Molecular Targets of Novel Therapeutics for Diabetic Kidney Disease: A New Era of Nephroprotection
Abstract
1. Introduction
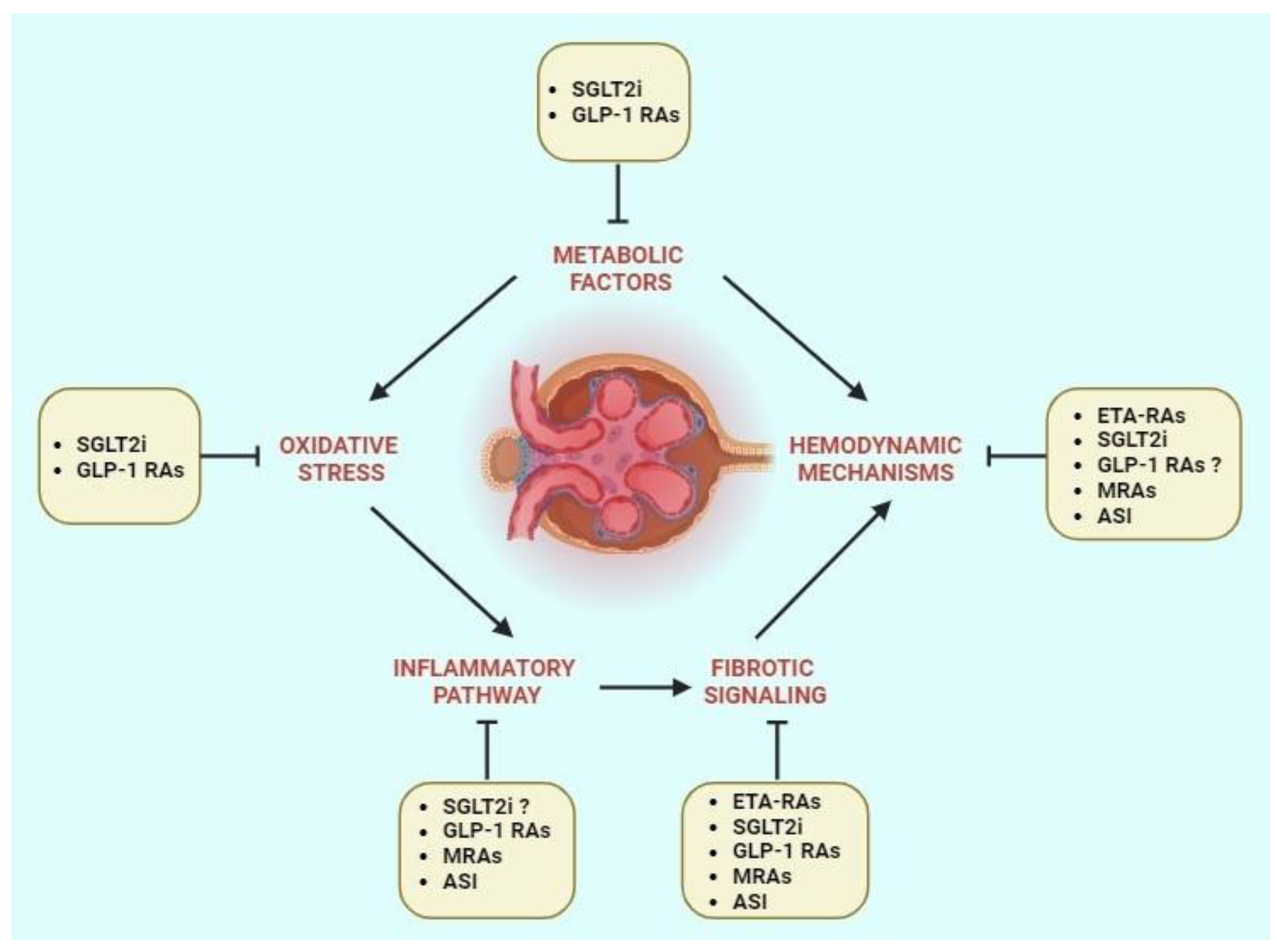
2. Molecular Mechanisms of DKD
2.1. Metabolic Factors
2.2. Oxidative Stress
2.3. Inflammatory Pathway
2.4. Fibrotic Signaling
2.5. Hemodynamic Mechanisms
3. Therapeutic Options for DKD
3.1. RAAS Blockers
3.2. Mineralcorticoid Receptor Antagonists
3.3. SGLT2 Inhibitors
3.4. Glucagon-like Peptide-1 Receptor Agonists
3.5. Endothelin Receptor Antagonists
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kim, M.K.; Kim, D.M. Current status of diabetic kidney disease and latest trends in management. J. Diabetes Investig. 2022, 13, 1961–1962. [Google Scholar] [CrossRef]
- Song, J.; Ni, J.; Yin, X. The genetic side of diabetic kidney disease: A review. Int. Urol. Nephrol. 2023, 55, 335–343. [Google Scholar] [CrossRef] [PubMed]
- Lassen, E.; Daehn, I.S. Molecular Mechanisms in Early Diabetic Kidney Disease: Glomerular Endothelial Cell Dysfunction. Int. J. Mol. Sci. 2020, 21, 9456. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Jin, M.; Cheng, C.K.; Li, Q. Tubular injury in diabetic kidney disease: Molecular mechanisms and potential therapeutic perspectives. Front. Endocrinol. 2023, 14, 1238927. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, K.; Sato, E.; Mishima, E.; Miyazaki, M.; Tanaka, T. What’s New in the Molecular Mechanisms of Diabetic Kidney Disease: Recent Advances. Int. J. Mol. Sci. 2022, 24, 570. [Google Scholar] [CrossRef] [PubMed]
- Lambers Heerspink, H.J.; Oberbauer, R.; Perco, P.; Heinzel, A.; Heinze, G.; Mayer, G.; Mayer, B. Drugs meeting the molecular basis of diabetic kidney disease: Bridging from molecular mechanism to personalized medicine. Nephrol. Dial. Transpl. 2015, 30 (Suppl. 4), iv105–iv112. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Tuttle, K.R.; Agarwal, R.; Alpers, C.E.; Bakris, G.L.; Brosius, F.C.; Kolkhof, P.; Uribarri, J. Molecular mechanisms and therapeutic targets for diabetic kidney disease. Kidney Int. 2022, 102, 248–260. [Google Scholar] [CrossRef] [PubMed]
- Naaman, S.C.; Bakris, G.L. Diabetic Nephropathy: Update on Pillars of Therapy Slowing Progression. Diabetes Care 2023, 46, 1574–1586. [Google Scholar] [CrossRef] [PubMed]
- Verma, S.; Pandey, A.; Pandey, A.K.; Butler, J.; Lee, J.S.; Teoh, H.; Mazer, C.D.; Kosiborod, M.N.; Cosentino, F.; Anker, S.D.; et al. Aldosterone and aldosterone synthase inhibitors in cardiorenal disease. Am. J. Physiol. Heart Circ. Physiol. 2024, 326, H670–H688. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Diaz, I.; Martos, N.; Llorens-Cebria, C.; Alvarez, F.J.; Bedard, P.W.; Vergara, A.; Jacobs-Cacha, C.; Soler, M.J. Endothelin Receptor Antagonists in Kidney Disease. Int. J. Mol. Sci. 2023, 24, 3427. [Google Scholar] [CrossRef] [PubMed]
- de Zeeuw, D.; Heerspink, H.J.L. Time for clinical decision support systems tailoring individual patient therapy to improve renal and cardiovascular outcomes in diabetes and nephropathy. Nephrol. Dial. Transpl. 2020, 35, ii38–ii42. [Google Scholar] [CrossRef] [PubMed]
- Davies, M.J.; Aroda, V.R.; Collins, B.S.; Gabbay, R.A.; Green, J.; Maruthur, N.M.; Rosas, S.E.; Del Prato, S.; Mathieu, C.; Mingrone, G.; et al. Management of Hyperglycemia in Type 2 Diabetes, 2022. A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 2022, 45, 2753–2786. [Google Scholar] [CrossRef] [PubMed]
- Rossing, P.; Caramori, M.L.; Chan, J.C.N.; Heerspink, H.J.L.; Hurst, C.; Khunti, K.; Liew, A.; Michos, E.D.; Navaneethan, S.D.; Olowu, W.A.; et al. Executive summary of the KDIGO 2022 Clinical Practice Guideline for Diabetes Management in Chronic Kidney Disease: An update based on rapidly emerging new evidence. Kidney Int. 2022, 102, 990–999. [Google Scholar] [CrossRef] [PubMed]
