Bioactive ZnO Coatings Deposited by MAPLE—An Appropriate Strategy to Produce Efficient Anti-Biofilm Surfaces
Abstract
:1. Introduction
2. Results
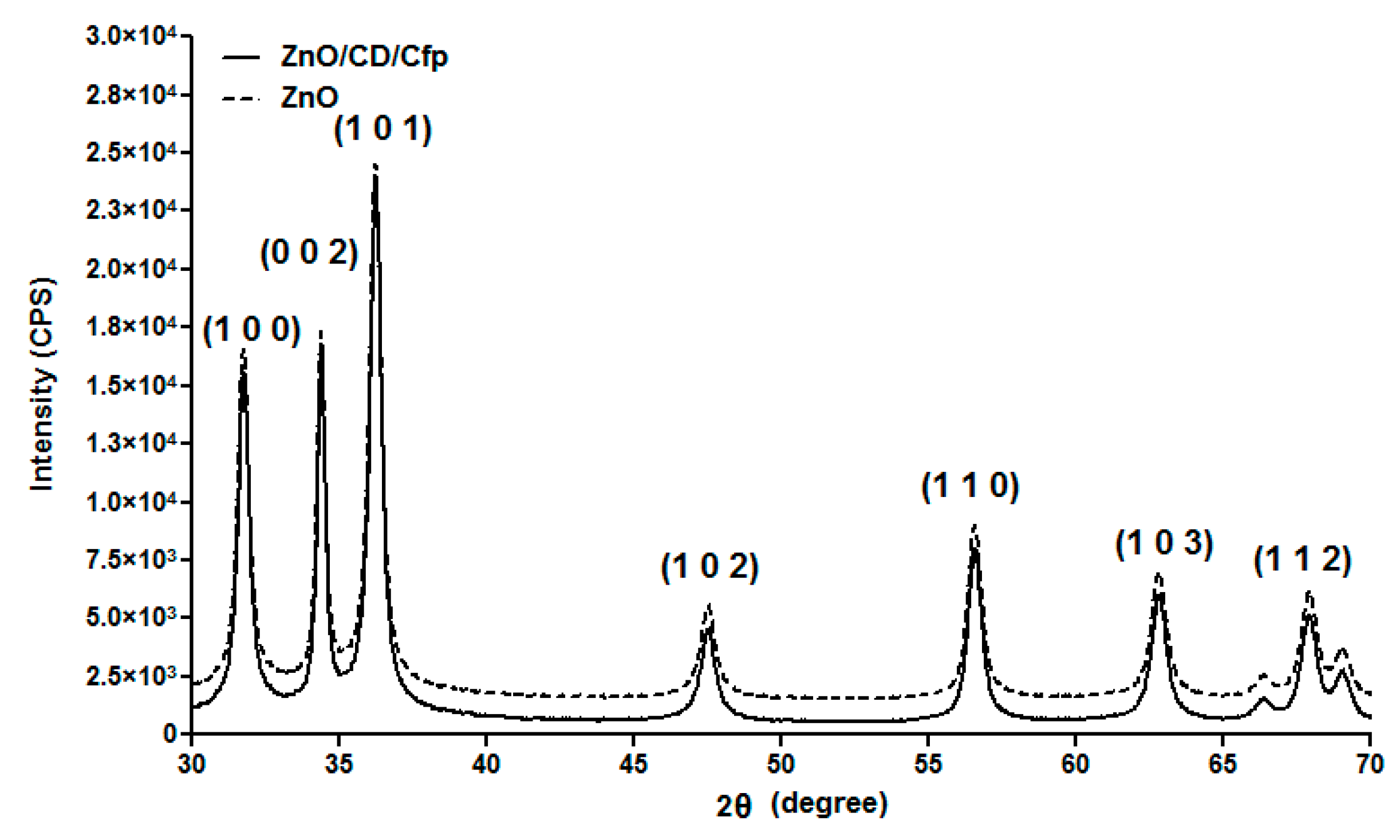
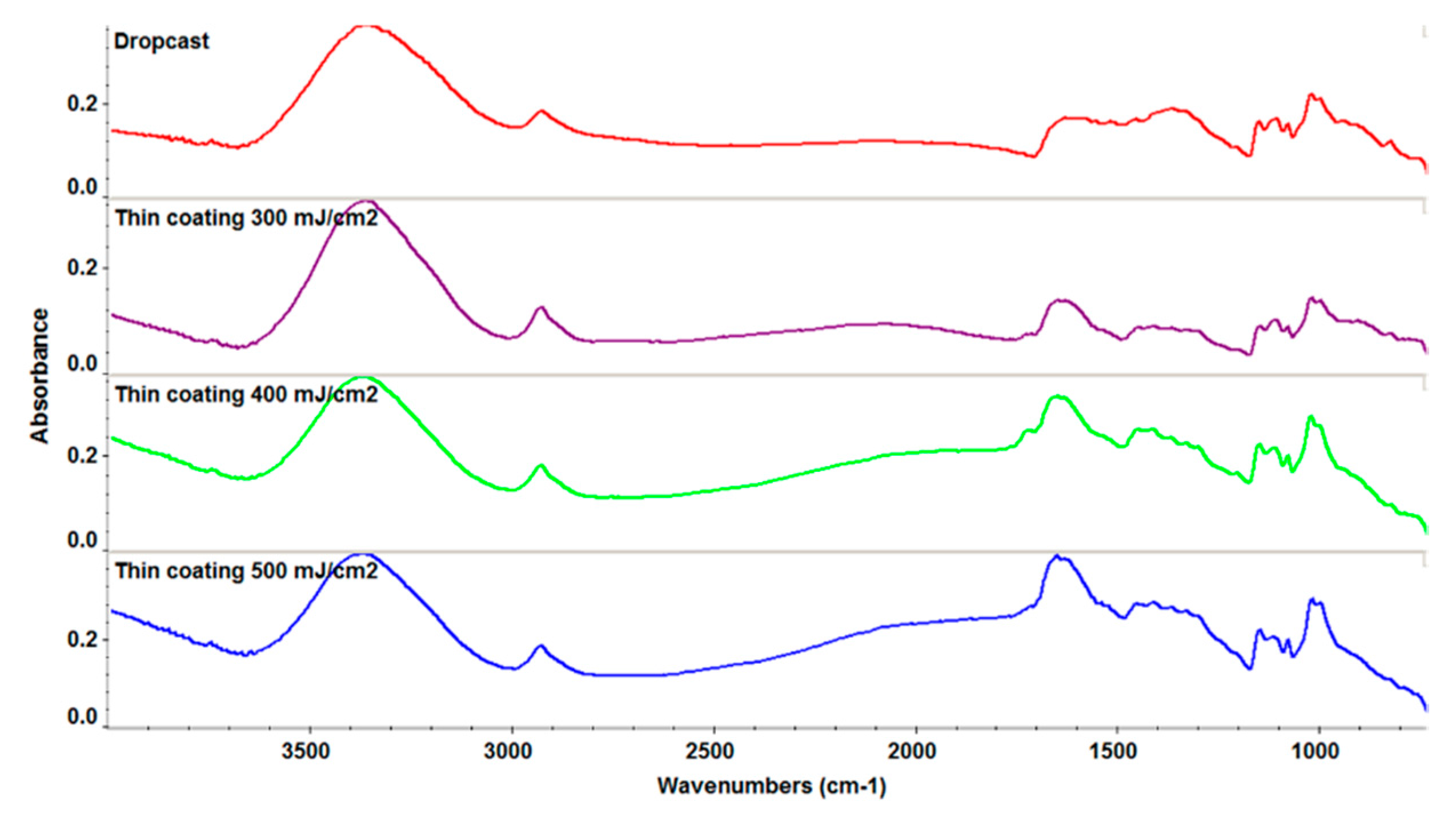
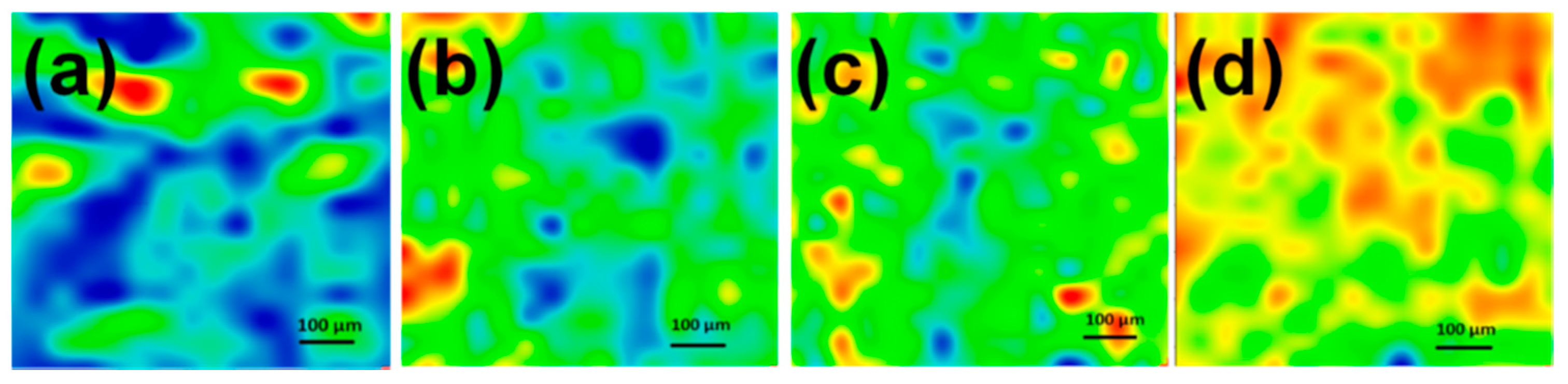


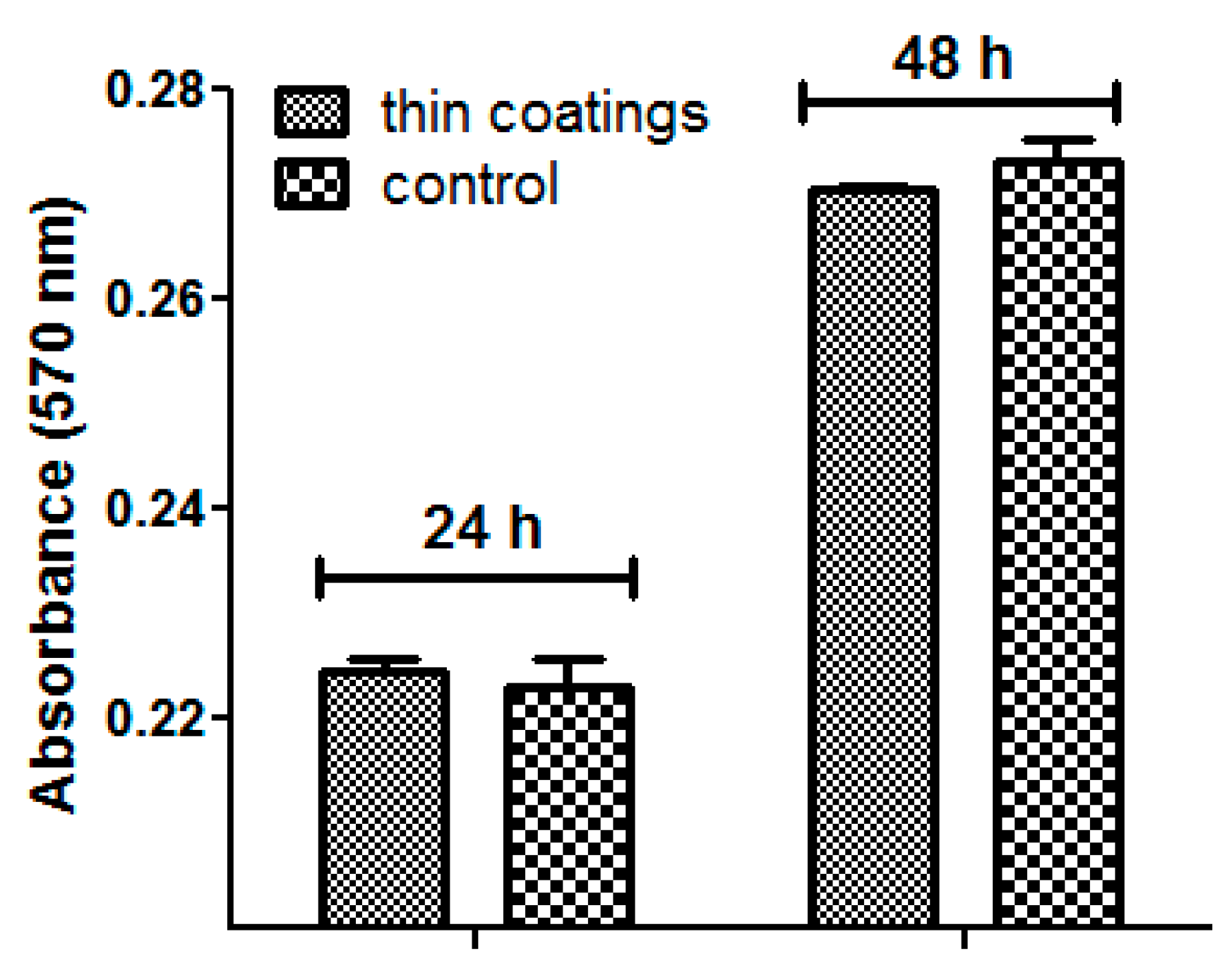
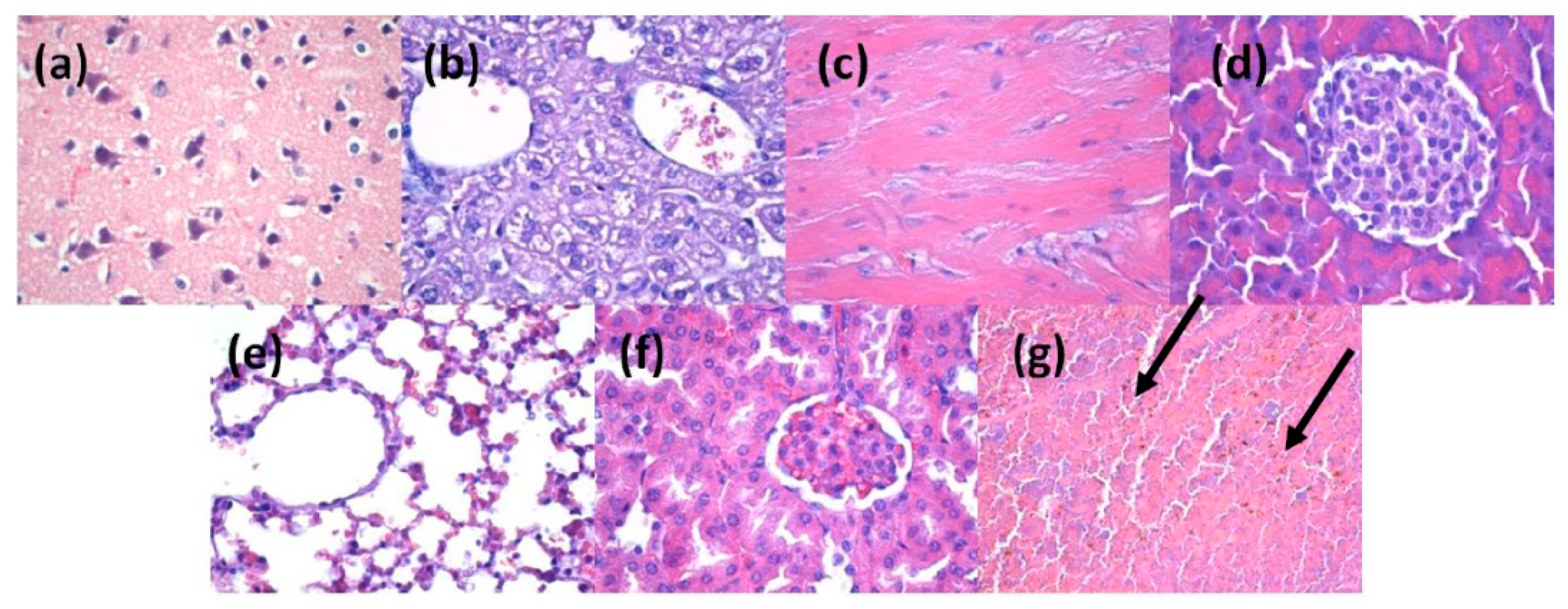
In Vivo Biocompatibility Assay


3. Materials and Methods
3.1. Materials
3.2. Preparation of ZnO/CD/Cfp
3.3. MAPLE Experiment
3.4. Characterization Methods
3.5. Biocompatibility
3.5.1. MTT Test (Using CellTiter 96® Non-Radioactive Cell Proliferation Assay, Promega, Madison, WI, USA)
3.5.2. CellTracker™ Red CMTPX Assay
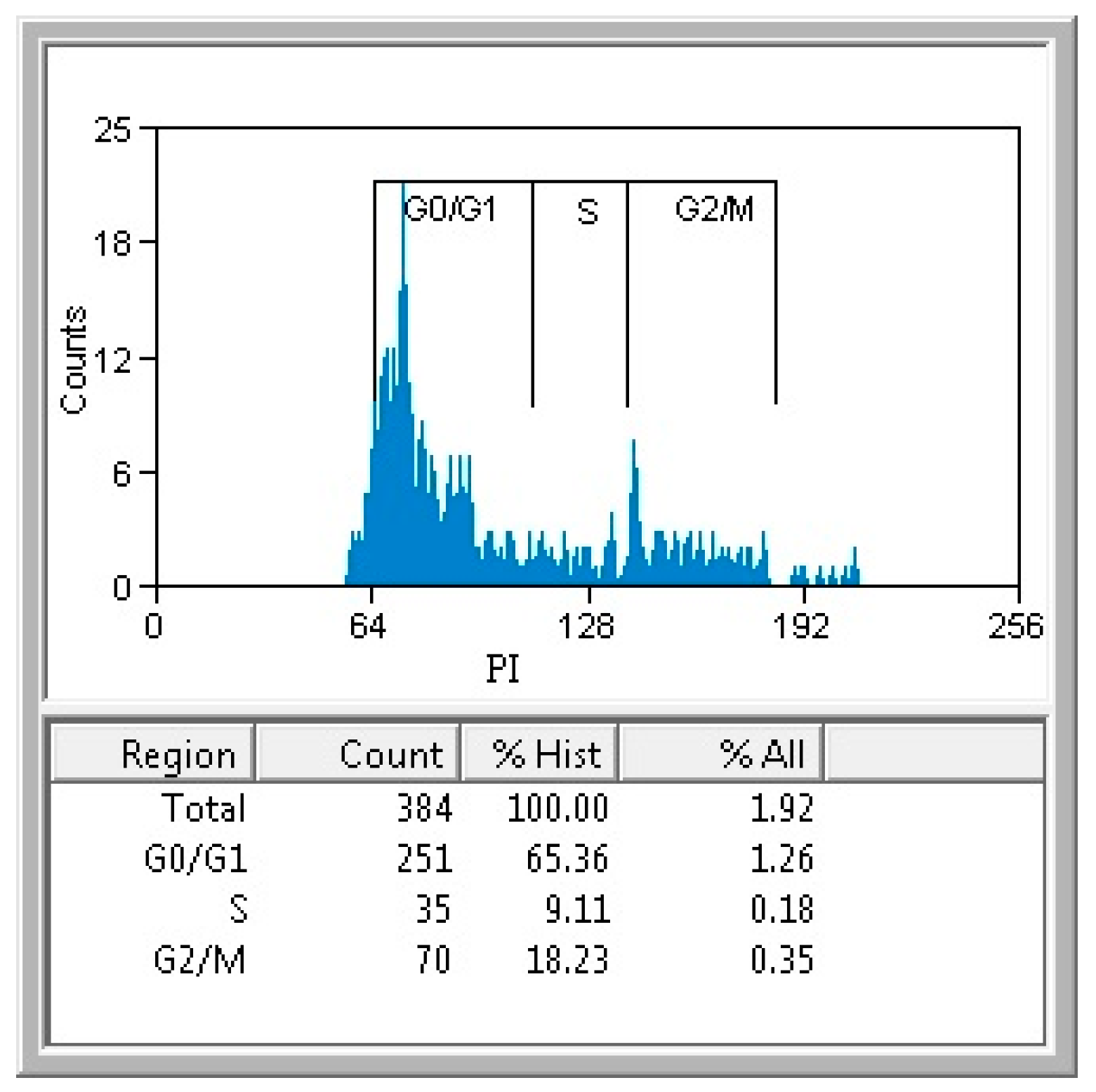
3.6. Analysis of Cell Cycleby Flow Cytometry Using Propidium Iodide
3.7. In Vivo Biocompatibility and Biodistribution of Nanostructures
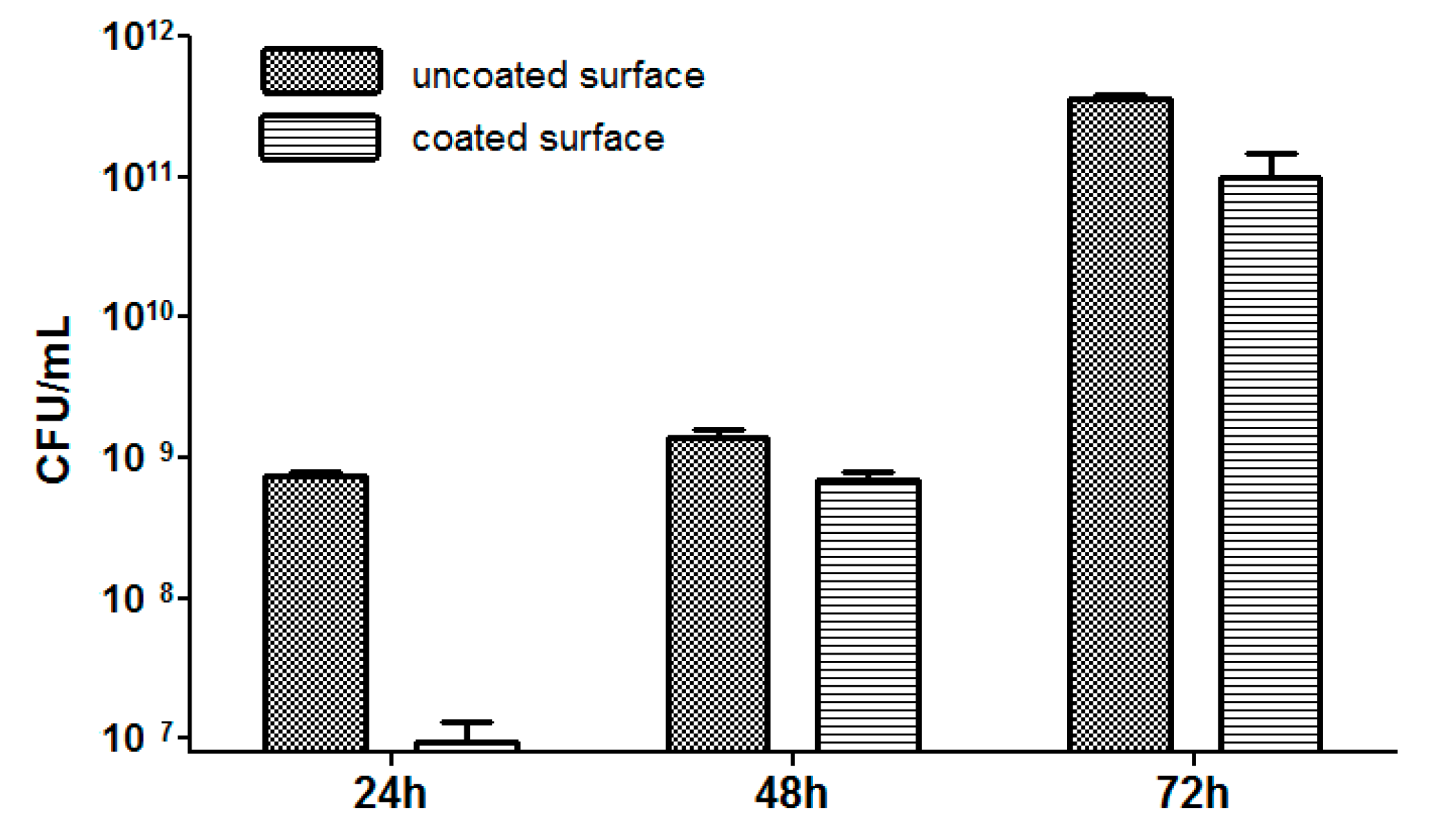
3.8. In Vitro Biofilm Assay
