Fabrication of Composite Microneedle Array Electrode for Temperature and Bio-Signal Monitoring
Abstract
:1. Introduction
2. Experimental
2.1. Fabrication of the CMAE
- (1)
- Fabrication of microneedle array. A 6 × 6 microneedle array was cut on a titanium alloy sheet (TC4, thickness of 100 μm, Baoji Titanium Industry Co., Ltd., Baoji, Shaanxi, China) by a focused beam laser with a pulse fiber laser machine (IPG, No.: YLP-1-100-20-20-CN, Burbach, Germany) as described previously [17]. The laser power was 15 W, laser frequency was 20 kHz, scanning speed was 500 mm/s, and scanning number was 50. The titanium sheet was completely cut through to form microneedles in a plane. These microneedles were manually bent 90° out of the plane. A microneedle array (MNA) was formed.
- (2)
- Spinning coating of the insulating layer. The MNA was assembled in a vacuum spinner (VTC-100, MTI Corporation, Richmond, CA, USA). 2 mL of SU-8 solution (Formlabs Inc., Somerville, MA, USA) was dropped on the upper surface of the MNA at 500 r/min. The MNA coated with the SU-8 layer was cured in a UV ultraviolet curing machine (Intelli-Ray 400, Uvitron, West Springfield, MA, USA) at 400 W for 10 min.
- (3)
- Sputter coating of Au layer. 100 nm thickness Au film was coated on the surface of the micro-needle array by a magnetron sputtering machine (VTC-16-SM, Shenyang Kejing Auto-instrument Co., Ltd., Jilin, China). A titanium line and a gold line were welded to the titanium layer and the gold layer, respectively. The CMAE was fabricated.
2.2. Mechanical Performance Test of the CMAE
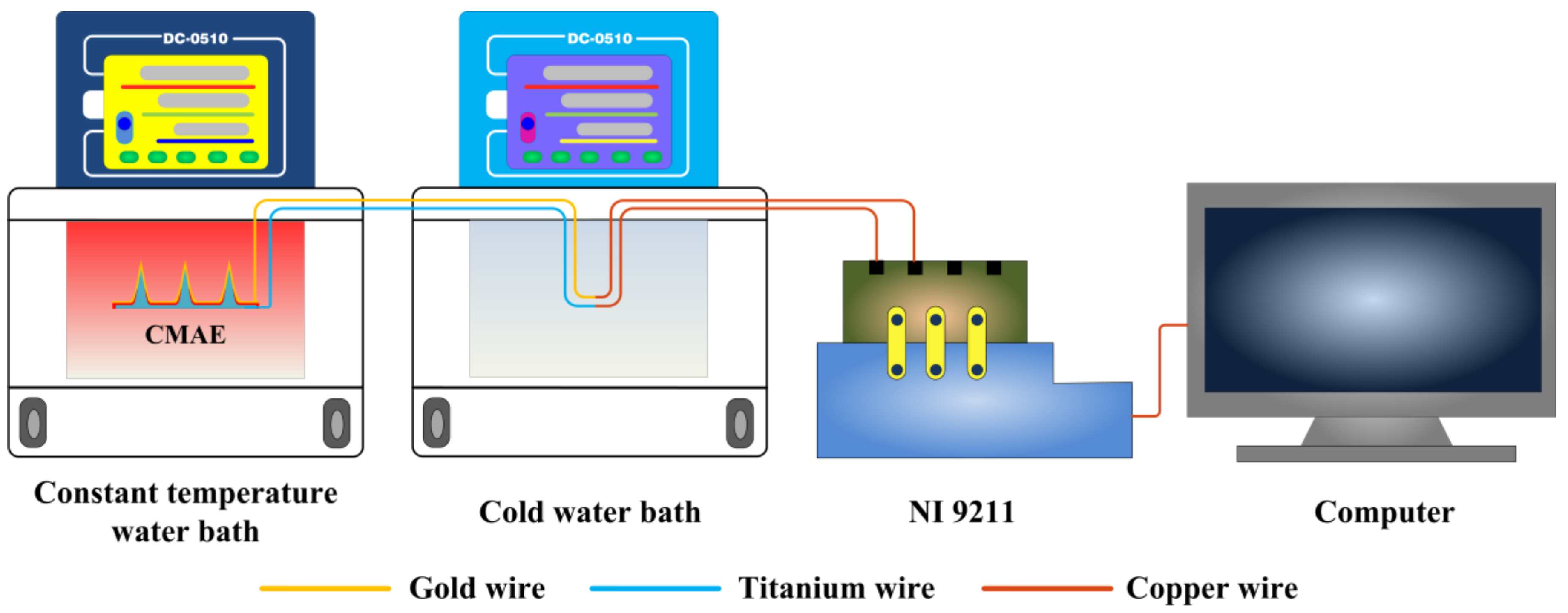
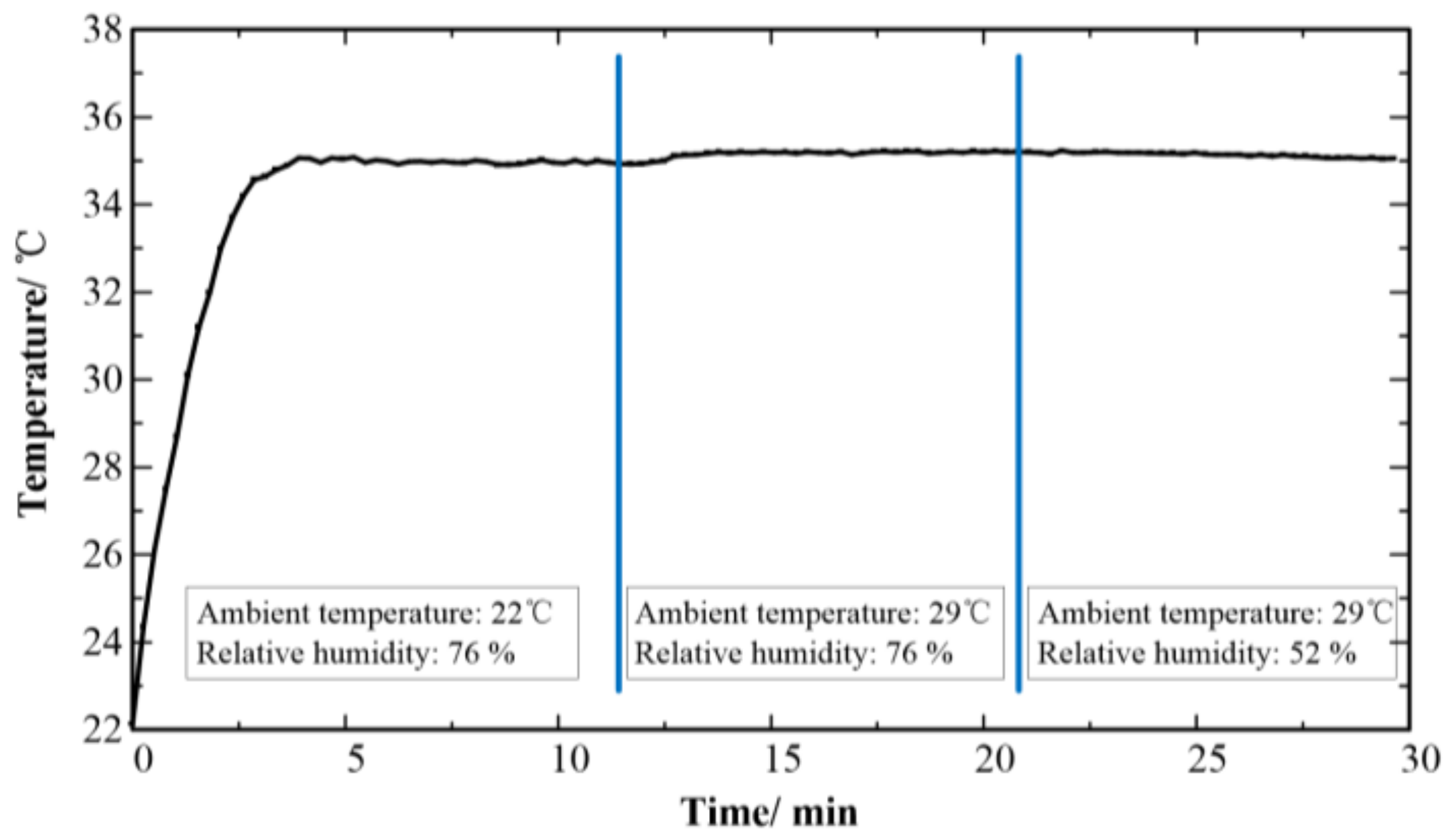
2.3. Temperature Measurement
2.4. Bio-Signals Recording
2.4.1. EII Test
