Assessment of Thyroid Carcinogenic Risk and Safety Profile of GLP1-RA Semaglutide (Ozempic) Therapy for Diabetes Mellitus and Obesity: A Systematic Literature Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol and Registration
2.2. Inclusion and Exclusion Criteria
2.3. Data Collection Process
2.4. Risk of Bias and Quality Assessment
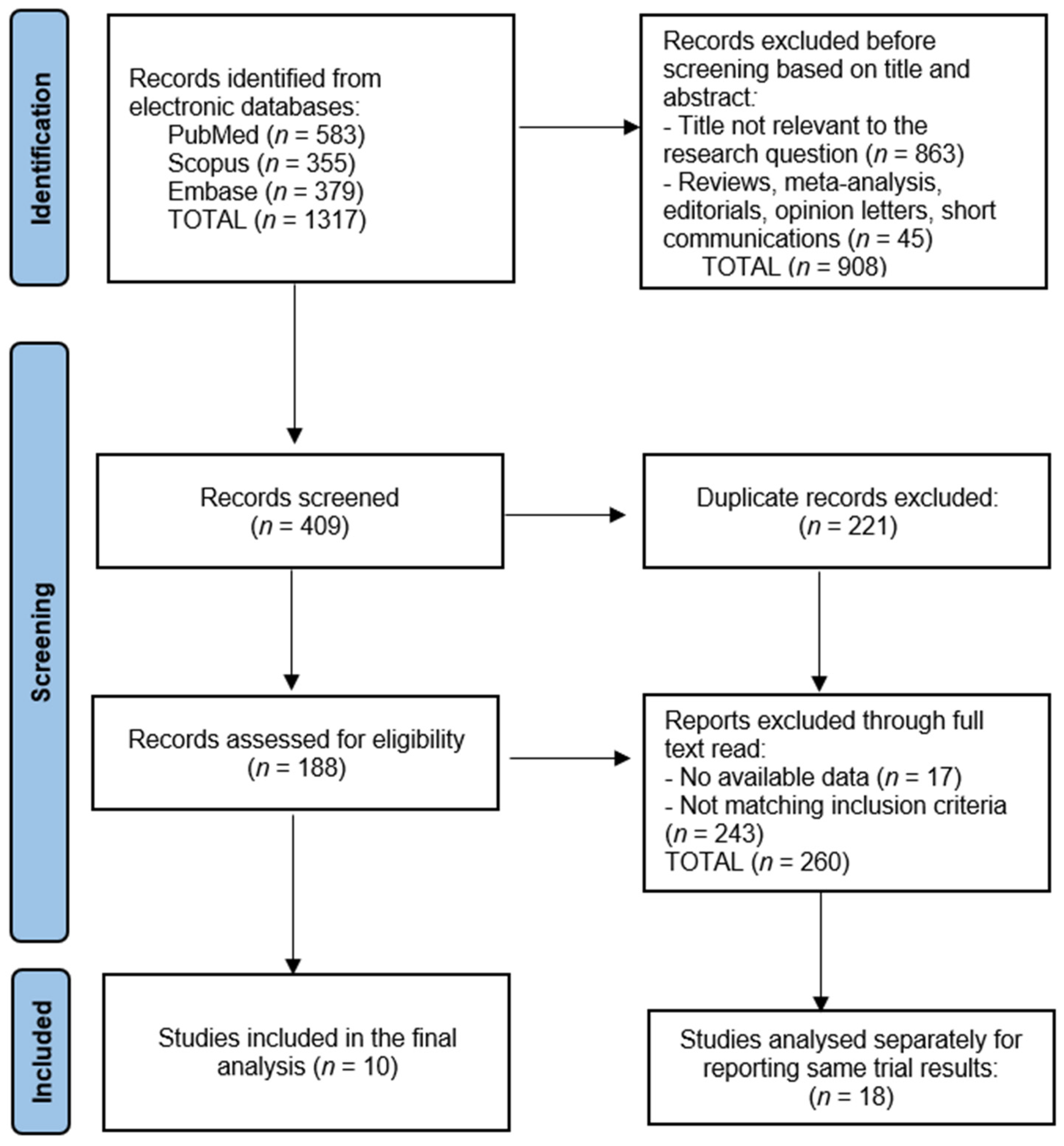
3. Results
3.1. Study Characteristics
3.2. Patients’ Characteristics
3.3. Weight and Glucose Levels
3.4. Thyroid Cancer Incidence and Complications
4. Discussion
4.1. Summary of Evidence
4.2. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Correction Statement
References
- O’Neill, E.S.; Wiegmann, A.L.; Parrella, N.; Pittman, T.; Hood, K.; Kurlander, D. Injectable Weight Loss Medications in Plastic Surgery: What We Know, Perioperative Considerations, and Recommendations for the Future. Plast. Reconstr. Surg. Glob. Open 2024, 12, e5516. [Google Scholar] [CrossRef]
- Constantino, A.K. Ozempic, Wegovy Drug Prescriptions Hit 9 Million, Surge 300% in under Three Years. CNBC. 2023. Available online: https://www.cnbc.com/2023/09/27/ozempic-wegovy-drug-prescriptions-hit-9-million.html (accessed on 14 October 2023).
- Lucas, A. Big Food vs. Big pharma: Companies Bet on Snacking Just as Weight Loss Drugs Boom. CNBC. 2023. Available online: https://www.cnbc.com/2023/10/01/kellanova-bets-on-snacking-as-ozempic-wegovy-take-off.html (accessed on 14 October 2023).
