Supersaturation and Precipitation Applicated in Drug Delivery Systems: Development Strategies and Evaluation Approaches
Abstract
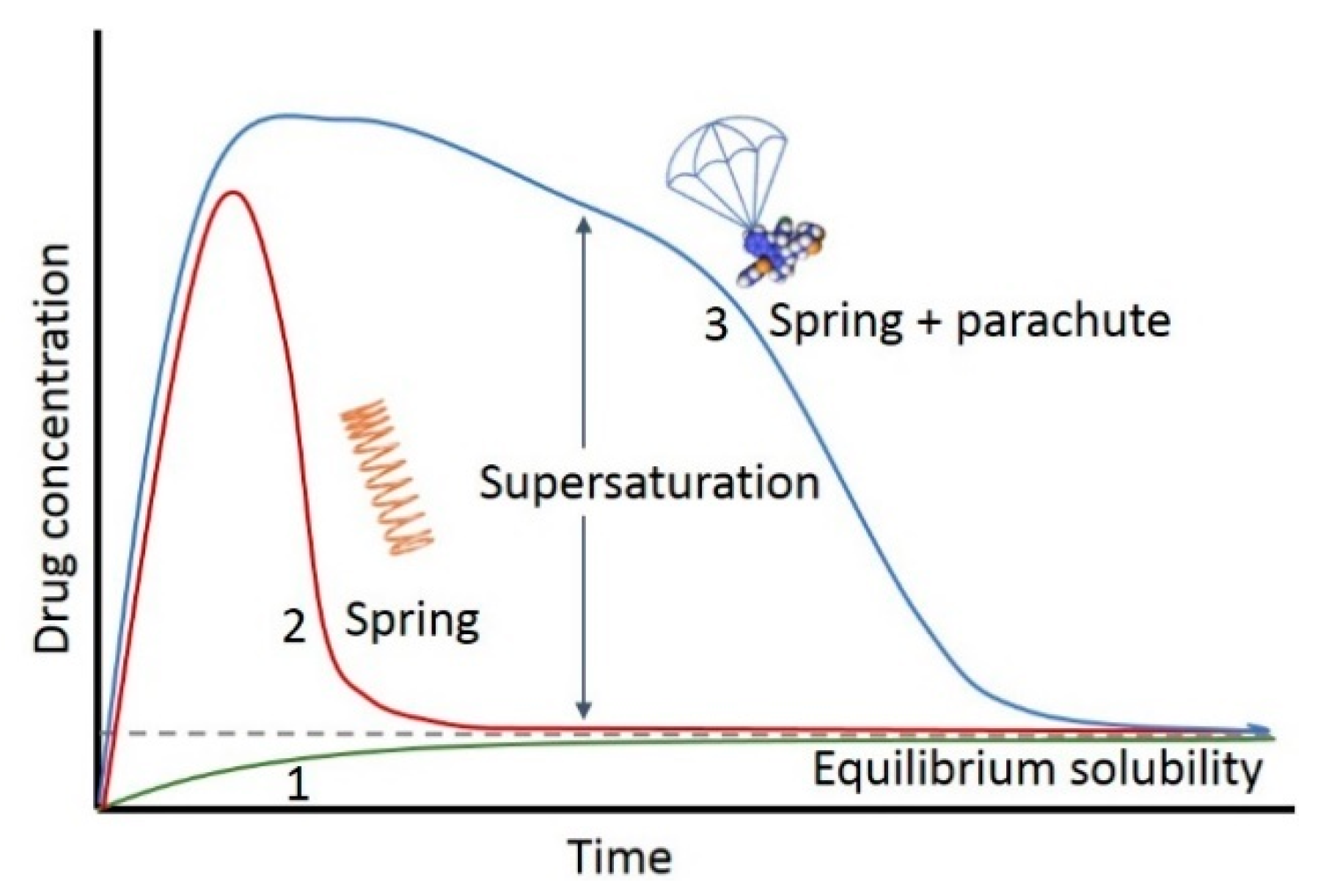
1. Introduction
- Generation of supersaturation;
- Inhibition of precipitation;
- Mechanism studies and evaluation approaches.
2. Generation of Supersaturation
2.1. pH-Shift
2.2. Supersaturating Drug Delivery System (SDDS)
2.2.1. Amorphous Solid Dispersion (ASD)
2.2.2. Self-Emulsifying Drug Delivery System (SEDDS)
2.2.3. Mesoporous Material-Based Dosage Form
3. Inhibition of Precipitation
3.1. Mechanism of Precipitation Inhibition
- (1)
- Enhancing viscosity to reduce molecular motion (hindering nucleation) and diffusion coefficient (impeding crystal growth);.
- (2)
- Improving mass-liquid surface energy;
- (3)
- Changing the absorption layer of the crystal surface, such as adhering to the crystal surface to block the growth of the crystal and influence the crystal properties;
- (4)
- Controlling the dissolution of the crystal surface, thus influencing the molecules to concentrate in the crystal;
- (5)
- Increasing solubility to decrease DS.
3.2. Character of Precipitation Inhibitors
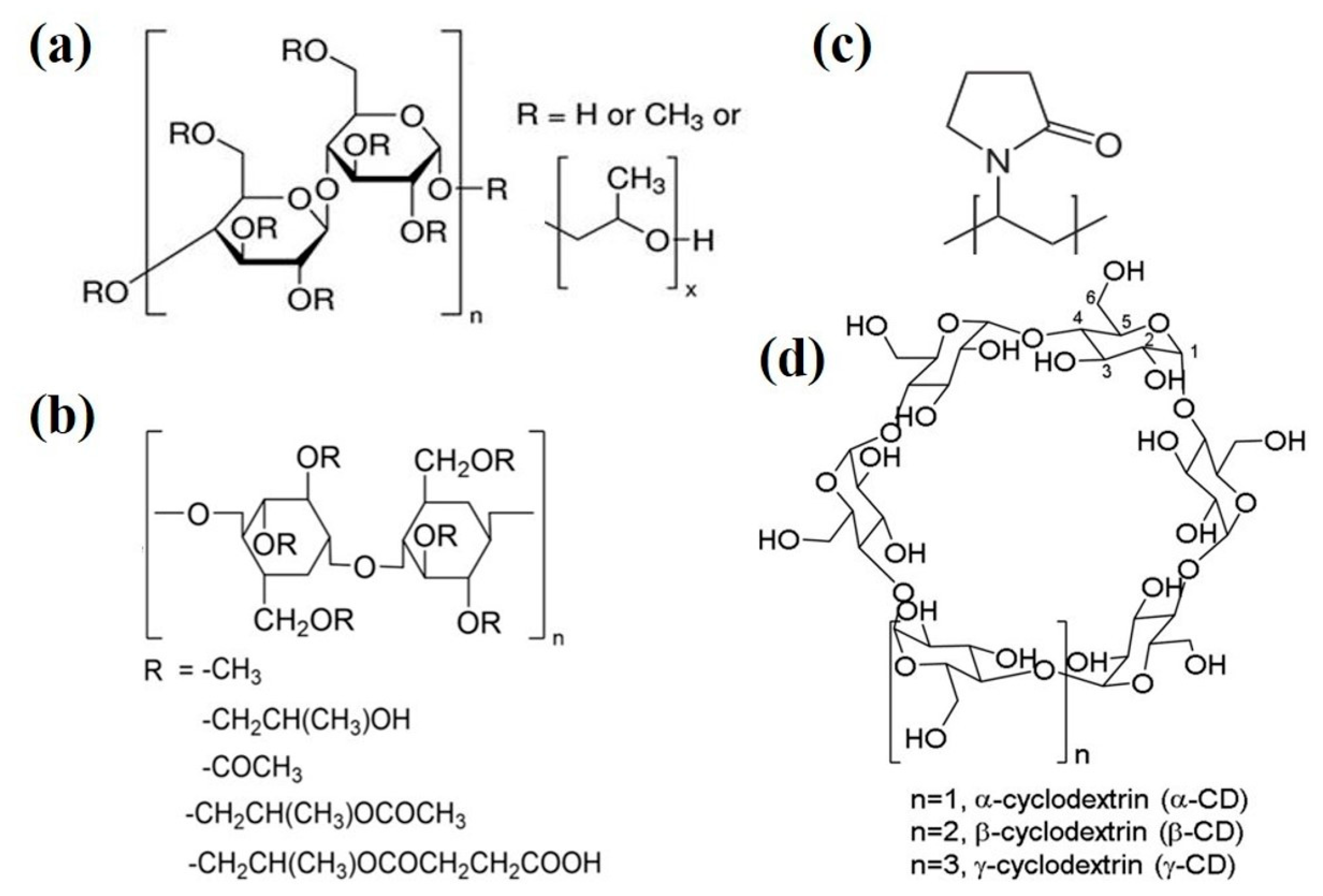
3.2.1. Hydroxypropyl Methylcellulose (HPMC)
3.2.2. Hydroxypropylmethylcellulose-Acetate Succinate (HPMCAS)
3.2.3. Polyvinyl Pyrrolidone (PVP)
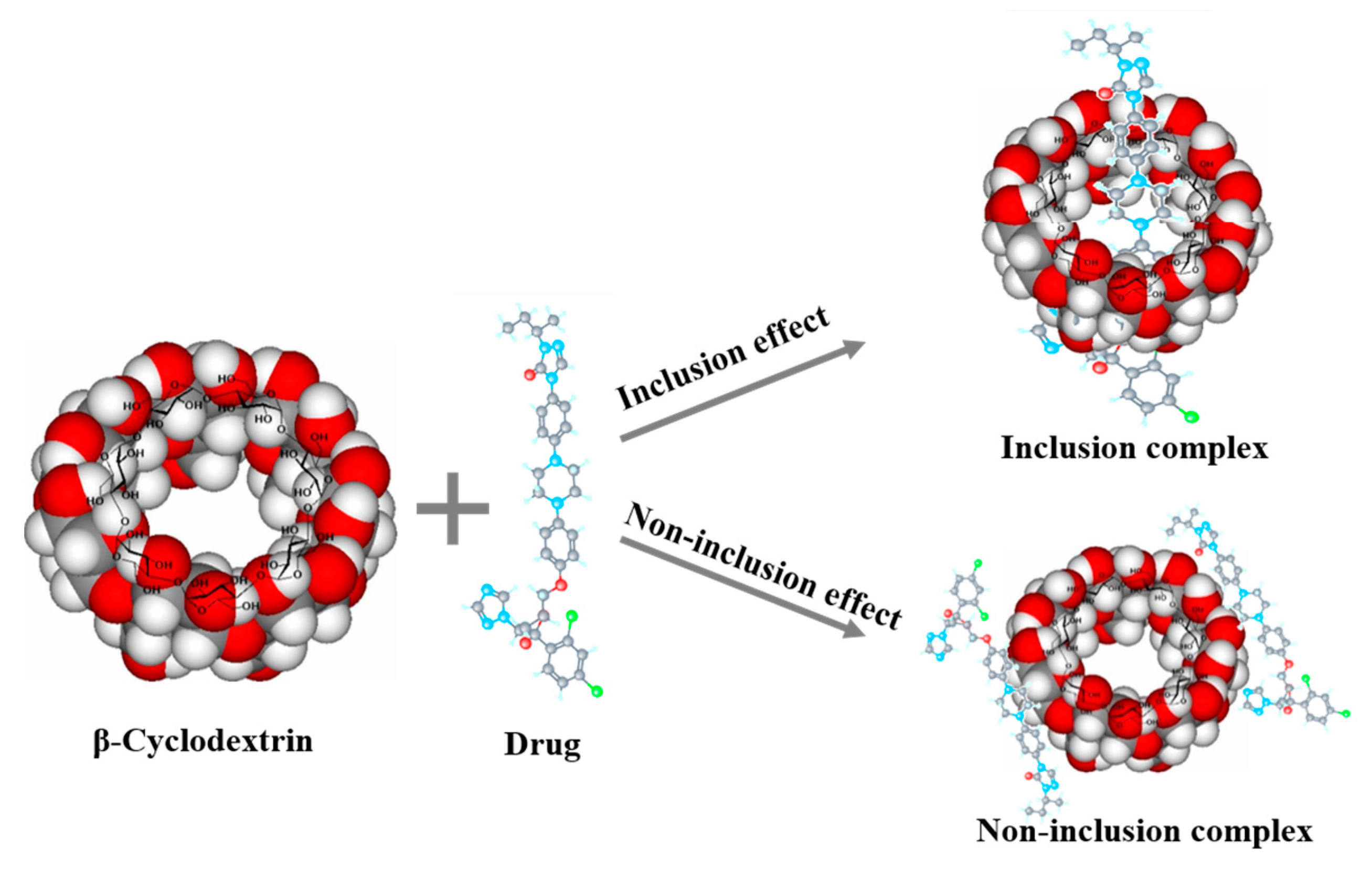
3.2.4. Cyclodextrins
3.2.5. Others Precipitation Inhibitors
3.3. Screening Precipitation Inhibitors
4. Mechanism Studies and Evaluation Approaches
4.1. In Vitro Studies
4.1.1. Biorelevant Media
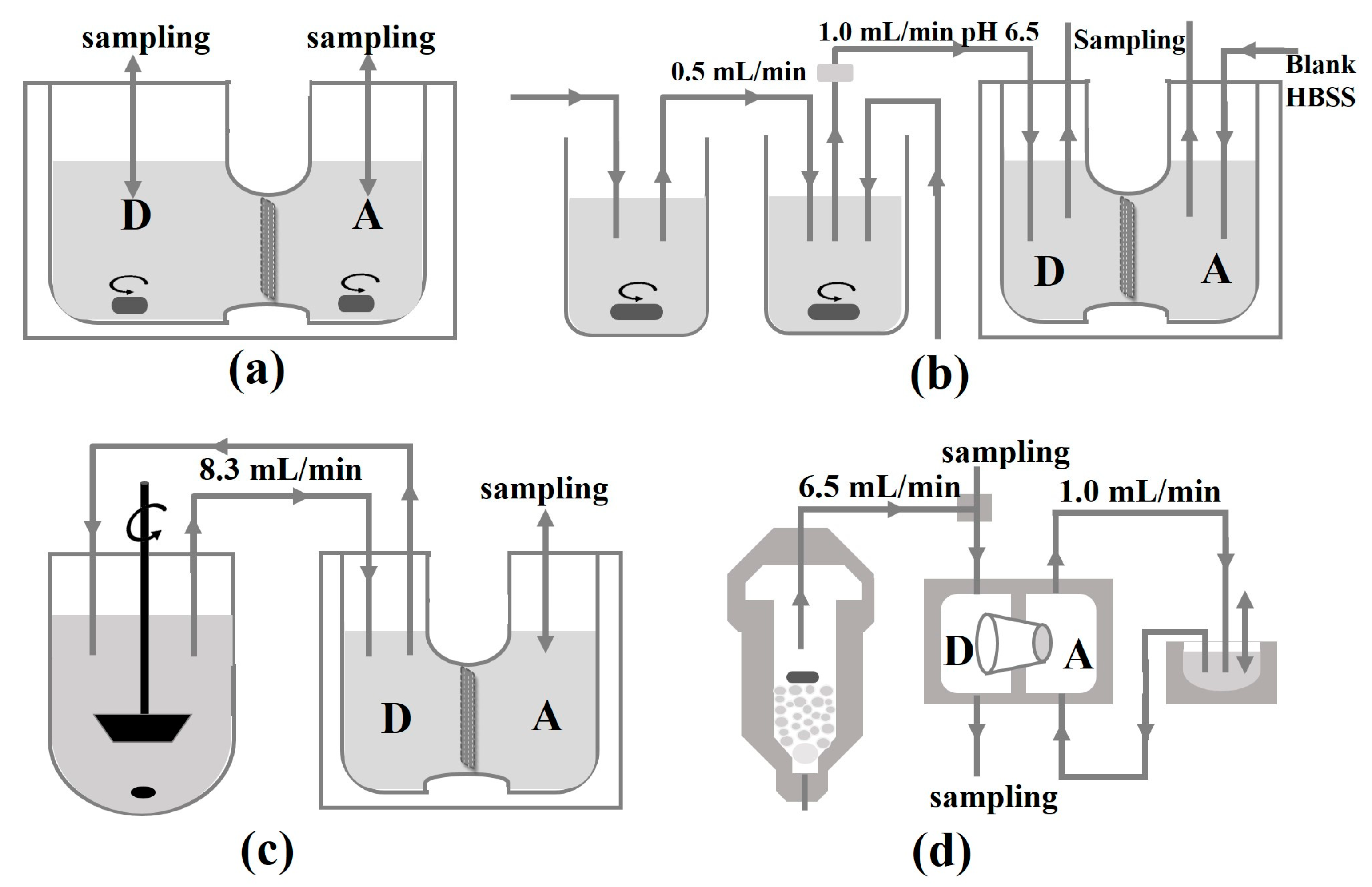
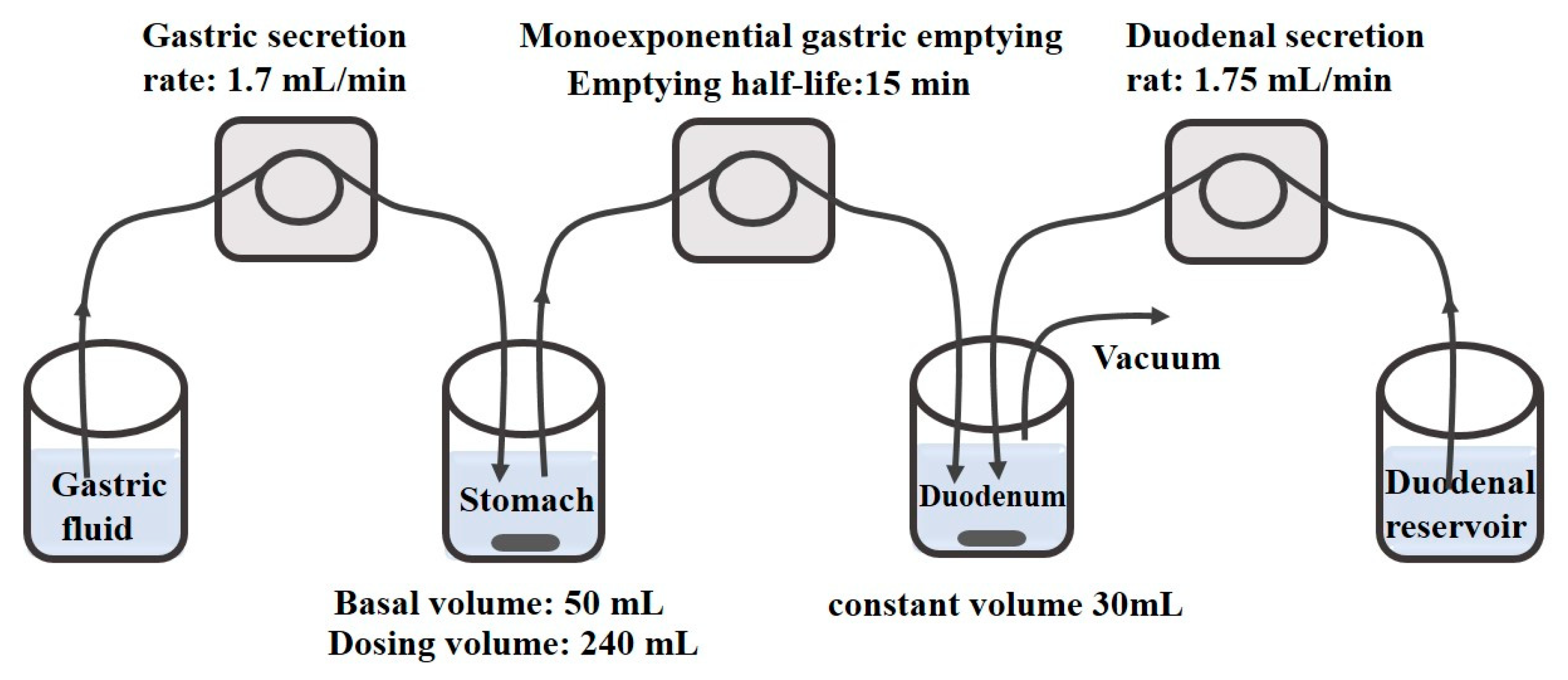
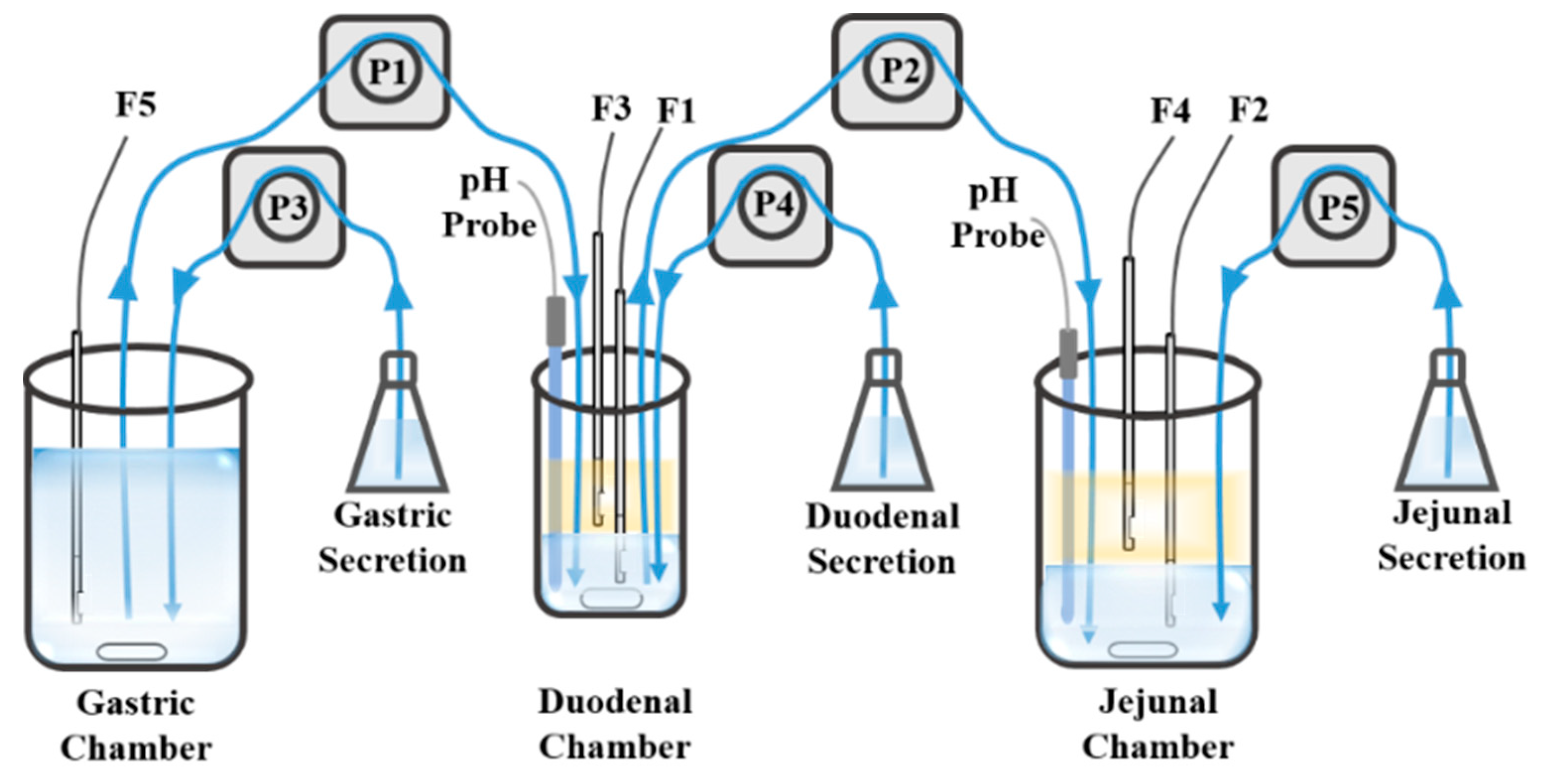
4.1.2. Biomimetic Apparatus
4.2. In Vivo Studies
4.2.1. Oral Absorption
4.2.2. Intestinal Perfusion
4.2.3. Intestinal Content Aspiration
4.3. In Silico Studies
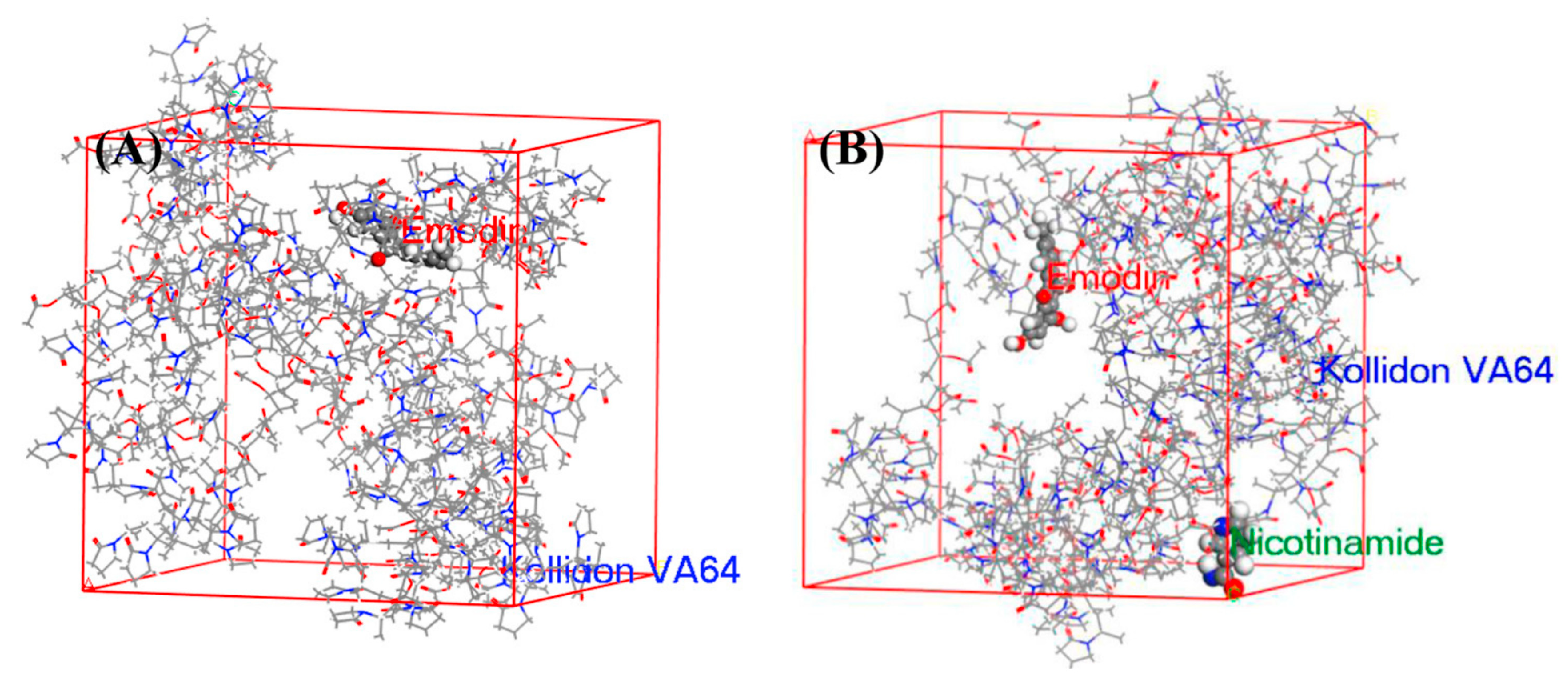
4.3.1. Molecular Modeling
4.3.2. Pharmacokinetic Simulation
4.4. In Vitro–In Vivo Correlation (IVIVC)
5. Discussion and Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Amidon, G.L.; Lennernas, H.; Shah, V.P.; Crison, J.R. A theoretical basis for a biopharmaceutic drug classification: The correlation of in vitro drug product dissolution and in vivo bioavailability. Pharm. Res. 1995, 12, 413–420. [Google Scholar] [CrossRef] [PubMed]
- Brouwers, J.; Brewster, M.E.; Augustijns, P. Supersaturating drug delivery systems: The answer to solubility-limited oral bioavailability? J. Pharm. Sci. 2009, 98, 2549–2572. [Google Scholar] [CrossRef] [PubMed]
- Guzmán, H.; Tawa, M.; Zhang, Z.; Ratanabanangkoon, P.; Shaw, P.; Mustonen, P.; Gardner, C.; Chen, H.; Moreau, J.-P.; Almarsson, O.; et al. Spring and parachute approach to designing solid celecoxib formulations having enhanced oral absorption. AAPS J. 2004, 6, T2189. [Google Scholar]
- Bevernage, J.; Brouwers, J.; Brewster, M.E.; Augustijns, P. Evaluation of gastrointestinal drug supersaturation and precipitation: Strategies and issues. Int. J. Pharm. 2013, 453, 25–35. [Google Scholar] [CrossRef]
- Fong, S.Y.; Bauer-Brandl, A.; Brandl, M. Oral bioavailability enhancement through supersaturation: An update and meta-analysis. Expert Opin. Drug Deliv. 2017, 14, 403–426. [Google Scholar] [CrossRef] [PubMed]
- Mitra, A.; Fadda, H.M. Effect of surfactants, gastric emptying, and dosage form on supersaturation of dipyridamole in an in vitro model simulating the stomach and duodenum. Mol. Pharm. 2014, 11, 2835–2844. [Google Scholar] [CrossRef]
- Plum, J.; Bavnhøj, C.; Palmelund, H.; Pérez-Alós, L.; Müllertz, A.; Rades, T. Comparison of induction methods for supersaturation: pH shift versus solvent shift. Int. J. Pharm. 2020, 573, 118862. [Google Scholar] [CrossRef]
- Wen, H.; Park, K. Introduction and Overview of Oral Controlled Release Formulation Design; John Wiley & Sons, Inc.: New York, NY, USA, 2010; pp. 271–272. [Google Scholar]
- Vertzoni, M.; Diakidou, A.; Chatzilias, M.; Söderlind, E.; Abrahamsson, B.; Dressman, J.B.; Reppas, C. Biorelevant Media to Simulate Fluids in the Ascending Colon of Humans and Their Usefulness in Predicting Intracolonic Drug Solubility. Pharm. Res. 2010, 27, 2187–2196. [Google Scholar] [CrossRef]
- Edwards, F.; Tsakmaka, C.; Mohr, S.; Fielden, P.R.; Goddard, N.J.; Booth, J.; Tam, K.Y. Using droplet-based microfluidic technology to study the precipitation of a poorly water-soluble weakly basic drug upon a pH-shift. Analyst 2013, 138, 339–345. [Google Scholar] [CrossRef]
- Sugihara, H.; Taylor, L.S. Evaluation of pazopanib phase behavior following pH-induced supersaturation. Mol. Pharm. 2018, 15, 1690–1699. [Google Scholar] [CrossRef]
- Chaudhuri, T.K.; Greenwald, A.J.; Heading, R.C. Measurement of gastric emptying time--a comparative study between nonisotopic aspiration method and new radioisotopic technique. Am. J. Dig. Dis. 1975, 20, 1063–1066. [Google Scholar] [CrossRef]
- Kostewicz, E.S.; Wunderlich, M.; Brauns, U.; Becker, R.; Bock, T.; Dressman, J.B. Predicting the precipitation of poorly soluble weak bases upon entry in the small intestine. J. Pharm. Pharmacol. 2004, 56, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Sekiguchi, K.; Obi, N. Studies on Absorption of Eutectic Mixture. I. A Comparison of the Behavior of Eutectic Mixture of Sulfathiazole and that of Ordinary Sulfathiazole in Man. Chem. Pharm. Bull. 1961, 9, 866–872. [Google Scholar] [CrossRef]
