Antiparasitic Activity of Natural and Semi-Synthetic Tirucallane Triterpenoids from Schinus terebinthifolius (Anacardiaceae): Structure/Activity Relationships
Abstract
:1. Introduction
2. Results and Discussion
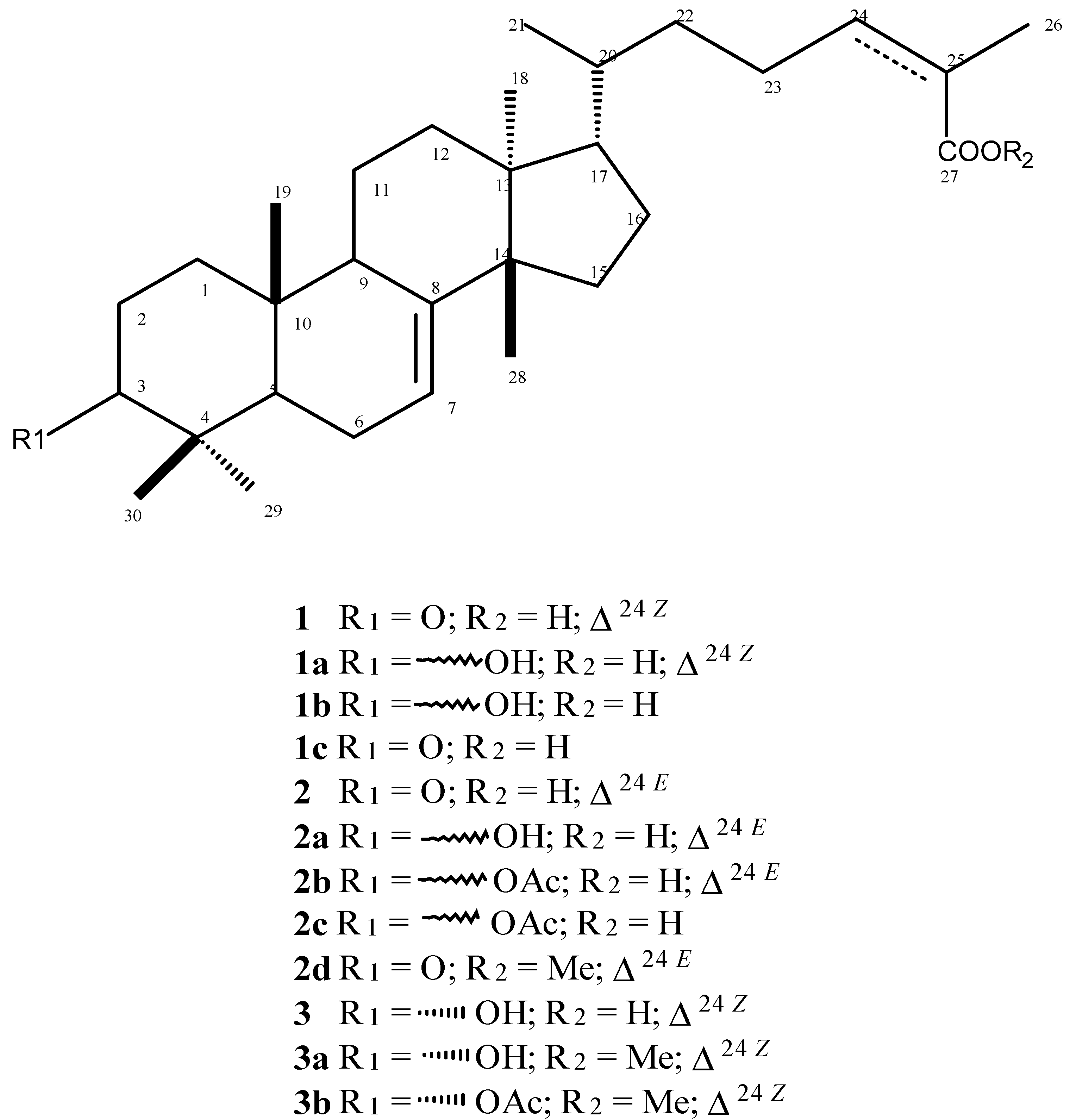
| IC50 (g/mL) a CI95% | CC50 (μg/mL) b CI95% | SI | ||||
| Compounds | L. infantum | L. infantum | T. cruzi | NCTC | AMAc | TRYd |
| Promastigotes | Amastigotes | Trypomastigotes | ||||
| 1 | NA | 66.51 (47.68–92.79) | NA | >200 | >3 | – |
| 1a | NA | NA | 20.18 (16.70–24.39) | 69.50 (64.01–75.45) | – | 3.4 |
| 1b | NA | NA | 17.64 (15.97-19.50) | 76.39 (70.02-83.33) | – | 4.3 |
| 1c | NA | NA | NA | >200 | – | – |
| 2 | NA | 64.90 (41.48–101.50) | 15.75 (9.80–25.30) | 96.48 (77.38–120.30) | 1.5 | 6.1 |
| 2a | NA | 97.59 (89.82–106.00) | 29.59 (25.61–34.18) | 95.49 (65.22–139.80) | 1.0 | 3.2 |
| 2b | NA | NA | 58.36 (42.82–79.55) | 69.31 (38.74–82.64) | – | 1.1 |
| 2c | NA | NA | 49.20 (41.69–58.05) | 57.78 (56.10–59.52) | – | 1.2 |
| 2d | NA | NA | NA | >200 | – | – |
| 3 | 57.82 (54.01–61.91) | 28.95 (19.87–42.16) | 16.28 (8.94–29.60) | 69.50 (64.01–75.45) | 2.4 | 4.3 |
| 3a | NA | NA | NA | >200 | – | – |
| 3b | NA | NA | NA | >200 | – | – |
| miltefosine | 6.87 | 7.25 | – | 49.72 | – | – |
| benznidazole | – | – | 114.68 | – | – | – |
| T. cruzi (Trypomastigotes) | L. infantum (Amastigotes) | NCTC | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Compounds | Experimental | Train | Validation | Experimental | Train | Validation | Experimental | Train | Validation |
