Polypharmacy in Older Adults with Alzheimer’s Disease
Abstract
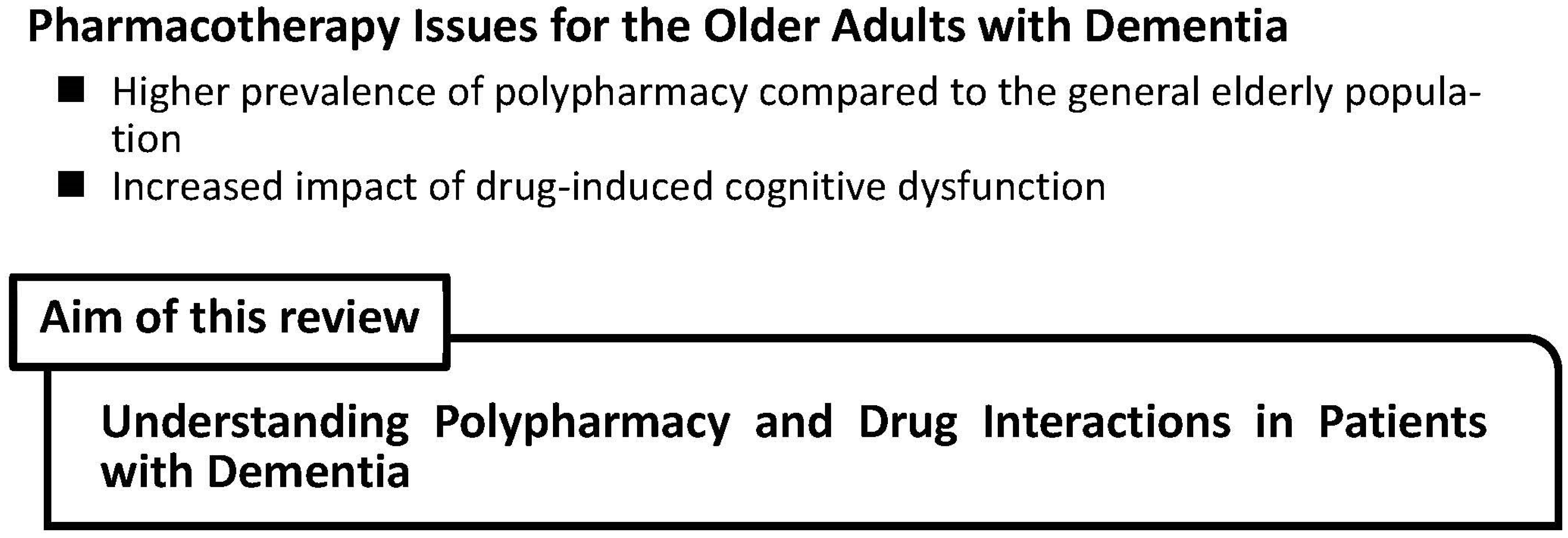
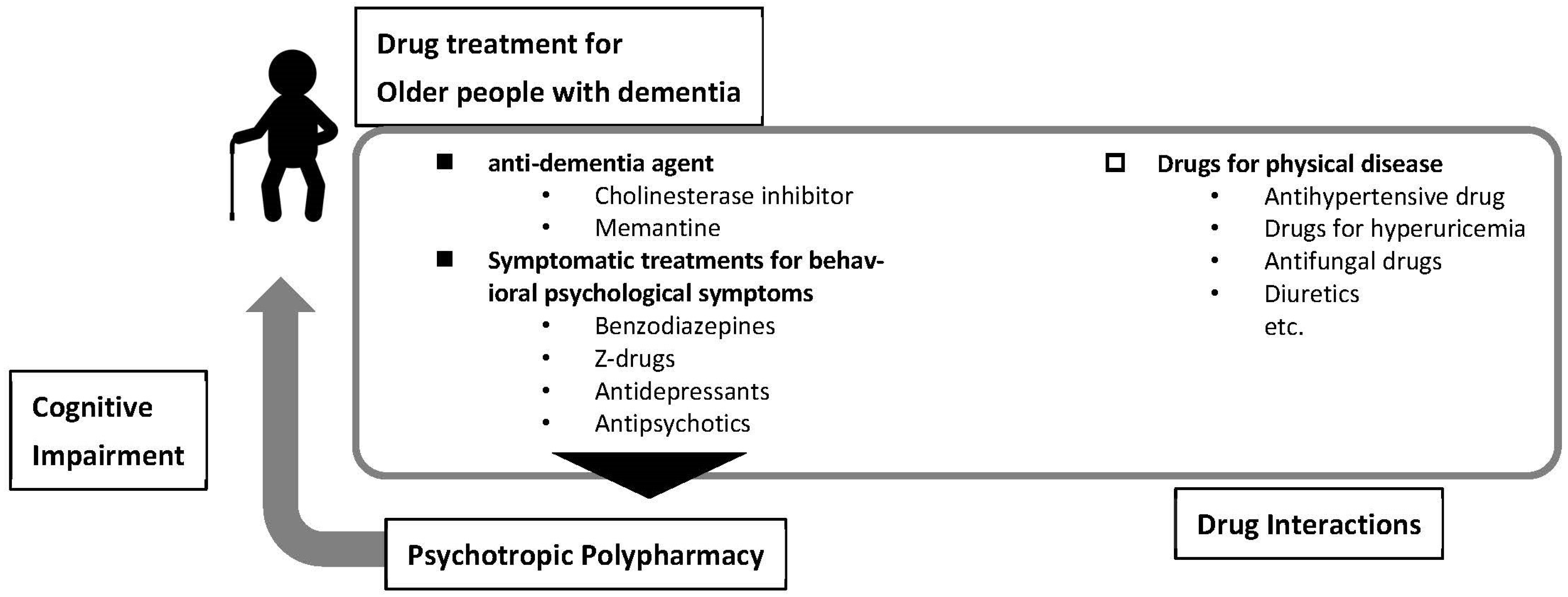
1. Introduction
2. Polypharmacy in Alzheimer’s Disease Patients
3. Cognitive Impairment Induced by Polypharmacy
4. Drug Interactions in Alzheimer’s Disease
4.1. Pharmacokinetic Drug Interactions
4.2. Pharmacodynamic Drug Interactions
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Maust, D.T.; Strominger, J.; Kim, H.M.; Langa, K.M.; Bynum, J.P.W.; Chang, C.-H.; Kales, H.C.; Zivin, K.; Solway, E.; Marcus, S.C. Prevalence of Central Nervous System-Active Polypharmacy among Older Adults with Dementia in the US. JAMA 2021, 325, 952–961. [Google Scholar] [CrossRef] [PubMed]
- Hebert, L.E.; Weuve, J.; Scherr, P.A.; Evans, D.A. Alzheimer disease in the United States (2010–2050) estimated using the 2010 census. Neurology 2013, 80, 1778. [Google Scholar] [CrossRef]
- Kim, Y.J.; Han, J.W.; So, Y.S.; Seo, J.Y.; Kim, K.Y.; Kim, K.W. Prevalence and trends of dementia in Korea: A systematic review and meta-analysis. J. Korean Med. Sci. 2014, 29, 903–912. [Google Scholar] [CrossRef] [PubMed]
- Choi, H.G.; Park, B.; Kim, J.H.; Kim, J.H.; Kwon, M.J.; Kim, M. Causes of Mortality in Korean Patients with Neurodegenerative Dementia. Biomed. Res. Int. 2022, 2022, 3206594. [Google Scholar] [CrossRef] [PubMed]
- Kasajima, M.; Eggleston, K.; Kusaka, S.; Matsui, H.; Tanaka, T.; Son, B.K.; Iijima, K.; Goda, K.; Kitsuregawa, M.; Bhattacharya, J.; et al. Projecting prevalence of frailty and dementia and the economic cost of care in Japan from 2016 to 2043: A microsimulation modelling study. Lancet Public Health 2022, 7, e458–e468. [Google Scholar] [CrossRef]
- Salisbury, C. Multimorbidity: Redesigning health care for people who use it. Lancet 2012, 380, 7–9. [Google Scholar] [CrossRef]
- Marengoni, A.; Angleman, S.; Melis, R.; Mangialasche, F.; Karp, A.; Garmen, A.; Meinow, B.; Fratiglioni, L. Aging with multimorbidity: A systematic review of the literature. Ageing Res. Rev. 2011, 10, 430–439. [Google Scholar] [CrossRef] [PubMed]
- Valderas, J.M.; Starfield, B.; Sibbald, B.; Salisbury, C.; Roland, M. Defining comorbidity: Implications for understanding health and health services. Ann. Fam. Med. 2009, 7, 357–363. [Google Scholar] [CrossRef] [PubMed]
- Fried, T.R.; O’Leary, J.; Towle, V.; Goldstein, M.K.; Trentalange, M.; Martin, D.K. Health outcomes associated with polypharmacy in community-dwelling older adults: A systematic review. J. Am. Geriatr. Soc. 2014, 62, 2261–2272. [Google Scholar] [CrossRef] [PubMed]
