Nitric Oxide Synthase Inhibitors as Antidepressants
Abstract
:1. Introduction
2. General aspects of Nitric Oxide
2.1. The Nitric Oxide Synthase enzymes
- is the NOS first identified in neurons and which is dependent of elevated Ca2+.
- is the NOS which is independent of elevated Ca2+.
- is the NOS first identified in endothelial cells and which is dependent of elevated Ca2+.
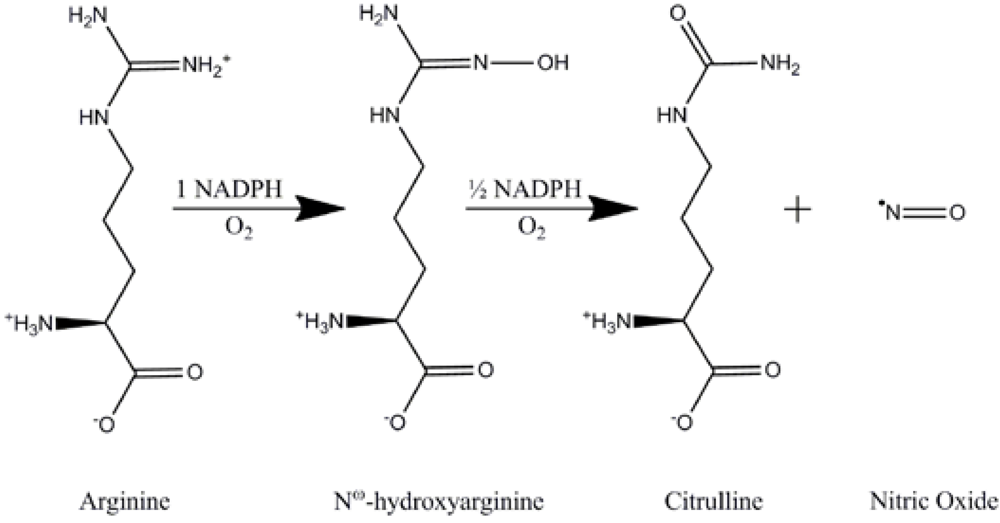
2.2. Synthesis of NO
2.3. Localization of NOS in the CNS
2.4. Regulation of NOS activity
2.5. Targets of NO
3. NO and Psychiatric Disorders
4. NOS inhibitors: Evidence for Efficacy in Depression and Anxiety
4.1. NOS inhibiting amino acids.
| INHIBITORAMINO ACIDS | ENZYME/POTENCY | DRUG STRUCTURE | DEPRES-SION | ANXIETY | DRUG REF |
| L-NMMA or L-NANA (L-NG-Methyl-L-arginine) | nNOS=eNOS>>iNOS |  | [70] | - | [68] |
| N-PLA (L-NG-Propyl-L-arginine) | nNOS>>eNOS>>iNOS |  | - | - | [75] |
| L-NNA (L-NG-Nitroarginine ) | nNOS>eNOS>>>iNOS |  | [69,70,72,76,77,78] | [79,80,81] | [68] |
| L-NAME (L-NG-Nitroarginine methyl ester) | nNOS>eNOS>iNOS |  | [70,71,82,83,84,85,86] | [81,87,88,89,90] | [68] |
| L-NAA NG-Amino-L-arginine | nNOS>eNOS>iNOS |  | - | - | [91] |
| ADMA (NG,NG-Dimethyl-L-arginine) | - |  | [92] | - | [93,94] |
| SDMA (NG,NG′-Dimethyl-L-arginine) | - |  | |||
| L-NIL (L-N6-(1-Imino-ethyl)lysine) | iNOS>>nNOS |  | - | - | [95] |
| L-Thiocitrulline | nNOS>iNOS>eNOS |  | - | - | [96] |
| S-Methyl-L-Thiocitrulline | nNOS>eNOS>iNOS |  | - | - | [97] |
| Agmatine (1-Amino-4-guanidinobutane) | Unspecific NOS inhibitor and ligand at imidazoline receptors |  | [98,99,100,101,102,103,104,105] | [102,106,107] | [108] |
| L-Canavanine | iNOS |  | - | - | [109] |
| AMIDINES | |||||
| L-NIO Nδ-(Iminoethyl)-L-ornithine | nNOS>eNOS=iNOS |  | - | - | [110] |
| Ethyl-L-NIO | nNOS>iNOS>eNOS |  | - | - | [111] |
| Vinyl-L-NIO | nNOS>>eNOS>iNOS |  | - | - | [111] |
| 1400W (N-(3-(Aminomethyl)benzyl)acetamidine) | iNOS>>>nNOS>eNOS |  | - | - | [112] |
| INDAZOLE DERIVATES | |||||
| 7-NI (7-Nitroindazole) | nNOS=eNOS>>iNOS |  | [72,89,113,114,115,116,117,118] | [89,119,120,121,122,123] | [124,125] |
| 7-NI-Br (7-Bromonitroindazole) | nNOS>eNOS>iNOS |  | |||
| IMIDAZOLE DERIVATES | |||||
| TRIM (1-[2-(Trifluoromethyl)phenyl-imidazole | iNOS=nNOS>eNOS |  | [115,126,127] | [128]. | [129] |
| 2-IMINOPIPERIDINE DERIVATES | |||||
| 2-Imino-4-methylpiperidine | iNOS>nNOS>eNOS |  | - | - | [130] |
| HYDRAZINE DERIVATES | |||||
| Aminoguanidine | iNOS>>nNOS |  | [98,131], [132] | [133] | [134] |
| ISOTHIOUREAS | |||||
| S-(2-Aminoethyl) isothiourea | iNOS=nNOS=eNOS |  | - | - | [135] |
| 1,3-PBIT (S,S'-(1,3-Phenylene-bis(1,2-ethanediyl))bis-isothiourea) | iNOS>>nNOS>eNOS |  | - | - | [135] |
| 1,4-PBIT (S,S'-(1,4-Phenylene-bis(1,2-ethanediyl))bis-isothiourea) | iNOS>nNOS>>eNOS |  | - | - | [135] |
| α-Guanidinoglutaric Acid | - |  | - | - | [136] |
| OTHER/MIXED | |||||
| Methylene blue | NNOS=eNOS=iNOS, sGC, MAO |  | [118,137,138,139,140] | [137,141] | |
| ODQ ( [1H-[1,2,4]Oxadiazole[4,3-a]quinoxalin-1-one] - | Inhibits NO sensitive cGMP formation |  | [116,142]. | [121] | |
4.2. Indazoles and Imidazole derivates
4.3. Hydrazine derivates and amidines
4.4. Other compounds/mixed
5. Interactions between NO and the Conventional Neurotransmitters
6. Conclusions
Acknowledgements
References and Notes
- Olesen, J.; Leonardi, M. The burden of brain diseases in Europe. Eur. J. Neurol. 2003, 10, 471–477. [Google Scholar] [CrossRef] [PubMed]
- Olesen, J.; Sobscki, P.; Truelsen, T.; Sestoft, D.; Jonsson, B. Cost of disorders of the brain in Denmark. Nord. J. Psychiatry 2008, 62, 114–120. [Google Scholar] [CrossRef] [PubMed]
- Caspi, A.; Sugden, K.; Moffitt, T.E.; Taylor, A.; Craig, I.W.; Harrington, H.; McClay, J.; Mill, J.; Martin, J.; Braithwaite, A.; Poulton, R. Influence of life stress on depression: moderation by a polymorphism in the 5-HTT gene. Science 2003, 301, 386–389. [Google Scholar] [CrossRef] [PubMed]
- Palmer, R.M.; Ferrige, A.G.; Moncada, S. Nitric oxide release accounts for the biological activity of endothelium-derived relaxing factor. Nature 1987, 327, 524–526. [Google Scholar] [CrossRef] [PubMed]
- Hibbs Jr., J.B.; Taintor, R.R.; Vavrin, Z. Macrophage cytotoxicity: role for L-arginine deiminase and imino nitrogen oxidation to nitrite . Science 1987, 235, 473–476. [Google Scholar] [PubMed]
- Bredt, D.S.; Snyder, S.H. Nitric oxide mediates glutamate-linked enhancement of cGMP levels in the cerebellum. Proc. Natl. Acad. Sci. USA 1989, 86, 9030–9033. [Google Scholar] [CrossRef]
- Garthwaite, J.; Garthwaite, G.; Palmer, R.M.; Moncada, S. NMDA receptor activation induces nitric oxide synthesis from arginine in rat brain slices. Eur. J. Pharmacol. 1989, 172, 413–416. [Google Scholar] [CrossRef] [PubMed]
- Knott, A.B.; Bossy-Wetzel, E. Nitric oxide in health and disease of the nervous system . Antioxid. Redox Signal. 2009, 11. [Google Scholar]
- Oosthuizen, F.; Wegener, G.; Harvey, B.H. Nitric oxide as inflammatory mediator in post-traumatic stress disorder (PTSD): evidence from an animal model. Neuropsychiat. Dis. Treatm. 2005, 1, 109–123. [Google Scholar] [CrossRef]
- Reif, A.; Herterich, S.; Strobel, A.; Ehlis, A.C.; Saur, D.; Jacob, C.P.; Wienker, T.; Topner, T.; Fritzen, S.; Walter, U.; Schmitt, A.; Fallgatter, A.J.; Lesch, K.P. A neuronal nitric oxide synthase (NOS-I) haplotype associated with schizophrenia modifies prefrontal cortex function. Mol. Psychiatry 2006, 11, 286–300. [Google Scholar] [CrossRef] [PubMed]
- Reif, A.; Jacob, C.P.; Rujescu, D.; Herterich, S.; Lang, S.; Gutknecht, L.; Baehne, C.G.; Strobel, A.; Freitag, C.M.; Giegling, I.; Romanos, M.; Hartmann, A.; Rosler, M.; Renner, T.J.; Fallgatter, A.J.; Retz, W.; Ehlis, A.C.; Lesch, K.P. Influence of functional variant of neuronal nitric oxide synthase on impulsive behaviors in humans. Arch. Gen. Psychiatry 2009, 66, 41–50. [Google Scholar] [CrossRef] [PubMed]
- Beckman, J.S. The Physiological and Pathological Chemistry of Nitric Oxide. In Nitric Oxide: Principles and Actions. Lancaster, J., Ed.; Academic Press, Inc.: San Diego, CA, USA, 1996; pp. 1–82. [Google Scholar]
- Stuehr, D.J.; Cho, H.J.; Kwon, N.S.; Weise, M.F.; Nathan, C.F. Purification and characterization of the cytokine-induced macrophage nitric oxide synthase: an FAD- and FMN-containing flavoprotein. Proc. Natl. Acad. Sci. USA 1991, 88, 7773–7777. [Google Scholar] [CrossRef]
- Bredt, D.S.; Snyder, S.H. Nitric oxide: a physiologic messenger molecule. Annu. Rev. Biochem. 1994, 63, 175–195. [Google Scholar] [PubMed]
- Garthwaite, J.; Charles, S.L.; Chess-Williams, R. Endothelium-derived relaxing factor release on activation of NMDA receptors suggests role as intercellular messenger in the brain. Nature 1988, 336, 385–388. [Google Scholar] [CrossRef] [PubMed]
- Kerwin Jr., J.F.; Heller, M. The arginine-nitric oxide pathway: a target for new drugs . Med. Res. Rev. 1994, 14, 23–74. [Google Scholar] [PubMed]
- Marletta, M.A. Nitric oxide synthase structure and mechanism. J. Biol. Chem. 1993, 268, 12231–12234. [Google Scholar] [PubMed]
