Screening of Active Ingredients from Wendan Decoction in Alleviating Palmitic Acid-Induced Endothelial Cell Injury
Abstract
1. Introduction
2. Result
2.1. Content Determination of Components in WDD
Method Validation
2.2. Cell Experiments
2.2.1. Screening of PA Concentration by MTT
2.2.2. Cell Protective Effect of WDD
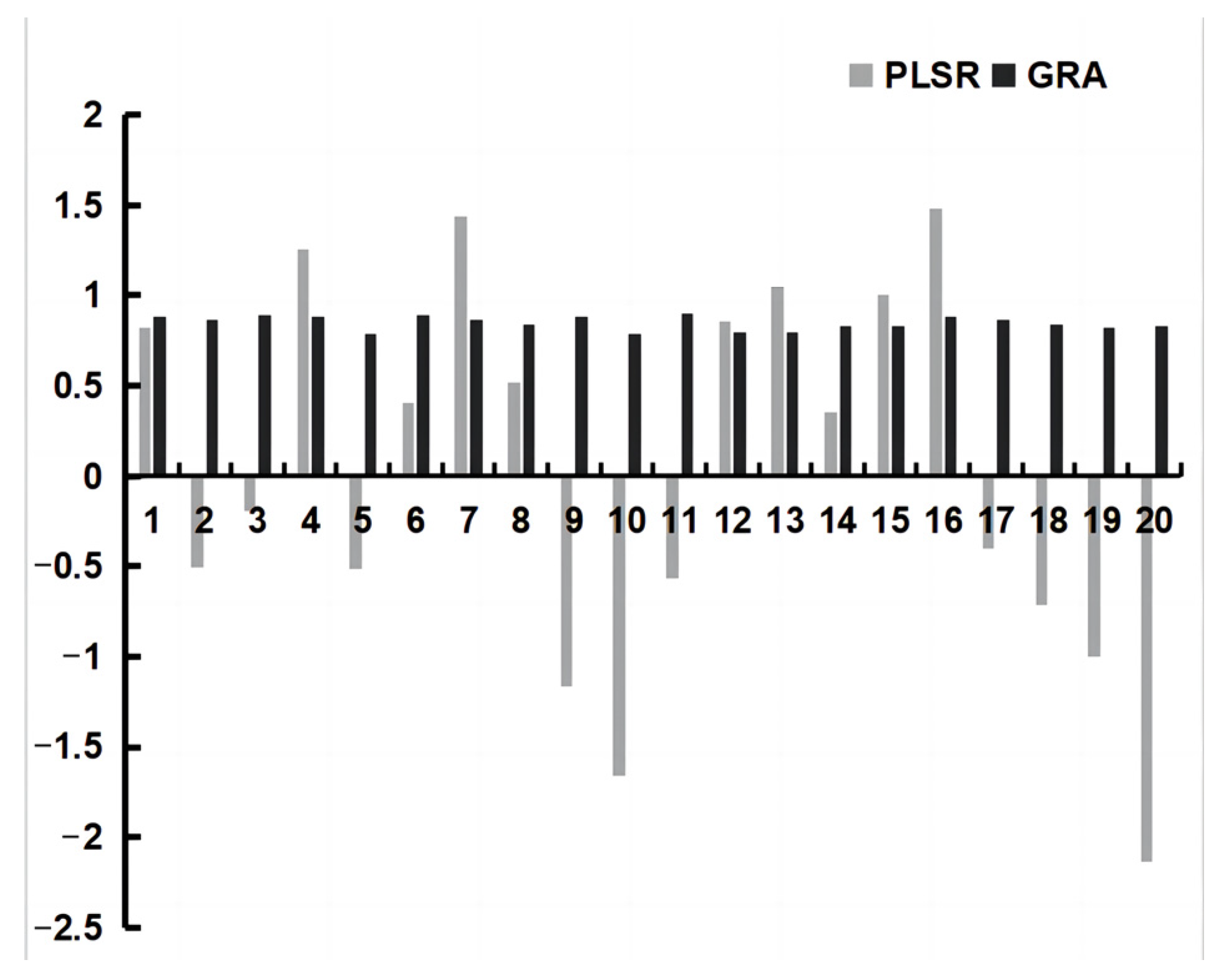
2.3. Statistical Analysis
3. Discussion
Limitations
4. Materials and Methods
4.1. Materials
4.2. Content Determination of Components in WDD
4.2.1. Preparation of Standard Solution
4.2.2. UPLC-QQQ-MS/MS Conditions
4.2.3. Methodology Validation
4.3. Cell Experiments
4.3.1. Screening of Palmitic Acid (PA) Concentration by MTT
4.3.2. Cell Protective Effect of WDD
4.4. Statistical Analysis
4.4.1. GRA
4.4.2. PLSR
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Kumar, S.; Mittal, A.; Babu, D.; Mittal, A. Herbal Medicines for Diabetes Management and its Secondary Complications. Curr. Diabetes Rev. 2021, 17, 437–456. [Google Scholar] [CrossRef] [PubMed]
- Boudina, S.; Sena, S.; Sloan, C.; Tebbi, A.; Han, Y.H.; O’Neill, B.T.; Cooksey, R.C.; Jones, D.; Holland, W.L.; McClain, D.A.; et al. Early mitochondrial adaptations in skeletal muscle to diet-induced obesity are strain dependent and determine oxidative stress and energy expenditure but not insulin sensitivity. Endocrinology 2012, 153, 2677–2688. [Google Scholar] [CrossRef] [PubMed]
- Poredos, P.; Jezovnik, M.K. Testing endothelial function and its clinical relevance. J. Atheroscler. Thromb. 2013, 20, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Villalta, S.A.; Lang, J.; Kubeck, S.; Kabre, B.; Szot, G.L.; Calderon, B.; Wasserfall, C.; Atkinson, M.A.; Brekken, R.A.; Pullen, N.; et al. Inhibition of VEGFR-2 reverses type 1 diabetes in NOD mice by abrogating insulitis and restoring islet function. Diabetes 2013, 62, 2870–2878. [Google Scholar] [CrossRef] [PubMed]
- Engin, A. Endothelial Dysfunction in Obesity. Adv. Exp. Med. Biol. 2017, 960, 345–379. [Google Scholar] [CrossRef] [PubMed]
- Taylor, F.C.; Dunstan, D.W.; Fletcher, E.; Townsend, M.K.; Larsen, R.N.; Rickards, K.; Maniar, N.; Buman, M.; Dempsey, P.C.; Joham, A.E.; et al. Interrupting Prolonged Sitting and Endothelial Function in Polycystic Ovary Syndrome. Med. Sci. Sport. Exerc. 2021, 53, 479–486. [Google Scholar] [CrossRef]
- Incalza, M.A.; D’Oria, R.; Natalicchio, A.; Perrini, S.; Laviola, L.; Giorgino, F. Oxidative stress and reactive oxygen species in endothelial dysfunction associated with cardiovascular and metabolic diseases. Vasc. Pharmacol. 2018, 100, 1–19. [Google Scholar] [CrossRef]
- Zhou, W.; Wang, J.; Wu, Z.; Huang, C.; Lu, A.; Wang, Y. Systems pharmacology exploration of botanic drug pairs reveals the mechanism for treating different diseases. Sci. Rep. 2016, 6, 36985. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhang, Y.; Liang, J.; Kuang, H.X.; Xia, Y.G. Exploring the effects of different processing techniques on the composition and biological activity of Platycodon grandiflorus (Jacq.) A.DC. by metabonomics and pharmacologic design. J. Ethnopharmacol. 2022, 289, 114991. [Google Scholar] [CrossRef]
- Yang, N.; Liu, F.L. Effect of Extracts from Broussonetia papyrifera (L.) Leaves on Blood Lipid and the Expression of Bax and Bcl-2 in Vascular Endothelial Cells in Rats with Hyperlipidemia. Guangming J. Chin. Med. 2019, 34, 1659–1661. [Google Scholar]
