Assessment of Bandaged Burn Wounds Using Porcine Skin and Millimetric Radiometry
Abstract
1. Introduction
2. Materials and Methods
2.1. Three Layer Model for Dressed Burn Wound
2.2. Experimental Work
Experimental Description
2.3. Methodologies Applied on Porcine Skin Samples
2.3.1. Methodology 1: Skin without Burns
2.3.2. Methodology 2: Skin with Burns
2.3.3. Methodology 3: Skin with Different Burn Depths
3. Results
3.1. Porcine Skin Measurements without Burns
3.2. Porcine Skin Measurements with Burns
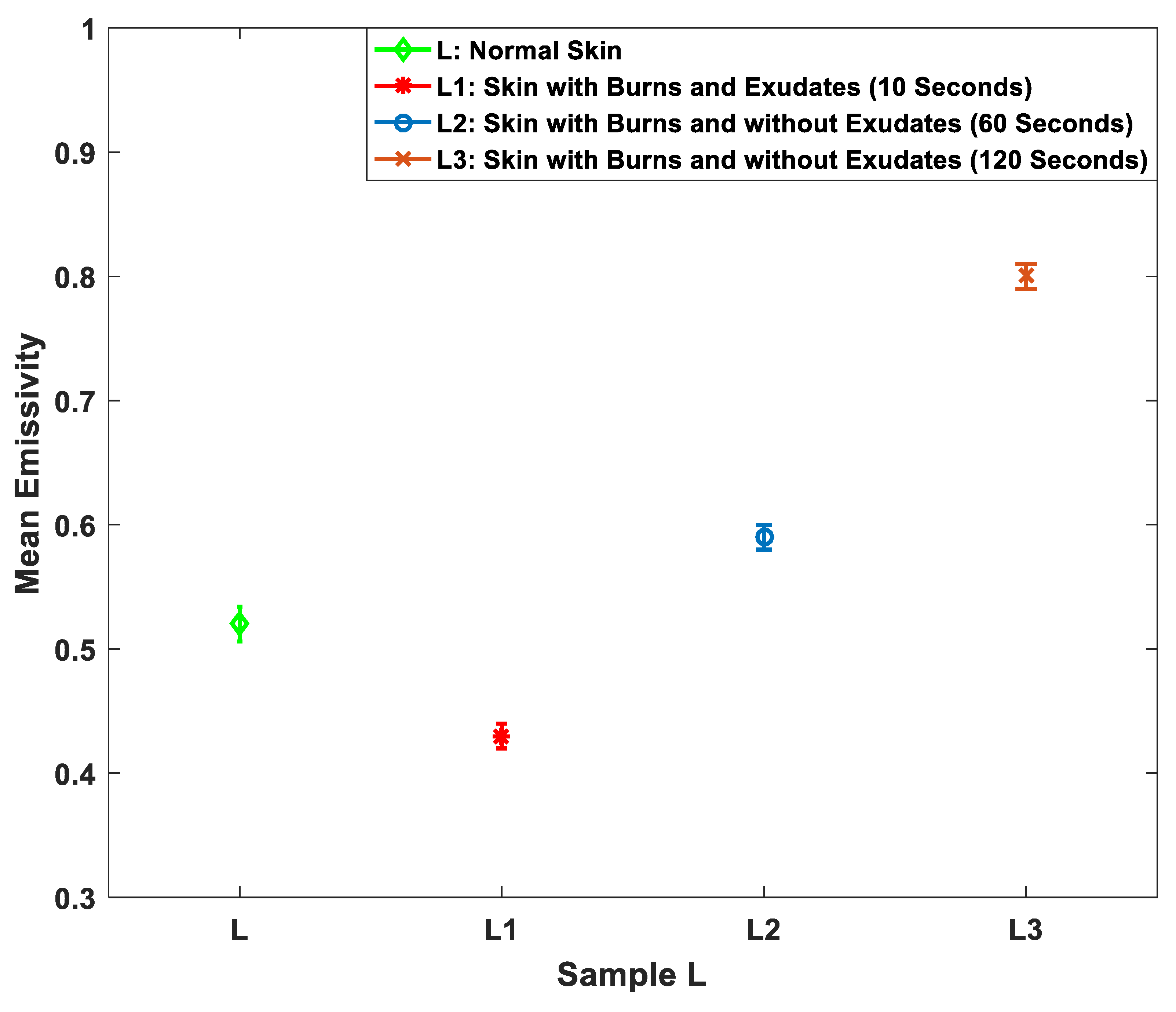
3.3. Porcine Skin Measurements with Different Burn Depth
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Stylianou, N.; Buchan, I.; Dunn, K.W. A review of the international Burn Injury Database (iBID) for England and Wales: Descriptive analysis of burn injuries 2003–2011. Epidemiology 2014, 5, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Park, B.H.; Saxer, C.; Srinivas, S.M.; Nelson, J.S.; de Boer, J.F. In vivo burn depth determination by high-speed fiber-based polarization sensitive optical coherence tomography. J. Biomed. Opt. 2001, 6, 474–479. [Google Scholar] [CrossRef] [PubMed]
- Jackson, D.M. The Diagnosis of the depth of burning. Br. J. Surg. 1953, 40, 588–596. [Google Scholar] [CrossRef] [PubMed]
- Chicago Burn Injury Attorneys. Chicago Burn Injury Attorneys Serving Illinois Victims. Chicago Burn Injury Attorneys Serving. January 2018. Available online: https://www.rosenfeldinjurylawyers.com/burns.html (accessed on 17 August 2018).
- Kurk, J. The Integumentary System. January 2016. Available online: http://slideplayer.com/slide/3478614 (accessed on 17 July 2018).
