Review
A total of 15 studies included in the review were: 5 RCT and 10 other study designs (7 case series, 2 one-arm non-RCT and 1 prospective study). Studies included data of 635 participants with different pelvic floor disorders (sexual function disorders, stress urinary incontinence, endometriosis-related pain, chronic pelvic pain, postpartum perineal pain, Peyronie’s disease and post-menopausal sexual symptoms). In addition, a summary of the main characteristics of the studies such as author, year, disorder, sample, outcomes, intervention and results are represented in Table 2 (randomized controlled trials) and Table 3 (other study designs).

Table 2.
Summary of the randomized controlled trials selected.

Table 3.
Summary of the other design of studies considered of interest.
3.3. Methodological Quality Assessment
The randomized controlled trials that were selected obtained moderate quality on the PEDro scale: three scored 5/10 [20,27,29], one 6/10 [21] and the last 7/10 [28]. These results suggest that higher quality randomized controlled trials are necessary on this topic, as the existing studies present several limitations. Concerning other study designs, they were assessed by the Newcastle and Ottawa scale, obtaining low scores: between 0 and 3 stars [22,23,24,25,26,30,31,33,34,35]. This poor result is explained by the lack of comparison groups in most of the designs and the possible risk of selection bias due to the lack of information about participants’ identity and recruitment. Supplementary Tables S1 and S2 show the score item by item of both methodological assessment scales.
3.4. Synthesis of Outcomes and Questionnaires Used in Studies Included in This Review
From the 15 studies selected, 6 were related to the effects of RFD in urinary incontinence (5 in women [22,23,29,31] and 1 in prostatectomized men [34]). With this aim, a variety of tools were used to assess the urinary loss of participants (Urogenital Distress Inventory (UDI-6), International Consultation on Incontinence Questionnaire for Urinary Incontinence Short Form (ICIQ-SF UI), Female Sexual Function Index (FSFI), International Consultation on Incontinence Questionnaire for Overactive Bladder (ICIQ-OAB) and the pad test), which made it difficult to meta-analyze the effects. All studies found improvements after treatment with RFD in some of the evaluation tools used. Considering the validity of the measures, most of them were validated tools (UDI-6 [36], ICIQ-SF UI [37], FSFI [38], ICIQ-OAB [39]), although the pad test suffers from frequent variations in how the test is performed, which reduces its generalizability [40].
3.5. Synthesis of Main Findings
Regarding sexual function, two RCTs measured the effects of RFD in FSFI, revealing improvements of 1.8 (p = 0.031) [21] and 3.51 (p = 0.03) [28], respectively. Another case series study [26] and a non-randomized trial [22] analyzed the effects of therapy on women orgasmic dysfunction, obtaining a self-perceived reduction of 50% in time to orgasm for the first [26] and no changes for the second [22].
Postpartum perineal pain was treated in the RCT of Bretelle et al., finding no differences in perineal pain but improvements in discomfort while walking in the experimental group [20]. A case series of Dayan et al. obtained improvements in muscle maximum contraction after postpartum, not in basal muscle tone [33], using a biofeedback device for this assessment.
There were also studies focused on pain. Fernández-Cuadros et al. obtained a reduction of 3.52 points on the VAS (p < 0.0001) in a case series of women with pelvic pain or dyspareunia [35], while Fortún-Rabadan reduced referral pain and dysmenorrhea intensity in a case series with five women [30]. Nonetheless, an RCT evaluated the effects of RFD in 94 participants with Peyronie’s disease, obtaining a reduction of 2 points on the VAS (p < 0.01) during erection, although no changes in curvature nor International Index of Erectile Function were observed [27].
4. Discussion
The application of RFD in pelvic floor disorders reports interesting perspectives, but undoubtedly, evidence is still far from supporting its use as a main therapy. In fact, very few studies have sufficient quality and are free of bias to support the use of RFD as something more than a complementary therapy to the main treatments. Most of the studies found are case series without control groups and/or participants were selected under biased conditions or non-independently from evaluation researchers. Moreover, poor explanations about treatment dosage were given in most of the cases, with high heterogeneity among the trials: one measured the dosage in joules [21], another facilitated the frequency of emission in kilohertz [20], another referred to a power percentage in watts and, in others, temperature was measured at the tissue surface [28,29]. On this line, future studies must explain the dosage according to frequency of emission, the pulse of the signal (continuous or pulsed in a percentage of time), intensity and periodicity of treatment. Although tissue surface temperature could also be interesting to investigate, due to types of emission temperature differing significantly from surface to deeper tissues [41], the latter is the target of treatment in most cases.
