StraightenUp+: Monitoring of Posture during Daily Activities for Older Persons Using Wearable Sensors
Abstract
1. Introduction
2. StraightenUp+: A Wearable Device to Monitor Posture for Older Users
2.1. StraightenUp: A First Prototype for Static Postures
2.2. StraightenUp+ Design Rationale and Functional Requirements
2.3. StraightenUp+: A Wearable for Older Users
2.4. StraightenUp+: Implementation
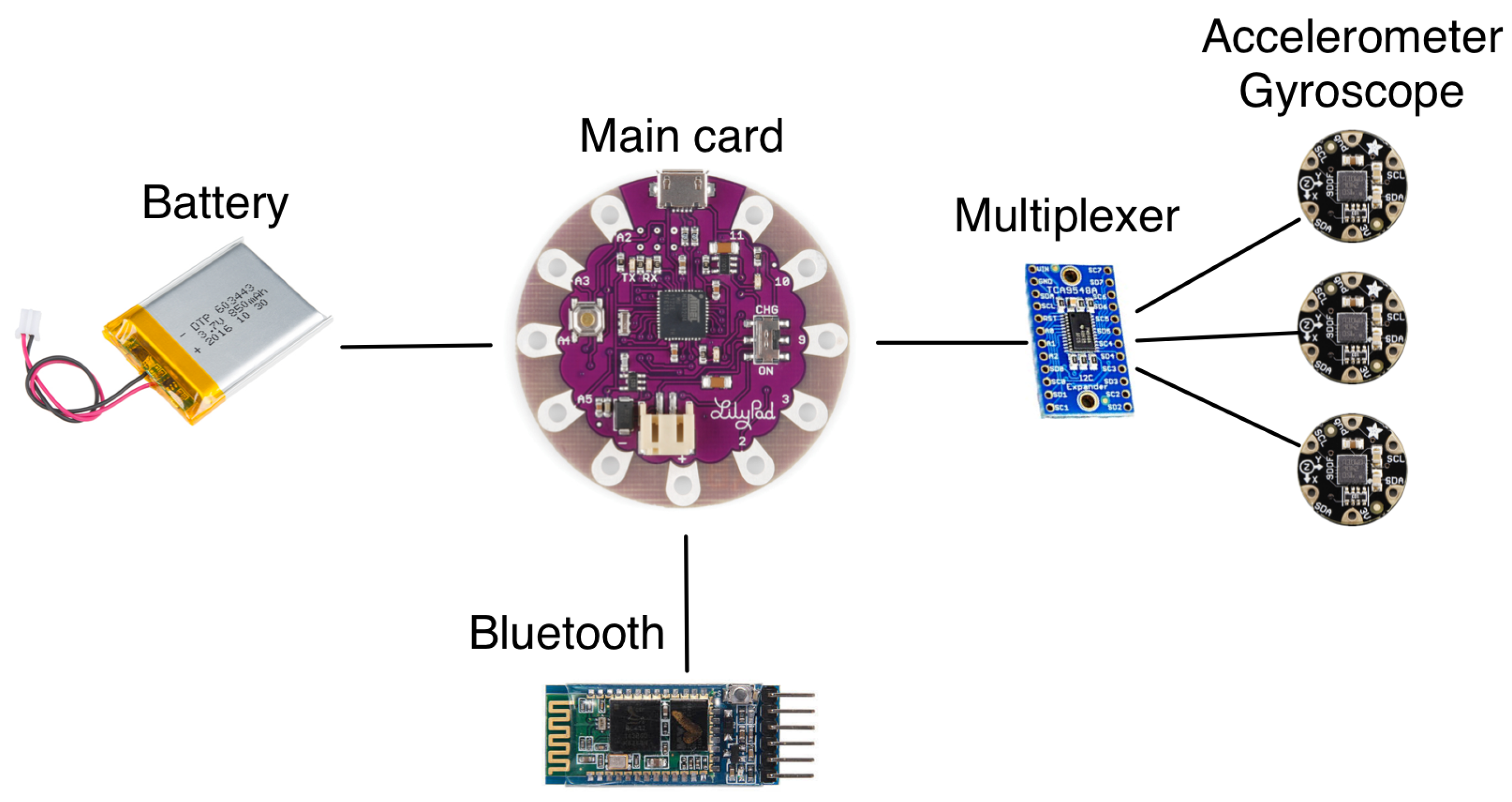
2.4.1. Hardware Components
2.4.2. Communication Protocols
2.4.3. Trunk Posture Measurement
3. Materials and Methods
3.1. Study Context
3.2. Collected Information
- DIGCOMP: DIGCOMP is a questionnaire used to assess four areas of digital competences: information, content creation, communication and problem solving. Each user is categorized into one of four possible groups: no, low, basic, or above basic [59].
- AttrakDiff: AttrakDiff is a questionnaire used to measure hedonic and pragmatic qualities of a device and it allows users to rate the usability and design of a product. It uses a scale of −3 to 3 (0 represents neutrality). The AttrakDiff questionnaire consists of four dimensions: pragmatic quality, hedonic quality identity (HQ-I), hedonic quality stimulation (HQ-S) and attraction [45,60].
- Frail Elderly Functional Assessment (FEFA) questionnaire: FEFA consists of 19 items and assesses function among frail older persons at a very low activity level [61].