- Su, W.; Cao, R.; He, Y.C.; Guan, Y.F.; Ruan, X.Z. Crosstalk of Hyperglycemia and Dyslipidemia in Diabetic Kidney Disease. Kidney Dis. 2017, 3, 171–180. [Google Scholar] [CrossRef] [PubMed]
- Mather, A.; Pollock, C. Glucose handling by the kidney. Kidney Int. Suppl. 2011, 79, S1–S6. [Google Scholar] [CrossRef]
- Wright, E.M.; Ghezzi, C.; Loo, D.D.F. Novel and Unexpected Functions of SGLTs. Physiology 2017, 32, 435–443. [Google Scholar] [CrossRef]
- Palm, F.; Cederberg, J.; Hansell, P.; Liss, P.; Carlsson, P.O. Reactive oxygen species cause diabetes-induced decrease in renal oxygen tension. Diabetologia 2003, 46, 1153–1160. [Google Scholar] [CrossRef] [PubMed]
- Matoba, K.; Takeda, Y.; Nagai, Y.; Kanazawa, Y.; Kawanami, D.; Yokota, T.; Utsunomiya, K.; Nishimura, R. ROCK Inhibition May Stop Diabetic Kidney Disease. JMA J. 2020, 3, 154–163. [Google Scholar] [CrossRef] [PubMed]
- Murea, M.; Freedman, B.I.; Parks, J.S.; Antinozzi, P.A.; Elbein, S.C.; Ma, L. Lipotoxicity in diabetic nephropathy: The potential role of fatty acid oxidation. Clin. J. Am. Soc. Nephrol. 2010, 5, 2373–2379. [Google Scholar] [CrossRef]
- Matoba, K.; Takeda, Y.; Nagai, Y.; Yokota, T.; Utsunomiya, K.; Nishimura, R. Targeting Redox Imbalance as an Approach for Diabetic Kidney Disease. Biomedicines 2020, 8, 40. [Google Scholar] [CrossRef]
- Wan, C.; Su, H.; Zhang, C. Role of NADPH Oxidase in Metabolic Disease-Related Renal Injury: An Update. Oxid. Med. Cell. Longev. 2016, 2016, 7813072. [Google Scholar] [CrossRef] [PubMed]
- Toth-Manikowski, S.; Atta, M.G. Diabetic Kidney Disease: Pathophysiology and Therapeutic Targets. J. Diabetes Res. 2015, 2015, 697010. [Google Scholar] [CrossRef] [PubMed]
- Akamine, T.; Takaku, S.; Suzuki, M.; Niimi, N.; Yako, H.; Matoba, K.; Kawanami, D.; Utsunomiya, K.; Nishimura, R.; Sango, K. Glycolaldehyde induces sensory neuron death through activation of the c-Jun N-terminal kinase and p-38 MAP kinase pathways. Histochem. Cell. Biol. 2020, 153, 111–119. [Google Scholar] [CrossRef] [PubMed]
- Inagi, R. Organelle Stress and Metabolic Derangement in Kidney Disease. Int. J. Mol. Sci. 2022, 23, 1723. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, Y.; Doi, T.; Kato, I.; Shinohara, H.; Sakurai, S.; Yonekura, H.; Watanabe, T.; Myint, K.M.; Harashima, A.; Takeuchi, M.; et al. Receptor for advanced glycation end products is a promising target of diabetic nephropathy. Ann. N Y Acad. Sci. 2005, 1043, 562–566. [Google Scholar] [CrossRef] [PubMed]
- Wan, S.; Wan, S.; Jiao, X.; Cao, H.; Gu, Y.; Yan, L.; Zheng, Y.; Niu, P.; Shao, F. Advances in understanding the innate immune-associated diabetic kidney disease. FASEB J. 2021, 35, e21367. [Google Scholar] [CrossRef] [PubMed]
- Pichler, R.; Afkarian, M.; Dieter, B.P.; Tuttle, K.R. Immunity and inflammation in diabetic kidney disease: Translating mechanisms to biomarkers and treatment targets. Am. J. Physiol. Renal. Physiol. 2017, 312, F716–F731. [Google Scholar] [CrossRef] [PubMed]
- Rayego-Mateos, S.; Morgado-Pascual, J.L.; Opazo-Rios, L.; Guerrero-Hue, M.; Garcia-Caballero, C.; Vazquez-Carballo, C.; Mas, S.; Sanz, A.B.; Herencia, C.; Mezzano, S.; et al. Pathogenic Pathways and Therapeutic Approaches Targeting Inflammation in Diabetic Nephropathy. Int. J. Mol. Sci. 2020, 21, 3798. [Google Scholar] [CrossRef]
- Hofherr, A.; Williams, J.; Gan, L.M.; Soderberg, M.; Hansen, P.B.L.; Woollard, K.J. Targeting inflammation for the treatment of Diabetic Kidney Disease: A five-compartment mechanistic model. BMC Nephrol. 2022, 23, 208. [Google Scholar] [CrossRef] [PubMed]
- Bulow, R.D.; Boor, P. Extracellular Matrix in Kidney Fibrosis: More Than Just a Scaffold. J. Histochem. Cytochem. 2019, 67, 643–661. [Google Scholar] [CrossRef] [PubMed]
- Turner-Stokes, T.; Garcia Diaz, A.; Pinheiro, D.; Prendecki, M.; McAdoo, S.P.; Roufosse, C.; Cook, H.T.; Pusey, C.D.; Woollard, K.J. Live Imaging of Monocyte Subsets in Immune Complex-Mediated Glomerulonephritis Reveals Distinct Phenotypes and Effector Functions. J. Am. Soc. Nephrol. 2020, 31, 2523–2542. [Google Scholar] [CrossRef] [PubMed]
