Cartilage Oligomeric Matrix Protein Gene Multilayers Inhibit Osteogenic Differentiation and Promote Chondrogenic Differentiation of Mesenchymal Stem Cells
Abstract
:1. Introduction
2. Results and Discussion
2.1. Characterization of the Multilayer Films
2.1.1. Contact Angle Measurement
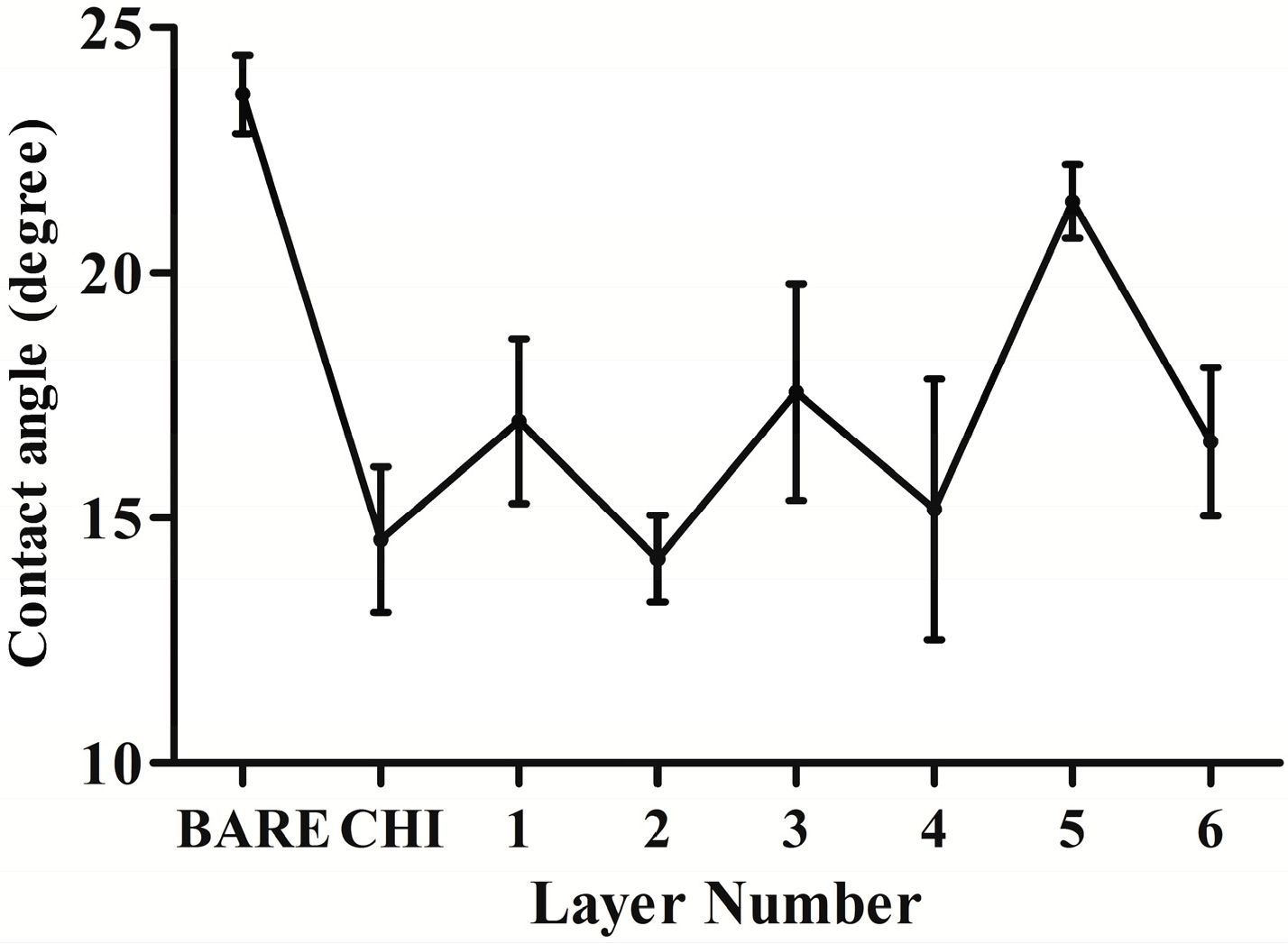
2.1.2. UV–Vis Absorption
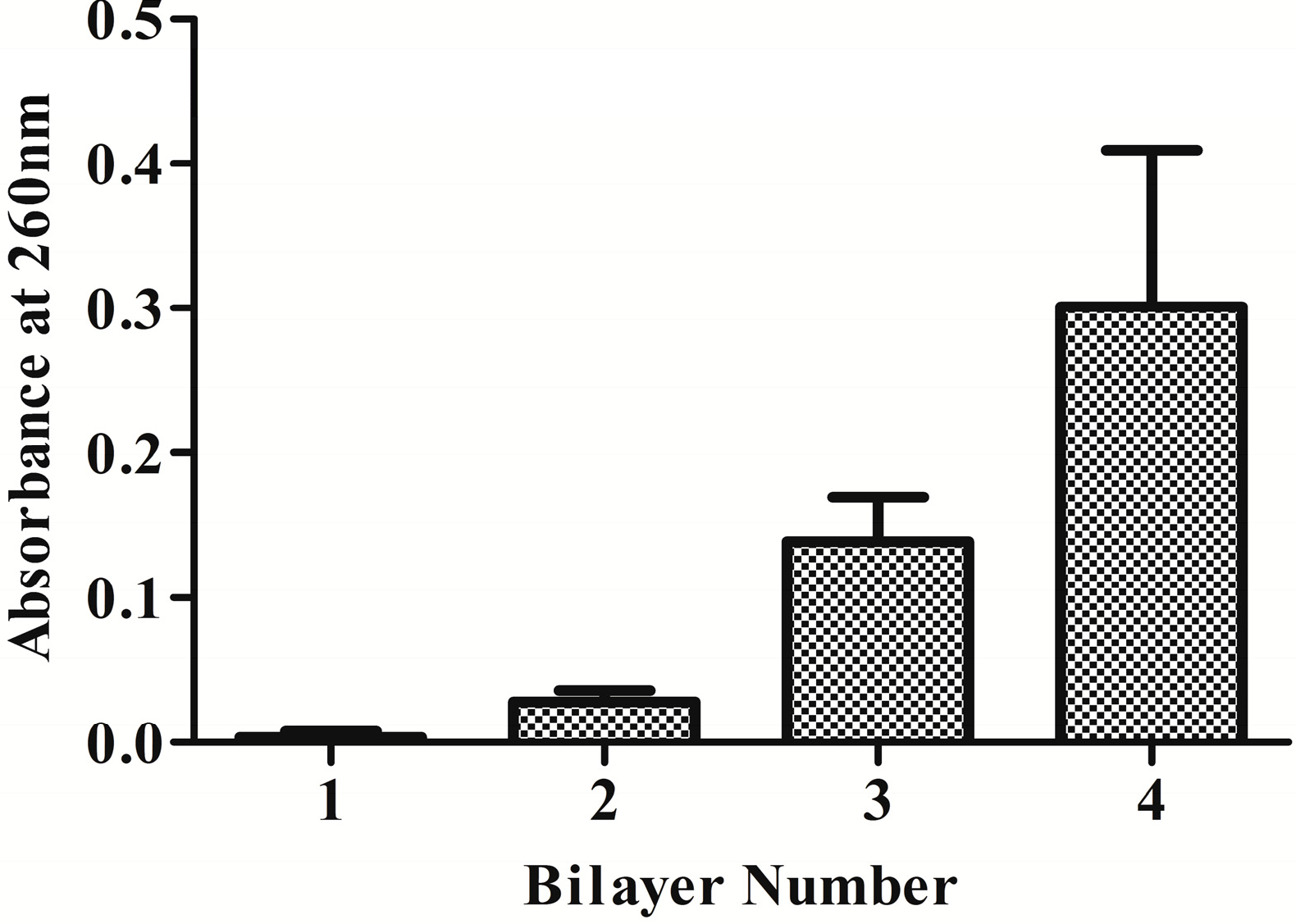
2.1.3. Surface Morphology

2.1.4. Stability Assay and Enzymatic Degradation of Multilayered Films
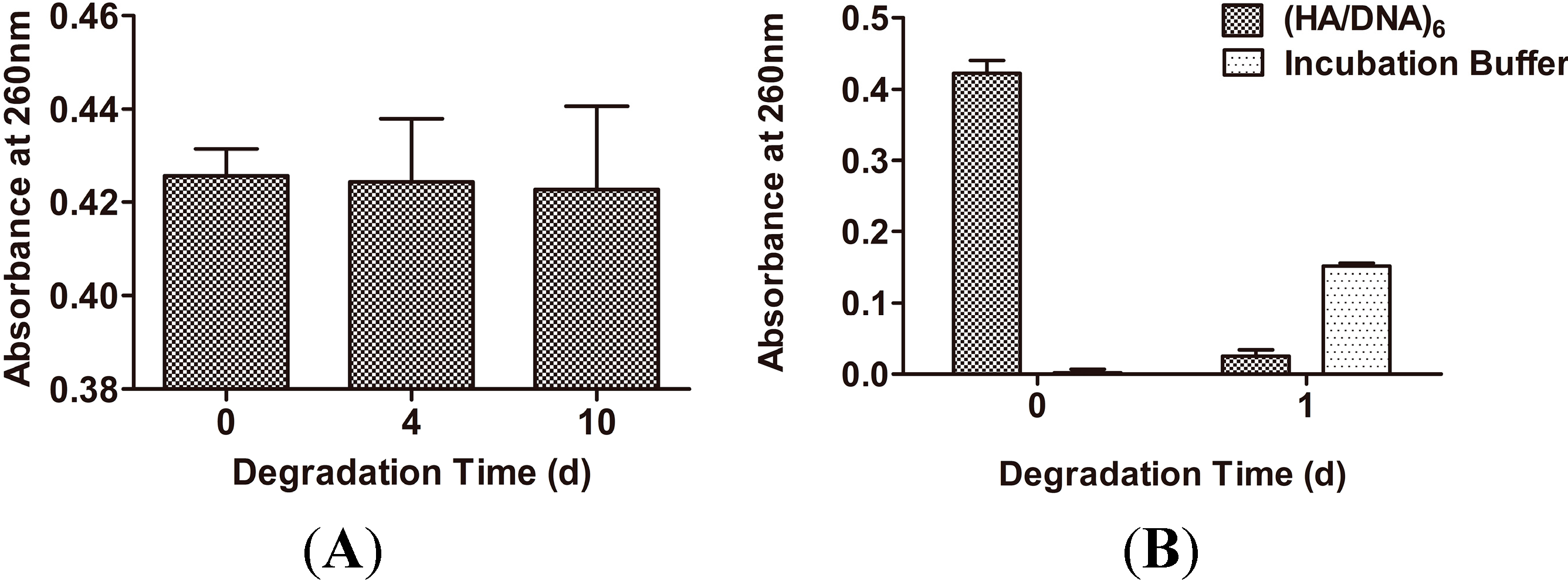
2.2. In Vitro Gene Transfection
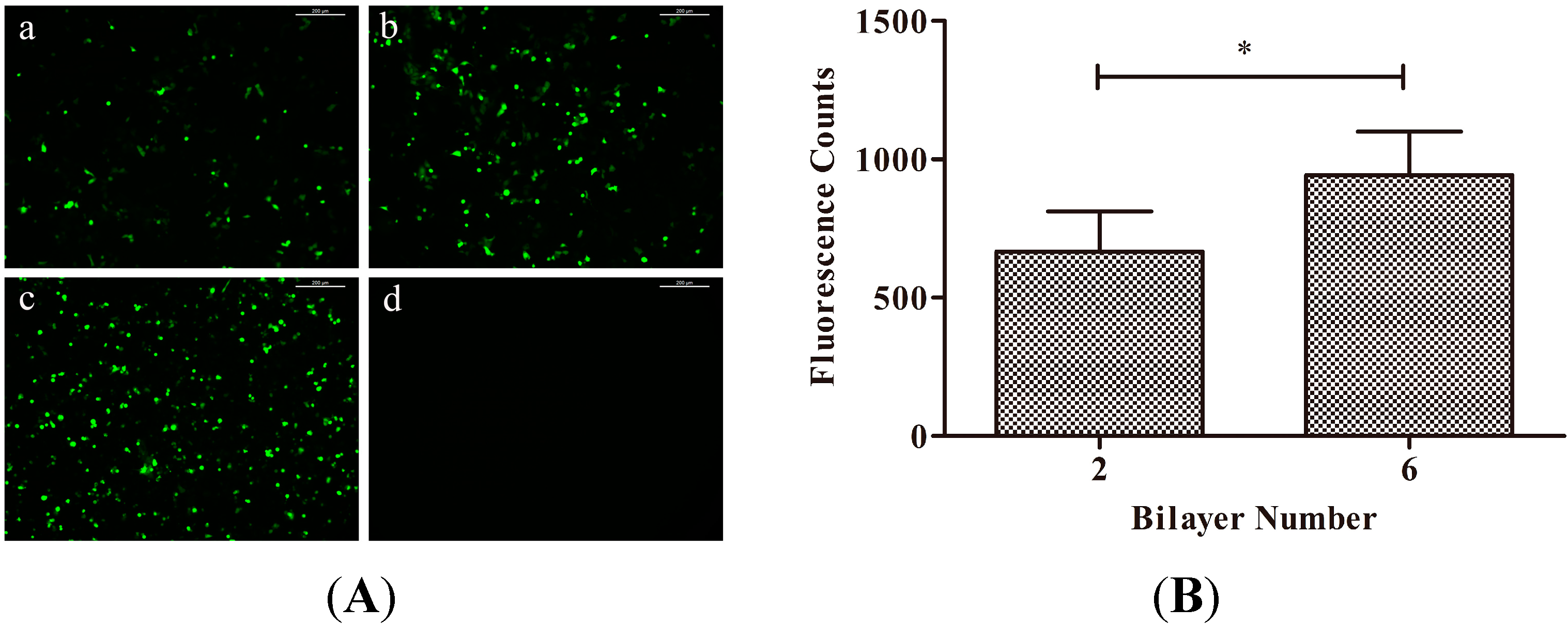
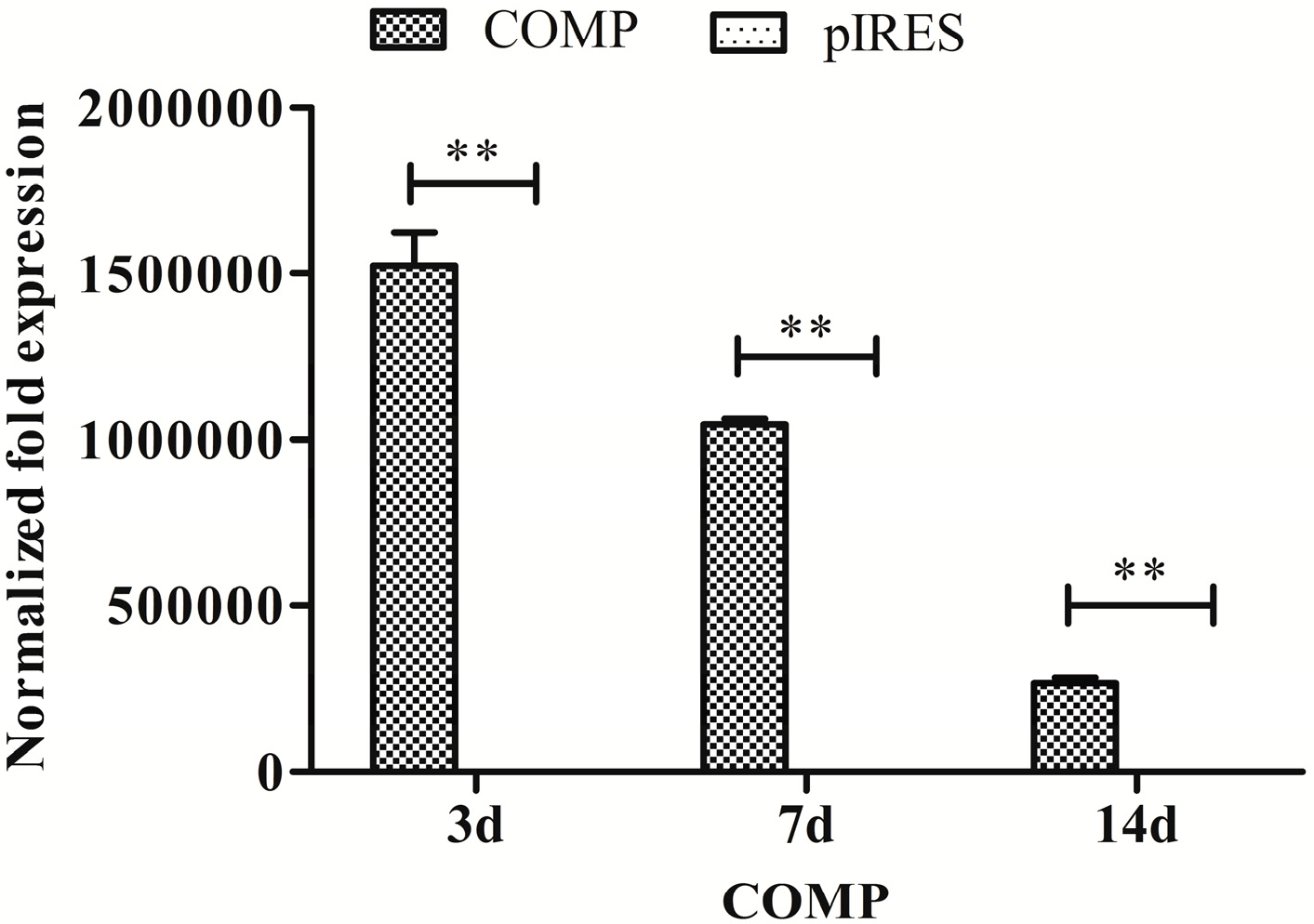
2.3. Cartilage Oligomeric Matrix Protein (COMP) Expression Detection
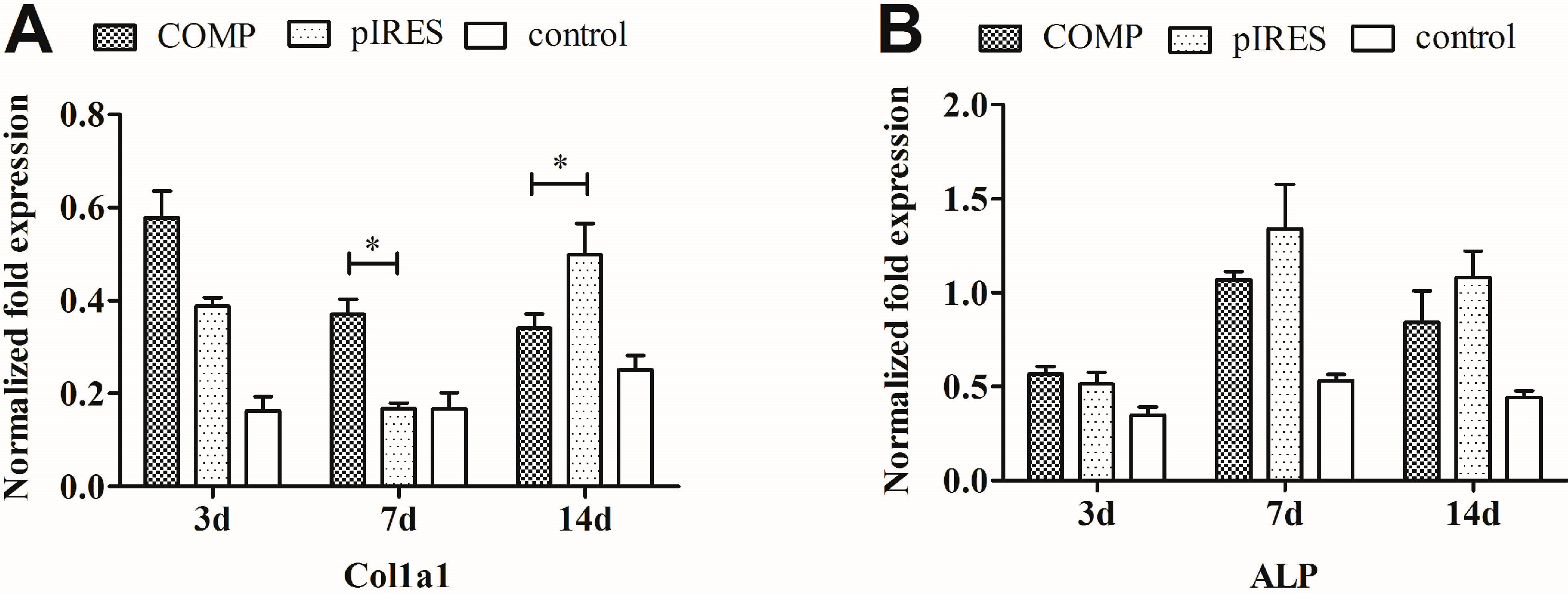
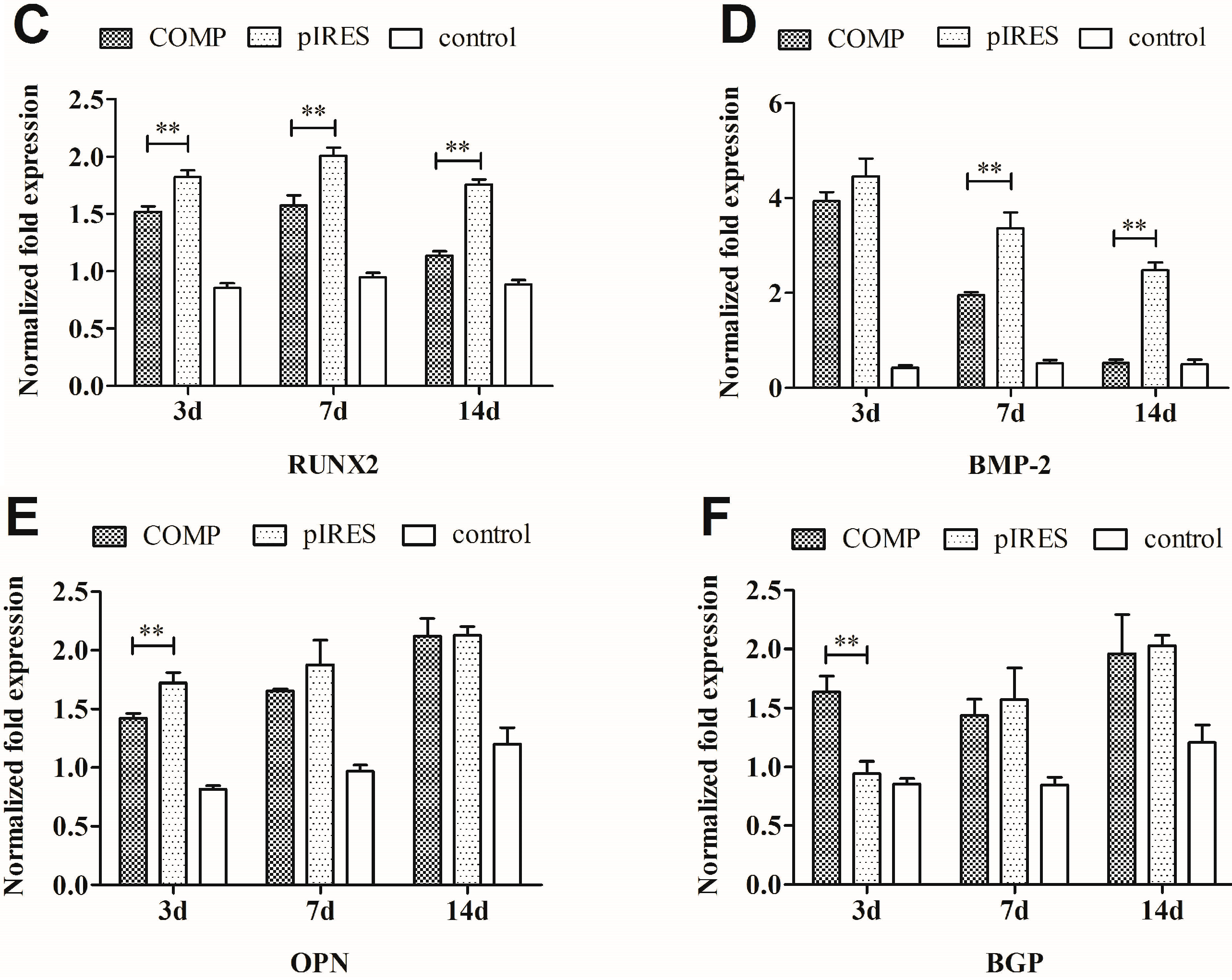
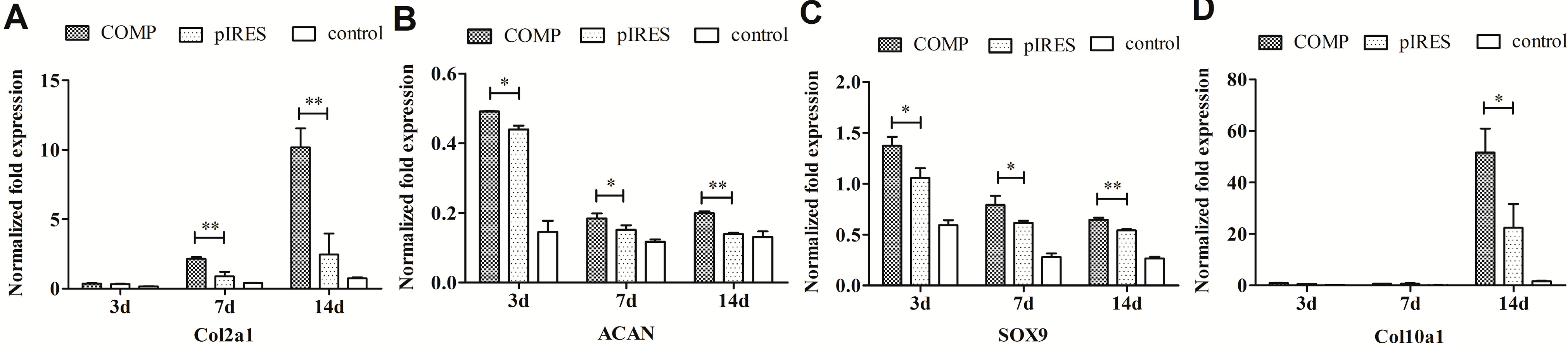
2.4. Osteogenic and Chondrogenic Gene Expression in Mesenchymal Stem Cells (MSCs)
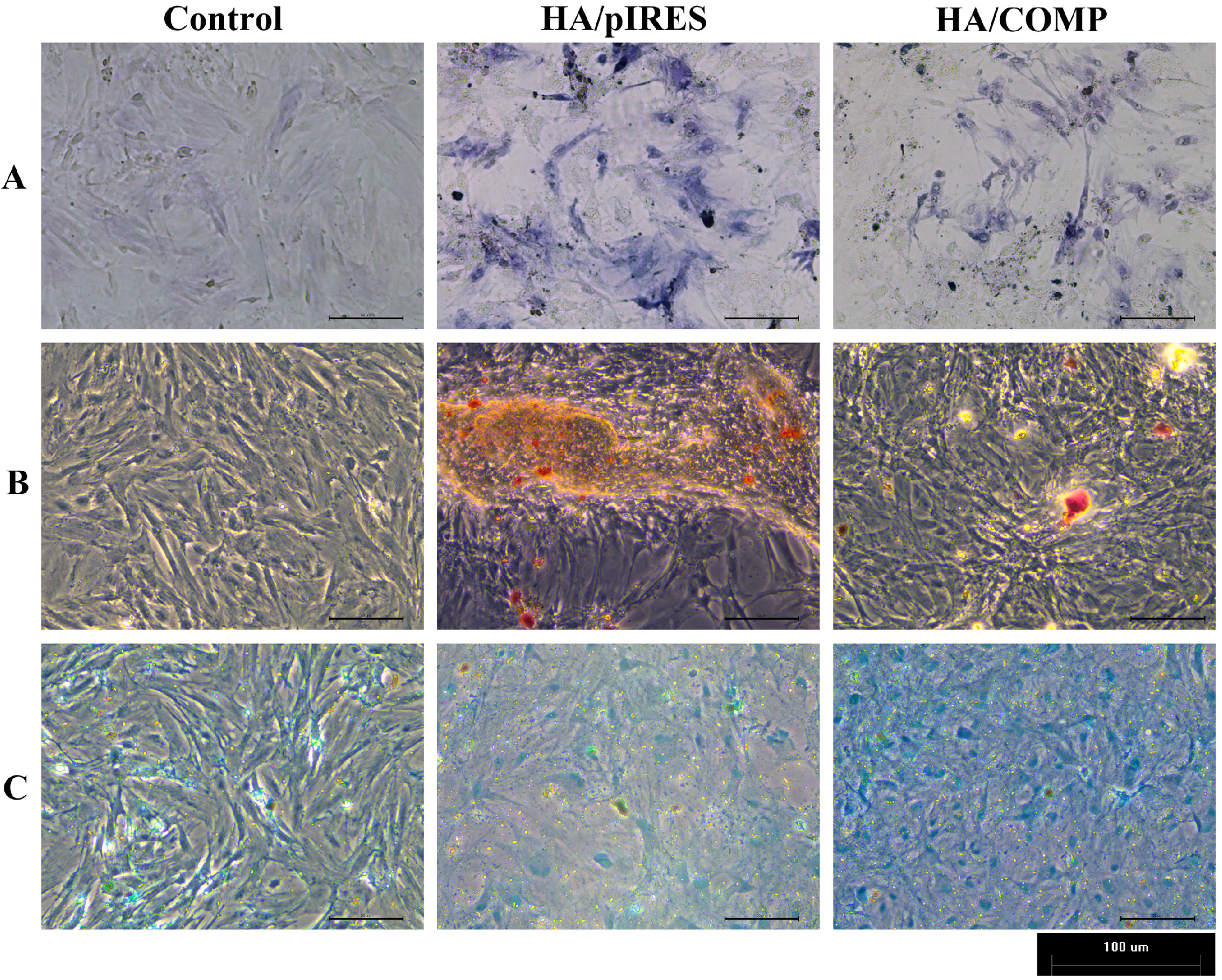
2.5. Cell Staining
2.6. Discussion
3. Experimental Section
3.1. Materials
3.2. DNA Complex Preparation
3.3. Pretreatment of Substrates
3.4. Fabrication of Multilayered Films

3.5. Characterization of the Multilayered Films
3.6. In Vitro Gene Transfection
3.7. Transfection and Differentiation of MSCs
3.8. RNA Isolation and Real-Time PCR
| Gene | Oligonucleotides (5'–3') | Gene Bank ID |
|---|---|---|
| GAPDH | F: GACATGCCGCCTGGAGAAAC | NM_017008.4 |
| R: AGCCCAGGATGCCCTTTAGT | ||
| RUNX2 | F: GCGTCCTATCAGTTCCCAAT | NM_001278483.1 |
| R: CAGCGTCAACACCATCATTC | ||
| OPN | F: CTTGGCTTACGGACTGAGG | NM_012881 |
| R: GCAACTGGGATGACCTTGAT | ||
| BMP2 | F: TGAGGATTAGCAGGTCTTTGC | NM_017178.1 |
| R: TCTCGTTTGTGGAGTGGATG | ||
| BGP | F: CAAGTCCCACACAGCAACTC | NM_013414.1 |
| R: CCAGGTCAGAGAGGCAGAAT | ||
| COMP | F: CCCAACTCAGACCAGAAGGA | NM_000095.2 |
| R: GTCACAAGCATCTCCCACAA | ||
| SOX9 | F: GACGTGCAAGCTGGGAAAGT | XM_001081628.3 |
| R: CGGCAGGTATTGGTCAAACTC | ||
