A Vismodegib Experience in Elderly Patients with Basal Cell Carcinoma: Case Reports and Review of the Literature
Abstract
1. Introduction
2. Local Treatment Options for BCC
2.1. Surgical Excision
2.2. Radiation Therapy
2.3. Destructive Therapies
2.4. Topical and Intralesional Therapies
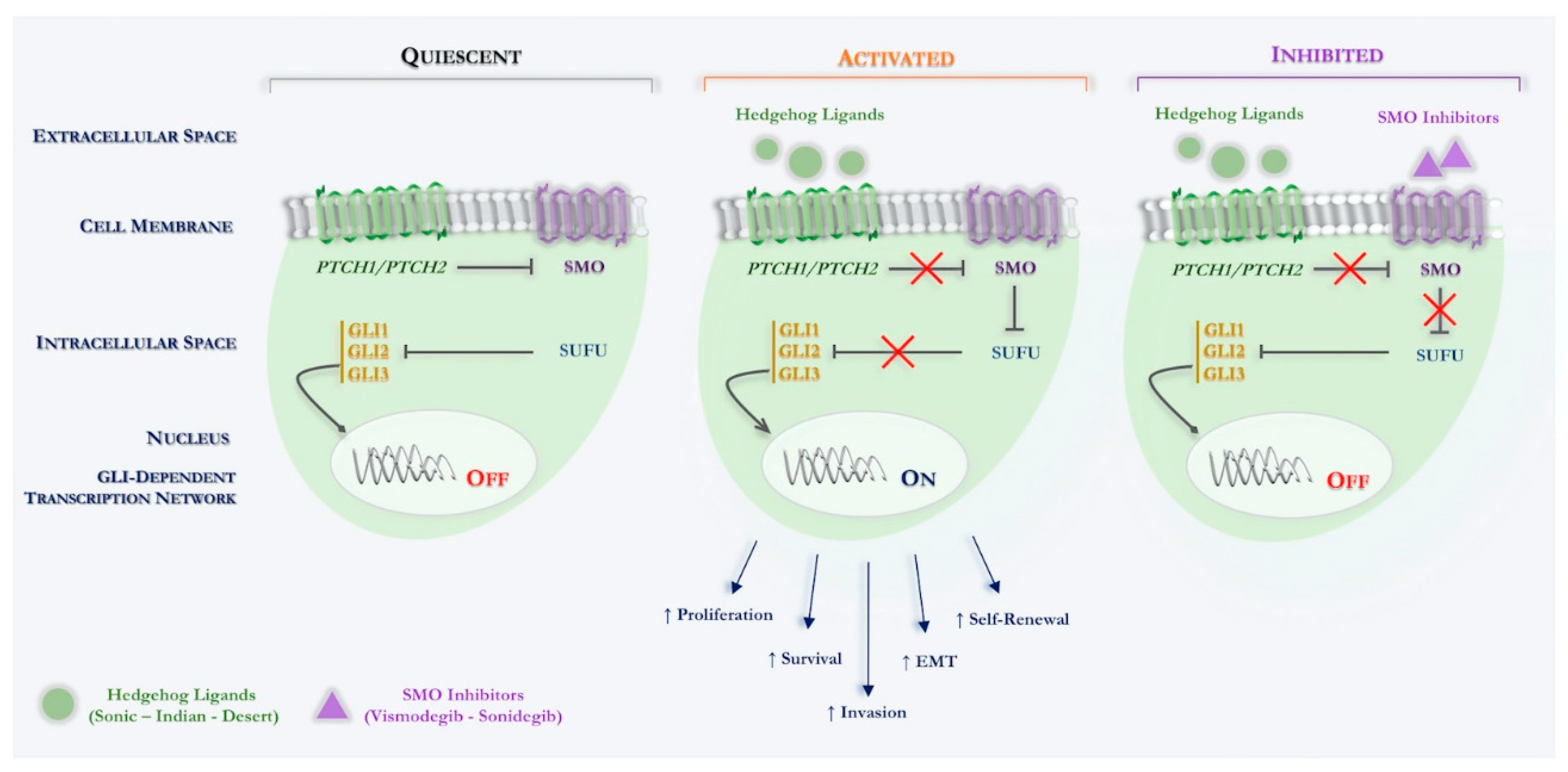
3. Role of Hedgehog Signaling Pathway in BCC
4. Hedgehog Pathway Inhibitors
4.1. Vismodegib
4.2. Sonidegib
5. Safety and Efficacy of Vismodegib in Advanced BCC Elderly Patients
6. Predictive Biomarkers of Response to Hedgehog Inhibitors
7. Case Reports
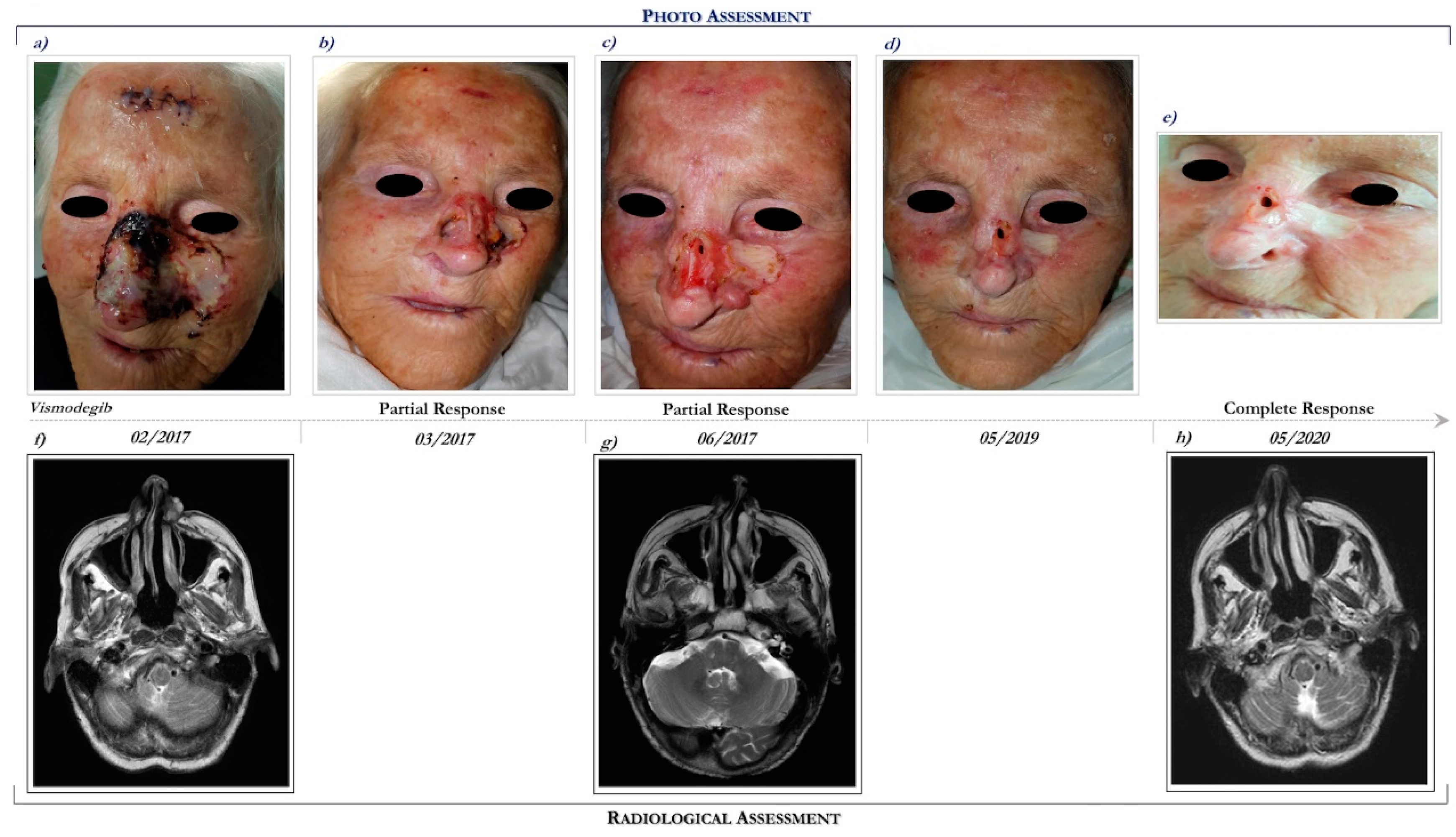
7.1. Case Report 1
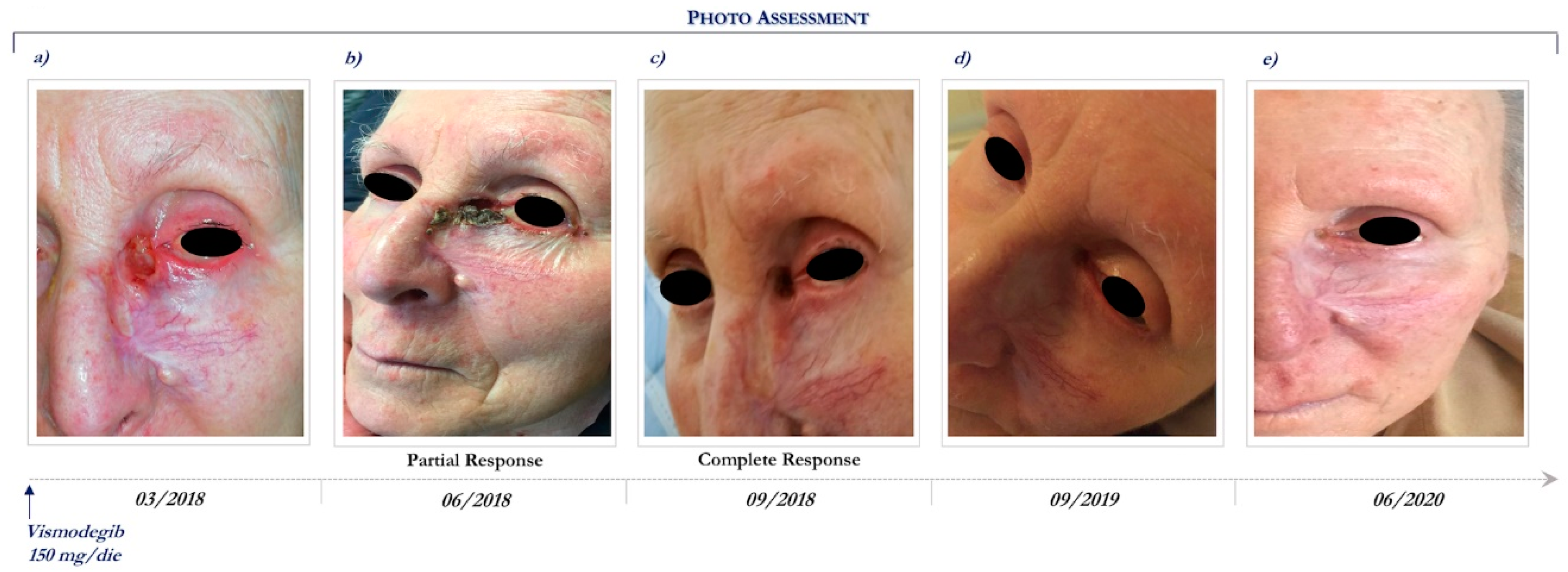
7.2. Case Report 2
8. Conclusions
Funding
Conflicts of Interest
References
- Ferlay, J.; Soerjomataram, I.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, D.M.; Forman, D.; Bray, F. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int. J. Cancer 2015, 136, E359–E386. [Google Scholar] [CrossRef]
- Jacob, A. Observations respecting an ulcer of peculiar character, which attacks the eyelids and other parts of the face. Dublin Hosp. Rep. Commun. Med. Surg. 1827, 4, 232–239. [Google Scholar]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2018. CA Cancer J. Clin. 2018, 68, 7–30. [Google Scholar] [CrossRef] [PubMed]
- Asgari, M.M.; Moffet, H.H.; Ray, G.T.; Quesenberry, C.P. Trends in basal cell carcinoma incidence and identification of high-risk subgroups, 1998–2012. JAMA Dermatol. 2015, 151, 976–978. [Google Scholar] [CrossRef] [PubMed]
- Sreekantaswamy, S.; Justin Endo, B.S.; Chen, A.; Butler, D.; Morrison, L.; Linos, E. Aging and the treatment of basal cell carcinoma. Clin. Dermatol. 2019, 37, 373–378. [Google Scholar] [CrossRef]
- Varga, E.; Korom, I.; Raskó, Z.; Kis, E.; Varga, J.; Olah, J.; Kemeny, L. Neglected basal cell carcinomas in the 21st century. J. Skin Cancer 2011, 2011, 4. [Google Scholar] [CrossRef]
- Wiznia, L.E.; Federman, D.G. Treatment of Basal Cell Carcinoma in the Elderly: What non-dermatologists need to know. Am. J. Med. 2016, 129, 655–660. [Google Scholar] [CrossRef]
- Sekulic, A.; Migden, M.R.; Basset-Seguin, N.; Garbe, C.; Gesierich, A.; Miller, C.L.; Mortier, L.; Murrel, D.F.; Hamid, O.; Quevedo, F.; et al. Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma: Final update (30-month) of the pivotal ERIVANCE BCC study [abstract]. J. Clin. Oncol. 2014, 32, 9013. [Google Scholar] [CrossRef]
- Wolf, D.J.; Zitelli, J.A. Surgical margins for basal cell carcinoma. Arch. Dermatol. 1987, 123, 340–344. [Google Scholar] [CrossRef]
- Gulleth, Y.; Goldberg, N.; Silverman, R.P.; Gastman, B.R. What is the best surgical margin for a Basal cell carcinoma: A meta-analysis of the literature. Plast. Reconstr. Surg. 2010, 126, 1222–1231. [Google Scholar] [CrossRef]
- Silverman, M.K.; Kopf, A.W.; Bart, R.S.; Grin, C.M.; Levenstein, M.S. Recurrence rated of treated basal cell carcinoma. Part 3: Surgical excision. J. Dermatol. Surg. Oncol. 1992, 18, 471–476. [Google Scholar] [CrossRef] [PubMed]
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology: Basal Cell Skin Cancer; Version, I; National Comprehensive Cancer Network: Chicago, IL, USA, 2019. [Google Scholar]