- Kornete, M.; Mason, E.S.; Piccirillo, C.A. Immune Regulation in T1D and T2D: Prospective Role of Foxp3+ Treg Cells in Disease Pathogenesis and Treatment. Front. Endocrinol. 2013, 4, 76. [Google Scholar] [CrossRef] [PubMed]
- Qi, R.; Yang, C. Renal tubular epithelial cells: The neglected mediator of tubulointerstitial fibrosis after injury. Cell Death Dis. 2018, 9, 1126. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Wang, H.L.; Liu, T.T.; Lan, H.Y. TGF-Beta as a Master Regulator of Diabetic Nephropathy. Int. J. Mol. Sci. 2021, 22, 7881. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.; Chen, X.C.; Li, Z.H.; Wu, H.L.; Jing, K.P.; Huang, X.R.; Ye, L.; Wei, B.; Lan, H.Y.; Liu, H.F. SMAD3 promotes autophagy dysregulation by triggering lysosome depletion in tubular epithelial cells in diabetic nephropathy. Autophagy 2021, 17, 2325–2344. [Google Scholar] [CrossRef] [PubMed]
- Hong, Q.; Zhang, L.; Fu, J.; Verghese, D.A.; Chauhan, K.; Nadkarni, G.N.; Li, Z.; Ju, W.; Kretzler, M.; Cai, G.Y.; et al. LRG1 Promotes Diabetic Kidney Disease Progression by Enhancing TGF-beta-Induced Angiogenesis. J. Am. Soc. Nephrol. 2019, 30, 546–562. [Google Scholar] [CrossRef] [PubMed]
- Lytvyn, Y.; Bjornstad, P.; van Raalte, D.H.; Heerspink, H.L.; Cherney, D.Z.I. The New Biology of Diabetic Kidney Disease-Mechanisms and Therapeutic Implications. Endocr. Rev. 2020, 41, 202–231. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Xue, S.; Hou, J.; Chen, G.; Xu, Z.G. Endothelin receptor antagonists for the treatment of diabetic nephropathy: A meta-analysis and systematic review. World J. Diabetes 2020, 11, 553–566. [Google Scholar] [CrossRef] [PubMed]
- Sorokin, A. Endothelin signaling and actions in the renal mesangium. Contrib. Nephrol. 2011, 172, 50–62. [Google Scholar] [CrossRef]
- Klemis, V.; Ghura, H.; Federico, G.; Wurfel, C.; Bentmann, A.; Gretz, N.; Miyazaki, T.; Grone, H.J.; Nakchbandi, I.A. Circulating fibronectin contributes to mesangial expansion in a murine model of type 1 diabetes. Kidney Int. 2017, 91, 1374–1385. [Google Scholar] [CrossRef] [PubMed]
- Toda, N.; Mukoyama, M.; Yanagita, M.; Yokoi, H. CTGF in kidney fibrosis and glomerulonephritis. Inflamm. Regen. 2018, 38, 14. [Google Scholar] [CrossRef] [PubMed]
- Alicic, R.Z.; Rooney, M.T.; Tuttle, K.R. Diabetic Kidney Disease: Challenges, Progress, and Possibilities. Clin. J. Am. Soc. Nephrol. 2017, 12, 2032–2045. [Google Scholar] [CrossRef] [PubMed]
- Vallon, V.; Thomson, S.C. The tubular hypothesis of nephron filtration and diabetic kidney disease. Nat. Rev. Nephrol. 2020, 16, 317–336. [Google Scholar] [CrossRef] [PubMed]
- Tuttle, K.R. Back to the Future: Glomerular Hyperfiltration and the Diabetic Kidney. Diabetes 2017, 66, 14–16. [Google Scholar] [CrossRef] [PubMed]
- Malek, V.; Suryavanshi, S.V.; Sharma, N.; Kulkarni, Y.A.; Mulay, S.R.; Gaikwad, A.B. Potential of Renin-Angiotensin-Aldosterone System Modulations in Diabetic Kidney Disease: Old Players to New Hope! Rev. Physiol. Biochem. Pharmacol. 2021, 179, 31–71. [Google Scholar] [CrossRef] [PubMed]
- Singh, R.; Singh, A.K.; Leehey, D.J. A novel mechanism for angiotensin II formation in streptozotocin-diabetic rat glomeruli. Am. J. Physiol. Renal. Physiol. 2005, 288, F1183–F1190. [Google Scholar] [CrossRef] [PubMed]
- Whaley-Connell, A.; Habibi, J.; Nistala, R.; Cooper, S.A.; Karuparthi, P.R.; Hayden, M.R.; Rehmer, N.; DeMarco, V.G.; Andresen, B.T.; Wei, Y.; et al. Attenuation of NADPH oxidase activation and glomerular filtration barrier remodeling with statin treatment. Hypertension 2008, 51, 474–480. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ilatovskaya, D.V.; Blass, G.; Palygin, O.; Levchenko, V.; Pavlov, T.S.; Grzybowski, M.N.; Winsor, K.; Shuyskiy, L.S.; Geurts, A.M.; Cowley, A.W., Jr.; et al. A NOX4/TRPC6 Pathway in Podocyte Calcium Regulation and Renal Damage in Diabetic Kidney Disease. J. Am. Soc. Nephrol. 2018, 29, 1917–1927. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.C.; Chang, Y.H.; Yang, S.Y.; Wu, K.D.; Chu, T.S. Update of pathophysiology and management of diabetic kidney disease. J. Formos. Med. Assoc. 2018, 117, 662–675. [Google Scholar] [CrossRef] [PubMed]
