Investigation of the Effects of Molecular Parameters on the Hemostatic Properties of Chitosan
Abstract
1. Introduction
2. Results and Discussion
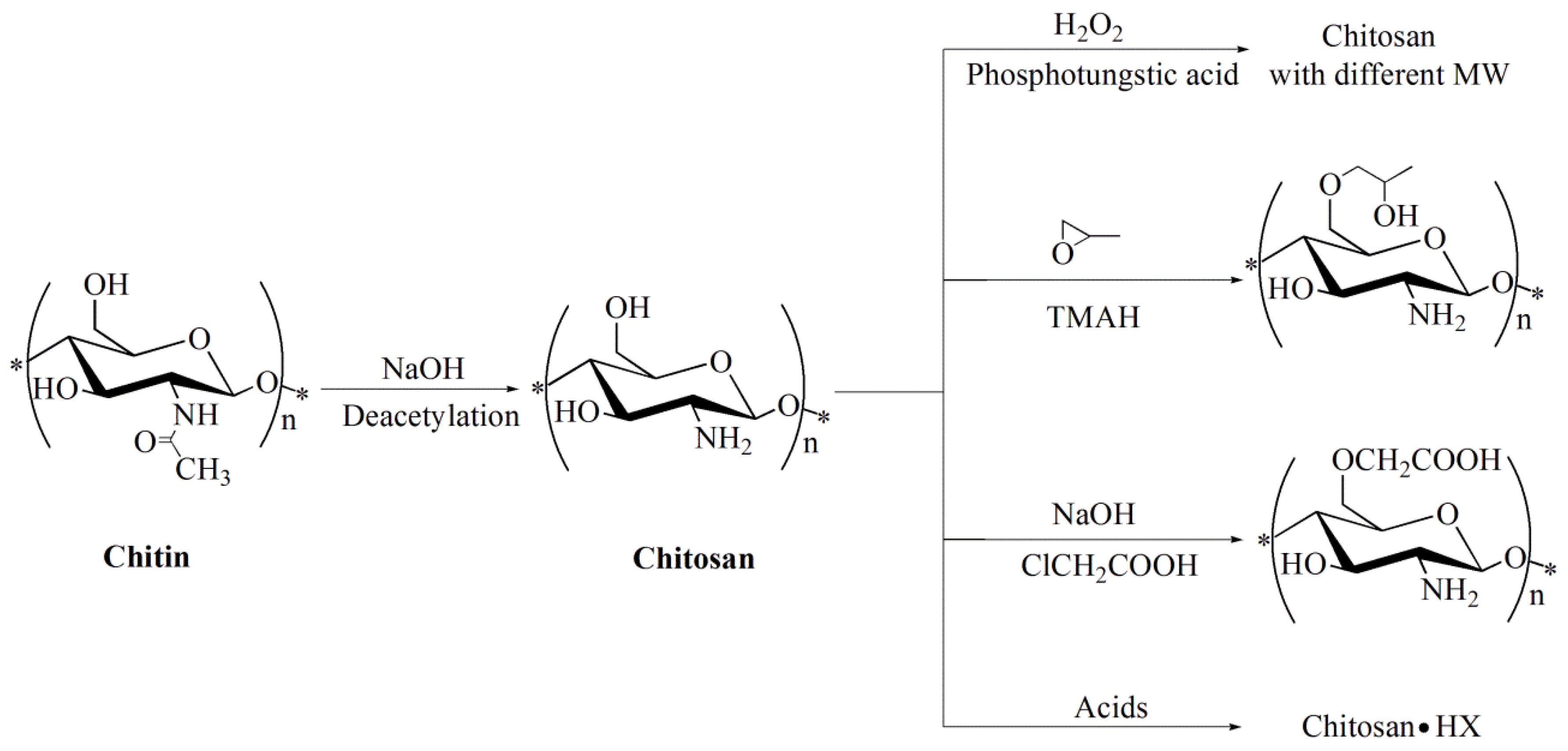
2.1. Preparation of Chitosan with Different Molecular Parameters
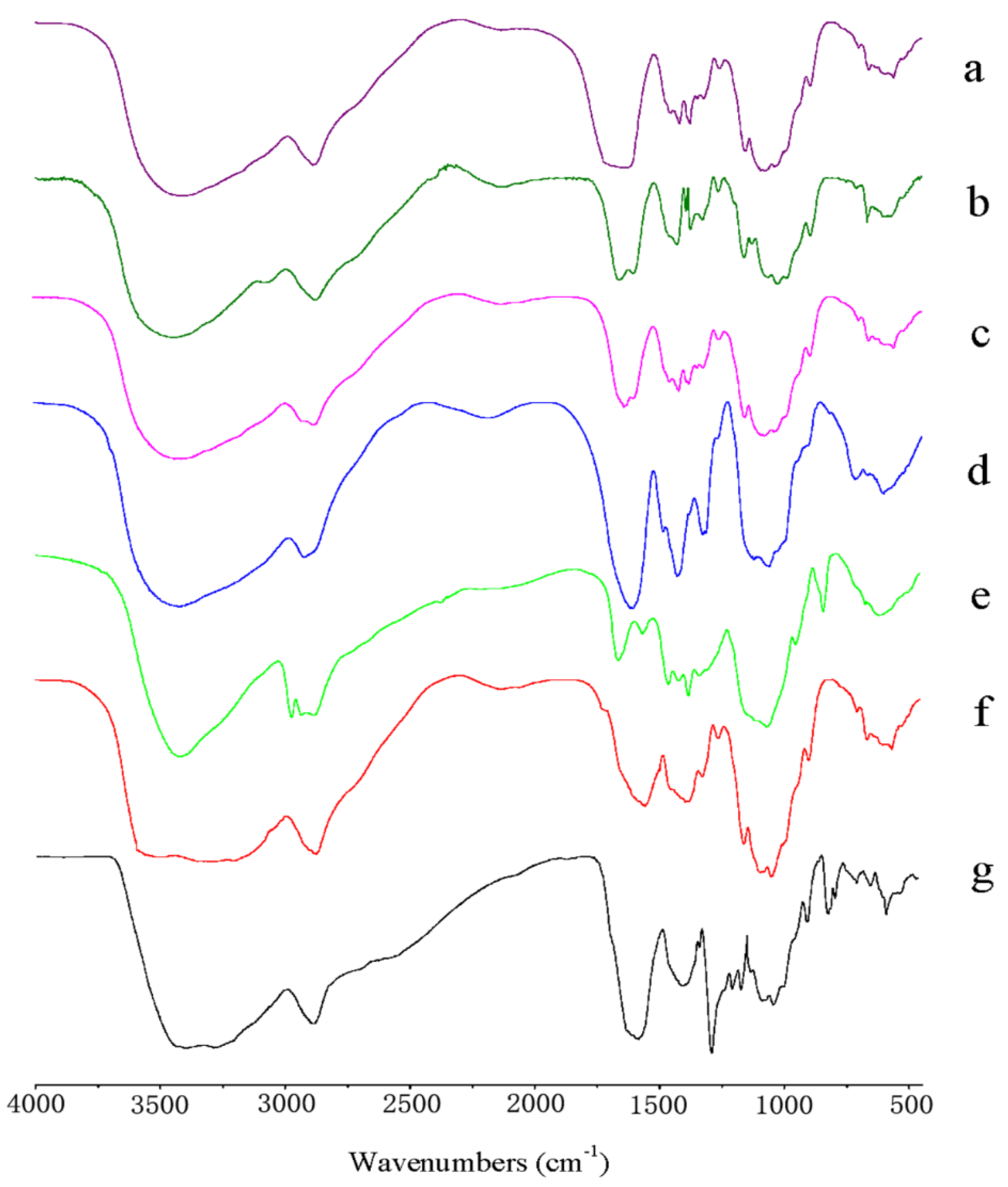
2.2. FTIR Analysis
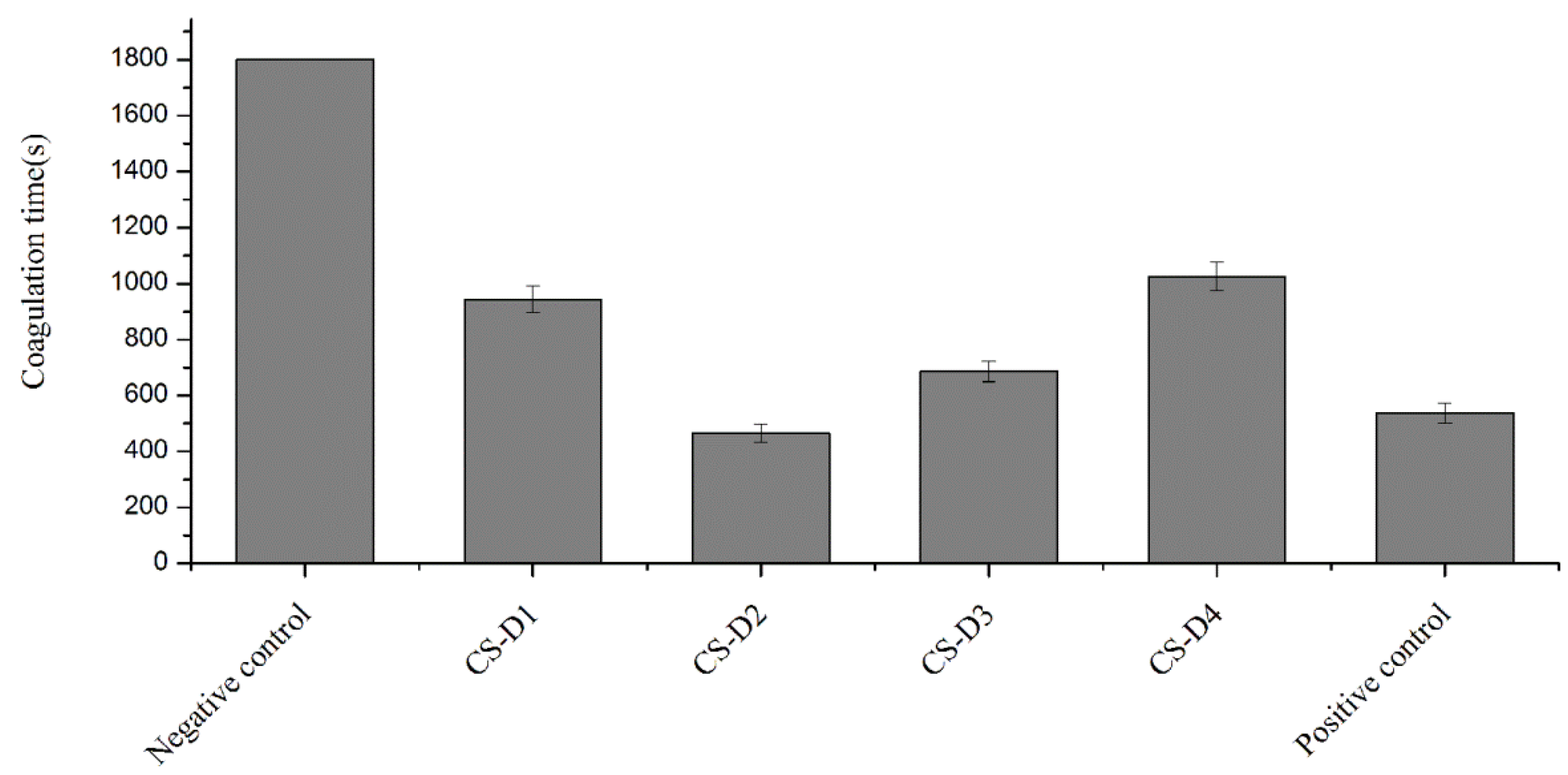
2.3. Effect of DD on the Procoagulant Activity of Chitosan
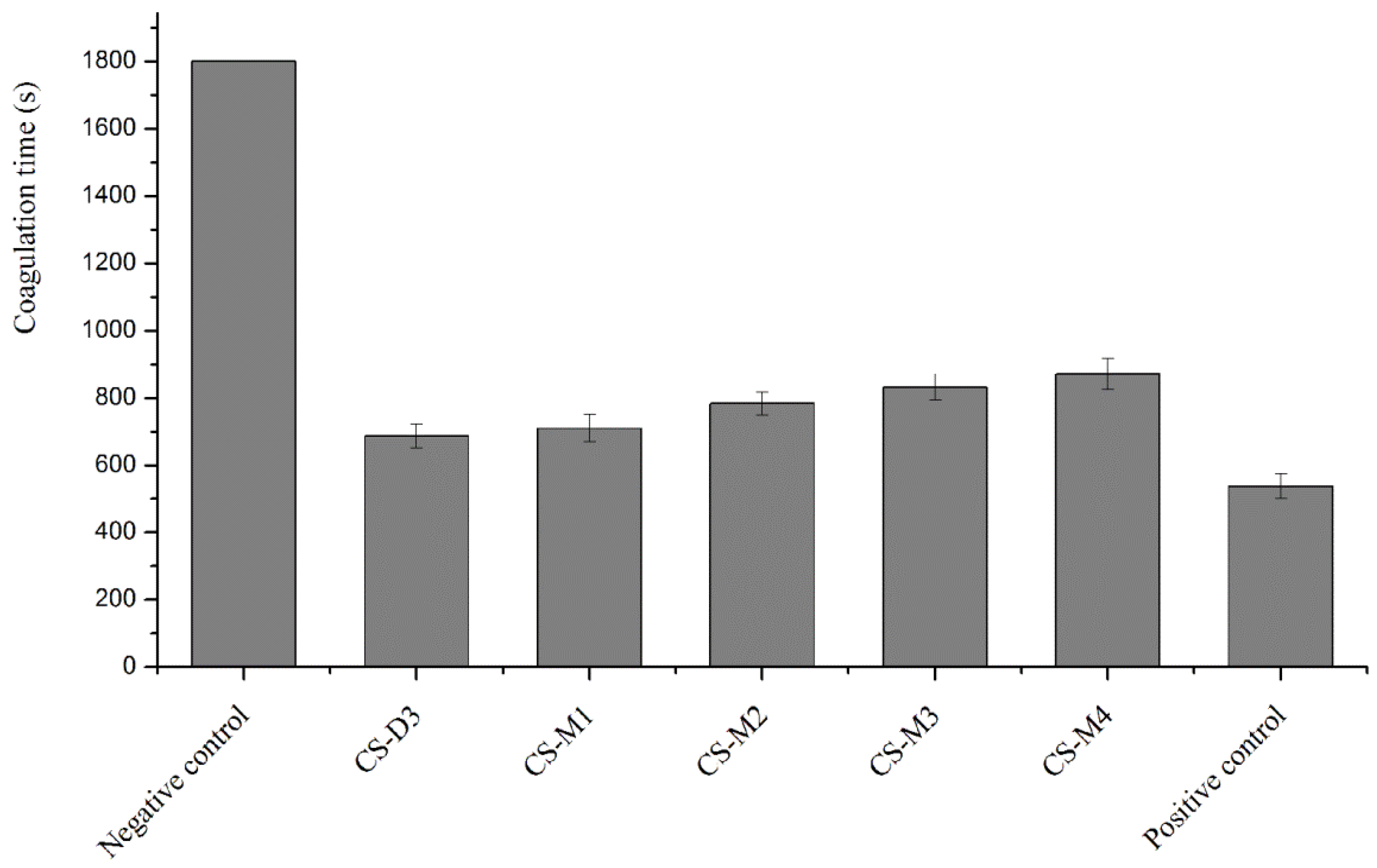
2.4. Effect of MW on the Procoagulant Activity of Chitosan
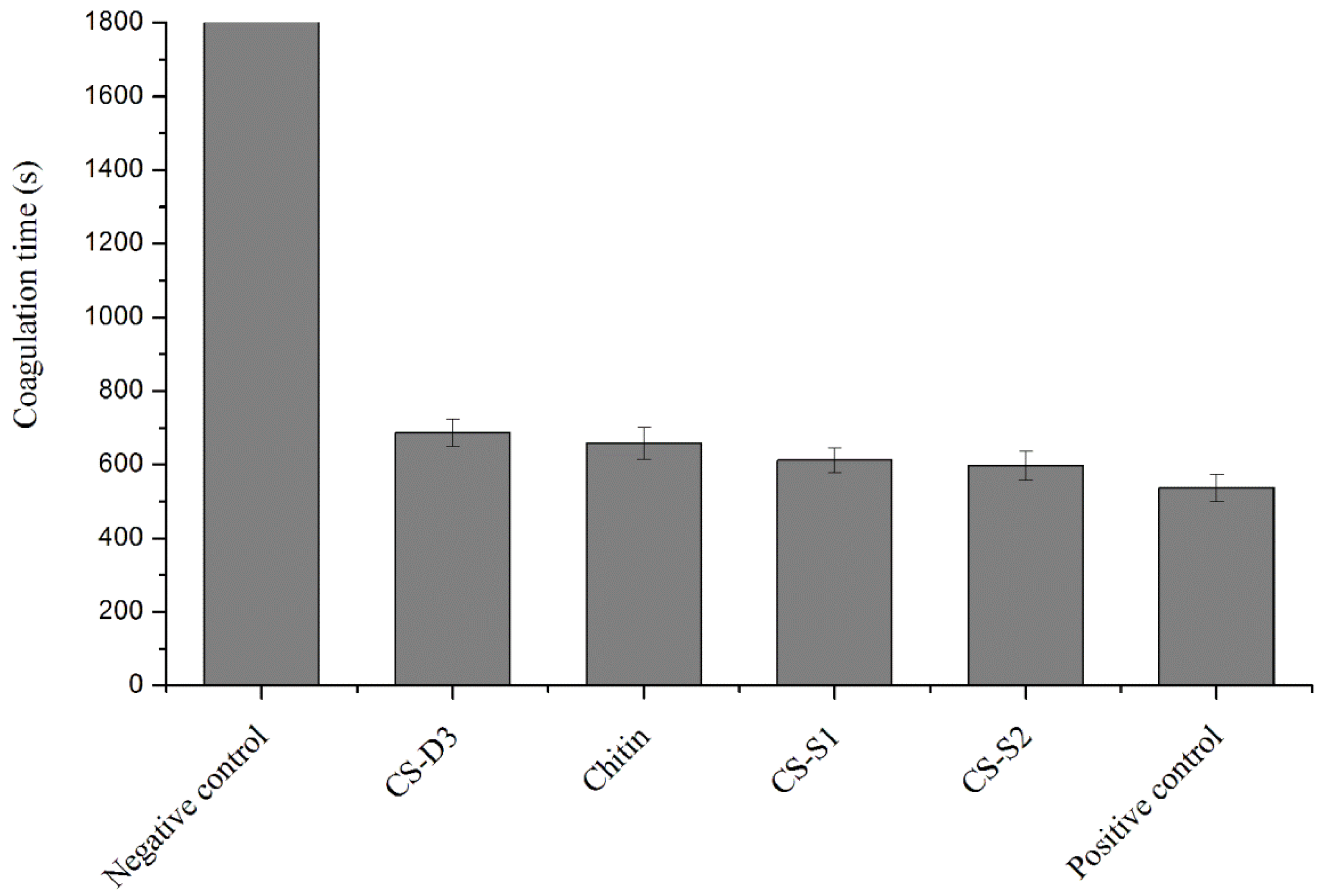
2.5. Effect of SG on the Procoagulant Activity of Chitosan
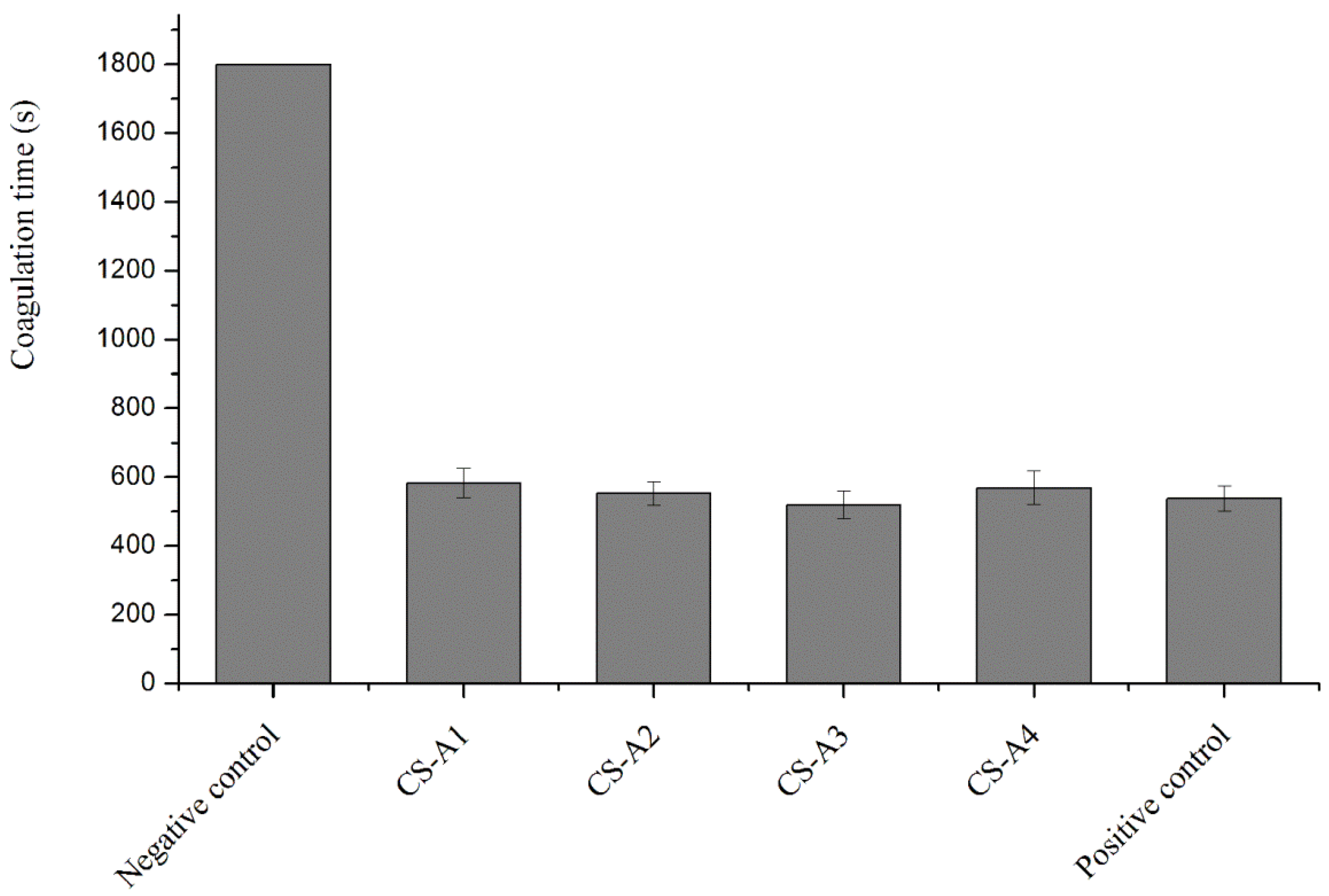
2.6. Effect of Chitosan Acid Salts on the Procoagulant Activity of Chitosan
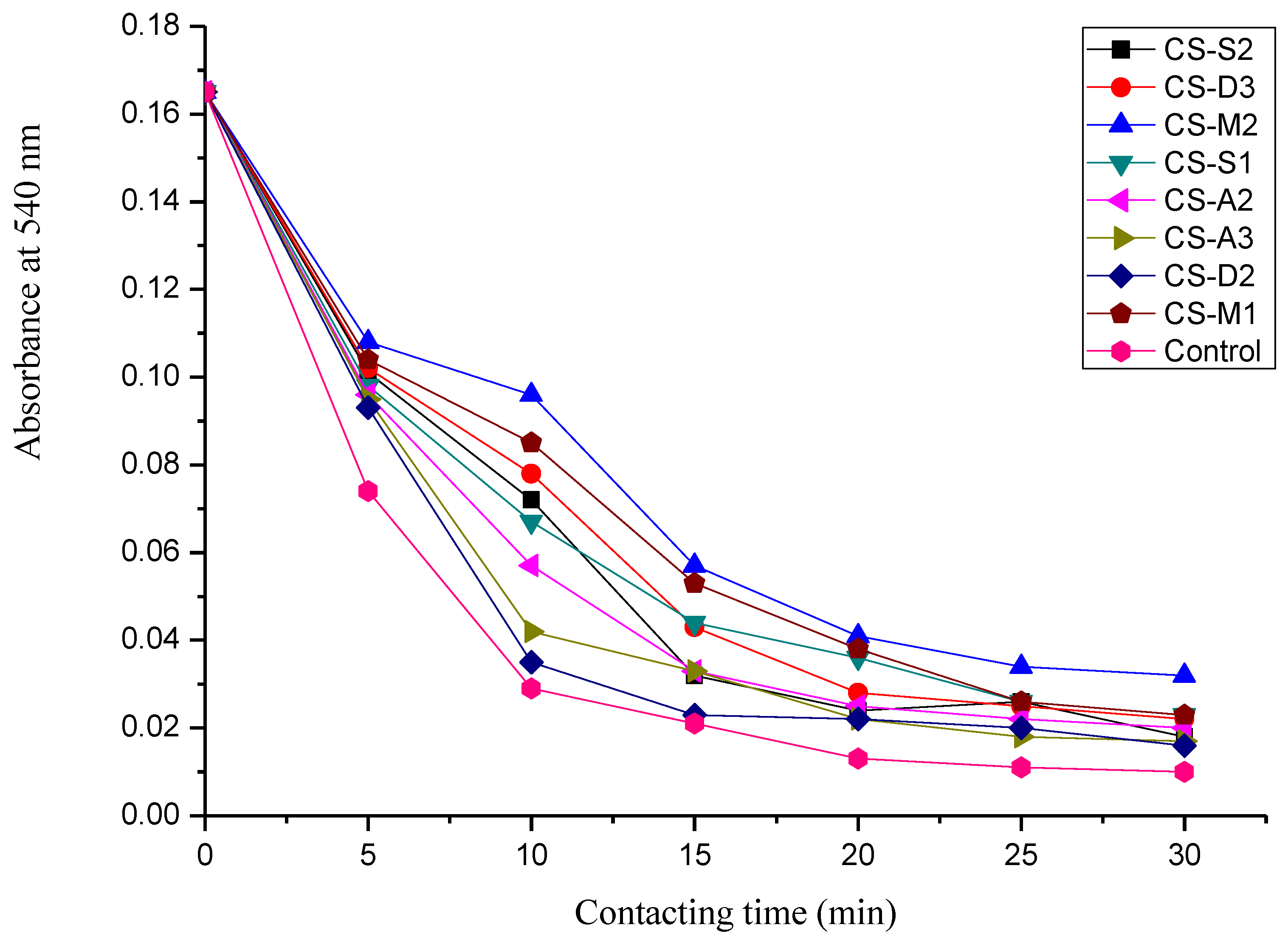
2.7. Dynamic Coagulation Time
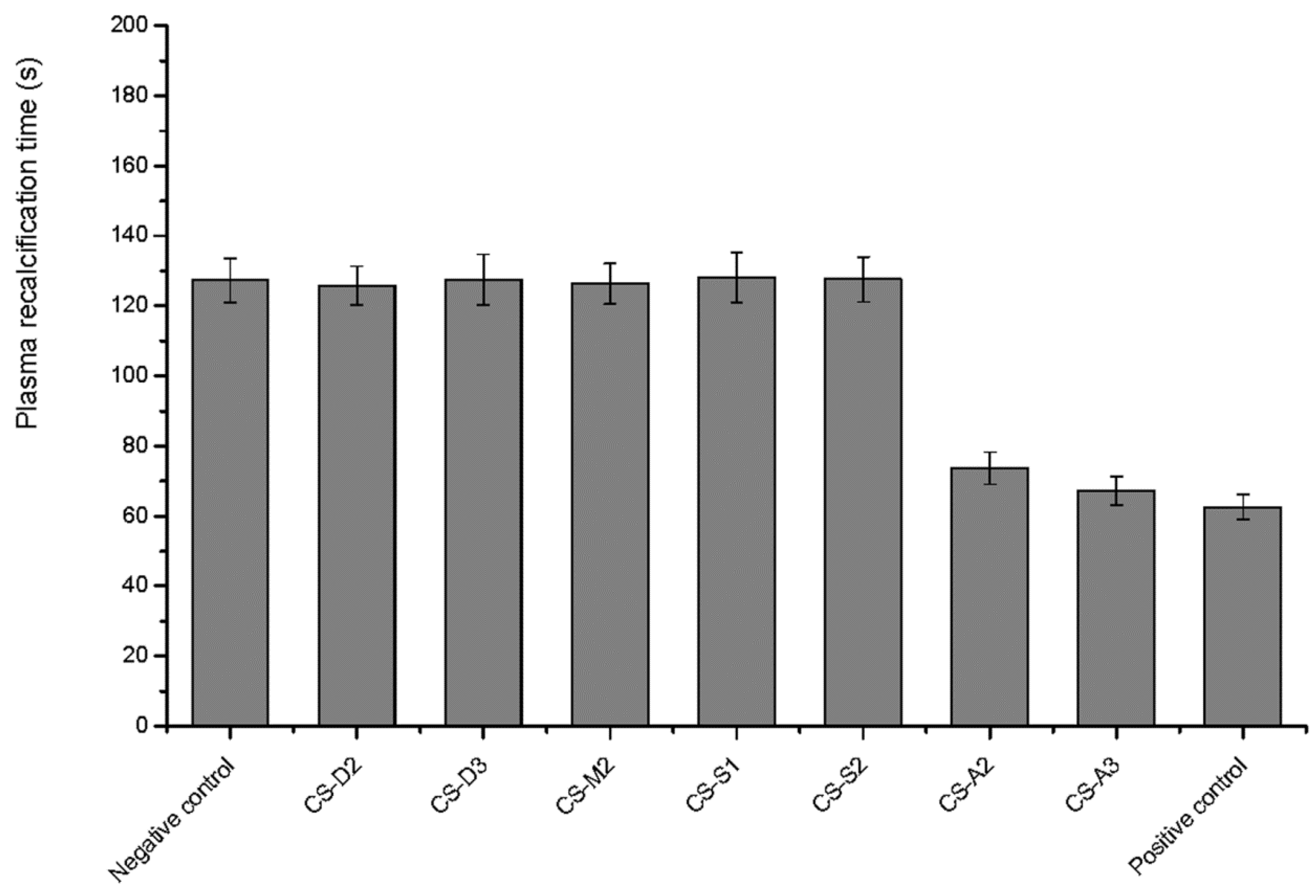
2.8. Plasma Recalcification Time
3. Materials and Methods
3.1. Materials
3.2. Preparation of Chitosan with Different Molecular Parameters
3.2.1. Preparation of Chitosan with Different Degrees of Deacetylation
3.2.2. Preparation of Chitosan with Different Molecular Weights
3.2.3. Preparation of Chitosan by Hydrophilic Modification
3.2.4. Preparation of Chitosan Acid Salts
3.3. Fourier Transform Infrared (FTIR) Spectroscopy
3.4. Procoagulant Activity Assay in Vitro
3.5. Dynamic Blood Coagulation Assay
3.6. Determination of Plasma Recalcification Time
3.7. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Wen, J.; Weinhart, M.; Lai, B.; Kizhakkedathu, J.; Brooks, D.E. Reversible hemostatic properties of sulfabetaine/quaternary ammonium modified hyperbranched polyglycerol. Biomaterials 2016, 86, 42–55. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Guo, B.; Wu, H.; Liang, Y.; Ma, P.X. Injectable antibacterial conductive nanocomposite cryogels with rapid shape recovery for noncompressible hemorrhage and wound healing. Nat. Commun. 2018, 9, 2784. [Google Scholar] [CrossRef] [PubMed]