- Clague, F.; Mercer, S.W.; Mclean, G.; Reynish, E.; Guthrie, B. Comorbidity and polypharmacy in people with dementia: Insights from a large, population-based cross-sectional analysis of primary care data. Age Ageing 2017, 46, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Parsons, C. Polypharmacy and inappropriate medication use in patients with dementia: An underresearched problem. Ther. Adv. Drug Saf. 2017, 8, 31–46. [Google Scholar] [CrossRef] [PubMed]
- Growdon, M.E.; Gan, S.; Yaffe, K.; Steinman, M.A. Polypharmacy among older adults with dementia compared with those without dementia in the United States. J. Am. Geriatr. Soc. 2021, 69, 2464–2475. [Google Scholar] [CrossRef] [PubMed]
- Charlesworth, C.J.; Smit, E.; Lee, D.S.H.; Alramadhan, F.; Odden, M.C. Polypharmacy among Adults Aged 65 Years and Older in the United States: 1988–2010. J. Gerontol. A Biol. Sci. Med. Sci. 2015, 70, 989–995. [Google Scholar] [CrossRef] [PubMed]
- Frazier, S.C. Health outcomes and polypharmacy in elderly individuals: An integrated literature review. J. Gerontol. Nurs. 2005, 31, 4–9. [Google Scholar] [CrossRef]
- Safran, D.G.; Neuman, P.; Schoen, C.; Kitchman, M.S.; Wilson, I.B.; Cooper, B.; Li, A.; Chang, H.; Rogers, W.H. Prescription drug coverage and seniors: Findings from a 2003 national survey. Health Aff. 2005, 24, W5–W152. [Google Scholar] [CrossRef]
- Mortazavi, S.S.; Shati, M.; Keshtkar, A.; Malakouti, S.K.; Bazargan, M.; Assari, S. Defining polypharmacy in the elderly: A systematic review protocol. BMJ Open 2016, 6. [Google Scholar] [CrossRef]
- Gnjidic, D.; Hilmer, S.N.; Blyth, F.M.; Naganathan, V.; Waite, L.; Seibel, M.J.; McLachlan, A.J.; Cumming, R.G.; Handelsman, D.J.; Le Couteur, D.G. Polypharmacy cutoff and outcomes: Five or more medicines were used to identify community-dwelling older men at risk of different adverse outcomes. J. Clin. Epidemiol. 2012, 65, 989–995. [Google Scholar] [CrossRef]
- Veronese, N.; Stubbs, B.; Noale, M.; Solmi, M.; Pilotto, A.; Vaona, A.; Demurtas, J.; Mueller, C.; Huntley, J.; Crepaldi, G.; et al. Polypharmacy Is Associated with Higher Frailty Risk in Older People: An 8-Year Longitudinal Cohort Study. J. Am. Med. Dir. Assoc. 2017, 18, 624–628. [Google Scholar] [CrossRef]
- Saum, K.U.; Schöttker, B.; Meid, A.D.; Holleczek, B.; Haefeli, W.E.; Hauer, K.; Brenner, H. Is Polypharmacy Associated with Frailty in Older People? Results from the ESTHER Cohort Study. J. Am. Geriatr. Soc. 2017, 65, e27–e32. [Google Scholar] [CrossRef]
- Morin, L.; Larrañaga, A.C.; Welmer, A.K.; Rizzuto, D.; Wastesson, J.W.; Johnell, K. Polypharmacy and injurious falls in older adults: A nationwide nested case-control study. Clin. Epidemiol. 2019, 11, 483–493. [Google Scholar] [CrossRef]
- Montero-Odasso, M.; Sarquis-Adamson, Y.; Song, H.Y.; Bray, N.W.; Pieruccini-Faria, F.; Speechley, M. Polypharmacy, Gait Performance, and Falls in Community-Dwelling Older Adults. Results from the Gait and Brain Study. J. Am. Geriatr. Soc. 2019, 67, 1182–1188. [Google Scholar] [CrossRef] [PubMed]
