Abstract
Cancer is a chronic disease with long-term consequences for health and quality of life and is more prevalent among older people. Therefore, comorbidity among cancer patients is commonly observed. Several data indicate that 40% of cancer patients have at least one other chronic condition recorded, and of these, 15% have two or more medical conditions, including cardiovascular disease, obesity and metabolic disease, mental health problems, and muscle-skeletal conditions. There is no gold-standard approach for measuring comorbidity in the context of cancer, especially in recent years, when health systems have dealt with a pandemic emergency that has negatively impacted the management of cancer patients. The purpose of this narrative review is to clarify and provide the necessary insights to optimize the care of cancer patients. Ensuring the continuum of care for cancer patients is of vital importance and is considered a top priority. It is necessary to overcome the model that considers neoplastic pathology as a single morbid condition. Instead, the complexity of a cancer patient’s problems must be considered and related to complex medical conditions. Addressing the problem of comorbidity in cancer more decisively will be a central challenge if we are to avert a crisis in the models of diagnosis and treatment of cancer patients.
1. Background
Chronic diseases are generally more common among older adults than younger adults, and though many of these are not life threatening in the short term, they can have serious effects on quality of life. As a result, many people live with chronic diseases that gradually worsen health, rather than dying from a single serious condition [1]. Cancer is a chronic disease with long-term consequences for health and quality of life and is more prevalent among older people. Aging is a determining factor in the development of cancer. In fact, over time, the aging body accumulates the effects of carcinogenic factors, reducing the ability to repair cells. In fact, the incidence of tumors clearly increases with age [2]. Comorbidity among cancer patients is therefore commonly observed. Several data indicate that cancer patients suffer at least one other recorded chronic condition or have two or more medical conditions [1]. The coexistence of cancer and other chronic conditions has major implications for treatment decisions and treatment outcomes for both cancer and its associated chronic diseases [2,3,4,5,6,7]. Most cancer treatment guidelines, which include conventional therapeutic protocols used in oncology, tend not to consider the complex interrelationships between cancer and comorbidities and instead adopt a single-disease approach, managing almost exclusively the type of oncological condition. Today, with the increase in sub-specialization in medicine and surgery, many healthcare providers are often not sufficiently qualified to manage a wide spectrum of different diseases. This aspect affects especially cancer patients, and potentially has a negative impact on patient therapies [7].
2. Methods
In this narrative review, we included clinical trials published by Pubmed through 28 February 2022. The keywords used were cancer, comorbidity, health organization, and gold-standard approach. All paper and clinical published by Pubmed were studied by two authors. We excluded studies written in languages other than English. Two authors (P.C., T.C.) reviewed all articles and all studies were qualitatively analyzed. The goal of this review is to provide the necessary decision support to public health agencies to promote sound public health approaches, facilitate transparency, and build trust in the community. The review of studies on tumor pathology clusters is difficult to provide definitive answers on the management of the disease. Furthermore, it is inherently difficult to study a cluster for a disease with complex etiology and long latency like most cancers. Despite this difficulty, cluster assessment remains an important function of local, state, and federal public health agencies. Prompt and timely involvement of public health agencies is critical because a poor initial response can result in the loss of opportunities for investigation and education and can increase the level of uncertainty and concern in a community, resulting in the potential need to spend further public health resources later.
The Concept of Comorbidity and Frailty
Comorbidity is generally defined as the coexistence of one or more disorders alongside a primary disease of interest [8]. In the care of cancer patients, comorbidity represents a substrate of the nature and severity of the health conditions that exist alongside the neoplasm and is distinct from another indicator, which is frailty, and which is more concerned with the preservation of functional status. The prevalence of comorbidities varies based on a patient’s non-modifiable factors. Like cancer itself, comorbidity increases in quantity and severity with age, even if the age and quantity of pathological conditions in older people do not necessarily coexist. Comorbidity depends on the patient’s social and economic condition, on the possibility of accessing the best center for treatment of every pathology, and on the difficulty of obtaining optimal care at home. Functional status, that is, the measure of a patients’ ability to perform daily tasks, is linked to both the presence and consequences of chronic diseases.
Frailty is defined as a physiological state of greater vulnerability to stress factors resulting from the variable but predictable decrease from subject to subject in physiological reserves, and from dysregulation of the organism’s multiple physiological systems [9]. With respect to comorbidity, frailty is strongly linked to increasing age, and refers to the quality of each subject’s senescence [9,10]. Although there is a strong association between them, comorbidities, functional status, and frailty sometimes concur in synergy in determining the clinical result and sometimes have independent effects in determining the predetermined results [3,9].
There is no gold-standard approach to measuring comorbidity in the context of cancer, because so far, no attention has been paid to data retention, resulting in loss of information. Furthermore, where the data have been stored, homogeneous standardized methods have not been used for their management. Both the lack of data collection and the lack of standardized data management methods represent an unsolved problem in defining the correlation between cancer and the coexistence of one or more disorders.
3. Results
3.1. The Prevalence of Comorbidity in Cancer Patients
Based on the above and considering that there is general agreement that comorbidity is common among cancer patients, it is difficult to state exactly how the two entities relate to each other. The cause of this is the heterogeneous method of measuring the prevalence of comorbidity in the study population, and the type of cancer. In various studies, comorbidity had a variable effect on the use of chemotherapy, and different results were observed among patients with solid tumours [11], particularly in older patients. Other studies conducted on cancer patients, based on administrative data, report lower levels of comorbidity than those based on the revision of medical notes or on self-assessment [12,13,14,15,16,17]. Overall, these results, and those of several other studies [1], are consistent with the presence of a prevalence spectrum of comorbidities among cancer patients. Furthermore, patients diagnosed with cancer are most often those who have pathological conditions most strongly associated with risk factors (especially smoking). There is a wide range of cancer types, such as breast and prostate cancer, which are not strongly linked to environmental factors such as age; these include exposure to ultraviolet (UV) radiation, alcohol use, smoking, and exposure to pollution, all of which further contribute to the chronic accumulation of DNA damage. Data from epidemiological studies suggest that the prevalence of comorbidity tends to be higher among racial/ethnic minority cancer patients and those living with higher levels of deprivation or poverty [18,19,20,21,22]. In some studies, comorbidity has been shown to be partly responsible for disparities in cancer survival among social groups, especially among racial/ethnic groups, compared to general population data [21,23,24,25,26,27,28,29,30,31].
3.2. Mechanisms of Interaction between Neoplasia and Comorbidities
There is a lot of evidence that comorbidities and their therapies can play a protective or pejorative role, depending on the type of cancer. For example, diabetes has been reported to play a protective role against some forms of cancers of the prostate and lung, and against Hodgkin’s lymphoma. On the other hand, patients with diabetes have an increased risk of getting other cancers [32,33]. The different role of metabolic disease is supported by various evidence linking the genesis of tumours with changes in hormone profiles, growth factors, and endogenous steroids [32]. Furthermore, according to various evidence, some treatments for diabetes or obesity, in particular metformin and thiazolidinediones, appear to have antineoplastic activity and may act in reducing the incidence of cancer and slow its progression, probably due to the reduction of cellular proliferation activity [32,34,35].
Similarly, it has been established that the use of non-steroidal anti-inflammatory drugs, commonly used in arthritis and common musculoskeletal diseases, is associated with a reduced risk of colorectal cancer [36,37]. Several studies have hypothesized that there is an inverse relationship between neurodegenerative diseases and cancer [37,38], affirming the presence of a protective balance between the DNA repair mechanisms that promote cell growth and those that inhibit it [38,39]. There may also be interactions between specific tumours with specific comorbid conditions. For example, some studies [40,41] have shown that, among patients on renal dialysis for end-stage renal disease, the possibility of diagnosing cancers of the digestive system occurs earlier, while prostate cancer is usually diagnosed later. This is possible because, in the group of dialysis patients, there is a higher incidence of bleeding or anaemia, and therefore a more frequent use of endoscopic examinations than in the general population. On the contrary, the same authors [40,41] have affirmed that dialysis patients paradoxically underestimate any urinary symptoms, resulting in the subsequent diagnosis of any malignant diseases.