- Holt, D.R.; Kirk, S.J.; Regan, M.C.; Hurson, M.; Lindblad, W.J.; Barbul, A. Effect of age on wound healing in healthy human beings. Surgery 1992, 112, 293–297. [Google Scholar] [PubMed]
- Sgonc, R.; Gruber, J. Age-related aspects of cutaneous wound healing: A mini-review. Gerontology 2013, 59, 159–164. [Google Scholar] [CrossRef] [PubMed]
- Gould, L.; Abadir, P.; Brem, H.; Carter, M.; Conner-Kerr, T.; Davidson, J.; DiPietro, L.; Falanga, V.; Fife, C.; Gardner, S.; et al. Chronic wound repair and healing in older adults: Current status and future research. J. Am. Geriatr. Soc. 2015, 63, 427–438. [Google Scholar] [CrossRef] [PubMed]
- Rowe, D.E.; Carroll, R.J.; Day, C.L. Long-term recurrence rates in previously untreated (primary) basal cell carcinoma: Implications for patient follow-up. J. Dermatol. Surg. Oncol. 1989, 5, 315–328. [Google Scholar] [CrossRef] [PubMed]
- Rowe, D.E.; Carroll, R.J.; Day, C.L. Mohs surgery is the treatment of choice for recurrent (previously treated) basal cell carcinoma. J. Dermatol. Surg. Oncol. 1989, 15, 424–431. [Google Scholar] [CrossRef]
- Dhiwakar, M.; Khan, N.A.; McClymont, L.G. Surgery for head and neck skin tumors in the elderly. Head Neck 2007, 29, 851–856. [Google Scholar] [CrossRef]
- Eide, M.J.; Weinstock, M.A.; Dufresne, R.G., Jr.; Neelagaru, S.; Risica, P.; Burkholder, G.J.; Upegui, D.; Phillips, K.A.; Armstrong, B.K.; Robinson-Bostom, L. Relationship of treatment delay with surgical defect size from keratinocyte carcinoma (basal cell carcinoma and squamous cell carcinoma of the skin). J. Investig. Dermatol. 2005, 124, 308–314. [Google Scholar] [CrossRef]
- Hoorens, I.; Batteauw, A.; Van Maele, G.; Lapiere, K.; Boone, B.; Ongenae, K. Mohs micrographic surgery for basal cell carcinoma: Evaluation of the indication criteria and predictive factors for extensive subclinical spread. Br. J. Dermatol. 2016, 174, 847–852. [Google Scholar] [CrossRef]
- Dinehart, S.M.; Dodge, R.; Stanley, W.E.; Franks, H.H.; Pollack, S.V. Basal cell carcinoma treated with Mohs surgery. A comparison of 54 younger patients with 1050 older patients. J. Dermatol. Surg. Oncol. 1992, 18, 560–566. [Google Scholar] [CrossRef]
- Camarero-Mulas, C.; Delgado Jiménez, Y.; Sanmartín-Jiménez, O.; Garcés, J.R.; Rodrìguez-Prieto, M.A.; Alonso-Alonso, T.; Minano Medrano, R.; Lòpez-Estebaranz, J.L.; de Eusebio Murillo, E.; Redondo, P.; et al. Mohs micrographic surgery in the elderly: Comparison of tumours, surgery and first-year follow-up in patients younger and older than 80 years old in REGESMOHS. J. Eur. Acad. Dermatol. Venereol. 2018, 32, 108–112. [Google Scholar] [CrossRef] [PubMed]
- Mueller, C.K.; Nicolaus, K.; Thorwarth, M.; Schultze-Mosgau, S. Multivariate analysis of the influence of patient-, tumor-, and management-related factors on the outcome of surgical therapy for facial basal-cell carcinoma. Oral. Maxillofac. Surg. 2010, 14, 163–168. [Google Scholar] [CrossRef] [PubMed]
- Linos, E.; Chren, M.M.; Stijacic Cenzer, I.; Covinsky, K.E. Skin Cancer in U.S. Elderly Adults: Does Life Expectancy Play a Role in Treatment Decisions? J. Am. Geriatr. Soc. 2016, 64, 1610–1615. [Google Scholar] [CrossRef] [PubMed]
