Plant-Based Indole Alkaloids: A Comprehensive Overview from a Pharmacological Perspective
Abstract
1. Introduction
2. Indole Alkaloids: An Overview
3. Pharmacological Activities
3.1. Antimicrobial Activity
3.2. Antiviral Activity
3.3. Antidepressant Activity
3.4. Anticancer Activity
3.5. Anti-Inflammatory Activity
3.6. Analgesic Activity
3.7. Antidiabetic Activity
3.8. Antimalarial Activity
3.9. Hypotensive Activity
3.10. Anticholinesterase Activity
3.11. Antiplatelet Activity
3.12. Antidiarrheal Activity
3.13. Spasmolytic Activity
3.14. Antileishmanial Activity
3.15. Lipid-Lowering Activity
3.16. Antimycobacterial Activity
4. Pharmacokinetic Profile
5. Conclusions and Future Perspectives
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Baeyer, A. Ueber die Reduction aromatischer Verbindungen mittelst Zinkstaub. Justus Liebigs Ann. Der Chem. 1866, 140, 295–296. [Google Scholar] [CrossRef]
- Kaushik, N.K.; Kaushik, N.; Attri, P.; Kumar, N.; Kim, C.H.; Verma, A.K.; Choi, E.H. Biomedical importance of indoles. Molecules 2013, 18, 6620–6662. [Google Scholar] [CrossRef]
- Otero, N.; Mandado, M.; Mosquera, R.A. Nucleophilicity of Indole Derivatives: Activating and Deactivating Effects Based on Proton Affinities and Electron Density Properties. J. Phys. Chem. A 2007, 111, 5557–5562. [Google Scholar] [CrossRef]
- Dewick, P.M. Essentials of Organic Chemistry: For Students of Pharmacy, Medicinal Chemistry and Biological Chemistry; John Wiley & Sons: Hoboken, NJ, USA, 2006. [Google Scholar]
- Wang, W.; Cheng, M.-H.; Wang, X.-H. Monoterpenoid indole alkaloids from Alstonia rupestris with cytotoxic, anti-inflammatory and antifungal activities. Molecules 2013, 18, 7309–7322. [Google Scholar] [CrossRef]
- Xu, S.Y.; Bian, R.L.; Chen, X. Methods of Pharmacology Experiment; People’s Sanitation Press: Beijing, China, 2003; pp. 1651–1653. [Google Scholar]
- Yu, H.-F.; Qin, X.-J.; Ding, C.-F.; Wei, X.; Yang, J.; Luo, J.-R.; Liu, L.; Khan, A.; Zhang, L.-C.; Xia, C.-F. Nepenthe-like indole alkaloids with antimicrobial activity from Ervatamia chinensis. Org. Lett. 2018, 20, 4116–4120. [Google Scholar] [CrossRef]
- Cheng, G.-G.; Li, D.; Hou, B.; Li, X.-N.; Liu, L.; Chen, Y.-Y.; Lunga, P.-K.; Khan, A.; Liu, Y.-P.; Zuo, Z.-L.; et al. Melokhanines A–J, Bioactive Monoterpenoid Indole Alkaloids with Diverse Skeletons from Melodinus khasianus. J. Nat. Prod. 2016, 79, 2158–2166. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Zhang, C.-J.; Zhang, D.-B.; Wen, J.; Zhao, X.-W.; Li, Y.; Gao, K. An unusual indole alkaloid with anti-adenovirus and anti-HSV activities from Alstonia scholaris. Tetrahedron Lett. 2014, 55, 1815–1817. [Google Scholar] [CrossRef]
- Tan, C.-J.; Di, Y.-T.; Wang, Y.-H.; Zhang, Y.; Si, Y.-K.; Zhang, Q.; Gao, S.; Hu, X.-J.; Fang, X.; Li, S.-F. Three new indole alkaloids from Trigonostemon lii. Org. Lett. 2010, 12, 2370–2373. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.-P.; Liu, Q.-L.; Zhang, X.-L.; Niu, H.-Y.; Guan, C.-Y.; Sun, F.-K.; Xu, W.; Fu, Y.-H. Bioactive monoterpene indole alkaloids from Nauclea officinalis. Bioorganic Chem. 2019, 83, 1–5. [Google Scholar] [CrossRef]
- Rahman, J.; Tareq, A.M.; Hossain, M.M.; Sakib, S.A.; Islam, M.N.; Uddin, A.B.M.N.; Hoque, M.; Nasrin, M.S.; Ali, M.H.; Caiazzo, E.; et al. Biological evaluation, DFT calculations and molecular docking studies on the antidepressant and cytotoxicity activities of Cycas pectinata Buch.-Ham. Compounds. Pharmaceuticals 2020, 13, 232. [Google Scholar] [CrossRef]
- Bristy, T.A.; Barua, N.; Tareq, A.M.; Sakib, S.A.; Etu, S.T.; Chowdhury, K.H.; Jyoti, M.A.; Aziz, M.; Ibn, A.; Reza, A. Deciphering the pharmacological properties of methanol extract of Psychotria calocarpa leaves by in vivo, in vitro and in silico approaches. Pharmaceuticals 2020, 13, 183. [Google Scholar] [CrossRef] [PubMed]