3.3. Impact of Comorbidities on the Time to Diagnosis of Neoplasms
As previously noted regarding the interaction between comorbidities and cancer, the presence of one or more comorbidities plays a double role, positive or negative, on the possibility of tumour diagnosis, and can limit the diagnostic possibilities in various cases of tumours, especially in those where the use of invasive procedures is necessary. In fact, the presence of comorbidities can lead to greater access to health services with consequently greater opportunities for screening and early diagnosis of cancers. The presence of different frailty conditions can cause the professional or the patient to lose interest in tracking health status, which consequently can increase the number of late diagnoses or diagnostic delays. In other cases, the presence of one or more comorbidities prevents the patient from making an exhaustive and complete diagnosis due to the impossibility of performing high-level or highly invasive diagnostic tests [42,43,44]. These two mechanisms, as mentioned, do not offer a simple explanation clarifying the relationship between the time of diagnosis of cancer and the type of comorbidity. Numerous studies in different populations indicate that a correct and timely diagnosis of cancer depends on social context, on the local organization of the health system service, and on the geographical distance of the main diagnostic centres that report a broad spectrum of data in comparison to the cancer population without comorbidities [45,46]. According to the literature, the interaction between various factors including those relating to the type of cancer, the type and severity of comorbidities, and the efficiency of the organization of the health system can affect cancer diagnosis [47,48].
3.4. Types and Severity of Comorbidities
According to the literature, patients with one or more comorbidities require more frequent medical visits, and therefore have greater opportunities to undergo screening or to have access to cancer screening investigations early, right from the first symptoms [41,42,43,44,45,46,47,48,49]. However, an inverse relationship between comorbidities and symptoms has been observed with consequent underestimation of the first manifestations of any neoplastic pathology, since the management of comorbidities can involve the total attention of the staff assigned to such treatments, thus limiting the possibility of an easy diagnosis of cancer. This is likely to be especially true for those with unstable and/or life-threatening conditions [50,51]. Additionally, there may be biological interactions between the specific circumstances of the comorbidity and cancer that may affect the stage of diagnosis. For example, the pathophysiological effects of diabetes mellitus, which results in an increased risk of cancer, may also be associated with more rapidly developing cancers, thereby leading to difficulties in early diagnosis. Siddiqui et al. [52] found that patients with uncontrolled type II diabetes tended to have more advanced forms of colorectal cancer diagnosed at a younger age than those with well-controlled diabetes despite having similar socio-demographic characteristics and equal number of outpatient visits.
3.5. The Impact of the Organization of the Health Service
The organization of health services can have an impact on the way in which comorbidity affects the stage of cancer diagnosis, particularly in the context of mass-screened cancers (Table 1). Cancers that are effectively diagnosed during screening procedures are more susceptible to early detection than other cancers, an effect that is most pronounced in the context of capillary screening [45,53]. Patients with comorbidities access health services more regularly and therefore may be more screened, particularly when screening participation rates are linked to massive funding from the health service or because they constitute quality indicators of the health system [54]. While these studies have shown that screening rates among patients with comorbidities in the context of these methods are like those without comorbidities, other studies [55,56] have not demonstrated this positive synergism, considering the presence of comorbidities an obstacle to achieving a correct diagnosis of cancer. Other authors have stigmatized the excessive use of diagnostic screening tools, often performed improperly in patients with severe comorbidities and limited life expectancy [57,58,59].

Table 1.
Type of comorbidities and preventive approaches in the various cancer.
3.6. Impact of Comorbidity on the Choice of Treatment for Neoplasms
Comorbidity patients are less likely to receive curative treatment for cancer than those with non-comorbid cancer [11,60,61,62,63,64,65,66,67,68,69,70]. Taking colorectal cancer as an example, numerous studies have found that the possibility of fully implementing chemotherapy protocols in these patients is lower among patients with comorbidities regardless of age [71,72,73,74]. The relationship between the number and type of co-morbidities and surgical treatment is less clear, with some studies reporting no association, and others showing an inverse relationship between increased comorbidity and decreased probability of surgery or reduced quality of surgical care for those with comorbidity [73,75,76,77]. Although most studies report that cancer patients with comorbidities receive less treatment than cancer patients without associated conditions, some studies have sometimes reported the presence of overtreatment in cancer patients with comorbidities [78]. Clinical evidence-based studies demonstrate the need to base decisions in cancer patients based on the number and type of comorbidities [79,80,81]. In the context of multi-disciplinary teams, in which many cancer treatment decisions are made, there is resistance to initiating chemotherapy in comorbid cancer patients [82]. There are numerous factors that can explain the negative effect of comorbidities with respect to a successful treatment outcome, starting with an increase in toxicity and side effects related to chemotherapy. It also seems clear that according to most clinicians in comorbidity patient groups, the treatments are less effective in these groups, and that the reduced life expectancy of these patients is a sufficient factor to sometimes justify the withdrawal of potentially harmful toxic agents [72,73,83,84,85]. It is also possible that these patients themselves refuse treatment, while it seems clear that cancer patients with comorbidities are usually less likely to receive curative treatment [84,85,86]. This is explained by the lack of significant evidence from the randomized controlled trials (RCTs) that often exclude older patients or those with comorbidities, which suggests that most therapeutic schemes are not directly applicable to these cancer patients [87,88].
3.7. Impact of Comorbidities on the Outcome of Cancer Treatment
The extent to which comorbidity can affect the success of treatments depends on the type and severity of the conditions and on the specific treatment to be implemented. For example, patients with severe chronic respiratory disease would hardly tolerate a pneumonectomy for lung cancer but could tolerate treatment that does not affect their already precarious respiratory function. Patients with severe renal damage would hardly tolerate a chemotherapy scheme conducted with nephrotoxic drugs but could benefit from other chemotherapy drugs. Numerous authors [89,90,91,92,93,94,95,96] have reported that, in general, comorbidity does not increase the frequency or severity of treatment-related complications. In contrast, other studies have reported higher complication rates among cancer patients with comorbidities [11,18,64,97,98,99,100] including patients treated only with surgery for curative removal of a neoplasm [97,98,99,100]. Studies evaluating the impact of comorbidity on the treatment of cancer have shown better survival in well attended patients with clinical conditions in equilibrium, compared to those who are not [72,78,101,102,103]. The interpretation of all these results, however, is always complicated by the fact that most clinical studies on cancer exclude patients with significant comorbidity, which makes it difficult to evaluate the real efficacy and toxicity of the treatment by comparing the results obtained in patients of cancer with and without comorbidities [88]. It was observed that patients with important comorbidities have the possibility of being treated and therefore of having better results than patients considered to be healthier [78,88,102,103]. The use of propensity scores could prove beneficial because they provide the possibility of determining the probability of success that an individual undergoing treatment has, regardless of whether he has received treatment [104]. Patients with similar propensity scores can be treated for malignancy and then their therapeutic results can be compared, depending on whether they received treatment. Bradley and colleagues [78] studied elderly prostate cancer patients with and without comorbidities, dividing their sample into men with high-risk, intermediate-risk, and low-risk prostate cancer, then calculated their propensity scores to determine the likelihood of receiving treatment. They found that men with both intermediate-risk and high-risk prostate cancer who were treated had substantially better survival rates than those who were not treated, with no difference in comorbid status [78]. Similarly, an observation of elderly patients with colorectal cancer showed that, by applying the propensity scores, there was less possibility of treatment in patients with comorbidities and advantage in survival in those with comorbidities who had been treated with curative intentions compared to those who had not [88]. These findings suggest that some comorbidity patients may benefit from potentially curative treatment. Another important consideration is the impact of cancer treatment with the interaction of other drugs. Patients with comorbidities certainly have a greater pharmacological load, which can interact with chemotherapeutic agents, potentially leading to greater toxicity and a reduction in the efficacy of a therapeutic regimen [104,105,106,107]. The few studies that have been done suggest that about one-third of treated cancer patients are exposed to potential interactions [108,109] and about one in ten unplanned hospitalizations of cancer patients are related to adverse drug reactions. It has been reported that polytherapy is associated with an increased risk of toxicity of chemotherapeutic agents compared to therapy with one or a few drugs [110,111]. In summary, while there is evidence that some cancer patients with comorbidities may be at an increased risk of post-therapeutic complications, this is not a constant occurrence. The extent to which treatments are tolerated will, of course, depend on several interacting and complex factors, including cancer treatment and the number, type, and severity of the specific comorbidities involved. However, what is clear is that there is substantial inconsistency in treatment decisions based on comorbidities and the lack of consensus on what should be done. It is possible that the lack of demonstrable differences in tolerability and treatment efficacy in patients with and without comorbidities suggests that the treatment recommendations available in the literature regarding these groups may not always be justifiable considering their actual clinical conditions.
