Comparison of Standard Clinical and Instrumented Physical Performance Tests in Discriminating Functional Status of High-Functioning People Aged 61–70 Years Old
Abstract
1. Introduction
2. Materials and Methods
2.1. Population
2.2. Outcome
2.3. Standard Clinical Physical Performance Tests
2.4. Instrumented Physical Performance Tests
2.5. Statistical Analysis
3. Results
3.1. Standard Clinical Physical Performance Measures
3.2. Instrumented Physical Performance Measures
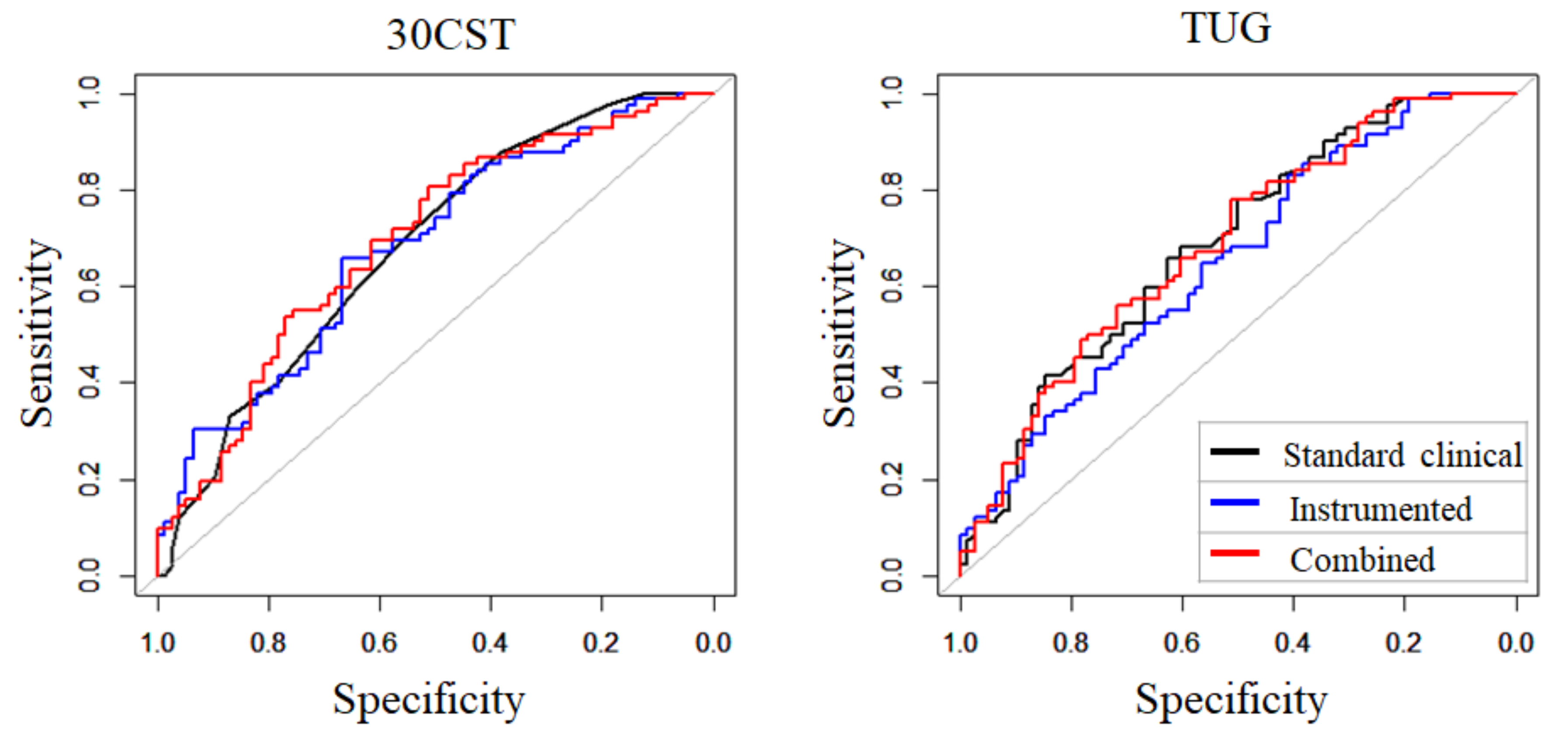
3.3. Comparison of AUC of Models with Standard Clinical, Instrumented, and Combined Measures
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Guralnik, J.M.; Ferrucci, L. Assessing the building blocks of function: Utilizing measures of functional limitation. Am. J. Prev. Med. 2003, 25, 112–121. [Google Scholar] [CrossRef]
- Jette, A.M.; Haley, S.M.; Kooyoomjian, J.T. Late-Life FDI Manual; Boston University: Boston, MA, USA, 2002; p. 73. [Google Scholar]
- Beauchamp, M.K.; Schmidt, C.T.; Pedersen, M.M.; Bean, J.F.; Jette, A.M. Psychometric properties of the Late-Life Function and Disability Instrument: A systematic review. BMC Geriatr. 2014, 14, 12. [Google Scholar] [CrossRef] [PubMed]
- Reuben, D.B.; Seeman, T.E.; Keeler, E.; Hayes, R.P.; Bowman, L.; Sewall, A.; Hirsch, S.H.; Wallace, R.B.; Guralnik, J.M. Refining the categorization of physical functional status: The added value of combining self-reported and performance-based measures. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2004, 59, 1056–1061. [Google Scholar] [CrossRef]
- Jones, C.J.; Rikli, R.E.; Beam, W.C. A 30-s chair-stand test as a measure of lower body strength in community-residing older adults. Res. Q. Exerc. Sport 1999, 70, 113–119. [Google Scholar] [CrossRef] [PubMed]