- Ritz, E.; Tomaschitz, A. Aldosterone, a vasculotoxic agent--novel functions for an old hormone. Nephrol. Dial. Transpl. 2009, 24, 2302–2305. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Kim, D.L.; Lee, S.E.; Kim, N.H. Renal Protection of Mineralocorticoid Receptor Antagonist, Finerenone, in Diabetic Kidney Disease. Endocrinol. Metab. 2023, 38, 43–55. [Google Scholar] [CrossRef] [PubMed]
- Heerspink, H.J.; Perkins, B.A.; Fitchett, D.H.; Husain, M.; Cherney, D.Z. Sodium Glucose Cotransporter 2 Inhibitors in the Treatment of Diabetes Mellitus: Cardiovascular and Kidney Effects, Potential Mechanisms, and Clinical Applications. Circulation 2016, 134, 752–772. [Google Scholar] [CrossRef] [PubMed]
- Lewis, E.J.; Hunsicker, L.G.; Bain, R.P.; Rohde, R.D. The effect of angiotensin-converting-enzyme inhibition on diabetic nephropathy. The Collaborative Study Group. N. Engl. J. Med. 1993, 329, 1456–1462. [Google Scholar] [CrossRef] [PubMed]
- Brenner, B.M.; Cooper, M.E.; de Zeeuw, D.; Keane, W.F.; Mitch, W.E.; Parving, H.H.; Remuzzi, G.; Snapinn, S.M.; Zhang, Z.; Shahinfar, S.; et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N. Engl. J. Med. 2001, 345, 861–869. [Google Scholar] [CrossRef] [PubMed]
- Lewis, E.J.; Hunsicker, L.G.; Clarke, W.R.; Berl, T.; Pohl, M.A.; Lewis, J.B.; Ritz, E.; Atkins, R.C.; Rohde, R.; Raz, I.; et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N. Engl. J. Med. 2001, 345, 851–860. [Google Scholar] [CrossRef] [PubMed]
- Barnett, A.H.; Bain, S.C.; Bouter, P.; Karlberg, B.; Madsbad, S.; Jervell, J.; Mustonen, J.; Diabetics Exposed to Telmisartan and Enalapril Study Group. Angiotensin-receptor blockade versus converting-enzyme inhibition in type 2 diabetes and nephropathy. N. Engl. J. Med. 2004, 351, 1952–1961. [Google Scholar] [CrossRef] [PubMed]
- Bakris, G.; Burgess, E.; Weir, M.; Davidai, G.; Koval, S.; Investigators, A.S. Telmisartan is more effective than losartan in reducing proteinuria in patients with diabetic nephropathy. Kidney Int. 2008, 74, 364–369. [Google Scholar] [CrossRef] [PubMed]
- Bakris, G.L.; Agarwal, R.; Anker, S.D.; Pitt, B.; Ruilope, L.M.; Rossing, P.; Kolkhof, P.; Nowack, C.; Schloemer, P.; Joseph, A.; et al. Effect of Finerenone on Chronic Kidney Disease Outcomes in Type 2 Diabetes. N. Engl. J. Med. 2020, 383, 2219–2229. [Google Scholar] [CrossRef] [PubMed]
- Perkovic, V.; Jardine, M.J.; Neal, B.; Bompoint, S.; Heerspink, H.J.L.; Charytan, D.M.; Edwards, R.; Agarwal, R.; Bakris, G.; Bull, S.; et al. Canagliflozin and Renal Outcomes in Type 2 Diabetes and Nephropathy. N. Engl. J. Med. 2019, 380, 2295–2306. [Google Scholar] [CrossRef] [PubMed]
- Heerspink, H.J.L.; Stefansson, B.V.; Correa-Rotter, R.; Chertow, G.M.; Greene, T.; Hou, F.F.; Mann, J.F.E.; McMurray, J.J.V.; Lindberg, M.; Rossing, P.; et al. Dapagliflozin in Patients with Chronic Kidney Disease. N. Engl. J. Med. 2020, 383, 1436–1446. [Google Scholar] [CrossRef] [PubMed]
- Herrington, W.G.; Staplin, N.; Wanner, C.; Green, J.B.; Hauske, S.J.; Emberson, J.R.; Preiss, D.; Judge, P.; Mayne, K.J.; Ng, S.Y.A.; et al. Empagliflozin in Patients with Chronic Kidney Disease. N. Engl. J. Med. 2023, 388, 117–127. [Google Scholar] [CrossRef] [PubMed]
- Rossing, P.; Baeres, F.M.M.; Bakris, G.; Bosch-Traberg, H.; Gislum, M.; Gough, S.C.L.; Idorn, T.; Lawson, J.; Mahaffey, K.W.; Mann, J.F.E.; et al. The rationale, design and baseline data of FLOW, a kidney outcomes trial with once-weekly semaglutide in people with type 2 diabetes and chronic kidney disease. Nephrol. Dial. Transpl. 2023, 38, 2041–2051. [Google Scholar] [CrossRef] [PubMed]
