A Method to Determine Human Skin Heat Capacity Using a Non-Invasive Calorimetric Sensor
Abstract
1. Introduction
2. Materials and Methods
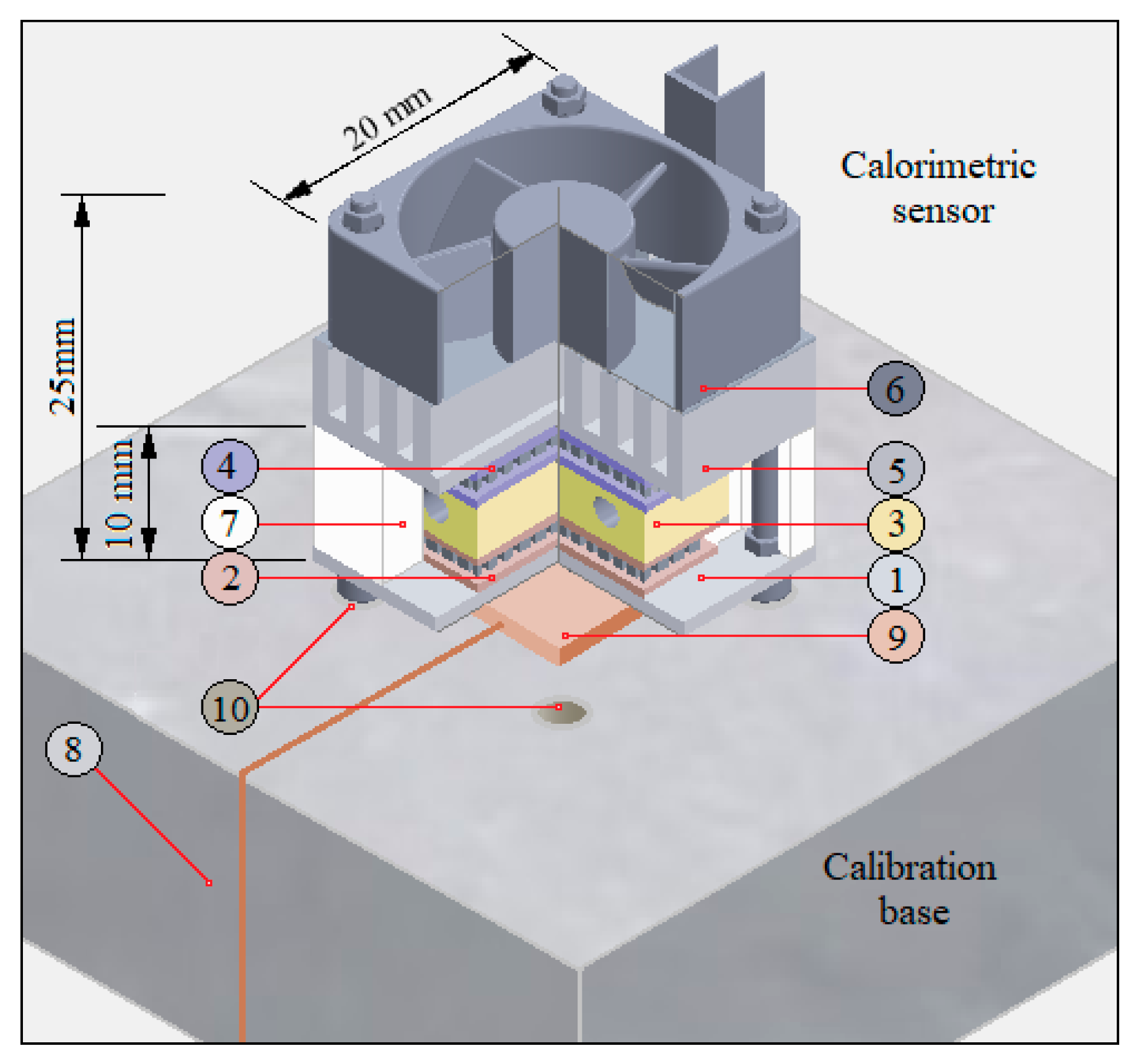
2.1. The Calorimetric Sensor
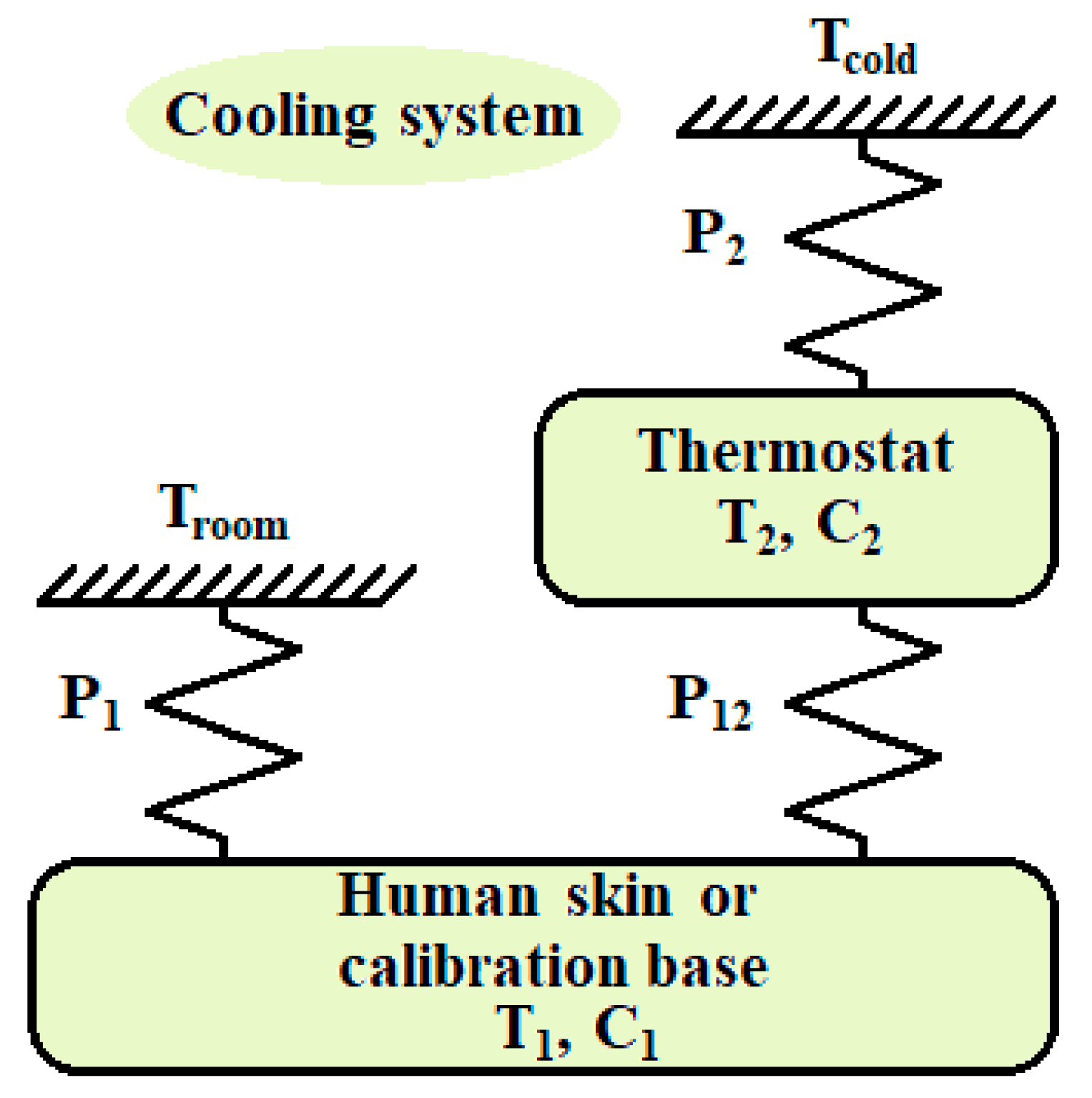
2.2. Calorimetric Model
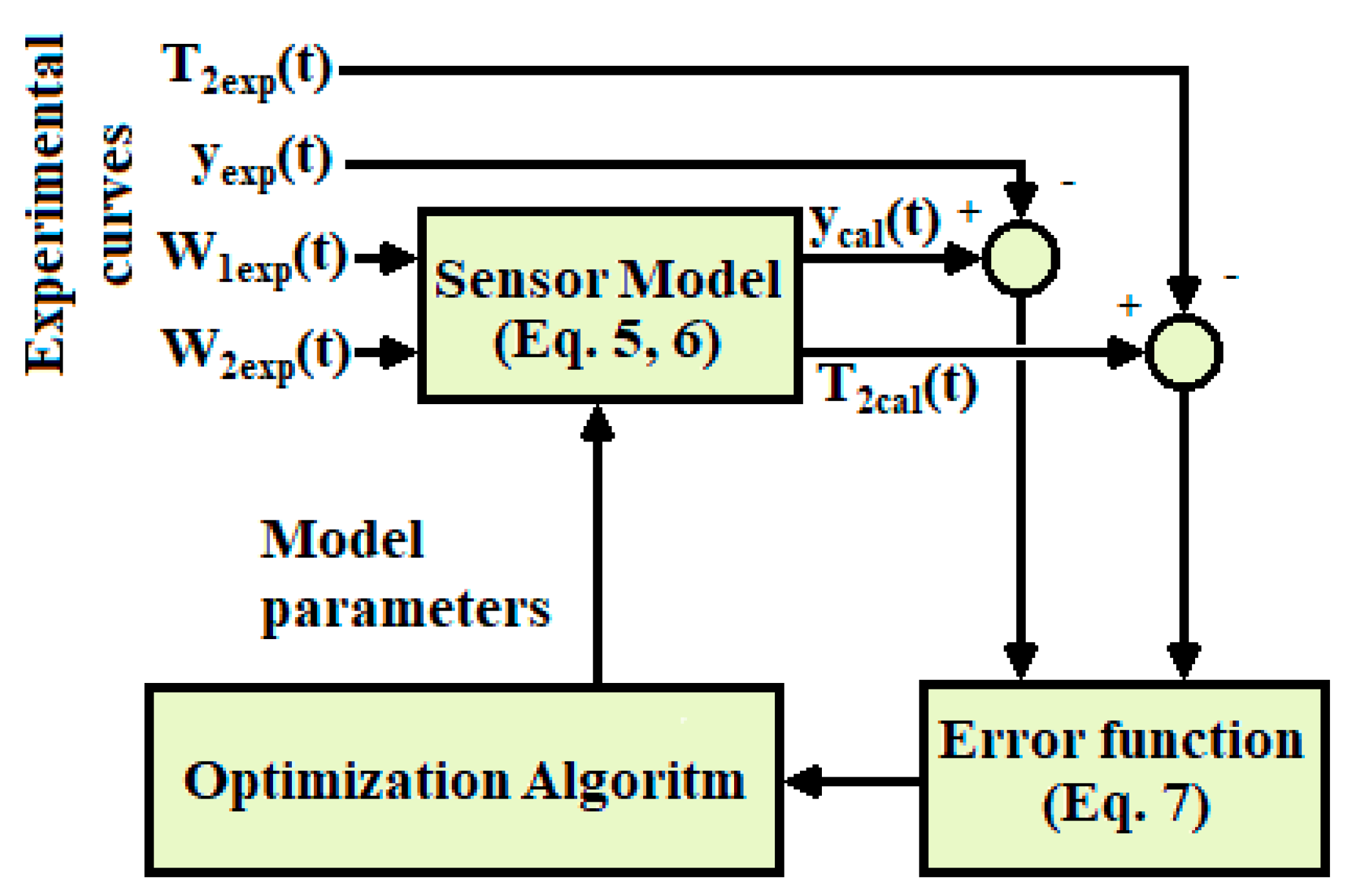
2.3. Identification of the Model
2.4. Simulation
2.4.1. Variation of the FT of the Model Depending on the Heat Capacity
2.4.2. Simulations in the Calibration Base and in the Human Body
- (1)
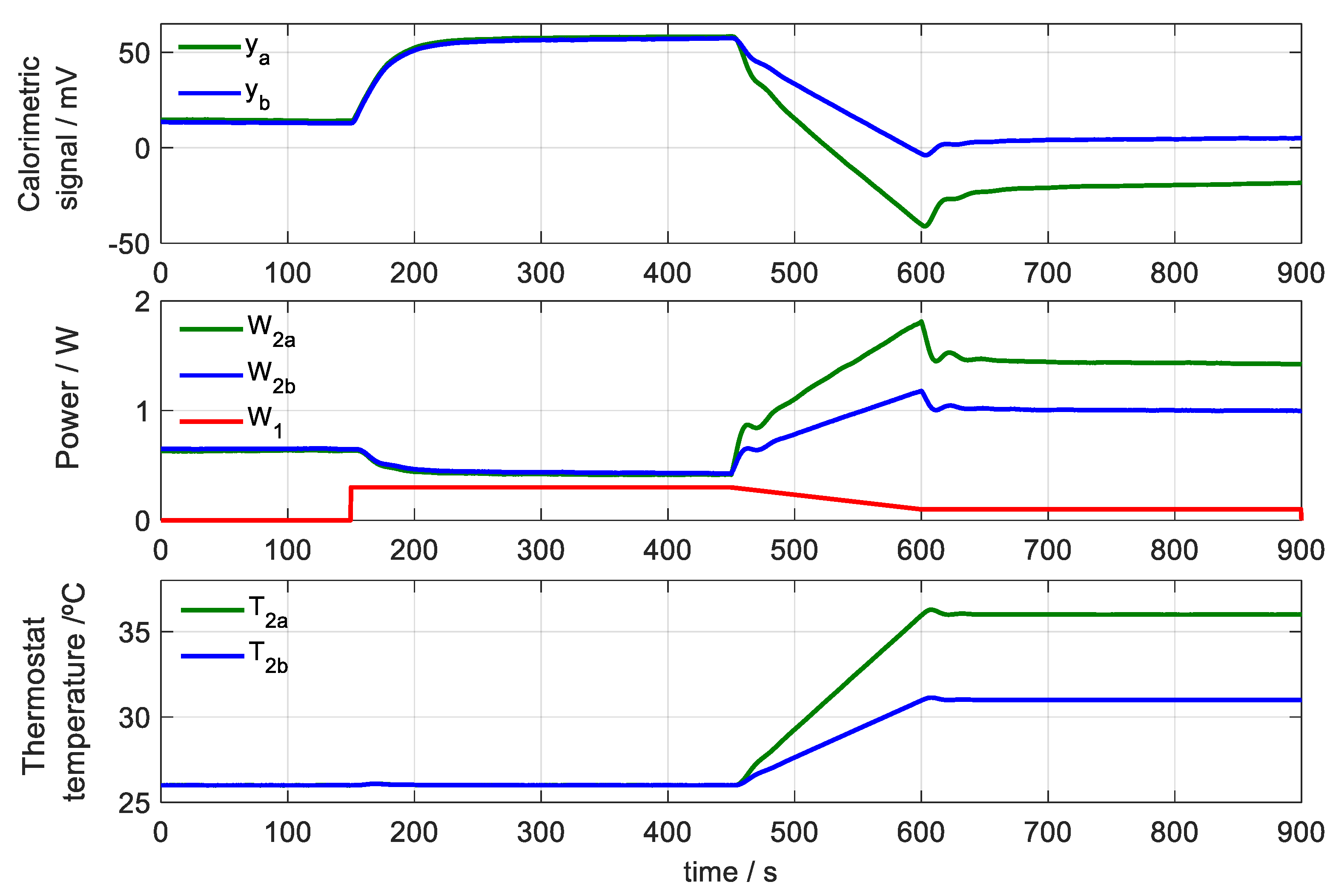
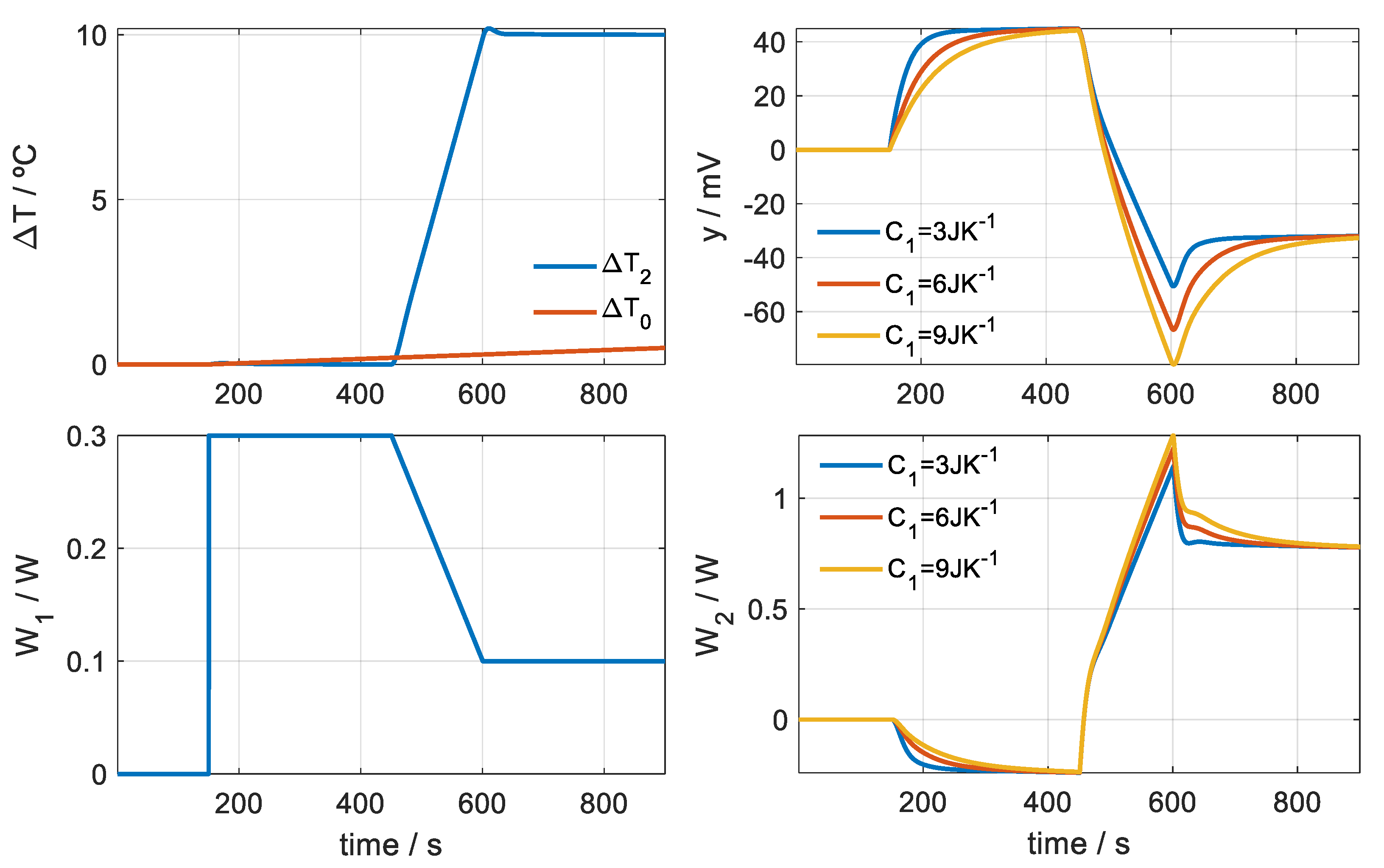