- Gao, Y.; Zoughi, R. Millimeter Wave Reflectometry and Imaging for Noninvasive Diagnosis of Skin Burn Injuries. IEEE Trans. Instrum. Meas. 2017, 66, 77–84. [Google Scholar] [CrossRef]
- Standring, S.; Borley, N.R.; Collins, P.; Crossman, A.R.; Gatzoulis, M.A. Gray’s Anatomy: The Anatomical Basis of Clinical Practice, 40th ed.; Elsevier Limited Publisher: Beijing, China, 2008. [Google Scholar]
- Bajwa, N. In Vivo Terahertz Imaging of Tissue Edema for Burn Wound and Flap Assessment. Ph.D. Thesis, University of California, Los Angeles, CA, USA, 2016. [Google Scholar]
- Branski, L.K.; Mittermayr, R.; Herndon, D.N.; Norbury, W.B.; Masters, O.E.; Hofmann, M.; Traber, D.L.; Redl, H.; Jeschke, M.G. A porcine model of full-thickness burn, excision and skin autografting. Burns 2008, 34, 1119–1127. [Google Scholar] [CrossRef] [PubMed]
- Dewey, W.C. Arrhenius relationships from the molecule and cell to the clinic. Int. J. Hyperth. 2009, 25, 3–20. [Google Scholar] [CrossRef] [PubMed]
- Dhivya, S.; Padma, V.V.; Santhini, E. Wound dressings—A review. Biomedicine 2015, 5, 24–28. [Google Scholar] [CrossRef]
- Jaskille, A.D.; Ramella-Roman, J.C.; Shupp, J.W.; Jordan, M.H.; Jeng, J.C. Critical review of burn depth assessment techniques: Part II. Review of laser doppler technology. J. Burn Care Res. 2010, 31, 151–157. [Google Scholar] [CrossRef]
- Janzekovic, Z. A new concept in the early excision and immediate grafting of burns. J. Trauma Acute Care Surg. 1970, 10, 1103–1108. [Google Scholar] [CrossRef]
- Cunha, J.P. MedicineNet.com. 2016. Available online: http://www.medicinenet.com/cuts_scrapes_and_puncture_wounds/article.htm (accessed on 19 August 2018).