- Alam, M.; Nanda, S.; Mittal, B.B.; Kim, N.A.; Yoo, S. The use of brachytherapy in the treatment of nonmelanoma skin cancer: A review. J. Am. Acad. Dermatol. 2011, 65, 377–388. [Google Scholar] [CrossRef] [PubMed]
- Knox, J.M.; Lyles, T.W.; Shapiro, E.M.; Martin, R.D. Curettage and electrodesiccation in the treatment of skin cancer. Arch. Dermatol. 1960, 82, 197–204. [Google Scholar] [CrossRef] [PubMed]
- Silverman, M.K.; Kopf, A.W.; Grin, C.M.; Bart, R.S.; Levenstein, M.J. Recurrence rates of treated basal cell carcinomas: Part 2: Curettage-electrodessication. J. Dermatol. Surg. Oncol. 1991, 17, 720–726. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Vigil, T.; Vazquez-Lopez, F.; Perez-Oliva, N. Recurrence rates of primary basal cell carcinoma in facial risk areas treated with curettage and electrodesiccation. J. Am. Acad. Dermatol. 2007, 56, 91–95. [Google Scholar] [CrossRef]
- Freiman, A.; Bouganim, N. History of cryotherapy. Dermatol. Online J. 2005, 11, 9. [Google Scholar]
- Kokoszka, A.; Scheinfeld, N. Evidence-based review of use of cryosurgery in treatment of BCC. Dermatol. Surg. 2003, 29, 566–571. [Google Scholar]
- Har-Shai, Y.; Sommer, A.; Gil, T.; Krausz, J.; Gal-Or, N.; Mettanes, I.; Lavi, I.; Eyal, N.; Brizgalin, L.; Taran, A.; et al. Intralesional cryosurgery for the treatment of basal cell carcinoma of the lower extremities in elderly subjects: A feasibility study. Int. J. Dermatol. 2016, 55, 342–350. [Google Scholar] [CrossRef]
- Lien, M.H.; Sondak, V.K. Nonsurgical treatment options for basal cell carcinoma. J. Skin Cancer 2011, 2011, 571734. [Google Scholar] [CrossRef] [PubMed]
- Mirza, F.N.; Khatri, K.A. The use of lasers in the treatment of skin cancer: A review. J. Cosmet. Laser Ther. 2017, 19, 451–458. [Google Scholar] [CrossRef] [PubMed]
- Konnikov, N.; Avram, M.; Jarell, A.; Tannous, Z. Pulsed dye laser as a novel non-surgical treatment for basal cell carcinomas: Response and follow up 12–21 months after treatment. Lasers Surg. Med. 2011, 43, 72–78. [Google Scholar] [CrossRef] [PubMed]
- Zane, C.; Facchinetti, E.; Arisi, M.; Ortel, B.; Calzavara-Pinton, P. Pulsed CO2 laser ablation of superficial basal cell of limbs and trunk: A comparative randomized clinical trial with cryotherapy and surgical ablation. Dermatol. Surg. 2017, 43, 920–927. [Google Scholar] [CrossRef] [PubMed]
- Hibler, B.P.; Sierra, H.; Cordova, M.; Phillips, W.; Rajadhyaksha, M.; Nehal, K.S.; Rossi, A.M. Carbon dioxide laser ablation of basal cell carcinoma with visual guidance by reflectance confocal microscopy: A proof-of-principle pilot study. Br. J. Dermatol. 2016, 174, 1359–1364. [Google Scholar] [CrossRef] [PubMed]
- Hengge, U.R.; Ruzicka, T. Topical immunomodulation in dermatology: Potential of toll-like receptor agonists. Dermatol. Surg. 2004, 30, 1101–1112. [Google Scholar] [CrossRef]
- Tucci, M.; Passarelli, A.; Mannavola, F.; Felici, C.; Stucci, L.S.; Cives, M.; Silvestris, F. Immune System Evasion as Hallmark of Melanoma Progression: The Role of Dendritic Cells. Front. Oncol. 2019, 9, 1148. [Google Scholar] [CrossRef]
- Collier, N.J.; Haylett, A.K.; Wong, T.H.; Morton, C.A.; Ibbotson, S.H.; McKenna, K.E.; Mallipeddi, R.; Moseley, H.; Seukeran, D.; Ward, K.A.; et al. Conventional and combination topical photodynamic therapy for basal cell carcinoma: Systematic re-view and meta-analysis. Br. J. Dermatol. 2018, 179, 1277–1296. [Google Scholar] [CrossRef]