- Farzin, D.; Mansouri, N. Antidepressant-like effect of harmane and other B-carbolines in the mouse forced swim test. Int. J. Neuropsychopharmacol. 2008, 11, 126. [Google Scholar] [CrossRef]
- Both, F.L.; Meneghini, L.; Kerber, V.A.; Henriques, A.T.; Elisabetsky, E. Psychopharmacological profile of the alkaloid psychollatine as a 5HT2A/C serotonin modulator. J. Nat. Prod. 2005, 68, 374–380. [Google Scholar] [CrossRef]
- Xiang-Hai, C.A.I.; Jiang, H.; Yan, L.I.; Cheng, G.-G.; Ya-Ping, L.I.U.; Tao, F.; Xiao-Dong, L.U.O. Cytotoxic indole alkaloids from Melodinus fusiformis and M. morsei. Chin. J. Nat. Med. 2011, 9, 259–263. [Google Scholar]
- Deng, X.-K.; Yin, W.; Li, W.-D.; Yin, F.-Z.; Lu, X.-Y.; Zhang, X.-C.; Hua, Z.-C.; Cai, B.-C. The anti-tumor effects of alkaloids from the seeds of Strychnos nux-vomica on HepG2 cells and its possible mechanism. J. Ethnopharmacol. 2006, 106, 179–186. [Google Scholar] [CrossRef] [PubMed]
- Sichaem, J.; Surapinit, S.; Siripong, P.; Khumkratok, S.; Jong-aramruang, J.; Tip-pyang, S. Two new cytotoxic isomeric indole alkaloids from the roots of Nauclea orientalis. Fitoterapia 2010, 81, 830–833. [Google Scholar] [CrossRef]
- Mishra, D.P.; Khan, M.A.; Yadav, D.K.; Rawat, A.K.; Singh, R.K.; Ahamad, T.; Hussain, M.K.; Saquib, M.; Khan, M.F. Monoterpene indole alkaloids from Anthocephalus cadamba fruits exhibiting anticancer activity in human lung cancer cell line H1299. ChemistrySelect 2018, 3, 8468–8472. [Google Scholar] [CrossRef]
- Guo, L.-L.; He, H.-P.; Di, Y.-T.; Li, S.-F.; Cheng, Y.-Y.; Yang, W.; Li, Y.; Yu, J.-P.; Zhang, Y.; Hao, X.-J. Indole alkaloids from Ervatamia chinensis. Phytochemistry 2012, 74, 140–145. [Google Scholar] [CrossRef] [PubMed]
- Raja, V.J.; Lim, K.-H.; Leong, C.-O.; Kam, T.-S.; Bradshaw, T.D. Novel antitumour indole alkaloid, Jerantinine A, evokes potent G2/M cell cycle arrest targeting microtubules. Investig. New Drugs 2014, 32, 838–850. [Google Scholar] [CrossRef] [PubMed]
- Fang, L.; Tian, S.-M.; Zhou, J.; Lin, Y.-L.; Wang, Z.-W.; Wang, X. Melaxillines A and B, monoterpenoid indole alkaloids from Melodinus axillaris. Fitoterapia 2016, 115, 173–176. [Google Scholar] [CrossRef]
- Cao, P.; Liang, Y.; Gao, X.; Li, X.-M.; Song, Z.-Q.; Liang, G. Monoterpenoid indole alkaloids from Alstonia yunnanensis and their cytotoxic and anti-inflammatory activities. Molecules 2012, 17, 13631–13641. [Google Scholar] [CrossRef]
- Jahan, I.; Tona, M.R.; Sharmin, S.; Sayeed, M.A.; Tania, F.Z.; Paul, A.; Chy, M.; Uddin, N.; Rakib, A.; Emran, T.B. GC-MS phytochemical profiling, pharmacological properties, and in silico studies of Chukrasia velutina leaves: A novel source for bioactive agents. Molecules 2020, 25, 3536. [Google Scholar] [CrossRef] [PubMed]
- Yin, W.; Wang, T.-S.; Yin, F.-Z.; Cai, B.-C. Analgesic and anti-inflammatory properties of brucine and brucine N-oxide extracted from seeds of Strychnos nux-vomica. J. Ethnopharmacol. 2003, 88, 205–214. [Google Scholar] [CrossRef]
- Shamima, A.R.; Fakurazi, S.; Hidayat, M.T.; Hairuszah, I.; Moklas, M.A.M.; Arulselvan, P. Antinociceptive action of isolated mitragynine from Mitragyna speciosa through activation of opioid receptor system. Int. J. Mol. Sci. 2012, 13, 11427–11442. [Google Scholar] [CrossRef] [PubMed]
- Rakib, A.; Ahmed, S.; Islam, M.A.; Uddin, M.M.N.; Paul, A.; Chy, M.N.U.; Emran, T.B.; Seidel, V. Pharmacological studies on the antinociceptive, anxiolytic and antidepressant activity of Tinospora crispa. Phytother. Res. 2020, 34, 2978–2984. [Google Scholar] [CrossRef] [PubMed]
- Rakib, A.; Ahmed, S.; Islam, M.A.; Haye, A.; Uddin, S.N.; Uddin, M.M.N.; Hossain, M.K.; Paul, A.; Emran, T.B. Antipyretic and hepatoprotective potential of Tinospora crispa and investigation of possible lead compounds through in silico approaches. Food Sci. Nutr. 2020, 8, 547–556. [Google Scholar] [CrossRef]
- Tiong, S.H.; Looi, C.Y.; Hazni, H.; Arya, A.; Paydar, M.; Wong, W.F.; Cheah, S.-C.; Mustafa, M.R.; Awang, K. Antidiabetic and antioxidant properties of alkaloids from Catharanthus roseus (L.) G. Don. Molecules 2013, 18, 9770–9784. [Google Scholar] [CrossRef]