- Mahapatra, M.K.; Karuppasamy, M.; Sahoo, B.M. Semaglutide, a glucagon like peptide-1 receptor agonist with cardiovascular benefits for management of type 2 diabetes. Rev. Endocr. Metab. Disord. 2022, 23, 521–539. [Google Scholar] [CrossRef]
- Wojtara, M.; Mazumder, A.; Syeda, Y.; Mozgała, N. Glucagon-Like Peptide-1 Receptor Agonists for Chronic Weight Management. Adv. Med. 2023, 2023, 9946924. [Google Scholar] [CrossRef]
- Lombrea, A.; Romanescu, M.; Jianu, N.; Andor, M.; Suciu, M.; Man, D.E.; Danciu, C.; Dehelean, C.A.; Buda, V. Sex-Related Differences in the Pharmacological Response in SARS-CoV-2 Infection, Dyslipidemia, and Diabetes Mellitus: A Narrative Review. Pharmaceuticals 2023, 16, 853. [Google Scholar] [CrossRef]
- Hjerpsted, J.B.; Flint, A.; Brooks, A.; Axelsen, M.B.; Kvist, T.; Blundell, J. Semaglutide improves postprandial glucose and lipid metabolism, and delays first-hour gastric emptying in subjects with obesity. Diabetes Obes. Metab. 2018, 20, 610–619. [Google Scholar] [CrossRef]
- Mahapatra, M.K.; Karuppasamy, M.; Sahoo, B.M. Therapeutic Potential of Semaglutide, a Newer GLP-1 Receptor Agonist, in Abating Obesity, Non-Alcoholic Steatohepatitis and Neurodegenerative diseases: A Narrative Review. Pharm. Res. 2022, 39, 1233–1248. [Google Scholar] [CrossRef]
- Clinical Review Report: Semaglutide (Ozempic): (Novo Nordisk Canada Inc.): Indication: For the Treatment of Adult Patients with Type 2 Diabetes Mellitus to Improve Glycemic Control, in Combination with Metformin (Second-Line Treatment), and in Combination with Metformin and Sulfonylurea (Third-Line Treatment) [Internet]; Canadian Agency for Drugs and Technologies in Health: Ottawa, ON, USA, 2019. Available online: https://www.ncbi.nlm.nih.gov/books/NBK544016/ (accessed on 15 February 2024).
- Overgaard, R.V.; Hertz, C.L.; Ingwersen, S.H.; Navarria, A.; Drucker, D.J. Levels of circulating semaglutide determine reductions in HbA1c and body weight in people with type 2 diabetes. Cell Rep. Med. 2021, 2, 100387. [Google Scholar] [CrossRef]
- Shu, Y.; He, X.; Wu, P.; Liu, Y.; Ding, Y.; Zhang, Q. Gastrointestinal adverse events associated with semaglutide: A pharmacovigilance study based on FDA adverse event reporting system. Front. Public Health 2022, 10, 996179. [Google Scholar] [CrossRef]
- Enatescu, V.R.; Kalinovic, R.; Vlad, G.; Nussbaum, L.A.; Hogea, L.; Enatescu, I.; Marinescu, I.; Ifteni, P.; Simu, M.; Marian, C. The presence of peripheral inflammatory markers in patients with major depressive disorder, the associated symptoms profiles and the antidepressant efficacy of celecoxib. Farmacia 2020, 68, 483–491. [Google Scholar] [CrossRef]
- Lajthia, E.; Bucheit, J.D.; Nadpara, P.A.; Dixon, D.L.; Caldas, L.M.; Murchie, M.; Sisson, E.M. Combination therapy with once-weekly glucagon like peptide-1 receptor agonists and dipeptidyl peptidase-4 inhibitors in type 2 diabetes: A case series. Pharm. Pract. 2019, 17, 1588. [Google Scholar] [CrossRef]
- Jianu, C.; Rusu, L.C.; Muntean, I.; Cocan, I.; Lukinich-Gruia, A.T.; Goleț, I.; Horhat, D.; Mioc, M.; Mioc, A.; Șoica, C.; et al. In Vitro and In Silico Evaluation of the Antimicrobial and Antioxidant Potential of Thymus pulegioides Essential Oil. Antioxidants 2022, 11, 2472. [Google Scholar] [CrossRef]
- Yang, Z.; Lv, Y.; Yu, M.; Mei, M.; Xiang, L.; Zhao, S.; Li, R. GLP-1 receptor agonist-associated tumor adverse events: A real-world study from 2004 to 2021 based on FAERS. Front. Pharmacol. 2022, 13, 925377. [Google Scholar] [CrossRef]
- Smits, M.M.; Van Raalte, D.H. Safety of Semaglutide. Front. Endocrinol. 2021, 12, 645563, Erratum in Front. Endocrinol. 2021, 12, 786732. [Google Scholar] [CrossRef]
- Bjerre Knudsen, L.; Madsen, L.W.; Andersen, S.; Almholt, K.; de Boer, A.S.; Drucker, D.J.; Gotfredsen, C.; Egerod, F.L.; Hegelund, A.C.; Jacobsen, H.; et al. Glucagon-like Peptide-1 receptor agonists activate rodent thyroid C-cells causing calcitonin release and C-cell proliferation. Endocrinology. 2010, 151, 1473–1486. [Google Scholar] [CrossRef]
- Thompson, C.A.; Stürmer, T. Putting GLP-1 RAs and Thyroid Cancer in Context: Additional Evidence and Remaining Doubts. Diabetes Care 2023, 46, 249–251. [Google Scholar] [CrossRef]
