A Multi-Sensor Wearable System for the Quantitative Assessment of Parkinson’s Disease
Abstract
1. Introduction
2. System Development
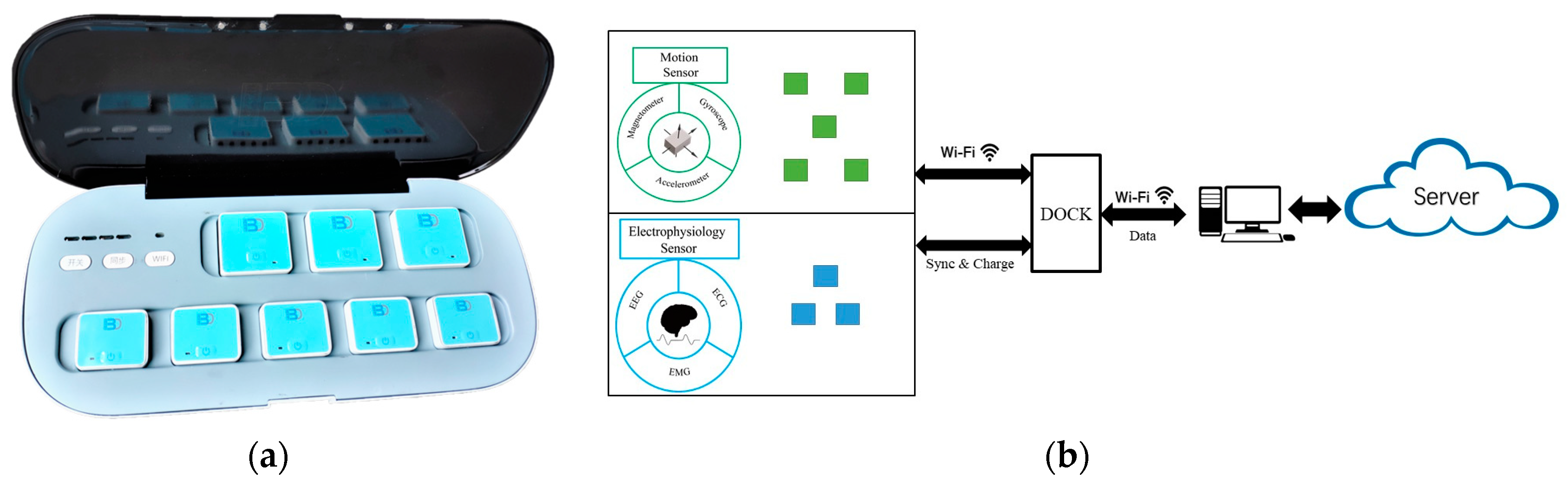
2.1. System Overview
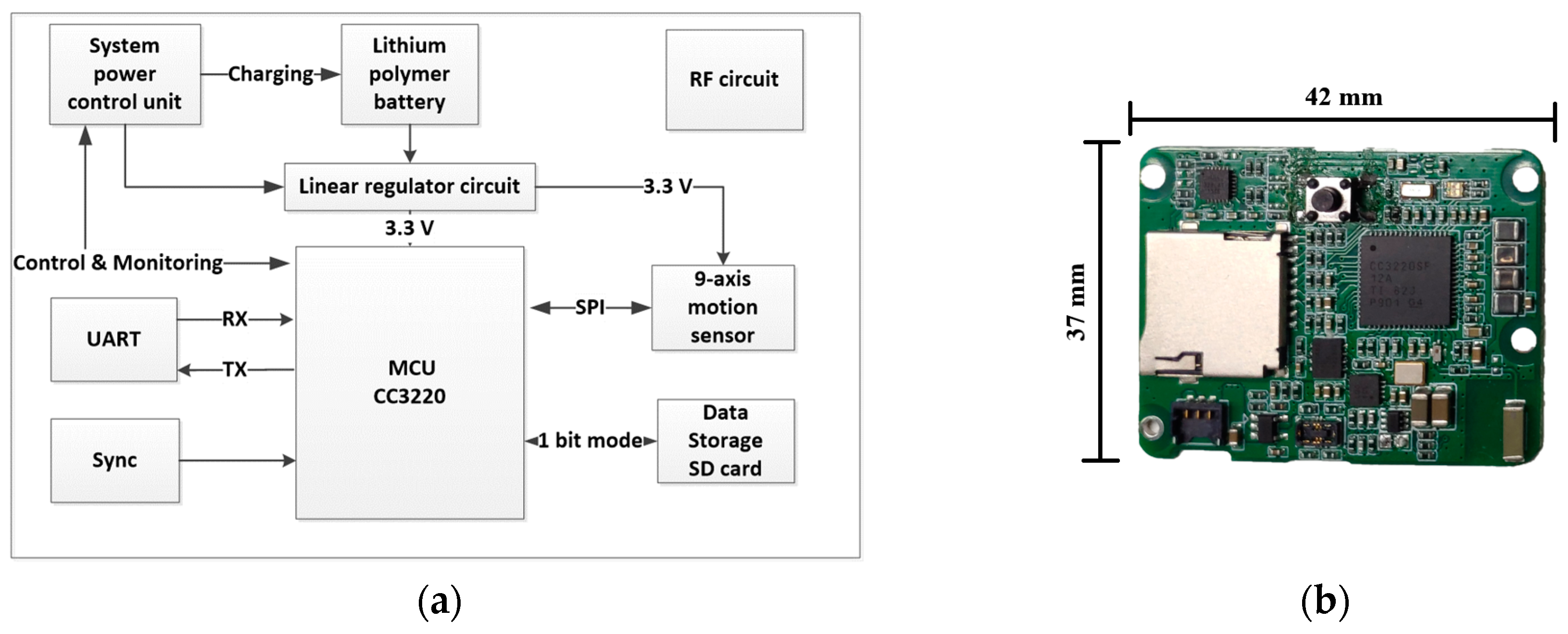
2.2. Hardware Framework
2.2.1. Motion Sensors
2.2.2. Electrophysiology Sensors
2.2.3. Docking Station
2.3. Firmware
3. Experimental Protocol
3.1. Experiment 1: Synchronous Acquisition Test
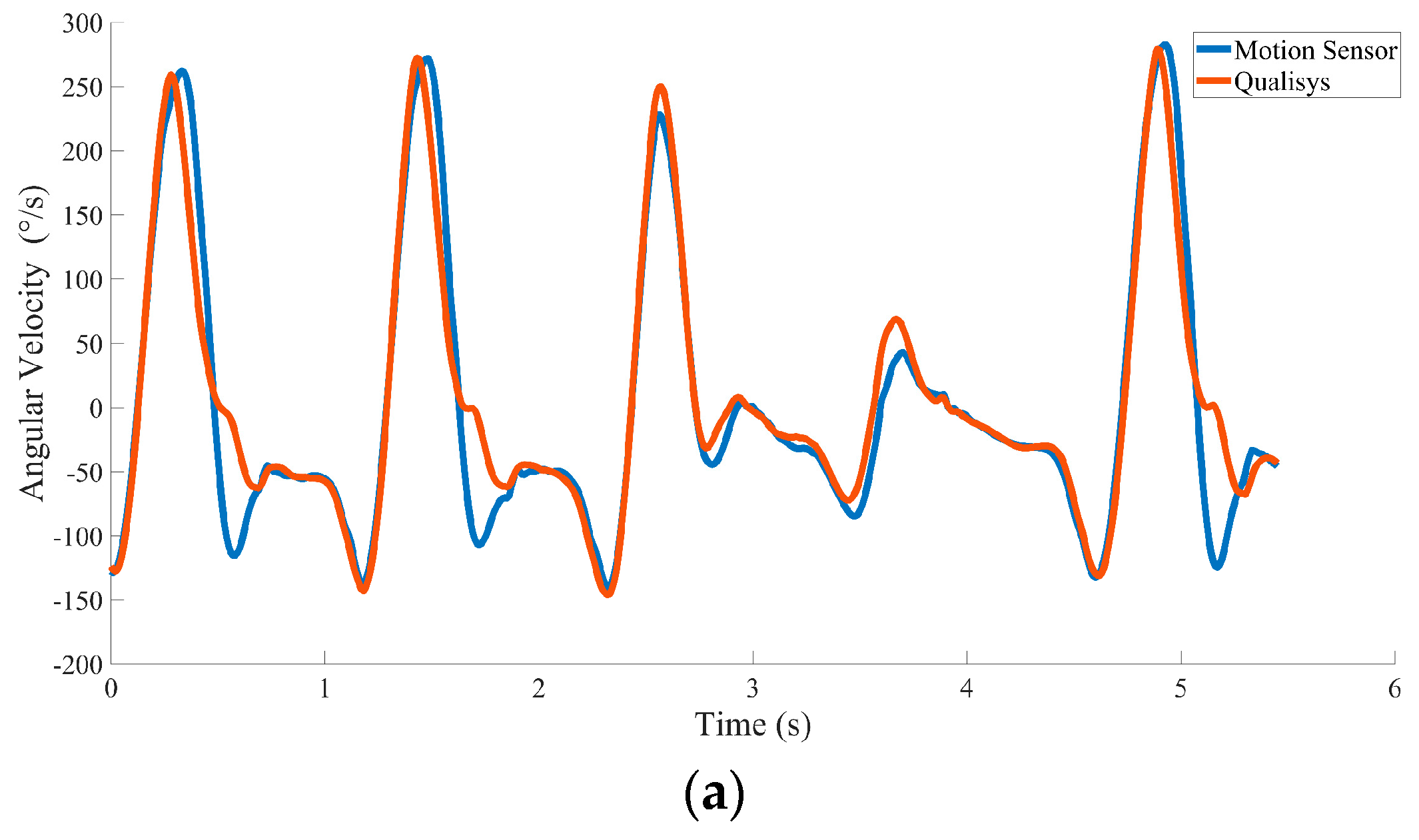
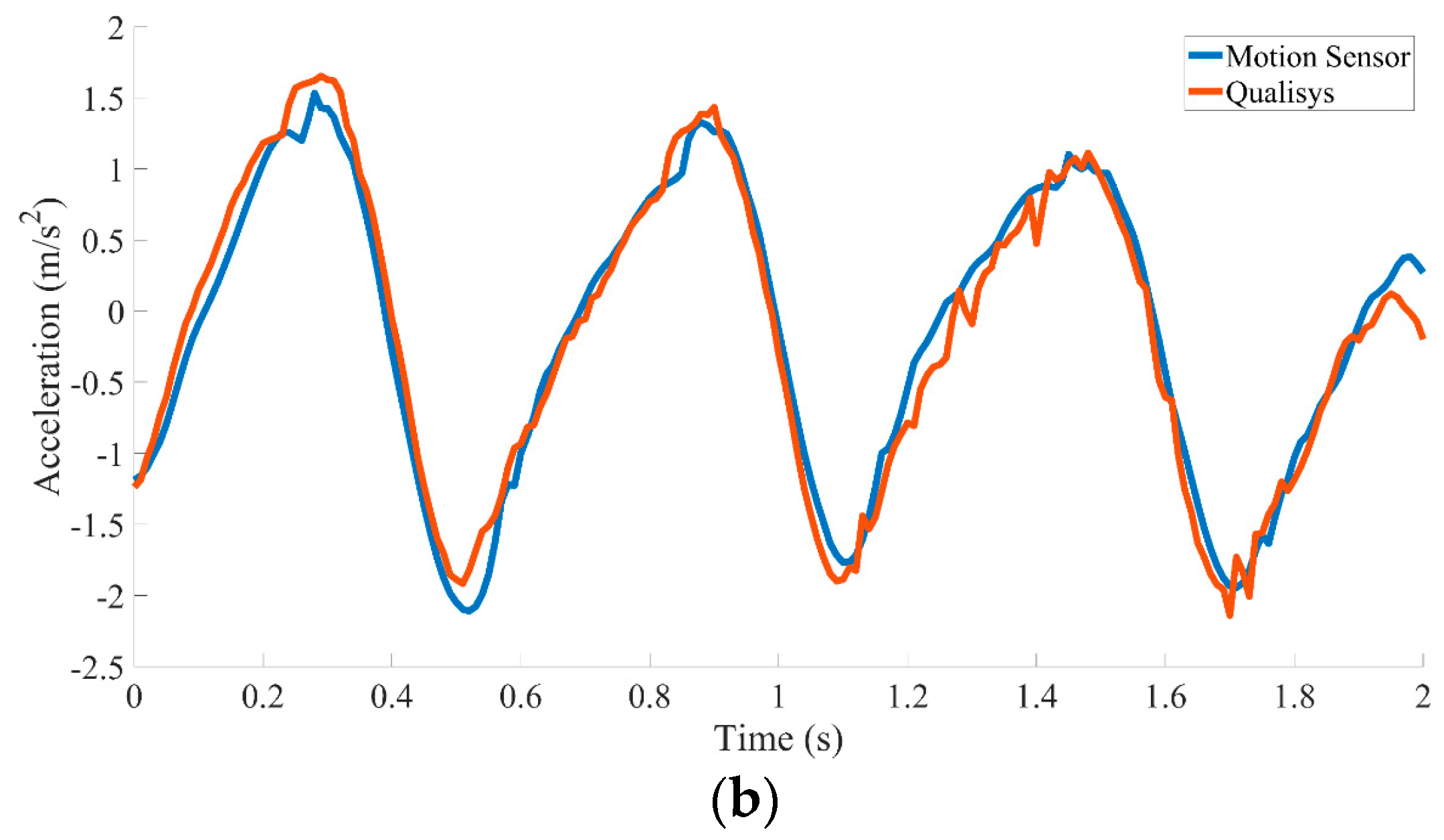
3.2. Experiment 2: Motion Sensor Validation Test
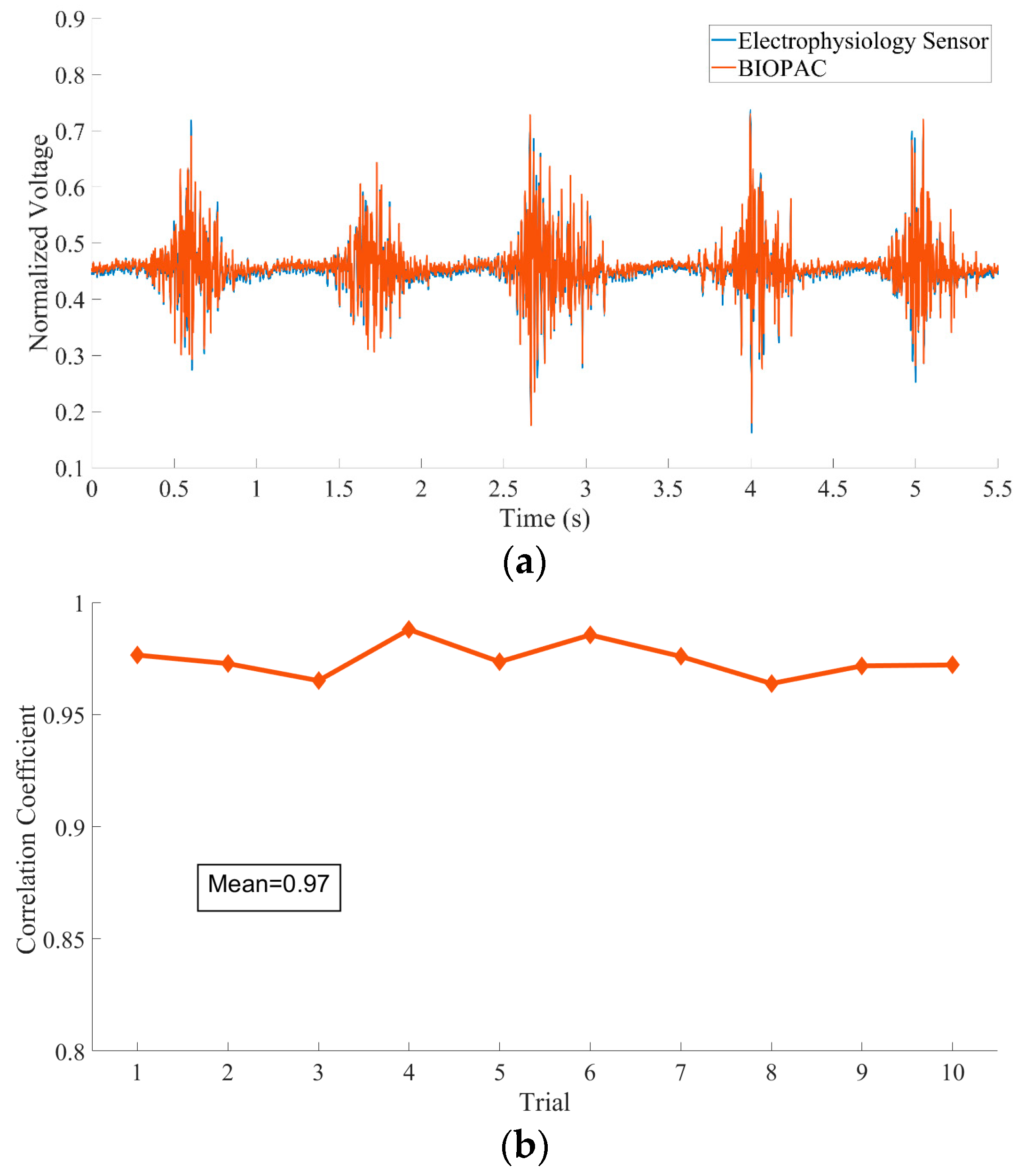
3.3. Experiment 3: Electrophysiology Sensor Validation Test
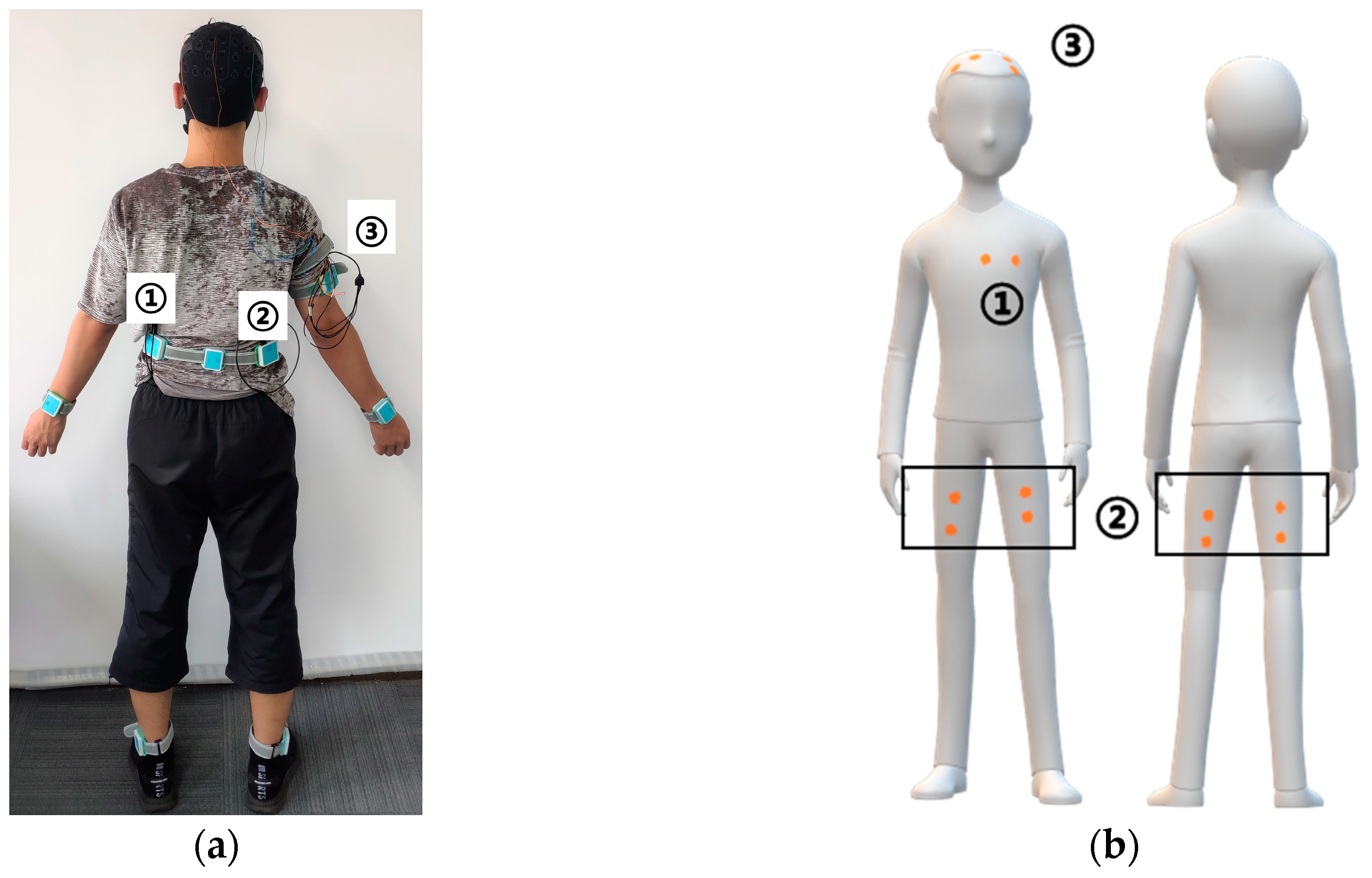
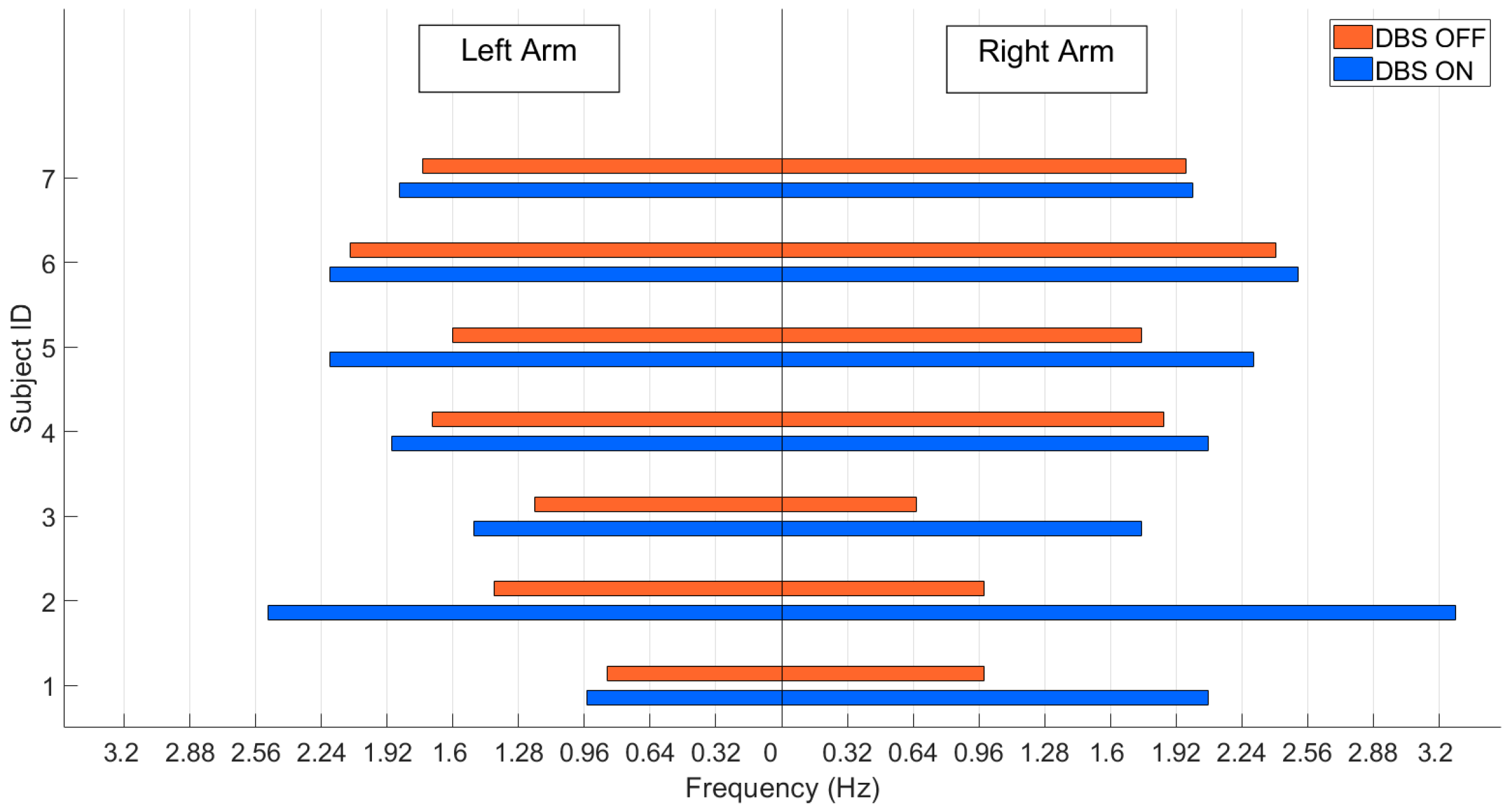
3.4. Experiment 4: Clinical Application
3.5. Data Processing
Statistical Analysis
4. Results
System Application in the Clinic
5. Discussion
Study Limitations and Future Work
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Dorsey, E.R.; Bloem, B.R. The Parkinson Pandemic—A Call to Action. JAMA Neurol. 2018, 75, 9–10. [Google Scholar] [CrossRef]
- Tysnes, O.B.; Storstein, A. Epidemiology of Parkinson’s Disease. J. Neural Transm. 2017, 124, 901–905. [Google Scholar] [CrossRef]
- Dorsey, E.R.; Glidden, A.M.; Holloway, M.R.; Birbeck, G.L.; Schwamm, L.H. Teleneurology and Mobile Technologies: The Future of Neurological Care. Nat. Rev. Neurol. 2018, 14, 285–297. [Google Scholar] [CrossRef]
- Willis, A.W.; Schootman, M.; Evanoff, B.A.; Perlmutter, J.S.; Racette, B.A. Neurologist Care in Parkinson Disease: A Utilization, Outcomes, and Survival Study. Neurology 2011, 77, 851–857. [Google Scholar] [CrossRef] [PubMed]
