Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options
Abstract
1. Introduction
2. Clinical Risk Factors
3. Biological Risk Factors
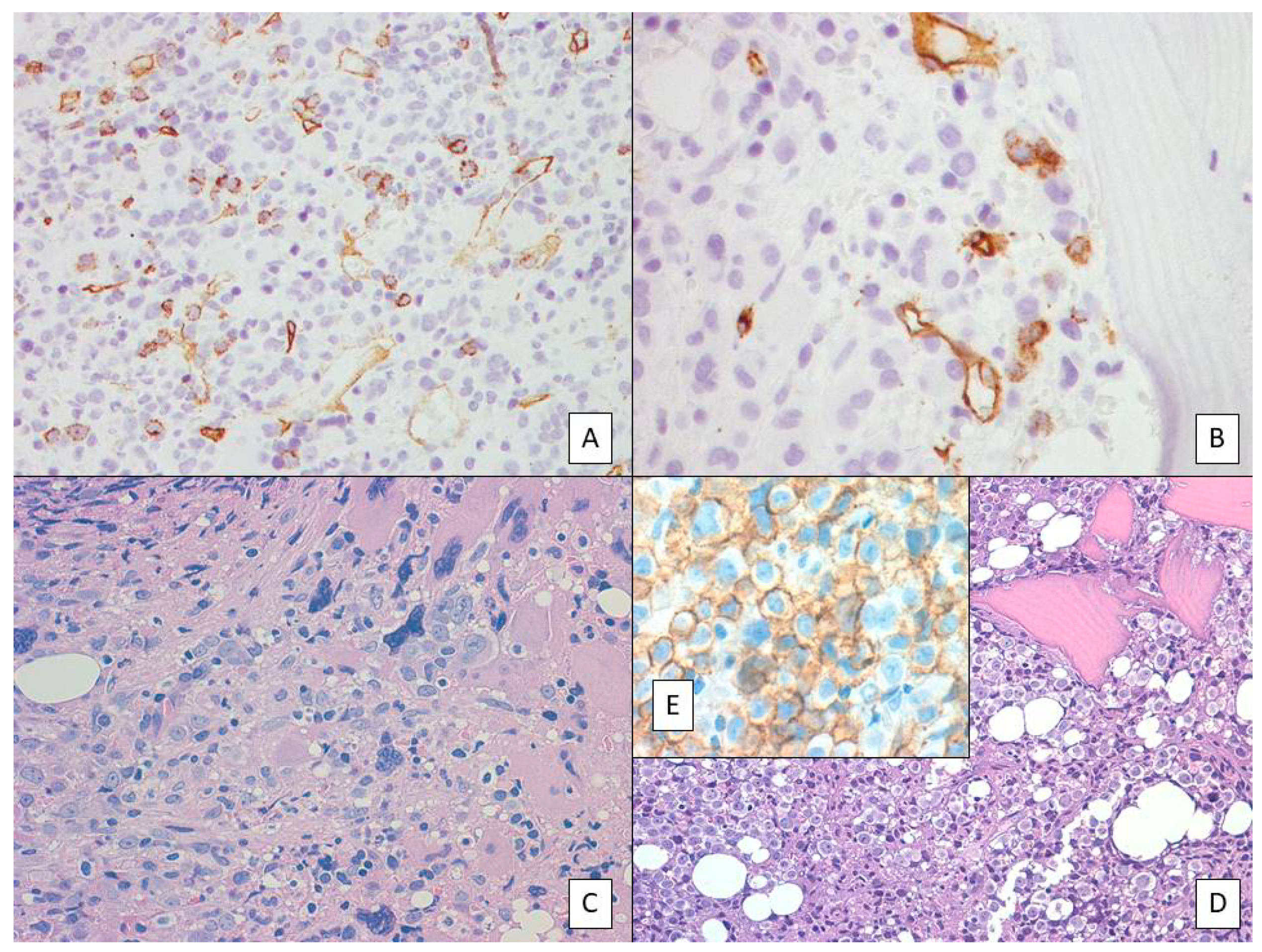
4. Morphological and Histological Characteristics of MPN Progression
5. Karyotype
6. Molecular Profile
7. Therapy
8. Supportive Therapy
9. Hypomethylating Agents
9.1. Azacitidine
9.2. Decitabine
10. Other Therapies
11. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Arber, D.A.; Orazi, A.; Hasserjian, R.; Thiele, J.; Borowitz, M.J.; Le Beau, M.M.; Bloomfield, C.D.; Cazzola, M.; Vardiman, J.W. The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 2016, 127, 2391–2405. [Google Scholar] [CrossRef] [PubMed]
- Tefferi, A.; Guglielmelli, P.; Larson, D.R.; Finke, C.; Wassie, E.A.; Pieri, L.; Gangat, N.; Fjerza, R.; Belachew, A.A.; Lasho, T.L.; et al. Long-term survival and blast transformation in molecularly annotated essential thrombocythemia, polycythemia vera, and myelofibrosis. Blood 2014, 124, 2507–2513. [Google Scholar] [CrossRef] [PubMed]
- Noor, S.J.; Tan, W.; Wilding, G.E.; Ford, L.A.; Barcos, M.; Sait, S.N.; Block, A.W.; Thompson, J.E.; Wang, E.S.; Wetzler, M.; et al. Myeloid blastic transformation of myeloproliferative neoplasms—A review of 112 cases. Leuk. Res. 2011, 35, 608–613. [Google Scholar] [CrossRef]
- Abdulkarim, K.; Girodon, F.; Johansson, P.; Maynadié, M.; Kutti, J.; Carli, P.M.; Bovet, E.; Andréasson, B. AML transformation in 56 patients with Ph- MPD in two well defined populations. Eur. J. Haematol. 2009, 82, 106–111. [Google Scholar] [CrossRef] [PubMed]
- Cervantes, F.; Tassies, D.; Salgado, C.; Rovira, M.; Pereira, A.; Rozman, C. Acute transformation in nonleukemic chronic myeloproliferative disorders: Actuarial probability and main characteristics in a series of 218 patients. Acta Haematol. 1991, 85, 124–127. [Google Scholar] [CrossRef] [PubMed]
- Tam, C.S.; Nussenzveig, R.M.; Popat, U.; Bueso-Ramos, C.E.; Thomas, D.A.; Cortes, J.A.; Champlin, R.E.; Ciurea, S.E.; Manshouri, T.; Pierce, S.M.; et al. The natural history and treatment outcome of blast phase BCR-ABL—Myeloproliferative neoplasms. Blood 2008, 112, 1628–1637. [Google Scholar] [CrossRef] [PubMed]
- Passamonti, F.; Rumi, E.; Arcaini, L.; Boveri, E.; Elena, C.; Pietra, D.; Boggi, S.; Astori, C.; Bernasconi, P.; Varettoni, M.; et al. Prognostic factors for thrombosis, myelofibrosis, and leukemia in essential thrombocythemia: A study of 605 patients. Haematologica 2008, 93, 1645–1651. [Google Scholar] [CrossRef]
- Chim, C.S.; Kwong, Y.L.; Lie, A.K.; Ma, S.K.; Chan, C.C.; Wong, L.G.; Kho, B.C.; Lee, H.K.; Sim, J.P.; Chan, C.H.; et al. Long-term outcome of 231 patients with essential thrombocythemia: Prognostic factors for thrombosis, bleeding, myelofibrosis, and leukemia. Arch. Intern. Med. 2005, 165, 2651–2658. [Google Scholar] [CrossRef] [PubMed]
- Girodon, F.; Dutrillaux, F.; Broséus, J.; Mounier, M.; Goussot, V.; Bardonnaud, P.; Chrétien, M.L.; Maynadié, M. Leukocytosis is associated with poor survival but not with increased risk of thrombosis in essential thrombocythemia: A population-based study of 311 patients. Leukemia 2010, 24, 900–903. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Cervantes, F.; Alvarez-Larrán, A.; Talarn, C.; Gómez, M.; Montserrat, E. Myelofibrosis with myeloid metaplasia following essential thrombocythaemia: Actuarial probability, presenting characteristics and evolution in a series of 195 patients. Br. J. Haematol. 2002, 118, 786–790. [Google Scholar] [CrossRef]