- Moncada, S.; Palmer, R.M.; Higgs, E.A. Biosynthesis of nitric oxide from L-arginine. A pathway for the regulation of cell function and communication. Biochem. Pharmacol 1989, 38, 1709–1715. [Google Scholar] [CrossRef] [PubMed]
- Nathan, C. Nitric oxide as a secretory product of mammalian cells. FASEB J. 1992, 6, 3051–3064. [Google Scholar] [PubMed]
- Forstermann, U.; Schmidt, H.H.; Pollock, J.S.; Sheng, H.; Mitchell, J.A.; Warner, T.D.; Nakane, M.; Murad, F. Isoforms of nitric oxide synthase. Characterization and purification from different cell types. Biochem. Pharmacol. 1991, 42, 1849–1857. [Google Scholar] [CrossRef] [PubMed]
- Forstermann, U.; Gath, I.; Schwarz, P.; Closs, E.I.; Kleinert, H. Isoforms of nitric oxide synthase. Properties, cellular distribution and expressional control. Biochem.Pharmacol. 1995, 50, 1321–1332. [Google Scholar] [CrossRef] [PubMed]
- O'Dell, T.J.; Hawkins, R.D.; Kandel, E.R.; Arancio, O. Tests of the roles of two diffusible substances in long-term potentiation: evidence for nitric oxide as a possible early retrograde messenger. Proc. Natl. Acad. Sci. USA 1991, 88, 11285–11289. [Google Scholar] [CrossRef]
- Dawson, T.M.; Snyder, S.H. Gases as biological messengers: nitric oxide and carbon monoxide in the brain. J. Neurosci. 1994, 14, 5147–5159. [Google Scholar] [PubMed]
- Knowles, R.G.; Moncada, S. Nitric oxide synthases in mammals . Biochem. J. 1994, 298 (Pt. 2), 249–258. [Google Scholar] [PubMed]
- Blottner, D.; Grozdanovic, Z.; Gossrau, R. Histochemistry of nitric oxide synthase in the nervous system. Histochem.J. 1995, 27, 785–811. [Google Scholar] [PubMed]
- de Vente, J.; Hopkins, D.A.; Markerink-Van, I.M.; Emson, P.C.; Schmidt, H.H.; Steinbusch, H.W. Distribution of nitric oxide synthase and nitric oxide-receptive, cyclic GMP-producing structures in the rat brain. Neuroscience 1998, 87, 207–241. [Google Scholar] [CrossRef] [PubMed]
- Hara, H.; Waeber, C.; Huang, P.L.; Fujii, M.; Fishman, M.C.; Moskowitz, M.A. Brain distribution of nitric oxide synthase in neuronal or endothelial nitric oxide synthase mutant mice using [3H]L-NG-nitro-arginine autoradiography. Neuroscience 1996, 75, 881–890. [Google Scholar] [CrossRef] [PubMed]
- Barjavel, M.J.; Bhargava, H.N. Nitric oxide synthase activity in brain regions and spinal cord of mice and rats: kinetic analysis. Pharmacology 1995, 50, 168–174. [Google Scholar] [CrossRef] [PubMed]
- Salter, M.; Duffy, C.; Garthwaite, J.; Strijbos, P.J. Substantial regional and hemispheric differences in brain nitric oxide synthase (NOS) inhibition following intracerebroventricular administration of N omega-nitro-L-arginine (L-NA) and its methyl ester (L-NAME). Neuropharmacology 1995, 34, 639–649. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.D.; Ma, P.M. Localization of NADPH diaphorase activity in monoaminergic neurons of the rat brain. J. Comp. Neurol. 1993, 332, 391–406. [Google Scholar] [CrossRef] [PubMed]
- Simonian, S.X.; Herbison, A.E. Localization of neuronal nitric oxide synthase-immunoreactivity within sub-populations of noradrenergic A1 and A2 neurons in the rat. Brain Res. 1996, 732, 247–252. [Google Scholar] [CrossRef] [PubMed]
- Valtschanoff, J.G.; Weinberg, R.J.; Kharazia, V.N.; Schmidt, H.H.; Nakane, M.; Rustioni, A. Neurons in rat cerebral cortex that synthesize nitric oxide: NADPH diaphorase histochemistry, NOS immunocytochemistry, and colocalization with GABA. Neurosci. Lett. 1993, 157, 157–161. [Google Scholar] [CrossRef] [PubMed]
- Kowall, N.W.; Ferrante, R.J.; Beal, M.F.; Richardson Jr., E.P.; Sofroniew, M.V.; Cuello, A.C.; Martin, J.B. Neuropeptide Y, somatostatin, and reduced nicotinamide adenine dinucleotide phosphate diaphorase in the human striatum: a combined immunocytochemical and enzyme histochemical study. Neuroscience 1987, 20, 817–828. [Google Scholar] [CrossRef] [PubMed]
- O'Dell, T.J.; Huang, P.L.; Dawson, T.M.; Dinerman, J.L.; Snyder, S.H.; Kandel, E.R.; Fishman, M.C. Endothelial NOS and the blockade of LTP by NOS inhibitors in mice lacking neuronal NOS. Science 1994, 265, 542–546. [Google Scholar] [PubMed]
- Kano, T.; Shimizu-Sasamata, M.; Huang, P.L.; Moskowitz, M.A.; Lo, E.H. Effects of nitric oxide synthase gene knockout on neurotransmitter release in vivo. Neuroscience 1998, 86, 695–699. [Google Scholar] [CrossRef] [PubMed]
- Yoshida, T.; Waeber, C.; Huang, Z.; Moskowitz, M.A. Induction of nitric oxide synthase activity in rodent brain following middle cerebral artery occlusion. Neurosci. Lett. 1995, 194, 214–218. [Google Scholar] [CrossRef] [PubMed]
- Nathan, C.; Xie, Q.W. Regulation of biosynthesis of nitric oxide. J. Biol. Chem. 1994, 269, 13725–13728. [Google Scholar] [PubMed]
- Schmidt, H.H.; Lohmann, S.M.; Walter, U. The nitric oxide and cGMP signal transduction system: regulation and mechanism of action. Biochim. Biophys. Acta 1993, 1178, 153–175. [Google Scholar] [CrossRef] [PubMed]
- Hindley, S.; Juurlink, B.H.; Gysbers, J.W.; Middlemiss, P.J.; Herman, M.A.; Rathbone, M.P. Nitric oxide donors enhance neurotrophin-induced neurite outgrowth through a cGMP-dependent mechanism. J. Neurosci. Res. 1997, 47, 427–439. [Google Scholar] [CrossRef] [PubMed]
- Contestabile, A. Roles of NMDA receptor activity and nitric oxide production in brain development. Brain Res. Rev. 2000, 32, 476–509. [Google Scholar] [CrossRef]
- Hess, D.T.; Patterson, S.I.; Smith, D.S.; Skene, J.H. Neuronal growth cone collapse and inhibition of protein fatty acylation by nitric oxide. Nature 1993, 366, 562–565. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, H.H.; Pollock, J.S.; Nakane, M.; Forstermann, U.; Murad, F. Ca2+/calmodulin-regulated nitric oxide synthases. Cell Calcium 1992, 13, 427–434. [Google Scholar] [CrossRef] [PubMed]
- Lowenstein, C.J.; Snyder, S.H. Nitric oxide, a novel biologic messenger. Cell 1992, 70, 705–707. [Google Scholar] [CrossRef] [PubMed]
- Assreuy, J.; Cunha, F.Q.; Liew, F.Y.; Moncada, S. Feedback inhibition of nitric oxide synthase activity by nitric oxide. Br. J. Pharmacol. 1993, 108, 833–837. [Google Scholar] [PubMed]
- Buga, G.M.; Griscavage, J.M.; Rogers, N.E.; Ignarro, L.J. Negative feedback regulation of endothelial cell function by nitric oxide. Circ.Res. 1993, 73, 808–812. [Google Scholar] [PubMed]
- Rengasamy, A.; Johns, R.A. Regulation of nitric oxide synthase by nitric oxide. Mol. Pharmacol. 1993, 44, 124–128. [Google Scholar] [PubMed]
- Gaston, B.M.; Carver, J.; Doctor, A.; Palmer, L.A. S-nitrosylation signaling in cell biology. Mol. Interv. 2003, 3, 253–263. [Google Scholar] [CrossRef] [PubMed]
- Denninger, J.W.; Marletta, M.A. Guanylate cyclase and the .NO/cGMP signaling pathway . Biochim. Biophys. Acta 1999, 1411, 334–350. [Google Scholar] [PubMed]
- Miki, N.; Kawabe, Y.; Kuriyama, K. Activation of cerebral guanylate cyclase by nitric oxide. Biochem. Biophys. Res. Commun. 1977, 75, 851–856. [Google Scholar] [CrossRef] [PubMed]
- Laitinen, J.T.; Laitinen, K.S.; Tuomisto, L.; Airaksinen, M.M. Differential regulation of cyclic GMP levels in the frontal cortex and the cerebellum of anesthetized rats by nitric oxide: an in vivo microdialysis study. Brain Res. 1994, 668, 117–121. [Google Scholar] [CrossRef] [PubMed]
