Early State Research on Antifungal Natural Products
Abstract
:1. Introduction
2. A Brief History of Antifungal Agents
3. Natural Derivatives with Antifungal Properties
3.1. Extracts
3.2. Essential Oils
| Essential oil | Main constituents | Fungus tested | Reference |
|---|---|---|---|
| Calea clematidea | Clemateol | Trichophytonrubrum, T. tonsurans, T. mentagrophytes, Microsporum gypseum, M. canis, M. nanum, Epidermophyton floccosum | [85] |
| Ocimum gratissimum | Eugenol | C. albicans, C. krusei, C. parapsilosis, C. tropicalis | [11] |
| Salvia officinalis | Camphor and cis-thujone | C. albicans, C. krusei, C. tropicalis, C. parapsilosis, C. glabrata, E. floccosum, T. rubrum, T. mentagrophytes, M. canis, M. gypseum, A. flavus, Fusarium moniliforme, Penicillium italicum, Cladosporium cladosporioides. | [86] |
| Calendula officinalis L. | δ-Cadinene, α-cadinol and epi-α-muurolol | C. albicans, C. dubliniensis, C. parapsilosis, C. glabrata, C. tropicalis, C. guilliermondii, C. krusei, Rhodotorulla sp. | [87] |
| Nandina domestica Thunb. | 1-Indolizinocarbazole, 2-pentanone, monophenol, azridine, methylcarbinol, ethanone, furfural, 1-hydroxy-4-methylbenzene, 2(5H)-furanone, and 3,5-dimethyl-pyrazole | T. rubrum, T. mentagrophytes, M. canis | [79] |
| Piper ovatum Vahl | δ-Amorphene, cis-muurola-4(14),5-diene and γ-muurolene | C. tropicalis | [88] |
| Piper amalago | β-Copaen-4-α-ol, 7-epi-α-eudesmol, epi-α-cadinol and n-hexyl benzoate | C. albicans, C. tropicalis, C. parapsilosis | [89] |
| Achillea millefolium | Azulene, chamazulene, pinene, cineole, camphor, α-bisabolol, monoterpenes, eucalyptol, borneol, terpene derivatives, sesquiterpenes, tannins, mucilage, coumarins, resins, saponins, steroids, fatty acids, alkaloids, bitter principle, lactones and flavonoids. | C. albicans, C. tropicalis, C. glabrata. | [78] |
| Curcuma longa L. | Curcumin | C. albicans, C. tropicalis, C. glabrata. | [78] |
| Boesenbergia pandurata | Geraniol and camphor | C. albicans | [90] |
| Coriandrum sativum L. | Linalool | C. albicans, C. tropicalis | [91] |
| Piper diospyrifolium | (E)-Eudesma-6,11-diene, γ-muuroleneandcaryophyllene-type (E)-caryophyllene | C. albicans, C. tropicalis, C. parapsilosis | [92] |
| Mentha piperita | Menthol, menthyl acetate and menthofuran | C. albicans, C. tropicalis, C. krusei, C. glabrata, C. dubliniensis, C. parapsilosis, C. neoformans, Aspergillus flavus, A. fumigatus, A. clavatus, and A. oryzae | [93] |
| Cymbopogon citratus | Citral | Malassezia spp. | [81] |
3.2.1. Terpenes or Terpenoids
3.3. Propolis
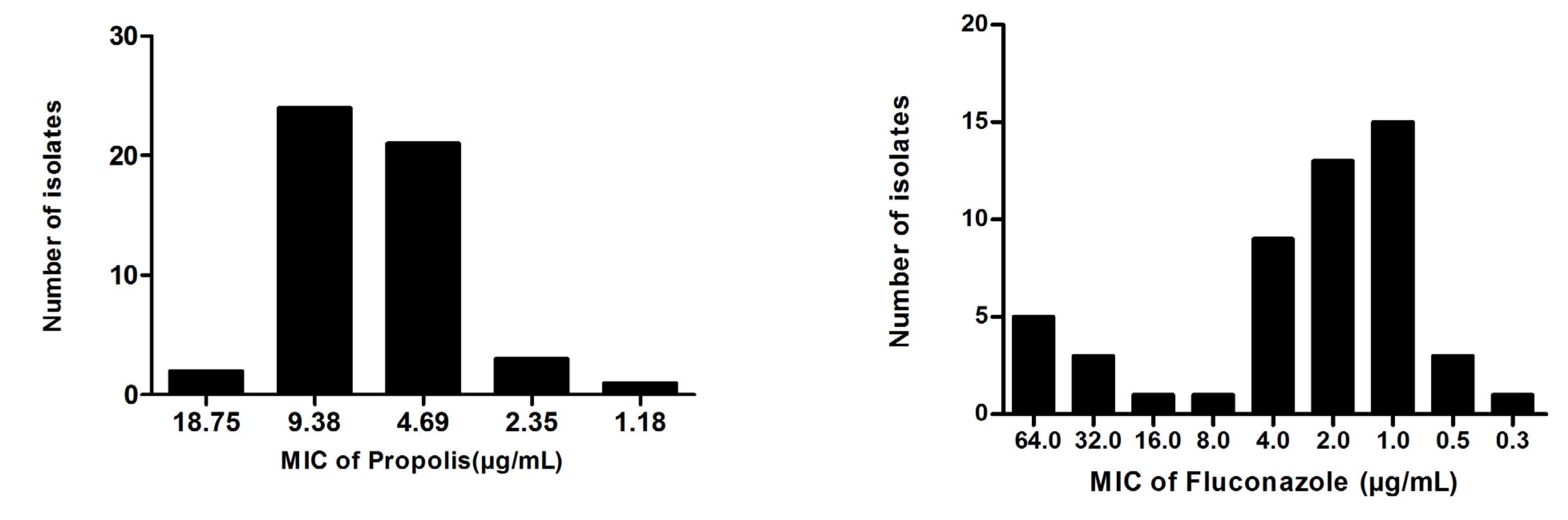
3.4. Ajoene Derived from Garlic
| Species (No. of Isolates) | MIC Range (µg/mL) | |
|---|---|---|
| Ajoene | Itraconazole | |
| Fusarium oxysporum (8) | 14.63–29.25 | 16–16 |
| Fusarium solani (8) | 3.65–29.25 | 16–16 |
| Fusarium sacchari (3) | 14.63–29.25 | 16–16 |
| Fusarium verticillioides (2) | 14.63 | 16–16 |
| Fusarium chlamydosporum (1) | 29.25 | 16 |
| Fusarium proliferatum(1) | 14.63 | 16 |
| Fusarium incarnatum(1) | 29.25 | 16 |
| Fusarium napiforme (1) | 14.63 | 16 |
| Fusarium subglutinans (1) | 7.3 | 16 |
| C. parapsilosis ATCC 22019 (1) | 29.25 | 0.125 |
3.5. Saponins

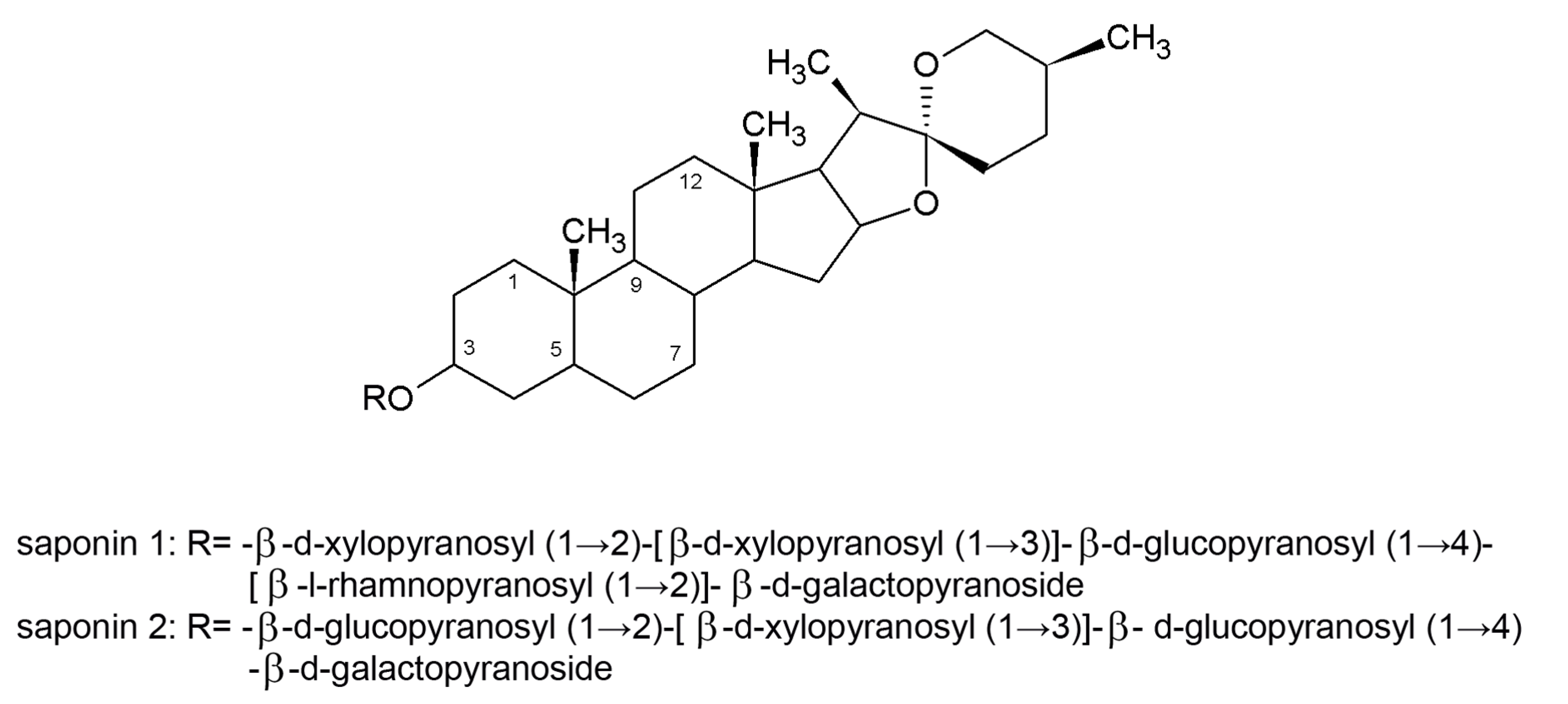
3.6. Alkaloids
3.7. Phenolic Compounds and Flavonoids
3.8. Coumarins and Xanthones
3.9. Lignans
3.10. Tannins
3.11. Secondary Metabolites
4. Perspectives
5. Conclusions
Acknowledgments
Conflictts of Interest
References
- Nucci, M.; Queiroz-Telles, F.; Alvarado-Matute, T.; Tiraboschi, I.N.; Cortes, J.; Zurita, J.; Guzman-Blanco, M.; Santolaya, M.E.; Thompson, L.; Sifuentes-Osornio, J.; et al. Epidemiology of candidemia in Latin America: A laboratory-based survey. PLoS One 2013, 8, e59373. [Google Scholar] [CrossRef]
- Arendrup, M.C.; Dzajic, E.; Jensen, R.H.; Johansen, H.K.; Kjældgaard, P.; Knudsen, J.D.; Kristensen, L.; Leitz, C.; Lemming, L.E.; Nielsen, L. Epidemiological changes with potential implication for antifungal prescription recommendations for fungaemia: Data from a nationwide fungaemia surveillance programme. Clin. Microbiol. Infect. 2013, 19, 343–353. [Google Scholar] [CrossRef]
- Butts, A.; Krysan, D.J. Antifungal drug discovery: Something old and something new. PLoS Pathog. 2012, 8, e1002870. [Google Scholar] [CrossRef]
- Shao, P.L.; Huang, L.M.; Hsueh, P.R. Recent advances and challenges in the treatment of invasive fungal infections. Int. J. Antimicrob. Agents 2007, 30, 487–495. [Google Scholar] [CrossRef]
- Ashcroft, D.M.; Po, A.L.W. Herbal remedies. Pharmacoeconomics 1999, 16, 321–328. [Google Scholar] [CrossRef]
- Kathiravan, M.K.; Salake, A.B.; Chothe, A.S.; Dudhe, P.B.; Watode, R.P.; Mukta, M.S.; Gadhwe, S. The biology and chemistry of antifungal agents: A review. Bioorg. Med. Chem. 2012, 20, 5678–5698. [Google Scholar] [CrossRef]
- Paiva, J.A.; Pereira, J.M. New antifungal antibiotics. Curr. Opin. Infect. Dis. 2013, 26, 168–174. [Google Scholar] [CrossRef]
- Iwu, M. International conference on ethnomedicine and drug discovery. J. Altern. Complem. Med. 2000, 6, 3–5. [Google Scholar] [CrossRef]
- Orafidiya, L.O.; Oyedele, A.O.; Shittu, A.O.; Elujoba, A.A. The formulation of an effective topical antibacterial product containing Ocimum gratissimum L. leaf essential oil. Int. J. Pharm. 2001, 224, 177–183. [Google Scholar] [CrossRef]
- Hernández Díaz, L.; Rodríguez Jorge, M. Actividad antimicrobiana de plantas que crecen en cuba. Rev. Cuba. Plant. Med. 2001, 6, 44–47. [Google Scholar]
- Nakamura, C.V.; Ishida, K.; Faccin, L.C.; Cortez, D.A.C.G.; Rozental, S.; de Souza, W.; Ueda-Nakamura, T. In vitro activity of essential oil from Ocimum gratissimum L against four Candida species. Res. Microbiol. 2004, 155, 579–586. [Google Scholar] [CrossRef]
- Wieder, L.M. Fungistatic and fungicidal effects of two wood-preserving chemicals on human dermatophytes: Ortho (2 chlorophenyl) phenol sodium and tetrachlorphenol sodium. Arch. Derm. 1935, 31, 644–657. [Google Scholar] [CrossRef]
- Davies, W.H.; Sexton, W.A. Chemical constitution and fungistatic action of organic sulphur compounds. Biochem. J. 1946, 40, 331–334. [Google Scholar]
- Hopkins, J.G.; Fisher, J.K.; Hillegas, A.B.; Ledin, R.B.; Rebell, G.C.; Camp, E. Fungistatic agents for treatment of dermatophytosis. J. Invest. Dermatol. 1946, 7, 239–253. [Google Scholar] [CrossRef]
- Lamb, J.H. Combined therapy in histoplasmosis and coccidioidomycosis; methyltestosterone and meth-dia-mer-sulfonamides. AMA Arch. Derm. Syphilol. 1954, 70, 695–712. [Google Scholar] [CrossRef]
- Oxford, A.E.; Raistrick, H.; Simonart, P. Griseofulvin, C17H1706Cl, a metabolic product of Penicillium griseo-fulvum Dierckx. Biochem. J. 1939, 33, 240–248. [Google Scholar]
- Odds, F.C. Antifungal agents: Their diversity and increasing sophistication. Mycologist 2003, 17, 51–55. [Google Scholar] [CrossRef]