- Barbui, T.; Thiele, J.; Passamonti, F.; Rumi, E.; Boveri, E.; Ruggeri, M.; Rodeghiero, F.; d’Amore, E.S.; Randi, M.L.; Bertozzi, I.; et al. Survival and disease progression in essential thrombocythemia are significantly influenced by accurate morphologic diagnosis: An international study. J. Clin. Oncol. 2011, 29, 3179–3184. [Google Scholar] [CrossRef]
- Passamonti, F.; Rumi, E.; Pungolino, E.; Malabarba, L.; Bertazzoni, P.; Valentini, M.; Orlandi, E.; Arcaini, L.; Brusamolino, E.; Pascutto, C.; et al. Life expectancy and prognostic factors for survival in patients with polycythemia vera and essential thrombocythemia. Am. J. Med. 2004, 117, 755–761. [Google Scholar] [CrossRef]
- Tallarico, M.; Odenike, O. Secondary acute myeloid leukemias arising from philadelphia chromosome negative myeloproliferative neoplasms: Pathogenesis, risk factors, and therapeutic strategies. Curr. Hematol. Malig. Rep. 2015, 10, 112–117. [Google Scholar] [CrossRef]
- Huang, J.; Li, C.Y.; Mesa, R.A.; Wu, W.; Hanson, C.A.; Pardanani, A.; Tefferi, A. Risk factors for leukemic transformation in patients with primary myelofibrosis. Cancer 2008, 112, 2726–2732. [Google Scholar] [CrossRef]
- Dupriez, B.; Morel, P.; Demory, J.L.; Lai, J.L.; Simon, M.; Plantier, I.; Bauters, F. Prognostic factors in agnogenic myeloid metaplasia: A report on 195 cases with a new scoring system. Blood 1996, 88, 1013–1018. [Google Scholar] [PubMed]
- Passamonti, F.; Rumi, E.; Elena, C.; Arcaini, L.; Merli, M.; Pascutto, C.; Cazzola, M.; Lazzarino, M. Incidence of leukaemia in patients with primary myelofibrosis and RBC-transfusion dependence. Br. J. Haematol. 2010, 150, 719–721. [Google Scholar] [CrossRef]
- Tefferi, A.; Vaidya, R.; Caramazza, D.; Finke, C.; Lasho, T.; Pardanani, A. Circulating interleukin (IL)-8, IL-2R, IL-12, and IL-15 levels are independently prognostic in primary myelofibrosis: Comprehensive cytokine profiling study. J. Clin. Oncol. 2011, 29, 1356–1363. [Google Scholar] [CrossRef]
- Barbui, T.; Carobbio, A.; Finazzi, G.; Guglielmelli, P.; Salmoiraghi, S.; Rosti, V.; Rambaldi, A.; Vannucchi, A.M.; Barosi, G. Elevated C-reactive protein is associated with shortened leukemia-free survival in patients with myelofibrosis. Leukemia 2013, 27, 2084–2086. [Google Scholar] [CrossRef]
- Gangat, N.; Caramazza, D.; Vaidya, R.; George, G.; Begna, K.; Schwager, S.; Van Dyke, D.; Hanson, C.; Wu, W.; Pardanani, A.; et al. DIPSS plus: A refined Dynamic International Prognostic Scoring System for primary myelofibrosis that incorporates prognostic information from karyotype, platelet count, and transfusion status. J. Clin. Oncol. 2011, 29, 392–397. [Google Scholar] [CrossRef] [PubMed]
- Vaidya, R.; Caramazza, D.; Begna, K.H.; Gangat, N.; Van Dyke, D.L.; Hanson, C.A.; Pardanani, A.; Tefferi, A. Monosomal karyotype in primary myelofibrosis is detrimental to both overall and leukemia-free survival. Blood 2011, 117, 5612–5615. [Google Scholar] [CrossRef][Green Version]
- Finazzi, G.; Caruso, V.; Marchioli, R.; Capnist, G.; Chisesi, T.; Finelli, C.; Gugliotta, L.; Landolfi, R.; Kutti, J.; Gisslinger, H.; et al. ECLAP Investigators. Acute leukemia in polycythemia vera: An analysis of 1638 patients enrolled in a prospective observational study. Blood 2005, 105, 2664–2670. [Google Scholar] [CrossRef] [PubMed]
