Natural Products in Mitigation of Bisphenol A Toxicity: Future Therapeutic Use
Abstract
1. Introduction
1.1. Bisphenol A
1.2. Conventional Methods for BPA Degradation and Removal
2. Effects of BPA Exposure on Different Body Systems
2.1. The Changes Occuring in Different Systems of the Body
2.1.1. Reproductive System
2.1.2. Cardiovascular System
2.1.3. Endocrine System
2.1.4. Urinary System
2.1.5. Gastrointestinal System
2.1.6. Immune System
2.1.7. Respiratory System
2.1.8. Nervous System
2.2. Underlying Mechanisms of BPA Exposure-Induced Toxicity
3. Various Natural Products That Are Effective against BPA-Induced Toxicity
3.1. Plant Extract/Mixture of Natural Compounds
3.1.1. Pistacia integerrima
3.1.2. Fenugreek (Trigonella foenum-graecum)
3.1.3. Kefir
3.1.4. Grape Seed (Vitis vinifera L.)
3.1.5. Ficus deltoidea (Mas Cotek)
3.1.6. Sweet Potato (Ipomoea batatas L. Lam.)
3.1.7. Quercus dilatata Lindl. ex Royle
3.1.8. Tualang Honey
3.1.9. Sesame Lignans
3.1.10. Propolis
3.1.11. Nigella sativa Oil
3.1.12. Green Tea
3.1.13. Soybean
3.1.14. Pumpkin Seed Oil
3.1.15. Ginkgo biloba
3.1.16. Ginseng
3.1.17. Murraya koenigii
3.1.18. Asparagus officinalis
3.1.19. Aloe vera (Aloe barbadensis Miller)
3.1.20. Tribulus terrestris L.
3.2. Natural Compounds
3.2.1. Resveratrol
3.2.2. Luteolin
3.2.3. Lycopene
3.2.4. Astragalus spinosus saponins and Astragaloside IV
3.2.5. Naringin
3.2.6. Taurine
3.2.7. Quercetin
3.2.8. Genistein
3.2.9. Curcumin
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Carcía-Córcoles, M.T.; Cipa, M.; Rodríguez-Gómez, R.; Rivas, A.; Olea-Serrano, F.; Vílchez, J.L.; Zafra-Gómez, A. Determination of bisphenols with estrogenic activity in plastic packaged baby food samples using solid-liquid extraction and clean-up with dispersive sorbents followed by gas chromatography tandem mass spectrometry analysis. Talanta 2018, 178, 441–448. [Google Scholar] [CrossRef] [PubMed]
- Eladak, S.; Grisin, T.; Moison, D.; Guerquin, M.J.; N’Tumba-Byn, T.; Pozzi-Gaudin, S.; Benachi, A.; Livera, G.; Rouiller-Fabre, V.; Habert, R. A new chapter in the bisphenol A story: Bisphenol S and bisphenol F are not safe alternatives to this compound. Fertil. Steril. 2015, 103, 11–21. [Google Scholar] [CrossRef] [PubMed]
- Huo, X.; Chen, D.; He, Y.; Zhu, W.; Zhou, W.; Zhang, J. Bisphenol-A and Female Infertility: A Possible Role of Gene-Environment Interactions. Int. J. Environ. Res. Public Health 2015, 12, 11101–11116. [Google Scholar] [CrossRef] [PubMed]
- Vandenberg, L.N.; Hunt, P.A.; Myers, J.P.; Vom Saal, F.S. Human exposures to bisphenol A: Mismatches between data and assumptions. Rev. Environ. Health 2013, 28, 37–58. [Google Scholar] [CrossRef]
- Zhang, Z.; Alomirah, H.; Cho, H.S.; Li, Y.F.; Liao, C.; Minh, T.B.; Mohd, M.A.; Nakata, H.; Ren, N.; Kannan, K. Urinary bisphenol A concentrations and their implications for human exposure in several Asian countries. Environ. Sci. Technol. 2011, 45, 7044–7050. [Google Scholar] [CrossRef]
- Cousins, I.T.; Staples, C.A.; Kleĉka, G.M.; Mackay, D. A Multimedia Assessment of the Environmental Fate of Bisphenol A. Hum. Ecol. Risk Assess. Int. J. 2002, 8, 1107–1135. [Google Scholar] [CrossRef]
- Le, H.H.; Carlson, E.M.; Chua, J.P.; Belcher, S.M. Bisphenol A is released from polycarbonate drinking bottles and mimics the neurotoxic actions of estrogen in developing cerebellar neurons. Toxicol. Lett. 2008, 176, 149–156. [Google Scholar] [CrossRef]
- Nam, S.H.; Seo, Y.M.; Kim, M.G. Bisphenol A migration from polycarbonate baby bottle with repeated use. Chemosphere 2010, 79, 949–952. [Google Scholar] [CrossRef]
- Cao, X.L.; Corriveau, J.; Popovic, S. Bisphenol a in canned food products from canadian markets. J. Food Prot. 2010, 73, 1085–1089. [Google Scholar] [CrossRef]
- Sajiki, J.; Miyamoto, F.; Fukata, H.; Mori, C.; Yonekubo, J.; Hayakawa, K. Bisphenol A (BPA) and its source in foods in Japanese markets. Food Addit. Contam. 2007, 24, 103–112. [Google Scholar] [CrossRef]
- Braunrath, R.; Podlipna, D.; Padlesak, S.; Cichna-Markl, M. Determination of bisphenol A in canned foods by immunoaffinity chromatography, HPLC, and fluorescence detection. J. Agric. Food Chem. 2005, 53, 8911–8917. [Google Scholar] [CrossRef]
- Biedermann, S.; Tschudin, P.; Grob, K. Transfer of bisphenol A from thermal printer paper to the skin. Anal. Bioanal. Chem. 2010, 398, 571–576. [Google Scholar] [CrossRef]
- Calafat, A.M.; Weuve, J.; Ye, X.; Jia, L.T.; Hu, H.; Ringer, S.; Huttner, K.; Hauser, R. Exposure to bisphenol A and other phenols in neonatal intensive care unit premature infants. Environ. Health Perspect. 2009, 117, 639–644. [Google Scholar] [CrossRef]
- Kanno, Y.; Okada, H.; Kobayashi, T.; Takenaka, T.; Suzuki, H. Effects of endocrine disrupting substance on estrogen receptor gene transcription in dialysis patients. Ther. Apher. Dial. Off. Peer-Rev. J. Int. Soc. Apher. Jpn. Soc. Apher. Jpn. Soc. Dial. Ther. 2007, 11, 262–265. [Google Scholar] [CrossRef]
- Zimmerman-Downs, J.M.; Shuman, D.; Stull, S.C.; Ratzlaff, R.E. Bisphenol A blood and saliva levels prior to and after dental sealant placement in adults. J. Dent. Hyg. JDH 2010, 84, 145–150. [Google Scholar]
- Husøy, T.; Beausoleil, C.; Benford, D.; Brantsaeter, A.L.; Calamandrei, G.; Doerge, D.; Fowler, P.; Greaves, P.; Gundert-Remy, U.; Hart, A.; et al. Scientific Opinion on the Risks to Public Health Related to the Presence of Bisphenol A (BPA) in Foodstuffs: Part I-Exposure Assessment. EFSA J. 2015, 13, 3978. [Google Scholar]
- Almeida, S.; Raposo, A.; Almeida-González, M.; Carrascosa, C. Bisphenol A: Food Exposure and Impact on Human Health. Compr. Rev. Food Sci. Food Saf. 2018, 17, 1503–1517. [Google Scholar] [CrossRef]
- Inoue, H.; Yuki, G.; Yokota, H.; Kato, S. Bisphenol A glucuronidation and absorption in rat intestine. Drug Metab. Dispos. Biol. Fate Chem. 2003, 31, 140–144. [Google Scholar] [CrossRef]
- Yokota, H.; Iwano, H.; Endo, M.; Kobayashi, T.; Inoue, H.; Ikushiro, S.; Yuasa, A. Glucuronidation of the environmental oestrogen bisphenol A by an isoform of UDP-glucuronosyltransferase, UGT2B1, in the rat liver. Biochem. J. 1999, 340 Pt 2, 405–409. [Google Scholar] [CrossRef]
- Genuis, S.J.; Beesoon, S.; Birkholz, D.; Lobo, R.A. Human excretion of bisphenol A: Blood, urine, and sweat (BUS) study. J. Environ. Public Health 2012, 2012, 185731. [Google Scholar] [CrossRef]
- Ginsberg, G.; Rice, D.C. Does rapid metabolism ensure negligible risk from bisphenol A? Environ. Health Perspect. 2009, 117, 1639–1643. [Google Scholar] [CrossRef]
- Martínez, M.; González, N.; Martí, A.; Marquès, M.; Rovira, J.; Kumar, V.; Nadal, M. Human biomonitoring of bisphenol A along pregnancy: An exposure reconstruction of the EXHES-Spain cohort. Environ. Res. 2021, 196, 110941. [Google Scholar] [CrossRef]
- Völkel, W.; Colnot, T.; Csanády, G.A.; Filser, J.G.; Dekant, W. Metabolism and kinetics of bisphenol a in humans at low doses following oral administration. Chem. Res. Toxicol. 2002, 15, 1281–1287. [Google Scholar] [CrossRef]
- Vandenberg, L.N.; Chahoud, I.; Heindel, J.J.; Padmanabhan, V.; Paumgartten, F.J.; Schoenfelder, G. Urinary, circulating, and tissue biomonitoring studies indicate widespread exposure to bisphenol A. Environ. Health Perspect. 2010, 118, 1055–1070. [Google Scholar] [CrossRef]
- Soriano, S.; Ripoll, C.; Alonso-Magdalena, P.; Fuentes, E.; Quesada, I.; Nadal, A.; Martinez-Pinna, J. Effects of Bisphenol A on ion channels: Experimental evidence and molecular mechanisms. Steroids 2016, 111, 12–20. [Google Scholar] [CrossRef]
- Hafezi, S.A.; Abdel-Rahman, W.M. The Endocrine Disruptor Bisphenol A (BPA) Exerts a Wide Range of Effects in Carcinogenesis and Response to Therapy. Curr. Mol. Pharmacol. 2019, 12, 230–238. [Google Scholar] [CrossRef]
- Csanády, G.A.; Oberste-Frielinghaus, H.R.; Semder, B.; Baur, C.; Schneider, K.T.; Filser, J.G. Distribution and unspecific protein binding of the xenoestrogens bisphenol A and daidzein. Arch. Toxicol. 2002, 76, 299–305. [Google Scholar] [CrossRef] [PubMed]
- Geens, T.; Neels, H.; Covaci, A. Distribution of bisphenol-A, triclosan and n-nonylphenol in human adipose tissue, liver and brain. Chemosphere 2012, 87, 796–802. [Google Scholar] [CrossRef] [PubMed]
- Staples, C.A.; Dorn, P.B.; Klecka, G.M.; O’Block, S.T.; Harris, L.R. A review of the environmental fate, effects, and exposures of bisphenol A. Chemosphere 1998, 36, 2149–2173. [Google Scholar] [CrossRef]
- Shehab, Z.N.; Jamil, N.R.; Aris, A.Z. Occurrence, environmental implications and risk assessment of Bisphenol A in association with colloidal particles in an urban tropical river in Malaysia. Sci. Rep. 2020, 10, 20360. [Google Scholar] [CrossRef]
- Selvaraj, K.K.; Shanmugam, G.; Sampath, S.; Larsson, D.G.; Ramaswamy, B.R. GC-MS determination of bisphenol A and alkylphenol ethoxylates in river water from India and their ecotoxicological risk assessment. Ecotoxicol. Environ. Saf. 2014, 99, 13–20. [Google Scholar] [CrossRef]
- Esteban, S.; Gorga, M.; Petrovic, M.; González-Alonso, S.; Barceló, D.; Valcárcel, Y. Analysis and occurrence of endocrine-disrupting compounds and estrogenic activity in the surface waters of Central Spain. Sci. Total Environ. 2014, 466–467, 939–951. [Google Scholar] [CrossRef]
- Heemken, O.P.; Reincke, H.; Stachel, B.; Theobald, N. The occurrence of xenoestrogens in the Elbe river and the North Sea. Chemosphere 2001, 45, 245–259. [Google Scholar] [CrossRef]
- Wang, Q.; Chen, M.; Shan, G.; Chen, P.; Cui, S.; Yi, S.; Zhu, L. Bioaccumulation and biomagnification of emerging bisphenol analogues in aquatic organisms from Taihu Lake, China. Sci. Total Environ. 2017, 598, 814–820. [Google Scholar] [CrossRef]
- Chiriac, F.L.; Paun, I.; Pirvu, F.; Pascu, L.F.; Galaon, T. Occurrence and Fate of Bisphenol A and its Congeners in Two Wastewater Treatment Plants and Receiving Surface Waters in Romania. Environ. Toxicol. Chem. 2021, 40, 435–446. [Google Scholar] [CrossRef]
- Kim, D.; Kwak, J.I.; An, Y.J. Effects of bisphenol A in soil on growth, photosynthesis activity, and genistein levels in crop plants (Vigna radiata). Chemosphere 2018, 209, 875–882. [Google Scholar] [CrossRef]
- Gibson, R.; Durán-Álvarez, J.C.; Estrada, K.L.; Chávez, A.; Jiménez Cisneros, B. Accumulation and leaching potential of some pharmaceuticals and potential endocrine disruptors in soils irrigated with wastewater in the Tula Valley, Mexico. Chemosphere 2010, 81, 1437–1445. [Google Scholar] [CrossRef]
- Staples, C.; Friederich, U.; Hall, T.; Klečka, G.; Mihaich, E.; Ortego, L.; Caspers, N.; Hentges, S. Estimating potential risks to terrestrial invertebrates and plants exposed to bisphenol A in soil amended with activated sludge biosolids. Environ. Toxicol. Chem. 2010, 29, 467–475. [Google Scholar] [CrossRef]
- Arp, H.P.H.; Morin, N.A.O.; Hale, S.E.; Okkenhaug, G.; Breivik, K.; Sparrevik, M. The mass flow and proposed management of bisphenol A in selected Norwegian waste streams. Waste Manag. 2017, 60, 775–785. [Google Scholar] [CrossRef]
- Bi, X.; Simoneit, B.; Wang, Z.; Wang, X.; Sheng, G.; Fu, J. The Major Components of Particles Emitted During Recycling of Waste Printed Circuit Boards in a Typical E-Waste Workshop of South China. Atmos. Environ. 2010, 44, 4440–4445. [Google Scholar] [CrossRef]
- Gasser, C.A.; Yu, L.; Svojitka, J.; Wintgens, T.; Ammann, E.M.; Shahgaldian, P.; Corvini, P.F.; Hommes, G. Advanced enzymatic elimination of phenolic contaminants in wastewater: A nano approach at field scale. Appl. Microbiol. Biotechnol. 2014, 98, 3305–3316. [Google Scholar] [CrossRef]
- Li, X.; Chen, S.; Li, L.; Quan, X.; Zhao, H. Electrochemically enhanced adsorption of nonylphenol on carbon nanotubes: Kinetics and isotherms study. J. Colloid Interface Sci. 2014, 415, 159–164. [Google Scholar] [CrossRef]
- Cajthaml, T.; Kresinová, Z.; Svobodová, K.; Möder, M. Biodegradation of endocrine-disrupting compounds and suppression of estrogenic activity by ligninolytic fungi. Chemosphere 2009, 75, 745–750. [Google Scholar] [CrossRef]
- Asgher, M.; Bhatti, H.N.; Ashraf, M.; Legge, R.L. Recent developments in biodegradation of industrial pollutants by white rot fungi and their enzyme system. Biodegradation 2008, 19, 771–783. [Google Scholar] [CrossRef] [PubMed]
- Hirano, T.; Honda, Y.; Watanabe, T.; Kuwahara, M. Degradation of bisphenol A by the lignin-degrading enzyme, manganese peroxidase, produced by the white-rot basidiomycete, Pleurotus ostreatus. Biosci. Biotechnol. Biochem. 2000, 64, 1958–1962. [Google Scholar] [CrossRef] [PubMed]
- Chouhan, S.; Yadav, S.K.; Prakash, J.; Swati; Singh, S.P. Effect of Bisphenol A on human health and its degradation by microorganisms: A review. Ann. Microbiol. 2014, 64, 13–21. [Google Scholar] [CrossRef]
