Novel Effective Small-Molecule Antibacterials against Enterococcus Strains
Abstract
1. Introduction
2. Results and Discussion
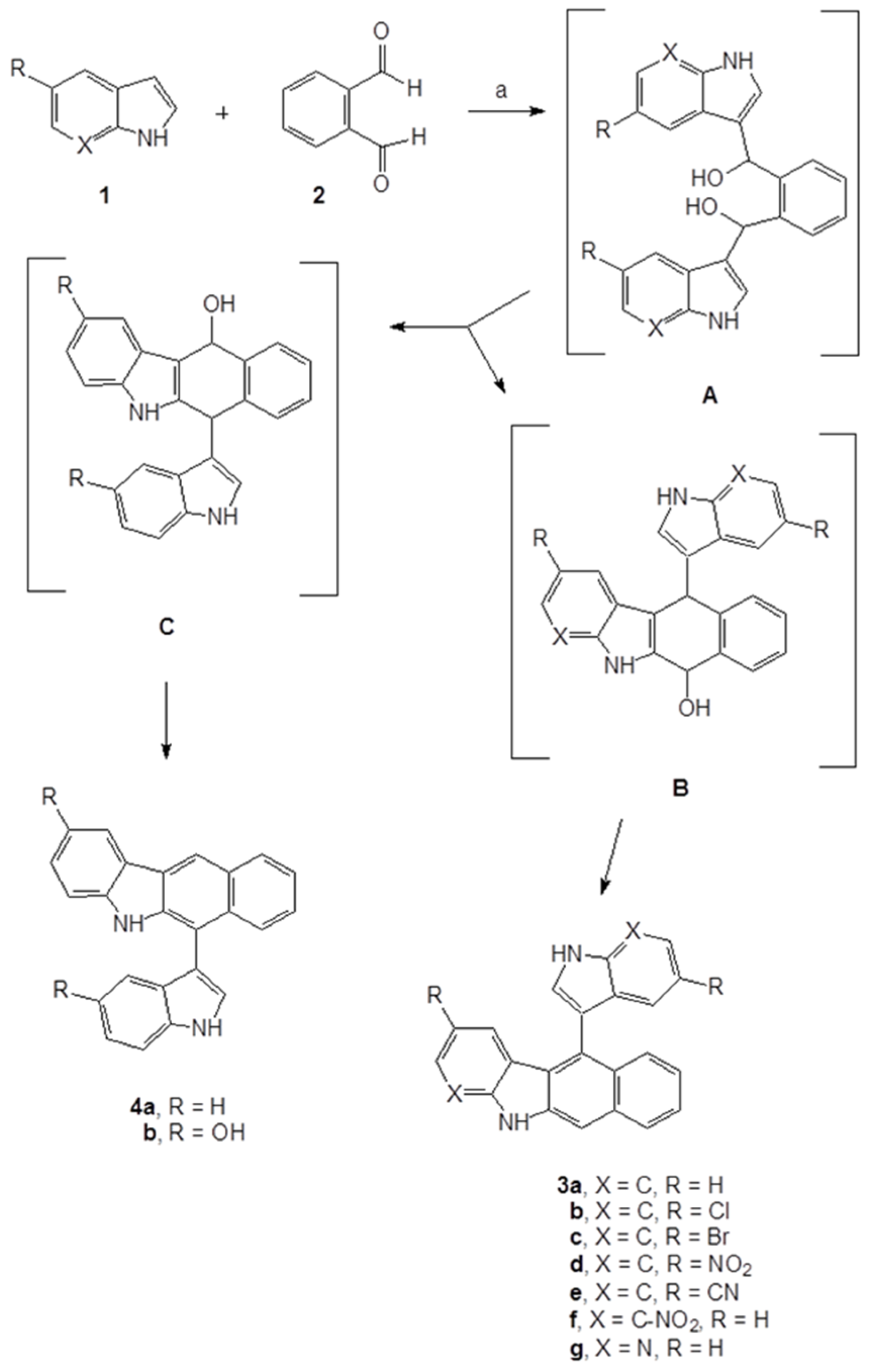
2.1. Synthesis of the Indolyl Benzocarbazoles
2.2. Antimicrobial Activity of the Indolyl Benzocarbazole Types 3 and 4
3. Material and Methods
3.1. Chemical Reagents and Instruments
3.2. General Procedure for the Synthesis of Compounds 3a–g and 4a,b
3.3. Antimicrobial Activity
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References and Note
- Enterococcal Infections. Available online: http://emedicine.medscape.com/article/216993-overview (accerssed on 18 September 2017).