- Roozeboom, M.H.; Arits, A.H.; Mosterd, K.; Sommer, A.; Essers, B.A.; de Rooij, M.J.; Quaedvlieg, P.J.F.; Steijlen, P.M.; Nelemans, P.J.; Kelleners-Smeets, N.W.J. Three-year follow-up results of photodynamic therapy vs. Imiquimod vs. Fluorouracil for treatment ofsuperficial basal cell carcinoma: A single-blind, noninferiority, randomized controlled trial. J. Investig. Dermatol. 2016, 136, 1568–1574. [Google Scholar] [CrossRef]
- Varjosalo, M.; Taipale, J. Hedgehog: Functions and mechanisms. Genes Dev. 2008, 22, 2454–2472. [Google Scholar] [CrossRef]
- Le, H.; Kleinerman, R.; Lerman, O.Z.; Brown, D.; Galiano, R.; Gurtner, G.C.; Warren, S.M.; Levine, J.P.; Saadeh, P.B. Hedgehog signalling is essential for normal wound healing. Wound Repair Regen. 2008, 16, 768–773. [Google Scholar] [CrossRef] [PubMed]
- Youssef, K.K.; Van Keymeulen, A.; Lapouge, G.; Beck, B.; Michaux, C.; Achouri, Y.; Sotiropoulou, P.A.; Blanpain, C. Identification of the cell lineage at the origin of basal cell carcinoma. Nat. Cell Biol. 2010, 12, 299–305. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.Y.; Wang, J.; Mancianti, M.L.; Epstein, E.H. Basal cell carcinomas arise from hair follicle stem cells in Ptch1(±) mice. Cancer Cell 2011, 19, 114–124. [Google Scholar] [CrossRef] [PubMed]
- Epstein, E.H. Basal cell carcinomas: Attack of the hedgehog. Nat. Rev. Cancer 2008, 8, 743–754. [Google Scholar] [CrossRef] [PubMed]
- Cazet, A.S.; Hui, M.N.; Elsworth, B.L.; Wu, S.Z.; Roden, D.; Chan, C.L.; Skhinas, J.N.; Collot, R.; Yang, J.; Harvey, K.; et al. Targeting stromal remodeling and cancer stem cell plasticity overcomes chemoresistance in triple negative breast cancer. Nat. Commun. 2018, 9, 2897. [Google Scholar] [CrossRef]
- Kinzler, K.W.; Vogelstein, B. The GLI Gene Encodes a Nuclear Protein Which Binds Specific Sequences in the Human Genome. Mol. Cell. Biol. 1990, 10, 634–642. [Google Scholar] [CrossRef] [PubMed]
- Sasaki, H.; Hui, C.; Nakafuku, M.; Kondoh, H. A Binding Site for Gli Proteins Is Essential for HNF-3beta Floor Plate Enhancer Activity in Transgenics and Can Respond to Shh In Vitro. Development 1997, 124, 1313–1322. [Google Scholar] [PubMed]
- Altaraihi, M.; Wadt, K.; Ek, J.; Gerdes, A.M.; Ostergaard, E. A healthy individual with a homozygous PTCH2 frameshift variant: Are variants of PTCH2 associated with nevoid basal cell carcinoma syndrome? Hum. Genome Var. 2019, 6, 10. [Google Scholar] [CrossRef]
- Ling, G.; Ahmadian, A.; Persson, A.; Undén, A.B.; Afink, G.; Williams, C.; Uhlén, M.; Toftgard, R.; Lundeberg, J.; Pontén, F. PATCHED and p53 gene alterations in sporadic and hereditary basal cell cancer. Oncogene 2001, 20, 7770–7778. [Google Scholar] [CrossRef]
- Di Magno, L.; Coni, S.; Di Marcotullio, L.; Canettieri, G. Digging a hole under Hedgehog: Downstream inhibition as an emerging anticancer strategy. Biochim. Biophys. Acta 2015, 1856, 62–72. [Google Scholar] [CrossRef]
- Sekulic, A.; Migden, M.R.; Oro, A.E.; Dirix, L.; Lewis, K.D.; Hainsworth, J.D.; Solomon, J.A.; Yoo, S.; Arron, S.T.; Friedlandre, P.A.; et al. Efficacy and safety of vismodegib in advanced basal-cell carcinoma. N. Engl. J. Med. 2012, 366, 2171–2179. [Google Scholar] [CrossRef] [PubMed]