- Tiong, S.H.; Looi, C.Y.; Arya, A.; Wong, W.F.; Hazni, H.; Mustafa, M.R.; Awang, K. Vindogentianine, a hypoglycemic alkaloid from Catharanthus roseus (L.) G. Don (Apocynaceae). Fitoterapia 2015, 102, 182–188. [Google Scholar] [CrossRef]
- Shittu, H.; Gray, A.; Furman, B.; Young, L. Glucose uptake stimulatory effect of akuammicine from Picralima nitida (Apocynaceae). Phytochem. Lett. 2010, 3, 53–55. [Google Scholar] [CrossRef]
- e Silva, L.F.R.; Montoia, A.; Amorim, R.C.N.; Melo, M.R.; Henrique, M.C.; Nunomura, S.M.; Costa, M.R.F.; Neto, V.F.A.; Costa, D.S.; Dantas, G. Comparative in vitro and in vivo antimalarial activity of the indole alkaloids ellipticine, olivacine, cryptolepine and a synthetic cryptolepine analog. Phytomedicine 2012, 20, 71–76. [Google Scholar] [CrossRef]
- Fernandez, L.S.; Buchanan, M.S.; Carroll, A.R.; Feng, Y.J.; Quinn, R.J.; Avery, V.M. Flinderoles a−c: Antimalarial bis-indole alkaloids from flindersia species. Org. Lett. 2009, 11, 329–332. [Google Scholar] [CrossRef]
- Mitaine-Offer, A.C.; Sauvain, M.; Valentin, A.; Callapa, J.; Mallié, M.; Zèches-Hanrot, M. Antiplasmodial activity of Aspidosperma indole alkaloids. Phytomedicine 2002, 9, 142–145. [Google Scholar] [CrossRef]
- Mbeunkui, F.; Grace, M.H.; Lategan, C.; Smith, P.J.; Raskin, I.; Lila, M.A. In vitro antiplasmodial activity of indole alkaloids from the stem bark of Geissospermum vellosii. J. Ethnopharmacol. 2012, 139, 471–477. [Google Scholar] [CrossRef]
- Liew, S.Y.; Mukhtar, M.R.; Hadi, A.H.A.; Awang, K.; Mustafa, M.R.; Zaima, K.; Morita, H.; Litaudon, M. Naucline, a new indole alkaloid from the bark of Nauclea officinalis. Molecules 2012, 17, 4028–4036. [Google Scholar] [CrossRef]
- Koyama, K.; Hirasawa, Y.; Zaima, K.; Hoe, T.C.; Chan, K.-L.; Morita, H. Alstilobanines A–E, new indole alkaloids from Alstonia angustiloba. Bioorganic Med. Chem. 2008, 16, 6483–6488. [Google Scholar] [CrossRef]
- Hirasawa, Y.; Dai, X.; Deguchi, J.; Hatano, S.; Sasaki, T.; Ohtsuka, R.; Nugroho, A.E.; Kaneda, T.; Morita, H. New vasorelaxant indole alkaloids, taberniacins A and B, from Tabernaemontana divaricata. J. Nat. Med. 2019, 73, 627–632. [Google Scholar] [CrossRef]
- Matsuo, H.; Okamoto, R.; Zaima, K.; Hirasawa, Y.; Ismail, I.S.; Lajis, N.H.; Morita, H. New vasorelaxant indole alkaloids, villocarines A–D from Uncaria villosa. Bioorganic Med. Chem. 2011, 19, 4075–4079. [Google Scholar] [CrossRef]
- Fadaeinasab, M.; Basiri, A.; Kia, Y.; Karimian, H.; Ali, H.M.; Murugaiyah, V. New indole alkaloids from the bark of Rauvolfia reflexa and their cholinesterase inhibitory activity. Cell. Physiol. Biochem. 2015, 37, 1997–2011. [Google Scholar] [CrossRef]
- Andrade, M.T.; Lima, J.A.; Pinto, A.C.; Rezende, C.M.; Carvalho, M.P.; Epifanio, R.A. Indole alkaloids from Tabernaemontana australis (Müell. Arg) Miers that inhibit acetylcholinesterase enzyme. Bioorganic Med. Chem. 2005, 13, 4092–4095. [Google Scholar] [CrossRef]
- Zhan, Z.-J.; Yu, Q.; Wang, Z.-L.; Shan, W.-G. Indole alkaloids from Ervatamia hainanensis with potent acetylcholinesterase inhibition activities. Bioorganic Med. Chem. Lett. 2010, 20, 6185–6187. [Google Scholar] [CrossRef]
- Liew, S.Y.; Khaw, K.Y.; Murugaiyah, V.; Looi, C.Y.; Wong, Y.L.; Mustafa, M.R.; Litaudon, M.; Awang, K. Natural indole butyrylcholinesterase inhibitors from Nauclea officinalis. Phytomedicine 2015, 22, 45–48. [Google Scholar] [CrossRef]
- Im, J.-H.; Jin, Y.-R.; Lee, J.-J.; Yu, J.-Y.; Han, X.-H.; Im, S.-H.; Hong, J.T.; Yoo, H.-S.; Pyo, M.-Y.; Yun, Y.-P. Antiplatelet activity of β-carboline alkaloids from Perganum harmala: A possible mechanism through inhibiting PLCγ2 phosphorylation. Vasc. Pharmacol. 2009, 50, 147–152. [Google Scholar] [CrossRef]