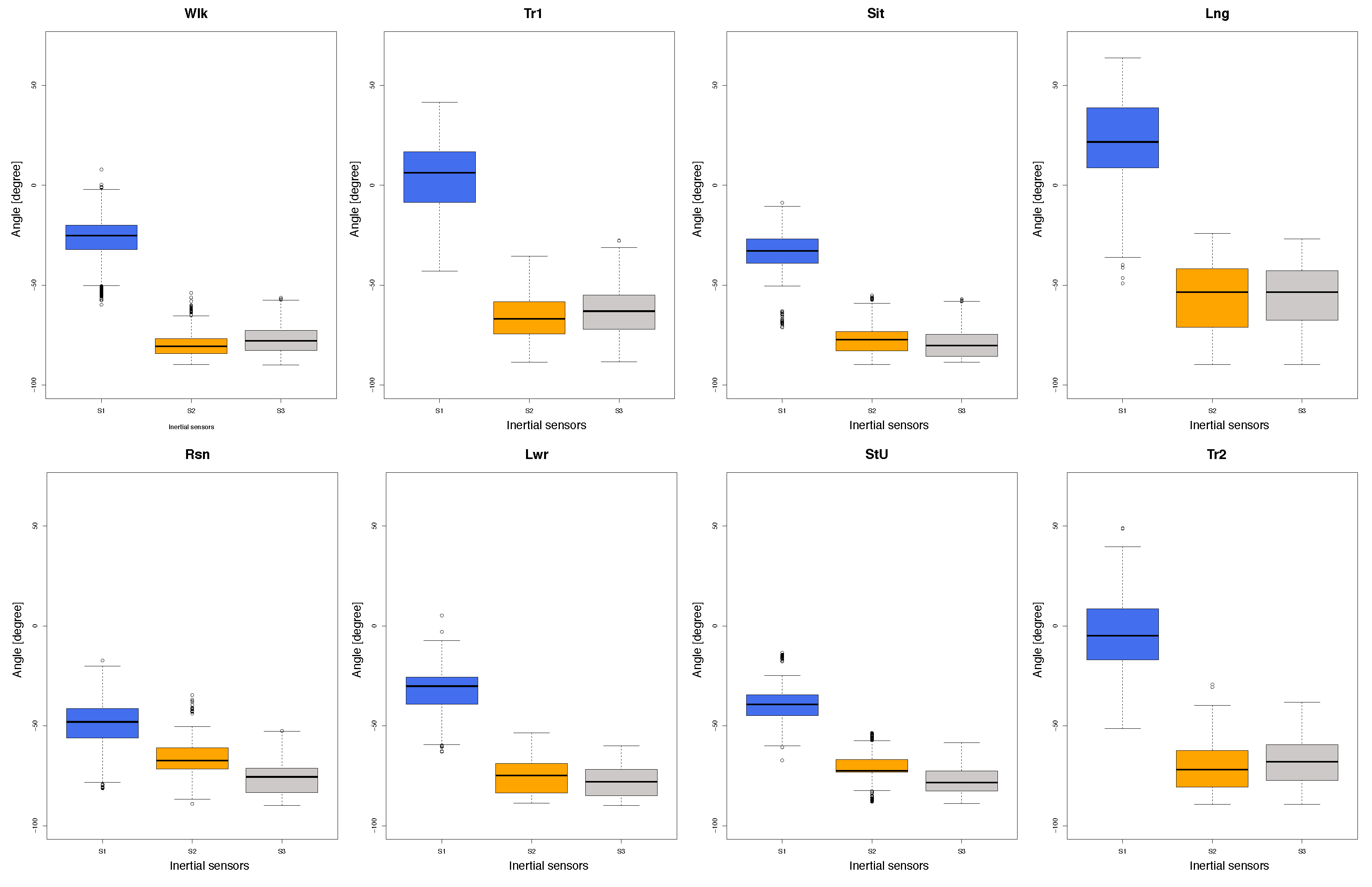
- Logged data: The StraightenUp+ prototype collected continuous information from the three inertial measurement units of 9 degrees of freedom of sensors (incorporated accelerometer and gyroscope). The recorded data relates to the inclination in the x- and y- axes. For our purposes of this study, the y-axis captures lateral movement (from left to right), while the x-axis captures horizontal movement (forward and backward).
- Observation data: One researcher observed the participants, noting the times in which they performed each posture in an audio recording, as well as any additional problem or issue that arose during the experiment.
- Interview data: A semi-structured interview was conducted to understand participant comfort, motive and frequency of use in relation to the device. Each interview was recorded (audio), transcribed and assigned a code (P1 to P30). Users were asked about the comfort of the device, whether they would use it, when and for how long, and what they liked and disliked about the device.