- Sekulic, A.; Migden, M.R.; Basset-Seguin, N.; Garbe, C.; Gesierich, A.; Lao, C.D.; Miller, C.; Mortier, L.; Murrell, D.F.; Hamid, O.; et al. Long-term safety and efficacy of vismodegib in patients with advanced basal cell carcinoma: Final update of the pivotal ERIVANCE BCC study. BMC Cancer 2017, 17, 332. [Google Scholar] [CrossRef] [PubMed]
- Basset-Seguin, N.; Hauschild, A.; Kunstfeld, R.; Grob, J.; Dréno, B.; Mortier, L.; Ascierto, P.A.; Licitra, L.; Dutriaux, C.; Thomas, L.; et al. Vismodegib in patients with advanced basal cell carcinoma: Primary analysis of STEVIE, an international, open-label trial. Eur. J. Cancer 2017, 86, 334–348. [Google Scholar] [CrossRef] [PubMed]
- Dreno, B.; Kunstfeld, R.; Hauschild, A.; Kosko, S.; Zloty, D.; Labeille, B.; Grob, J.-J.; Puig, S.; Gilberg, F.; Bergstrom, D.; et al. Two intermittent vismodegib dosing regimens in patients with multiple basal-cell carcinomas (MIKIE): A randomised, regimen-controlled, double-blind, phase 2 trial. Lancet Oncol. 2017, 18, 404–412. [Google Scholar] [CrossRef]
- Morinello, E.; Pignatello, M.; Villabruna, L.; Goelzer, P.; Burgin, H. Embryofetal development study of vismodegib, a hedgehog pathway inhibitor, in rats. Birth Defects Res. B Dev. Reprod. Toxicol. 2014, 101, 135–143. [Google Scholar] [CrossRef] [PubMed]
- Alfieri, S.; Bergamini, C.; Granata, R.; Locati, L.; Licitra, L.; Bossi, P. Retreatment with vismodegib after progression in advanced basal cell carcinoma: First-time report of a single-institution experience. Target. Oncol. 2018, 13, 253–256. [Google Scholar] [CrossRef]
- Pan, S.; Wu, X.; Jiang, J.; Gao, W.; Wan, Y.; Cheng, D.; Han, D.; Liu, J.; Englund, N.P.; Wang, Y.; et al. Discovery of NVP- LDE225, a potent and selective smoothened antagonist. ACS Med. Chem. Lett. 2010, 1, 130–134. [Google Scholar] [CrossRef]
- Rodon, J.; Tawbi, H.A.; Thomas, A.L.; Stoller, R.G.; Turtschi, C.P.; Baselga, J.; Sarantopoulos, J.; Mahalingam, D.; Shou, Y.; Moles, M.A.; et al. A phase I, multicenter, open-label, first-in-human, dose escalation study of the oral smoothened inhibitor Sonidegib (LDE225) in patients with advanced solid tumors. Clin. Cancer Res. 2014, 20, 1900–1909. [Google Scholar] [CrossRef]
- Migden, M.R.; Guminski, A.; Gutzmer, R.; Gutzmer, R.; Dirix, L.; Lewis, K.D.; Combemale, P.; Herd, R.M.; Kudchadkar, R.; Trefzer, U.; et al. Treatment with two dif- ferent doses of sonidegib in patients with locally advanced or metastatic basal cell carcinoma (BOLT): A multicentre, randomised, double-blind phase 2 trial. Lancet Oncol. 2015, 16, 716–728. [Google Scholar] [CrossRef]
- Lear, J.T.; Migden, M.R.; Lewis, K.D.; Chang, A.L.S.; Guminski, A.; Gutzmer, R.; Dirix, L.; Combemale, P.; Stratigos, A.; Plummer, R.; et al. Long-term efficacy and safety of sonidegib in patients with locally advanced and metastatic basal cell carcinoma: 30-month analysis of the randomized phase 2 BOLT study. J. Eur. Acad. Dermatol. Venereol. 2018, 32, 372–381. [Google Scholar] [CrossRef]