- Luo, D.; Vincent, S.R. NMDA-dependent nitric oxide release in the hippocampus in vivo: interactions with noradrenaline. Neuropharmacology 1994, 33, 1345–1350. [Google Scholar] [CrossRef] [PubMed]
- Vallebuona, F.; Raiteri, M. Extracellular cGMP in the hippocampus of freely moving rats as an index of nitric oxide (NO) synthase activity. J. Neurosci. 1994, 14, 134–139. [Google Scholar] [PubMed]
- Yun, H.Y.; Gonzalez-Zulueta, M.; Dawson, V.L.; Dawson, T.M. Nitric oxide mediates N-methyl-D-aspartate receptor-induced activation of p21ras. Proc. Natl. Acad. Sci. USA 1998, 95, 5773–5778. [Google Scholar] [CrossRef]
- Dawson, T.M.; Sasaki, M.; Gonzalez-Zulueta, M.; Dawson, V.L. Regulation of neuronal nitric oxide synthase and identification of novel nitric oxide signaling pathways. Prog. Brain Res. 1998, 118, 3–11. [Google Scholar]
- Dawson, T.M.; Dawson, V.L. ADP-ribosylation as a mechanism for the action of nitric oxide in the nervous system. New Horiz. 1995, 3, 85–92. [Google Scholar]
- Garthwaite, J.; Boulton, C.L. Nitric oxide signaling in the central nervous system. Annu. Rev. Physiol 1995, 57, 683–706. [Google Scholar] [PubMed]
- Stamler, J.S. Redox signaling: nitrosylation and related target interactions of nitric oxide. Cell 1994, 78, 931–936. [Google Scholar] [CrossRef] [PubMed]
- Stamler, J.S. S-nitrosothiols and the bioregulatory actions of nitrogen oxides through reactions with thiol groups. Curr. Top. Microbiol. Immunol. 1995, 196, 19–36. [Google Scholar] [PubMed]
- Stamler, J.S.; Lamas, S.; Fang, F.C. Nitrosylation. the prototypic redox-based signaling mechanism. Cell 2001, 106, 675–683. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, H.G.; Heinemann, A.; Krell, D.; Dobrowolny, H.; Bielau, H.; Keilhoff, G.; Bogerts, B. Hypothalamic nitric oxide synthase in affective disorder: focus on the suprachiasmatic nucleus. Cell. Mol. Biol. (Noisy-le-grand) 2005, 51, 279–284. [Google Scholar] [PubMed]
- Bernstein, H.G.; Stanarius, A.; Baumann, B.; Henning, H.; Krell, D.; Danos, P.; Falkai, P.; Bogerts, B. Nitric oxide synthase-containing neurons in the human hypothalamus: reduced number of immunoreactive cells in the paraventricular nucleus of depressive patients and schizophrenics. Neuroscience 1998, 83, 867–875. [Google Scholar] [CrossRef] [PubMed]
- Oliveira, R.M.; Guimaraes, F.S.; Deakin, J.F. Expression of neuronal nitric oxide synthase in the hippocampal formation in affective disorders. Braz. J. Med. Biol. Res. 2008, 41, 333–341. [Google Scholar] [PubMed]
- Lee, B.H.; Lee, S.W.; Yoon, D.; Lee, H.J.; Yang, J.C.; Shim, S.H.; Kim, D.H.; Ryu, S.H.; Han, C.; Kim, Y.K. Increased plasma nitric oxide metabolites in suicide attempters. Neuropsychobiology 2006, 53, 127–132. [Google Scholar] [CrossRef] [PubMed]
- Chrapko, W.E.; Jurasz, P.; Radomski, M.W.; Lara, N.; Archer, S.L.; Le Melledo, J.M. Decreased platelet nitric oxide synthase activity and plasma nitric oxide metabolites in major depressive disorder. Biol. Psychiatry 2004, 56, 129–134. [Google Scholar] [CrossRef] [PubMed]
- Chrapko, W.; Jurasz, P.; Radomski, M.W.; Archer, S.L.; Newman, S.C.; Baker, G.; Lara, N.; Le Melledo, J.M. Alteration of decreased plasma NO metabolites and platelet NO synthase activity by paroxetine in depressed patients. Neuropsychopharmacol. 2006, 31, 1286–1293. [Google Scholar]
- Yanik, M.; Vural, H.; Tutkun, H.; Zoroglu, S.S.; Savas, H.A.; Herken, H.; Kocyigit, A.; Keles, H.; Akyol, O. The role of the arginine-nitric oxide pathway in the pathogenesis of bipolar affective disorder. Eur.Arch.Psychiatry Clin.Neurosci. 2004, 254, 43–47. [Google Scholar] [CrossRef] [PubMed]
- Reif, A.; Strobel, A.; Jacob, C.P.; Herterich, S.; Freitag, C.M.; Topner, T.; Mossner, R.; Fritzen, S.; Schmitt, A.; Lesch, K.P. A NOS-III haplotype that includes functional polymorphisms is associated with bipolar disorder. Int. J. Neuropsychopharmacol. 2006, 9, 13–20. [Google Scholar] [CrossRef] [PubMed]
- Griffith, O.W.; Kilbourn, R.G. Nitric oxide synthase inhibitors: amino acids. Methods Enzymol. 1996, 268, 375–392. [Google Scholar] [PubMed]
- da Silva, G.D.; Matteussi, A.S.; dos Santos, A.R.; Calixto, J.B.; Rodrigues, A.L. Evidence for dual effects of nitric oxide in the forced swimming test and in the tail suspension test in mice. Neuroreport 2000, 11, 3699–3702. [Google Scholar] [CrossRef] [PubMed]
- Harkin, A.J.; Bruce, K.H.; Craft, B.; Paul, I.A. Nitric oxide synthase inhibitors have antidepressant-like properties in mice. 1. Acute treatments are active in the forced swim test. Eur. J. Pharmacol. 1999, 372, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Jefferys, D.; Funder, J. Nitric oxide modulates retention of immobility in the forced swimming test in rats. Eur. J. Pharmacol. 1996, 295, 131–135. [Google Scholar] [CrossRef] [PubMed]
- Harkin, A.; Connor, T.J.; Walsh, M.; St John, N.; Kelly, J.P. Serotonergic mediation of the antidepressant-like effects of nitric oxide synthase inhibitors. Neuropharmacol. 2003, 44, 616–623. [Google Scholar] [CrossRef]
- Karolewicz, B.; Paul, I.A.; Antkiewicz-Michaluk, L. Effect of NOS inhibitor on forced swim test and neurotransmitters turnover in the mouse brain. Pol. J. Pharmacol. 2001, 53, 587–596. [Google Scholar] [PubMed]
- Inan, S.Y.; Yalcin, I.; Aksu, F. Dual effects of nitric oxide in the mouse forced swimming test: possible contribution of nitric oxide-mediated serotonin release and potassium channel modulation. Pharmacol. Biochem. Behav. 2004, 77, 457–464. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.Q.; Fast, W.; Marletta, M.A.; Martasek, P.; Silverman, R.B. Potent and selective inhibition of neuronal nitric oxide synthase by N omega-propyl-L-arginine. J. Med. Chem. 1997, 40, 3869–3870. [Google Scholar] [CrossRef] [PubMed]
- Bohme, G.A.; Bon, C.; Lemaire, M.; Reibaud, M.; Piot, O.; Stutzmann, J.M.; Doble, A.; Blanchard, J.C. Altered synaptic plasticity and memory formation in nitric oxide synthase inhibitor-treated rats. Proc. Natl. Acad. Sci. USA 1993, 90, 9191–9194. [Google Scholar] [CrossRef]
- Mogensen, J.; Wortwein, G.; Gustafson, B.; Ermens, P. L-nitroarginine reduces hippocampal mediation of place learning in the rat. Neurobiol. Learn. Mem. 1995, 64, 17–24. [Google Scholar] [CrossRef] [PubMed]
- Mogensen, J.; Wortwein, G.; Hasman, A.; Nielsen, P.; Wang, Q. Functional and neurochemical profile of place learning after L-nitro-arginine in the rat. Neurobiol. Learn. Mem. 1995, 63, 54–65. [Google Scholar] [CrossRef] [PubMed]
- De Oliveira, C.L.; Del Bel, E.A.; Guimaraes, F.S. Effects of L-NOARG on plus-maze performance in rats. Pharmacol. Biochem. Behav. 1997, 56, 55–59. [Google Scholar] [CrossRef] [PubMed]
- Czech, D.A.; Jacobson, E.B.; LeSueur-Reed, K.T.; Kazel, M.R. Putative anxiety-linked effects of the nitric oxide synthase inhibitor L-NAME in three murine exploratory behavior models. Pharmacol. Biochem. Behav. 2003, 75, 741–748. [Google Scholar] [CrossRef] [PubMed]
- Pokk, P.; Vali, M. The effects of the nitric oxide synthase inhibitors on the behaviour of small-platform-stressed mice in the plus-maze test. Prog. Neuropsychopharmacol. Biol. Psychiatry 2002, 26, 241–247. [Google Scholar] [CrossRef] [PubMed]
