Trends in Quantification of HbA1c Using Electrochemical and Point-of-Care Analyzers
Abstract
1. Introduction
2. Sensors for Quantification of HbA1c
2.1. Electrochemical Sensors for Direct HbA1c Detection Using Boronate Chemistry
| Electrochemical Technique | Interface | Detection Range (HbA1c) | LoD | Ref. |
|---|---|---|---|---|
| Amperometric | APBA-pTTBA/AuNP/SPCE | 0.1–1.5% | 0.052% | [35] |
| APBA/RVC | 0.2–12 mg/mL | 89 µg/mL | [34] | |
| MPBA/AuNF/SPCE | 2–20% 5–1000 μg/mL | 0.65% | [36] | |
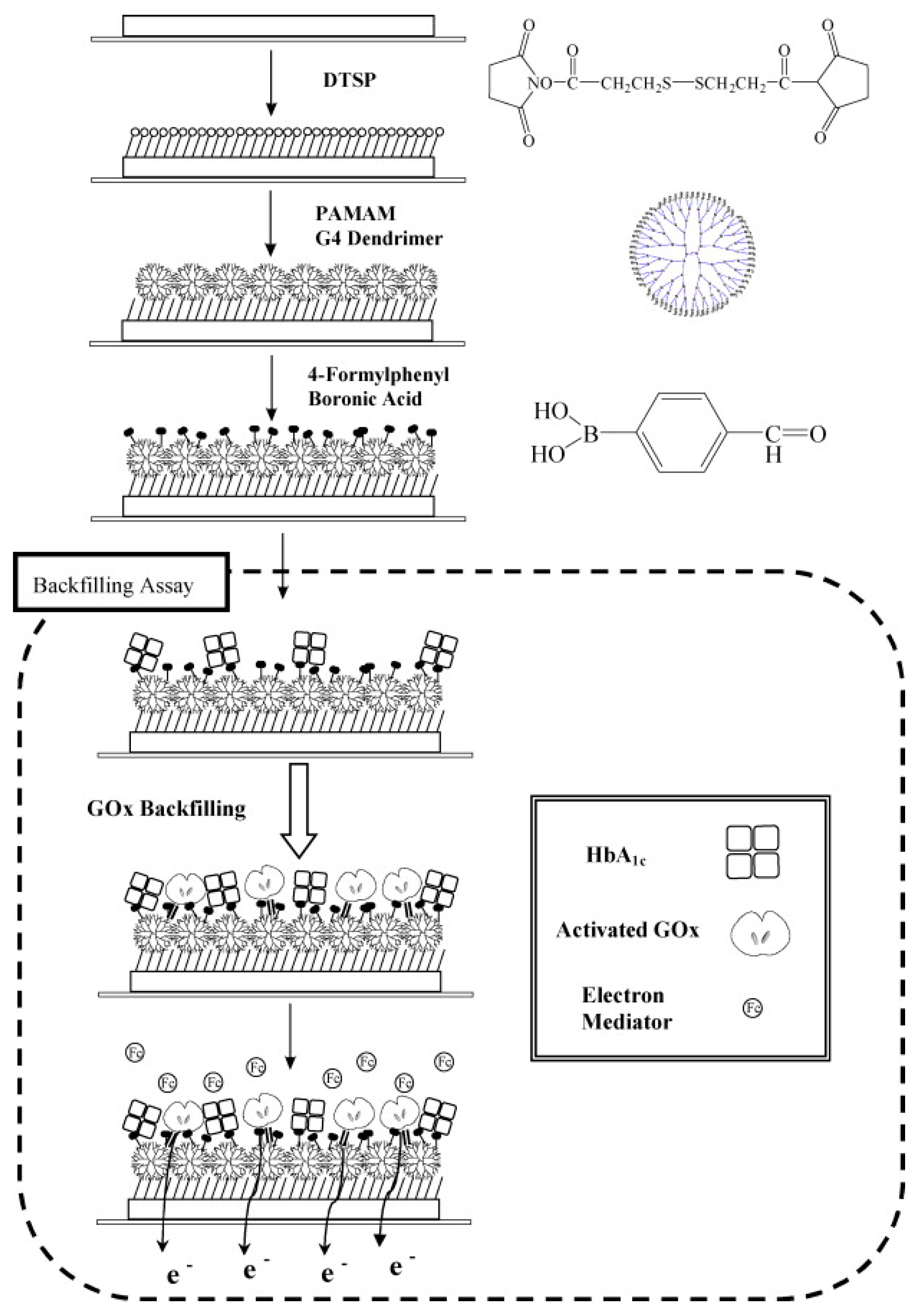
| FPBA/PAMAM/DTSP/Au (GOx Backfilling) | 2.5–15% | NA | [37] | |
| TiO2(G) NW@PAPBA–Au/ITO | 2–10% | 0.17% | [47] | |
| AQBA/SPCE | 31.2–500 nM | 4.2 nM | [40] | |
| ZrO2-DDAB/PG | 6.8–14% | NA | [33] | |
| PAPBA/SPCE | 0.975–156 μM | NA | [39] | |
| Impedometric | APBA/ESM | 2.3–14% | 0.19% | [41] |
| APBA/ESM | 2.3–14% | 0.21% | [48] | |
| APBA/GA/Cys/Au | 0.1–8.36% | 0.024% | [42] | |
| T3BA/Au | 4.5–11.5% | NA | [43] | |
| GO-APBA/GCE | 8% | NA | [44] | |
| T3BA | 10–100 ng/µL | 1 ng/µL | [45] | |
| APBA/BSA/MWCNTs/GA/SPCE | 4–15% | 1.2% | [46] |
2.2. Electrochemical Immunosensors for HbA1c Detection Using Antibodies
3. Aptamer-Based Sensors for HbA1c Detection
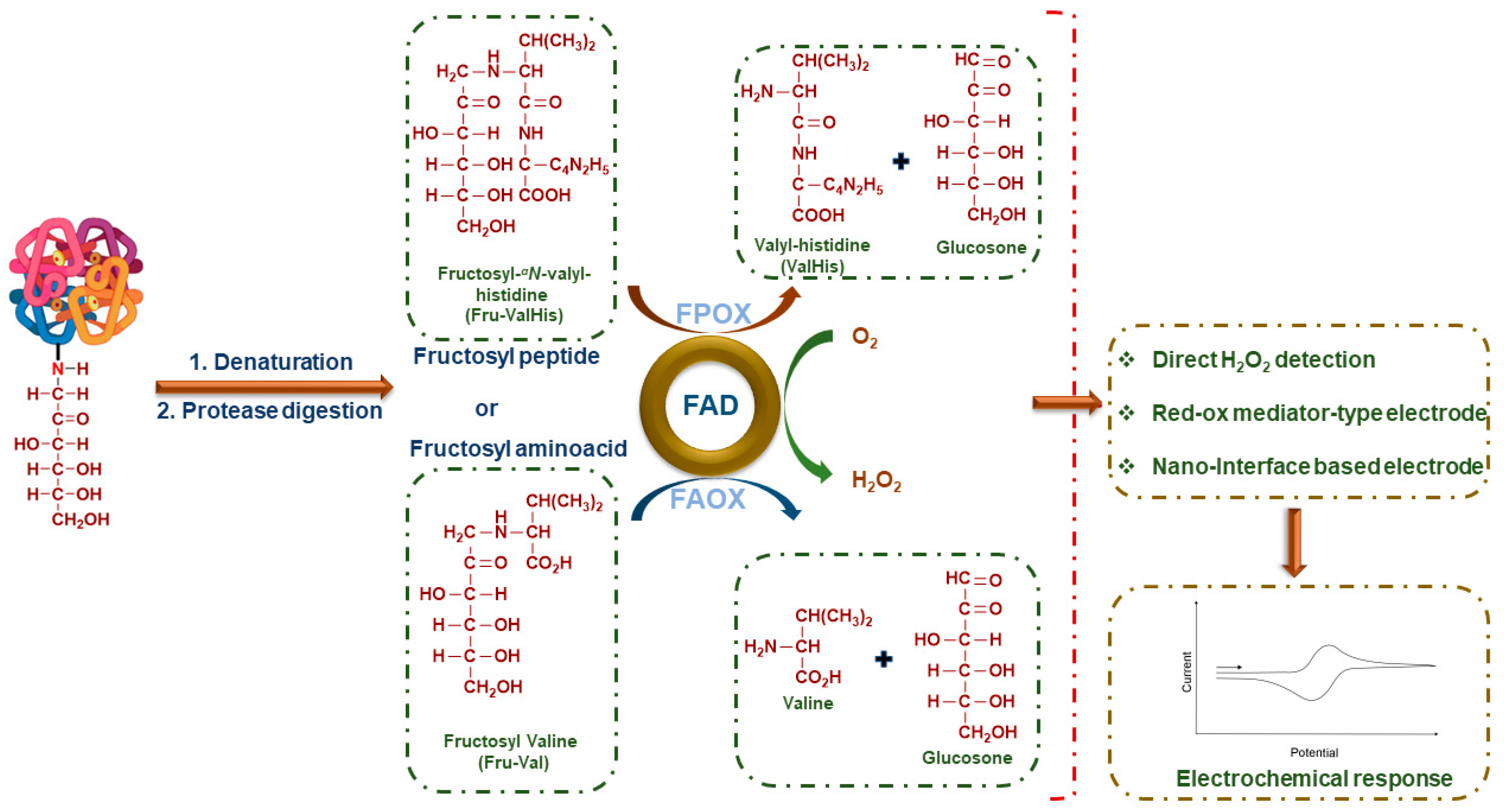
4. Non-Enzymatic HbA1c Sensors Based on FV Detection Principle
5. Biosensors Based on FV Detection
| Transducers | Detection Range (FV) | Sensitivity | LoD | Ref. |
|---|---|---|---|---|
| FAO/Carbon paste (in methoxy phenazine methosulfate) | 0.2–2.7 mM | 1.1 µA mM−1 cm−2 | NA | [71] |
| FAO-(PVA-SbQ)/Pt | 0.05–1.8 mM | 0.42 µA mM−1 cm−2 | NA | [71] |
| FAO-POD-Ferrocene-(PVA-SbQ)/Pt | 0.1–0.3 mM | 0.4 µA mM−1 cm−2 | NA | [72] |
| FAO-(PVA-SbQ)/PB /GCE | 0.1–0.3 mM | 1.3 µA mM−1 cm−2 | NA | [72] |
| FAO-(PVA-SbQ)/Pt (flow injection analysis) | 0.2–10 mM | 4.6 nA mM−1 cm–2 | NA | [83] |
| FAO/ZnONPs/PPy/Au | 0.1–3.0 mM | 38.42 μA mM−1 | 50 µM | [73] |
| FAO/MNPs/Au | 0–2 mM | NA | 0.1 mM | [74] |
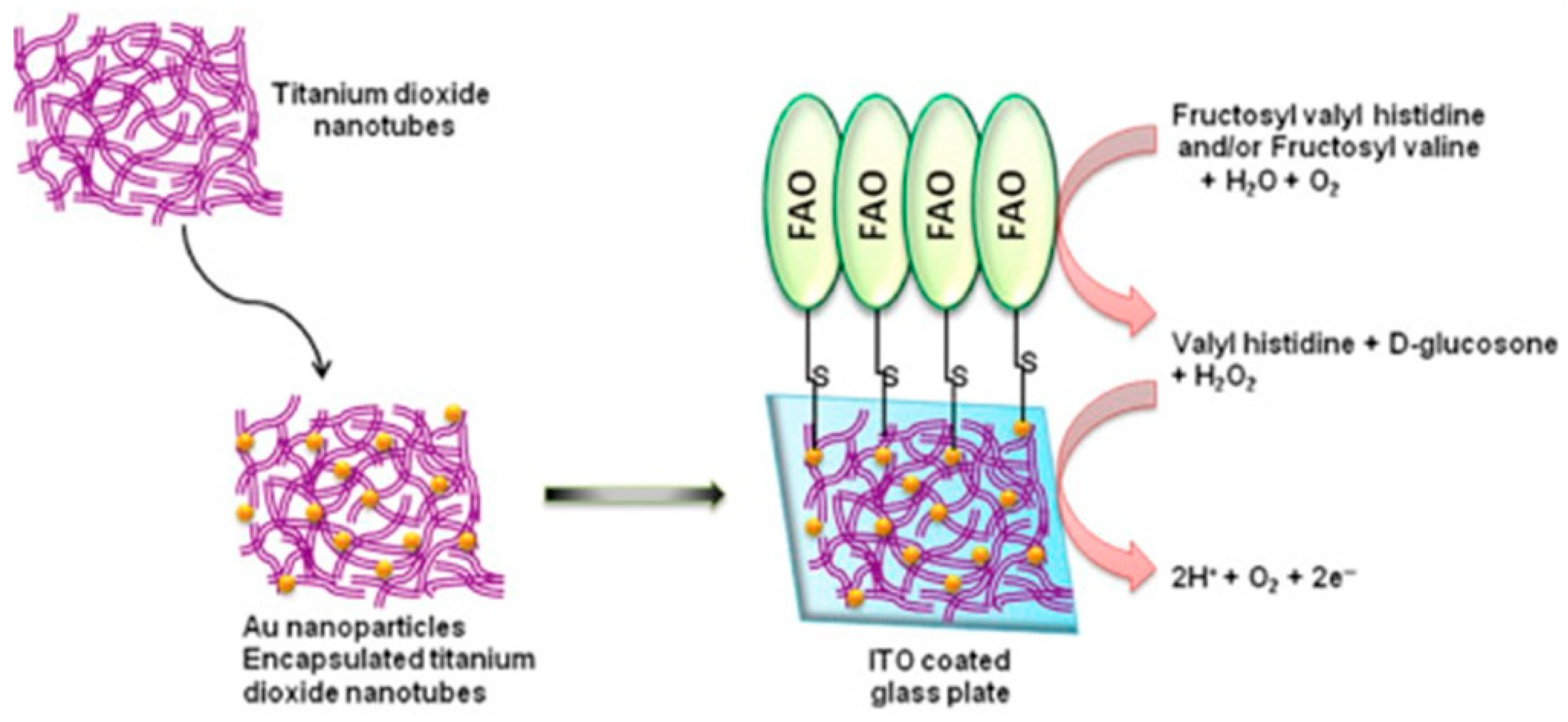
| FAO/GNPs-PTA-TiO2/ITO | 0.5–2000 μM | NA | 0.5 µM | [75] |
| FAO/AuNPs-PtNPs/PIN5COOH | 0.1–1000 μM | 0.316 μM/mA | 0.2 µM | [76] |
| FAO/AuNPs/GNs/FTO | 0.3–2000 μM | NA | 0.2 µM | [77] |
| FAO/PtNPs/rGO–MWCNT/Au | 0.05–1000 μM | 0.562 mA/μM | 0.1 µM | [78] |
| FAO/Iridium-Carbon ink | NA | 21.5 μA mM−1 cm−2 | NA | [79] |
| FAO/Graphite ink | 0–8 mM | NA | NA | [80] |
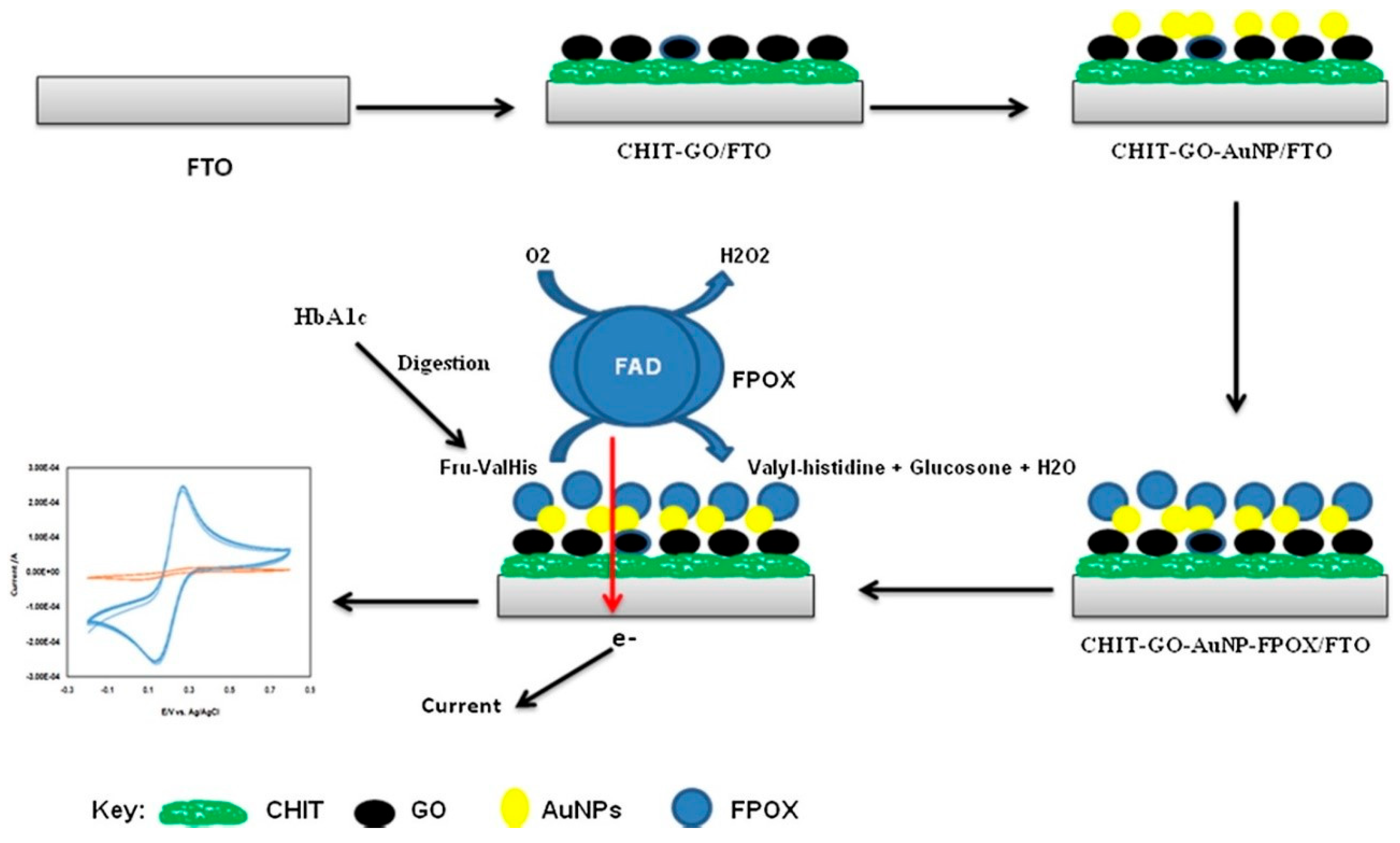
| FPOX/CHIT-GO-AuNPs/FTO | 0.1–2 mM | 8.45 µA mM−1 cm−2 | 0.3 µM | [81] |
| GCPE/ITO | 0–1 mM | 5.26 μA mM−1 | 0.05 mM | [64] |
| Carbon–PVI (in methoxy phenazine methosulfate) | 20–700 μM | NA | 20 μM | [65] |
6. Multi-Analyte Sensors
7. Strategies for Measurement of HbA1c
8. Challenges in Diagnosis Based on HbA1c Measurements