- Harmer, S.W.; Shylo, S.; Shah, M.; Bowring, N.J.; Owda, A.Y. On the feasibility of assessing burn wound healing without removal of dressings using radiometric millimetre-wave sensing. Prog. Electromagn. Res. M 2016, 45, 173–183. [Google Scholar] [CrossRef]
- Jaskille, A.D.; Shupp, J.W.; Jordan, M.H.; Jeng, J.C. Critical Review of Burn Depth Assessment Techniques: Part I. Historical Review. J. Burn Care Res. 2009, 30, 937–947. [Google Scholar] [CrossRef] [PubMed]
- Heimbach, D.M.; Afromowitz, M.A.; Engrav, L.H.; Marvin, J.A.; Perry, B. Burn Depth Estimation-Man or Machine. J. Trauma 1984, 24, 373–378. [Google Scholar] [CrossRef] [PubMed]
- Hlava, P.; Moserová, J.; Königová, R. Validity of clinical assessment of the depth of a thermal injury. Acta Chir. Plast. 1983, 25, 202–208. [Google Scholar] [PubMed]
- Steiner, R.; Kunzi-Rapp, K.; Scharffetter-Kochanek, K. Optical Coherence Tomography: Clinical Applications in Dermatology. Med. Laser Appl. 2003, 18, 249–259. [Google Scholar] [CrossRef]
- Jiao, S.; Yu, W.; Stoica, G.; Wang, L.V. Contrast mechanisms in polarization-sensitive Mueller-matrix optical coherence tomography and application in burn imaging. Appl. Opt. 2003, 42, 5191–5197. [Google Scholar] [CrossRef] [PubMed]
- Cobb, M.J.; Chen, Y.; Underwood, R.A.; Usui, M.L.; Olerud, J.; Li, X. Noninvasive assessment of cutaneous wound healing using ultrahigh-resolution optical coherence tomography. J. Biomed. Opt. 2006, 11, 064002. [Google Scholar] [CrossRef] [PubMed]
- Hackett, M.E. The use of thermography in the assessment of depth of burn and blood supply of flaps, with preliminary reports on its use in Dupuytren’s contracture and treatment of varicose ulcers. Br. J. Plast. Surg. 1974, 27, 311–317. [Google Scholar] [CrossRef]
- Anselmo, V.J.; Zawacki, B.E. Effect of evaporative surface cooling on thermographic assessment of burn depth. Radiology 1977, 123, 331–332. [Google Scholar] [CrossRef] [PubMed]