- Mandal, S.; Nayak, A.; Kar, M.; Banerjee, S.K.; Das, A.; Upadhyay, S.N.; Singh, R.K.; Banerji, A.; Banerji, J. Antidiarrhoeal activity of carbazole alkaloids from Murraya koenigii Spreng (Rutaceae) seeds. Fitoterapia 2010, 81, 72–74. [Google Scholar] [CrossRef]
- Jyoti, M.A.; Barua, N.; Hossain, M.S.; Hoque, M.; Bristy, T.A.; Mahmud, S.; Adnan, M.; Chy, M.; Uddin, N.; Paul, A.; et al. Unravelling the biological activities of the Byttneria pilosa leaves using experimental and computational approaches. Molecules 2020, 25, 4737. [Google Scholar] [CrossRef]
- Diniz, M.F.M.; Da Silva, B.A.; Mukherjee, R. Spasmolytic actions of the new indole alkaloid trinervine from Strychnos trinervis root. Phytomedicine 1994, 1, 205–207. [Google Scholar] [CrossRef]
- Da Silva, B.A.; de Araujo Filho, A.P.; Mukherjee, R.; Chiappeta, A.D.A. Bisnordihydrotoxiferine and vellosimine from Strychnos divaricans root: Spasmolytic properties of bisnordihydrotoxiferine. Phytother. Res. 1993, 7, 419–424. [Google Scholar] [CrossRef]
- Al Mahmud, Z.; Qais, N.; Bachar, S.C.; Hasan, C.M.; Emran, T.B.; Uddin, M.M.N. Phytochemical investigations and antioxidant potential of leaf of Leea macrophylla (Roxb.). BMC Res. Notes 2017, 10, 245. [Google Scholar] [CrossRef]
- Shi, C.C.; Liao, J.F.; Chen, C.F. Spasmolytic Effects of Three Harmala Alkaloids on Guinea-Pig Isolated Trachea. Pharmacol. Toxicol. 2001, 89, 259–264. [Google Scholar] [CrossRef]
- Tanaka, J.C.A.; Da Silva, C.C.; Ferreira, I.C.P.; Machado, G.M.C.; Leon, L.L.; De Oliveira, A.J.B. Antileishmanial activity of indole alkaloids from Aspidosperma ramiflorum. Phytomedicine 2007, 14, 377–380. [Google Scholar] [CrossRef]
- Yao-Hao, X.U.; Wei, L.I.; Yong, R.A.O.; Huang, Z.-S.; Sheng, Y.I.N. Pyridocarbazole alkaloids from Ochrosia borbonica: Lipid-lowering agents inhibit the cell proliferation and adipogenesis of 3T3-L1 adipocyte via intercalating into supercoiled DNA. Chin. J. Nat. Med. 2019, 17, 663–671. [Google Scholar]
- Tanaka, N.; Takao, M.; Matsumoto, T. Vincamine production in multiple shoot culture derived from hairy roots of Vinca minor. Plant Cell Tissue Organ Cult. 1995, 41, 61–64. [Google Scholar] [CrossRef]
- Nandini, H.S.; Naik, P.R. Antidiabetic, antihyperlipidemic and antioxidant effect of Vincamine, in streptozotocin-induced diabetic rats. Eur. J. Pharmacol. 2019, 843, 233–239. [Google Scholar] [CrossRef] [PubMed]
- Garcellano, R.C.; Cort, J.R.; Moinuddin, S.G.A.; Franzblau, S.G.; Ma, R.; Aguinaldo, A.M. An iboga alkaloid chemotaxonomic marker from endemic Tabernaemontana ternifolia with antitubercular activity. Nat. Prod. Res. 2020, 34, 1175–1179. [Google Scholar] [CrossRef] [PubMed]
- Macabeo, A.P.G.; Vidar, W.S.; Chen, X.; Decker, M.; Heilmann, J.; Wan, B.; Franzblau, S.G.; Galvez, E.V.; Aguinaldo, M.A.M.; Cordell, G.A. Mycobacterium tuberculosis and cholinesterase inhibitors from Voacanga globosa. Eur. J. Med. Chem. 2011, 46, 3118–3123. [Google Scholar] [CrossRef] [PubMed]
- Rahman, M.A.; bin Imran, T.; Islam, S. Antioxidative, antimicrobial and cytotoxic effects of the phenolics of Leea indica leaf extract. Saudi J. Biol. Sci. 2013, 20, 213–225. [Google Scholar] [CrossRef] [PubMed]
- Guzmán-Gutiérrez, S.L.; Silva-Miranda, M.; Krengel, F.; Huerta-Salazar, E.; León-Santiago, M.; Díaz-Cantón, J.K.; Pinzón, C.E.; Reyes-Chilpa, R. Antimycobacterial Activity of Alkaloids and Extracts from Tabernaemontana alba and T. arborea. Planta Med. 2020. [Google Scholar] [CrossRef]
- Saghir, S.A.; Ansari, R.A. Pharmacokinetics. In Reference Module in Biomedical Sciences; Elsevier: Amsterdam, The Netherlands, 2018. [Google Scholar]
- Chen, J.; Xiao, H.-L.; Hu, R.-R.; Hu, W.; Chen, Z.-P.; Cai, H.; Liu, X.; Lu, T.-L.; Fang, Y.; Cai, B.-C. Pharmacokinetics of brucine after intravenous and oral administration to rats. Fitoterapia 2011, 82, 1302–1308. [Google Scholar] [CrossRef]