9. Concluding Remarks
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Nomenclature
| 3D-PEID | Three-dimensional paper-based electrochemical impedance device |
| 4-MPBA | 4-mercaptophenylboronic acid |
| ADAG | A1c-dervied average glucose |
| AG | Average glucose |
| AGE | Advanced glycation end products |
| ANBA | 2-anthraceneboronic acid |
| APBA | Aminophenyl boronic acid |
| AQBA | Anthraquinone boronic acid |
| AuNF | Gold nanoflowers |
| AuNPs | Gold nanoparticles |
| BSA | Bovine serum albumin |
| CdTe | Cadmium telluride |
| CE | Certification Europe |
| CLIA | Clinical laboratory improvement amendments |
| CMOS | Complementary Metal-Oxide-Semiconductor Transistor |
| CNF | Carbon nanofibers |
| CS | Chitosan |
| Cys | Cystamine |
| DCIP | Dichlorophenol indophenol |
| DMSO | Dimethylsulphoxide |
| DPV | Differential pulse voltammetry |
| DTSP | 3,3′-Dithio-bis-propionic acid N-hydroxysuccinimide ester |
| EDC-NHS | ethyl (dimethylamino propyl) carbodiimide-N-hydroxysuccinimide |
| EIS | Electrochemical impedance spectroscopy |
| ELISA | Enzyme-linked immunosorbent assay |
| ESM | Egg-shell membranes |
| FAO | Fructosyl amino acid oxidase |
| FcBA | Ferrocene boronic acid |
| FDA | US Food and Drug Administration |
| FDMA | 1,1′-Di(aminomethyl)ferrocene |
| FET | Field-effect transistor |
| FPBA | 4-formyl-phenylboronic acid |
| FPBA | Formylphenyl boronic acid |
| FPBA2 | 3-Formylphenyl boronic acid (2 moiety) |
| FPOX | Fructosyl peptide oxidase |
| FTO | Fluorine-doped tin oxide |
| FV | Fructosyl-valine |
| GA | Glutaraldehyde |
| GCE | Glassy carbon electrode |
| G-COOH | Carboxylic acid-functionalized graphene |
| GCPE | Glassy carbon paste electrode |
| GG | Glycation gap |
| GN | Graphene nanosheets |
| GO | Graphene oxide |
| GOx | Glucose oxidase |
| GPP | Glycosylated pentapeptide |
| GS | Graphite sheets |
| Hb | Hemoglobin |
| HbA1c | Glycated hemoglobin |
| HGI | Hemoglobin glycation index |
| HPLC | High-Performance liquid chromatography |
| IFCC | International Federation of Clinical Chemistry and Laboratory Medicine |
| ISFETs | Ion-sensitive field-effect transistors |
| ITO | Indium-doped tin oxide |
| IVD | In vitro diagnostics |
| LoD | Limit of detection |
| MEMS | Micro-electro-mechanical system |
| MIP | Molecularly imprinted polymer |
| MNP | Magnetic bio-nanoparticles |
| MPA | 3-Mercaptopropionic acid |
| m-PMS | meta-phenazinemethosulphate |
| MU | 11-mercapto-1-undecanol |
| MUA | 11-Mercaptoundecanoic acid |
| MW | Oligo (phenyl ethynylene) molecular wires |
| MWCNTs | Multi-walled carbon nanotubes |
| NGSP | National Glycohemoglobin Standardization Program |
| OEG | Oligo (ethylene glycol) |
| PAMAM | Poly(amidoamine) G4 dendrimer |
| PAPBA | Poly(3-aminophenyl boronic acid) |