- Mistry, P.; Mohapatra, S.; Gopinath, T.; Vogt, F.G.; Suryanarayanan, R. Role of the Strength of Drug-Polymer Interactions on the Molecular Mobility and Crystallization Inhibition in Ketoconazole Solid Dispersions. Mol. Pharm. 2015, 12, 3339–3350. [Google Scholar] [CrossRef] [PubMed]
- Ashwathy, P.; Anto, A.T.; Sudheesh, M.S. A mechanistic review on the dissolution phase behavior and supersaturation stabilization of amorphous solid dispersions. Drug Dev. Ind. Pharm. 2021, 47, 1–11. [Google Scholar] [CrossRef]
- Zhao, P.; Han, W.; Shu, Y.; Li, M.; Sun, Y.; Sui, X.; Liu, B.; Tian, B.; Liu, Y.; Fu, Q. Liquid-liquid phase separation drug aggregate: Merit for oral delivery of amorphous solid dispersions. J. Control. Release Off. J. Control. Release Soc. 2023, 353, 42–50. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, K.; Kawakami, K.; Fukiage, M.; Oikawa, M.; Nishida, Y.; Matsuda, M.; Fujita, T. Relevance of Liquid-Liquid Phase Separation of Supersaturated Solution in Oral Absorption of Albendazole from Amorphous Solid Dispersions. Pharmaceutics 2021, 13, 220. [Google Scholar] [CrossRef]
- Kong, Y.; Wang, W.; Wang, C.; Li, L.; Peng, D.; Tian, B. Supersaturation and phase behavior during dissolution of amorphous solid dispersions. Int. J. Pharm. 2023, 631, 122524. [Google Scholar] [CrossRef]
- Miao, L.; Liang, Y.; Pan, W.; Gou, J.; Yin, T.; Zhang, Y.; He, H.; Tang, X. Effect of supersaturation on the oral bioavailability of paclitaxel/polymer amorphous solid dispersion. Drug Deliv. Transl. Re. 2019, 9, 344–356. [Google Scholar] [CrossRef]
- Baghel, S.; Cathcart, H.; O’Reilly, N.J. Polymeric Amorphous Solid Dispersions: A Review of Amorphization, Crystallization, Stabilization, Solid-State Characterization, and Aqueous Solubilization of Biopharmaceutical Classification System Class II Drugs. J. Pharm. Sci. 2016, 105, 2527–2544. [Google Scholar] [CrossRef]
- Li, Y.-W.; Zhang, H.-M.; Cui, B.-J.; Hao, C.-Y.; Zhu, H.-Y.; Guan, J.; Wang, D.; Jin, Y.; Feng, B.; Cai, J.-H.; et al. “Felodipine-indomethacin” co-amorphous supersaturating drug delivery systems: “Spring-parachute” process, stability, in vivo bioavailability, and underlying molecular mechanisms. Eur. J. Pharm. Biopharm. 2021, 166, 111–125. [Google Scholar] [CrossRef] [PubMed]
- Pinto, J.M.O.; Leão, A.F.; Bazzo, G.C.; Mendes, C.; Madureira, L.M.P.; Caramori, G.F.; Parreira, R.L.T.; Stulzer, H.K. Supersaturating drug delivery systems containing fixed-dose combination of two antihypertensive drugs: Formulation, in vitro evaluation and molecular metadynamics simulations. Eur. J. Pharm. Sci. 2021, 163, 105860. [Google Scholar] [CrossRef]
- Fael, H.; Demirel, A.L. Indomethacin co-amorphous drug-drug systems with improved solubility, supersaturation, dissolution rate and physical stability. Int. J. Pharm. 2021, 600, 120448. [Google Scholar] [CrossRef] [PubMed]
- Han, J.; Wei, Y.; Li, L.; Song, Y.; Pang, Z.; Qian, S.; Zhang, J.; Gao, Y.; Heng, W. Gelation Elimination and Crystallization Inhibition by Co-Amorphous Strategy for Amorphous Curcumin. J. Pharm. Sci. 2023, 112, 182–194. [Google Scholar] [CrossRef] [PubMed]
- Shi, Q.; Wang, Y.; Moinuddin, S.M.; Feng, X.; Ahsan, F. Co-amorphous Drug Delivery Systems: A Review of Physical Stability, In Vitro and In Vivo Performance. AAPS PharmSciTech 2022, 23, 259. [Google Scholar] [CrossRef]
- Stillhart, C.; Kuentz, M. Trends in the Assessment of Drug Supersaturation and Precipitation In Vitro Using Lipid-Based Delivery Systems. J. Pharm. Sci. 2016, 105, 2468–2476. [Google Scholar] [CrossRef] [PubMed]
- Koehl, N.J.; Henze, L.J.; Bennett-Lenane, H.; Faisal, W.; Price, D.J.; Holm, R.; Kuentz, M.; Griffin, B.T. In Silico, In Vitro, and In Vivo Evaluation of Precipitation Inhibitors in Supersaturated Lipid-Based Formulations of Venetoclax. Mol. Pharm. 2021, 18, 2174–2188. [Google Scholar] [CrossRef]
- Rani, S.; Rana, R.; Saraogi, G.K.; Kumar, V.; Gupta, U. Self-Emulsifying Oral Lipid Drug Delivery Systems: Advances and Challenges. AAPS PharmSciTech 2019, 20, 129. [Google Scholar] [CrossRef]
- Tung, N.T.; Tran, C.S.; Nguyen, H.A.; Nguyen, T.D.; Chi, S.C.; Pham, D.V.; Bui, Q.D.; Ho, X.H. Formulation and biopharmaceutical evaluation of supersaturatable self-nanoemulsifying drug delivery systems containing silymarin. Int. J. Pharm. 2019, 555, 63–76. [Google Scholar] [CrossRef]
- Bannow, J.; Yorulmaz, Y.; Löbmann, K.; Müllertz, A.; Rades, T. Improving the drug load and in vitro performance of supersaturated self-nanoemulsifying drug delivery systems (super-SNEDDS) using polymeric precipitation inhibitors. Int. J. Pharm. 2020, 575, 118960. [Google Scholar] [CrossRef]
- Anby, M.U.; Williams, H.D.; McIntosh, M.; Benameur, H.; Edwards, G.A.; Pouton, C.W.; Porter, C.J. Lipid digestion as a trigger for supersaturation: Evaluation of the impact of supersaturation stabilization on the in vitro and in vivo performance of self-emulsifying drug delivery systems. Mol. Pharm. 2012, 9, 2063–2079. [Google Scholar] [CrossRef] [PubMed]
- Park, H.; Ha, E.S.; Kim, M.S. Current Status of Supersaturable Self-Emulsifying Drug Delivery Systems. Pharmaceutics 2020, 12, 365. [Google Scholar] [CrossRef] [PubMed]
- Van Speybroeck, M.; Mellaerts, R.; Mols, R.; Thi, T.D.; Martens, J.A.; Van Humbeeck, J.; Annaert, P.; Van den Mooter, G.; Augustijns, P. Enhanced absorption of the poorly soluble drug fenofibrate by tuning its release rate from ordered mesoporous silica. Eur. J. Pharm. Sci. 2010, 41, 623–630. [Google Scholar] [CrossRef] [PubMed]