| Col2α1 | F: CGCCACGGTCCTACAATGTC | NM_012929.1 |
| R: GTCACCTCTGGGTCCTTGTTCAC | ||
| ACAN | F: TGGCATTGAGGACAGCGAAG | NM_022190.1 |
| R: TCCAGTGTGTAGCGTGTGGAAATAG | ||
| Col10α1 | F: GGGATGCCTCTTGTCAGTGC | XM_001053056.4 |
| R: ATCTTGGGTCATAGTGCTGCTG | ||
| Col1α1 | F: GACATGTTCAGCTTTGTGGACCTC | NM_053304.1 |
| R: GGGACCCTTAGGCCATTGTGTA |
3.9. Cell Staining
3.10. Statistical Analysis
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Williams, D.F. On the nature of biomaterials. Biomaterials 2009, 30, 5897–5909. [Google Scholar] [CrossRef] [PubMed]
- Samuel, R.E.; Shukla, A.; Paik, D.H.; Wang, M.X.; Fang, J.C.; Schmidt, D.J.; Hammond, P.T. Osteoconductive protamine-based polyelectrolyte multilayer functionalized surfaces. Biomaterials 2011, 32, 7491–7502. [Google Scholar] [CrossRef] [PubMed]
- Liang, M.; Yao, J.; Chen, X.; Huang, L.; Shao, Z. Silk fibroin immobilization on poly(ethylene terephthalate) films: Comparison of two surface modification methods and their effect on mesenchymal stem cells culture. Mater. Sci. Eng. 2013, 33, 1409–1416. [Google Scholar] [CrossRef]
- Holmes, C.A.; Tabrizian, M. Substrate-mediated gene delivery from glycol-chitosan/hyaluronic acid polyelectrolyte multilayer films. Appl. Mater. Interf. 2013, 5, 524–531. [Google Scholar] [CrossRef]
- Ji, J.; Zhu, H.; Shen, J. Surface tailoring of poly(d,l-lactic acid) by ligand-tethered amphiphilic polymer for promoting chondrocyte attachment and growth. Biomaterials 2004, 25, 1859–1867. [Google Scholar] [CrossRef] [PubMed]
- Petrie, T.A.; Raynor, J.E.; Reyes, C.D.; Burns, K.L.; Collard, D.M.; García, A.J. The effect of integrin-specific bioactive coatings on tissue healing and implant osseointegration. Biomaterials 2008, 29, 2849–2857. [Google Scholar] [CrossRef] [PubMed]
- Roach, P.; Eglin, D.; Rohde, K.; Perry, C.C. Modern biomaterials: A review—Bulk properties and implications of surface modifications. J. Mater. Sci. 2007, 18, 1263–1277. [Google Scholar]