3.3. Participants
3.4. Procedure
4. Results
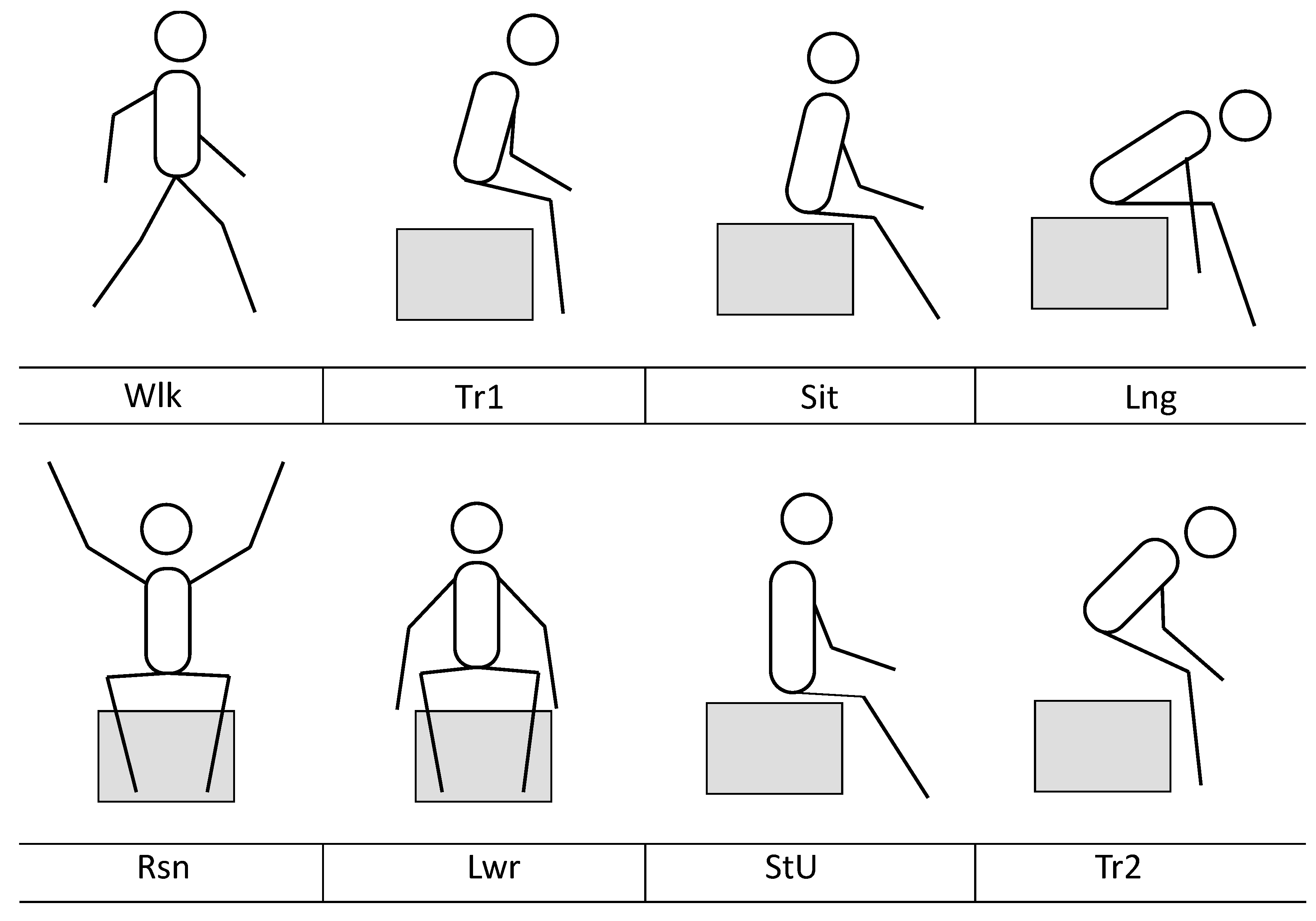
4.1. Descriptive Statistics
4.2. Posture Classification
4.3. Experience with StraightenUp+
4.4. Interviews
- Perception of device: Twenty-eight of the participants felt that StraightenUp is comfortable, and two felt that it was uncomfortable. Furthermore, four participants commented that the device felt imperceptible, and one that the straps made it adaptable to different bodily physiques. “I think it’s comfortable, it doesn’t bother me at all when I move, the straps don’t bother me one bit” (P4). One participant expressed their perception of the device using a comparison: “It was normal, I didn’t notice it, it was like a regular backpack” (P25). One participant indicated the need to include instructions or indicators to improve user experience in putting it on and taking it off. “You could improve it to make it so that I can’t make a mistake, something that prevents mistakes when putting it on” (P18).
- Motivation for use: Participants valued the device as an article that can have a positive health impact. Five participants stated that it could prevent them from adopting bad postures, three participants valued that it could help them understand or diagnose their posture, and two participants that it could improve their health. One participant views the device as a support tool. “When I’m walking, it (the device) helps me to stay on my feet and I feel like I’m walking okay. I go out a lot, I’m 84 years old, I take the bus, I take the subway, and I would like to be sure that I’m not going to fall over or that I won’t be knocked down” (P24).
- Frequency of use: Fourteen participants thought the best moment to use StraightenUp+ is during physical activities, e.g., walking and exercising. “I mean, during more physical activities, like running, walking, biking during the morning” (P10). Conversely, three participants claim the device is best used during periods of rest, when the user cannot be seen or is largely inactive. “Well, it’s complicated because the jokes would start, the negative comments and all that, and here it’s difficult, so I would say during the two hours dedicated to rest” (P7).