- Herman, T.; Giladi, N.; Hausdorff, J.M. Properties of the “Timed Up and Go” test: More than meets the eye. Gerontology 2011, 57, 203–210. [Google Scholar] [CrossRef] [PubMed]
- Podsiadlo, D.; Richardson, S. The Timed “Up & Go”: A Test of Basic Functional Mobility for Frail Elderly Persons. J. Am. Geriatr. Soc. 1991, 39, 142–148. [Google Scholar] [CrossRef] [PubMed]
- Grimm, B.; Bolink, S. Evaluating physical function and activity in the elderly patient using wearable motion sensors. EFORT Open Rev. 2016, 1, 112–120. [Google Scholar] [CrossRef]
- Weiss, A.; Herman, T.; Plotnik, M.; Brozgol, M.; Giladi, N.; Hausdorff, J.M. An instrumented timed up and go: The added value of an accelerometer for identifying fall risk in idiopathic fallers. Physiol. Meas. 2011, 32, 2003–2018. [Google Scholar] [CrossRef]
- Schwenk, M.; Gogulla, S.; Englert, S.; Czempik, A.; Hauer, K. Test-retest reliability and minimal detectable change of repeated sit-to-stand analysis using one body fixed sensor in geriatric patients. Physiol. Meas. 2012, 33, 1931–1946. [Google Scholar] [CrossRef]
- Van Lummel, R.C.; Walgaard, S.; Maier, A.B.; Ainsworth, E.; Beek, P.J.; van Dieën, J.H. The Instrumented Sit-to-Stand Test (iSTS) Has Greater Clinical Relevance than the Manually Recorded Sit-to-Stand Test in Older Adults. PLoS ONE 2016, 11, e0157968. [Google Scholar] [CrossRef]
- Helbostad, J.L.; Vereijken, B.; Becker, C.; Todd, C.; Taraldsen, K.; Pijnappels, M.; Aminian, K.; Mellone, S. Mobile Health Applications to Promote Active and Healthy Ageing. Sensors 2017, 17, 622. [Google Scholar] [CrossRef] [PubMed]
- PreventIT Project. Available online: http://www.preventit.eu/ (accessed on 21 January 2019).