- Lontie, R. Copper Proteins and Copper Enzymes; CRC Press: Boca Raton, FL, USA, 1984; Volume 1. [Google Scholar]
- Tsutsumi, Y.; Haneda, T.; Nishida, T. Removal of estrogenic activities of bisphenol A and nonylphenol by oxidative enzymes from lignin-degrading basidiomycetes. Chemosphere 2001, 42, 271–276. [Google Scholar] [CrossRef]
- Temuujin, J.; Surenjav, E.; Ruescher, C.H.; Vahlbruch, J. Processing and uses of fly ash addressing radioactivity (critical review). Chemosphere 2019, 216, 866–882. [Google Scholar] [CrossRef]
- Xie, J.; Meng, W.; Wu, D.; Zhang, Z.; Kong, H. Removal of organic pollutants by surfactant modified zeolite: Comparison between ionizable phenolic compounds and non-ionizable organic compounds. J. Hazard. Mater. 2012, 231–232, 57–63. [Google Scholar] [CrossRef]
- Dong, Y.; Wu, D.; Chen, X.; Lin, Y. Adsorption of bisphenol A from water by surfactant-modified zeolite. J. Colloid Interface Sci. 2010, 348, 585–590. [Google Scholar] [CrossRef]
- Karim, Z.; Husain, Q. Application of fly ash adsorbed peroxidase for the removal of bisphenol A in batch process and continuous reactor: Assessment of genotoxicity of its product. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2010, 48, 3385–3390. [Google Scholar] [CrossRef]
- Galloway, T.; Cipelli, R.; Guralnik, J.; Ferrucci, L.; Bandinelli, S.; Corsi, A.M.; Money, C.; McCormack, P.; Melzer, D. Daily bisphenol A excretion and associations with sex hormone concentrations: Results from the InCHIANTI adult population study. Environ. Health Perspect. 2010, 118, 1603–1608. [Google Scholar] [CrossRef]
- Arase, S.; Ishii, K.; Igarashi, K.; Aisaki, K.; Yoshio, Y.; Matsushima, A.; Shimohigashi, Y.; Arima, K.; Kanno, J.; Sugimura, Y. Endocrine disrupter bisphenol A increases in situ estrogen production in the mouse urogenital sinus. Biol. Reprod. 2011, 84, 734–742. [Google Scholar] [CrossRef]
- Pivonello, C.; Muscogiuri, G.; Nardone, A.; Garifalos, F.; Provvisiero, D.P.; Verde, N.; de Angelis, C.; Conforti, A.; Piscopo, M.; Auriemma, R.S.; et al. Bisphenol A: An emerging threat to female fertility. Reprod. Biol. Endocrinol. RBE 2020, 18, 22. [Google Scholar] [CrossRef]
- La Rocca, C.; Tait, S.; Guerranti, C.; Busani, L.; Ciardo, F.; Bergamasco, B.; Stecca, L.; Perra, G.; Mancini, F.R.; Marci, R.; et al. Exposure to endocrine disrupters and nuclear receptor gene expression in infertile and fertile women from different Italian areas. Int. J. Environ. Res. Public Health 2014, 11, 10146–10164. [Google Scholar] [CrossRef]
- Tachibana, T.; Wakimoto, Y.; Nakamuta, N.; Phichitraslip, T.; Wakitani, S.; Kusakabe, K.; Hondo, E.; Kiso, Y. Effects of bisphenol A (BPA) on placentation and survival of the neonates in mice. J. Reprod. Dev. 2007, 53, 509–514. [Google Scholar] [CrossRef]
- Honma, S.; Suzuki, A.; Buchanan, D.L.; Katsu, Y.; Watanabe, H.; Iguchi, T. Low dose effect of in utero exposure to bisphenol A and diethylstilbestrol on female mouse reproduction. Reprod. Toxicol. 2002, 16, 117–122. [Google Scholar] [CrossRef]
- Lawson, C.; Gieske, M.; Murdoch, B.; Ye, P.; Li, Y.; Hassold, T.; Hunt, P.A. Gene expression in the fetal mouse ovary is altered by exposure to low doses of bisphenol A. Biol. Reprod. 2011, 84, 79–86. [Google Scholar] [CrossRef]
- Rodríguez, H.A.; Santambrosio, N.; Santamaría, C.G.; Muñoz-de-Toro, M.; Luque, E.H. Neonatal exposure to bisphenol A reduces the pool of primordial follicles in the rat ovary. Reprod. Toxicol. 2010, 30, 550–557. [Google Scholar] [CrossRef]
- Sugiura-Ogasawara, M.; Ozaki, Y.; Sonta, S.; Makino, T.; Suzumori, K. Exposure to bisphenol A is associated with recurrent miscarriage. Hum. Reprod. 2005, 20, 2325–2329. [Google Scholar] [CrossRef]
- Mínguez-Alarcón, L.; Gaskins, A.J.; Chiu, Y.H.; Williams, P.L.; Ehrlich, S.; Chavarro, J.E.; Petrozza, J.C.; Ford, J.B.; Calafat, A.M.; Hauser, R. Urinary bisphenol A concentrations and association with in vitro fertilization outcomes among women from a fertility clinic. Hum. Reprod. 2015, 30, 2120–2128. [Google Scholar] [CrossRef] [PubMed]
- Vahedi, M.; Saeedi, A.; Poorbaghi, S.L.; Sepehrimanesh, M.; Fattahi, M. Metabolic and endocrine effects of bisphenol A exposure in market seller women with polycystic ovary syndrome. Environ. Sci. Pollut. Res. Int. 2016, 23, 23546–23550. [Google Scholar] [CrossRef] [PubMed]
- Shen, Y.; Zheng, Y.; Jiang, J.; Liu, Y.; Luo, X.; Shen, Z.; Chen, X.; Wang, Y.; Dai, Y.; Zhao, J.; et al. Higher urinary bisphenol A concentration is associated with unexplained recurrent miscarriage risk: Evidence from a case-control study in eastern China. PLoS ONE 2015, 10, e0127886. [Google Scholar] [CrossRef] [PubMed]
- Schönfelder, G.; Friedrich, K.; Paul, M.; Chahoud, I. Developmental effects of prenatal exposure to bisphenol a on the uterus of rat offspring. Neoplasia 2004, 6, 584–594. [Google Scholar] [CrossRef]
- Markey, C.M.; Luque, E.H.; Munoz De Toro, M.; Sonnenschein, C.; Soto, A.M. In utero exposure to bisphenol A alters the development and tissue organization of the mouse mammary gland. Biol. Reprod. 2001, 65, 1215–1223. [Google Scholar] [CrossRef]
- Ehrlich, S.; Williams, P.L.; Missmer, S.A.; Flaws, J.A.; Berry, K.F.; Calafat, A.M.; Ye, X.; Petrozza, J.C.; Wright, D.; Hauser, R. Urinary bisphenol A concentrations and implantation failure among women undergoing in vitro fertilization. Environ. Health Perspect. 2012, 120, 978–983. [Google Scholar] [CrossRef]
- Ji, H.; Miao, M.; Liang, H.; Shi, H.; Ruan, D.; Li, Y.; Wang, J.; Yuan, W. Exposure of environmental Bisphenol A in relation to routine sperm parameters and sperm movement characteristics among fertile men. Sci. Rep. 2018, 8, 17548. [Google Scholar] [CrossRef]
- Li, D.; Zhou, Z.; Qing, D.; He, Y.; Wu, T.; Miao, M.; Wang, J.; Weng, X.; Ferber, J.R.; Herrinton, L.J.; et al. Occupational exposure to bisphenol-A (BPA) and the risk of self-reported male sexual dysfunction. Hum. Reprod. 2010, 25, 519–527. [Google Scholar] [CrossRef]
- Jin, P.; Wang, X.; Chang, F.; Bai, Y.; Li, Y.; Zhou, R.; Chen, L. Low dose bisphenol A impairs spermatogenesis by suppressing reproductive hormone production and promoting germ cell apoptosis in adult rats. J. Biomed. Res. 2013, 27, 135–144. [Google Scholar] [CrossRef]
- Sirasanagandla, S.R.; Al-Huseini, I.; Sofin, R.G.S.; Das, S. Perinatal exposure to Bisphenol A and developmental programming of the cardiovascular changes in the offspring. Curr. Med. Chem. 2022, 29, 4235–4250. [Google Scholar] [CrossRef]
- Wei, J.; Lin, Y.; Li, Y.; Ying, C.; Chen, J.; Song, L.; Zhou, Z.; Lv, Z.; Xia, W.; Chen, X.; et al. Perinatal exposure to bisphenol A at reference dose predisposes offspring to metabolic syndrome in adult rats on a high-fat diet. Endocrinology 2011, 152, 3049–3061. [Google Scholar] [CrossRef]
- Ma, Y.; Xia, W.; Wang, D.Q.; Wan, Y.J.; Xu, B.; Chen, X.; Li, Y.Y.; Xu, S.Q. Hepatic DNA methylation modifications in early development of rats resulting from perinatal BPA exposure contribute to insulin resistance in adulthood. Diabetologia 2013, 56, 2059–2067. [Google Scholar] [CrossRef]
- Alonso-Magdalena, P.; Vieira, E.; Soriano, S.; Menes, L.; Burks, D.; Quesada, I.; Nadal, A. Bisphenol A exposure during pregnancy disrupts glucose homeostasis in mothers and adult male offspring. Environ. Health Perspect. 2010, 118, 1243–1250. [Google Scholar] [CrossRef]
- Miyawaki, J.; Sakayama, K.; Kato, H.; Yamamoto, H.; Masuno, H. Perinatal and postnatal exposure to bisphenol a increases adipose tissue mass and serum cholesterol level in mice. J. Atheroscler. Thromb. 2007, 14, 245–252. [Google Scholar] [CrossRef]
- Chen, X.; Bao, H.H.; Wu, W.K.; Yan, S.Q.; Sheng, J.; Xu, Y.Y.; Gu, C.L.; Huang, K.; Cao, H.; Su, P.Y.; et al. Exposure to bisphenol A during maternal pregnancy and the emotional and behavioral impact on their preschool children. Zhonghua Liu Xing Bing Xue Za Zhi = Zhonghua Liuxingbingxue Zazhi 2018, 39, 188–193. [Google Scholar] [CrossRef]
- Perera, F.; Nolte, E.L.R.; Wang, Y.; Margolis, A.E.; Calafat, A.M.; Wang, S.; Garcia, W.; Hoepner, L.A.; Peterson, B.S.; Rauh, V.; et al. Bisphenol A exposure and symptoms of anxiety and depression among inner city children at 10-12 years of age. Environ. Res. 2016, 151, 195–202. [Google Scholar] [CrossRef]
- Lang, I.A.; Galloway, T.S.; Scarlett, A.; Henley, W.E.; Depledge, M.; Wallace, R.B.; Melzer, D. Association of urinary bisphenol A concentration with medical disorders and laboratory abnormalities in adults. JAMA 2008, 300, 1303–1310. [Google Scholar] [CrossRef]
- Melzer, D.; Gates, P.; Osborne, N.J.; Henley, W.E.; Cipelli, R.; Young, A.; Money, C.; McCormack, P.; Schofield, P.; Mosedale, D.; et al. Urinary bisphenol a concentration and angiography-defined coronary artery stenosis. PLoS ONE 2012, 7, e43378. [Google Scholar] [CrossRef]
- Xiong, Q.; Liu, X.; Shen, Y.; Yu, P.; Chen, S.; Hu, J.; Yu, J.; Li, J.; Wang, H.S.; Cheng, X.; et al. Elevated serum Bisphenol A level in patients with dilated cardiomyopathy. Int. J. Environ. Res. Public Health 2015, 12, 5329–5337. [Google Scholar] [CrossRef]
- Patel, B.B.; Raad, M.; Sebag, I.A.; Chalifour, L.E. Lifelong exposure to bisphenol a alters cardiac structure/function, protein expression, and DNA methylation in adult mice. Toxicol. Sci. Off. J. Soc. Toxicol. 2013, 133, 174–185. [Google Scholar] [CrossRef]
- Posnack, N.G.; Jaimes, R., 3rd; Asfour, H.; Swift, L.M.; Wengrowski, A.M.; Sarvazyan, N.; Kay, M.W. Bisphenol A exposure and cardiac electrical conduction in excised rat hearts. Environ. Health Perspect. 2014, 122, 384–390. [Google Scholar] [CrossRef]
- Cagampang, F.R.; Torrens, C.; Anthony, F.W.; Hanson, M.A. Developmental exposure to bisphenol A leads to cardiometabolic dysfunction in adult mouse offspring. J. Dev. Orig. Health Dis. 2012, 3, 287–292. [Google Scholar] [CrossRef]
- Yan, S.; Chen, Y.; Dong, M.; Song, W.; Belcher, S.M.; Wang, H.S. Bisphenol A and 17β-estradiol promote arrhythmia in the female heart via alteration of calcium handling. PLoS ONE 2011, 6, e25455. [Google Scholar] [CrossRef]
- O’Reilly, A.O.; Eberhardt, E.; Weidner, C.; Alzheimer, C.; Wallace, B.A.; Lampert, A. Bisphenol A binds to the local anesthetic receptor site to block the human cardiac sodium channel. PLoS ONE 2012, 7, e41667. [Google Scholar] [CrossRef] [PubMed]
- Belcher, S.M.; Chen, Y.; Yan, S.; Wang, H.S. Rapid estrogen receptor-mediated mechanisms determine the sexually dimorphic sensitivity of ventricular myocytes to 17β-estradiol and the environmental endocrine disruptor bisphenol A. Endocrinology 2012, 153, 712–720. [Google Scholar] [CrossRef] [PubMed]
- Lind, P.M.; Lind, L. Circulating levels of bisphenol A and phthalates are related to carotid atherosclerosis in the elderly. Atherosclerosis 2011, 218, 207–213. [Google Scholar] [CrossRef] [PubMed]
- Shankar, A.; Teppala, S.; Sabanayagam, C. Bisphenol A and peripheral arterial disease: Results from the NHANES. Environ. Health Perspect. 2012, 120, 1297–1300. [Google Scholar] [CrossRef] [PubMed]
- Sui, Y.; Park, S.H.; Helsley, R.N.; Sunkara, M.; Gonzalez, F.J.; Morris, A.J.; Zhou, C. Bisphenol A increases atherosclerosis in pregnane X receptor-humanized ApoE deficient mice. J. Am. Heart Assoc. 2014, 3, e000492. [Google Scholar] [CrossRef]
- Choi, Y.J.; Lee, Y.A.; Hong, Y.C.; Cho, J.; Lee, K.S.; Shin, C.H.; Kim, B.N.; Kim, J.I.; Park, S.J.; Bisgaard, H.; et al. Effect of prenatal bisphenol A exposure on early childhood body mass index through epigenetic influence on the insulin-like growth factor 2 receptor (IGF2R) gene. Environ. Int. 2020, 143, 105929. [Google Scholar] [CrossRef]
- Junge, K.M.; Leppert, B.; Jahreis, S.; Wissenbach, D.K.; Feltens, R.; Grützmann, K.; Thürmann, L.; Bauer, T.; Ishaque, N.; Schick, M.; et al. MEST mediates the impact of prenatal bisphenol A exposure on long-term body weight development. Clin. Epigenetics 2018, 10, 58. [Google Scholar] [CrossRef]
- Ropero, A.B.; Alonso-Magdalena, P.; García-García, E.; Ripoll, C.; Fuentes, E.; Nadal, A. Bisphenol-A disruption of the endocrine pancreas and blood glucose homeostasis. Int. J. Androl. 2008, 31, 194–200. [Google Scholar] [CrossRef]
- Moon, M.K.; Jeong, I.K.; Oh, T.J.; Ahn, H.Y.; Kim, H.H.; Park, Y.J.; Jang, H.C.; Park, K.S. Long-term oral exposure to bisphenol A induces glucose intolerance and insulin resistance. J. Endocrinol. 2015, 226, 35–42. [Google Scholar] [CrossRef]
- Duan, Y.; Yao, Y.; Wang, B.; Han, L.; Wang, L.; Sun, H.; Chen, L. Association of urinary concentrations of bisphenols with type 2 diabetes mellitus: A case-control study. Environ. Pollut. 2018, 243, 1719–1726. [Google Scholar] [CrossRef]