| 1 | I | I | I | A | A | A | I | I | I |
| 2 | A | A | A | A | A | A | I | I | I |
| 2a | A | A | A | A | I | I | I | I | I |
| 1a | A | A | A | I | A | A | A | A | A |
| 1b | A | A | A | I | I | I | A | A | I |
| 2b | A | A | A | I | I | I | I | I | I |
| 2d | I | I | A | I | I | I | I | I | A |
| 3 | A | A | A | A | A | A | A | A | A |
| 1c | I | I | I | I | I | I | I | I | A |
| 2c | A | A | A | I | I | I | I | I | I |
| 3a | A | A | A | I | I | I | I | I | I |
| 3b | A | A | A | I | I | I | I | I | I |
3. Experimental
3.1. General Experimental Procedures
3.2. Plant Material
3.3. Extraction and Isolation of Natural Triterpenoids 1–3
3.4. Preparation of Semi-Synthetic Compounds
3.4.1. Reduction of the Carbonyl Group at C-3 (Compounds 1 and 2)
3.4.2. Hydrogenation of Δ24 (Compounds 1, 1a, 2b)
3.4.3. Acetylation of Hydroxyl Group at C-3 (Compounds 2a and 3a)
3.4.4. Methylation of Carboxylic Acid (Compounds 2 and 3)
3.5. Bioassay Procedures
3.6. Parasite Maintenance
3.7. Mammalian Cells
3.8. Determination of the Activity Against L. infantum-Promastigotes.
3.9. Determination of the Activity Against L. infantum-Intracellular Amastigotes
3.10. Determination of the Activity Against Trypanosoma cruzi-Trypomastigotes
3.11. Determination of the Cytotoxicity Against Mammalian Cells
3.12. Statistical Analysis
3.13. Molecular Interaction Fields (MIF)
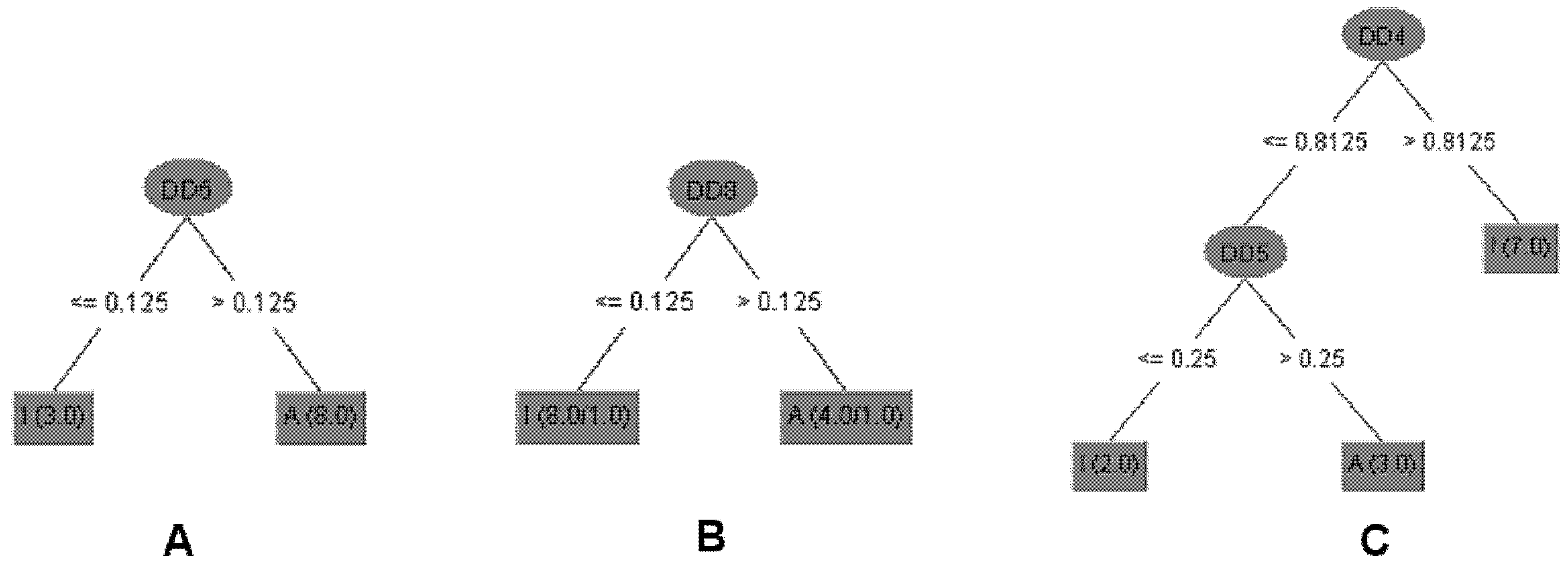
3.14. Decision Tree
4. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Corrêa, M.P. Dicionário de Plantas Úteis do Brasil e das Exóticas Cultivadas; Imprensa Nacional: Rio de Janeiro, Brazil, 1984; Volume 1, p. 311. [Google Scholar]
- Lorenzi, H. Árvores Brasileiras: Manual de Identificação e Cultivo de Plantas Arbóreas Nativas do Brasil; Plantarum: São Paulo, Brazil, 1992; p. 384. [Google Scholar]
- Morton, J.F. Brazilian pepper-its impact on people, animals and the environment. Econ. Bot. 1978, 32, 353–359. [Google Scholar] [CrossRef]
- Schmourlo, G.; Mendonça-Filho, R.R.; Alviano, C.S.; Costa, S.S. Screening of antifungal agents using ethanol precipitation and bioautography of medicinal and food plants. J. Ethnopharmacol. 2005, 96, 563–568. [Google Scholar] [CrossRef]
- Jain, M.K.; Yu, B.Z.; Rogers, J.M.; Smith, A.E.; Boger, E.T.A.; Ostrander, R.L.; Rheingold, A.L. Specific competitive inhibitor of secreted phospholipase A2 from berries of Schinus terebinthifolius. Phytochemistry 1995, 39, 537–547. [Google Scholar] [CrossRef]