- Sevgi, S.; Ozek, M.; Eroglu, L. L-NAME prevents anxiety-like and depression-like behavior in rats exposed to restraint stress. Methods Find. Exp. Clin. Pharmacol. 2006, 28, 95–99. [Google Scholar] [CrossRef] [PubMed]
- Chapman, P.F.; Atkins, C.M.; Allen, M.T.; Haley, J.E.; Steinmetz, J.E. Inhibition of nitric oxide synthesis impairs two different forms of learning. Neuroreport 1992, 3, 567–570. [Google Scholar] [CrossRef] [PubMed]
- Estall, L.B.; Grant, S.J.; Cicala, G.A. Inhibition of nitric oxide (NO) production selectively impairs learning and memory in the rat. Pharmacol. Biochem. Behav. 1993, 46, 959–962. [Google Scholar] [CrossRef] [PubMed]
- Ohno, M.; Yamamoto, T.; Watanabe, S. Deficits in working memory following inhibition of hippocampal nitric oxide synthesis in the rat. Brain Res. 1993, 632, 36–40. [Google Scholar] [CrossRef] [PubMed]
- Ohno, M.; Yamamoto, T.; Watanabe, S. Intrahippocampal administration of the NO synthase inhibitor L-NAME prevents working memory deficits in rats exposed to transient cerebral ischemia. Brain Res. 1994, 634, 173–177. [Google Scholar] [CrossRef] [PubMed]
- Volke, V.; Koks, S.; Vasar, E.; Bourin, M.; Bradwejn, J.; Mannisto, P.T. Inhibition of nitric oxide synthase causes anxiolytic-like behaviour in an elevated plus-maze. Neuroreport 1995, 6, 1413–1416. [Google Scholar] [CrossRef]
- Faria, M.S.; Muscara, M.N.; Moreno Junior, H.; Teixeira, S.A.; Dias, H.B.; De Oliveira, B.; Graeff, F.G.; De Nucci, G. Acute inhibition of nitric oxide synthesis induces anxiolysis in the plus maze test. Eur. J. Pharmacol. 1997, 323, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Spiacci Jr., A.; Kanamaru, F.; Guimaraes, F.S.; Oliveira, R.M. Nitric oxide-mediated anxiolytic-like and antidepressant-like effects in animal models of anxiety and depression . Pharmacol. Biochem. Behav. 2008, 88, 247–255. [Google Scholar] [PubMed]
- Guimaraes, F.S.; de Aguiar, J.C.; Del Bel, E.A.; Ballejo, G. Anxiolytic effect of nitric oxide synthase inhibitors microinjected into the dorsal central grey. Neuroreport 1994, 5, 1929–1932. [Google Scholar] [CrossRef] [PubMed]
- Fukuto, J.M.; Wood, K.S.; Byrns, R.E.; Ignarro, L.J. NG-amino-L-arginine: a new potent antagonist of L-arginine-mediated endothelium-dependent relaxation. Biochem. Biophys. Res. Commun. 1990, 168, 458–465. [Google Scholar] [CrossRef] [PubMed]
- Selley, M.L. Increased (E)-4-hydroxy-2-nonenal and asymmetric dimethylarginine concentrations and decreased nitric oxide concentrations in the plasma of patients with major depression. J. Affect. Disord. 2004, 80, 249–256. [Google Scholar] [CrossRef] [PubMed]
- Matsuoka, H.; Itoh, S.; Kimoto, M.; Kohno, K.; Tamai, O.; Wada, Y.; Yasukawa, H.; Iwami, G.; Okuda, S.; Imaizumi, T. Asymmetrical dimethylarginine, an endogenous nitric oxide synthase inhibitor, in experimental hypertension. Hypertension 1997, 29, 242–247. [Google Scholar] [PubMed]
- Matsuguma, K.; Ueda, S.; Yamagishi, S.; Matsumoto, Y.; Kaneyuki, U.; Shibata, R.; Fujimura, T.; Matsuoka, H.; Kimoto, M.; Kato, S.; Imaizumi, T.; Okuda, S. Molecular mechanism for elevation of asymmetric dimethylarginine and its role for hypertension in chronic kidney disease. J. Am. Soc. Nephrol. 2006, 17, 2176–2183. [Google Scholar] [CrossRef] [PubMed]
- Moore, W.M.; Webber, R.K.; Jerome, G.M.; Tjoeng, F.S.; Misko, T.P.; Currie, M.G. L-N6-(1-iminoethyl)lysine: a selective inhibitor of inducible nitric oxide synthase. J. Med. Chem. 1994, 37, 3886–3888. [Google Scholar] [CrossRef] [PubMed]
- Frey, C.; Narayanan, K.; McMillan, K.; Spack, L.; Gross, S.S.; Masters, B.S.; Griffith, O.W. L-thiocitrulline. A stereospecific, heme-binding inhibitor of nitric-oxide synthases. J. Biol. Chem. 1994, 269, 26083–26091. [Google Scholar] [PubMed]
- Narayanan, K.; Spack, L.; McMillan, K.; Kilbourn, R.G.; Hayward, M.A.; Masters, B.S.; Griffith, O.W. S-alkyl-L-thiocitrullines. Potent stereoselective inhibitors of nitric oxide synthase with strong pressor activity in vivo. J. Biol. Chem. 1995, 270, 11103–11110. [Google Scholar] [CrossRef] [PubMed]
- Taksande, B.G.; Kotagale, N.R.; Tripathi, S.J.; Ugale, R.R.; Chopde, C.T. Antidepressant like effect of selective serotonin reuptake inhibitors involve modulation of imidazoline receptors by agmatine. Neuropharmacology 2009, 57, 415–424. [Google Scholar] [CrossRef] [PubMed]
- Krass, M.; Wegener, G.; Vasar, E.; Volke, V. Antidepressant-like effect of agmatine is not mediated by serotonin. Behav. Brain Res. 2008, 188, 324–328. [Google Scholar] [CrossRef] [PubMed]
- Zomkowski, A.D.; Santos, A.R.; Rodrigues, A.L. Putrescine produces antidepressant-like effects in the forced swimming test and in the tail suspension test in mice. Prog. Neuropsychopharmacol. Biol. Psychiatry 2006, 30, 1419–1425. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.F.; Gong, Z.H.; Cao, J.B.; Wang, H.L.; Luo, Z.P.; Li, J. Antidepressant-like effect of agmatine and its possible mechanism. Eur. J. Pharmacol. 2003, 469, 81–88. [Google Scholar] [CrossRef] [PubMed]
- Aricioglu, F.; Altunbas, H. Is agmatine an endogenous anxiolytic/antidepressant agent? Ann. N. Y. Acad. Sci. 2003, 1009, 136–140. [Google Scholar] [CrossRef] [PubMed]
- Zomkowski, A.D.; Hammes, L.; Lin, J.; Calixto, J.B.; Santos, A.R.; Rodrigues, A.L. Agmatine produces antidepressant-like effects in two models of depression in mice. Neuroreport 2002, 13, 387–391. [Google Scholar] [CrossRef] [PubMed]
- Dias Elpo Zomkowski, A.; Oscar Rosa, A.; Lin, J.; Santos, A.R.; Calixto, J.B.; Lucia Severo Rodrigues, A. Evidence for serotonin receptor subtypes involvement in agmatine antidepressant like-effect in the mouse forced swimming test. Brain Res. 2004, 1023, 253–263. [Google Scholar] [CrossRef] [PubMed]
- Halaris, A.; Zhu, H.; Feng, Y.; Piletz, J.E. Plasma agmatine and platelet imidazoline receptors in depression. Ann. N. Y. Acad. Sci. 1999, 881, 445–451. [Google Scholar] [CrossRef] [PubMed]
- Gong, Z.H.; Li, Y.F.; Zhao, N.; Yang, H.J.; Su, R.B.; Luo, Z.P.; Li, J. Anxiolytic effect of agmatine in rats and mice. Eur. J. Pharmacol. 2006, 550, 112–116. [Google Scholar] [CrossRef] [PubMed]
- Lavinsky, D.; Arteni, N.S.; Netto, C.A. Agmatine induces anxiolysis in the elevated plus maze task in adult rats. Behav. Brain Res. 2003, 141, 19–24. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.C.; Reis, D.J. Agmatine selectively blocks the N-methyl-D-aspartate subclass of glutamate receptor channels in rat hippocampal neurons. J. Pharmacol. Exp. Ther. 1999, 288, 544–549. [Google Scholar] [PubMed]
- Levy, B.; Valtier, M.; de Chillou, C.; Bollaert, P.E.; Cane, D.; Mallie, J.P. Beneficial effects of L-canavanine, a selective inhibitor of inducible nitric oxide synthase, on lactate metabolism and muscle high energy phosphates during endotoxic shock in rats. Shock 1999, 11, 98–103. [Google Scholar] [CrossRef] [PubMed]
- Rees, D.D.; Palmer, R.M.; Schulz, R.; Hodson, H.F.; Moncada, S. Characterization of three inhibitors of endothelial nitric oxide synthase in vitro and in vivo. Br. J. Pharmacol. 1990, 101, 746–752. [Google Scholar] [PubMed]