Urinary incontinence was the most treated pelvic floor condition, obtaining favorable results in all the studies, both in women and prostatectomized men. The RCT of Leibaschoff et al. evidenced significant improvements after short RFD applications where temperature remained under 45 °C [29], which is the top temperature threshold within safety limits [42]. The rest of the studies were case series that performed similar applications regarding temperature increment [23,24,34], with changes in frequencies and place of the application with similar results, so it seems that the key point for effectiveness could be related with reaching a temperature between 40 and 45 °C for almost two minutes [23,24,29,34]. Only Razzaghi et al. extended the treatments to 3 weeks [31]. Prostatectomized men mentioned discomfort while introducing the endoanal applicator, this being the only side effect mentioned [34]. The lack of control groups in the case series reduced the possibility of reaching stronger conclusions, as there was a high risk of selection and comparison bias.
Pelvic floor pain was also a frequent outcome in the results of this review. Postpartum perineal pain and related disturbances in the first and second day seem to have poor improvements with RFD, although participants mentioned a reduction in painkillers intake, which is positive despite no changes in pain being observed [20]. More success was obtained by Fernández-Cuadros et al. with chronic pelvic pain and dyspareunia participants, observing an important reduction in pain and improvements in pelvic floor muscle strength [32]. However, the lack of a control group limits the strengths of this case series, as well as the heterogeneity of the participants selected; thus, a randomized clinical trial would be needed to confirm these results. Another condition where the effects of RFD were considered was endometriosis, a complex syndrome that severely affects women, conditioning their whole life [30]. Five participants were intensively treated over three menstrual cycles, obtaining improvements in dysmenorrhea intensity, sex interference and myofascial and referral pain [30]. These results support the design of a larger trial, as results cannot be generalizable due to sample limitations and inexistence of a control group. Last but not least, 96 participants with Peyronie’s disease benefit from RFD treatment, obtaining a reduction of 2 points in VAS during erection [27]. No changes were observed in penis curvature, despite RFD being accepted as an influence in collagenesis and fibroblast proliferation because of the heat produced in the tissue [15,43].
Two RCTs, a non-randomized trial and a case series assessed the effects of RFD in sexual function and orgasmic dysfunction. Both RCTs show significant improvements in FSFI after treatment [21,28]. Similar results were obtained by Alinsod et al. in a case series with 25 participants, although the changes were self-reported by the participants based on time to orgasm, which may lead to bias. Notwithstanding, the non-randomized trial showed no improvements in FSFI, which makes us think that the differences should be based on the treatment applied [22]. In this case, an intensive treatment regimen (daily [21] or weekly [28]) would be more effective than a monthly one [22], as temperatures reached in the treatments were similar.
This review also found RFD applications that targeted pelvic floor muscles contraction. Dayan et al. observed that the treatment with RFD produced an increment in maximal pelvic floor muscles contraction but no changes were perceived in base muscle tone [33]. Similar results regarding muscle strength were reported by Fernández-Cuadros et al. [35]. In any case, once again, these results must be considered with caution due to the low-quality evidence that the case series offer.
Concerning the safety of the RFD application in the pelvic floor muscles, five studies identified that the treatment presents a low risk of adverse effects due to their lack of appearance [22,23,24,31,33]. Only Krychman et al. reported some adverse events, which resolved spontaneously [21].
The limited data do not allow us to compare between different types of RFD application. Only one study used a monopolar dielectric transmission device [30], which is relevant because this system produces low surface heating [44] compared with the capacitive–resistive method. The rest of the studies used bipolar devices, although some of them were named as monopolar (despite being composed of a return plate and an applicator) or quadripolar (despite only having two poles: the emitting and the return poles). This issue is probably due to marketing concerns over technical characteristics and must be clarified in future works.