| PB | Prussian blue |
| PBS | Phosphate-buffered saline |
| PEEK | Polyether ether ketone |
| PET | Polyethylene terephthalate |
| PGE | Pyrolytic graphite working electrode |
| Ph-NH2 | 4-Aminophenyl |
| PIN5COOH | Poly indole-5-carboxylic acid |
| PoC | Point-of-care |
| POD | Peroxidase |
| PPy | Polypyrrole |
| PTA | 12-phosphotungstic acid |
| PtNPs | Platinum nanoparticles |
| pTTBA | Poly (terthiophene benzoic acid) |
| PVA–SbQ | Poly(vinyl alcohol)–stylbazole |
| PVI | Polyvinylimidazole |
| QD | Quantum Dots |
| RBC | Red blood cells |
| rGO | Reduced graphene oxide |
| RSIDE | Ring-shaped interdigitated electrode |
| RVC | Reticulated vitreous carbon |
| SAM | Self-assembled monolayer |
| SoCA | Fructosyl amino acid-binding protein |
| SPCE | Screen-printed carbon electrode |
| SRA | Stringent Regulatory Authority |
| SRMPs | Secondary reference measurement procedures |
| SWV | Square wave voltammetry |
| T3BA | Thiophene-3-boronic acid |
| TEOS | Tetraethyl orthosilicate |
| tHb | Total Hb |
| TiNT | Titania nanotubes |
| TiO2(G) NW | Graphene-embedded TiO2 nanowires |
| TTBA | 2,2′:5′,5″-terthiophene-3′-p-benzoic acid |
| WS2NPs | Tungsten disulfide nanoparticles |
| UCNPs | Upconversion nanoparticles |
| ZnONPs | Zinc oxide nanoparticles |
| ZrO2 | Zirconium dioxide |
References
- Vinik, A.; Flemmer, M. Diabetes and Macrovascular Disease. J. Diabetes Its Complicat. 2002, 16, 235–245. [Google Scholar] [CrossRef] [PubMed]
- Genuth, S.; Eastman, R.; Kahn, R.; Klein, R.; Lachin, J.; Lebovitz, H.; Nathan, D.; Vinicor, F. Implications of the United Kingdom Prospective Diabetes Study. Diabetes Care 2003, 26, S28–S32. [Google Scholar] [CrossRef]
- Shalini Devi, K.S.; Sasya, M.; Krishnan, U.M. Emerging Vistas on Electrochemical Detection of Diabetic Retinopathy Biomarkers. TrAC Trends Anal. Chem. 2020, 125, 115838. [Google Scholar] [CrossRef]
- Gross, J.L.; de Azevedo, M.J.; Silveiro, S.P.; Canani, L.H.; Caramori, M.L.; Zelmanovitz, T. Diabetic Nephropathy: Diagnosis, Prevention, and Treatment. Diabetes Care 2005, 28, 164–176. [Google Scholar] [CrossRef]
- Brown, M.J.; Asbury, A.K. Diabetic Neuropathy. Ann. Neurol. 1984, 15, 2–12. [Google Scholar] [CrossRef]
- International Diabetes Federation Facts & Figures. Available online: https://idf.org/aboutdiabetes/what-is-diabetes/facts-figures.html (accessed on 5 January 2023).
- Harris-Hayes, M.; Schootman, M.; Schootman, J.C.; Hastings, M.K. The Role of Physical Therapists in Fighting the Type 2 Diabetes Epidemic. J. Orthop. Sports Phys. Ther. 2020, 50, 5–16. [Google Scholar] [CrossRef]
- Diabetes Australia Diabetes Australia | Support for People Living with Diabetes. Available online: https://www.diabetesaustralia.com.au/ (accessed on 5 January 2023).