- Hazen, E.L.; Mason, A. Effect of fungicidin (nystatin) in mice injected with lethal mixtures of aureomycin and Candida albicans. Science 1953, 117, 609–610. [Google Scholar]
- Brown, R.; Hazen, E.L. Production of actidione by Streptomyces noursei. Antibiot. Annu. 1955, 3, 245–248. [Google Scholar]
- Brown, R.; Hazen, E.L. Present knowledge of nystatin, an antifungal antibiotic. Trans. N. Y. Acad. Sci. 1957, 19, 447–456. [Google Scholar]
- Brezis, M.; Rosen, S.; Silva, P.; Spokes, K.; Epstein, F.H. Polyene toxicity in renal medulla:Injury mediated by transport activity. Science 1984, 224, 66–68. [Google Scholar]
- Gupta, A.K.; Tomas, E. New antifungal agents. Dermatol. Clin. 2003, 21, 565–576. [Google Scholar] [CrossRef]
- Grunberg, E.; Berger, J.; Titsworth, E. Chemotherapeutic studies on a new antifungal agent, x-5079c, effective against systemic mycoses. Am. Rev. Respir. Dis. 1961, 84, 504–506. [Google Scholar]
- Li, M.; Liao, Y.; Chen, M.; Pan, W.; Weng, L. Antifungal susceptibilities of Cryptococcus species complex isolates from aids and non-aids patients in southeast China. Braz. J. Infect. Dis. 2012, 16, 175–179. [Google Scholar] [CrossRef]
- Heeres, J.; Meerpoel, L.; Lewi, P. Conazoles. Molecules 2010, 15, 4129–4188. [Google Scholar] [CrossRef]
- Gleason, T.G.; May, A.K.; Caparelli, D.; Farr, B.M.; Sawyer, R.G. Emerging evidence of selection of fluconazole-tolerant fungi in surgical intensive care units. Arch. Surg. 1997, 132, 1197–1201. [Google Scholar] [CrossRef]
- Salci, T.P.; Gimenes, M.; dos Santos, C.A.; Svidzinski, T.I.E.; Caparroz-Assef, S.M. Utilization of fluconazole in an intensive care unit at a university hospital in Brazil. Int. J. Clin. Pharm. 2013, 35, 176–180. [Google Scholar] [CrossRef]
- Odds, F.C.; Brown, A.J.P.; Gow, N.A.R. Antifungal agents: Mechanisms of action. Trends Microbiol. 2003, 11, 272–279. [Google Scholar] [CrossRef]
- Barrett, D. From natural products to clinically useful antifungals. Biochim. Biophys. Acta 2002, 1587, 224–233. [Google Scholar]
- Denning, D.W. Echinocandin antifungal drugs. Lancet 2003, 362, 1142–1151. [Google Scholar] [CrossRef]
- Cappelletty, D.; Eiselstein‐McKitrick, K. The echinocandins. Pharmacotherapy 2007, 27, 369–388. [Google Scholar] [CrossRef]
- Pappas, P.G.; Kauffman, C.A.; Andes, D.; Benjamin, D.K., Jr.; Calandra, T.F.; Edwards, J.E., Jr.; Filler, S.G.; Fisher, J.F.; Kullberg, B.J.; Ostrosky-Zeichner, L. Guías de práctica clínica para el manejo de la candidiasis: Actualización del 2009, de la infectious diseases society of america. Clin. Infect. Dis. 2009, 48, 503–537. [Google Scholar] [CrossRef]
- Herreros, E.; Martinez, C.M.; Almela, M.J.; Marriot, M.S.; de las Heras, F.G.; Gargallo-Viola, D. Sordarins: In vitro activities of new antifungal derivatives against pathogenic yeasts, Pneumocystis. carinii and filamentous fungi. Antimicrob. Agents Chemother. 1998, 42, 2863–2869. [Google Scholar]
- Clemons, K.V.; Stevens, D.A. Efficacies of sordarin derivatives gm193663, gm211676, and gm237354 in a murine model of systemic coccidioidomycosis P6. Antimicrob. Agents Chemother. 2000, 44, 1874–1877. [Google Scholar] [CrossRef]
- Castro, J.; Cuevas, J.C.; Fiandor, J.M.; Fraile, M.T.; Gomez De Las Heras, F.; Ruiz, J.R. Antifungal sordarins. Part 3: Synthesis and structure-activity relationships of 2′,3′-fused oxirane derivatives. Bioorg. Med. Chem. Lett. 2002, 12, 1371–1374. [Google Scholar] [CrossRef]
- Kamai, Y.; Kakuta, M.; Shibayama, T.; Fukuoka, T.; Kuwahara, S. Antifungal activities of r-135853, a sordarin derivative, in experimental candidiasis in mice. Antimicrob. Agents Chemother. 2005, 49, 52–56. [Google Scholar] [CrossRef]
- Hanadate, T.; Tomishima, M.; Shiraishi, N.; Tanabe, D.; Morikawa, H.; Barrett, D.; Matsumoto, S.; Ohtomo, K.; Maki, K. Fr290581, a novel sordarin derivative: Synthesis and antifungal activity. Bioorg. Med. Chem. Lett. 2009, 19, 1465–1468. [Google Scholar] [CrossRef]
- Ostrosky-Zeichner, L.; Casadevall, A.; Galgiani, J.N.; Odds, F.C.; Rex, J.H. An insight into the antifungal pipeline: Selected new molecules and beyond. Nat. Rev. Drug Discov. 2010, 9, 719–727. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Castanheira, M.; Messer, S.A.; Moet, G.J.; Jones, R.N. Echinocandin and triazole antifungal susceptibility profiles for Candida spp., Cryptococcus neoformans and Aspergillus. fumigatus: Application of new CLSI clinical breakpoints and epidemiologic cutoff values to characterize resistance in the Sentry Antimicrobial Surveillance Program (2009). Diagn. Microbiol. Infect. Dis. 2011, 69, 45–50. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Duncanson, F.; Messer, S.A.; Moet, G.J.; Jones, R.N.; Castanheira, M. In vitro activity of a novel broad-spectrum antifungal, E1210, tested against Aspergillus spp. determined by CLSI and EUCAST broth microdilution methods. Antimicrob. Agents Chemother. 2011, 55, 5155–5158. [Google Scholar] [CrossRef]
- Hata, K.; Horii, T.; Miyazaki, M.; Watanabe, N.-A.; Okubo, M.; Sonoda, J.; Nakamoto, K.; Tanaka, K.; Shirotori, S.; Mura, N.; et al. Efficacy of oral E1210, a new broad-spectrum antifungal with a novel mechanism of action, in murine models of candidiasis, aspergillosis, and fusariosis. Antimicrob. Agents Chemother. 2011, 55, 4543–4551. [Google Scholar] [CrossRef]
- Miyazaki, M.; Horii, T.; Hata, K.; Watanabe, N.A.; Nakamoto, K.; Tanaka, K.; Shirotori, S.; Murai, N.; Inoue, S.; Matsukura, M.; et al. In vitro activity of E1210, a novel antifungal, against clinically important yeasts and molds. Antimicrob. Agents Chemother. 2011, 55, 4652–4658. [Google Scholar] [CrossRef]
- U.S. Food and Drug Administration. Informations for Clinical Investigators (INDs). Available online: http://www.fda.gov/Drugs/DevelopmentApprovalProcess/HowDrugsareDevelopedandApproved/ApprovalApplications/InvestigationalNewDrugINDApplication/ucm176259.htm (accessed on 16 January 2014).
- Hope, P.R.P. Intellectual property protections are vital to continuing innovation in the biopharmaceutical industry. 2013. Available online: http://www.phrma.org/innovation/intellectual-property (accessed on 16 January 2014).
- Drews, J. Drug discovery: A historical perspective. Science 2000, 287, 1960–1964. [Google Scholar] [CrossRef]
- Takeshita, H.; Watanabe, J.; Kimura, Y.; Kawakami, K.; Takahashi, H.; Takemura, M.; Kitamura, A.; Someya, K.; Nakajima, R. Novel pyridobenzimidazole derivatives exhibiting antifungal activity by the inhibition of beta-1,6-glucan synthesis. Bioorg. Med. Chem. Lett. 2010, 20, 3893–3896. [Google Scholar] [CrossRef]
- Kuroyanagi, J.; Sugimoto, Y.; Fujisawa, T.; Morita, C.; Suzuki, T.; Kawakami, K.; Takemura, M. Novel antifungal agents: Triazolopyridines as inhibitors of beta-1,6-glucan synthesis. Bioorg. Med. Chem. 2010, 18, 5845–5854. [Google Scholar] [CrossRef]
