Biological Effects of Shikonin in Human Gingival Fibroblasts via ERK 1/2 Signaling Pathway
Abstract
1. Introduction
2. Results
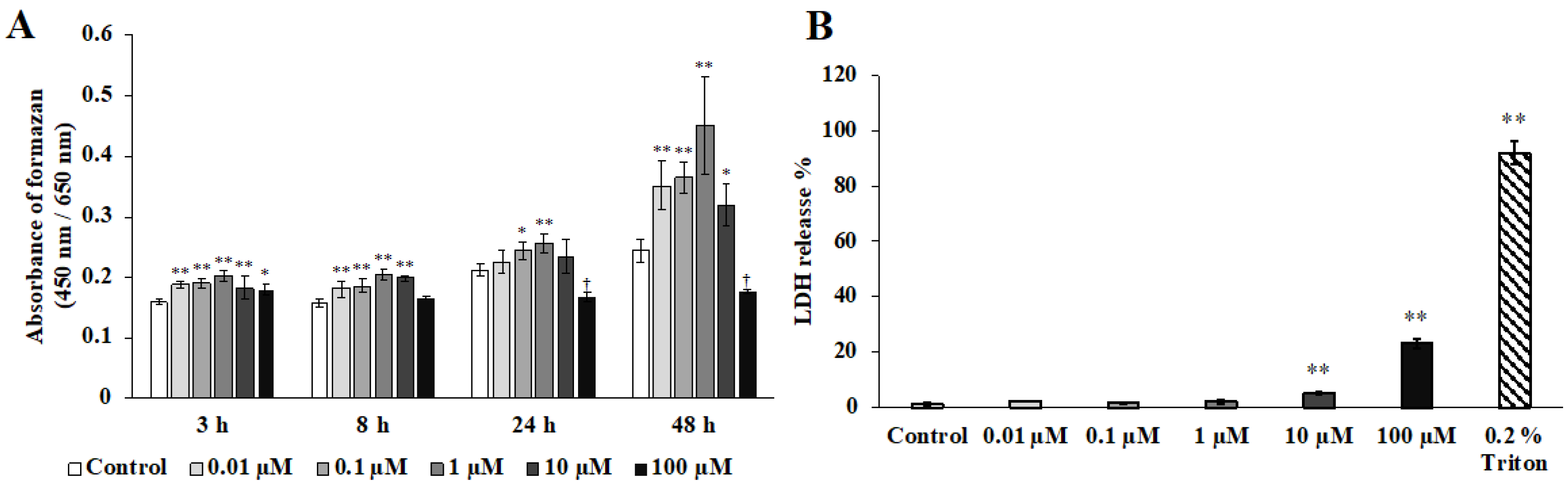
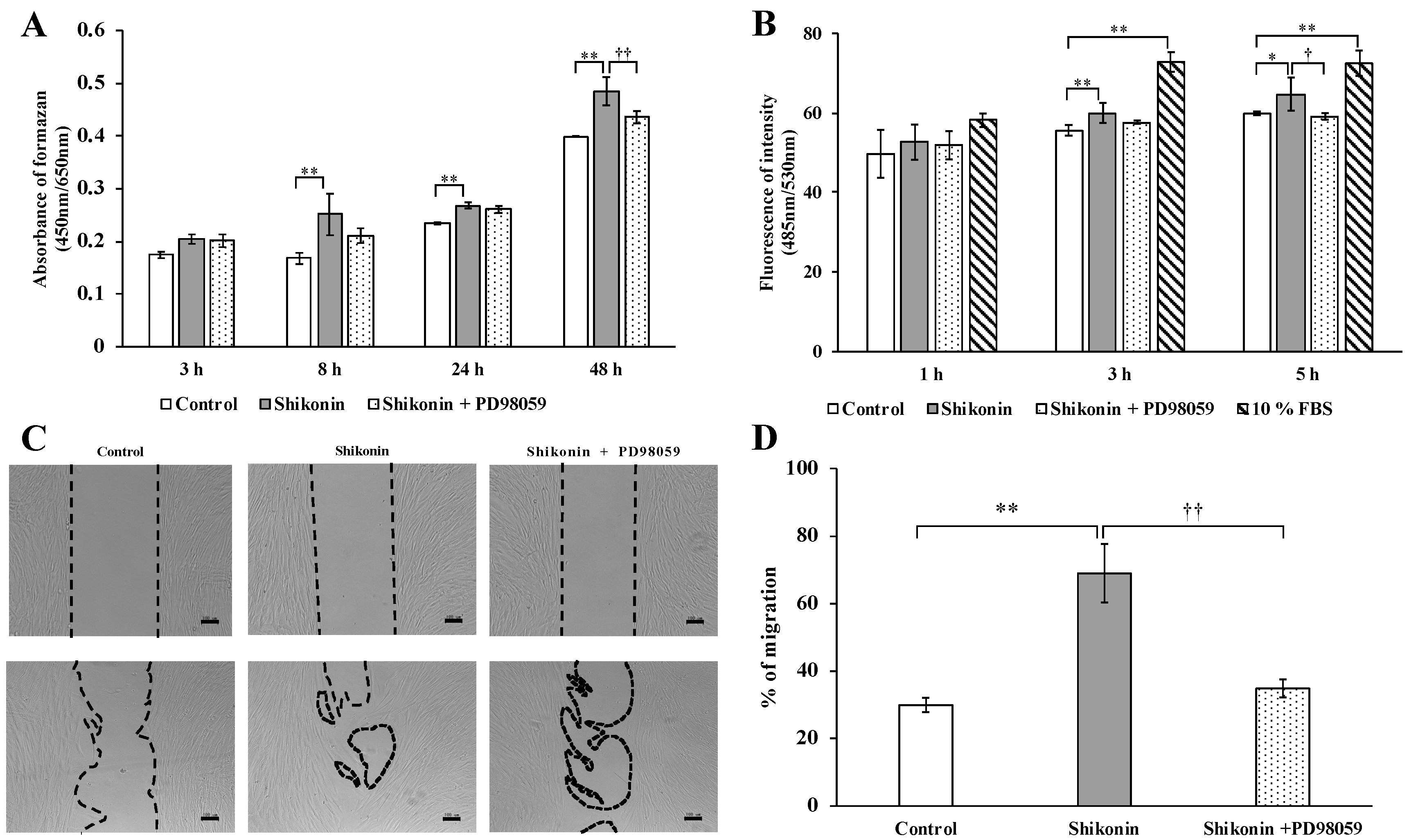
2.1. Cell Proliferation Assay and LDH Activity
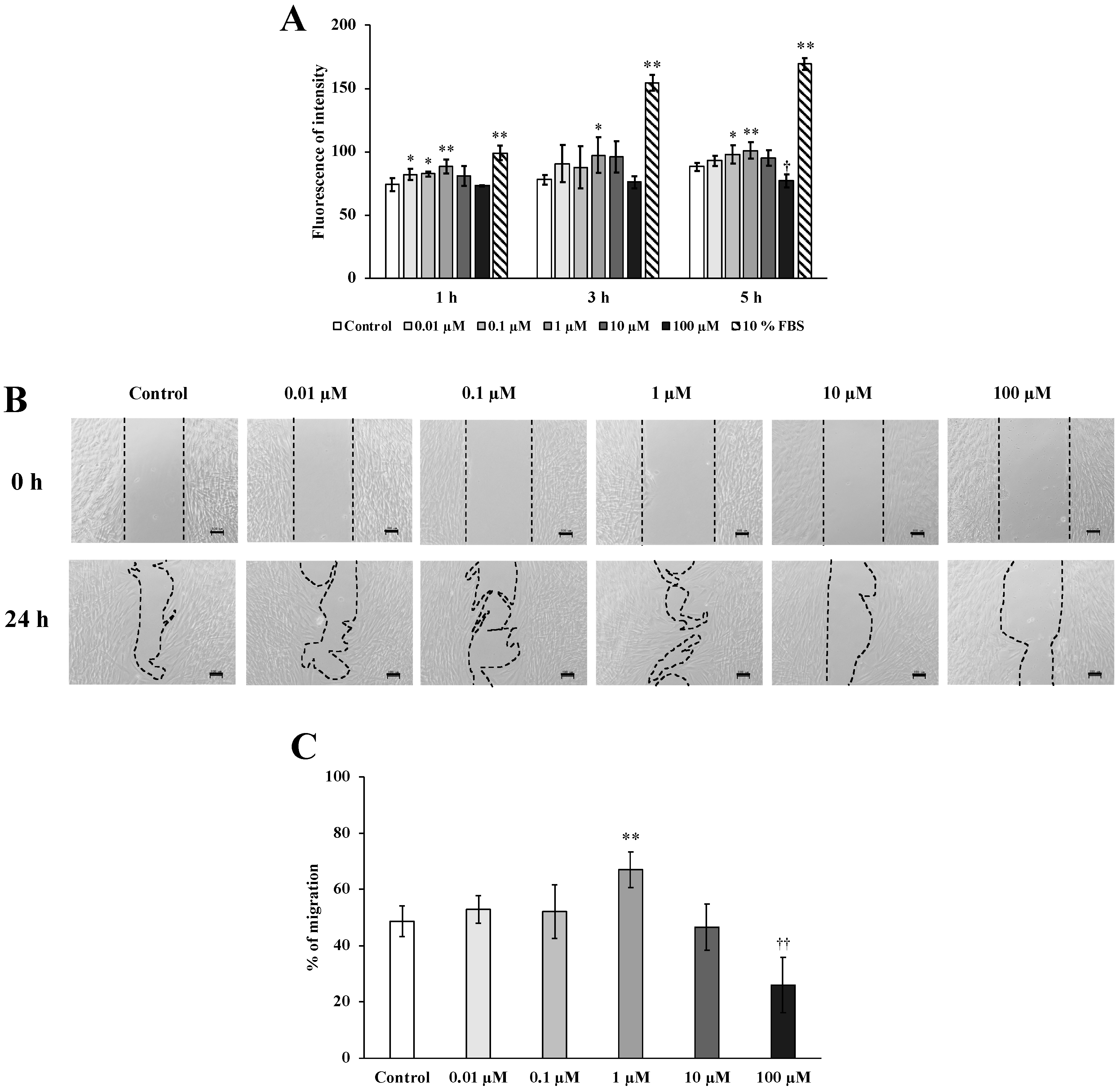
2.2. Cell Migration and Wound Healing Assays
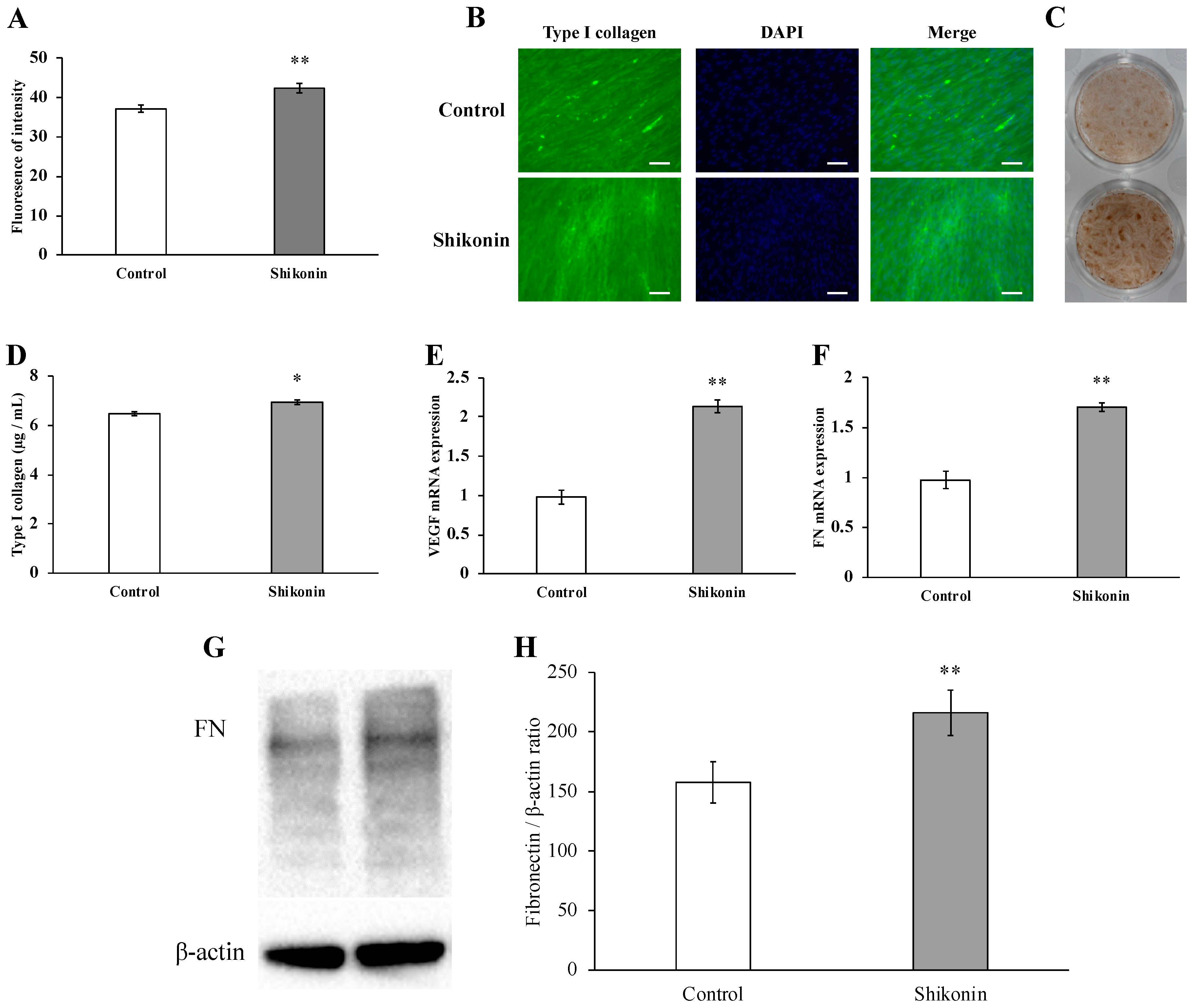
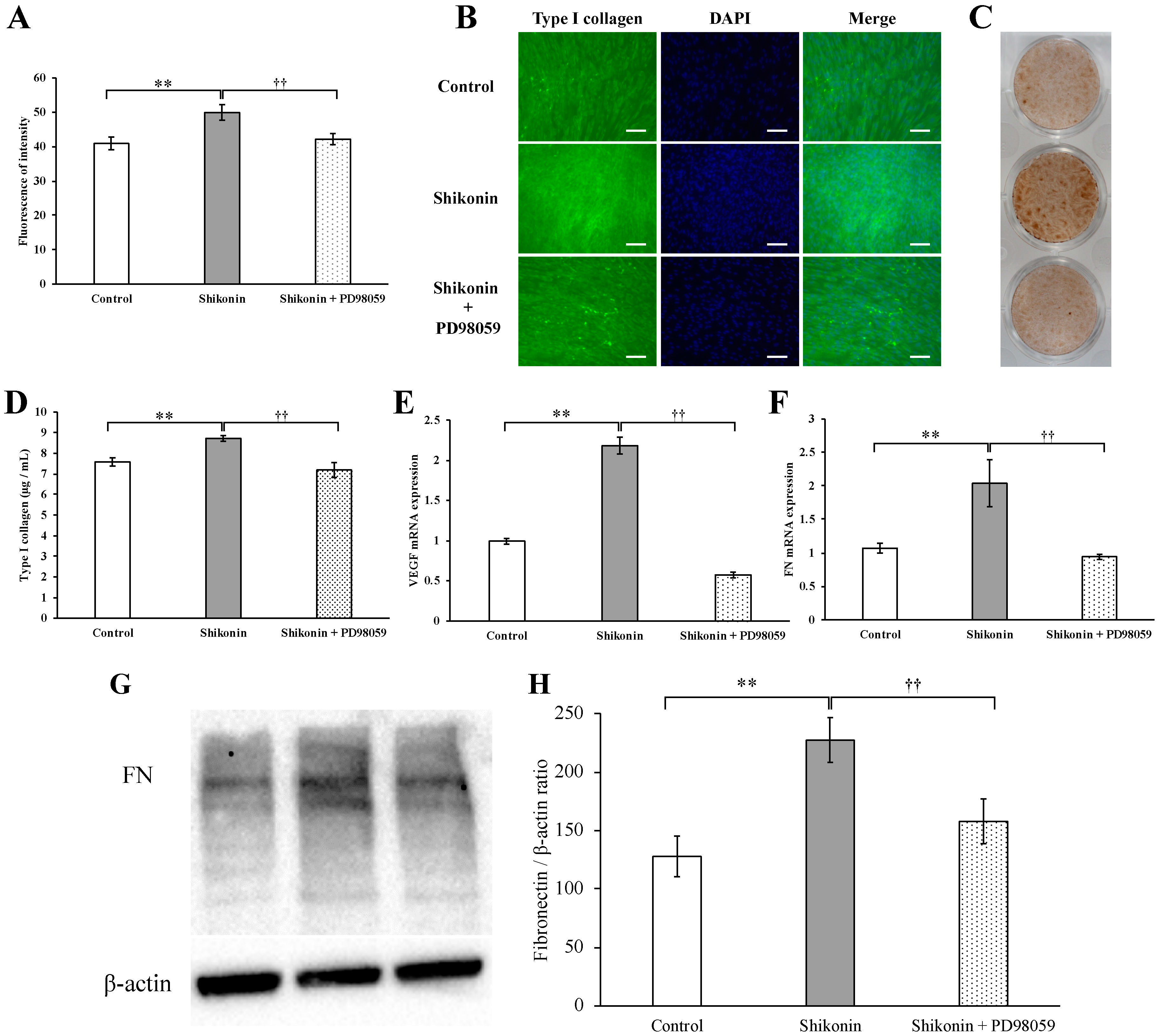
2.3. Synthesis of Type I Collagen and FN, Gene Expression of VEGF and FN
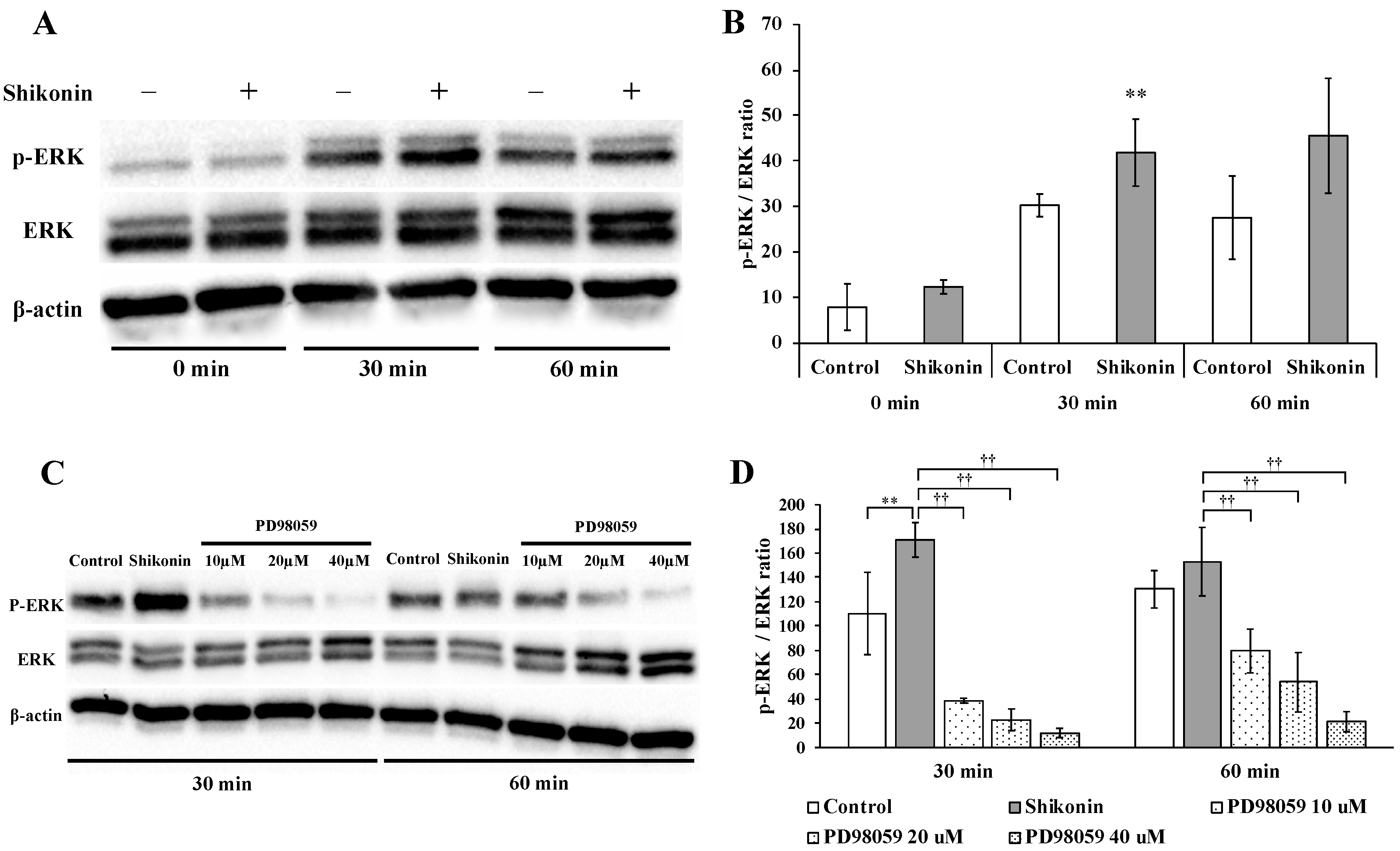
2.4. Shikonin Activated the ERK 1/2 Signaling Pathway in hGFs
2.5. ERK 1/2 Inhibition
3. Discussion
4. Materials and Methods
4.1. Cell Culture
4.2. Preparation of Shikonin
4.3. Cell Proliferation Assay
4.4. Cell Cytotoxicity Assay
4.5. Cell Migration Assay
4.6. Wound Healing Assay
4.7. Gene Expression
4.8. Type I Collagen Synthesis
4.9. Western Blots
4.10. ERK 1/2 Inhibition
4.11. Statistical Analyses
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Gurtner, G.C.; Werner, S.; Barrandon, Y.; Longaker, M.T. Wound repair and regeneration. Nature 2008, 453, 314–321. [Google Scholar] [CrossRef] [PubMed]
- Smith, P.C.; Cáceres, M.; Martínez, C.; Oyarzún, A.; Martínez, J. Gingival wound healing: An essential response disturbed by aging? J. Dent. Res. 2015, 94, 395–402. [Google Scholar] [CrossRef] [PubMed]
- Aukhil, I. Biology of wound healing. Periodontol. 2000 2000, 22, 44–50. [Google Scholar] [CrossRef] [PubMed]