- Johann, S.; Sá, N.P.; Lima, L.A.R.S.; Cisalpino, P.S.; Costa, B.B.; Alves, T.M.A.; Siqueira, E.P.; Zani, C.L. Antifungal activity of schinol and a new biphenyl compound isolated from Schinus terebinthifolius against the pathogenic fungus Paracoccidioides brasiliensis. Ann. Clin. Microbiol. Antimicrob. 2010, 9, 30–35. [Google Scholar] [CrossRef]
- Ceruks, M.; Romoff, P.; Fávero, O.A.; Lago, J.H.G. Constituintes fenólicos polares de Schinus terebinthifolius Raddi (Anacardiaceae). Quim. Nova 2007, 30, 597–599. [Google Scholar] [CrossRef]
- Santana, J.S.; Sartorelli, P.; Lago, J.H.G.; Matsuo, A.L. Isolamento e avaliação do potencial citotóxico de derivados fenólicos de Schinus terebinthifolius Raddi (Anacardiaceae). Quim. Nova 2012, 35, 2245–2248. [Google Scholar] [CrossRef]
- Lima, M.R.F.; Luna, J.S.; Santos, A.F.; Andrade, M.C.C.; Sant’ana, A.E.G.; Genet, J.P.; Marquez, B.; Neuville, L.; Moreau, N. Anti-bacterial activity of some Brazilian medicinal plants. J. Ethnopharmacol. 2006, 105, 137–147. [Google Scholar] [CrossRef]
- Ibrahim, M.T.; Fobbe, R.; Nolte, J. Chemical composition and biological studies of Egyptian Schinus molle L. and Schinus terebinthifolius Raddi oils. Bull. Fac. Pharm. 2004, 42, 289–296. [Google Scholar]
- Singh, A.K.; Singh, A.K.; Gupta, K.C.; Brophy, J.J. Essential oil of leaves and inflorescence of Schinus terebinthifolius: An exotic plant of India. J. Essent. Oil Res. 1998, 10, 697–699. [Google Scholar] [CrossRef]
- Barbosa, L.C.A.; Demuner, A.J.; Clemente, A.D.; Paula, V.F.; Ismail, F.M.D. Seasonal variation in the composition of volatile oils from Schinus terebinthifolius Raddi. Quim. Nova 2007, 30, 1959–1965. [Google Scholar] [CrossRef]
- Bendaoud, H.; Romdhane, M.; Souchard, J.P.; Cazaux, S.; Bouajila, J. Chemical composition and anticancer and antioxidant activities of Schinus molle L. and Schinus terebinthifolius Raddi berries essential oils. J. Food Sci. 2010, 75, C466–C472. [Google Scholar] [CrossRef]
- Sartorelli, P.; Santana, J.S.; Guadagnin, R.C.; Lago, J.H.G.; Pinto, E.G.; Tempone, A.G.; Stefani, H.A.; Soares, M.G.; Silva, A.M. In vitro trypanocidal evaluation of pinane derivatives from essential oils of ripe fruits from Schinus terebinthifolius Raddi (Anacardiaceae). Quim. Nova 2012, 35, 743–747. [Google Scholar] [CrossRef]
- Santana, J.S.; Sartorelli, P.; Guadagnin, R.C.; Matsuo, A.L.; Figueiredo, C.R.; Soares, M.G.; Zanin, J.L.B.; Silva, A.M.; Lago, J.H.G. Essential oils from Schinus terebinthifolius leaves chemical composition and in vitro cytotoxicity evaluation. Pharm. Biol. 2012, 50, 1248–1253. [Google Scholar] [CrossRef]