- Mann, J.F.; Green, D.; Jamerson, K.; Ruilope, L.M.; Kuranoff, S.J.; Littke, T.; Viberti, G.; Group, A.S. Avosentan for overt diabetic nephropathy. J. Am. Soc. Nephrol. 2010, 21, 527–535. [Google Scholar] [CrossRef] [PubMed]
- Heerspink, H.J.L.; Parving, H.H.; Andress, D.L.; Bakris, G.; Correa-Rotter, R.; Hou, F.F.; Kitzman, D.W.; Kohan, D.; Makino, H.; McMurray, J.J.V.; et al. Atrasentan and renal events in patients with type 2 diabetes and chronic kidney disease (SONAR): A double-blind, randomised, placebo-controlled trial. Lancet 2019, 393, 1937–1947. [Google Scholar] [CrossRef] [PubMed]
- Heerspink, H.J.L.; Kiyosue, A.; Wheeler, D.C.; Lin, M.; Wijkmark, E.; Carlson, G.; Mercier, A.K.; Astrand, M.; Ueckert, S.; Greasley, P.J.; et al. Zibotentan in combination with dapagliflozin compared with dapagliflozin in patients with chronic kidney disease (ZENITH-CKD): A multicentre, randomised, active-controlled, phase 2b, clinical trial. Lancet 2023, 402, 2004–2017. [Google Scholar] [CrossRef] [PubMed]
- Tuttle, K.R.; Hauske, S.J.; Canziani, M.E.; Caramori, M.L.; Cherney, D.; Cronin, L.; Heerspink, H.J.L.; Hugo, C.; Nangaku, M.; Rotter, R.C.; et al. Efficacy and safety of aldosterone synthase inhibition with and without empagliflozin for chronic kidney disease: A randomised, controlled, phase 2 trial. Lancet 2024, 403, 379–390. [Google Scholar] [CrossRef] [PubMed]
- Gansevoort, R.T.; de Zeeuw, D.; de Jong, P.E. ACE inhibitors and proteinuria. Pharm. World Sci. 1996, 18, 204–210. [Google Scholar] [CrossRef]
- Ontarget Investigators; Yusuf, S.; Teo, K.K.; Pogue, J.; Dyal, L.; Copland, I.; Schumacher, H.; Dagenais, G.; Sleight, P.; Anderson, C. Telmisartan, ramipril, or both in patients at high risk for vascular events. N. Engl. J. Med. 2008, 358, 1547–1559. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J.B.; Bress, A.P. Entering a New Era of Antihypertensive Therapy. Am. J. Kidney Dis. 2023, 83, 411–414. [Google Scholar] [CrossRef] [PubMed]
- Cruz-Lopez, E.O.; Ye, D.; Wu, C.; Lu, H.S.; Uijl, E.; Mirabito Colafella, K.M.; Danser, A.H.J. Angiotensinogen Suppression: A New Tool to Treat Cardiovascular and Renal Disease. Hypertension 2022, 79, 2115–2126. [Google Scholar] [CrossRef] [PubMed]
- Desai, A.S.; Webb, D.J.; Taubel, J.; Casey, S.; Cheng, Y.; Robbie, G.J.; Foster, D.; Huang, S.A.; Rhyee, S.; Sweetser, M.T.; et al. Zilebesiran, an RNA Interference Therapeutic Agent for Hypertension. N. Engl. J. Med. 2023, 389, 228–238. [Google Scholar] [CrossRef] [PubMed]
- Bakris, G.L.; Saxena, M.; Gupta, A.; Chalhoub, F.; Lee, J.; Stiglitz, D.; Makarova, N.; Goyal, N.; Guo, W.; Zappe, D.; et al. RNA Interference with Zilebesiran for Mild to Moderate Hypertension: The KARDIA-1 Randomized Clinical Trial. JAMA 2024, 331, 740. [Google Scholar] [CrossRef] [PubMed]
- Touyz, R.M. Silencing Angiotensinogen in Hypertension. N. Engl. J. Med. 2023, 389, 278–281. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, R.; Kolkhof, P.; Bakris, G.; Bauersachs, J.; Haller, H.; Wada, T.; Zannad, F. Steroidal and non-steroidal mineralocorticoid receptor antagonists in cardiorenal medicine. Eur. Heart. J. 2021, 42, 152–161. [Google Scholar] [CrossRef] [PubMed]
- Amazit, L.; Le Billan, F.; Kolkhof, P.; Lamribet, K.; Viengchareun, S.; Fay, M.R.; Khan, J.A.; Hillisch, A.; Lombes, M.; Rafestin-Oblin, M.E.; et al. Finerenone Impedes Aldosterone-dependent Nuclear Import of the Mineralocorticoid Receptor and Prevents Genomic Recruitment of Steroid Receptor Coactivator-1. J. Biol. Chem. 2015, 290, 21876–21889. [Google Scholar] [CrossRef] [PubMed]
- Barrera-Chimal, J.; Bonnard, B.; Jaisser, F. Roles of Mineralocorticoid Receptors in Cardiovascular and Cardiorenal Diseases. Annu. Rev. Physiol. 2022, 84, 585–610. [Google Scholar] [CrossRef] [PubMed]
