Imaging of a Cilioretinal Artery Embolisation
Abstract
:1. Introduction
2. Case Report
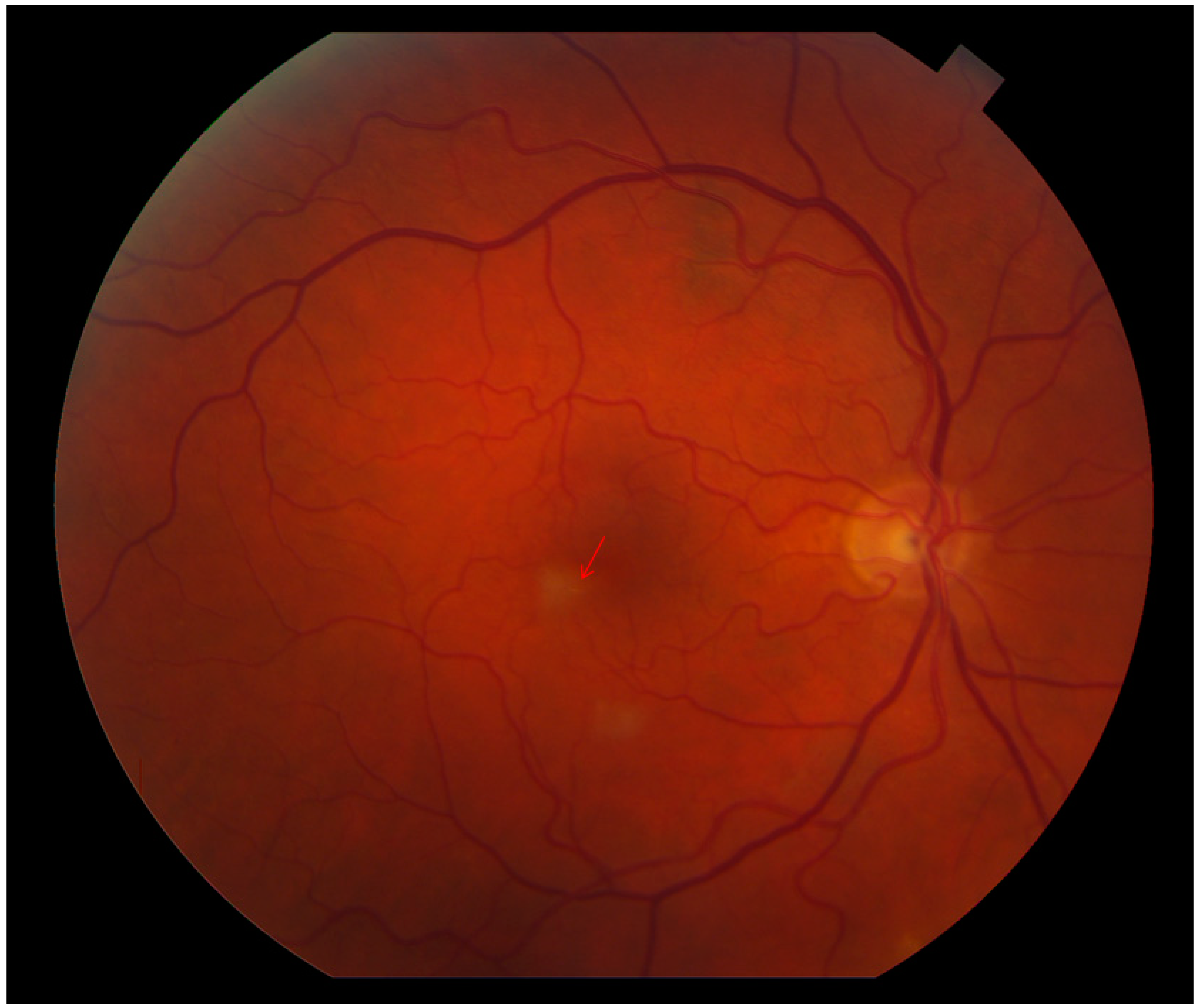
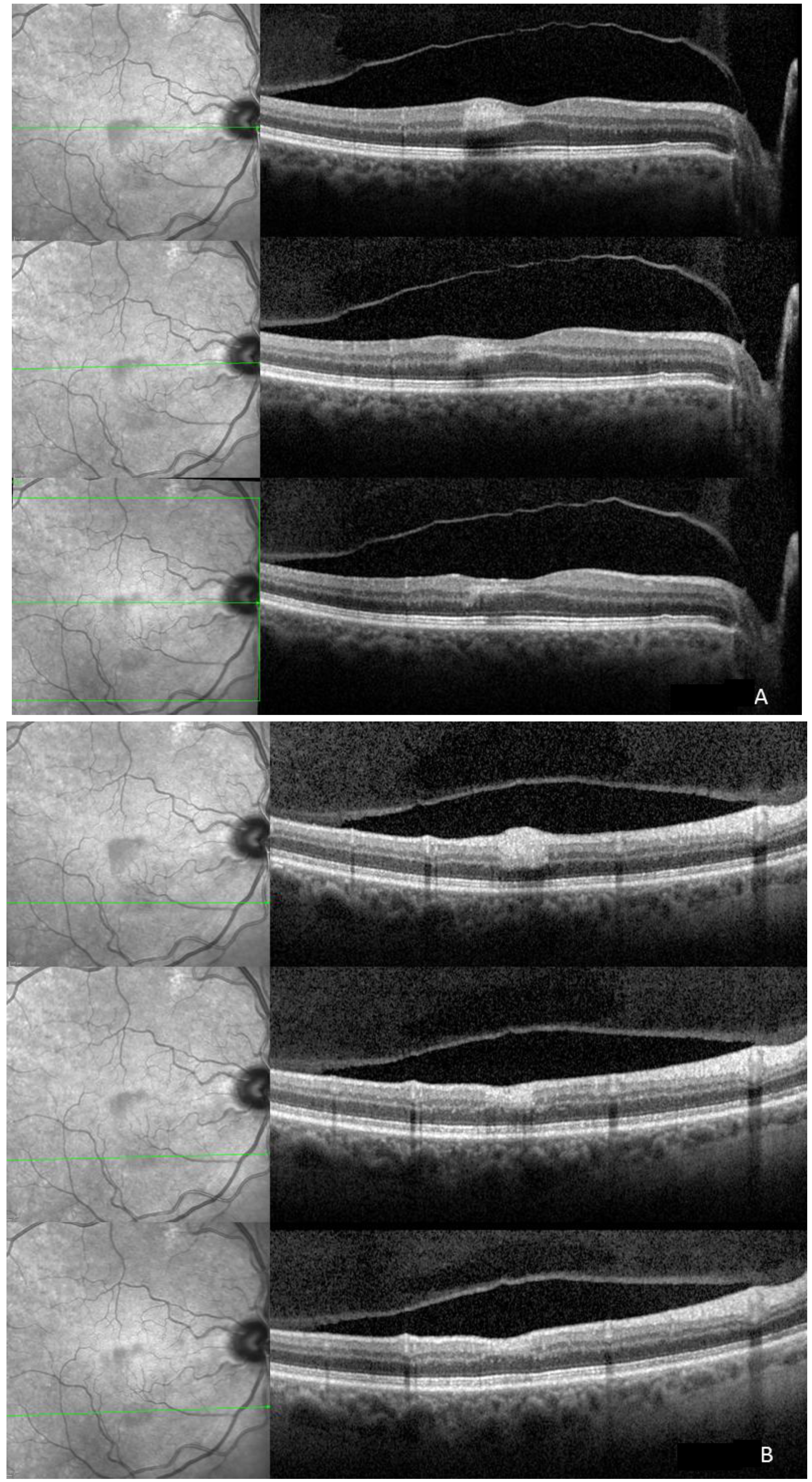
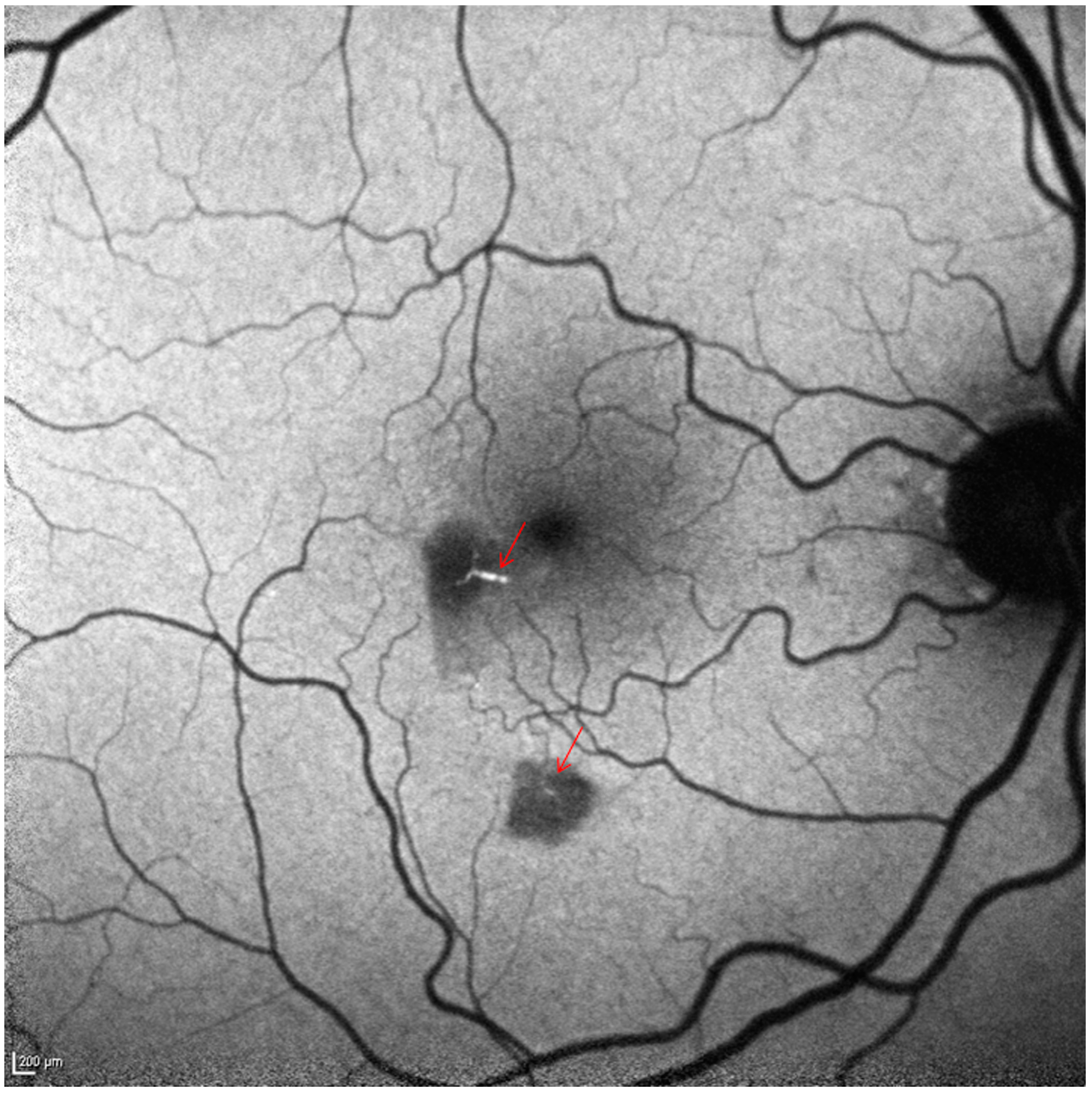
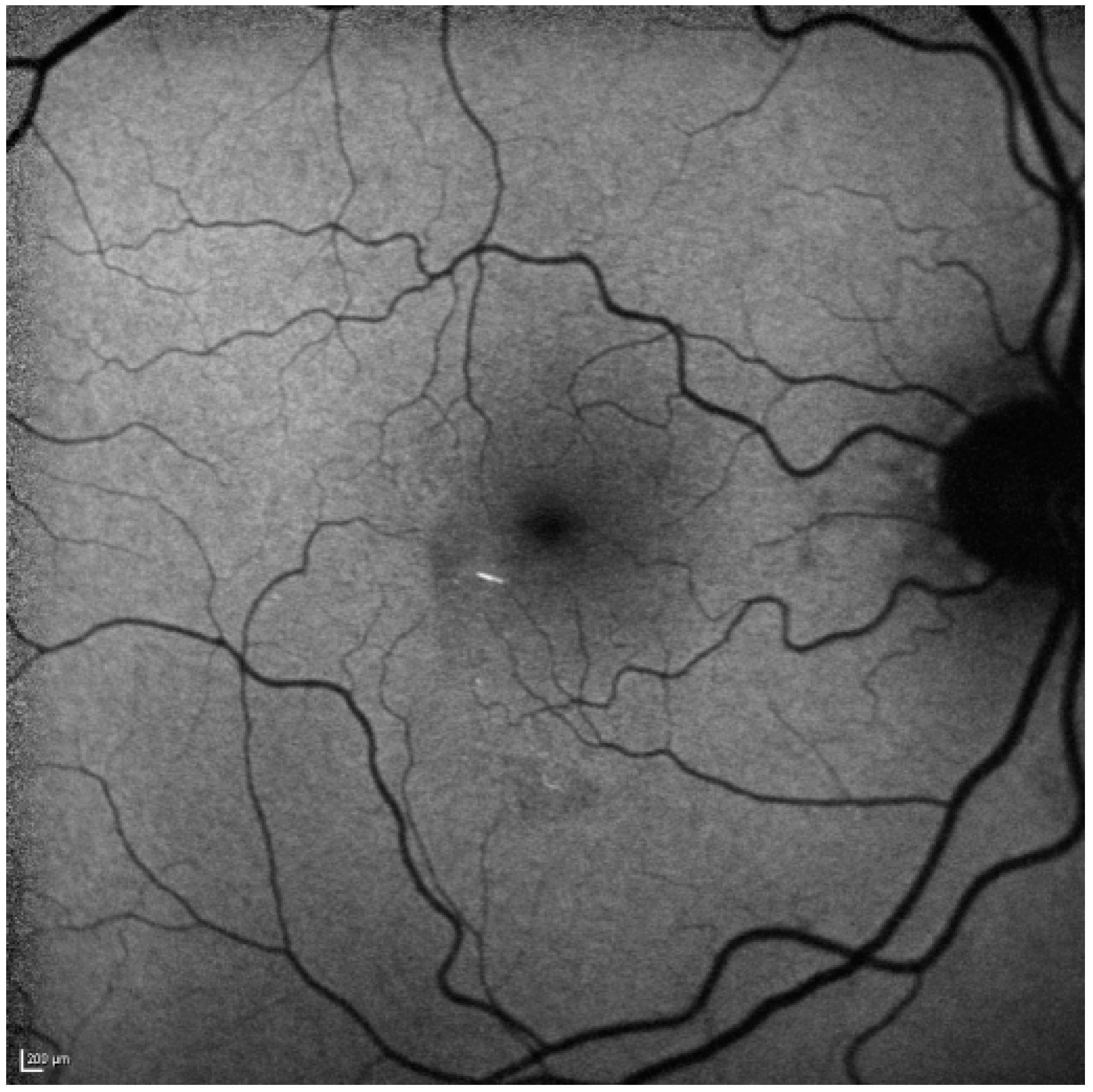
3. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Toussaint, D.; Kuwabara, T.; Cogan, D.G. Retinal vascular patterns. II. Human retinal vessels studied in three dimensions. Arch. Ophthalmol. 1961, 65, 575–581. [Google Scholar] [CrossRef]
- Sarraf, D.; Rahimy, E.; Fawzi, A.A.; Sohn, E.; Barbazetto, I.; Zacks, D.N.; Mittra, R.A.; Klancnik, J.M.; Mrejen, S.; Goldberg, N.R.; et al. Paracentral acute middle maculopathy: A new variant of acute macular neuroretinopathy associated with retinal capillary ischemia. JAMA Ophthalmol. 2013, 131, 1275–1287. [Google Scholar] [CrossRef]