- Renkielska, A.; Nowakowski, A.; Kaczmarek, M.; Ruminski, J. Burn depths evaluation based on active dynamic IR thermal imaging-a preliminary study. Burns 2006, 32, 867–875. [Google Scholar] [CrossRef]
- Saxena, A.K.; Willital, G.H. Infrared thermography: Experience from a decade of pediatric imaging. Eur. J. Pediatr. 2008, 167, 757–764. [Google Scholar] [CrossRef]
- Brink, J.A.; Sheets, P.W.; Dines, K.A.; Etchison, M.R.; Hanke, C.W.; Sadove, A.M. Quantitative assessment of burn injury in porcine skin with high-frequency ultrasonic imaging. Investig. Radiol. 1986, 21, 645–651. [Google Scholar] [CrossRef]
- Kalus, A.M.; Aindow, J.; Caulfield, M.R. Application of ultrasound in assessing burn depth. Lancet 1979, 1, 188–189. [Google Scholar] [CrossRef]
- Burns, P.N. The physical principles of Doppler and spectral analysis. J. Clin. Ultrasound 1987, 15, 567–590. [Google Scholar] [CrossRef]
- Waxman, K.; Lefcourt, N.; Achauer, B. Heated laser Doppler flow measurements to determine depth of burn injury. Am. J. Surg. 1989, 157, 541–543. [Google Scholar] [CrossRef]
- Gao, Y.; Zoughi, R. Millimeter reflectometry as an effective diagnosis tool for skin burn injuries. In Proceedings of the IEEE International Instrumentation and Measurement Technology Conference Proceedings, Taipei, Taiwan, 23–26 May 2016. [Google Scholar]
- Owda, A.Y.; Salmon, N.; Harmer, S.W.; Shylo, S.; Bowring, N.J.; Rezgu, N.D.; Shah, M. Millimeter-wave emissivity as a metric for the non-contact diagnosis of human skin conditions. Bioelectromagnetics 2017, 38, 559–569. [Google Scholar] [CrossRef] [PubMed]
- Andrews, C.J.; Kempf, M.; Kimble, R.; Cuttle, L. Development of a Consistent and Reproducible Porcine Scald Burn Model. PLoS ONE 2016, 11, e0162888. [Google Scholar] [CrossRef]
