Orally Administered NSAIDs—General Characteristics and Usage in the Treatment of Temporomandibular Joint Osteoarthritis—A Narrative Review
Abstract
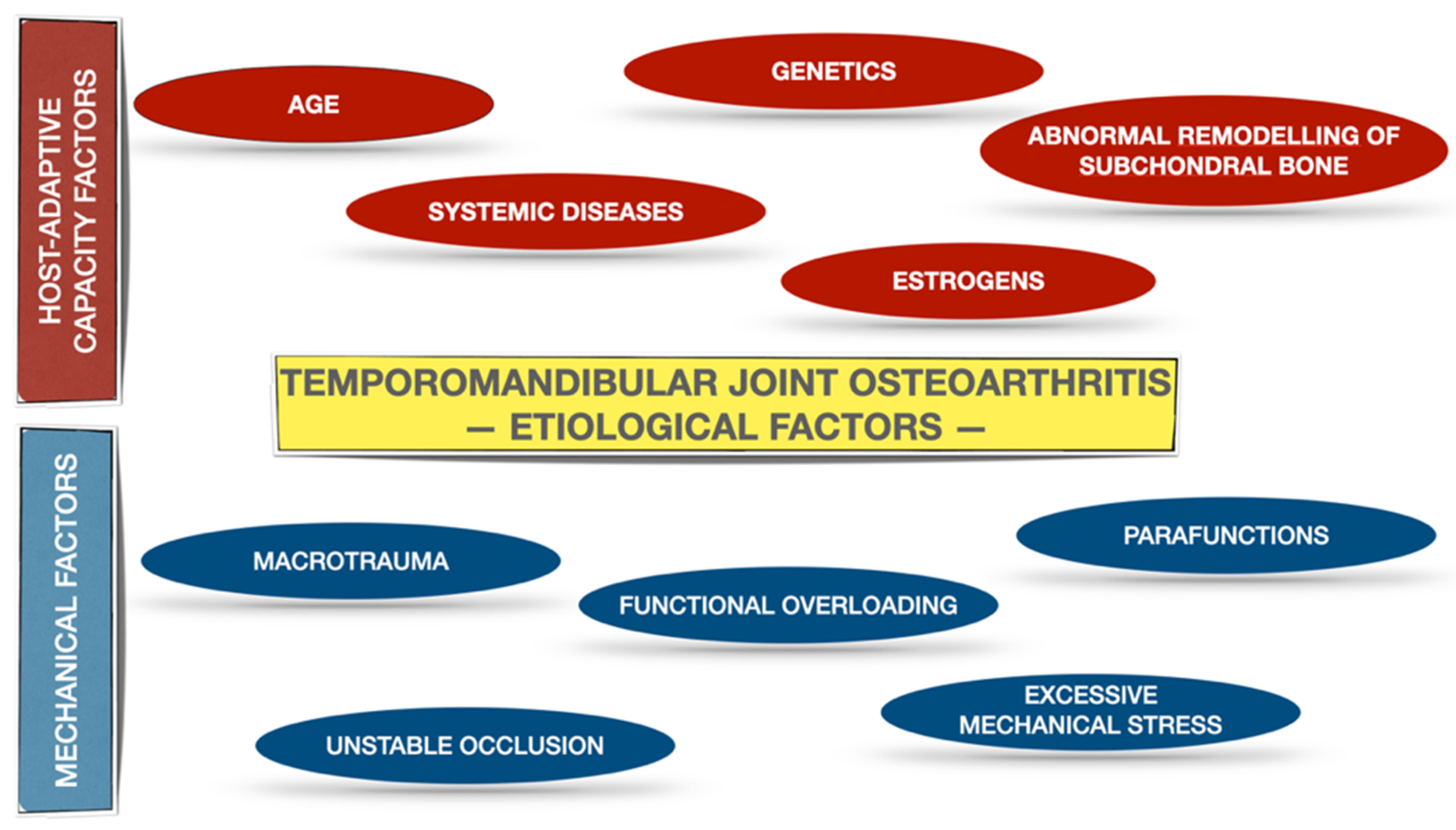
1. Temporomandibular Joint Osteoarthritis (TMJ OA)
2. Treatment of TMJ OA
3. Biosynthesis of Eicosanoids
4. NSAIDs Inhibit the Activity of Cyclooxygenases
5. COX-1 and COX-2 Selectivity of NSAIDs
6. Adverse Effects of NSAIDs
7. Prevention of Adverse Effects of NSAIDs
8. Recent Advances in NSAIDs Development
9. NSAIDs in the Treatment of TMJ OA
10. Materials and Methods
10.1. Clinical Question
10.2. The PICO Approach
10.3. Search Strategy
11. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Glyn-Jones, S.; Palmer, A.J.; Agricola, R.; Price, A.J.; Vincent, T.L.; Weinans, H.; Carr, A.J. Osteoarthritis. Lancet 2015, 386, 376–387. [Google Scholar] [CrossRef]
- Hunter, D.J.; Bierma-Zeinstra, S. Osteoarthritis. Lancet 2019, 393, 1745–1759. [Google Scholar] [CrossRef]
- Wang, X.D.; Zhang, J.N.; Gan, Y.H.; Zhou, Y.H. Current understanding of pathogenesis and treatment of TMJ osteoarthritis. J. Dent. Res. 2015, 94, 666–673. [Google Scholar] [CrossRef]
- Tanaka, E.; Detamore, M.S.; Mercuri, L.G. Degenerative disorders of the temporomandibular joint: Etiology, diagnosis, and treatment. J. Dent. Res. 2008, 87, 296–307. [Google Scholar] [CrossRef] [PubMed]
- Schiffman, E.; Ohrbach, R.; Truelove, E.; Look, J.; Anderson, G.; Goulet, J.-P.; List, T.; Svensson, P.; Gonzalez, Y.; Lobbezoo, F.; et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: Recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Group. J. Oral Facial Pain Headache 2014, 28, 6–27. [Google Scholar] [CrossRef]
- Pantoja, L.L.Q.; de Toledo, I.P.; Pupo, Y.M.; Porporatti, A.L.; De Luca Canto, G.; Zwir, L.F.; Guerra, E.N.S. Prevalence of degenerative joint disease of the temporomandibular joint: A systematic review. Clin. Oral Investig. 2019, 23, 2475–2488. [Google Scholar] [CrossRef] [PubMed]
- Whyte, A.; Boeddinghaus, R.; Bartley, A.; Vijeyaendra, R. Imaging of the temporomandibular joint. Clin. Radiol. 2021, 76, 76.e21–76.e35. [Google Scholar] [CrossRef] [PubMed]
- Dos Anjos Pontual, M.L.; Freire, J.S.; Barbosa, J.M.; Frazão, M.A.; dos Anjos Pontual, A. Evaluation of bone changes in the temporomandibular joint using cone beam CT. Dentomaxillofac. Radiol. 2012, 41, 24–29. [Google Scholar] [CrossRef] [PubMed]
- Ottersen, M.K.; Abrahamsson, A.K.; Larheim, T.A.; Arvidsson, L.Z. CBCT characteristics and interpretation challenges of temporomandibular joint osteoarthritis in a hand osteoarthritis cohort. Dentomaxillofac. Radiol. 2019, 48, 20180245. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, M.; Schiffman, E.L. Temporomandibular Joint Disorders and Orofacial Pain. Dent. Clin. N. Am. 2016, 60, 105–124. [Google Scholar] [CrossRef]