- Berk, P.D.; Wasserman, L.R.; Fruchtman, S.M.; Goldberg, J.D. Treatment of polycythemia vera: A summary of clinical trials conducted by the Polycythemia Vera Study Group. In Polycythemia Vera and the Myeloproliferative Disorders; Wasserman, L.R., Berk, P.D., Berlin, N.I., Eds.; WB Saunders: Philadelphia, PA, USA, 1995; pp. 166–194. [Google Scholar]
- Tefferi, A.; Rumi, E.; Finazzi, G.; Gisslinger, H.; Vannucchi, A.M.; Rodeghiero, F.; Randi, M.L.; Vaidya, R.; Cazzola, M.; Rambaldi, A.; et al. Survival and prognosis among 1545 patients with contemporary polycythemia vera: An international study. Leukemia 2013, 27, 1874–1881. [Google Scholar] [CrossRef]
- Marchioli, R.; Finazzi, G.; Landolfi, R.; Kutti, J.; Gisslinger, H.; Patrono, C.; Marilus, R.; Villegas, A.; Tognoni, G.; Barbui, T. Vascular and neoplastic risk in a large cohort of patients with polycythemia vera. J. Clin. Oncol. 2005, 23, 2224–2232. [Google Scholar] [CrossRef]
- Gangat, N.; Strand, J.; Li, C.Y.; Wu, W.; Pardanani, A.; Tefferi, A. Leucocytosis in polycythaemia vera predicts both inferior survival and leukaemic transformation. Br. J. Haematol. 2007, 138, 354–358. [Google Scholar] [CrossRef]
- Gangat, N.; Wolanskyj, A.P.; McClure, R.F.; Li, C.Y.; Schwager, S.; Wu, W.; Tefferi, A. Risk stratification for survival and leukemic transformation in essential thrombocythemia: A single institutional study of 605 patients. Leukemia 2007, 21, 270–276. [Google Scholar] [CrossRef]
- Palandri, F.; Catani, L.; Testoni, N.; Ottaviani, E.; Polverelli, N.; Fiacchini, M.; De Vivo, A.; Salmi, F.; Lucchesi, A.; Baccarani, M.; et al. Long-term follow-up of 386 consecutive patients with essential thrombocythemia: Safety of cytoreductive therapy. Am. J. Hematol. 2009, 84, 215–220. [Google Scholar] [CrossRef]
- Vannucchi, A.M.; Lasho, T.L.; Guglielmelli, P.; Biamonte, F.; Pardanani, A.; Pereira, A.; Finke, C.; Score, J.; Gangat, N.; Mannarelli, C.; et al. Mutations and prognosis in primary myelofibrosis. Leukemia 2013, 27, 1861–1869. [Google Scholar] [CrossRef] [PubMed]
- Tefferi, A.; Guglielmelli, P.; Lasho, T.L.; Rotunno, G.; Finke, C.; Mannarelli, C.; Belachew, A.A.; Pancrazzi, A.; Wassie, E.A.; Ketterling, R.P.; et al. CALR and ASXL1 mutations-based molecular prognostication in primary myelofibrosis: An international study of 570 patients. Leukemia 2014, 28, 1494–1500. [Google Scholar] [CrossRef]
- Tefferi, A.; Lasho, T.; Finke, C.; Elala, Y.; Hanson, C.A.; Ketterling, R.P.; Gangat, N.; Pardanani, A. Targeted deep sequencing in primary myelofibrosis. Blood Adv. 2016, 1, 105–111. [Google Scholar] [CrossRef] [PubMed]
- Tefferi, A.; Lasho, T.L.; Abdel-Wahab, O.; Guglielmelli, P.; Patel, J.; Caramazza, D.; Pieri, L.; Finke, C.M.; Kilpivaara, O.; Wadleigh, M.; et al. IDH1 and IDH2 mutation studies in 1473 patients with chronic-, fibrotic- or blast-phase essential thrombocythemia, polycythemia vera or myelofibrosis. Leukemia 2010, 24, 1302–1309. [Google Scholar] [CrossRef] [PubMed]
- Pardanani, A.; Lasho, T.L.; Finke, C.M.; Mai, M.; McClure, R.F.; Tefferi, A. IDH1 and IDH2 mutation analysis in chronic- and blast-phase myeloproliferative neoplasms. Leukemia 2010, 24, 1146–1151. [Google Scholar] [CrossRef] [PubMed]