- De Perio, M.A.; Yarnold, P.R.; Warren, J.; Noskin, G.A. Risk factors and outcomes associated with non-Enterococcus faecalis, non-Enterococcus faecium enterococcal bacteremia. Infect. Control Hosp. Epidemiol. 2006, 27, 28–33. [Google Scholar] [CrossRef] [PubMed]
- Ceci, M.; Delpech, G.; Sparo, M.; Mezzina, V.; Sánchez Bruni, S.; Baldaccini, B. Clinical and microbiological features of bacteremia caused by Enterococcus faecalis. J. Infect. Dev. Ctries. 2015, 9, 1195–1203. [Google Scholar] [CrossRef] [PubMed]
- Schmidt-Hieber, M.; Blau, I.W.; Schwartz, S.; Uharek, L.; Weist, K.; Eckmanns, T.; Jonas, D.; Rüden, H.; Thiel, E.; Brandt, C. Intensified strategies to control vancomycin-resistant enterococci in immunocompromised patients. Int. J. Hematol. 2007, 86, 158–162. [Google Scholar] [CrossRef] [PubMed]
- DiazGranados, C.A.; Zimmer, S.M.; Klein, M.; Jernigan, J.A. Comparison of mortality associated with vancomycin-resistant and vancomycin-susceptible enterococcal bloodstream infections: A meta-analysis. Clin. Infect. Dis. 2005, 41, 327–333. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). Vancomycin-resistant Staphylococcus aureus. Morb. Mortal. Wkly. Rep. 2004, 53, 322–332. [Google Scholar]
- Chang, S.; Sievert, D.M.; Hageman, J.C.; Boulton, M.L.; Tenover, F.C.; Downes, F.P.; Shah, S.; Rudrik, J.T.; Pupp, G.R.; Brown, W.J.; et al. Infection with vancomycin-resistant Staphylococcus aureus containing the vanA resistance gene. N. Engl. J. Med. 2003, 348, 1342–1347. [Google Scholar] [CrossRef] [PubMed]
- Deshpande, L.M.; Fritsche, T.R.; Moet, G.J.; Biedenbach, D.J.; Jones, R.N. Antimicrobial resistance and molecular epidemiology of vancomycin-resistant enterococci from North America and Europe: A report from the SENTRY antimicrobial surveillance program. Diagn. Microbiol. Infect. Dis. 2007, 58, 163–170. [Google Scholar] [CrossRef] [PubMed]
- Long, J.K.; Choueiri, T.K.; Hall, G.S.; Avery, R.K.; Sekeres, M.A. Daptomycin-resistant Enterococcus faecium in a patient with acute myeloid leukemia. Mayo Clin. Proc. 2005, 80, 1215–1216. [Google Scholar] [CrossRef] [PubMed]
- Abdallah, E.M. Plants: An alternative source for antimicrobials. J. Appl. Pharm. Sci. 2011, 1, 16–20. [Google Scholar]
- Imhoff, J.F. Natural Products from Marine Fungi—Still an Underrepresented Resource. Mar. Drugs 2016, 14, 19. [Google Scholar] [CrossRef] [PubMed]
- Biswas, K.; Paul, D.; Sinha, S.N. Marine Bacteria: A Potential Tool for Antibacterial Activity. J. Appl. Environ. Microbiol. 2016, 4, 25–29. [Google Scholar]
- Xu, S.; Nijampatman, B.; Dutta, S.; Velu, S.E. Cyanobacterial Metabolite Calothrixins: Recent Advances in Synthesis and Biological Evaluation. Mar. Drugs 2016, 14, 17. [Google Scholar] [CrossRef] [PubMed]
- Doi, T.; Numajiri, Y.; Takahashi, T.; Takagi, M.; Shin-Ya, K. Solid-phase total synthesis of (−)-apratoxin A and its analogues and their biological evaluation. Chem. Asian J. 2011, 6, 180–188. [Google Scholar] [CrossRef] [PubMed]
- Doan, N.T.; Stewart, R.; Smith, G.D. Inhibition of bacterial RNA polymerase by the cyanobacterial metabolites 12-epi-hapalindole E isonitrile and calothrixin A. FEMS Microbiol. Lett. 2001, 196, 135–139. [Google Scholar] [CrossRef] [PubMed]
- Yudin, L.G.; Pavlyuchenko, A.I.; Budylin, V.A.; Minkin, V.P.I.; Kost, A.N. Nitration of 3-Acylindoles. Khim. Geterotsikl. Soedin. 1971, 11, 1506–1511. [Google Scholar]
- Spectroscopical data of intermediate compound B with X = N and R = H. 5-(1H-pyrrolo[2,3-b]pyridine-3-yl)-10,11-dihydro-5H-benzo[f]pyrido[2,3-b]indol-10-ol. Yield 10%; mp 285–290 °C; IR (ATR) ν = 3128 (NH), 1687 (C=N) cm−1; 1H-NMR (DMSO-d6) δ = 13.04 (s, 1H, NH), 11.15 (s, 1H, NH), 8.34 (m, 1H), 8.14 (m, 1H), 7.84 (m, 1H), 7.60 (m, 1H), 7.46 (m, 5H), 7.22 (m, 2H), 6.90 (m, 1H), 6.42 (m, 1H), 5.95 (s, 1H, OH); m/z (ESI) 335.7 (M + H+).