- Pitt, B.; Kober, L.; Ponikowski, P.; Gheorghiade, M.; Filippatos, G.; Krum, H.; Nowack, C.; Kolkhof, P.; Kim, S.Y.; Zannad, F. Safety and tolerability of the novel non-steroidal mineralocorticoid receptor antagonist BAY 94-8862 in patients with chronic heart failure and mild or moderate chronic kidney disease: A randomized, double-blind trial. Eur. Heart J. 2013, 34, 2453–2463. [Google Scholar] [CrossRef] [PubMed]
- Pitt, B.; Filippatos, G.; Agarwal, R.; Anker, S.D.; Bakris, G.L.; Rossing, P.; Joseph, A.; Kolkhof, P.; Nowack, C.; Schloemer, P.; et al. Cardiovascular Events with Finerenone in Kidney Disease and Type 2 Diabetes. N. Engl. J. Med. 2021, 385, 2252–2263. [Google Scholar] [CrossRef]
- Agarwal, R.; Filippatos, G.; Pitt, B.; Anker, S.D.; Rossing, P.; Joseph, A.; Kolkhof, P.; Nowack, C.; Gebel, M.; Ruilope, L.M.; et al. Cardiovascular and kidney outcomes with finerenone in patients with type 2 diabetes and chronic kidney disease: The FIDELITY pooled analysis. Eur. Heart J. 2022, 43, 474–484. [Google Scholar] [CrossRef] [PubMed]
- Ando, H. Inhibition of aldosterone synthase: Does this offer advantages compared with the blockade of mineralocorticoid receptors? Hypertens. Res. 2023, 46, 1056–1057. [Google Scholar] [CrossRef] [PubMed]
- Freeman, M.W.; Halvorsen, Y.D.; Marshall, W.; Pater, M.; Isaacsohn, J.; Pearce, C.; Murphy, B.; Alp, N.; Srivastava, A.; Bhatt, D.L.; et al. Phase 2 Trial of Baxdrostat for Treatment-Resistant Hypertension. N. Engl. J. Med. 2023, 388, 395–405. [Google Scholar] [CrossRef] [PubMed]
- Laffin, L.J.; Rodman, D.; Luther, J.M.; Vaidya, A.; Weir, M.R.; Rajicic, N.; Slingsby, B.T.; Nissen, S.E.; Target, H.T.N.I. Aldosterone Synthase Inhibition with Lorundrostat for Uncontrolled Hypertension: The Target-HTN Randomized Clinical Trial. JAMA 2023, 330, 1140–1150. [Google Scholar] [CrossRef] [PubMed]
- Zoccali, C.; Mallamaci, F.; De Nicola, L.; Minutolo, R. New trials in resistant hypertension: Mixed blessing stories. Clin. Kidney J. 2024, 17, sfad251. [Google Scholar] [CrossRef] [PubMed]
- Bakris, G.L. Major Advancements in Slowing Diabetic Kidney Disease Progression: Focus on SGLT2 Inhibitors. Am. J. Kidney Dis. 2019, 74, 573–575. [Google Scholar] [CrossRef] [PubMed]
- Sinha, S.K.; Nicholas, S.B. Pathomechanisms of Diabetic Kidney Disease. J. Clin. Med. 2023, 12, 7349. [Google Scholar] [CrossRef] [PubMed]
- Michos, E.D.; Bakris, G.L.; Rodbard, H.W.; Tuttle, K.R. Glucagon-like peptide-1 receptor agonists in diabetic kidney disease: A review of their kidney and heart protection. Am. J. Prev. Cardiol. 2023, 14, 100502. [Google Scholar] [CrossRef] [PubMed]
- Alicic, R.Z.; Cox, E.J.; Neumiller, J.J.; Tuttle, K.R. Incretin drugs in diabetic kidney disease: Biological mechanisms and clinical evidence. Nat. Rev. Nephrol. 2021, 17, 227–244. [Google Scholar] [CrossRef]
- Rode, A.K.O.; Buus, T.B.; Mraz, V.; Al-Jaberi, F.A.H.; Lopez, D.V.; Ford, S.L.; Hennen, S.; Eliasen, I.P.; Klewe, I.V.; Gharehdaghi, L.; et al. Induced Human Regulatory T Cells Express the Glucagon-like Peptide-1 Receptor. Cells 2022, 11, 2587. [Google Scholar] [CrossRef] [PubMed]
- Moellmann, J.; Klinkhammer, B.M.; Onstein, J.; Stohr, R.; Jankowski, V.; Jankowski, J.; Lebherz, C.; Tacke, F.; Marx, N.; Boor, P.; et al. Glucagon-like Peptide 1 and Its Cleavage Products Are Renoprotective in Murine Diabetic Nephropathy. Diabetes 2018, 67, 2410–2419. [Google Scholar] [CrossRef] [PubMed]
- Sourris, K.C.; Ding, Y.; Maxwell, S.S.; Al-Sharea, A.; Kantharidis, P.; Mohan, M.; Rosado, C.J.; Penfold, S.A.; Haase, C.; Xu, Y.; et al. Glucagon-like peptide-1 receptor signaling modifies the extent of diabetic kidney disease through dampening the receptor for advanced glycation end products-induced inflammation. Kidney Int. 2024, 105, 132–149. [Google Scholar] [CrossRef] [PubMed]
- Farah, L.X.; Valentini, V.; Pessoa, T.D.; Malnic, G.; McDonough, A.A.; Girardi, A.C. The physiological role of glucagon-like peptide-1 in the regulation of renal function. Am. J. Physiol. Renal. Physiol. 2016, 310, F123–F127. [Google Scholar] [CrossRef] [PubMed]