- Nasreddine, Z.S.; Phillips, N.A.; Bédirian, V.; Charbonneau, S.; Whitehead, V.; Collin, I.; Cummings, J.L.; Chertkow, H. The Montreal Cognitive Assessment, MoCA: A Brief Screening Tool For Mild Cognitive Impairment. J. Am. Geriatr. Soc. 2005, 53, 695–699. [Google Scholar] [CrossRef] [PubMed]
- Peolsson, A.; Massy-Westropp, N.M.; Bear-Lehman, J. Reference values for adult grip strength measured with a Jamar dynamometer: A descriptive meta-analysis. Physiotherapy 2006, 92, 11–15. [Google Scholar] [CrossRef]
- Haley, S.M.; Jette, A.M.; Coster, W.J.; Kooyoomjian, J.T.; Levenson, S.; Heeren, T.; Ashba, J. Late Life Function and Disability Instrument: II. Development and evaluation of the function component. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2002, 57, M217–M222. [Google Scholar] [CrossRef]
- Mellone, S.; Tacconi, C.; Chiari, L. Validity of a Smartphone-based instrumented Timed Up and Go. Gait Posture 2012, 36, 163–165. [Google Scholar] [CrossRef]
- Mellone, S.; Tacconi, C.; Schwickert, L.; Klenk, J.; Becker, C.; Chiari, L. Smartphone-based solutions for fall detection and prevention: The FARSEEING approach. Z. Gerontol. Geriatr. 2012, 45, 722–727. [Google Scholar] [CrossRef] [PubMed]
- MATLAB and Statistics Toolbox Release 2017b; The MathWorks Inc.: Natick, MA, USA, 2017.
- Mellone, S. Movement Analysis by Mean of Interial Sensors: From Bench to Bedside. Ph.D. Thesis, Alma Mater Studiorum Università di Bologna, Bologna, Italy, 2013. [Google Scholar]
- Weiss, A.; Herman, T.; Plotnik, M.; Brozgol, M.; Maidan, I.; Giladi, N.; Gurevich, T.; Hausdorff, J.M. Can an accelerometer enhance the utility of the Timed Up and Go Test when evaluating patients with Parkinson’s disease? Med. Eng. Phys. 2010, 32, 119–125. [Google Scholar] [CrossRef]
- Zijlstra, A.; Mancini, M.; Lindemann, U.; Chiari, L.; Zijlstra, W. Sit-stand and stand-sit transitions in older adults and patients with Parkinson’s disease: Event detection based on motion sensors versus force plates. J. Neuroeng. Rehabil. 2012, 9, 75. [Google Scholar] [CrossRef]
- Palmerini, L.; Mellone, S.; Avanzolini, G.; Valzania, F.; Chiari, L. Quantification of Motor Impairment in Parkinson’s Disease Using an Instrumented Timed Up and Go Test. IEEE Trans. Neural Syst. Rehabil. Eng. 2013, 21, 664–673. [Google Scholar] [CrossRef]
- Weiss, A.; Mirelman, A.; Buchman, A.S.; Bennett, D.A.; Hausdorff, J.M.; Kado, D. Using a Body-Fixed Sensor to Identify Subclinical Gait Difficulties in Older Adults with IADL Disability: Maximizing the Output of the Timed Up and Go. PLoS ONE 2013, 8, e68885. [Google Scholar] [CrossRef]
- Moe-Nilssen, R.; Helbostad, J.L. Estimation of gait cycle characteristics by trunk accelerometry. J. Biomech. 2004, 37, 121–126. [Google Scholar] [CrossRef]
- Zijlstra, W. Assessment of spatio-temporal parameters during unconstrained walking. Eur. J. Appl. Physiol. 2004, 92, 39–44. [Google Scholar] [CrossRef] [PubMed]
- El-Gohary, M.; Pearson, S.; McNames, J.; Mancini, M.; Horak, F.; Mellone, S.; Chiari, L. Continuous monitoring of turning in patients with movement disability. Sensors 2013, 14, 356–369. [Google Scholar] [CrossRef] [PubMed]
- Salarian, A.; Horak, F.B.; Zampieri, C.; Carlson-Kuhta, P.; Nutt, J.G.; Aminian, K. iTUG, a sensitive and reliable measure of mobility. IEEE Trans. Neural Syst. Rehabil. Eng. 2010, 18, 303–310. [Google Scholar] [CrossRef] [PubMed]
- R Core Team (2018). R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2018; Available online: https://www.R-project.org/ (accessed on 21 January 2019).
- Harrell, F.E., Jr.; Charles Dupont and Many Others. Hmisc: Harrell Miscellaneous. R Package Version 4.1-1. 2018. Available online: https://CRAN.R-project.org/package=Hmisc (accessed on 21 January 2019).