2.4.2. EMG Test
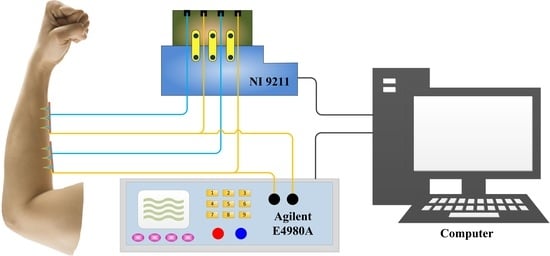
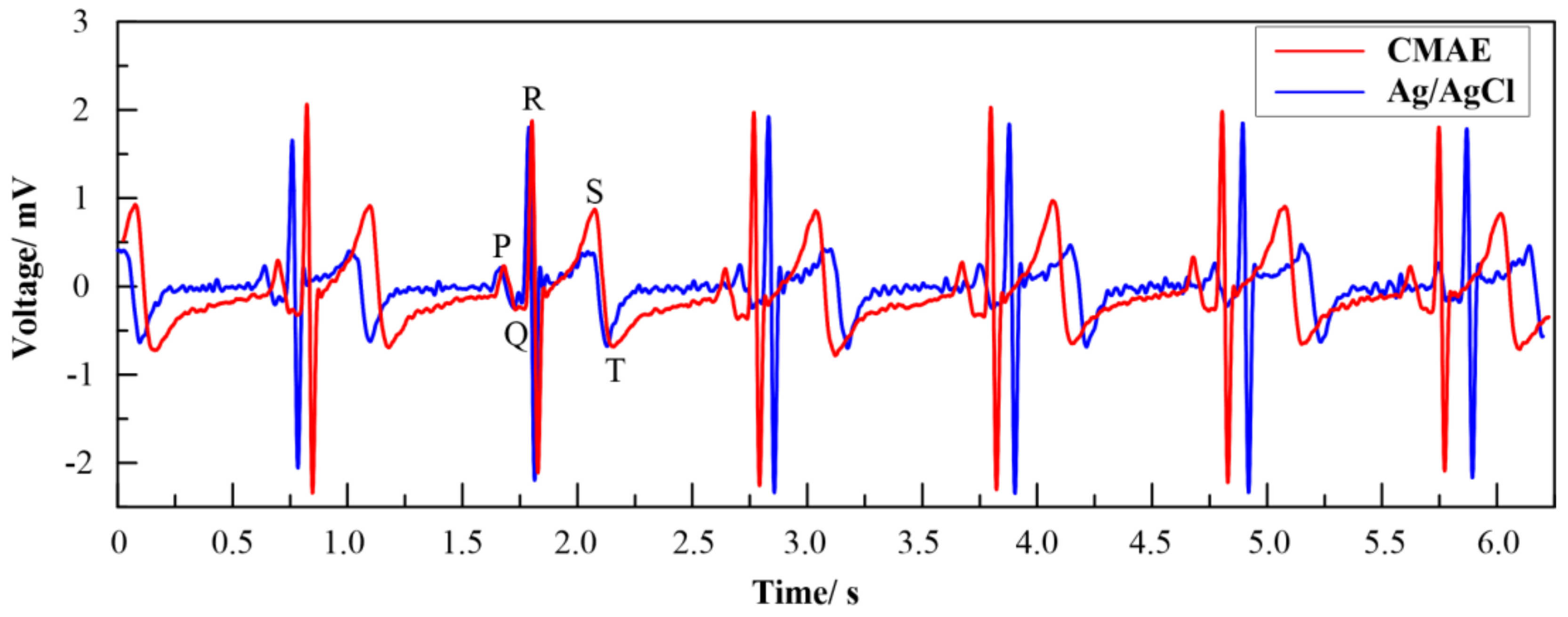
2.4.3. ECG Test
3. Results and Discussion
3.1. Measure Mechanism of the CMAE
3.2. Characterization
3.3. Mechanical Properties
3.4. Temperature Measurement Performance of the CMAE
3.5. Performance of the CMAE for Recording Bio-Signals
3.5.1. EII Measurement
3.5.2. EMG Measurement
3.5.3. ECG Measurement
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Nakamura, K. Central circuitries for body temperature regulation and fever. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2011, 301, R1207–R1228. [Google Scholar] [CrossRef] [PubMed]
- Murphy, P.J.; Campbell, S.S. Nighttime Drop in Body Temperature A Physiological Trigger for Sleep Onset? Sleep 1997, 20, 505–511. [Google Scholar] [CrossRef] [PubMed]
- Hamilos, D.L.; Nutter, D.; Gershtenson, J.; Redmond, D.P.; Di Clementi, J.D.; Schmaling, K.B.; Make, B.J.; Jones, J.F. Core body temperature is normal in chronic fatigue syndrome. Biol. Psychiatry 1998, 43, 293–302. [Google Scholar] [CrossRef]
- Geiser, F. Metabolic rate and body temperature reduction during hibernation and daily torpor. Annu. Rev. Physiol. 2004, 66, 239–274. [Google Scholar] [CrossRef] [PubMed]
- Martin, P.; Szuba, B.H.G.; Baxter, L.R., Jr. Electroconvulsive therapy in creases circadian amplitude and lowers core body temperature in depressed subjects. Biol. Psychiatry 1997, 42, 1130–1137. [Google Scholar]
- Li, Z.; Li, Y.; Liu, M.; Cui, L.; Yu, Y. Microneedle Electrode Array for Electrical Impedance Myography to Characterize Neurogenic Myopathy. Ann. Biomed. Eng. 2016, 44, 1566–1575. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.S.; Hwang, T.H.; Song, J.Y.; Park, S.H.; Park, J.; Yoo, E.S.; Lee, N.K.; Park, J.S. Design and Fabrication of Smart Band Module for Measurement of Temperature and GSR (Galvanic Skin Response) from Human Body. Procedia Eng. 2016, 168, 1577–1580. [Google Scholar] [CrossRef]