- Tefferi, A.; Lasho, T.; Guglielmelli, P.; Finke, C.M.; Rotunno, G.; Elala, Y.; Pacilli, A.; Hanson, C.A.; Pancrazzi, A.; Ketterling, R.P.; et al. Targeted deep sequencing in polycythemia vera and essential thrombocythemia. Blood Adv. 2016, 1, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Thiele, J.; Kvasnicka, H.M. Hematopathologic findings in chronic idiopathic myelofibrosis. Semin. Oncol. 2005, 32, 380–394. [Google Scholar] [CrossRef] [PubMed]
- Thiele, J.; Kvasnicka, H.M.; Diehl, V. Bone marrow CD34+ progenitor cells in Philadelphia chromosome-negative chronic myeloproliferative disorders—A clinicopathological study on 575 patients. Leuk. Lymphoma 2005, 46, 709–715. [Google Scholar] [CrossRef]
- Orazi, A.; O’Malley, D.P.; Jiang, J.; Vance, G.H.; Thomas, J.; Czader, M.; Fang, W.; An, C.; Banks, P.M. Acute panmyelosis with myelofibrosis: An entity distinct from acute megakaryoblastic leukemia. Mod. Pathol. 2005, 18, 603–614. [Google Scholar] [CrossRef] [PubMed]
- Geyer, J.T.; Margolskee, E.; Boiocchi, L.; Hasserjian, R.P.; Gianelli, U.; Orazi, A. Disease Progression in Myeloproliferative Neoplasms: Revisiting the Criteria for “Accelerated Phase”. Mod. Pathol. 2018, 31, 517. [Google Scholar]
- Boiocchi, L.; Espinal-Witter, R.; Geyer, J.T.; Steinhilber, J.; Bonzheim, I.; Knowles, D.M.; Fend, F.; Orazi, A. Development of monocytosis in patients with primary myelofibrosis indicates an accelerated phase of the disease. Mod. Pathol. 2013, 26, 204–212. [Google Scholar] [CrossRef]
- Boiocchi, L.; Gianelli, U.; Iurlo, A.; Fend, F.; Bonzheim, I.; Cattaneo, D.; Knowles, D.M.; Orazi, A. Neutrophilic leukocytosis in advanced stage polycythemia vera: hematopathologic features and prognostic implications. Mod. Pathol. 2015, 28, 1448–1457. [Google Scholar] [CrossRef] [PubMed]
- Tefferi, A.; Nicolosi, M.; Mudireddy, M.; Lasho, T.L.; Gangat, N.; Begna, K.H.; Hanson, C.A.; Ketterling, R.P.; Pardanani, A. Revised cytogenetic risk stratification in primary myelofibrosis: Analysis based on 1002 informative patients. Leukemia 2018, 32, 1189–1199. [Google Scholar] [CrossRef]
- Campbell, P.J.; Baxter, E.J.; Beer, P.A.; Scott, L.M.; Bench, A.J.; Huntly, B.J.; Erber, W.N.; Kusec, R.; Larsen, T.S.; Giraudier, S.; et al. Mutation of JAK2 in the myeloproliferative disorders: Timing, clonality studies, cytogenetic associations, and role in leukemic transformation. Blood 2006, 108, 3548–3555. [Google Scholar] [CrossRef]
- Theocharides, A.; Boissinot, M.; Girodon, F.; Garand, R.; Teo, S.S.; Lippert, E.; Talmant, P.; Tichelli, A.; Hermouet, S.; Skoda, R.C. Leukemic blasts in transformed JAK2-V617F-positive myeloproliferative disorders are frequently negative for the JAK2-V617F mutation. Blood 2007, 110, 375–379. [Google Scholar] [CrossRef]
- Green, A.; Beer, P. Somatic mutations of IDH1 and IDH2 in the leukemic transformation of myeloproliferative neoplasms. N. Engl. J. Med. 2010, 362, 369–370. [Google Scholar] [CrossRef]
- Abdel-Wahab, O.; Manshouri, T.; Patel, J.; Harris, K.; Yao, J.; Hedvat, C.; Heguy, A.; Bueso-Ramos, C.; Kantarjian, H.; Levine, R.L.; et al. Genetic analysis of transforming events that convert chronic myeloproliferative neoplasms to leukemias. Cancer Res. 2010, 70, 447–452. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.J.; Rampal, R.; Manshouri, T.; Patel, J.; Mensah, N.; Kayserian, A.; Hricik, T.; Heguy, A.; Hedvat, C.; Gönen, M.; et al. Genetic analysis of patients with leukemic transformation of myeloproliferative neoplasms shows recurrent SRSF2 mutations that are associated with adverse outcome. Blood 2012, 119, 4480–4485. [Google Scholar] [CrossRef] [PubMed]