- Odom, D.; Mladsi, D.; Purser, M.; Kaye, J.A.; Palaka, E.; Charter, A.; Jensen, J.A.; Sellami, D. A matching- adjusted indirect comparison of sonidegib and vismodegib in advanced basal cell carcinoma. J. Skin Cancer 2017, 2017, 6121760. [Google Scholar] [CrossRef] [PubMed]
- Dummer, R.; Guminksi, A.; Gutzmer, R.; Lear, J.T.; Lewis, K.D.; Chang, A.L.S.; Combemale, P.; Dirix, L.; Kaatz, M.; Kudchadkar, R.; et al. Long-term efficacy and safety of sonidegib in patients with advanced basal cell carcinoma: 42-month analysis of the phase II randomized, double-blind BOLT study. Br. J. Dermatol. 2020, 182, 1369–1378. [Google Scholar] [CrossRef] [PubMed]
- Otsuka, A.; Dreier, J.; Cheng, P.F.; Nageli, M.; Lehmann, H.; Felderer, L.; Frew, I.J.; Matsushita, S.; Levesque, M.P.; Dummer, R. Hedgehog pathway inhibitors promote adaptive immune responses in basal cell carcinoma. Clin. Cancer Res. 2015, 21, 1289–1297. [Google Scholar] [CrossRef] [PubMed]
- Chang, A.L.S.; Lewis, K.D.; Arron, S.T.; Migden, M.R.; Solomon, J.A.; Yoo, S.; Day, B.-M.; McKenna, E.F.; Sekulic, A. Safety and efficacy of vismodegib in patients aged ≥65 years with advanced basal cell carcinoma. Oncotarget 2016, 7, 76118–76124. [Google Scholar] [CrossRef] [PubMed]
- Maul, L.V.; Kähler, K.C.; Hauschild, A. Effective and tolerable treatment of advanced basal cell carcinoma with Vismodegib despite renal insufficiency. JAMA Dermatol. 2016, 152, 1387–1388. [Google Scholar] [CrossRef]
- Spallone, G.; Sollena, P.; Ventura, A.; Fargnoli, M.C.; Gutierrez, C.; Piccerillo, A.; Tambone, S.; Bianchi, L.; Peris, K. Efficacy and safety of Vismodegib treatment in patients with advanced basal cell carcinoma and multiple comorbidities. Dermatol. Ther. 2019, 32, e13108. [Google Scholar] [CrossRef]
- Castillo, J.M.; Knol, A.C.; Nguyen, J.M.; Khammari, A.; Saint-Jean, M.; Dreno, B. Immunohistochemical markers of advanced basal cell carcinoma: CD56 is associated with a lack of response to vismodegib. Eur. J. Dermatol. 2016, 26, 452–459. [Google Scholar] [CrossRef]
- Sternfeld, A.; Rosenwasser-Weiss, S.; Ben-Yehuda, G.; Kreizman Shefer, H.; Friedman-Gohas, M.; Yassur, I.; Tauber, G.; Bejar, J.; Olshinka, A.; Vardizer, Y.; et al. Gene-Related Response of Basal Cell Carcinoma to Biologic Treatment with Vismodegib. Sci. Rep. 2020, 10, 1244. [Google Scholar] [CrossRef]
- Tucci, M.; Passarelli, A.; Mannavola, F.; Stucci, L.S.; Ascierto, P.A.; Capone, M.; Madonna, G.; Lopalco, P.; Silvestris, F. Serum exosomes as predictors of clinical response to ipilimumab in metastatic melanoma. Oncoimmunology 2017, 7, e1387706. [Google Scholar] [CrossRef]
- Passarelli, A.; Mannavola, F.; Stucci, L.S.; Tucci, M.; Silvestris, F. Immune system and melanoma biology: A balance between immuno- surveillance and immune escape. Oncotarget 2017, 8, 106132–106142. [Google Scholar] [CrossRef]
- Goodman, A.M.; Kato, S.; Bazhenova, L.; Patel, S.P.; Frampton, G.M.; Miller, V.; Stephens, P.J.; Daniels, G.A.; Kurzrock, R. Tumor mutational burden as an independent predictor of response to immunotherapy in diverse cancers. Mol. Cancer Ther. 2017, 16, 2598–2608. [Google Scholar] [CrossRef] [PubMed]
- Ikeda, S.; Goodman, A.M.; Cohen, P.R.; Jensen, T.J.; Ellison, C.K.; Frampton, G.; Miller, V.; Patel, S.P.; Kurzrock, R. Metastatic basal cell carcinoma with amplification of PD-L1: Exceptional response to anti-PD1 therapy. NPJ Genom. Med. 2016, 1, 16037. [Google Scholar] [CrossRef] [PubMed]