- Derwich, M.; Mitus-Kenig, M.; Pawlowska, E. Interdisciplinary Approach to the Temporomandibular Joint Osteoarthritis-Review of the Literature. Medicina 2020, 56, 225. [Google Scholar] [CrossRef] [PubMed]
- Gauer, R.L.; Semidey, M.J. Diagnosis and treatment of temporomandibular disorders. Am. Fam. Physician 2015, 91, 378–386. [Google Scholar]
- Al-Moraissi, E.A.; Wolford, L.M.; Ellis, E., 3rd; Neff, A. The hierarchy of different treatments for arthrogenous temporomandibular disorders: A network meta-analysis of randomized clinical trials. J. Craniomaxillofac. Surg. 2020, 48, 9–23. [Google Scholar] [CrossRef]
- Murakami, M.; Kudo, I. Phospholipase A2. J. Biochem. 2002, 131, 285–292. [Google Scholar] [CrossRef]
- Mitchell, J.A.; Kirkby, N.S. Eicosanoids, prostacyclin and cyclooxygenase in the cardiovascular system. Br. J. Pharmacol. 2019, 176, 1038–1050. [Google Scholar] [CrossRef] [PubMed]
- Kurumbail, R.G.; Kiefer, J.R.; Marnett, L.J. Cyclooxygenase enzymes: Catalysis and inhibition. Curr. Opin. Struct. Biol. 2001, 11, 752–760. [Google Scholar] [CrossRef]
- Ozen, G.; Norel, X. Prostanoids in the pathophysiology of human coronary artery. Prostaglandins Other Lipid Mediat. 2017, 133, 20–28. [Google Scholar] [CrossRef]
- Takeuchi, K. Gastric cytoprotection by prostaglandin E₂ and prostacyclin: Relationship to EP1 and IP receptors. J. Physiol. Pharmacol. 2014, 65, 3–14. [Google Scholar]
- Jang, Y.; Kim, M.; Hwang, S.W. Molecular mechanisms underlying the actions of arachidonic acid-derived prostaglandins on peripheral nociception. J. Neuroinflammation. 2020, 17, 30. [Google Scholar] [CrossRef] [PubMed]
- Smith, H.S. Arachidonic acid pathways in nociception. J. Support. Oncol. 2006, 4, 277–287. [Google Scholar] [PubMed]
- Ouanounou, A.; Goldberg, M.; Haas, D.A. Pharmacotherapy in Temporomandibular Disorders: A Review. J. Can. Dent. Assoc. 2017, 83, h7. [Google Scholar]
- Smith, T.J. Cyclooxygenases as the principal targets for the actions of NSAIDs. Rheum. Dis Clin. N. Am. 1998, 24, 501–523. [Google Scholar] [CrossRef]
- Bindu, S.; Mazumder, S.; Bandyopadhyay, U. Non-steroidal anti-inflammatory drugs (NSAIDs) and organ damage: A current perspective. Biochem. Pharmacol. 2020, 180, 114147. [Google Scholar] [CrossRef] [PubMed]
- Vane, J.R.; Bakhle, Y.S.; Botting, R.M. Cyclooxygenases 1 and 2. Annu. Rev. Pharmacol. Toxicol. 1998, 38, 97–120. [Google Scholar] [CrossRef]
- Botting, R.; Ayoub, S.S. COX-3 and the mechanism of action of paracetamol/acetaminophen. Prostaglandins Leukot. Essent. Fatty Acids 2005, 72, 85–87. [Google Scholar] [CrossRef] [PubMed]
