Effect of Different Skin Penetration Promoters in Halobetasol Propionate Permeation and Retention in Human Skin
Abstract
:1. Introduction
2. Results
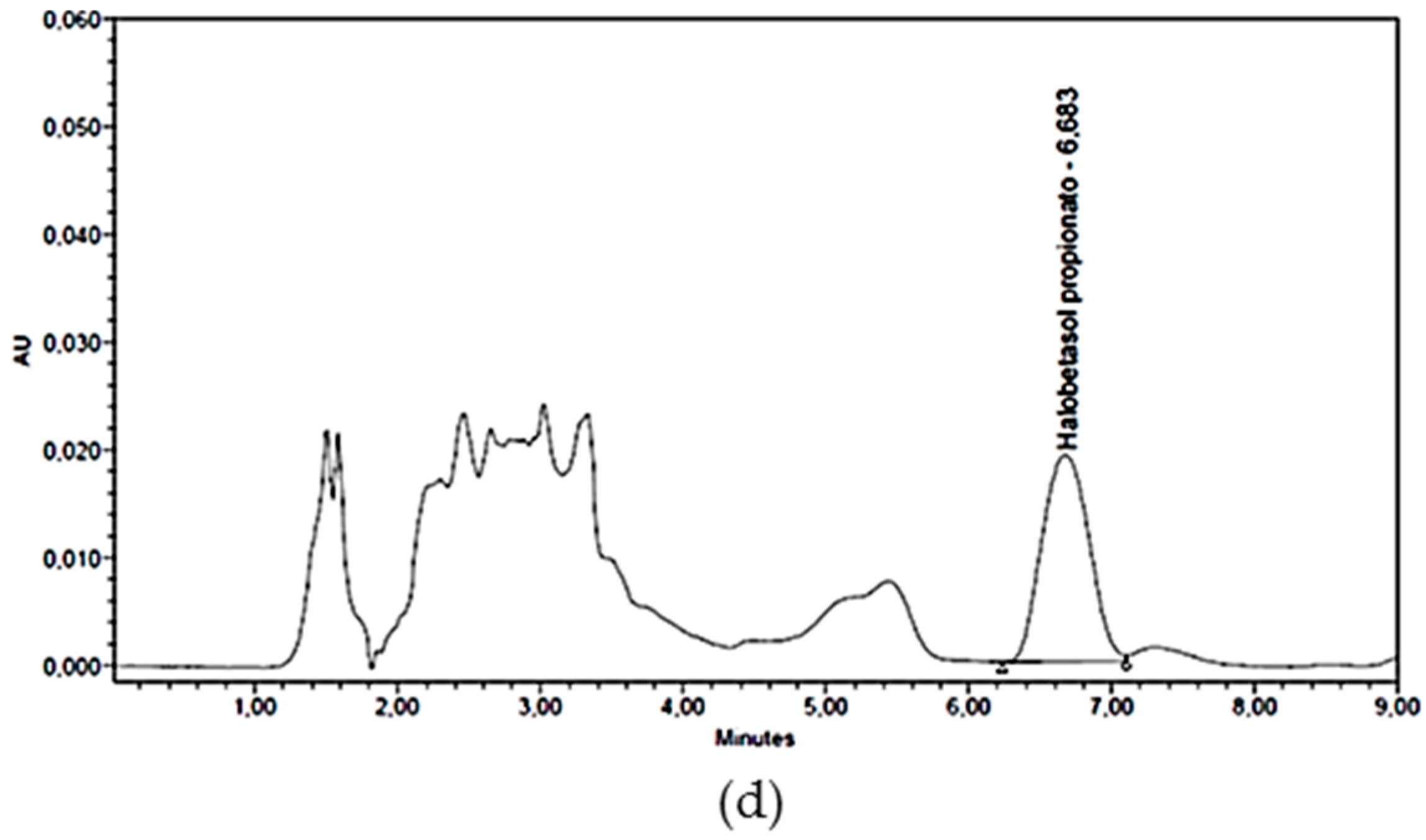
2.1. HPLC Validation Methodology
2.2. Skin Permeation Assay and Permeation Parameters
2.3. In Vivo Draize Skin Test
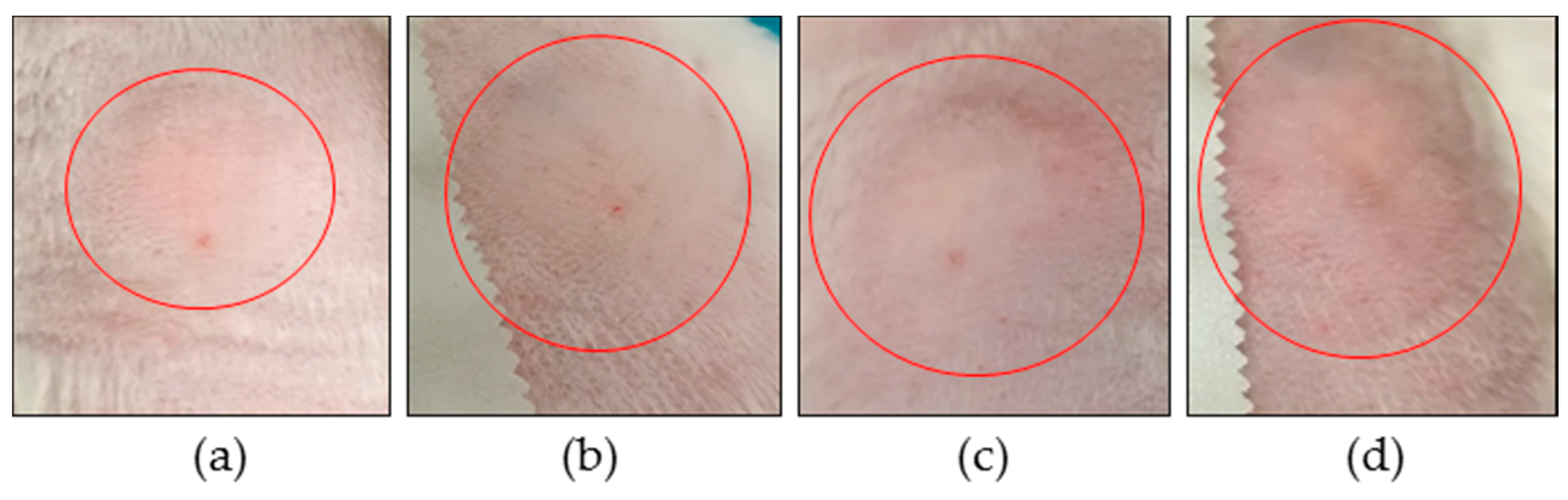
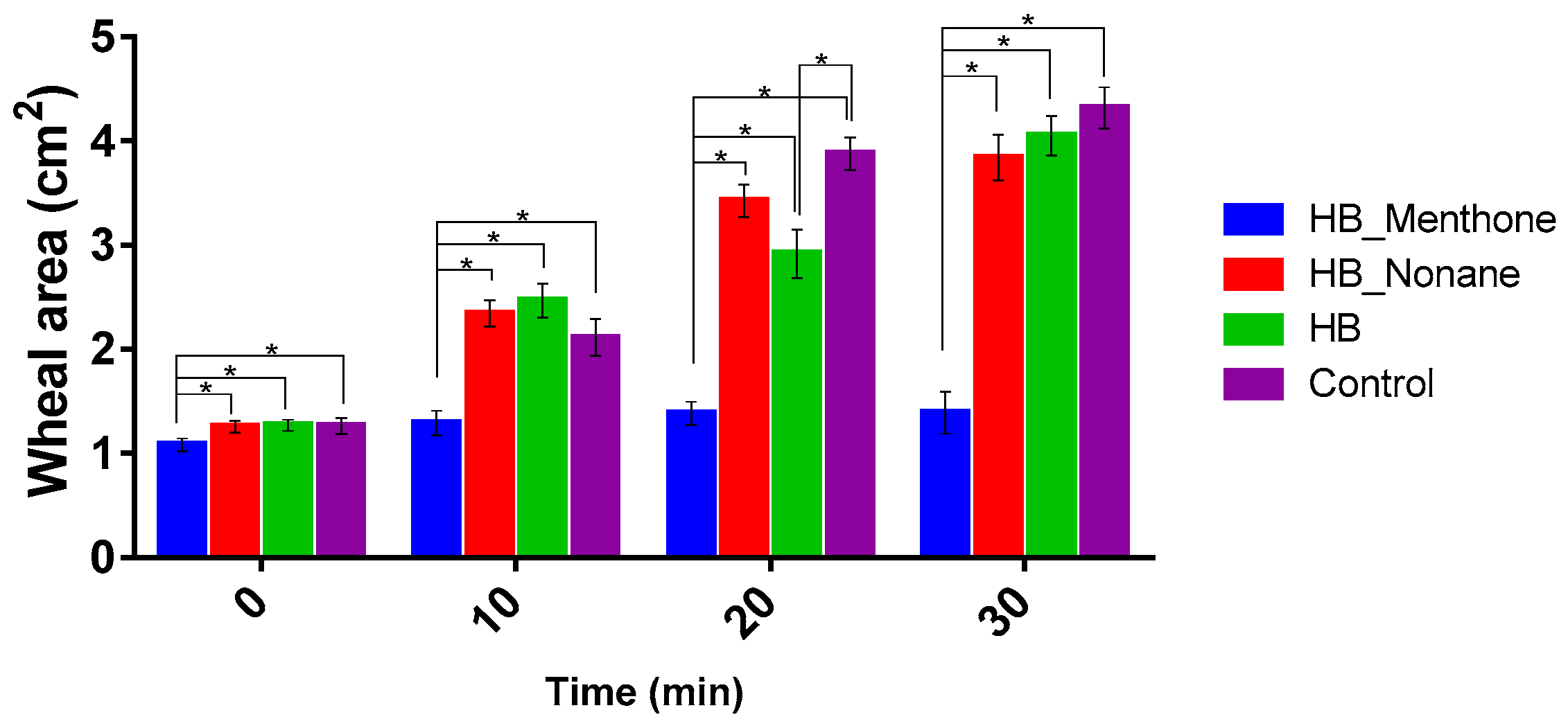
2.4. Efficacy Assay
3. Discussion
3.1. HPLC Validation Methodology
3.2. Ex Vivo Studies
3.3. In Vivo Studies
4. Materials and Methods
4.1. Materials
4.2. Methods
4.2.1. HPLC Validation Methodology
4.2.2. Ex Vivo Assays
Skin Permeation Assay
Amount of Drug Retained in Skin
Recovery Percentage
4.2.3. In Vivo Assays
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Hadgraft, J. Modulation of the barrier function of the skin. Skin Pharmacol. Appl. Skin Physiol. 2001, 14, 72–81. [Google Scholar] [CrossRef] [PubMed]
- Bouwstra, J.A.; Honeywell-Nguyen, P.L.; Gooris, G.S.; Ponec, M. Structure of the skin barrier and its modulation by vesicular formulations. Prog. Lipid Res. 2003, 42, 1–36. [Google Scholar] [CrossRef]
- Walters, K.; Roberts, M. The structure and function of skin. In Dermatological and Transdermal Formulations, 1st ed.; CRC Press: London, UK, 2002; Volume 119, pp. 1–41. ISBN 978-0-8247-4323-9. [Google Scholar]
- Hsieh, D. Drug Permeation Enhancement: Theory and Applications, 1st ed.; CRC Press: Boca Raton, FL, USA, 1993; pp. 3–25. ISBN 978-0824790158. [Google Scholar]
- Otberg, N.; Patzelt, A.; Rasulev, U.; Hagemeister, T.; Linscheid, M.; Sinkgraven, R. The role of hair follicles in the percutaneous absorption of caffeine. Br. J. Clin. Pharmacol. 2008, 1, 488–492. [Google Scholar] [CrossRef] [PubMed]