- Guangzhi, X.; Yuzhen, W.; Zhuting, W.; Qifeng, S.; Youqi, T. The Nuclear Magnetic Resonances of Carbazole Derivatives. Sci. Sin. 1980, 23, 6–10. [Google Scholar]
- Ike, Y.; Craig, R.A.; White, B.A.; Yagi, Y.; Clewell, D.B. Modification of Streptococcus faecalis sex pheromones after acquisition of plasmid DNA. Proc. Natl. Acad. Sci. USA 1983, 80, 5369–5373. [Google Scholar] [CrossRef] [PubMed]
- Jacob, A.E.; Hobbs, S.J. Conjugal transfer of plasmid-borne multiple antibiotic resistance in Streptococcus faecalis var. zymogenes. J. Bacteriol. 1974, 117, 360–372. [Google Scholar] [PubMed]
- Riedl, S.; Ohlsen, K.; Werner, G.; Witte, W.; Hacker, J. Impact of flavophospholipol and vancomycin on conjugational transfer of vancomycin resistance plasmids. Antimicrob. Agents Chemother. 2000, 44, 3189–3192. [Google Scholar] [CrossRef] [PubMed]
- Klare, I.; Heier, H.; Claus, H.; Witte, W. Environmental strains of Enterococcus faecium with inducible high-level resistance to glycopeptides. FEMS Microbiol. Lett. 1993, 106, 23–29. [Google Scholar] [CrossRef] [PubMed]
Sample Availability: Samples of the compounds are not available from the authors. |
| MIC (μM) | ||||
|---|---|---|---|---|
| Compound | E. faecalis OG1X | E. faecalis JH2-2 | E. faecium 2121198 | E. faecium AW2VR 1 |
| 3a | 386 | 386 | 6 | 48 |
| 3b | 319 | 20 | 2 | 319 |
| 3c | 261 | 16 | 1 | 261 |
| 3d | 19 | 19 | 607 | 303 |
| 3e | 42 | 10 | 10 | 166 |
| 3f | 303 | 607 | 607 | 303 |
| 3g | 48 | 767 | 24 | 383 |
| 4a | 12 | 24 | 6 | 12 |
| 4b | 11 | 44 | 5 | 22 |
| Vancomycin | 1 | 1 | 1 | n.d. 2 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ashraf, K.; Yasrebi, K.; Hertlein, T.; Ohlsen, K.; Lalk, M.; Hilgeroth, A. Novel Effective Small-Molecule Antibacterials against Enterococcus Strains. Molecules 2017, 22, 2193. https://doi.org/10.3390/molecules22122193
Ashraf K, Yasrebi K, Hertlein T, Ohlsen K, Lalk M, Hilgeroth A. Novel Effective Small-Molecule Antibacterials against Enterococcus Strains. Molecules. 2017; 22(12):2193. https://doi.org/10.3390/molecules22122193
Chicago/Turabian StyleAshraf, Kerolos, Kaveh Yasrebi, Tobias Hertlein, Knut Ohlsen, Michael Lalk, and Andreas Hilgeroth. 2017. "Novel Effective Small-Molecule Antibacterials against Enterococcus Strains" Molecules 22, no. 12: 2193. https://doi.org/10.3390/molecules22122193
APA StyleAshraf, K., Yasrebi, K., Hertlein, T., Ohlsen, K., Lalk, M., & Hilgeroth, A. (2017). Novel Effective Small-Molecule Antibacterials against Enterococcus Strains. Molecules, 22(12), 2193. https://doi.org/10.3390/molecules22122193