- Yu, Y.; Yan, R.; Chen, X.; Sun, T.; Yan, J. Paeonol suppresses the effect of ox-LDL on mice vascular endothelial cells by regulating miR-338-3p/TET2 axis in atherosclerosis. Mol. Cell. Biochem. 2020, 475, 127–135. [Google Scholar] [CrossRef] [PubMed]
- Su, J.; Zhou, H.; Tao, Y.; Guo, J.; Guo, Z.; Zhang, S.; Zhang, Y.; Huang, Y.; Tang, Y.; Dong, Q.; et al. G-CSF protects human brain vascular endothelial cells injury induced by high glucose, free fatty acids and hypoxia through MAPK and Akt signaling. PLoS ONE 2015, 10, e0120707. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.; Liu, H.; Xiang, H.; Zhou, J.; Zeng, Z.; Chen, R.; Zhao, S.; Xiao, J.; Shu, Z.; Chen, S.; et al. Palmitic acid-induced autophagy increases reactive oxygen species via the Ca2+/PKCα/NOX4 pathway and impairs endothelial function in human umbilical vein endothelial cells. Exp. Ther. Med. 2019, 17, 2425–2432. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.B.; Zhang, W.H.; Liu, H.D.; Liu, Z.; Ma, S.P. Protective effects of Huanglian Wendan Decoction aganist cognitive deficits and neuronal damages in rats with diabetic encephalopathy by inhibiting the release of inflammatory cytokines and repairing insulin signaling pathway in hippocampus. Chin. J. Nat. Med. 2016, 14, 813–822. [Google Scholar] [CrossRef]
- Huang, Y.M.; Xu, J.H.; Ling, W.; Li, Y.; Zhang, X.X.; Dai, Z.K.; Sui, Y.; Zhao, H.L. Efficacy of the wen dan decoction, a Chinese herbal formula, for metabolic syndrome. Altern. Ther. Health Med. 2015, 21, 54–67. [Google Scholar]
- Zhang, X.; Wang, Y.; Liu, L.; Jiang, H.; Wang, J.; Xiao, Y.; Wang, J. Efficacy of Wen-Dan Decoction in the treatment of patients with coronary heart disease: A protocol for systematic review and meta-analysis. Medicine 2022, 101, e28041. [Google Scholar] [CrossRef]
- Willson, C.; Watanabe, M.; Tsuji-Hosokawa, A.; Makino, A. Pulmonary vascular dysfunction in metabolic syndrome. J. Physiol. 2019, 597, 1121–1141. [Google Scholar] [CrossRef]
- Murni, I.K.; Sulistyoningrum, D.C.; Susilowati, R.; Julia, M. Risk of metabolic syndrome and early vascular markers for atherosclerosis in obese Indonesian adolescents. Paediatr. Int. Child Health 2020, 40, 117–123. [Google Scholar] [CrossRef]
- Hong, F.; Yan, Y.; Zhao, L.; Yu, B.Y.; Chai, C.Z. Analysis on ingredients and metabolites of Gegen Decoction absorbed into blood based on UHPLC-Q-TOF-MS. China J. Chin. Mater. Med. 2021, 46, 5944–5952. [Google Scholar] [CrossRef]
- Kumar, R.; Akhtar, F.; Rizvi, S.I. Protective effect of hesperidin in Poloxamer-407 induced hyperlipidemic experimental rats. Biol. Futur. 2021, 72, 201–210. [Google Scholar] [CrossRef]
- Wang, F.; Zhao, C.; Tian, G.; Wei, X.; Ma, Z.; Cui, J.; Wei, R.; Bao, Y.; Kong, W.; Zheng, J. Naringin Alleviates Atherosclerosis in ApoE−/− Mice by Regulating Cholesterol Metabolism Involved in Gut Microbiota Remodeling. J. Agric. Food Chem. 2020, 68, 12651–12660. [Google Scholar] [CrossRef] [PubMed]
- George, M.Y.; Menze, E.T.; Esmat, A.; Tadros, M.G.; El-Demerdash, E. Naringin treatment improved main clozapine-induced adverse effects in rats; emphasis on weight gain, metabolic abnormalities, and agranulocytosis. Drug Dev. Res. 2021, 82, 980–989. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zhao, H.; Li, X.; Wang, Q.; Yan, M.; Zhang, H.; Zhao, T.; Zhang, N.; Zhang, P.; Peng, L.; et al. Formononetin alleviates hepatic steatosis by facilitating TFEB-mediated lysosome biogenesis and lipophagy. J. Nutr. Biochem. 2019, 73, 108214. [Google Scholar] [CrossRef] [PubMed]
