Smart Optical Catheters for Epidurals
Abstract
:1. Introduction
2. Materials and Methods
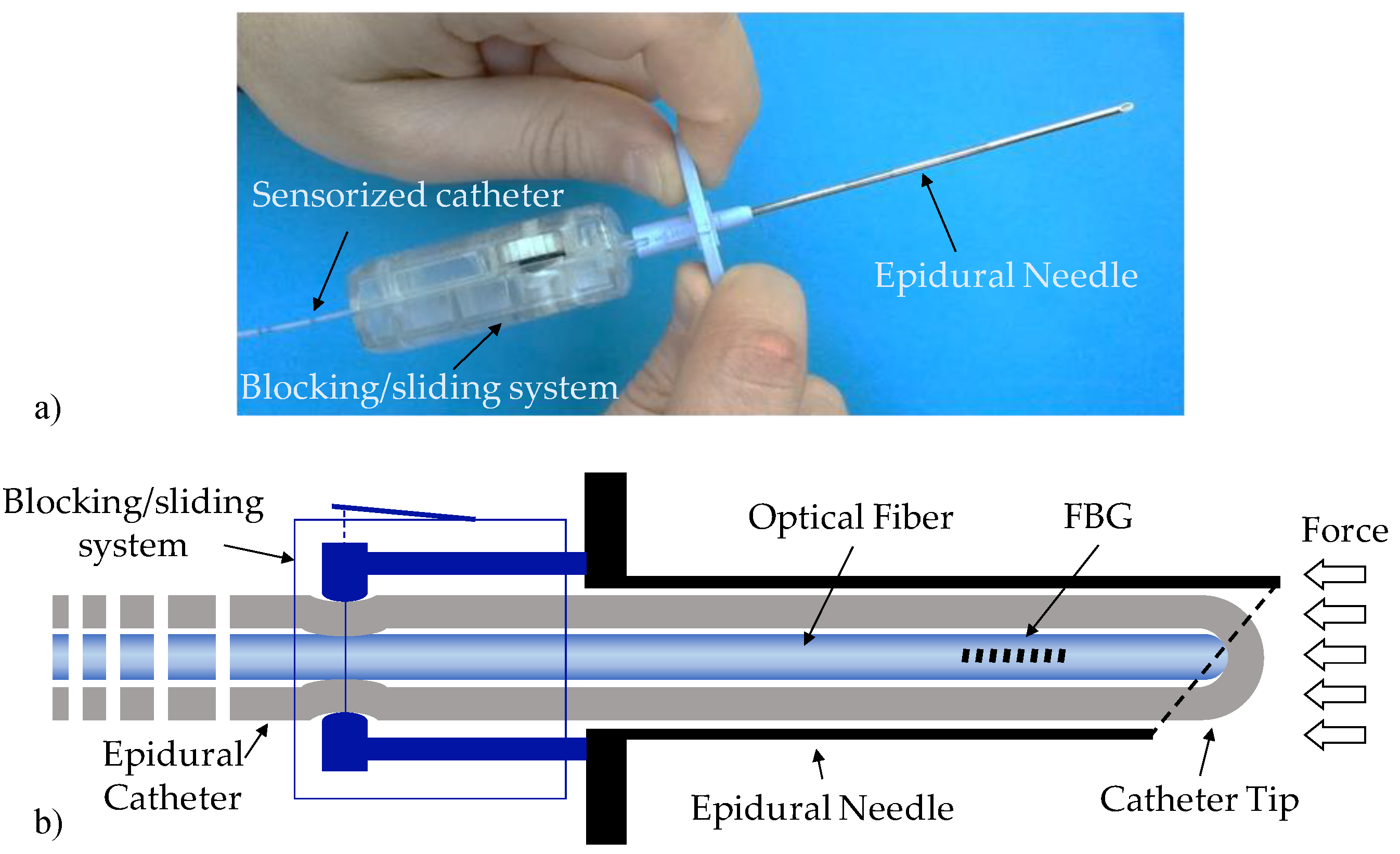
2.1. Sensorized Epidural Needle
2.2. The Fiber Bragg Grating
2.3. Console
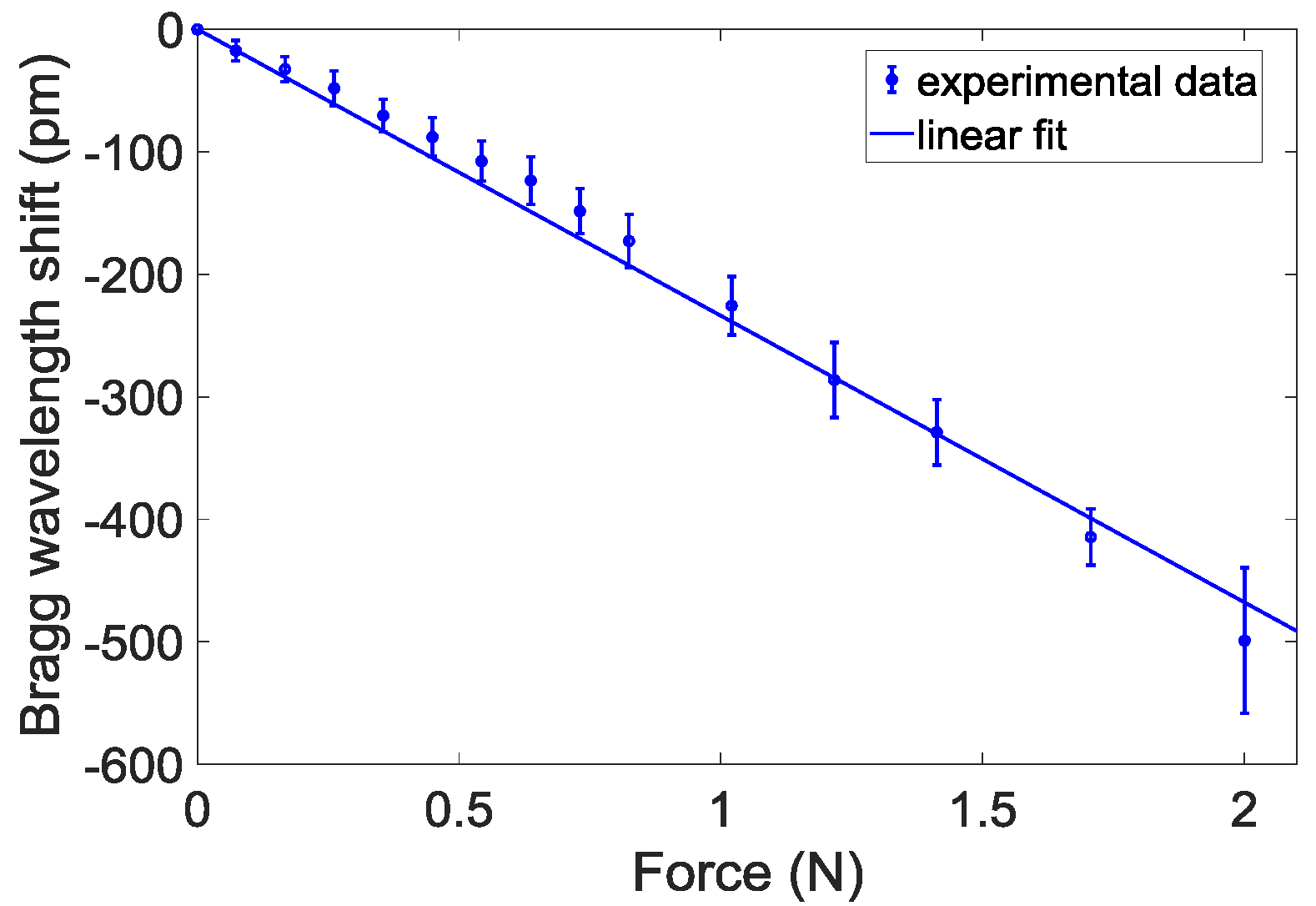
2.4. Calibration Tests
2.5. Experimental Methodology
3. Results
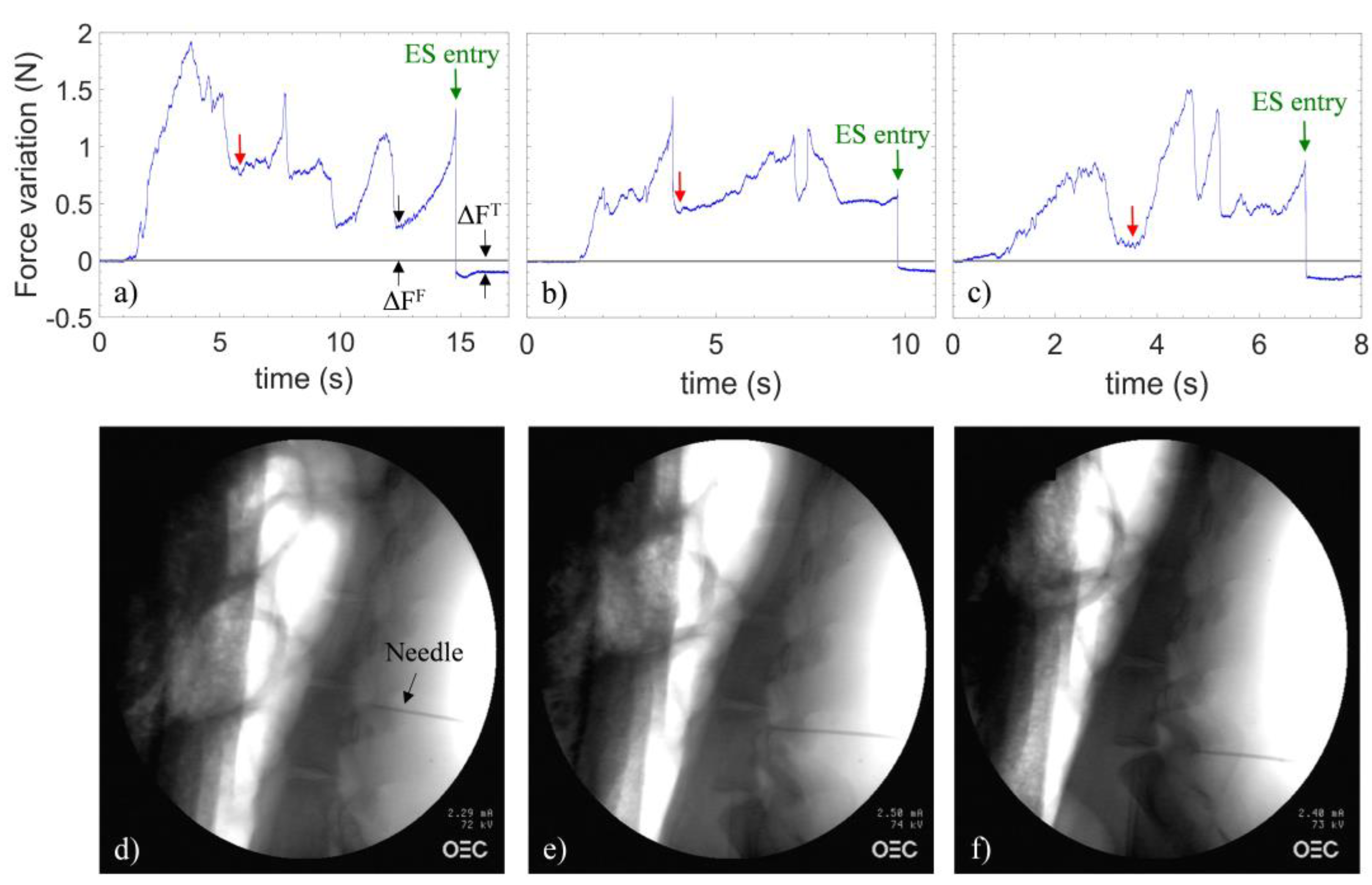
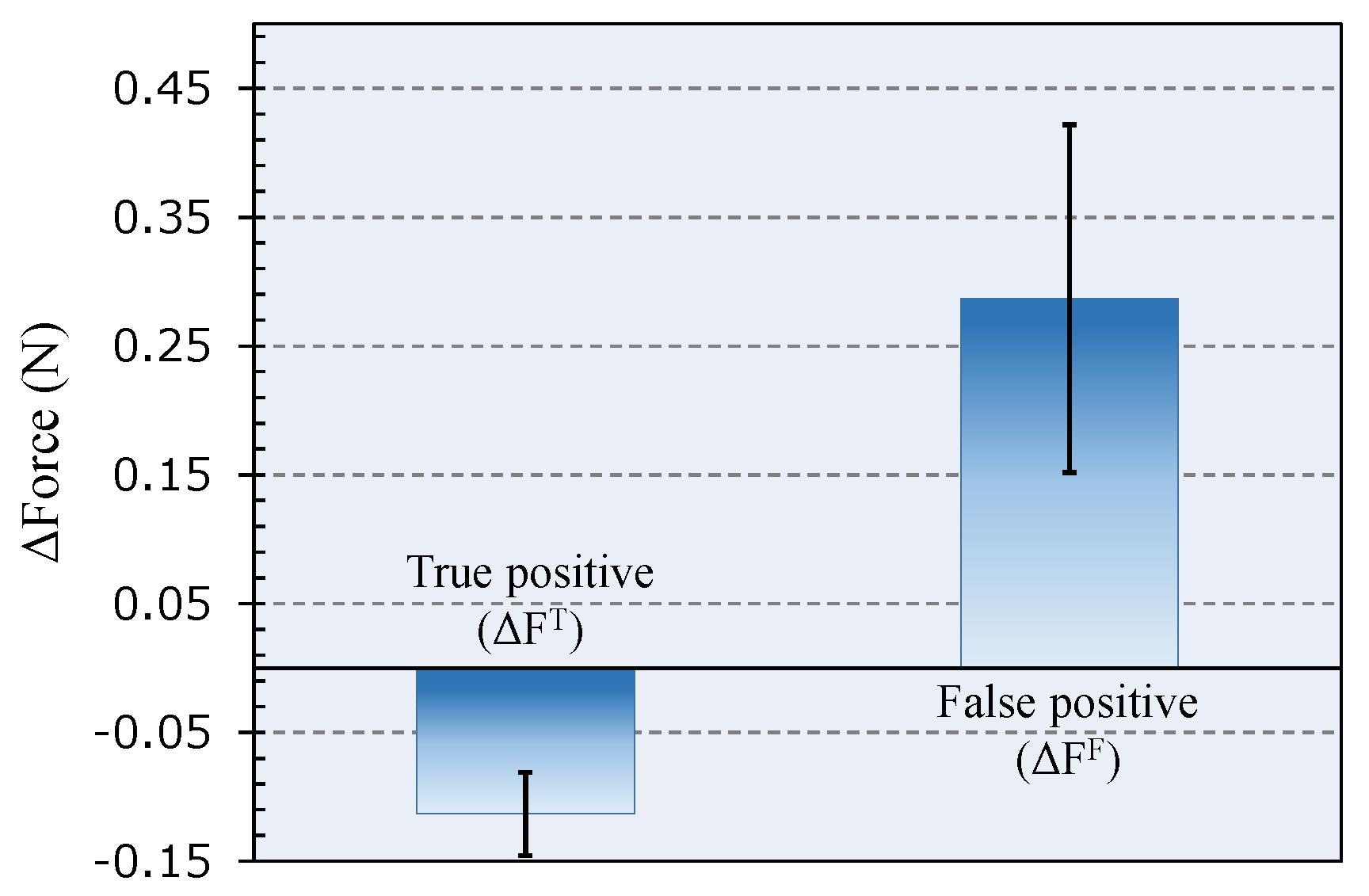
3.1. Epidural Space Identification
Discrimination Algorithm
3.2. Catheter Kinking Detection
4. Discussion
5. Conclusions
Author Contributions
Conflicts of Interest
Ethical Statement
References
- White, H.; Derby, R.; Wynne, G.A.R. Epidural injections for the diagnosis and treatment of low-back pain. Spine 1980, 5, 78–86. [Google Scholar] [CrossRef] [PubMed]
- Arendt, K.; Segal, S. Why epidurals do not always work. Rev. Obstet. Gynecol. 2008, 1, 49–55. [Google Scholar] [PubMed]
- Elsharkawy, H.; Sonny, A.; Chin, K.J. Localization of epidural space: A review of available technologies. J. Anaesthesiol. Clin. Pharmacol. 2017, 33, 16–27. [Google Scholar] [CrossRef] [PubMed]