- Lademann, J.; Otberg, N.; Jacobi, U.; Hoffman, R.M.; Blume-Peytavi, U. Follicular penetration and targeting. J. Investig. Dermatol. Symp. Proc. 2005, 1, 301–303. [Google Scholar] [CrossRef] [PubMed]
- Greaves, M.W.; Weinstein, G.D. Treatment of psoriasis. N. Engl. J. Med. 1995, 2, 581–589. [Google Scholar] [CrossRef] [PubMed]
- Liem, W.H.; McCullough, J.L.; Weinstein, G.D. Effectiveness of topical therapy for psoriasis: Results of a national survey. Cutis 1995, 55, 306–310. [Google Scholar] [PubMed]
- Yawalkar, S.; Wiesenberg-Boettcher, I.; Gibson, J.R.; Siskin, S.B.; Pignant, W. Dermatopharmacologic investigations of halobetasol propionate in comparison with clobetasol 17-propionate. J. Am. Acad. Dermatol. 1991, 25, 1137–1144. [Google Scholar] [CrossRef]
- Long, C. Common skin disorder and Their Topical Treatment. In Dermatological and Transdermal Formulations, 1st ed.; CRC Press: London, UK, 2002; Volume 119, pp. 41–60. ISBN 978-0-8247-4323-9. [Google Scholar]
- Blum, G.; Yawalkar, S. A comparative, multicenter, double blind trial of 0.05% halobetasol propionate ointment and 0.1% betamethasone valerate ointment in the treatment of patients with chronic, localized plaque psoriasis. J. Am. Acad. Dermatol. 1991, 25, 1153–1156. [Google Scholar] [CrossRef]
- Herz, G.; Blum, G.; Yawalkar, S. Halobetasol propionate cream by day and halobetasol propionate ointment at night for the treatment of pediatric patients with chronic, localized plaque psoriasis and atopic dermatitis. J. Am. Acad. Dermatol. 1991, 25, 1166–1169. [Google Scholar] [CrossRef]
- Cevc, G.; Blume, G. Hydrocortisone and dexamethasone in very deformable drug carriers have increased biological potency, prolonged effect, and reduced therapeutic dosage. Biochim. Biophys. Acta 2004, 1663, 61–73. [Google Scholar] [CrossRef] [PubMed]