- Babu, B.R.; Griffith, O.W. N5-(1-Imino-3-butenyl)-L-ornithine. A neuronal isoform selective mechanism-based inactivator of nitric oxide synthase. J. Biol. Chem. 1998, 273, 8882–8889. [Google Scholar] [CrossRef] [PubMed]
- Garvey, E.P.; Oplinger, J.A.; Furfine, E.S.; Kiff, R.J.; Laszlo, F.; Whittle, B.J.; Knowles, R.G. 1400W is a slow, tight binding, and highly selective inhibitor of inducible nitric-oxide synthase in vitro and in vivo. J. Biol. Chem. 1997, 272, 4959–4963. [Google Scholar] [CrossRef] [PubMed]
- Yildiz, F.; Erden, B.F.; Ulak, G.; Utkan, T.; Gacar, N. Antidepressant-like effect of 7-nitroindazole in the forced swimming test in rats. Psychopharmacology (Berl). 2000, 149, 41–44. [Google Scholar] [CrossRef] [PubMed]
- Joca, S.R.; Guimaraes, F.S. Inhibition of neuronal nitric oxide synthase in the rat hippocampus induces antidepressant-like effects. Psychopharmacology (Berl). 2006, 185, 298–305. [Google Scholar] [CrossRef] [PubMed]
- Volke, V.; Wegener, G.; Bourin, M.; Vasar, E. Antidepressant- and anxiolytic-like effects of selective neuronal NOS inhibitor 1-(2-trifluoromethylphenyl)-imidazole in mice. Behav. Brain Res. 2003, 140, 141–147. [Google Scholar] [CrossRef] [PubMed]
- Heiberg, I.L.; Wegener, G.; Rosenberg, R. Reduction of cGMP and nitric oxide has antidepressant-like effects in the forced swimming test in rats. Behav. Brain Res. 2002, 134, 479–484. [Google Scholar] [CrossRef] [PubMed]
- Holscher, C. 7-Nitro indazole, a neuron-specific nitric oxide synthase inhibitor, produces amnesia in the chick. Learn. Mem. 1994, 1, 213–216. [Google Scholar]
- Wegener, G.; Volke, V.; Bandpey, Z.; Rosenberg, R. Nitric oxide modulates lithium-induced conditioned taste aversion. Behav. Brain Res. 2001, 118, 195–200. [Google Scholar] [CrossRef] [PubMed]
- Yildiz, F.; Ulak, G.; Erden, B.F.; Gacar, N. Anxiolytic-like effects of 7-nitroindazole in the rat plus-maze test. Pharmacol. Biochem. Behav. 2000, 65, 199–202. [Google Scholar] [CrossRef] [PubMed]
- Volke, V.; Soosaar, A.; Koks, S.; Bourin, M.; Mannisto, P.T.; Vasar, E. 7-Nitroindazole, a nitric oxide synthase inhibitor, has anxiolytic-like properties in exploratory models of anxiety. Psychopharmacology (Berl). 1997, 131, 399–405. [Google Scholar] [CrossRef] [PubMed]
- Spolidorio, P.C.; Echeverry, M.B.; Iyomasa, M.; Guimaraes, F.S.; Del Bel, E.A. Anxiolytic effects induced by inhibition of the nitric oxide-cGMP pathway in the rat dorsal hippocampus. Psychopharmacology (Berl). 2007, 195, 183–192. [Google Scholar] [CrossRef] [PubMed]
- Dunn, R.W.; Reed, T.A.; Copeland, P.D.; Frye, C.A. The nitric oxide synthase inhibitor 7-nitroindazole displays enhanced anxiolytic efficacy without tolerance in rats following subchronic administration. Neuropharmacology 1998, 37, 899–904. [Google Scholar] [CrossRef] [PubMed]
- Yildiz Akar, F.; Ulak, G.; Tanyeri, P.; Erden, F.; Utkan, T.; Gacar, N. 7-Nitroindazole, a neuronal nitric oxide synthase inhibitor, impairs passive-avoidance and elevated plus-maze memory performance in rats. Pharmacol. Biochem. Behav. 2007, 87, 434–443. [Google Scholar] [CrossRef] [PubMed]
- Moore, P.K.; Babbedge, R.C.; Wallace, P.; Gaffen, Z.A.; Hart, S.L. 7-Nitro indazole, an inhibitor of nitric oxide synthase, exhibits anti-nociceptive activity in the mouse without increasing blood pressure. Br. J. Pharmacol. 1993, 108, 296–297. [Google Scholar] [PubMed]
- Bland-Ward, P.A.; Moore, P.K. 7-Nitro indazole derivatives are potent inhibitors of brain, endothelium and inducible isoforms of nitric oxide synthase . Life Sci. 1995, 57, PL131–PL135. [Google Scholar] [CrossRef] [PubMed]
- Matsumura, N.; Kikuchi-Utsumi, K.; Nakaki, T. Activities of 7-nitroindazole and 1-(2-(trifluoromethylphenyl)-imidazole independent of neuronal nitric-oxide synthase inhibition. J. Pharmacol. Exp. Ther. 2008, 325, 357–362. [Google Scholar] [CrossRef] [PubMed]
- Ulak, G.; Mutlu, O.; Akar, F.Y.; Komsuoglu, F.I.; Tanyeri, P.; Erden, B.F. Neuronal NOS inhibitor 1-(2-trifluoromethylphenyl)-imidazole augment the effects of antidepressants acting via serotonergic system in the forced swimming test in rats. Pharmacol. Biochem. Behav. 2008, 90, 563–568. [Google Scholar] [CrossRef] [PubMed]
- Mutlu, O.; Ulak, G.; Laugeray, A.; Belzung, C. Effects of neuronal and inducible NOS inhibitor 1-[2-(trifluoromethyl) phenyl] imidazole (TRIM) in unpredictable chronic mild stress procedure in mice. Pharmacol. Biochem. Behav. 2009, 92, 82–87. [Google Scholar] [CrossRef] [PubMed]
- Handy, R.L.; Moore, P.K. Mechanism of the inhibition of neuronal nitric oxide synthase by 1-(2- trifluoromethylphenyl) imidazole (TRIM) . Life Sci. 1997, 60, L389–L394. [Google Scholar] [CrossRef]
- Webber, R.K.; Metz, S.; Moore, W.M.; Connor, J.R.; Currie, M.G.; Fok, K.F.; Hagen, T.J.; Hansen, D.W.; Jerome, G.M.; Manning, P.T.; Pitzele, B.S.; Toth, M.V.; Trivedi, M.; Zupec, M.E.; Tjoeng, F.S. Substituted 2-iminopiperidines as inhibitors of human nitric oxide synthase isoforms . J. Med. Chem. 1998, 41, 96–101. [Google Scholar] [PubMed]
- Wang, D.; An, S.C.; Zhang, X. Prevention of chronic stress-induced depression-like behavior by inducible nitric oxide inhibitor. Neurosci. Lett. 2008, 433, 59–64. [Google Scholar] [CrossRef] [PubMed]
- Harvey, B.H.; Oosthuizen, F.; Brand, L.; Wegener, G.; Stein, D.J. Stress-restress evokes sustained iNOS activity and altered GABA levels and NMDA receptors in rat hippocampus. Psychopharmacology 2004, 175, 494–502. [Google Scholar] [CrossRef] [PubMed]
- Gilhotra, N.; Dhingra, D. Involvement of NO-cGMP pathway in anti-anxiety effect of aminoguanidine in stressed mice . Prog. Neuropsychopharmacol. Biol. Psychiatry 2009, 1506–1507. [Google Scholar]
- Joly, G.A.; Ayres, M.; Chelly, F.; Kilbourn, R.G. Effects of NG-methyl-L-arginine, NG-nitro-L-arginine, and aminoguanidine on constitutive and inducible nitric oxide synthase in rat aorta. Biochem. Biophys. Res. Commun. 1994, 199, 147–154. [Google Scholar] [CrossRef] [PubMed]
- Garvey, E.P.; Oplinger, J.A.; Tanoury, G.J.; Sherman, P.A.; Fowler, M.; Marshall, S.; Harmon, M.F.; Paith, J.E.; Furfine, E.S. Potent and selective inhibition of human nitric oxide synthases. Inhibition by non-amino acid isothioureas. J. Biol. Chem. 1994, 269, 26669–26676. [Google Scholar] [PubMed]
- Yokoi, I.; Kabuto, H.; Habu, H.; Mori, A. alpha-Guanidinoglutaric acid, an endogenous convulsant, as a novel nitric oxide synthase inhibitor. J. Neurochem. 1994, 63, 1565–1567. [Google Scholar] [PubMed]
- Eroglu, L.; Caglayan, B. Anxiolytic and antidepressant properties of methylene blue in animal models. Pharmacol. Res. 1997, 36, 381–385. [Google Scholar] [CrossRef] [PubMed]
- Narsapur, S.L.; Naylor, G.J. Methylene blue. A possible treatment for manic depressive psychosis. J. Affect. Disord. 1983, 5, 155–161. [Google Scholar] [CrossRef] [PubMed]
- Naylor, G.J.; Martin, B.; Hopwood, S.E.; Watson, Y. A two-year double-blind crossover trial of the prophylactic effect of methylene blue in manic-depressive psychosis. Biol. Psychiatry 1986, 21, 915–920. [Google Scholar] [CrossRef] [PubMed]
- Naylor, G.J.; Smith, A.H.; Connelly, P. A controlled trial of methylene blue in severe depressive illness. Biol. Psychiatry 1987, 22, 657–659. [Google Scholar] [CrossRef] [PubMed]