- Svidzinski, T.I.E.; Franco, S.L.; Moura, L.M.P.; Oliveira, A.C.P.; Longhini, R. Obtenção de extratos de própolis sobre diferentes condições e avaliação de sua atividade antifúngica. Rev. Bras. Farmacogn. 2005, 17, 388–395. [Google Scholar]
- Franco, S.L.; Svidzinski, T.I.E.; Ogawa, S.E.N.; Novelo, C.R. Composições Farmacêuticas com Atividade Antifúngica Contendo Extratos de Cymbopogon nardus, Processo de Obtenção dos Extratos de Cymbopogon narduse seus usos. Braz. Patent number BRPI0702622; (WO2008113146), 25 September 2008. [Google Scholar]
- Ferreira, I.C.P.; Estivalet, T.I.E.; Tsuzuki, J.C.; Cortez, D.A.G. Uso do Extrato da Planta Sapindus saponaria e de seus Princípios Ativos Para o Controle e Tratamento de Infecções por Fungos. Braz. Patent BRPI0506075, 12 September 2005. [Google Scholar]
- Shinobu-Mesquita, C.S.; Bertoni, T.A.; Guilhermetti, E.; Svidzinski, T.I.E.I.E. Antifungal activity of the extract of Curcuma zedoaria (christm.) roscoe, zingiberaceae, against yeasts of the genus Candida isolated from the oral cavity of patients infected with the human immunodeficiency virus. Rev. Bras. Farmacogn. 2011, 21, 128–132. [Google Scholar] [CrossRef]
- Pessini, G.L.; Holetz, F.B.; Sanches, N.R.; Cortez, D.A.G.; Dias Filho, B.P.; Nakamura, C.V. Avaliação da atividade antibacteriana e antifúngica de extratos de plantas utilizados na medicina popular. Rev. Bras. Farmacogn. 2003, 13, 21–24. [Google Scholar] [CrossRef]
- Tempone, A.G.; Sartorelli, P.; Teixeira, D.; Prado, F.O.; Calixto, I.A.R.L.; Lorenzi, H.; Melhem, M.S.C. Brazilian flora extracts as source of novel antileishmanial and antifungal compounds. Mem. Inst. Oswaldo Cruz 2008, 103, 443–449. [Google Scholar] [CrossRef]
- Rajeh, M.A.B.; Zuraini, Z.; Sasidharan, S.; Latha, L.Y.; Amutha, S. Assessment of Euphorbia hirta L. leaf, flower, stem and root extracts for their antibacterial and antifungal activity and brine shrimp lethality. Molecules 2010, 15, 6008–6018. [Google Scholar] [CrossRef]
- Polaquini, S.R.B.; Svidzinski, T.I.E.; Kemmelmeier, C.; Gasparetto, A. Effect of aqueous extract from neem (Azadirachta indica A. Juss) on hydrophobicity, biofilm formation and adhesion in composite resin by Candida albicans. Arch. Oral Biol. 2006, 51, 482–490. [Google Scholar]
- Niño, J.; Mosquera, O.M.; Correa, Y.M. Antibacterial and antifungal activities of crude plant extracts from colombian biodiversity. Rev. Biol. Trop. 2012, 60, 1535–1542. [Google Scholar]
- Zabka, M.; Pavela, R.; Gabrielova‐Slezakova, L. Promising antifungal effect of some euro-asiatic plants against dangerous pathogenic and toxinogenic fungi. J. Sci. Food Agric. 2011, 91, 492–497. [Google Scholar] [CrossRef]
- Madhumitha, G.; Saral, A.M. Preliminary phytochemical analysis, antibacterial, antifungal and anticandidal activities of successive extracts of Crossandra infundibuliformis. Asian Pac. J. Trop. Med. 2011, 4, 192–195. [Google Scholar] [CrossRef]
- Karimi, E.; Jaafar, H.Z.E.; Ahmad, S. Antifungal, anti-inflammatory and cytotoxicity activities of three varieties of Labisia pumila benth: from microwave obtained extracts. BMC Complement. Altern. Med. 2013, 13, 20. [Google Scholar] [CrossRef]
- Hamza, O.J.M.; van den Bout-Van den Beukel, C.J.P.; Matee, M.I.N.; Moshi, M.J.; Mikx, F.H.M.; Selemani, H.O.; Mbwambo, Z.H.; van der Ven, A.J.A.M.; Verweij, P.E. Antifungal activity of some tanzanian plants used traditionally for the treatment of fungal infections. J. Ethnopharmacol. 2006, 108, 124–132. [Google Scholar] [CrossRef]
- Phongpaichit, S.; Subhadhirasakul, S.; Wattanapiromsakul, C. Antifungal activities of extracts from thai medicinal plants against opportunistic fungal pathogens associated with aids patients. Mycoses 2005, 48, 333–338. [Google Scholar] [CrossRef]
- Naghdi, B.H.; Soroushzadeh, A.; Rezazadeh, S.A.; Sharifi, M.; Ghalavand, A.; Rezaei, A. Evaluation of phytochemical and production potential of borage (Borago. officinalis L.) during the growth cycle. J. Med. Plants 2008, 7, 37–43. [Google Scholar]
- Binns, S.E.; Arnason, J.T.; Baum, B.R. Phytochemical variation within populations of Echinacea angustifolia (asteraceae). Biochem. Sys. Ecol. 2002, 30, 837–854. [Google Scholar] [CrossRef]
- Zhao, Y.P.; Li, J.H.; Yang, S.T.; Fan, J.; Fu, C.X. Effects of postharvest processing and geographical source on phytochemical variation of Corydalis rhizoma. Chin. Herbal Med. 2013, 5, 151–157. [Google Scholar]
- Silva-Santos, A.; Antunes, A.M.S.; Bizzo, H.R.; d’Avila, L.A. A participação da indústria óleo-citrícola na balança comercial brasileira. Rev. Bras. Plant. Med. 2006, 8, 8–13. [Google Scholar]
- Craveiro, A.A.; Queiroz, D.C. Óleos essenciais e química fina. Quím. Nova 1993, 16, 224–228. [Google Scholar]
- Karlberg, A.T.; Dooms‐Goossens, A. Contact allergy to oxidized d-limonene among dermatitis patients. Contact Derm. 1997, 36, 201–206. [Google Scholar] [CrossRef]
- Siani, A.C.; Sampaio, A.L.F.; Souza, M.C.; Henriques, M.; Ramos, M.F.S. Óleos essenciais: Potencial antiinflamatório. Biotecnol.: Ciênc. Desenvolv. 2000, 16, 38–43. [Google Scholar]
- Maruzzella, J.C.; Liguori, L. The in vitro antifungal activity of essential oils. J. Am. Pharm. Assoc. 1958, 47, 250–254. [Google Scholar] [CrossRef]
- Toama, M.A.; El-Alfy, T.S.; El-Fatatry, H.M. Antimicrobial activity of the volatile oil of Nigella sativa linneaus seeds. Antimicrob. Agents Chemother. 1974, 6, 225–226. [Google Scholar] [CrossRef]
- Banerjee, A.; Nigam, S.S. Antifungal activity of the essential oil of Curcuma caesia roxb. Indian J. Med. Res. 1976, 64, 1318–1321. [Google Scholar]
- Nenoff, P.; Haustein, U.F.; Brandt, W. Antifungal activity of the essential oil of Melaleuca alternifolia (tea tree oil) against pathogenic fungi in vitro. Skin Pharmacol. 1996, 9, 388–394. [Google Scholar] [CrossRef]
- Mastura, M.; Azah, M.A.N.; Khozirah, S.; Mawardi, R.; Manaf, A.A. Anticandidal and antidermatophytic activity of Cinnamomum species essential oils. Cytobios 1999, 98, 17–23. [Google Scholar]
- Viollon, C.; Chaumont, J.-P. Antifungal properties of essential oils and their main components upon Cryptococcus neoformans. Mycopathologia 1994, 128, 151–153. [Google Scholar] [CrossRef]
- Corrêa, M.P. Dicionário de Plantas úteis do Brasil e das Exóticas Cultivadas; Ministério da Agricultura, Instituto Brasileiro de Desenvolvimento Florestal: Rio de Janeiro, Brasil, 1984. [Google Scholar]
- Cortez, D.A.G.; Cortez, L.E.R.; Pessini, G.L.; Doro, D.L.; Nakamura, C.V. Analysis of essential oil of alfavaca Ocimum. gratissimum L. (labiatae). Arq. Ciênc. Saúde UNIPAR 1998, 2, 125–127. [Google Scholar]
- De Oliveira Lima, I.; Oliveira, R.D.A.G.; de Oliveira Lima, E.; Farias, N.M.P.; de Souza, E.L. Atividade antifúngica de óleos essenciais sobre espécies de Candida. Rev. Bras. Farmacogn. 2006, 16, 197–201. [Google Scholar]