- Teng, W.N.; Tsou, M.Y.; Chang, W.K.; Ting, C.K. Eyes on the needle: Identification and confirmation of the epidural space. Asian J. Anesthesiol. 2017, 55, 30–34. [Google Scholar] [CrossRef] [PubMed]
- Ting, C.K.; Tsou, M.Y.; Chen, P.T.; Chang, K.Y.; Mandell, M.S.; Chan, K.H.; Chang, Y.A. New Technique to Assist Epidural Needle Placement Fiber Optic-Guided Insertion Using Two Wavelengths. Anesthesiology 2010, 112, 1128–1135. [Google Scholar] [CrossRef] [PubMed]
- Rathmell, J.P.; Desjardins, A.E.; van der Voort, M.; Hendriks, B.H.W.; Nachabe, R.; Roggeveen, S.; Babic, D.; Söderman, M.; Brynolf, M.; Holmström, B. Identification of the Epidural Space with Optical Spectroscopy An In Vivo Swine Study. Anesthesiology 2010, 113, 1406–1418. [Google Scholar] [CrossRef] [PubMed]
- Anderson, T.A.; Kang, J.W.; Gubin, T.; Dasari, R.R.; So, P.T. Raman Spectroscopy Differentiates Each Tissue from the Skin to the Spinal Cord A Novel Method for Epidural Needle Placement? Anesthesiology 2016, 125, 793–804. [Google Scholar] [CrossRef] [PubMed]