- Sanders, J.E.; Chuang, A.; Swiec, G.D.; Bisch, F.C.; Herold, R.W.; Buxton, T.B.; McPherson, J.C., 3rd. The effects of enamel matrix derivative and cyclic mechanical strain on human gingival fibroblasts in an in vitro defect healing model. Int. J. Periodontics Restor. Dent. 2011, 31, 671–678. [Google Scholar] [PubMed]
- Cate, A.R.; Deporter, D.A. The degradative role of the fibroblast in the remodelling and turnover of collagen in soft connective tissue. Anat. Rec. 1975, 182, 1–13. [Google Scholar] [CrossRef]
- Pérez-Tamayo, R. Collagen resorption in carrageenin granulomas. I. Collagenolytic activity in in vitro explants. Lab. Investig. 1970, 22, 137–141. [Google Scholar]
- Bainbridge, P. Wound healing and the role of fibroblasts. J. Wound Care 2013, 22, 407–412. [Google Scholar]
- Toume, S.; Gefen, A.; Weihs, D. Low-level stretching accelerates cell migration into a gap. Int. Wound J. 2017, 14, 698–703. [Google Scholar] [CrossRef]
- Thangapazham, R.L.; Sharad, S.; Maheshwari, R.K. Phytochemicals in wound healing. Adv. Wound Care 2016, 5, 208–229. [Google Scholar] [CrossRef]
- Kuo, Y.T.; Lin, C.C.; Kuo, H.T.; Hung, J.H.; Liu, C.H.; Jassey, A.; Yen, M.H.; Wu, S.J.; Lin, L.T. Identification of baicalin from Bofutsushosan and Daisaikoto as a potent inducer of glucose uptake and modulator of insulin signaling-associated pathways. J. Food Drug Anal. 2019, 27, 240–248. [Google Scholar] [CrossRef]
- Kato, T.; Segami, N.; Sakagami, H. Anti-inflammatory activity of Hangeshashinto in IL-1β-stimulated gingival and periodontal ligament fibroblasts. In Vivo 2016, 30, 257–263. [Google Scholar] [PubMed]