- Schwab, J.M.; Schluesener, H.J.; Laufer, S. COX-3: Just another COX or the solitary elusive target of paracetamol? Lancet 2003, 361, 981–982. [Google Scholar] [CrossRef]
- Griswold, D.E.; Adams, J.L. Constitutive cyclooxygenase (COX-1) and inducible cyclooxygenase (COX-2): Rationale for selective inhibition and progress to date. Med. Res. Rev. 1996, 16, 181–206. [Google Scholar] [CrossRef]
- Amin, A.R.; Attur, M.; Patel, R.N.; Thakker, G.D.; Marshall, P.J.; Rediske, J.; Stuchin, S.A.; Patel, I.R.; Abramson, S.B. Superinduction of cyclooxygenase-2 activity in human osteoarthritis-affected cartilage. Influence of nitric oxide. J. Clin. Investig. 1997, 99, 1231–1237. [Google Scholar] [CrossRef] [PubMed]
- Hardy, M.M.; Seibert, K.; Manning, P.T.; Currie, M.G.; Woerner, B.M.; Edwards, D.; Koki, A.; Tripp, C.S. Cyclooxygenase 2-dependent prostaglandin E2 modulates cartilage proteoglycan degradation in human osteoarthritis explants. Arthritis Rheum. 2002, 46, 1789–1803. [Google Scholar] [CrossRef]
- Seki, H.; Fukuda, M.; Iino, M.; Takahashi, T.; Yoshioka, N. Immunohistochemical localization of cyclooxygenase-1 and -2 in synovial tissues from patients with internal derangement or osteoarthritis of the temporomandibular joint. Int. J. Oral Maxillofac. Surg. 2004, 33, 687–692. [Google Scholar] [CrossRef]
- Su, S.C.; Tanimoto, K.; Tanne, Y.; Kunimatsu, R.; Hirose, N.; Mitsuyoshi, T.; Okamoto, Y.; Tanne, K. Celecoxib exerts protective effects on extracellular matrix metabolism of mandibular condylar chondrocytes under excessive mechanical stress. Osteoarthr. Cartil. 2014, 22, 845–851. [Google Scholar] [CrossRef]
- Cryer, B.; Feldman, M. Cyclooxygenase-1 and cyclooxygenase-2 selectivity of widely used nonsteroidal anti-inflammatory drugs. Am. J. Med. 1998, 104, 413–421. [Google Scholar] [CrossRef]
- Ho, K.Y.; Cardosa, M.S.; Chaiamnuay, S.; Hidayat, R.; Ho, H.Q.T.; Kamil, O.; Mokhtar, S.A.; Nakata, K.; Navarra, S.V.; Nguyen, V.H.; et al. Practice Advisory on the Appropriate Use of NSAIDs in Primary Care. J. Pain Res. 2020, 13, 1925–1939. [Google Scholar] [CrossRef]
- Lanas, A.; García-Rodríguez, L.A.; Arroyo, M.T.; Gomollón, F.; Feu, F.; González-Pérez, A.; Zapata, E.; Bástida, G.; Rodrigo, L.; Santolaria, S.; et al. Risk of upper gastrointestinal ulcer bleeding associated with selective cyclo-oxygenase-2 inhibitors, traditional non-aspirin non-steroidal anti-inflammatory drugs, aspirin and combinations. Gut 2006, 55, 1731–1738. [Google Scholar] [CrossRef]
- Rafaniello, C.; Ferrajolo, C.; Sullo, M.G.; Sessa, M.; Sportiello, L.; Balzano, A.; Manguso, F.; Aiezza, M.L.; Rossi, F.; Scarpignato, C.; et al. Risk of gastrointestinal complications associated to NSAIDs, low-dose aspirin and their combinations: Results of a pharmacovigilance reporting system. Pharmacol. Res. 2016, 104, 108–114. [Google Scholar] [CrossRef] [PubMed]