Findings of this systematic review must be taken into account with caution due to the presence of several limitations. (1) This review combines randomized controlled trials, observational studies and case series, which reduces the quality of the evidence. (2) The low number of studies included and the low number of participants reported can reduce the accuracy and generalization of our findings. (3) The data publication limits may have left out some studies, although it must be considered that this is a new application and that no studies were found before 2016. (4) The low-moderate methodological quality of the studies included increases the risk of bias. (5) It is important to consider the possible risk of publication bias in our finding that can affect to the true effect of experimental therapy. (6) The last limitation is related with the level of evidence of our findings. According to the Oxford Centre for Evidence-Based Medicine, our review presents a level of evidence of III, due to it being a review composed of different study designs, with the majority being non-RCTs. The findings of this review may be classified as level C of the recommendation, due to the scientific evidence being conflicting and the fact that new studies may change our findings. However, meta-analysis could not be performed because studies did not report homogenous quantitative data to be integrated. Further research must be carried out to increase knowledge of the effect of non-invasive radiofrequency diathermy in pelvic floor disorders, especially randomized clinical trials that include follow-up of the participants.
5. Conclusions
Despite having low-quality evidence, the main findings in our review showed that RFD could be effective for improving urinary incontinence, pelvic floor muscles’ strength, sexual function and different pelvic pain conditions. Nevertheless, the high risk of bias among the existing literature forces us to consider these results with caution. In addition, it is necessary to carry out more clinical trials to assess the effect of RFD on different pelvic floor outcomes, minimizing the risk of selection and confusion bias.
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/medicina58030437/s1, Supplementary Table S1. PEDro Assessment Scores. Supplementary Table S2. Newcastle-Ottawa Assessment Scores.
Author Contributions
Conceptualization, M.D.G.-G., E.O.-G. and A.J.I.-V.; methodology, M.D.G.-G., A.J.I.-V., E.O.-G. and I.C.-P.; validation, E.O.-G., I.C.-P., F.L.-M. and Á.L.-G.; formal analysis, M.D.G.-G. and A.J.I.-V.; investigation, M.D.G.-G., A.J.I.-V., I.C.-P., E.O.-G., F.L.-M. and Á.L.-G.; resources, A.J.I.-V. and E.O.-G.; data curation, M.D.G.-G., I.C.-P., F.L.-M. and Á.L.-G.; writing—original draft preparation, M.D.G.-G. and A.J.I.-V.; writing—review and editing, M.D.G.-G., A.J.I.-V. and E.O.-G.; visualization, M.D.G.-G., A.J.I.-V., I.C.-P., E.O.-G., F.L.-M. and Á.L.-G.; supervision, I.C.-P. and F.L.-M.; project administration, A.J.I.-V. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data of the study are available under request to the corresponding author.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Kumaran, B.; Herbland, A.; Watson, T. Continuous-mode 448 kHz capacitive resistive monopolar radiofrequency induces greater deep blood flow changes compared to pulsed mode shortwave: A crossover study in healthy adults. Eur. J. Physiother. 2017, 19, 137–146. [Google Scholar] [CrossRef]
- Kumaran, B.; Watson, T. Thermal build-up, decay and retention responses to local therapeutic application of 448 kHz capacitive resistive monopolar radiofrequency: A prospective randomised crossover study in healthy adults. Int. J. Hyperth. 2015, 6736, 1–13. [Google Scholar] [CrossRef]
- Kumaran, B.; Watson, T. Radiofrequency-based treatment in therapy-related clinical practice—A narrative review. Part II: Chronic conditions. Phys. Ther. Rev. 2015, 20, 241–254. [Google Scholar] [CrossRef] [Green Version]