- Chen, B.; Bestetti, G.; Day, R.M.; Turner, A.P.F. The Synthesis and Screening of a Combinatorial Peptide Library for Affinity Ligands for Glycosylated Haemoglobin1This Paper Was a Finalist for the Biosensors & Bioelectronics Award for the Most Original Contribution to the Congress, but Was Withdrawn from the Competition by the Authors.1. Biosens. Bioelectron. 1998, 13, 779–785. [Google Scholar] [CrossRef]
- Sherwani, S.I.; Khan, H.A.; Ekhzaimy, A.; Masood, A.; Sakharkar, M.K. Significance of HbA1c Test in Diagnosis and Prognosis of Diabetic Patients. Biomark. Insights 2016, 11, 95–104. [Google Scholar] [CrossRef]
- Koval, D.; Kašička, V.; Cottet, H. Analysis of Glycated Hemoglobin A1c by Capillary Electrophoresis and Capillary Isoelectric Focusing. Anal. Biochem. 2011, 413, 8–15. [Google Scholar] [CrossRef]
- Jeppsson, J.-O.; Kobold, U.; Barr, J.; Finke, A.; Hoelzel, W.; Hoshino, T.; Miedema, K.; Mosca, A.; Mauri, P.; Paroni, R.; et al. Approved IFCC Reference Method for the Measurement of HbA1c in Human Blood. Clin. Chem. Lab. Med. 2002, 40, 78–89. [Google Scholar] [CrossRef]
- Pohanka, M. Glycated Hemoglobin and Methods for Its Point of Care Testing. Biosensors 2021, 11, 70. [Google Scholar] [CrossRef]
- Ang, S.H.; Thevarajah, M.; Alias, Y.; Khor, S.M. Current Aspects in Hemoglobin A1c Detection: A Review. Clin. Chim. Acta 2015, 439, 202–211. [Google Scholar] [CrossRef]
- Nathan, D.M.; Kuenen, J.; Borg, R.; Zheng, H.; Schoenfeld, D.; Heine, R.J. Translating the A1C Assay into Estimated Average Glucose Values. Diabetes Care 2008, 31, 1473–1478. [Google Scholar] [CrossRef]
- Association, A.D. 2. Classification and Diagnosis of Diabetes. Diabetes Care 2017, 40, S11–S24. [Google Scholar] [CrossRef] [PubMed]
- John, W.G. Haemoglobin A1c: Analysis and Standardisation. Clin. Chem. Lab. Med. 2003, 41, 1199–1212. [Google Scholar] [CrossRef] [PubMed]
- Ejaz, H.; Alsrhani, A.; Zafar, A.; Javed, H.; Junaid, K.; Abdalla, A.E.; Abosalif, K.O.A.; Ahmed, Z.; Younas, S. COVID-19 and Comorbidities: Deleterious Impact on Infected Patients. J. Infect. Public Health 2020, 13, 1833–1839. [Google Scholar] [CrossRef]
- Lim, S.; Bae, J.H.; Kwon, H.-S.; Nauck, M.A. COVID-19 and Diabetes Mellitus: From Pathophysiology to Clinical Management. Nat. Rev. Endocrinol. 2021, 17, 11–30. [Google Scholar] [CrossRef] [PubMed]
- Apicella, M.; Campopiano, M.C.; Mantuano, M.; Mazoni, L.; Coppelli, A.; Prato, S.D. COVID-19 in People with Diabetes: Understanding the Reasons for Worse Outcomes. Lancet Diabetes Endocrinol. 2020, 8, 782–792. [Google Scholar] [CrossRef]
- Ardestani, A.; Azizi, Z. Targeting Glucose Metabolism for Treatment of COVID-19. Signal Transduct. Target. Ther. 2021, 6, 112. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Bai, X.; Han, X.; Jiang, W.; Qiu, L.; Chen, S.; Yu, X. The Association of Diabetes and the Prognosis of COVID-19 Patients: A Retrospective Study. Diabetes Res. Clin. Pract. 2020, 169, 108386. [Google Scholar] [CrossRef]
- Zhan, Z.; Li, Y.; Zhao, Y.; Zhang, H.; Wang, Z.; Fu, B.; Li, W.J. A Review of Electrochemical Sensors for the Detection of Glycated Hemoglobin. Biosensors 2022, 12, 221. [Google Scholar] [CrossRef]
- Grieshaber, D.; MacKenzie, R.; Vörös, J.; Reimhult, E. Electrochemical Biosensors—Sensor Principles and Architectures. Sensors 2008, 8, 1400–1458. [Google Scholar] [CrossRef] [PubMed]
- Mandal, S.; Manasreh, M.O. An In-Vitro Optical Sensor Designed to Estimate Glycated Hemoglobin Levels. Sensors 2018, 18, 1084. [Google Scholar] [CrossRef]
- Sundararajan, J.; Palanisamy, V.; Sandeep, M. A Novel and Proven System for Non-Invasive Blood Glucose Monitoring Using HbA1C. Asian J. Appl. Sci. 2009, 2, 253–274. [Google Scholar] [CrossRef]
- Halámek, J.; Wollenberger, U.; Stöcklein, W.; Scheller, F.W. Development of a Biosensor for Glycated Hemoglobin. Electrochim. Acta 2007, 53, 1127–1133. [Google Scholar] [CrossRef]
- Ahn, K.-S.; Lee, J.H.; Park, J.-M.; Choi, H.N.; Lee, W.-Y. Luminol Chemiluminescence Biosensor for Glycated Hemoglobin (HbA1c) in Human Blood Samples. Biosens. Bioelectron. 2016, 75, 82–87. [Google Scholar] [CrossRef]
- Lin, Y.-C.; Lin, C.-Y.; Chen, H.-M.; Kuo, L.-P.; Hsieh, C.-E.; Wang, X.-H.; Cheng, C.-W.; Wu, C.-Y.; Chen, Y.-S. Direct and Label-Free Determination of Human Glycated Hemoglobin Levels Using Bacteriorhodopsin as the Biosensor Transducer. Sensors 2020, 20, 7274. [Google Scholar] [CrossRef]
- Li, H.; Huo, W.; He, M.; Lian, J.; Zhang, S.; Gao, Y. On-Chip Determination of Glycated Hemoglobin with a Novel Boronic Acid Copolymer. Sens. Actuators B Chem. 2017, 253, 542–551. [Google Scholar] [CrossRef]
- Wang, B.; Anzai, J. Recent Progress in Electrochemical HbA1c Sensors: A Review. Materials 2015, 8, 1187–1203. [Google Scholar] [CrossRef]
- Nanjo, Y.; Hayashi, R.; Yao, T. An Enzymatic Method for the Rapid Measurement of the Hemoglobin A1c by a Flow-Injection System Comprised of an Electrochemical Detector with a Specific Enzyme-Reactor and a Spectrophotometer. Anal. Chim. Acta 2007, 583, 45–54. [Google Scholar] [CrossRef]
- Liu, S.; Wollenberger, U.; Katterle, M.; Scheller, F.W. Ferroceneboronic Acid-Based Amperometric Biosensor for Glycated Hemoglobin. Sens. Actuators B Chem. 2006, 113, 623–629. [Google Scholar] [CrossRef]
- Liu, A.; Xu, S.; Deng, H.; Wang, X. A New Electrochemical HbA1c Biosensor Based on Flow Injection and Screen-Printed Electrode. Int. J. Electrochem. Sci. 2016, 11, 3086–3094. [Google Scholar] [CrossRef]
- Kim, D.-M.; Shim, Y.-B. Disposable Amperometric Glycated Hemoglobin Sensor for the Finger Prick Blood Test. Anal. Chem. 2013, 85, 6536–6543. [Google Scholar] [CrossRef]
- Wang, X.; Su, J.; Zeng, D.; Liu, G.; Liu, L.; Xu, Y.; Wang, C.; Liu, X.; Wang, L.; Mi, X. Gold Nano-Flowers (Au NFs) Modified Screen-Printed Carbon Electrode Electrochemical Biosensor for Label-Free and Quantitative Detection of Glycated Hemoglobin. Talanta 2019, 201, 119–125. [Google Scholar] [CrossRef]
- Song, S.Y.; Yoon, H.C. Boronic Acid-Modified Thin Film Interface for Specific Binding of Glycated Hemoglobin (HbA1c) and Electrochemical Biosensing. Sens. Actuators B Chem. 2009, 140, 233–239. [Google Scholar] [CrossRef]
- Song, S.Y.; Han, Y.D.; Park, Y.M.; Jeong, C.Y.; Yang, Y.J.; Kim, M.S.; Ku, Y.; Yoon, H.C. Bioelectrocatalytic Detection of Glycated Hemoglobin (HbA1c) Based on the Competitive Binding of Target and Signaling Glycoproteins to a Boronate-Modified Surface. Biosens. Bioelectron. 2012, 35, 355–362. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.-Y.; Chou, T.-C.; Chen, L.-C.; Ho, K.-C. Using Poly(3-Aminophenylboronic Acid) Thin Film with Binding-Induced Ion Flux Blocking for Amperometric Detection of Hemoglobin A1c. Biosens. Bioelectron. 2015, 63, 317–324. [Google Scholar] [CrossRef] [PubMed]
- Thiruppathi, M.; Lee, J.-F.; Chen, C.C.; Ho, J.A. A Disposable Electrochemical Sensor Designed to Estimate Glycated Hemoglobin (HbA1c) Level in Whole Blood. Sens. Actuators B Chem. 2021, 329, 129119. [Google Scholar] [CrossRef]