- Sostres, C.; Gargallo, C.J.; Arroyo, M.T.; Lanas, A. Adverse effects of non-steroidal anti-inflammatory drugs (NSAIDs, aspirin and coxibs) on upper gastrointestinal tract. Best Pract. Res. Clin. Gastroenterol. 2010, 24, 121–132. [Google Scholar] [CrossRef] [PubMed]
- Risser, A.; Donovan, D.; Heintzman, J.; Page, T. NSAID prescribing precautions. Am. Fam. Physician 2009, 80, 1371–1378. [Google Scholar] [PubMed]
- Harirforoosh, S.; Asghar, W.; Jamali, F. Adverse effects of nonsteroidal antiinflammatory drugs: An update of gastrointestinal, cardiovascular and renal complications. J. Pharm. Pharm. Sci. 2013, 16, 821–847. [Google Scholar] [CrossRef]
- Larkai, E.N.; Smith, J.L.; Lidsky, M.D.; Graham, D.Y. Gastroduodenal mucosa and dyspeptic symptoms in arthritic patients during chronic nonsteroidal anti-inflammatory drug use. Am. J. Gastroenterol. 1987, 82, 1153–1158. [Google Scholar]
- Sostres, C.; Gargallo, C.J.; Lanas, A. Nonsteroidal anti-inflammatory drugs and upper and lower gastrointestinal mucosal damage. Arthritis Res. Ther. 2013, 15, S3. [Google Scholar] [CrossRef]
- Aalykke, C.; Lauritsen, K. Epidemiology of NSAID-related gastroduodenal mucosal injury. Best Pract. Res. Clin. Gastroenterol. 2001, 15, 705–722. [Google Scholar] [CrossRef] [PubMed]
- Yeomans, N.D.; Lanas, A.I.; Talley, N.J.; Thomson, A.B.; Daneshjoo, R.; Eriksson, B.; Appelman-Eszczuk, S.; Långström, G.; Naesdal, J.; Serrano, P.; et al. Prevalence and incidence of gastroduodenal ulcers during treatment with vascular protective doses of aspirin. Aliment. Pharmacol. Ther. 2005, 22, 795–801. [Google Scholar] [CrossRef] [PubMed]
- Graham, D.Y.; Opekun, A.R.; Willingham, F.F.; Qureshi, W.A. Visible small-intestinal mucosal injury in chronic NSAID users. Clin. Gastroenterol. Hepatol. 2005, 3, 55–59. [Google Scholar] [CrossRef]
- Watanabe, T.; Fujiwara, Y.; Chan, F.K.L. Current knowledge on non-steroidal anti-inflammatory drug-induced small-bowel damage: A comprehensive review. J. Gastroenterol. 2020, 55, 481–495. [Google Scholar] [CrossRef] [PubMed]
- Bjarnason, I.; Scarpignato, C.; Holmgren, E.; Olszewski, M.; Rainsford, K.D.; Lanas, A. Mechanisms of Damage to the Gastrointestinal Tract from Nonsteroidal Anti-Inflammatory Drugs. Gastroenterology 2018, 154, 500–514. [Google Scholar] [CrossRef]
- Scarpignato, C.; Hunt, R.H. Nonsteroidal antiinflammatory drug-related injury to the gastrointestinal tract: Clinical picture, pathogenesis, and prevention. Gastroenterol. Clin. N. Am. 2010, 39, 433–464. [Google Scholar] [CrossRef]