- Xunquan, L.; Changgeng, S.; Peiying, J.; Huaiqu, W.; Gan-Yun, Y.; Yawalkar, S. Treatment of localized vitiligo with Ulobetasol cream. Int. J. Dermatol. 1990, 29, 295–297. [Google Scholar] [CrossRef]
- Horn, E.J.; Domm, S.; Katz, H.I.; Lebwohl, M.; Mrowietz, U.; Kragballe, K. Topical corticosteroids in psoriasis: Strategies for improving safety. J. Eur. Acad. Dermatol. Venereol. 2010, 24, 119–124. [Google Scholar] [CrossRef] [PubMed]
- Loder, J.S.; Gibson, J.R.; Yawalkar, S.J.; White, R.J.; Maibach, H.I.; Surber, C. Halobetasol propionate. In Topical Corticosteroids; Maibach, H.I., Surber, C., Eds.; Karger: Basel, Switzerland, 1992; pp. 423–434. ISBN 978-3-318-05207-7. [Google Scholar]
- Food and Drug Administration. Available online: https://www.fda.gov/ (accessed on 21 September 2017).
- Katz, V.L.; Thorp, J.M.; Bowes, W.A. Severe symmetric intrauterine growth retardation associated with the topical use of triamcinolone. Am. J. Obstet. Gynecol. 1990, 162, 396–397. [Google Scholar] [CrossRef]
- Goldberg, B.; Hartdegen, R.; Presbury, D.; Harvey-Smith, E.; Yawalkar, S. A double-blind, multicenter comparison of 0.05% halobetasol propionate ointment and 0.05% clobetasol propionate ointment in patients with chronic, localized plaque psoriasis. J. Am. Acad. Dermatol. 1992, 25, 1145–1148. [Google Scholar] [CrossRef]
- Vademecum. Halobetasol Propionate. Available online: http://www.iqb.es/cbasicas/farma/farma04/h014.htm (accessed on 24 August 2017).
- Banga, A.K. Transdermal and Intradermal Delivery of Therapeutic Agents: Application of Physical Technologies, 1st ed.; CRC Press: Boca Raton, FL, USA, 2011; pp. 8–12. ISBN 9781439805091. [Google Scholar]