- Huang, X.; Sun, Y.; Nie, J.; Lu, W.; Yang, L.; Zhang, Z.; Yin, H.; Wang, Z.; Hu, Q. Using absorbable chitosan hemostatic sponges as a promising surgical dressing. Int. J. Biol. Macromol. 2015, 75, 322–329. [Google Scholar] [CrossRef] [PubMed]
- Seo, Y.; Lee, O.; Sultan, M.; Lee, J.; Park, Y.; Yeon, Y.; Lee, J.; Lee, Y.; Kim, S.; Park, C. In vitro and in vivo evaluation of the duck’s feet collagen sponge for hemostatic applications. J. Biomater. Appl. 2017, 32, 484–491. [Google Scholar] [CrossRef] [PubMed]
- Dai, C.; Liu, C.; Jie, W.; Hua, H.; Zhao, Q. Molecular imprinted macroporous chitosan coated mesoporous silica xerogels for hemorrhage control. Biomaterials 2010, 31, 7620–7630. [Google Scholar] [CrossRef] [PubMed]
- Sun, X.; Tang, Z.; Pan, M.; Wang, Z.; Yang, H.; Liu, H. Chitosan/kaolin composite porous microspheres with high hemostatic efficacy. Carbohydr. Polym. 2017, 177, 135–143. [Google Scholar] [CrossRef] [PubMed]
- Pan, H.; Fan, D.; Cao, W.; Zhu, C.; Duan, Z.; Fu, R.; Li, X.; Ma, X. Preparation and Characterization of Breathable Hemostatic Hydrogel Dressings and Determination of Their Effects on Full-Thickness Defects. Polymers 2017, 9, 727. [Google Scholar] [CrossRef]
- Nie, W.; Yuan, X.; Zhao, J.; Zhou, Y.; Bao, H. Rapidly in situ forming chitosan/ε-polylysine hydrogels for adhesive sealants and hemostatic materials. Carbohydr. Polym. 2013, 96, 342–348. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Cheng, F.; Gao, S.; Wu, Z.; Dong, L.; Lin, S.; Luo, Z.; Li, X. Preparation, characterization, antibacterial properties, and hemostatic evaluation of ibuprofen-loaded chitosan/gelatin composite films. J. Appl. Polym. Sci. 2017, 134, 45441. [Google Scholar] [CrossRef]
- Huang, X.; Jia, J.; Wang, Z.; Hu, Q. A Novel Chitosan-based Sponge Coated with Self-assembled Thrombin/Tannic Acid Multilayer Films as a Hemostatic Dressing. Chin. J. Polym. Sci. 2015, 33, 284–290. [Google Scholar] [CrossRef]