- Expectations: Sixteen participants would like to use StraightenUp+ permanently to gain greater understanding of the system and to become more accustomed to how it works. “I’ve never seen anything like it, it helps you to ask yourself things and then they become second nature… I’ve never used it, I asked how I was going to get around with this thing on, if I used it at all that is, everything you get used to using… I have got used to using so many things over the years but I never thought I’d use this, but if it can help you, you should use it” (P23). Ten participants would use it when required or when they felt pain or had a health problem. Finally, four participants were not interested in using the device at all, or unsure about wanting to use it. “I wouldn’t use it, for one. I’m not used to it, and second, it would mean being constantly concerned with walking perfectly, like a machine” (P1). Furthermore, three participants commented that the device should be used under the clothes rather than over them. “It should be used under your clothes because nobody would notice, nobody would criticise me, nobody would be pointing out that I use it or not” (P4).
5. Discussion
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Sallis, J.F.; Haskell, W.L.; Wood, P.D.; Fortmann, S.P.; Rogers, T.; Blair, S.N.; Paffenbarger, R.S., Jr. Physical activity assessment methodology in the Five-City Project. Am. J. Epidemiol. 1985, 121, 91–106. [Google Scholar] [CrossRef] [PubMed]
- Glassman, S.D.; Bridwell, K.; Dimar, J.R.; Horton, W.; Berven, S.; Schwab, F. The impact of positive sagittal balance in adult spinal deformity. Spine 2005, 30, 2024–2029. [Google Scholar] [CrossRef] [PubMed]
- Groessl, E.J.; Kaplan, R.M.; Rejeski, W.J.; Katula, J.A.; King, A.C.; Frierson, G.; Glynn, N.W.; Hsu, F.C.; Walkup, M.; Pahor, M. Health-related quality of life in older adults at risk for disability. A. J. Prev. Med. 2007, 33, 214–218. [Google Scholar] [CrossRef] [PubMed]
- Godfrey, A.; Conway, R.; Meagher, D.; ÓLaighin, G. Direct measurement of human movement by accelerometry. Med. Eng. Phys. 2008, 30, 1364–1386. [Google Scholar] [CrossRef] [PubMed]
- Schrack, J.A.; Cooper, R.; Koster, A.; Shiroma, E.J.; Murabito, J.M.; Rejeski, W.J.; Ferrucci, L.; Harris, T.B. Assessing daily physical activity in older adults: Unraveling the complexity of monitors, measures, and methods. J. Gerontol. Ser. A 2016, 71, 1039–1048. [Google Scholar] [CrossRef] [PubMed]
- Tedesco, S.; Barton, J.; O’Flynn, B. A review of activity trackers for senior citizens: Research perspectives, commercial landscape and the role of the insurance industry. Sensors 2017, 17, 1277. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.; Wei, Y.; Liu, L.; Zhong, J.; Sun, L.; Liu, Y. Towards unsupervised physical activity recognition using smartphone accelerometers. Multimed. Tools Appl. 2017, 76, 10701–10719. [Google Scholar] [CrossRef]
- Shahmohammadi, F.; Hosseini, A.; King, C.E.; Sarrafzadeh, M. Smartwatch Based Activity Recognition Using Active Learning. In Proceedings of the 2017 IEEE/ACM International Conference on Connected Health: Applications, Systems and Engineering Technologies (CHASE), Philadelphia, PA, USA, 17–19 July 2017; pp. 321–329. [Google Scholar] [CrossRef]
- Freedson, P.S.; Miller, K. Objective monitoring of physical activity using motion sensors and heart rate. Res. Q. Exerc. Sport 2000, 71, 21–29. [Google Scholar] [CrossRef] [PubMed]
- Bertolotti, G.M.; Cristiani, A.M.; Colagiorgio, P.; Romano, F.; Bassani, E.; Caramia, N.; Ramat, S. A wearable and modular inertial unit for measuring limb movements and balance control abilities. IEEE Sens. J. 2016, 16, 790–797. [Google Scholar] [CrossRef]
- Fanchamps, M.H.; Horemans, H.L.; Ribbers, G.M.; Stam, H.J.; Bussmann, J.B. The Accuracy of the Detection of Body Postures and Movements Using a Physical Activity Monitor in People after a Stroke. Sensors 2018, 18, 2167. [Google Scholar] [CrossRef] [PubMed]