- Budiman, A.; Aulifa, D.L. Characterization of Drugs with Good Glass Formers in Loaded-Mesoporous Silica and Its Theoretical Value Relevance with Mesopores Surface and Pore-Filling Capacity. Pharmaceuticals 2022, 15, 93. [Google Scholar] [CrossRef]
- Dening, T.J.; Taylor, L.S. Supersaturation Potential of Ordered Mesoporous Silica Delivery Systems. Part 1: Dissolution Performance and Drug Membrane Transport Rates. Mol. Pharm. 2018, 15, 3489–3501. [Google Scholar] [CrossRef]
- Budiman, A.; Aulifa, D.L. A Comparative Study of the Pharmaceutical Properties between Amorphous Drugs Loaded-Mesoporous Silica and Pure Amorphous Drugs Prepared by Solvent Evaporation. Pharmaceuticals 2022, 15, 730. [Google Scholar] [CrossRef]
- Zhang, P.; Zardan Gomez de la Torre, T.; Welch, K.; Bergstrom, C.; Stromme, M. Supersaturation of poorly soluble drugs induced by mesoporous magnesium carbonate. Eur. J. Pharm. Sci. 2016, 93, 468–474. [Google Scholar] [CrossRef]
- Gómez de la Torre, J.; Bergström, C.; Zardán Gómez de la Torre, T. Increasing the Transport of Celecoxib over a Simulated Intestine Cell Membrane Model Using Mesoporous Magnesium Carbonate. Molecules 2021, 26, 6353. [Google Scholar] [CrossRef]
- Sun, R.; Zhang, P.; Bajnóczi, É.G.; Neagu, A.; Tai, C.-W.; Persson, I.; Strømme, M.; Cheung, O. Amorphous Calcium Carbonate Constructed from Nanoparticle Aggregates with Unprecedented Surface Area and Mesoporosity. ACS Appl. Mater. Inter. 2018, 10, 21556–21564. [Google Scholar] [CrossRef]
- Warren, D.B.; Benameur, H.; Porter, C.J.H.; Pouton, C.W. Using polymeric precipitation inhibitors to improve the absorption of poorly water-soluble drugs: A mechanistic basis for utility. J. Drug Target. 2010, 18, 704–731. [Google Scholar] [CrossRef]
- Price, D.J.; Ditzinger, F.; Koehl, N.J.; Jankovic, S.; Tsakiridou, G.; Nair, A.; Holm, R.; Kuentz, M.; Dressman, J.B.; Saal, C. Approaches to increase mechanistic understanding and aid in the selection of precipitation inhibitors for supersaturating formulations—A PEARRL review. J. Pharm. Pharmacol. 2019, 71, 483–509. [Google Scholar] [CrossRef] [PubMed]
- Terebetski, J.L.; Cummings, J.J.; Fauty, S.E.; Michniak-Kohn, B. Combined use of crystalline sodium salt and polymeric precipitation inhibitors to improve pharmacokinetic profile of ibuprofen through supersaturation. AAPS PharmSciTech 2014, 15, 1334–1344. [Google Scholar] [CrossRef] [PubMed]
- Ochi, M.; Kawachi, T.; Toita, E.; Hashimoto, I.; Yuminoki, K.; Onoue, S.; Hashimoto, N. Development of nanocrystal formulation of meloxicam with improved dissolution and pharmacokinetic behaviors. Int. J. Pharm. 2014, 474, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Geng, W.-C.; Sessler, J.L.; Guo, D.-S. Supramolecular prodrugs based on host–guest interactions. Chem. Soc. Rev. 2020, 49, 2303–2315. [Google Scholar] [CrossRef]
- Singh, R.; Thorat, V.; Kaur, H.; Sodhi, I.; Samal, S.K.; Jena, K.C.; Sangamwar, A.T. Elucidating the Molecular Mechanism of Drug-Polymer Interplay in a Polymeric Supersaturated System of Rifaximin. Mol. Pharm. 2021, 18, 1604–1621. [Google Scholar] [CrossRef]
- Xiao, L.; Yi, T. Mechanisms of hydroxypropyl methylcellulose for the precipitation inhibitor of supersaturatable self-emulsifying drug delivery systems. Yao Xue Xue Bao 2013, 48, 767–772. [Google Scholar]
- Oucherif, K.A.; Raina, S.; Taylor, L.S.; Litster, J.D. Quantitative analysis of the inhibitory effect of HPMC on felodipine crystallization kinetics using population balance modeling. CrystEngComm 2013, 15, 2197–2205. [Google Scholar] [CrossRef]
- Zhang, X.; Wang, A.; Yang, X.; Wang, Y.; Wang, Q.; Hu, R.; Anwaier, G.; Di, C.; Qi, R.; Huang, Y. HPMC improves protective effects of naringenin and isonicotinamide co-crystals against abdominal aortic aneurysm. Cardiovasc. Drugs Ther. 2022, 36, 1109–1119. [Google Scholar] [CrossRef]
- Aung, W.T.; Khine, H.E.E.; Chaotham, C.; Boonkanokwong, V. Production, physicochemical investigations, antioxidant effect, and cellular uptake in Caco-2 cells of the supersaturable astaxanthin self-microemulsifying tablets. Eur. J. Pharm. Sci. 2022, 176, 106263. [Google Scholar] [CrossRef]
- Curatolo, W.; Nightingale, J.A.; Herbig, S.M. Utility of hydroxypropylmethylcellulose acetate succinate (HPMCAS) for initiation and maintenance of drug supersaturation in the GI milieu. Pharm. Res. 2009, 26, 1419–1431. [Google Scholar] [CrossRef]
- Stillhart, C.; Durr, D.; Kuentz, M. Toward an improved understanding of the precipitation behavior of weakly basic drugs from oral lipid-based formulations. J. Pharm. Sci. 2014, 103, 1194–1203. [Google Scholar] [CrossRef] [PubMed]
- Ueda, K.; Higashi, K.; Yamamoto, K.; Moribe, K. The effect of HPMCAS functional groups on drug crystallization from the supersaturated state and dissolution improvement. Int. J. Pharm. 2014, 464, 205–213. [Google Scholar] [CrossRef] [PubMed]
- Fukiage, M.; Suzuki, K.; Matsuda, M.; Nishida, Y.; Oikawa, M.; Fujita, T.; Kawakami, K. Inhibition of Liquid-Liquid Phase Separation for Breaking the Solubility Barrier of Amorphous Solid Dispersions to Improve Oral Absorption of Naftopidil. Pharmaceutics 2022, 14, 2664. [Google Scholar] [CrossRef] [PubMed]
- Sethi, S.; Rana, V. In silico-assisted development of supersaturable preconcentrated isotropic mixture of atazanavir for augmenting biopharmaceutical performance in the presence of H2-receptor antagonist. Drug Deliv. Transl. Res. 2023, 13, 339–355. [Google Scholar] [CrossRef] [PubMed]