- Gu, B.K.; Park, S.J.; Kim, M.S.; Lee, Y.J.; Kim, J.I.; Kim, C.H. Gelatin blending and sonication of chitosan nanofiber mats produce synergistic effects on hemostatic functions. Int. J. Biol. Macromol. 2016, 82, 89–96. [Google Scholar] [CrossRef] [PubMed]
- Knidri, H.E.; Belaabed, R.; Addaou, A.; Laajeb, A.; Lahsini, A. Extraction, chemical modification and characterization of chitin and chitosan. Int. J. Biol. Macromol. 2018, 120, 1181–1189. [Google Scholar] [CrossRef] [PubMed]
- Muxika, A.; Etxabide, A.; Uranga, J.; Guerrero, P.; de la Caba, K. Chitosan as a bioactive polymer: Processing, properties and applications. Int. J. Biol. Macromol. 2017, 105, 1358–1368. [Google Scholar] [CrossRef] [PubMed]
- Rinaudo, M. Chitin and chitosan: Properties and applications. Prog. Polym. Sci. 2006, 31, 603–632. [Google Scholar] [CrossRef]
- Duta, P.K.; Ravikumar, M.N.V.; Dutta, J. Chitin and chitosan for versatile applications. J. Macromol. Sci. Part C Polym. Rev. 2002, 42, 307–354. [Google Scholar] [CrossRef]
- Foster, A.B.; Webber, J.M. Chitin. Adv. Carbohydr. Chem. 1961, 15, 371–393. [Google Scholar]
- Santhosh, S.; Mathew, P.T. Preparation and properties of glucosamine and carboxymethylchitin from shrimp shell. J. Appl. Polym. Sci. 2008, 107, 280–285. [Google Scholar] [CrossRef]
- Pluemsab, W.; Fukazawa, Y.; Furuike, T.; Nodasaka, Y.; Sakairi, N. Cyclodextrin-linked alginate beads as supporting materials for Sphingomonas cloacae, a nonylphenol degrading bacteria. Bioresour. Technol. 2007, 98, 2076–2081. [Google Scholar] [CrossRef] [PubMed]
- Şenel, S.; Kremer, M.J.; Kaş, S.; Wertz, P.W.; Hincal, A.A.; Squier, C.A. Enhancing effect of chitosan on peptide drug delivery across buccal mucosa. Biomaterials 2000, 21, 2067–2071. [Google Scholar] [CrossRef]
- Tanida, F.; Tojima, T.; Han, S.M.; Nishi, N.; Tokura, S.; Sakairi, N.; Seino, H.; Hamada, K. Novel synthesis of a water-soluble cyclodextrin-polymer having a chitosan skeleton. Polymer 1998, 39, 5261–5263. [Google Scholar] [CrossRef]