- Gao, W.; Emaminejad, S.; Nyein, H.Y.Y.; Challa, S.; Chen, K.; Peck, A.; Fahad, H.M.; Ota, H.; Shiraki, H.; Kiriya, D.; et al. Fully integrated wearable sensor arrays for multiplexed in situ perspiration analysis. Nature 2016, 529, 509–514. [Google Scholar] [CrossRef] [PubMed]
- Ota, H.; Chao, M.; Gao, Y.; Wu, E.; Tai, L.C.; Chen, K.; Matsuoka, Y.; Iwai, K.; Fahad, H.M.; Gao, W.; et al. 3D Printed “Earable” Smart Devices for Real-Time Detection of Core Body Temperature. ACS Sens. 2017, 2, 990–997. [Google Scholar] [CrossRef] [PubMed]
- Salvo, P.; Calisi, N.; Melai, B.; Cortigiani, B.; Mannini, M.; Caneschi, A.; Lorenzetti, G.; Paoletti, C.; Lomonaco, T.; Paolicchi, A.; et al. Temperature and pH sensors based on graphenic materials. Biosens. Bioelectron. 2017, 91, 870–877. [Google Scholar] [CrossRef] [PubMed]
- Zhou, W.; Song, R.; Pan, X.; Peng, Y.; Qi, X.; Peng, J.; Hui, K.S.; Hui, K.N. Fabrication and impedance measurement of novel metal dry bioelectrode. Sens. Actuators A Phys. 2013, 201, 127–133. [Google Scholar] [CrossRef]
- O’Mahony, C.; Pini, F.; Blake, A.; Webster, C.; O’Brien, J.; McCarthy, K.G. Microneedle-based electrodes with integrated through-silicon via for biopotential recording. Sens. Actuators A Phys. 2012, 186, 130–136. [Google Scholar] [CrossRef]
- Kim, M.; Kim, T.; Kim, D.S.; Chung, W.K. Curved Microneedle Array-Based sEMG Electrode for Robust Long-Term Measurements and High Selectivity. Sensors 2015, 15, 16265–16280. [Google Scholar] [CrossRef] [PubMed]