- Meyer, W.; Schwarz, R.; Neurand, K. The skin of domestic mammals as a model for the human skin, with special reference to the domestic pig. Curr. Probl. Dermatol. 1978, 7, 39–52. [Google Scholar]
- Dewhirst, M.W.; Viglianti, B.L.; Lora-Michiels, M.; Hoopes, P.J.; Hanson, M. Thermal dose requirement for tissue effect: Experimental and clinical findings. SPIE Therm. Treat. Tissue Energy Deliv. Assess. II 2003, 4954, 37. [Google Scholar]
- Gray, G.M.; White, R.J.; Williams, R.H.; Yardley, H.J. Lipid composition of the superficial stratum corneum cells of pig epidermis. Br. J. Dermatol. 1982, 106, 59–63. [Google Scholar] [CrossRef]
- Bardati, F.; Brown, V.; Ross, M.; Tognolatti, P. Microwave radiometry for medical thermal imaging: Theory and experiment. In Proceedings of the IEEE MTT-S International in Microwave Symposium Digest, Albuquerque, NM, USA, 1–5 June 1992. [Google Scholar]
- Pozar, D.M. Microwave Engineering, 4th ed.; John Wiley & Sons Publisher: Hoboken, NJ, USA, 2011. [Google Scholar]
- Salmon, N.A.; Borrill, J.R.; Gleed, D.G. Absolute temperature stability of passive imaging radiometers. In Proceedings of the Passive Millimeter-Wave Imaging Technology, Orlando, FL, USA, 21–25 April 1997. [Google Scholar]
- Ulaby, F.T.; Moore, R.K.; Fung, A.K. Microwave Remote Sensing: Active and Passive Volume I: Microwave Remote Sensing Fundamentals and Radiometry; Artech House Publisher: London, UK, 1981; Volume I. [Google Scholar]
- Wyatt, C. Radiometric Calibration: Theory and Methods, 1st ed.; Elsevier Publisher: New York, NY, USA, 1978. [Google Scholar]
- Rose, L.A.; Asher, W.E.; Reising, S.C.; Gaiser, P.W.; Germain, K.M.S.; Dowgiallo, D.J.; Horgan, K.A.; Farquharson, G.; Knapp, E.J. Radiometric measurements of the microwave emissivity of foam. IEEE Trans. Geosci. Remote Sens. 2002, 40, 2619–2625. [Google Scholar] [CrossRef]
