Antifungal Properties of Essential Oils and Their Compounds for Application in Skin Fungal Infections: Conventional and Nonconventional Approaches
Abstract
1. Introduction
2. Results
3. Discussion
3.1. EOs in Conventional Approaches
3.2. EOs in Nonconventional Approaches
3.3. EOs in Clinical Interventions
3.4. EOs in Other Nonconventional Approaches and Their Advantages
4. Materials and Methods
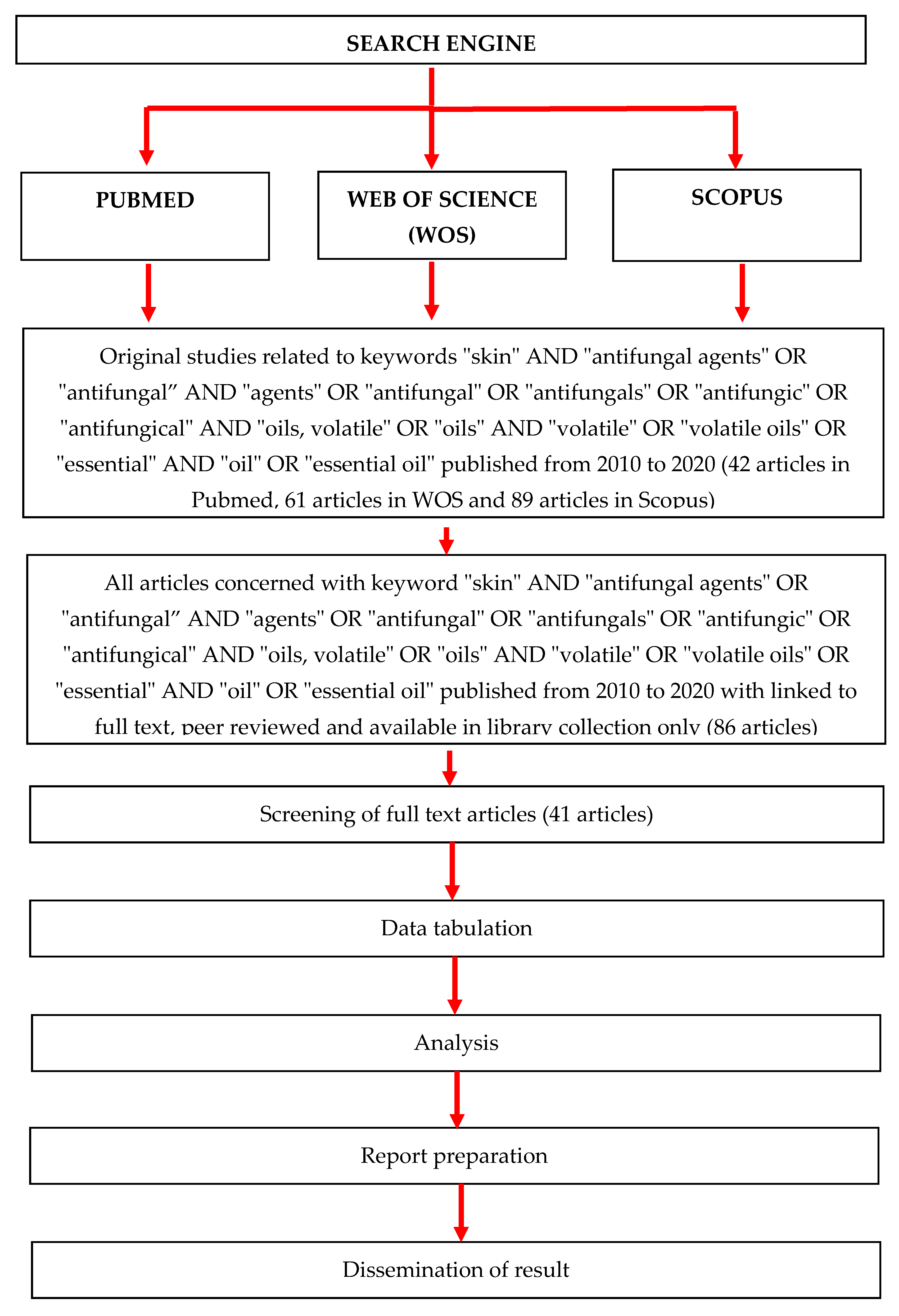
Search Strategy
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
List of Abbreviations
| ATCC | American Type Culture Collection |
| BTEO | EO of B. tripartita |
| BP | British Pharmacopoeia method |
| CECT | Colección Española de Cultivos Tipo |
| CLZ-NLC | Clotrimazole- nanostructured lipid carriers |
| CNS | Central nervous systems |
| CD | Cyclodextrin |
| DGIZ | Diameter of the growth inhibition zone |
| EO | Essential oil |
| EUCAST | European committee on antimicrobial susceptibility testing |
| FGI | Fungal growth index |
| FT-IR | Fourier Transformed- Infrared spectroscopy |
| GC-FID | Gas chromatography-flame ionisation detector |
| GC-MS | Gas chromatography-mass spectrometry |
| IZD | Different inhibition zone diameter |
| KOH | Potassium hydroxide |
| LGEO | Cymbopogon citratus EO |
| LPS | Lipopolysaccharide |
| MFC | Minimum fungicidal concentrations |
| MIC | Minimum inhibitory concentrations |
| MLC | Minimum lethal concentrations |
| MTT | 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide |
| NLC | Clotrimazole-loaded nanoparticles |
| NO | Nitric oxide |
| PE | Pickering emulsion |
| PTCC | Persian Type Culture Collection |
| PV | Pityriasis versicolor |
| RCT | Randomised controlled trial |
| ROS | Reactive oxygen species |
| SEM | Scanning electron microscopy |
| ZOI | Zone of inhibition test |
References
- Guarner, J.; Brandt, M.E. Histopathologic diagnosis of fungal infections in the 21st century. Clin. Microbiol. Rev. 2011, 24, 247–280. [Google Scholar] [CrossRef]
- Natu, K.N.; Tatke, P.A. Essential oils—Prospective candidates for antifungal treatment? J. Essent. Oil Res. 2019, 31, 347–360. [Google Scholar] [CrossRef]
- Warnock, D.W. Trends in the epidemiology of invasive fungal infections. Nihon Ishinkin Gakkai Zasshi Jpn. J. Med. Mycol. 2007, 48, 1–12. [Google Scholar] [CrossRef]
- Yoon, H.J.; Choi, H.Y.; Kim, Y.K.; Song, Y.J.; Ki, M. Prevalence of fungal infections using National Health Insurance data from 2009–2013, South Korea. Epidemiol. Health 2014, 36, 1–10. [Google Scholar] [CrossRef]
- Weiskopf, D.; Weinberger, B.; Grubeck-Loebenstein, B. The aging of the immune system. Transpl. Int. 2009, 22, 1041–1050. [Google Scholar] [CrossRef]
- Singh, N. Trends in the epidemiology of opportunistic fungal infections: Predisposing factors and the impact of antimicrobial use practices. Clin. Infect. Dis. 2001, 33, 1692–1696. [Google Scholar] [CrossRef] [PubMed]
- Nucci, M.; Marr, K.A. Emerging fungal diseases. Clin. Infect. Dis. 2005, 41, 521–526. [Google Scholar] [CrossRef]
- Riscili, B.P.; Wood, K.L. Noninvasive pulmonary Aspergillus infections. Clin. Chest Med. 2009, 30, 315–335, vii. [Google Scholar] [CrossRef]
- Garbino, D.J. Aspergillosis. In Orphanet Encyclopedia; Lew, D., Ed.; Orphanet: Paris, France, 2004; pp. 1–7. [Google Scholar]
- Dignani, M.C.; Anaissie, E. Human fusariosis. Clin. Microbiol. Infect. 2004, 10 (Suppl. 1), 67–75. [Google Scholar] [CrossRef] [PubMed]
- Godoy, P.; Nunes, E.; Silva, V.; Tomimori-Yamashita, J.; Zaror, L.; Fischman, O. Onychomycosis caused by Fusarium solani and Fusarium oxysporum in São Paulo, Brazil. Mycopathologia 2004, 157, 287–290. [Google Scholar] [CrossRef]
- Brilhante, R.; Cordeiro, R.; Medrano, D.; Rocha, M.; Monteiro, A.; Cavalcante, C.; Meireles, T.; Sidrim, J. Onychomycosis in Ceará (Northeast Brazil): Epidemiological and laboratory aspects. Mem. Inst. Oswaldo Cruz 2005, 100, 131–135. [Google Scholar] [CrossRef] [PubMed]
- Ninet, B.; Jan, I.; Bontems, O.; Léchenne, B.; Jousson, O.; Lew, D.; Schrenzel, J.; Panizzon, R.G.; Monod, M. Molecular identification of Fusarium species in onychomycoses. Dermatology 2005, 210, 21–25. [Google Scholar] [CrossRef]
- Vazquez, J.A.; Sobel, J.D. Candidiasis. In Essentials of Clinical Mycology; Kauffman, C.A., Pappas, P.G., Sobel, J.D., Dismukes, W.E., Eds.; Springer: New York, NY, USA, 2011; pp. 167–206. [Google Scholar]
- Darouiche, R.O. Candida in the ICU. Clin. Chest Med. 2009, 30, 287–293. [Google Scholar] [CrossRef] [PubMed]
- Bommanavar, S.; Gugwad, S.; Malik, N. Phenotypic switch: The enigmatic white-gray-opaque transition system of Candida albicans. J. Oral Maxillofac. Surg. Med. Pathol. 2017, 21, 82–86. [Google Scholar] [CrossRef]
- Chakrabarti, A.; Sood, P.; Rudramurthy, S.M.; Chen, S.; Kaur, H.; Capoor, M.; Chhina, D.; Rao, R.; Eshwara, V.K.; Xess, I.; et al. Incidence, characteristics and outcome of ICU-acquired candidemia in India. Intensiv. Care Med. 2015, 41, 285–295. [Google Scholar] [CrossRef]
- Noble, S.L.; Forbes, R.C.; Stamm, P.L. Diagnosis and management of common tinea infections. Am. Fam. Physician 1998, 58, 163–174, 177–178. [Google Scholar] [PubMed]
- Aguilar, C.V.J.; Alanio, A.S.B.; Frange, P.; Lanternier, F.; Lortholary, O. Antifungals. Available online: https://www.em-consulte.com/article/946740/antifongiques (accessed on 24 December 2020).
- Chanthaphon, S.; Chanthachum, S.; Hongpattarakere, T. Antimicrobial activities of essential oils and crude extracts from tropical Citrus spp. against food-related microorganisms. Songklanakarin J. Sci. Technol. 2008, 30, 125–131. [Google Scholar]
- Da Cruz Cabral, L.; Fernández Pinto, V.; Patriarca, A. Application of plant derived compounds to control fungal spoilage and mycotoxin production in foods. Int. J. Food Microbiol. 2013, 166, 1–14. [Google Scholar] [CrossRef]
