Aggression in Women with Schizophrenia Is Associated with Lower HDL Cholesterol Levels
Abstract
1. Introduction
2. Results
3. Discussion
4. Materials and Methods
4.1. Participants
4.2. Determination of Serum Lipid Levels (Cholesterol, Triglycerides, HDL Cholesterol, LDL Cholesterol)
4.3. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Volavka, J.; Citrome, L. Pathways to aggression in schizophrenia affect results of treatment. Schizophr. Bull. 2011, 37, 921–929. [Google Scholar] [CrossRef] [PubMed]
- Puljic, K.; Herceg, M.; Tudor, L.; Pivac, N. The association between prolactin concentration and aggression in female patients with schizophrenia. World J. Biol. Psychiatry 2020, 22, 301–309. [Google Scholar] [CrossRef]
- Štraus, B.; Petrik, J. Lipidi i lipoproteini. In Štrausova Medicinska Biokemija, 3rd ed.; Čvorišćec, D., Čepelak, I., Eds.; Medicinska Naklada: Zagreb, Croatia, 2009; pp. 124–151. [Google Scholar]
- Berg, J.M.; Tymoczko, J.L.; Stryer, L. Biochemistry, 6th ed.; W. H. Freeman and Company: New York, NY, USA, 2007. [Google Scholar]
- Tuccori, M.; Montagnani, S.; Mantarro, S.; Capogrosso-Sansone, A.; Ruggiero, E.; Saporiti, A.; Antonioli, L.; Fornai, M.; Blandizzi, C. Neuropsychiatric adverse events associated with statins: Epidemiology, pathophysiology, prevention and management. Cns Drugs 2014, 28, 249–272. [Google Scholar] [CrossRef] [PubMed]
- Da Graça Cantarelli, M.; Tramontina, A.C.; Leite, M.C.; Gonçalves, C.A. Potential neurochemical links between cholesterol and suicidal behavior. Psychiatry Res. 2014, 220, 745–751. [Google Scholar] [CrossRef] [PubMed]
- Tomson-Johanson, K.; Harro, J. Low cholesterol, impulsivity and violence revisited. Curr. Opin. Endocrinol. Diabetes Obes. 2018, 25, 103–107. [Google Scholar] [CrossRef]
- Misiak, B.; Stańczykiewicz, B.; Łaczmański, L.; Frydecka, D. Lipid profile disturbances in antipsychotic-naive patients with first-episode non-affective psychosis: A systematic review and meta-analysis. Schizophr. Res. 2017, 190, 18–27. [Google Scholar] [CrossRef]
- Mimica, N.; Uzun, S.; Makarić, G.; Kozumplik, O.; Ljubin Golub, T.; Folnegović Grošić, P. Clonazepam augmentation during treatment with antipsychotics in aggressive psychiatric inpatients—Pilot study. Med. Jad. 2018, 48, 217–223. [Google Scholar]
- Uzun, S.; Kozumplik, O.; Mimica, N.; Folnegovic-Smalc, V. Patients with schizophrenia and aggressive behaviour: Treatment with combination of risperidone and topiramat. Ceska Slov. Psychiatr. 2008, 104, 1257. [Google Scholar]