- Disalvo, D.; Luckett, T.; Luscombe, G.; Bennett, A.; Davidson, P.; Chenoweth, L.; Mitchell, G.; Pond, D.; Phillips, J.; Beattie, E.; et al. Potentially Inappropriate Prescribing in Australian Nursing Home Residents with Advanced Dementia: A Substudy of the IDEAL Study. J. Palliat. Med. 2018, 21, 1472–1479. [Google Scholar] [CrossRef] [PubMed]
- Hukins, D.; Macleod, U.; Boland, J.W. Identifying potentially inappropriate prescribing in older people with dementia: A systematic review. Eur. J. Clin. Pharm. 2019, 75, 467–481. [Google Scholar] [CrossRef] [PubMed]
- Barry, H.E.; Cooper, J.A.; Ryan, C.; Passmore, A.P.; Robinson, A.L.; Molloy, G.J.; Darcy, C.M.; Buchanan, H.; Hughes, C.M. Potentially Inappropriate Prescribing among People with Dementia in Primary Care: A Retrospective Cross-Sectional Study Using the Enhanced Prescribing Database. J. Alzheimers Dis. 2016, 52, 1503–1513. [Google Scholar] [CrossRef]
- Spinewine, A.; Schmader, K.E.; Barber, N.; Hughes, C.; Lapane, K.L.; Swine, C.; Hanlon, J.T. Appropriate prescribing in elderly people: How well can it be measured and optimised? Lancet 2007, 370, 173–184. [Google Scholar] [CrossRef]
- O’mahony, D.; O’sullivan, D.; Byrne, S.; O’connor, M.N.; Ryan, C.; Gallagher, P. STOPP/START criteria for potentially inappropriate prescribing in older people: Version 2. Age Ageing 2015, 44, 213–218. [Google Scholar] [CrossRef]
- Xing, X.X.; Zhu, C.; Liang, H.Y.; Wang, K.; Chu, Y.Q.; Zhao, L.B.; Jiang, D.C.; Wang, Y.Q.; Yan, S.Y. Associations between Potentially Inappropriate Medications and Adverse Health Outcomes in the Elderly: A Systematic Review and Meta-analysis. Ann. Pharmacother. 2019, 53, 1005–1019. [Google Scholar] [CrossRef]
- Porter, B.; Arthur, A.; Savva, G.M. How do potentially inappropriate medications and polypharmacy affect mortality in frail and non-frail cognitively impaired older adults? A cohort study. BMJ Open 2019, 9, e026171. [Google Scholar] [CrossRef]
- Harrison, S.L.; Kouladjian O’Donnell, L.; Bradley, C.E.; Milte, R.; Dyer, S.M.; Gnanamanickam, E.S.; Liu, E.; Hilmer, S.N.; Crotty, M. Associations between the Drug Burden Index, Potentially Inappropriate Medications and Quality of Life in Residential Aged Care. Drugs Aging 2018, 35, 83–91. [Google Scholar] [CrossRef]
- Renom-Guiteras, A.; Thürmann, P.A.; Miralles, R.; Klaaßen-Mielke, R.; Thiem, U.; Stephan, A.; Bleijlevens, M.H.C.; Jolley, D.; Leino-Kilpi, H.; Hallberg, I.R.; et al. Potentially inappropriate medication among people with dementia in eight European countries. Age Ageing 2018, 47, 68–74. [Google Scholar] [CrossRef]
- Murphy, C.; Dyer, A.H.; Lawlor, B.; Kennelly, S. Potentially inappropriate medication use in older adults with mild-moderate Alzheimer’s disease: Prevalence and associations with adverse events. Age Ageing 2020, 49, 580–587. [Google Scholar] [CrossRef] [PubMed]