- Vemula, H.; Villanueva, F.S.; Nguyen, H.D.; Mohan, A.; Potluri, S. Medullary Carcinoma of Thyroid Due to GLP-1 Receptor Agonist. J. Endocr. Soc. 2021, 5 (Suppl. 1), A893. [Google Scholar] [CrossRef]
- Chao, A.M.; Tronieri, J.S.; Amaro, A.; Wadden, T.A. Clinical Insight on Semaglutide for Chronic Weight Management in Adults: Patient Selection and Special Considerations. Drug Des. Devel. Ther. 2022, 16, 4449–4461. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Syst. Rev. 2021, 10, 89. [Google Scholar] [CrossRef]
- Stang, A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur. J. Epidemiol. 2010, 25, 603–605. [Google Scholar] [CrossRef]
- Ahrén, B.; Masmiquel, L.; Kumar, H.; Sargin, M.; Karsbøl, J.D.; Jacobsen, S.H.; Chow, F. Efficacy and safety of once-weekly semaglutide versus once-daily sitagliptin as an add-on to metformin, thiazolidinediones, or both, in patients with type 2 diabetes (SUSTAIN 2): A 56-week, double-blind, phase 3a, randomised trial. Lancet Diabetes Endocrinol. 2017, 5, 341–354. [Google Scholar] [CrossRef]
- Buse, J.B.; Bode, B.W.; Mertens, A.; Cho, Y.M.; Christiansen, E.; Hertz, C.L.; Nielsen, M.A.; Pieber, T.R.; PIONEER 7 investigators. Long-term efficacy and safety of oral semaglutide and the effect of switching from sitagliptin to oral semaglutide in patients with type 2 diabetes: A 52-week, randomized, open-label extension of the PIONEER 7 trial. BMJ Open Diabetes Res. Care 2020, 8, e001649. [Google Scholar] [CrossRef]
- Husain, M.; Birkenfeld, A.L.; Donsmark, M.; Dungan, K.; Eliaschewitz, F.G.; Franco, D.R.; Jeppesen, O.K.; Lingvay, I.; Mosenzon, O.; Pedersen, S.D.; et al. Oral Semaglutide and Cardiovascular Outcomes in Patients with Type 2 Diabetes. N. Engl. J. Med. 2019, 381, 841–851. [Google Scholar] [CrossRef]
- Marso, S.P.; Bain, S.C.; Consoli, A.; Eliaschewitz, F.G.; Jódar, E.; Leiter, L.A.; Lingvay, I.; Rosenstock, J.; Seufert, J.; Warren, M.L.; et al. Semaglutide and Cardiovascular Outcomes in Patients with Type 2 Diabetes. N. Engl. J. Med. 2016, 375, 1834–1844. [Google Scholar] [CrossRef]
- Pratley, R.; Amod, A.; Hoff, S.T.; Kadowaki, T.; Lingvay, I.; Nauck, M.; Pedersen, K.B.; Saugstrup, T.; Meier, J.J.; PIONEER 4 investigators. Oral semaglutide versus subcutaneous liraglutide and placebo in type 2 diabetes (PIONEER 4): A randomised, double-blind, phase 3a trial. Lancet 2019, 394, 39–50, Erratum in Lancet 2019, 394, e1.. [Google Scholar] [CrossRef]
- Rosenstock, J.; Allison, D.; Birkenfeld, A.L.; Blicher, T.M.; Deenadayalan, S.; Jacobsen, J.B.; Serusclat, P.; Violante, R.; Watada, H.; Davies, M.; et al. Effect of Additional Oral Semaglutide vs Sitagliptin on Glycated Hemoglobin in Adults with Type 2 Diabetes Uncontrolled with Metformin Alone or with Sulfonylurea: The PIONEER 3 Randomized Clinical Trial. JAMA 2019, 321, 1466–1480. [Google Scholar] [CrossRef]
- Sorli, C.; Harashima, S.I.; Tsoukas, G.M.; Unger, J.; Karsbøl, J.D.; Hansen, T.; Bain, S.C. Efficacy and safety of once-weekly semaglutide monotherapy versus placebo in patients with type 2 diabetes (SUSTAIN 1): A double-blind, randomised, placebo-controlled, parallel-group, multinational, multicentre phase 3a trial. Lancet Diabetes Endocrinol. 2017, 5, 251–260. [Google Scholar] [CrossRef]
- Wadden, T.A.; Bailey, T.S.; Billings, L.K.; Davies, M.; Frias, J.P.; Koroleva, A.; Lingvay, I.; O’Neil, P.M.; Rubino, D.M.; Skovgaard, D.; et al. Effect of Subcutaneous Semaglutide vs Placebo as an Adjunct to Intensive Behavioral Therapy on Body Weight in Adults with Overweight or Obesity: The STEP 3 Randomized Clinical Trial. JAMA 2021, 325, 1403–1413. [Google Scholar] [CrossRef]
- Wilding, J.P.H.; Batterham, R.L.; Davies, M.; Van Gaal, L.F.; Kandler, K.; Konakli, K.; Lingvay, I.; McGowan, B.M.; Oral, T.K.; Rosenstock, J.; et al. Weight regain and cardiometabolic effects after withdrawal of semaglutide: The STEP 1 trial extension. Diabetes Obes. Metab. 2022, 24, 1553–1564. [Google Scholar] [CrossRef]
- Yamada, Y.; Katagiri, H.; Hamamoto, Y.; Deenadayalan, S.; Navarria, A.; Nishijima, K.; Seino, Y. PIONEER 9 investigators. Dose-response, efficacy, and safety of oral semaglutide monotherapy in Japanese patients with type 2 diabetes (PIONEER 9): A 52-week, phase 2/3a, randomised, controlled trial. Lancet Diabetes Endocrinol. 2020, 8, 377–391. [Google Scholar] [CrossRef] [PubMed]