- Goodman, A.M.; Kato, S.; Cohen, P.R.; Boichard, A.; Frampton, G.; Miller, V.; Stephens, P.J.; Daniels, G.A.; Kurzrock, R. Genomic landscape of advanced basal cell carcinoma: Implications for precision treatment with targeted and immune therapies. Oncoimmunology 2019, 7, e1404217. [Google Scholar] [CrossRef] [PubMed]
- Gutzmer, R.; Solomon, J.A. Hedgehog Pathway Inhibition for the Treatment of Basal Cell Carcinoma. Target. Oncol. 2019, 14, 253–267. [Google Scholar] [CrossRef] [PubMed]
- Passarelli, A.; Tucci, M.; Mannavola, F.; Felici, C.; Silvestris, F. The metabolic milieu in melanoma: Role of immune suppression by CD73/adenosine. Tumor Biol. 2019, 42. [Google Scholar] [CrossRef] [PubMed]
- Passarelli, A.; Aieta, M.; Sgambato, A.; Gridelli, C. Targeting Immunometabolism Mediated by CD73 Pathway in EGFR-Mutated Non-small Cell Lung Cancer: A New Hope for Overcoming Immune Resistance. Front. Immunol. 2020, 11, 1479. [Google Scholar] [CrossRef]
- Hanahan, D.; Weinberg, R.A. Hallmarks of cancer: The next generation. Cell 2011, 144, 646–674. [Google Scholar] [CrossRef]
- Sabbatino, F.; Marra, A.; Liguori, L.; Scognamiglio, G.; Fusciello, C.; Botti, G.; Ferrone, S.; Pepe, S. Resistance to anti-PD-1-based immunotherapy in basal cell carcinoma: A case report and review of the literature. J. Immunother. Cancer 2018, 6, 126. [Google Scholar] [CrossRef]
| Results | Primary Analysis (Follow up 9 Months) | Long Term Analysis (Follow up 39 Months) | ||
|---|---|---|---|---|
| mBCC (n = 33) | laBCC (n = 63) | mBCC (n = 33) | laBCC (n = 63) | |
| ORR n (%) (95%CI) | 15 (45.5) (28.1–62.2) | 38(60.3) (47.2–71.7) | 16(48.5) (30.8–66.2) | 38(60.3) (47.2–71.7) |
| CR | 0 | 20 | 0 | 20 |
| PR | 15 | 18 | 16 | 18 |
| SD | 15 | 15 | 14 | 15 |
| PD | 2 | 6 | 2 | 6 |
| Median DOR, m (95%CI) | 12.9 (5.6–12.9) | 7.6 (7.4–NE) | 14.8 (5.6–17.0) | 26.2 (9.0–37.6) |
| Median PFS, m (95%CI] | 9.2 (7.4–NE] | 11.3 (9.5–16.8] | 9.3 (7.4–16.6) | 12.9 (10.2–28.0) |
| Median OS, m(95%CI) | NE (13.9–NE) | NE (17.6–NE) | 33.4 (18.1–NE) | NE (NE) |
| 1 year OS % | 75.5 (57.3–93.6) | 91.6 (83.5–99.7) | 78.7 (64.7–92.7) | 93.2 (86.8–99.6) |
| 2 year OS % | NE | NE | 62.3 (45.4–79.3) | 85.5 (76.1–94.8) |
| Results | Locally Advanced BCC | Metastatic BCC | Total |
|---|---|---|---|
| Response rate n (%) [95%CI] | 738 (68.5) [65.66–71.29] | 31 (36.9) [26.63–48.13] | 769 (66.2) [63.43–68.96] |
| Complete response, n (%) | 360 (33.4) | 4 (4.8) | 364 (31.4) |
| Partial response, n (%) | 378 (35.1) | 27 (32.1) | 405 (34.9) |
| Stable disease, n (%) | 270 (25.1) | 39 (46.4) | 309 (26.6) |
| Progressive disease, n (%) | 21 (1.9) | 9 (10.7) | 30 (2.6) |
| Missing or not evaluable, n (%) | 48 (4.5) | 5 (6.0) | 53 (4.6) |
| Median time to response, n | 1077 | 84 | 1161 |
| months (95% CI) | 3.7 (2.9–3.7) | NE (5.5-NE) | 3.7 (3.5–3.7) |
| Median duration of response, n | 738 | 31 | 175 |
| months (95% CI) | 23.0 (20.4–26.7) | 13.9 (9.2-NE) | 22.7 (20.3–24.8) |
| Median progression-free survival, n | 1103 | 89 | 1192 |
| months (95% CI) | 23.2 (21.4–26.0) | 13.1 (12–0-17.7) | 22.1 (20.3–24.7) |
| ERIVANCE BCC (N = 104) | EAS (N = 119) | |||||||