- There is an instantaneous contact between the sensor surface and the skin surface that are at different temperatures. This produces a peak in the calorimetric signal, caused by an instantaneous power that is transmitted from the highest temperature surface to the lowest temperature. This instantaneous power that is transmitted from the skin to the sensor is represented with an exponential function of the formwhere A0 is the power transmitted in steady state and A1 is the amplitude of the decreasing exponential due to instantaneous contact between the sensor surfaces and the skin. In the simulated case represented in Figure 8, we assume a power of A0 = 0.3 W for the initial temperature of the thermostat and a power of A0 = 0.1 W for the final temperature. We assume an amplitude of A1 = 2 W and a time constant of τ1 = 9 s.
- (2)
- The temperature surrounding the sensor has changed and is not the same temperature surrounding the sensor when it is in the base. In general, the temperature in the neighbourhood of the skin is higher. This temperature difference is represented by ΔT0 and responds to the expression given by (Equation (4)). In the simulated case A = 2.5 K, B = 1 K and a time constant of 9 s are considered.
- (3)
- The skin has a heat capacity typical of the area where it is being measured and therefore the transient response will depend on that heat capacity. Figure 8 shows these differences in the calorimetric signal. Three heat capacities for the skin have been used in the simulation: 3, 6 and 9 JK−1.