3.8. Impact on Survival
Comorbidity has always been considered to have a negative impact on cancer survival [3,6,11] (Figure 1). The impact of comorbidity tends to increase with the increasing severity of clinical conditions, although not necessarily linearly [78,84,112]. Very high levels of comorbidities are often associated with a considerably higher risk of death than no comorbidities. The impact of comorbidity on cancer-specific survival is less constant and variable, depending on cancer prognosis, stage, treatment effect, and severity of comorbidity [1,6]. The impact of comorbidity tends to be greater for tutors with a better prognosis [113,114,115,116] while those affected by cancer associated with a high mortality rate will be more likely to die from same cancer, regardless of other concomitant diseases than patients who have a less severe prognosis. For example, Piccirillo et al. [114] have covered that, the impact of comorbidity is greater for cancer diagnosed at an early stage than for advanced cancer. There are several reasons why comorbidity impacts survival. The most obvious is the direct and independent impact of the concomitant disease on non-cancer mortality. In addition, cancer-specific survival can sometimes be reduced among those with comorbidities. A possible explanation for this is related to the fact that some cancer patients who die from circumstances related to comorbidities are wrongly categorized as dying of their cancer [117]. As described above, there is evidence that cancer patients with comorbidities receive less effective treatment than those without, and this has a major impact on their likelihood of survival. Comorbidity patients may also experience higher levels of treatment toxicity, negatively impacting their cancer-specific survival [11]. Another mechanism of interaction between comorbidity and survival is through a direct effect of the former on cancer progression. Meyerhardt et al. [89] studied the prognosis of patients with and without diabetes on adjuvant therapy for colon cancer, finding that diabetics had an increased risk of relapse. Piccirillo et al. [115] found that the likelihood of developing cancer recurrence increases proportionally with an increasing level of comorbidity. In contrast, Kiderlan [118] observed that, among breast cancer patients, those with diabetes have a lower relapse rate linked to the favorable effect of metformin in counteracting neoplastic growth.
Figure 1.
Comprovate comorbidities and cancer prognosis.
3.9. Impact on Quality of Life
Non-cancer studies have always associated comorbidity with a poorer quality of life [119,120,121,122]. There are few studies that investigate the subject in cancer patients. In a group of lung cancer patients, Gronberg et al. [91] found that all patients had poor quality of life and that this did not depend on the comorbid state. Studies on patients with early-stage prostate cancer have suggested that comorbidity leads to a lower quality of life during the treatment period but is common to all patients with the same cancer without other pathologies [123,124]. However, higher levels of disease, related to a delay in cancer diagnosis, are correlated with greater health care needs, greater likelihood of disability, higher costs of care, and higher financial commitment, and therefore to greater socioeconomic disadvantage [125,126,127] (Figure 2).
Figure 2.
Quality of life in cancer patients.
3.10. Impact of Cancer Treatments on Comorbidities
In addition to the impact of comorbidities on the outcome of cancer treatments, it is worth noting that cancer itself, or more specifically, the treatment, can influence the results related to the treatment of comorbidities. Cancer therapies can increase the risk of cardiovascular, metabolic, musculoskeletal, and other diseases, and can worsen pre-existing comorbidities. For example, metabolic changes associated with hormone treatment for cancer can lead to worsening diabetic control and an increased risk of diabetes-related complications [128]. Many chemotherapeutic agents are implicated in the development of heart failure [129]. Androgen deprivation therapy for prostate cancer is associated with an increased risk of cardiovascular problems and worsening of pre-existing heart disease [130,131]. Furthermore, hormone treatment for breast and prostate cancer is known to lead to or aggravate osteoporosis [132,133]. In addition to these direct effects, it is likely that, during cancer treatment, there may be a lack of attention to chronic disease management by both patients and clinicians, which, in turn, can negatively impact overall care outcomes. Little is known about how much cancer and its treatment impact the treatment outcomes of comorbidities, in part because patients with significant comorbidities are usually excluded from clinical trials, and in part because most of the data for cancer patients are concentrated on the evaluation of cancer-specific outcomes rather than on the evaluation of outcomes related to other conditions.
3.11. COVID-19 and Management of Cancer Patients
Cancer is a disease characterized by uncontrolled cell growth that can involve any tissue in the body and has the potential risk of spreading to target organs by contiguity or direct invasion, by haematogenic, lymphatic, and more rarely, neurogenic routes. The most frequently used cancer treatments work by killing or blocking the growth and spread of rapidly dividing cancer cells in target organs. However, some cancer treatments suppress other rapidly growing cells, such as white blood cells, and the cancer itself can affect the immune system by spreading to the bone marrow. Therefore, people with weak immune systems have a higher risk of getting frequent infections and are more likely to get COVID-19. The increased susceptibility of cancer patients to the serious complications of COVID-19 can be attributed to the state of immunosuppression caused by anticancer treatments, such as chemotherapy or surgery. Immunosuppression can also expose cancer patients to serious complications from an infection, which can lead to delayed treatment and unnecessary hospitalizations that could adversely affect disease prognosis. It has also been shown that patients undergoing different types of cancer treatment show disparity in response to COVID-19 compared to non-cancer patients. Finally, patients who received immunotherapy or surgery tend to have higher death rates and a greater chance of developing critical symptoms than those who received chemotherapy or radiotherapy [134,135,136]. Liang et al. [137] showed that patients who had undergone cancer-type surgery in the 30 days prior to presenting with COVID-19 had a greater risk of serious events than patients who had not been treated with chemotherapy or surgery. Cancer history was also found to confer the highest risk of serious complications and correlated with worse outcomes from COVID-19. Liang et al. [137] demonstrated that patients with cancer consistently show a higher risk of serious infections, with an approximately 3.5-fold increased risk of needing mechanical ventilation, intensive care unit (ICU) admission, or death compared to patients without cancer. Today, there are no sufficiently shared guidelines regarding the association of COVID-19 infection and the management of cancer patients. The same authors [137] indicated three strategies that may be applied to cancer patients during the COVID-19 pandemic: postponing chemotherapy treatment or elective surgical procedures in stable cancer cases, implementing strict personal precautions in cancer patients or cancer survivors, and providing more intensive care and treatment to cancer patients with COVID-19. These strategies may not be wholly sufficient since they do not consider elderly patients or those who may have other comorbidities. In our opinion, the cancer patient’s demand for care must be managed by creating paths within the cancer centres, capable of combining treatment efficacy and safety [137]. This would have been possible by placing hospitals and cancer centres in a common network, giving space to multidisciplinary teams, and more effectively separating these patients from the flow of those who crowded emergency and intensive care facilities during the pandemic. Ultimately, the demand for treatment of cancer patients had to be conveyed to suitable structures where every moment of treatment was guaranteed in complete safety and was effective in contrasting the progression of cancer.