- Laine, L. Gastrointestinal effects of NSAIDs and coxibs. J. Pain Symptom Manag. 2003, 25, S32–S40. [Google Scholar] [CrossRef]
- Goldstein, J.L.; Cryer, B. Gastrointestinal injury associated with NSAID use: A case study and review of risk factors and preventative strategies. Drug Healthc. Patient Saf. 2015, 7, 31–41. [Google Scholar] [CrossRef]
- Strand, V. Are COX-2 inhibitors preferable to non-selective non-steroidal anti-inflammatory drugs in patients with risk of cardiovascular events taking low-dose aspirin? Lancet 2007, 370, 2138–2151. [Google Scholar] [CrossRef]
- Schink, T.; Kollhorst, B.; Varas Lorenzo, C.; Arfe, A.; Herings, R.; Lucchi, S.; Romio, S.; Schade, R.; Schuemie, M.J.; Straatman, H.; et al. Risk of ischemic stroke and the use of individual non-steroidal anti-inflammatory drugs: A multi-country European database study within the SOS Project. PLoS ONE 2018, 13, e0203362. [Google Scholar] [CrossRef]
- Moore, N. Coronary Risks Associated with Diclofenac and Other NSAIDs: An Update. Drug Saf. 2020, 43, 301–318. [Google Scholar] [CrossRef]
- Coxib and Traditional NSAID Trialists’ (CNT) Collaboration; Bhala, N.; Emberson, J.; Merhi, A.; Abramson, S.; Arber, N.; Baron, J.A.; Bombardier, C.; Cannon, C.; Farkouh, M.E.; et al. Vascular and upper gastrointestinal effects of non-steroidal anti-inflammatory drugs: Meta-analyses of individual participant data from randomised trials. Lancet 2013, 382, 769–779. [Google Scholar] [CrossRef]
- Ghosh, R.; Alajbegovic, A.; Gomes, A.V. NSAIDs and Cardiovascular Diseases: Role of Reactive Oxygen Species. Oxid. Med. Cell. Longev. 2015, 2015, 536962. [Google Scholar] [CrossRef]
- Abdu, N.; Mosazghi, A.; Teweldemedhin, S.; Asfaha, L.; Teshale, M.; Kibreab, M.; Anand, I.S.; Tesfamariam, E.H.; Russom, M. Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Usage and co-prescription with other potentially interacting drugs in elderly: A cross-sectional study. PLoS ONE 2020, 15, e0238868. [Google Scholar] [CrossRef]
- Russell, R.I. Non-steroidal anti-inflammatory drugs and gastrointestinal damage-problems and solutions. Postgrad. Med. J. 2001, 77, 82–88. [Google Scholar] [CrossRef]
- Gwee, K.A.; Goh, V.; Lima, G.; Setia, S. Coprescribing proton-pump inhibitors with nonsteroidal anti-inflammatory drugs: Risks versus benefits. J. Pain Res. 2018, 11, 361–374. [Google Scholar] [CrossRef]
- Scheiman, J.M. The use of proton pump inhibitors in treating and preventing NSAID-induced mucosal damage. Arthritis Res. Ther. 2013, 15, S5. [Google Scholar] [CrossRef] [PubMed]
- Jackson, M.A.; Goodrich, J.K.; Maxan, M.E.; Freedberg, D.E.; Abrams, J.A.; Poole, A.C.; Sutter, J.L.; Welter, D.; Ley, R.E.; Bell, J.T.; et al. Proton pump inhibitors alter the composition of the gut microbiota. Gut 2016, 65, 749–756. [Google Scholar] [CrossRef] [PubMed]