- Goetz, C.G.; Tilley, B.C.; Shaftman, S.R.; Stebbins, G.T.; Fahn, S.; Martinez-Martin, P.; Poewe, W.; Sampaio, C.; Stern, M.B.; Dodel, R.; et al. Movement Disorder Society-Sponsored Revision of the Unified Parkinson’s Disease Rating Scale (MDS-UPDRS): Scale Presentation and Clinimetric Testing Results. Mov. Disord. 2008, 23, 2129–2170. [Google Scholar] [CrossRef]
- Espay, A.J.; Hausdorff, J.M.; Sánchez-Ferro, Á.; Klucken, J.; Merola, A.; Bonato, P.; Paul, S.S.; Horak, F.B.; Vizcarra, J.A.; Mestre, T.A.; et al. A Roadmap for Implementation of Patient-centered Digital Outcome Measures in Parkinson’s Disease Obtained Using Mobile Health Technologies. Mov. Disord. 2019, 34, 657–663. [Google Scholar] [CrossRef]
- Channa, A.; Popescu, N.; Ciobanu, V. Wearable Solutions for Patients with Parkinson’s Disease and Neurocognitive Disorder: A Systematic Review. Sensors 2020, 20, 2713. [Google Scholar] [CrossRef] [PubMed]
- Teshuva, I.; Hillel, I.; Gazit, E.; Giladi, N.; Mirelman, A.; Hausdorff, J.M. Using Wearables to Assess Bradykinesia and Rigidity in Patients with Parkinson’s Disease: A Focused, Narrative Review of the Literature. J. Neural Transm. 2019, 126, 699–710. [Google Scholar] [CrossRef] [PubMed]
- Asakawa, T.; Sugiyama, K.; Nozaki, T.; Sameshima, T.; Kobayashi, S.; Wang, L.; Hong, Z.; Chen, S.; Li, C.; Namba, H. Can the Latest Computerized Technologies Revolutionize Conventional Assessment Tools and Therapies for a Neurological Disease? The Example of Parkinson’s Disease. Neurol. Med. Chir. 2019, 59, 69–78. [Google Scholar] [CrossRef] [PubMed]
- FitzGerald, J.J.; Lu, Z.; Jareonsettasin, P.; Antoniades, C.A. Quantifying Motor Impairment in Movement Disorders. Front. Neurosci. 2018, 12. [Google Scholar] [CrossRef]