- Schroeder, M.A.; Lander, J.; Levine-Silverman, S. Diagnosing and Dealing with Multicollinearity. West. J. Nurs. Res. 1990, 12, 175–187. [Google Scholar] [CrossRef] [PubMed]
- Imdadullah, M.; Aslam, M. Mctest: An R Package for Deteection of Collinearity among Regressors. R J. 2016, 8, 499–509. [Google Scholar]
- DeLong, E.R.; DeLong, D.M.; Clarke-Pearson, D.L. Comparing the areas under two or more correlated receiver operating characteristic curves: A nonparametric approach. Biometrics 1988, 44, 837–845. [Google Scholar] [CrossRef] [PubMed]
- Harrell, F.E., Jr. Rms: Regression Modeling Strategies. R Package Version 5.1-2. 2018. Available online: https://CRAN.R-project.org/package=rms (accessed on 21 January 2019).
- Van Lummel, R.; Evers, J.; Niessen, M.; Beek, P.; van Dieën, J. Older Adults with Weaker Muscle Strength Stand up from a Sitting Position with More Dynamic Trunk Use. Sensors 2018, 18, 1235. [Google Scholar] [CrossRef] [PubMed]
- Ferrucci, L.; Cooper, R.; Shardell, M.; Simonsick, E.M.; Schrack, J.A.; Kuh, D. Age-Related Change in Mobility: Perspectives From Life Course Epidemiology and Geroscience. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2016, 71, 1184–1194. [Google Scholar] [CrossRef]
- Mirelman, A.; Weiss, A.; Buchman, A.S.; Bennett, D.A.; Giladi, N.; Hausdorff, J.M. Association between performance on Timed Up and Go subtasks and mild cognitive impairment: Further insights into the links between cognitive and motor function. J. Am. Geriatr. Soc. 2014, 62, 673–678. [Google Scholar] [CrossRef]
- Stijntjes, M.; Meskers, C.G.M.; De Craen, A.J.M.; Van Lummel, R.C.; Rispens, S.M.; Slagboom, P.E.; Maier, A.B. Effect of calendar age on physical performance: A comparison of standard clinical measures with instrumented measures in middle-aged to older adults. Gait Posture 2016, 45, 12–18. [Google Scholar] [CrossRef] [PubMed]
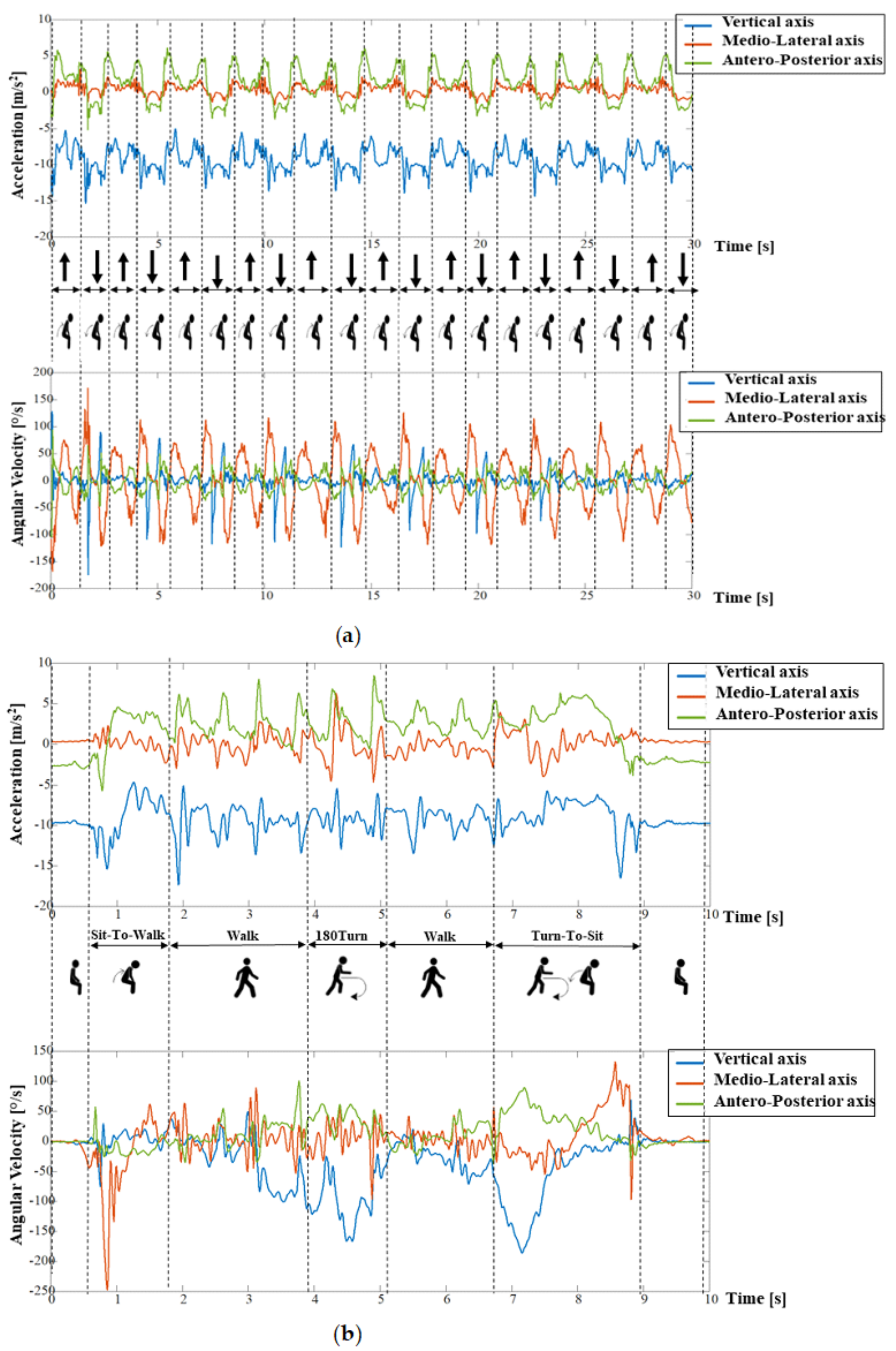
| Feature | Sensor | (Sub)Phases | Description |
|---|---|---|---|
| Repetitions [number] | Accelerometer/ Gyroscope | Total | Total number of repetitions |
| SD Duration | Accelerometer/ Gyroscope | Sit-to-Stand, Stand-to-Sit subphases | Standard deviation of the duration of each subphase of the 30CST |
| Duration [s] | Accelerometer/ Gyroscope | Sit-to-Stand, Stand-to-Sit subphases | Duration of each subphase of the 30CST |
| NJS AP ML V [m] | Accelerometer | Sit-to-Stand, Stand-to-Sit subphases | Time-normalized Jerk Score of the acceleration: where T is the duration (Tend-Tstart) of the considered submovement and a is the acceleration measured in m/s2. |