- Janchawee, B.; Keawpradub, N.; Chittrakarn, S.; Prasettho, S.; Wararatananurak, P.; Sawangjareon, K. A high-performance liquid chromatographic method for determination of mitragynine in serum and its application to a pharmacokinetic study in rats. Biomed. Chromatogr. 2007, 21, 176–183. [Google Scholar] [CrossRef]
- Manda, V.K.; Avula, B.; Ali, Z.; Khan, I.A.; Walker, L.A.; Khan, S.I. Evaluation of in vitro absorption, distribution, metabolism, and excretion (ADME) properties of mitragynine, 7-hydroxymitragynine, and mitraphylline. Planta Med. 2014, 80, 568–576. [Google Scholar] [CrossRef]
- Lin, C.; Cai, J.; Yang, X.; Hu, L.; Lin, G. Liquid chromatography mass spectrometry simultaneous determination of vindoline and catharanthine in rat plasma and its application to a pharmacokinetic study. Biomed. Chromatogr. 2015, 29, 97–102. [Google Scholar] [CrossRef]
- Li, S.; Teng, L.; Liu, W.; Cheng, X.; Jiang, B.; Wang, Z.; Wang, C.-h. Pharmacokinetic study of harmane and its 10 metabolites in rat after intravenous and oral administration by UPLC-ESI-MS/MS. Pharm. Biol. 2016, 54, 1768–1781. [Google Scholar] [CrossRef] [PubMed]





| Compounds | Plant Source | Posology (Route, Dose) | Subject | Method | Identified Effect | References |
|---|---|---|---|---|---|---|
| Scholarisine I, II, III, F | Alstonia rupestris | - | Fungi | Disc diffusion method | Antifungal | [5] |
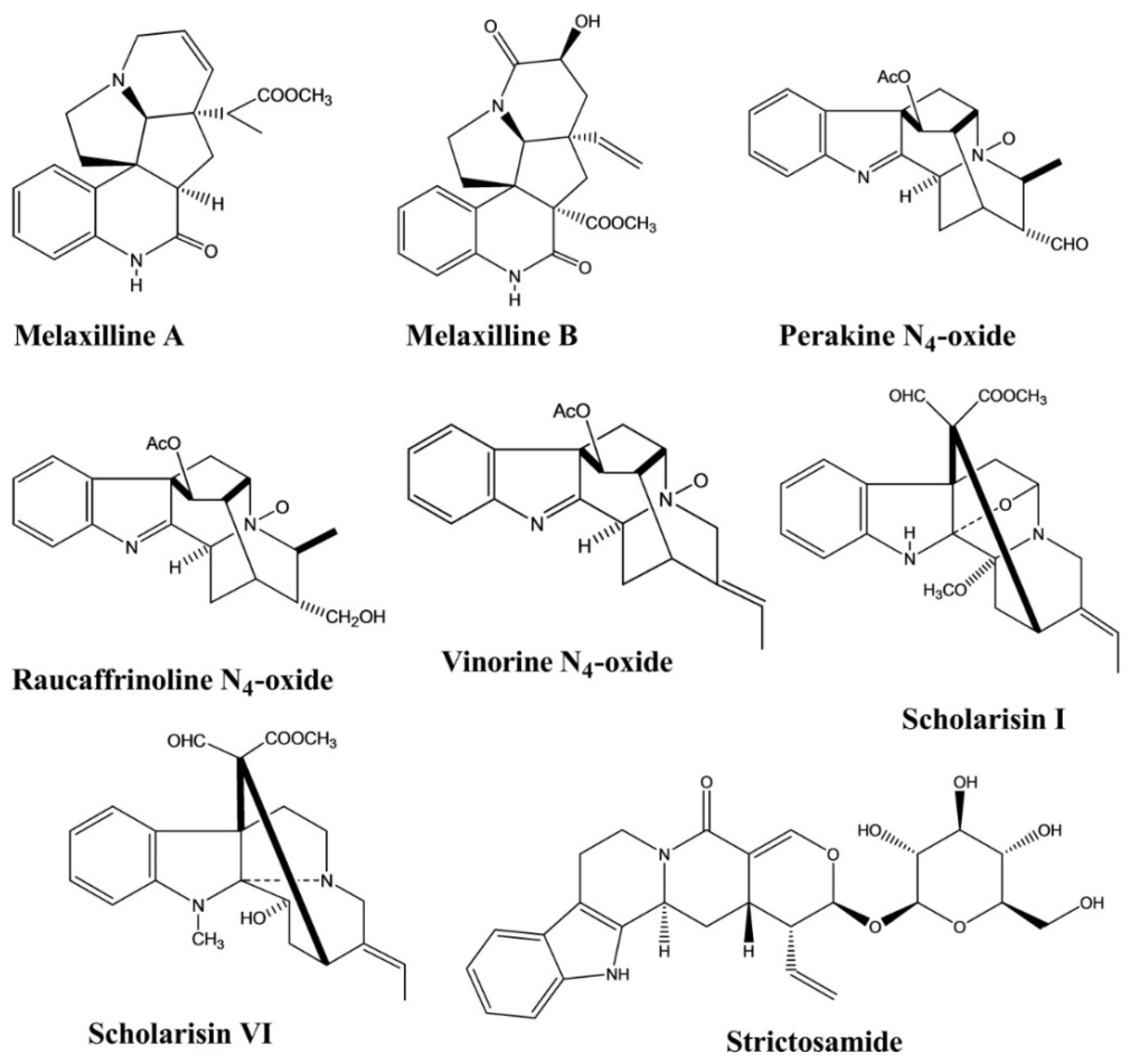
| Scholarisine I, VI | Alstonia rupestris | - | Enzyme | Enzyme inhibition assay | Anti-inflammatory | [5] |
| Kopsihainin D, E, F | Kopsia hainanensis | - | Bacteria | Disc agar diffusion method | Antibacterial | [6] |
| Kopsiflorine | Kopsia hainanensis | - | Bacteria | Disc agar diffusion method | Antibacterial | [6] |
| Erchinine A, B | Ervatamia chinensis | - | Bacteria Fungus | Broth microdilution method | Antibacterial, Antifungal | [7] |
| Melokhanine B, D, E, F | Melodinus khasianus | - | Bacteria | Broth microdilution method | Antibacterial | [8] |
| Melokhanine B, D, E, F | Melodinus khasianus | - | Bacteria | Broth microdilution method | Antibacterial | [8] |
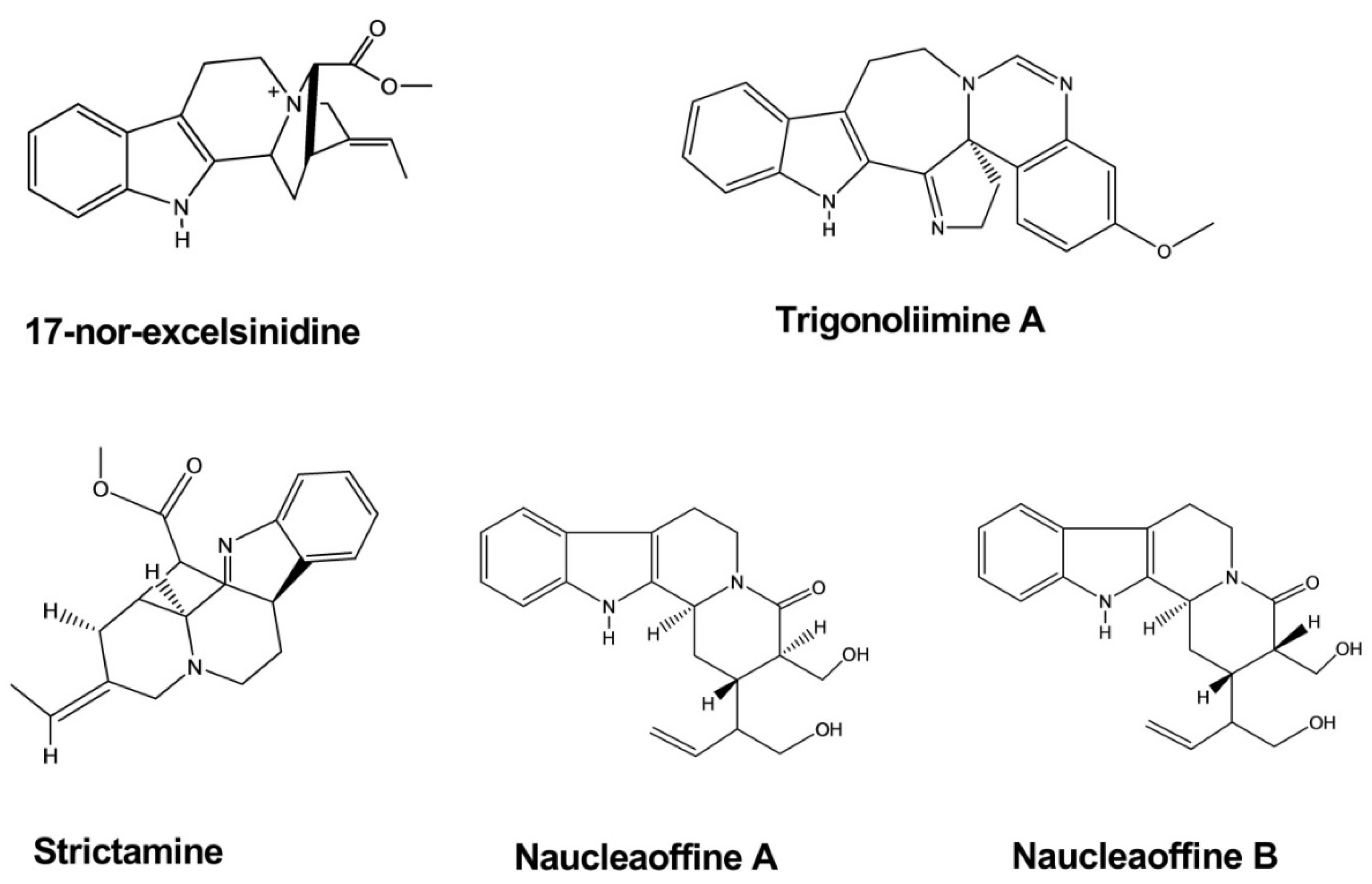
| Strictamine | Alstonia scholaris | - | Virus | - | Antiviral | [9] |
| 17-nor-excelsinidine | Alstonia scholaris | - | Virus | - | Antiviral | [9] |
| Trigonoliimine | Trigonostemon lii | - | Virus | Microtiter syncytium formation infectivity assay | Antiviral | [10] |
| Naucleaoffine A, B | Nauclea officinalis | Virus | Antiviral | [11] | ||
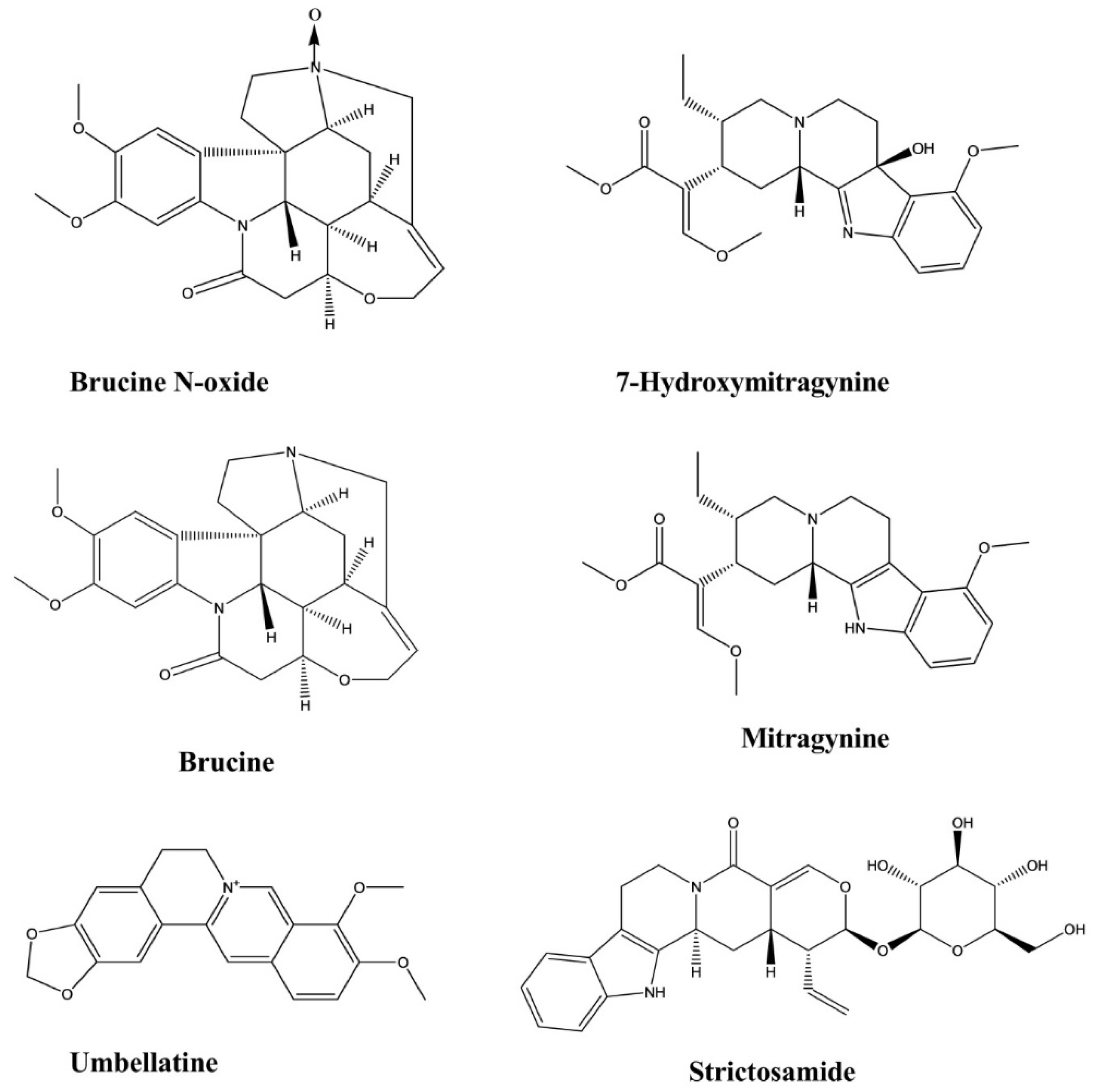
| Mitragynine | Mitragyna speciosa | Intraperitoneal, 10 and 30 mg/kg | Mice | Forced swim test, Tail suspension test | Antidepressant | [12] |
| Lyaloside | Psychotria suterella | - | Rat brain mitochondria | Enzymatic assay | Antidepressant | [13] |
| Strictosamide | Psychotria laciniata | - | Rat brain mitochondria | Enzymatic assay | Antidepressant | [13] |
| Harmane | Peganum harmala | Intraperitoneal, 5–15 mg/kg | Mice | Forced swim test | Antidepressant | [14] |
| Norharmane | Peganum harmala | Intraperitoneal, 2.5–10 mg/kg | Mice | Forced swim test | Antidepressant | [14] |
| Harmine | Peganum harmala | Intraperitoneal, 5–15 mg/kg | Mice | Forced swim test | Antidepressant | [14] |
| Psychollatine | Psychotria umbellate | 3, 7.5, and 15 mg/kg | Mice | Hole-board test, Forced swim test | Antidepressant | [15] |
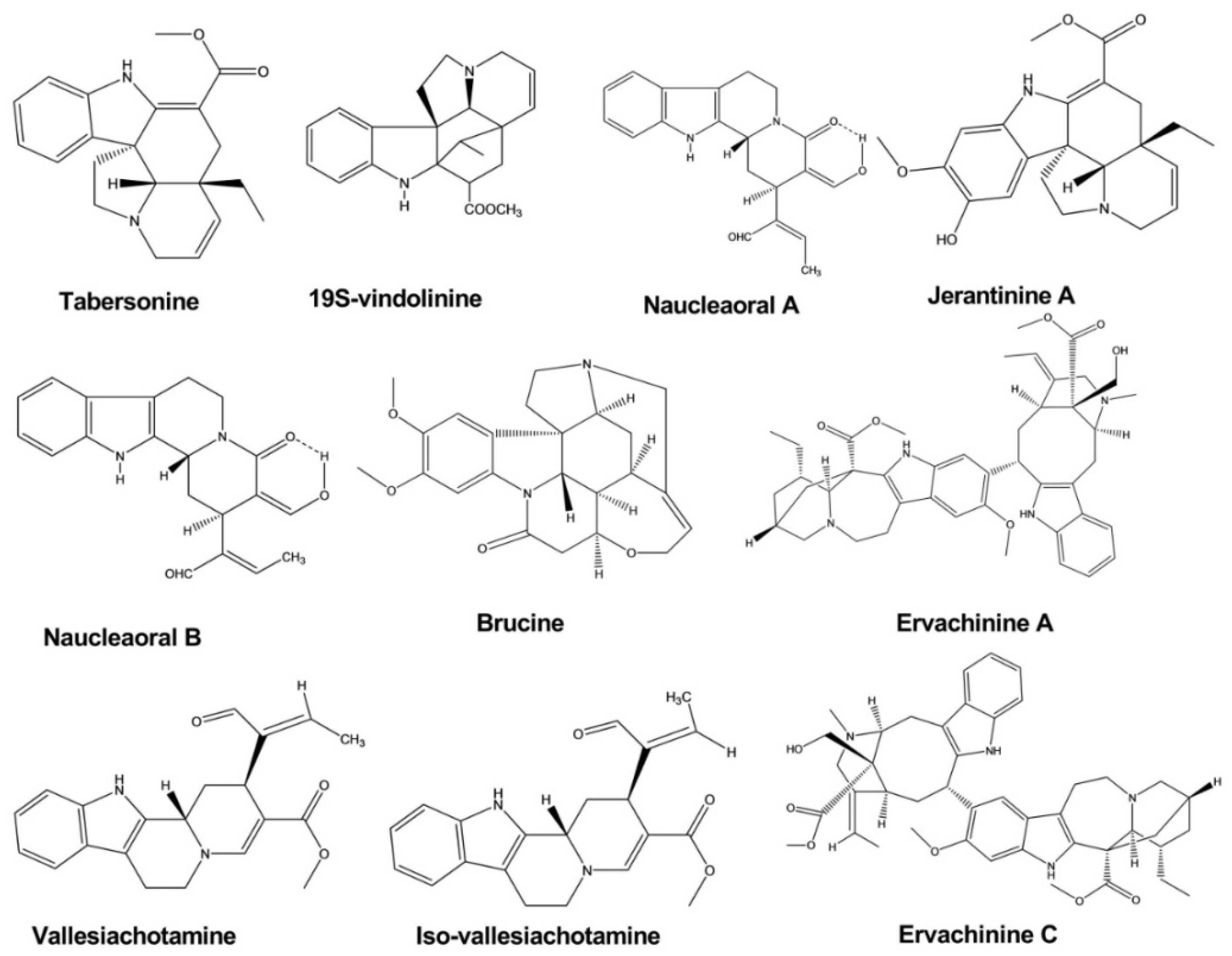
| Tabersonine | Melodinus fusiformis | - | Human tumor cell line | MTT assay | Anticancer | [16] |
| Brucine | Strychnos nux-vomica | - | Human hepatoma cell line | MTT-colorimetric assay | Anticancer | [17] |
| Naucleaoral A, B | Nauclea orientalis | - | Human cancer cell line | MTT-colorimetric assay | Anticancer | [18] |
| Vallesiachotamine | Anthocephalus cadamba | - | Human lung cancer cell line | MTT assay | Anticancer | [19] |
| Iso-vallesiachotamine | Anthocephalus cadamba | - | Human lung cancer cell line | MTT assay | Anticancer | [19] |