- Van Speybroeck, M.; Mols, R.; Mellaerts, R.; Thi, T.D.; Martens, J.A.; Van Humbeeck, J.; Annaert, P.; Van den Mooter, G.; Augustijns, P. Combined use of ordered mesoporous silica and precipitation inhibitors for improved oral absorption of the poorly soluble weak base itraconazole. Eur. J. Pharm. Biopharm. 2010, 75, 354–365. [Google Scholar] [CrossRef] [PubMed]
- Zhang, G.; Guan, H.; Li, J.; Li, M.; Sui, X.; Tian, B.; Dong, H.; Liu, B.; He, Z.; Li, N.; et al. Roles of effective stabilizers in improving oral bioavailability of naringenin nanocrystals: Maintenance of supersaturation generated upon dissolution by inhibition of drug dimerization. Asian J. Pharm. Sci. 2022, 17, 741–750. [Google Scholar] [CrossRef]
- Baghel, S.; Cathcart, H.; O’Reilly, N.J. Theoretical and experimental investigation of drug-polymer interaction and miscibility and its impact on drug supersaturation in aqueous medium. Eur. J. Pharm. Biopharm. 2016, 107, 16–31. [Google Scholar] [CrossRef]
- Madsen, C.M.; Boyd, B.; Rades, T.; Mullertz, A. Supersaturation of zafirlukast in fasted and fed state intestinal media with and without precipitation inhibitors. Eur. J. Pharm. Sci. 2016, 91, 31–39. [Google Scholar] [CrossRef]
- Ban, E.; An, S.H.; Park, B.; Park, M.; Yoon, N.E.; Jung, B.H.; Kim, A. Improved Solubility and Oral Absorption of Emodin-Nicotinamide Cocrystal Over Emodin with PVP as a Solubility Enhancer and Crystallization Inhibitor. J. Pharm. Sci. 2020, 109, 3660–3667. [Google Scholar] [CrossRef]
- Holm, T.P.; Knopp, M.M.; Berthelsen, R.; Löbmann, K. Supersaturated amorphous solid dispersions of celecoxib prepared in situ by microwave irradiation. Int. J. Pharm. 2022, 626, 122115. [Google Scholar] [CrossRef]
- Zhou, J.; Yu, G.; Huang, F. Supramolecular chemotherapy based on host–guest molecular recognition: A novel strategy in the battle against cancer with a bright future. Chem. Soc. Rev. 2017, 46, 7021–7053. [Google Scholar] [CrossRef]
- Chen, Y.; Huang, Z.; Zhao, H.; Xu, J.-F.; Sun, Z.; Zhang, X. Supramolecular Chemotherapy: Cooperative Enhancement of Antitumor Activity by Combining Controlled Release of Oxaliplatin and Consuming of Spermine by Cucurbit [7]uril. ACS Appl. Mater. Interfaces 2017, 9, 8602–8608. [Google Scholar] [CrossRef] [PubMed]
- Wada-Hirai, A.; Shimizu, S.; Ichii, R.; Tsunoda, C.; Hiroshige, R.; Fujita, M.; Li, Y.P.; Shimada, Y.; Otsuka, Y.; Goto, S. Stabilization of the Metastable α-Form of Indomethacin Induced by the Addition of 2-Hydroxypropyl-β-Cyclodextrin, Causing Supersaturation (Spring) and Its Sustaining Deployment (Parachute). J. Pharm Sci. 2021, 110, 3623–3630. [Google Scholar] [CrossRef] [PubMed]
- Brewster, M.E.; Vandecruys, R.; Peeters, J.; Neeskens, P.; Verreck, G.; Loftsson, T. Comparative interaction of 2-hydroxypropyl-beta-cyclodextrin and sulfobutylether-beta-cyclodextrin with itraconazole: Phase-solubility behavior and stabilization of supersaturated drug solutions. Eur. J. Pharm. Sci. Off. J. Eur. Fed. Pharm. Sci. 2008, 34, 94–103. [Google Scholar]
- Berben, P.; Mols, R.; Brouwers, J.; Tack, J.; Augustijns, P. Gastrointestinal behavior of itraconazole in humans—Part 2: The effect of intraluminal dilution on the performance of a cyclodextrin-based solution. Int. J. Pharm. 2017, 526, 235–243. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.R.; Ho, M.J.; Jung, H.J.; Cho, H.R.; Park, J.S.; Yoon, S.H.; Choi, Y.S.; Choi, Y.W.; Oh, C.H.; Kang, M.J. Enhanced dissolution and oral absorption of tacrolimus by supersaturable self-emulsifying drug delivery system. Int. J. Nanomed. 2016, 11, 1109–1117. [Google Scholar]
- Zhong, Y.; Jing, G.; Tian, B.; Huang, H.; Zhang, Y.; Gou, J.; Tang, X.; He, X.; Wang, Y. Supersaturation induced by Itraconazole/Soluplus® micelles provided high GI absorption in vivo. Asian J. Pharm. Sci. 2016, 11, 255–264. [Google Scholar] [CrossRef][Green Version]
- Dereymaker, A.; Cinghia, G.; Van den Mooter, G. Eudragit(R) RL as a stabilizer for supersaturation and a substrate for nanocrystal formation. Eur. J. Pharm. Biopharm. 2017, 114, 250–262. [Google Scholar] [CrossRef]
- Budiman, A.; Higashi, K.; Ueda, K.; Moribe, K. Effect of drug-coformer interactions on drug dissolution from a coamorphous in mesoporous silica. Int. J. Pharm. 2021, 600, 120492. [Google Scholar] [CrossRef]
- Ting, J.M.; Tale, S.; Purchel, A.A.; Jones, S.D.; Widanapathirana, L.; Tolstyka, Z.P.; Guo, L.; Guillaudeu, S.J.; Bates, F.S.; Reineke, T.M. High-Throughput Excipient Discovery Enables Oral Delivery of Poorly Soluble Pharmaceuticals. ACS Cent. Sci. 2016, 2, 748–755. [Google Scholar] [CrossRef]
- Vandecruys, R.; Peeters, J.; Verreck, G.; Brewster, M.E. Use of a screening method to determine excipients which optimize the extent and stability of supersaturated drug solutions and application of this system to solid formulation design. Int. J. Pharm. 2007, 342, 168–175. [Google Scholar] [CrossRef] [PubMed]
- Brewster, M.E.; Vandecruys, R.; Verreck, G.; Peeters, J. Supersaturating drug delivery systems: Effect of hydrophilic cyclodextrins and other excipients on the formation and stabilization of supersaturated drug solutions. Pharmazie Die 2008, 63, 217–220. [Google Scholar]
- Vora, C.; Patadia, R.; Mittal, K.; Mashru, R. Preparation and characterization of dipyridamole solid dispersions for stabilization of supersaturation: Effect of precipitation inhibitors type and molecular weight. Pharm. Dev. Technol. 2016, 21, 847–855. [Google Scholar] [CrossRef] [PubMed]