- Yan, T.; Cheng, F.; Wei, X.; Huang, Y.; He, J. Biodegradable collagen sponge reinforced with chitosan/calcium pyrophosphate nanoflowers for rapid hemostasis. Carbohydr. Polym. 2017, 170, 271–280. [Google Scholar] [CrossRef] [PubMed]
- Li, T.; Lou, C.; Chen, A.; Lee, M.; Ho, T.; Chen, Y.; Lin, J. Highly Absorbent Antibacterial Hemostatic Dressing for Healing Severe Hemorrhagic Wounds. Materials 2016, 9, 793. [Google Scholar] [CrossRef] [PubMed]
- Song, H.F.; Chen, A.Z.; Wang, S.B.; Kang, Y.Q.; Ye, S.F.; Liu, Y.G.; Wu, W.G. Preparation of Chitosan-Based Hemostatic Sponges by Supercritical Fluid Technology. Materials 2014, 7, 2459–2473. [Google Scholar] [CrossRef] [PubMed]
- Rúnarsson, O.V.; Holappa, J.; Nevalainen, T.; Hjálmarsdóttir, M.; Järvinen, T.; Loftsson, T.; Einarsson, J.M.; Jónsdóttir, S.; Valdimarsdóttir, M.; Másson, M. Antibacterial activity of methylated chitosan and chitooligomer derivatives: Synthesis and structure activity relationships. Eur. Polym. J. 2007, 43, 2660–2671. [Google Scholar] [CrossRef]
- Yang, R.; Li, H.; Huang, M.; Yang, H.; Li, A. A review on chitosan-based flocculants and their applications in water treatment. Water Res. 2016, 95, 59–89. [Google Scholar] [CrossRef] [PubMed]
- Sahariah, P.; Gaware, V.S.; Lieder, R.; Jónsdóttir, S.; Hjálmarsdóttir, M.Á.; Sigurjonsson, O.E.; Másson, M. The effect of substituent, degree of acetylation and positioning of the cationic charge on the antibacterial activity of quaternary chitosan derivatives. Mar. Drugs 2014, 12, 4635. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.; Zhou, X.; Yi, J.; Tong, J.; Wu, H.; Fan, L. Preparation and biological activity of quaternized carboxymethyl chitosan conjugated with collagen peptide. Int. J. Biol. Macromol. 2014, 70, 300–305. [Google Scholar] [CrossRef] [PubMed]
- Zhu, C.; Zou, S.; Rao, Z.; Min, L.; Liu, M.; Liu, L.; Fan, L. Preparation and characterization of hydroxypropyl chitosan modified with nisin. Int. J. Biol. Macromol. 2017, 105, 1017–1024. [Google Scholar] [CrossRef] [PubMed]