- Rampal, R.; Ahn, J.; Abdel-Wahab, O.; Nahas, M.; Wang, K.; Lipson, D.; Otto, G.A.; Yelensky, R.; Hricik, T.; McKenney, A.S.; et al. Genomic and functional analysis of leukemic transformation of myeloproliferative neoplasms. Proc. Natl. Acad. Sci. USA 2014, 111, E5401–E5410. [Google Scholar] [CrossRef]
- Lundberg, P.; Karow, A.; Nienhold, R.; Looser, R.; Hao-Shen, H.; Nissen, I.; Girsberger, S.; Lehmann, T.; Passweg, J.; Stern, M.; et al. Clonal evolution and clinical correlates of somatic mutations in myeloproliferative neoplasms. Blood 2014, 123, 2220–2228. [Google Scholar] [CrossRef]
- Tefferi, A. Primary myelofibrosis: 2019 update on diagnosis, risk-stratification and management. Am. J. Hematol. 2018, 93, 1551–1560. [Google Scholar] [CrossRef]
- Mesa, R.A.; Li, C.Y.; Ketterling, R.P.; Schroeder, G.S.; Knudson, R.A.; Tefferi, A. Leukemic transformation in myelofibrosis with myeloid metaplasia: A single-institution experience with 91 cases. Blood 2005, 105, 973–977. [Google Scholar] [CrossRef]
- Cervantes, F.; Mesa, R.; Barosi, G. New and old treatment modalities in primary myelofibrosis. Cancer J. 2007, 13, 377–383. [Google Scholar] [CrossRef]
- Passamonti, F.; Rumi, E.; Arcaini, L.; Castagnola, C.; Lunghi, M.; Bernasconi, P.; Della Porta, M.G.; Columbo, N.; Pascutto, C.; Cazzola, M.; et al. Leukemic transformation of polycythemia vera: A single center study of 23 patients. Cancer 2005, 104, 1032–1036. [Google Scholar] [CrossRef]
- Thepot, S.; Itzykson, R.; Seegers, V.; Raffoux, E.; Quesnel, B.; Chait, Y.; Sorin, L.; Dreyfus, F.; Cluzeau, T.; Delaunay, J.; et al. Groupe Francophone des Myelodysplasies (GFM). Treatment of progression of Philadelphia-negative myeloproliferative neoplasms to myelodysplastic syndrome or acute myeloid leukemia by azacitidine: A report on 54 cases on the behalf of the Groupe Francophone des Myelodysplasies (GFM). Blood 2010, 116, 3735–3742. [Google Scholar] [PubMed]
- Andriani, A.; Montanaro, M.; Voso, M.T.; Villivà, N.; Ciccone, F.; Andrizzi, C.; De Gregoris, C.; Di Veroli, A.; Maurillo, L.; Alimena, G.; et al. Azacytidine for the treatment of retrospective analysis from the Gruppo Laziale for the study of Ph-negative MPN. Leuk. Res. 2015, 39, 801–814. [Google Scholar] [CrossRef] [PubMed]
- Badar, T.; Kantarjian, H.M.; Ravandi, F.; Jabbour, E.; Borthakur, G.; Cortes, J.E.; Pemmaraju, N.; Pierce, S.R.; Newberry, K.J.; Daver, N.; et al. Therapeutic benefit of decitabine, a hypomethylating agent, in patients with high-risk primary myelofibrosis and myeloproliferative neoplasm in accelerated or blastic/acute myeloid leukemia phase. Leuk. Res. 2015, 39, 950–956. [Google Scholar] [CrossRef]
- Eghtedar, A.; Verstovsek, S.; Estrov, Z.; Burger, J.; Cortes, J.; Bivins, C.; Faderl, S.; Ferrajoli, A.; Borthakur, G.; George, S.; et al. Phase 2 study of the JAK kinase inhibitor ruxolitinib in patients with refractory leukemias, including postmyeloproliferative neoplasm acute myeloid leukemia. Blood 2012, 119, 4614–4618. [Google Scholar] [CrossRef]