- Veilleux, M.P.; Moriyama, S.; Yoshioka, M.; Hinode, D.; Grenier, D. A review of evidence for a therapeutic application of traditional Japanese Kampo medicine for oral diseases/disorders. Medicines 2018, 5, 35. [Google Scholar] [CrossRef]
- Surathu, N.; Kurumathur, A.V. Traditional therapies in the management of periodontal disease in India and China. Periodontol. 2000 2011, 56, 14–24. [Google Scholar] [CrossRef] [PubMed]
- Jettanacheawchankit, S.; Sasithanasate, S.; Sangvanich, P.; Banlunara, W.; Thunyakitpisal, P. Acemannan stimulates gingival fibroblast proliferation; expressions of keratinocyte growth factor-1, vascular endothelial growth factor, and type I collagen; and wound healing. J. Pharmacol. Sci. 2009, 109, 525–531. [Google Scholar] [CrossRef]
- Chen, X.; Yang, L.; Oppenheim, J.J.; Howard, M.Z. Cellular pharmacology studies of shikonin derivatives. Phytother. Res. 2002, 16, 199–209. [Google Scholar] [CrossRef] [PubMed]
- Papageorgiou, V.P.; Assimopoulou, A.; Ballis, A.C. Alkannins and shikonins: A new class of wound healing agents. Curr. Med. Chem. 2008, 15, 3248–3267. [Google Scholar] [CrossRef]
- Andújar, I.; Ríos, J.L.; Giner, R.M.; Recio, M.C. Shikonin promotes intestinal wound healing in vitro via induction of TGF-β release in IEC-18 cells. Eur. J. Pharm. Sci. 2013, 49, 637–641. [Google Scholar] [CrossRef] [PubMed]
- Shindo, S.; Hosokawa, Y.; Hosokawa, I.; Shiba, H. Shikonin inhibits inflammatory cytokine production in human periodontal ligament cells. Inflammation 2016, 39, 1124–1129. [Google Scholar] [CrossRef] [PubMed]