- Boonyasit, Y.; Heiskanen, A.; Chailapakul, O.; Laiwattanapaisal, W. Selective Label-Free Electrochemical Impedance Measurement of Glycated Haemoglobin on 3-Aminophenylboronic Acid-Modified Eggshell Membranes. Anal. Bioanal. Chem. 2015, 407, 5287–5297. [Google Scholar] [CrossRef] [PubMed]
- Boonyasit, Y.; Laiwattanapaisal, W.; Chailapakul, O.; Emnéus, J.; Heiskanen, A.R. Boronate-Modified Interdigitated Electrode Array for Selective Impedance-Based Sensing of Glycated Hemoglobin. Anal. Chem. 2016, 88, 9582–9589. [Google Scholar] [CrossRef]
- Park, J.-Y.; Chang, B.-Y.; Nam, H.; Park, S.-M. Selective Electrochemical Sensing of Glycated Hemoglobin (HbA1c) on Thiophene-3-Boronic Acid Self-Assembled Monolayer Covered Gold Electrodes. Anal. Chem. 2008, 80, 8035–8044. [Google Scholar] [CrossRef]
- Krishna, V.S.R.; Bhat, N.; Amrutur, B.; Chakrapani, K.; Sampath, S. Detection of Glycated Hemoglobin Using 3-Aminophenylboronic Acid Modified Graphene Oxide. In Proceedings of the 2011 IEEE/NIH Life Science Systems and Applications Workshop (LiSSA), Bethesda, MD, USA, 9–10 April 2011; pp. 1–4. [Google Scholar]
- Hsieh, K.-M.; Lan, K.-C.; Hu, W.-L.; Chen, M.-K.; Jang, L.-S.; Wang, M.-H. Glycated Hemoglobin (HbA1c) Affinity Biosensors with Ring-Shaped Interdigital Electrodes on Impedance Measurement. Biosens. Bioelectron. 2013, 49, 450–456. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Li, J.; Dou, Y.; Wang, L.; Song, S. A Carbon-Based Antifouling Nano-Biosensing Interface for Label-Free POCT of HbA1c. Biosensors 2021, 11, 118. [Google Scholar] [CrossRef]
- Nallal, M.; Anantha Iyengar, G.; Pill-Lee, K. New Titanium Dioxide-Based Heterojunction Nanohybrid for Highly Selective Photoelectrochemical–Electrochemical Dual-Mode Sensors. ACS Appl. Mater. Interfaces 2017, 9, 37166–37183. [Google Scholar] [CrossRef] [PubMed]
- Boonyasit, Y.; Chailapakul, O.; Laiwattanapaisal, W. A Multiplexed Three-Dimensional Paper-Based Electrochemical Impedance Device for Simultaneous Label-Free Affinity Sensing of Total and Glycated Haemoglobin: The Potential of Using a Specific Single-Frequency Value for Analysis. Anal. Chim. Acta 2016, 936, 1–11. [Google Scholar] [CrossRef]
- Molazemhosseini, A.; Magagnin, L.; Vena, P.; Liu, C.-C. Single-Use Disposable Electrochemical Label-Free Immunosensor for Detection of Glycated Hemoglobin (HbA1c) Using Differential Pulse Voltammetry (DPV). Sensors 2016, 16, 1024. [Google Scholar] [CrossRef]
- Liu, G.; Khor, S.M.; Iyengar, S.G.; Gooding, J.J. Development of an Electrochemical Immunosensor for the Detection of HbA1c in Serum. Analyst 2012, 137, 829–832. [Google Scholar] [CrossRef] [PubMed]
- Liu, G.; Iyengar, S.G.; Gooding, J.J. An Electrochemical Impedance Immunosensor Based on Gold Nanoparticle-Modified Electrodes for the Detection of HbA1c in Human Blood. Electroanalysis 2012, 24, 1509–1516. [Google Scholar] [CrossRef]
- Liu, G.; Iyengar, S.G.; Gooding, J.J. An Amperometric Immunosensor Based on a Gold Nanoparticle-Diazonium Salt Modified Sensing Interface for the Detection of HbA1c in Human Blood. Electroanalysis 2013, 25, 881–887. [Google Scholar] [CrossRef]
- Qu, L.; Xia, S.; Bian, C.; Sun, J.; Han, J. A Micro-Potentiometric Hemoglobin Immunosensor Based on Electropolymerized Polypyrrole–Gold Nanoparticles Composite. Biosens. Bioelectron. 2009, 24, 3419–3424. [Google Scholar] [CrossRef]
- Xue, Q.; Bian, C.; Tong, J.; Sun, J.; Zhang, H.; Xia, S. A Micro Potentiometric Immunosensor for Hemoglobin-A1c Level Detection Based on Mixed SAMs Wrapped Nano-Spheres Array. Biosens. Bioelectron. 2011, 26, 2689–2693. [Google Scholar] [CrossRef] [PubMed]
- Bian, C.; Tong, J.; Sun, J.; Zhang, H.; Xue, Q.; Xia, S. A Field Effect Transistor (FET)-Based Immunosensor for Detection of HbA1c and Hb. Biomed. Microdevices 2011, 13, 345–352. [Google Scholar] [CrossRef]
- Xue, Q.; Bian, C.; Tong, J.; Sun, J.; Zhang, H.; Xia, S. FET Immunosensor for Hemoglobin A1c Using a Gold Nanofilm Grown by a Seed-Mediated Technique and Covered with Mixed Self-Assembled Monolayers. Microchim. Acta 2012, 176, 65–72. [Google Scholar] [CrossRef]
- Tanaka, J.; Ishige, Y.; Iwata, R.; Maekawa, B.; Nakamura, H.; Sawazaki, T.; Kamahori, M. Direct Detection for Concentration Ratio of HbA1c to Total Hemoglobin by Using Potentiometric Immunosensor with Simple Process of Denaturing HbA1c. Sens. Actuators B Chem. 2018, 260, 396–399. [Google Scholar] [CrossRef]
- Chopra, A.; Tuteja, S.; Sachdeva, N.; Bhasin, K.K.; Bhalla, V.; Suri, C.R. CdTe Nanobioprobe Based Optoelectrochemical Immunodetection of Diabetic Marker HbA1c. Biosens. Bioelectron. 2013, 44, 132–135. [Google Scholar] [CrossRef] [PubMed]
- Zhao, H.; Qiu, X.; Su, E.; Huang, L.; Zai, Y.; Liu, Y.; Chen, H.; Wang, Z.; Chen, Z.; Li, S.; et al. Multiple Chemiluminescence Immunoassay Detection of the Concentration Ratio of Glycosylated Hemoglobin A1c to Total Hemoglobin in Whole Blood Samples. Anal. Chim. Acta 2022, 1192, 339379. [Google Scholar] [CrossRef]
- Zhou, W.; Huang, P.-J.J.; Ding, J.; Liu, J. Aptamer-Based Biosensors for Biomedical Diagnostics. Analyst 2014, 139, 2627–2640. [Google Scholar] [CrossRef]
- Shajaripour Jaberi, S.Y.; Ghaffarinejad, A.; Omidinia, E. An Electrochemical Paper Based Nano-Genosensor Modified with Reduced Graphene Oxide-Gold Nanostructure for Determination of Glycated Hemoglobin in Blood. Anal. Chim. Acta 2019, 1078, 42–52. [Google Scholar] [CrossRef]
- Eissa, S.; Zourob, M. Aptamer-Based Label-Free Electrochemical Biosensor Array for the Detection of Total and Glycated Hemoglobin in Human Whole Blood. Sci. Rep. 2017, 7, 1016. [Google Scholar] [CrossRef]
- Eissa, S.; Almusharraf, A.Y.; Zourob, M. A Comparison of the Performance of Voltammetric Aptasensors for Glycated Haemoglobin on Different Carbon Nanomaterials-Modified Screen Printed Electrodes. Mater. Sci. Eng. C 2019, 101, 423–430. [Google Scholar] [CrossRef]
- Chien, H.-C.; Chou, T.-C. Glassy Carbon Paste Electrodes for the Determination of Fructosyl Valine. Electroanalysis 2010, 22, 688–693. [Google Scholar] [CrossRef]
- Sode, K.; Takahashi, Y.; Ohta, S.; Tsugawa, W.; Yamazaki, T. A New Concept for the Construction of an Artificial Dehydrogenase for Fructosylamine Compounds and Its Application for an Amperometric Fructosylamine Sensor. Anal. Chim. Acta 2001, 435, 151–156. [Google Scholar] [CrossRef]
- Chuang, S.-W.; Rick, J.; Chou, T.-C. Electrochemical Characterisation of a Conductive Polymer Molecularly Imprinted with an Amadori Compound. Biosens. Bioelectron. 2009, 24, 3170–3173. [Google Scholar] [CrossRef]
- Pandey, I.; Tiwari, J.D. A Novel Dual Imprinted Conducting Nanocubes Based Flexible Sensor for Simultaneous Detection of Hemoglobin and Glycated Haemoglobin in Gestational Diabetes Mellitus Patients. Sens. Actuators B Chem. 2019, 285, 470–478. [Google Scholar] [CrossRef]
- Rick, J.; Chou, T.-C. Amperometric Protein Sensor—Fabricated as a Polypyrrole, Poly-Aminophenylboronic Acid Bilayer. Biosens. Bioelectron. 2006, 22, 329–335. [Google Scholar] [CrossRef] [PubMed]