- Pemmaraju, N.; Kantarjian, H.; Kadia, T.; Cortes, J.; Borthakur, G.; Newberry, K.; Garcia-Manero, G.; Ravandi, F.; Jabbour, E.; Dellasala, S.; et al. A phase I/II study of the Janus kinase (JAK)1 and 2 inhibitor ruxolitinib in patients with relapsed or refractory acute myeloid leukemia. Clin. Lymphoma Myeloma Leuk. 2015, 15, 171–176. [Google Scholar] [CrossRef] [PubMed]
- Rampal, R.K.; Mascarenhas, J.O.; Kosiorek, H.E.; Price, L.; Berenzon, D.; Hexner, E.; Abboud, C.N.; Kremyanskaya, M.; Weinberg, R.S.; Salama, M.E.; et al. Safety and efficacy of combined ruxolitinib and decitabine in accelerated and blast-phase myeloproliferative neoplasms. Blood Adv. 2018, 2, 3572–3580. [Google Scholar] [CrossRef]
- Bose, P.; Verstovsek, S.; Gasior, Y.; Jain, N.; Jabbour, E.J.; Estrov, Z.; Alvarado, Y.; DiNardo, C.D.; Pemmaraju, N.; Kornblau, S.M.; et al. Phase I/II study of ruxolitinib (RUX) with decitabine (DAC) in patients with post-myeloproliferative neoplasm acute myeloid leukemia (post-MPN AML): Phase I results [abstract]. Blood 2016, 128, 4262. [Google Scholar]
- Odenike, O. How I treat the blast phase of Philadelphia chromosome-negative myeloproliferative neoplasms. Blood 2018, 132, 2339–2350. [Google Scholar]
- Wang, J.C.; Chen, W.; Nallusamy, S.; Chen, C.; Novetsky, A.D. Hypermethylation of the P15INK4b and P16INK4a in agnogenic myeloid metaplasia (AMM) and AMM in leukaemic transformation. Br. J. Haematol. 2002, 116, 582–586. [Google Scholar] [CrossRef]
- Chen, J.; Odenike, O.; Rowley, J.D. Leukaemogenesis: More than mutant genes. Nat. Rev. Cancer 2010, 10, 23–36. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.; Siddiqi, R.; Gangat, N. Therapeutic options for leukemic transformation in patients with myeloproliferative neoplasms. Leuk. Res. 2017, 63, 78–84. [Google Scholar] [CrossRef] [PubMed]
- Mascarenhas, J.; Navada, S.; Malone, A.; Rodriguez, A.; Najfeld, V.; Hoffman, R. Therapeutic options for patients with myelofibrosis in blast phase. Leuk. Res. 2010, 34, 1246–1249. [Google Scholar] [CrossRef]
- Kim, H.P.; Gerhard, B.; Harasym, T.O.; Mayer, L.D.; Hogge, D.E. Liposomal encapsulation of a synergistic molar ratio of cytarabine and daunorubicin enhances selective toxicity for acute myeloid leukemia progenitors as compared to analogous normal hematopoietic cells. Exp. Hematol. 2011, 39, 741–750. [Google Scholar] [CrossRef] [PubMed]
- Lim, W.S.; Tardi, P.G.; Xie, X.; Fan, M.; Huang, R.; Ciofani, T.; Harasym, T.O.; Mayer, L.D. Schedule- and dose-dependency of CPX-351, a synergistic fixed ratio cytarabine:daunorubicin formulation, in consolidation treatment against human leukemia xenografts. Leuk. Lymphoma 2010, 51, 1536–1542. [Google Scholar] [CrossRef]
- Brunetti, C.; Anelli, L.; Zagaria, A.; Specchia, G.; Albano, F. CPX-351 in acute myeloid leukemia: Can a new formulation maximize the efficacy of old compounds? Expert Rev. Hematol. 2017, 10, 853–862. [Google Scholar] [CrossRef] [PubMed]
- Lancet, J.E.; Uy, G.L.; Cortes, J.E.; Newell, L.F.; Lin, T.L.; Ritchie, E.K.; Stuart, R.K.; Strickland, S.A.; Hogge, D.; Solomon, S.R.; et al. CPX-351 (cytarabine and daunorubicin) Liposome for Injection Versus Conventional Cytarabine Plus Daunorubicin in Older Patients with Newly Diagnosed Secondary Acute Myeloid Leukemia. J. Clin. Oncol. 2018, 36, 2684–2692. [Google Scholar] [CrossRef]