- Sharifi-Rad, J.; Sureda, A.; Tenore, G.C.; Daglia, M.; Sharifi-Rad, M.; Valussi, M.; Tundis, R.; Sharifi-Rad, M.; Loizzo, M.R.; Ademiluyi, A.O.; et al. Biological Activities of Essential Oils: From Plant Chemoecology to Traditional Healing Systems. Molecules 2017, 22, 70. [Google Scholar] [CrossRef]
- Rajkowska, K.; Otlewska, A.; Kunicka-Styczyńska, A.; Krajewska, A. Candida albicans Impairments Induced by Peppermint and Clove Oils at Sub-Inhibitory Concentrations. Int. J. Mol. Sci. 2017, 18, 1307. [Google Scholar] [CrossRef]
- Tullio, V.; Roana, J.; Scalas, D.; Mandras, N. Evaluation of the Antifungal Activity of Mentha x piperita (Lamiaceae) of Pancalieri (Turin, Italy) Essential Oil and Its Synergistic Interaction with Azoles. Molecules 2019, 24, 3148. [Google Scholar] [CrossRef] [PubMed]
- Tullio, V.; Roana, J.; Scalas, D.; Mandras, N. Enhanced Killing of Candida krusei by Polymorphonuclear Leucocytes in the Presence of Subinhibitory Concentrations of Melaleuca alternifolia and “Mentha of Pancalieri” Essential Oils. Molecules 2019, 24, 3824. [Google Scholar] [CrossRef] [PubMed]
- Scalas, D.; Mandras, N.; Roana, J.; Tardugno, R.; Cuffini, A.M.; Ghisetti, V.; Benvenuti, S.; Tullio, V. Use of Pinus sylvestris L. (Pinaceae), Origanum vulgare L. (Lamiaceae), and Thymus vulgaris L. (Lamiaceae) essential oils and their main components to enhance itraconazole activity against azole susceptible/not-susceptible Cryptococcus neoformans strains. BMC Complement. Altern. Med. 2018, 18, 143. [Google Scholar] [CrossRef]
- D’Agostino, M.; Tesse, N.; Frippiat, J.P.; Machouart, M.; Debourgogne, A. Essential Oils and Their Natural Active Compounds Presenting Antifungal Properties. Molecules 2019, 24, 3713. [Google Scholar] [CrossRef] [PubMed]
- Pinto, E.; Pina-Vaz, C.; Salgueiro, L.; Gonçalves, M.J.; Costa-de-Oliveira, S.; Cavaleiro, C.; Palmeira, A.; Rodrigues, A.; Martinez-de-Oliveira, J. Antifungal activity of the essential oil of Thymus pulegioides on Candida, Aspergillus and dermatophyte species. J. Med. Microbiol. 2006, 55, 1367–1373. [Google Scholar] [CrossRef]
- Omidbeygi, M.; Barzegar, M.; Hamidi, Z.; Naghdibadi, H. Antifungal activity of thyme, summer savory and clove essential oils against Aspergillus flavus in liquid medium and tomato paste. Food Control 2007, 18, 1518–1523. [Google Scholar] [CrossRef]
- Rasooli, I.; Rezaei, M.B.; Allameh, A. Growth inhibition and morphological alterations of Aspergillus niger by essential oils from Thymus eriocalyx and Thymus x-porlock. Food Control 2006, 17, 359–364. [Google Scholar] [CrossRef]
- Khan, M.S.; Ahmad, I. In vitro antifungal, anti-elastase and anti-keratinase activity of essential oils of Cinnamomum-, Syzygium- and Cymbopogon-species against Aspergillus fumigatus and Trichophyton rubrum. Phytomedicine 2011, 19, 48–55. [Google Scholar] [CrossRef]
- Khan, M.S.; Ahmad, I. Antifungal activity of essential oils and their synergy with fluconazole against drug-resistant strains of Aspergillus fumigatus and Trichophyton rubrum. Appl. Microbiol. Biotechnol. 2011, 90, 1083–1094. [Google Scholar] [CrossRef]
- Angelini, P.; Pagiotti, R.; Menghini, A.; Vianello, B. Antimicrobial activities of various essential oils against foodborne pathogenic or spoilage moulds. Ann. Microbiol. 2006, 56, 65–69. [Google Scholar] [CrossRef]
- Vilela, G.R.; de Almeida, G.S.; D’Arce, M.A.B.R.; Moraes, M.H.D.; Brito, J.O.; da Silva, M.F.d.G.; Silva, S.C.; de Stefano Piedade, S.M.; Calori-Domingues, M.A.; da Gloria, E.M. Activity of essential oil and its major compound, 1, 8-cineole, from Eucalyptus globulus Labill., against the storage fungi Aspergillus flavus Link and Aspergillus parasiticus Speare. J. Stored Prod. Res. 2009, 45, 108–111. [Google Scholar] [CrossRef]
- Uniyal, V.; Bhatt, R.; Saxena, S.; Talwar, A. Antifungal activity of essential oils and their volatile constituents against respiratory tract pathogens causing Aspergilloma and Aspergillosis by gaseous contact. J. Appl. Nat. Sci. 2012, 4, 65–70. [Google Scholar] [CrossRef]
- Verma, R.K.; Chaurasia, L.; Kumar, M. Antifungal activity of essential oils against selected building fungi. Indian J. Nat. Prod. Resour. 2011, 2, 448–451. [Google Scholar]
- Pinto, E.; Vale-Silva, L.; Cavaleiro, C.; Salgueiro, L. Antifungal activity of the clove essential oil from Syzygium aromaticum on Candida, Aspergillus and dermatophyte species. J. Med. Microbiol. 2009, 58, 1454–1462. [Google Scholar] [CrossRef]
- Naeini, A.; Shokri, H. Chemical composition and in vitro antifungal activity of the essential oil from Cuminum cyminum against various Aspergillus strains. J. Med. Plants Res. 2012, 6, 1702–1706. [Google Scholar] [CrossRef]
- Kanafani, Z.A.; Perfect, J.R. Antimicrobial resistance: Resistance to antifungal agents: Mechanisms and clinical impact. Clin. Infect. Dis. 2008, 46, 120–128. [Google Scholar] [CrossRef]
- Low, C.Y.; Rotstein, C. Emerging fungal infections in immunocompromised patients. F1000 Med. Rep. 2011, 3, 14. [Google Scholar] [CrossRef] [PubMed]
- Mondello, F.; De Bernardis, F.; Girolamo, A.; Salvatore, G.; Cassone, A. In vitro and in vivo activity of tea tree oil against azole-susceptible and -resistant human pathogenic yeasts. J. Antimicrob. Chemother. 2003, 51, 1223–1229. [Google Scholar] [CrossRef]
- Stringaro, A.; Colone, M.; Angiolella, L. Antioxidant, Antifungal, Antibiofilm, and Cytotoxic Activities of Mentha spp. Essential Oils. Medicines 2018, 5, 112. [Google Scholar] [CrossRef] [PubMed]
- D’Auria, F.D.; Tecca, M.; Strippoli, V.; Salvatore, G.; Battinelli, L.; Mazzanti, G. Antifungal activity of Lavandula angustifolia essential oil against Candida albicans yeast and mycelial form. Med. Mycol. 2005, 43, 391–396. [Google Scholar] [CrossRef] [PubMed]
- Behmanesh, F.; Pasha, H.; Sefidgar, A.A.; Taghizadeh, M.; Moghadamnia, A.A.; Adib Rad, H.; Shirkhani, L. Antifungal Effect of Lavender Essential Oil (Lavandula angustifolia) and Clotrimazole on Candida albicans: An In Vitro Study. Scientifica (Cairo) 2015, 2015, 1–5. [Google Scholar] [CrossRef]