- Wang, R.; Jiang, X.; Wang, W.; Li, Z. A microneedle electrode array on flexible substrate for long-term EEG monitoring. Sens. Actuators B Chem. 2017, 244, 750–758. [Google Scholar] [CrossRef]
- Ma, G.; Wu, C. Microneedle, bio-microneedle and bio-inspired microneedle: A review. J. Control. Release 2017, 251, 11–23. [Google Scholar] [CrossRef] [PubMed]
- Donnelly, R.F.; Moffatt, K.; Alkilani, A.Z.; Vicente-Perez, E.M.; Barry, J.; McCrudden, M.T.; Woolfson, A.D. Hydrogel-forming microneedle arrays can be effectively inserted in skin by self-application: A pilot study centred on pharmacist intervention and a patient information leaflet. Pharm. Res. 2014, 31, 1989–1999. [Google Scholar] [CrossRef] [PubMed]
- Martanto, W.; Davis, S.P.; Holiday, N.R.; Wang, J.; Gill, H.S.; Prausnitz, M.R. Transdermal delivery of insulin using microneedles in vivo. Pharm. Res. 2004, 21, 947–952. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.Y.; Zhang, J.N.; Chen, B.Z.; Wang, Q.L.; Guo, X.D. A solid polymer microneedle patch pretreatment enhances the permeation of drug molecules into the skin. RSC Adv. 2017, 7, 15408–15415. [Google Scholar] [CrossRef]
- Chen, Y.; Jiang, H.; Zhao, W.; Zhang, W.; Liu, X.; Jiang, S. Fabrication and calibration of Pt—10%Rh/Pt thin film thermocouples. Measurement 2014, 48, 248–251. [Google Scholar] [CrossRef]
- Mutyala, M.S.K.; Zhao, J.; Li, J.; Pan, H.; Yuan, C.; Li, X. In-situ temperature measurement in lithium ion battery by transferable flexible thin film thermocouples. J. Power Sources 2014, 260, 43–49. [Google Scholar] [CrossRef]
- Ren, L.; Jiang, Q.; Chen, K.; Chen, Z.; Pan, C.; Jiang, L. Fabrication of a Micro-Needle Array Electrode by Thermal Drawing for Bio-Signals Monitoring. Sensors 2016, 16, 908. [Google Scholar] [CrossRef] [PubMed]