- Kuo, W.C.; Kao, M.C.; Chang, K.Y.; Teng, W.N.; Tsou, M.Y.; Chang, Y.; Ting, C.K. Fiber-needle Swept-source Optical Coherence Tomography System for the Identification of the Epidural Space in Piglets. Anesthesiology 2015, 122, 585–594. [Google Scholar] [CrossRef] [PubMed]
- Kuo, W.C.; Kao, M.C.; Tsou, M.Y.; Ting, C.K. In vivo images of the epidural space with two-and three-dimensional optical coherence tomography in a porcine model. PLoS ONE 2017, 12, e0172149. [Google Scholar] [CrossRef] [PubMed]
- Ding, Z.; Tang, Q.; Liang, C.P.; Wu, K.; Sandlerc, A.; Li, H.; Chen, Y. Imaging Spinal Structures with Polarization-Sensitive Optical Coherence Tomography. IEEE Photonics J. 2016, 8, 1–8. [Google Scholar] [CrossRef]
- Carotenuto, B.; Micco, A.; Ricciardi, A.; Amorizzo, E.; Mercieri, M.; Cutolo, A.; Cusano, A. Optical Guidance Systems for Epidural Space Identification. IEEE J. Sel. Top. Q. Electron. 2017, 23, 1–9. [Google Scholar] [CrossRef]