- Kubota, K.J.; Chen, J.A.; Little, M.A. Machine Learning for Large-Scale Wearable Sensor Data in Parkinson’s Disease: Concepts, Promises, Pitfalls, and Futures. Mov. Disord. 2016, 31, 1314–1326. [Google Scholar] [CrossRef]
- Maetzler, W.; Domingos, J.; Srulijes, K.; Ferreira, J.J.; Bloem, B.R. Quantitative Wearable Sensors for Objective Assessment of Parkinson’s Disease. Mov. Disord. 2013, 28, 1628–1637. [Google Scholar] [CrossRef] [PubMed]
- Monje, M.H.G.; Foffani, G.; Obeso, J.; Sánchez-Ferro, A. New Sensor and Wearable Technologies to Aid in the Diagnosis and Treatment Monitoring of Parkinson’s Disease. Annu. Rev. Biomed. Eng. 2019, 21, 111–143. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, M.; Mitoma, H.; Yoneyama, M. Quantitative Analysis of Motor Status in Parkinson’s Disease Using Wearable Devices: From Methodological Considerations to Problems in Clinical Applications. Parkinsons. Dis. 2017, 2017. [Google Scholar] [CrossRef]
- Rovini, E.; Maremmani, C.; Cavallo, F. Automated Systems Based on Wearable Sensors for the Management of Parkinson’s Disease at Home: A Systematic Review. Telemed. e-Health 2019, 25, 167–183. [Google Scholar] [CrossRef]
- Rodríguez-Martín, D.; Pérez-López, C.; Samà, A.; Català, A.; Arostegui, J.M.M.; Cabestany, J.; Mestre, B.; Alcaine, S.; Prats, A.; De La Cruz Crespo, M.; et al. A Waist-Worn Inertial Measurement Unit for Long-Term Monitoring of Parkinson’s Disease Patients. Sensors 2017, 17, 827. [Google Scholar] [CrossRef]
- Rodríguez-Martín, D.; Pérez-López, C.; Samà, A.; Cabestany, J.; Català, A. A Wearable Inertial Measurement Unit for Long-Term Monitoring in the Dependency Care Area. Sensors 2013, 13, 14079–14104. [Google Scholar] [CrossRef]