- Williams, G. Microwave emissivity measurements of bubbles and foam. IEEE Trans. Geosci. Electron. 1971, 9, 221–224. [Google Scholar] [CrossRef]
- Salmon, N.A.; Kirkham, L.; Wilkinson, P.N. Characterisation and calibration of a large aperture (1.6 m) ka-band indoor passive millimeter wave. In Proceedings of the SPIE Millimeter Wave and Terahertz Sensors and Technology V, Edinburgh, UK, 24–27 September 2012. [Google Scholar]
- Andrews, C.J.; Cuttle, L.; Simpson, M.J. Quantifying the role of burn temperature, burn duration and skin thickness in an in vivo animal skin model of heat conduction. Int. J. Heat Mass Transf. 2016, 101, 542–549. [Google Scholar] [CrossRef]
- Log, T. Modeling Burns for Pre-Cooled Skin Flame Exposure. Int. J. Environ. Res. Public Health 2017, 14, 1024. [Google Scholar] [CrossRef] [PubMed]
- Ibrani, M.; Ahma, L.; Hamiti, E. The Age-Dependence of Microwave Dielectric Parameters of Biological Tissues. In Microwave Materials Characterization; InTech Publisher: London, UK, 2012; pp. 140–158. [Google Scholar]
- Karacolak, T.; Cooper, R.; Ünlü, E.S.; Topsakal, E. Dielectric Properties of Porcine Skin Tissue and In Vivo Testing of Implantable Antennas Using Pigs as Model Animals. IEEE Antennas Wirel. Propag. Lett. 2012, 11, 1686–1689. [Google Scholar] [CrossRef]
- Gabriel, C.; Peyman, A. Dielectric measurement: Error analysis and assessment of uncertainty. Phys. Med. Biol. 2006, 51, 6043–6046. [Google Scholar] [CrossRef] [PubMed]
- Owda, A.Y.; Salmon, N.; Rezgui, N.-D. Electromagnetic Signatures of Human Skin in the Millimeter Wave Band 80–100 GHz. Prog. Electromagn. Res. B 2018, 80, 79–99. [Google Scholar] [CrossRef]
- Gandhi, O.P.; Riazi, A. Absorption of millimeter waves by human beings and its biological implications. IEEE Trans. Microw. Theory Tech. 1986, 34, 228–235. [Google Scholar] [CrossRef]