- Qiu, M.; Huang, K.; Liu, Y.; Yang, Y.; Tang, H.; Liu, X.; Wang, C.; Chen, H.; Xiong, Y.; Zhang, J.; et al. Modulation of intestinal microbiota by glycyrrhizic acid prevents high-fat diet-enhanced pre-metastatic niche formation and metastasis. Mucosal Immunol. 2019, 12, 945–957. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Yang, S.; Wang, K.; Lu, J.; Bao, X.; Wang, R.; Qiu, Y.; Wang, T.; Yu, H. Cellular senescence and cancer: Focusing on traditional Chinese medicine and natural products. Cell Prolif. 2020, 53, e12894. [Google Scholar] [CrossRef]
- Liu, Z.; Guo, F.; Wang, Y.; Li, C.; Zhang, X.; Li, H.; Diao, L.; Gu, J.; Wang, W.; Li, D.; et al. BATMAN-TCM: A Bioinformatics Analysis Tool for Molecular mechANism of Traditional Chinese Medicine. Sci. Rep. 2016, 6, 21146. [Google Scholar] [CrossRef]
- Wang, Z.Y.; Yang, S.Y.; Lyu, W.; Ding, J.B.; Ma, J.L.; Yang, J. Analysis of spectrum-activity relationship among antioxidant parts of Lycii Fructus using three different chemometrics methods. China J. Chin. Mater. Med. 2021, 46, 3377–3387. [Google Scholar] [CrossRef]
- Li, S.; Xu, T.; Liu, S.; Liu, Z.; Pi, Z.; Song, F.; Jin, Y. Exploring the potential pharmacodynamic material basis and pharmacologic mechanism of the Fufang-Xialian-Capsule in chronic atrophic gastritis by network pharmacology approach based on the components absorbed into the blood. R. Soc. Open Sci. 2018, 5, 171806. [Google Scholar] [CrossRef]
- Wang, Y.L.; Liu, Y.T.; Tao, Y.Y.; Liu, C.H.; Qu, H.Y.; Zhou, H.; Yang, T. Research ideas and method on screening active components of traditional Chinese medicine against hepatotoxicity with mitochondria as target. China J. Chin. Mater. Med. 2021, 46, 306–311. [Google Scholar] [CrossRef]
- Tian, X.; Wang, P.; Li, T.; Huang, X.; Guo, W.; Yang, Y.; Yan, M.; Zhang, H.; Cai, D.; Jia, X.; et al. Self-assembled natural phytochemicals for synergistically antibacterial application from the enlightenment of traditional Chinese medicine combination. Acta Pharm. Sin. B 2020, 10, 1784–1795. [Google Scholar] [CrossRef]
- Amtaghri, S.; Akdad, M.; Slaoui, M.; Eddouks, M. Traditional Uses, Pharmacological, and Phytochemical Studies of Euphorbia: A Review. Curr. Top. Med. Chem. 2022, 22, 1553–1570. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.X.; Du, G.H.; Qin, X.M.; Gao, L. 1H-NMR-based metabolomics reveals the biomarker panel and molecular mechanism of hepatocellular carcinoma progression. Anal. Bioanal. Chem. 2022, 414, 1525–1537. [Google Scholar] [CrossRef] [PubMed]
- Wei, J.; Lu, Y.; Wang, R.; Xu, X.; Liu, Q.; He, S.; Pan, H.; Liu, X.; Yuan, B.; Ding, Y.; et al. MicroRNA-375: Potential cancer suppressor and therapeutic drug. Biosci. Rep. 2021, 41, BSR20211494. [Google Scholar] [CrossRef]
- Chen, J.; Zhang, X.; Wang, Y.; Ye, Y.; Huang, Z. Differential ability of formononetin to stimulate proliferation of endothelial cells and breast cancer cells via a feedback loop involving MicroRNA-375, RASD1, and ERα. Mol. Carcinog. 2018, 57, 817–830. [Google Scholar] [CrossRef]
- Kim, G.D. Hesperetin Inhibits Vascular Formation by Suppressing of the PI3K/AKT, ERK, and p38 MAPK Signaling Pathways. Prev. Nutr. Food Sci. 2014, 19, 299–306. [Google Scholar] [CrossRef]
- Wang, C.; Chen, Y.; Wang, Y.; Liu, X.; Liu, Y.; Li, Y.; Chen, H.; Fan, C.; Wu, D.; Yang, J. Inhibition of COX-2, mPGES-1 and CYP4A by isoliquiritigenin blocks the angiogenic Akt signaling in glioma through ceRNA effect of miR-194-5p and lncRNA NEAT1. J. Exp. Clin. Cancer Res. CR 2019, 38, 371. [Google Scholar] [CrossRef] [PubMed]