- Prescribing cascade: Calcium-channel blockers and diuretics. Drug Ther. Bull 2021, 59, 19. [CrossRef] [PubMed]
- Kverno, K. First Do No Harm: Psychotropic Prescribing Principles and Guidelines for Older Adults. J. Psychosoc. Nurs. Ment. Health Serv. 2020, 58, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Singh, S.; Cocoros, N.M.; Haynes, K.; Nair, V.P.; Harkins, T.P.; Rochon, P.A.; Platt, R.; Dashevsky, I.; Reynolds, J.; Mazor, K.M.; et al. Antidopaminergic-Antiparkinsonian Medication Prescribing Cascade in Persons with Alzheimer’s Disease. J. Am. Geriatr. Soc. 2021, 69, 1328–1333. [Google Scholar] [CrossRef] [PubMed]
- Storms, H.; Marquet, K.; Aertgeerts, B.; Claes, N. Prevalence of inappropriate medication use in residential long-term care facilities for the elderly: A systematic review. Eur. J. Gen. Pract. 2017, 23, 69–77. [Google Scholar] [CrossRef]
- Sköldunger, A.; Fastbom, J.; Wimo, A.; Fratiglioni, L.; Johnell, K. Impact of Inappropriate Drug Use on Hospitalizations, Mortality, and Costs in Older Persons and Persons with Dementia: Findings from the SNAC Study. Drugs Aging 2015, 32, 671–678. [Google Scholar] [CrossRef]
- Lyketsos, C.G.; Lopez, O.; Jones, B.; Fitzpatrick, A.L.; Breitner, J.; Dekosky, S. Prevalence of neuropsychiatric symptoms in dementia and mild cognitive impairment: Results from the cardiovascular health study. JAMA 2002, 288, 1475–1483. [Google Scholar] [CrossRef]
- Kaufer, D.I.; Cummings, J.L.; Christine, D.; Bray, T.; Castellon, S.; Masterman, D.; MacMillan, A.; Ketchel, P.; DeKosky, S.T. Assessing the impact of neuropsychiatric symptoms in Alzheimer’s disease: The Neuropsychiatric Inventory Caregiver Distress Scale. J. Am. Geriatr. Soc. 1998, 46, 210–215. [Google Scholar] [CrossRef]
- Gauthier, S.; Molinuevo, J.L. Benefits of combined cholinesterase inhibitor and memantine treatment in moderate-severe Alzheimer’s disease. Alzheimers Dement 2013, 9, 326–331. [Google Scholar] [CrossRef]
- Krolak-Salmon, P.; Dubois, B.; Sellal, F.; Delabrousse-Mayoux, J.P.; Vandel, P.; Amieva, H.; Jeandel, C.; Andrieu, S.; Perret-Liaudet, A. France Will No More Reimburse Available Symptomatic Drugs against Alzheimer’s Disease. J. Alzheimers Dis. 2018, 66, 425–427. [Google Scholar] [CrossRef]
- Moore, T.J.; Mattison, D.R. Adult Utilization of Psychiatric Drugs and Differences by Sex, Age, and Race. JAMA Intern. Med. 2017, 177, 274–275. [Google Scholar] [CrossRef] [PubMed]
- Maust, D.T.; Strominger, J.; Bynum, J.P.W.; Langa, K.M.; Gerlach, L.B.; Zivin, K.; Marcus, S.C. Prevalence of Psychotropic and Opioid Prescription Fills among Community-Dwelling Older Adults with Dementia in the US. JAMA 2020, 324, 706–709. [Google Scholar] [CrossRef] [PubMed]