- Pasluosta, C.F.; Gassner, H.; Winkler, J.; Klucken, J.; Eskofier, B.M. An Emerging Era in the Management of Parkinson’s Disease: Wearable Technologies and the Internet of Things. IEEE J. Biomed. Heal. Inform. 2015, 19, 1873–1881. [Google Scholar] [CrossRef]
- Hasan, H.; Athauda, D.S.; Foltynie, T.; Noyce, A.J. Technologies Assessing Limb Bradykinesia in Parkinson’s Disease. J. Parkinsons. Dis. 2017, 7, 65–77. [Google Scholar] [CrossRef]
- Sano, Y.; Kandori, A.; Shima, K.; Tamura, Y.; Takagi, H.; Tsuji, T.; Noda, M.; Higashikawa, F.; Yokoe, M.; Sakoda, S. Reliability of Finger Tapping Test Used in Diagnosis of Movement Disorders. In Proceedings of the 2011 5th International Conference on Bioinformatics and Biomedical Engineering, Wuhan, China, 10–12 May 2011; pp. 1–4. [Google Scholar] [CrossRef]
- Antos, S.A.; Albert, M.V.; Kording, K.P. Hand, Belt, Pocket or Bag: Practical Activity Tracking with Mobile Phones. J. Neurosci. Methods 2014, 231, 22–30. [Google Scholar] [CrossRef]
- Patel, S.; Lorincz, K.; Hughes, R.; Huggins, N.; Growdon, J.; Standaert, D.; Akay, M.; Dy, J.; Welsh, M.; Bonato, P. Monitoring Motor Fluctuations in Patients with Parkinson’s Disease Using Wearable Sensors. In IEEE Transactions on Information Technology in Biomedicine; IEEE: New York, NY, USA, 2009; Volume 13, pp. 864–873. [Google Scholar] [CrossRef]
- Maetzler, W.; Klucken, J.; Horne, M. A Clinical View on the Development of Technology-Based Tools in Managing Parkinson’s Disease. Mov. Disord. 2016, 31, 1263–1271. [Google Scholar] [CrossRef] [PubMed]
- Caldas, R.; Mundt, M.; Potthast, W.; Buarque de Lima Neto, F.; Markert, B. A Systematic Review of Gait Analysis Methods Based on Inertial Sensors and Adaptive Algorithms. Gait Posture 2017, 57, 204–210. [Google Scholar] [CrossRef]