- Carotenuto, B.; Ricciardi, A.; Micco, A.; Amorizzo, E.; Mercieri, M.; Cutolo, A.; Cusano, A. Optical Fiber Technology enables Smart Needles for Epidurals: An in-vivo swine study. Biomed. Opt. Express 2018. under review. [Google Scholar]
- Hermanides, J.; Hollmann, M.W.; Stevens, M.F.; Lirk, P. Failed epidural: Causes and management. Br. J. Anaesth. 2012, 109, 144–154. [Google Scholar] [CrossRef] [PubMed]
- Lim, K.S.; Yang, H.Z.; Becir, A.; Lai, M.H.; Ali, M.M.; Qiao, X.; Ahmad, H. Spectral analysis of bent fiber Bragg gratings: Theory and experiment. Opt. Lett. 2013, 38, 4409–4412. [Google Scholar] [CrossRef] [PubMed]
- Hill, K.O.; Meltz, G. Fiber Bragg grating technology fundamentals and overview. J. Lightwave Technol. 1997, 15, 1263–1276. [Google Scholar] [CrossRef]
- Reina, M.A.; Lirk, P.; Puigdellívol-Sánchez, A.; Mavar, M.; Prats-Galino, A. Human lumbar ligamentum flavum anatomy for epidural anesthesia: Reviewing a 3D MR-based interactive model and postmortem samples. Anesth. Analg. 2016, 122, 903–907. [Google Scholar] [CrossRef] [PubMed]