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Limban, V.; Grumezescu, A.M.; Chifiriuc, M.C. Thiourea Derivatives as Antimicrobials: Synthesis, Biological Activity and Potentiation by Nanotechnological Solutions; Lambert Academic Publishing: Saarbrücken, Germany, 2013. [Google Scholar]
- Rawat, D.; Nair, D. Extended-Spectrum β-Lactamases in Gram Negative Bacteria. J. Glob. Infect. Dis. 2010, 2, 263–274. [Google Scholar] [CrossRef] [PubMed]
- Eftekhar, F.; Naseh, Z. Extended-spectrum β-lactamase and carbapenemase production among burn and non-burn clinical isolates of Klebsiella pneumonia. Iran J. Microbiol. 2015, 7, 144–149. [Google Scholar] [PubMed]
- Boucher, H.W.; Talbot, G.H.; Bradley, J.S.; Edwards, J.E.; Gilbert, D.; Rice, L.B.; Scheld, M.; Spellberg, B.; Bartlett, J. Bad Bugs, No Drugs: No ESKAPE! An Update from the Infectious Diseases Society of America. Clin. Infect. Dis. 2009, 48, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Pasquet, Y.; Chevalier, E.; Couval, E.; Bouvier, D.; Bolzinger, M.A. Zinc