- Soangra, R.; Lockhart, T.E. Inertial Sensor-Based Variables Are Indicators of Frailty and Adverse Post-Operative Outcomes in Cardiovascular Disease Patients. Sensors 2018, 18, 1792. [Google Scholar] [CrossRef] [PubMed]
- Bourke, A.; O’brien, J.; Lyons, G. Evaluation of a threshold-based tri-axial accelerometer fall detection algorithm. Gait Posture 2007, 26, 194–199. [Google Scholar] [CrossRef] [PubMed]
- Howcroft, J.; Kofman, J.; Lemaire, E.D. Prospective fall-risk prediction models for older adults based on wearable sensors. IEEE Trans. Neural Syst. Rehabil. Eng. 2017, 25, 1812–1820. [Google Scholar] [CrossRef] [PubMed]
- Cola, G.; Avvenuti, M.; Vecchio, A.; Yang, G.Z.; Lo, B. An on-node processing approach for anomaly detection in gait. IEEE Sens. J. 2015, 15, 6640–6649. [Google Scholar] [CrossRef]
- Ermes, M.; Pärkkä, J.; Mäntyjärvi, J.; Korhonen, I. Detection of daily activities and sports with wearable sensors in controlled and uncontrolled conditions. IEEE Trans. Inf. Technol. Biomed. 2008, 12, 20–26. [Google Scholar] [CrossRef] [PubMed]
- Montalto, F.; Guerra, C.; Bianchi, V.; De Munari, I.; Ciampolini, P. MuSA: Wearable multi sensor assistant for human activity recognition and indoor localization. In Ambient Assisted Living; Springer: New York, NY, USA, 2015; pp. 81–92. [Google Scholar]
- Awais, M.; Palmerini, L.; Bourke, A.K.; Ihlen, E.A.; Helbostad, J.L.; Chiari, L. Performance Evaluation of State of the Art Systems for Physical Activity Classification of Older Subjects Using Inertial Sensors in a Real Life Scenario: A Benchmark Study. Sensors 2016, 16, 2105. [Google Scholar] [CrossRef] [PubMed]
- Cheung, V.H.; Gray, L.; Karunanithi, M. Review of accelerometry for determining daily activity among elderly patients. Arch. Phys. Med. Rehabil. 2011, 92, 998–1014. [Google Scholar] [CrossRef] [PubMed]
- Gupta, P.; Dallas, T. Feature selection and activity recognition system using a single triaxial accelerometer. IEEE Trans. Biomed. Eng. 2014, 61, 1780–1786. [Google Scholar] [CrossRef] [PubMed]
- Papadopoulos, A.; Vivaldi, N.; Crump, C.; Silvers, C.T. Differentiating walking from other activities of daily living in older adults using wrist-based accelerometers. Curr. Aging Sci. 2015, 8, 266–275. [Google Scholar] [CrossRef] [PubMed]
- Weiss, A.; Brozgol, M.; Giladi, N.; Hausdorff, J.M. Can a single lower trunk body-fixed sensor differentiate between level-walking and stair descent and ascent in older adults? Preliminary findings. Med. Eng. Phys. 2016, 38, 1146–1151. [Google Scholar] [CrossRef] [PubMed]
- Pannurat, N.; Thiemjarus, S.; Nantajeewarawat, E.; Anantavrasilp, I. Analysis of Optimal Sensor Positions for Activity Classification and Application on a Different Data Collection Scenario. Sensors 2017, 17, 774. [Google Scholar] [CrossRef] [PubMed]
- Doughty, K.; Lewis, R.; McIntosh, A. The design of a practical and reliable fall detector for community and institutional telecare. J. Telemed. Telecare 2000, 6, 150–154. [Google Scholar] [CrossRef]
- Sazonov, E.S.; Hegde, N.; Tang, W. Development of SmartStep: An insole-based physical activity monitor. In Proceedings of the 2013 35th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Osaka, Japan, 3–7 July 2013; pp. 7209–7212. [Google Scholar]
- Saito, M.; Nakajima, K.; Takano, C.; Ohta, Y.; Sugimoto, C.; Ezoe, R.; Sasaki, K.; Hosaka, H.; Ifukube, T.; Ino, S.; et al. An in-shoe device to measure plantar pressure during daily human activity. Med. Eng. Phys. 2011, 33, 638–645. [Google Scholar] [CrossRef] [PubMed]
- Moschetti, A.; Fiorini, L.; Esposito, D.; Dario, P.; Cavallo, F. Recognition of Daily Gestures with Wearable Inertial Rings and Bracelets. Sensors 2016, 16, 1341. [Google Scholar] [CrossRef] [PubMed]
- Cates, B.; Sim, T.; Heo, H.M.; Kim, B.; Kim, H.; Mun, J.H. A novel detection model and its optimal features to classify falls from low-and high-acceleration activities of daily life using an insole sensor system. Sensors 2018, 18, 1227. [Google Scholar] [CrossRef] [PubMed]