- Aleman, T.S.; Tapino, P.J.; Brucker, A.J. Evidence of recurrent microvascular occlusions associated with acute branch retinal artery occlusion demonstrated with spectral-domain optical coherence tomography. Retina 2012, 32, 1687–1688. [Google Scholar]
- Ritter, M.; Sacu, S.; Deak, G.G.; Kircher, K.; Sayegh, R.G.; Pruente, C.; Schmidt-Erfurth, U.M. In vivo identification of alteration of inner neurosensory layers in branch retinal artery occlusion. Br. J. Ophthalmol. 2012, 96, 201–207. [Google Scholar] [CrossRef]
- Mathew, R.; Papavasileiou, E.; Sivaprasad, S. Autofluorescence and high-definition optical coherence tomography of retinal artery occlusions. Clin. Ophthalmol. 2010, 4, 1159–1163. [Google Scholar]
- Coady, P.A.; Cunningham, E.T., Jr.; Vora, R.A.; McDonald, H.R.; Johnson, R.N.; Jumper, J.M.; Fu, A.D.; Haug, S.J.; Williams, S.L.; Lujan, B.J. Spectral domain optical coherence tomography findings in eyes with acute ischaemic retinal whitening. Br. J. Ophthalmol. 2014. [Google Scholar] [CrossRef]
- Siddiqui, A.A.; Paulus, Y.M.; Scott, A.W. Use of fundus autofluoresecence to evaluate retinal artery occlusion. Retina 2014, in press. [Google Scholar]
- Fawzi, A.A.; Pappuru, R.R.; Sarraf, D.; Le, P.P.; McCannel, C.A.; Sobrin, L.; Goldstein, D.A.; Honowitz, S.; Walsh, A.C.; Sadda, S.R.; et al. Acute macular neuroretinopathy: Long-term insights revealed by multimodal imaging. Retina 2012, 32, 1500–1513. [Google Scholar]