oxide as a new antimicrobial preservative of topical products: Interactions with common formulation ingredients. Int. J. Pharm. 2015, 479, 88–95. [Google Scholar] [CrossRef] [PubMed]
- Pasquet, J.; Chevalier, Y.; Couval, E.; Bouvier, D.; Noizet, G.; Morlière, C.; Bolzinger, M.A. Antimicrobial activity of zinc oxide particles on five micro-organisms of the Challenge Tests related to their physicochemical properties. Int. J. Pharm. 2014, 460, 92–100. [Google Scholar] [CrossRef] [PubMed]
- Petrochenko, P.E.; Skoog, S.A.; Zhang, Q.; Comstock, D.J.; Elam, J.W.; Goering, P.L.; Narayan, R.J. Cytotoxicity of cultured macrophages exposed to antimicrobial zinc oxide (ZnO) coatings on nanoporous aluminum oxide membranes. Biomatter 2013, 3. [Google Scholar] [CrossRef] [PubMed]
- Brewster, M.E.; Loftsson, T. Cyclodextrins as pharmaceutical solubilizers. Adv. Drug Deliv. Rev. 2007, 59, 645–666. [Google Scholar] [CrossRef] [PubMed]
- Loftsson, T.; Brewster, M.E. Pharmaceutical applications of cyclodextrins. 1. Drug solubilization and stabilization. J. Pharm. Sci. 1996, 85, 1017–1125. [Google Scholar] [CrossRef] [PubMed]
- Mura, P. Analytical techniques for characterization of cyclodextrin complexes in the solid state: A review. J. Pharm. Biomed. Anal. 2015, 113, 226–238. [Google Scholar] [CrossRef] [PubMed]
- Loftsson, T.; Brewster, M.E. Cyclodextrins as functional excipients: Methods to enhance complexation efficiency. J. Pharm. Sci. 2012, 101, 3019–3032. [Google Scholar] [CrossRef] [PubMed]
- Nardello-Rataj, V.; Leclercq, L. Encapsulation of biocides by cyclodextrins: Toward synergistic effects against pathogens. Beilstein J. Org. Chem. 2014, 10, 2603–2622. [Google Scholar] [CrossRef] [PubMed]