- Beltrame, R.; Ronconi, G.; Ferrara, P.E.; Salgovic, L.; Vercelli, S.; Solaro, C.; Ferriero, G. Capacitive and resistive electric transfer therapy in rehabilitation: A systematic review. Int. J. Rehabil. Res. 2020, 43, 291–298. [Google Scholar] [CrossRef]
- Ibáñez-Vera, A.J. Radiofrequency in aesthetics skin treatment: Classification and modalities. J. Dermatol. Res. Ski. Care 2017, 1, 8–10. [Google Scholar]
- Wallace, S.L.; Miller, L.D.; Mishra, K. Pelvic floor physical therapy in the treatment of pelvic floor dysfunction in women. Curr. Opin. Obstet. Gynecol. 2019, 31, 485–493. [Google Scholar] [CrossRef]
- Bradley, M.H.; Rawlins, A.; Brinker, C.A. Physical Therapy Treatment of Pelvic Pain. Phys. Med. Rehabil. Clin. N. Am. 2017, 28, 589–601. [Google Scholar] [CrossRef]
- Albornoz-Cabello, M.; Barrios-Quinta, C.J.; Escobio-Prieto, I.; Sobrino-Sánchez, R.; Ibáñez-Vera, A.J.; Espejo-Antúnez, L. Treatment of Patellofemoral Pain Syndrome with Dielectric Radiofrequency Diathermy: A Preliminary Single—Group Study with Six-Month Follow-Up. Medicina 2021, 57, 429. [Google Scholar] [CrossRef]
- Albornoz-Cabello, M.; Ibáñez-Vera, A.J.; Aguilar-Ferrándiz, M.E.; Espejo-Antúnez, L. Monopolar dielectric diathermy by emission of radiofrequency in Patellofemoral pain. A single-blind-randomized clinical trial. Electromagn. Biol. Med. 2020, 39, 1–8. [Google Scholar] [CrossRef]
- Kumaran, B.; Watson, T. Treatment using 448 kHz capacitive resistive monopolar radiofrequency improves pain and function in patients with osteoarthritis of the knee joint: A randomised controlled trial. Physiotheraphy 2019, 105, 98–107. [Google Scholar] [CrossRef] [Green Version]
- Hochsprung, A.; Escudero-Uribe, S.; Ibáñez-Vera, A.J.; Izquierdo-Ayuso, G. Effectiveness of monopolar dielectric transmission of pulsed electromagnetic fields for multiple sclerosis-related pain: A pilot study. Neurologia 2021, 36, 433–439. [Google Scholar] [CrossRef]
- Ibáñez-Vera, A.J.; García-Romero, J.C.; Alvero-Cruz, J.R.; Lomas-vega, R. Effects of Monopolar Dielectric Radiofrequency Signals on the Symptoms of Fibromyalgia: A Single-Blind Randomized Controlled Trial. Int. J. Environ. Res. Public Health 2020, 17, 2465. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- García-Marín, M.; Rodríguez-Almagro, D.; Castellote-Caballero, Y.; Achalandabaso-Ochoa, A.; Lomas-Vega, R.; Ibáñez-Vera, A.J. Efficacy of Non-Invasive Radiofrequency-Based Diathermy in the Postoperative Phase of Knee Arthroplasty: A Double-Blind Randomized Clinical Trial. J. Clin. Med. 2021, 10, 1611. [Google Scholar] [CrossRef] [PubMed]
- Gold, M.; Andriessen, A.; Bader, A.; Alinsod, R.; French, E.S.; Guerette, N.; Kolodchenko, Y.; Krychman, M.; Murrmann, S.; Samuels, J. Review and clinical experience exploring evidence, clinical efficacy, and safety regarding nonsurgical treatment of feminine rejuvenation. J. Cosmet. Dermatol. 2018, 17, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Hantash, B.M.; Ubeid, A.A.; Chang, H.; Kafi, R.; Renton, B. Bipolar fractional radiofrequency treatment induces neoelastogenesis and neocollagenesis. Lasers Surg. Med. 2009, 41, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Int. J. Surg. 2021, 88, 105906. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions; The Cochrane Collaboration: London, UK, 2011. [Google Scholar]
- Moseley, A.M.; Herbert, R.D.; Sherrington, C.; Maher, C.G. Evidence for physiotherapy practice: A survey of the Physiotherapy Evidence Database (PEDro). Aust. J. Physiother. 2002, 48, 43–49. [Google Scholar] [CrossRef] [Green Version]
- Wells, G.; Shea, B.; O’Connel, D. The Newcastle-Ottawa Scale (NOS) for Assessing the Quailty of Nonrandomised Studies in Meta-Analysis. 2009. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 19 November 2021).