| RMS AP, ML, V [m/s2], [°/s] | Accelerometer, Gyroscope | Sit-to-Stand, Stand-to-Sit subphases | Root Mean Square of the signal, s, during the considered submovement (hence a measure of dispersion): where N is the total number of points of the signal s, and m is the mean value: |
| Feature | Sensor | (Sub)Phases | Description |
|---|---|---|---|
| Duration [s] | Accelerometer/ Gyroscope | Total, Sit-to-Walk, Walk, 180Turn, Turn-to-Sit | Total duration and duration of each subphase of the TUG |
| Number of Steps | Accelerometer/ Gyroscope | 180Turn, Walk | Number of steps during each subphase of the TUG |
| RMS AP, ML, V [m/s2] | Accelerometer | Sit-to-Walk, Walk, Turn-to-Sit | Root Mean Square of the signal, s, during the considered subphase (hence a measure of dispersion): where N is the total number of points of the signal s, and m is the mean value: mean(s) |
| NJS AP, ML, V [m] | Accelerometer | Sit-to-Walk, Turn-to-Sit | Time-Normalized Jerk Score of the acceleration: where T is the turn duration (Tend-Tstart) of the considered subphase, a is the acceleration measured in m/s2. |
| NJS V [-] | Gyroscope | 180Turn, Turn-to-Sit Turning | Normalized angular Jerk Score: ; where T is the turn duration (Tend-Tstart) of the considered component, ɷ is the angular velocity °/s, and TA is the Turning Angle in °. |
| Mean Velocity [°/s] | Gyroscope | 180Turn, Turn-to-Sit Turning | Mean Velocity, as the mean value of the angular velocity along the vertical axis during the turn: where is the angular velocity in °/s; NE and NS are the index of the end and the index of the beginning of the turn, respectively. |
| Maximum Velocity [°/s] | Gyroscope | 180Turn, Turn-to-Sit Turning | Maximum Velocity as the maximum value of the angular velocity along the vertical axis during the turn: where is the angular velocity in °/s; NE and NS are the index of the end and the index of the beginning of the turn, respectively. |
| Total Population N = 160 | HFS N = 78 | VHFS N = 82 | |
|---|---|---|---|
| Gender, Female | 87 (54.38%) | 52 (66.67%) | 35 (42.68%) |
| Age, years | 66.29 (2.40) | 66.13 (2.44) | 66.45 (2.37) |
| Height, cm | 170.94 (9.35) | 169.32 (9.86) | 172.49 (8.63) |
| Weight, kg | 79.49 (15.61) | 79.97 (16.35) | 79.04 (14.95) |
| Handgrip strength, kg | 34.41 (11.19) | 31.06 (10.75) | 37.61 (10.71) |
| Gait speed, m/s | 2.05 (0.46) | 1.82 (0.41) | 2.27 (0.40) |