- Cai, K.; Hu, Y.; Luo, Z.; Kong, T.; Lai, M.; Sui, X.; Wang, Y.; Yang, L.; Deng, L. Cell-specific gene transfection from a gene-functionalized poly(d,l-lactic acid) substrate fabricated by the layer-by-layer assembly technique. Angew. Chem. Int. Ed. 2008, 47, 7479–7481. [Google Scholar] [CrossRef]
- Jessel, N.; Oulad-Abdelghani, M.; Meyer, F.; Lavalle, P.; Haîkel, Y.; Schaaf, P.; Voegel, J.-C. Multiple and time-scheduled in situ DNA delivery mediated by β-cyclodextrin embedded in a polyelectrolyte multilayer. Proc. Natl. Acad. Sci. USA 2006, 103, 8618–8621. [Google Scholar] [CrossRef] [PubMed]
- Kong, H.J.; Liu, J.; Riddle, K.; Matsumoto, T.; Leach, K.; Mooney, D.J. Non-viral gene delivery regulated by stiffness of cell adhesion substrates. Nat. Mater. 2005, 4, 460–464. [Google Scholar] [CrossRef] [PubMed]
- Shen, H.; Tan, J.; Saltzman, W.M. Surface-mediated gene transfer from nanocomposites of controlled texture. Nat. Mater. 2004, 3, 569–574. [Google Scholar] [CrossRef] [PubMed]
- Decher, G.; Hong, J.D.; Schmitt, J. Buildup of ultrathin multilayer films by a self-assembly process: III. Consecutively alternating adsorption of anionic and cationic polyelectrolytes on charged surfaces. Thin Solid Films 1992, 210–211, 831–835. [Google Scholar] [CrossRef]
- Decher, G. Fuzzy nanoassemblies: Toward layered polymeric multicomposites. Science 1997, 277, 1232–1237. [Google Scholar] [CrossRef]
- Ren, K.; Wang, Y.; Ji, J.; Lin, Q.; Shen, J. Construction and deconstruction of PLL/DNA multilayered films for DNA delivery: Effect of ionic strength. Colloids Surf. B 2005, 46, 63–69. [Google Scholar] [CrossRef]
- Liu, L.; Song, L.-N.; Yang, G.-L.; Zhao, S.-F.; He, F.-M. Fabrication, characterization, and biological assessment of multilayer DNA coatings on sandblasted-dual acid etched titanium surface. J. Biomed. Mater. Res. 2011, 97, 300–310. [Google Scholar] [CrossRef]