- Bevernage, J.; Hens, B.; Brouwers, J.; Tack, J.; Annaert, P.; Augustijns, P. Supersaturation in human gastric fluids. Eur. J. Pharm. Biopharm. 2012, 81, 184–189. [Google Scholar] [CrossRef]
- Yamashita, T.; Ozaki, S.; Kushida, I. Solvent shift method for anti-precipitant screening of poorly soluble drugs using biorelevant medium and dimethyl sulfoxide. Int. J. Pharm. 2011, 419, 170–174. [Google Scholar] [CrossRef]
- Price, D.J.; Nair, A.; Kuentz, M.; Dressman, J.; Saal, C. Calculation of drug-polymer mixing enthalpy as a new screening method of precipitation inhibitors for supersaturating pharmaceutical formulations. Eur. J. Pharm. Sci. 2019, 132, 142–156. [Google Scholar] [CrossRef]
- Raghavan, S.L.; Trividic, A.; Davis, A.F.; Hadgraft, J. Effect of cellulose polymers on supersaturation and in vitro membrane transport of hydrocortisone acetate. Int. J. Pharm. 2000, 193, 231–237. [Google Scholar] [CrossRef]
- Janssens, S.; De Zeure, A.; Paudel, A.; Van Humbeeck, J.; Rombaut, P.; Van den Mooter, G. Influence of preparation methods on solid state supersaturation of amorphous solid dispersions: A case study with itraconazole and eudragit e100. Pharm. Res. 2010, 27, 775–785. [Google Scholar] [CrossRef]
- Enright, E.F.; Joyce, S.A.; Gahan, C.G.M.; Taylor, L.S. Impact of phospholipid digests and bile acid pool variations on the crystallization of atazanavir from supersaturated solutions. Eur. J. Pharm. Biopharm. 2020, 153, 68–83. [Google Scholar] [CrossRef]
- Galia, E.; Nicolaides, E.; Hörter, D.; Löbenberg, R.; Reppas, C.; Dressman, J.B. Evaluation of various dissolution media for predicting in vivo performance of class I and II drugs. Pharm. Res. 1998, 15, 698–705. [Google Scholar] [CrossRef]
- Jantratid, E.; Janssen, N.; Reppas, C.; Dressman, J.B. Dissolution media simulating conditions in the proximal human gastrointestinal tract: An update. Pharm. Res. 2008, 25, 1663. [Google Scholar] [CrossRef] [PubMed]
- Fuchs, A.; Leigh, M.; Kloefer, B.; Dressman, J.B. Advances in the design of fasted state simulating intestinal fluids: FaSSIF-V3. Eur. J. Pharm. Biopharm. 2015, 94, 229–240. [Google Scholar] [CrossRef] [PubMed]
- Holmstock, N.; De, B.T.; Bevernage, J.; Annaert, P.; Mols, R.; Tack, J.; Augustijns, P. Exploring food effects on indinavir absorption with human intestinal fluids in the mouse intestine. Eur. J. Pharm. Sci. 2013, 49, 27. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; AbuBaker, O.; Shao, Z.J. Characterization of poly(ethylene oxide) as a drug carrier in hot-melt extrusion. Drug Dev. Ind. Pharm. 2006, 32, 991–1002. [Google Scholar] [CrossRef]
- Bevernage, J.; Brouwers, J.; Clarysse, S.; Vertzoni, M.; Tack, J.; Annaert, P.; Augustijns, P. Drug supersaturation in simulated and human intestinal fluids representing different nutritional states. J. Pharm. Sci. 2010, 99, 4525–4534. [Google Scholar] [CrossRef]
- Soderlind, E.; Karlsson, E.; Carlsson, A.; Kong, R.; Lenz, A.; Lindborg, S.; Sheng, J.J. Simulating fasted human intestinal fluids: Understanding the roles of lecithin and bile acids. Mol. Pharm. 2010, 7, 1498–1507. [Google Scholar] [CrossRef]
- Leigh, M.; Kloefer, B.; Schaich, M. Comparison of the solubility and dissolution of drugs in fasted-state biorelevant media (FaSSIF and FaSSIF-V2). Dissolution Technol. 2013, 20, 44–50. [Google Scholar] [CrossRef]
- Klumpp, L.; Leigh, M.; Dressman, J. Dissolution behavior of various drugs in different FaSSIF versions. Eur. J. Pharm. Sci. 2020, 142, 105138. [Google Scholar] [CrossRef]
- Pinnamaneni, S.; Rinaldi, F.A.; Jayawickrama, D.A.; Li, J.; Dali, M.V. Effect of pepsin on maintaining the supersaturation of the HCl salt of a weakly basic drug: A case study. Pharm. Dev. Technol. 2016, 21, 311–320. [Google Scholar] [CrossRef]
- Yeap, Y.Y.; Lock, J.; Lerkvikarn, S.; Semin, T.; Nguyen, N.; Carrier, R.L. Intestinal mucus is capable of stabilizing supersaturation of poorly water-soluble drugs. J. Control. Release 2019, 296, 107–113. [Google Scholar] [CrossRef]
- McConnell, E.L.; Fadda, H.M.; Basit, A.W. Gut instincts: Explorations in intestinal physiology and drug delivery. Int. J. Pharm. 2008, 364, 213–226. [Google Scholar] [CrossRef] [PubMed]
- Jede, C.; Wagner, C.; Kubas, H.; Weigandt, M.; Weber, C.; Lecomte, M.; Badolo, L.; Koziolek, M.; Weitschies, W. Improved Prediction of in Vivo Supersaturation and Precipitation of Poorly Soluble Weakly Basic Drugs Using a Biorelevant Bicarbonate Buffer in a Gastrointestinal Transfer Model. Mol. Pharm. 2019, 16, 3938–3947. [Google Scholar] [CrossRef] [PubMed]
- Boni, J.E.; Brickl, R.S.; Dressman, J. Is bicarbonate buffer suitable as a dissolution medium? J. Pharm. Pharmacol. 2007, 59, 1375–1382. [Google Scholar] [CrossRef] [PubMed]
- Amaral Silva, D.; Al-Gousous, J.; Davies, N.M.; Bou Chacra, N.; Webster, G.K.; Lipka, E.; Amidon, G.; Lobenberg, R. Simulated, biorelevant, clinically relevant or physiologically relevant dissolution media: The hidden role of bicarbonate buffer. Eur. J. Pharm. Biopharm. 2019, 142, 8–19. [Google Scholar] [CrossRef] [PubMed]
- Brouwers, J.; Tack, J.; Augustijns, P. In vitro behavior of a phosphate ester prodrug of amprenavir in human intestinal fluids and in the Caco-2 system: Illustration of intraluminal supersaturation. Int. J. Pharm. 2007, 336, 302–309. [Google Scholar] [CrossRef] [PubMed]
- Bevernage, J.; Forier, T.; Brouwers, J.; Tack, J.; Annaert, P.; Augustijns, P. Excipient-mediated supersaturation stabilization in human intestinal fluids. Mol. Pharm. 2011, 8, 564–570. [Google Scholar] [CrossRef]