3.11.1. A. Risk Factors Associated with the Severity of COVID-19 in Cancer Patients
From the data available in the literature [138,139,140], severe COVID-19 disease and mortality in cancer patients are significantly associated with advanced age and disease severity, especially the pulmonary pathological picture, the presence of multiple comorbidities, and harmful habits such as cigarette smoking. Mehta et al. [138] demonstrated that advanced age in cancer patients is significantly associated with increased mortality, more severe disease manifestation, and an increased need for ventilatory support or intensive care. It is interesting to note that, in this study, there was no statistically significant difference between advanced metastatic tumour disease or localized tumour and death from COVID-19 [138]. Furthermore, patients undergoing chemotherapy or radiotherapy did not show a significant difference in COVID-related deaths compared to patients currently not on treatment. Conversely, comorbidities, including heart disease (hypertension, coronary heart disease, congestive heart failure) and chronic lung disease led to an increased risk of COVID-19-related deaths in cancer patients [138]. Furthermore, the same study and other studies [139,140] admitted that cancer patients die predominantly in old age, but the mortality rate is significantly higher in all age groups than in for non-cancer patients, suggesting the COVID-19 virus affects cancer patients more severely than the general population. Additionally notable are the data regarding the severity of COVID-19 in lung cancer patients, where a worse prognosis was observed in those with advanced age, history of smoking, chronic obstructive pulmonary disease (COPD), and chronic heart failure [141] (Figure 3). However, the severe disease and mortality rate from COVID-19 did not differ in patients receiving chemotherapy or tyrosine kinase inhibitors compared to other patients with lung cancer [141]. Another study conducted by Garassino et al. [142] considered patients with thoracic malignancies, showing that age (>65 years), cigarette smoking, chemotherapy treatment, and any comorbidities were associated with an increased risk of death due to COVID-19.
Figure 3.
Comprovate risk factors in COVID-19 cancer patients.
The evidence that emerged from patients with haematological malignancies and concomitant COVID-19 infection is also of great interest. Passamonti et al. [143] found in an observation study that the main risk factors associated with worse overall survival were advanced age, the level of disease progression, the diagnosis of acute myeloid leukaemia, indolent non-Hodgkin’s lymphoma, aggressive non-Hodgkin’s lymphoma or plasma cell neoplasms, and severe pulmonary involvement of COVID-19 infection. Furthermore, patients were at higher risk of mortality regardless of whether they had recent illness or were on specific therapy, or both [144]. Active chemotherapy treatment and viral load at diagnosis were not predictors of COVID-19 hematologic patient mortality [139,145]. As we have seen, multiple prognostic variables have been associated with COVID-19-related mortality in cancer patients, such advanced age, male sex, cigarette smoking, number of comorbidities, and the presence of solid versus haematological tumours. Instead, race, ethnicity, obesity, malignancy, or type of cancer treatment were not associated with high mortality [136,145].
3.11.2. B. Health Organization and Cancer Treatment in the Pandemic Period
Wang and Zhang [146] pointed out that, during the COVID-19 pandemic, the main risk for cancer patients was limited access to necessary health care and the inability to receive necessary medical services in a timely manner, especially in high-risk epidemic areas where a large percentage of medical personnel and health facilities were required for the fight against the pandemic. In our opinion, the limited access to treatment of cancer patients was not only a problem in the areas with the highest incidence but also in other areas, not necessarily those with a high population density, but also in more isolated areas, in which the most advanced treatments in the oncology field were unavailable. The blocking of diagnostics, outpatient services, surgical interventions in the oncological field, and the administration of chemotherapy and radiotherapy sessions led to a worsening of mortality and disease progression in patients under treatment. During the most critical period of the pandemic, the rationing of care, the cancellation of appointments, and the postponement of surgeries led to difficult decisions. In the case of critically ill patients, care plans had to be revised and end-of-life plans and palliative care had to be revisited. Faced with limited resources during the COVID-19 pandemic, greater organizational effort was required, making the formation of multidisciplinary cancer treatment teams including medical ethics experts and palliative care specialists far more difficult. In this scenario, it was very difficult and complicated to decide which patients should undergo more intensive therapies because they were complicated or critical, and it was difficult to postpone the appropriate treatments, having to review the outcomes for each patient, without being able to obtain the expected clinical results [147]. The experience of the pandemic in the future will have to involve greater levels of organization of our health systems to guarantee the most appropriate treatments for all while still adhering to high safety standards.
4. Future Directions
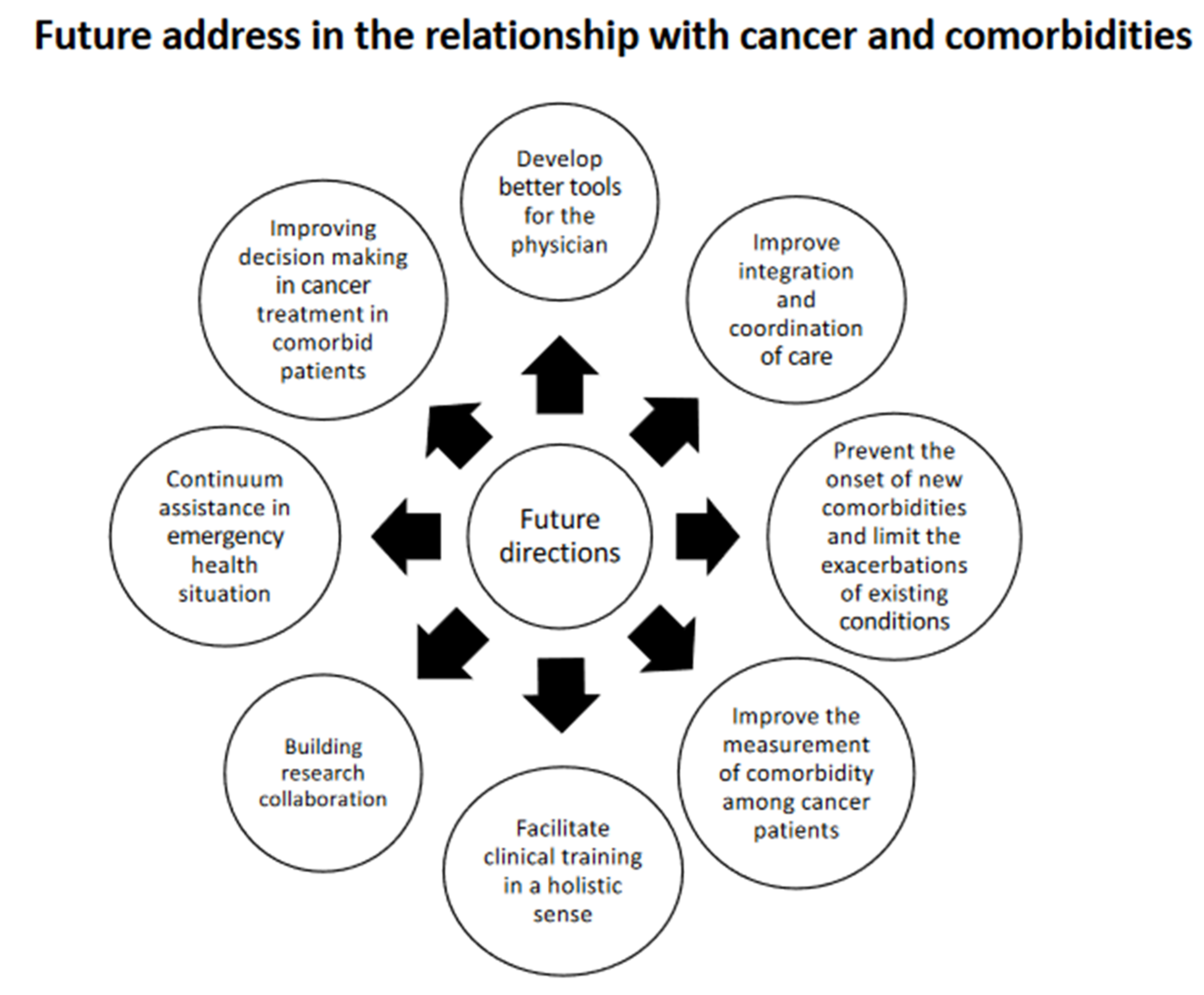
The multitude of challenges related to the coexistence of comorbidities and cancer require a multidisciplinary approach to address them with solutions ranging from clinical practice to research. Below is a list of key strategies that offer hope for progress in this area (Figure 4).