- Wysokinski, A.; Strzelecki, D.; Kloszewska, I. Levels of triglycerides, cholesterol, LDL, HDL and glucose in patients with schizophrenia, unipolar depression and bipolar disorder. Diabetes Metab. Syndr. 2015, 9, 168–176. [Google Scholar] [CrossRef]
- Solberg, D.K.; Bentsen, H.; Refsum, H.; Andreassen, O.A. Association between serum lipids and membrane fatty acids and clinical characteristics in patients with schizophrenia. Acta Psychiatr. Scand. 2015, 132, 293–300. [Google Scholar] [CrossRef]
- Sen, P.; Adewusi, D.; Blakemore, A.I.; Kumari, V. How do lipids influence risk of violence, self-harm and suicidality in people with psychosis? A systematic review. Aust. N. Z. J. Psychiatry 2022, 56, 451–488. [Google Scholar] [CrossRef]
- Muldoon, M.F.; Manuck, S.B.; Mathews, K.M. Lowering cholesterol concentrations and mortality: A quantitative review of primary prevention trials. Br. Med. J. 1990, 301, 309–314. [Google Scholar] [CrossRef] [PubMed]
- Engelberg, H. Low serum cholesterol and suicide. Lancet 1992, 339, 727–729. [Google Scholar] [CrossRef]
- González-Castro, T.B.; Genis-Mendoza, A.D.; León-Escalante, D.I.; Hernández-Díaz, Y.; Juárez-Rojop, I.E.; Tovilla-Zárate, C.A.; López-Narváez, M.L.; Marín-Medina, A.; Nicolini, H.; Castillo-Avila, R.G.; et al. Possible Association of Cholesterol as a Biomarker in Suicide Behavior. Biomedicines 2021, 9, 1559. [Google Scholar] [CrossRef] [PubMed]
- Weltens, I.; Bak, M.; Verhagen, S.; Vandenberk, E.; Domen, P.; van Amelsvoort, T.; Drukker, M. Aggression on the psychiatric ward: Prevalence and risk factors: A systematic review of the literature. PLoS ONE 2021, 16, e0258346. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.; Ding, Y.; Wu, F.; Xie, G.; Hou, J.; Mao, P. Serum lipid levels and suicidality: A meta-analysis of 65 epidemiological studies. J. Psychiatry Neurosci. 2016, 41, 56–69. [Google Scholar] [CrossRef]
- Svensson, T.; Inoue, M.; Sawada, N.; Charvat, H.; Mimura, M.; Tsugane, S.; JPHC Study Group. High serum total cholesterol is associated with suicide mortality in Japanese women. Acta Psychiatr. Scand. 2017, 136, 259–268. [Google Scholar] [CrossRef]
- Vevera, J.; Žukov, I.; Morcinek, T.; Papežova, H. Cholesterol concentrations in violent and non-violent women suicide attempters. Eur. Psychiatry 2003, 18, 23–27. [Google Scholar] [CrossRef]