- Wang, J.; Gong, D.; Luo, H.; Zhang, W.; Zhang, L.; Zhang, H.; Zhou, J.; Wang, S. Measurement of Step Angle for Quantifying the Gait Impairment of Parkinson’s Disease by Wearable Sensors: Controlled Study. JMIR mHealth uHealth 2020, 8, e16650. [Google Scholar] [CrossRef] [PubMed]
- Spasojević, S.; Ilić, T.V.; Stojković, I.; Potkonjak, V.; Rodić, A.; Santos-Victor, J. Quantitative Assessment of the Arm/Hand Movements in Parkinson’s Disease Using a Wireless Armband Device. Front. Neurol. 2017, 8, 388. [Google Scholar] [CrossRef] [PubMed]
- Pahwa, R.; Isaacson, S.H.; Torres-Russotto, D.; Nahab, F.B.; Lynch, P.M.; Kotschet, K.E. Role of the Personal KinetiGraph in the Routine Clinical Assessment of Parkinson’s Disease: Recommendations from an Expert Panel. Expert Rev. Neurother. 2018, 18, 669–680. [Google Scholar] [CrossRef]
- Cancela, J.; Pastorino, M.; Arredondo, M.T.; Nikita, K.S.; Villagra, F.; Pastor, M.A. Feasibility Study of a Wearable System Based on a Wireless Body Area Network for Gait Assessment in Parkinson’s Disease Patients. Sensors 2014, 14, 4618–4633. [Google Scholar] [CrossRef]
- Mariani, B.; Jiménez, M.C.; Vingerhoets, F.J.G.; Aminian, K. On-Shoe Wearable Sensors for Gait and Turning Assessment of Patients with Parkinson’s Disease. In IEEE Transactions on Biomedical Engineering; IEEE: New York, NY, USA, 2013; Volume 60, pp. 155–158. [Google Scholar] [CrossRef]
- De Venuto, D.; Annese, V.F.; Mezzina, G.; Defazio, G. FPGA-Based Embedded Cyber-Physical Platform to Assess Gait and Postural Stability in Parkinson’s Disease. In IEEE Transactions on Components, Packaging and Manufacturing Technology; IEEE: New York, NY, USA, 2018; Volume 8, pp. 1167–1179. [Google Scholar] [CrossRef]