- Soto-Astorga, R.P.; West, S.; Putnis, S.; Hebden, J.C.; Desjardins, A.E. Epidural catheter with integrated light guides for spectroscopic tissue characterization. Biomed. Opt. Express 2013, 4, 2619–2628. [Google Scholar] [CrossRef] [PubMed]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Carotenuto, B.; Ricciardi, A.; Micco, A.; Amorizzo, E.; Mercieri, M.; Cutolo, A.; Cusano, A. Smart Optical Catheters for Epidurals. Sensors 2018, 18, 2101. https://doi.org/10.3390/s18072101
Carotenuto B, Ricciardi A, Micco A, Amorizzo E, Mercieri M, Cutolo A, Cusano A. Smart Optical Catheters for Epidurals. Sensors. 2018; 18(7):2101. https://doi.org/10.3390/s18072101
Chicago/Turabian StyleCarotenuto, Benito, Armando Ricciardi, Alberto Micco, Ezio Amorizzo, Marco Mercieri, Antonello Cutolo, and Andrea Cusano. 2018. "Smart Optical Catheters for Epidurals" Sensors 18, no. 7: 2101. https://doi.org/10.3390/s18072101
APA StyleCarotenuto, B., Ricciardi, A., Micco, A., Amorizzo, E., Mercieri, M., Cutolo, A., & Cusano, A. (2018). Smart Optical Catheters for Epidurals. Sensors, 18(7), 2101. https://doi.org/10.3390/s18072101