- Li, A.J.; Xue, J.; Lin, S.; Al-Malki, A.L.; Al-Ghamdi, M.A.; Kumosani, T.A.; Kannan, K. Urinary concentrations of environmental phenols and their association with type 2 diabetes in a population in Jeddah, Saudi Arabia. Environ. Res. 2018, 166, 544–552. [Google Scholar] [CrossRef]
- Bellavia, A.; Cantonwine, D.E.; Meeker, J.D.; Hauser, R.; Seely, E.W.; McElrath, T.F.; James-Todd, T. Pregnancy urinary bisphenol-A concentrations and glucose levels across BMI categories. Environ. Int. 2018, 113, 35–41. [Google Scholar] [CrossRef]
- Chiu, Y.H.; Mínguez-Alarcón, L.; Ford, J.B.; Keller, M.; Seely, E.W.; Messerlian, C.; Petrozza, J.; Williams, P.L.; Ye, X.; Calafat, A.M.; et al. Trimester-Specific Urinary Bisphenol A Concentrations and Blood Glucose Levels Among Pregnant Women From a Fertility Clinic. J. Clin. Endocrinol. Metab. 2017, 102, 1350–1357. [Google Scholar] [CrossRef]
- Eng, D.S.; Lee, J.M.; Gebremariam, A.; Meeker, J.D.; Peterson, K.; Padmanabhan, V. Bisphenol A and chronic disease risk factors in US children. Pediatrics 2013, 132, e637–e645. [Google Scholar] [CrossRef]
- Akash, M.S.H.; Sabir, S.; Rehman, K. Bisphenol A-induced metabolic disorders: From exposure to mechanism of action. Environ. Toxicol. Pharmacol. 2020, 77, 103373. [Google Scholar] [CrossRef]
- Poormoosavi, S.M.; Najafzadehvarzi, H.; Behmanesh, M.A.; Amirgholami, R. Protective effects of Asparagus officinalis extract against Bisphenol A- induced toxicity in Wistar rats. Toxicol. Rep. 2018, 5, 427–433. [Google Scholar] [CrossRef]
- Nicholson, T.M.; Nguyen, J.L.; Leverson, G.E.; Taylor, J.A.; Vom Saal, F.S.; Wood, R.W.; Ricke, W.A. Endocrine disruptor bisphenol A is implicated in urinary voiding dysfunction in male mice. Am. J. Physiol. Ren. Physiol. 2018, 315, F1208–F1216. [Google Scholar] [CrossRef]
- Kataria, A.; Trasande, L.; Trachtman, H. The effects of environmental chemicals on renal function. Nat. Rev Nephrol. 2015, 11, 610–625. [Google Scholar] [CrossRef] [PubMed]
- Priego, A.R.; Parra, E.G.; Mas, S.; Morgado-Pascual, J.L.; Ruiz-Ortega, M.; Rayego-Mateos, S. Bisphenol A Modulates Autophagy and Exacerbates Chronic Kidney Damage in Mice. Int. J. Mol. Sci. 2021, 22, 7189. [Google Scholar] [CrossRef] [PubMed]
- Bosch-Panadero, E.; Mas, S.; Civantos, E.; Abaigar, P.; Camarero, V.; Ruiz-Priego, A.; Ortiz, A.; Egido, J.; González-Parra, E. Bisphenol A is an exogenous toxin that promotes mitochondrial injury and death in tubular cells. Environ. Toxicol. 2018, 33, 325–332. [Google Scholar] [CrossRef] [PubMed]
- Gassman, N.R. Induction of oxidative stress by bisphenol A and its pleiotropic effects. Environ. Mol. Mutagenesis 2017, 58, 60–71. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.R.; Park, H.; Bae, S.; Lim, Y.H.; Kim, J.H.; Cho, S.H.; Hong, Y.C. Urinary bisphenol A concentrations are associated with abnormal liver function in the elderly: A repeated panel study. J. Epidemiol. Community Health 2014, 68, 312–317. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.; Yoo, E.R.; Li, A.A.; Cholankeril, G.; Tighe, S.P.; Kim, W.; Harrison, S.A.; Ahmed, A. Elevated urinary bisphenol A levels are associated with non-alcoholic fatty liver disease among adults in the United States. Liver Int. Off. J. Int. Assoc. Study Liver 2019, 39, 1335–1342. [Google Scholar] [CrossRef] [PubMed]
- Mahdavinia, M.; Alizadeh, S.; Raesi Vanani, A.; Dehghani, M.A.; Shirani, M.; Alipour, M.; Shahmohammadi, H.A.; Rafiei Asl, S. Effects of quercetin on bisphenol A-induced mitochondrial toxicity in rat liver. Iran. J. Basic Med. Sci. 2019, 22, 499–505. [Google Scholar] [CrossRef]
- Martella, A.; Silvestri, C.; Maradonna, F.; Gioacchini, G.; Allarà, M.; Radaelli, G.; Overby, D.R.; Di Marzo, V.; Carnevali, O. Bisphenol A Induces Fatty Liver by an Endocannabinoid-Mediated Positive Feedback Loop. Endocrinology 2016, 157, 1751–1763. [Google Scholar] [CrossRef]
- Geng, S.; Wang, S.; Zhu, W.; Xie, C.; Li, X.; Wu, J.; Zhu, J.; Jiang, Y.; Yang, X.; Li, Y.; et al. Curcumin attenuates BPA-induced insulin resistance in HepG2 cells through suppression of JNK/p38 pathways. Toxicol. Lett. 2017, 272, 75–83. [Google Scholar] [CrossRef]
- Nakagawa, Y.; Tayama, S. Metabolism and cytotoxicity of bisphenol A and other bisphenols in isolated rat hepatocytes. Arch. Toxicol. 2000, 74, 99–105. [Google Scholar] [CrossRef]
- Lin, Y.; Ding, D.; Huang, Q.; Liu, Q.; Lu, H.; Lu, Y.; Chi, Y.; Sun, X.; Ye, G.; Zhu, H.; et al. Downregulation of miR-192 causes hepatic steatosis and lipid accumulation by inducing SREBF1: Novel mechanism for bisphenol A-triggered non-alcoholic fatty liver disease. Biochim. Biophys. Acta. Mol. Cell Biol. Lipids 2017, 1862, 869–882. [Google Scholar] [CrossRef]
- Ratajczak-Wrona, W.; Nowak, K.; Garley, M.; Grubczak, K.; Dabrowska, D.; Iwaniuk, A.; Wilk, S.; Moniuszko, M.; Czerniecki, J.; Wolczynski, S.; et al. Expression of serine proteases in neutrophils from women and men: Regulation by endocrine disruptor bisphenol A. Environ. Toxicol. Pharmacol. 2019, 71, 103212. [Google Scholar] [CrossRef]
- Ratajczak-Wrona, W.; Rusak, M.; Nowak, K.; Dabrowska, M.; Radziwon, P.; Jablonska, E. Effect of bisphenol A on human neutrophils immunophenotype. Sci. Rep. 2020, 10, 3083. [Google Scholar] [CrossRef]
- Baralla, E.; Demontis, M.P.; Varoni, M.V.; Pasciu, V. Bisphenol A and Bisphenol S Oxidative Effects in Sheep Red Blood Cells: An In Vitro Study. BioMed Res. Int. 2021, 2021, 6621264. [Google Scholar] [CrossRef]
- Michałowicz, J. Bisphenol A—Sources, toxicity and biotransformation. Environ. Toxicol. Pharmacol. 2014, 37, 738–758. [Google Scholar] [CrossRef]
- Wang, I.J.; Chen, C.Y.; Bornehag, C.G. Bisphenol A exposure may increase the risk of development of atopic disorders in children. Int. J. Hyg. Environ. Health 2016, 219, 311–316. [Google Scholar] [CrossRef]
- Donohue, K.M.; Miller, R.L.; Perzanowski, M.S.; Just, A.C.; Hoepner, L.A.; Arunajadai, S.; Canfield, S.; Resnick, D.; Calafat, A.M.; Perera, F.P.; et al. Prenatal and postnatal bisphenol A exposure and asthma development among inner-city children. J. Allergy Clin. Immunol. 2013, 131, 736–742. [Google Scholar] [CrossRef]
- Spanier, A.J.; Kahn, R.S.; Kunselman, A.R.; Hornung, R.; Xu, Y.; Calafat, A.M.; Lanphear, B.P. Prenatal exposure to bisphenol A and child wheeze from birth to 3 years of age. Environ. Health Perspect. 2012, 120, 916–920. [Google Scholar] [CrossRef]
- Gascon, M.; Casas, M.; Morales, E.; Valvi, D.; Ballesteros-Gómez, A.; Luque, N.; Rubio, S.; Monfort, N.; Ventura, R.; Martínez, D.; et al. Prenatal exposure to bisphenol A and phthalates and childhood respiratory tract infections and allergy. J. Allergy Clin. Immunol. 2015, 135, 370–378. [Google Scholar] [CrossRef]
- Leung, Y.K.; Govindarajah, V.; Cheong, A.; Veevers, J.; Song, D.; Gear, R.; Zhu, X.; Ying, J.; Kendler, A.; Medvedovic, M.; et al. Gestational high-fat diet and bisphenol A exposure heightens mammary cancer risk. Endocr.-Relat. Cancer 2017, 24, 365–378. [Google Scholar] [CrossRef]
- Tse, L.A.; Lee, P.M.Y.; Ho, W.M.; Lam, A.T.; Lee, M.K.; Ng, S.S.M.; He, Y.; Leung, K.S.; Hartle, J.C.; Hu, H.; et al. Bisphenol A and other environmental risk factors for prostate cancer in Hong Kong. Environ. Int. 2017, 107, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Rahbar, M.H.; Swingle, H.M.; Christian, M.A.; Hessabi, M.; Lee, M.; Pitcher, M.R.; Campbell, S.; Mitchell, A.; Krone, R.; Loveland, K.A.; et al. Environmental Exposure to Dioxins, Dibenzofurans, Bisphenol A, and Phthalates in Children with and without Autism Spectrum Disorder Living near the Gulf of Mexico. Int. J. Environ. Res. Public Health 2017, 14, 1425. [Google Scholar] [CrossRef] [PubMed]
- Metwally, F.M.; Rashad, H.; Zeidan, H.M.; Kilany, A.; Abdol Raouf, E.R. Study of the Effect of Bisphenol A on Oxidative Stress in Children with Autism Spectrum Disorders. Indian J. Clin. Biochem. IJCB 2018, 33, 196–201. [Google Scholar] [CrossRef] [PubMed]
- Wu, M.; Wang, S.; Weng, Q.; Chen, H.; Shen, J.; Li, Z.; Wu, Y.; Zhao, Y.; Li, M.; Wu, Y.; et al. Prenatal and postnatal exposure to Bisphenol A and Asthma: A systemic review and meta-analysis. J. Thorac. Dis. 2021, 13, 1684–1696. [Google Scholar] [CrossRef] [PubMed]
- Midoro-Horiuti, T.; Tiwari, R.; Watson, C.S.; Goldblum, R.M. Maternal bisphenol a exposure promotes the development of experimental asthma in mouse pups. Environ. Health Perspect. 2010, 118, 273–277. [Google Scholar] [CrossRef]
- Foundation, E.L. Exposure to BPA in the Womb Linked to Wheezing and Poorer Lung Function in Children. Available online: https://www.sciencedaily.com/releases/2019/10/191001094205.htm#:~:text=2-,Exposure%20to%20BPA%20in%20the%20womb%20linked%20to,poorer%20lung%20function%20in%20children&text=Summary%3A,function%2C%20according%20to%20new%20research.%20Accessed%20on%202.4.2022 (accessed on 2 April 2022).
- He, M.; Ichinose, T.; Yoshida, S.; Takano, H.; Nishikawa, M.; Shibamoto, T.; Sun, G. Exposure to bisphenol A enhanced lung eosinophilia in adult male mice. Allergy Asthma Clin. Immunol. Off. J. Can. Soc. Allergy Clin. Immunol. 2016, 12, 16. [Google Scholar] [CrossRef]
- Gu, J.; Guo, M.; Yin, X.; Huang, C.; Qian, L.; Zhou, L.; Wang, Z.; Wang, L.; Shi, L.; Ji, G. A systematic comparison of neurotoxicity of bisphenol A and its derivatives in zebrafish. Sci. Total Environ. 2022, 805, 150210. [Google Scholar] [CrossRef]
- Tonini, C.; Segatto, M.; Gagliardi, S.; Bertoli, S.; Leone, A.; Barberio, L.; Mandalà, M.; Pallottini, V. Maternal Dietary Exposure to Low-Dose Bisphenol A Affects Metabolic and Signaling Pathways in the Brain of Rat Fetuses. Nutrients 2020, 12, 1448. [Google Scholar] [CrossRef]
- McIlwraith, E.K.; Lieu, C.V.; Belsham, D.D. Bisphenol A induces miR-708-5p through an ER stress-mediated mechanism altering neuronatin and neuropeptide Y expression in hypothalamic neuronal models. Mol. Cell. Endocrinol. 2022, 539, 111480. [Google Scholar] [CrossRef]
- Dodds, E.C.; Lawson, W. Synthetic strogenic Agents without the Phenanthrene Nucleus. Nature 1936, 137, 996. [Google Scholar] [CrossRef]
- Kuiper, G.G.; Carlsson, B.; Grandien, K.; Enmark, E.; Häggblad, J.; Nilsson, S.; Gustafsson, J.A. Comparison of the ligand binding specificity and transcript tissue distribution of estrogen receptors alpha and beta. Endocrinology 1997, 138, 863–870. [Google Scholar] [CrossRef] [PubMed]
- Mileva, G.; Baker, S.L.; Konkle, A.T.; Bielajew, C. Bisphenol-A: Epigenetic reprogramming and effects on reproduction and behavior. Int. J. Environ. Res. Public Health 2014, 11, 7537–7561. [Google Scholar] [CrossRef] [PubMed]
- Thomas, P.; Dong, J. Binding and activation of the seven-transmembrane estrogen receptor GPR30 by environmental estrogens: A potential novel mechanism of endocrine disruption. J. Steroid Biochem. Mol. Biol. 2006, 102, 175–179. [Google Scholar] [CrossRef] [PubMed]
- Watson, C.S.; Bulayeva, N.N.; Wozniak, A.L.; Alyea, R.A. Xenoestrogens are potent activators of nongenomic estrogenic responses. Steroids 2007, 72, 124–134. [Google Scholar] [CrossRef] [PubMed]
- Qie, Y.; Qin, W.; Zhao, K.; Liu, C.; Zhao, L.; Guo, L.H. Environmental Estrogens and Their Biological Effects through GPER Mediated Signal Pathways. Environ. Pollut. 2021, 278, 116826. [Google Scholar] [CrossRef]
- Carmeci, C.; Thompson, D.A.; Ring, H.Z.; Francke, U.; Weigel, R.J. Identification of a gene (GPR30) with homology to the G-protein-coupled receptor superfamily associated with estrogen receptor expression in breast cancer. Genomics 1997, 45, 607–617. [Google Scholar] [CrossRef]
- Wang, H.; Ding, Z.; Shi, Q.M.; Ge, X.; Wang, H.X.; Li, M.X.; Chen, G.; Wang, Q.; Ju, Q.; Zhang, J.P.; et al. Anti-androgenic mechanisms of Bisphenol A involve androgen receptor signaling pathway. Toxicology 2017, 387, 10–16. [Google Scholar] [CrossRef]
- Matsushima, A.; Liu, X.; Okada, H.; Shimohigashi, M.; Shimohigashi, Y. Bisphenol AF is a full agonist for the estrogen receptor ERalpha but a highly specific antagonist for ERbeta. Environ. Health Perspect. 2010, 118, 1267–1272. [Google Scholar] [CrossRef]
- Takeda, Y.; Liu, X.; Sumiyoshi, M.; Matsushima, A.; Shimohigashi, M.; Shimohigashi, Y. Placenta expressing the greatest quantity of bisphenol A receptor ERR{gamma} among the human reproductive tissues: Predominant expression of type-1 ERRgamma isoform. J. Biochem. 2009, 146, 113–122. [Google Scholar] [CrossRef]
- Sun, H.; Xu, L.C.; Chen, J.F.; Song, L.; Wang, X.R. Effect of bisphenol A, tetrachlorobisphenol A and pentachlorophenol on the transcriptional activities of androgen receptor-mediated reporter gene. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2006, 44, 1916–1921. [Google Scholar] [CrossRef]