| Ervachinine A, C, D | Ervatamia chinensis | - | Human cancer cell line | MTT assay | Anticancer | [20] |
| Jerantinine A, B | Tabernaemontana corymbosa | Human cancer cell line | MTT assay | Anticancer | [21] | |
| Melaxilline A, B | Melodinus axillaris. | - | Rat | Platelet-activating factor induced inhibition assay | Anti-inflammatory | [22] |
| Perakine N4-oxide | Alstonia yunnanensis. | - | Enzyme | Enzyme inhibition assay | Anti-inflammatory | [23] |
| Raucaffrinoline N4-oxide | Alstonia yunnanensis. | - | Enzyme | Enzyme inhibition assay | Anti-inflammatory | [23] |
| Vinorine N4-oxide | Alstonia yunnanensis. | - | Enzyme | Enzyme inhibition assay | Anti-inflammatory | [23] |
| Strictosamide | Nauclea officinalis | Intraperitoneal, 20 and 40 mg/kg | Mice | Hot plate test, Writhing test | Analgesic | [24] |
| Strictosamide | Psychotria laciniata | Intravenous, 20 and 40 mg/kg | Mice | Acetic acid and TPA-induced assay | Anti-inflammatory | [24] |
| Brucine | Strychnos nux-vomica | Intraperitoneal, 30, 15, and 7.5 mg/kg | Mice | Formalin test | Analgesic | [25] |
| Brucine | Strychnos nux-vomica | Intraperitoneal, 30, 20, 14.7, and 10.3 mg/kg | Mice | Hot plate test | Analgesic | [25] |
| Brucine | Strychnos nux-vomica | Intraperitoneal, 30, 15, 7.5, and 3.75 mg/kg | Mice | Writhing test | Analgesic | [25] |
| Brucine N-oxide | Strychnos nux-vomica | Intraperitoneal, 200, 100 and 50 mg/kg | Mice | Formalin test | Analgesic | [25] |
| Brucine N-oxide | Strychnos nux-vomica | Intraperitoneal, 200, 140, 98, and 68 mg/kg | Mice | Hot plate test | Analgesic | [25] |
| Brucine N-oxide | Strychnos nux-vomica | Intraperitoneal, 200, 100, 50, and 25 mg/kg | Mice | Writhing test | Analgesic | [25] |
| Mitragynine | Mitragyna speciosa | Intraperitoneal, 3–35 mg/kg | Mice | Hot plate test | Analgesic | [26] |
| 7-hydroxymitragynine | Mitragyna speciosa | Subcutaneous, 2.5–10 mg/kg | Mice | Hot plate test, Tail flick test | Analgesic | [27] |
| Umbellatine | Psychotria umbellate | 100–300 mg/kg | Mice | Tail-flick test, Hot-plate test, Formalin test and Capsaicin-induced pain test | Analgesic | [28] |
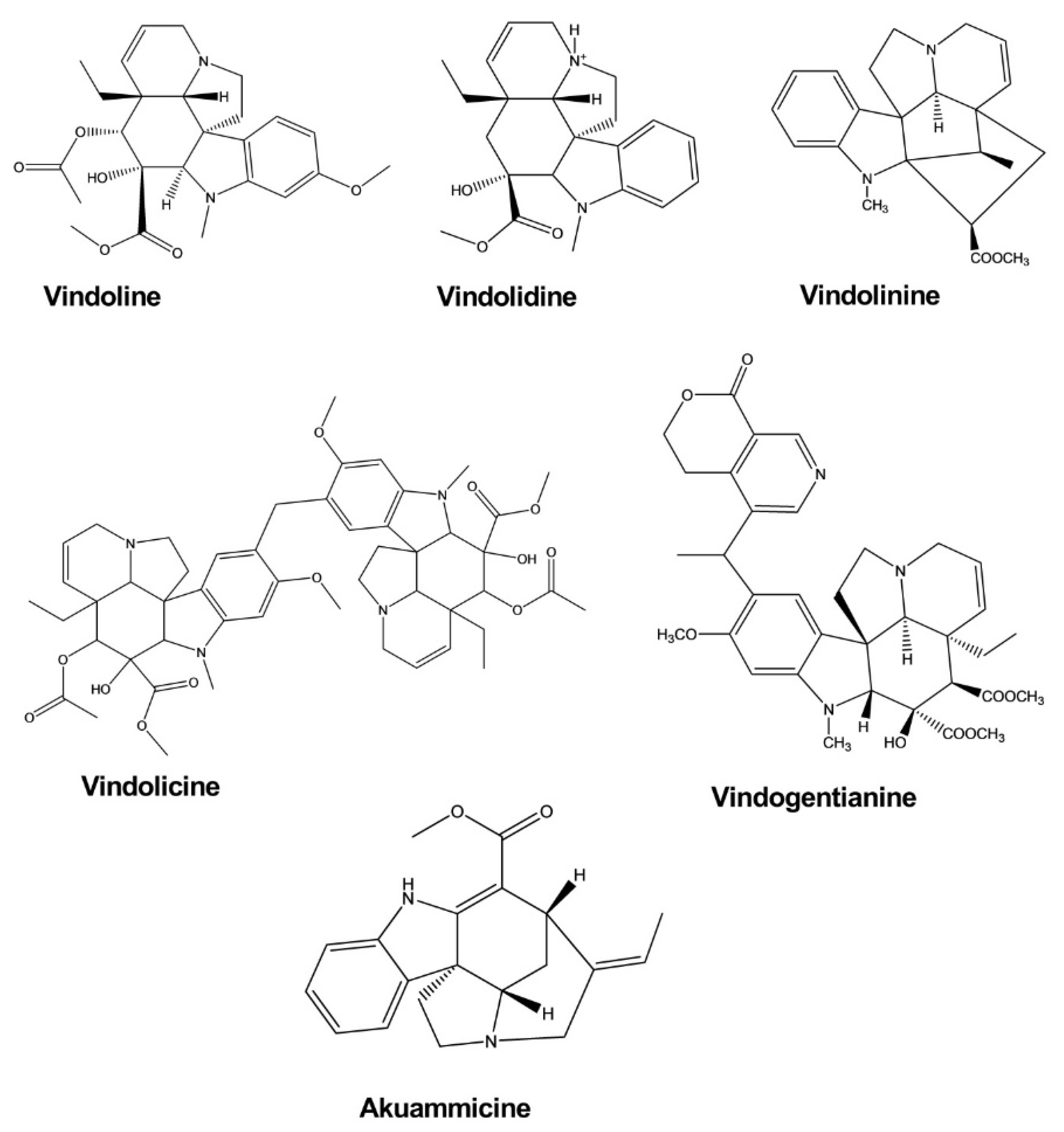
| Vindoline | Catharanthus roseus | - | Enzyme, Myoblast cell | Enzyme inhibition assay, Glucose uptake activity assay | Antidiabetic | [29] |
| Vindolidine | Catharanthus roseus | - | Enzyme, Myoblast cell | Enzyme inhibition assay, Glucose uptake activity assay | Antidiabetic | [29] |
| Vindolicine | Catharanthus roseus | - | Enzyme, Myoblast cell | Enzyme inhibition assay, Glucose uptake activity assay | Antidiabetic | [29] |
| Vindolinine | Catharanthus roseus | - | Enzyme, Myoblast cell | Enzyme inhibition assay, Glucose uptake activity assay | Antidiabetic | [29] |
| Vindogentianine | Catharanthus roseus | - | Enzyme, Myoblast cell | Enzyme inhibition assay, Glucose uptake activity assay | Antidiabetic | [30] |
| Akuammicine | Picralima nitida | - | Myoblast cell | Glucose uptake activity assay | Antidiabetic | [31] |
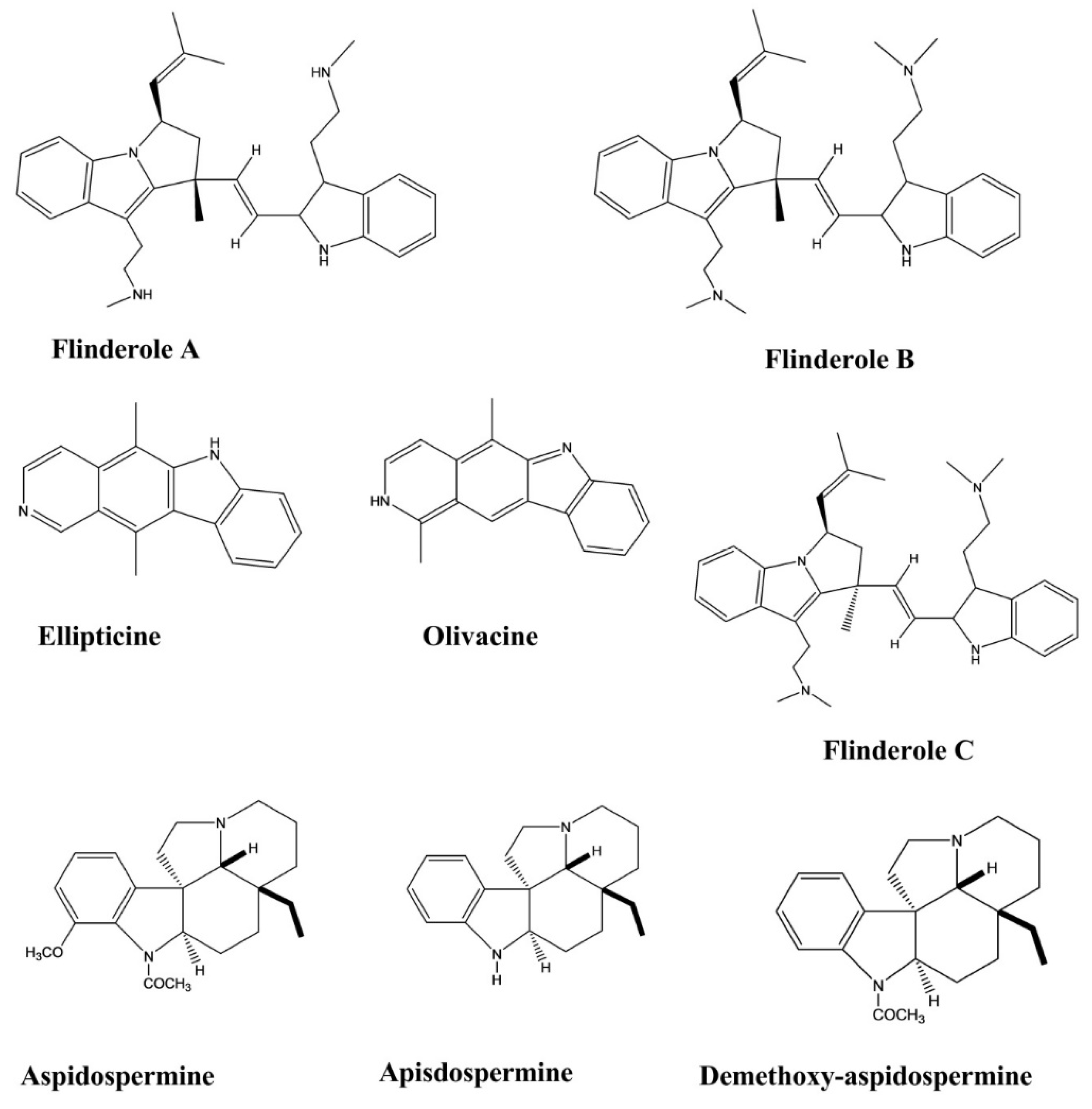
| Ellipticine | Aspidosperma vargasii | Oral, Subcutaneous, 50, 10 and 1 mg/kg/day | Mice | Suppressive test | Antimalarial | [32] |
| Olivacine | Aspidosperma olivaceum. | Oral, Subcutaneous, 100, 50, 10, and 1 mg/kg/day | Mice | Suppressive test | Antimalarial | [32] |
| Flinderole A, B, C | Flindersia acuminate F. amboinensis | - | Malarial Parasite | Micrdilution method | Antimalarial | [33] |
| Apisdospermin | - | Malarial Parasite | Micrdilution method | Antimalarial | [34] | |
| Aspidospermine | Aspidosperma pyrifolium | - | Malarial Parasite | Micrdilution method | Antimalarial | [34] |
| Demethoxy-aspidospermine | Aspidosperma pyrifolium | - | Malarial Parasite | Micrdilution method | Antimalarial | [34] |
| Vallesine | Aspidosperma pyrifolium | - | Malarial Parasite | Micrdilution method | Antimalarial | [34] |
| Palosine | Aspidosperma pyrifolium | - | Malarial Parasite | Micrdilution method | Antimalarial | [34] |