- Aroda, V.R.; Rosenstock, J.; Terauchi, Y.; Altuntas, Y.; Lalic, N.M.; Morales Villegas, E.C.; Jeppesen, O.K.; Christiansen, E.; Hertz, C.L.; Haluzík, M.; et al. PIONEER 1: Randomized Clinical Trial of the Efficacy and Safety of Oral Semaglutide Monotherapy in Comparison with Placebo in Patients with Type 2 Diabetes. Diabetes Care 2019, 42, 1724–1732. [Google Scholar] [CrossRef] [PubMed]
- Mosenzon, O.; Blicher, T.M.; Rosenlund, S.; Eriksson, J.W.; Heller, S.; Hels, O.H.; Pratley, R.; Sathyapalan, T.; Desouza, C.; PIONEER 5 Investigators. Efficacy and safety of oral semaglutide in patients with type 2 diabetes and moderate renal impairment (PIONEER 5): A placebo-controlled, randomised, phase 3a trial. Lancet Diabetes Endocrinol. 2019, 7, 515–527, Erratum in Lancet Diabetes Endocrinol. 2019, 7, e21. [Google Scholar] [CrossRef] [PubMed]
- Zinman, B.; Aroda, V.R.; Buse, J.B.; Cariou, B.; Harris, S.B.; Hoff, S.T.; Pedersen, K.B.; Tarp-Johansen, M.J.; Araki, E.; PIONEER 8 Investigators. Efficacy, Safety, and Tolerability of Oral Semaglutide Versus Placebo Added to Insulin with or without Metformin in Patients with Type 2 Diabetes: The PIONEER 8 Trial. Diabetes Care 2019, 42, 2262–2271. [Google Scholar] [CrossRef] [PubMed]
- Davies, M.; Færch, L.; Jeppesen, O.K.; Pakseresht, A.; Pedersen, S.D.; Perreault, L.; Rosenstock, J.; Shimomura, I.; Viljoen, A.; Wadden, T.A.; et al. Semaglutide 2·4 mg once a week in adults with overweight or obesity, and type 2 diabetes (STEP 2): A randomised, double-blind, double-dummy, placebo-controlled, phase 3 trial. Lancet 2021, 397, 971–984. [Google Scholar] [CrossRef] [PubMed]
- Loomba, R.; Abdelmalek, M.F.; Armstrong, M.J.; Jara, M.; Kjær, M.S.; Krarup, N.; Lawitz, E.; Ratziu, V.; Sanyal, A.J.; Schattenberg, J.M.; et al. Semaglutide 2·4 mg once weekly in patients with non-alcoholic steatohepatitis-related cirrhosis: A randomised, placebo-controlled phase 2 trial. Lancet Gastroenterol. Hepatol. 2023, 8, 511–522. [Google Scholar] [CrossRef] [PubMed]
- Rubino, D.; Abrahamsson, N.; Davies, M.; Hesse, D.; Greenway, F.L.; Jensen, C.; Lingvay, I.; Mosenzon, O.; Rosenstock, J.; Rubio, M.A.; et al. Effect of Continued Weekly Subcutaneous Semaglutide vs Placebo on Weight Loss Maintenance in Adults with Overweight or Obesity: The STEP 4 Randomized Clinical Trial. JAMA 2021, 325, 1414–1425. [Google Scholar] [CrossRef] [PubMed]
- Garvey, W.T.; Batterham, R.L.; Bhatta, M.; Buscemi, S.; Christensen, L.N.; Frias, J.P.; Jódar, E.; Kandler, K.; Rigas, G.; Wadden, T.A.; et al. Two-year effects of semaglutide in adults with overweight or obesity: The STEP 5 trial. Nat. Med. 2022, 28, 2083–2091. [Google Scholar] [CrossRef] [PubMed]
- Kadowaki, T.; Isendahl, J.; Khalid, U.; Lee, S.Y.; Nishida, T.; Ogawa, W.; Tobe, K.; Yamauchi, T.; Lim, S.; STEP 6 investigators. Semaglutide once a week in adults with overweight or obesity, with or without type 2 diabetes in an east Asian population (STEP 6): A randomised, double-blind, double-dummy, placebo-controlled, phase 3a trial. Lancet Diabetes Endocrinol. 2022, 10, 193–206. [Google Scholar] [CrossRef]
- Weghuber, D.; Barrett, T.; Barrientos-Pérez, M.; Gies, I.; Hesse, D.; Jeppesen, O.K.; Kelly, A.S.; Mastrandrea, L.D.; Sørrig, R.; Arslanian, S.; et al. Once-Weekly Semaglutide in Adolescents with Obesity. N. Engl. J. Med. 2022, 387, 2245–2257. [Google Scholar] [CrossRef]
- Newsome, P.N.; Buchholtz, K.; Cusi, K.; Linder, M.; Okanoue, T.; Ratziu, V.; Sanyal, A.J.; Sejling, A.S.; Harrison, S.A.; NN9931-4296 Investigators. A Placebo-Controlled Trial of Subcutaneous Semaglutide in Nonalcoholic Steatohepatitis. N. Engl. J. Med. 2021, 384, 1113–1124. [Google Scholar] [CrossRef]
- O’Neil, P.M.; Birkenfeld, A.L.; McGowan, B.; Mosenzon, O.; Pedersen, S.D.; Wharton, S.; Carson, C.G.; Jepsen, C.H.; Kabisch, M.; Wilding, J.P.H. Efficacy and safety of semaglutide compared with liraglutide and placebo for weight loss in patients with obesity: A randomised, double-blind, placebo and active controlled, dose-ranging, phase 2 trial. Lancet. 2018, 392, 637–649. [Google Scholar] [CrossRef]