- Ren, K.; Ji, J.; Shen, J. Tunable DNA release from cross-linked ultrathin DNA/PLL multilayered films. Bioconjug. Chem. 2006, 17, 77–83. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Q.-H.; Liu, L.; Shen, J.-W.; Peel, S.; Yang, G.-L.; Zhao, S.-F.; He, F.-M. Influence of multilayer rhBMP-2 DNA coating on the proliferation and differentiation of MC3T3-E1 cells seeded on roughed titanium surface. J. Biomed. Mater. Res. 2012, 100, 2766–2774. [Google Scholar] [CrossRef]
- Hu, Y.; Cai, K.; Luo, Z.; Zhang, Y.; Li, L.; Lai, M.; Hou, Y.; Huang, Y.; Li, J.; Ding, X.; et al. Regulation of the differentiation of mesenchymal stem cells in vitro and osteogenesis in vivo by microenvironmental modification of titanium alloy surfaces. Biomaterials 2012, 33, 3515–3528. [Google Scholar] [CrossRef] [PubMed]
- Hu, Y.; Cai, K.; Luo, Z.; Zhang, R.; Yang, L.; Deng, L.; Jandt, K.D. Surface mediated in situ differentiation of mesenchymal stem cells on gene-functionalized titanium films fabricated by layer-by-layer technique. Biomaterials 2009, 30, 3626–3635. [Google Scholar] [CrossRef] [PubMed]
- Yang, P.J.; Temenoff, J.S. Engineering orthopedic tissue interfaces. Tissue Eng. 2009, 15, 127–141. [Google Scholar] [CrossRef]
- Rock, M.J.; Holden, P.; Horton, W.A.; Cohn, D.H. Cartilage oligomeric matrix protein promotes cell attachment via two independent mechanisms involving CD47 and αVβ3 integrin. Mol. Cell. Biochem. 2010, 338, 215–224. [Google Scholar] [CrossRef] [PubMed]
- Tan, K.; Duquette, M.; Joachimiak, A.; Lawler, J. The crystal structure of the signature domain of cartilage oligomeric matrix protein: Implications for collagen, glycosaminoglycan and integrin binding. FASEB J. 2009, 23, 2490–2501. [Google Scholar] [CrossRef] [PubMed]
- Chen, F.H.; Herndon, M.E.; Patel, N.; Hecht, J.T.; Tuan, R.S.; Lawler, J. Interaction of cartilage oligomeric matrix protein/thrombospondin 5 with aggrecan. J. Biol. Chem. 2007, 282, 24591–24598. [Google Scholar] [CrossRef] [PubMed]