- Savegnago, L.; Jesse, C.R.; Pinto, L.G.; Rocha, J.B.; Barancelli, D.A.; Nogueira, C.W.; Zeni, G. Diphenyl diselenide exerts antidepressant-like and anxiolytic-like effects in mice: involvement of L-arginine-nitric oxide-soluble guanylate cyclase pathway in its antidepressant-like action. Pharmacol. Biochem. Behav. 2008, 88, 418–426. [Google Scholar] [CrossRef] [PubMed]
- Ergun, Y.; Ergun, U.G. Prevention of pro-depressant effect of L-arginine in the forced swim test by NG-nitro-L-arginine and [1H-[1,2,4]Oxadiazole[4,3-a]quinoxalin-1-one]. Eur. J. Pharmacol. 2007, 554, 150–154. [Google Scholar] [CrossRef] [PubMed]
- Prast, H.; Philippu, A. Nitric oxide as modulator of neuronal function. Prog. Neurobiol. 2001, 64, 51–68. [Google Scholar] [CrossRef] [PubMed]
- Papa, M.; Pellicano, M.P.; Sadile, A.G. Nitric oxide and long-term habituation to novelty in the rat. Ann. N. Y. Acad. Sci. 1994, 738, 316–324. [Google Scholar] [PubMed]
- Schuman, E.M.; Madison, D.V. A requirement for the intercellular messenger nitric oxide in long-term potentiation. Science 1991, 254, 1503–1506. [Google Scholar] [PubMed]
- Bliss, T.V.P.; Collingridge, G.L. A synaptic model of memory: Long-term potentiation in the hippocampus. Nature 1993, 361, 31–39. [Google Scholar] [CrossRef] [PubMed]
- Madison, D.V.; Malenka, R.C.; Nicoll, R.A. Mechanisms underlying long-term potentiation of synaptic transmission. Annu. Rev. Neurosci. 1991, 14, 379–397. [Google Scholar] [PubMed]
- Malenka, R.C. Synaptic plasticity in the hippocampus: LTP and LTD. Cell 1994, 78, 535–538. [Google Scholar] [CrossRef] [PubMed]
- Linden, D.J.; Dawson, T.M.; Dawson, V.L. An evaluation of the nitric oxide/cGMP/cGMP-dependent protein kinase cascade in the induction of cerebellar long-term depression in culture. J. Neurosci. 1995, 15, 5098–5105. [Google Scholar] [PubMed]
- Wiley, J.L.; Willmore, C.B. Effects of nitric oxide synthase inhibitors on timing and short-term memory in rats. Behav. Pharmacol. 2000, 11, 421–429. [Google Scholar] [PubMed]
- Bannerman, D.M.; Chapman, P.F.; Kelly, P.A.; Butcher, S.P.; Morris, R.G. Inhibition of nitric oxide synthase does not impair spatial learning. J. Neurosci. 1994, 14, 7404–7414. [Google Scholar] [PubMed]
- Plech, A.; Klimkiewicz, T.; Maksym, B. Effect of L-arginine on memory in rats. Pol. J. Pharmacol. 2003, 55, 987–992. [Google Scholar] [PubMed]
- Siepmann, M.; Grossmann, J.; Muck-Weymann, M.; Kirch, W. Effects of sertraline on autonomic and cognitive functions in healthy volunteers. Psychopharmacology (Berl). 2003, 168, 293–298. [Google Scholar] [CrossRef] [PubMed]
- Herrera-Guzman, I.; Gudayol-Ferre, E.; Herrera-Guzman, D.; Guardia-Olmos, J.; Hinojosa-Calvo, E.; Herrera-Abarca, J.E. Effects of selective serotonin reuptake and dual serotonergic-noradrenergic reuptake treatments on memory and mental processing speed in patients with major depressive disorder. J. Psychiatr. Res. 2009, 43, 855–863. [Google Scholar] [CrossRef] [PubMed]
- Naudon, L.; Hotte, M.; Jay, T.M. Effects of acute and chronic antidepressant treatments on memory performance: a comparison between paroxetine and imipramine. Psychopharmacology (Berl). 2007, 191, 353–364. [Google Scholar] [CrossRef] [PubMed]
- Cobb, B.L.; Ryan, K.L.; Frei, M.R.; Guel-Gomez, V.; Mickley, G.A. Chronic administration of L-NAME in drinking water alters working memory in rats. Brain Res. Bull. 1995, 38, 203–207. [Google Scholar] [CrossRef] [PubMed]
- Bannerman, D.M.; Chapman, P.F.; Kelly, P.A.; Butcher, S.P.; Morris, R.G. Inhibition of nitric oxide synthase does not prevent the induction of long-term potentiation in vivo. J. Neurosci. 1994, 14, 7415–7425. [Google Scholar] [PubMed]
- Wiesinger, H. Arginine metabolism and the synthesis of nitric oxide in the nervous system. Prog. Neurobiol. 2001, 64, 365–391. [Google Scholar] [CrossRef] [PubMed]
- Halaris, A.; Piletz, J.E. Imidazoline receptors: possible involvement in the pathophysiology and treatment of depression. Hum. Psychopharmacol. Clin. Exp. 2001, 16, 65–69. [Google Scholar] [CrossRef]
- Halaris, A.; Piletz, J.E. Relevance of imidazoline receptors and agmatine to psychiatry: a decade of progress. Ann. N. Y. Acad. Sci. 2003, 1009, 1–20. [Google Scholar] [CrossRef] [PubMed]
- Regunathan, S.; Reis, D.J. Imidazoline receptors and their endogenous ligands. Annu. Rev. Pharmacol. Toxicol. 1996, 36, 511–544. [Google Scholar] [PubMed]
- Li, G.; Regunathan, S.; Barrow, C.J.; Eshraghi, J.; Cooper, R.; Reis, D.J. Agmatine: an endogenous clonidine-displacing substance in the brain. Science 1994, 263, 966–969. [Google Scholar] [PubMed]
- Olmos, G.; DeGregorio-Rocasolano, N.; Paz Regalado, M.; Gasull, T.; Assumpcio Boronat, M.; Trullas, R.; Villarroel, A.; Lerma, J.; Garcia-Sevilla, J.A. Protection by imidazol(ine) drugs and agmatine of glutamate-induced neurotoxicity in cultured cerebellar granule cells through blockade of NMDA receptor. Br. J. Pharmacol. 1999, 127, 1317–1326. [Google Scholar] [CrossRef] [PubMed]
- Ogawa, T.; Kimoto, M.; Watanabe, H.; Sasaoka, K. Metabolism of NG,NG-and NG,N'G-dimethylarginine in rats. Arch. Biochem. Biophys. 1987, 252, 526–537. [Google Scholar] [CrossRef] [PubMed]
- Boger, R.H.; Diemert, A.; Schwedhelm, E.; Luneburg, N.; Maas, R.; Hecher, K. The Role of Nitric Oxide Synthase Inhibition by Asymmetric Dimethylarginine in the Pathophysiology of Preeclampsia. Gynecol. Obstet. Invest. 2009, 69, 1–13. [Google Scholar]
- Boger, R.H.; Maas, R.; Schulze, F.; Schwedhelm, E. Asymmetric dimethylarginine (ADMA) as a prospective marker of cardiovascular disease and mortality-An update on patient populations with a wide range of cardiovascular risk . Pharmacol. Res. 2009, 481–487. [Google Scholar]
- Boger, R.H.; Sullivan, L.M.; Schwedhelm, E.; Wang, T.J.; Maas, R.; Benjamin, E.J.; Schulze, F.; Xanthakis, V.; Benndorf, R.A.; Vasan, R.S. Plasma asymmetric dimethylarginine and incidence of cardiovascular disease and death in the community. Circulation 2009, 119, 1592–1600. [Google Scholar] [CrossRef] [PubMed]
- Das, I.; Khan, N.S.; Puri, B.K.; Hirsch, S.R. Elevated endogenous nitric oxide synthase inhibitor in schizophrenic plasma may reflect abnormalities in brain nitric oxide production. Neurosci. Lett. 1996, 215, 209–211. [Google Scholar] [CrossRef] [PubMed]
- Arlt, S.; Schulze, F.; Eichenlaub, M.; Maas, R.; Lehmbeck, J.T.; Schwedhelm, E.; Jahn, H.; Boger, R.H. Asymmetrical dimethylarginine is increased in plasma and decreased in cerebrospinal fluid of patients with Alzheimer's disease. Dement. Geriatr. Cogn. Disord. 2008, 26, 58–64. [Google Scholar] [CrossRef] [PubMed]
- Babbedge, R.C.; Bland-Ward, P.A.; Hart, S.L.; Moore, P.K. Inhibition of rat cerebellar nitric oxide synthase by 7-nitro indazole and related substituted indazoles. Br. J. Pharmacol. 1993, 110, 225–228. [Google Scholar] [PubMed]
- Mayer, B.; Klatt, P.; Werner, E.R.; Schmidt, K. Molecular mechanisms of inhibition of porcine brain nitric oxide synthase by the antinociceptive drug 7-nitro-indazole [published erratum appears in Neuropharmacology 1995 Feb;34(2):243]. Neuropharmacology 1994, 33, 1253–1259. [Google Scholar] [CrossRef] [PubMed]