- Fujimori, S. What are the effects of proton pump inhibitors on the small intestine? World J. Gastroenterol. 2015, 21, 6817–6819. [Google Scholar] [CrossRef] [PubMed]
- Freedberg, D.E.; Kim, L.S.; Yang, Y.X. The Risks and Benefits of Long-term Use of Proton Pump Inhibitors: Expert Review and Best Practice Advice from the American Gastroenterological Association. Gastroenterology 2017, 152, 706–715. [Google Scholar] [CrossRef]
- Ng, S.C.; Chan, F.K. NSAID-induced gastrointestinal and cardiovascular injury. Curr. Opin. Gastroenterol. 2010, 26, 611–617. [Google Scholar] [CrossRef]
- Rao, P.P.; Kabir, S.N.; Mohamed, T. Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Progress in Small Molecule Drug Development. Pharmaceuticals 2010, 3, 1530–1549. [Google Scholar] [CrossRef]
- Abdellatif, K.R.; Abdelall, E.K.; Bakr, R.B. Nitric Oxide-NASIDS Donor Prodrugs as Hybrid Safe Anti-Inflammatory Agents. Curr. Top. Med. Chem. 2017, 17, 941–955. [Google Scholar] [CrossRef]
- Pereira-Leite, C.; Nunes, C.; Bozelli, J.C., Jr.; Schreier, S.; Kamma-Lorger, C.S.; Cuccovia, I.M.; Reis, S. Can NO-indomethacin counteract the topical gastric toxicity induced by indomethacin interactions with phospholipid bilayers? Colloids Surf. B Biointerfaces 2018, 169, 375–383. [Google Scholar] [CrossRef] [PubMed]
- Aisa, M.C.; Datti, A.; Orlacchio, A.; Di Renzo, G.C. COX inhibitors and bone: A safer impact on osteoblasts by NO-releasing NSAIDs. Life Sci. 2018, 208, 10–19. [Google Scholar] [CrossRef] [PubMed]
- Jacob, J.; Manju, S.L.; Ethiraj, K.R.; Elias, G. Safer anti-inflammatory therapy through dual COX-2/5-LOX inhibitors: A structure-based approach. Eur. J. Pharm. Sci. 2018, 121, 356–381. [Google Scholar] [CrossRef]
- Jacob, P.J.; Manju, S.L. Identification and development of thiazole leads as COX-2/5-LOX inhibitors through in-vitro and in-vivo biological evaluation for anti-inflammatory activity. Bioorg. Chem. 2020, 100, 103882. [Google Scholar] [CrossRef]
- Shen, F.Q.; Wang, Z.C.; Wu, S.Y.; Ren, S.Z.; Man, R.J.; Wang, B.Z.; Zhu, H.L. Synthesis of novel hybrids of pyrazole and coumarin as dual inhibitors of COX-2 and 5-LOX. Bioorg. Med. Chem. Lett. 2017, 27, 3653–3660. [Google Scholar] [CrossRef]
- Li, Z.; Wang, Z.C.; Li, X.; Abbas, M.; Wu, S.Y.; Ren, S.Z.; Liu, Q.X.; Liu, Y.; Chen, P.W.; Duan, Y.T.; et al. Design, synthesis and evaluation of novel diaryl-1,5-diazoles derivatives bearing morpholine as potent dual COX-2/5-LOX inhibitors and antitumor agents. Eur. J. Med. Chem. 2019, 169, 168–184. [Google Scholar] [CrossRef]
- Liaras, K.; Fesatidou, M.; Geronikaki, A. Thiazoles and Thiazolidinones as COX/LOX Inhibitors. Molecules 2018, 23, 685. [Google Scholar] [CrossRef]