- Block, T.J.; Cooper, M.E. Clinical trials with reno-vascular end points in patients with diabetes: Changing the scenario over the past 20 years. Presse Med. 2023, 52, 104178. [Google Scholar] [CrossRef] [PubMed]
- Marso, S.P.; Daniels, G.H.; Brown-Frandsen, K.; Kristensen, P.; Mann, J.F.; Nauck, M.A.; Nissen, S.E.; Pocock, S.; Poulter, N.R.; Ravn, L.S.; et al. Liraglutide and Cardiovascular Outcomes in Type 2 Diabetes. N. Engl. J. Med. 2016, 375, 311–322. [Google Scholar] [CrossRef] [PubMed]
- Marso, S.P.; Bain, S.C.; Consoli, A.; Eliaschewitz, F.G.; Jodar, E.; Leiter, L.A.; Lingvay, I.; Rosenstock, J.; Seufert, J.; Warren, M.L.; et al. Semaglutide and Cardiovascular Outcomes in Patients with Type 2 Diabetes. N. Engl. J. Med. 2016, 375, 1834–1844. [Google Scholar] [CrossRef] [PubMed]
- Tuttle, K.R.; Lakshmanan, M.C.; Rayner, B.; Busch, R.S.; Zimmermann, A.G.; Woodward, D.B.; Botros, F.T. Dulaglutide versus insulin glargine in patients with type 2 diabetes and moderate-to-severe chronic kidney disease (AWARD-7): A multicentre, open-label, randomised trial. Lancet Diabetes Endocrinol. 2018, 6, 605–617. [Google Scholar] [CrossRef] [PubMed]
- Gerstein, H.C.; Colhoun, H.M.; Dagenais, G.R.; Diaz, R.; Lakshmanan, M.; Pais, P.; Probstfield, J.; Riesmeyer, J.S.; Riddle, M.C.; Ryden, L.; et al. Dulaglutide and cardiovascular outcomes in type 2 diabetes (REWIND): A double-blind, randomised placebo-controlled trial. Lancet 2019, 394, 121–130. [Google Scholar] [CrossRef] [PubMed]
- Gerstein, H.C.; Sattar, N.; Rosenstock, J.; Ramasundarahettige, C.; Pratley, R.; Lopes, R.D.; Lam, C.S.P.; Khurmi, N.S.; Heenan, L.; Del Prato, S.; et al. Cardiovascular and Renal Outcomes with Efpeglenatide in Type 2 Diabetes. N. Engl. J. Med. 2021, 385, 896–907. [Google Scholar] [CrossRef] [PubMed]
- Gragnano, F.; De Sio, V.; Calabro, P. FLOW trial stopped early due to evidence of renal protection with semaglutide. Eur. Heart J. Cardiovasc. Pharmacother. 2024, 10, 7–9. [Google Scholar] [CrossRef] [PubMed]
- Heerspink, H.J.L.; Sattar, N.; Pavo, I.; Haupt, A.; Duffin, K.L.; Yang, Z.; Wiese, R.J.; Tuttle, K.R.; Cherney, D.Z.I. Effects of tirzepatide versus insulin glargine on kidney outcomes in type 2 diabetes in the SURPASS-4 trial: Post-hoc analysis of an open-label, randomised, phase 3 trial. Lancet Diabetes Endocrinol. 2022, 10, 774–785. [Google Scholar] [CrossRef] [PubMed]
- Solini, A. Tirzepatide and kidney function: An intriguing and promising observation. Lancet Diabetes Endocrinol. 2022, 10, 762–763. [Google Scholar] [CrossRef] [PubMed]
- Parker, V.E.R.; Hoang, T.; Schlichthaar, H.; Gibb, F.W.; Wenzel, B.; Posch, M.G.; Rose, L.; Chang, Y.T.; Petrone, M.; Hansen, L.; et al. Efficacy and safety of cotadutide, a dual glucagon-like peptide-1 and glucagon receptor agonist, in a randomized phase 2a study of patients with type 2 diabetes and chronic kidney disease. Diabetes Obes. Metab. 2022, 24, 1360–1369. [Google Scholar] [CrossRef] [PubMed]
- Wang, M.Y.; Zhang, Z.; Zhao, S.; Onodera, T.; Sun, X.N.; Zhu, Q.; Li, C.; Li, N.; Chen, S.; Paredes, M.; et al. Downregulation of the kidney glucagon receptor, essential for renal function and systemic homeostasis, contributes to chronic kidney disease. Cell Metab. 2024, 36, 575–597.e577. [Google Scholar] [CrossRef] [PubMed]
- Tan, S.K.; Cooper, M.E. Is clinical trial data showing positive progress for the treatment of diabetic kidney disease? Expert Opin. Emerg. Drugs 2023, 28, 217–226. [Google Scholar] [CrossRef] [PubMed]
- Eli Lilly Company. A Study of Retatrutide (LY3437943) on Renal Function in Participants with Overweight or Obesity and Chronic Kidney Disease with or without Type 2 Diabetes. Available online: https://classic.clinicaltrials.gov/show/NCT05936151 (accessed on 20 March 2024).