- Du, Y.; Wang, Y.; Wang, L.; Liu, B.; Tian, Q.; Liu, C.-J.; Zhang, T.; Xu, Q.; Zhu, Y.; Ake, O.; et al. Cartilage oligomeric matrix protein inhibits vascular smooth muscle calcification by interacting with bone morphogenetic protein-2. Circ. Res. 2011, 108, 917–928. [Google Scholar] [CrossRef] [PubMed]
- Yamauchi, F.; Koyamatsu, Y.; Kato, K.; Iwata, H. Layer-by-layer assembly of cationic lipid and plasmid DNA onto gold surface for stent-assisted gene transfer. Biomaterials 2006, 27, 3497–3504. [Google Scholar] [CrossRef] [PubMed]
- Suci, P.A.; Klem, M.T.; Arce, F.T.; Douglas, T.; Young, M. Assembly of multilayer films incorporating a viral protein cage architecture. Langmuir 2006, 22, 8891–8896. [Google Scholar] [CrossRef] [PubMed]
- Li, G.; Yang, P.; Qin, W.; Maitz, M.F.; Zhou, S.; Huang, N. The effect of coimmobilizing heparin and fibronectin on titanium on hemocompatibility and endothelialization. Biomaterials 2011, 32, 4691–4703. [Google Scholar] [CrossRef] [PubMed]
- Lin, Q.; Ding, X.; Qiu, F.; Song, X.; Fu, G.; Ji, J. In situ endothelialization of intravascular stents coated with an anti-CD34 antibody functionalized heparin-collagen multilayer. Biomaterials 2010, 31, 4017–4025. [Google Scholar] [CrossRef] [PubMed]
- Zan, X.; Sitasuwan, P.; Powell, J.; Dreher, T.W.; Wang, Q. Polyvalent display of RGD motifs on turnip yellow mosaic virus for enhanced stem cell adhesion and spreading. Acta Biomater. 2012, 8, 2978–2985. [Google Scholar] [CrossRef] [PubMed]
- Richert, L.; Schneider, A.; Vautier, D.; Vodouhe, C.; Jessel, N.; Payan, E.; Schaaf, P.; Voegel, J.-C.; Picart, C. Imaging cell interactions with native and crosslinked polyelectrolyte multilayers. Cell Biochem. Biophys. 2006, 44, 273–285. [Google Scholar] [CrossRef] [PubMed]