- Ribeiro, D.I.; Alves, M.D.S.; Faria, M.G.I.; Svidzinski, T.I.E.; Nascimento, I.A.; Ferreira, F.B.P.; Ferreira, G.A.; Gazim, Z.C. Determination of antifungal activity of essential oils of Curcuma longa L. (Zingiberaceae) and Achillea. millefolium (Asteraceae) grown in the northwest Paraná. Arq. Ciênc. Saúde UNIPAR 2010, 14, 103–109. [Google Scholar]
- Bajpai, V.K.; Yoon, J.I.; Kang, S.C. Antifungal potential of essential oil and various organic extracts of Nandina domestica thunb. against skin infectious fungal pathogens. Appl. Microbiol. Biotechnol. 2009, 83, 1127–1133. [Google Scholar] [CrossRef]
- Pandey, A.K.; Mishra, A.K.; Mishra, A. Antifungal and antioxidative potential of oil and extracts derived from leaves of indian spice plant Cinnamomum tamala. Cell. Mol. Biol. 2012, 58, 142–147. [Google Scholar]
- Carmo, E.S.; Pereira, F.d.O.; Cavalcante, N.M.; Gayoso, C.W.; Lima, E.O. Treatment of pityriasis versicolor with topical application of essential oil of Cymbopogon citratus (DC) stapf-therapeutic pilot study. An. Bras. Dermatol. 2013, 88, 381–385. [Google Scholar] [CrossRef]
- Bouzabata, A.; Bazzali, O.; Cabral, C.; Gonçalves, M.J.; Teresa Cruz, M.; Bighelli, A.; Cavaleiro, C.; Casanova, J.; Salgueiro, L.; Tomi, F. New compounds, chemical composition, antifungal activity and cytotoxicity of the essential oil from Myrtus nivellei batt. & trab., an endemic species of central sahara. J. Ethnopharmacol. 2013, 149, 613–620. [Google Scholar] [CrossRef]
- Sookto, T.; Srithavaj, T.; Thaweboon, S.; Thaweboon, B.; Shrestha, B.; Nakazawa, F. In vitro effects of Salvia officinalis L. essential oil on Candida albicans. Asian Pac. J. Trop. Biomed. 2013, 3, 376–380. [Google Scholar] [CrossRef]
- Souza, E.L.D.; Lima, E.D.O.; Freire, K.R.D.L.; Sousa, C.P.D. Inhibitory action of some essential oils and phytochemicals on the growth of various moulds isolated from foods. Braz. Arch. Biol. Technol. 2005, 48, 245–250. [Google Scholar] [CrossRef]
- Flach, A.; Gregel, B.; Simionatto, E.; da Silva, U.F.; Zanatta, N.; Morel, A.F.; Linares, C.E.B.; Alves, S.H. Chemical analysis and antifungal activity of the essential oil of Calea. clematidea. Planta Med. 2002, 68, 836–838. [Google Scholar] [CrossRef]
- Pinto, E.; Salgueiro, L.R.; Cavaleiro, C.; Palmeira, A.; Gonçalves, M.J. In vitro susceptibility of some species of yeasts and filamentous fungi to essential oils of Salvia officinalis. Ind. Crop. Prod. 2007, 26, 135–141. [Google Scholar] [CrossRef]
- Gazim, Z.C.; Rezende, C.M.; Fraga, S.R.; Svidzinski, T.I.E.; Cortez, D.A.G. Antifungal activity of the essential oil from Calendula officinalis L. (Asteraceae) growing in Brazil. Braz. J. Microbiol. 2008, 39, 61–63. [Google Scholar]
- Silva, D.R.; Endo, E.H.; Nakamura, C.V.; Svidzinski, T.I.E.; de Souza, A.; Young, M.C.M.; Ueda-Nakamura, T.; Cortez, D.A.G. Chemical composition and antimicrobial properties of Piper ovatum Vahl. Molecules 2009, 14, 1171–1182. [Google Scholar] [CrossRef]
- Nakamura, C.V.; de Paulo, L.F.; Young, M.C.M.; Svidzinski, T.I.E.I.E. Chemical composition and antifungal activity of the essential oil from Piper amalago L. Lat. Am. J. Pharm. 2010, 29, 1459–1462. [Google Scholar]
- Taweechaisupapong, S.; Singhara, S.; Lertsatitthanakorn, P.; Khunkitti, W. Antimicrobial effects of Boesenbergia. pandurata and Piper sarmentosum leaf extracts on planktonic cells and biofilm of oral pathogens. Pak. J. Pharm. Sci. 2010, 23, 224–231. [Google Scholar]
- Silva, F.; Ferreira, S.; Duarte, A.; Mendonça, D.I.; Domingues, F.C. Antifungal activity of Coriandrum sativum essential oil, its mode of action against Candida species and potential synergism with amphotericin B. Phytomedicine 2011, 19, 42–47. [Google Scholar] [CrossRef]
- Vieira, S.C.H.; Paulo, L.F.D.; Svidzinski, T.I.E.; Dias Filho, B.P.; Nakamura, C.V.; Souza, A.D.; Young, M.C.M.; Cortez, D.A.G. Antifungal activity of Piper diospyrifolium Kunth (Piperaceae) essential oil. Braz. J. Microbiol. 2011, 42, 1001–1006. [Google Scholar] [CrossRef]
- Saharkhiz, M.J.; Motamedi, M.; Zomorodian, K.; Pakshir, K.; Miri, R.; Hemyari, K. Chemical composition, antifungal and antibiofilm activities of the essential oil of Mentha. piperita L. ISRN Pharm. 2012, 2012, 1–6. [Google Scholar]
- Mello, J.C.P.D.; Mentz, L.A.; Petrovick, P.R. Farmacognosia: Da Planta ao Medicamento; Porto Alegre, EFRGS: Porto Alegre, Brazil, 2003. [Google Scholar]
- Barchiesi, F.; Silvestri, C.; Arzeni, D.; Ganzetti, G.; Castelletti, S.; Simonetti, O.; Cirioni, O.; Kamysz, W.; Kamysz, E.; Spreghini, E. In vitro susceptibility of dermatophytes to conventional and alternative antifungal agents. Med. Mycol. 2008, 47, 321–326. [Google Scholar]
- Hammer, K.A.; Carson, C.F.; Riley, T.V. Melaleuca alternifolia (tea tree) oil inhibits germ tube formation by Candida albicans. Med. Mycol. 2000, 38, 354–361. [Google Scholar] [CrossRef]
- Palmeira-de-Oliveira, A.; Salgueiro, L.; Palmeira-de-Oliveira, R.; Martinez-de-Oliveira, J.; Pina-Vaz, C.; Queiroz, J.A.; Rodrigues, A.G. Anti-candida activity of essential oils. Mini. Rev. Med. Chem. 2009, 9, 1292–1305. [Google Scholar]
- Pauli, A. Anticandidal low molecular compounds from higher plants with special reference to compounds from essential oils. Med. Res. Rev. 2006, 26, 223–268. [Google Scholar] [CrossRef]
- Marcos-Arias, C.; Eraso, E.; Madariaga, L.; Quindós, G. In vitro activities of natural products against oral Candida isolates from denture wearers. BMC Complement. Altern. Med. 2011, 11, 119–126. [Google Scholar] [CrossRef]
- Machumi, F.; Samoylenko, V.; Yenesew, A.; Derese, S.; Midiwo, J.O.; Wiggers, F.T.; Jacob, M.R.; Tekwani, B.L.; Khan, S.I.; Walker, L.A. Antimicrobial and antiparasitic abietane diterpenoids from the roots of Clerodendrum. eriophyllum. Nat. Prod. Commun. 2010, 5, 853–858. [Google Scholar]
- Amber, K.; Aijaz, A.; Immaculata, X.; Luqman, K.A.; Nikhat, M. Anticandidal effect of Ocimum sanctum essential oil and its synergy with fluconazole and ketoconazole. Phytomedicine 2010, 17, 921–925. [Google Scholar] [CrossRef]
- Burdock, G.A. Review of the biological properties and toxicity of bee propolis (propolis). Food Chem. Toxicol. 1998, 36, 347–363. [Google Scholar] [CrossRef]
- Bankova, V.S.; de Castro, S.L.; Marcucci, M.C. Propolis: Recent advances in chemistry and plant origin. Apidologie 2000, 31, 3–16. [Google Scholar] [CrossRef]
- Teixeira, E.W.; Negri, G.; Salatino, A.; Stringheta, P.C. Seasonal variation, chemical composition and antioxidant activity of Brazilian propolis samples. Evid. Based Complement. Alternat. Med. 2010, 7, 307–315. [Google Scholar] [CrossRef]