- Xu, S.; Dai, M.; Xu, C.; Chen, C.; Tang, M.; Shi, X.; Dong, X. Performance evaluation of five types of Ag/AgCl bio-electrodes for cerebral electrical impedance tomography. Ann. Biomed. Eng. 2011, 39, 2059–2067. [Google Scholar] [CrossRef] [PubMed]
- Chen, K.; Ren, L.; Chen, Z.; Pan, C.; Zhou, W.; Jiang, L. Fabrication of Micro-Needle Electrodes for Bio-Signal Recording by a Magnetization-Induced Self-Assembly Method. Sensors 2016, 16, 1533. [Google Scholar] [CrossRef] [PubMed]
- Merletti, R. The electrode–skin interface and optimal detection of bioelectric signals. Physiol. Meas. 2010, 31. [Google Scholar] [CrossRef]
- Kim, K.; Park, D.S.; Lu, H.M.; Che, W.; Kim, K.; Lee, J.B.; Ahn, C.H. A tapered hollow metallic microneedle array using backside exposure of SU-8. J. Micromech. Microeng. 2004, 14, 597–603. [Google Scholar] [CrossRef]
- Stavrinidis, G.; Michelakis, K.; Kontomitrou, V.; Giannakakis, G.; Sevrisarianos, M.; Sevrisarianos, G.; Chaniotakis, N.; Alifragis, Y.; Konstantinidis, G. SU-8 microneedles based dry electrodes for Electroencephalogram. Microelectron. Eng. 2016, 159, 114–120. [Google Scholar] [CrossRef]
- Jeong, H.R.; Lee, H.S.; Choi, I.J.; Park, J.H. Considerations in the use of microneedles: Pain, convenience, anxiety and safety. J. Drug Target 2017, 25, 29–40. [Google Scholar] [CrossRef] [PubMed]
- Gill, H.S.; Denson, D.D.; Burris, B.A.; Prausnitz, M.R. Effect of microneedle design on pain in human volunteers. Clin. J. Pain 2008, 24, 585–594. [Google Scholar] [CrossRef] [PubMed]
- Werschmoeller, D.; Li, X. Measurement of tool internal temperatures in the tool-chip contact region by embedded micro thin film thermocouples. J. Manuf. Process. 2011, 13, 147–152. [Google Scholar] [CrossRef]