- Selvam, S.; Gandhi, R.R.; Suresh, J.; Gowri, S.; Ravikumar, S.; Sundrarajan, M. Antibacterial effect of novel synthesized sulfated-cyclodextrin crosslinked cotton fabric and its improved antibacterial activities with ZnO, TiO2 and Ag nanoparticles coating. Int. J. Pharm. 2012, 434, 366–374. [Google Scholar] [CrossRef] [PubMed]
- Rice, L.B. Federal Funding for the Study of Antimicrobial Resistance in Nosocomial Pathogens: No ESKAPE. J. Infect. Dis. 2008, 197, 1079–1081. [Google Scholar] [CrossRef] [PubMed]
- Hall-Stoodley, L.; Costerton, J.W.; Stoodley, P. Bacterial biofilms: From the natural environment to infectious diseases. Nat. Rev. Microbiol. 2004, 2, 95–108. [Google Scholar] [CrossRef] [PubMed]
- Blango, M.G.; Mulvey, M.A. Persistence of uropathogenic Escherichia coli in the face of multiple antibiotics. Antimicrob. Agents Chemother. 2010, 54, 1855–1863. [Google Scholar] [CrossRef] [PubMed]
- Bai, X.; Lin, L.; Liu, H.; Tan, L.; Liu, T.; Meng, X. Solvothermal Synthesis of ZnO Nanoparticles and Anti-Infection Application in Vivo. ACS Appl. Mater. Interfaces 2015, 7, 1307–1317. [Google Scholar] [CrossRef] [PubMed]