- Lingvay, I.; Catarig, A.M.; Frias, J.P.; Kumar, H.; Lausvig, N.L.; le Roux, C.W.; Thielke, D.; Viljoen, A.; McCrimmon, R.J. Efficacy and safety of once-weekly semaglutide versus daily canagliflozin as add-on to metformin in patients with type 2 diabetes (SUSTAIN 8): A double-blind, phase 3b, randomised controlled trial. Lancet Diabetes Endocrinol. 2019, 7, 834–844. [Google Scholar] [CrossRef] [PubMed]
- Frías, J.P.; Davies, M.J.; Rosenstock, J.; Pérez Manghi, F.C.; Fernández Landó, L.; Bergman, B.K.; Liu, B.; Cui, X.; Brown, K.; SURPASS-2 Investigators. Tirzepatide versus Semaglutide Once Weekly in Patients with Type 2 Diabetes. N. Engl. J. Med. 2021, 385, 503–515. [Google Scholar] [CrossRef] [PubMed]
- Capehorn, M.S.; Catarig, A.M.; Furberg, J.K.; Janez, A.; Price, H.C.; Tadayon, S.; Vergès, B.; Marre, M. Efficacy and safety of once-weekly semaglutide 1.0mg vs once-daily liraglutide 1.2mg as add-on to 1-3 oral antidiabetic drugs in subjects with type 2 diabetes (SUSTAIN 10). Diabetes Metab. 2020, 46, 100–109. [Google Scholar] [CrossRef]
- Kellerer, M.; Kaltoft, M.S.; Lawson, J.; Nielsen, L.L.; Strojek, K.; Tabak, Ö.; Jacob, S. Effect of once-weekly semaglutide versus thrice-daily insulin aspart, both as add-on to metformin and optimized insulin glargine treatment in participants with type 2 diabetes (SUSTAIN 11): A randomized, open-label, multinational, phase 3b trial. Diabetes Obes. Metab. 2022, 24, 1788–1799. [Google Scholar] [CrossRef] [PubMed]
- Ji, L.; Dong, X.; Li, Y.; Li, Y.; Lim, S.; Liu, M.; Ning, Z.; Rasmussen, S.; Skjøth, T.V.; Yuan, G.; et al. Efficacy and safety of once-weekly semaglutide versus once-daily sitagliptin as add-on to metformin in patients with type 2 diabetes in SUSTAIN China: A 30-week, double-blind, phase 3a, randomized trial. Diabetes Obes. Metab. 2021, 23, 404–414. [Google Scholar] [CrossRef]
- Kaku, K.; Yamada, Y.; Watada, H.; Abiko, A.; Nishida, T.; Zacho, J.; Kiyosue, A. Safety and efficacy of once-weekly semaglutide vs additional oral antidiabetic drugs in Japanese people with inadequately controlled type 2 diabetes: A randomized trial. Diabetes Obes. Metab. 2018, 20, 1202–1212. [Google Scholar] [CrossRef] [PubMed]
- Nagendra, L.; Bg, H.; Sharma, M.; Dutta, D. Semaglutide and cancer: A systematic review and meta-analysis. Diabetes Metab. Syndr. 2023, 17, 102834. [Google Scholar] [CrossRef] [PubMed]
- Silverii, G.A.; Monami, M.; Gallo, M.; Ragni, A.; Prattichizzo, F.; Renzelli, V.; Ceriello, A.; Mannucci, E. Glucagon-like peptide-1 receptor agonists and risk of thyroid cancer: A systematic review and meta-analysis of randomized controlled trials. Diabetes Obes. Metab. 2024, 26, 891–900. [Google Scholar] [CrossRef]
- Bezin, J.; Gouverneur, A.; Pénichon, M.; Mathieu, C.; Garrel, R.; Hillaire-Buys, D.; Pariente, A.; Faillie, J.L. GLP-1 Receptor Agonists and the Risk of Thyroid Cancer. Diabetes Care 2023, 46, 384–390. [Google Scholar] [CrossRef]
- Schmid, D.; Ricci, C.; Behrens, G.; Leitzmann, M.F. Adiposity and risk of thyroid cancer: A systematic review and meta-analysis. Obes. Rev. 2015, 16, 1042–1054. [Google Scholar] [CrossRef]
- Hu, W.; Song, R.; Cheng, R.; Liu, C.; Guo, R.; Tang, W.; Zhang, J.; Zhao, Q.; Li, X.; Liu, J. Use of GLP-1 Receptor Agonists and Occurrence of Thyroid Disorders: A Meta-Analysis of Randomized Controlled Trials. Front. Endocrinol. 2022, 13, 927859. [Google Scholar] [CrossRef] [PubMed]
- Brubaker, P.L. Minireview: Update on incretin biology: Focus on glucagon-like peptide-1. Endocrinology 2010, 151, 1984–1989. [Google Scholar] [CrossRef] [PubMed]
- European Medicines Agency. Meeting Highlights from the Pharmacovigilance Risk Assessment Committee (PRAC) 23–26 October 2023. EMA. 27 October 2023. Available online: https://www.ema.europa.eu/en/news/meeting-highlights-pharmacovigilance-risk-assessment-committee-prac-23-26-october-2023 (accessed on 15 February 2024).
| Study & Author | Country | YOP | Study Design | Quality of Evidence |
|---|---|---|---|---|
| 1 [23] Ahrén et al. | Multi-national | 2017 | RCT SUSTAIN 2 DB—Phase IIIa | High |
| 2 [24] Buse et al. | Multi-national | 2020 | RCT PIONEER 7 Open-label extension | High |
| 3 [25] Husain et al. | Multi-national | 2019 | RCT PIONEER 6 Phase IIIa | High |
| 4 [26] Marso et al. | Multi-national | 2016 | RCT SUSTAIN 6 DB—Phase III | High |
| 5 [27] Pratley et al. | Multi-national | 2019 | RCT PIONEER 4 Phase IIIa | High |