2.5. Method for Determining Heat Flux and Heat Capacity
- (1)
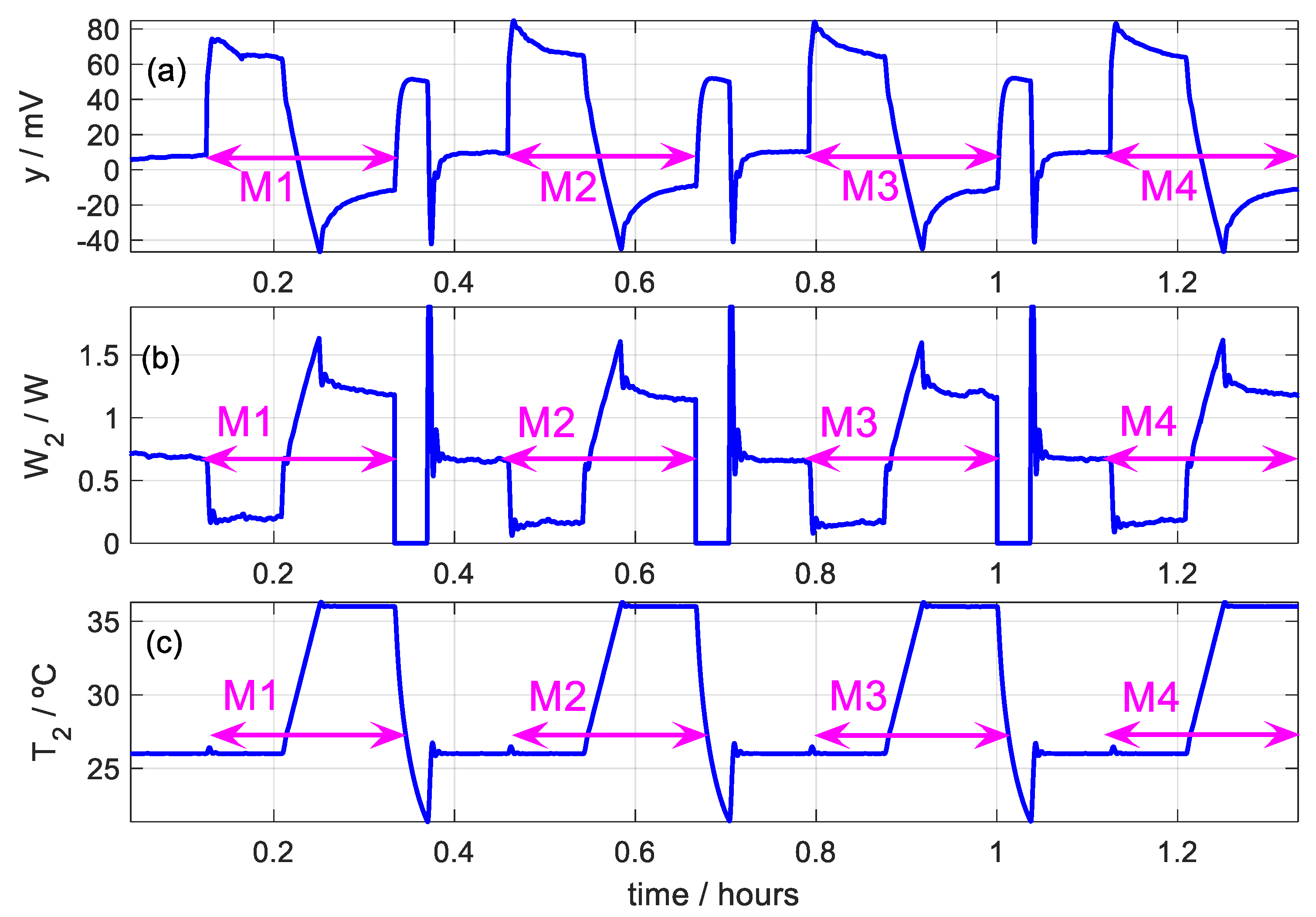
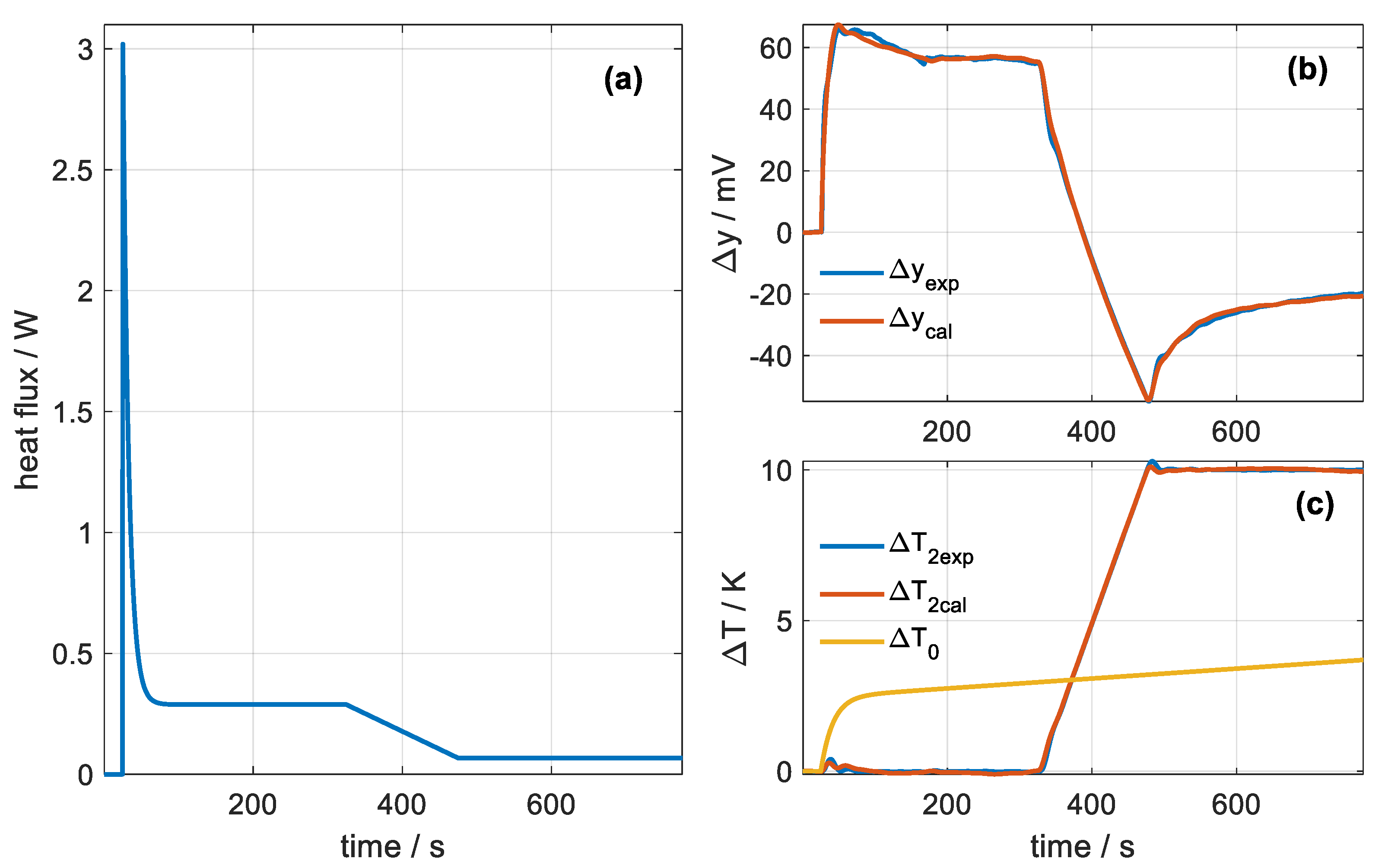
- When the temperature of the thermostat is constant (T2initial) and the sensor is applied to the skin, the heat flow W1 that passes through the sensor obeys (Equation (9)). Contrastingly, when there is a linear variation in the temperature of the thermostat (from T2initial to T2end), we assume that the power W1 decreases linearly to a final value, which remains constant while the temperature of the thermostat remains constant at its final value (T2end). Thus, the heat flux can be described with (Equation (10)):In this equation, t1 is the instant in which the sensor is applied to the skin, t2 is the instant in which the linear increase in the temperature of the thermostat begins, t3 is the instant in which the aforementioned linear variation ends and starts to keep the temperature constant, and tend is the final instant of the measurement.
- (2)
- The difference in ambient temperature ΔT0 obeys (Equation (4)).
- (3)
- The relationships between all the system variables obey the equations of the model (Equation (5)). The model parameters have been determined in the calibration (Table 1) except for the value of C1 which depends on the place of measurement.