- Minooeianhaghighi, M.H.; Sepehrian, L.; Shokri, H. Antifungal effects of Lavandula binaludensis and Cuminum cyminum essential oils against Candida albicans strains isolated from patients with recurrent vulvovaginal candidiasis. J. Mycol. Med. 2017, 27, 65–71. [Google Scholar] [CrossRef]
- Dhifi, W.; Bellili, S.; Jazi, S.; Bahloul, N.; Mnif, W. Essential Oils’ Chemical Characterization and Investigation of Some Biological Activities: A Critical Review. Medicines 2016, 3, 25. [Google Scholar] [CrossRef] [PubMed]
- Dias Ferreira, F.; Mossini, S.A.; Dias Ferreira, F.M.; Arrotéia, C.C.; da Costa, C.L.; Nakamura, C.V.; Machinski, M., Jr. The inhibitory effects of Curcuma longa L. essential oil and curcumin on Aspergillus flavus link growth and morphology. Sci. World J. 2013, 2013, 1–6. [Google Scholar] [CrossRef]
- Tolouee, M.; Alinezhad, S.; Saberi, R.; Eslamifar, A.; Zad, S.J.; Jaimand, K.; Taeb, J.; Rezaee, M.B.; Kawachi, M.; Shams-Ghahfarokhi, M.; et al. Effect of Matricaria chamomilla L. flower essential oil on the growth and ultrastructure of Aspergillus niger van Tieghem. Int. J. Food Microbiol. 2010, 139, 127–133. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.; Ahmad, A.; Akhtar, F.; Yousuf, S.; Xess, I.; Khan, L.A.; Manzoor, N. Ocimum sanctum essential oil and its active principles exert their antifungal activity by disrupting ergosterol biosynthesis and membrane integrity. Res. Microbiol. 2010, 161, 816–823. [Google Scholar] [CrossRef]
- Chen, Y.; Zeng, H.; Tian, J.; Ban, X.; Ma, B.; Wang, Y. Dill (Anethum graveolens L.) seed essential oil induces Candida albicans apoptosis in a metacaspase-dependent manner. Fungal Biol. 2014, 118, 394–401. [Google Scholar] [CrossRef] [PubMed]
- Kumar, R.; Mishra, A.K.; Dubey, N.K.; Tripathi, Y.B. Evaluation of Chenopodium ambrosioides oil as a potential source of antifungal, antiaflatoxigenic and antioxidant activity. Int. J. Food Microbiol. 2007, 115, 159–164. [Google Scholar] [CrossRef]
- Yahyaraeyat, R.; Khosravi, A.; Shahbazzadeh, D.; Khalaj, V. The potential effects of Zataria multiflora Boiss essential oil on growth, aflatoxin production and transcription of aflatoxin biosynthesis pathway genes of toxigenic Aspergillus parasiticus. Braz. J. Microbiol. 2013, 44, 649–655. [Google Scholar] [CrossRef]
- De Oliveira Lima, M.I.; Araújo de Medeiros, A.C.; Souza Silva, K.V.; Cardoso, G.N.; de Oliveira Lima, E.; de Oliveira Pereira, F. Investigation of the antifungal potential of linalool against clinical isolates of fluconazole resistant Trichophyton rubrum. J. Mycol. Med. 2017, 27, 195–202. [Google Scholar] [CrossRef]
- Shreaz, S.; Shiekh, R.A.; Raja, V.; Wani, W.A.; Behbehani, J.M. Impaired ergosterol biosynthesis mediated fungicidal activity of Co(II) complex with ligand derived from cinnamaldehyde. Chem. Biol. Interact. 2016, 247, 64–74. [Google Scholar] [CrossRef] [PubMed]
- Kurita, N.; Koike, S. Synergistic Antimicrobial Effect of Ethanol, Sodium Chloride, Acetic Acid and Essential Oil Components. Agric. Biol. Chem. 1983, 47, 67–75. [Google Scholar] [CrossRef]
- Satpathy, B.; Sahoo, M.; Sahoo, P.; Patra, S. Formulation and evaluation of herbal gel containing essential oils of piper betle against skin infecting pathogens. Int. J. Res. Pharm. Sci. 2011, 2, 373–378. [Google Scholar]
- Sharma, R.; Pathak, K. Polymeric nanosponges as an alternative carrier for improved retention of econazole nitrate onto the skin through topical hydrogel formulation. Pharm. Dev. Technol. 2011, 16, 367–376. [Google Scholar] [CrossRef]
- Kozics, K.; Bučková, M.; Puškárová, A.; Kalászová, V.; Cabicarová, T.; Pangallo, D. The Effect of Ten Essential Oils on Several Cutaneous Drug-Resistant Microorganisms and Their Cyto/Genotoxic and Antioxidant Properties. Molecules 2019, 24, 4570. [Google Scholar] [CrossRef] [PubMed]
- Mahboubi, M.; Kazempour, N. The antifungal activity of Artemisia sieberi essential oil from different localities of Iran against dermatophyte fungi. J. Mycol. Med. 2015, 25, e65–e71. [Google Scholar] [CrossRef] [PubMed]
- Khoury, M.; Stien, D.; Eparvier, V.; Ouaini, N.; El Beyrouthy, M. Report on the medicinal use of eleven Lamiaceae species in Lebanon and rationalization of their antimicrobial potential by examination of the chemical composition and antimicrobial activity of their essential oils. Evid. Based Complement. Altern. Med. 2016, 2016, 1–17. [Google Scholar] [CrossRef]
- Mary, H.; Tina, A.V.; Jeeja, K.J.; Abiramy, M. Phytochemical analysis and anticancer activity of essential oil from Myristica fragrans. Int. J. Curr. Pharm. Res. 2012, 2, 188–198. [Google Scholar]
- Singh, P.; Bundiwale, R.; Dwivedi, L. In-Vitro study of antifungal activity of various commercially available itra (Volatile plant oil) against the keratinophilic fungi isolated from soil. Int. J. Pharma Bio Sci. 2011, 2, 178–184. [Google Scholar]
- Gonçalves, M.; Cruz, M.; Cavaleiro, C.; Lopes, M.; Salgueiro, L. Chemical, antifungal and cytotoxic evaluation of the essential oil of Thymus zygis subsp. sylvestris. Ind. Crop. Prod. 2010, 32, 70–75. [Google Scholar] [CrossRef]
- Mahboubi, M.; Kazempour, N. Comparison of antifungal activity of different extracts from Satureja khuzistanica Jamzad against dermatophytes. Biharean Biol. 2015, 9, 105–107. [Google Scholar]
- Valente, J.; Zuzarte, M.; Resende, R.; Gonçalves, M.; Cavaleiro, C.; Pereira, C.; Cruz, M.; Salgueiro, L. Daucus carota subsp. gummifer essential oil as a natural source of antifungal and anti-inflammatory drugs. Ind. Crop. Prod. 2015, 65, 361–366. [Google Scholar] [CrossRef]
- Abu-Darwish, M.; Cabral, C.; Ferreira, I.; Gonçalves, M.; Cavaleiro, C.; Cruz, M.; Al-Bdour, T.; Salgueiro, L. Essential oil of common sage (Salvia officinalis L.) from Jordan: Assessment of safety in mammalian cells and its antifungal and anti-inflammatory potential. BioMed Res. Int. 2013, 2013, 1–9. [Google Scholar] [CrossRef]