Figure 4.
Future address in the relationship with cancer and comorbidities.
5. Preventive Measures for Clustering Disease
- Improving decision making in cancer treatment in comorbid patients
We have seen how RCTs frequently exclude older patients or those with comorbidities. It is recommended that researchers evaluate interventions and technologies in at-risk populations by more closely analyzing the age distribution and health risk profile of cancer patients. Interventions by pharmaceutical companies are suggested to promote clinical trials of cancer treatments in elderly patients or patients with comorbidities [7]. Similarly, research-funding bodies may require cancer treatment studies to be carried out within these populations.
- Improve the measurement of comorbidity among cancer patients
To better understand the influence of comorbidity on efficacy in cancer treatment, the former must be measured with greater precision. First, it is necessary to recognize comorbidity as an important variable to be considered as a determinant of the success of cancer diagnosis and therapy. Second, careful consideration is required regarding how best to measure the impact of comorbidities on the overall care outcomes of cancer patients. Some guidelines are already present in the literature and should help to take measures in this direction [148,149]. The impact of comorbidities in cancer care and outcomes should be examined both from the perspective of people with cancer (such as the impact of comorbidities on survival, disability, and individual costs of care), and from the perspective of the health system (such as the overall cost of care and use of health care).
- Improve integration and coordination of care
Mismanagement of patients with multiple health problems can lead to fragmentation in care. The coordination of care has previously been identified as critical for both the effective delivery of cancer care and effective care for those with multiple chronic conditions [150,151]. It is essential to ensure that coordination and integration of care extends beyond the domain of cancer and includes all other patient needs. There are many approaches that can be helpful in improving the coordination of care for cancer patients within and outside cancer care services, including growing collaboration with primary care services, more effectively using technology, distributing health information to facilitate coordination, and sharing and promoting intervention plans [7,150,151]. It is likely that the usefulness of each model will depend on the context and setting, and in the future, more effort will be required to evaluate which models are the most useful and convenient in setting up cancer treatment. The use of comprehensive geriatric assessments in geriatric oncology provides an excellent example of integrated care. Complete geriatric assessments provide data on the patient’s functional status, comorbidity, polytherapy, the existence of geriatric syndromes, nutritional status, social support, and psychological status. Many studies show that incorporating such assessment into the care of older people with cancer can be useful in predicting complications of care, estimating mortality or survival, and assisting in the decision-making process [152,153,154,155,156,157,158,159,160,161]. More effort is needed to assess whether such wide-ranging interventions are generally beneficial (even for non-geriatric patients with comorbidities) and whether they are profitable in terms of resource optimization [162].
- Prevent the onset of new comorbidities and limit the exacerbations of existing conditions
New comorbidities can emerge during or after cancer and cancer treatment, and the latter can exacerbate the underlying circumstances. So far, most research has focused on managing comorbid conditions among cancer survivors, whereas there is very little research on the impact of careful comorbid management and polypharmacy in the patient’s active treatment phase oncology [161,162]. Furthermore, research has shown that polypharmacy and adverse drug reactions are important causes of unplanned hospitalization and higher toxicity rates [108,109,110,111]. Yet the studies that have been conducted to date are small and insufficient in terms of knowledge of the frequency, severity, and effect of drug interactions during cancer treatment. Furthermore, it would be useful to understand whether an intervention to reduce polypharmacy among cancer patients receiving chemotherapy can improve the survival of such patients [163,164,165,166,167].
- Develop better tools for clinicians
There have always been limited resources available to clinicians for managing multiple health care problems affecting patients with comorbidities or for providing accurate prognostic information regarding cancer interaction outcomes and coexisting conditions. Some decision aids have been developed in the context of geriatric oncology, including the impact of all chronic diseases on survival or life expectancy, which have proven useful in evaluating treatment decisions for people with comorbidities [168,169].
- Facilitate clinical training in a holistic sense
Today, most physician training programs focus on the development of specialists rather than focusing on knowledge and skills in a holistic sense. Specialist knowledge is clearly required in cancer management. However, current models of cancer care require new skills for health care providers, and still further efforts are needed to develop skills and capabilities among both cancer care professionals as well as those who are not directly involved in cancer care. Skills include understanding the risk, prevalence, and management of comorbidities in cancer, a but also the ability to achieve integration of care and communication between the various professionals who deal with the health of the cancer patient [170].
- Building research collaborations
Many of the proposed strategies are currently in an early stage of development and are not yet ready to be adapted to routine clinical practice. Research is needed in the field of epidemiology regarding cancer comorbidities, their mechanisms and models of care, and the execution of the latter. To truly accelerate research work in this area, it is essential that strong research collaborations be built in both medicine and the cross-disciplinary multidisciplinary field to be implemented with disciplines including epidemiology, biology, cancer medicine, population health and human research.
- Continuum of assistance in emergency health situations
Ensuring the continuum of care for cancer patients is of vital importance and is considered a top priority in this pandemic period, as many hospitals and health centres have been overwhelmed by the increase in the number of COVID-19 cases, and from the high application for unforeseen medical services for a particularly large number of cases. During the COVID-19 virus epidemic, greater use of online medical advice and telemedicine were necessary, moving treatments to the homes of cancer patients. It would have been beneficial to identify, in the oncology centres of territorial reference, the places to be reserved for the most appropriate diagnoses and treatments of critical cancer cases to minimize the exposure of patients to COVID-19. Using outpatient health facilities for the medical treatment of cancer patients and more effective screening to exclude COVID-19 infection before hospitalizing patients would have preserved the hospitals involved in the emergency by allocating local cancer centres to oncological care. Comprehensive multidisciplinary assistance, including the presence of experts in palliative and end-of-life care, would be desirable in the management of the critically ill patient in health emergencies, such as that of COVID-19. Clinical judgment is of fundamental importance in determining crucial choices, and from an ethical point of view, regarding the continuation or suspension of cancer therapy in patients with COVID-19. It would also be necessary that healthcare professionals who take care of cancer patients have greater access to professional updating of literature data, given the rapid evolution of the flow of information relating to the delicate relationship between cancer and COVID-19 to provide management based on scientific evidence on a case-by-case basis, and to address any new pandemic challenges in the future.
6. Conclusions
With a population increasingly predisposed to aging and a growing number of patients diagnosed with cancer, the management of comorbidities assumes an increasing role in modern health services. To address this growing challenge, we need to go beyond the current model that considers cancer as a single morbid condition; we need to consider cancer as part of the complexity of people’s problems and relate it to complex medical conditions. Measures should be taken to improve the measurement of comorbidities among cancer patients, decision-making regarding cancer patients, integration and coordination of care, prevention of the onset of new comorbidities by limiting exacerbations of existing conditions and ensuring the continuum of assistance in health emergency situations, focusing on holistic medicine and better collaboration between professionals of the various health systems. These considerations may constitute the foundations of a new way of meeting the needs of cancer patients.
Author Contributions
Conceptualization, P.C. and T.C.; methodology, T.C.; software, P.C.; validation, M.G., P.C. and T.C.; formal analysis, P.C.; investigation, O.P.; resources, O.P.; data curation, P.C.; writing—original draft preparation, T.C.; writing—review and editing, O.P.; visualization, O.P.; supervision, M.G.; project administration, M.G.; funding acquisition, M.G. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not Applicable.
Informed Consent Statement
Not Applicable.