- Fan, C.; Zhang, X.; Upton, Z. Anti-inflammatory effects of shikonin in human periodontal ligament cells. Pharm. Biol. 2018, 56, 415–421. [Google Scholar] [CrossRef] [PubMed]
- Ruan, M.; Yan, M.; Yang, W.J.; Qu, X.Z.; Zhou, X.J.; Chen, W.T.; Zhang, C.P. Role of NF-kappaB pathway in shikonin induced apoptosis in oral squamous cell carcinoma Tca-8113 cells. Shanghai J. Stomatol. 2010, 19, 66–71. [Google Scholar]
- Kim, D.J.; Lee, J.H.; Park, H.R.; Choi, Y.W. Acetylshikonin inhibits growth of oral squamous cell carcinoma by inducing apoptosis. Arch. Oral Biol. 2016, 70, 149–157. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.S.; Lee, D.Y.; Kim, Y.B.; Lee, S.W.; Cha, S.W.; Park, H.; Kim, G.S.; Kwon, D.Y.; Lee, M.H.; Han, S.H. The mechanism underlying the antibacterial activity of shikonin against methicillin-resistant Staphylococcus aureus. Evid. Based Complement. Alternat. Med. 2015, 2015, 1–9. [Google Scholar]
- Andújar, I. Pharmacological properties of shikonin—A review of literature since 2002. Planta Med. 2013, 79, 1685–1697. [Google Scholar] [CrossRef] [PubMed]
- Papageorgiou, V.P. Wound healing properties of naphthaquinone pigments from Alkanna tinctoria. Experientia 1978, 34, 1499–1501. [Google Scholar] [CrossRef] [PubMed]
- Papageorgiou, V.P. Naturally occurring isohexenylnaphthazarin pigments: A new class of drugs. Planta Med. 1980, 38, 193–203. [Google Scholar] [CrossRef] [PubMed]
- Papageorgiou, V.P.; Assimopoulou, A.N.; Samanidou, V.F.; Papadoyannis, I.N. Recent advances in chemistry, biology and biotechnology of alkannins and shikonins. Curr. Org. Chem. 2006, 10, 2123–2142. [Google Scholar] [CrossRef]