- Monzote, L.; Cuesta-Rubio, O.; Campo Fernandez, M.; Márquez Hernandez, I.; Fraga, J.; Pérez, K.; Kerstens, M.; Maes, L.; Cos, P. In vitro antimicrobial assessment of Cuban propolis extracts. Mem. Inst. Oswaldo Cruz 2012, 107, 978–984. [Google Scholar] [CrossRef]
- Bonvehí, J.S.; Gutiérrez, A.L. The antimicrobial effects of propolis collected in different regions in the Basque country (northern Spain). World J. Microbiol. Biotechnol. 2012, 28, 1351–1358. [Google Scholar]
- Kujumgiev, A.; Tsvetkova, I.; Serkedjieva, Y.; Bankova, V.; Christov, R.; Popov, S. Antibacterial, antifungal and antiviral activity of propolis of different geographic origin. J. Ethnopharmacol. 1999, 64, 235–240. [Google Scholar] [CrossRef]
- Ota, C.; Unterkircher, C.; Fantinato, V.; Shimizu, M.T. Antifungal activity of propolis on different species of Candida. Mycoses 2001, 44, 375–378. [Google Scholar] [CrossRef]
- Dalben-Dota, K.F.; Faria, M.G.I.; Bruschi, M.L.; Pelloso, S.M.; Lopes-Consolaro, M.E.; Svidzinski, T.I.E.I.E. Antifungal activity of propolis extract against yeasts isolated from vaginal exudates. J. Altern. Complement. Med. 2010, 16, 285–290. [Google Scholar] [CrossRef]
- Oliveira, A.C.P.; Shinobu, C.S.; Longhini, R.; Franco, S.L.; Svidzinski, T.I.E.I.E. Antifungal activity of propolis extract against yeasts isolated from onychomycosis lesions. Mem. Inst. Oswaldo Cruz 2006, 101, 493–497. [Google Scholar] [CrossRef]
- Fernandes, F.F.; Dias, A.L.T.; Ramos, C.L.; Ikegaki, M.; Siqueira, A.M.D.; Franco, M.C. The “in vitro” antifungal activity evaluation of propolis g12 ethanol extract on Cryptococcus neoformans. Rev. Inst. Med. Trop. São Paulo 2007, 49, 93–95. [Google Scholar] [CrossRef]
- Murad, J.M.; Calvi, S.A.; Soares, A.; Bankova, V.; Sforcin, J.M. Effects of propolis from Brazil and Bulgaria on fungicidal activity of macrophages against Paracoccidioides brasiliensis. J. Ethnopharmacol. 2002, 79, 331–334. [Google Scholar] [CrossRef]
- Avanço, G.B.; Bruschi, M.L. Preparation and characterisation of ethylcellulose microparticles containing propolis. Rev. Ciênc. Farm. Básica Apl. 2009, 29, 129–135. [Google Scholar]
- Dota, K.F.D.; Consolaro, M.E.L.; Svidzinski, T.I.E.; Bruschi, M.L. Antifungal activity of Brazilian propolis microparticles against yeasts isolated from vulvovaginal candidiasis. Evid. Based Complement. Alternat. Med. 2011, 2011, 201953. [Google Scholar]
- Harris, J.C.; Cottrell, S.; Plummer, S.; Lloyd, D. Antimicrobial properties of Allium sativum (garlic). Appl. Microbiol. Biotechnol. 2001, 57, 282–286. [Google Scholar] [CrossRef]
- Block, E. The organosulfur chemistry of the genus allium-implications for the organic chemistry of sulfur. Angewandte. Chemie. Angew. Chem. Int. Ed. Engl. 1992, 31, 1135–1178. [Google Scholar] [CrossRef]
- Yoshida, H.; Iwata, N.; Katsuzaki, H.; Naganawa, R.; Ishikawa, K.; Fukuda, H.; Fujino, T.; Suzuki, A. Antimicrobial activity of a compound isolated from an oil-macerated garlic extract. Biosci. Biotechnol. Biochem. 1998, 62, 1014–1017. [Google Scholar] [CrossRef]
- Rev, N. Efectos del ajoeno sobre dermatofitos, Candida albicans y Malassezia furfur. Rev. Iberoam. Micol. 1998, 15, 277–281. [Google Scholar]
- Ledezma, E.; Apitz-Castro, R. Ajoene the main active compound of garlic (Allium sativum): A new antifungal agent. Rev. Iberoam. Micol. 2006, 23, 75–80. [Google Scholar] [CrossRef]
- Yoshida, S.; Kasuga, S.; Hayashi, N.; Ushiroguchi, T.; Matsuura, H.; Nakagawa, S. Antifungal activity of ajoene derived from garlic. Appl. Environ. Microbiol. 1987, 53, 615–617. [Google Scholar]
- Davis, S.R.; Perrie, R.; Apitz-Castro, R. The in vitro susceptibility of Scedosporium prolificans to ajoene, allitridium and a raw extract of garlic (Allium sativum). J. Antimicrob. Chemother. 2003, 51, 593–597. [Google Scholar] [CrossRef]
- San-Blas, G.; San-Blas, F.; Gil, F.; Marino, L.; Apitz-Castro, R. Inhibition of growth of the dimorphic fungus Paracoccidioides brasiliensis by ajoene. Antimicrob. Agents Chemother. 1989, 33, 1641–1644. [Google Scholar] [CrossRef]
- Visbal, G.; San-Blas, G.; Murgich, J.; Franco, H. Paracoccidioides brasiliensis, paracoccidioidomycosis, and antifungal antibiotics. Curr. Drug Targets Infect. Disord. 2005, 5, 211–226. [Google Scholar] [CrossRef]
- Alastruey-Izquierdo, A.; Cuenca-Estrella, M.; Monzón, A.; Mellado, E.; Rodríguez-Tudela, J.L. Antifungal susceptibility profile of clinical Fusarium spp. isolates identified by molecular methods. J. Antimicrob. Chemother. 2008, 61, 805–809. [Google Scholar] [CrossRef]
- Lalitha, P.; Shapiro, B.L.; Srinivasan, M.; Prajna, N.V.; Acharya, N.R.; Fothergill, A.W.; Ruiz, J.; Chidambaram, J.D.; Maxey, K.J.; Hong, K.C. Antimicrobial susceptibility of Fusarium, Aspergillus, and other filamentous fungi isolated from keratitis. Arch. Ophthalmol. 2007, 125, 789–793. [Google Scholar] [CrossRef]
- Lewis, R.E.; Wiederhold, N.P.; Klepser, M.E. In vitro pharmacodynamics of amphotericin B, itraconazole, and voriconazole against Aspergillus, Fusarium, and Scedosporium spp. Antimicrob. Agents Chemother. 2005, 49, 945–951. [Google Scholar] [CrossRef]
- San-Blas, G.; Marino, L.; San-Blas, F.; Apitz-Castro, R. Effect of ajoene on dimorphism of Paracoccidioides brasiliensis. Med. Mycol. 1993, 31, 133–141. [Google Scholar] [CrossRef]
- Maluf, M.L.; Takahachi, G.; Svidzinski, T.I.; Xander, P.; Apitz-Castro, R.; Bersani-Amado, C.A.; Cuman, R.K.N. Antifungal activity of ajoene on experimental murine paracoccidioidomycosis. Rev. Iberoam. Micol. 2008, 25, 163–166. [Google Scholar] [CrossRef]
- Ledezma, E.; Marcano, K.; Jorquera, A.; de Sousa, L.; Padilla, M.; Pulgar, M.; Apitz-Castro, R. Efficacy of ajoene in the treatment of tinea pedis: A double-blind and comparative study with terbinafine. J. Am. Acad. Dermatol. 2000, 43, 829–832. [Google Scholar] [CrossRef]
- Ledezma, E.; Sousa, L.D.; Jorquera, A.; Sanchez, J.; Lander, A.; Rodriguez, E.; Jain, M.K.; Apitz‐Castro, R. Efficacy of ajoene, an organosulphur derived from garlic, in the short-term therapy of tinea pedis. Mycoses 1996, 39, 393–395. [Google Scholar]
- Ledezma, E.; López, J.C.; Marin, P.; Romero, H.; Ferrara, G.; de Sousa, L.; Jorquera, A.; Castro, R.A. Ajoene in the topical short-term treatment of tinea cruris and tinea corporis in humans. Arzneimittelforschung 1999, 49, 544–547. [Google Scholar]
- Pérez-Blanco, M.; Hernández Valles, R.; Fernández Zeppenfeldt, G.; Apitz-Castro, R. Ajoene and 5-fluorouracil in the topical treatment of Cladophialophora carrionii chromoblastomycosis in humans: A comparative open study. Med. Mycol. 2003, 41, 517–520. [Google Scholar] [CrossRef]
- Marston, A.; Hostettmann, K. Review article number 6: Plant molluscicides. Phytochemistry 1985, 24, 639–652. [Google Scholar] [CrossRef]
- Connolly, J.D.; Hill, R.A. Triterpenoids. Nat. Prod. Rep. 2005, 22, 230–248. [Google Scholar] [CrossRef]