Data Availability Statement
Not Applicable.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Edwards, B.K.; Noone, M.A.; Mariotto, B.A.; Simard, P.E.; Boscoe, P.F.; Henley, J.S.; Jemal, A.; Cho, H.; Anderson, N.R.; Kohler, A.; et al. Annual report to the Nation on the status of cancer, 1975–2010, featuring prevalence of comorbidity and impact on survival among persons with lung, colorectal, breast, or prostate cancer. Cancer 2014, 120, 1290–1314. [Google Scholar]
- Fane, M.; Weeraratna, A.T. How the ageing microenvironment influences tumour progression. Nat. Rev. Cancer 2020, 20, 89–106. [Google Scholar] [CrossRef] [PubMed]
- Extermann, M. Measurement and impact of comorbidity in older cancer patients. Crit. Rev. Oncol. Hematol. 2000, 35, 181–200. [Google Scholar] [CrossRef]
- Extermann, M. Measuring comorbidity in older cancer patients. Eur. J. Cancer 2000, 36, 453–471. [Google Scholar] [CrossRef]
- Satariano, W.A.; Silliman, R.A. Comorbidity: Implications for research and practice in geriatric oncology. Crit. Rev. Oncol. Hematol. 2003, 48, 239–248. [Google Scholar] [CrossRef]
- Sogaard, M.; Thomsen, R.; Bossen, K.S.; Sørensen, H.T.; Nørgaard, M. The impact of comorbidity on cancer survival: A review. Clin. Epidemiol. 2013, 5, 3–29. [Google Scholar] [CrossRef]
- Institute of Medicine. Delivering High-Quality Cancer Care: Charting a New Course for a System in Crisis; The National Academies Press: Washington, DC, USA, 2013. [Google Scholar]
- Feinstein, A. The pre-therapeutic classification of co-morbidity in chronic disease. J. Chronic. Dis. 1970, 23, 455–469. [Google Scholar] [CrossRef]
- Fried, L.P.; Ferrucci, L.; Darer, J.; Williamson, J.D.; Anderson, G. Untangling the concepts of disability, frailty, and comorbidity: Implications for improved targeting and care. J. Gerontol. A Biol. Sci. Med. Sci. 2004, 59, 255–263. [Google Scholar] [CrossRef]
- Ness, K.K.; Krull, K.R.; Jones, K.E.; Mulrooney, D.A.; Armstrong, G.T.; Green, D.M.; Chemaitilly, W.; Smith, W.A.; Wilson, C.L.; Sklar, C.A.; et al. Physiologic frailty as a sign of accelerated aging among adult survivors of childhood cancer: A report from the St Jude Lifetime cohort study. J. Clin. Oncol. 2013, 31, 4496–4503. [Google Scholar] [CrossRef]
- Lee, L.; Cheung, W.Y.; Atkinson, E.; Krzyzanowska, M.K. Impact of comorbidity on chemotherapy use and out-comes in solid tumors: A systematic review. J. Clin. Oncol. 2011, 29, 106–117. [Google Scholar] [CrossRef]
- Newschaffer, C.J.; Bush, T.L.; Penberthy, L.T. Comorbidity measurement in elderly female breast cancer patients with administrative and medical records data. J. Clin. Epidemiol. 1997, 50, 725–733. [Google Scholar] [CrossRef]
- Kieszak, S.M.; Flanders, W.D.; Kosinski, A.S.; Shipp, C.C.; Karp, H. A comparison of the Charlson comorbidity index derived from medical record data and administrative billing data. J. Clin. Epidemiol. 1999, 52, 137–142. [Google Scholar] [CrossRef]
- Malenka, D.J.; McLerran, D.; Roos, N.; Fisher, E.S.; Wennberg, J.E. Using administrative data to describe casemix: A comparison with the medical record. J. Clin. Epidemiol. 1994, 47, 1027–1032. [Google Scholar] [CrossRef]
- Romano, P.S.; Roos, L.L.; Jollis, J.G. Further evidence concerning the use of a clinical comorbidity index with ICD-9-CM administrative data. J. Clin. Epidemiol. 1993, 46, 1085–1090. [Google Scholar] [CrossRef]
- Sarfati, D.; Hill, S.; Purdie, G.; Dennett, E.; Blakely, T. How well does routine hospitalisation data capture information on comorbidity in New Zealand? N. Z. Med. J. 2010, 123, 50–61. [Google Scholar]
- Van Doorn, C.; Bogardus, S.T.; Williams, C.S.; Concato, J.; Towle, V.R.; Inouye, S.K. Risk adjustment for older hospitalized persons: A comparison of two methods of data collection for the Charlson index. J. Clin. Epidemiol. 2001, 54, 694–701. [Google Scholar] [CrossRef]
- Sarfati, D.; Tan, L.; Blakely, T.; Pearce, N. Comorbidity among patients with colon cancer in New Zealand. N. Z. Med. J. 2011, 124, 76–88. [Google Scholar]
- Centers for Disease Control and Prevention (CDC). CDC Health Disparities and Inequalities Report—United States. MMWR 2013, 62, 1–187. [Google Scholar]
- Valery, P.C.; Coory, M.; Stirling, J.; Green, A.C. Cancer diagnosis, treatment, and survival in indigenous and non-Indigenous Australians: A matched cohort study. Lancet 2006, 367, 1842–1848. [Google Scholar] [CrossRef]
- Schrijvers, C.T.; Coebergh, J.W.; van der Heijden, L.H.; Mackenbach, J.P. Socioeconomic variation in cancer survival in the southeastern Netherlands, 1980–1989. Cancer 1995, 75, 2946–2953. [Google Scholar] [CrossRef]
- Louwman, W.J.; Aarts, M.J.; Houterman, S.; van Lenthe, F.J.; Coebergh, J.W.W.; Janssen-Heijnen, M.L.G. A 50% higher prevalence of life-shortening chronic conditions among cancer patients with low socioeconomic status. Br. J. Cancer 2010, 103, 1742–1748. [Google Scholar] [CrossRef]
- Hill, S.; Sarfati, D.; Blakely, T.; Robson, B.; Purdie, G.; Chen, J.; Dennett, E.; Cormack, D.; Cunningham, R.; Dew, K.; et al. Survival disparities in Indigenous and non-Indigenous New Zealanders with colon cancer: The role of patient comorbidity, treatment and health service factors. J. Epidemiol. Community Health 2010, 64, 117–123. [Google Scholar] [CrossRef]
- Sheppard, A.J.; Chiarelli, A.M.; Marrett, L.D.; Nishri, E.D.; Trudeau, M.E. Stage at diagnosis and comorbidity influence breast cancer survival in First Nations women in Ontario, Canada. Cancer Epidemiol. Biomark. Prev. 2011, 20, 2160–2167. [Google Scholar] [CrossRef]
- Martin, J.H.; Coory, M.D.; Valery, P.C.; Green, A.C. Association of diabetes with survival among cohorts of indigenous and non-indigenous Australians with cancer. Cancer Causes Control 2009, 20, 355–360. [Google Scholar] [CrossRef]
- Putt, M.; Long, J.A.; Montagnet, C.; Silber, J.H.; Chang, V.W.; Liao, K.; Schwartz, J.S.; Pollack, C.E.; Wong, Y.U.; Armstrong, K. Racial differences in the impact of comorbidities on survival among elderly men with prostate cancer. Med. Care Res. Rev. 2009, 66, 409–435. [Google Scholar] [CrossRef]
- Allard, J.E.; Maxwell, G.L. Race disparities between black and white women in the incidence, treatment, and prognosis of endometrial cancer. Cancer Control 2009, 16, 53–56. [Google Scholar] [CrossRef]
- Braithwaite, D.; Tammemagi, C.M.; Moore, D.H.; Ozanne, E.M.; Hiatt, R.A.; Belkora, J.; West, D.W.; Satariano, W.A.; Liebman, M.; Esserman, L. Hypertension is an independent predictor of survival disparity between African-American and white breast cancer patients. Int. J. Cancer 2009, 124, 1213–1219. [Google Scholar] [CrossRef] [PubMed]