- Sepehri, B.; Esteki, A.; Shahidi, G.A.; Moinodin, M. Analysis of Quantified Indices of EMG for Evaluation of Parkinson’s Disease. In 13th International Conference on Biomedical Engineering. IFMBE Proceedings; Springer: Berlin/Heidelberg, Germany, 2009; Volume 23, pp. 765–768. [Google Scholar] [CrossRef]
- Levin, J.; Krafzcyk, S.; Valkovič, P.; Eggert, T.; Claassen, J.; Bötzel, K. Objective Measurement of Muscle Rigidity in Parkinsonian Patients Treated with Subthalamic Stimulation. Mov. Disord. 2009, 24, 57–63. [Google Scholar] [CrossRef]
- Lukhanina, E.P.; Kapoustina, M.T.; Karaban, I.N. A Quantitative Surface Electromyogram Analysis for Diagnosis and Therapy Control in Parkinson’s Disease. Park. Relat. Disord. 2000, 6, 77–86. [Google Scholar] [CrossRef]
- Breit, S.; Spieker, S.; Schulz, J.B.; Gasser, T. Long-Term EMG Recordings Differentiate between Parkinsonian and Essential Tremor. J. Neurol. 2008, 255, 103–111. [Google Scholar] [CrossRef]
- Arnao, V.; Cinturino, A.; Mastrilli, S.; Buttà, C.; Maida, C.; Tuttolomondo, A.; Aridon, P.; Amelio, M.D. Impaired Circadian Heart Rate Variability in Parkinson’s Disease: A Time-Domain Analysis in Ambulatory Setting. BMC Neurol. 2020, 20, 152. [Google Scholar]
- Grimaldi, G.; Lammertse, P.; Van Den Braber, N.; Meuleman, J.; Manto, M. Effects of Inertia and Wrist Oscillations on Contralateral Neurological Postural Tremor Using the Wristalyzer, a New Myohaptic Device. In IEEE Transactions on Biomedical Circuits and Systems; IEEE: New York, NY, USA, 2008; Volume 2, pp. 269–279. [Google Scholar] [CrossRef]