| Geissolosimine | Geissospermum vellosii | - | Malarial Parasite | Parasite lactate dehydrogenase assay | Antimalarial | [35] |
| Geissospermine | Geissospermum vellosii | - | Malarial Parasite | Parasite lactate dehydrogenase assay | Antimalarial | [35] |
| Geissoschizoline | Geissospermum vellosii | - | Malarial Parasite | Parasite lactate dehydrogenase assay | Antimalarial | [35] |
| Geissoschizone | Geissospermum vellosii | - | Malarial Parasite | Parasite lactate dehydrogenase assay | Antimalarial | [35] |
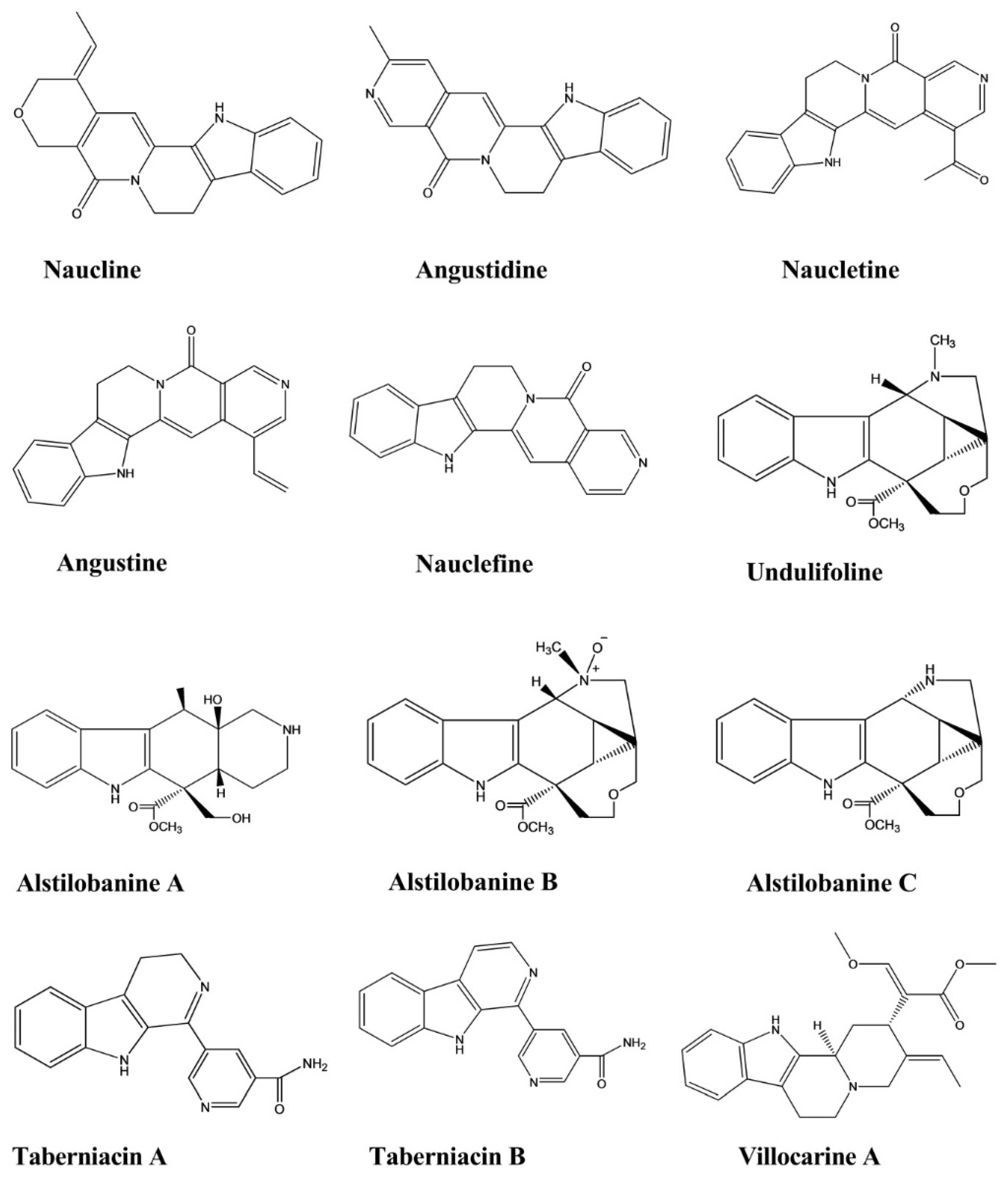
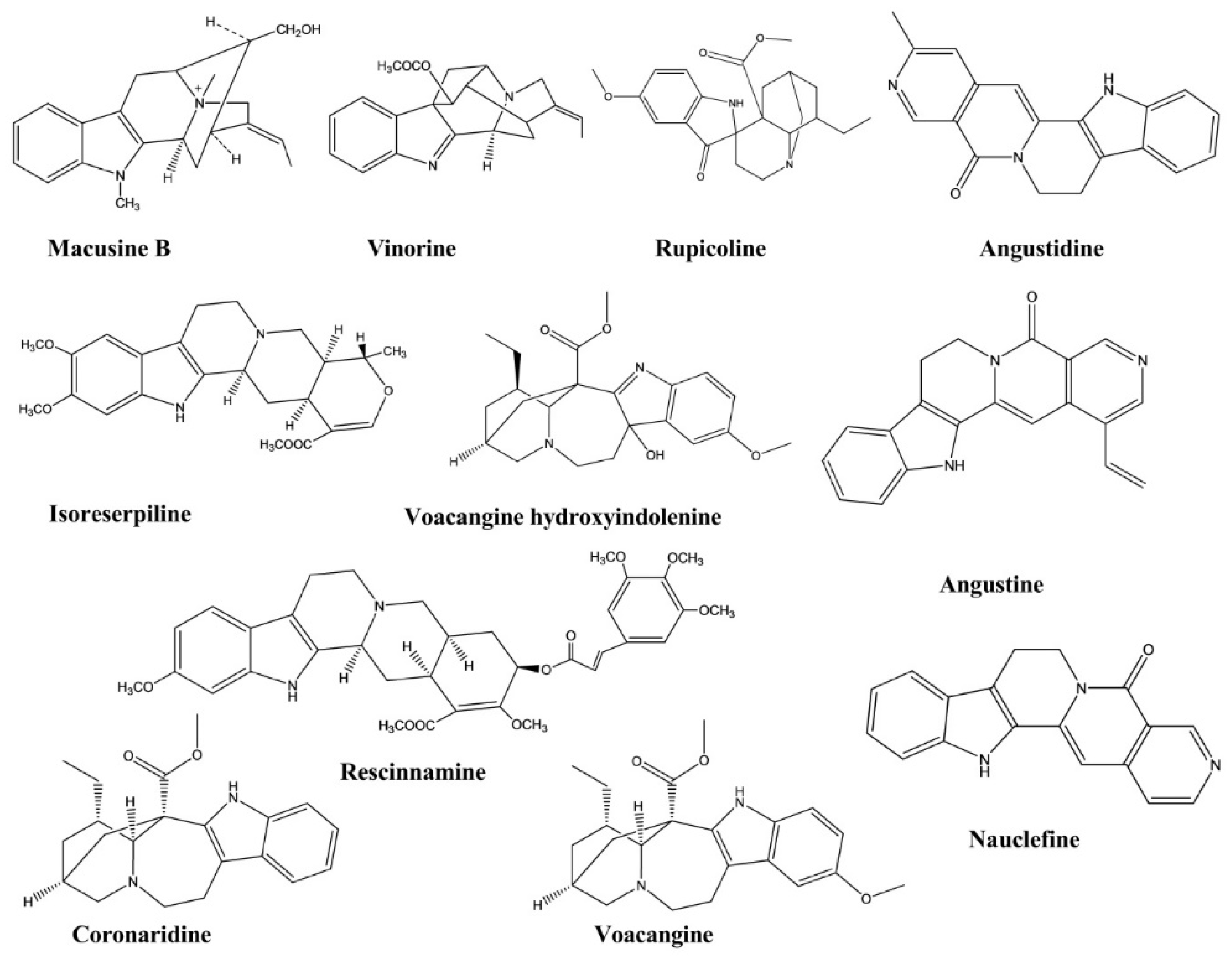
| Naucline | Nauclea officinalis | Injection, 1 × 10−5 M | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [36] |
| Angustine | Nauclea officinalis | Injection, 1 × 10−5 M | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [36] |
| Angustidine | Nauclea officinalis | Injection, 1 × 10−5 M | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [36] |
| Nauclefine | Nauclea officinalis | Injection, 1 × 10−5 M | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [36] |
| Naucletine | Nauclea officinalis | Injection, 1 × 10−5 M | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [36] |
| Alstilobanine A, B, C | Alstonia angustiloba | - | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [37] |
| Undulifoline | Alstonia undulifolia | - | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [37] |
| Taberniacin A, B | Tabernaemontana divaricata | - | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [38] |
| Villocarine A | Uncaria villosa | Injection, 30 μM | Rat | Phenylephrine-induced vasodilation assay | Hypotensive | [39] |
| Macusine B | Rauvolfia reflexa | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [40] |
| Vinorine | Rauvolfia reflexa | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [40] |
| Isoreserpiline | Rauvolfia reflexa | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [40] |
| Rescinnamine | Rauvolfia reflexa | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [40] |
| Voacangine hydroxyindolenine | Tabernaemontana australis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [41] |
| Rupicoline | Tabernaemontana australis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [41] |
| Coronaridine | Ervatamia hainanensis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [42] |
| Voacangine | Ervatamia hainanensis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [42] |
| Angustidine | Nauclea officinalis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [43] |
| Nauclefine | Nauclea officinalis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [43] |
| Angustine | Nauclea officinalis | - | Cholinesterase Enzyme | Cholinesterase Inhibition assay | Anticholinesterase | [43] |
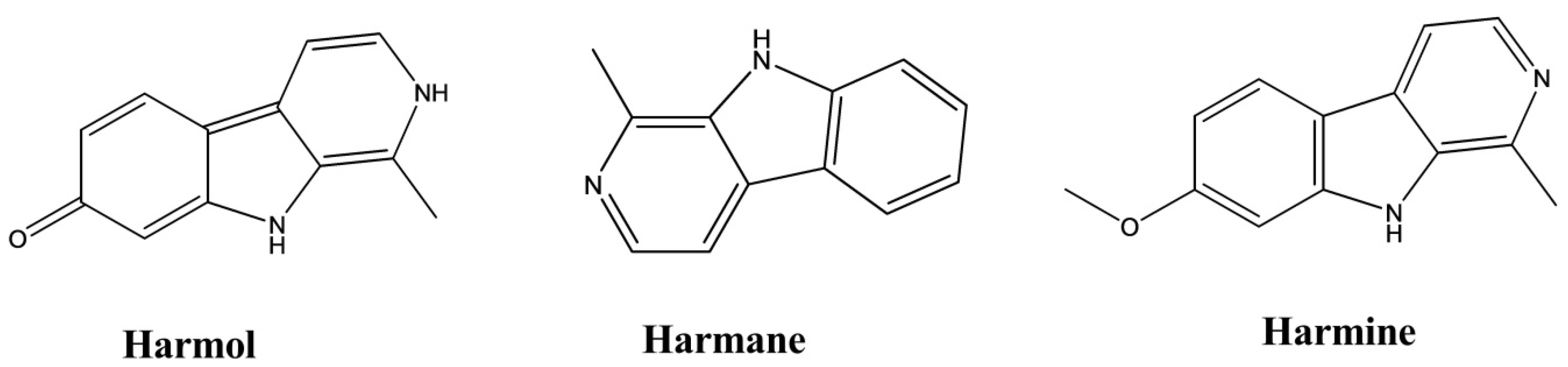
| Harmane | Perganum harmala | 100–200 µM | Rabbit Platelet | - | Antiplatelet | [44] |
| Harmine | Perganum harmala | 100–200 µM | Rabbit Platelet | - | Antiplatelet | [44] |
| Harmol | Perganum harmala | 100–200 µM | Rabbit Platelet | - | Antiplatelet | [44] |
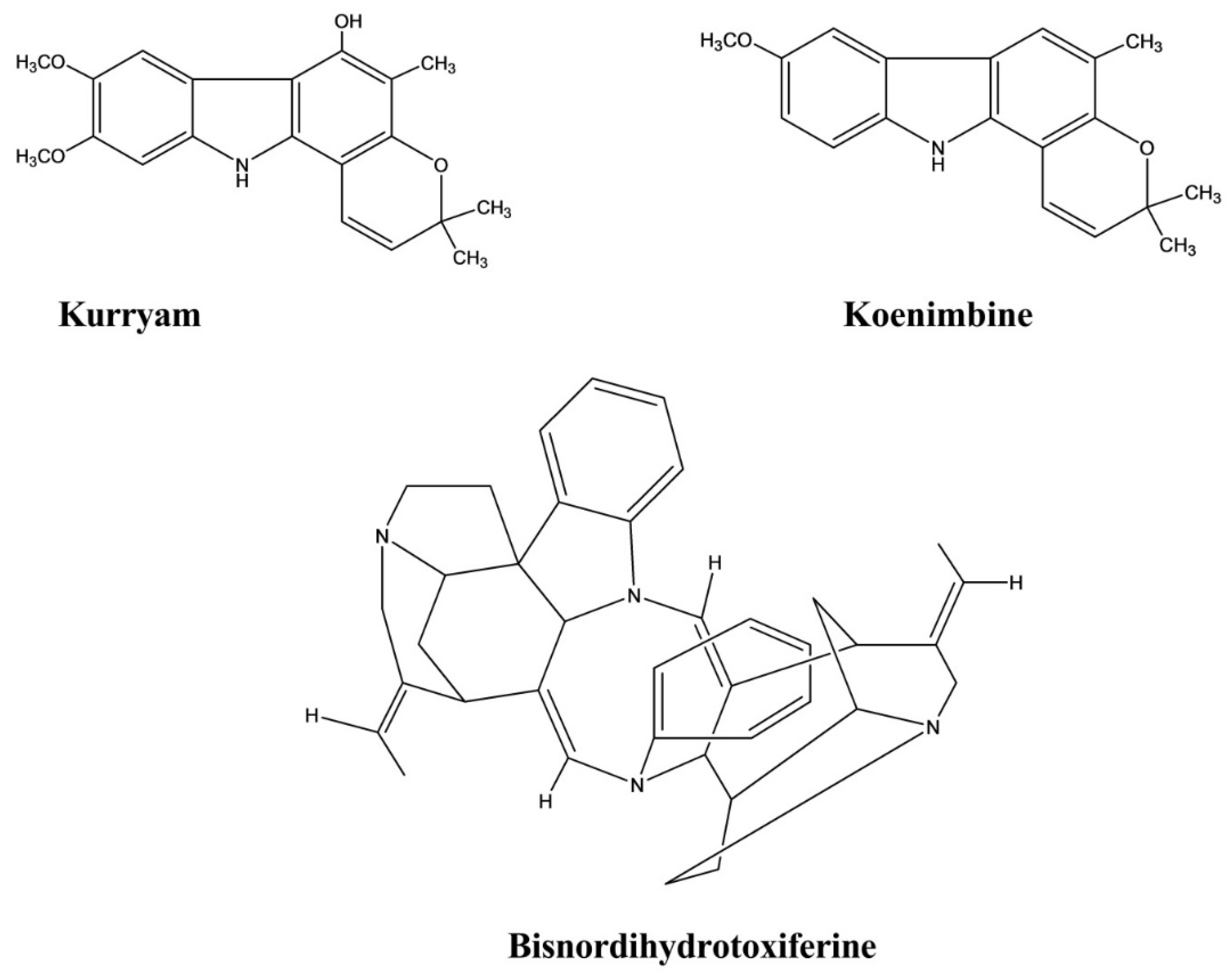
| Kurryam | Murraya koenigii | 10, 30, and 50 mg/kg | Rat | Castor oil-induced test | Antidiarrheal | [45] |
| Koenimbine | Murraya koenigii | 10, 30, and 50 mg/kg | Rat | Castor oil-induced test | Antidiarrheal | [45] |
| Bisnordihydrotoxiferine | Strychnos trinervis | Intraperitoneal, 3.12–25.00 mg/kg | Rat, Mice | Castor oil, Magnesium sulfate, and Arachidonic acid-induced diarrhea test | Antidiarrheal | [46] |
| Trinervine | Strychnos trinervis | - | Rat fundic strip, Guinea-pig ileum | Arachidonic acid, 5-hydroxytryptamine, Histamine, and Carbachol mediated contractions | Spasmolytic | [47] |
| Bisnordihydrotoxiferine | Strychnos diuaricuns | - | Rat uterus Guinea-pig ileum | Acetylcholine, Oxytocin-induced contraction, and Histamine-induced contractions | Spasmolytic | [48] |