- Hirokawa, K.; Nakamura, K.; Kajiyama, N. Enzymes Used for the Determination of HbA1C. FEMS Microbiol. Lett. 2004, 235, 157–162. [Google Scholar] [CrossRef]
- Pundir, C.S.; Chawla, S. Determination of Glycated Hemoglobin with Special Emphasis on Biosensing Methods. Anal. Biochem. 2014, 444, 47–56. [Google Scholar] [CrossRef]
- Tsugawa, W.; Ishimura, F.; Ogawa, K.; Sode, K. Development of an Enzyme Sensor Utilizing a Novel Fructosyl Amine Oxidase from a Marine Yeast. Electrochemistry 2000, 68, 869–871. [Google Scholar] [CrossRef]
- Tsugawa, W.; Ogawa, K.; Ishimura, F.; Sode, K. Fructosyl Amine Sensing Based on Prussian Blue Modified Enzyme Electrode. Electrochemistry 2001, 69, 973–975. [Google Scholar] [CrossRef]
- Chawla, S.; Pundir, C.S. An Amperometric Hemoglobin A1c Biosensor Based on Immobilization of Fructosyl Amino Acid Oxidase onto Zinc Oxide Nanoparticles–Polypyrrole Film. Anal. Biochem. 2012, 430, 156–162. [Google Scholar] [CrossRef]
- Chawla, S.; Pundir, C.S. An Electrochemical Biosensor for Fructosyl Valine for Glycosylated Hemoglobin Detection Based on Core–Shell Magnetic Bionanoparticles Modified Gold Electrode. Biosens. Bioelectron. 2011, 26, 3438–3443. [Google Scholar] [CrossRef]
- Jain, U.; Singh, A.; Kuchhal, N.K.; Chauhan, N. Glycated Hemoglobin Biosensing Integration Formed on Au Nanoparticle-Dotted Tubular TiO2 Nanoarray. Anal. Chim. Acta 2016, 945, 67–74. [Google Scholar] [CrossRef] [PubMed]
- Jain, U.; Gupta, S.; Chauhan, N. Construction of an Amperometric Glycated Hemoglobin Biosensor Based on Au–Pt Bimetallic Nanoparticles and Poly (Indole-5-Carboxylic Acid) Modified Au Electrode. Int. J. Biol. Macromol. 2017, 105, 549–555. [Google Scholar] [CrossRef]
- Jain, U.; Chauhan, N. Glycated Hemoglobin Detection with Electrochemical Sensing Amplified by Gold Nanoparticles Embedded N-Doped Graphene Nanosheet. Biosens. Bioelectron. 2017, 89, 578–584. [Google Scholar] [CrossRef]
- Jain, U.; Gupta, S.; Chauhan, N. Detection of Glycated Hemoglobin with Voltammetric Sensing Amplified by 3D-Structured Nanocomposites. Int. J. Biol. Macromol. 2017, 101, 896–903. [Google Scholar] [CrossRef] [PubMed]
- Fang, L.; Li, W.; Zhou, Y.; Liu, C.-C. A Single-Use, Disposable Iridium-Modified Electrochemical Biosensor for Fructosyl Valine for the Glycoslated Hemoglobin Detection. Sens. Actuators B Chem. 2009, 137, 235–238. [Google Scholar] [CrossRef]
- Liu, S.; Leng, J.; Aquino, T.C. Development of Disposable Single-Use Biosensor for Fructosyl Valine and Glycated Hemoglobin A1c. J. Sens. Technol. 2019, 9, 45–53. [Google Scholar] [CrossRef]
- Shahbazmohammadi, H.; Sardari, S.; Omidinia, E. An Amperometric Biosensor for Specific Detection of Glycated Hemoglobin Based on Recombinant Engineered Fructosyl Peptide Oxidase. Int. J. Biol. Macromol. 2020, 142, 855–865. [Google Scholar] [CrossRef]
- Lee, T.-H.; Lin, C.-L.; Wu, C.-C.; Lee, G.-B. An Integrated Microfluidic System for Rapid HbA1c and Glucose Measurement. In Proceedings of the 2013 Transducers & Eurosensors XXVII: The 17th International Conference on Solid-State Sensors, Actuators and Microsystems (TRANSDUCERS & EUROSENSORS XXVII), Barcelona, Spain, 16–20 June 2013; pp. 860–863. [Google Scholar]
- Ogawa, K.; Stöllner, D.; Scheller, F.; Warsinke, A.; Ishimura, F.; Tsugawa, W.; Ferri, S.; Sode, K. Development of a Flow-Injection Analysis (FIA) Enzyme Sensor for Fructosyl Amine Monitoring. Anal. Bioanal. Chem. 2002, 373, 211–214. [Google Scholar] [CrossRef]
- Zhao, Q.; Tang, S.; Fang, C.; Tu, Y.-F. Titania Nanotubes Decorated with Gold Nanoparticles for Electrochemiluminescent Biosensing of Glycosylated Hemoglobin. Anal. Chim. Acta 2016, 936, 83–90. [Google Scholar] [CrossRef]
- Hatada, M.; Tran, T.-T.; Tsugawa, W.; Sode, K.; Mulchandani, A. Affinity Sensor for Haemoglobin A1c Based on Single-Walled Carbon Nanotube Field-Effect Transistor and Fructosyl Amino Acid Binding Protein. Biosens. Bioelectron. 2019, 129, 254–259. [Google Scholar] [CrossRef] [PubMed]
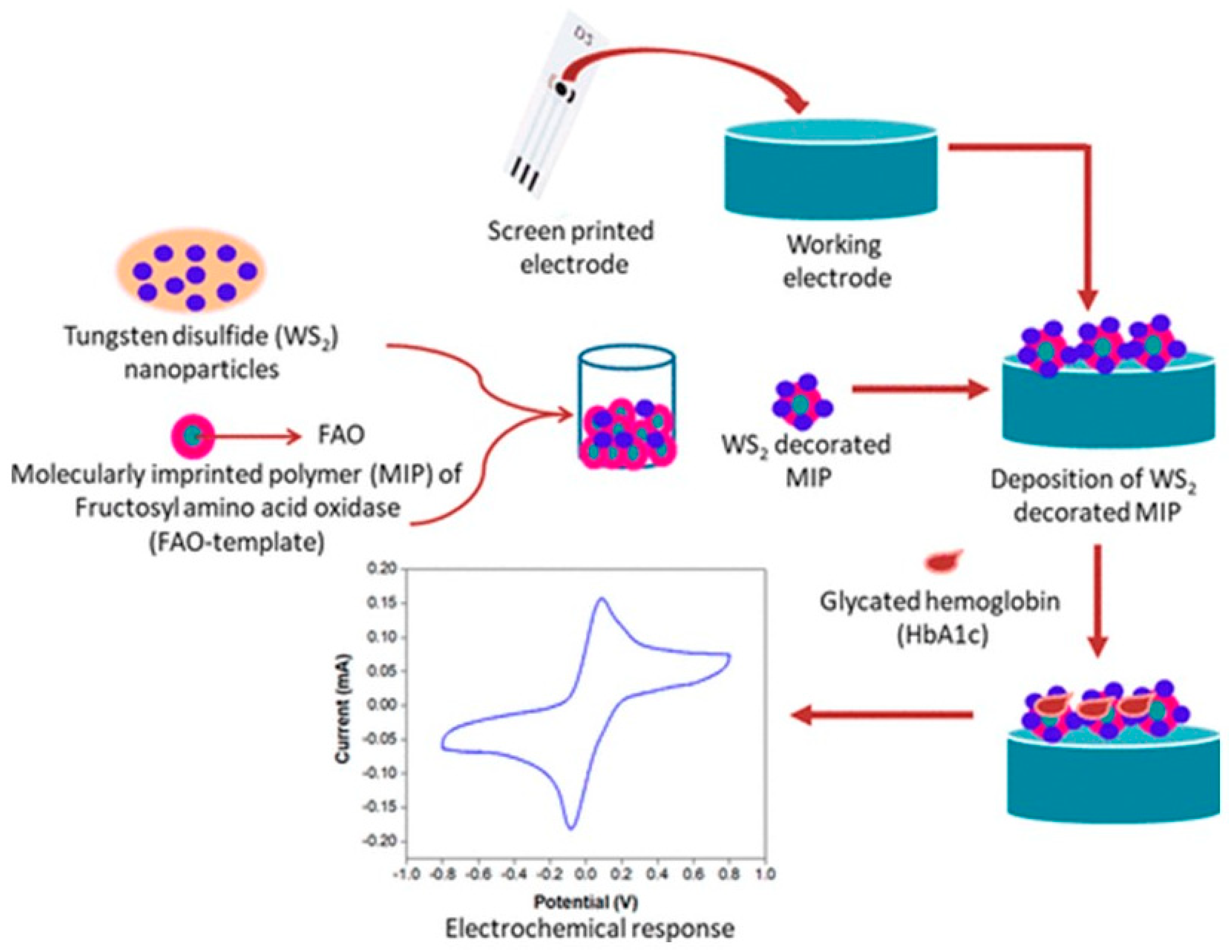
- Mahobiya, S.K.; Balayan, S.; Chauhan, N.; Khanuja, M.; Kuchhal, N.K.; Islam, S.S.; Jain, U. Tungsten Disulfide Decorated Screen-Printed Electrodes for Sensing of Glycated Hemoglobin. ACS Omega 2022, 7, 34676–34684. [Google Scholar] [CrossRef]
- Kumar, V.; Hebbar, S.; Bhat, A.; Panwar, S.; Vaishnav, M.; Muniraj, K.; Nath, V.; Vijay, R.B.; Manjunath, S.; Thyagaraj, B.; et al. Application of a Nanotechnology-Based, Point-of-Care Diagnostic Device in Diabetic Kidney Disease. Kidney Int. Rep. 2018, 3, 1110–1118. [Google Scholar] [CrossRef]
- Bry, L.; Chen, P.C.; Sacks, D.B. Effects of Hemoglobin Variants and Chemically Modified Derivatives on Assays for Glycohemoglobin. Clin. Chem. 2001, 47, 153–163. [Google Scholar] [CrossRef] [PubMed]
- Turpeinen, U.; Karjalainen, U.; Stenman, U.H. Three Assays for Glycohemoglobin Compared. Clin. Chem. 1995, 41, 191–195. [Google Scholar] [CrossRef]
- Sharma, P.; Panchal, A.; Yadav, N.; Narang, J. Analytical Techniques for the Detection of Glycated Haemoglobin Underlining the Sensors. Int. J. Biol. Macromol. 2020, 155, 685–696. [Google Scholar] [CrossRef] [PubMed]
- Lenters-Westra, E.; English, E. Evaluation of Four HbA1c Point-of-Care Devices Using International Quality Targets: Are They Fit for the Purpose? J. Diabetes Sci. Technol. 2018, 12, 762–770. [Google Scholar] [CrossRef]
- Lenters-Westra, E.; English, E. Evaluating New HbA1c Methods for Adoption by the IFCC and NGSP Reference Networks Using International Quality Targets. Clin. Chem. Lab. Med. (CCLM) 2017, 55, 1426–1434. [Google Scholar] [CrossRef]
- Chang, A.; Frank, J.; Knaebel, J.; Fullam, J.; Pardo, S.; Simmons, D.A. Evaluation of an Over-the-Counter Glycated Hemoglobin (A1C) Test Kit. J. Diabetes Sci. Technol. 2010, 4, 1495–1503. [Google Scholar] [CrossRef]
- Joergensen, B.; Zidek, A.S. A New Point-of-Care Analyzer for Rapid and Precise Determination of Lipid Profile and Hba1c. Atherosclerosis 2014, 235, e288–e289. [Google Scholar] [CrossRef]
- Arabadjief, M.; Nichols, J.H. Evaluation of the Afinion AS100 Point-of-Care Analyzer for Hemoglobin A1c. Point Care 2009, 8, 11. [Google Scholar] [CrossRef]
- Menéndez-Valladares, P.; Fernández-Riejos, P.; Sánchez-Mora, C.; Pérez-Pérez, A.; Sánchez-Margalet, V.; González-Rodríguez, C. Evaluation of a HbA1c Point-of-Care Analyzer. Clin. Biochem. 2015, 48, 686–689. [Google Scholar] [CrossRef]
- Lee, K.; Jun, S.-H.; Han, M.; Song, S.H.; Park, K.U.; Song, W.H.; Song, J. Performance Evaluation of SD A1cCare as a HbA1c Analyzer for Point-of-Care Testing. Clin. Biochem. 2015, 48, 625–627. [Google Scholar] [CrossRef] [PubMed]
- Lau, C.S.; Tong, C.H.; Goh, R.; Aw, T.C. Evaluation of a New Point-of-Care HbA1c Assay: The Pixotest. Int. J. Clin. Chem. Lab. Med. 2019, 5, 1–5. [Google Scholar] [CrossRef]
- Jana Care Jana Care—Diabetes. Available online: https://www.janacare.com/diabetes.html (accessed on 6 January 2023).