| 6 [28] Rosenstock et al. | Multi-national | 2019 | RCT PIONEER 3 DB—Phase IIIa | High |
| 7 [29] Sorli et al. | Multi-national | 2017 | RCT SUSTAIN 1 DB—Phase IIIa | High |
| 8 [30] Wadden et al. | United States | 2021 | RCT Phase III | High |
| 9 [31] Wilding et al. | Multi-national | 2022 | RCT STEP 1 DB | High |
| 10 [32] Yamada et al. | Multi-national | 2020 | RCT PIONEER 9 DB—Phase II/IIIa | High |
| Study Number | Sample Size | Age (Years) | Gender (Male) | Comparison Group | Disease Duration |
|---|---|---|---|---|---|
| 1 [23] Ahrén et al. | Semaglutide 0.5 mg: 409, Semaglutide 1.0 mg: 409 | Semaglutide 0.5 mg: 54.8, Semaglutide 1.0 mg: 56.0, Sitagliptin: 54.6 | Semaglutide 0.5 mg: 51%, Semaglutide 1.0 mg: 50%, Sitagliptin: 51% | Sitagliptin 100 mg: 407 | Semaglutide 0.5 mg: 6.4 years, Semaglutide 1.0 mg: 6.7 years, Sitagliptin: 6.6 years |
| 2 [24] Buse et al. | Oral Semaglutide: 100 | Oral Semaglutide: 58, Sitagliptin: 58 | Oral Semaglutide: 43.0%, Sitagliptin: 43.9% | Sitagliptin: 98 | Oral Semaglutide: 8.1 years, Sitagliptin: 9.6 years |
| 3 [25] Husain et al. | Oral Semaglutide: 1591 | Mean: 66 | 68.1% | Placebo: 1592 | Semaglutide: 14.7 years, Placebo: 15.1 years |
| 4 [26] Marso et al. | Subcutaneous Semaglutide: 1648 (0.5 mg: 826, 1.0 mg: 822) | Semaglutide 0.5 mg: 64.6, Semaglutide 1.0 mg: 64.7 | 34.1% | Placebo: 1649 | Semaglutide: 14.2 years, Placebo: 13.6 years |
| 5 [27] Pratley et al. | Oral Semaglutide 14 mg: 285, Liraglutide 1.8 mg: 284 | Semaglutide: 56, Liraglutide: 56 | Oral Semaglutide: 52%, Liraglutide: 52% | Placebo: 142 | Semaglutide: 7.8 years, Liraglutide: 7.3 years, Placebo: 7.8 years |
| 6 [28] Rosenstock et al. | Oral Semaglutide: 1396 (3 mg: 466, 7 mg: 466, 14 mg: 465), Sitagliptin: 467 | Oral Semaglutide: Mean 58, Sitagliptin: Mean 58 | Oral Semaglutide: 53.1%, Sitagliptin: 51.0% | Sitagliptin 100 mg: 467 | Oral Semaglutide: Mean 8.6 years, Sitagliptin: Mean 8.8 years |
| 7 [29] Sorli et al. | Semaglutide: 258 | Semaglutide: 53.7, Placebo: 53.9 | Semaglutide: 54%, Placebo: 54% | Placebo: 129 | Semaglutide: 4.18 years, Placebo: 4.06 years |
| 8 [30] Wadden et al. | Semaglutide: 407 | Mean: 46 | Semaglutide: 22.6%, Placebo: 11.8% | Placebo: 204 | NR |
| 9 [31] Wilding et al. | Semaglutide: 1306 | Mean: 46 | Semaglutide: 26.9%, Placebo: 24.0% | Placebo: 655 | NR |
| 10 [32] Yamada et al. | Oral Semaglutide 3 mg: 49, 7 mg: 49, 14 mg: 48 | Semaglutide: 60, Placebo: 59, Liraglutide: 59 | Semaglutide: 76.3%, Placebo: 82%, Liraglutide: 81% | Placebo: 49, Liraglutide: 48 | Semaglutide: 7.6 years, Placebo: 8.4 years, Liraglutide 6.7 |
| Study Number | Follow-Up | Dose | HbA1c/Fasting Glucose | Weight (Initial, Weight Change) |
|---|---|---|---|---|
| 1 [23] Ahrén et al. | 56 weeks | Semaglutide: 0.5 mg, 1.0 mg; Sitagliptin: 100 mg | Semaglutide: −1.3% (0.5 mg), −1.6% (1.0 mg); Sitagliptin: −0.5% | Initial: 89.5 kg; Change: −4.3 kg (Semaglutide 0.5 mg), −6.1 kg (Semaglutide 1.0 mg), −1.9 kg (Sitagliptin) |
| 2 [24] Buse et al. | 52 weeks | Oral semaglutide: flexible dose (0.5–1 mg); sitagliptin: 100 mg | Oral Semaglutide: −0.2%; Sitagliptin: +0.1% | Initial: 85.8 kg (Oral Semaglutide), 86.9 kg (Sitagliptin); Change: −2.4 kg (Oral Semaglutide), −0.9 kg (Sitagliptin) |
| 3 [25] Husain et al. | 15.9 months | Oral semaglutide: 14 mg target dose | Baseline: 8.2 ± 1.6% HbA1c; decrease: oral semaglutide −1.0%, placebo −0.3% | Initial: 90.9 ± 21.2 kg; Change: −4.2 kg (Oral Semaglutide) |
| 4 [26] Marso et al. | 104 weeks | Semaglutide subcutaneous: 0.5 mg, 1.0 mg | Baseline HbA1c 8.7%; reduction: −1.1% (0.5 mg), −1.4% (1.0 mg) | Initial: 92.1 kg; Change: −3.6 kg (0.5 mg), −4.9 kg (1.0 mg) |
| 5 [27] Pratley et al. | 52 weeks | Oral semaglutide (escalated to 14 mg), liraglutide (escalated to 1.8 mg), placebo | HbA1c: Oral semaglutide: −1.2%, liraglutide: −1.1%, placebo: −0.2% | Initial: 94.0 kg; Change: Oral semaglutide: −4.4 kg, Liraglutide: −3.1 kg, Placebo: −0.5 kg |
| 6 [28] Rosenstock et al. | 78 weeks | Oral semaglutide (3 mg, 7 mg, 14 mg), sitagliptin 100 mg | Oral semaglutide: decrease in HbA1c −0.6% (3 mg), −1.0% (7 mg), −1.3% (14 mg); sitagliptin: decrease in HbA1c −0.8% | Oral Semaglutide: Initial 91.2 kg, Weight change −1.2 kg (3 mg), −2.2 kg (7 mg), −3.1 kg (14 mg), Sitagliptin: Initial 90.9 kg, Weight change −0.6 kg |