- Fahed, L.; Khoury, M.; Stien, D.; Ouaini, N.; Eparvier, V.; El Beyrouthy, M. Essential oils composition and antimicrobial activity of six conifers harvested in Lebanon. Chem. Biodivers. 2017, 14, e1600235. [Google Scholar] [CrossRef] [PubMed]
- Tavares, A.C.; Gonçalves, M.J.; Cruz, M.T.; Cavaleiro, C.; Lopes, M.C.; Canhoto, J.; Salgueiro, L.R. Essential oils from Distichoselinum tenuifolium: Chemical composition, cytotoxicity, antifungal and anti-inflammatory properties. J. Ethnopharmacol. 2010, 130, 593–598. [Google Scholar] [CrossRef]
- Fajinmi, O.; Kulkarni, M.; Benická, S.; Zeljković, S.Ć.; Doležal, K.; Tarkowski, P.; Finnie, J.; Van Staden, J. Antifungal activity of the volatiles of Agathosma betulina and Coleonema album commercial essential oil and their effect on the morphology of fungal strains Trichophyton rubrum and T. mentagrophytes. S. Afr. J. Bot. 2019, 122, 492–497. [Google Scholar] [CrossRef]
- Fajinmi, O.O.; Grúz, J.; Tarkowski, P.; Kulkarni, M.G.; Finnie, J.F.; Van Staden, J. Antifungal and antioxidant activities of Coleonema album and C. pulchellum against skin diseases. Pharm. Biol. 2017, 55, 1249–1255. [Google Scholar] [CrossRef]
- Canales-Martinez, M.; Rivera-Yañez, C.; Salas-Oropeza, J.; Lopez, H.; Jimenez-Estrada, M.; Rosas-Lopez, R.; Duran, D.; Flores, C.; Hernandez, L.; Rodriguez-Monroy, M. Antimicrobial activity of Bursera morelensis ramírez essential oil. Afr. J. Tradit. Complement. Altern. Med. 2017, 14, 74–82. [Google Scholar]
- Osho, A.; Adetunji, T.; Fayemi, S.O.; Moronkola, D.O. Antimicrobial activity of essential oils of Physalis angulata. L. Afr. J. Tradit. Complement. Altern. Med. 2010, 7, 303–306. [Google Scholar] [CrossRef]
- Rezgui, M.; Majdoub, N.; Mabrouk, B.; Baldisserotto, A.; Bino, A.; Kaab, L.B.; Manfredini, S. Antioxidant and antifungal activities of marrubiin, extracts and essential oil from Marrubium vulgare L. against pathogenic dermatophyte strains. J. Mycol. Med. 2020, 100927. [Google Scholar] [CrossRef] [PubMed]
- Nyegue, M.A.; Ndoyé-Foe, F.-C.; Essama, S.R.; Hockmeni, T.; Etoa, F.-X.; Menut, C. Chemical composition of essential oils of Eugenia caryophylla and Mentha sp cf piperita and their in vitro antifungal activities on six human pathogenic fungi. Afr. J. Tradit. Complement. Altern. Med. 2014, 11, 40–46. [Google Scholar] [CrossRef][Green Version]
- Cabral, C.; Francisco, V.; Cavaleiro, C.; Gonçalves, M.J.; Cruz, M.T.; Sales, F.; Batista, M.T.; Salgueiro, L. Essential Oil of Juniperus communis subsp. alpina (Suter) Čelak Needles: Chemical Composition, Antifungal Activity and Cytotoxicity. Phytother. Res. 2012, 26, 1352–1357. [Google Scholar] [CrossRef]
- Prakash, R.; Agarwal, S.; Srivastava, A.; Nigam, V. GC-MS Analysis of essential oil of Turmeric rhizome and its activity against Sporothrix schenckii fungus. Orient. J. Chem. 2015, 31, 2213–2214. [Google Scholar] [CrossRef]
- Dias, N.; Dias, M.; Cavaleiro, C.; Sousa, M.; Lima, N.; Machado, M. Oxygenated monoterpenes-rich volatile oils as potential antifungal agents for dermatophytes. Nat. Prod. Res. 2017, 31, 460–464. [Google Scholar] [CrossRef] [PubMed]
- Sadhasivam, S.; Palanivel, S.; Ghosh, S. Synergistic antimicrobial activity of Boswellia serrata Roxb. ex Colebr. (Burseraceae) essential oil with various azoles against pathogens associated with skin, scalp and nail infections. Lett. Appl. Microbiol. 2016, 63, 495–501. [Google Scholar] [CrossRef]
- Białoń, M.; Krzyśko-Łupicka, T.; Koszałkowska, M.; Wieczorek, P.P. The influence of chemical composition of commercial lemon essential oils on the growth of Candida strains. Mycopathologia 2014, 177, 29–39. [Google Scholar] [CrossRef] [PubMed]
- Rahman, A.; Al-Reza, S.M.; Siddiqui, S.A.; Chang, T.; Kang, S.C. Antifungal potential of essential oil and ethanol extracts of Lonicera japonica Thunb. against dermatophytes. EXCLI J. 2014, 13, 427–436. [Google Scholar]
- Tangarife Castaño, V.; Roa Linares, V.; Betancur, L.; Durán, D.; Stashenko, E.; Mesa, A. Antifungal activity of Verbenaceae and Labiatae families essential oils. Pharmacologyonline 2012, 1, 133–145. [Google Scholar]
- Sharma, R.; Sharma, G.; Sharma, M. Anti-Malassezia furfur activity of essential oils against causal agent of Pityriasis versicolor disease. Afr. J. Pharm. Pharmacol. 2012, 6, 979–983. [Google Scholar] [CrossRef]
- da Cruz, R.C.; Denardi, L.B.; Mossmann, N.J.; Piana, M.; Alves, S.H.; de Campos, M.M. Antimicrobial Activity and Chromatographic Analysis of Extracts from Tropaeolum pentaphyllum Lam. Tubers. Molecules 2016, 21, 566. [Google Scholar] [CrossRef] [PubMed]
- Tabassum, N.M.V. Antimicrobial activity of medicinal oil plants against human pathogens from Hyderabad Karnataka Region. Int. J. Pharm. Sci. Rev. Res. 2014, 26, 182–188. [Google Scholar]
- Oladimeji, F.A.; Akinkunmi, E.O.; Raheem, A.I.; Abiodun, G.O.; Bankole, V.O. Evaluation of topical antimicrobial ointment formulations of essential oil of Lippia multiflora moldenke. Afr. J. Tradit. Complement. Altern. Med. 2015, 12, 135–144. [Google Scholar] [CrossRef]
- Tomczykowa, M.; Wróblewska, M.; Winnicka, K.; Wieczorek, P.; Majewski, P.; Celińska-Janowicz, K.; Sawczuk, R.; Miltyk, W.; Tryniszewska, E.; Tomczyk, M. Novel gel formulations as topical carriers for the essential oil of Bidens tripartita for the treatment of candidiasis. Molecules 2018, 23, 2517. [Google Scholar] [CrossRef] [PubMed]
- Carbone, C.; Teixeira, M.d.C.; Sousa, M.d.C.; Martins-Gomes, C.; Silva, A.M.; Souto, E.M.B.; Musumeci, T. Clotrimazole-Loaded mediterranean essential oils NLC: A synergic treatment of Candida skin infections. Pharmaceutics 2019, 11, 231. [Google Scholar] [CrossRef]
- Rabadia, A.G.; Kamat, S.; Kamat, D. Antifungal activity of essential oils against fluconazole resistant fungi. Int. J. Phytomed. 2011, 3, 506. [Google Scholar]