- Uchida, Y.; Uchida, Y.; Kawai, S.; Kanamaru, R.; Sugiyama, Y.; Tomaru, T.; Maezawa, Y.; Kameda, N. Detection of vulnerable coronary plaques by color fluorescent angioscopy. JACC Cardiovasc. Imaging 2010, 3, 398–408. [Google Scholar]
- Ramakrishna, G.; Malouf, J.F.; Younge, B.R.; Connolly, H.M.; Miller, F.A. Calcific retinal embolism as an indicator of severe unrecognised cardiovascular disease. Heart 2005, 91, 1154–1157. [Google Scholar] [CrossRef]
- Mughal, M.M.; Khan, M.K.; DeMarco, J.K.; Majid, A.; Shamoun, F.; Abela, G.S. Symptomatic and asymptomatic carotid artery plaque. Expert Rev. Cardiovasc. Ther. 2011, 9, 1315–1330. [Google Scholar] [CrossRef]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Munk, M.R.; Mirza, R.G.; Jampol, L.M. Imaging of a Cilioretinal Artery Embolisation. Int. J. Mol. Sci. 2014, 15, 15734-15740. https://doi.org/10.3390/ijms150915734
Munk MR, Mirza RG, Jampol LM. Imaging of a Cilioretinal Artery Embolisation. International Journal of Molecular Sciences. 2014; 15(9):15734-15740. https://doi.org/10.3390/ijms150915734
Chicago/Turabian StyleMunk, Marion R., Rukhsana G. Mirza, and Lee M. Jampol. 2014. "Imaging of a Cilioretinal Artery Embolisation" International Journal of Molecular Sciences 15, no. 9: 15734-15740. https://doi.org/10.3390/ijms150915734
APA StyleMunk, M. R., Mirza, R. G., & Jampol, L. M. (2014). Imaging of a Cilioretinal Artery Embolisation. International Journal of Molecular Sciences, 15(9), 15734-15740. https://doi.org/10.3390/ijms150915734