- Singer, A.J.; Clark, R. Cutaneous wound healing. N. Engl. J. Med. 1999, 341, 738–746. [Google Scholar] [CrossRef] [PubMed]
- Jones, S.G.; Edwards, R.; Thomas, D.W. Inflammation and wound healing: The role of bacteria in the immuno-regulation of wound healing. Int. J. Low Extrem. Wounds 2004, 3, 201–208. [Google Scholar] [CrossRef]
- Seger, R.; Krebs, E.G. The MAPK signaling cascade. FASEB J. 1995, 9, 726–735. [Google Scholar] [CrossRef]
- Park, J.Y.; Kwak, J.H.; Kang, K.S.; Jung, E.B.; Lee, D.S.; Lee, S.; Jung, Y.; Kim, K.H.; Hwang, G.S.; Lee, H.L.; et al. Wound healing effects of deoxyshikonin isolated from Jawoongo: In vitro and in vivo studies. J. Ethnopharmacol. 2017, 199, 128–137. [Google Scholar] [CrossRef]
- Yan, Y.; Furumura, M.; Gouya, T.; Iwanaga, A.; Teye, K.; Numata, S.; Karashima, T.; Li, X.G.; Hashimoto, T. Shikonin promotes skin cell proliferation and inhibits nuclear factor-κB translocation via proteasome inhibition in vitro. Chin. Med. J. 2015, 128, 2228–2233. [Google Scholar] [CrossRef] [PubMed]
- Wagner, H.; Kreher, B.; Jurcic, K. In vitro stimulation of human granulocytes and lymphocytes by pico-and femtogram quantities of cytostatic agents. Arzneimittelforschung 1988, 38, 273–275. [Google Scholar] [PubMed]
- Fan, C.; Xie, Y.; Dong, Y.; Su, Y.; Upton, Z. Investigating the potential of Shikonin as a novel hypertrophic scar treatment. J. Biomed. Sci. 2015, 22, 70. [Google Scholar] [CrossRef] [PubMed]