- Maust, D.T.; Gerlach, L.B.; Gibson, A.; Kales, H.C.; Blow, F.C.; Olfson, M. Trends in Central Nervous System-Active Polypharmacy among Older Adults Seen in Outpatient Care in the United States. JAMA Intern. Med. 2017, 177, 583–585. [Google Scholar] [CrossRef] [PubMed]
- Fick, D.M.; Semla, T.P.; Steinman, M.; Beizer, J.; Brandt, N.; Dombrowski, R.; DuBeau, C.E.; Pezzullo, L.; Epplin, J.J.; Flanagan, N.; et al. American Geriatrics Society 2019 Updated AGS Beers Criteria® for Potentially Inappropriate Medication Use in Older Adults. J. Am. Geriatr. Soc. 2019, 67, 674–694. [Google Scholar] [CrossRef]
- Girotra, P.; Behl, T.; Sehgal, A.; Singh, S.; Bungau, S. Investigation of the Molecular Role of Brain-Derived Neurotrophic Factor in Alzheimer’s Disease. J. Mol. Neurosci. 2022, 72, 173–186. [Google Scholar] [CrossRef]
- Gnjidic, D.; Hilmer, S.N.; Hartikainen, S.; Tolppanen, A.M.; Taipale, H.; Koponen, M.; Bell, J.S. Impact of high risk drug use on hospitalization and mortality in older people with and without Alzheimer’s disease: A national population cohort study. PLoS ONE 2014, 9, 1–8. [Google Scholar] [CrossRef]
- Thorpe, J.M.; Thorpe, C.T.; Gellad, W.F.; Good, C.B.; Hanlon, J.T.; Mor, M.K.; Pleis, J.R.; Schleiden, L.J.; Van Houtven, C.H. Dual Health Care System Use and High-Risk Prescribing in Patients with Dementia: A National Cohort Study. Ann. Intern. Med. 2017, 166, 157–163. [Google Scholar] [CrossRef]
- Bayliss, E.A.; Shetterly, S.M.; Drace, M.L.; Norton, J.; Green, A.R.; Reeve, E.; Weffald, L.A.; Wright, L.; Maciejewski, M.L.; Sheehan, O.C.; et al. The OPTIMIZE patient- and family-centered, primary care-based deprescribing intervention for older adults with dementia or mild cognitive impairment and multiple chronic conditions: Study protocol for a pragmatic cluster randomized controlled trial. Trials 2020, 21, 542. [Google Scholar] [CrossRef]
- Rasu, R.S.; Shrestha, N.; Karpes Matusevich, A.R.; Zalmai, R.; Large, S.; Johnson, L.; O’Bryant, S.E. Polypharmacy and Cognition Function among Rural Adults. J. Alzheimers Dis. 2021, 82, 607–619. [Google Scholar] [CrossRef]
- Stoehr, G.P.; Lu, S.Y.; Lavery, L.; Bilt J vander Saxton, J.A.; Chang, C.C.H.; Ganguli, M. Factors associated with adherence to medication regimens in older primary care patients: The Steel Valley Seniors Survey. Am. J. Geriatr. Pharm. 2008, 6, 255–263. [Google Scholar] [CrossRef]
- Turner, B.J.; Hollenbeak, C.; Weiner, M.G.; ten Have, T.; Roberts, C. Barriers to adherence and hypertension control in a racially diverse representative sample of elderly primary care patients. Pharm. Drug Saf. 2009, 18, 672–681. [Google Scholar] [CrossRef] [PubMed]
- Gray, S.L.; Mahoney, J.E.; Blough, D.K. Medication adherence in elderly patients receiving home health services following hospital discharge. Ann. Pharm. 2001, 35, 539–545. [Google Scholar] [CrossRef]