- Holmes, L., Jr.; Chan, W.; Jiang, Z.; Ward, D.; Essien, E.J.; Du, X.L. Impact of androgen deprivation therapy on racial/ethnic disparities in the survival of older men treated for locoregional prostate cancer. Cancer Control 2009, 16, 176–185. [Google Scholar] [CrossRef]
- Yang, R.; Cheung, M.C.; Byrne, M.M.; Huang, Y.; Nguyen, D.; Lally, B.E.; Koniaris, L.G. Do racial or socioeconomic disparities exist in lung cancer treatment? Cancer 2010, 116, 2437–2447. [Google Scholar] [CrossRef]
- Cook, L.S.; Nelson, H.E.; Cockburn, M.; Olson, S.H.; Muller, C.Y.; Wiggins, C.L. Comorbidities and endometrial cancer survival in Hispanics and non-Hispanic whites. Cancer Causes Control 2013, 24, 61–69. [Google Scholar] [CrossRef]
- Giovannucci, E.; Harlan, D.M.; Archer, M.C.; Bergenstal, R.M.; Gapstur, S.M.; Habel, L.A.; Pollak, M.; Regensteiner, J.G.; Yee, D. Diabetes and cancer: A consensus report. Diabetes Care 2010, 33, 1674–1685. [Google Scholar] [CrossRef] [PubMed]
- Tabares-Seisdedos, R.; Dumont, N.; Baudot, A.; Valderas, J.M.; Climent, J.; Valencia, A.; Crespo-Facorro, B.; Vieta, E.; Gómez-Beneyto, M.; Martínez, S.; et al. No paradox, no progress: Inverse cancer comorbidity in people with other complex diseases. Lancet Oncol. 2011, 12, 604–608. [Google Scholar] [CrossRef]
- Renehan, A.; Smith, U.; Kirkman, M.S. Linking diabetes and cancer: A consensus on complexity. Lancet 2010, 375, 2201–2202. [Google Scholar] [CrossRef]
- Onitilo, A.; Engel, J.; Glurich, I.; Stankowski, R.V.; Williams, G.M.; Doi, S.A. Diabetes and cancer II: Role of diabetes medications and influence of shared risk factors. Cancer Causes Control 2012, 23, 991–1008. [Google Scholar] [CrossRef] [PubMed]
- Din, F.V.N.; Theodoratou, E.; Farrington, S.M.; Tenesa, A.; Barnetson, R.A.; Cetnarskyj, R.; Stark, L.; Porteous, M.E.; Campbell, H.; Dunlop, M.G. Effect of aspirin and NSAIDs on risk and survival from colorectal cancer. Gut 2010, 59, 1670–1679. [Google Scholar] [CrossRef]
- Flossmann, E.; Rothwell, P.M.; British Doctors Aspirin Trial and the UK-TIA Aspirin Trial. Effect of aspirin on long-term risk of colorectal cancer: Consistent evidence from randomised and observational studies. Lancet 2007, 369, 1603–1613. [Google Scholar] [CrossRef]
- Roe, C.M.; Fitzpatrick, A.L.; Xiong, C.; Sieh, W.; Kuller, L.; Miller, J.P.; Williams, M.M.; Kopan, R.; Behrens, M.I.; Morris, J.C. Cancer linked to Alzheimer disease but not vascular dementia. Neurology 2010, 74, 106–112. [Google Scholar] [CrossRef]
- West, A.B.; Dawson, V.L.; Dawson, T.M. To die or grow: Parkinson’s disease and cancer. Trends Neurosci. 2005, 28, 348–352. [Google Scholar] [CrossRef]
- Walter, L.C.; Bertenthal, D.; Lindquist, K.; Konety, B.R. PSA screening among elderly men with limited life expectancies. JAMA 2006, 296, 2336–2342. [Google Scholar] [CrossRef]
- Taneja, S.; Mandayam, S.; Kayani, Z.Z.; Kuo, Y.; Shahinian, V.B. Comparison of stage at diagnosis of cancer in patients who are on dialysis versus the general population. Clin. J. Am. Soc. Nephrol. 2007, 2, 1008–1013. [Google Scholar] [CrossRef]
- Fleming, S.T.; Pursley, H.G.; Newman, B.; Pavlov, D.; Chen, K. Comorbidity as a predictor of stage of illness for patients with breast cancer. Med. Care 2005, 43, 132–140. [Google Scholar] [CrossRef]
- Terret, C.; Castel-Kremer, E.; Albrand, G.; Droz, J.P. Effects of comorbidity on screening and early diagnosis of cancer in elderly people. Lancet Oncol. 2009, 10, 80–87. [Google Scholar] [CrossRef]
- Corkum, M.; Urquhart, R.; Kendell, C.; Burge, F.; Porter, G.; Johnston, G. Impact of co- morbidity and healthcare utilization on colorectal cancer stage at diagnosis: Literature review. Cancer Causes Control 2012, 23, 213–220. [Google Scholar] [CrossRef]
- Satariano, W.A.; Ragland, D.R. The effect of comorbidity on 3-year survival of women with primary breast cancer. Ann. Intern. Med. 1994, 120, 104–110. [Google Scholar] [CrossRef]
- Seok-Jun, Y.; Eun-Jung, K.; Hyun-Ju, S.; In-Hwan, O. The Association between Charlson Comorbidity Index and the Medical Care Cost of Cancer: A Retrospective Study. BioMed Res. Int. 2015, 2015, 259341. [Google Scholar] [CrossRef]
- Ng, H.S.; Roder, D.; Koczwara, B.; Vitry, A. Comorbidity, physical and mental health among cancer patients and survivors: An Australian population-based study. Asia-Pac. J. Clin. Oncol. 2018, 14, e181–e192. [Google Scholar] [CrossRef]
- Vaeth, P.A.; Satariano, W.A.; Ragland, D.R. Limiting comorbid conditions and breast cancer stage at diagnosis. J. Gerontol. A Biol. Sci. Med. Sci. 2000, 55, M593–M600. [Google Scholar] [CrossRef]
- Gross, C.P.; Andersen, M.S.; Krumholz, H.M.; McAvay, G.J.; Proctor, D.; Tinetti, M.E. Relation between Medicare screening reimbursement and stage at diagnosis for older patients with colon cancer. JAMA 2006, 296, 2815–2822. [Google Scholar]
- Reid, B.C.; Warren, J.L.; Rozier, G. Comorbidity and early diagnosis of head and neck cancer in a Medicare population. Am. J. Prev. Med. 2004, 27, 373–378. [Google Scholar] [CrossRef]
- Walter, L.C.; Lindquist, K.; Nugent, S.; Schult, T.; Lee, S.J.; Casadei, M.A.; Partin, M.R. Impact of age and comorbidity on colorectal cancer screening among older veterans. Ann. Intern. Med. 2009, 150, 465–473. [Google Scholar]
- Fleming, S.T.; McDavid, K.; Pearce, K.; Pavlov, D. Comorbidities and the risk of late-stage prostate cancer. Sci. World J. 2006, 6, 2460–2470. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yasmeen, S.; Chlebowski, R.T.; Xing, G.; Morris, C.R.; Romano, P.S. Severity of comorbid conditions and early-stage breast cancer therapy: Linked SEER-Medicare data from 1993 to 2005. Cancer Med. 2013, 2, 526–536. [Google Scholar] [CrossRef] [PubMed]
- Gurney, J.; Sarfati, D.; Stanley, J. The impact of patient co- morbidity on cancer stage at diagnosis. Br. J. Cancer 2015, 113, 1375–1380. [Google Scholar] [CrossRef] [PubMed]
- Siddiqui, A.A.; Spechler, S.J.; Huerta, S.; Dredar, S.; Little, B.B.; Cryer, B. Elevated HbA1c is an independent predictor of aggressive clinical behaviour in patients with colorectal cancer: A case-control study. Dig. Dis. Sci. 2008, 53, 2486–2494. [Google Scholar] [CrossRef]
- Zafar, S.Y.; Abernethy, A.P.; Abbott, D.H.; Grambow, S.C.; Marcello, J.E.; Herndon, J.E., 2nd; Rowe, K.L.; Kolimaga, J.T.; Zullig, L.L.; Patwardhan, M.B.; et al. Comorbidity, age, race and stage at diagnosis in colorectal cancer: A retrospective, parallel analysis of two health systems. BMC Cancer 2008, 8, 345. [Google Scholar] [CrossRef]