- Park, S.M.; Ki, S.H.; Han, N.R.; Cho, I.J.; Ku, S.K.; Kim, S.C.; Zhao, R.J.; Kim, Y.W. Tacrine, an oral acetylcholinesterase inhibitor, induced hepatic oxidative damage, which was blocked by liquiritigenin through GSK3-beta inhibition. Biol. Pharm. Bull. 2015, 38, 184–192. [Google Scholar] [CrossRef]
- Zeng, J.; Chen, Y.; Ding, R.; Feng, L.; Fu, Z.; Yang, S.; Deng, X.; Xie, Z.; Zheng, S. Isoliquiritigenin alleviates early brain injury after experimental intracerebral hemorrhage via suppressing ROS- and/or NF-κB-mediated NLRP3 inflammasome activation by promoting Nrf2 antioxidant pathway. J. Neuroinflammation 2017, 14, 119. [Google Scholar] [CrossRef]
- Shi, C.; Wu, H.; Xu, K.; Cai, T.; Qin, K.; Wu, L.; Cai, B. Liquiritigenin-Loaded Submicron Emulsion Protects Against Doxorubicin-Induced Cardiotoxicity via Antioxidant, Anti-Inflammatory, and Anti-Apoptotic Activity. Int. J. Nanomed. 2020, 15, 1101–1115. [Google Scholar] [CrossRef]
- Wang, X.; Xue, X.; Wang, H.; Xu, F.; Xin, Z.; Wang, K.; Cui, M.; Qin, W. Quercetin inhibits human microvascular endothelial cells viability, migration and tube-formation in vitro through restraining microRNA-216a. J. Drug Target. 2020, 28, 609–616. [Google Scholar] [CrossRef]
- Xiong, Y.; Hu, Y.; Li, F.; Chen, L.; Dong, Q.; Wang, J.; Gullen, E.A.; Cheng, Y.C.; Xiao, X. Promotion of quality standard of Chinese herbal medicine by the integrated and efficacy-oriented quality marker of Effect-constituent Index. Phytomed. Int. J. Phytother. Phytopharm. 2018, 45, 26–35. [Google Scholar] [CrossRef] [PubMed]
- Chen, R.S.; Li, Y.; Lu, Y.; Li, L.J. A textual research on the key information of the famous classical formula Wendan Decoction based on ancient bibliometric analysis. J. Nanjing Univ. TCM 2021, 37, 439–445. [Google Scholar]
- Zhou, L.; Shi, H.Y.; Shi, Y.P.; Wang, P.; Xu, N. Optimization of extraction technology of Classical Mingfang Wendan decoction by fingerprint combined with chemometrics. Chin. J. Hosp. Pharm. 2020, 40, 2214–2219. [Google Scholar]
- Rehman, E.; Ikram, M.; Feng, M.T.; Rehman, S. Sectoral-based CO2 emissions of Pakistan: A novel Grey Relation Analysis (GRA) approach. Environ. Sci. Pollut. Res. Int. 2020, 27, 29118–29129. [Google Scholar] [CrossRef] [PubMed]
- Foodeh, R.; Ebadollahi, S.; Daliri, M.R. Regularized Partial Least Square Regression for Continuous Decoding in Brain-Computer Interfaces. Neuroinformatics 2020, 18, 465–477. [Google Scholar] [CrossRef] [PubMed]



| NO. | Compound | Formula | Mass | tr (min) | Polarity | Precursor Ion (m/z) | Product Ion (m/z) | Collision Energy (V) | Radio Frequency Lens (V) |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Trigonelline | C7H7NO2 | 137.14 | 0.84 | + | 138.01 | 92.13 | 19.91 | 97 |
| 2 | Synephrine | C9H13NO2 | 167.21 | 0.97 | + | 168.03 | 150.13 | 8.16 | 49 |
| 3 | Isoquercitrin | C21H20O12 | 464.38 | 3.69 | + | 465.17 | 229.05 | 44.22 | 106 |
| 4 | Liquiritin | C21H22O9 | 418.39 | 3.69 | - | 417.13 | 135.04 | 31.41 | 147 |
| 5 | Naringin | C27H32O14 | 580.53 | 3.71 | - | 579.2 | 459.16 | 22.99 | 234 |
| 6 | Hesperidin | C28H34O15 | 610.56 | 3.73 | - | 609.21 | 286.08 | 41.73 | 170 |
| 7 | Hesperetin | C16H14O6 | 302.28 | 3.74 | + | 303.11 | 177.13 | 16.84 | 133 |
| 8 | Scopoletin | C10H8O4 | 192.17 | 3.89 | - | 190.97 | 103.99 | 25.05 | 83 |
| 9 | Daidzein | C15H10O4 | 254.24 | 4.08 | - | 253.04 | 223.07 | 33.81 | 151 |
| 10 | Naringenin | C15H12O5 | 272.25 | 4.51 | - | 271.03 | 119.05 | 26.52 | 124 |