- Handy, R.L.; Wallace, P.; Gaffen, Z.A.; Whitehead, K.J.; Moore, P.K. The antinociceptive effect of 1-(2-trifluoromethylphenyl) imidazole (TRIM), a potent inhibitor of neuronal nitric oxide synthase in vitro, in the mouse. Br. J. Pharmacol. 1995, 116, 2349–2350. [Google Scholar] [PubMed]
- Handy, R.L.; Harb, H.L.; Wallace, P.; Gaffen, Z.; Whitehead, K.J.; Moore, P.K. Inhibition of nitric oxide synthase by 1-(2-trifluoromethylphenyl) imidazole (TRIM) in vitro: antinociceptive and cardiovascular effects. Br. J. Pharmacol. 1996, 119, 423–431. [Google Scholar] [PubMed]
- Holscher, C.; McGlinchey, L.; Anwyl, R.; Rowan, M.J. 7-Nitro indazole, a selective neuronal nitric oxide synthase inhibitor in vivo, impairs spatial learning in the rat. Learn. Mem. 1996, 2, 267–278. [Google Scholar] [CrossRef] [PubMed]
- Mizuno, M.; Yamada, K.; Olariu, A.; Nawa, H.; Nabeshima, T. Involvement of brain-derived neurotrophic factor in spatial memory formation and maintenance in a radial arm maze test in rats. J. Neurosci. 2000, 20, 7116–7121. [Google Scholar] [PubMed]
- Zou, L.B.; Yamada, K.; Tanaka, T.; Kameyama, T.; Nabeshima, T. Nitric oxide synthase inhibitors impair reference memory formation in a radial arm maze task in rats. Neuropharmacology 1998, 37, 323–330. [Google Scholar] [CrossRef] [PubMed]
- Yildiz Akar, F.; Celikyurt, I.K.; Ulak, G.; Mutlu, O. Effects of L-arginine on 7-nitroindazole-induced reference and working memory performance of rats. Pharmacology 2009, 84, 211–218. [Google Scholar] [CrossRef] [PubMed]
- Yang, B.; Larson, D.F.; Watson, R.R. Modulation of iNOS activity in age-related cardiac dysfunction. Life Sci. 2004, 75, 655–667. [Google Scholar] [CrossRef] [PubMed]
- Ishibashi, Y.; Shimada, T.; Murakami, Y.; Takahashi, N.; Sakane, T.; Sugamori, T.; Ohata, S.; Inoue, S.; Ohta, Y.; Nakamura, K.; Shimizu, H.; Katoh, H.; Hashimoto, M. An inhibitor of inducible nitric oxide synthase decreases forearm blood flow in patients with congestive heart failure. J. Am. Coll. Cardiol. 2001, 38, 1470–1476. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Yang, X.P.; Liu, Y.H.; Carretero, O.A.; LaPointe, M.C. Reduction of myocardial infarct size by inhibition of inducible nitric oxide synthase. Am. J. Hypertens. 1999, 12, 174–182. [Google Scholar] [CrossRef] [PubMed]
- Takano, H.; Manchikalapudi, S.; Tang, X.L.; Qiu, Y.; Rizvi, A.; Jadoon, A.K.; Zhang, Q.; Bolli, R. Nitric oxide synthase is the mediator of late preconditioning against myocardial infarction in conscious rabbits. Circulation 1998, 98, 441–449. [Google Scholar] [PubMed]
- Gardiner, S.M.; Kemp, P.A.; March, J.E.; Bennett, T. Influence of aminoguanidine and the endothelin antagonist, SB 209670, on the regional haemodynamic effects of endotoxaemia in conscious rats. Br. J. Pharmacol. 1996, 118, 1822–1828. [Google Scholar] [PubMed]
- Rydgren, T.; Sandler, S. Efficacy of 1400 W, a novel inhibitor of inducible nitric oxide synthase, in preventing interleukin-1beta-induced suppression of pancreatic islet function in vitro and multiple low-dose streptozotocin-induced diabetes in vivo. Eur. J. Endocrinol. 2002, 147, 543–551. [Google Scholar] [CrossRef] [PubMed]
- Suarez-Pinzon, W.L.; Mabley, J.G.; Strynadka, K.; Power, R.F.; Szabo, C.; Rabinovitch, A. An inhibitor of inducible nitric oxide synthase and scavenger of peroxynitrite prevents diabetes development in NOD mice. J. Autoimmun. 2001, 16, 449–455. [Google Scholar] [CrossRef] [PubMed]
- Shimabukuro, M.; Ohneda, M.; Lee, Y.; Unger, R.H. Role of nitric oxide in obesity-induced beta cell disease. J. Clin. Invest. 1997, 100, 290–295. [Google Scholar] [CrossRef] [PubMed]
- Holstad, M.; Jansson, L.; Sandler, S. Effects of aminoguanidine on rat pancreatic islets in culture and on the pancreatic islet blood flow of anaesthetized rats. Biochem. Pharmacol. 1996, 51, 1711–1717. [Google Scholar] [CrossRef] [PubMed]
- Corbett, J.A.; McDaniel, M.L. The Use of Aminoguanidine, a Selective iNOS Inhibitor, to Evaluate the Role of Nitric Oxide in the Development of Autoimmune Diabetes. Methods 1996, 10, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Hasan, K.; Heesen, B.J.; Corbett, J.A.; McDaniel, M.L.; Chang, K.; Allison, W.; Wolffenbuttel, B.H.; Williamson, J.R.; Tilton, R.G. Inhibition of nitric oxide formation by guanidines. Eur. J. Pharmacol. 1993, 249, 101–106. [Google Scholar] [CrossRef] [PubMed]
- Griffiths, M.J.; Messent, M.; MacAllister, R.J.; Evans, T.W. Aminoguanidine selectively inhibits inducible nitric oxide synthase. Br. J. Pharmacol. 1993, 110, 963–968. [Google Scholar] [PubMed]
- Griffiths, M.J.; Messent, M.; Curzen, N.P.; Evans, T.W. Aminoguanidine selectively decreases cyclic GMP levels produced by inducible nitric oxide synthase. Am. J. Respir. Crit. Care Med. 1995, 152, 1599–1604. [Google Scholar] [PubMed]
- Olivenza, R.; Moro, M.A.; Lizasoain, I.; Lorenzo, P.; Fernandez, A.P.; Rodrigo, J.; Bosca, L.; Leza, J.C. Chronic stress induces the expression of inducible nitric oxide synthase in rat brain cortex. J. Neurochem. 2000, 74, 785–791. [Google Scholar] [CrossRef] [PubMed]
- Mori, K.; Togashi, H.; Ueno, K.I.; Matsumoto, M.; Yoshioka, M. Aminoguanidine prevented the impairment of learning behavior and hippocampal long-term potentiation following transient cerebral ischemia. Behav. Brain Res. 2001, 120, 159–168. [Google Scholar] [CrossRef] [PubMed]
- Naylor, G.J.; Smith, A.H.; Connelly, P. Methylene blue in mania [letter]. Biol. Psychiatry 1988, 24, 941–942. [Google Scholar] [CrossRef] [PubMed]
- Salaris, S.C.; Babbs, C.F.; Voorhees, W.D. Methylene blue as an inhibitor of superoxide generation by xanthine oxidase. A potential new drug for the attenuation of ischemia/reperfusion injury. Biochem. Pharmacol. 1991, 42, 499–506. [Google Scholar] [CrossRef] [PubMed]
- Murad, F.; Mittal, C.K.; Arnold, W.P.; Katsuki, S.; Kimura, H. Guanylate cyclase: activation by azide, nitro compounds, nitric oxide, and hydroxyl radical and inhibition by hemoglobin and myoglobin. Adv. Cyclic Nucleotide Res. 1978, 9, 145–158. [Google Scholar] [PubMed]
- Bodoni, P. Le bleu de méthylène comme calmant chez le aliénés . La Semaine Médicale 1899, 56. [Google Scholar]
- Naylor, G.G.; Smith, A.H. Reduction of vanadate, a possible explanation of the effect of phenothiazines in manic-depressive psychosis. Lancet 1982, 1, 395–396. [Google Scholar] [CrossRef] [PubMed]
- Naylor, G.G.; Smith, A.H. Reduction of vanadate, a possible explanation of the effect of phenothiazines in manic-depressive psychosis [letter]. Lancet 1982, 1, 395–396. [Google Scholar] [CrossRef] [PubMed]
- Naylor, G.J. Vanadium and manic depressive psychosis. Nutr. Health 1984, 3, 79–85. [Google Scholar] [PubMed]
- Naylor, G.J.; Dick, D.A.; Johnston, B.B.; Hopwood, S.E.; Dick, E.G.; Smith, A.H.; Kay, D. Possible explanation for therapeutic action of lithium, and a possible substitute (methylene-blue) [letter]. Lancet 1981, 2, 1175–1176. [Google Scholar] [CrossRef]
- Alda, M. NCT00214877: Methylene Blue for Cognitive Dysfunction in Bipolar Disorder . Available online: http://clinicaltrials.gov/show/NCT00214877/, Access 8 November 2009.