- Teng, C.; Goodwin, B.; Shockley, K.; Xia, M.; Huang, R.; Norris, J.; Merrick, B.A.; Jetten, A.M.; Austin, C.P.; Tice, R.R. Bisphenol A affects androgen receptor function via multiple mechanisms. Chem.-Biol. Interact. 2013, 203, 556–564. [Google Scholar] [CrossRef]
- Moriyama, K.; Tagami, T.; Akamizu, T.; Usui, T.; Saijo, M.; Kanamoto, N.; Hataya, Y.; Shimatsu, A.; Kuzuya, H.; Nakao, K. Thyroid hormone action is disrupted by bisphenol A as an antagonist. J. Clin. Endocrinol. Metab. 2002, 87, 5185–5190. [Google Scholar] [CrossRef]
- Prasanth, G.K.; Divya, L.M.; Sadasivan, C. Bisphenol-A can bind to human glucocorticoid receptor as an agonist: An in silico study. J. Appl. Toxicol. JAT 2010, 30, 769–774. [Google Scholar] [CrossRef]
- Chen, F.; Zhou, L.; Bai, Y.; Zhou, R.; Chen, L. Sex differences in the adult HPA axis and affective behaviors are altered by perinatal exposure to a low dose of bisphenol A. Brain Res. 2014, 1571, 12–24. [Google Scholar] [CrossRef]
- Pfeifer, D.; Chung, Y.M.; Hu, M.C. Effects of Low-Dose Bisphenol A on DNA Damage and Proliferation of Breast Cells: The Role of c-Myc. Environ. Health Perspect. 2015, 123, 1271–1279. [Google Scholar] [CrossRef]
- Kim, S.; Mun, G.I.; Choi, E.; Kim, M.; Jeong, J.S.; Kang, K.W.; Jee, S.; Lim, K.M.; Lee, Y.S. Submicromolar bisphenol A induces proliferation and DNA damage in human hepatocyte cell lines in vitro and in juvenile rats in vivo. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2018, 111, 125–132. [Google Scholar] [CrossRef]
- Ramos, C.; Ladeira, C.; Zeferino, S.; Dias, A.; Faria, I.; Cristovam, E.; Gomes, M.; Ribeiro, E. Cytotoxic and genotoxic effects of environmental relevant concentrations of bisphenol A and interactions with doxorubicin. Mutat. Res. Genet. Toxicol. Environ. Mutagenesis 2019, 838, 28–36. [Google Scholar] [CrossRef]
- Olukole, S.G.; Lanipekun, D.O.; Ola-Davies, E.O.; Oke, B.O. Melatonin attenuates bisphenol A-induced toxicity of the adrenal gland of Wistar rats. Environ. Sci. Pollut. Res. Int. 2019, 26, 5971–5982. [Google Scholar] [CrossRef]
- Ma, L.; Hu, J.; Li, J.; Yang, Y.; Zhang, L.; Zou, L.; Gao, R.; Peng, C.; Wang, Y.; Luo, T.; et al. Bisphenol A promotes hyperuricemia via activating xanthine oxidase. FASEB J. Off. Publ. Fed. Am. Soc. Exp. Biol. 2018, 32, 1007–1016. [Google Scholar] [CrossRef]
- Lee, H.S.; Park, Y. Identification of metabolic pathways related to the bisphenol A-induced adipogenesis in differentiated murine adipocytes by using RNA-sequencing. Environ. Res. 2019, 171, 161–169. [Google Scholar] [CrossRef]
- Zbucka-Kretowska, M.; Zbucki, R.; Parfieniuk, E.; Maslyk, M.; Lazarek, U.; Miltyk, W.; Czerniecki, J.; Wolczynski, S.; Kretowski, A.; Ciborowski, M. Evaluation of Bisphenol A influence on endocannabinoid system in pregnant women. Chemosphere 2018, 203, 387–392. [Google Scholar] [CrossRef]
- Onuzulu, C.D.; Rotimi, O.A.; Rotimi, S.O. Epigenetic modifications associated with in utero exposure to endocrine disrupting chemicals BPA, DDT and Pb. Rev. Environ. Health 2019, 34, 309–325. [Google Scholar] [CrossRef]
- Sirasanagandla, S.R.; Al-Huseini, I.; Al Mushaiqri, M.; Al-Abri, N.; Al-Ghafri, F. Maternal resveratrol supplementation ameliorates bisphenol A-induced atherosclerotic lesions formation in adult offspring ApoE(-/-) mice. 3 Biotech 2022, 12, 36. [Google Scholar] [CrossRef]
- Sirasanagandla, S.R.; Sofin, R.G.S.; Al-Huseini, I.; Das, S. Role of Bisphenol A in Autophagy Modulation: Understanding the Molecular Concepts and Therapeutic Options. Mini Rev. Med. Chem. 2022, 22, 2513–2523. [Google Scholar] [CrossRef]
- Ishtiaq, A.; Bakhtiar, A.; Silas, E.; Saeed, J.; Ajmal, S.; Mushtaq, I.; Ali, T.; Wahedi, H.M.; Khan, W.; Khan, U.; et al. Pistacia integerrima alleviated Bisphenol A induced toxicity through Ubc13/p53 signalling. Mol. Biol. Rep. 2020, 47, 6545–6559. [Google Scholar] [CrossRef] [PubMed]
- Rana, S.; Shahzad, M.; Shabbir, A. Pistacia integerrima ameliorates airway inflammation by attenuation of TNF-α, IL-4, and IL-5 expression levels, and pulmonary edema by elevation of AQP1 and AQP5 expression levels in mouse model of ovalbumin-induced allergic asthma. Phytomedicine Int. J. Phytother. Phytopharm. 2016, 23, 838–845. [Google Scholar] [CrossRef] [PubMed]
- Bibi, Y.; Zia, M.; Qayyum, A. Review-An overview of Pistacia integerrima a medicinal plant species: Ethnobotany, biological activities and phytochemistry. Pak. J. Pharm. Sci. 2015, 28, 1009–1013. [Google Scholar] [PubMed]
- Hsu, C.N.; Lin, Y.J.; Tain, Y.L. Maternal Exposure to Bisphenol A Combined with High-Fat Diet-Induced Programmed Hypertension in Adult Male Rat Offspring: Effects of Resveratrol. Int. J. Mol. Sci. 2019, 20, 4382. [Google Scholar] [CrossRef]
- Petropoulos, G.A. Fenugreek: The Genus Trigonella; CRC Press: Boca Raton, FL, USA, 2002; Volume 1. [Google Scholar]
- Gautam, S.; Ishrat, N.; Yadav, P.; Singh, R.; Narender, T.; Srivastava, A.K. 4-Hydroxyisoleucine attenuates the inflammation-mediated insulin resistance by the activation of AMPK and suppression of SOCS-3 coimmunoprecipitation with both the IR-β subunit as well as IRS-1. Mol. Cell Biochem. 2016, 414, 95–104. [Google Scholar] [CrossRef]
- Dixit, P.; Ghaskadbi, S.; Mohan, H.; Devasagayam, T.P. Antioxidant properties of germinated fenugreek seeds. Phytother. Res. PTR 2005, 19, 977–983. [Google Scholar] [CrossRef]
- Raju, J.; Gupta, D.; Rao, A.R.; Yadava, P.K.; Baquer, N.Z. Trigonellafoenum graecum (fenugreek) seed powder improves glucose homeostasis in alloxan diabetic rat tissues by reversing the altered glycolytic, gluconeogenic and lipogenic enzymes. Mol. Cell Biochem. 2001, 224, 45–51. [Google Scholar] [CrossRef]
- Shabbeer, S.; Sobolewski, M.; Anchoori, R.K.; Kachhap, S.; Hidalgo, M.; Jimeno, A.; Davidson, N.; Carducci, M.A.; Khan, S.R. Fenugreek: A naturally occurring edible spice as an anticancer agent. Cancer Biol. Ther. 2009, 8, 272–278. [Google Scholar] [CrossRef]
- Gao, F.; Du, W.; Zafar, M.I.; Shafqat, R.A.; Jian, L.; Cai, Q.; Lu, F. 4-Hydroxyisoleucine ameliorates an insulin resistant-like state in 3T3-L1 adipocytes by regulating TACE/TIMP3 expression. Drug Des. Dev. Ther. 2015, 9, 5727–5736. [Google Scholar] [CrossRef]
- Ulbricht, C.; Basch, E.; Burke, D.; Cheung, L.; Ernst, E.; Giese, N.; Foppa, I.; Hammerness, P.; Hashmi, S.; Kuo, G.; et al. Fenugreek (Trigonella foenum-graecum L. Leguminosae): An evidence-based systematic review by the natural standard research collaboration. J. Herb. Pharmacother. 2007, 7, 143–177. [Google Scholar] [CrossRef]
- Doshi, M.; Mirza, A.; Umarji, B.; Karambelkar, R. Effect of Trigonella foenum-graecum (fenugreek/methi) on hemoglobin levels in females of child bearing age. Biomed. Res. Int. 2012, 23, 47–50. [Google Scholar]
- Chaturvedi, U.; Shrivastava, A.; Bhadauria, S.; Saxena, J.K.; Bhatia, G. A mechanism-based pharmacological evaluation of efficacy of Trigonella foenum graecum (fenugreek) seeds in regulation of dyslipidemia and oxidative stress in hyperlipidemic rats. J. Cardiovasc. Pharmacol. 2013, 61, 505–512. [Google Scholar] [CrossRef]
- Aswar, U.; Bodhankar, S.L.; Mohan, V.; Thakurdesai, P.A. Effect of furostanol glycosides from Trigonella foenum-graecum on the reproductive system of male albino rats. Phytother. Res. PTR 2010, 24, 1482–1488. [Google Scholar] [CrossRef]
- Kaur, S.; Sadwal, S. Studies on the phytomodulatory potential of fenugreek (Trigonella foenum-graecum) on bisphenol-A induced testicular damage in mice. Andrologia 2020, 52, e13492. [Google Scholar] [CrossRef]
- Dobson, A.; O’Sullivan, O.; Cotter, P.D.; Ross, P.; Hill, C. High-throughput sequence-based analysis of the bacterial composition of kefir and an associated kefir grain. FEMS Microbiol. Lett. 2011, 320, 56–62. [Google Scholar] [CrossRef]
- Bengoa, A.A.; Iraporda, C.; Garrote, G.L.; Abraham, A.G. Kefir micro-organisms: Their role in grain assembly and health properties of fermented milk. J. Appl. Microbiol. 2019, 126, 686–700. [Google Scholar] [CrossRef]
- Friques, A.G.F.; Santos, F.D.N.; Angeli, D.B.; Silva, F.A.C.; Dias, A.T.; Aires, R.; Leal, M.A.S.; Nogueira, B.V.; Amorim, F.G.; Campagnaro, B.P.; et al. Bisphenol A contamination in infant rats: Molecular, structural, and physiological cardiovascular changes and the protective role of kefir. J. Nutr. Biochem. 2020, 75, 108254. [Google Scholar] [CrossRef] [PubMed]
- Unusan, N. Proanthocyanidins in grape seeds: An updated review of their health benefits and potential uses in the food industry. J. Funct. Foods 2020, 67, 103861. [Google Scholar] [CrossRef]
- Kamran, H.; Raza, I.; Saleem, Y.; Aslam, M. Health perspectives of grape seed extract (GSE). Asian J. Allied Health Sci. 2020, 5, 88–98. [Google Scholar]
- Chu, K.O.; Chan, S.O.; Pang, C.P.; Wang, C.C. Pro-oxidative and antioxidative controls and signaling modification of polyphenolic phytochemicals: Contribution to health promotion and disease prevention? J. Agric. Food Chem. 2014, 62, 4026–4038. [Google Scholar] [CrossRef]
- Sutcliffe, T.C.; Winter, A.N.; Punessen, N.C.; Linseman, D.A. Procyanidin B2 Protects Neurons from Oxidative, Nitrosative, and Excitotoxic Stress. Antioxidants 2017, 6, 77. [Google Scholar] [CrossRef]
- Abdou, H.M.; Abd Elkader, H.A.E.; El-Gendy, A.H.; Eweda, S.M. Neurotoxicity and neuroinflammatory effects of bisphenol A in male rats: The neuroprotective role of grape seed proanthocyanidins. Environ. Sci. Pollut. Res. Int. 2022, 29, 9257–9268. [Google Scholar] [CrossRef]
- Fesharaki, M.; Nasimi, A.; Mokhtari, S.; Mokhtari, R.; Moradian, R.; Amirpoor, N. Reactive oxygen metabolites and anti-oxidative defenses in aspirin-induced gastric damage in rats: Gastroprotection by Vitamin E. Pathophysiol. Off. J. Int. Soc. Pathophysiol. 2006, 13, 237–243. [Google Scholar] [CrossRef]
- Abbas, A.M.; Sakr, H.F. Effect of selenium and grape seed extract on indomethacin-induced gastric ulcers in rats. J. Physiol. Biochem. 2013, 69, 527–537. [Google Scholar] [CrossRef]
- Rameshrad, M.; Imenshahidi, M.; Razavi, B.M.; Iranshahi, M.; Hosseinzadeh, H. Bisphenol A vascular toxicity: Protective effect of Vitis vinifera (grape) seed extract and resveratrol. Phytother. Res. PTR 2018, 32, 2396–2407. [Google Scholar] [CrossRef]
- Rameshrad, M.; Razavi, B.M.; Imenshahidi, M.; Hosseinzadeh, H. Vitis vinifera (grape) seed extract and resveratrol alleviate bisphenol-A-induced metabolic syndrome: Biochemical and molecular evidences. Phytother. Res. PTR 2019, 33, 832–844. [Google Scholar] [CrossRef]
- Corner, E.J.H. The complex of Fixcus Deltoidea; A recent invasion of the sunda shelf. Philosophical Transactions of the Royal Society of London. Biol. Sci. 1969, 256, 281–317. [Google Scholar]
- Lip, J.M.; Hisham, D.N.; Zaidi, J.A.; Musa, Y.; Ahmad, A.W.; Normah, A.; Sharizan, A. Isolation and identification of moretenol from Ficus deltoidea leaves. J. Trop. Agric. Food Sci. 2009, 37, 195–201. [Google Scholar]
- Omar, M.H.; Mullen, W.; Crozier, A. Identification of proanthocyanidin dimers and trimers, flavone C-Glycosides, and antioxidants in Ficus deltoidea, a malaysian herbal tea. J. Agric. Food Chem. 2011, 59, 1363–1369. [Google Scholar] [CrossRef]
- Ong, S.L.; Ling, A.P.K.; Poospooragi, R.; Moosa, S. Production of flavonoid compounds in cell cultures of Ficus deltoidea as influenced by medium composition. Int. J. Med. Aromat. Plants 2011, 1, 62–74. [Google Scholar]
- Suryati; Nurdin, H.; Hamidi, D.; Lajis, M. STRUCTURE ELUCIDATION OF ANTIBACTERIAL COMPOUND FROM Ficus deltoidea Jack LEAVES. Indones. J. Chem. 2011, 11, 67–70. [Google Scholar] [CrossRef]
- Bunawan, H.; Amin, N.M.; Bunawan, S.N.; Baharum, S.N.; Mohd Noor, N. Ficus deltoidea Jack: A Review on Its Phytochemical and Pharmacological Importance. Evid.-Based Complementary Altern. Med. 2014, 2014, 902734. [Google Scholar] [CrossRef]
- Zaid, S.S.M.; Othman, S.; Kassim, N.M. Protective role of Mas Cotek (Ficus deltoidea) against the toxic effects of bisphenol A on morphology and sex steroid receptor expression in the rat uterus. Biomed. Pharmacother. 2021, 140, 111757. [Google Scholar] [CrossRef]
- Zaid, S.S.M.; Othman, S.; Kassim, N.M. Protective role of Ficus deltoidea against BPA-induced impairments of the follicular development, estrous cycle, gonadotropin and sex steroid hormones level of prepubertal rats. J. Ovarian Res. 2018, 11, 99. [Google Scholar] [CrossRef]
- Sun, H.; Mu, T.; Xi, L.; Zhang, M.; Chen, J. Sweet potato (Ipomoea batatas L.) leaves as nutritional and functional foods. Food Chem. 2014, 156, 380–389. [Google Scholar] [CrossRef]
- Revathy, R.; Langeswaran, K.; Ponnulakshmi, R.; Balasubramanian, M.P.; Selvaraj, J. Ipomoea batatas Tuber Efficiency on Bisphenol A-induced Male Reproductive Toxicity in Sprague Dawley Rats. J. Biol. Act. Prod. Nat. 2017, 7, 118–130. [Google Scholar] [CrossRef]