- Heerspink, H.J.L.; Greasley, P.J.; Ahlstrom, C.; Althage, M.; Dwyer, J.P.; Law, G.; Wijkmark, E.; Lin, M.; Mercier, A.K.; Sunnaker, M.; et al. Efficacy and safety of zibotentan and dapagliflozin in patients with chronic kidney disease: Study design and baseline characteristics of the ZENITH-CKD trial. Nephrol. Dial. Transpl. 2023, 39, 414–425. [Google Scholar] [CrossRef] [PubMed]
- Dhaun, N.; Chapman, G.B. Endothelin antagonism: Stepping into the spotlight. Lancet 2023, 402, 1945–1947. [Google Scholar] [CrossRef] [PubMed]
- Sawaf, H.; Thomas, G.; Taliercio, J.J.; Nakhoul, G.; Vachharajani, T.J.; Mehdi, A. Therapeutic Advances in Diabetic Nephropathy. J. Clin. Med. 2022, 11, 378. [Google Scholar] [CrossRef] [PubMed]
- Kearney, J.; Gnudi, L. The Pillars for Renal Disease Treatment in Patients with Type 2 Diabetes. Pharmaceutics 2023, 15, 1343. [Google Scholar] [CrossRef] [PubMed]
- de Vries, J.K.; Levin, A.; Loud, F.; Adler, A.; Mayer, G.; Pena, M.J. Implementing personalized medicine in diabetic kidney disease: Stakeholders’ perspectives. Diabetes Obes. Metab. 2018, 20 (Suppl. 3), 24–29. [Google Scholar] [CrossRef] [PubMed]
- Heerspink, H.J.L.; List, J.; Perkovic, V. New clinical trial designs for establishing drug efficacy and safety in a precision medicine era. Diabetes Obes. Metab. 2018, 20 (Suppl. 3), 14–18. [Google Scholar] [CrossRef] [PubMed]
- de Zeeuw, D.; Heerspink, H.J.L. Unmet need in diabetic nephropathy: Failed drugs or trials? Lancet Diabetes Endocrinol. 2016, 4, 638–640. [Google Scholar] [CrossRef] [PubMed]
- Idzerda, N.M.A.; Pena, M.J.; Heerspink, H.J.L. Personalized medicine in diabetic kidney disease: A novel approach to improve trial design and patient outcomes. Curr. Opin. Nephrol. Hypertens. 2018, 27, 426–432. [Google Scholar] [CrossRef]

| Study, Year | Experimental Drug | Class | Study Population | Kidney Outcome | Reference |
|---|---|---|---|---|---|
| CSG Captopril, 1993 | Captopril | ACEi | DKD | Doubling of base-line serum creatinine concentration | [53] |
| RENAAL, 2001 | Losartan | ARB | DKD | Doubling of serum creatinine, ESKD or death | [54] |
| IDNT, 2001 | Irbesartan | ARB | DKD | Doubling of serum creatinine, ESKD or death | [55] |
| DETAIL, 2005 | Telmisartan | ARB | DKD | Change in measured GFR | [56] |
| AMADEO, 2008 | Telmisartan | ARB | DKD | Change in UACR | [57] |
| FIDELIO-DKD, 2020 | Finerenone | NS-MRA | DKD | Kidney failure, >40% decrease in eGFR, death from kidney cause | [58] |
| CREDENCE, 2019 | Canagliflozin | SGLT2i | DKD | ESKD, doubling of the serum creatinine level, or death from renal or cardiovascular causes | [59] |
| DAPA-CKD, 2020 | Dapagliflozin | SGLT2i | CKD/DKD | Sustained ≥ 50% reduction in eGFR, ESKD, or death from renal or cardiovascular cause | [60] |
| EMPA-KIDNEY, 2023 | Empagliflozin | SGLT2i | CKD/DKD | ESKD, a sustained reduction in eGFR to <10 mL/min/1.73 m2, renal death, or a sustained decline ≥ 40% in eGFR | [61] |
| FLOW, 2024 | Semaglutide | GLP-1 RA | DKD | Persistent ≥ 50% reduction in eGFR, reaching ESKD, death from kidney disease or death from CV cause | [62] |
| ASCEND, 2010 | Avosentan | ETA RA | DKD | Doubling of serum creatinine, ESKD, death | [63] |
| SONAR, 2019 | Atrasentan | ETA RA | DKD | Doubling of serum creatinine, ESKD | [64] |
| ZENITH-CKD, 2023 | Zibotentan + Dapaglifozin | ETA RA + SGLT2i | CKD | Change in UACR | [65] |
| NCT05182840, 2024 | BI 690517 | ASI ± SGLT2i | CKD | Change in UACR | [66] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mazzieri, A.; Porcellati, F.; Timio, F.; Reboldi, G. Molecular Targets of Novel Therapeutics for Diabetic Kidney Disease: A New Era of Nephroprotection. Int. J. Mol. Sci. 2024, 25, 3969. https://doi.org/10.3390/ijms25073969
Mazzieri A, Porcellati F, Timio F, Reboldi G. Molecular Targets of Novel Therapeutics for Diabetic Kidney Disease: A New Era of Nephroprotection. International Journal of Molecular Sciences. 2024; 25(7):3969. https://doi.org/10.3390/ijms25073969
Chicago/Turabian StyleMazzieri, Alessio, Francesca Porcellati, Francesca Timio, and Gianpaolo Reboldi. 2024. "Molecular Targets of Novel Therapeutics for Diabetic Kidney Disease: A New Era of Nephroprotection" International Journal of Molecular Sciences 25, no. 7: 3969. https://doi.org/10.3390/ijms25073969
APA StyleMazzieri, A., Porcellati, F., Timio, F., & Reboldi, G. (2024). Molecular Targets of Novel Therapeutics for Diabetic Kidney Disease: A New Era of Nephroprotection. International Journal of Molecular Sciences, 25(7), 3969. https://doi.org/10.3390/ijms25073969