| 11 | Glycyrrhizic acid | C42H62O16 | 822.93 | 4.55 | + | 823.52 | 453.39 | 19.87 | 171 |
| 12 | Morin | C15H10O7 | 302.24 | 4.59 | - | 301.04 | 125.04 | 20.25 | 137 |
| 13 | Quercetin | C15H10O7 | 302.24 | 4.61 | - | 301.06 | 151.04 | 21.09 | 149 |
| 14 | Isoliquiritigenin | C15H12O4 | 256.25 | 4.78 | - | 254.97 | 134.97 | 15.7 | 104 |
| 15 | Liquiritigenin | C15H12O4 | 256.25 | 4.79 | - | 254.98 | 135.04 | 15.24 | 118 |
| 16 | Formononetin | C16H12O4 | 268.26 | 4.96 | - | 267.03 | 223.04 | 32.21 | 127 |
| 17 | Nobiletin | C21H22O8 | 402.4 | 5.43 | + | 403.17 | 327.13 | 32.17 | 182 |
| 18 | Tangeretin | C20H20O7 | 372.37 | 6.03 | + | 373.17 | 358.13 | 19.07 | 167 |
| 19 | Obacunone | C26H30O7 | 454.51 | 6.05 | + | 455.22 | 161.07 | 23.28 | 137 |
| 20 | Glycyrrhetinic acid | C30H46O4 | 470.68 | 8.29 | - | 469.36 | 355.33 | 46.45 | 261 |
| 21 | Furosemide | C12H11ClN2O5S | 330.74 | 4.49 | - | 328.95 | 204.99 | 21.51 | 113 |
| NO. | Compound | S1 | S2 | S3 | S4 | S5 | S6 | S7 | S8 | S9 | S10 | S11 | S12 | S13 | S14 | S15 | S16 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Trigonelline | 1081.13 ± 115.55 | 1214.56 ± 98.98 | 968.28 ± 78.62 | 986.33 ± 54.57 | 2132.75 ± 248.64 | 1667.38 ± 253.09 | 2644.48 ± 250.17 | 1542.58 ± 182.98 | 2016.93 ± 213.55 | 2241.31 ± 238.07 | 1969.98 ± 67.36 | 798.42 ± 34.41 | 567.43 ± 71.72 | 1778.26 ± 45.44 | 2003.50 ± 273.90 | 1674.62 ± 261.21 |
| 2 | Synephrine | 13147.38 ± 1846.14 | 17359.46 ± 1855.39 | 18033.69 ± 165.49 | 12952.94 ± 1978.05 | 38277.40 ± 4178.07 | 36066.95 ± 4630.68 | 68086.80 ± 9517.01 | 18511.95 ± 2834.50 | 25981.23 ± 3620.37 | 58408.02 ± 3153.10 | 36739.46 ± 2112.75 | 27157.50 ± 965.88 | 6773.77 ± 960.51 | 37962.47 ± 1573.09 | 28646.49 ± 2927.31 | 38754.01 ± 4227.24 |
| 3 | Isoquercitrin | 123.85 ± 6.77 | 107.03 ± 2.40 | 123.63 ± 4.37 | 33.89 ± 3.42 | 80.13 ± 8.19 | 58.89 ± 6.21 | 95.03 ± 11.35 | 94.24 ± 2.64 | 100.42 ± 13.38 | 78.47 ± 13.19 | 96.81 ± 8.38 | 78.29 ± 6.24 | 91.47 ± 12.04 | 84.97 ± 4.08 | 60.87 ± 5.10 | 94.16 ± 10.12 |
| 4 | Liquiritin | 489.62 ± 58.75 | 1729.21 ± 240.56 | 601.38 ± 15.65 | 440.53 ± 33.29 | 995.53 ± 51.83 | 624.55 ± 59.79 | 1754.29 ± 222.48 | 764.55 ± 94.22 | 1717.53 ± 206.92 | 639.79 ± 57.67 | 621.43 ± 82.80 | 657.53 ± 43.81 | 774.28 ± 56.84 | 1159.37 ± 20.32 | 663.45 ± 53.62 | 1135.81 ± 163.75 |
| 5 | Naringin | 4293.99 ± 694.84 | 544.19 ± 57.61 | 2330.00 ± 62.10 | 43.33 ± 5.88 | 183.49 ± 21.41 | 493.23 ± 77.71 | 133.77 ± 22.64 | 1972.70 ± 308.36 | 1907.97 ± 298.14 | 155.73 ± 15.23 | 4980.87 ± 716.43 | 856.40 ± 27.96 | 1003.64 ± 121.72 | 2221.39 ± 43.38 | 966.65 ± 106.91 | 251.75 ± 39.35 |
| 6 | Hesperidin | 3874.78 ± 652.37 | 4160.72 ± 528.16 | 3091.37 ± 148.23 | 1195.08 ± 80.82 | 3060.41 ± 269.90 | 2626.72 ± 259.04 | 3575.26 ± 467.00 | 3227.13 ± 494.79 | 3102.85 ± 409.92 | 2480.56 ± 231.93 | 4758.26 ± 689.58 | 3177.08 ± 196.28 | 3868.27 ± 317.84 | 2890.70 ± 92.02 | 3181.91 ± 368.53 | 3125.96 ± 179.77 |
| 7 | Hesperetin | 5837.87 ± 264.68 | 3048.85 ± 303.57 | 2239.34 ± 96.43 | 814.26 ± 68.23 | 1993.62 ± 77.28 | 1807.70 ± 127.78 | 2145.84 ± 144.19 | 2330.46 ± 243.40 | 2295.72 ± 329.59 | 1834.12 ± 181.45 | 7156.59 ± 316.95 | 2489.32 ± 129.60 | 2786.83 ± 294.40 | 2006.73 ± 48.25 | 3308.82 ± 266.13 | 1839.25 ± 192.44 |
| 8 | Scopoletin | 150.36 ± 3.34 | 76.50 ± 12.71 | 69.38 ± 4.00 | 34.08 ± 5.08 | 64.44 ± 7.10 | 60.95 ± 1.04 | 44.94 ± 5.80 | 56.11 ± 6.83 | 86.36 ± 4.00 | 34.28 ± 4.00 | 237.55 ± 13.04 | 57.43 ± 2.46 | 64.86 ± 10.42 | 69.80 ± 4.72 | 69.86 ± 11.88 | 45.06 ± 3.03 |