- Wright, D.; Nakamura, K.; Maeda, T.; Kutsuzawa, K.; Miyawaki, K.; Nagata, K. Research and Development of a Portable Device to Quantify Muscle Tone in Patients with Parkinsons Disease. In Proceedings of the 2008 30th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Vancouver, BC, Canada, 20–25 August 2008; pp. 2825–2827. [Google Scholar] [CrossRef]
- Espay, A.J.; Bonato, P.; Nahab, F.B.; Maetzler, W.; Dean, J.M.; Klucken, J.; Eskofier, B.M.; Merola, A.; Horak, F.; Lang, A.E.; et al. Technology in Parkinson’s Disease: Challenges and Opportunities. Mov. Disord. 2016, 31, 1272–1282. [Google Scholar] [CrossRef] [PubMed]
- Dean, C.M.; Richards, C.L.; Malouin, F. Walking Speed over 10 Metres Overestimates Locomotor Capacity after Stroke. Clin. Rehabil. 2001, 15, 415–421. [Google Scholar] [CrossRef]
- Garza-Rodríguez, A.; Sánchez-Fernández, L.P.; Sánchez-Pérez, L.A.; Ornelas-Vences, C.; Ehrenberg-Inzunza, M. Pronation and Supination Analysis Based on Biomechanical Signals from Parkinson’s Disease Patients. Artif. Intell. Med. 2018, 84, 7–22. [Google Scholar] [CrossRef] [PubMed]
- Esser, P.; Dawes, H.; Collett, J.; Feltham, M.G.; Howells, K. Validity and Inter-Rater Reliability of Inertial Gait Measurements in Parkinson’s Disease: A Pilot Study. J. Neurosci. Methods 2012, 205, 177–181. [Google Scholar] [CrossRef] [PubMed]
- Bai, Q.; Shen, T.; Xu, B.; Yu, Q.; Zhang, H.; Mao, C.; Liu, C.; Wang, S. Quantification of the Motor Symptoms of Parkinson’s Disease. In Proceedings of the 2017 8th International IEEE/EMBS Conference on Neural Engineering (NER), Shanghai, China, 25–28 May 2017; pp. 82–85. [Google Scholar] [CrossRef]