- Moura-Costa, G.F.; Nocchi, S.R.; Ceole, L.F.; de Mello, J.C.; Nakamura, C.V.; Dias-Filho, B.P.; Temponi, L.G.; Ueda-Nakamura, T. Antimicrobial activity of plants used as medicinal on an indigenous reserve in Rio das Cobras, Paraná, Brazil. J. Ethnopharmacol. 2012, 143, 631–638. [Google Scholar] [CrossRef]
- Abdel-Sattar, E.; Maes, L.; Salama, M.M. In vitro activities of plant extracts from Saudi Arabia against malaria, leishmaniasis, sleeping sickness and Chagas disease. Phytother. Res. 2010, 24, 1322–1328. [Google Scholar] [CrossRef]
- Barrett, M.P.; Croft, S.L. Management of trypanosomiasis and leishmaniasis. Br. Med. Bull. 2012, 104, 175–196. [Google Scholar] [CrossRef]
- Palavani, E.B.; Mariane, B.; Vallim, M.A.; Pascon, R.C.; Sartorelli, P.; Soares, M.G.; Lago, J.H.G. The seasonal variation if the chemical composition of essential oils from Porcelia macrocarpa R.E. Fries (Annonaceae) and their antimicrobial activity. Molecules 2013, 18, 13574–13587. [Google Scholar] [CrossRef]
- Bou, D.D.; Lago, J.H.G.; Figueiredo, C.R.; Matsuo, A.L.; Guadagnin, R.C.; Soares, M.G.; Sartorelli, P. Chemical composition and cytotoxicity evaluation of essential oil from leaves of Casearia sylvestris, its main compound α-zingiberene and derivatives. Molecules 2013, 18, 9477–9487. [Google Scholar] [CrossRef] [Green Version]
- Rea, A.; Tempone, A.G.; Pinto, E.G.; Mesquita, J.T.; Silva, L.G.; Rodrigues, E.; Sartorelli, P.; Lago, J.H.G. Soulamarin isolated from Calophyllum brasiliense (Clusiaceae) induces plasma membrane permeabilization of Trypanosoma cruzi and mitochondrial dysfunction. PLoS Negl. Trop. Dis. 2013, 7, e2556–e2563. [Google Scholar]
- Yamamoto, E.S.; Campos, B.L.S.; Laurenti, M.D.; Lago, J.H.G.; Grecco, S.S.; Corbett, C.E.P.; Passero, L.F.D. Treatment with triterpenic fraction purified from Baccharis uncinella leaves inhibits Leishmania (Leishmania) amazonensis spreading and improves Th1 immune response in infected mice. Parasitol. Res. 2014, 113, 333–339. [Google Scholar] [CrossRef]
- Mulholland, D.A.; Nair, J.J. Triterpenes from Dysoxylum pettigrewianum. Phytochemistry 1994, 37, 1409–1411. [Google Scholar] [CrossRef]
- Department of health and human services food and drug administration. Guidance for industry antiviral product development-conducting and submitting Virology-studies to the agency. Available online: http://www.fda.gov/OHRMS/DOCKETS/98fr/05d-0183-gdl0002-01.pdf (accessed on 17th April 2014).