- Johnson, M.; Pace, R.D. Sweet potato leaves: Properties and synergistic interactions that promote health and prevent disease. Nutr. Rev. 2010, 68, 604–615. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, M.; Fatima, H.; Qasim, M.; Gul, B.; Ihsan Ul, H. Polarity directed optimization of phytochemical and in vitro biological potential of an indigenous folklore: Quercus dilatata Lindl. ex Royle. BMC Complementary Altern. Med. 2017, 17, 386. [Google Scholar] [CrossRef] [PubMed]
- Taib, M.; Rezzak, Y.; Bouyazza, L.; Lyoussi, B. Medicinal Uses, Phytochemistry, and Pharmacological Activities of Quercus Species. Evid.-Based Complementary Altern. Med. 2020, 2020, 1920683. [Google Scholar] [CrossRef] [PubMed]
- Jamil, M.; ul Haq, I.; Mirza, B.; Qayyum, M. Isolation of antibacterial compounds from Quercus dilatata L. through bioassay guided fractionation. Ann. Clin. Microbiol. Antimicrob. 2012, 11, 11. [Google Scholar] [CrossRef]
- Ismail, H.; Rasheed, A.; Haq, I.U.; Jafri, L.; Ullah, N.; Dilshad, E.; Sajid, M.; Mirza, B. Five Indigenous Plants of Pakistan with Antinociceptive, Anti-Inflammatory, Antidepressant, and Anticoagulant Properties in Sprague Dawley Rats. Evid.-Based Complementary Altern. Med. 2017, 2017, 7849501. [Google Scholar] [CrossRef]
- Kazmi, S.T.B.; Majid, M.; Maryam, S.; Rahat, A.; Ahmed, M.; Khan, M.R.; Haq, I.U. Quercus dilatata Lindl. ex Royle ameliorates BPA induced hepatotoxicity in Sprague Dawley rats. Biomed. Pharmacother. 2018, 102, 728–738. [Google Scholar] [CrossRef]
- Mohamed, M.; Sirajudeen, K.; Swamy, M.; Yaacob, N.S.; Sulaiman, S.A. Studies on the antioxidant properties of Tualang honey of Malaysia. Afr. J. Tradit. Complementary Altern. Med. AJTCAM 2009, 7, 59–63. [Google Scholar] [CrossRef]
- Khalil, M.I.; Alam, N.; Moniruzzaman, M.; Sulaiman, S.A.; Gan, S.H. Phenolic acid composition and antioxidant properties of Malaysian honeys. J. Food Sci. 2011, 76, C921–C928. [Google Scholar] [CrossRef]
- Qaid, E.Y.A.; Zakaria, R.; Mohd Yusof, N.A.; Sulaiman, S.F.; Shafin, N.; Othman, Z.; Ahmad, A.H.; Abd Aziz, C.B.; Muthuraju, S. Tualang Honey Ameliorates Hypoxia-induced Memory Deficits by Reducing Neuronal Damage in the Hippocampus of Adult Male Sprague Dawley Rats. Turk. J. Pharm. Sci. 2020, 17, 555–564. [Google Scholar] [CrossRef]
- Kishore, R.K.; Halim, A.S.; Syazana, M.S.; Sirajudeen, K.N. Tualang honey has higher phenolic content and greater radical scavenging activity compared with other honey sources. Nutr. Res. 2011, 31, 322–325. [Google Scholar] [CrossRef]
- Mohamad Zaid, S.S.; Kassim, N.M.; Othman, S. Tualang Honey Protects against BPA-Induced Morphological Abnormalities and Disruption of ERα, ERβ, and C3 mRNA and Protein Expressions in the Uterus of Rats. Evid.-Based Complementary Altern. Med. 2015, 2015, 202874. [Google Scholar] [CrossRef]
- Zaid, S.S.; Othman, S.; Kassim, N.M. Potential protective effect of Tualang honey on BPA-induced ovarian toxicity in prepubertal rat. BMC Complementary Altern. Med. 2014, 14, 509. [Google Scholar] [CrossRef]
- Mahendra Kumar, C.; Singh, S.A. Bioactive lignans from sesame (Sesamum indicum L.): Evaluation of their antioxidant and antibacterial effects for food applications. J. Food Sci. Technol. 2015, 52, 2934–2941. [Google Scholar] [CrossRef]
- Wan, Y.; Li, H.; Fu, G.; Chen, X.; Chen, F.; Xie, M. The relationship of antioxidant components and antioxidant activity of sesame seed oil. J. Sci. Food Agric. 2015, 95, 2571–2578. [Google Scholar] [CrossRef]
- Dar, A.A.; Arumugam, N. Lignans of sesame: Purification methods, biological activities and biosynthesis—A review. Bioorganic Chem. 2013, 50, 1–10. [Google Scholar] [CrossRef]
- Eweda, S.M.; Newairy, A.S.A.; Abdou, H.M.; Gaber, A.S. Bisphenol A-induced oxidative damage in the hepatic and cardiac tissues of rats: The modulatory role of sesame lignans. Exp. Ther. Med. 2020, 19, 33–44. [Google Scholar] [CrossRef]
- Abo El Wafa, S. The protective role of sesame oil against bisphenol A-induced cardiotoxicity: A histological and immunohistochemical study. Kasr Al Ainy Med. J. 2020, 25, 87–98. [Google Scholar]
- Wagh, V.D. Propolis: A wonder bees product and its pharmacological potentials. Adv. Pharmacol. Sci. 2013, 2013, 308249. [Google Scholar] [CrossRef]
- Burdock, G.A. Review of the biological properties and toxicity of bee propolis (propolis). Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 1998, 36, 347–363. [Google Scholar] [CrossRef]
- Farooqui, T.; Farooqui, A.A. Beneficial effects of propolis on human health and neurological diseases. Front. Biosci. 2012, 4, 779–793. [Google Scholar] [CrossRef]
- Pasupuleti, V.R.; Sammugam, L.; Ramesh, N.; Gan, S.H. Honey, Propolis, and Royal Jelly: A Comprehensive Review of Their Biological Actions and Health Benefits. Oxid. Med. Cell Longev. 2017, 2017, 1259510. [Google Scholar] [CrossRef] [PubMed]
- Hamed, H.S.; Abdel-Tawwab, M. Ameliorative effect of propolis supplementation on alleviating bisphenol-A toxicity: Growth performance, biochemical variables, and oxidative stress biomarkers of Nile tilapia, Oreochromis niloticus (L.) fingerlings. Comp. Biochem. Physiology. Toxicol. Pharmacol. CBP 2017, 202, 63–69. [Google Scholar] [CrossRef] [PubMed]
- Soliman, M.A.E.; Noya, D.A.E. Effect of Bisphenol A on the lung of adult male albino rats and the possible protective role of propolis: Light and electron microscopic study. Egypt. J. Histol. 2021. [Google Scholar] [CrossRef]
- Hannan, M.A.; Rahman, M.A.; Sohag, A.A.M.; Uddin, M.J.; Dash, R.; Sikder, M.H.; Rahman, M.S.; Timalsina, B.; Munni, Y.A.; Sarker, P.P.; et al. Black Cumin (Nigella sativa L.): A Comprehensive Review on Phytochemistry, Health Benefits, Molecular Pharmacology, and Safety. Nutrients 2021, 13, 1784. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, A.; Husain, A.; Mujeeb, M.; Khan, S.A.; Najmi, A.K.; Siddique, N.A.; Damanhouri, Z.A.; Anwar, F. A review on therapeutic potential of Nigella sativa: A miracle herb. Asian Pac. J. Trop. Biomed. 2013, 3, 337–352. [Google Scholar] [CrossRef]
- Kooti, W.; Hasanzadeh-Noohi, Z.; Sharafi-Ahvazi, N.; Asadi-Samani, M.; Ashtary-Larky, D. Phytochemistry, pharmacology, and therapeutic uses of black seed (Nigella sativa). Chin. J. Nat. Med. 2016, 14, 732–745. [Google Scholar] [CrossRef]
- Sujan, K.; Haque, E.; Rakib, M.; Haque, M.; Mustari, A.; Miah, M.; Islam, M. Effects of Bisphenol-A (BPA) and black seed oil on body weight, lipid profile and serum glucose in male and female mice. Bangladesh J. Vet. Med. 2019, 17, 77–82. [Google Scholar] [CrossRef][Green Version]
- Sujan, K.M.; Hoque, E.; Haque, M.I.; Mustari, A.; Miah, M.A.; Islam, M.K. Ameliorating Effects of Black Seed Oil on Bisphenol-A Induced Abnormality of Blood, Hormone Profile and Gonadal Histology of Female Mice. J. Adv. Biotechnol. Exp. Ther. 2020, 3, 43–48. [Google Scholar] [CrossRef]
- Fadishei, M.; Ghasemzadeh Rahbardar, M.; Imenshahidi, M.; Mohajeri, A.; Razavi, B.M.; Hosseinzadeh, H. Effects of Nigella sativa oil and thymoquinone against bisphenol A-induced metabolic disorder in rats. Phytother. Res. PTR 2021, 35, 2005–2024. [Google Scholar] [CrossRef]
- Abdel-Wahab, W.M. Thymoquinone attenuates toxicity and oxidative stress induced by bisphenol A in liver of male rats. Pak. J. Biol. Sci. 2014, 17, 1152–1160. [Google Scholar] [CrossRef][Green Version]
- Cabrera, C.; Artacho, R.; Giménez, R. Beneficial effects of green tea—A review. J. Am. Coll. Nutr. 2006, 25, 79–99. [Google Scholar] [CrossRef]
- Chacko, S.M.; Thambi, P.T.; Kuttan, R.; Nishigaki, I. Beneficial effects of green tea: A literature review. Chin. Med. 2010, 5, 13. [Google Scholar] [CrossRef]
- Ohishi, T.; Goto, S.; Monira, P.; Isemura, M.; Nakamura, Y. Anti-inflammatory Action of Green Tea. Anti-Inflamm. Anti-Allergy Agents Med. Chem. 2016, 15, 74–90. [Google Scholar] [CrossRef]
- Chatterjee, P.; Chandra, S.; Dey, P.; Bhattacharya, S. Evaluation of anti-inflammatory effects of green tea and black tea: A comparative in vitro study. J. Adv. Pharm. Technol. Res. 2012, 3, 136–138. [Google Scholar] [CrossRef]
- Maiti, S.; Nazmeen, A.; Medda, N.; Patra, R.; Ghosh, T.K. Flavonoids green tea against oxidant stress and inflammation with related human diseases. Clin. Nutr. Exp. 2019, 24, 1–14. [Google Scholar] [CrossRef]
- Tallei, T.E.; Fatimawali; Niode, N.J.; Idroes, R.; Zidan, B.; Mitra, S.; Celik, I.; Nainu, F.; Ağagündüz, D.; Emran, T.B.; et al. A Comprehensive Review of the Potential Use of Green Tea Polyphenols in the Management of COVID-19. Evid.-Based Complementary Altern. Med. 2021, 2021, 7170736. [Google Scholar] [CrossRef]
- Mohsenzadeh, M.S.; Razavi, B.M.; Imenshahidi, M.; Mohajeri, S.A.; Rameshrad, M.; Hosseinzadeh, H. Evaluation of green tea extract and epigallocatechin gallate effects on bisphenol A-induced vascular toxicity in isolated rat aorta and cytotoxicity in human umbilical vein endothelial cells. Phytother. Res. PTR 2021, 35, 996–1009. [Google Scholar] [CrossRef]
- Mohsenzadeh, M.S.; Razavi, B.M.; Imenshahidi, M.; Tabatabaee Yazdi, S.A.; Mohajeri, S.A.; Hosseinzadeh, H. Potential role of green tea extract and epigallocatechin gallate in preventing bisphenol A-induced metabolic disorders in rats: Biochemical and molecular evidence. Phytomedicine Int. J. Phytother. Phytopharm. 2021, 92, 153754. [Google Scholar] [CrossRef]
- Suthar, H.; Verma, R.J.; Patel, S.; Jasrai, Y.T. Green tea potentially ameliorates bisphenol a-induced oxidative stress: An in vitro and in silico study. Biochem. Res. Int. 2014, 2014, 259763. [Google Scholar] [CrossRef]
- Chatterjee, C.; Gleddie, S.; Xiao, C.W. Soybean Bioactive Peptides and Their Functional Properties. Nutrients 2018, 10, 1211. [Google Scholar] [CrossRef]
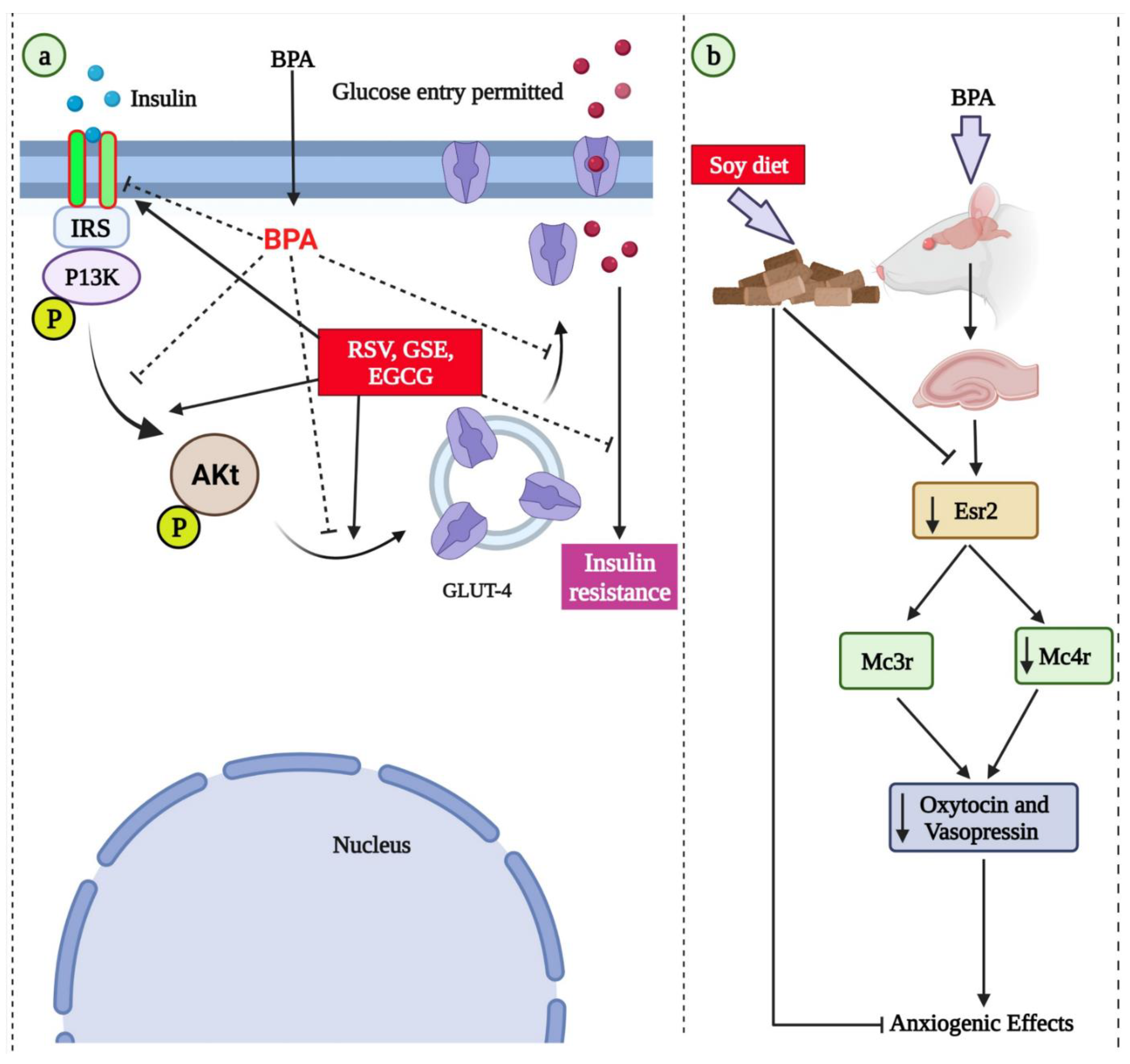
- Veissi, M.; Jafarirad, S.; Ahangarpour, A.; Mohaghegh, S.M.; Malehi, A.S. Co-exposure to endocrine disruptors: Effect of bisphenol A and soy extract on glucose homeostasis and related metabolic disorders in male mice. Endocr. Regul. 2018, 52, 76–84. [Google Scholar] [CrossRef]
- Patisaul, H.B.; Sullivan, A.W.; Radford, M.E.; Walker, D.M.; Adewale, H.B.; Winnik, B.; Coughlin, J.L.; Buckley, B.; Gore, A.C. Anxiogenic effects of developmental bisphenol A exposure are associated with gene expression changes in the juvenile rat amygdala and mitigated by soy. PLoS ONE 2012, 7, e43890. [Google Scholar] [CrossRef]
- Procida, G.; Stancher, B.; Cateni, F.; Zacchigna, M. Chemical composition and functional characterisation of commercial pumpkin seed oil. J. Sci. Food Agric. 2013, 93, 1035–1041. [Google Scholar] [CrossRef]
- Shahidi, F.; de Camargo, A.C. Tocopherols and Tocotrienols in Common and Emerging Dietary Sources: Occurrence, Applications, and Health Benefits. Int. J. Mol. Sci. 2016, 17, 1745. [Google Scholar] [CrossRef]
- Fawzy, E.I.; El Makawy, A.I.; El-Bamby, M.M.; Elhamalawy, H.O. Improved effect of pumpkin seed oil against the bisphenol-A adverse effects in male mice. Toxicol. Rep. 2018, 5, 857–863. [Google Scholar] [CrossRef]
- Jahanshahi, M.; Nickmahzar, E.G.; Babakordi, F. Effect of Gingko biloba extract on scopolamine-induced apoptosis in the hippocampus of rats. Anat. Sci. Int. 2013, 88, 217–222. [Google Scholar] [CrossRef]
- Wu, Y.; Sun, J.; George, J.; Ye, H.; Cui, Z.; Li, Z.; Liu, Q.; Zhang, Y.; Ge, D.; Liu, Y. Study of neuroprotective function of Ginkgo biloba extract (EGb761) derived-flavonoid monomers using a three-dimensional stem cell-derived neural model. Biotechnol. Prog. 2016, 32, 735–744. [Google Scholar] [CrossRef]
- Kleijnen, J.; Knipschild, P. Ginkgo biloba for cerebral insufficiency. Br. J. Clin. Pharmacol. 1992, 34, 352–358. [Google Scholar] [CrossRef] [PubMed]
- Dias, M.C.; Furtado, K.S.; Rodrigues, M.A.; Barbisan, L.F. Effects of Ginkgo biloba on chemically-induced mammary tumors in rats receiving tamoxifen. BMC Complementary Altern. Med. 2013, 13, 93. [Google Scholar] [CrossRef] [PubMed]
- Yallapragada, P.R.; Velaga, M.K. Effect of Ginkgo biloba Extract on Lead-Induced Oxidative Stress in Different Regions of Rat Brain. J. Environ. Pathol. Toxicol. Oncol. Off. Organ Int. Soc. Environ. Toxicol. Cancer 2015, 34, 161–173. [Google Scholar] [CrossRef] [PubMed]
- Lim, S.; Yoon, J.W.; Kang, S.M.; Choi, S.H.; Cho, B.J.; Kim, M.; Park, H.S.; Cho, H.J.; Shin, H.; Kim, Y.B.; et al. EGb761, a Ginkgo biloba extract, is effective against atherosclerosis in vitro, and in a rat model of type 2 diabetes. PLoS ONE 2011, 6, e20301. [Google Scholar] [CrossRef] [PubMed]
- El Tabaa, M.M.; Sokkar, S.S.; Ramadan, E.S.; Abd El Salam, I.Z.; Zaid, A. Neuroprotective role of Ginkgo biloba against cognitive deficits associated with Bisphenol A exposure: An animal model study. Neurochem. Int. 2017, 108, 199–212. [Google Scholar] [CrossRef] [PubMed]