- Troiano, R.P.; McClain, J.J.; Brychta, R.J.; Chen, K.Y. Evolution of accelerometer methods for physical activity research. Br. J. Sports Med. 2014, 48, 1019–1023. [Google Scholar] [CrossRef] [PubMed]
- Berlin, J.E.; Storti, K.L.; Brach, J.S. Using activity monitors to measure physical activity in free-living conditions. Phys. Ther. 2006, 86, 1137–1145. [Google Scholar] [PubMed]
- Innerd, P.; Harrison, R.; Coulson, M. Using open source accelerometer analysis to assess physical activity and sedentary behaviour in overweight and obese adults. BMC Public Health 2018, 18, 543. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.H.; Macfarlane, D.J.; Sobko, T. Feasibility of a Chest-worn accelerometer for physical activity measurement. J. Sci. Med. Sport 2016, 19, 1015–1019. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez, I.; Cajamarca, G.; Herskovic, V.; Fuentes, C.; Campos, M. Helping Elderly Users Report Pain Levels: A Study of User Experience with Mobile and Wearable Interfaces. Mob. Inf. Syst. 2017, 2017, 9302328. [Google Scholar] [CrossRef]
- Nag, A.; Mukhopadhyay, S.C.; Kosel, J. Wearable Flexible Sensors: A Review. IEEE Sens. J. 2017, 17, 3949–3960. [Google Scholar] [CrossRef]
- Cha, Y.; Nam, K.; Kim, D. Patient Posture Monitoring System Based on Flexible Sensors. Sensors 2017, 17, 584. [Google Scholar] [CrossRef] [PubMed]
- Feldhege, F.; Mau-Moeller, A.; Lindner, T.; Hein, A.; Markschies, A.; Zettl, U.K.; Bader, R. Accuracy of a custom physical activity and knee angle measurement sensor system for patients with neuromuscular disorders and gait abnormalities. Sensors 2015, 15, 10734–10752. [Google Scholar] [CrossRef] [PubMed]
- Massé, F.; Gonzenbach, R.R.; Arami, A.; Paraschiv-Ionescu, A.; Luft, A.R.; Aminian, K. Improving activity recognition using a wearable barometric pressure sensor in mobility-impaired stroke patients. J. Neuroeng. Rehabil. 2015, 12, 72. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Sohn, J.; Kim, S. Classification of Daily Activities for the Elderly Using Wearable Sensors. J. Healthc. Eng. 2017, 2017, 8934816. [Google Scholar] [CrossRef] [PubMed]
- Wu, A.Y.; Munteanu, C. Understanding Older Users’ Acceptance of Wearable Interfaces for Sensor-based Fall Risk Assessment. In Proceedings of the 2018 CHI Conference on Human Factors in Computing Systems, Montreal, QC, Canada, 21–26 April 2018; ACM: New York, NY, USA, 2018; pp. 119:1–119:13. [Google Scholar] [CrossRef]
- Stedmon, A.W.; Howells, H.; Wilson, J.R.; Dianat, I. Ergonomics/human factors needs of an ageing workforce in the manufacturing sector. Health Promot. Perspect. 2012, 2, 112–125. [Google Scholar]
- Hamine, S.; Gerth-Guyette, E.; Faulx, D.; Green, B.B.; Ginsburg, S.A. Impact of mHealth Chronic Disease Management on Treatment Adherence and Patient Outcomes: A Systematic Review. J. Med. Internet Res. 2015, 17, e52. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Luximon, Y. Older Adults and Digital Technology: A Study of User Perception and Usage Behavior. In Advances in Intelligent Systems and Computing, Proceedings of the AHFE 2016 International Conference on Physical Ergonomics and Human Factors, Walt Disney World, FL, USA, 27–31 July 2016; Springer: New York, NY, USA, 2016; Volume 489, pp. 155–163. [Google Scholar] [CrossRef]
- Hentschel, M.; Haaksma, M.; van de Belt, T. Wearable technology for the elderly: Underutilized solutions. Eur. Geriatr. Med. 2016, 7, 399–401. [Google Scholar] [CrossRef]
- Mikkonen, M.; Va, S.; Ikonen, V.; Heikkila, M. User and concept studies as tools in developing mobile communication services for the elderly. Pers. Ubiquitous Comput. 2002, 6, 113–124. [Google Scholar] [CrossRef]
- Attrakdiff. 2017. Available online: http://www.attrakdiff.de (accessed on 30 March 2017).
- Cajamarca, G.; Rodríguez, I.; Herskovic, V.; Campos, M. StraightenUp: Implementation and Evaluation of a Spine Posture Wearable. In Proceedings of the International Conference on Ubiquitous Computing and Ambient Intelligence, Philadelphia, PA, USA, 7–10 November 2017; Springer: New York, NY, USA, 2017; pp. 655–665. [Google Scholar]