- Shao, K.; Han, B.; Dong, W.; Song, F.; Liu, W.; Liu, W. Pharmacokinetics and biodegradation performance of a hydroxypropyl chitosan derivative. J. Ocean Univ. China 2015, 14, 888–896. [Google Scholar] [CrossRef]
- Yang, J.; Tian, F.; Wang, Z.; Wang, Q.; Zeng, Y.J.; Chen, S.Q. Effect of chitosan molecular weight and deacetylation degree on hemostasis. J. Biomed. Mater. Res. Part B 2010, 84B, 131–137. [Google Scholar] [CrossRef] [PubMed]
- Edwards, J.V.; Howley, P.; Prevost, N.; Condon, B.; Arnold, J.; Diegelmann, R. Positively and negatively charged ionic modifications to cellulose assessed as cotton-based protease-lowering and hemostatic wound agents. Cellulose 2009, 16, 911–921. [Google Scholar] [CrossRef]
- Zhou, X.; Zhang, X.; Zhou, J.; Li, L. An investigation of chitosan and its derivatives on red blood cell agglutination. Rsc Adv. 2017, 7, 12247–12254. [Google Scholar] [CrossRef]
- Mohammadi, A.; Hashemi, M.; Hosseini, S.M. Effect of chitosan molecular weight as micro and nanoparticles on antibacterial activity against some soft rot pathogenic bacteria. Lwt-Food Sci. Technol. 2016, 71, 347–355. [Google Scholar] [CrossRef]
- Liu, N.; Chen, X.; Park, H.; Liu, C.; Liu, C.; Meng, X.; Yu, L. Effect of MW and concentration of chitosan on antibacterial activity of Escherichia coli. Carbohydr. Polym. 2006, 64, 60–65. [Google Scholar] [CrossRef]
- Li, J.; Wu, Y.; Zhao, L. Antibacterial activity and mechanism of chitosan with ultra high molecular weight. Carbohydr. Polym. 2016, 148, 200–205. [Google Scholar] [CrossRef] [PubMed]
- Klokkevold, P.R.; Fukayama, H.; Sung, E.C.; Bertolami, C.N. The effect of chitosan (poly-N-acetyl glucosamine) on lingual hemostasis in heparinized rabbits. J. Oral Maxillofac. Surg. 1999, 57, 49–52. [Google Scholar] [CrossRef]
- Hattori, H.; Ishihara, M. Changes in blood aggregation with differences in molecular weight and degree of deacetylation of chitosan. Biomed. Mater. 2015, 10, 15014. [Google Scholar] [CrossRef] [PubMed]