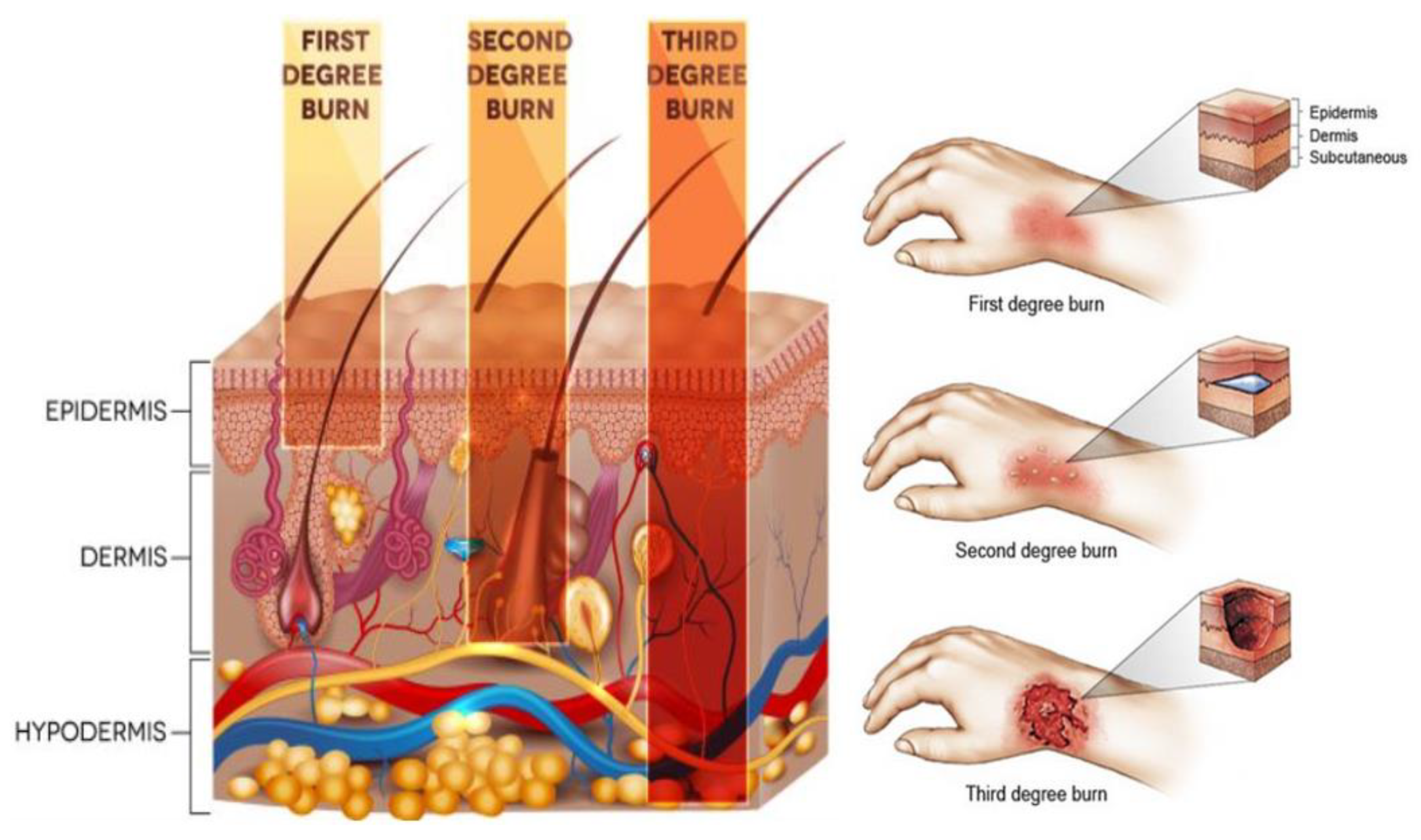
| Degree of Burn | Depth of Invasion | Signs | Degree of Pain |
|---|---|---|---|
| First degree or Superficial | Epidermis | Looks red without blisters and scars. | Painful |
| Second degree or Superficial dermal | Papillary dermis | Looks red with swelling, blisters, moisture, and scars. | Severe pain |
| Third degree or Deep dermal | Reticular dermis | Looks dry with pink and white color and severe scarring. | Pain and sensitivity are minimal |
| Fourth degree or Full thickness | The tissue under the skin (fat layer and beyond) | Looks dry with white, brown or black color and serious scarring. | No pain and no sensitivity because of the nerve ending destruction |
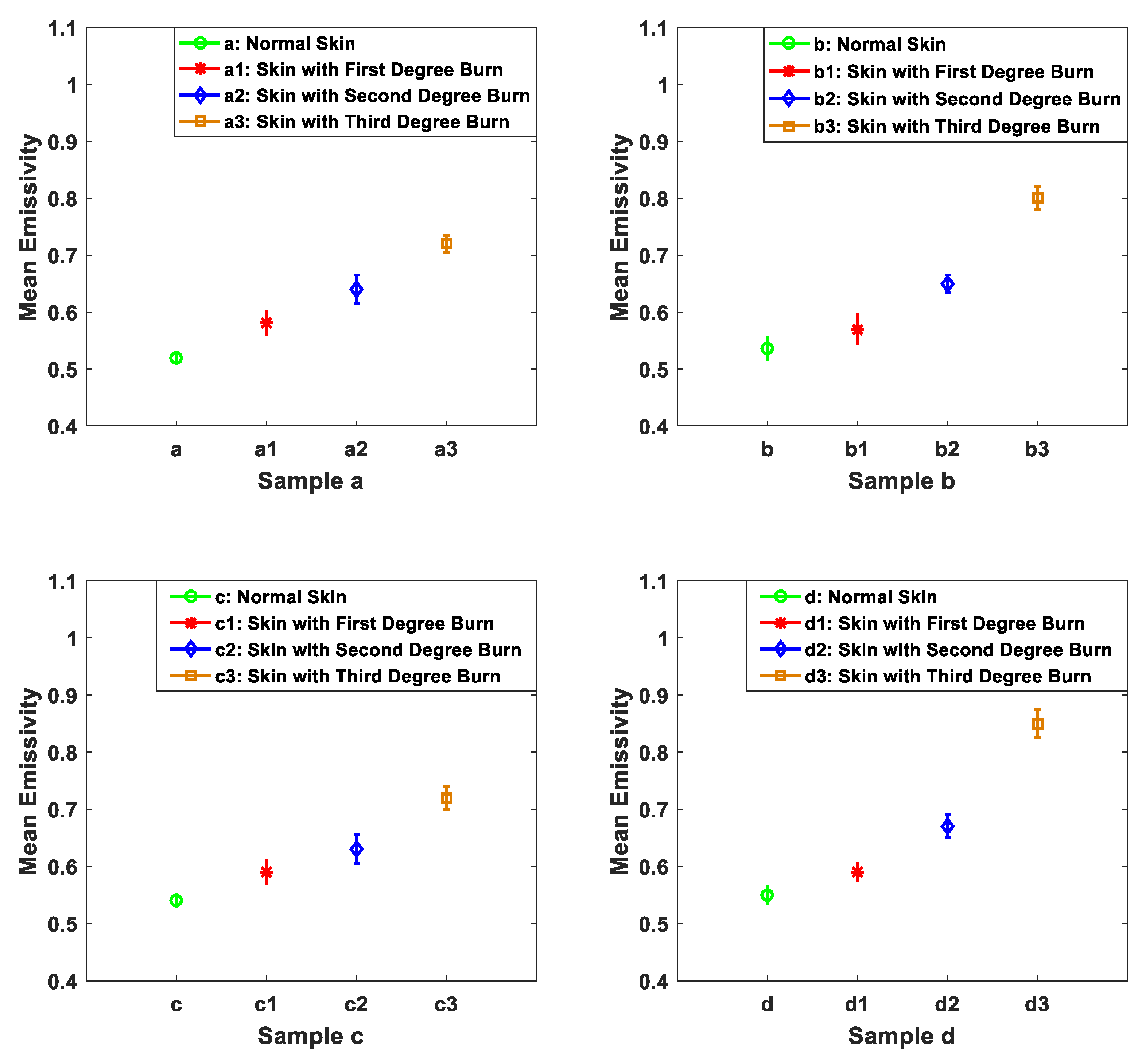
| Time Period for Heat Treatment (in Seconds) | Sample (a) | Sample (b) | Sample (c) | Sample (d) |
|---|---|---|---|---|
| 0 | 0.52 | 0.536 | 0.54 | 0.55 |
| 10 | 0.58 | 0.57 | 0.59 | 0.59 |
| 60 | 0.64 | 0.65 | 0.63 | 0.67 |
| 120 | 0.72 | 0.8 | 0.72 | 0.85 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Owda, A.Y.; Salmon, N.; Shylo, S.; Owda, M. Assessment of Bandaged Burn Wounds Using Porcine Skin and Millimetric Radiometry. Sensors 2019, 19, 2950. https://doi.org/10.3390/s19132950
Owda AY, Salmon N, Shylo S, Owda M. Assessment of Bandaged Burn Wounds Using Porcine Skin and Millimetric Radiometry. Sensors. 2019; 19(13):2950. https://doi.org/10.3390/s19132950
Chicago/Turabian StyleOwda, Amani Yousef, Neil Salmon, Sergiy Shylo, and Majdi Owda. 2019. "Assessment of Bandaged Burn Wounds Using Porcine Skin and Millimetric Radiometry" Sensors 19, no. 13: 2950. https://doi.org/10.3390/s19132950
APA StyleOwda, A. Y., Salmon, N., Shylo, S., & Owda, M. (2019). Assessment of Bandaged Burn Wounds Using Porcine Skin and Millimetric Radiometry. Sensors, 19(13), 2950. https://doi.org/10.3390/s19132950