- O’Dwyer, P.J.; Box, K.J.; Dressman, J.; Griffin, B.T.; Henze, L.J.; Litou, C.; Pentafragka, C.; Statelova, M.; Vertzoni, M.; Reppas, C. Oral biopharmaceutics tools: Recent progress from partnership through the Pharmaceutical Education and Research with Regulatory Links collaboration. J. Pharm. Pharmacol. 2021, 73, 437–446. [Google Scholar] [CrossRef]
- Motz, S.A.; Bur, M.; Schaefer, U.F.; Lehr, C.M. Drug Absorption Studies; Springer: Berlin/Heidelberg, Germany, 2008; pp. 430–455. [Google Scholar]
- Shi, Y.; Erickson, B.; Jayasankar, A.; Lu, L.; Marsh, K.; Menon, R.; Gao, P. Assessing Supersaturation and Its Impact on In Vivo Bioavailability of a Low-Solubility Compound ABT-072 With a Dual pH, Two-Phase Dissolution Method. J. Pharm. Sci. 2016, 105, 2886–2895. [Google Scholar] [CrossRef]
- López Mármol, Á.; Denninger, A.; Touzet, A.; Dauer, K.; Becker, T.; Pöstges, F.; Pellequer, Y.; Lamprecht, A.; Wagner, K.G. The relevance of supersaturation and solubilization in the gastrointestinal tract for oral bioavailability: An in vitro vs. in vivo approach. Int. J. Pharm. 2021, 603, 120648. [Google Scholar] [CrossRef]
- Masada, T.; Takagi, T.; Minami, K.; Kataoka, M.; Takeyama, S.; Fujii, Y.; Takahashi, M.; Yamashita, S. New biphasic system in side-by-side chambers for testing drug dissolution and permeation in vitro (BiDP system). J. Drug Deliv. Sci. Technol. 2021, 65, 102747. [Google Scholar] [CrossRef]
- Berben, P.; Brouwers, J.; Augustijns, P. The artificial membrane insert system as predictive tool for formulation performance evaluation. Int. J. Pharm. 2018, 537, 22–29. [Google Scholar] [CrossRef]
- Puppolo, M.M.; Hughey, J.R.; Dillon, T.; Storey, D.; Jansen-Varnum, S. Biomimetic Dissolution: A Tool to Predict Amorphous Solid Dispersion Performance. AAPS PharmSciTech 2017, 18, 2841–2853. [Google Scholar] [CrossRef] [PubMed]
- Ruponen, M.; Visti, M.; Ojarinta, R.; Laitinen, R. Permeability of glibenclamide through a PAMPA membrane: The effect of co-amorphization. Eur. J. Pharm. Biopharm. 2018, 129, 247–256. [Google Scholar] [CrossRef] [PubMed]
- Hate, S.S.; Mosquera-Giraldo, L.I.; Taylor, L.S. A mechanistic study of drug mass transport from supersaturated solutions across PAMPA membranes. J. Pharm. Sci. 2021, 111, 102–115. [Google Scholar] [CrossRef] [PubMed]
- Bibi, H.A.; Holm, R.; Bauer-Brandl, A. Use of Permeapad® for prediction of buccal absorption: A comparison to in vitro, ex vivo and in vivo method. Eur. J. Pharm. Sci. 2016, 93, 399–404. [Google Scholar] [CrossRef]
- Bevernage, J.; Brouwers, J.; Annaert, P.; Augustijns, P. Drug precipitation–permeation interplay: Supersaturation in an absorptive environment. Eur. J. Pharm. Biopharm. 2012, 82, 424–428. [Google Scholar] [CrossRef] [PubMed]
- Takagi, T.; Masada, T.; Minami, K.; Kataoka, M.; Izutsu, K.I.; Matsui, K.; Yamashita, S. In Vitro Sensitivity Analysis of the Gastrointestinal Dissolution Profile of Weakly Basic Drugs in the Stomach-to-Intestine Fluid Changing System: Explanation for Variable Plasma Exposure after Oral Administration. Mol. Pharm. 2021, 18, 1711–1719. [Google Scholar] [CrossRef]
- Takeuchi, S.; Tsume, Y.; Amidon, G.E.; Amidon, G.L. Evaluation of a three compartment in vitro gastrointestinal simulator dissolution apparatus to predict in vivo dissolution. J. Pharm. Sci. 2014, 103, 3416–3422. [Google Scholar] [CrossRef]
- Tsume, Y.; Matsui, K.; Searls, A.L.; Takeuchi, S.; Amidon, G.E.; Sun, D.; Amidon, G.L. The impact of supersaturation level for oral absorption of BCS class IIb drugs, dipyridamole and ketoconazole, using in vivo predictive dissolution system: Gastrointestinal Simulator (GIS). Eur. J. Pharm. Sci. 2017, 102, 126–139. [Google Scholar] [CrossRef]
- Matsui, K.; Tsume, Y.; Amidon, G.E.; Amidon, G.L. In vitro dissolution of fluconazole and dipyridamole in gastrointestinal simulator (GIS), predicting in vivo dissolution and drug–drug interaction caused by acid-reducing agents. Mol. Pharm. 2015, 12, 2418–2428. [Google Scholar] [CrossRef]
- Hens, B.; Bermejo, M.; Tsume, Y.; Gonzalez-Alvarez, I.; Ruan, H.; Matsui, K.; Amidon, G.E.; Cavanagh, K.L.; Kuminek, G.; Benninghoff, G. Evaluation and optimized selection of supersaturating drug delivery systems of posaconazole (BCS class 2b) in the gastrointestinal simulator (GIS): An in vitro-in silico-in vivo approach. Eur. J. Pharm. Sci. 2018, 115, 258–269. [Google Scholar] [CrossRef] [PubMed]
- Bermejo, M.; Kuminek, G.; Al-Gousous, J.; Ruiz-Picazo, A.; Tsume, Y.; Garcia-Arieta, A.; González-Alvarez, I.; Hens, B.; Amidon, G.; Rodriguez-Hornedo, N. Exploring Bioequivalence of Dexketoprofen Trometamol Drug Products with the Gastrointestinal Simulator (GIS) and Precipitation Pathways Analyses. Pharmaceutics 2019, 11, 18. [Google Scholar] [CrossRef] [PubMed]
- Gan, Y.; Zhang, X.; Xu, D.; Zhang, H.; Baak, J.P.; Luo, L.; Xia, Y.; Wang, J.; Ke, X.; Sun, P. Evaluating supersaturation in vitro and predicting its performance in vivo with Biphasic gastrointestinal Simulator: A case study of a BCS IIB drug. Int. J. Pharm. 2020, 578, 119043. [Google Scholar] [CrossRef] [PubMed]
- Minami, H.; Mccallum, R.W. The physiology and pathophysiology of gastric emptying in humans. Gastroenterology 1984, 86, 1592. [Google Scholar] [CrossRef] [PubMed]
- Talattof, A.; Amidon, G.L. Pulse Packet Stochastic Model for Gastric Emptying in the Fasted State: A Physiological Approach. Mol. Pharm. 2018, 15, 2107–2115. [Google Scholar] [CrossRef] [PubMed]