- Reimão, J.Q.; Scotti, M.T.; Tempone, A.G. Anti-leishmanial and anti-trypanosomal activities of 1,4-dihydropyridines: In vitro evaluation and structure-activity relationship study. Bioorg. Med. Chem. 2010, 18, 8044–8053. [Google Scholar] [CrossRef]
- Murray, H.W.; Delph-Etienne, S. Roles of endogenous gamma interferon and macrophage microbicidal mechanisms in host response to chemotherapy in experimental visceral leishmaniasis. Infect. Immun. 2000, 68, 288–293. [Google Scholar]
- Mesquita, J.T.; Costa-Silva, T.A.; Borborema, S.E.; Tempone, A.G. Activity of imidazole compounds on Leishmania (L.) infantum chagasi: Reactive oxygen species induced by econazole. Mol. Cell. Biochem. 2014, 389, 293–300. [Google Scholar] [CrossRef]
- Cruciani, G.; Crivori, P.; Carrupt, P.A.; Testa, B. Molecular fields in quantitative structure-permeation relationships: The VolSurf approach. J. Mol. Struc-Theochem. 2000, 503, 17–30. [Google Scholar] [CrossRef]
- Quinlan, J.R. C4.5: Programs for Machine Learning, 1st ed.; Morgan Kaufmann Publishers: London, UK, 1993; p. 302. [Google Scholar]
- Stauber, L.A.; Franchino, E.M.; Grun, J. An eight-day method for screening compounds against Leishmania donovani in golden hamsters. J. Protozool. 1985, 5, 269–273. [Google Scholar] [CrossRef]
- Corrêa, D.S.; Tempone, A.G.; Reimão, J.Q.; Taniwaki, N.N.; Romoff, P.; Fávero, O.A.; Sartorelli, P.; Mecchi, M.C.; Lago, J.H.G. Anti-leishmanial and anti-trypanosomal potential of polygodial isolated from stem barks of Drimys brasiliensis Miers (Winteraceae). Parasitol. Res. 2011, 109, 231–236. [Google Scholar] [CrossRef]
- Tempone, A.G.; Pimenta, D.C.; Lebrun, I.; Sartorelli, P.; Taniwaki, N.N.; Andrade, H.F., Jr.; Antoniazzi, M.M.; Jared, C. Antileishmanial and antitrypanosomal activity of bufadienolides isolated from the toad Rhinella jimi parotoid macrogland secretion. Toxicon 2008, 52, 13–21. [Google Scholar] [CrossRef]
- Tempone, A.G.; Oliveira, C.M.; Berlinck, R.G.S. Current approaches to discover marine antileishmanial natural products. Planta Med. 2011, 77, 572–585. [Google Scholar] [CrossRef]
- Tada, H.; Shiho, O.; Kuroshima, K.; Koyama, M.; Tsukamoto, K. An improved colorimetric assay for interleukin 2. J. Immunol. Methods 1986, 93, 157–165. [Google Scholar] [CrossRef]
- Lane, J.E.; Ribeiro-Rodrigues, R.; Suarez, C.C.; Bogitsh, B.J.; Jones, M.M.; Singh, P.K.; Carter, C.E. In vitro trypanocidal activity of tetraethylthiuram disulfide and sodium diethylamine-N-carbodithioate on Trypanosoma cruzi. Am. J. Trop. Med. Hyg. 1996, 55, 263–266. [Google Scholar]