- Szymezak, J.; Leroy, N.; Lavalard, E.; Gillery, P. Evaluation of the DCA Vantage Analyzer for HbA1c Assay. Clin. Chem. Lab. Med. 2008, 46, 1195–1198. [Google Scholar] [CrossRef]
- Gallagher, E.J.; Le Roith, D.; Bloomgarden, Z. Review of Hemoglobin A1c in the Management of Diabetes. J. Diabetes 2009, 1, 9–17. [Google Scholar] [CrossRef]
- Kaur, J.; Jiang, C.; Liu, G. Different Strategies for Detection of HbA1c Emphasizing on Biosensors and Point-of-Care Analyzers. Biosens. Bioelectron. 2019, 123, 85–100. [Google Scholar] [CrossRef]
- Lenters-Westra, E.; Slingerland, R.J. Six of Eight Hemoglobin A1c Point-of-Care Instruments Do Not Meet the General Accepted Analytical Performance Criteria. Clin. Chem. 2010, 56, 44–52. [Google Scholar] [CrossRef] [PubMed]
- Paknikar, S.; Sarmah, R.; Sivaganeshan, L.; Welke, A.; Rizzo, A.; Larson, K.; Rendell, M. Long-Term Performance of Point-of-Care Hemoglobin A1c Assays. J. Diabetes Sci. Technol. 2016, 10, 1308–1315. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.-J.; Lim, S.; Kwon, M.-J.; Woo, H.-Y.; Park, H. Evaluation of Cobas b 101 HbA1c Analyzer Performance for Point-of-Care Testing. Lab. Med. Online 2017, 7, 182–188. [Google Scholar] [CrossRef]
- FIND Page Not Found. Available online: https://www.finddx.org/reports-and-landscapes/ (accessed on 5 January 2023).
- Liddy, A.M.; Grundy, S.; Sreenan, S.; Tormey, W. Impact of Haemoglobin Variants on the Use of Haemoglobin A1c for the Diagnosis and Monitoring of Diabetes: A Contextualised Review. Ir. J. Med. Sci. 2022, 192, 69–176. [Google Scholar] [CrossRef] [PubMed]
- Bain, B.J. Haemoglobinopathy Diagnosis: Algorithms, Lessons and Pitfalls. Blood Rev. 2011, 25, 205–213. [Google Scholar] [CrossRef]
- Aljenaee, K.; Hakami, O.; Davenport, C.; Farrell, G.; Tun, T.K.; Pazderska, A.; Phelan, N.; Healy, M.-L.; Sreenan, S.; McDermott, J.H. Spurious HbA1c Results in Patients with Diabetes Treated with Dapsone. Endocrinol. Diabetes Metab. Case Rep. 2019, 2019, 19–27. [Google Scholar] [CrossRef]
- Kim, M.K.; Jeong, J.S.; Kwon, H.-S.; Baek, K.H.; Song, K.-H. Concordance the Hemoglobin Glycation Index with Glycation Gap Using Glycated Albumin in Patients with Type 2 Diabetes. J. Diabetes Its Complicat. 2017, 31, 1127–1131. [Google Scholar] [CrossRef] [PubMed]
- Zafon, C.; Ciudin, A.; Valladares, S.; Mesa, J.; Simó, R. Variables Involved in the Discordance between HbA1c and Fructosamine: The Glycation Gap Revisited. PLoS ONE 2013, 8, e66696. [Google Scholar] [CrossRef] [PubMed]

| Biosensors | Transducers | Type | Detection Range (HbA1c) | Sensitivity | LoD | Ref. |
|---|---|---|---|---|---|---|
| Aptamer | Aptamer/rGO-Au/GS | DPV | 1–13.83 μM | 269.2 μA·cm−2 | 1 nM | [61] |
| Aptamer/AuNP/SPCE | SWV | 100 pg/mL–100 ng/mL | NA | 0.2 ng/mL | [62] | |
| Aptamer/SWCNT/SPCE | SWV | 0.1 pg/mL–1000 ng/mL | NA | 0.03 pg/mL | [63] | |
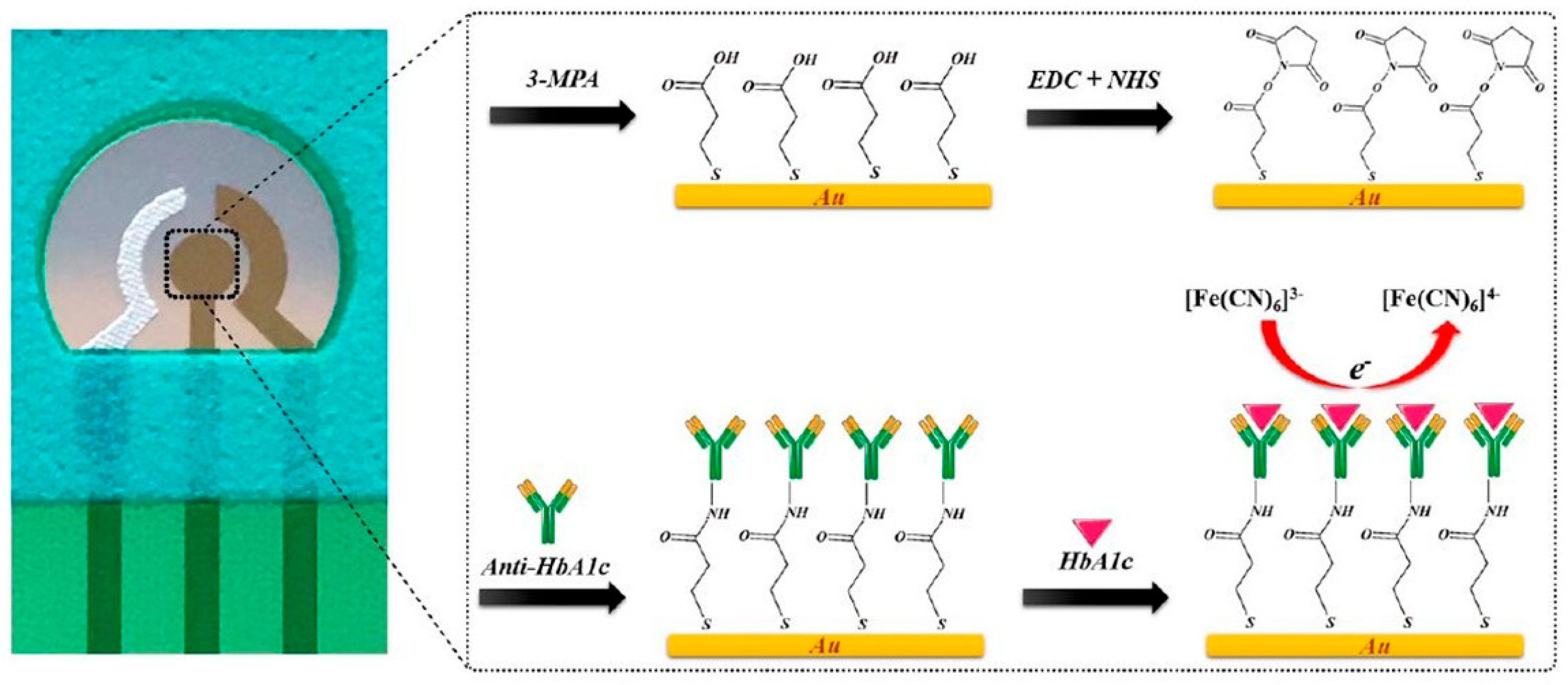
| Immunosensors | Anti-HbA1c/MPA/Au | DPV | 7.5–20 μg/mL (0.1 M PBS) 0.10–0.25 mg/mL (undiluted human serum) | NA | NA | [49] |
| GPP/FDMA/MW/GCE (Competitive inhibition assay) | SWV | 4.5–15.1% | NA | NA | [50] | |
| GPP/Ph-NH2/Au/Ph-NH2/GCE (Competitive inhibition assay) | Impedimetric | 0–23.3% | NA | NA | [51] | |
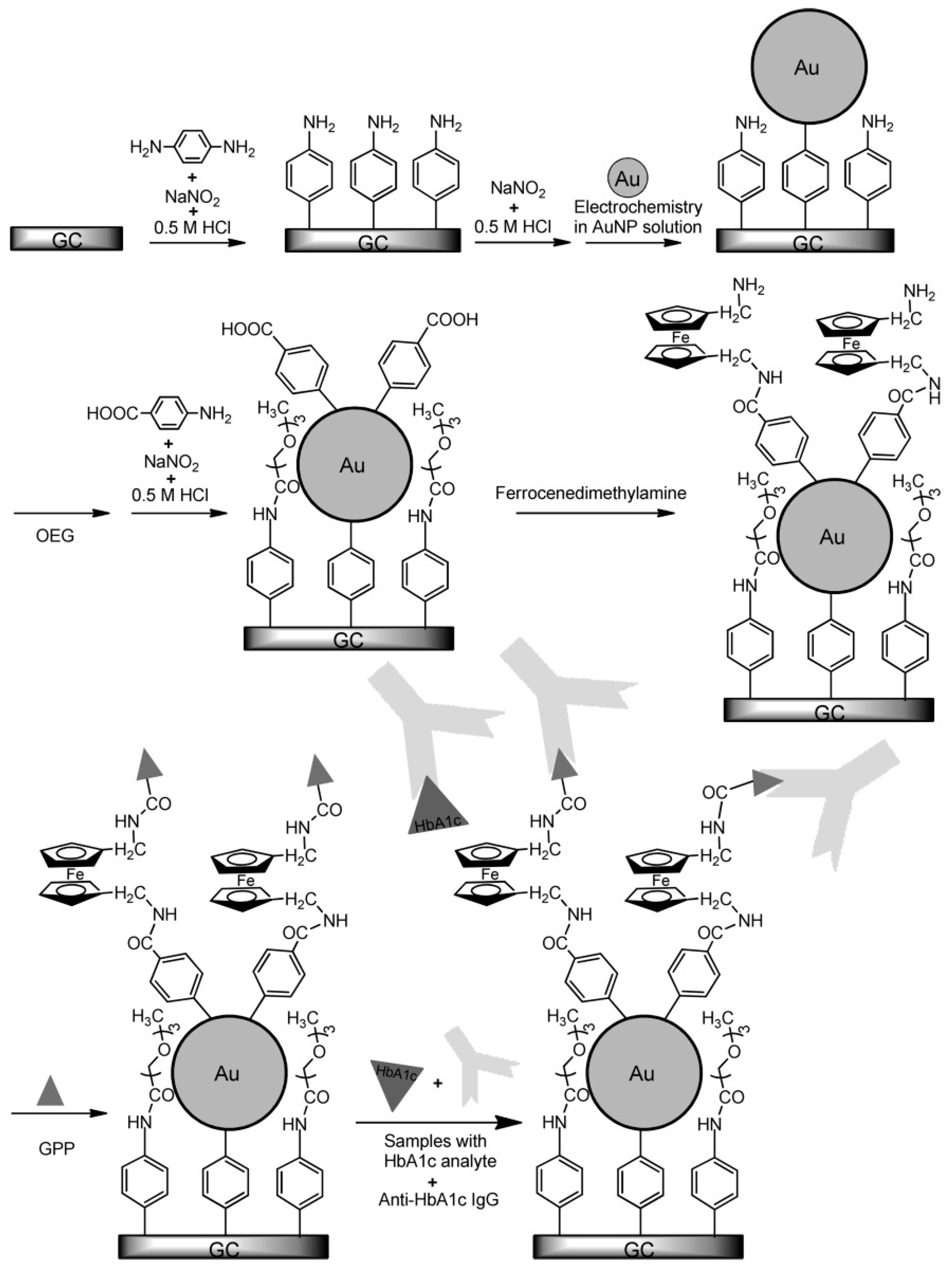
| GPP/FDMA/4ABA/Au/Ph-NH2/GCE (Competitive inhibition assay) | Amperometric | 4.6–15.1% | NA | NA | [52] | |
| Anti-HbA1c/Au/PPy/Au | Potentiometric | 4–18 μg/mL | 1.5087 Mv μg−1 mL | NA | [53] | |
| Anti-HbA1c/Mixed SAM-wrapped Au spheres/Au | Potentiometric | 50–170.5 ng/mL | 94.73 μV ng−1 mL | NA | [54] | |
| Anti-HbA1c/AuNP/SAM/Au | Potentiometric | 4–24 μg/mL | −90.6 mV/[log(μg/mL)] | NA | [55] | |