- Banga, A.K. Electrically Assisted Transdermal and Topical Drug Delivery, 1st ed.; CRC Press: London, UK, 1998; pp. 1–10. ISBN 0748406875. [Google Scholar]
- Banga, A.K. Microporation applications for enhancing drug delivery. Exp. Opin. Drug Deliv. 2009, 6, 343–354. [Google Scholar] [CrossRef] [PubMed]
- Williams, A.C.; Barry, B.W. Penetration enhancers. Adv. Drug Deliv. Rev. 2012, 64, 128–137. [Google Scholar] [CrossRef]
- Song, W.; Cun, D.; Quan, P.; Liu, N.; Chen, Y.; Cui, H.; Xiang, R.W.; Fang, L. Dual-directional regulation of drug permeating amount by combining the technique of ion-pair complexation with chemical enhancers for the synchronous permeation of indapamide and bisoprolol in their compound patch through rabbit skin. Eur. J. Pharm. Biopharm. 2015, 91, 59–65. [Google Scholar] [CrossRef] [PubMed]
- Cato, A.; Swinehart, J.M.; Griffin, E.I.; Sutton, L.; Kaplan, A.S. Azone® enhances clinical effectiveness of an optimized formulation of triamcinolone acetonide in atopic dermatitis. Int. J. Dermatol. 2001, 40, 232–236. [Google Scholar] [CrossRef] [PubMed]
- Asbill, C.S.; Michniak, B.B. Percutaneous penetration enhancers: Local versus transdermal activity. Pharm. Sci. Technol. Today 2000, 3, 36–41. [Google Scholar] [CrossRef]
- Kanikkannan, N.; Kandimalla, K.; Lamba, S.S.; Singh, M. Structure-activity relationship of chemical penetration enhancers in transdermal drug delivery. Curr. Med. Chem. 2000, 7, 593–608. [Google Scholar] [CrossRef] [PubMed]
- Maibach, H. Dermatological formulations: Percutaneous absorption. J. Pharm. Sci. 1984, 73, 3–57. [Google Scholar] [CrossRef]
- Badische Anilin- und Soda-Fabrik (BASF). Available online: https://www.ulprospector.com/es/eu/PersonalCare/Detail/804/31779/Cetiol-CC (accessed on 2 October 2017).