- Ali, S.; Khan, M.R.; Batool, R.; Maryam, S.; Majid, M. Wound healing potential of oil extracted from Parrotiopsis jacquemontiana (Decne) Rehder. J. Ethnopharmacol. 2019, 236, 354–365. [Google Scholar] [CrossRef] [PubMed]
- Jain, N.; Sharma, M.; Joshi, S.; Kaushik, U. Chemical composition, toxicity and antidermatophytic activity of essential oil of Trachyspermum ammi. Indian J. Pharm. Sci. 2018, 80, 135–142. [Google Scholar] [CrossRef]
- Boukhatem, M.N.; Ferhat, M.A.; Kameli, A.; Saidi, F.; Kebir, H.T. Lemon grass (Cymbopogon citratus) essential oil as a potent anti-inflammatory and antifungal drugs. Libyan J. Med. 2014, 9, 1–10. [Google Scholar] [CrossRef]
- Njateng, G.; Kuiate, J.; Gatsing, D.; Tamokou, J.; Mouokeu, R.; Kuete, V. Antidermatophytic activity and dermal toxicity of essential oil from the leaves of Ageratum houstonianum (Asteraceae). J. Biol. Sci. 2010, 10, 448–454. [Google Scholar] [CrossRef][Green Version]
- Aldawsari, H.M.; Badr-Eldin, S.M.; Labib, G.S.; El-Kamel, A.H. Design and formulation of a topical hydrogel integrating lemongrass-loaded nanosponges with an enhanced antifungal effect: In vitro/in vivo evaluation. Int. J. Nanomed. 2015, 10, 893–902. [Google Scholar]
- Gemeda, N.; Tadele, A.; Lemma, H.; Girma, B.; Addis, G.; Tesfaye, B.; Abebe, A.; Gemechu, W.; Yirsaw, K.; Teka, F. Development, characterization, and evaluation of novel broad-spectrum antimicrobial topical formulations from Cymbopogon martini (Roxb.) W. Watson essential oil. Evid. Based Complement. Altern. Med. 2018, 2018, 1–16. [Google Scholar] [CrossRef]
- Prasad, C.S.; Shukla, R.; Kumar, A.; Dubey, N.K. In vitro and in vivo antifungal activity of essential oils of Cymbopogon martini and Chenopodium ambrosioides and their synergism against dermatophytes. Mycoses 2010, 53, 123–129. [Google Scholar] [CrossRef]
- Pandey, K.P.; Mishra, R.K.; Kamran, A.; Mishra, P.; Bajaj, A.K.; Dikshit, A. Studies on antidermatophytic activity of waste leaves of Curcuma longa L. Physiol. Mol. Biol. Plants 2010, 16, 177–185. [Google Scholar] [CrossRef][Green Version]
- Barac, A.; Donadu, M.; Usai, D.; Spiric, V.T.; Mazzarello, V.; Zanetti, S.; Aleksic, E.; Stevanovic, G.; Nikolic, N.; Rubino, S. Antifungal activity of Myrtus communis against Malassezia sp. isolated from the skin of patients with pityriasis versicolor. Infection 2018, 46, 253–257. [Google Scholar] [CrossRef]
- Borda, L.J.; Wikramanayake, T.C. Seborrheic Dermatitis and Dandruff: A Comprehensive Review. J. Clin. Investig. Dermatol. 2015, 3, 1–22. [Google Scholar] [CrossRef]
- Pugliarello, S.; Cozzi, A.; Gisondi, P.; Girolomoni, G. Phenotypes of atopic dermatitis. JDDG J. Dtsch. Dermatol. Ges. 2011, 9, 12–20. [Google Scholar] [CrossRef]
- Gallitano, S.M.; Berson, D.S. How Acne Bumps Cause the Blues: The Influence of Acne Vulgaris on Self-Esteem. Int. J. Womens Dermatol. 2017, 4, 12–17. [Google Scholar] [CrossRef] [PubMed]
- Casadevall, A.; Pirofski, L.A. Host-Pathogen interactions: Redefining the basic concepts of virulence and pathogenicity. Infect. Immun. 1999, 67, 3703–3713. [Google Scholar] [CrossRef]
- Casadevall, A.; Pirofski, L.A. The damage-response framework of microbial pathogenesis. Nat. Rev. Microbiol. 2003, 1, 17–24. [Google Scholar] [CrossRef] [PubMed]
- Naggie, S.; Perfect, J.R. Molds: Hyalohyphomycosis, phaeohyphomycosis, and zygomycosis. Clin. Chest Med. 2009, 30, 337–353, vii–viii. [Google Scholar] [CrossRef] [PubMed]
- Kohler, J.; Hube, B.; Puccia, R.; Casadevall, A.; Perfect, J. Fungi that infect humans. Microbiol. Spectr. 2017, 5, 1–29. [Google Scholar] [CrossRef]
- Guruprasad, B.; Famna Roohi, N.; Gowda, D. A Review on Candidiasis resistance current drug development process in its prevention and treatment. Int. J. Res. Pharm. Sci. 2020, 11, 1073–1079. [Google Scholar] [CrossRef]
- Farjon, A.; Juniperus, L. Flora of Turkey and the East Aegean Islands; Davis, P.H., Cullen, J., Coode, M.J.E., Eds.; Ediburgh University Press: Ediburgh, UK, 2000; Volume 11, pp. 8–10. [Google Scholar]
- Shah, P.P.; Mello, P. A review of medicinal uses and pharmacological effects of Mentha piperita. Nat. Prod. Radiance 2004, 3, 214–221. [Google Scholar]
- Nurdjannah, N.; Bermawie, N. Clove. In Handbook of Herbs and Spices; Elsevier: Amsterdam, The Netherlands, 2001; pp. 154–163. [Google Scholar]
- Weedon, D. 25—Mycoses and algal infections. In Weedon’s Skin Pathology, 3rd ed.; Weedon, D., Ed.; Churchill Livingstone: Edinburgh, UK, 2010; pp. 581–606.e24. [Google Scholar]
- Karpiński, T.M. Essential Oils of Lamiaceae Family Plants as Antifungals. Biomolecules 2020, 10, 103. [Google Scholar] [CrossRef] [PubMed]
- Malik, A.; Siddique, M.; Sofi, P.; Butola, J. Ethnomedicinal practices and conservation status of medicinal plants of North Kashmir Himalayas. Res. J. Med. Plant 2011, 5, 515–530. [Google Scholar]
- Kumar, K.; Sharma, Y.P.; Manhas, R.; Bhatia, H. Ethnomedicinal plants of Shankaracharya Hill, Srinagar, J&K, India. J. Ethnopharmacol. 2015, 170, 255–274. [Google Scholar]
- Ali, S.; Khan, M.R.; Sajid, M. Protective potential of Parrotiopsis jacquemontiana (Decne) Rehder on carbon tetrachloride induced hepatotoxicity in experimental rats. Biomed. Pharmacother. 2017, 95, 1853–1867. [Google Scholar] [CrossRef]
- Bruni, R.; Medici, A.; Andreotti, E.; Fantin, C.; Muzzoli, M.; Dehesa, M.; Romagnoli, C.; Sacchetti, G. Chemical composition and biological activities of Ishpingo essential oil, a traditional Ecuadorian spice from Ocotea quixos (Lam.) Kosterm.(Lauraceae) flower calices. Food Chem. 2004, 85, 415–421. [Google Scholar] [CrossRef]
- Fox, L.T.; Mazumder, A.; Dwivedi, A.; Gerber, M.; du Plessis, J.; Hamman, J.H. In vitro wound healing and cytotoxic activity of the gel and whole-leaf materials from selected aloe species. J. Ethnopharmacol. 2017, 200, 1–7. [Google Scholar] [CrossRef]
- India, G.O. Ayurvedic Pharmacopoeia of India, Part 11999; Ministry of Health and Family Welfare, Department of Ayush: New Delhi, India, 2011; Volume 1, p. 170.