- Hjell, G.; Mørch-Johnsen, L.; Holst, R.; Tesli, N.; Bell, C.; Lunding, S.H.; Rødevand, L.; Werner, M.C.F.; Melle, I.; Andreassen, O.A.; et al. Disentangling the relationship between cholesterol, aggression, and impulsivity in severe mental disorders. Brain Behav. 2020, 10, e01751. [Google Scholar] [CrossRef]
- Marcinko, D.; Pivac, N.; Martinac, M.; Jakovljević, M.; Mihaljević-Peles, A.; Muck-Seler, D. Platelet serotonin and serum cholesterol concentrations in suicidal and non-suicidal male patients with a first episode of psychosis. Psychiatry Res. 2007, 150, 105–108. [Google Scholar] [CrossRef]
- Eriksen, B.M.S.; Bjørkly, S.; Lockertsen, Ø.; Færden, A.; Roaldset, J.O. Low cholesterol as a risk marker of inpatient and post-discharge violence in acute psychiatry—A prospective study with focus on gender. Psychiatry Res. 2017, 255, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Ainiyet, B.; Rybakowski, J.K. Suicidal behavior in schizophrenia may be related to low lipid levels. Med. Sci. Monit. 2014, 20, 1486–1490. [Google Scholar] [CrossRef] [PubMed]
- Paavola, P.; Repo-Tiihonen, E.; Tiihonen, J. Serum lipid levels and violence among Finnish male forensic psychiatric patients. J. Forensic Psychiatry 2002, 13, 555–568. [Google Scholar] [CrossRef]
- Roaldset, J.O.; Bakken, A.M.; Bjørkly, S. A prospective study of lipids and serotonin as risk markers of violence and self-harm in acute psychiatric patients. Psychiatry Res. 2011, 186, 293–299. [Google Scholar] [CrossRef] [PubMed]
- Chen, S.C.; Chu, N.H.; Hwu, H.G.; Chen, W.J. Trajectory classes of violent behavior and their relationship to lipid levels in schizophrenia inpatients. J. Psychiatr. Res. 2015, 66–67, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Xu, J.; Tang, J.; Dai, X.; Huang, H.; Cao, R.; Hu, J. Dysregulation of amino acids and lipids metabolism in schizophrenia with violence. BMC Psychiatry 2020, 20, 97. [Google Scholar] [CrossRef] [PubMed]
- Kay, S.R.; Fiszbein, A.; Opler, L.A. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr. Bull. 1987, 13, 261–276. [Google Scholar] [CrossRef]
- Silver, J.M.; Yudofsky, S.C. The Overt Aggression Scale: Overview and guiding principles. J. Neuropsychiatry Clin. Neurosci. 1991, 3, 22–29. [Google Scholar]
| Subjects with Schizophrenia | ||||
|---|---|---|---|---|
| Nonaggressive (N = 60) | Aggressive (N = 60) | Statistics | ||