- Okabe, H.; Takayama, K.; Ogura, A.; Nagai, T. Effect of limonene and related compounds on the percutaneous absorption of indomethacin. Drug Des. Deliv. 1989, 4, 313–321. [Google Scholar] [PubMed]
- González-Mira, E.; Nikolić, S.; García, M.L.; Egea, M.A.; Souto, E.B.; Calpena, A. Potential use of nanostructured lipid carriers for topical delivery of flurbiprofen. J. Pharm. Sci. 2011, 100, 242–251. [Google Scholar] [CrossRef] [PubMed]
- Fernández-Campos, F.; Clares, B.; López, O.; Alonso, C.; Calpena, A. Evaluation of novel nystatin nanoemulsion for skin candidosis infections. Mycoses 2013, 56, 70–81. [Google Scholar] [CrossRef] [PubMed]
- Scientific Committee on Consumer Safety 2017. Available online: https://ec.europa.eu/health/sites/health/files/scientific_committees/consumer_safety/docs/sccs_o_206.pdf (accessed on 15 September 2017).
- Organization for Economic Co-Operation and Development (OECD), Guidelines for the Testing of Chemicals, Section 4 Test No. 404: Acute Dermal Irritation/Corrosion. Available online: http://www.oecd.org/env/test-no-404-acute-dermal-irritation-corrosion-9789264242678-en.htm (accessed on 2 August 2017).
- Michaels, A.S.; Chandrasekaran, S.K.; Shaw, J.E. Drug permeation through human skin: Theory and in-vitro experimental measurement. AIChE J. 1975, 21, 985–996. [Google Scholar] [CrossRef]
- Williams, A.C.; Cornwell, P.A.; Barry, B.W. On the non-Gaussian distribution of human skin permeabilities. Int. J. Pharm. 1992, 86, 69–77. [Google Scholar] [CrossRef]
- Draize, J.H.; Woodard, G.; Calvery, H.O. Methods for the Study of irritation and toxicity of substances applied topically to the skin and mucous membranes. J. Pharmacol. Exp. Ther. 1944, 82, 377–390. [Google Scholar]
- Abidi, A.; Ahmad, F.; Singh, S.K.; Kumar, A. Study of reservoir effect of clobetasol propionate cream in an experimental animal model using histamine-induced wheal suppression test. Indian J. Dermatol. 2010, 55, 329–333. [Google Scholar] [CrossRef] [PubMed]
- United States Pharmacopeia Convention Inc. The United States Pharmacopeia, the National Formulary, USP40/NF35; National Publishing for the United States Pharmacopeial Convention, Inc.: Philadelphia, PA, USA, 2017; pp. 4925–4927. [Google Scholar]
- Mostafa, A.A.; Bebawy, L.I.; Refaat, H.H. Spectrophotometric determination of clobetasol propionate, halobetasol propionate, quinagolide hydrochloride, through charge transfer complexation. J. Pharm. Biomed. Anal. 2002, 27, 889–899. [Google Scholar] [CrossRef]
- Chakole, C.M.; Shende, M.A.; Khadatkar, S.N. Formulation and evaluation of novel combined halobetasol propionate and fusidic acid ointment. Int. J. Chem. Tech. Res. 2009, 1, 103–116. [Google Scholar]
- Nalwade, S.; Reddy, V.R.; Kulkarni, D.; Todamal, S. Quantification of halobetasol propionate and its impurities present in topical dosage forms by stability-indicating LC method. J. Chromatogr. Sci. 2015, 53, 127–134. [Google Scholar] [CrossRef] [PubMed]
- Goyal, R.N.; Agrawal, B. Carbon nanotube-based electrochemical sensor for the determination of halobetasol propionate, a topical corticosteroid. J. Appl. Electrochem. 2012, 42, 31–39. [Google Scholar] [CrossRef]
- Prakash, L.; Malipeddi, H.; Subbaiah, B.V.; Lakka, N.S. Impurity profiling and a stability-indicating UPLC method development and validation for the estimation of related impurities of halobetasol propionate in halobetasol propionate 0.05% (w/w) cream. J. Chromatogr. Sci. 2015, 53, 112–121. [Google Scholar] [CrossRef] [PubMed]
- Bikkad, M.L.; Nathani, A.H.; Mandlik, S.K.; Shrotriya, S.N.; Ranpise, N.S. Halobetasol propionate-loaded solid lipid nanoparticles (SLN) for skin targeting by topical delivery. J. Liposome Res. 2014, 24, 113–123. [Google Scholar] [CrossRef] [PubMed]
- Gattefossé. Available online: https://www.gattefosse.com/transcutol-p (accessed on 8 September 2017).