- Jaisamut, P.; Wiwattanawongsa, K.; Graidist, P.; Sangsen, Y.; Wiwattanapatapee, R. Enhanced Oral Bioavailability of Curcumin Using a Supersaturatable Self-Microemulsifying System Incorporating a Hydrophilic Polymer; In Vitro and In Vivo Investigations. AAPS PharmSciTech 2018, 19, 730–740. [Google Scholar] [CrossRef]
- O’Shea, J.P.; Nagarsekar, K.; Wieber, A.; Witt, V.; Herbert, E.; O’Driscoll, C.M.; Saal, C.; Lubda, D.; Griffin, B.T.; Dressman, J.B. Mesoporous silica-based dosage forms improve bioavailability of poorly soluble drugs in pigs: Case example fenofibrate. J. Pharm. Pharmacol. 2017, 69, 1284–1292. [Google Scholar] [CrossRef] [PubMed]
- Michaelsen, M.H.; Siqueira Jorgensen, S.D.; Abdi, I.M.; Wasan, K.M.; Rades, T.; Mullertz, A. Fenofibrate oral absorption from SNEDDS and super-SNEDDS is not significantly affected by lipase inhibition in rats. Eur. J. Pharm. Biopharm. 2019, 142, 258–264. [Google Scholar] [CrossRef]
- Ruff, A.; Holm, R.; Kostewicz, E.S. Evaluating the predictability of the in vitro transfer model and in vivo rat studies as a surrogate to investigate the supersaturation and precipitation behaviour of different Albendazole formulations for humans. Eur. J. Pharm. Sci. 2017, 105, 108–118. [Google Scholar] [CrossRef]
- Tanaka, Y.; Sugihara, M.; Kawakami, A.; Imai, S.; Itou, T.; Murase, H.; Saiki, K.; Kasaoka, S.; Yoshikawa, H. In vivo analysis of supersaturation/precipitation/absorption behavior after oral administration of pioglitazone hydrochloride salt; determinant site of oral absorption. Eur. J. Pharm. Sci. 2017, 106, 431–438. [Google Scholar] [CrossRef]
- Feng, D.; Peng, T.; Huang, Z.; Singh, V.; Shi, Y.; Wen, T.; Lu, M.; Quan, G.; Pan, X.; Wu, C. Polymer–Surfactant System Based Amorphous Solid Dispersion: Precipitation Inhibition and Bioavailability Enhancement of Itraconazole. Pharmaceutics 2018, 10, 53. [Google Scholar] [CrossRef] [PubMed]
- Suys, E.J.A.; Chalmers, D.K.; Pouton, C.W.; Porter, C.J.H. Polymeric Precipitation Inhibitors Promote Fenofibrate Supersaturation and Enhance Drug Absorption from a Type IV Lipid-Based Formulation. Mol. Pharm. 2018, 15, 2355–2371. [Google Scholar] [CrossRef] [PubMed]
- Hens, B.; Brouwers, J.; Corsetti, M.; Augustijns, P. Supersaturation and Precipitation of Posaconazole Upon Entry in the Upper Small Intestine in Humans. J. Pharm. Sci. 2016, 105, 2677–2684. [Google Scholar] [CrossRef] [PubMed]
- Rubbens, J.; Brouwers, J.; Tack, J.; Augustijns, P. Gastrointestinal dissolution, supersaturation and precipitation of the weak base indinavir in healthy volunteers. Eur. J. Pharm. Biopharm. 2016, 109, 122–129. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Spivey, N.; Silchenko, S.; Gonzalez-Alvarez, I.; Bermejo, M.; Hidalgo, I.J. A differential equation based modelling approach to predict supersaturation and in vivo absorption from in vitro dissolution-absorption system (idas2) data. Eur. J. Pharm. Biopharm. 2021, 165, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Edueng, K.; Mahlin, D.; Larsson, P.; Bergstrom, C.A.S. Mechanism-based selection of stabilization strategy for amorphous formulations: Insights into crystallization pathways. J. Control. Release 2017, 256, 193–202. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Mosquera-Giraldo, L.I.; Borca, C.H.; Ormes, J.D.; Lowinger, M.; Higgins, J.D.; Slipchenko, L.V.; Taylor, L.S. A Comparison of the Crystallization Inhibition Properties of Bile Salts. Cryst. Growth Des. 2016, 16, 7286–7300. [Google Scholar] [CrossRef]
- Maniruzzaman, M.; Pang, J.; Morgan, D.J.; Douroumis, D. Molecular modeling as a predictive tool for the development of solid dispersions. Mol. Pharm. 2015, 12, 1040–1049. [Google Scholar] [CrossRef]
- Maniruzzaman, M.; Snowden, M.J.; Bradely, M.S.; Douroumis, D. Studies of intermolecular interactions in solid dispersions using advanced surface chemical analysis. RSC Adv. 2015, 5, 74212–74219. [Google Scholar] [CrossRef]
- Zhang, Z.; Li, L.; Dong, L.; Tian, J.; Meng, T.; Zhao, Q.; Yang, J. Molecular Mechanisms Involved in Supersaturation of Emodin Ternary Solid Dispersions Based on Bonding Agents. J. Pharm Sci. 2022, 111, 2000–2010. [Google Scholar] [CrossRef]
- Lindfors, L.; Forssen, S.; Westergren, J.; Olsson, U. Nucleation and crystal growth in supersaturated solutions of a model drug. J. Colloid Interface Sci. 2008, 325, 404–413. [Google Scholar] [CrossRef] [PubMed]
- Hens, B.; Bolger, M.B. Application of a Dynamic Fluid and pH Model to Simulate Intraluminal and Systemic Concentrations of a Weak Base in GastroPlus™. J. Pharm. Sci. 2019, 108, 305–315. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, A.; Pepin, X.; Aarons, L.; Wang, Y.; Darwich, A.S.; Wood, J.M.; Tannergren, C.; Karlsson, E.; Patterson, C.; Thörn, H.; et al. IMI—Oral biopharmaceutics tools project—Evaluation of bottom-up PBPK prediction success part 4: Prediction accuracy and software comparisons with improved data and modelling strategies. Eur. J. Pharm. Biopharm. 2020, 156, 50–63. [Google Scholar] [CrossRef] [PubMed]
- Liu, B.; Crewe, H.K.; Ozdemir, M.; Rowland Yeo, K.; Tucker, G.; Rostami-Hodjegan, A. The absorption kinetics of ketoconazole plays a major role in explaining the reported variability in the level of interaction with midazolam: Interplay between formulation and inhibition of gut wall and liver metabolism. Biopharm. Drug Dispos. 2017, 38, 260–270. [Google Scholar] [CrossRef]