|---|---|---|---|---|---|---|---|---|
| laBCC | mBCC | laBCC | mBCC | |||||
| ≥65 years | <65 years | ≥65 years | <65 years | ≥65 years | <65 years | ≥65 years | <65 years | |
| (n = 33) | (n = 38) | (n = 14) | (n = 19) | (n = 27) | (n = 35) | (n = 26) | (n = 31) | |
| Median age, years | 75 | 50.5 | 71.5 | 53 | 77 | 53 | 71.5 | 55 |
| ECOG PS, n (%) | ||||||||
| 0 | 22 (66.7) | 29 (76.3) | 5 (53.7) | 8 (42.1) | 12 (44.4) | 27 (77.1) | 14 (53.8) | 16 (51.6) |
| 1 | 7 (21.2) | 8 (21.1) | 9 (64.3) | 10 (52.6) | 12 (44.4) | 7 (20.0) | 10 (38.5) | 12 (38.7) |
| 2 | 4 (12.1) | 1 (2.6) | 0 | 1 (5.3) | 3 (11.1) | 1 (2.9) | 2 (7.7) | 3 (9.7) |
| Prior treatment, n (%) | ||||||||
| Surgery | 27 (81.8) | 35 (92.1) | 14 (100) | 18 (94.7) | 25 (92.6) | 32 (91.4) | 25 (96.2) | 29 (93.5) |
| Radiotherapy | 13 (39.4) | 9 (23.7) | 9 (64.3) | 10 (52.6) | 11 (40.7) | 9 (25.7) | 18 (69.2) | 17 (54.8) |
| Systemic therapy | 2 (6.1) | 6 (15.8) | 2 (14.3) | 8 (42.1) | 7 (25.9) | 4 (11.4) | 7 (26.9) | 13 (41.9) |
| Surgery contraindicated, n (%) | 14 (42.4) | 29 (76.3) | NA | NA | 18 (66.7) | 17 (48.6) | NA | NA |
| ERIVANCE BCC (N = 96) | EAS (N = 95) | |||||||
|---|---|---|---|---|---|---|---|---|
| laBCC | mBCC | laBCC | mBCC | |||||
| ≥65 years | <65 years | ≥65 years | <65 years | ≥65 years | <65 years | ≥65 years | <65 years | |
| (n = 30) | (n = 33) | (n = 14) | (n = 19) | (n = 24) | (n = 32) | (n = 18) | (n = 21) | |
| BORR, n (%) | 14 (46.7) | 24 (72.7) | 5 (35.7) | 10 (52.6) | 11 (45.8) | 15 (46.9) | 6 (33.3) | 6 (28.6) |
| Complete response | 8 (26) | 12 (36) | 0 | 0 | 2 (8) | 4 (12) | 1 (6) | 1 (5) |
| Partial response | 6 (20) | 12 (36) | 5 (36) | 10 (53) | 9 (38) | 11 (34) | 5 (28) | 5 (24) |
| Stable disease | 11 (37) | 4 (12) | 7 (50) | 8 (42) | 12 (50) | 15 (47) | 9 (50) | 11 (52) |
| Progressive disease | 2 (7) | 4 (12) | 1 (7) | 1 (5) | 0 | 0 | 1 (6) | 2 (10) |
| Not evaluable/missing | 3 (10) | 1 (3) | 1 (7) | 0 | 1 (4) | 2 (6) | 2 (11) | 2 (10) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Passarelli, A.; Galdo, G.; Aieta, M.; Fabrizio, T.; Villonio, A.; Conca, R. A Vismodegib Experience in Elderly Patients with Basal Cell Carcinoma: Case Reports and Review of the Literature. Int. J. Mol. Sci. 2020, 21, 8596. https://doi.org/10.3390/ijms21228596
Passarelli A, Galdo G, Aieta M, Fabrizio T, Villonio A, Conca R. A Vismodegib Experience in Elderly Patients with Basal Cell Carcinoma: Case Reports and Review of the Literature. International Journal of Molecular Sciences. 2020; 21(22):8596. https://doi.org/10.3390/ijms21228596
Chicago/Turabian StylePassarelli, Anna, Giovanna Galdo, Michele Aieta, Tommaso Fabrizio, Antonio Villonio, and Raffaele Conca. 2020. "A Vismodegib Experience in Elderly Patients with Basal Cell Carcinoma: Case Reports and Review of the Literature" International Journal of Molecular Sciences 21, no. 22: 8596. https://doi.org/10.3390/ijms21228596
APA StylePassarelli, A., Galdo, G., Aieta, M., Fabrizio, T., Villonio, A., & Conca, R. (2020). A Vismodegib Experience in Elderly Patients with Basal Cell Carcinoma: Case Reports and Review of the Literature. International Journal of Molecular Sciences, 21(22), 8596. https://doi.org/10.3390/ijms21228596