3. Results
3.1. Measurements in the Junior Subject
3.2. Measurements in Senior Subject
3.3. Discussion
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Brooks, A.G.; Withers, R.T.; Gore, C.J.; Vogler, A.J.; Plummer, J.; Cormack, J. Measurement and prediction of METs during household activities in 35- to 45-year-old females. Eur. J. Appl. Physiol. 2004, 91, 638–648. [Google Scholar] [CrossRef] [PubMed]
- Taylor, N.A.S.; Tipton, M.J.; Kenny, G.P. Considerations for the measurement of core, skin and mean body temperatures. J. Therm. Biol. 2014, 46, 72–101. [Google Scholar] [CrossRef]
- Wiegand, N.; Naumov, I.; Nőt, L.G.; Vámhidy, L.; Lőrinczy, D. Differential scanning calorimetric examination of pathologic scar tissues of human skin. J. Therm. Anal. Calorim. 2013, 111, 1897–1902. [Google Scholar] [CrossRef]
- Mehdi, M.; Fekecs, T.; Zapf, I.; Fekecs, T.; Lőrinczy, D. Differential scanning calorimetry (DSC) analysis of human plasma in different psoriasis stages. J. Therm. Anal. Calorim. 2013, 111, 1801–1804. [Google Scholar] [CrossRef]
- Deng, Z.-S.; Liu, J. Blood perfusion-based model for characterizing the temperature fluctuation in living tissues. Physica A 2001, 300, 521–530. [Google Scholar] [CrossRef]
- Hassanpour, S.; Saboonchi, A. Modeling of heat transfer in a vascular tissue-like medium during an interstitial hyperthermia process. J. Therm. Biol. 2016, 62, 150–158. [Google Scholar] [CrossRef]
- Agrawal, M.; Pardasani, K.R. Finite element model to study temperature distribution in skin and deep tissues of human limbs. J. Therm. Biol. 2016, 62, 98–105. [Google Scholar] [CrossRef]
- Lee, E.K.; Kim, M.K.; Lee, C.H. Skin-Mountable Biosensors and Therapeutics: A Review. Annu. Rev. Biomed. Eng. 2019, 21, 299–323. [Google Scholar] [CrossRef]
- Liu, Y.; Wang, H.; Zhao, W.; Zhang, M.; Qin, H.; Xie, Y. Flexible, Stretchable Sensors for Wearable Health Monitoring: Sensing Mechanisms, Materials, Fabrication Strategies and Features. Sensors 2018, 18, 645. [Google Scholar] [CrossRef]
- Okabe, T.; Fujimura, T.; Okajima, J.; Aiba, S.; Maruyama, S. Non-invasive measurement of effective thermal conductivity of human skin with a guard-heated thermistor probe. Int. J. Heat Mass Tran. 2018, 126, 625–635. [Google Scholar] [CrossRef]
- Gunga, H.-C.; Werner, A.; Stahn, A.; Steinach, M.; Schlabs, T.; Koralewski, E.; Kunz, D.; Belavy, D.L.; Felsenberg, D.; Sattler, F.; et al. The Double Sensor—A non-invasive device to continuously monitor core temperature in humans on earth and in space. Respir. Physiol. Neurobiol. 2009, 169, S63–S68. [Google Scholar] [CrossRef] [PubMed]
- Mazgaoker, S.; Ketko, I.; Yanovich, R.; Heled, Y.; Epstein, Y. Measuring core body temperature with a non-invasive sensor. J. Therm. Biol. 2017, 66, 17–20. [Google Scholar] [CrossRef] [PubMed]
- Marchiori, B.; Regal, S.; Arango, Y.; Delattre, R.; Blayac, S.; Ramuz, M. PVDF-TrFE-Based Stretchable Contact and Non-Contact Temperature Sensor for E-Skin Application. Sensors 2020, 20, 623. [Google Scholar] [CrossRef] [PubMed]
- Gao, L.; Zhang, Y.; Malyarchuk, V.; Jia, L.; Jang, K.-I.; Webb, R.C.; Fu, H.; Shi, Y.; Zhou, G.; Shi, L.; et al. Epidermal photonic devices for quantitative imaging of temperature and thermal transport characteristics of the skin. Nat. Commun. 2014, 5, 4938. [Google Scholar] [CrossRef] [PubMed]
- Webb, R.C.; Pielak, R.M.; Bastien, P.; Ayers, J.; Niittynen, J.; Kurniawan, J.; Manco, M.; Lin, A.; Cho, N.H.; Malyrchuk, V.; et al. Thermal transport characteristics of human skin measured in vivo using ultrathin conformal arrays of thermal sensors and actuators. PLoS ONE 2015, 10, e0118131. [Google Scholar] [CrossRef]
- Tian, L.; Li, Y.; Webb, R.C.; Krishnan, S.; Bian, Z.; Song, J.; Ning, X.; Crawford, K.; Kurniawan, J.; Bonifas, A.; et al. Flexible and stretchable 3ω sensors for thermal characterization of human skin. Adv. Funct. Mater. 2017, 27, 1701282. [Google Scholar] [CrossRef]
- Jesús, C.; Socorro, F.; Rodríguez de Rivera, M. Development of a calorimetric sensor for medical application. Part III. Operating methods and applications. J. Therm. Anal. Calorim. 2013, 113, 1009–1013. [Google Scholar] [CrossRef]