- Bergqvist, F.; Morgenstern, R.; Jakobsson, P.J. A review on mPGES-1 inhibitors: From preclinical studies to clinical applications. Prostaglandins Other Lipid Mediat. 2020, 147, 106383. [Google Scholar] [CrossRef]
- Ding, K.; Zhou, Z.; Hou, S.; Yuan, Y.; Zhou, S.; Zheng, X.; Chen, J.; Loftin, C.; Zheng, F.; Zhan, C.G. Structure-based discovery of mPGES-1 inhibitors suitable for preclinical testing in wild-type mice as a new generation of anti-inflammatory drugs. Sci. Rep. 2018, 8, 5205. [Google Scholar] [CrossRef]
- Mejersjö, C.; Wenneberg, B. Diclofenac sodium and occlusal splint therapy in TMJ osteoarthritis: A randomized controlled trial. J. Oral Rehabil. 2008, 35, 729–738. [Google Scholar] [CrossRef] [PubMed]
- Kurita Varoli, F.; Sucena Pita, M.; Sato, S.; Issa, J.P.; do Nascimento, C.; Pedrazzi, V. Analgesia evaluation of 2 NSAID drugs as adjuvant in management of chronic temporomandibular disorders. Sci. World J. 2015, 2015, 359152. [Google Scholar] [CrossRef] [PubMed]
- Song, H.; Lee, J.Y.; Huh, K.H.; Park, J.W. Long-term Changes of Temporomandibular Joint Osteoarthritis on Computed Tomography. Sci. Rep. 2020, 10, 6731. [Google Scholar] [CrossRef] [PubMed]
- Dalewski, B.; Kamińska, A.; Szydłowski, M.; Kozak, M.; Sobolewska, E. Comparison of Early Effectiveness of Three Different Intervention Methods in Patients with Chronic Orofacial Pain: A Randomized, Controlled Clinical Trial. Pain Res. Manag. 2019, 2019, 7954291. [Google Scholar] [CrossRef] [PubMed]
- Di Rienzo Businco, L.; Di Rienzo Businc, A.; D’Emilia, M.; Lauriello, M.; Coen Tirelli, G. Topical versus systemic diclofenac in the treatment of temporo-mandibular joint dysfunction symptoms. Acta Otorhinolaryngol. Ital. 2004, 24, 279–283. [Google Scholar] [PubMed]
- Ta, L.E.; Dionne, R.A. Treatment of painful temporomandibular joints with a cyclooxygenase-2 inhibitor: A randomized placebo-controlled comparison of celecoxib to naproxen. Pain 2004, 111, 13–21. [Google Scholar] [CrossRef]
- Kulkarni, S.; Thambar, S.; Arora, H. Evaluating the effectiveness of nonsteroidal anti-inflammatory drug(s) for relief of pain associated with temporomandibular joint disorders: A systematic review. Clin. Exp. Dent. Res. 2020, 6, 134–146. [Google Scholar] [CrossRef]
- Häggman-Henrikson, B.; Alstergren, P.; Davidson, T.; Högestätt, E.D.; Östlund, P.; Tranaeus, S.; Vitols, S.; List, T. Pharmacological treatment of oro-facial pain—Health technology assessment including a systematic review with network meta-analysis. J. Oral Rehabil. 2017, 44, 800–826. [Google Scholar] [CrossRef]
- Pharmindex. Available online: https://pharmindex.pl (accessed on 21 January 2021).