- Lee, J.S.; Su, Y.W.; Shen, C.C. A comparative study of wireless protocols: Bluetooth, UWB, ZigBee, and Wi-Fi. In Proceedings of the IECON 2007 33rd Annual Conference of the IEEE Industrial Electronics Society, Taipei, Taiwan, 5–8 November 2007; pp. 46–51. [Google Scholar]
- Chatfield, A.B. Fundamentals of High Accuracy Inertial Navigation; American Institute of Aeronautics and Astronautics: Reston, VA, USA, 1997. [Google Scholar]
- Kim, A.; Golnaraghi, M. Initial calibration of an inertial measurement unit using an optical position tracking system. In Proceedings of the 2004 PLANS IEEE Position Location and Navigation Symposium, Monterey, CA, USA, 26–29 April 2004; pp. 96–101. [Google Scholar]
- Shin, E.H.; El-Sheimy, N. A new calibration method for strapdown inertial navigation systems. Z. Vermess 2002, 127, 1–10. [Google Scholar]
- Dwiputra, F.A.; Achmad, B. Accelerometer-Based Recorder of Fingers Dynamic Movements for Post-Stroke Rehabilitation. Int. J. Adv. Sci. Eng. Inf. Technol. 2017, 7, 299–304. [Google Scholar] [CrossRef]
- Luinge, H.J.; Veltink, P.H.; Baten, C.T. Estimation of orientation with gyroscopes and accelerometers. In Proceedings of the First Joint BMES/EMBS Conference 1999 IEEE Engineering in Medicine and Biology 21st Annual Conference and the 1999 Annual Fall Meetring of the Biomedical Engineering Society, Atlanta, GA, USA, 13–16 October 1999; Volume 2, p. 844. [Google Scholar]
- Ghanbari, M.; Yazdanpanah, M.J. Delay compensation of tilt sensors based on MEMS accelerometer using data fusion technique. IEEE Sens. J. 2015, 15, 1959–1966. [Google Scholar] [CrossRef]
- Herrera, M.; Fernández, B.; Rossel, J.; Rojas, M. Chile y Sus Mayores: 10 años de la Encuesta Calidad de Vida en la Vejez UC; Caja Los Andes: Santiago, Chile, 2017. [Google Scholar]
- Marín, P.P.; Guzmán, J.M.; Araya, A. Adultos Mayores institucionalizados en Chile: Cómo saber cuántos son? Rev. Méd. Chile 2004, 132, 832–838. [Google Scholar] [CrossRef] [PubMed]
- Ouslander, J.G. Medical care in the nursing home. JAMA 1989, 262, 2582–2590. [Google Scholar] [CrossRef] [PubMed]
- Diamond, T. Making Gray Gold: Narratives of Nursing Home Care; University of Chicago Press: Chicago, IL, USA, 2009. [Google Scholar]
- OECD Skills Studies. Skills Matter: Further Results from the Survey of Adult Skills; OECD Publishing: Paris, France, 2016. [Google Scholar] [CrossRef]
- Ferrari, A. Digital Competence in Practice: An Analysis of Frameworks; Technical Report; Research Centre of the European Commission: Ispra, Italy, 2012. [Google Scholar]
- Isleifsdottir, J.; Larusdottir, M. Measuring the user experience of a task oriented software. In Proceedings of the International Workshop on Meaningful Measures: Valid Useful User Experience Measurement, Reykjavik, Iceland, 18 June 2008; Institut de Recherche en Informatique de Toulouse: Toulouse, France, 2008; pp. 97–101. [Google Scholar]
- Gloth, F.; Walston, J.; Meyer, J.; Pearson, J. Reliability and validity of the Frail Elderly Functional Assessment questionnaire. Am. J. Phys. Med. Rehabil. 1995, 74, 45–53. [Google Scholar] [CrossRef] [PubMed]
- The R Project for Statistical. Available online: https://www.r-project.org/ (accessed on 1 October 2018).
- Weka. Available online: https://www.cs.waikato.ac.nz/ml/weka/ (accessed on 1 October 2018).
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Van Lummel, R.C.; Evers, J.; Niessen, M.; Beek, P.J.; van Dieën, J.H. Older Adults with Weaker Muscle Strength Stand up from a Sitting Position with More Dynamic Trunk Use. Sensors 2018, 18, 1235. [Google Scholar] [CrossRef] [PubMed]
- Scarborough, D.M.; McGibbon, C.A.; Krebs, D.E. Chair rise strategies in older adults with functional limitations. J. Rehabil. Res. Dev. 2007, 44, 33–42. [Google Scholar] [CrossRef] [PubMed]