| Age (years) | 37 ± 8 | 35 ± 7 | t = 1.383; p = 0.169 | |
| Length of illness (years) | 9 ± 6 | 8 ± 6 | t = 0.183; p = 0.855 | |
| Length of hospitalization (days) | 24 ± 8 | 28 ± 10 | t = 2.287; p = 0.024 | |
| Antipsychotic dose * (mg/day) | 180.9 ± 115.5 | 343.8 ± 154.7 | t = 6.533; p < 0.001 | |
| Smoking (N; %) | Yes | 40 (66.7%) | 42 (70.0%) | χ2 = 0.154; p = 0.422 |
| No | 20 (33.3%) | 18 (30.0%) | ||
| Number of cigarettes (/day) | 11 ± 9 | 16 ± 11 | t = 2.380; p = 0.020 | |
| PANSS total scores | 94 ± 9 | 103 ± 11 | t = 4.905; p < 0.001 | |
| PANSS subscale scores for aggression | - | 10 ± 5 | - | |
| OAS scores | - | 12 ± 6 | - | |
| Suicidal behavior (N; %) | Yes | 0 (0.0%) | 18 (30.0%) | χ2 = 27.176; p < 0.001 |
| No | 60 (100.0%) | 42 (70.0%) | ||
| Female Subjects with Schizophrenia | |||
|---|---|---|---|
| Nonaggressive (N = 60) | Aggressive (N = 60) | Statistics | |
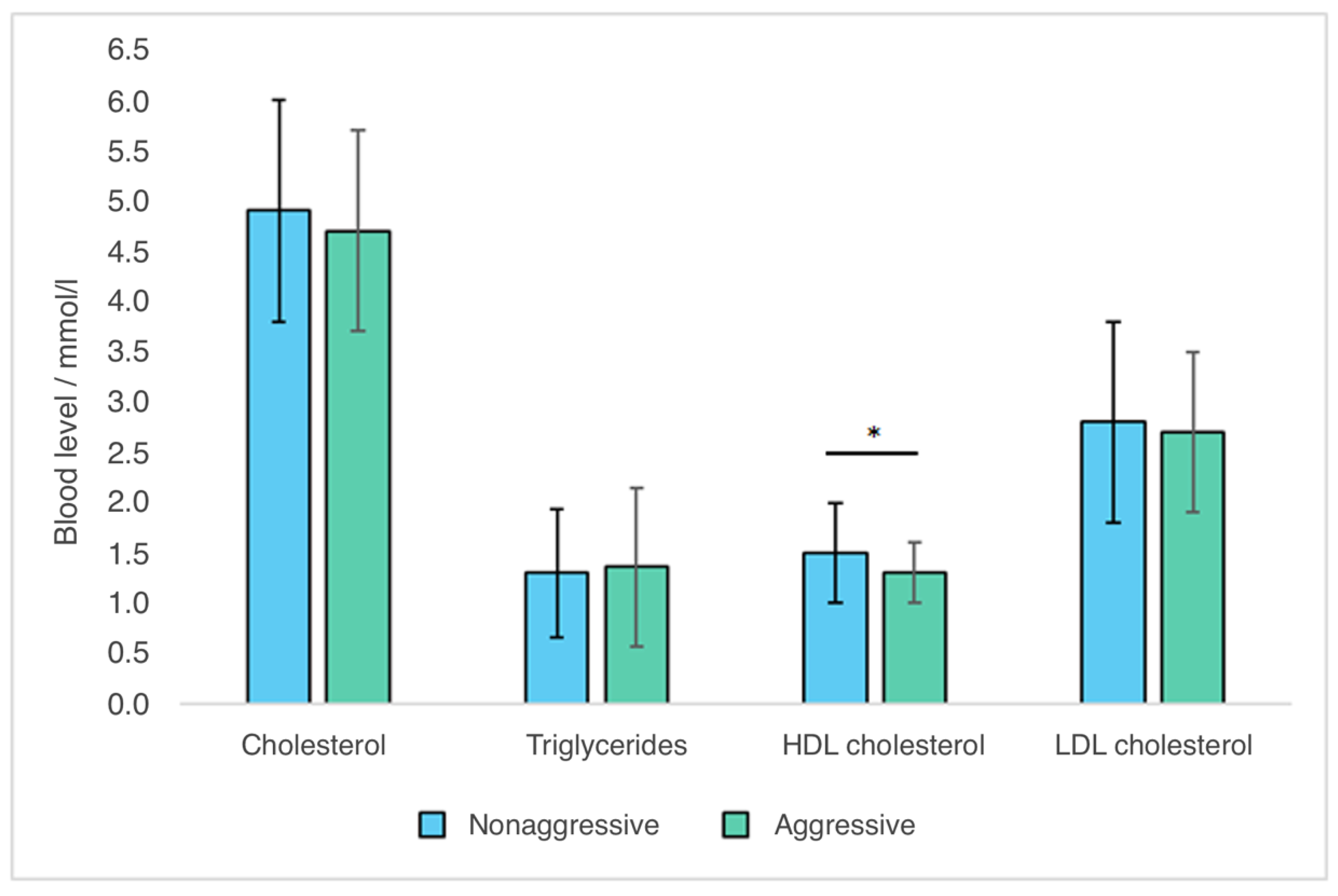
| Cholesterol/mmol/L | 4.9 ± 1.1 | 4.7 ± 1.0 | t = 1.320; p = 0.190 * |
| Cholesterol ≤ 5 mmol/L (N; %) | 33 (55.0%) | 37 (61.7%) | χ2 = 0.549 p = 0.459 ** |
| Cholesterol > 5 mmol/L (N; %) | 27 (45.0%) | 23 (38.3%) | |
| Triglycerides/mmol/L | 1.30 ± 0.64 | 1.36 ± 0.79 | t = −0.450; p = 0.653 * |
| Triglycerides ≤ 1.7 mmol/L (N; %) | 48 (80.0%) | 47 (78.3%) | χ2 = 0.051 p = 0.822 ** |
| Triglycerides > 1.7 mmol/L (N; %) | 12 (20.0%) | 19 (31.7%) | |
| HDL cholesterol/mmol/L | 1.5 ± 0.5 | 1.3 ± 0.3 | t = 2.540; p = 0.012 * |
| HDL cholesterol ≥ 1.2 mmol/L (N; %) | 53 (38.3%) | 41 (68.3%) | χ2 = 7.007 p = 0.008 ** |
| HDL cholesterol < 1.2 mmol/L (N; %) | 7 (11.7%) | 19 (31.7) | |
| LDL cholesterol/mmol/L | 2.8 ± 1.0 | 2.7 ± 0.8 | t = 0.683; p = 0.496 * |
| LDL cholesterol ≤ 3 mmol/L (N; %) | 38 (63.3%) | 36 (60.0%) | χ2 = 0.141; p = 0.707 ** |
| LDL cholesterol > 3 mmol/L (N; %) | 22 (36.7%) | 24 (40.0%) | |
| Female Subjects with Schizophrenia | ||
|---|---|---|
| Nonaggressive | Aggressive | |
| Age | β = 0.081; p= 0.519 | β = 0.255; p = 0.057 |
| Antipsychotic dose * | β = 0.097; p = 0.461 | β = −0.060; p = 0.718 |
| Smoking | β = 0.208; p = 0.095 | β = 0.135; p = 0.333 |
| PANSS | β = 0.298; p = 0.024 | β = 0.329; p = 0.022 |
| PANSS-AG | - | β = −0.128; p = 0.455 |
| OAS | - | β = 0.001; p = 0.993 |
| Suicidality | - | β = 0.019; p = 0.893 |
| Model | ** R2 = 0.124; F = 3.079; p = 0.023 | ** R2 = 0.076; F = 1.694; p = 0.139 |
| Aggression (YES/NO) | |