| 7 [29] Sorli et al. | 30 weeks | Semaglutide (0.5 mg, 1.0 mg), placebo | Semaglutide: −1.5% (1.0 mg), −1.45% (0.5 mg) vs. placebo: −0.02% | Semaglutide: −4.53 kg (1.0 mg), −3.73 kg (0.5 mg) vs. Placebo: −0.98 kg |
| 8 [30] Wadden et al. | 68 weeks | Semaglutide subcutaneous 2.4 mg | Fasting plasma glucose: semaglutide (−6.73 mg/dL), placebo (−0.65 mg/dL) | Weight loss: Semaglutide:(−16.0%), Placebo: (−5.7%) |
| 9 [31] Wilding et al. | 68 weeks (main phase) + 52 weeks (extension) | Semaglutide subcutaneous 2.4 mg once weekly | Reversion to normal blood glucose levels at 120 weeks: semaglutide (43.3%), placebo (34.0%) | By week 68: Semaglutide: 17.3%, Placebo: 2.0%. Regain by week 120: Semaglutide: 11.6%, Placebo: 1.9%. Net loss from baseline to week 120: Semaglutide: 5.6%, Placebo: 0.1% |
| 10 [32] Yamada et al. | 52 weeks | Oral semaglutide (3 mg, 7 mg, 14 mg), liraglutide 0.9 mg | Baseline HbA1c: 8.3% across all groups. Significant reductions compared to placebo: −1.1% for 3 mg, −1.5% for 7 mg, and −1.7% for 14 mg | Baseline weight 71.1 kg. Significantly more patients achieved a weight loss reduction of 5.0% or greater with oral semaglutide 14 mg than those who received placebo or liraglutide at both weeks 26 and 52 |
| Risk Factors | Thyroid Cancer | Adverse Events | Major Side Complications | Conclusions |
|---|---|---|---|---|
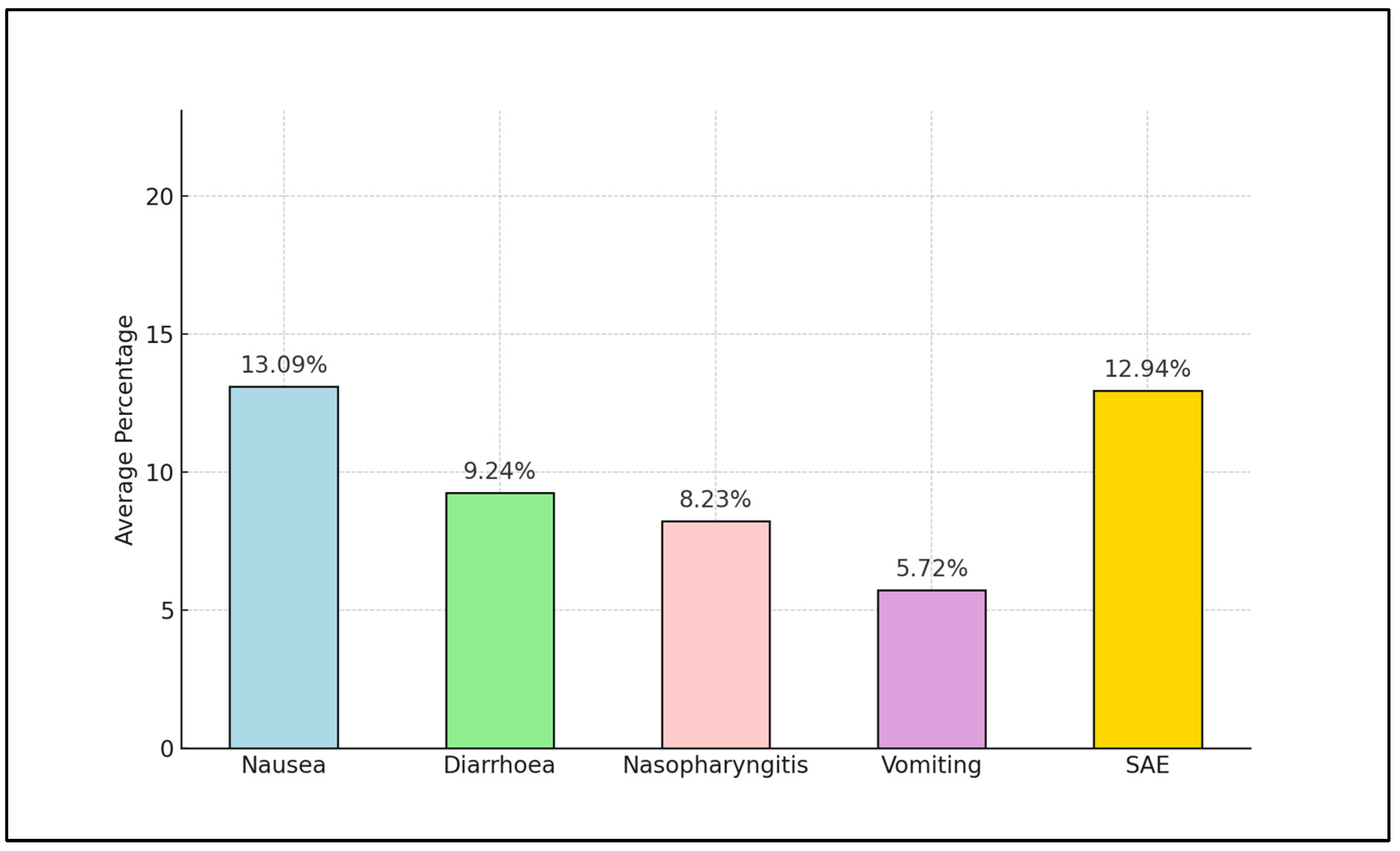
| 1 [23] Ahrén et al. | PTC: 1 patient (<1%) in the 1.0 mg group OR: 1.50–NS | Nausea: 18%, diarrhea: 13%, nasopharyngitis: 9.5%, vomiting: 9%, lipase increased: 8%, headache: 6.5%, decreased appetite: 7%, influenza: 4.5%, dyspepsia: 5.5%, constipation: 5% | Severe hypoglycemia: 33, pancreatitis: 2 | Once-weekly semaglutide superior to Sitagliptin in glycemic control and weight reduction for diabetes patients on metformin, thiazolidinediones, or both. Safety profile similar to other GLP-1 receptor agonists. No significant risk for thyroid cancer. |
| 2 [24] Buse et al. | Thyroid cancer: 0% | Nausea: 19.95%, nasopharyngitis: 10.2%, diarrhea: 10.75%, headache: 7.75%, abdominal pain, upper: 6.95%, dyspepsia: 5.55%, vomiting: 7.05%, upper respiratory tract infection: 4.05%, arthralgia: 4.85%, back pain: 4.85%, influenza: 5.95%, gastroenteritis: 4.05%, constipation: 4.65% | SAE: 9.1% for oral semaglutide, 8.0% after sitagliptin switched to semaglutide | Long-term oral semaglutide treatment maintained HbA1c reductions with additional body weight reductions. Switching from sitagliptin to oral semaglutide maintained HbA1c reductions with potential for additional weight loss. No significant risk for thyroid cancer. |
| 3 [25] Husain et al. | MTC: 1 patient (<1%) | Nausea: 2.9% (oral semaglutide group), 0.5% (placebo group); Vomiting: 1.5% (oral semaglutide), 0.3% (placebo); Diarrhea: 1.4% (oral semaglutide), 0.4% (placebo) | SAE: 18.9% (oral semaglutide) vs. 22.5% (placebo). Deaths lower in the oral semaglutide group (1.4%) compared to placebo (2.8%) | Cardiovascular risk profile of oral semaglutide not inferior to placebo in type 2 diabetes patients. No significant risk for thyroid cancer. |
| 4 [26] Marso et al. | MTC: 0% | Adverse event leading to discontinuation: 13%, nausea: 3.4%, vomiting: 2.25%, diarrhea: 2.05%, gastrointestinal disorder: 51.5%, cardiac disorder: 19.55%, atrial fibrillation: 3.05% | SAE: 24.2% (semaglutide 0.5 mg), 25.2% (semaglutide 1.0 mg), placebo: 26.2% (0.5 mg) vs. 23.5% (1.0 mg) | Semaglutide significantly reduced primary composite cardiovascular outcome compared to placebo in high cardiovascular risk type 2 diabetes patients. No significant risk for thyroid cancer. |
| 5 [27] Pratley et al. | Thyroid cancer: 0% | GI adverse events: oral semaglutide (80%), liraglutide (74%), placebo (67%). Hypoglycemic episodes: oral semaglutide (1%), liraglutide (2%), placebo (2%) | Nausea: oral semaglutide (20%), liraglutide (18%). Diarrhea: oral semaglutide (15%), liraglutide (11%). Vomiting: oral semaglutide (9%). Early discontinuation due to adverse events: semaglutide (11%), liraglutide (9%), placebo (4%) | Oral semaglutide demonstrated non-inferiority to subcutaneous liraglutide and superiority to placebo in reducing HbA1c and body weight. The safety and tolerability profile was consistent with the GLP-1 receptor agonist class, predominantly gastrointestinal events. No significant risk for thyroid cancer. |