- Phillips, D.R.; Rasbery, J.M.; Bartel, B.; Matsuda, S. Biosynthetic diversity in plant triterpene cyclization. Curr. Opin. Plant. Biol. 2006, 9, 305–314. [Google Scholar] [CrossRef]
- Vincken, J.-P.; Heng, L.; de Groot, A.; Gruppen, H. Saponins, classification and occurrence in the plant kingdom. Phytochemistry 2007, 68, 275–297. [Google Scholar] [CrossRef]
- Yendo, A.C.A.; de Costa, F.; Gosmann, G.; Fett-Neto, A.G. Production of plant bioactive triterpenoid saponins: Elicitation strategies and target genes to improve yields. Mol. Biotechnol. 2010, 46, 94–104. [Google Scholar] [CrossRef]
- Osbourn, A.E. Saponins in cereals. Phytochemistry 2003, 62, 1–4. [Google Scholar] [CrossRef]
- Dini, I.; Tenore, G.C.; Schettino, O.; Dini, A. New oleanane saponins in Chenopodium. quinoa. J. Agric. Food Chem. 2001, 49, 3976–3981. [Google Scholar] [CrossRef]
- Dini, I.; Schettino, O.; Simioli, T.; Dini, A. Studies on the constituents of Chenopodium quinoa seeds: Isolation and characterization of new triterpene saponins. J. Agric. Food Chem. 2001, 49, 741–746. [Google Scholar] [CrossRef]
- Sparg, S.G.; Light, M.E.; van Staden, J. Biological activities and distribution of plant saponins. J. Ethnopharmacol. 2004, 94, 219–243. [Google Scholar] [CrossRef]
- Escalante, A.M.; Santecchia, C.B.; López, S.N.; Gattuso, M.A.; Gutiérrez Ravelo, A.; Delle Monache, F.; Gonzalez Sierra, M.; Zacchino, S.A. Isolation of antifungal saponins from Phytolacca tetramera, an Argentinean species in critic risk. J. Ethnopharmacol. 2002, 82, 29–34. [Google Scholar] [CrossRef]
- Liberto, M.D.; Svetaz, L.; Furlán, R.L.E.; Zacchino, S.A.; Delporte, C.; Novoa, M.A.; Asencio, M.; Cassels, B.K. Antifungal activity of saponin-rich extracts of Phytolacca dioica and of the sapogenins obtained through hydrolysis. Nat. Prod. Commun. 2010, 5, 1013–1018. [Google Scholar]
- Houghton, P.; Patel, N.; Jurzysta, M.; Biely, Z.; Cheung, C. Antidermatophyte activity of medicago extracts and contained saponins and their structure-activity relationships. Phytother. Res. 2006, 20, 1061–1066. [Google Scholar] [CrossRef]
- Zhang, J.D.; Cao, Y.B.; Xu, Z.; Sun, H.H.; An, M.M.; Yan, L.; Chen, H.S.; Gao, P.H.; Wang, Y.; Jia, X.M. In vitro and in vivo antifungal activities of the eight steroid saponins from Tribulus terrestris L. with potent activity against fluconazole-resistant fungal. Biol. Pharm. Bull. 2005, 28, 2211–2215. [Google Scholar] [CrossRef]
- Zhang, J.D.; Xu, Z.; Cao, Y.B.; Chen, H.S.; Yan, L.; An, M.M.; Gao, P.H.; Wang, Y.; Jia, X.M.; Jiang, Y.Y. Antifungal activities and action mechanisms of compounds from Tribulus terrestris L. J. Ethnopharmacol. 2006, 103, 76–84. [Google Scholar] [CrossRef]
- Coleman, J.J.; Okoli, I.; Tegos, G.P.; Holson, E.B.; Wagner, F.F.; Hamblin, M.R.; Mylonakis, E. Characterization of plant-derived saponin natural products against Candida albicans. ACS Chem. Biol. 2010, 5, 321–332. [Google Scholar] [CrossRef]
- Tsuzuki, J.K.; Svidzinski, T.I.E.; Shinobu, C.S.; Silva, L.F.A.; Rodrigues-Filho, E.; Cortez, D.A.G.; Ferreira, I.C.P. Antifungal activity of the extracts and saponins from Sapindus saponaria L. Anais Acad. Bras. Ciênc. 2007, 79, 577–583. [Google Scholar]
- Damke, E.; Tsuzuki, J.K.; Cortez, D.A.; Ferreira, I.C.; Bertoni, T.A.; Batista, M.R.; Donati, L.; Svidzinski, T.I.; Consolaro, M.E. In vivo activity of Sapindus saponaria against azole-susceptible and -resistant human vaginal Candida species. BMC Complement. Altern. Med. 2011, 11, 35. [Google Scholar] [CrossRef]
- Evans, W.C. Trease and Evans' Pharmacognosy; Elsevier Health Sciences: New York, NY, USA, 2009. [Google Scholar]
- Mollataghi, A.; Coudiere, E.; Hadi, A.H.A.; Mukhtar, M.R.; Awang, K.; Litaudon, M.; Ata, A. Anti-acetylcholinesterase, anti-α-glucosidase, anti-leishmanial and anti-fungal activities of chemical constituents of Beilschmiedia species. Fitoterapia 2012, 83, 298–302. [Google Scholar] [CrossRef]
- Meng, F.; Zuo, G.; Hao, X.; Wang, G.; Xiao, H.; Zhang, J.; Xu, G. Antifungal activity of the benzo[c]phenanthridine alkaloids from Chelidonium. majus Linn against resistant clinical yeast isolates. J. Ethnopharmacol. 2009, 125, 494–496. [Google Scholar] [CrossRef]
- Rankovič, B.; Rankovic, D.; Maric, D. Antioxidant and antimicrobial activity of some Lichen species. Microbiology 2010, 79, 809–815. [Google Scholar] [CrossRef]
- Ayala-Zavala, J.F.; Silva-Espinoza, B.A.; Cruz-Valenzuela, M.R.; Villegas-Ochoa, M.A.; Esqueda, M.; González-Aguilar, G.A.; Calderón-López, Y. Antioxidant and antifungal potential of methanol extracts of Phellinus spp. from sonora, mexico. Rev. Iberoam. Micol. 2012, 29, 132–138. [Google Scholar] [CrossRef]
- Vijayarathna, S.; Zakaria, Z.; Chen, Y.; Latha, L.Y.; Kanwar, J.R.; Sasidharan, S. The antimicrobial efficacy of Elaeis guineensis: Characterization, in vitro and in vivo studies. Molecules 2012, 17, 4860–4877. [Google Scholar] [CrossRef]
- Kumar, R.S.; Sivakumar, T.; Sunderam, R.S.; Gupta, M.; Mazumdar, U.K.; Gomathi, P.; Rajeshwar, Y.; Saravanan, S.; Kumar, M.S.; Murugesh, K. Antioxidant and antimicrobial activities of Bauhinia racemosa L. Stem bark. Stem bark. Braz. J. Med. Biol. Res. 2005, 38, 1015–1024. [Google Scholar] [CrossRef]
- Chaieb, K.; Zmantar, T.; Ksouri, R.; Hajlaoui, H.; Mahdouani, K.; Abdelly, C.; Bakhrouf, A. Antioxidant properties of the essential oil of Eugenia caryophyllata and its antifungal activity against a large number of clinical Candida species. Mycoses 2007, 50, 403–406. [Google Scholar] [CrossRef]
- ElSohly, H.N.; Joshi, A.S.; Nimrod, A.C.; Walker, L.A.; Clark, A.M. Antifungal chalcones from Maclura. tinctoria. Planta Med. 2001, 67, 87–89. [Google Scholar] [CrossRef]
- Sathiamoorthy, B.; Gupta, P.; Kumar, M.; Chaturvedi, A.K.; Shukla, P.K.; Maurya, R. New antifungal flavonoid glycoside from Vitex. negundo. Bioorg. Med. Chem. Lett. 2007, 17, 239–242. [Google Scholar] [CrossRef]
- Martins, C.V.B.; da Silva, D.L.; Neres, A.T.M.; Magalhaes, T.F.F.; Watanabe, G.A.; Modolo, L.V.; Sabino, A.A.; de Fátima, A.; de Resende, M.A. Curcumin as a promising antifungal of clinical interest. J. Antimicrob. Chemother. 2009, 63, 337–339. [Google Scholar]
- Mbaveng, A.T.; Kuete, V.; Ngameni, B.; Beng, V.P.; Ngadjui, B.T.; Meyer, J.J.M.; Lall, N. Antimicrobial activities of the methanol extract and compounds from the twigs of Dorstenia mannii (Moraceae). BMC Complement. Alter. Med. 2012, 12, 83–88. [Google Scholar] [CrossRef]
- Sanguinetti, M.; Posteraro, B.; Romano, L.; Battaglia, F.; Lopizzo, T.; de Carolis, E.; Fadda, G. In vitro activity of Citrus bergamia (Bergamot) oil against clinical isolates of dermatophytes. J. Antimicrob. Chemother. 2007, 59, 305–308. [Google Scholar]
- Verzera, A.; Trozzi, A.; Gazea, F.; Cicciarello, G.; Cotroneo, A. Effects of rootstock on the composition of bergamot (Citrus bergamia risso et poiteau) essential oil. J. Agric. Food Chem. 2003, 51, 206–210. [Google Scholar] [CrossRef]