- Yanagita, M.; Kojima, Y.; Kubota, M.; Mori, K.; Yamashita, M.; Yamada, S.; Kitamura, M.; Murakami, S. Cooperative effects of FGF-2 and VEGF-A in periodontal ligament cells. J. Dent. Res. 2014, 93, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Silva, D.; Cáceres, M.; Arancibia, R.; Martínez, C.; Martínez, J.; Smith, P.C. Effects of cigarette smoke and nicotine on cell viability, migration and myofibroblastic differentiation. J. Periodontal Res. 2012, 47, 599–607. [Google Scholar] [CrossRef] [PubMed]
- Karayannopoulou, M.; Tsioli, V.; Loukopoulos, P.; Anagnostou, T.L.; Giannakas, N.; Savvas, I.; Papazoglou, L.G.; Kaldrymidou, E. Evaluation of the effectiveness of an ointment based on alkannins/shikonins on second intention wound healing in the dog. Can. J. Vet. Res. 2011, 75, 42–48. [Google Scholar]
- Yin, S.Y.; Peng, A.P.; Huang, L.T.; Wang, Y.T.; Lan, C.W.; Yang, N.S. The phytochemical shikonin stimulates epithelial-mesenchymal transition (EMT) in skin wound healing. Evid. Based Complement. Alternat. Med. 2013, 2013, 262796. [Google Scholar] [CrossRef]
- Liu, Y.C.; Lerner, U.H.; Teng, Y.T. Cytokine responses against periodical infection: Protective and destructive roles. Periodontol. 2000 2010, 52, 163–206. [Google Scholar] [CrossRef] [PubMed]
- Mimura, Y.; Ihn, H.; Jinnin, M.; Asano, Y.; Yamane, K.; Tamaki, K. Epidermal growth factor induces fibronectin expression in human dermal fibroblasts via protein kinase C delta signaling pathway. J. Investig. Dermatol. 2004, 122, 1390–1398. [Google Scholar] [CrossRef]
- Ozgen, U.; Ikbal, M.; Hacimuftuoglu, A.; Houghton, P.J.; Gocer, F.; Dogan, H.; Coskun, M. Fibroblast growth stimulation by extracts and compounds of Onosma argentatum roots. J. Ethnopharmacol. 2006, 104, 100–103. [Google Scholar] [CrossRef]