- Blin, G.; Lablack, N.; Louis-Tisserand, M.; Nicolas, C.; Picart, C.; Pucéat, M. Nano-scale control of cellular environment to drive embryonic stem cells selfrenewal and fate. Biomaterials 2010, 31, 1742–1750. [Google Scholar] [CrossRef] [PubMed]
- Blacklock, J.; Vetter, A.; Lankenau, A.; Oupický, D.; Möhwald, H. Tuning the mechanical properties of bioreducible multilayer films for improved cell adhesion and transfection activity. Biomaterials 2010, 31, 7167–7174. [Google Scholar] [CrossRef] [PubMed]
- Keeney, M.; van den Beucken, J.J.J.P.; van der Kraan, P.M.; Jansen, J.A.; Pandit, A. The ability of a collagen/calcium phosphate scaffold to act as its own vector for gene delivery and to promote bone formation via transfection with VEGF165. Biomaterials 2010, 31, 2893–2902. [Google Scholar] [CrossRef] [PubMed]
- Milz, S.; Aktas, T.; Putz, R.; Benjamin, M. Expression of extracellular matrix molecules typical of articular cartilage in the human scapholunate interosseous ligament. J. Anat. 2006, 208, 671–679. [Google Scholar] [CrossRef] [PubMed]
- Zaucke, F.; Grässel, S. Genetic mouse models for the functional analysis of the perifibrillar components collagen IX, COMP and matrilin-3: Implications for growth cartilage differentiation and endochondral ossification. Histol. Histopathol. 2009, 24, 1067–1079. [Google Scholar] [PubMed]
- Ren, K.; Ji, J.; Shen, J. Construction and enzymatic degradation of multilayered poly-l-lysine/DNA films. Biomaterials 2006, 27, 1152–1159. [Google Scholar] [CrossRef] [PubMed]
- Chang, H.; Ren, K.-F.; Wang, J.-L.; Zhang, H.; Wang, B.-L.; Zheng, S.-M.; Zhou, Y.-Y.; Ji, J. Surface-mediated functional gene delivery: An effective strategy for enhancing competitiveness of endothelial cells over smooth muscle cells. Biomaterials 2013, 34, 3345–3354. [Google Scholar] [CrossRef] [PubMed]
- Larchian, W.A.; Horiguchi, Y.; Nair, S.K.; Fair, W.R.; Heston, W.D.; Gilboa, E. Effectiveness of combined interleukin 2 and B7.1 vaccination strategy is dependent on the sequence and order: A liposome-mediated gene therapy treatment for bladder cancer. Clin. Cancer Res. 2000, 6, 2913–2920. [Google Scholar] [PubMed]