| 9 | Daidzein | 14.06 ± 0.94 | 17.63 ± 1.57 | 9.12 ± 0.78 | 1.95 ± 0.28 | 9.00 ± 0.75 | 6.81 ± 0.91 | 6.31 ± 0.81 | 13.53 ± 1.14 | 12.57 ± 0.84 | 10.28 ± 1.19 | 6.89 ± 0.71 | 8.58 ± 1.20 | 9.99 ± 1.24 | 6.57 ± 0.83 | 9.20 ± 1.35 | 5.17 ± 0.10 |
| 10 | Naringenin | 2600.18 ± 217.74 | 379.36 ± 18.67 | 784.54 ± 27.63 | 35.69 ± 0.54 | 113.35 ± 12.30 | 206.63 ± 18.81 | 71.18 ± 4.94 | 425.68 ± 35.30 | 525.10 ± 70.04 | 227.03 ± 19.17 | 3259.16 ± 241.86 | 206.70 ± 8.61 | 246.75 ± 10.36 | 397.22 ± 10.40 | 153.62 ± 22.52 | 179.03 ± 12.65 |
| 11 | Glycyrrhizic acid | 3070.18 ± 175.29 | 4269.03 ± 199.04 | 3065.04 ± 77.75 | 1164.14 ± 183.71 | 3355.01 ± 426.61 | 2576.06 ± 255.23 | 4157.77 ± 211.33 | 3826.32 ± 335.32 | 3899.42 ± 542.40 | 3107.87 ± 378.10 | 2768.07 ± 250.76 | 2558.80 ± 180.03 | 2942.77 ± 268.86 | 3080.26 ± 131.21 | 3006.57 ± 333.22 | 3113.40 ± 136.04 |
| 12 | Morin | 3813.18 ± 383.83 | 708.37 ± 28.98 | 844.89 ± 111.80 | 105.58 ± 13.89 | 110.88 ± 16.48 | 563.48 ± 63.58 | 170.98 ± 23.36 | 539.10 ± 49.68 | 550.87 ± 49.07 | 311.26 ± 26.17 | 4019.50 ± 136.56 | 374.92 ± 20.03 | 449.90 ± 49.18 | 727.34 ± 59.61 | 379.26 ± 31.03 | 201.83 ± 22.11 |
| 13 | Quercetin | 2902.92 ± 420.22 | 464.34 ± 27.99 | 576.66 ± 67.05 | 81.35 ± 11.27 | 129.22 ± 16.14 | 455.71 ± 31.50 | 145.68 ± 12.20 | 378.52 ± 26.58 | 395.13 ± 41.98 | 252.14 ± 31.94 | 3107.47 ± 277.25 | 301.80 ± 24.18 | 344.56 ± 42.39 | 599.26 ± 51.07 | 304.66 ± 20.80 | 231.75 ± 22.44 |
| 14 | Isoliquiritigenin | 123.33 ± 1.54 | 107.88 ± 0.74 | 80.49 ± 2.98 | 17.05 ± 1.62 | 22.02 ± 1.40 | 42.85 ± 3.26 | 34.17 ± 5.03 | 142.57 ± 16.27 | 129.15 ± 11.10 | 65.46 ± 4.92 | 199.95 ± 8.58 | 16.57 ± 0.55 | 19.10 ± 0.64 | 61.64 ± 1.80 | 26.24 ± 1.75 | 17.41 ± 0.71 |
| 15 | Liquiritigenin | 392.14 ± 7.16 | 356.60 ± 0.22 | 263.01 ± 5.46 | 54.58 ± 5.33 | 67.60 ± 3.23 | 133.48 ± 17.50 | 113.34 ± 10.75 | 466.33 ± 60.63 | 408.01 ± 56.91 | 213.66 ± 28.54 | 649.33 ± 28.39 | 51.91 ± 2.90 | 58.18 ± 4.37 | 201.42 ± 3.37 | 85.16 ± 9.88 | 57.06 ± 6.40 |
| 16 | Formononetin | 146.95 ± 8.45 | 139.01 ± 3.45 | 107.96 ± 3.51 | 17.32 ± 2.04 | 110.97 ± 8.81 | 66.66 ± 9.18 | 55.63 ± 5.85 | 150.10 ± 11.65 | 92.85 ± 9.92 | 92.21 ± 7.64 | 115.78 ± 2.23 | 73.09 ± 3.82 | 81.79 ± 9.80 | 89.48 ± 4.13 | 74.02 ± 6.13 | 65.94 ± 5.70 |
| 17 | Nobiletin | 4129.53 ± 49.24 | 1783.50 ± 20.77 | 2515.31 ± 77.18 | 1850.06 ± 156.62 | 1954.99 ± 191.13 | 3735.75 ± 474.17 | 4389.54 ± 507.72 | 2561.99 ± 276.92 | 5054.44 ± 659.23 | 2330.66 ± 252.21 | 2747.98 ± 84.84 | 3001.93 ± 283.54 | 3325.35 ± 186.39 | 5093.37 ± 125.05 | 3912.02 ± 401.66 | 2206.13 ± 167.75 |
| 18 | Tangeretin | 2239.72 ± 63.67 | 692.66 ± 23.77 | 781.88 ± 35.83 | 764.14 ± 108.30 | 775.59 ± 80.63 | 1638.23 ± 199.89 | 1865.95 ± 205.54 | 750.53 ± 69.41 | 2278.55 ± 273.85 | 674.31 ± 71.45 | 1527.77 ± 102.02 | 1410.63 ± 114.69 | 1628.44 ± 71.47 | 2597.79 ± 53.12 | 1789.81 ± 206.46 | 684.47 ± 51.29 |
| 19 | Obacunone | 1826.45 ± 219.79 | 1392.87 ± 138.75 | 346.31 ± 12.17 | 178.50 ± 2.65 | 1142.22 ± 153.81 | 540.02 ± 80.23 | 725.34 ± 55.98 | 428.33 ± 51.34 | 303.89 ± 51.81 | 329.90 ± 10.00 | 1818.21 ± 207.43 | 481.09 ± 58.54 | 580.77 ± 17.44 | 224.79 ± 29.90 | 441.34 ± 26.66 | 298.26 ± 20.22 |
| 20 | Glycyrrhetinic acid | 40.62 ± 4.81 | 32.24 ± 1.36 | 19.98 ± 2.46 | 2.86 ± 0.20 | 14.83 ± 2.20 | 7.85 ± 0.78 | 11.66 ± 1.95 | 34.82 ± 4.88 | 31.69 ± 2.53 | 13.99 ± 0.90 | 80.30 ± 11.80 | 3.27 ± 0.21 | 4.79 ± 0.42 | 13.26 ± 0.93 | 3.68 ± 0.27 | 6.10 ± 0.46 |