- Al-Tabakha, M.M.; Alomar, M.J. In Vitro Dissolution and in Silico Modeling Shortcuts in Bioequivalence Testing. Pharmaceutics 2020, 12, 45. [Google Scholar] [CrossRef]
- Sjogren, E.; Thorn, H.; Tannergren, C. In Silico Modeling of Gastrointestinal Drug Absorption: Predictive Performance of Three Physiologically Based Absorption Models. Mol. Pharm. 2016, 13, 1763–1778. [Google Scholar] [CrossRef]
- Turner, D.B.; Liu, B.; Patel, N.; Pathak, S.M.; Polak, S.; Jamei, M.; Dressman, J.; Rostami-Hodjegan, A. Comment on “In Silico Modeling of Gastrointestinal Drug Absorption: Predictive Performance of Three Physiologically-Based Absorption Models”. Mol. Pharm. 2017, 14, 336–339. [Google Scholar] [CrossRef]
- Sjogren, E.; Thorn, H.; Tannergren, C. Reply to “Comment on ‘In Silico Modeling of Gastrointestinal Drug Absorption: Predictive Performance of Three Physiologically Based Absorption Models’”. Mol. Pharm. 2017, 14, 340–343. [Google Scholar] [CrossRef]
- Petrakis, O.; Vertzoni, M.; Angelou, A.; Kesisoglou, F.; Bentz, K.; Goumas, K.; Reppas, C. Identification of key factors affecting the oral absorption of salts of lipophilic weak acids: A case example. J. Pharm. Pharmacol. 2015, 67, 56–67. [Google Scholar] [CrossRef]
- Kostewicz, E.S.; Aarons, L.; Bergstrand, M.; Bolger, M.B.; Galetin, A.; Hatley, O.; Jamei, M.; Lloyd, R.; Pepin, X.; Rostami-Hodjegan, A.; et al. PBPK models for the prediction of in vivo performance of oral dosage forms. Eur. J. Pharm. Sci. 2014, 57, 300–321. [Google Scholar] [CrossRef]
- Jiang, W.; Kim, S.; Zhang, X.; Lionberger, R.A.; Davit, B.M.; Conner, D.P.; Yu, L.X. The role of predictive biopharmaceutical modeling and simulation in drug development and regulatory evaluation. Int. J. Pharm. 2011, 418, 151–160. [Google Scholar] [CrossRef] [PubMed]
- Lionberger, R.A. FDA critical path initiatives: Opportunities for generic drug development. Aaps J. 2008, 10, 103–109. [Google Scholar] [CrossRef] [PubMed]
- Takano, R.; Takata, N.; Saito, R.; Furumoto, K.; Higo, S.; Hayashi, Y.; Machida, M.; Aso, Y.; Yamashita, S. Quantitative analysis of the effect of supersaturation on in vivo drug absorption. Mol. Pharm. 2010, 7, 1431–1440. [Google Scholar] [CrossRef] [PubMed]
- Dressman, J.B.; Reppas, C. In vitro-in vivo correlations for lipophilic, poorly water-soluble drugs. Eur. J. Pharm. Sci. 2000, 11, S73–S80. [Google Scholar] [CrossRef] [PubMed]
- Sigfridsson, K.; Andreasson, T.; Fihn, B.-M.; Kearns, M.; Lindblom, S. Supersaturated formulations of poorly soluble weak acid drugs evaluated in rodents; a case study. Int. J. Pharm. 2021, 606, 120883. [Google Scholar] [CrossRef]
- Cilurzo, F.; Casiraghi, A.; Selmin, F.; Minghetti, P. Supersaturation as a tool for skin penetration enhancement. Curr. Pharm. Des. 2015, 21, 2733–2744. [Google Scholar] [CrossRef]

| Fasted State | Fed State | |||
|---|---|---|---|---|
| Anatomic Site | pH | Transit Time (h) | pH | Transit Time (h) |
| Stomach | 1–3.5 | 0.25 | 4.3–5.4 | 1 |
| Duodenum | 5–7 | 0.26 | 5.4 | 0.26 |
| Jejunum | 6–7 | 1.7 | 5.4–6 | 1.7 |
| Ileum | 6.6–7.4 | 1.3 | 6.6–7.4 | 1.3 |
| Cecum | 6.4 | 4.5 | 6.4 | 4.5 |
| Colon | 7.8 [9] | 13.5 | 6.0 [9] | 13.5 |
| DSmax | AUC Ratio | Cmax Ratio | Tmax Ratio | Permeability Ratio | ||
|---|---|---|---|---|---|---|
| ASDs | 28.2 | 6.95 | 7.31 | 0.66 | 2.39 | |
| SEDDS | 17.4 | 3.22 | 3.68 | 0.57 | 3.06 | |
| Mesoporous-based systems | 47.4 | 4.52 | 4.63 | 0.80 | / | |
| FaSSIF | FeSSIF [81] | FaSSIF-V2 | FeSSIF-V2 [82] | FaSSIF-V3 [83] | FaHIF [84] | FeHIF | |
|---|---|---|---|---|---|---|---|
| Taurocholate | 3 | 15 | 3 | 10 | 1.4 | 0.768 | 0.789 |
| Taurodeoxycholate | 0.381 | 0.283 | |||||
| Taurochenodeoxycholate | 0.622 | 0.748 | |||||
| Glycocholate | 1.4 | 2.766 | 2.585 | ||||
| Glycodeoxycholate | 1.016 | 1.25 | |||||
| Glycochenodeoxycholate | 2.281 | 2.371 | |||||
| Lecithin | 0.75 | 3.75 | 0.2 | 2 | 0.035 | 2.06 | 5.81 |
| Lysolecithin | 0.315 | ||||||
| Cholesterol | 0.2 | ||||||
| Sodium oleate | 0.8 | 0.315 | |||||
| Glycerol monoleate | 5 | ||||||
| Buffer | Phosphate | Acetate | Maleate | Maleate | |||
| pH | 6.5 | 5.0 | 6.5 | 5.8 | 6.7 | 7.5 | 6.0 |
| Osmolarity (mOsm/kg) | 270 | 670 | 180 | 390 | 220 | 224 | 379 |
| Buffer Capacity (mM/dpH) | 12 | 76 | 10 | 25 | 5.6 | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gan, Y.; Baak, J.P.A.; Chen, T.; Ye, H.; Liao, W.; Lv, H.; Wen, C.; Zheng, S. Supersaturation and Precipitation Applicated in Drug Delivery Systems: Development Strategies and Evaluation Approaches. Molecules 2023, 28, 2212. https://doi.org/10.3390/molecules28052212
Gan Y, Baak JPA, Chen T, Ye H, Liao W, Lv H, Wen C, Zheng S. Supersaturation and Precipitation Applicated in Drug Delivery Systems: Development Strategies and Evaluation Approaches. Molecules. 2023; 28(5):2212. https://doi.org/10.3390/molecules28052212
Chicago/Turabian StyleGan, Yanxiong, Jan P. A. Baak, Taijun Chen, Hua Ye, Wan Liao, Huixia Lv, Chuanbiao Wen, and Shichao Zheng. 2023. "Supersaturation and Precipitation Applicated in Drug Delivery Systems: Development Strategies and Evaluation Approaches" Molecules 28, no. 5: 2212. https://doi.org/10.3390/molecules28052212
APA StyleGan, Y., Baak, J. P. A., Chen, T., Ye, H., Liao, W., Lv, H., Wen, C., & Zheng, S. (2023). Supersaturation and Precipitation Applicated in Drug Delivery Systems: Development Strategies and Evaluation Approaches. Molecules, 28(5), 2212. https://doi.org/10.3390/molecules28052212