- Chapman, R.H.; Petrilla, A.A.; Benner, J.S.; Schwartz, J.S.; Tang, S.S.K. Predictors of adherence to concomitant antihypertensive and lipid-lowering medications in older adults: A retrospective, cohort study. Drugs Aging 2008, 25, 885–892. [Google Scholar] [CrossRef]
- Ginsberg, G.; Hattis, D.; Russ, A.; Sonawane, B. Pharmacokinetic and pharmacodynamic factors that can affect sensitivity to neurotoxic sequelae in elderly individuals. Environ. Health Perspect. 2005, 113, 1243–1249. [Google Scholar] [CrossRef] [PubMed]
- McLean, A.J.; le Couteur, D.G. Aging biology and geriatric clinical pharmacology. Pharm. Rev. 2004, 56, 163–184. [Google Scholar] [CrossRef] [PubMed]
- Fülöp, T.; Wórum, I.; Csongor, J.; Fóris, G.; Leövey, A. Body composition in elderly people. I. Determination of body composition by multiisotope method and the elimination kinetics of these isotopes in healthy elderly subjects. Gerontology 1985, 31, 6–14. [Google Scholar] [CrossRef]
- Bentué-Ferrer, D.; Tribut, O.; Polard, E.; Allain, H. Clinically significant drug interactions with cholinesterase inhibitors: A guide for neurologists. CNS Drugs 2003, 17, 947–963. [Google Scholar] [CrossRef]
- Wynne, H.A.; Cope, L.H.; Mutch, E.; Rawlins, M.D.; Woodhouse, K.W.; James, O.F.W. The effect of age upon liver volume and apparent liver blood flow in healthy man. Hepatology 1989, 9, 297–301. [Google Scholar] [CrossRef]
- Zoli, M.; Magalotti, D.; Bianchi, G.; Gueli, C.; Orlandini, C.; Grimaldi, M.; Marchesini, G. Total and functional hepatic blood flow decrease in parallel with ageing. Age Ageing 1999, 28, 29–34. [Google Scholar] [CrossRef]
- Spina, E.; Scordo, M.G.; D’Arrigo, C. Metabolic drug interactions with new psychotropic agents. Fundam. Clin. Pharm. 2003, 17, 517–538. [Google Scholar] [CrossRef]
- Sweeney, B.P.; Bromilow, J. Liver enzyme induction and inhibition: Implications for anaesthesia. Anaesthesia 2006, 61, 159–177. [Google Scholar] [CrossRef] [PubMed]
- Tiseo, P.J.; Perdomo, C.A.; Friedhoff, L.T. Concurrent administration of donepezil HCl and ketoconazole: Assessment of pharmacokinetic changes following single and multiple doses. Br. J. Clin. Pharmacol. 1998, 46 (Suppl. S1), 30–34. [Google Scholar] [CrossRef]
- Huang, F.; Fu, Y. A review of clinical pharmacokinetics and pharmacodynamics of galantamine, a reversible acetylcholinesterase inhibitor for the treatment of Alzheimer’s disease, in healthy subjects and patients. Curr. Clin. Pharm. 2010, 5, 115–124. [Google Scholar] [CrossRef] [PubMed]
- Polinsky, R.J. Clinical pharmacology of rivastigmine: A new-generation acetylcholinesterase inhibitor for the treatment of Alzheimer’s disease. Clin. Ther. 1998, 20, 634–647. [Google Scholar] [CrossRef]