- Romano, L.; Battaglia, F.; Masucci, L.; Sanguinetti, M.; Posteraro, B.; Plotti, G.; Zanetti, S.; Fadda, G. In vitro activity of bergamot natural essence and furocoumarin-free and distilled extracts, and their associations with boric acid, against clinical yeast isolates. J. Antimicrob. Chemother. 2005, 55, 110–114. [Google Scholar]
- Fotie, J.; Bohle, D.S. Pharmacological and biological activities of xanthones. Antiinfect. Agents Med. Chem. 2006, 5, 15–31. [Google Scholar] [CrossRef]
- Sousa, M.E.; Pinto, M.M.M. Synthesis of xanthones: An overview. Curr. Med. Chem. 2005, 12, 2447–2479. [Google Scholar] [CrossRef]
- Na, Y. Recent cancer drug development with xanthone structures. J. Pharm. Pharmacol. 2009, 61, 707–712. [Google Scholar] [CrossRef]
- Pinto, D.C.G.; Fuzzati, N.; Pazmino, X.C.; Hostettmann, K. Xanthone and antifungal constituents from Monnina obtusifolia. Phytochemistry 1994, 37, 875–878. [Google Scholar] [CrossRef]
- Pinto, E.; Afonso, C.; Duarte, S.; Vale‐Silva, L.; Costa, E.; Sousa, E.; Pinto, M. Antifungal activity of xanthones: Evaluation of their effect on ergosterol biosynthesis by high-performance liquid chromatography. Chem. Biol. Drug Des. 2011, 77, 212–222. [Google Scholar] [CrossRef]
- Tocci, N.; D’Auria, F.D.; Simonetti, G.; Panella, S.; Palamara, A.T.; Debrassi, A.; Clovis, A.R.; Cechinel Filho, V.; Sciubba, F.; Pasqua, G. Bioassay-guided fractionation of extracts from Hypericum perforatum in vitro roots treated with carboxymethylchitosans and determination of antifungal activity against human fungal pathogens. Plant Physiol. Biochem. 2013, 70, 342–347. [Google Scholar] [CrossRef]
- Peterson, J.; Dwyer, J.; Adlercreutz, H.; Scalbert, A.; Jacques, P.; McCullough, M.L. Dietary lignans: Physiology and potential for cardiovascular disease risk reduction. Nutr. Rev. 2010, 68, 571–603. [Google Scholar] [CrossRef]
- Kim, M.-R.; Moon, H.T.; Lee, D.G.; Woo, E.-R. A new lignan glycoside from the stem bark of Styrax japonica s. Et z. Arch. Pharm. Res. 2007, 30, 425–430. [Google Scholar] [CrossRef]
- Park, C.; Woo, E.-R.; Lee, D.G. Anti-candida property of a lignan glycoside derived from Styrax japonica s. Et z. via membrane-active mechanisms. Mol. Cells 2010, 29, 581–584. [Google Scholar] [CrossRef]
- Koroishi, A.M.; Foss, S.R.; Cortez, D.A.G.; Ueda-Nakamura, T.; Nakamura, C.V.; Dias Filho, B.P. In vitro antifungal activity of extracts and neolignans from Piper regnellii against dermatophytes. J. Ethnopharmacol. 2008, 117, 270–277. [Google Scholar] [CrossRef]
- Liu, M.; Katerere, D.R.; Gray, A.I.; Seidel, V. Phytochemical and antifungal studies on Terminalia. mollis and Terminalia brachystemma. Fitoterapia 2009, 80, 369–373. [Google Scholar] [CrossRef]
- Santos, C.A.D.M.; Torres, K.R.; Leonart, R. Plantas. Medicinais: Herbarium, Flora et Scientia; Medicinal Plants: Herbariun., Flora et Scientia. Scientia et labor: Curitiba, Brazil, 1988. [Google Scholar]
- Alzugaray, D.; Alzugaray, C. Plantas Que Curam, 3rd ed.; M.V.P. Publisher: São Paulo, Brazil, 1983. [Google Scholar]
- Ishida, K.; de Mello, J.C.P.; Cortez, D.A.G.; Dias Filho, B.P.; Ueda-Nakamura, T.; Nakamura, C.V. Influence of tannins from Stryphnodendron adstringens on growth and virulence factors of Candida albicans. J. Antimicrob. Chemother. 2006, 58, 942–949. [Google Scholar] [CrossRef]
- Ishida, K.; Rozental, S.; de Mello, J.C.P.; Nakamura, C.V. Activity of tannins from Stryphnodendron adstringens on Cryptococcus neoformans: Effects on growth, capsule size and pigmentation. Ann. Clin. Microbiol. Antimicrob. 2009, 8, 29–38. [Google Scholar] [CrossRef]
- Berdy, J. Bioactive microbial metabolites. J. Antibiot. 2005, 58, 1–26. [Google Scholar] [CrossRef]
- Demain, A.L.; Sanchez, S. Microbial drug discovery: 80 years of progress. J. Antibiot. 2009, 62, 5–16. [Google Scholar] [CrossRef]
- Phongpaichit, S.; Rungjindamai, N.; Rukachaisirikul, V.; Sakayaroj, J. Antimicrobial activity in cultures of endophytic fungi isolated from Garcinia species. FEMS Immunol. Med. Microbiol. 2006, 48, 367–372. [Google Scholar] [CrossRef]
- Gao, X.; Lu, Y.; Xing, Y.; Ma, Y.; Lu, J.; Bao, W.; Wang, Y.; Xi, T. A novel anticancer and antifungus phenazine derivative from a marine actinomycete bm-17. Microbiol. Res. 2012, 167, 616–622. [Google Scholar] [CrossRef]
- Xu, L.L.; Han, T.; Wu, J.Z.; Zhang, Q.Y.; Zhang, H.; Huang, B.K.; Rahman, K.; Qin, L.P. Comparative research of chemical constituents, antifungal and antitumor properties of ether extracts of Panax ginseng and its endophytic fungus. Phytomedicine 2009, 16, 609–616. [Google Scholar] [CrossRef]
- Hertzberg, R.P.; Pope, A.J. High-throughput screening: New technology for the 21st century. Curr. Opin. Chem. Boil. 2000, 4, 445–451. [Google Scholar] [CrossRef]
- Congreve, M.; Murray, C.W.; Blundell, T.L. Keynote review: Structural biology and drug discovery. Drug Discov. Today 2005, 10, 895–907. [Google Scholar] [CrossRef]
- Kitamura, A.; Someya, K.; Hata, M.; Nakajima, R.; Takemura, M. Discovery of a small-molecule inhibitor of β-1,6-glucan synthesis. Antimicrob. Agents Chemother. 2009, 53, 670–677. [Google Scholar] [CrossRef]
- Kitamura, A.; Someya, K.; Okumura, R.; Hata, M.; Takeshita, H.; Nakajima, R. In vitro antifungal activities of D11–2040, a beta-1,6-glucan inhibitor, with or without currently available antifungal drugs. Biol. Pharm. Bull. 2010, 33, 192–197. [Google Scholar] [CrossRef]
- Bauer, J.R.; Kinast, S.; Burger-Kentischer, A.; Finkelmeier, D.; Kleymann, G.; Rayyan, W.A.; Schröppel, K.; Singh, A.; Jung, G.N.; Wiesmüller, K.H. High-throughput-screening-based identification and structure–activity relationship characterization defined (S)-2-(1-aminoisobutyl)-1-(3-chlorobenzyl) benzimidazole as a highly antimycotic agent nontoxic to cell lines. J. Med. Chem. 2011, 54, 6993–6997. [Google Scholar] [CrossRef]
- Burger-Kentischer, A.; Finkelmeier, D.; Keller, P.; Bauer, J.; Eickhoff, H.; Kleymann, G.; Rayyan, W.A.; Singh, A.; Schröppel, K.; Lemuth, K. A screening assay based on host-pathogen interaction models identifies a set of novel antifungal benzimidazole derivatives. Antimicrob. Agents Chemother. 2011, 55, 4789–4801. [Google Scholar] [CrossRef]
- Chaturvedi, S.; Rajkumar, S.S.; Li, X.; Hurteau, G.J.; Shtutman, M.; Chaturvedi, V. Antifungal testing and high-throughput screening of compound library against Geomyces destructans, the etiologic agent of geomycosis (wns) in bats. PLoS One 2011, 6, e17032. [Google Scholar]
- Sun, W.; Park, Y.D.; Sugui, J.A.; Fothergill, A.; Southall, N.; Shinn, P.; McKew, J.C.; Kwon-Chung, K.J.; Zheng, W.; Williamson, P.R. Rapid identification of antifungal compounds against exserohilum rostratum using high throughput drug repurposing screens. PloS One 2013, 8, e70506. [Google Scholar] [CrossRef]