- Jesús, C.; Socorro, F.; Rodríguez de Rivera, H.J.; Rodriguez de Rivera, M. Development of a calorimetric sensor for medical application. Part IV. Deconvolution of the calorimetric signal. J. Therm. Anal. Calorim. 2014, 116, 151–155. [Google Scholar] [CrossRef]
- Socorro, F.; Rodríguez de Rivera, P.J.; Rodríguez de Rivera, M. Calorimetric minisensor for the localized measurement of surface heat dissipated from the human body. Sensors 2016, 16, 1864. [Google Scholar] [CrossRef]
- Socorro, F.; Rodríguez de Rivera, P.J.; Rodríguez de Rivera, M.; Rodríguez de Rivera, M. Mathematical model for localised and surface heat flux of the human body obtained from measurements performed with a calorimetry minisensor. Sensors 2017, 17, 2749. [Google Scholar] [CrossRef]
- Rodríguez de Rivera, P.J.; Rodríguez de Rivera, M.; Socorro, F.; Rodríguez de Rivera, M. Method for transient heat flux determination in human body surface using a direct calorimetry sensor. Measurement 2019, 39, 1–9. [Google Scholar] [CrossRef]
- Rodríguez de Rivera, P.J.; Rodríguez de Rivera, M.; Socorro, F.; Rodríguez de Rivera, M. Measurement of human body surface heat flux using a calorimetric sensor. J. Therm. Biol. 2019, 81, 178–184. [Google Scholar] [CrossRef]
- Rodríguez de Rivera, M.; Socorro, F. Baseline changes in an isothermal titration microcalorimeter. J. Therm. Anal. Calorim. 2005, 80, 769–773. [Google Scholar] [CrossRef]
- Lahiri, B.B.; Bagavathiaappan, S.; Jayakumar, T.; Philip, J. Medical applications of infrared thermography: A review. Infrared Phys. Technol. 2012, 55, 221–235. [Google Scholar] [CrossRef] [PubMed]
- Godoy, S.E.; Hayat, M.M.; Ramirez, D.A.; Myers, S.A.; Padilla, R.S.; Krishna, S. Detection theory for accurate and non-invasive skin cancer diagnosis using dynamic thermal imaging. Biomed. Opt. Express. 2017, 8, 2301–2323. [Google Scholar] [CrossRef] [PubMed]
- Haidar, S.G.; Charity, R.M.; Bassi, R.S.; Nicolai, P.; Singh, B.K. Knee skin temperature following uncomplicated total knee replacement. Knee 2006, 13, 422–426. [Google Scholar] [CrossRef] [PubMed]
- Rajapakse, C.; Grennan, D.M.; Jones, C.; Wilkinson, L.; Jayson, M. Thermography in the assessment of peripheral joint inflammation—A re-evaluation. Rheumatol. Rehabil. 1981, 20, 81–87. [Google Scholar] [CrossRef]
- Rokita, E.; Rok, T.; Taton, G. Application of thermography for the assessment of allergen-induced skin reactions. Med. Phys. 2011, 38, 765–772. [Google Scholar] [CrossRef]
- Vecchio, P.C.; Adebajo, A.O.; Chard, M.D.; Thomas, P.P.; Hazleman, B.L. Thermography of frozen sholder and rotator cuff tendinitis. Clin. Rheumatol. 1992, 11, 382–384. [Google Scholar] [CrossRef]
- Rodríguez de Rivera, M.; Socorro, F.; Dubes, J.P.; Tachoire, H.; Torra, V. Microcalorimetrie: Identification et déconvolotion automatique à l’aide de modéles physiques. Thermochim. Acta 1989, 150, 11–25. [Google Scholar] [CrossRef]
- Socorro, F.; Rodríguez de Rivera, M.; Jesús, C. A thermal model of a flow calorimeter. J. Therm. Anal. Calorim. 2001, 64, 357–366. [Google Scholar] [CrossRef]
- Auguet, C.; Lerchner, J.; Marinelli, P.; Martorell, F.; Rodríguez de Rivera, M.; Torra, V.; Wolf, G. Identification of micro-scale calorimetric devices IV. Descriptive models in 3-D. J. Therm. Anal. Calorim. 2003, 71, 951–966. [Google Scholar] [CrossRef]
- Lagarias, J.C.; Reeds, J.A.; Wright, M.H.; Wright, P.E. Convergence Properties of the Nelder-Mead Simplex Method in Low Dimensions. SIAM J. Opt. 1998, 9, 112–147. [Google Scholar] [CrossRef]
- Nelder, J.A.; Mead, C. A simplex method for function minimization. Comput. J. 1965, 7, 308–313. [Google Scholar] [CrossRef]
- Optimization ToolboxTM User’s Guide; 5th Printing; Revised for Version 3.0 (Release 14); The MathWorks, Inc.: Natic, MA, USA, June 2004.
- Cetingul, M.P.; Herman, C. A heat transfer model of skin tissue for the detection of lesions: Sensitivity analysis. Phys. Med. Biol. 2010, 55, 5933–5951. [Google Scholar] [CrossRef] [PubMed]
- McBride, A.; Bargmann, S.; Pond, D.; Limbert, G. Thermoelastic modelling of the skin at finite deformations. J. Therm. Biol. 2016, 62, 201–209. [Google Scholar] [CrossRef] [PubMed]





| Parameter | C1/JK−1 | C2/JK−1 | P1/mWK−1 | P2/mWK−1 | P12/mWK−1 | k/mVK−1 |
|---|---|---|---|---|---|---|
| Mean | 3.00 | 3.98 | 33.38 | 64.83 | 96.07 | 19.02 |
| SD | 0.11 | 0.10 | 2.77 | 3.91 | 7.19 | 1.09 |