| NO. | Compound | Regression Equation | r2 | LLOQ ng/mL | Linear Range ng/mL | Precision RSD, n = 6 | Stability RSD, 24 h, n = 6 | Repeatability RSD, n = 6 | Recovery % mean ± SD |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Trigonelline | Y = 0.00299197X + 0.0378053 | 0.9904 | 120 | 120–60,000 | 13.98 | 7.44 | 8.54 | 94.48 ± 7.50 |
| 2 | Synephrine | Y = 0.0900787X + 0.463625 | 0.9911 | 8 | 8–4000 | 13.79 | 6.91 | 11.87 | 104.74 ± 8.29 |
| 3 | Isoquercitrin | Y = 0.00046952X−0.00753226 | 0.9907 | 140 | 140–70,000 | 14.75 | 13.05 | 10.49 | 94.13 ± 6.43 |
| 4 | Liquiritin | Y = 0.00497658X − 0.00447113 | 0.9968 | 6 | 6–3000 | 8.83 | 3.63 | 11.53 | 93.91 ± 5.71 |
| 5 | Naringin | Y = 0.00275605X − 0.0152202 | 0.9913 | 12 | 12–6000 | 11.31 | 6.63 | 12.38 | 102.78 ± 7.37 |
| 6 | Hesperidin | Y = 0.00185764X−0.0162377 | 0.9926 | 24 | 24–12,000 | 10.96 | 5.71 | 13.37 | 100.97 ± 6.38 |
| 7 | Hesperetin | Y = 0.00747729X + 0.0165338 | 0.9924 | 60 | 60–30,000 | 11.36 | 5.54 | 5.87 | 96.00 ± 5.06 |
| 8 | Scopoletin | Y = 0.00145419X−0.0126843 | 0.9917 | 16 | 16–8000 | 12.2 | 7.17 | 7.38 | 101.27 ± 8.60 |
| 9 | Daidzein | Y = 0.00364942X + 0.0178624 | 0.9948 | 4 | 4–2000 | 9.82 | 13.04 | 12.79 | 111.84 ± 10.65 |
| 10 | Naringenin | Y = 0.0144335X − 0.0633108 | 0.993 | 14 | 14–7000 | 6.82 | 7.71 | 6.62 | 93.33 ± 5.30 |
| 11 | Glycyrrhizic acid | Y = 0.0419993X − 0.197051 | 0.9905 | 10 | 10–5000 | 7.60 | 6.45 | 6.21 | 96.27 ± 9.18 |
| 12 | Morin | Y = 0.0005182X + 0.130608 | 0.9932 | 20 | 20–10,000 | 10.6 | 13.25 | 11.03 | 97.35 ± 7.92 |
| 13 | Quercetin | Y = 0.00131174X−0.00216878 | 0.9921 | 26 | 26–13,000 | 11.65 | 7.66 | 8.00 | 98.59 ± 10.04 |
| 14 | Isoliquiritigenin | Y = 0.0370696X − 0.106264 | 0.9910 | 6 | 6–3000 | 8.00 | 7.50 | 4.77 | 111.43 ± 1.22 |
| 15 | Liquiritigenin | Y = 0.0114821X + 0.0776073 | 0.9992 | 4 | 4–2000 | 10.33 | 6.54 | 8.89 | 89.62 ± 3.19 |
| 16 | Formononetin | Y = 0.0197593X − 0.0374138 | 0.9903 | 4 | 4–2000 | 7.41 | 7.49 | 5.89 | 112.36 ± 3.13 |
| 17 | Nobiletin | Y = 0.047895X − 0.0133269 | 0.9942 | 1 | 1–500 | 8.52 | 6.06 | 9.76 | 92.59 ± 3.64 |
| 18 | Tangeretin | Y = 0.188519X + 0.0417842 | 0.9948 | 0.4 | 0.4–200 | 8.74 | 6.05 | 9.44 | 99.47 ± 8.74 |
| 19 | Obacunone | Y = 0.000297133X − 0.00452012 | 0.9902 | 50 | 50–25,000 | 11.95 | 13.62 | 13.09 | 90.47 ± 7.57 |
| 20 | Glycyrrhetinic acid | Y = 0.000755862X − 0.00133086 | 0.9946 | 60 | 60–30,000 | 11.89 | 6.39 | 12.95 | 102.81 ± 10.84 |
| Samples | 0.25 mg/mL | 0.5 mg/mL | 1 mg/mL | 2 mg/mL | 4 mg/mL |
|---|---|---|---|---|---|
| S1 | 0.27 ± 0.16 | 0.38 ± 0.12 | 0.57 ± 0.05 | 0.24 ± 0.09 | −0.03 ± 0.17 |
| S2 | 0.19 ± 0.08 | 0.25 ± 0.10 | 0.53 ± 0.24 | 0.07 ± 0.02 | −0.14 ± 0.12 |
| S3 | 0.28 ± 0.20 | 0.33 ± 0.08 | 0.50 ± 0.13 | 0.10 ± 0.23 | −0.10 ± 0.03 |
| S4 | 0.19 ± 0.14 | 0.36 ± 0.07 | 0.59 ± 0.21 | 0.08 ± 0.23 | −0.01 ± 0.16 |
| S5 | 0.25 ± 0.25 | 0.32 ± 0.12 | 0.52 ± 0.16 | 0.08 ± 0.25 | −0.10 ± 0.15 |
| S6 | 0.18 ± 0.04 | 0.39 ± 0.26 | 0.58 ± 0.08 | 0.08 ± 0.06 | −0.08 ± 0.21 |
| S7 | 0.18 ± 0.04 | 0.39 ± 0.26 | 0.58 ± 0.08 | 0.08 ± 0.06 | −0.08 ± 0.21 |
| S8 | 0.18 ± 0.10 | 0.31 ± 0.11 | 0.61 ± 0.23 | 0.10 ± 0.18 | −0.08 ± 0.25 |
| S9 | 0.20 ± 0.15 | 0.30 ± 0.18 | 0.52 ± 0.13 | 0.17 ± 0.20 | −0.22 ± 0.08 |
| S10 | 0.12 ± 0.15 | 0.25 ± 0.11 | 0.48 ± 0.14 | 0.08 ± 0.11 | −0.10 ± 0.11 |
| S11 | 0.17 ± 0.19 | 0.26 ± 0.04 | 0.53 ± 0.12 | 0.22 ± 0.10 | −0.05 ± 0.16 |