- Mayer, B.; Brunner, F.; Schmidt, K. Inhibition of nitric oxide synthesis by methylene blue. Biochem.Pharmacol. 1993, 45, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Mayer, B.; Brunner, F.; Schmidt, K. Novel actions of methylene blue . Eur.Heart J. 1993, 14 (Suppl. I), 22–26. [Google Scholar] [PubMed]
- Volke, V.; Wegener, G.; Vasar, E.; Rosenberg, R. Methylene blue inhibits hippocampal nitric oxide synthase activity in vivo. Brain Res. 1999, 826, 303–305. [Google Scholar] [CrossRef] [PubMed]
- Ehringer, H.; Hornykiewicz, O.; Lechner, K. Die Wirkung von Methylenblau auf die Monoaminoxydase und den Katecholamin-und 5-Hydroxytryptaminstoffwechsel des Gehirnes. Naunyn. Schmiedebergs Arch. Exp. Pathol. Pharmakol. 1961, 241, 568–582. [Google Scholar] [CrossRef] [PubMed]
- Gillman, P.K. Methylene blue is a potent monoamine oxidase inhibitor. Can. J. Anaesth. 2008, 55, 311–312. [Google Scholar] [CrossRef] [PubMed]
- Jakubovic, A.; Necina, J. The effect of methylene blue on the monoamine oxidase activity of the liver and brain of rats after various routes of administration. Arzneimittelforschung 1963, 13, 134–136. [Google Scholar] [PubMed]
- Stanford, S.C.; Stanford, B.J.; Gillman, P.K. Risk of severe serotonin toxicity following co-administration of methylene blue and serotonin reuptake inhibitors: an update on a case report of post-operative delirium . J. Psychopharmacol. (Oxf). 2009, in press. [Google Scholar]
- Kurt, M.; Bilge, S.S.; Aksoz, E.; Kukula, O.; Celik, S.; Kesim, Y. Effect of sildenafil on anxiety in the plus-maze test in mice. Pol. J. Pharmacol. 2004, 56, 353–357. [Google Scholar] [PubMed]
- Volke, V.; Wegener, G.; Vasar, E. Augmentation of the NO-CGMP cascade induces anxiogenic-like effect in mice. J. Physiol. Pharmacol. 2003, 54, 653–660. [Google Scholar] [PubMed]
- Brink, C.B.; Clapton, J.D.; Eagar, B.E.; Harvey, B.H. Appearance of antidepressant-like effect by sildenafil in rats after central muscarinic receptor blockade: evidence from behavioural and neuro-receptor studies. J. Neural Transm. 2008, 115, 117–125. [Google Scholar] [CrossRef] [PubMed]
- Kaehler, S.T.; Singewald, N.; Sinner, C.; Philippu, A. Nitric oxide modulates the release of serotonin in the rat hypothalamus. Brain Res. 1999, 835, 346–349. [Google Scholar] [CrossRef] [PubMed]
- Lorrain, D.S.; Hull, E.M. Nitric oxide increases dopamine and serotonin release in the medial preoptic area. Neuroreport 1993, 5, 87–89. [Google Scholar] [CrossRef]
- Segovia, G.; Del Arco, A.; Mora, F. Endogenous glutamate increases extracellular concentrations of dopamine, GABA, and taurine through NMDA and AMPA/kainate receptors in striatum of the freely moving rat: a microdialysis study. J. Neurochem. 1997, 69, 1476–1483. [Google Scholar] [PubMed]
- Segovia, G.; Del Arco, A.; Mora, F. Role of glutamate receptors and glutamate transporters in the regulation of the glutamate-glutamine cycle in the awake rat. Neurochem. Res. 1999, 24, 779–783. [Google Scholar] [CrossRef] [PubMed]
- Segovia, G.; Porras, A.; Mora, F. Effects of a nitric oxide donor on glutamate and GABA release in striatum and hippocampus of the conscious rat. Neuroreport 1994, 5, 1937–1940. [Google Scholar] [CrossRef] [PubMed]
- Strasser, A.; McCarron, R.M.; Ishii, H.; Stanimirovic, D.; Spatz, M. L-arginine induces dopamine release from the striatum in vivo. Neuroreport 1994, 5, 2298–2300. [Google Scholar] [CrossRef]
- Wegener, G.; Volke, V.; Rosenberg, R. Endogenous nitric oxide decreases hippocampal levels of serotonin and dopamine in vivo. Br. J. Pharmacol. 2000, 130, 575–580. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, D.M.; Arthur Jr., R. Molecular mechanism of the inactivation of tryptophan hydroxylase by nitric oxide: attack on critical sulfhydryls that spare the enzyme iron center . J. Neurosci. 1997, 17, 7245–7251. [Google Scholar] [PubMed]
- Kuhn, D.M.; Arthur Jr., R.E. Inactivation of brain tryptophan hydroxylase by nitric oxide . J. Neurochem. 1996, 67, 1072–1077. [Google Scholar] [PubMed]
- Meffert, M.K.; Calakos, N.C.; Scheller, R.H.; Schulman, H. Nitric oxide modulates synaptic vesicle docking fusion reactions. Neuron 1996, 16, 1229–1236. [Google Scholar] [CrossRef] [PubMed]
- Meffert, M.K.; Premack, B.A.; Schulman, H. Nitric oxide stimulates Ca(2+)-independent synaptic vesicle release. Neuron 1994, 12, 1235–1244. [Google Scholar] [CrossRef] [PubMed]
- Pogun, S.; Baumann, M.H.; Kuhar, M.J. Nitric oxide inhibits [3H]dopamine uptake. Brain Res. 1994, 641, 83–91. [Google Scholar] [CrossRef] [PubMed]
- Pogun, S.; Dawson, V.; Kuhar, M.J. Nitric oxide inhibits 3H-glutamate transport in synaptosomes. Synapse 1994, 18, 21–26. [Google Scholar] [CrossRef] [PubMed]
- Pogun, S.; Kuhar, M.J. Regulation of neurotransmitter reuptake by nitric oxide. Ann. N.Y. Acad. Sci. 1994, 738, 305–315. [Google Scholar] [PubMed]
- Lonart, G.; Cassels, K.L.; Johnson, K.M. Nitric oxide induces calcium-dependent [3H]dopamine release from striatal slices. J Neurosci. Res. 1993, 35, 192–198. [Google Scholar] [CrossRef] [PubMed]
- Lonart, G.; Johnson, K.M. Inhibitory effects of nitric oxide on the uptake of [3H]dopamine and [3H]glutamate by striatal synaptosomes. J. Neurochem. 1994, 63, 2108–2117. [Google Scholar] [PubMed]
- Fossier, P.; Blanchard, B.; Ducrocq, C.; Leprince, C.; Tauc, L.; Baux, G. Nitric oxide transforms serotonin into an inactive form and this affects neuromodulation. Neuroscience 1999, 93, 597–603. [Google Scholar] [CrossRef] [PubMed]
- Chanrion, B.; Mannoury la Cour, C.; Bertaso, F.; Lerner-Natoli, M.; Freissmuth, M.; Millan, M.J.; Bockaert, J.; Marin, P. Physical interaction between the serotonin transporter and neuronal nitric oxide synthase underlies reciprocal modulation of their activity. Proc. Natl. Acad. Sci. USA 2007, 104, 8119–8124. [Google Scholar] [CrossRef]
- Lassen, L.H.; Ashina, M.; Christiansen, I.; Ulrich, V.; Grover, R.; Donaldson, J.; Olesen, J. Nitric oxide synthase inhibition: A new principle in the treatment of migraine attacks. Cephalgia 1998, 18, 27–32. [Google Scholar] [CrossRef]
- Lassen, L.H.; Ashina, M.; Christiansen, I.; Ulrich, V.; Olesen, J. Nitric oxide synthase inhibition in migraine [letter]. Lancet 1997, 349, 401–402. [Google Scholar] [CrossRef] [PubMed]
- Thomsen, L.L. Investigations into the role of nitric oxide and the large intracranial arteries in migraine headache. Cephalgia 1997, 17, 873–895. [Google Scholar]
- Thomsen, L.L.; Olesen, J. Nitric oxide theory of migraine. Clin.Neurosci. 1998, 5, 28–33. [Google Scholar] [CrossRef]
- Harkin, A.; Connor, T.J.; Burns, M.P.; Kelly, J.P. Nitric oxide synthase inhibitors augment the effects of serotonin re-uptake inhibitors in the forced swimming test. Eur. Neuropsychopharmacol. 2004, 14, 274–281. [Google Scholar] [CrossRef] [PubMed]
- Jesse, C.R.; Bortolatto, C.F.; Savegnago, L.; Rocha, J.B.; Nogueira, C.W. Involvement of L-arginine-nitric oxide-cyclic guanosine monophosphate pathway in the antidepressant-like effect of tramadol in the rat forced swimming test. Prog. Neuropsychopharmacol. Biol. Psychiatry 2008, 32, 1838–1843. [Google Scholar] [CrossRef] [PubMed]
- Dhir, A.; Kulkarni, S.K. Involvement of nitric oxide (NO) signaling pathway in the antidepressant action of bupropion, a dopamine reuptake inhibitor. Eur. J. Pharmacol. 2007, 568, 177–185. [Google Scholar] [CrossRef] [PubMed]
- Ghasemi, M.; Sadeghipour, H.; Mosleh, A.; Sadeghipour, H.R.; Mani, A.R.; Dehpour, A.R. Nitric oxide involvement in the antidepressant-like effects of acute lithium administration in the mouse forced swimming test. Eur. Neuropsychopharmacol. 2008, 18, 323–332. [Google Scholar] [CrossRef] [PubMed]
- Wegener, G.; Volke, V.; Harvey, B.H.; Rosenberg, R. Local, but not systemic, administration of serotonergic antidepressants decreases hippocampal nitric oxide synthase activity. Brain Res. 2003, 959, 128–134. [Google Scholar] [CrossRef] [PubMed]
© 2010 by the authors; licensee Molecular Diversity Preservation International, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Wegener, G.; Volke, V. Nitric Oxide Synthase Inhibitors as Antidepressants. Pharmaceuticals 2010, 3, 273-299. https://doi.org/10.3390/ph3010273
Wegener G, Volke V. Nitric Oxide Synthase Inhibitors as Antidepressants. Pharmaceuticals. 2010; 3(1):273-299. https://doi.org/10.3390/ph3010273
Chicago/Turabian StyleWegener, Gregers, and Vallo Volke. 2010. "Nitric Oxide Synthase Inhibitors as Antidepressants" Pharmaceuticals 3, no. 1: 273-299. https://doi.org/10.3390/ph3010273
APA StyleWegener, G., & Volke, V. (2010). Nitric Oxide Synthase Inhibitors as Antidepressants. Pharmaceuticals, 3(1), 273-299. https://doi.org/10.3390/ph3010273