| Normacusine B | Strychnos atlantica | 0.1, 0.3, 1.0, and 3.0 μM | Rat aorta | Phenylephrine and Serotonin-induced contractions. | Spasmolytic | [49] |
| Harmine | Perganum harmala | 1–100 μM | Guinea-Pig Trachea | Histamine, Carbachol, and KCl-induced contractions | Spasmolytic | [50] |
| Harmane | Perganum harmala | 1–100 μM | Guinea-Pig Trachea | Histamine, Carbachol, and KCl-induced contractions | Spasmolytic | [50] |
| Harmaline | Perganum harmala | 1–100 Μm | Guinea-Pig Trachea | Histamine, Carbachol, and KCl-induced contractions | Spasmolytic | [50] |
| Ramiflorine A, B | Aspidosperma ramiflorum | - | Parasite | Antileishmanial | [51] | |
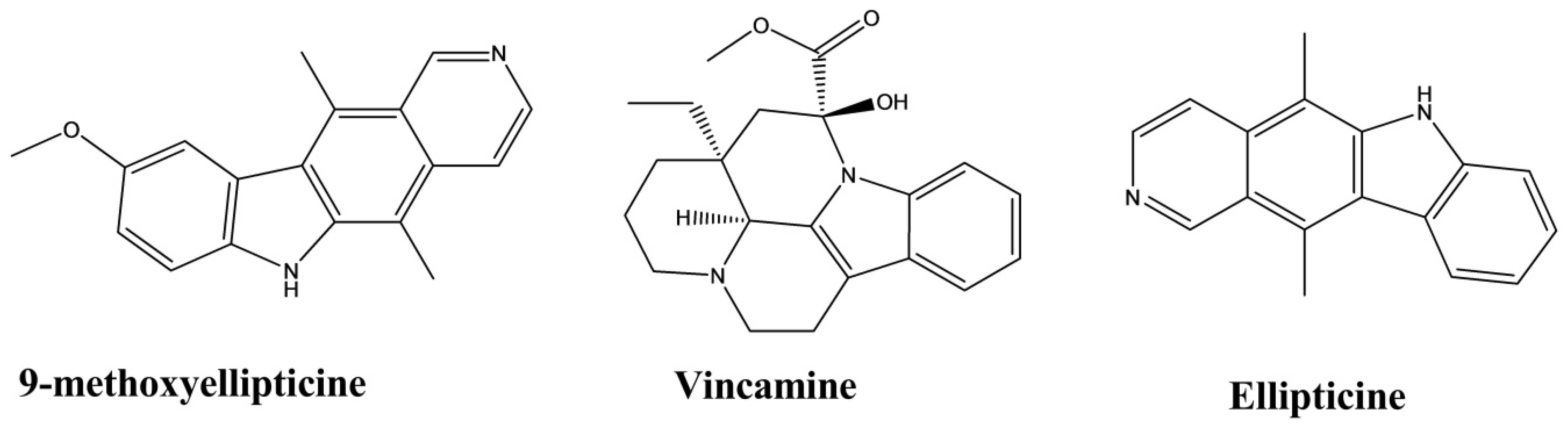
| Ellipticine | Ochrosia borbonica | 0.01–10 µmol·L−1 | Mouse fibroblast cells | Triglyceride assay | Lipid-lowering | [52] |
| 9-methoxyellipticine | Ochrosia borbonica | 0.01–10 µmol·L−1 | Mouse fibroblast cells | Triglyceride assay | Lipid-lowering | [52] |
| Vincamine | Vinca minor | Oral, 20 and 30 mg/kg | Rat | Lipid-lowering | [53,54] | |
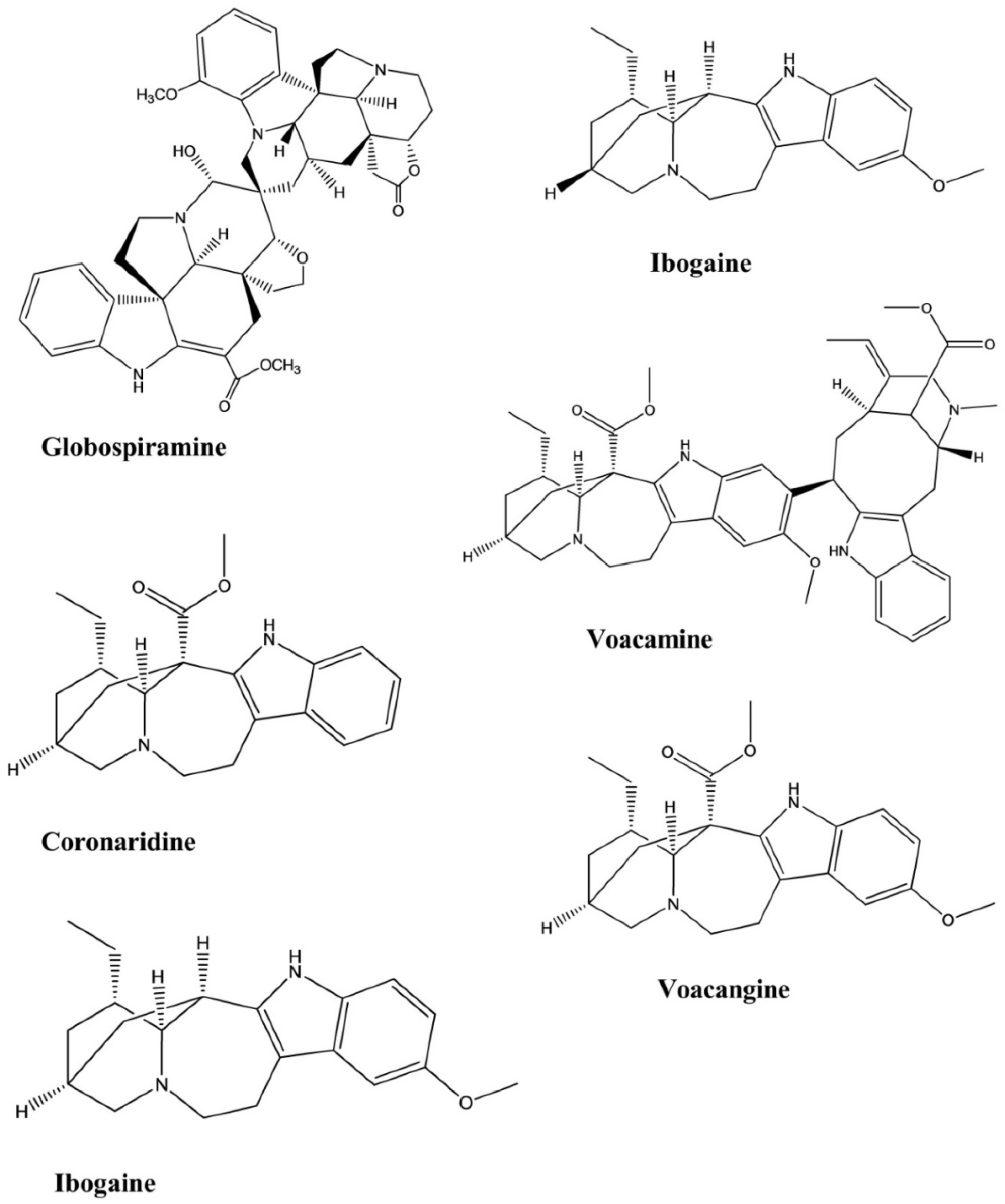
| Coronaridine | Tabernaemontana ternifolia | - | Bacteria | Microplate Alamar blue assay | Antimycobacterial | [55] |
| Globospiramine | Voacanga globosa | - | Bacteria | Microplate Alamar blue assay and Low-oxygen recovery assay | Antimycobacterial | [56] |
| Ibogaine | Tabernaemontana citrifolia | - | Bacteria | Bactec radiometric methodology | Antimycobacterial | [57] |
| Voacangine | Tabernaemontana citrifolia | - | Bacteria | Bactec radiometric methodology | Antimycobacterial | [57] |
| Voacamine | Tabernaemontana arborea. | - | Bacteria | Resazurin microtiter assay | Antimycobacterial | [58] |
| Parameters | Compound Name | ||||
|---|---|---|---|---|---|
| Brucine | Harmane | Vindoline | Mitragynine | 7-OH-mitragynine | |
| Administration Route | Oral, IV | Oral, IV | Oral, IV | Oral | Oral |
| Oral Bioavailability | 40.31%–47.15% | 19.41% | 5.4% | - | - |
| AUC | Ratio: 1:1.9:5.3 (at different doses) | - | Oral: 606.3 ng/mL h, IV: 2245.7 (first dose), 2258.0 (second dose) ng/mL h | - | - |
| Cmax | 929.22–1451.58 μg/L | Oral: 1059.56 ± 91.06 ng/mL, IV: 583.19 ng/mL | Oral: 606.6 ng/mL, IV: 1595.9 (first dose), 2913.9 ng/mL (second dose) | 0.63 ± 0.18 µg/mL | - |
| Tmax | 0.3–0.5 h | Oral: 0.23 ± 0.06 h, IV: 0.03 h | Oral: 0.3 h | 1.83 ± 1.25 h | - |
| t1/2 | - | - | Oral: 0.5 h IV: 1.0 h (first dose), 1.4 h (second dose) | - | 24 min |
| Vd | - | - | Oral; 21.6 L/kg IV: 2.0 L/kg (first dose), 3.3 L/kg (second dose) | 89.50 ± 30.30 L/kg | - |
| CL | - | - | Oral: 26.6 L/h/kg IV: 1.4 L/h/kg (first dose), 1.4 L/h/kg (second dose) | - | 43.2 ± 3.5 mL/min/kg |
| References | [60] | [64] | [63] | [61] | [62] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Omar, F.; Tareq, A.M.; Alqahtani, A.M.; Dhama, K.; Sayeed, M.A.; Emran, T.B.; Simal-Gandara, J. Plant-Based Indole Alkaloids: A Comprehensive Overview from a Pharmacological Perspective. Molecules 2021, 26, 2297. https://doi.org/10.3390/molecules26082297
Omar F, Tareq AM, Alqahtani AM, Dhama K, Sayeed MA, Emran TB, Simal-Gandara J. Plant-Based Indole Alkaloids: A Comprehensive Overview from a Pharmacological Perspective. Molecules. 2021; 26(8):2297. https://doi.org/10.3390/molecules26082297
Chicago/Turabian StyleOmar, Faisal, Abu Montakim Tareq, Ali M. Alqahtani, Kuldeep Dhama, Mohammed Abu Sayeed, Talha Bin Emran, and Jesus Simal-Gandara. 2021. "Plant-Based Indole Alkaloids: A Comprehensive Overview from a Pharmacological Perspective" Molecules 26, no. 8: 2297. https://doi.org/10.3390/molecules26082297
APA StyleOmar, F., Tareq, A. M., Alqahtani, A. M., Dhama, K., Sayeed, M. A., Emran, T. B., & Simal-Gandara, J. (2021). Plant-Based Indole Alkaloids: A Comprehensive Overview from a Pharmacological Perspective. Molecules, 26(8), 2297. https://doi.org/10.3390/molecules26082297