| S12 | 0.12 ± 0.08 | 0.29 ± 0.14 | 0.47 ± 0.16 | 0.12 ± 0.10 | −0.12 ± 0.18 |
| S13 | 0.12 ± 0.10 | 0.26 ± 0.12 | 0.47 ± 0.06 | 0.06 ± 0.07 | −0.11 ± 0.11 |
| S14 | 0.09 ± 0.13 | 0.29 ± 0.21 | 0.47 ± 0.18 | 0.23 ± 0.05 | 0.04 ± 0.12 |
| S15 | 0.20 ± 0.09 | 0.33 ± 0.15 | 0.52 ± 0.21 | 0.13 ± 0.15 | −0.11 ± 0.13 |
| S16 | 0.17 ± 0.13 | 0.33 ± 0.19 | 0.52 ± 0.26 | 0.16 ± 0.08 | 0.00 ± 0.13 |
| NO. | Compounds | GRA | PLSR | NO. | Compounds | GRA | PLSR |
|---|---|---|---|---|---|---|---|
| 1 | Trigonelline | 0.88 | 0.822 | 11 | Glycyrrhizic acid | 0.901 | −0.565 |
| 2 | Synephrine | 0.869 | −0.507 | 12 | Morin | 0.795 | 0.856 |
| 3 | Isoquercitrin | 0.888 | −0.193 | 13 | Quercetin | 0.798 | 1.044 |
| 4 | Liquiritin | 0.886 | 1.259 | 14 | Isoliquiritigenin | 0.828 | 0.349 |
| 5 | Naringin | 0.789 | −0.513 | 15 | Liquiritigenin | 0.828 | 1.001 |
| 6 | Hesperidin | 0.892 | 0.404 | 16 | Formononetin | 0.883 | 1.477 |
| 7 | Hesperetin | 0.865 | 1.438 | 17 | Nobiletin | 0.864 | −0.403 |
| 8 | Scopoletin | 0.843 | 0.521 | 18 | Tangeretin | 0.838 | −0.716 |
| 9 | Daidzein | 0.885 | −1.167 | 19 | Obacunone | 0.819 | −1.003 |
| 10 | Naringenin | 0.785 | −1.659 | 20 | Glycyrrhetinic acid | 0.829 | −2.138 |
| Samples | BX | ZR | ZS | CP | GC |
|---|---|---|---|---|---|
| S1 | Shandong | Guangdong | Jiangxi | Sichuan | Baotou, Inner Mongolia |
| S2 | Shandong | Zhejiang | Chongqing | Fujian | Chifeng, Inner Mongolia |
| S3 | Shandong | Hubei | Sichuan | Guangdong | Ordos, Inner Mongolia |
| S4 | Shandong | Sichuan | Hunan | Hunan | Gansu |
| S5 | Sichuan | Guangdong | Chongqing | Guangdong | Gansu |
| S6 | Sichuan | Zhejiang | Jiangxi | Hunan | Ordos, Inner Mongolia |
| S7 | Sichuan | Hubei | Hunan | Sichuan | Chifeng, Inner Mongolia |
| S8 | Sichuan | Sichuan | Sichuan | Fujian | Baotou, Inner Mongolia |
| S9 | Gansu | Guangdong | Sichuan | Hunan | Chifeng, Inner Mongolia |
| S10 | Gansu | Zhejiang | Hunan | Guangdong | Baotou, Inner Mongolia |
| S11 | Gansu | Hubei | Jiangxi | Fujian | Gansu |
| S12 | Gansu | Sichuan | Chongqing | Sichuan | Ordos, Inner Mongolia |
| S13 | Guangxi | Guangdong | Hunan | Fujian | Ordos, Inner Mongolia |
| S14 | Guangxi | Zhejiang | Sichuan | Sichuan | Gansu |
| S15 | Guangxi | Hubei | Chongqing | Hunan | Baotou, Inner Mongolia |
| S16 | Guangxi | Sichuan | Jiangxi | Guangdong | Chifeng, Inner Mongolia |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Xu, N.; Ijaz, M.; Shi, H.; Shahbaz, M.; Cai, M.; Wang, P.; Guo, X.; Ma, L. Screening of Active Ingredients from Wendan Decoction in Alleviating Palmitic Acid-Induced Endothelial Cell Injury. Molecules 2023, 28, 1328. https://doi.org/10.3390/molecules28031328
Xu N, Ijaz M, Shi H, Shahbaz M, Cai M, Wang P, Guo X, Ma L. Screening of Active Ingredients from Wendan Decoction in Alleviating Palmitic Acid-Induced Endothelial Cell Injury. Molecules. 2023; 28(3):1328. https://doi.org/10.3390/molecules28031328
Chicago/Turabian StyleXu, Nan, Muhammad Ijaz, Haiyan Shi, Muhammad Shahbaz, Meichao Cai, Ping Wang, Xiuli Guo, and Lei Ma. 2023. "Screening of Active Ingredients from Wendan Decoction in Alleviating Palmitic Acid-Induced Endothelial Cell Injury" Molecules 28, no. 3: 1328. https://doi.org/10.3390/molecules28031328
APA StyleXu, N., Ijaz, M., Shi, H., Shahbaz, M., Cai, M., Wang, P., Guo, X., & Ma, L. (2023). Screening of Active Ingredients from Wendan Decoction in Alleviating Palmitic Acid-Induced Endothelial Cell Injury. Molecules, 28(3), 1328. https://doi.org/10.3390/molecules28031328