- Lampe, M.A.; Williams, M.L.; Elias, P.M. Human epidermal lipids: Characterization and modulations during differentiation. J. Lipid Res. 1983, 24, 131–140. [Google Scholar] [PubMed]
- Swarbrick, J.; Boylan, J.C. Encyclopedia of Pharmaceutical Technology: Preservation of Pharmaceutical Products to Salt Forms of Drugs and Absorption; CRC Press: London, UK, 1995; pp. 23–52. [Google Scholar]
- Bonina, F.P.; Montenegro, L. Effects of some non-toxic penetration enhancers on in vitro heparin skin permeation from gel vehicles. Int. J. Pharm. 1994, 111, 191–196. [Google Scholar] [CrossRef]
- Stoughton, R.B. Enhanced percutaneous penetration with 1-dodecylazacycloheptan-2-one. Arch. Dermatol. 1982, 118, 474–477. [Google Scholar] [CrossRef] [PubMed]
- Chow, D.S.; Kaka, I.; Wang, T.I. Concentration-dependent enhancement of 1dodecylazacycloheptan-2-one on the percutaneous penetration kinetics of triamcinolone acetonide. J. Pharm. Sci. 1984, 73, 1794–1799. [Google Scholar] [CrossRef] [PubMed]
- Smith, E.W.; Maibach, H.I. Percutaneous Penetration Enhancers, 1st ed.; Smith, E.W., Maibach, H.I., Eds.; CRC Press: Boca Raton, FL, USA, 1995; pp. 16–33. ISBN 978-0849326059. [Google Scholar]
- Melendres, J.L.; Nangia, A.; Sedik, L.; Hori, M.; Maibach, H.I. Nonane enhances propranolol hydrochloride penetration in human skin. Int. J. Pharm. 1993, 92, 243–248. [Google Scholar] [CrossRef]
- Hori, M.; Satoh, S.; Maibach, H.I.; Guy, R.H. Enhancement of propranolol hydrochloride and diazepam skin absorption in vitro: Effect of enhancer lipophilicity. J. Pharm. Sci. 1991, 80, 32–35. [Google Scholar] [CrossRef] [PubMed]
- Aungst, B.J. Structure/Effect studies of fatty acid isomers as skin penetration enhancers and skin irritants. Pharm. Res. 1989, 6, 244–247. [Google Scholar] [CrossRef] [PubMed]
- Bennett, S.L.; Barry, B.W.; Woodford, R. Optimization of bioavailability of topical steroids: Non-occluded penetration enhancers under thermodynamic control. J. Pharm. Pharmacol. 1985, 37, 298–304. [Google Scholar] [CrossRef] [PubMed]
- Bach, M.; Lippold, B.C. Influence of penetration enhancers on the blanching intensity of betamethasone 17-benzoate. Int. J. Pharm. 1998, 168, 97–108. [Google Scholar] [CrossRef]
- Barry, B.W.; Bennett, S.L. Effect of penetration enhancers on the permeation of mannitol, hydrocortisone and progesterone through human skin. J. Pharm. Pharmacol. 1987, 39, 535–546. [Google Scholar] [CrossRef] [PubMed]
- Sun, J. d-Limonene: Safety and clinical applications. Altern. Med. Rev. 2007, 12, 259–264. [Google Scholar] [PubMed]
- Dragicevic, N.; Maibach, H.I. Percutaneous Penetration Enhancers Chemical Methods in Penetration Enhancement: Nanocarriers; Springer: New York, NY, USA, 2016; 387p. [Google Scholar]
- Chang, J.; Gupta, G. Tissue Engineering for the Hand: Research Advances and Clinical Applications; World Scientific: London, UK, 2010; pp. 95–124. ISBN 978-9814313551. [Google Scholar]
- Sullivan, T.P.; Eaglstein, W.H.; Davis, S.C.; Mertz, P. The pig as a model for human wound healing. Wound Repair Regen. 2001, 9, 66–76. [Google Scholar] [CrossRef] [PubMed]
- Greenhalgh, D.G. Models of Wound Healing. J. Burn Care Res. 2005, 26, 293–305. [Google Scholar] [CrossRef]