- Tanswell, A.K.; Staub, O.; Iles, R.; Belcastro, R.; Cabacungan, J.; Sedlackova, L.; Steer, B.; Wen, Y.; Hu, J.; O’Brodovich, H. Liposome-mediated transfection of fetal lung epithelial cells: DNA degradation and enhanced superoxide toxicity. Am. J. Phys. 1998, 275, L452–L460. [Google Scholar]
- Lian, J.B.; Stein, G.S.; Javed, A.; van Wijnen, A.J.; Stein, J.L.; Montecino, M.; Hassan, M.Q.; Gaur, T.; Lengner, C.J.; Young, D.W. Networks and hubs for the transcriptional control of osteoblastogenesis. Rev. Endocr. Metab. Disord. 2006, 7, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.S.; Kim, H.J.; Li, Q.L.; Chi, X.Z.; Ueta, C.; Komori, T.; Wozney, J.M.; Kim, E.G.; Choi, J.Y.; Ryoo, H.M.; et al. Runx2 is a common target of transforming growth factor β1 and bone morphogenetic protein 2, and cooperation between Runx2 and Smad5 induces osteoblast-specific gene expression in the pluripotent mesenchymal precursor cell line C2C12. Mol. Cell. Biol. 2000, 20, 8783–8792. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.H.; Javed, A.; Kim, H.J.; Shin, H.I.; Gutierrez, S.; Choi, J.Y.; Rosen, V.; Stein, J.L.; van Wijnen, A.J.; Stein, G.S.; et al. Transient upregulation of CBFA1 in response to bone morphogenetic protein-2 and transforming growth factor β1 in C2C12 myogenic cells coincides with suppression of the myogenic phenotype but is not sufficient for osteoblast differentiation. J. Cell. Biochem. 1999, 73, 114–125. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Sun, J.; Ji, J. pH modulated layer-by-layer assembly as a new approach to tunable formulating of DNA within multilayer coating. React. Funct. Polym. 2011, 71, 254–260. [Google Scholar] [CrossRef]