- Sakaguchi, I.; Tsujimura, M.; Ikeda, N.; Minamino, M.; Kato, Y.; Watabe, K.; Yano, I.; Kaneda, K. Granulomatous tissue formation of shikon and shikonin by air pouch method. Biol. Pharm. Bull. 2001, 24, 650–655. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yang, H.L.; Tsai, Y.C.; Korivi, M.; Chang, C.T.; Hseu, Y.C. Lucidone promotes the cutaneous wound healing process via activation of the PI3K/AKT, Wnt/β-catenin and NF-κB signaling pathways. Biochim. Biophys. Acta Mol. Cell Res. 2017, 1864, 151–168. [Google Scholar] [CrossRef] [PubMed]
- Park, J.Y.; Shin, M.S.; Hwang, G.S.; Yamabe, N.; Yoo, J.E.; Kang, K.S.; Kim, J.C.; Lee, J.G.; Ham, J.; Lee, H.L. Beneficial effects of deoxyshikonin on delayed wound healing in diabetic mice. Int. J. Mol. Sci. 2018, 19, 3660. [Google Scholar] [CrossRef] [PubMed]
- Roskoski, R., Jr. ERK1/2 MAP kinases: Structure, function, and regulation. Pharmacol. Res. 2012, 66, 105–143. [Google Scholar] [CrossRef] [PubMed]
- Huang, C.; Jacobson, K.; Schaller, M.D. MAP kinases and cell migration. J. Cell Sci. 2004, 117, 4619–4628. [Google Scholar] [CrossRef] [PubMed]
- Hafner, C.; Meyer, S.; Hagen, I.; Becker, B.; Roesch, A.; Landthaler, M.; Vogt, T. Ephrin-B reverse signaling induces expression of wound healing associated genes in IEC-6 intestinal epithelial cells. World J. Gastroenterol. 2005, 11, 4511–4518. [Google Scholar] [CrossRef] [PubMed]
- Falasca, M.; Raimondi, C.; Maffucci, T. Boyden chamber. Methods Mol. Biol. 2011, 769, 87–95. [Google Scholar]