- Forvi, E.; Bedoni, M.; Carabalona, R.; Soncini, M.; Mazzoleni, P.; Rizzo, F.; O’Mahony, C.; Morasso, C.; Cassarà, D.G.; Gramatica, F. Preliminary technological assessment of microneedles-based dry electrodes for biopotential monitoring in clinical examinations. Sens. Actuators A Phys. 2012, 180, 177–186. [Google Scholar] [CrossRef]
- Chi, Y.M.; Jung, T.P.; Cauwenberghs, G. Dry-contact and noncontact biopotential electrodes methodological review. IEEE Rev. Biomed. Eng. 2010, 3, 106–119. [Google Scholar] [CrossRef] [PubMed]
- Salvo, P.; Raedt, R.; Carrette, E.; Schaubroeck, D.; Vanfleteren, J.; Cardon, L. A 3D printed dry electrode for ECG/EEG recording. Sens. Actuators A Phys. 2012, 174, 96–102. [Google Scholar] [CrossRef]







© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sun, Y.; Ren, L.; Jiang, L.; Tang, Y.; Liu, B. Fabrication of Composite Microneedle Array Electrode for Temperature and Bio-Signal Monitoring. Sensors 2018, 18, 1193. https://doi.org/10.3390/s18041193
Sun Y, Ren L, Jiang L, Tang Y, Liu B. Fabrication of Composite Microneedle Array Electrode for Temperature and Bio-Signal Monitoring. Sensors. 2018; 18(4):1193. https://doi.org/10.3390/s18041193
Chicago/Turabian StyleSun, Yiwei, Lei Ren, Lelun Jiang, Yong Tang, and Bin Liu. 2018. "Fabrication of Composite Microneedle Array Electrode for Temperature and Bio-Signal Monitoring" Sensors 18, no. 4: 1193. https://doi.org/10.3390/s18041193
APA StyleSun, Y., Ren, L., Jiang, L., Tang, Y., & Liu, B. (2018). Fabrication of Composite Microneedle Array Electrode for Temperature and Bio-Signal Monitoring. Sensors, 18(4), 1193. https://doi.org/10.3390/s18041193