| Exemplary Medicinal Product | Oral Dosage (Only for Adults) | Maximum Daily Dose | Additional Information |
|---|---|---|---|
| Ibuprofen | 400 mg every 6–8 h | 2400 mg | Single dose more than 400 mg does not cause stronger analgesic effect. |
| Ketoprofen | 100 mg every 12 h | 200 mg | Tablets should be taken with food and at least 100 mL of milk or water. |
| Naproxen | 250–500 mg every 12 h | 1250 mg | In case of acute OA, it is recommended to increase the oral dosage from 750 mg to 1000 mg. |
| Diclofenac | 75 mg once daily or 75 mg every 12 h | 150 mg | The extended-release tablets should be taken once a dayin the dosage of 100 mg. |
| Celecoxib | 200 mg once daily or 100 mg every 12 h | 400 mg | Capsules should be taken with 200 mL of water; celecoxib may be taken with or without food; in case of acute pain patient may be prescribed initial dose of 400 mg. |
| Meloxicam | 7.5 mg once daily | 15 mg | Used for short-term treatment in case of OA exacerbation; patients aged 65 or more should not take more than 7.5 mg of Meloxicam per day. |
| Nimesulide | 100 mg every 12 h | 200 mg | Medicament should be taken after meal; the maximum duration of a treatment cycle with nimesulide is 15 days. |
| Reference | Study Design | Participants and Intervention | Endpoint and Results |
|---|---|---|---|
| Mejersjö et al. (2008) [73] | Randomized, single-blind study | 29 patients (27 women, 2 men, aged 39–76 years):
| Endpoint: three months (one year follow-up) Both methods led to significant reduction of symptoms of TMJ OA within three months, but the Diclofenac group presented more rapid improvement. |
| Kurita Varoli et al. (2015) [74] | Randomized, triple-blind clinical trial; crossover methodology | 18 patients (no precise information regarding sex, aged 35–70). All patients submitted all treatments in different moments):
| Endpoint: 10 days (each treatment modality) All therapies were effective for pain relief after 10 days of therapy. Sodium diclofenac used in combination with occlusal splint (both NSAID and panacea groups) led to earlier pain relief (third day) compared to placebo (eighth day). |
| Song et al. (2020) [75] | Case-control study | 89 patients (76 women and 13 men, 152 joints), mean age of 33.17 ± 17.65 years. Treatment modalities applied to the patients:
| Mean follow-up period: 376.61 ± 94.49 days Mean occlusal splint therapy period: 524.49 ± 258.57 days Mean duration of NSAID prescription: 61.91 ± 42.15 days Occlusal stabilization splint therapy and NSAIDs had a significant influence on TMJ OA prognosis. The authors recommended a combination of both methods of treatment. |
| Dalewski et al. (2019) [76] | Randomized controlled clinical trial | 90 patients (72 women, 18 men, aged 18–65 years):
| Endpoint: three weeks Combination of occlusal splint with nimesulide led to better pain relief compared to the remaining two groups. |
| Di Rienzo Businco et al. (2004) [77] | Randomized clinical trial | 36 patients (19 women, 17 men, aged 34–61 years):
| Endpoint: 14 days All patients showed relief from pain after the treatment. The efficacy of both oral administration and multidose topical application of diclofenac sodium was similar. |
| Ta et al. (2004) [78] | Randomized, double-blindcontrolled clinical trial | 68 patients (46 women, 22 men, aged 18–65 years):
| Endpoint: six weeks Naproxen appeared to be most effective in TMJ pain reduction, whereas celecoxib was just slightly better than placebo. Naproxen reduced significantly TMJ pain intensity within three weeks of treatment. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Derwich, M.; Mitus-Kenig, M.; Pawlowska, E. Orally Administered NSAIDs—General Characteristics and Usage in the Treatment of Temporomandibular Joint Osteoarthritis—A Narrative Review. Pharmaceuticals 2021, 14, 219. https://doi.org/10.3390/ph14030219
Derwich M, Mitus-Kenig M, Pawlowska E. Orally Administered NSAIDs—General Characteristics and Usage in the Treatment of Temporomandibular Joint Osteoarthritis—A Narrative Review. Pharmaceuticals. 2021; 14(3):219. https://doi.org/10.3390/ph14030219
Chicago/Turabian StyleDerwich, Marcin, Maria Mitus-Kenig, and Elzbieta Pawlowska. 2021. "Orally Administered NSAIDs—General Characteristics and Usage in the Treatment of Temporomandibular Joint Osteoarthritis—A Narrative Review" Pharmaceuticals 14, no. 3: 219. https://doi.org/10.3390/ph14030219
APA StyleDerwich, M., Mitus-Kenig, M., & Pawlowska, E. (2021). Orally Administered NSAIDs—General Characteristics and Usage in the Treatment of Temporomandibular Joint Osteoarthritis—A Narrative Review. Pharmaceuticals, 14(3), 219. https://doi.org/10.3390/ph14030219