- Bretelle, F.; Fabre, C.; Golka, M.; Pauly, V.; Roth, B.; Bechadergue, V.; Blanc, J. Capacitive–resistive radiofrequency therapy to treat postpartum perineal pain: A randomized study. PLoS ONE 2020, 15, e0231869. [Google Scholar] [CrossRef] [PubMed]
- Krychman, M.; Rowan, C.G.; Allan, B.B.; DeRogatis, L.; Durbin, S.; Yacoubian, A.; Wilkerson, D. Effect of Single-Treatment, Surface-Cooled Radiofrequency Therapy on Vaginal Laxity and Female Sexual Function: The VIVEVE I Randomized Controlled Trial. J. Sex. Med. 2017, 14, 215–225. [Google Scholar] [CrossRef] [PubMed]
- Vanaman Wilson, M.J.; Bolton, J.; Jones, I.T.; Wu, D.C.; Calame, A.; Goldman, M.P. Histologic and Clinical Changes in Vulvovaginal Tissue After Treatment With a Transcutaneous Temperature-Controlled Radiofrequency Device. Dermatol. Surg. 2018, 44, 705–713. [Google Scholar] [CrossRef]
- Caruth, J.C. Evaluation of the Safety and Efficacy of a Novel Radiofrequency Device for Vaginal Treatment. Surg. Technol. Int. 2018, 32, 145–149. [Google Scholar]
- Lordelo, P.; Boas, A.V.; Sodré, D.; Lemos, A.; Tozetto, S.; Brasil, C. New concept for treating female stress urinary incontinence with radiofrequency. Int. Braz. J. Urol. 2017, 43, 896–902. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vicariotto, F.; Raichi, M. Technological evolution in the radiofrequency treatment of vaginal laxity and menopausal vulvo-vaginal atrophy and other genitourinary symptoms: First experiences with a novel dynamic quadripolar device. Minerva Ginecol. 2016, 68, 225–236. [Google Scholar] [PubMed]
- Alinsod, R.M. Transcutaneous temperature controlled radiofrequency for orgasmic dysfunction. Lasers Surg. Med. 2016, 48, 641–645. [Google Scholar] [CrossRef] [PubMed]
- Pavone, C.; Romeo, S.; D’Amato, F.; Usala, M.; Letizia Mauro, G.; Caruana, G. Does Transfer Capacitive Resistive Energy Has a Therapeutic Effect on Peyronie’s Disease? Randomized, Single-Blind, Sham-Controlled Study on 96 Patients: Fast Pain Relief. Urol. Int. 2017, 99, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Lordêlo, P.; Leal, M.R.D.; Brasil, C.A.; Santos, J.M.; Lima, M.C.N.P.C.; Sartori, M.G.F. Radiofrequency in female external genital cosmetics and sexual function: A randomized clinical trial. Int. Urogynecol. J. 2016, 27, 1681–1687. [Google Scholar] [CrossRef] [PubMed]
- Leibaschoff, G.; Gonzalez Izasa, P.; Cardona, J.L.; Miklos, J.R.; Moore, R.D. Trascutaneous Temperature Controlled Radiofrequency (TTCRF) for the Treatment of Menopausal Vaginal/Genitourinary Symptoms. Surg. Technol. Int. 2016, 26, 149–159. [Google Scholar]
- Fortún-Rabadán, R.; Sierra-Artal, B.; Jiménez-Sánchez, C. Effectiveness of intracavitary monopolar dielectric radiofrequency in women with endometriosis-associated pain: A case series. Complement. Ther. Clin. Pract. 2022, 46, 101517. [Google Scholar] [CrossRef]
- Razzaghi, M.; Asghari-azghan, A.; Montazeri, S.; Razzaghi, Z.; Mazloomfard, M.M.; Vafaee, R. Intravaginal Pulsed Contractile Radiofrequency for Stress Urinary Incontinence Treatment; A Safety Study. J. Lasers Med. Sci. 2021, 12, 1–5. [Google Scholar] [CrossRef]
- Fernández-Cuadros, M.E.; Kazlauskas, S.G.; Albaladejo-Florin, M.J.; Robles-López, M.; Laborda-Delgado, A.; de la Cal-Alvarez, C.; Pérez-Moro, O. Effectiveness of multimodal rehabilitation (biofeedback plus capacitive–resistive radiofrequency) on chronic pelvic pain and dyspareunia: Prospective study and literature review. Rehabilitacion 2020, 54, 154–161. [Google Scholar] [CrossRef]