| 30CST, number of repetitions | 13.41 (3.29) | 12.36 (3.13) | 14.40 (3.14) |
| TUG duration, s | 8.70 (1.60) | 9.25 (1.85) | 8.17 (1.10) |
| PA >=3 | 144 (90%) | 71 (91.03%) | 73 (89.02%) |
| Falls, number >=2 | 23 (14.38%) | 15 (19.23%) | 8 (9.76%) |
| MoCA, points | 27.08 (1.85) | 27.06 (1.89) | 27.09 (1.83) |
| Medications, number >=4 | 44 (27.50%) | 29 (37.18%) | 15 (18.29%) |
| LLFDI, points, median [range] | 72.31 [44.33 100] | 65.57 [44.33 71.33] | 79.35 [72.31 100] |
| AUC | 95% CI | p-Value of the DeLong Test | |||
|---|---|---|---|---|---|
| 30CST | Standard clinical | 0.68 | [0.60–0.76] | Standard clinical—Instrumented | 0.97 |
| Instrumented | 0.68 | [0.60–0.76] | Instrumented—Combined | 0.74 | |
| Combined | 0.69 | [0.61–0.77] | Standard clinical—Combined | 0.48 | |
| TUG | Standard clinical | 0.68 | [0.60–0.77] | Standard clinical—Instrumented | 0.26 |
| Instrumented | 0.65 | [0.56–0.73] | Instrumented—Combined | 0.94 | |
| Combined | 0.69 | [0.60–0.77] | Standard clinical—Combined | 0.12 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Coni, A.; Van Ancum, J.M.; Bergquist, R.; Mikolaizak, A.S.; Mellone, S.; Chiari, L.; Maier, A.B.; Pijnappels, M. Comparison of Standard Clinical and Instrumented Physical Performance Tests in Discriminating Functional Status of High-Functioning People Aged 61–70 Years Old. Sensors 2019, 19, 449. https://doi.org/10.3390/s19030449
Coni A, Van Ancum JM, Bergquist R, Mikolaizak AS, Mellone S, Chiari L, Maier AB, Pijnappels M. Comparison of Standard Clinical and Instrumented Physical Performance Tests in Discriminating Functional Status of High-Functioning People Aged 61–70 Years Old. Sensors. 2019; 19(3):449. https://doi.org/10.3390/s19030449
Chicago/Turabian StyleConi, Alice, Jeanine M. Van Ancum, Ronny Bergquist, A. Stefanie Mikolaizak, Sabato Mellone, Lorenzo Chiari, Andrea B. Maier, and Mirjam Pijnappels. 2019. "Comparison of Standard Clinical and Instrumented Physical Performance Tests in Discriminating Functional Status of High-Functioning People Aged 61–70 Years Old" Sensors 19, no. 3: 449. https://doi.org/10.3390/s19030449
APA StyleConi, A., Van Ancum, J. M., Bergquist, R., Mikolaizak, A. S., Mellone, S., Chiari, L., Maier, A. B., & Pijnappels, M. (2019). Comparison of Standard Clinical and Instrumented Physical Performance Tests in Discriminating Functional Status of High-Functioning People Aged 61–70 Years Old. Sensors, 19(3), 449. https://doi.org/10.3390/s19030449