- Grossberg, G.T.; Stahelin, H.B.; Messina, J.C.; Anand, R.; Veach, J. Lack of adverse pharmacodynamic drug interactions with rivastigmine and twenty-two classes of medications. Int. J. Geriatr. Psychiatry 2000, 15, 242–247. [Google Scholar] [CrossRef]
- Noetzli, M.; Eap, C.B. Pharmacodynamic, pharmacokinetic and pharmacogenetic aspects of drugs used in the treatment of Alzheimer’s disease. Clin. Pharm. 2013, 52, 225–241. [Google Scholar] [CrossRef] [PubMed]
- Maekawa, Y.; Hasegawa, S.; Ishizuka, T.; Shiosakai, K.; Ishizuka, H. Pharmacokinetics and Bioequivalence of Memantine Tablet and a New Dry Syrup Formulation in Healthy Japanese Males: Two Single-Dose Crossover Studies. Adv. Ther. 2019, 36, 2930. [Google Scholar] [CrossRef]
- Freudenthaler, S.; Meineke, I.; Schreeb, K.H.; Boakye, E.; Gundert-Remy, U.; Gleiter, C.H. Influence of urine pH and urinary flow on the renal excretion of memantine. Br. J. Clin. Pharm. 1998, 46, 541–546. [Google Scholar] [CrossRef]
- Müller, F.; Weitz, D.; Derdau, V.; Sandvoss, M.; Mertsch, K.; König, J.; Fromm, M.F. Contribution of MATE1 to Renal Secretion of the NMDA Receptor Antagonist Memantine. Mol. Pharm. 2017, 14, 2991–2998. [Google Scholar] [CrossRef]
- Whitehouse, P.J.; Price, D.L.; Struble, R.G.; Clark, A.W.; Coyle, J.T.; DeLong, M.R. Alzheimer’s disease and senile dementia: Loss of neurons in the basal forebrain. Science 1982, 215, 1237–1239. [Google Scholar] [CrossRef] [PubMed]
- Roe, C.M.; Anderson, M.J.; Spivack, B. Use of anticholinergic medications by older adults with dementia. J. Am. Geriatr. Soc. 2002, 50, 836–842. [Google Scholar] [CrossRef] [PubMed]
- Carnahan, R.M.; Lund, B.C.; Perry, P.J.; Chrischilles, E.A. The concurrent use of anticholinergics and cholinesterase inhibitors: Rare event or common practice? J. Am. Geriatr. Soc. 2004, 52, 2082–2087. [Google Scholar] [CrossRef] [PubMed]
- Shepherd, G.; Klein-Schwartz, W.; Edwards, R. Donepezil overdose: A tenfold dosing error. Ann. Pharm. 1999, 33, 812–815. [Google Scholar] [CrossRef] [PubMed]
- Hong, Y.J.; Han, H.J.; Youn, Y.C.; Park, K.W.; Yang, D.W.; Kim, S.; Kim, H.J.; Kim, J.E.; Lee, J.H. Safety and tolerability of donepezil 23 mg with or without intermediate dose titration in patients with Alzheimer’s disease taking donepezil 10 mg: A multicenter, randomized, open-label, parallel-design, three-arm, prospective trial. Alzheimers Res. Ther. 2019, 11, 37. [Google Scholar] [CrossRef]
- Herrmann, N.; Li, A.; Lanctôt, K. Memantine in dementia: A review of the current evidence. Expert Opin. Pharm. 2011, 12, 787–800. [Google Scholar] [CrossRef] [PubMed]
- Spanagel, R.; Eilbacher, B.; Wilke, R. Memantine-induced dopamine release in the prefrontal cortex and striatum of the rat—A pharmacokinetic microdialysis study. Eur. J. Pharm. 1994, 262, 21–26. [Google Scholar] [CrossRef]