| SD: Standard deviation. Number of measurements: 20. Maximum RMSE: εy = 14 μV, εT2 = 4 mK (Equation (7)) | ||||||
| Heat Flux (Equation (9)) | Model (Equation (5)) | ΔT0 (Equation (4)) | Errors (Equation (7)) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| A0/mW | A1/mW | τ1/s | ΔA0/mW | C1/JK−1 | A/K | B/K | τT | εy/µV | εT/mK | |
| (1) | 300.5 | 2125.9 | 8.4 | −200.3 | 3.01 | 2.51 | 0.99 | 9.0 | 8.88 | 0.13 |
| (2) | 300.4 | 2125.5 | 8.4 | −200.5 | 6.00 | 2.50 | 0.99 | 9.0 | 4.70 | 0.09 |
| (3) | 300.3 | 2123.6 | 8.4 | −200.6 | 8.98 | 2.50 | 0.99 | 9.0 | 3.29 | 0.08 |
| Subject | Gender | Age | Weight (kg) | Height (m) |
|---|---|---|---|---|
| Junior | Male | 28 | 67 | 1.72 |
| Senior | Male | 62 | 71 | 1.65 |
| Measure | Heat Flux (Equation (9)) | Model (Equation (5)) | ΔT0 (Equation (4)) | Errors (Equation (7)) | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| A0/mW | A1/W | τ1/s | ΔA0/mW | C1/JK−1 | A/K | B/K | τT | εy/µV | εT/mK | |
| M1 | 288 | 2.73 | 7.9 | −221 | 5.69 | 2.46 | 1.23 | 16.6 | 29.7 | 1.47 |
| M2 | 279 | 3.24 | 8.1 | −216 | 5.82 | 2.68 | 1.60 | 9.00 | 33.5 | 2.03 |
| M3 | 272 | 3.38 | 8.0 | −203 | 5.96 | 2.80 | 1.05 | 9.00 | 34.7 | 3.78 |
| M4 | 272 | 3.82 | 7.0 | −214 | 6.17 | 2.86 | 1.11 | 9.00 | 29.1 | 2.55 |
| Mean | 278 | 3.29 | 7.8 | −214 | 5.91 | 2.70 | 1.25 | 10.9 | ||
| SD | 7.6 | 0.45 | 0.5 | 7.6 | 0.21 | 0.18 | 0.15 | 3.80 | ||
| Measure Day | Heat Flux (Equation (9)) | Model (Equation (5)) | ΔT0 (Equation (4)) | Errors (Equation (7)) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| A0/mW | A1/W | τ1/s | ΔA0/mW | C1/JK−1 | A/K | B/K | τT | εy/µV | εT/mK | ||
| M1 | 1 | 310.4 | 3.03 | 7.3 | −223.6 | 5.53 | 2.10 | 0.80 | 9.00 | 24.4 | 2.59 |
| M2 | 325.9 | 4.89 | 5.3 | −251.2 | 6.08 | 2.41 | 1.46 | 9.00 | 32.3 | 1.75 | |
| M3 | 338.2 | 3.21 | 7.4 | −250.8 | 5.37 | 2.26 | 1.16 | 30.0 | 32.6 | 2.00 | |
| M4 | 324.8 | 3.55 | 7.0 | −241.3 | 5.91 | 2.57 | 0.69 | 21.0 | 28.3 | 2.69 | |
| M1 | 2 | 295.4 | 2.98 | 7.5 | −240.2 | 5.91 | 2.59 | 0.84 | 30.0 | 29.2 | 1.15 |
| M2 | 316.4 | 2.82 | 9.1 | −253.2 | 5.83 | 2.45 | 0.81 | 9.00 | 35.7 | 2.02 | |
| M3 | 330.9 | 3.73 | 6.6 | −255.1 | 6.00 | 3.08 | 0.60 | 30.0 | 25.8 | 1.54 | |
| M4 | 340.1 | 3.29 | 8.0 | −276.4 | 5.85 | 2.71 | 1.09 | 22.9 | 32.1 | 1.31 | |
| Measure Day | Heat Flux (Equation (9)) | Model (Equation (5)) | ΔT0 (Equation (4)) | Errors (Equation (7)) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| A0/mW | A1/W | τ1/s | ΔA0/mW | C1/JK−1 | A/K | B/K | τT | εy/µV | εT/mK | ||
| M1 | 3 | 15.5 | −0.271 | 5.0 | −202.0 | 5.08 | 0.61 | 0.49 | 9.30 | 42.3 | 1.60 |
| M2 | 12.9 | −0.037 | 17.9 | −200.3 | 5.23 | 0.63 | 0.60 | 9.00 | 23.6 | 1.96 | |
| M3 | 26.1 | 0.055 | 10.7 | −205.8 | 4.83 | 0.93 | 0.93 | 9.80 | 17.0 | 0.97 | |
| M1 | 4 | 295.5 | 2.114 | 6.9 | −248.4 | 4.85 | 1.88 | 0.96 | 9.00 | 26.3 | 1.70 |
| M2 | 300.4 | 3.217 | 6.4 | −247.2 | 6.04 | 1.96 | 0.73 | 30.0 | 35.3 | 2.75 | |
| M3 | 284.1 | 2.335 | 7.7 | −259.8 | 5.50 | 1.73 | 0.71 | 9.60 | 24.1 | 1.62 | |
| M4 | 246.9 | 1.935 | 8.3 | −263.7 | 5.31 | 1.43 | 0.81 | 9.00 | 26.6 | 2.42 | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rodríguez de Rivera, P.J.; Rodríguez de Rivera, M.; Socorro, F.; Rodríguez de Rivera, M.; Callicó, G.M. A Method to Determine Human Skin Heat Capacity Using a Non-Invasive Calorimetric Sensor. Sensors 2020, 20, 3431. https://doi.org/10.3390/s20123431
Rodríguez de Rivera PJ, Rodríguez de Rivera M, Socorro F, Rodríguez de Rivera M, Callicó GM. A Method to Determine Human Skin Heat Capacity Using a Non-Invasive Calorimetric Sensor. Sensors. 2020; 20(12):3431. https://doi.org/10.3390/s20123431
Chicago/Turabian StyleRodríguez de Rivera, Pedro Jesús, Miriam Rodríguez de Rivera, Fabiola Socorro, Manuel Rodríguez de Rivera, and Gustavo Marrero Callicó. 2020. "A Method to Determine Human Skin Heat Capacity Using a Non-Invasive Calorimetric Sensor" Sensors 20, no. 12: 3431. https://doi.org/10.3390/s20123431
APA StyleRodríguez de Rivera, P. J., Rodríguez de Rivera, M., Socorro, F., Rodríguez de Rivera, M., & Callicó, G. M. (2020). A Method to Determine Human Skin Heat Capacity Using a Non-Invasive Calorimetric Sensor. Sensors, 20(12), 3431. https://doi.org/10.3390/s20123431