- Ishwar, S.; Singh, V. Antifungal properties of aqueous and organic solution extracts of seed plants against Aspergillus flavus and A. niger. Phytomorphology 2000, 50, 151–157. [Google Scholar]
- Singh, V.; Ali, M.; Saxena, R.; Shekhar, C.; Anand, D. Volatile constituents and antimicrobial and antifungal activities of immature green seeds of Trachyspermum ammi Linn. J. Essent. Oil Bear. Plants 2008, 11, 120–123. [Google Scholar] [CrossRef]
- Paul, S.; Dubey, R.; Maheswari, D.; Kang, S.C. Trachyspermum ammi (L.) fruit essential oil influencing on membrane permeability and surface characteristics in inhibiting food-borne pathogens. Food Control 2011, 22, 725–731. [Google Scholar] [CrossRef]
- Umar, S.; Asif, M.; Sajad, M.; Ansari, M.M.; Hussain, U.; Ahmad, W.; Siddiqui, S.A.; Ahmad, S.; Khan, H.A. Anti-Inflammatory and antioxidant activity of Trachyspermum ammi seeds in collagen induced arthritis in rats. Int. J. Drug Dev. Res. 2012, 4, 210–219. [Google Scholar]
- Roy, S.; Chaurvedi, P.; Chowdhary, A. Evaluation of antiviral activity of essential oil of Trachyspermum Ammi against Japanese encephalitis virus. Pharmacogn. Res. 2015, 7, 263–267. [Google Scholar] [CrossRef] [PubMed]
- Pozzatti, P.; Scheid, L.A.; Spader, T.B.; Atayde, M.L.; Santurio, J.M.; Alves, S.H. In vitro activity of essential oils extracted from plants used as spices against fluconazole-resistant and fluconazole-susceptible Candida spp. Can. J. Microbiol. 2008, 54, 950–956. [Google Scholar] [CrossRef] [PubMed]
- Gatsing, D.; Tchakoute, V.; Ngamga, D.; Kuiate, J.; Tamokou, J.d.D.; Nji-Nkah, B.; Tchouanguep, F.; Fodouop, S. In vitro antibacterial activity of Crinum purpurascens Herb. leaf extract against the Salmonella species causing typhoid fever and its toxicological evaluation. Iran. J. Med. Sci. 2009, 34, 126–136. [Google Scholar]
- Akhila, A. Essential Oil-Bearing Grasses: The Genus Cymbopogon; CRC Press: New York, NY, USA, 2009. [Google Scholar]
- Hood, J.R.; Wilkinson, J.M.; Cavanagh, H.M.A. Evaluation of Common Antibacterial Screening Methods Utilized in Essential Oil Research. J. Essent. Oil Res. 2003, 15, 428–433. [Google Scholar] [CrossRef]
- Ezadi, F.; Ardebili, A.; Mirnejad, R. Antimicrobial Susceptibility Testing for Polymyxins: Challenges, Issues, and Recommendations. J. Clin. Microbiol. 2019, 57, 1–20. [Google Scholar] [CrossRef] [PubMed]
- Griffin, S.G.; Markham, J.L.; Leach, D.N. An Agar Dilution Method for the Determination of the Minimum Inhibitory Concentration of Essential Oils. J. Essent. Oil Res. 2000, 12, 249–255. [Google Scholar] [CrossRef]
- Chouhan, S.; Sharma, K.; Guleria, S. Antimicrobial Activity of Some Essential Oils-Present Status and Future Perspectives. Medicines 2017, 4, 58. [Google Scholar] [CrossRef]
- Chu, Y.; Xu, T.; Gao, C.; Liu, X.; Zhang, N.; Feng, X.; Liu, X.; Shen, X.; Tang, X. Evaluations of physicochemical and biological properties of pullulan-based films incorporated with cinnamon essential oil and Tween 80. Int. J. Biol. Macromol. 2019, 122, 388–394. [Google Scholar] [CrossRef] [PubMed]
- Selvamuthukumar, S.; Anandam, S.; Krishnamoorthy, K.; Rajappan, M. Nanosponges: A novel class of drug delivery system-review. J. Pharm. Pharm. Sci. 2012, 15, 103–111. [Google Scholar]
- Minelli, R.; Cavalli, R.; Ellis, L.; Pettazzoni, P.; Trotta, F.; Ciamporcero, E.; Barrera, G.; Fantozzi, R.; Dianzani, C.; Pili, R. Nanosponge-Encapsulated camptothecin exerts anti-tumor activity in human prostate cancer cells. Eur. J. Pharm. Sci. 2012, 47, 686–694. [Google Scholar] [CrossRef] [PubMed]
- Prajapati, N.D.; Purohit, S.; Sharma, A.K.; Kumar, T. Handbook of Medicinal Plants: A Complete Source Book; Agrobios Publishers: Jodhpur, India, 2003. [Google Scholar]
- Kumar, R.; Srivastava, M.; Dubey, N.K. Evaluation of Cymbopogon martinii oil extract for control of postharvest insect deterioration in cereals and legumes. J. Food Prot. 2007, 70, 172–178. [Google Scholar] [CrossRef]
- Gaitanis, G.; Velegraki, A.; Mayser, P.; Bassukas, I.D. Skin diseases associated with Malassezia yeasts: Facts and controversies. Clin. Dermatol. 2013, 31, 455–463. [Google Scholar] [CrossRef]
- Velegraki, A.; Cafarchia, C.; Gaitanis, G.; Iatta, R.; Boekhout, T. Malassezia infections in humans and animals: Pathophysiology, detection, and treatment. PLoS Pathog. 2015, 11, e1004523. [Google Scholar] [CrossRef] [PubMed]
- Sharma, A.; Rabha, D.; Ahmed, G. In vitro antifungal susceptibility of Malassezia isolates from pityriasis versicolor lesions. Indian J. Dermatol. Venereol. Leprol. 2017, 83, 249–251. [Google Scholar] [CrossRef]
- Kordali, S.; Usanmaz, A.; Cakir, A.; Komaki, A.; Ercisli, S. Antifungal and Herbicidal Effects of Fruit Essential Oils of Four Myrtus communis Genotypes. Chem. Biodivers. 2016, 13, 77–84. [Google Scholar] [CrossRef]
- Sara, C.; Paola, M.; Melania, R.; Marina, C.; Maurizio, S.; Bruno, M.; Stefania, Z. Antimycotic activity of Myrtus communis L. towards Candida spp. from clinical isolates. J. Infect. Dev. Ctries. 2013, 7. [Google Scholar] [CrossRef]
- Deriu, A.; Branca, G.; Molicotti, P.; Pintore, G.; Chessa, M.; Tirillini, B.; Paglietti, B.; Mura, A.; Sechi, L.A.; Fadda, G.; et al. In vitro activity of essential oil of Myrtus communis L. against Helicobacter pylori. Int. J. Antimicrob. Agents 2007, 30, 562–563. [Google Scholar] [CrossRef]
- Aleksic, V.; Knezevic, P. Antimicrobial and antioxidative activity of extracts and essential oils of Myrtus communis L. Microbiol. Res. 2014, 169, 240–254. [Google Scholar] [CrossRef]
- Jain, S.; Shrivastava, S.; Nayak, S.; Sumbhate, S. PHCOG MAG: Plant review recent trends in Curcuma Longa Linn. Pharmacogn. Rev. 2007, 1, 119–128. [Google Scholar]
- Mochizuki, T.; Watanabe, S.; Kawasaki, M.; Tanabe, H.; Ishizaki, H. A Japanese case of tinea corporis caused by Arthroderma benhamiae. J. Dermatol. 2002, 29, 221–225. [Google Scholar] [CrossRef] [PubMed]
- Roxburgh, A.C.; Borrie, P. Roxburgh’s Common Skin Diseases, 12th ed.; The English Language Book Society and H.K. Lewis and Co. Ltd.: London, UK, 1973. [Google Scholar]