- Miller, E.K. The prefrontal cortex and cognitive control. Nat. Rev. Neurosci. 2000, 1, 59–65. [Google Scholar] [CrossRef]
- Davis, K.L.; Kahn, R.S.; Ko, G.; Davidson, M. Dopamine in schizophrenia: A review and reconceptualization. Am. J. Psychiatry 1991, 148, 1474–1486. [Google Scholar] [CrossRef]
- Hassanpour, F.; Zarghami, M.; Mouodi, S.; Moosazadeh, M.; Barzegar, F.; Bagheri, M.; Hendouei, N. Adjunctive Memantine Treatment of Schizophrenia: A Double-Blind, Randomized Placebo-Controlled Study. J. Clin. Psychopharmacol. 2019, 39, 634–638. [Google Scholar] [CrossRef] [PubMed]
- Sandström, K.O.; Baltzersen, O.B.; Marsman, A.; Lemvigh, C.K.; Boer, V.O.; Bojesen, K.B.; Nielsen, M.Ø.; Lundell, H.; Sulaiman, D.K.; Sørensen, M.E.; et al. Add-on MEmaNtine to Dopamine Antagonism to Improve Negative Symptoms at First Psychosis—the AMEND Trial Protocol. Front. Psychiatry 2022, 13. [Google Scholar] [CrossRef]

| Drugs | Extinction Pathway | Mechanisms of Drug Interactions | Typical Drugs in Drug Interactions |
|---|---|---|---|
| Donepezil Galantamine | Hepatic metabolism (CYP3A4 and CYP2D6) | Inhibition of CYP3A4 | ketoconazole, itraconazole, erythromycin, ritonavir, atazanavir |
| Inhibition of CYP2D6 (especially, in galantamine) | bupropion, fluoxetine, paroxetine, quinidine | ||
| Induction of CYP3A4 | carbamazepine, phenytoin, rifampin | ||
| Rivastigmine | Metabolism by blood esterase | not reported | |
| Memantine | Urinary excretion | Change in urinary pH | acetazolamide, citric acid, sodium bicarbonate |
| Drugs | Mechanisms of Drug Interactions | Typical Drugs in Drug Interactions |
|---|---|---|
| Donepezil Galantamine Rivastigmine | Attenuation of antidementia drugs by anticholinergic action | trihexyphenidyl, biperiden, butylscopolamine, atropine amitriptyline, clomipramine |
| Enhanced peripheral cholinergic stimulation by cholinergic agonist | acetylcholine, betanechol, distigmine, neostigmine | |
| Memantine | Enhancement of NMDA receptor antagonism | amantadine, ketamine, dextromethorphan |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Esumi, S.; Ushio, S.; Zamami, Y. Polypharmacy in Older Adults with Alzheimer’s Disease. Medicina 2022, 58, 1445. https://doi.org/10.3390/medicina58101445
Esumi S, Ushio S, Zamami Y. Polypharmacy in Older Adults with Alzheimer’s Disease. Medicina. 2022; 58(10):1445. https://doi.org/10.3390/medicina58101445
Chicago/Turabian StyleEsumi, Satoru, Soichiro Ushio, and Yoshito Zamami. 2022. "Polypharmacy in Older Adults with Alzheimer’s Disease" Medicina 58, no. 10: 1445. https://doi.org/10.3390/medicina58101445
APA StyleEsumi, S., Ushio, S., & Zamami, Y. (2022). Polypharmacy in Older Adults with Alzheimer’s Disease. Medicina, 58(10), 1445. https://doi.org/10.3390/medicina58101445