- So, S.H.; Lee, J.W.; Kim, Y.S.; Hyun, S.H.; Han, C.K. Red ginseng monograph. J. Ginseng Res. 2018, 42, 549–561. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.M.; Yoon, H.; Park, H.M.; Song, B.C.; Yeum, K.J. Implications of red Panax ginseng in oxidative stress associated chronic diseases. J. Ginseng Res. 2017, 41, 113–119. [Google Scholar] [CrossRef]
- Kim, K.H.; Lee, D.; Lee, H.L.; Kim, C.E.; Jung, K.; Kang, K.S. Beneficial effects of Panax ginseng for the treatment and prevention of neurodegenerative diseases: Past findings and future directions. J. Ginseng Res. 2018, 42, 239–247. [Google Scholar] [CrossRef]
- Ahuja, A.; Kim, J.H.; Kim, J.H.; Yi, Y.S.; Cho, J.Y. Functional role of ginseng-derived compounds in cancer. J. Ginseng Res. 2018, 42, 248–254. [Google Scholar] [CrossRef]
- Saba, E.; Lee, Y.Y.; Kim, M.; Kim, S.H.; Hong, S.B.; Rhee, M.H. A comparative study on immune-stimulatory and antioxidant activities of various types of ginseng extracts in murine and rodent models. J. Ginseng Res. 2018, 42, 577–584. [Google Scholar] [CrossRef]
- Song, H.; Lee, Y.Y.; Park, J.; Lee, Y. Korean Red Ginseng suppresses bisphenol A-induced expression of cyclooxygenase-2 and cellular migration of A549 human lung cancer cell through inhibition of reactive oxygen species. J. Ginseng Res. 2021, 45, 119–125. [Google Scholar] [CrossRef]
- Ok, S.; Kang, J.S.; Kim, K.M. Cultivated wild ginseng extracts upregulate the anti-apoptosis systems in cells and mice induced by bisphenol A. Mol. Cell. Toxicol. 2017, 13, 73–82. [Google Scholar] [CrossRef]
- Lee, J.; Park, J.; Lee, Y.Y.; Lee, Y. Comparative transcriptome analysis of the protective effects of Korean Red Ginseng against the influence of bisphenol A in the liver and uterus of ovariectomized mice. J. Ginseng Res. 2020, 44, 519–526. [Google Scholar] [CrossRef]
- Park, J.; Choi, K.; Lee, J.; Jung, J.M.; Lee, Y. The Effect of Korean Red Ginseng on Bisphenol A-Induced Fatty Acid Composition and Lipid Metabolism-Related Gene Expression Changes. Am. J. Chin. Med. 2020, 48, 1841–1858. [Google Scholar] [CrossRef]
- Saadeldin, I.M.; Hussein, M.A.; Suleiman, A.H.; Abohassan, M.G.; Ahmed, M.M.; Moustafa, A.A.; Moumen, A.F.; Abdel-Aziz Swelum, A. Ameliorative effect of ginseng extract on phthalate and bisphenol A reprotoxicity during pregnancy in rats. Environ. Sci. Pollut. Res. Int. 2018, 25, 21205–21215. [Google Scholar] [CrossRef]
- Balakrishnan, R.; Vijayraja, D.; Jo, S.H.; Ganesan, P.; Su-Kim, I.; Choi, D.K. Medicinal Profile, Phytochemistry, and Pharmacological Activities of Murraya koenigii and its Primary Bioactive Compounds. Antioxidants 2020, 9, 101. [Google Scholar] [CrossRef]
- Ma, Q.G.; Xu, K.; Sang, Z.P.; Wei, R.R.; Liu, W.M.; Su, Y.L.; Yang, J.B.; Wang, A.G.; Ji, T.F.; Li, L.J. Alkenes with antioxidative activities from Murraya koenigii (L.) Spreng. Bioorganic Med. Chem. Lett. 2016, 26, 799–803. [Google Scholar] [CrossRef]
- Tripathi, Y.; Anjum, N.; Rana, A. Chemical Composition and In vitro Antifungal and Antioxidant Activities of Essential Oil from Murraya koenigii (L.) Spreng. Leaves. Asian J. Biomed. Pharm. Sci. 2018, 8, 6–13. [Google Scholar] [CrossRef]
- Rautela, R.; Das, G.; Khan, F.; Prasad, S.; Kumar, A.; Prasad, J.; Ghosh, S.; Dhanze, H.; Katiyar, R.; Srivastava, S.K. Antibacterial, anti-inflammatory and antioxidant effects of Aegle marmelos and Murraya koenigii in dairy cows with endometritis. Livest. Sci. 2018, 214, 142–148. [Google Scholar] [CrossRef]
- Ningappa, M.B.; Dinesha, R.; Srinivas, L. Antioxidant and free radical scavenging activities of polyphenol-enriched curry leaf (Murraya koenigii L.) extracts. Food Chem. 2008, 106, 720–728. [Google Scholar] [CrossRef]
- Kaur, S.; Singh, G.; Sadwal, S.; Aniqa, A. Alleviating impact of hydroethanolic Murraya koenigii leaves extract on bisphenol A instigated testicular lethality and apoptosis in mice. Andrologia 2020, 52, e13504. [Google Scholar] [CrossRef]
- Huang, X.F.; Lin, Y.Y.; Kong, L.Y. Steroids from the roots of Asparagus officinalis and their cytotoxic activity. J. Integr. Plant Biol. 2008, 50, 717–722. [Google Scholar] [CrossRef]
- Schilcher, H.R.H. Nachweis der aquaretischen Wirkung von Birkenblätter- und Goldrutenkrautauszügen im Tierversuch. Urol. B 1988, 28, 274–280. [Google Scholar]
- Somania, R.; Singhai, A.K.; Shivgunde, P.; Jain, D. Asparagus racemosus Willd (Liliaceae) ameliorates early diabetic nephropathy in STZ induced diabetic rats. Indian J. Exp. Biol. 2012, 50, 469–475. [Google Scholar] [PubMed]
- Dohare, S.; Shuaib, M.; Naquvi, K. In vitro antioxidant activity of Asparagus racemose roots. Int. J. Bio. Res. 2011, 4, 228–235. [Google Scholar]
- Rajasekaran, S.; Sivagnanam, K.; Subramanian, S. Antioxidant effect of Aloe vera gel extract in streptozotocin-induced diabetes in rats. Pharmacol. Rep. PR 2005, 57, 90–96. [Google Scholar] [PubMed]
- Sánchez, M.; González-Burgos, E.; Iglesias, I.; Gómez-Serranillos, M.P. Pharmacological Update Properties of Aloe Vera and its Major Active Constituents. Molecules 2020, 25, 1324. [Google Scholar] [CrossRef] [PubMed]
- Shahraki, A.; Mojahed, A.S.; Afshar-Goli, J. The effects of hydroalcoholic extract of Aloe vera gel on spermatogenesis of adult male rats. Int. J. Biosci. 2014, 5, 158–165. [Google Scholar]
- Behmanesh, M.A.; Najafzadehvarzi, H.; Poormoosavi, S.M. Protective Effect of Aloe vera Extract against Bisphenol A Induced Testicular Toxicity in Wistar Rats. Cell J. 2018, 20, 278–283. [Google Scholar] [CrossRef] [PubMed]
- Chhatre, S.; Nesari, T.; Somani, G.; Kanchan, D.; Sathaye, S. Phytopharmacological overview of Tribulus terrestris. Pharmacogn. Rev. 2014, 8, 45–51. [Google Scholar] [CrossRef] [PubMed]
- Saied, N.M.; Darwish, S.K. A possible ameliorating effects of Tribulus terrestris on testicular dysfunction induced by xenoestrogens exposure in adult rats. Curr. Sci. Int. 2015, 4, 73–89. [Google Scholar]
- Kamenov, Z.; Fileva, S.; Kalinov, K.; Jannini, E.A. Evaluation of the efficacy and safety of Tribulus terrestris in male sexual dysfunction-A prospective, randomized, double-blind, placebo-controlled clinical trial. Maturitas 2017, 99, 20–26. [Google Scholar] [CrossRef]
- Munir, B.; Qadir, A.; Tahir, M. Negative effects of bisphenol A on testicular functions in albino rats and their abolitions with Tribulus terristeris L. Braz. J. Pharm. Sci. 2017, 53, e00104. [Google Scholar] [CrossRef]
- Renaud, S.; de Lorgeril, M. Wine, alcohol, platelets, and the French paradox for coronary heart disease. Lancet 1992, 339, 1523–1526. [Google Scholar] [CrossRef]
- Nawaz, W.; Zhou, Z.; Deng, S.; Ma, X.; Ma, X.; Li, C.; Shu, X. Therapeutic Versatility of Resveratrol Derivatives. Nutrients 2017, 9, 1188. [Google Scholar] [CrossRef]
- Li, M.; Kildegaard, K.R.; Chen, Y.; Rodriguez, A.; Borodina, I.; Nielsen, J. De novo production of resveratrol from glucose or ethanol by engineered Saccharomyces cerevisiae. Metab. Eng. 2015, 32, 1–11. [Google Scholar] [CrossRef]
- Wang, Y.; Halls, C.; Zhang, J.; Matsuno, M.; Zhang, Y.; Yu, O. Stepwise increase of resveratrol biosynthesis in yeast Saccharomyces cerevisiae by metabolic engineering. Metab. Eng. 2011, 13, 455–463. [Google Scholar] [CrossRef]
- Shih, M.K.; Tain, Y.L.; Chen, Y.W.; Hsu, W.H.; Yeh, Y.T.; Chang, S.K.C.; Liao, J.X.; Hou, C.Y. Resveratrol Butyrate Esters Inhibit Obesity Caused by Perinatal Exposure to Bisphenol A in Female Offspring Rats. Molecules 2021, 26, 4010. [Google Scholar] [CrossRef]
- Fouad, H.; Faruk, E.M.; Alasmari, W.A.; Nadwa, E.H.; Ebrahim, U.F.A. Structural and chemical role of mesenchymal stem cells and resveratrol in regulation of apoptotic -induced genes in Bisphenol-A induced uterine damage in adult female albino rats. Tissue Cell 2021, 70, 101502. [Google Scholar] [CrossRef]
- Çetin, Y.S.; Altındağ, F.; Berköz, M. Protective role of resveratrol and apigenin against toxic effects of bisphenol a in rat salivary gland. Drug Chem. Toxicol. 2021, 1–9. [Google Scholar] [CrossRef]
- Bordbar, H.; Soleymani, F.; Nadimi, E.; Yahyavi, S.S.; Fazelian-Dehkordi, K. A Quantitative Study on the Protective Effects of Resveratrol against Bisphenol A-induced Hepatotoxicity in Rats: A Stereological Study. Iran. J. Med. Sci. 2021, 46, 218–227. [Google Scholar] [CrossRef]
- Kang, N.H.; Hwang, K.A.; Lee, H.R.; Choi, D.W.; Choi, K.C. Resveratrol regulates the cell viability promoted by 17β-estradiol or bisphenol A via down-regulation of the cross-talk between estrogen receptor α and insulin growth factor-1 receptor in BG-1 ovarian cancer cells. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2013, 59, 373–379. [Google Scholar] [CrossRef]
- Çiğ, B.; Yildizhan, K. Resveratrol diminishes bisphenol A-induced oxidative stress through TRPM2 channel in the mouse kidney cortical collecting duct cells. J. Recept. Signal Transduct. Res. 2020, 40, 570–583. [Google Scholar] [CrossRef]
- Liao, J.X.; Chen, Y.W.; Shih, M.K.; Tain, Y.L.; Yeh, Y.T.; Chiu, M.H.; Chang, S.K.C.; Hou, C.Y. Resveratrol Butyrate Esters Inhibit BPA-Induced Liver Damage in Male Offspring Rats by Modulating Antioxidant Capacity and Gut Microbiota. Int. J. Mol. Sci. 2021, 22, 5273. [Google Scholar] [CrossRef]
- Golmohammadi, M.G.; Khoshdel, F.; Salimnejad, R. Protective effect of resveratrol against bisphenol A-induced reproductive toxicity in male mice. Toxin Rev. 2021, 1–9. [Google Scholar] [CrossRef]
- Rahmani Moghadam, E.; Nadimi, E.; Bordbar, A.; Ayareh, N.; Bordbar, E.; Bordbar, H. A Quantitative Study on the Protective Effect of Resveratrol against Bisphenol-A-Induced Oral Mucosa and Tongue Toxicity in Male Rats: A Stereological Study. Iran. Red Crescent Med. J. 2022, 24, e992. [Google Scholar] [CrossRef]
- Miceli, N.; Cavò, E.; Ragusa, S.; Cacciola, F.; Dugo, P.; Mondello, L.; Marino, A.; Cincotta, F.; Condurso, C.; Taviano, M.F. Phytochemical Characterization and Biological Activities of a Hydroalcoholic Extract Obtained from the Aerial Parts of Matthiola incana (L.) R.Br. subsp. incana (Brassicaceae) Growing Wild in Sicily (Italy). Chem. Biodivers. 2019, 16, e1800677. [Google Scholar] [CrossRef] [PubMed]
- Soheili, M.; Salami, M. Lavandula angustifolia biological characteristics: An in vitro study. J. Cell. Physiol. 2019, 234, 16424–16430. [Google Scholar] [CrossRef] [PubMed]
- López-Lázaro, M. Distribution and biological activities of the flavonoid luteolin. Mini Rev. Med. Chem. 2009, 9, 31–59. [Google Scholar] [CrossRef]
- Adesanoye, O.A.; Farombi, E.O. Hepatoprotective effects of Vernonia amygdalina (astereaceae) in rats treated with carbon tetrachloride. Exp. Toxicol. Pathol. Off. J. Ges. Fur Toxikol. Pathol. 2010, 62, 197–206. [Google Scholar] [CrossRef] [PubMed]
- Sun, D.W.; Zhang, H.D.; Mao, L.; Mao, C.F.; Chen, W.; Cui, M.; Ma, R.; Cao, H.X.; Jing, C.W.; Wang, Z.; et al. Luteolin Inhibits Breast Cancer Development and Progression In Vitro and In Vivo by Suppressing Notch Signaling and Regulating MiRNAs. Cell. Physiol. Biochem. 2015, 37, 1693–1711. [Google Scholar] [CrossRef]
- Zhang, B.C.; Zhang, C.W.; Wang, C.; Pan, D.F.; Xu, T.D.; Li, D.Y. Luteolin Attenuates Foam Cell Formation and Apoptosis in Ox-LDL-Stimulated Macrophages by Enhancing Autophagy. Cell. Physiol. Biochem. 2016, 39, 2065–2076. [Google Scholar] [CrossRef]
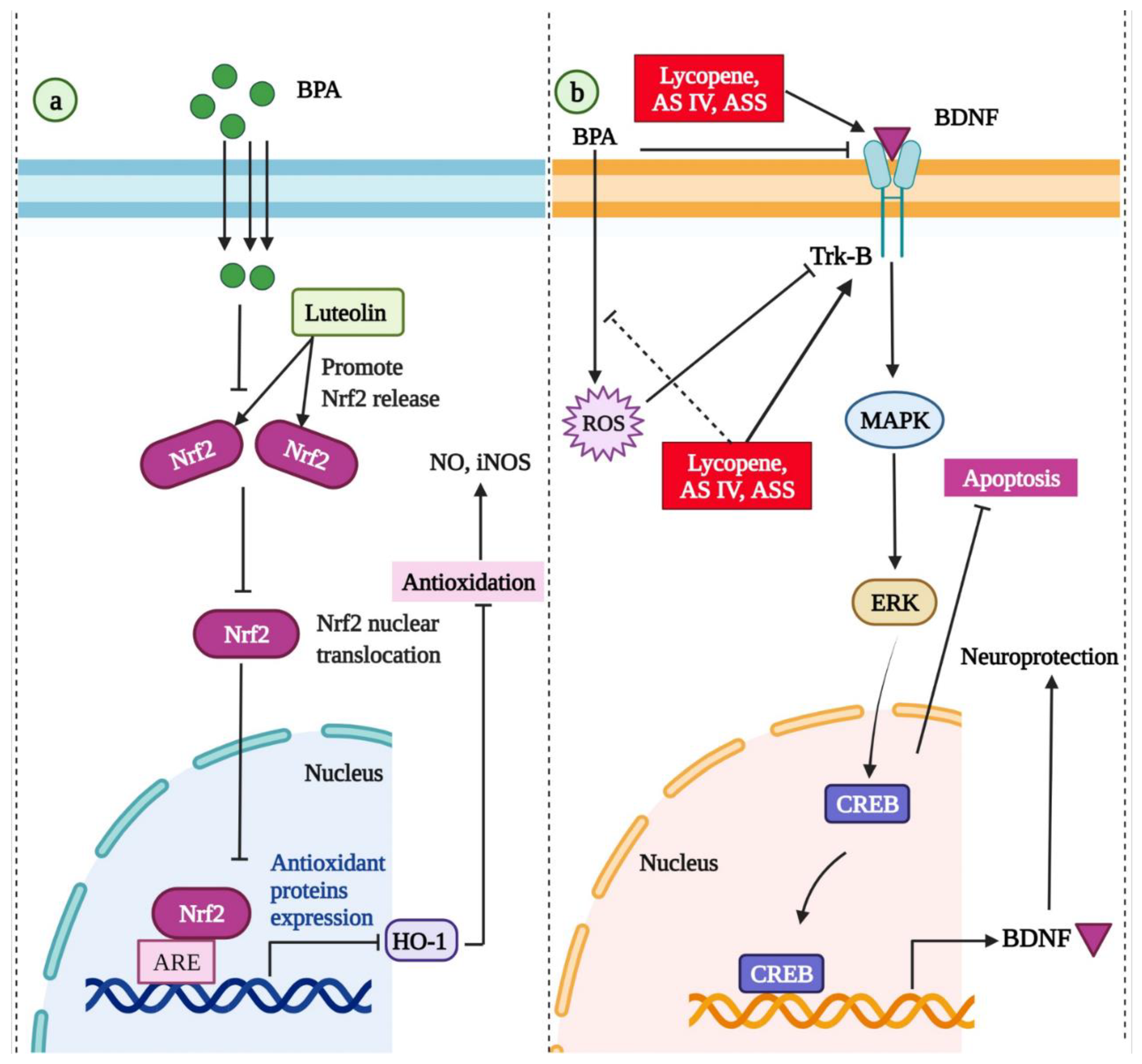
- Alekhya Sita, G.J.; Gowthami, M.; Srikanth, G.; Krishna, M.M.; Rama Sireesha, K.; Sajjarao, M.; Nagarjuna, K.; Nagarjuna, M.; Chinnaboina, G.K.; Mishra, A.; et al. Protective role of luteolin against bisphenol A-induced renal toxicity through suppressing oxidative stress, inflammation, and upregulating Nrf2/ARE/HO-1 pathway. IUBMB Life 2019, 71, 1041–1047. [Google Scholar] [CrossRef]
- Adesanoye, O.A.; Abolaji, A.O.; Faloye, T.R.; Olaoye, H.O.; Adedara, A.O. Luteolin-Supplemented diets ameliorates Bisphenol A-Induced toxicity in Drosophila melanogaster. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2020, 142, 111478. [Google Scholar] [CrossRef]
- Kong, K.W.; Khoo, H.E.; Prasad, K.N.; Ismail, A.; Tan, C.P.; Rajab, N.F. Revealing the power of the natural red pigment lycopene. Molecules 2010, 15, 959–987. [Google Scholar] [CrossRef]
- Kumar, P.; Kalonia, H.; Kumar, A. Lycopene modulates nitric oxide pathways against 3-nitropropionic acid-induced neurotoxicity. Life Sci. 2009, 85, 711–718. [Google Scholar] [CrossRef]
- Datta, S.; Jamwal, S.; Deshmukh, R.; Kumar, P. Beneficial effects of lycopene against haloperidol induced orofacial dyskinesia in rats: Possible neurotransmitters and neuroinflammation modulation. Eur. J. Pharmacol. 2016, 771, 229–235. [Google Scholar] [CrossRef]