- Vickers, C.F. Existence of reservoir in the stratum corneum: Experimental proof. Arch. Dermatol. 1963, 88, 20–23. [Google Scholar] [CrossRef] [PubMed]
- Schaefer, H.; Stüttgen, G.; Zesch, A.; Schalla, W.; Gazith, J. Quantitative determination of percutaneous absorption of radiolabeled drugs in vitro and in vivo by human skin. Curr. Probl. Dermatol. 1978, 7, 80–94. [Google Scholar] [PubMed]
- Benfeldt, E.; Serup, J.; Menné, T. Effect of barrier perturbation on cutaneous salicylic acid penetration in human skin: In vivo pharmacokinetics using micro dialysis and non-invasive quantification of barrier function. Br. J. Dermatol. 1999, 140, 739–748. [Google Scholar] [CrossRef] [PubMed]
- International Conference on Harmonisation (ICH) of Technical Requirements for Registration of Pharmaceuticals for Human Use. Validation of Analytical Procedures: Text and Methodology. Q2 (R1). Available online: https://www.ich.org/fileadmin/Public_Web_Site/ICH_Products/Guidelines/Quality/Q2_R1/Step4/Q2_R1__Guideline.pdf (accessed on 25 August 2017).
- Pubchem. Open Chemistry Database. Available online: https://pubchem.ncbi.nlm.nih.gov/compound/Halobetasol#section=Top (accessed on 26 August 2017).
- ECVAM. Test Guideline for Skin Absorption: In Vitro Method. Official Journal of the European Union Method B.45 of Annex to 440/2008/EC (EU Test Methods Regulation) and Its Corrigendum. 2008. Available online: http://www.iss.it/binary/hclp/cont/Reg._440_2008.pdf (accessed on 20 August 2017).
- Franz, T.J. Percutaneous Absorption: On the Relevance of in Vitro Data. J. Investig. Dermatol. 1975, 64, 190–195. [Google Scholar] [CrossRef] [PubMed]
- Mallandrich, M.; Fernández-Campos, F.; Clares, B.; Halbaut, L.; Alonso, C.; Coderch, L.; Garduño-Ramírez, M.L.; Andrade, B.; del Pozo, A.; Lane, M.E. Developing transdermal applications of ketorolac tromethamine entrapped in stimuli sensitive block copolymer hydrogels. Pharm. Res. 2017, 34, 1728–1740. [Google Scholar] [CrossRef] [PubMed]
- Campos, F.F.; Calpena, A.C.; Delgado, G.R.; Serrano, O.L.; Naveros, B.C. Development and characterization of a novel nystatin-loaded nanoemulsion for the buccal treatment of candidiasis: Ultrastructural effects and release studies. J. Pharm. Sci. 2012, 101, 3739–3752. [Google Scholar] [CrossRef] [PubMed]
- Passantino, A. Application of the 3Rs principles for animals used for experiments at the beginning of the 21st century. Ann. Rev. Biomed. Sci. 2008, 10. [Google Scholar] [CrossRef]


| Chemical Class | Example(s) |
|---|---|
| Fatty acids | Oleic acid, Undecanoic acid, Linoleic acid |
| Alcohols and Alkanols | Octanol, Nonanol, Decanol |
| Terpenes | Menthol, Thymol, Limonene, Carene |
| Sulfoxides | Dimethyl sulfoxide, Dodecyl methyl sulfoxide |
| Surfactants | Sodium lauryl sulfate, Cetiol, Sorbitan mono-oleate |
| Polyols | Propylene glycol, Polyethylene glycol |
| Amides | n,n-Dimethyl-m-toluamide |
| Ureas | Urea |
| Lactam | Laurocapram (Azone®) |
| Sugars | Cyclodextrins |
| Standard Concentration (μg/mL) | Calculated Concentration (μg/mL) | %RE | %CV |
|---|---|---|---|
| 0.50 | 0.46 ± 0.04 | 7.52 | 8.12 |