|---|---|
| Independent variable | Odds ratio (95% Confidence Interval) |
| Age | 0.970 (0.911–1.032); p = 0.338 |
| PANSS | 1.224 (1.108–1.353); p < 0.001 |
| Smoking | 0.787 (0.321–1.930); p = 0.604 |
| Cholesterol | 1.301 (0.182–9.314); p = 0.794 |
| Triglycerides | 0.743 (0.249–2.217); p = 0.594 |
| HDL cholesterol | 0.115 (0.014–0.968); p = 0.047 |
| LDL cholesterol | 0.723 (0.098–5.322); p = 0.723 |
| Model | * PAC = 74.2; ** R2 = 0.291; x2 = 28.943; p < 0.001 |
| Aggressive Subjects Divided with Respect to Suicidal Behavior | |||
|---|---|---|---|
| Non-Suicidal (N = 42) | Suicidal (N = 18) | Statistics | |
| HDL cholesterol (mmol/L) | 1.340 ± 0.346 | 1.322 ± 0.364 | t = 0.184; p = 0.854 * |
| HDL cholesterol ≥ 1.2 mmol/L (N; %) | 29 (69.0%) | 12 (66.7%) | χ2 = 0.033; p = 0.856 ** |
| HDL cholesterol < 1.2 mmol/L (N; %) | 13 (31.0%) | 6 (33.3%) | |
| Suicidal Behavior (YES/NO) | |
|---|---|
| Independent variable | Odds ratio (95% Confidence Interval) |
| Age | 0.963 (0.882–1.051); p = 0.401 |
| PANSS | 1.067 (0.937–1.214); p = 0.330 |
| Smoking | 2.367 (0.647–8.664); p = 0.193 |
| Cholesterol | 0.040 (0.000–5.439); p = 0.199 |
| Triglycerides | 3.922 (0.429–35.904); p = 0.226 |
| HDL cholesterol | 10.311 (0.116–919.05); p = 0.308 |
| LDL cholesterol | 23.409 (0.152–3604.981); p = 0.163 |
| Model | * PAC = 70.0; ** R2 = 0.116; x2 = 5.137; p = 0.643 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Herceg, D.; Mimica, N.; Herceg, M.; Puljić, K. Aggression in Women with Schizophrenia Is Associated with Lower HDL Cholesterol Levels. Int. J. Mol. Sci. 2022, 23, 11858. https://doi.org/10.3390/ijms231911858
Herceg D, Mimica N, Herceg M, Puljić K. Aggression in Women with Schizophrenia Is Associated with Lower HDL Cholesterol Levels. International Journal of Molecular Sciences. 2022; 23(19):11858. https://doi.org/10.3390/ijms231911858
Chicago/Turabian StyleHerceg, Dora, Ninoslav Mimica, Miroslav Herceg, and Krešimir Puljić. 2022. "Aggression in Women with Schizophrenia Is Associated with Lower HDL Cholesterol Levels" International Journal of Molecular Sciences 23, no. 19: 11858. https://doi.org/10.3390/ijms231911858
APA StyleHerceg, D., Mimica, N., Herceg, M., & Puljić, K. (2022). Aggression in Women with Schizophrenia Is Associated with Lower HDL Cholesterol Levels. International Journal of Molecular Sciences, 23(19), 11858. https://doi.org/10.3390/ijms231911858