- Palabiyik, S.S.; Erkekoglu, P.; Zeybek, N.D.; Kizilgun, M.; Baydar, D.E.; Sahin, G.; Giray, B.K. Protective effect of lycopene against ochratoxin A induced renal oxidative stress and apoptosis in rats. Exp. Toxicol. Pathol. Off. J. Ges. Fur Toxikol. Pathol. 2013, 65, 853–861. [Google Scholar] [CrossRef]
- Faheem, N.M.; El Askary, A.; Gharib, A.F. Lycopene attenuates bisphenol A-induced lung injury in adult albino rats: A histological and biochemical study. Environ. Sci. Pollut. Res. Int. 2021, 28, 49139–49152. [Google Scholar] [CrossRef]
- Abdel-Rahman, H.G.; Abdelrazek, H.M.A.; Zeidan, D.W.; Mohamed, R.M.; Abdelazim, A.M. Lycopene: Hepatoprotective and Antioxidant Effects toward Bisphenol A-Induced Toxicity in Female Wistar Rats. Oxid. Med. Cell Longev. 2018, 2018, 5167524. [Google Scholar] [CrossRef]
- Ma, S.; Li, R.; Gong, X.; Shi, W.; Zhong, X. Lycopene reduces in utero bisphenol A exposure-induced mortality, benefits hormones, and development of reproductive organs in offspring mice. Environ. Sci. Pollut. Res. Int. 2018, 25, 24041–24051. [Google Scholar] [CrossRef]
- Elgawish, R.A.; El-Beltagy, M.A.; El-Sayed, R.M.; Gaber, A.A.; Abdelrazek, H.M.A. Protective role of lycopene against metabolic disorders induced by chronic bisphenol A exposure in rats. Environ. Sci. Pollut. Res. Int. 2020, 27, 9192–9201. [Google Scholar] [CrossRef]
- El Morsy, E.M.; Ahmed, M. Protective effects of lycopene on hippocampal neurotoxicity and memory impairment induced by bisphenol A in rats. Hum. Exp. Toxicol. 2020, 39, 1066–1078. [Google Scholar] [CrossRef]
- Essawy, A.E.; Abd Elkader, H.A.E.; Khamiss, O.A.; Eweda, S.M.; Abdou, H.M. Therapeutic effects of astragaloside IV and Astragalus spinosus saponins against bisphenol A-induced neurotoxicity and DNA damage in rats. PeerJ 2021, 9, e11930. [Google Scholar] [CrossRef] [PubMed]
- Ionkova, I.; Shkondrov, A.; Krasteva, I.; Ionkov, T. Recent progress in phytochemistry, pharmacology and biotechnology of Astragalus saponins. Phytochem. Rev. 2014, 13, 343–374. [Google Scholar] [CrossRef]
- Lu, M.; Tang, F.; Zhang, J.; Luan, A.; Mei, M.; Xu, C.; Zhang, S.; Wang, H.; Maslov, L.N. Astragaloside IV attenuates injury caused by myocardial ischemia/reperfusion in rats via regulation of toll-like receptor 4/nuclear factor-κB signaling pathway. Phytother. Res. PTR 2015, 29, 599–606. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.P.; Tan, H.; Chen, B.Y.; Deng, C.Q. Combination of total Astragalus extract and total Panax notoginseng saponins strengthened the protective effects on brain damage through improving energy metabolism and inhibiting apoptosis after cerebral ischemia-reperfusion in mice. Chin. J. Integr. Med. 2017, 23, 445–452. [Google Scholar] [CrossRef]
- Yang, L.P.; Shen, J.G.; Xu, W.C.; Li, J.; Jiang, J.Q. Secondary metabolites of the genus Astragalus: Structure and biological-activity update. Chem. Biodivers. 2013, 10, 1004–1054. [Google Scholar] [CrossRef]
- Kamal, M.; Arif, D.M.; Jawaid, T. Adaptogenic medicinal plants utilized for strengthening the power of resistance during chemotherapy—A review. Orient. Pharm. Exp. Med. 2017, 17, 1–18. [Google Scholar] [CrossRef]
- Abd Elkader, H.A.E.; Abdou, H.M.; Khamiss, O.A.; Essawy, A.E. Anti-anxiety and antidepressant-like effects of astragaloside IV and saponins extracted from Astragalus spinosus against the bisphenol A-induced motor and cognitive impairments in a postnatal rat model of schizophrenia. Environ. Sci. Pollut. Res. Int. 2021, 28, 35171–35187. [Google Scholar] [CrossRef]
- Podder, B.; Song, H.Y.; Kim, Y.S. Naringenin exerts cytoprotective effect against paraquat-induced toxicity in human bronchial epithelial BEAS-2B cells through NRF2 activation. J. Microbiol. Biotechnol. 2014, 24, 605–613. [Google Scholar] [CrossRef]
- Joshi, R.; Kulkarni, Y.A.; Wairkar, S. Pharmacokinetic, pharmacodynamic and formulations aspects of Naringenin: An update. Life Sci. 2018, 215, 43–56. [Google Scholar] [CrossRef]
- Rivoira, M.A.; Rodriguez, V.; Talamoni, G.; Tolosa de Talamoni, N. New Perspectives in the Pharmacological Potential of Naringin in Medicine. Curr. Med. Chem. 2021, 28, 1987–2007. [Google Scholar] [CrossRef]
- Khodayar, M.J.; Kalantari, H.; Mahdavinia, M.; Khorsandi, L.; Alboghobeish, S.; Samimi, A.; Alizadeh, S.; Zeidooni, L. Protective effect of naringin against BPA-induced cardiotoxicity through prevention of oxidative stress in male Wistar rats. Drug Chem. Toxicol. 2020, 43, 85–95. [Google Scholar] [CrossRef]
- Mahdavinia, M.; Ahangarpour, A.; Zeidooni, L.; Samimi, A.; Alizadeh, S.; Dehghani, M.A.; Alboghobeish, S. Protective Effect of Naringin on Bisphenol A-Induced Cognitive Dysfunction and Oxidative Damage in Rats. Int. J. Mol. Cell. Med. 2019, 8, 141–153. [Google Scholar] [CrossRef]
- De Luca, A.; Pierno, S.; Camerino, D.C. Taurine: The appeal of a safe amino acid for skeletal muscle disorders. J. Transl. Med. 2015, 13, 243. [Google Scholar] [CrossRef]
- Sarkar, P.; Basak, P.; Ghosh, S.; Kundu, M.; Sil, P.C. Prophylactic role of taurine and its derivatives against diabetes mellitus and its related complications. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2017, 110, 109–121. [Google Scholar] [CrossRef]
- Abdel-Moneim, A.M.; Al-Kahtani, M.A.; El-Kersh, M.A.; Al-Omair, M.A. Free Radical-Scavenging, Anti-Inflammatory/Anti-Fibrotic and Hepatoprotective Actions of Taurine and Silymarin against CCl4 Induced Rat Liver Damage. PLoS ONE 2015, 10, e0144509. [Google Scholar] [CrossRef]
- Rashid, K.; Das, J.; Sil, P.C. Taurine ameliorate alloxan induced oxidative stress and intrinsic apoptotic pathway in the hepatic tissue of diabetic rats. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2013, 51, 317–329. [Google Scholar] [CrossRef]
- Yang, J.; Zong, X.; Wu, G.; Lin, S.; Feng, Y.; Hu, J. Taurine increases testicular function in aged rats by inhibiting oxidative stress and apoptosis. Amino Acids 2015, 47, 1549–1558. [Google Scholar] [CrossRef]
- Rezaee-Tazangi, F.; Zeidooni, L.; Rafiee, Z.; Fakhredini, F.; Kalantari, H.; Alidadi, H.; Khorsandi, L. Taurine effects on Bisphenol A-induced oxidative stress in the mouse testicular mitochondria and sperm motility. JBRA Assist. Reprod. 2020, 24, 428–435. [Google Scholar] [CrossRef]
- Pradhan, L.K.; Sahoo, P.K.; Aparna, S.; Sargam, M.; Biswal, A.K.; Polai, O.; Chauhan, N.R.; Das, S.K. Suppression of bisphenol A-induced oxidative stress by taurine promotes neuroprotection and restores altered neurobehavioral response in zebrafish (Danio rerio). Environ. Toxicol. 2021, 36, 2342–2353. [Google Scholar] [CrossRef]
- Fraga, C.G.; Galleano, M.; Verstraeten, S.V.; Oteiza, P.I. Basic biochemical mechanisms behind the health benefits of polyphenols. Mol. Asp. Med. 2010, 31, 435–445. [Google Scholar] [CrossRef]
- Zou, W.; Liu, W.; Yang, B.; Wu, L.; Yang, J.; Zou, T.; Liu, F.; Xia, L.; Zhang, D. Quercetin protects against perfluorooctanoic acid-induced liver injury by attenuating oxidative stress and inflammatory response in mice. Int. Immunopharmacol. 2015, 28, 129–135. [Google Scholar] [CrossRef] [PubMed]
- Erden Inal, M.; Kahraman, A. The protective effect of flavonol quercetin against ultraviolet a induced oxidative stress in rats. Toxicology 2000, 154, 21–29. [Google Scholar] [CrossRef]
- Shirani, M.; Alizadeh, S.; Mahdavinia, M.; Dehghani, M.A. The ameliorative effect of quercetin on bisphenol A-induced toxicity in mitochondria isolated from rats. Environ. Sci. Pollut. Res. Int. 2019, 26, 7688–7696. [Google Scholar] [CrossRef] [PubMed]
- Jahan, S.; Ain, Q.U.; Ullah, H. Therapeutic effects of quercetin against bisphenol A induced testicular damage in male Sprague Dawley rats. Syst. Biol. Reprod. Med. 2016, 62, 114–124. [Google Scholar] [CrossRef]
- Sahoo, P.K.; Pradhan, L.K.; Aparna, S.; Agarwal, K.; Banerjee, A.; Das, S.K. Quercetin abrogates bisphenol A induced altered neurobehavioral response and oxidative stress in zebrafish by modulating brain antioxidant defence system. Environ. Toxicol. Pharmacol. 2020, 80, 103483. [Google Scholar] [CrossRef] [PubMed]
- Sangai, N.P.; Patel, C.N.; Pandya, H.A. Ameliorative effects of quercetin against bisphenol A-caused oxidative stress in human erythrocytes: An in vitro and in silico study. Toxicol. Res. 2018, 7, 1091–1099. [Google Scholar] [CrossRef] [PubMed]
- Sangai, N.P.; Verma, R.J.; Trivedi, M.H. Testing the efficacy of quercetin in mitigating bisphenol A toxicity in liver and kidney of mice. Toxicol. Ind. Health 2014, 30, 581–597. [Google Scholar] [CrossRef] [PubMed]
- Coughlin, J.L.; Thomas, P.E.; Buckley, B. Inhibition of genistein glucuronidation by bisphenol A in human and rat liver microsomes. Drug Metab. Dispos. Biol. Fate Chem. 2012, 40, 481–485. [Google Scholar] [CrossRef]
- Sharifi-Rad, J.; Quispe, C.; Imran, M.; Rauf, A.; Nadeem, M.; Gondal, T.A.; Ahmad, B.; Atif, M.; Mubarak, M.S.; Sytar, O.; et al. Genistein: An Integrative Overview of Its Mode of Action, Pharmacological Properties, and Health Benefits. Oxidative Med. Cell. Longev. 2021, 2021, 3268136. [Google Scholar] [CrossRef]
- Bernardo, B.D.; Brandt, J.Z.; Grassi, T.F.; Silveira, L.T.; Scarano, W.R.; Barbisan, L.F. Genistein reduces the noxious effects of in utero bisphenol A exposure on the rat prostate gland at weaning and in adulthood. Food Chem. Toxicol. Int. J. Publ. Br. Ind. Biol. Res. Assoc. 2015, 84, 64–73. [Google Scholar] [CrossRef]
- Yakimchuk, K.; Bangalore Revanna, C.; Huang, D.; Inzunza, J.; Okret, S. Suppression of lymphoma growth by the xenoestrogens bisphenol A and genistein. Endocr. Connect. 2018, 7, 1472–1479. [Google Scholar] [CrossRef]
- Betancourt, A.; Mobley, J.A.; Wang, J.; Jenkins, S.; Chen, D.; Kojima, K.; Russo, J.; Lamartiniere, C.A. Alterations in the rat serum proteome induced by prepubertal exposure to bisphenol a and genistein. J. Proteome Res. 2014, 13, 1502–1514. [Google Scholar] [CrossRef]
- Priyadarsini, K.I. The chemistry of curcumin: From extraction to therapeutic agent. Molecules 2014, 19, 20091–20112. [Google Scholar] [CrossRef]
- Gupta, S.C.; Sung, B.; Kim, J.H.; Prasad, S.; Li, S.; Aggarwal, B.B. Multitargeting by turmeric, the golden spice: From kitchen to clinic. Mol. Nutr. Food Res. 2013, 57, 1510–1528. [Google Scholar] [CrossRef]
- Yu, C.; Mei, X.T.; Zheng, Y.P.; Xu, D.H. Zn(II)-curcumin protects against hemorheological alterations, oxidative stress and liver injury in a rat model of acute alcoholism. Environ. Toxicol. Pharmacol. 2014, 37, 729–737. [Google Scholar] [CrossRef]
- Sankar, P.; Gopal Telang, A.; Kalaivanan, R.; Karunakaran, V.; Manikam, K.; Sarkar, S.N. Effects of nanoparticle-encapsulated curcumin on arsenic-induced liver toxicity in rats. Environ. Toxicol. 2015, 30, 628–637. [Google Scholar] [CrossRef] [PubMed]
- Benzer, F.; Kandemir, F.M.; Kucukler, S.; Comaklı, S.; Caglayan, C. Chemoprotective effects of curcumin on doxorubicin-induced nephrotoxicity in wistar rats: By modulating inflammatory cytokines, apoptosis, oxidative stress and oxidative DNA damage. Arch. Physiol. Biochem. 2018, 124, 448–457. [Google Scholar] [CrossRef] [PubMed]
- Uzunhisarcikli, M.; Aslanturk, A. Hepatoprotective effects of curcumin and taurine against bisphenol A-induced liver injury in rats. Environ. Sci. Pollut. Res. Int. 2019, 26, 37242–37253. [Google Scholar] [CrossRef]
- Panpatil, V.V.; Kumari, D.; Chatterjee, A.; Kumar, S.; Bhaskar, V.; Polasa, K.; Ghosh, S. Protective Effect of Turmeric against Bisphenol-A Induced Genotoxicity in Rats. J. Nutr. Sci. Vitaminol. 2020, 66, S336–S342. [Google Scholar] [CrossRef] [PubMed]
- Apaydin, F.G.; Aslanturk, A.; Uzunhisarcikli, M.; Bas, H.; Kalender, S.; Kalender, Y. Histopathological and biochemical studies on the effect of curcumin and taurine against bisphenol A toxicity in male rats. Environ. Sci. Pollut. Res. Int. 2019, 26, 12302–12310. [Google Scholar] [CrossRef] [PubMed]
- Kalender, S.; Apaydin, F.G.; Kalender, Y. Testicular toxicity of orally administrated bisphenol A in rats and protective role of taurine and curcumin. Pak. J. Pharm. Sci. 2019, 32, 1043–1047. [Google Scholar]
- Newman, D.J. Are Microbial Endophytes the ’Actual’ Producers of Bioactive Antitumor Agents? Trends Cancer 2018, 4, 662–670. [Google Scholar] [CrossRef]
- Tintore, M.; Vidal-Jordana, A.; Sastre-Garriga, J. Treatment of multiple sclerosis-success from bench to bedside. Nat. Rev. Neurol. 2019, 15, 53–58. [Google Scholar] [CrossRef]
- Yang, Y.; Wei, S.; Zhang, B.; Li, W. Recent Progress in Environmental Toxins-Induced Cardiotoxicity and Protective Potential of Natural Products. Front. Pharmacol. 2021, 12, 699193. [Google Scholar] [CrossRef]
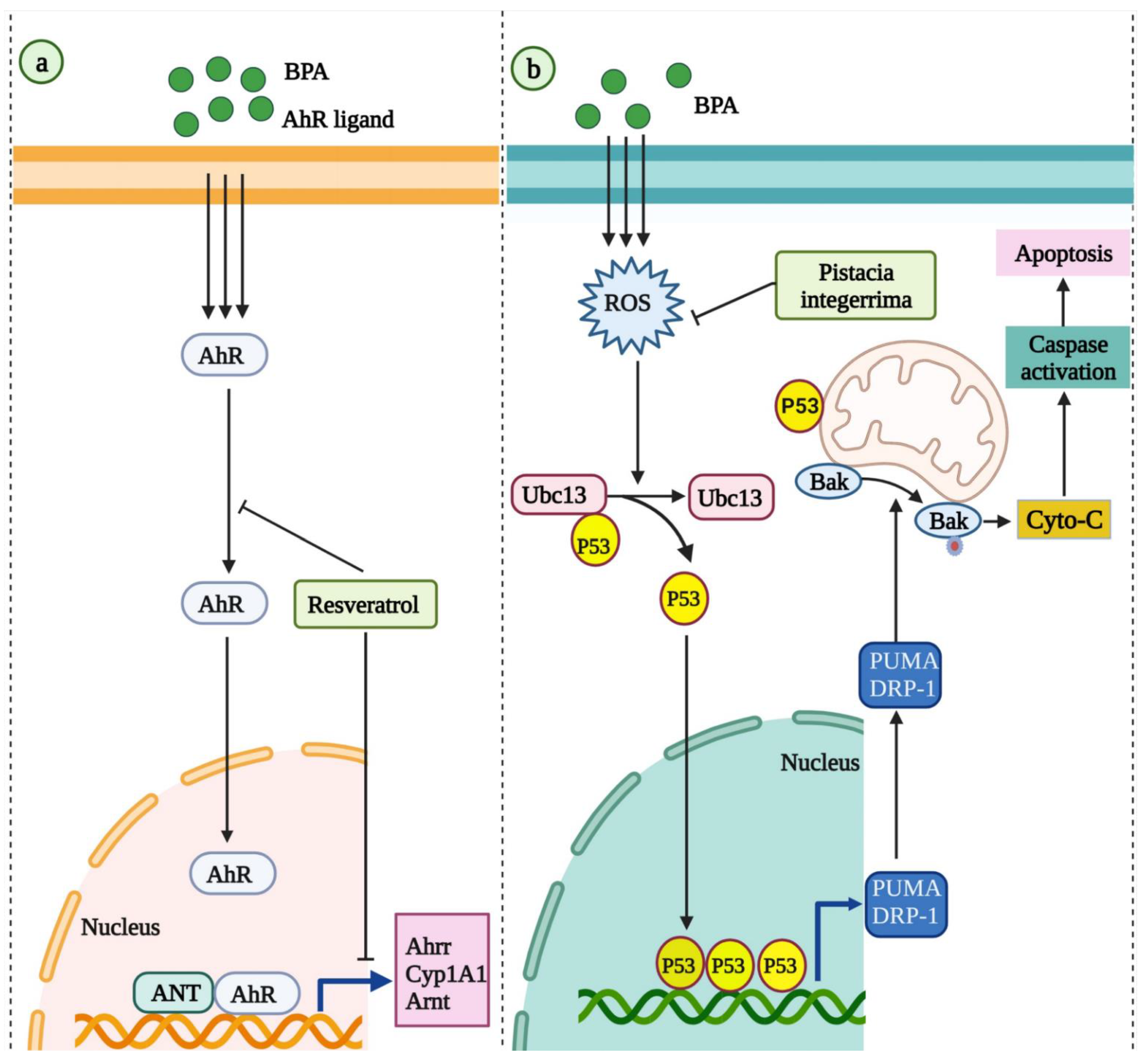
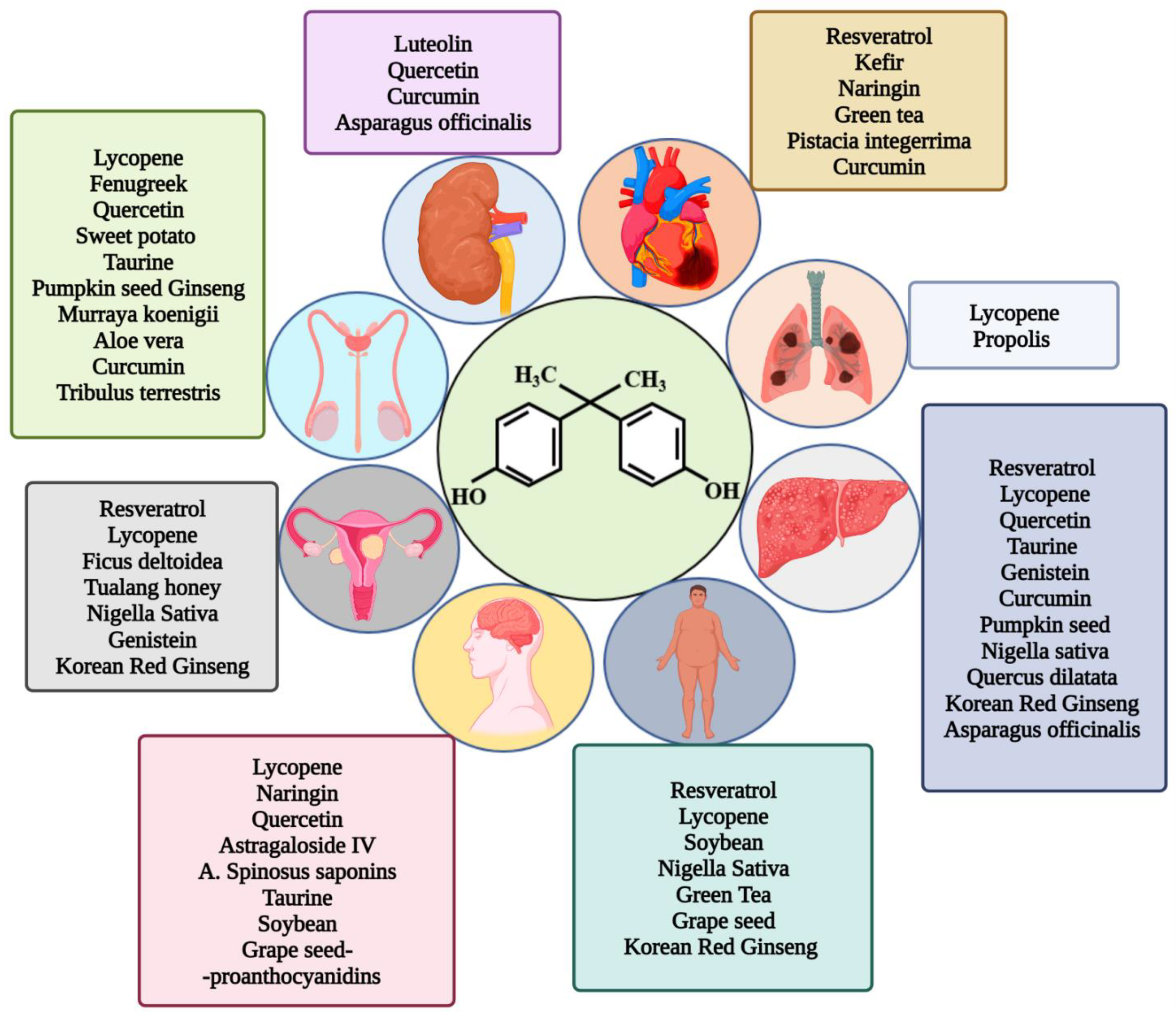
| Author; Year | Animal Model | BPA Dose | Natural Product/Natural Compound and Its Dose | BPA Induced Toxicity | Mechanism of Actions |