- Cheung, E.; Perissinotti, A.J.; Bixby, D.L.; Burke, P.W.; Pettit, K.M.; Benitez, L.L.; Brown, J.; Scappaticci, G.B.; Marini, B.L. The leukemia strikes back: A review of pathogenesis and treatment of secondary AML. Ann. Hematol. 2019, 98, 541–559. [Google Scholar] [CrossRef] [PubMed]
- Shi, J.; Vakoc, C.R. The mechanisms behind the therapeutic activity of BET bromodomain inhibition. Mol. Cell 2014, 54, 728–736. [Google Scholar] [CrossRef]
- Saenz, D.T.; Fiskus, W.; Manshouri, T.; Rajapakshe, K.; Krieger, S.; Sun, B.; Mill, C.P.; DiNardo, C.; Pemmaraju, N.; Kadia, T.; et al. BET protein bromodomain inhibitor-based combinations are highly active against post-myeloproliferative neoplasm secondary AML cells. Leukemia 2017, 31, 678–687. [Google Scholar] [CrossRef] [PubMed]
- Wei, A.H.; Tiong, I.S. Midostaurin, enasidenib, CPX-351, gemtuzumab ozogamicin, and venetoclax bring new hope to AML. Blood 2017, 130, 2469–2474. [Google Scholar] [CrossRef]
- Mascarenhas, J.; Wang, X.; Rodriguez, A.; Xu, M.; Gorman, E.; Zhang, W.; Goldberg, J.D.; Najfeld, V.; Hoffman, R. A phase I study of LBH589, a novel histone deacetylase inhibitor in patients with primary myelofibrosis (PMF) and post-polycythemia/essential thrombocythemia myelofibrosis (post-PV/ET MF) [abstract]. Blood 2009, 114, 308. [Google Scholar]
- Rambaldi, A.; Dellacasa, C.M.; Salmoiraghi, S.; Spinelli, O.; Ferrari, M.L.; Gattoni, E.; Guglielmelli, P.; Vannucchi, A.M.; Barosi, G.; Barbui, T. A phase 2a study of the histone-deacetylase inhibitor ITF2357 in patients with JAK2V617F positive chronic myeloproliferative neoplasms [abstract]. Blood 2008, 112, 100. [Google Scholar]
- Amatangelo, M.D.; Quek, L.; Shih, A.; Stein, E.M.; Roshal, M.; David, M.D.; Marteyn, B.; Farnoud, N.R.; de Botton, S.; Bernard, O.A.; et al. Enasidenib induces acute myeloid leukemia cell differentiation to promote clinical response. Blood 2017, 130, 732–741. [Google Scholar] [CrossRef]
- Stein, E.M.; DiNardo, C.D.; Pollyea, D.A.; Fathi, A.T.; Roboz, G.J.; Altman, J.K.; Stone, R.M.; DeAngelo, D.J.; Levine, R.L.; Flinn, I.W.; et al. Enasidenib in mutant IDH2 relapsed or refractory acute myeloid leukemia. Blood 2017, 130, 722–731. [Google Scholar] [CrossRef]
- Petersdorf, S.H.; Kopecky, K.J.; Slovak, M.; Willman, C.; Nevill, T.; Brandwein, J.; Larson, R.A.; Erba, H.P.; Stiff, P.J.; Stuart, R.K.; et al. A phase 3 study of gemtuzumab ozogamicin during induction and postconsolidation therapy in younger patients with acute myeloid leukemia. Blood 2013, 121, 4854–4860. [Google Scholar] [CrossRef]
- Castaigne, S.; Pautas, C.; Terré, C.; Renneville, A.; Gardin, C.; Suarez, F.; Caillot, D.; Berthon, C.; Rousselot, P.; Preudhomme, C.; et al. Final analysis of the ALFA 0701 study [abstract]. Blood 2014, 124, 376. [Google Scholar]
- Hills, R.K.; Castaigne, S.; Appelbaum, F.R.; Delaunay, J.; Petersdorf, S.; Othus, M.; Estey, E.H.; Dombret, H.; Chevret, S.; Ifrah, N.; et al. Addition of gemtuzumab ozogamicin to induction chemotherapy in adult patients with acute myeloid leukaemia: A meta-analysis of individual patient data from randomised controlled trials. Lancet Oncol. 2014, 15, 986–996. [Google Scholar] [CrossRef]
- Konopleva, M.; Pollyea, D.A.; Potluri, J.; Chyla, B.; Hogdal, L.; Busman, T.; McKeegan, E.; Salem, A.H.; Zhu, M.; Ricker, J.L.; et al. Efficacy and Biological Correlates of Response in a Phase II Study of Venetoclax Monotherapy in Patients with Acute Myelogenous Leukemia. Cancer Discov. 2016, 6, 1106–1117. [Google Scholar] [CrossRef]