- Prabaharan, M. Chitosan derivatives as promising materials for controlled drug delivery. J. Biomater. Appl. 2008, 23, 5–36. [Google Scholar] [CrossRef] [PubMed]
- Periayah, M.H.; Halim, A.S.; Hussein, A.R.; Saad, A.Z.M.; Rashid, A.H.A.; Noorsal, K. In vitro capacity of different grades of chitosan derivatives to induce platelet adhesion and aggregation. Int. J. Biol. Macromol. 2013, 52, 244–249. [Google Scholar] [CrossRef] [PubMed]
- Fischer, T.H.; Connolly, R.; Thatte, H.S.; Schwaitzberg, S.S. Comparison of structural and hemostatic properties of the poly-N-acetyl glucosamine Syvek Patch with products containing chitosan. Microsc. Res. Tech. 2004, 63, 168–174. [Google Scholar] [CrossRef] [PubMed]
- He, Q.; Gong, K.; Ao, Q.; Ma, T.; Yan, Y.; Gong, Y.; Zhang, X. Positive charge of chitosan retards blood coagulation on chitosan films. J. Biomater. Appl. 2013, 27, 1032–1045. [Google Scholar] [CrossRef] [PubMed]
- Beaulieu, C.; Blais, A. Stable solutions having antiviral, antibacterial and hemostatic properties and methods of making thereof. U.S. Patent US 2009,0117,213, 7 May 2009. [Google Scholar]
- Paun, I.; Ion, V.; Luculescu, C.; Dinescu, M.; Canulescu, S.; Schou, J. In vitro studies of PEG thin films with different molecular weights deposited by MAPLE. Appl. Phys. A Mater. Sci. Process. 2012, 109, 223–232. [Google Scholar] [CrossRef]
- Li, L.; Cao, X.; Shen, X.; Yu, S.; Su, F.; Liu, S.; Liu, F.; Xie, C. Alkyl chitosan film-high strength, functional biomaterials. J. Biomed. Mater. Res. Part A 2017, 105, 3034–3041. [Google Scholar]
- Gentry, P.A.; Liptrap, R.M. Comparative hemostatic protein alterations accompanying pregnancy and parturition. Can. J. Physiol. Pharmacol. 1988, 66, 671–678. [Google Scholar] [CrossRef] [PubMed]