- Torres-Alvarez, C.; Castillo, S.; Sánchez-García, E.; Aguilera González, C.; Galindo-Rodríguez, S.A.; Gabaldón-Hernández, J.A.; Báez-González, J.G. Inclusion Complexes of Concentrated Orange Oils and β-Cyclodextrin: Physicochemical and Biological Characterizations. Molecules 2020, 25, 5109. [Google Scholar] [CrossRef] [PubMed]
- Vörös-Horváth, B.; Das, S.; Salem, A.; Nagy, S.; Böszörményi, A.; Kőszegi, T.; Pál, S.; Széchenyi, A. Formulation of Tioconazole and Melaleuca alternifolia Essential Oil Pickering Emulsions for Onychomycosis Topical Treatment. Molecules 2020, 25, 5544. [Google Scholar] [CrossRef]
| No. | Techniques | Reference | Type of Skin Infections/ Fungi Species | Essential Oils | Methods | Findings | Conclusion |
|---|---|---|---|---|---|---|---|
| 1. | In vitro—Conventional technology | [58] | Skin infections (C. albicans, C. parapsilosis) | Ten EOs: oregano, thyme, clove, arborvitae, cassia, lemongrass, melaleuca, eucalyptus, lavender, and clary sage |
|
|
|
| 2. | [59] | Dermatophytosis by dermatophytes (Trichophyton rubrum PTCC (Persian Type Culture Collection)5143, T. mentagrophytes PTCC5054, Microsporum canis PTCC5069, M. gypseum PTCC 5070, T. schoenleinii PTCC5221, T. verrucosum var. album PTCC 5056) | Artemisia sieberi oils |
|
|
| |
| 3. | In vitro—Conventional technology | [60] | Various skin infection due to pathogens (C. albicans ATCC 10231, and dermatophyte T. rubrum SNB-TR) | Coridothymus capitatus L., |
|
|
|
| Lavandula stoechas L., | |||||||
| Lavandula angustifolia Mill., | |||||||
| Mentha spicata L. subsp. condensata, | |||||||
| Origanum syriacum L., | |||||||
| Rosmarinus officinalis, | |||||||
| Salvia fruticosa Miller., | |||||||
| Satureja cuneifolia Ten., | |||||||
| Satureja thymbra L., | |||||||
| Thymbra spicata L., and Vitex agnus-castus L. | |||||||
| 4. | [61] | Skin disease due to six fungal strains (C. tropicalis, C. albicans, Rhizomucor miehei, C. glabrata, A. niger and A. fumigates) | Myristica fragrans |
|
|
| |
| 5. | [62] | Keratophilic fungi, a type of dermatophytes causing infection to hair, glabrous skin and nails (A. flavus, T. mentagrophytes, T. tonsurans, T. verrucosum, Epidermatophyton floccosum and Microsporum nanum) | Four different commercially available Itra (Volatile plant oils): Bella (Lonicera x bella zabel), Kewda (Pandanus odoratissimus), Rajnigandha (Polianthes tuberosa) and Mogra (Jasminum sambac) |
|
|
| |
| 6. | In vitro—Conventional technology | [63] | Various skin diseases (C. krusei H9, C. guillermondii MAT23, C. albicans ATCC 10231, C. tropicalis ATCC 13803, C. parapsilosis ATCC 90018, Cryptococcus neoformans CECT 1078, T. mentagrophytes FF7, Microsporum canis FF, T. rubrum CECT 2794, M. gypseum CECT 2908, A. niger F01, A. fumigatus F05, A. fumigatus F07, A. fumigatus F17, A. flavus F44, A. niger ATCC 16404, A. fumigatus ATCC 46645 | Four type oils obtained from Thymus zygis subsp. Sylvestris (collected at four sites) |
|
|
|
| 7. | [64] | Dermatophytosis or ring worm infections (T. rubrum PTCC 5143, T. mentagrophytes PTCC 5054, M. canis PTCC 5069, M. gypseum PTCC 5070, T. schoenleinii PTCC 5221, T verrucosum var. album PTCC 5056) | Satureja khuzistanica |
|
|
| |
| 8. | In vitro—Conventional technology | [65] | Management of dermatophytosis (Candida krusei H9, C. guillermondii MAT 23, C. albicans ATCC 10231, C. tropicalis ATCC 13803, C. parapsilosis ATCC 90018, C. neoformans CECT 1078; T. mentagrophytes FF7, M. canis FF, E. FF9, T. rubrum CECT 2794, M. gypseum CECT 2908, A. flavus F44, A. niger ATCC 16404, A. fumigatus ATCC 46645 | D. carota subsp. gummifer (Syme) Hook.f. |
|
|
|
| 9. | In vitro—Conventional technology | [66] | Various skin diseases (C. albicans ATCC 10231, C. parapsilosis ATCC 90018, C. tropicalis ATCC 13803, C. neoformans CECT 1078, C. guillermondii MAT2, C. krusei H9, A. niger ATCC 16404, A. fumigatus ATCC 46645, A. flavus F44, E. floccosum FF9, T. mentagrophytes FF7, M. canis FF1, T. rubrum CECT 2794, M. gypseum CECT 2908, T. mentagrophytes var. interdigitale CECT 2958, and T. verrucosum CECT 2992) | Salvia officinalis L. |
|
|
|
| 10. | [67] | Various skin diseases (C. albicans ATCC 10231, T. rubrum SNB-TR1, T. mentagrophytes SNBTM1, T. soudanense SNB-TS1, T. violaceum SNB-TV1 and T. tonsurans SNB-TT1) | Abies cilicica, Cupressus sempervirens, Juniperus excelsa, Juniperus oxycedrus, Cedrus libani and Cupressus macrocarpa gold crest |
|
|
| |
| 11. | In vitro—Conventional technology | [68] | Contact dermatitis and skin infections (C. krusei H9, C. guillermondii MAT23, C. albicans ATCC 10231, C. tropicalis ATCC 13803, C. parapsilosis ATCC 90018, C. neoformans CECT 1078, E. floccosum FF9, T. mentagrophytes FF7, M. canis FF1, T. rubrum CECT 2794, Microsporum gypseum CECT 2908, A. flavus F44, A. niger ATCC 16404, A. fumigatus ATCC 46645) | Distichoselinum tenuifolium |
|
|
|
| 12. | In vitro—Conventional technology | [69] | Skin infections (T. rubrum and T. mentagrophytes) | Agathosma betulina and Coleonema album |
|
|
|
| 13. | [70] | Skin infections (T. rubrum and T. mentagrophytes) | C. album and C. pulchellum |
|
|
| |
| 14. | In vitro—Conventional technology | [71] | Skin infections (Fusarium sporotrichioides, F. moniliforme, T.n mentagrophytes, A. niger, and Rhizoctonia lilacina) | Bursera morelensis |
|
|
|
| 15. | [72] | Skin infections (C. albicans, Candida stellatoidea and Candida torulopsis) | Physalis angulata |
|
|
| |
| 16. | In vitro—Conventional technology | [73] | Dermatophytes and fungi infections (Microsporum gypseum, M. canis, Arthroderma cajetani, T. mentagrophytes, T. tonsurans, E. floccosum, Botrytis cinerea, Pythium ultimum) | Marrubium vulgare L. |
|
|
|
| 17. | [74] | Skin infections (C.a albicans 1, C. albicans 2, T. rubrum 1, T. rubrum 2, T. violaceum, and T. soudanensis) | Eugenia caryophylla and Mentha sp cf piperita |
|
|
| |