- Oliveira, A.; Mesquita, J.T.; Tempone, A.G.; Lago, J.H.G.; Guimarães, E.F.; Kato, M.J. Leishmanicidal activity of an alkenylphenol from Piper malacophyllum is related to plasma membrane disruption. Exp. Parasitol. 2012, 132, 383–387. [Google Scholar]
- ChemAxon–cheminformatic platforms and desktop applications. Available online: http://www.chemaxon.com (accessed on 30 April 2014).
- Knime–Konstanz Information Miner. Available online: http://www.knime.org (accessed on 30 April 2014).
- Sample Availability: Samples of compounds 1–3, 1a–c, 2a–d, 3a, and 3b are available from the authors.
© 2014 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Morais, T.R.; Da Costa-Silva, T.A.; Tempone, A.G.; Borborema, S.E.T.; Scotti, M.T.; De Sousa, R.M.F.; Araujo, A.C.C.; De Oliveira, A.; De Morais, S.A.L.; Sartorelli, P.; et al. Antiparasitic Activity of Natural and Semi-Synthetic Tirucallane Triterpenoids from Schinus terebinthifolius (Anacardiaceae): Structure/Activity Relationships. Molecules 2014, 19, 5761-5776. https://doi.org/10.3390/molecules19055761
Morais TR, Da Costa-Silva TA, Tempone AG, Borborema SET, Scotti MT, De Sousa RMF, Araujo ACC, De Oliveira A, De Morais SAL, Sartorelli P, et al. Antiparasitic Activity of Natural and Semi-Synthetic Tirucallane Triterpenoids from Schinus terebinthifolius (Anacardiaceae): Structure/Activity Relationships. Molecules. 2014; 19(5):5761-5776. https://doi.org/10.3390/molecules19055761
Chicago/Turabian StyleMorais, Thiago R., Thais A. Da Costa-Silva, Andre G. Tempone, Samanta Etel T. Borborema, Marcus T. Scotti, Raquel Maria F. De Sousa, Ana Carolina C. Araujo, Alberto De Oliveira, Sérgio Antônio L. De Morais, Patricia Sartorelli, and et al. 2014. "Antiparasitic Activity of Natural and Semi-Synthetic Tirucallane Triterpenoids from Schinus terebinthifolius (Anacardiaceae): Structure/Activity Relationships" Molecules 19, no. 5: 5761-5776. https://doi.org/10.3390/molecules19055761
APA StyleMorais, T. R., Da Costa-Silva, T. A., Tempone, A. G., Borborema, S. E. T., Scotti, M. T., De Sousa, R. M. F., Araujo, A. C. C., De Oliveira, A., De Morais, S. A. L., Sartorelli, P., & Lago, J. H. G. (2014). Antiparasitic Activity of Natural and Semi-Synthetic Tirucallane Triterpenoids from Schinus terebinthifolius (Anacardiaceae): Structure/Activity Relationships. Molecules, 19(5), 5761-5776. https://doi.org/10.3390/molecules19055761