- Abraham, S.; So, A.; Unsworth, L. Poly(carboxybetaine methacrylamide)-Modified Nanoparticles: A Model System for Studying the Effect of Chain Chemistry on Film Properties, Adsorbed Protein Conformation, and Clot Formation Kinetics. Biomacromolecules 2011, 12, 3567–3580. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.-A.; Kim, S.; Kim, J.-E.; Gu, J.-Y.; Yoo, H.-R.; Kang, H.-R.; Kim, H. Activation of the Intrinsic Coagulation Pathway in Patients With Chronic Urticaria. Allergy Asthma Immunol. Res. 2015, 7, 476–482. [Google Scholar] [CrossRef] [PubMed]
- Chou, T.; Fu, C.E.; Wu, C.; Yeh, J. Chitosan enhances platelet adhesion and aggregation. Biochem. Biophys. Res. Commun. 2003, 302, 480–483. [Google Scholar] [CrossRef]
- Suzuki, Y.; Okamoto, Y.; Morimoto, M.; Sashiwa, H.; Saimoto, H.; Tanioka, S.I.; Shigemasa, Y.; Minami, S. Influence of physico-chemical properties of chitin and chitosan on complement activation. Carbohydr. Polym. 2000, 42, 307–310. [Google Scholar] [CrossRef]
- Rasti, H.; Parivar, K.; Baharara, J.; Iranshahi, M.; Namvar, F. Chitin from the Mollusc Chiton: Extraction, Characterization and Chitosan Preparation. Iran. J. Pharm. Res. 2017, 16, 366–379. [Google Scholar] [PubMed]
- Huang, Q.Z.; Wang, S.M.; Huang, J.F.; Zhuo, L.H.; Guo, Y.C. Study on the heterogeneous degradation of chitosan with hydrogen peroxide under the catalysis of phosphotungstic acid. Carbohydr. Polym. 2007, 68, 761–765. [Google Scholar] [CrossRef]
- Fan, L.; Zou, S.; Ge, H.; Xiao, Y.; Wen, H.; Feng, H.; Liu, M.; Nie, M. Preparation and characterization of hydroxypropyl chitosan modified with collagen peptide. Int. J. Biol. Macromol. 2016, 93, 636–643. [Google Scholar] [CrossRef] [PubMed]
- Fukuda, T.; Nakashima, Y.; Harada, M.; Toyoshima, S.; Koshitani, O.; Kawaguchi, Y.; Nakayama, M. Effect of whole blood clotting time in rats with ionized hypocalcemia induced by rapid intravenous citrate infusion. J. Toxicol. Sci. 2006, 31, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Gao, A.; Liu, F.; Xue, L. Preparation and evaluation of heparin-immobilized poly (lactic acid) (PLA) membrane for hemodialysis. J. Membr. Sci. 2014, 452, 390–399. [Google Scholar] [CrossRef]