- Gross, M.; Stevenson, P.; Charette, S.; Pyka, G.; Marcus, R. Effect of muscle strength and movement speed on the biomechanics of rising from a chair in healthy elderly and young women. Gait Posture 1998, 8, 175–185. [Google Scholar] [CrossRef]
- Ellis, K.; Kerr, J.; Godbole, S.; Lanckriet, G. Multi-sensor physical activity recognition in free-living. In Proceedings of the 2014 ACM International Joint Conference on Pervasive and Ubiquitous Computing: Adjunct Publication, Seattle, WA, USA, 13–17 September 2014; ACM: New York, NY, USA, 2014; pp. 431–440. [Google Scholar]
- He, B.; Bai, J.; Zipunnikov, V.V.; Koster, A.; Caserotti, P.; Lange-Maia, B.; Glynn, N.W.; Harris, T.B.; Crainiceanu, C.M. Predicting human movement with multiple accelerometers using movelets. Med. Sci. Sports Exerc. 2014, 46, 1859. [Google Scholar] [CrossRef] [PubMed]
- Chang, S.J.; Im, E.O. A path analysis of Internet health information seeking behaviors among older adults. Geriatr. Nurs. 2014, 35, 137–141. [Google Scholar] [CrossRef] [PubMed]
- Hsiao, C.H.; Tang, K.Y. Examining a model of mobile healthcare technology acceptance by the elderly in Taiwan. J. Glob. Inf. Technol. Manag. 2015, 18, 292–311. [Google Scholar] [CrossRef]
- Zamarrón Cassinello, M.; Fernandez Ballesteros, R. Satisfacción con la vida en personas mayores que viven en sus domicilios y en residencias: Factores determinantes. Rev. Esp. Geriatr. Gerontol. 2000, 35, 17–29. [Google Scholar]
- Fernández-Mayoralas, G.; Rojo-Pérez, F.; Martínez-Martín, P.; Prieto-Flores, M.E.; Rodríguez-Blázquez, C.; Martín-García, S.; Rojo-Abuín, J.M.; Forjaz, M.J. Active ageing and quality of life: Factors associated with participation in leisure activities among institutionalized older adults, with and without dementia. Aging Ment. Health 2015, 19, 1031–1041. [Google Scholar] [CrossRef] [PubMed]
- Salguero, A.; Martinez-Garcia, R.; Molinero, O.; Marquez, S. Physical activity, quality of life and symptoms of depression in community-dwelling and institutionalized older adults. Arch. Gerontol. Geriatr. 2011, 53, 152–157. [Google Scholar] [CrossRef] [PubMed]

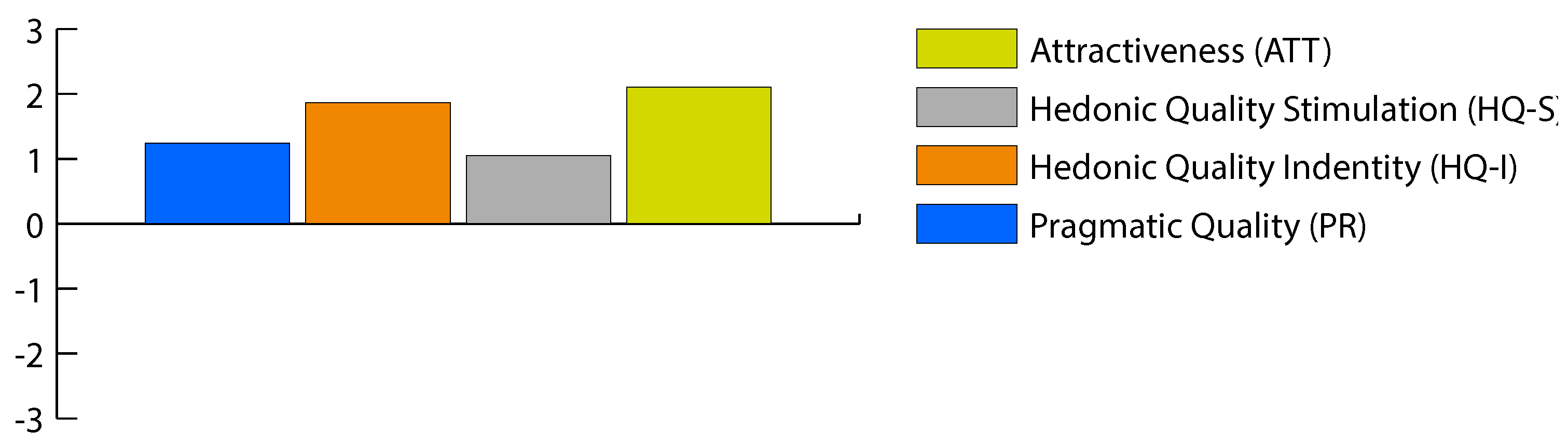
| Wlk | Tr1 | Lng | Sit | Rsn | Lwr | StU | Tr2 | TP Rate % | Precision % | |
|---|---|---|---|---|---|---|---|---|---|---|
| Wlk | 3158 | 6 | 25 | 6 | 4 | 3 | 4 | 3 | 98.4% | 93.1% |
| Tr1 | 43 | 289 | 2 | 41 | 1 | 0 | 2 | 9 | 74.7% | 85.8% |
| Lng | 60 | 2 | 772 | 0 | 10 | 5 | 3 | 0 | 90.6% | 93.1% |
| Sit | 34 | 12 | 5 | 1213 | 2 | 2 | 1 | 4 | 95.3% | 94.0% |
| Rsn | 12 | 3 | 14 | 1 | 709 | 9 | 16 | 0 | 92.8% | 95.1% |
| Lwr | 18 | 1 | 4 | 5 | 7 | 443 | 4 | 1 | 91.7% | 96.4% |
| StU | 18 | 1 | 5 | 2 | 9 | 2 | 882 | 0 | 96% | 90.3% |
| Tr2 | 49 | 23 | 2 | 23 | 5 | 2 | 3 | 159 | 59.8% | 93.5% |
| S1 | S2 | S3 | Correctly Classified Instances % |
|---|---|---|---|
| X | - | - | 73.7 % |
| - | X | - | 76.6 % |
| - | - | X | 76.8 % |
| X | X | - | 90.1 % |
| - | X | X | 90.1 % |
| X | - | X | 90.4 % |
| X | X | X | 93.5 % |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cajamarca, G.; Rodríguez, I.; Herskovic, V.; Campos, M.; Riofrío, J.C. StraightenUp+: Monitoring of Posture during Daily Activities for Older Persons Using Wearable Sensors. Sensors 2018, 18, 3409. https://doi.org/10.3390/s18103409
Cajamarca G, Rodríguez I, Herskovic V, Campos M, Riofrío JC. StraightenUp+: Monitoring of Posture during Daily Activities for Older Persons Using Wearable Sensors. Sensors. 2018; 18(10):3409. https://doi.org/10.3390/s18103409
Chicago/Turabian StyleCajamarca, Gabriela, Iyubanit Rodríguez, Valeria Herskovic, Mauricio Campos, and Juan Carlos Riofrío. 2018. "StraightenUp+: Monitoring of Posture during Daily Activities for Older Persons Using Wearable Sensors" Sensors 18, no. 10: 3409. https://doi.org/10.3390/s18103409
APA StyleCajamarca, G., Rodríguez, I., Herskovic, V., Campos, M., & Riofrío, J. C. (2018). StraightenUp+: Monitoring of Posture during Daily Activities for Older Persons Using Wearable Sensors. Sensors, 18(10), 3409. https://doi.org/10.3390/s18103409