- Grada, A.; Otero-Vinas, M.; Prieto-Castrillo, F.; Obagi, Z.; Falanga, V. Research techniques made simple: Analysis of collective cell migration using the wound healing assay. J. Investig. Dermatol. 2017, 37, e11–e16. [Google Scholar] [CrossRef]
- Kato, H.; Taguchi, Y.; Tominaga, K.; Kimura, D.; Yamawaki, I.; Noguchi, M.; Yamauchi, N.; Tamura, I.; Tanaka, A.; Umeda, M. High glucose concentrations suppress the proliferation of human periodontal ligament stem cells and their differentiation into osteoblasts. J. Periodontol. 2016, 87, e44–e51. [Google Scholar] [CrossRef]
Sample Availability: Samples of the compounds are available from the authors. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Imai, K.; Kato, H.; Taguchi, Y.; Umeda, M. Biological Effects of Shikonin in Human Gingival Fibroblasts via ERK 1/2 Signaling Pathway. Molecules 2019, 24, 3542. https://doi.org/10.3390/molecules24193542
Imai K, Kato H, Taguchi Y, Umeda M. Biological Effects of Shikonin in Human Gingival Fibroblasts via ERK 1/2 Signaling Pathway. Molecules. 2019; 24(19):3542. https://doi.org/10.3390/molecules24193542
Chicago/Turabian StyleImai, Kazutaka, Hirohito Kato, Yoichiro Taguchi, and Makoto Umeda. 2019. "Biological Effects of Shikonin in Human Gingival Fibroblasts via ERK 1/2 Signaling Pathway" Molecules 24, no. 19: 3542. https://doi.org/10.3390/molecules24193542
APA StyleImai, K., Kato, H., Taguchi, Y., & Umeda, M. (2019). Biological Effects of Shikonin in Human Gingival Fibroblasts via ERK 1/2 Signaling Pathway. Molecules, 24(19), 3542. https://doi.org/10.3390/molecules24193542