| Anti-HbA1c/Mixed SAM/AuNP/Au | Potentiometric | 1.67–72.14 ng/mL | 165.2 μV ng−1 mL | NA | [56] | |
| CdTe | Anodic stripping voltammetry (ASV) | 4–16% | NA | NA | [58] | |
| Anti-HbA1c/BSA/MWCNTs/GA/SPCE | Voltametric | 2–15% | NA | 0.4% | [46] |
| Manufacturer | Device Name | Method | Sample Volume (µL) | Detection Range | Analysis Time (s) | SRA Approvals | Ref. |
|---|---|---|---|---|---|---|---|
| Abbott (Scarborough, ME, USA) | Afinion 2 | Boronate affinity | 1.5 | 4.0–15.0%/ 20–140 mmol/mol | 180 | CE-IVD, FDA (CLIA waived), Japan | [91] |
| NycoCard Reader II | 5.0 | 4.0–15.0%/ 20–140 mmol/mol | 180 | CE-IVD | [92] | ||
| Aidian (Espoo, Finland) | QuikRead go | Immunoassay | 1.0 | 4.0–15.0%/ 20–151 mmol/mol | 350 | CE-IVD | [93] |
| Arkray Inc. (Kyoto, Japan) | The Lab 001 | Capillary electrophoresis | 1.5 | 4.0–16.0%/ 20–151 mmol/mol | 90 | Japan | [93] |
| Boditech Med (Gang-won-do, Republic of Korea) | Ichroma II | Immunoassay | 5 | 4.0–15.0%/ 20–140 mmol/mol | 720 | CE-IVD | [94] |
| DiaSys (Holzheim, Germany) | InnovaStar | Enzymatic | 10 | 3.0–14.0%/ 9–130 mmol/mol | <300 | CE-IVD | [93] |
| EKF Diagnostics (Penarth, UK) | Quo-Lab | Boronate affinity | 4 | 4.0–15.0%/ 20–140 mmol/mol | 240 | CE-IVD | [95] |
| Quo-Test | CE-IVD, FDA | [95] | |||||
| Green Cross MEDIS Corp. (Yongin, Republic of Korea) | CERA STAT 2000 | Boronate affinity | 5 | 3.0–15.0%/ 9–140 mmol/mol | <180 | CE-IVD | [96] |
| HemoCue (Ängelholm, Sweden) | HbA1c 501 | Boronate affinity | 4 | 4–14.0% 20–130 mmol/mol | 300 | CE-IVD | [91] |
| Human Gesellschaft für Biochemica und Diagnostica GmbH (Wiesbaden, Germany) | HumaMeter A1c | Boronate affinity | 4 | 4.0–15.0%/ 20–140 mmol/mol | 240 | CE-IVD | [97] |
| i-SENS Inc. (Seoul, Republic of Korea) | A1Care | Enzymatic | 2.5 | 4.0–15.0%/ 20–140 mmol/mol | 260 | CE-IVD | [93] |
| iXensor (Taipei City, Taiwan) | PixoTest | Immunoassay | 5 | 4.0–15.0%/ 20–140 mmol/mol | 180 | CE-IVD, FDA | [98] |
| Jana Care (Bangalore, Karnataka, India) | Aina | Boronate affinity | 5 | 4–15%/20–140 mmol/mol | 180 | CE-IVD | [99] |
| OSANG Healthcare (Gyeonggi-do, Republic of Korea) | Clover A1c Plus | Boronate affinity | 4 | 4.0–14.0%/ 20–130 mmol/mol | 300 | CE-IVD, FDA | [93] |
| PTS Diagnostics (Whitestown, IN, USA) | A1cNow+ | Immunoassay | 5 | 4.0–13.0%/ 20–120 mmol/mol | 300 | CE-IVD, FDA (CLIA waived) | [100] |
| Roche Diagnostics (Risch-Rotkreuz, Switzerland) | Cobas b 101 | Immunoassay | 2 | 4.0–14.0%/ 20–130 mmol/mol | 320 | CE-IVD, FDA | [93] |
| Siemens Healthineers (Erlangen, Germany) | DCA Vantage | Immunoassay | 1 | 2.5–14.0%/ 4–130 mmol/mol | 360 | CE-IVD, FDA (CLIA waived) | [93] |
| Wuxi BioHermes Biomedical Technology Co. (Wuxi, China) | A1C EZ 2.0 | Boronate affinity | 3 | 4.0–14.0%/ 20.2–129.5 mmol/mol | 360 | CE-IVD | [101] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mandali, P.K.; Prabakaran, A.; Annadurai, K.; Krishnan, U.M. Trends in Quantification of HbA1c Using Electrochemical and Point-of-Care Analyzers. Sensors 2023, 23, 1901. https://doi.org/10.3390/s23041901
Mandali PK, Prabakaran A, Annadurai K, Krishnan UM. Trends in Quantification of HbA1c Using Electrochemical and Point-of-Care Analyzers. Sensors. 2023; 23(4):1901. https://doi.org/10.3390/s23041901
Chicago/Turabian StyleMandali, Pavan Kumar, Amrish Prabakaran, Kasthuri Annadurai, and Uma Maheswari Krishnan. 2023. "Trends in Quantification of HbA1c Using Electrochemical and Point-of-Care Analyzers" Sensors 23, no. 4: 1901. https://doi.org/10.3390/s23041901
APA StyleMandali, P. K., Prabakaran, A., Annadurai, K., & Krishnan, U. M. (2023). Trends in Quantification of HbA1c Using Electrochemical and Point-of-Care Analyzers. Sensors, 23(4), 1901. https://doi.org/10.3390/s23041901