- Sharff, K.A.; Song, W.-X.; Luo, X.; Tang, N.; Luo, J.; Chen, J.; Bi, Y.; He, B.-C.; Huang, J.; Li, X.; et al. Hey1 basic helix-loop-helix protein plays an important role in mediating BMP9-induced osteogenic differentiation of mesenchymal progenitor cells. J. Biol. Chem. 2009, 284, 649–659. [Google Scholar] [CrossRef] [PubMed]
- Liao, J.; Hu, N.; Zhou, N.; Lin, L.; Zhao, C.; Yi, S.; Fan, T.; Bao, W.; Liang, X.; Chen, H.; et al. Sox9 potentiates BMP2-induced chondrogenic differentiation and inhibits BMP2-induced osteogenic differentiation. PLoS One 2014, 9, e89025. [Google Scholar] [CrossRef] [PubMed]
© 2014 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Guo, P.; Shi, Z.-L.; Liu, A.; Lin, T.; Bi, F.-G.; Shi, M.-M.; Yan, S.-G. Cartilage Oligomeric Matrix Protein Gene Multilayers Inhibit Osteogenic Differentiation and Promote Chondrogenic Differentiation of Mesenchymal Stem Cells. Int. J. Mol. Sci. 2014, 15, 20117-20133. https://doi.org/10.3390/ijms151120117
Guo P, Shi Z-L, Liu A, Lin T, Bi F-G, Shi M-M, Yan S-G. Cartilage Oligomeric Matrix Protein Gene Multilayers Inhibit Osteogenic Differentiation and Promote Chondrogenic Differentiation of Mesenchymal Stem Cells. International Journal of Molecular Sciences. 2014; 15(11):20117-20133. https://doi.org/10.3390/ijms151120117
Chicago/Turabian StyleGuo, Peng, Zhong-Li Shi, An Liu, Tiao Lin, Fang-Gang Bi, Ming-Min Shi, and Shi-Gui Yan. 2014. "Cartilage Oligomeric Matrix Protein Gene Multilayers Inhibit Osteogenic Differentiation and Promote Chondrogenic Differentiation of Mesenchymal Stem Cells" International Journal of Molecular Sciences 15, no. 11: 20117-20133. https://doi.org/10.3390/ijms151120117
APA StyleGuo, P., Shi, Z.-L., Liu, A., Lin, T., Bi, F.-G., Shi, M.-M., & Yan, S.-G. (2014). Cartilage Oligomeric Matrix Protein Gene Multilayers Inhibit Osteogenic Differentiation and Promote Chondrogenic Differentiation of Mesenchymal Stem Cells. International Journal of Molecular Sciences, 15(11), 20117-20133. https://doi.org/10.3390/ijms151120117