|---|---|---|---|---|---|
| Ishtiaq et al., 2020 [157] | Sprague Dawley rats | 100 µg/kg B.wt/day | Pistacia integerrima— 200 mg/kg B.wt/day | Cardiotoxicity | Neutralizing the oxidative stress through Ubc13/p53 pathway |
| Kaur, S., and Sadwal, S. 2020 [171] | Mice (BALB/c) | 1 mg/kg B.wt/day | Fenugreek seed extract—200 mg/ kg B.wt/day | Testicular damage | -Antioxidant effects |
| Friques et al., 2020 [174] | Wistar rats | 100 μg/kg B.wt/day | Kefir—0.3 mL/100 g B.wt/day | Hypertension and vascular toxicity | -Antioxidant effects -Increasing NO bioavailability |
| Abdou et al., 2022 [179] | Wistar rats | 50 mg B.wt/day/kg | Grape seed proanthocyanidins—200 mg/kg B.wt/day | Neurotoxicity | -Anti-inflammatory effects -Antioxidant effects |
| Zaid et al., 2021 [190] | Sprague Dawley rats | 10 mg/kg B.wt/day | Ficus deltoidea—100 mg/kg B.wt/day | Female reproductive toxicity (Uterus) | NA |
| Zaid et al., 2018 [191] | Sprague Dawley rats | 10 mg/kg B.wt/day | Ficus deltoidea—100 mg/kg B.wt/day | Female reproductive system (ovary) | NA |
| Revathy et al., 2017 [193] | Sprague Dawley rats | 200 mg/kg B.wt/day | Ipomoea batatas—400 mg/kg B.wt/day | Male reproductive toxicity | NA |
| Kazmi et al., 2018 [199] | Sprague Dawley rats | 25 mg/kg B.wt/day | Quercus dilatata Lindl. ex Royle—300 mg/kg B.wt/day | Hepatotoxicity | Antioxidant effects |
| Mohamad Zaid et al., 2015 [204] | Sprague Dawley rats | 10 mg/kg B.wt/day | Tualang honey—200 mg/kg B.wt/day | Uterine toxicity | -Normalizing ERα, ERβ, and C3 expression and distribution -Reducing lipid peroxidation |
| Zaid et al., 2014 [205] | Sprague Dawley rats | 10 mg/kg B.wt/day | Tualang honey—200 mg/kg B.wt/day | Ovarian toxicity | Antioxidant effects |
| Eweda et al., 2020 [209] | Albino Wistar rats | 30 mg/kg B.wt/day | Sesame lignans—20 mg/kg B.wt/day | Hepatotoxicity and cardiotoxicity | -Antioxidant effects -Improving lipid profile |
| Abo et al., 2020 [210] | Sprague Dawley rats | 25 and 50 mg/kg B.wt/day | Sesame oil—10 mL/kg B.wt/day | Cardiotoxicity | Antioxidant effects |
| Soliman et al., 2021 [216] | Albino rats | 500 mg/kg B.wt/day | Propolis—50 mg/kg B.wt/day | Lung injury | Anti-inflammatory and antioxidant effects |
| Sujan et al., 2019 [220] | Swiss albino mice | 50 mg/kg B.wt/day | Nigella Sativa oil— 1 mL/kg B.wt/day | Hyperlipidemia and obesity | Antioxidant effects |
| Sujan et al., 2020 [221] | Swiss albino mice | 50 mg/kg B.wt/day | Nigella Sativa oil— 1 mL/kg B.wt/day | Blood and reproductive organ | Antioxidant effects |
| Fadishei. et al., 2021 [222] | Albino Wistar rats | 10 mg/kg B.wt/day | Nigella Sativa oil— 21, 42, 84 μL/kg B.wt/day Thymoquinone—0.5, 1, 2 mg/kg B.wt/day | Metabolic disorder | Antioxidant effects |
| Abdel-Wahab et al., 2014 [223] | Sprague Dawley (SD) rats | 10 mg/kg B.wt/day | Thymoquinone—10 mg/kg B.wt/day | Hepatoxicity | Antioxidant effects |
| Mohsenzadeh et al., 2021a [230] | Wistar rats | 10 mg/kg B.wt/day | Green tea— 25, 50, and 100 mg/kg B.wt/day Epigallocatechin gallate—10, 20, and 40 mg/kg/day | Vascular toxicity | Antioxidant effects |
| Mohsenzadeh et al., 2021b [231] | Albino Wistar rats | 10 mg/kg B.wt/day | Green tea— 25, 50, and 100 mg/kg B.wt/day Epigallocatechin gallate—10, 20, and 40 mg/kg/day | Metabolic disorders | -Anti-inflammatory effects -Regulating the metabolism of lipids -Improving insulin signaling pathways |
| Veissi et al., 2018 [234] | NMRI mice | 100 μg/kg B.wt/day | Soy extract— 60, 150 mg/kg B.wt/day | Metabolic disorder | Antioxidant effects |
| Patisaul et al., 2012 [235] | Wistar rats | 1 mg/L | Soy rich diet | Anxiogenic behavior | Estrogen receptor beta, melanocortin receptors, oxytocin/vasopressin signaling pathways |
| Fawzy et al., 2018 [238] | Swiss albino mice | 50 mg/kg B.wt/day | Pumpkin seed oil—1 mL/kg B.wt/day | DNA damage in the liver and testes | Decreasing DNA damage |
| El Tabaa et al., 2017 [245] | Wistar rats | 250 mg/kg B.wt/day | Ginkgo biloba extract— mg/kg B.wt/day | Neurotoxicity | -Increasing biogenic amines release -Antioxidant effects adiponectin pro-secretory effects |
| Lee et al., 2020 [253] | CD-1 mice | 200 mg/kg B.wt/day | Korean red ginseng—1.2 g/kg/day | Inflammation in liver and uterus | Anti-inflammatory effects |
| Park et al., 2020 [254] | ICR mice | 800 mg/kg B.wt/day | Korean red ginseng—1.2 g/kg/day | Increased lipid profile | Regulating lipid metabolic process-related genes |
| Saadeldin et al., 2018 [255] | Albino rats | 150 mg/kg B.wt/day | Ginseng—200 mg/kg B.wt/day | Reproductive toxicity | Modulating mRNA transcripts of STAR, HSD17B3, and CYP17B, via AKT/PTEN pathway |
| Kaur et al., 2020 [261] | BALB/c mice | 1 mg/kg B.wt/day | Murraya koenigii—200 mg/kg B.wt/day | Testicular toxicity | -Antioxidant effects -Antiapoptotic effects |
| Poormoosavi et al., 2018 [100] | Wistar rats | 10 mg/kg B.wt/day | Asparagus officinalis— 200 mg/kg B.wt/day | Hepatic and renal toxicity | Antioxidant effects |
| Behmanesh et al., 2018 [269] | Wistar rats | 20 μg/kg B.wt/day | Aloe vera gel—300 mg/kg B.wt/day | Testicular toxicity | Antioxidant effects |
| Munir et al., 2017 [273] | Sprague Dawley rats | 25 mg/kg B.wt/day | Tribulus terrestris L. —20 mg/kg B.wt/day | Testicular toxicity | NA |
| Sirasanagandla et al., 2022 [155] | Apo E mice | 1 μg/ml | Resveratrol—20 mg/kg B.wt/day | Atherosclerosis | Autophagy modulation |
| Rameshrad et al., 2018 [182] | Albino Wistar rats | 35 mg/kg B.wt/day | Resveratrol—100 mg/kg B.wt/day Grape Seed Extract—3, and 12 mg/kg B.wt/day | Vascular toxicity | Antioxidant effects |
| Rameshrad et al., 2019 [183] | Wistar rats | 35 mg/kg B.wt/day | Resveratrol—25, 50, and 100 mg/kg B.wt/day Grape seed extract—3, 6, 12 mg/kg B.wt/day | Metabolic syndrome and insulin resistance | -Promoting insulin signaling -Increasing ABCG8 expression in the liver -Antioxidant activity |
| Shih et al., 2021 [278] | Sprague Dawley rats | 50 μg/kg B.wt/day | Resveratrol butyrate esters— 30 mg/kg B.wt/day | Obesity | Modulatory activity in intestinal microbiota |
| Fouad et al., 2021 [279] | Wistar rats | 20 mg/kg B.wt/day | Resveratrol— 20 mg/kg B.wt/day | Uterine damage | -Antioxidant activity -Antiapoptotic effects |
| Cetin et al., 2021 [280] | Wistar albino rats | 130 mg/kg B.wt/day | Resveratrol—100 and 200 mg/kg/day Apigenin—100 and 200 mg/kg B.wt/day | Salivary gland cytotoxicity | -Antioxidant effects -Antiapoptotic effects |
| Bordbar et al., 2021 [281] | Sprague Dawley rats | 50 mg/kg B.wt/day | Resveratrol—100 mg/kg B.wt/day | Hepatotoxicity | NA |
| Hsu et al., 2019 [160] | Sprague Dawley rats | 50 μg/kg B.wt/day | Resveratrol—50 mg/L | Developmental programming of hypertension | -Increasing NO bioavailability -Antioxidant effects -Suppressing the AHR signaling pathway |
| Liao et al., 2021 [284] | Sprague Dawley rats | 50 μg/kg B.wt/day | Resveratrol butyrate esters—30 mg/kg B.wt/day | Hepatic toxicity | -Antioxidant effects -Modulating gut microbiota |
| Rahmani-Moghadam et al., 2022 [286] | Sprague Dawley rats | 50 mg/kg B.wt/day | Resveratrol—100 mg/kg B.wt/day | Oral mucosa and tongue toxicity | NA |
| Alekhya Sita al., 2019 [293] | Wistar rats | 250 mg/kg B.wt/day | Luteolin—100 and 200 mg/kg B.wt/day | Nephron toxicity | Nrf2/ antioxidant response element (ARE)/HO-1 pathway regulation |
| Adesanoye et al., 2020 [294] | Drosophila melanogaster (Canton-S strain) | 0.05 mM | Luteolin—150 and 300 mg/kg B.wt/day | Oxidative stress, locomotor deficit, reduction in offspring emergence rate, cell viability, inhibition of acetylcholinesterase activity | -Antioxidant and chemo-preventive properties |
| Faheem et al., 2021 [299] | Albino Wistar rats | 50 mg/kg B.wt/day | Lycopene—10 mg/kg B.wt/day | Lung injury | -Anti-inflammatory effects -Antioxidant effects -Antiapoptotic effects |
| Abdel-Rahman et al., 2018 [300] | Wistar rats | 10 mg/kg B.wt/day | Lycopene—10 mg/kg B.wt/day | Hepatotoxicity | -Antioxidant effects -Antiapoptotic effects |
| Ma et al., 2018 [301] | Kunming mice | 500 mg/kg B.wt/day | Lycopene—20 mg B.wt/day/kg | Reproductive toxicity | NA |
| Elgawish et al., 2020 [302] | Wistar rats | 10 mg/kg B.wt/day | Lycopene—10 mg/kg B.wt/day | Metabolic syndrome | -Antioxidant effects -Anti-inflammatory effects |
| El Morsy et al., 2020 [303] | Albino rats | 50 mg/kg B.wt/day | Lycopene—10 mg/kg B.wt/day | Hippocampal neurotoxicity and defective memory function | -Antioxidant effects -Activation of MAPK/ERK pathway -Antiapoptotic effects |
| Essawy et al., 2021 [304] | Sprague Dawley rats | 125 mg/kg B.wt/day | Astragaloside IV—80 mg/kg B.wt/day A. spinosus saponins-100 mg/kg B.wt/day | DNA damage and Neurotoxicity | -Antioxidant effects -Anti-inflammatory and anti-apoptotic effects -Reducing DNA damage -Regulating the BDNF and NR2A and NR2B gene expression |
| Abd Elkader et al., 2021 [310] | Sprague Dawley rats | 125 mg/kg B.wt/day | Astragaloside IV—80 mg/kg B.wt/day A. spinosus saponins-100 mg/kg B.wt/day | Long-lasting anxiety-like behavior and depression in schizophrenia | -Neuroprotective activity |
| Khodayar et al., 2020 [314] | Wistar rats | 50 mg/kg B.wt/day | Naringin—40, 80, and 160 mg/kg B.wt/day | Cardiotoxicity | -Lipid-lowering properties -Antioxidant effects -Decreasing lipid peroxidation |
| Mahdavinia et al., 2019 [315] | Wistar rats | 50 mg/kg B.wt/day | Naringin—40, 80, and 160 mg/kg B.wt/day | Cognitive impairment and oxidative damage | -Antioxidant and neuroprotective effects |
| Rezaee-Tazangi et al., 2020 [321] | NMRI mice | 0.8 mmol/mL | Taurine—5, 10, 30, and 50 µmol/L | Mitochondrial toxicity and impaired sperm quality | Antioxidant effects |
| Mahdavinia et al., 2019 [108] | Wistar rats | 250 mg/kg B.wt/day | Quercetin—75 mg/kg B.wt/day | Hepatotoxicity (liver) | -Antioxidant effects -Preventing mitochondrial damage |
| Pradhan et al., 2021 [322] | Zebrafish | 17.52 μM | Taurine—63.9233 μM | Neurotoxicity | Antioxidant effects |
| Shirani et al., 2019 [326] | Wistar rats | 250 mg/kg B.wt/day | Quercetin—75 mg/kg B.wt/day | Nephrotoxicity (through uric acid and creatinine) | Antioxidant effects |
| Jahan et al., 2016 [327] | Sprague Dawley rats | 50 mg/kg B.wt/day | Quercetin—50 mg/kg B.wt/day | Testicular toxicity | NA |
| Sahoo et al., 2020 [328] | Zebrafish | 17.52 μM | Quercetin—2.96 μM | Neurotoxicity | Antioxidant effects |
| Sangai et al., 2014 [330] | Swiss albino mice | 120 and 240 mg/kg B.wt/day | Quercetin—60 mg/kg B.wt/day | Hepatotoxicity and nephrotoxicity | Antioxidant effects |
| Bernardo et al., 2015 [333] | Sprague Dawley rats | 25 and 250 μg/kg B.wt/day | Genistein— 5.5 mg/kg B.wt/day | Reproductive organs | Antitumor effects |
| Betancourt et al., 2014 [335] | Sprague Dawley rats | 250 μg/kg B.wt/day | Genistein— 250 mg/kg B.wt/day | Cancer | Anticancer and chemoprotective effects |
| Uzunhisarcikli and Aslanturk, 2019 [341] | Wistar rats | 130 mg/kg B.wt/day | Curcumin—100 mg/kg/day Taurine—100 mg/kg B.wt/day | Hepatotoxicity | Antioxidant effects |
| Panpatil et al., 2020 [342] | Wistar NIN (WNIN) rats | 0, 50 and 100 ug/kg B.wt/day | Turmeric in diet 3% (wt/wt) | Liver and kidney | Decreasing DNA migration and genotoxicity |
| Apaydin et al., 2019 [343] | Albino rats | 130 mg/kg B.wt/day | Curcumin—100 mg/kg B.wt/day Taurine—100 mg/kg B.wt/day | Cardiotoxicity | Antioxidant effects |
| Kalender et al., 2019 [344] | Wistar rats | 130 mg/kg B.wt/day | Curcumin—100 mg/kg B.wt/day Taurine—100 mg/kg B.wt/day | Testicular toxicity | Antioxidant effects |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sirasanagandla, S.R.; Al-Huseini, I.; Sakr, H.; Moqadass, M.; Das, S.; Juliana, N.; Abu, I.F. Natural Products in Mitigation of Bisphenol A Toxicity: Future Therapeutic Use. Molecules 2022, 27, 5384. https://doi.org/10.3390/molecules27175384
Sirasanagandla SR, Al-Huseini I, Sakr H, Moqadass M, Das S, Juliana N, Abu IF. Natural Products in Mitigation of Bisphenol A Toxicity: Future Therapeutic Use. Molecules. 2022; 27(17):5384. https://doi.org/10.3390/molecules27175384
Chicago/Turabian StyleSirasanagandla, Srinivasa Rao, Isehaq Al-Huseini, Hussein Sakr, Marzie Moqadass, Srijit Das, Norsham Juliana, and Izuddin Fahmy Abu. 2022. "Natural Products in Mitigation of Bisphenol A Toxicity: Future Therapeutic Use" Molecules 27, no. 17: 5384. https://doi.org/10.3390/molecules27175384
APA StyleSirasanagandla, S. R., Al-Huseini, I., Sakr, H., Moqadass, M., Das, S., Juliana, N., & Abu, I. F. (2022). Natural Products in Mitigation of Bisphenol A Toxicity: Future Therapeutic Use. Molecules, 27(17), 5384. https://doi.org/10.3390/molecules27175384