| 18. | In vitro—Conventional technology | [75] | Skin diseases (E. floccosum, M. canis, M. gypseum, T. mentagrophytes, T. mentagrophytes var. interdigitale, T. rubrum, T. verrucosum, C. albicans, C. guilliermondii, C. krusei, C. parapsilosis, C. tropicalis, C. neoformans, A. flavus, A. fumigatus, A. niger). | Juniperus communis subsp. alpina (Suter) Celak |
|
|
|
| 19. | [76] | Skin infection sporotrichosis (Sporothrix schenckii fungus) | Turmeric (Curcuma longa) |
|
|
| |
| 20. | [77] | Skin infections (T. rubrum and T. mentagrophytes) | Lavandula luisieri and Cymbopogon citratus |
|
|
| |
| 21. | In vitro—Conventional technology | [78] | Skin diseases (Propionibacterium acnes, Malassezia spp., C. albicans and Trichophyton spp.) | Nine EOs (Cyperus scariosus R. Br., Syzgium aromaticum L. Merr et L.M. Perry, Carum carvi L., Coriandrum sativum L., Boswellia serrata Roxb. Ex Colebr., Syzgium cumini L. Skeels, Elettaria cardamom L. Maton, Occimum sanctum L. and Piper nigrum L.) |
|
|
|
| 22. | In vitro—Conventional technology | [79] | Skin infections by yeast (C. albicans 31, C. tropicalis 32, C. glabrata 33, C. glabrata 35 and C. glabrata 38) | Six commercial lemon EOs (ETJA, Vera-Nord, Avicenna-Oil, Dufti by Gies, Art, and Croce Azzurra |
|
|
|
| 23. | [80] | Skin diseases (M. canis KCTC 6348, 6349, 6591, T. rubrum KCTC 6345, 6352, 6375, T. mentagrophytes KCTC 6077 and 6085) | Lonicera japonica Thunb. |
|
|
| |
| 24. | In vitro—Conventional technology | [81] | Skin diseases (Fusarium oxysporum, T. rubrum and T. mentagrophytes) | Seventeen EOs |
|
|
|
| 25. | In vitro—Conventional technology | [82] | Pityriasis versicolor (Malassezia furfur) | Citrus lemon (lemon) and Citrus sinensis (orange) |
|
|
|
| 26. | [83] | Skin infections (C. albicans, C. dubliniensis, C. glabrata, C. guilliermondii, C. parapsilosis, C. tropicalis, C. neoformans, Sacharomyces cerevisiae, A. fumigatus, A. flavus, A. niger, T. rubrum, M. canis, Fonsecaea pedrosoi, Pseudallescheria boydii, Fusarium solani, S. schenckii) | Tropaeolum pentaphyllum Lam. tubers |
|
|
| |
| 27. | In vitro—Conventional technology | [84] | Skin infections (T. rubrum and C. albicans) | Twenty-nine oils |
|
|
|
| 28. | In vitro—Nonconventional technology | [85] | Skin infections (Candida pseudotropicalis) | Lippia multiflora (lippia oil) |
|
|
|
| 29. | In vitro—Nonconventional technology | [56] | Different skin infecting pathogens (C. albicans, A. niger) | Piper betle |
|
|
|
| 30. | [86] | Candidiasis (C. krusei ATCC 6528, C. parapsilosis ATCC 22019, C. krusei, C. parapsilosis, C. albicans, C. glabrata, C. tropicalis | Bidens tripartita |
|
|
| |
| 31. | [87] | Candidiasis (C. albicans ATCC 10231, C. krusei ATCC 6258 and C. parapsilosis ATCC 90098) | Mediterranean EOs (Rosmarinus officinalis, Lavandula x intermedia “Sumian”, Origanum vulgare subsp. hirtum) |
|
|
| |
| 32. | In vitro—Nonconventional technology | [88] | Skin infections due to pathogenic fungi(C. albicans, C. tropicalis and T. mentagrophytes) | Black pepper, Cardamom, Cumin, Boswellia and Patcholi |
|
|
|
| 33. | In vitro and In vivo—Conventional technology | [89] | Body aches and dermatitis (A. flavus, A. niger, F. solani, Mucor piriformis, Wickerhamomyces anomalus, Wickerhamomyces anomalus, Deboromyces hansenii, and C. albicans) | Parrotiopsis jacquemontiana |
|
|
|
| 34. | In vitro and In vivo—Conventional technology | [90] | Skin infections (Chrysosporium tropicum, Trichophyton simii, T. rubrum and Chrysosporium indicum) | Trachyspermum ammi |
|
|
|
| 35. | [91] | Skin disease due to fungi strains(C. albicans, C. parapsilosis, C. tropicalis; A. niger, A. terreus, A. flavus, A. fumigatus, Penicillium sp. and Mucor sp. | Lemon grass (Cymbopogon citratus (DC.) Stapf) |
|
|
| |
| 36. | In vitro and In vivo—Conventional technology | [92] | Skin infections (M. gypseum and T. mentagrophytes) | Ageratum houstonianum Mill., |
|
|
|
| 37. | In vitro and In vivo—Nonconventional technology | [93] | Skin disease (C. albicans strain ATC 100231) | Lemongrass oil (LGO) is a volatile oil extracted from the leaves of C. citratus |
|
|
|
| 38. | In vitro and In vivo—Nonconventional technology | [94] | Skin infections (T. mentagrophytes, T. rubrum, T. verrucosum and M. canis) | Cymbopogon martini |
|
|
|
| 39. | In vitro and In vivo—Nonconventional technology | [95] | Dermatophytes and some filamentous fungi (A. flavus, A. niger, A. fumigatus, Microspoum audouni, M. nanum, T. mentagrophytes, T. verrucosm and T. violaceum) | C. martini and Chenopodium ambrosioides |
|
|
|
| 40. | Clinical Interventions | [96] | Ringworm (tenia corporis) (M. and T. mentagrophytes) | Curcuma longa L. |
|
|
|
| 41. | [97] | Pityriasis versicolor (Malassezia sp.) | Myrtus communis |
|
|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Abd Rashed, A.; Rathi, D.-N.G.; Ahmad Nasir, N.A.H.; Abd Rahman, A.Z. Antifungal Properties of Essential Oils and Their Compounds for Application in Skin Fungal Infections: Conventional and Nonconventional Approaches. Molecules 2021, 26, 1093. https://doi.org/10.3390/molecules26041093
Abd Rashed A, Rathi D-NG, Ahmad Nasir NAH, Abd Rahman AZ. Antifungal Properties of Essential Oils and Their Compounds for Application in Skin Fungal Infections: Conventional and Nonconventional Approaches. Molecules. 2021; 26(4):1093. https://doi.org/10.3390/molecules26041093
Chicago/Turabian StyleAbd Rashed, Aswir, Devi-Nair Gunasegavan Rathi, Nor Atikah Husna Ahmad Nasir, and Ahmad Zuhairi Abd Rahman. 2021. "Antifungal Properties of Essential Oils and Their Compounds for Application in Skin Fungal Infections: Conventional and Nonconventional Approaches" Molecules 26, no. 4: 1093. https://doi.org/10.3390/molecules26041093
APA StyleAbd Rashed, A., Rathi, D.-N. G., Ahmad Nasir, N. A. H., & Abd Rahman, A. Z. (2021). Antifungal Properties of Essential Oils and Their Compounds for Application in Skin Fungal Infections: Conventional and Nonconventional Approaches. Molecules, 26(4), 1093. https://doi.org/10.3390/molecules26041093