| 6 [28] Rosenstock et al. | Thyroid cancer: 0% | Nausea: semaglutide (11–20%), sitagliptin (6.5%). Diarrhea: semaglutide (9.7–10.6%), sitagliptin (6.4%). Hypoglycemia: semaglutide 3 mg (4.9%), 7 mg (5.2%), 14 mg (7.7%); sitagliptin (8.4%) | Symptomatic hypoglycemia: 3 mg/d (4.9%), 7 mg/d (5.2%), and 14 mg/d (7.7%); and in the sitagliptin group (8.4%). SAE: semaglutide 3 mg (10.1%), 7 mg (8.0%), and 14 mg (8.6%) | Oral semaglutide at 7 mg and 14 mg resulted in significantly greater reductions in HbA1c compared to sitagliptin over 26 weeks, with the 3 mg dosage showing no significant benefit over sitagliptin. The safety profile was consistent with expectations for the class. No significant risk for thyroid cancer. |
| 7 [29] Sorli et al. | Thyroid cancer: 0% | Nausea: 22%, diarrhea: 12%, headache: 9.5%, lipase increased: 5%, constipation: 5%, dyspepsia: 4.5%, nasopharyngitis: 5%, vomiting: 5.5% | SAE: semaglutide 0.5 mg (7%), 1.0 mg (6%), placebo (3%) | Semaglutide significantly improved HbA1c and body weight in treatment-naive patients with type 2 diabetes compared to placebo. The safety profile was consistent with the GLP-1 receptor agonist class, with no significant risk for thyroid cancer. |
| 8 [30] Wadden et al. | PTC: 1 patient (<1%) | Gastrointestinal adverse events: semaglutide (82.8%) vs. placebo (63.2%). Discontinuation due to adverse events: semaglutide (3.4%) vs. placebo (0%) | SAE: semaglutide (9.1%), placebo (2.9%) | Semaglutide, combined with intensive behavioral therapy and initial low-calorie diet, led to a significantly greater weight loss compared to placebo over 68 weeks in adults with overweight or obesity, with no significant risk for thyroid cancer. |
| 9 [31] Wilding et al. | Thyroid cancer: 0% | NR | NR | After the withdrawal of semaglutide and lifestyle intervention, participants regained a significant portion of the weight they had lost, highlighting the chronic nature of obesity and the need for ongoing treatment to maintain weight loss and health improvements. No significant risk for thyroid cancer. |
| 10 [32] Yamada et al. | Thyroid cancer: 1 patient in the oral semaglutide 7 mg | Constipation: semaglutide (10–13%), placebo (6%), liraglutide (19%). Nausea: semaglutide (7.5%), placebo (8%), liraglutide (2%) | SAE: semaglutide all dosages (3.4%), placebo (6%), liraglutide (0%) | Oral semaglutide significantly reduces HbA1c and induces weight loss in a dose-dependent manner in patients with T2DM, with a safety profile consistent with GLP-1 receptor agonists. No significant risk for thyroid cancer. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Feier, C.V.I.; Vonica, R.C.; Faur, A.M.; Streinu, D.R.; Muntean, C. Assessment of Thyroid Carcinogenic Risk and Safety Profile of GLP1-RA Semaglutide (Ozempic) Therapy for Diabetes Mellitus and Obesity: A Systematic Literature Review. Int. J. Mol. Sci. 2024, 25, 4346. https://doi.org/10.3390/ijms25084346
Feier CVI, Vonica RC, Faur AM, Streinu DR, Muntean C. Assessment of Thyroid Carcinogenic Risk and Safety Profile of GLP1-RA Semaglutide (Ozempic) Therapy for Diabetes Mellitus and Obesity: A Systematic Literature Review. International Journal of Molecular Sciences. 2024; 25(8):4346. https://doi.org/10.3390/ijms25084346
Chicago/Turabian StyleFeier, Catalin Vladut Ionut, Razvan Constantin Vonica, Alaviana Monique Faur, Diana Raluca Streinu, and Calin Muntean. 2024. "Assessment of Thyroid Carcinogenic Risk and Safety Profile of GLP1-RA Semaglutide (Ozempic) Therapy for Diabetes Mellitus and Obesity: A Systematic Literature Review" International Journal of Molecular Sciences 25, no. 8: 4346. https://doi.org/10.3390/ijms25084346
APA StyleFeier, C. V. I., Vonica, R. C., Faur, A. M., Streinu, D. R., & Muntean, C. (2024). Assessment of Thyroid Carcinogenic Risk and Safety Profile of GLP1-RA Semaglutide (Ozempic) Therapy for Diabetes Mellitus and Obesity: A Systematic Literature Review. International Journal of Molecular Sciences, 25(8), 4346. https://doi.org/10.3390/ijms25084346