- Dayan, E.; Ramirez, H.; Westfall, L.; Theodorou, S. Role of Radiofrequency (Votiva, InMode) in Pelvic Floor Restoration. Plast. Reconstr. Surg. Glob. Open 2019, 7, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Sodré, D.S.M.; Sodré, P.R.S.; Brasil, C.; Teles, A.; Dória, M.; Café, L.E.; Lordelo, P. New concept for treating urinary incontinence after radical prostatectomy with radiofrequency: Phase 1 clinical trial. Lasers Med. Sci. 2019, 34, 1865–1871. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Cuadros, M.E.; Kazlauskas, S.G.; Albaladejo-Florin, M.J.; Robles-López, M.; Laborda-Delgado, A.; de la Cal-Alvarez, C.; Pérez-Moro, O. Efectividad de la rehabilitación multimodal (biofeedback más radiofrecuencia capacitiva-resistiva) sobre el dolor pélvico crónico y la dispareunia: Estudio prospectivo y revisión de la bibliografía. Rehabilitación 2020, 54, 154–161. [Google Scholar] [CrossRef]
- Harvey, M.A.; Kristjansson, B.; Griffith, D.; Versi, E. The Incontinence Impact Questionnaire and the Urogenital Distress Inventory: A revisit of their validity in women without a urodynamic diagnosis. Am. J. Obstet. Gynecol. 2001, 185, 25–30. [Google Scholar] [CrossRef] [Green Version]
- Hajebrahimi, S.; Corcos, J.; Lemieux, M.C. International consultation on incontinence questionnaire short form: Comparison of physician versus patient completion and immediate and delayed self-administration. Urology 2004, 63, 1076–1078. [Google Scholar] [CrossRef]
- Rosen, R.; Brown, C.; Heiman, J.; Leiblum, S.; Meston, C.; Shabsigh, R.; Ferguson, D.; D’agostino, R. The Female Sexual Function Index (FSFI): A Multidimensional Self-Report Instrument for the Assessment of Female Sexual Function D’Agostino (2000) The Female Sexual Function Index (FSFI): A Multidimensional Self-Report Instrument for the Assessment of Female Sexual Function. J. Sex Marital Ther. 2011, 26, 191–208. [Google Scholar]
- Abrams, P.; Avery, K.; Gardener, N.; Donovan, J. The international consultation on incontinence modular questionnaire: www.iciq.net. J. Urol. 2006, 175, 1063–1066. [Google Scholar] [CrossRef]
- Krhut, J.; Zachoval, R.; Smith, P.P.; Rosier, P.F.W.M.; Valansk, L.; Martan, A.; Zvara, P. Pad Weight Testing in the Evaluation of Urinary Incontinence. Neurourol. Urodyn. 2014, 33, 507–510. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez-Sanz, J.; Pérez-Bellmunt, A.; López-de-Celis, C.; Lucha-López, O.M.; González-Rueda, V.; Tricás-Moreno, J.M.; Simon, M.; Hidalgo-García, C. Thermal and non-thermal effects of capacitive–resistive electric transfer application on different structures of the knee: A cadaveric study. Sci. Rep. 2020, 10, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Yarmolenko, P.S.; Moon, E.J.; Landon, C.; Manzoor, A.; Hochman, D.W.; Viglianti, B.L.; Dewhirst, M.W. Thresholds for thermal damage to normal tissues: An update. Int. J. Hyperth. 2011, 27, 320–343. [Google Scholar] [CrossRef] [PubMed]
- Meyer, P.F.; de Oliveira, P.; Silva, F.K.B.A.; da Costa, A.C.S.; Pereira, C.R.A.; Casenave, S.; Valentim Silva, R.M.; Araújo-Neto, L.G.; Santos-Filho, S.D.; Aizamaque, E.; et al. Radiofrequency treatment induces fibroblast growth factor 2 expression and subsequently promotes neocollagenesis and neoangiogenesis in the skin tissue. Lasers Med. Sci. 2017, 32, 1727–1736. [Google Scholar] [CrossRef] [PubMed]
- Albornoz-Cabello, M.; Ibáñez-Vera, A.J.; de la Cruz-Torres, B. Efficacy of monopolar dielectric transmission radio frequency in panniculus adiposus and cellulite reduction Efficacy of monopolar dielectric transmission radio frequency in panniculus adiposus and cellulite reduction. J. Cosmet. Laser Ther. 2017, 19, 422–426. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).