- Macarron, R.; Banks, M.N.; Bojanic, D.; Burns, D.J.; Cirovic, D.A.; Garyantes, T.; Green, D.V.S.; Hertzberg, R.P.; Janzen, W.P.; Paslay, J.W. Impact of high-throughput screening in biomedical research. Nat. Rev. Drug Discov. 2011, 10, 188–195. [Google Scholar] [CrossRef]
- Sukumar, N.; Krein, M.P.; Embrechts, M.J. Predictive cheminformatics in drug discovery: Statistical modeling for analysis of micro-array and gene expression data. In Bioinformatics and Drug Discovery; Larson, R.S., Ed.; Springer: New York, NY, USA, 2012; Volume 910, pp. 165–194. [Google Scholar]
- Bredel, M.; Jacoby, E. Chemogenomics: An emerging strategy for rapid target and drug discovery. Nat. Rev. Genet. 2004, 5, 262–275. [Google Scholar] [CrossRef]
- Bleicher, K.H.; Böhm, H.J.; Müller, K.; Alanine, A.I. Hit and lead generation: Beyond high-throughput screening. Nat. Rev. Drug Discov. 2003, 2, 369–378. [Google Scholar] [CrossRef]
- Stumpfe, D.; Ripphausen, P.; Bajorath, J. Virtual compound screening in drug discovery. Future Med. Chem. 2012, 4, 593–602. [Google Scholar] [CrossRef]
- Basak, S.C. Chemobioinformatics: The advancing frontier of computer-aided drug design in the post-genomic era. Curr. Comput. Aided. Drug Des. 2012, 8, 1–2. [Google Scholar] [CrossRef]
- Abadio, A.K.R.; Kioshima, E.S.; Teixeira, M.M.; Martins, N.F.; Maigret, B.; Felipe, M.S.S. Comparative genomics allowed the identification of drug targets against human fungal pathogens. BMC Genomics 2011, 12. [Google Scholar] [CrossRef]
- Pierce, C.G.; Lopez-Ribot, J.L. Candidiasis drug discovery and development: New approaches targeting virulence for discovering and identifying new drugs. Expert Opin. Drug Discov. 2013, 8, 1–10. [Google Scholar] [CrossRef]
- Pierri, C.L.; Parisi, G.; Porcelli, V. Computational approaches for protein function prediction: A combined strategy from multiple sequence alignment to molecular docking-based virtual screening. Biochim. Biophys. Acta 2010, 1804, 1695–1712. [Google Scholar] [CrossRef]
- Cavasotto, C.N.; Phatak, S.S. Homology modeling in drug discovery: Current trends and applications. Drug Discov. Today 2009, 14, 676–683. [Google Scholar] [CrossRef]
- Swinney, D.C.; Anthony, J. How were new medicines discovered? Nat. Rev. Drug Discov. 2011, 10, 507–519. [Google Scholar]
- Berne, S.; Podobnik, B.; Zupanec, N.; Novak, M.; Kraševec, N.; Turk, S.; Korošec, B.; Lah, L.; Šuligoj, E.; Stojan, J. Virtual screening yields inhibitors of novel antifungal drug target, benzoate 4-monooxygenase. J. Chem. Inf. Model. 2012, 52, 3053–3063. [Google Scholar] [CrossRef]
- Morya, V.K.; Kumari, S.; Kim, E.K. Virtual screening and evaluation of ketol-acid reducto-isomerase (kari) as a putative drug target for aspergillosis. Clin. Proteomics 2012, 9, 1–12. [Google Scholar] [CrossRef]
- Sheng, C.; Wang, W.; Che, X.; Dong, G.; Wang, S.; Ji, H.; Miao, Z.; Yao, J.; Zhang, W. Improved model of lanosterol 14alpha-demethylase by ligand-supported homology modeling: Validation by virtual screening and azole optimization. Chem. Med. Chem. 2010, 5, 390–397. [Google Scholar] [CrossRef]
- Sheng, C.; Che, X.; Wang, W.; Wang, S.; Cao, Y.; Miao, Z.; Yao, J.; Zhang, W. Design and synthesis of novel triazole antifungal derivatives by structure-based bioisosterism. Eur. J. Med. Chem. 2011, 46, 5276–5282. [Google Scholar] [CrossRef]
- Zou, Y.; Zhao, Q.; Liao, J.; Hu, H.; Yu, S.; Chai, X.; Xu, M.; Wu, Q. New triazole derivatives as antifungal agents: Synthesis via click reaction, in vitro evaluation and molecular docking studies. Bioorg. Med. Chem. Lett. 2012, 22, 2959–2962. [Google Scholar] [CrossRef]
- Xu, J.; Cao, Y.; Zhang, J.; Yu, S.; Zou, Y.; Chai, X.; Wu, Q.; Zhang, D.; Jiang, Y.; Sun, Q. Design, synthesis and antifungal activities of novel 1, 2, 4-triazole derivatives. Eur. J. Med. Chem. 2011, 46, 3142–3148. [Google Scholar] [CrossRef]
- Chai, X.; Yang, G.; Zhang, J.; Yu, S.; Zou, Y.; Wu, Q.; Zhang, D.; Jiang, Y.; Cao, Y.; Sun, Q. Synthesis and biological evaluation of triazole derivatives as potential antifungal agent. Chem. Biol. Drug. Des. 2012, 80, 382–387. [Google Scholar] [CrossRef]
- Hata, M.; Ishii, Y.; Watanabe, E.; Uoto, K.; Kobayashi, S.; Yoshida, K.-I.; Otani, T.; Ando, A. Inhibition of ergosterol synthesis by novel antifungal compounds targeting c-14 reductase. Med. Mycol. 2010, 48, 613–621. [Google Scholar] [CrossRef]
- Cadicamo, C.D.; Mortier, M.J.; Wolber, G.; Hell, M.; Heinrich, I.E.; Michel, D.; Semlin, L.; Berger, U.; Korting, H.C.; Höltje, H.; et al. Design, synthesis, inhibition studies, and molecular modeling of pepstatin analogues addressing different secreted aspartic proteinases of Candida albicans. Biochem. Pharmacol. 2013, 85, 881–887. [Google Scholar] [CrossRef]
- Amaral, A.C.; Felipe, M.S.S. Nanobiotechnology: An efficient approach to drug delivery of unstable biomolecules. Curr. Protein Pept. Sci. 2013, 14, 588–594. [Google Scholar] [CrossRef]
- Van de Ven, H.; Paulussen, C.; Feijens, P.B.; Matheeussen, A.; Rombaut, P.; Kayaert, P.; van den Mooter, G.; Weyenberg, W.; Cos, P.; Maes, L. Plga nanoparticles and nanosuspensions with amphotericin B: Potent in vitro and in vivo alternatives to fungizone and ambisome. J. Controlled Release 2012, 161, 795–803. [Google Scholar] [CrossRef]
- Amaral, A.C.; Bocca, A.L.; Ribeiro, A.M.; Nunes, J.; Peixoto, D.L.G.; Simioni, A.R.; Primo, F.L.; Lacava, Z.G.M.; Bentes, R.; Titze-de-Almeida, R. Amphotericin B in poly (lactic-co-glycolic acid)(plga) and dimercaptosuccinic acid (dmsa) nanoparticles against paracoccidioidomycosis. J. Antimicrob. Chemother. 2009, 63, 526–533. [Google Scholar] [CrossRef]
© 2014 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license ( http://creativecommons.org/licenses/by/3.0/).
Share and Cite
Negri, M.; Salci, T.P.; Shinobu-Mesquita, C.S.; Capoci, I.R.G.; Svidzinski, T.I.E.; Kioshima, E.S. Early State Research on Antifungal Natural Products. Molecules 2014, 19, 2925-2956. https://doi.org/10.3390/molecules19032925
Negri M, Salci TP, Shinobu-Mesquita CS, Capoci IRG, Svidzinski TIE, Kioshima ES. Early State Research on Antifungal Natural Products. Molecules. 2014; 19(3):2925-2956. https://doi.org/10.3390/molecules19032925
Chicago/Turabian StyleNegri, Melyssa, Tânia P. Salci, Cristiane S. Shinobu-Mesquita, Isis R. G. Capoci, Terezinha I. E. Svidzinski, and Erika Seki Kioshima. 2014. "Early State Research on Antifungal Natural Products" Molecules 19, no. 3: 2925-2956. https://doi.org/10.3390/molecules19032925
APA StyleNegri, M., Salci, T. P., Shinobu-Mesquita, C. S., Capoci, I. R. G., Svidzinski, T. I. E., & Kioshima, E. S. (2014). Early State Research on Antifungal Natural Products. Molecules, 19(3), 2925-2956. https://doi.org/10.3390/molecules19032925