- Kumar, R.; Anandan, S.; Hembram, K.; Rao, T.N. Efficient ZnO-Based Visible-Light-Driven Photocatalyst for Antibacterial Applications. ACS Appl. Mater. Interfaces 2014, 6, 13138–13148. [Google Scholar] [CrossRef] [PubMed]
- Fufă, M.O.M.; Mihaiescu, D.E.; Mogoantă, L.; Bălşeanu, T.A.; Mogoşanu, G.D.; Grumezescu, A.M.; Bolocan, A. In vivo biodistribution of CNTs using a BALB/c mouse experimental model. Rom. J. Morphol. Embryol. 2015, 56, 1481–1493. [Google Scholar] [PubMed]
- Istrate, C.M.; Holban, A.M.; Grumezescu, A.M.; Mogoantă, L.; Mogoşanu, G.D.; Savopol, T.; Moisescu, M.; Iordache, M.; Vasile, B.Ş.; Kovacs, E. Iron oxide nanoparticles modulate the interaction of different antibiotics with cellular membranes. Rom. J. Morphol. Embryol. 2014, 55, 849–856. [Google Scholar]
- Grumezescu, V.; Socol, G.; Grumezescu, A.M.; Holban, A.M.; Ficai, A.; Truşcǎ, R.; Bleotu, C.; Balaure, P.C.; Cristescu, R.; Chifiriuc, M.C. Functionalized antibiofilm thin coatings based on PLA-PVA microspheres loaded with usnic acid natural compounds fabricated by MAPLE. Appl. Surf. Sci. 2014, 302, 262–267. [Google Scholar] [CrossRef]
- Sample Availability: Samples of the compounds presented in the manuscript are available from the authors.
© 2016 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oprea, A.E.; Pandel, L.M.; Dumitrescu, A.M.; Andronescu, E.; Grumezescu, V.; Chifiriuc, M.C.; Mogoantă, L.; Bălşeanu, T.-A.; Mogoşanu, G.D.; Socol, G.; et al. Bioactive ZnO Coatings Deposited by MAPLE—An Appropriate Strategy to Produce Efficient Anti-Biofilm Surfaces. Molecules 2016, 21, 220. https://doi.org/10.3390/molecules21020220
Oprea AE, Pandel LM, Dumitrescu AM, Andronescu E, Grumezescu V, Chifiriuc MC, Mogoantă L, Bălşeanu T-A, Mogoşanu GD, Socol G, et al. Bioactive ZnO Coatings Deposited by MAPLE—An Appropriate Strategy to Produce Efficient Anti-Biofilm Surfaces. Molecules. 2016; 21(2):220. https://doi.org/10.3390/molecules21020220
Chicago/Turabian StyleOprea, Alexandra Elena, Loredana Mihaela Pandel, Ana Maria Dumitrescu, Ecaterina Andronescu, Valentina Grumezescu, Mariana Carmen Chifiriuc, Laurenţiu Mogoantă, Tudor-Adrian Bălşeanu, George Dan Mogoşanu, Gabriel Socol, and et al. 2016. "Bioactive ZnO Coatings Deposited by MAPLE—An Appropriate Strategy to Produce Efficient Anti-Biofilm Surfaces" Molecules 21, no. 2: 220. https://doi.org/10.3390/molecules21020220
APA StyleOprea, A. E., Pandel, L. M., Dumitrescu, A. M., Andronescu, E., Grumezescu, V., Chifiriuc, M. C., Mogoantă, L., Bălşeanu, T.-A., Mogoşanu, G. D., Socol, G., Grumezescu, A. M., Iordache, F., Maniu, H., Chirea, M., & Holban, A. M. (2016). Bioactive ZnO Coatings Deposited by MAPLE—An Appropriate Strategy to Produce Efficient Anti-Biofilm Surfaces. Molecules, 21(2), 220. https://doi.org/10.3390/molecules21020220