- Santanna, A.; Salarian, A.; Wickstrom, N. A New Measure of Movement Symmetry in Early Parkinsons Disease Patients Using Symbolic Processing of Inertial Sensor Data. In IEEE Transactions on Biomedical Engineering; IEEE: New York, NY, USA, 2011; Volume 58, pp. 2127–2135. [Google Scholar] [CrossRef]
- Endo, T.; Okuno, R.; Yokoe, M.; Akazawa, K.; Sakoda, S. A Novel Method for Systematic Analysis of Rigidity in Parkinson’s Disease. Mov. Disord. 2009, 24, 2218–2224. [Google Scholar] [CrossRef] [PubMed]





| Quantity | 1 | 2 | 3 | 4 | 5 |
|---|---|---|---|---|---|
| Acceleration | 0.98 ** | 0.96 ** | 0.96 ** | 0.96 ** | 0.95 ** |
| Angular Velocity | 0.96 ** | 0.94 ** | 0.93 ** | 0.95 ** | 0.95 ** |
| Quantity | 1 | 2 | 3 | 4 | 5 | SD |
|---|---|---|---|---|---|---|
| Acceleration | 0.1579 | 0.1603 | 0.2402 | 0.2926 | 0.2736 | 0.0630 |
| Angular Velocity | 18.07 | 25.02 | 27.74 | 22.87 | 19.72 | 3.9092 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, H.; Li, C.; Liu, W.; Wang, J.; Zhou, J.; Wang, S. A Multi-Sensor Wearable System for the Quantitative Assessment of Parkinson’s Disease. Sensors 2020, 20, 6146. https://doi.org/10.3390/s20216146
Zhang H, Li C, Liu W, Wang J, Zhou J, Wang S. A Multi-Sensor Wearable System for the Quantitative Assessment of Parkinson’s Disease. Sensors. 2020; 20(21):6146. https://doi.org/10.3390/s20216146
Chicago/Turabian StyleZhang, Han, Chuantao Li, Wei Liu, Jingying Wang, Junhong Zhou, and Shouyan Wang. 2020. "A Multi-Sensor Wearable System for the Quantitative Assessment of Parkinson’s Disease" Sensors 20, no. 21: 6146. https://doi.org/10.3390/s20216146
APA StyleZhang, H., Li, C., Liu, W., Wang, J., Zhou, J., & Wang, S. (2020). A Multi-Sensor Wearable System for the Quantitative Assessment of Parkinson’s Disease. Sensors, 20(21), 6146. https://doi.org/10.3390/s20216146