- Pratz, K.; Pollyea, D.A.; Jonas, B.A.; Pullarkat, V.; Wei, A.; Arellano, M.; Becker, P.S.; Frankfurt, O.; Thirman, M.; Pigneux, A.; et al. Safety and efficacy of venetoclax (Ven) in combination with decitabine or azacitidine in treatment-naive, elderly patients (≥65 years) with acute myeloid leukemia (AML) [abstract]. Haematologica 2017, 102, S472. [Google Scholar]
- Wei, A.H.; Strickland, S.A.; Roboz, G.J.; Hou, J.-Z.; Fiedler, W.; Lin, T.L.; Martinelli, G.; Walter, R.B.; Enjeti, A.; Fakouhi, K.M.; et al. Venetoclax plus low-dose cytarabine in treatment-naïve acute myeloid leukemia patients aged >65 years and unfit for standard induction therapy [abstract]. Haematologica 2017, 102, S473. [Google Scholar]
| Gene | Gene Function | Chromosome Location | Prognostic Significance | References |
|---|---|---|---|---|
| ASXL1 | Epigenetic regulation | 20q11.1 | Adverse in PV and PMF | [28,29,30] |
| SRSF2 | mRNA processing | 17q25.1 | Adverse in PV, ET and PMF | [28,30] |
| EZH2 | Epigenetic regulation | 7q36.1 | Adverse in ET and PMF | [28,30] |
| IDH1 | Epigenetic regulation | 2q33.3 | Adverse in PMF | [28,30,31,32] |
| IDH2 | Epigenetic regulation | 15q26.1 | Adverse in PV, ET and PMF | [28,30,31,32] |
| CBL | Cell signaling pathways | 11q23.3 | Adverse in PMF | [30] |
| RUNX1 | Transcriptional regulation | 21q22.12 | Adverse in PV and PMF | [30] |
| CEBPA | Transcriptional regulation | 19q13.1 | Adverse in PMF | [30] |
| SH2B3 | mRNA processing | 12q24 | Adverse in ET and PMF | [30] |
| KIT | Tyrosine kinase receptor | 4q11 | Adverse in PMF | [30] |
| TP53 | Transcriptional regulation | 17p13.1 | Adverse in ET | [33] |
| Treatment Approach | Patient Population | Results | Survival | References |
|---|---|---|---|---|
| HMAs | MPN-BP (n = 26); MPN-AP (n = 28) | ORR, 52% with azacitidine | 11 months | [52] |
| MPN-BP (n = 19) | ORR, 47% with azacitidine | 9.9 months | [53] | |
| MPN-BP (n = 21); MPN-AP (n = 13); PMF (n = 11) | ORR in MPN-BP, 29% with decitabine | 6.9 months | [54] | |
| JAK inhibition | R/R AML (n = 38), including MPN-BP (n = 18) | CR/CRi 17% | NR | [55] |
| R/R AML (n = 28), including MPN-BP (n = 7) | ORR, 0% | NR | [56] | |
| JAK inhibition + HMAs | MPN-BP/AP (n = 21) | ORR; 33% | 10.4 months | [57] |
| MPN-BP (n = 10) | ongoing | NR | [58] |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Iurlo, A.; Cattaneo, D.; Gianelli, U. Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options. Int. J. Mol. Sci. 2019, 20, 1839. https://doi.org/10.3390/ijms20081839
Iurlo A, Cattaneo D, Gianelli U. Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options. International Journal of Molecular Sciences. 2019; 20(8):1839. https://doi.org/10.3390/ijms20081839
Chicago/Turabian StyleIurlo, Alessandra, Daniele Cattaneo, and Umberto Gianelli. 2019. "Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options" International Journal of Molecular Sciences 20, no. 8: 1839. https://doi.org/10.3390/ijms20081839
APA StyleIurlo, A., Cattaneo, D., & Gianelli, U. (2019). Blast Transformation in Myeloproliferative Neoplasms: Risk Factors, Biological Findings, and Targeted Therapeutic Options. International Journal of Molecular Sciences, 20(8), 1839. https://doi.org/10.3390/ijms20081839