| 1.00 | 1.01 ± 0.09 | −1.29 | 9.18 |
| 5.00 | 4.97 ± 0.06 | 0.55 | 1.11 |
| 10.00 | 10.00 ± 0.12 | 0.01 | 1.15 |
| 15.00 | 14.97 ± 0.16 | 0.18 | 1.06 |
| 20.00 | 20.15 ± 0.50 | −0.73 | 2.48 |
| 25.00 | 24.90 ± 0.26 | 0.38 | 1.05 |
| Concentration (μg/mL) | Ratio 1 | Ratio 2 | Ratio 3 | Ratio 4 | Ratio 5 |
|---|---|---|---|---|---|
| 0.5 | 120,731.26 | 102,721.10 | 121,211.86 | 146,101.52 | 121,400.90 |
| 1 | 127,756.00 | 107,598.30 | 118,281.10 | 124,086.20 | 149,836.40 |
| 5 | 117,370.32 | 111,500.02 | 115,936.50 | 124,473.88 | 118,584.80 |
| 10 | 116,073.00 | 111,987.70 | 116,643.40 | 123,272.40 | 119,428.40 |
| 15 | 115,639.87 | 112,150.33 | 115,545.20 | 122,871.87 | 119,042.87 |
| 20 | 120,423.60 | 117,231.60 | 115,496.90 | 117,671.60 | 118,850.15 |
| 25 | 115,293.64 | 112,280.36 | 114,267.60 | 122,551.44 | 118,734.48 |
| Permeation Enhancer | J (μg·h−1 cm−2) (min–max) | Kp (cm h−1)·105 (min–max) | A24 (μg) | As (μg·g−1 cm−2) (min–max) |
|---|---|---|---|---|
| Nonane | 0.141 b,c,d,e,f,g,h | 14.1 b,c,d,e,f,g,h | 2.74 b,c,d,e,f,g,h | 302.70 b,c,d,e,f,g,h |
| (0.138–0.167) | (13.8–16.7) | (2.57–3.82) | (280.04–315.76) | |
| Menthone | 2.588 a,c,d,e,f,g,h | 25.9 a,c,d,e,f,g,h | 35.47 a,c,d,e,f,g,h | 214.04 c,d,e,f,g,h |
| (2.476–2.734) | (248–273) | (31.84–9.27) | (203.06–226.87) | |
| Limonene | 0.073 | 7.29 × 10−5 | 1.49 | 62.62 d,e,f,g,h |
| (0.061–0.078) | (6.10–7.81) | (1.40–1.77) | (55.57–68.34) | |
| Azone | 0.052 f,g | 5.19 f,g | 1.2 | 71.17 e,g,h |
| (0.046–0.056) | (4.60–5.56) | (0.93–1.55) | (65.75–76.45) | |
| Carene | 0.060 f | 6.03 f | 1.28 | 41.39 f,g,h |
| (0.059–0.064) | (5.90–6.40) | (1.09–1.61) | (36.57–45.02) | |
| Decanol | 0.082 | 8.22 | 1.57 | 74.85 g,h |
| (0.077–0.087) | (7.70–8.70) | (1.17–1.78) | (69.86–78.85) | |
| Linoleic acid | 0.078 | 7.79 | 1.52 | 24.74 |
| (0.073–0.087) | (7.30–8.70) | (1.22–1.72) | (18.76–26.02) | |
| Cetiol | 0.071 | 7.06 | 1.6 | 22.04 |
| (0.063–0.075) | (6.30–7.50) | (1.31–1.73) | (18.56–24.98) |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Carvajal-Vidal, P.; Mallandrich, M.; García, M.L.; Calpena, A.C. Effect of Different Skin Penetration Promoters in Halobetasol Propionate Permeation and Retention in Human Skin. Int. J. Mol. Sci. 2017, 18, 2475. https://doi.org/10.3390/ijms18112475
Carvajal-Vidal P, Mallandrich M, García ML, Calpena AC. Effect of Different Skin Penetration Promoters in Halobetasol Propionate Permeation and Retention in Human Skin. International Journal of Molecular Sciences. 2017; 18(11):2475. https://doi.org/10.3390/ijms18112475
Chicago/Turabian StyleCarvajal-Vidal, Paulina, Mireia Mallandrich, María Luisa García, and Ana Cristina Calpena. 2017. "Effect of Different Skin Penetration Promoters in Halobetasol Propionate Permeation and Retention in Human Skin" International Journal of Molecular Sciences 18, no. 11: 2475. https://doi.org/10.3390/ijms18112475
APA StyleCarvajal-Vidal, P., Mallandrich, M., García, M. L., & Calpena, A. C. (2017). Effect of Different Skin Penetration Promoters in Halobetasol Propionate Permeation and Retention in Human Skin. International Journal of Molecular Sciences, 18(11), 2475. https://doi.org/10.3390/ijms18112475