Sample Availability: Samples of the compounds are available from the authors. |

| Chitosan with Different Molecular Parameters | DD (%) | MW (kDa) | DS (%) | Marked | |
|---|---|---|---|---|---|
| Chitosan with different DD | 52.68 | 1010 | - | CS-D1 | |
| 68.36 | 933 | - | CS-D2 | ||
| 81.72 | 891 | - | CS-D3 | ||
| 92.21 | 877 | - | CS-D4 | ||
| Chitosan with different MW | 81.72 | 485 | - | CS-M1 | |
| 81.72 | 212 | - | CS-M2 | ||
| 81.72 | 56 | - | CS-M3 | ||
| 81.72 | 27 | - | CS-M4 | ||
| Chitosan with different SGs | N-Acetyl | 10 | 1150 | 90 | Chitin |
| O-carboxymethyl | - | - | 58.36 | CS-S1 | |
| O-hydroxypropyl | - | - | 63.13 | CS-S2 | |
| Chitosan-acid salts | Chitosan-HI | - | - | - | CS-A1 |
| Chitosan-CH3COOH | - | - | - | CS-A2 | |
| Chitosan-lactic acid | - | - | - | CS-A3 | |
| Chitosan-gentisic acid | - | - | - | CS-A4 | |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hu, Z.; Lu, S.; Cheng, Y.; Kong, S.; Li, S.; Li, C.; Yang, L. Investigation of the Effects of Molecular Parameters on the Hemostatic Properties of Chitosan. Molecules 2018, 23, 3147. https://doi.org/10.3390/molecules23123147
Hu Z, Lu S, Cheng Y, Kong S, Li S, Li C, Yang L. Investigation of the Effects of Molecular Parameters on the Hemostatic Properties of Chitosan. Molecules. 2018; 23(12):3147. https://doi.org/10.3390/molecules23123147
Chicago/Turabian StyleHu, Zhang, Sitong Lu, Yu Cheng, Songzhi Kong, Sidong Li, Chengpeng Li, and Lei Yang. 2018. "Investigation of the Effects of Molecular Parameters on the Hemostatic Properties of Chitosan" Molecules 23, no. 12: 3147. https://doi.org/10.3390/molecules23123147
APA StyleHu, Z., Lu, S., Cheng, Y., Kong, S., Li, S., Li, C., & Yang, L. (2018). Investigation of the Effects of Molecular Parameters on the Hemostatic Properties of Chitosan. Molecules, 23(12), 3147. https://doi.org/10.3390/molecules23123147