- Fisher, D.A.; Judd, L.; Sanford, N.S. Inappropriate colorectal cancer screening: Findings and implications. Am. J. Gastroenterol. 2005, 100, 2526–2530. [Google Scholar] [CrossRef]
- McBean, A.M.; Yu, X. The underuse of screening services among elderly women with diabetes. Diabetes Care 2007, 30, 1466–1472. [Google Scholar] [CrossRef]
- Kiefe, C.I.; Funkhouser, E.; Fouad, M.N.; May, D.S. Chronic disease as a barrier to breast and cervical cancer screening. J. Gen. Intern. Med. 1998, 13, 357–365. [Google Scholar] [CrossRef]
- Gross, C.P.; McAvay, G.J.; Krumholz, H.M.; Paltiel, A.D.; Bhasin, D.; Tinetti, M.E. The effect of age and chronic illness on life expectancy after a diagnosis of colorectal cancer: Implications for screening. Ann. Intern. Med. 2006, 145, 646–653. [Google Scholar] [CrossRef]
- Schonberg, M.A.; McCarthy, E.P.; Davis, R.B.; Phillips, R.S.; Hamel, M.B. Breast cancer screening in women aged 80 and older: Results from a national survey. J. Am. Geriatr. Soc. 2004, 52, 1688–1695. [Google Scholar] [CrossRef]
- Koppie, T.M.; Serio, A.M.; Vickers, A.J.; Vora, K.; Dalbagni, G.; Donat, S.M.; Herr, H.W.; Bochner, B.H. Age-adjusted Charlson comorbidity score is associated with treatment decisions and clinical outcomes for patients undergoing radical cystectomy for bladder cancer. Cancer 2008, 112, 2384–2392. [Google Scholar] [CrossRef]
- Blanco, J.A.; Toste, I.S.; Alvarez, R.F.; Cuadrado, G.R.; Gonzalvez, A.M.; Martín, I.J.G. Age, comorbidity, treatment decision and prognosis in lung cancer. Age Ageing 2008, 37, 715–718. [Google Scholar] [CrossRef]
- Etzioni, D.A.; El-Khoueiry, A.B.; Beart, R.W. Rates and predictors of chemotherapy use for stage III colon cancer. Cancer 2008, 113, 3279–3289. [Google Scholar] [CrossRef]
- Hall, W.H.; Jani, A.B.; Ryu, J.K.; Narayan, S.; Vijayakumar, S. The impact of age and comorbidity on survival outcomes and treatment patterns in prostate cancer. Prostate Cancer Prostatic Dis. 2005, 8, 22–30. [Google Scholar] [CrossRef]
- Janssen-Heijnen, M.L.; Houterman, S.; Lemmens, V.E.; Louwman, M.W.J.; Maas, H.A.A.M.; Coebergh, J.W. Prognostic impact of increasing age and co-morbidity in cancer patients: A population-based approach. Crit. Rev. Oncol. Hematol. 2005, 55, 231–240. [Google Scholar] [CrossRef]
- Van der Aa, M.A.; Siesling, S.; Kruitwagen, R.F.; Lybeert, M.L.M.; Coebergh, J.W.W.; Janssen-Heijnen, M.L.G. Comorbidity and age affect treatment policy for cervical cancer: A population-based study in the south of The Netherlands, 1995–2004. Eur. J. Gynaecol. Oncol. 2008, 29, 493–498. [Google Scholar]
- Land, L.H.; Dalton, S.O.; Jensen, M.B.; Ewertz, M. Influence of comorbidity on the effect of adjuvant treatment and age in patients with early-stage breast cancer. Br. J. Cancer 2012, 107, 1901–1907. [Google Scholar] [CrossRef]
- Rodrigues, G.; Sanatani, M. Age and comorbidity considerations related to radiotherapy and chemotherapy administration. Semin. Radiat. Oncol 2012, 22, 277–283. [Google Scholar] [CrossRef]
- Sarfati, D.; Gurney, J.; Stanley, J.; Koea, J. A retrospective cohort study of patients with stomach and liver cancers: The impact of comorbidity and ethnicity on cancer care and outcomes. BMC Cancer 2014, 14, 821. [Google Scholar] [CrossRef]
- Cronin, D.P.; Harlan, L.C.; Potosky, A.L.; Clegg, L.X.; Stevens, J.L.; Mooney, M.M. Patterns of care for adjuvant therapy in a random population-based sample of patients diagnosed with colorectal cancer. Am. J. Gastroenterol. 2006, 101, 2308–2318. [Google Scholar] [CrossRef]
- Gross, C.P.; McAvay, G.J.; Guo, Z.; Tinetti, M.E. The impact of chronic illnesses on the use and effectiveness of adjuvant chemotherapy for colon cancer. Cancer 2007, 109, 2410–2419. [Google Scholar] [CrossRef]
- Lemmens, V.E.; Janssen-Heijnen, M.L.; Verheij, C.D.; Houterman, S.; van Driel, O.J.R.; Coebergh, J.W.W. Comorbidity leads to altered treatment and worse survival of elderly patients with colorectal cancer. Br. J. Surg. 2005, 92, 615–623. [Google Scholar] [CrossRef]
- Sarfati, D.; Hill, S.; Blakely, T.; Robson, B.; Purdie, G.; Dennett, E.; Cormack, D.; Dew, K. The effect of comorbidity on the use of adjuvant chemotherapy and survival from colon cancer: A retrospective cohort study. BMC Cancer 2009, 9, 116. [Google Scholar] [CrossRef]
- Khrizman, P.; Niland, J.C.; Ter Veer, A.; Milne, D.; Dunn, K.B.; William, E.C., 3rd; Engstrom, P.F.; Shibata, S.; Skibber, J.M.; Weiser, M.R.; et al. Postoperative adjuvant chemotherapy use in patients with stage II/III rectal cancer treated with neoadjuvant therapy: A National Comprehensive Cancer Network analysis. J. Clin. Oncol. 2013, 31, 30–38. [Google Scholar] [CrossRef]
- Iversen, L.H.; Norgaard, M.; Jacobsen, J.; Laurberg, S.; Sørensen, H.T. The impact of comorbidity on survival of Danish colorectal cancer patients from 1995 to 2006—A population-based cohort study. Dis. Colon Rectum 2009, 52, 71–78. [Google Scholar] [CrossRef]
- Zhang, W.; Ayanian, J.Z.; Zaslavsky, A.M. Patient characteristics and hospital quality for colorectal cancer surgery. Int. J. Qual. Health Care 2007, 19, 11–20. [Google Scholar] [CrossRef]
- Bradley, C.J.; Dahman, B.; Anscher, M. Prostate cancer treatment and survival: Evidence for men with prevalent comorbid conditions. Med. Care 2014, 52, 482–489. [Google Scholar] [CrossRef] [PubMed]
- Keating, N.L.; Landrum, M.B.; Klabunde, C.N.; Fletcher, R.H.; Rogers, S.O.; Doucette, W.R.; Tisnado, D.; Clauser, S.; Kahn, K.L. Adjuvant chemotherapy for stage III colon cancer: Do physicians agree about the importance of patient age and comorbidity? J. Clin. Oncol. 2008, 26, 2532–2537. [Google Scholar] [CrossRef] [PubMed]
- Krzyzanowska, M.K.; Regan, M.M.; Powell, M.; Earle, C.C.; Weeks, J.C. Impact of patient age and comorbidity on surgeon versus oncologist preferences for adjuvant chemotherapy for stage III colon cancer. J. Am. Coll. Surg. 2009, 208, 202–209. [Google Scholar] [CrossRef] [PubMed]
- Ring, A. The influences of age and co-morbidities on treatment decisions for patients with HEr2-positive early breast cancer. Crit. Rev. Oncol. Hematol. 2010, 76, 127–132. [Google Scholar] [CrossRef]
- Stairmand, J.; Signal, L.; Sarfati, D.; Jackson, C.; Batten, L.; Holdaway, M.; Cunningham, C. Consideration of comorbidity in treatment decision-making in multidisciplinary cancer team meetings: A systematic review. Ann. Oncol. 2015, 26, 1325–1332. [Google Scholar] [CrossRef]
- Schrag, D.; Cramer, L.D.; Bach, P.B.; Begg, C.B. Age and adjuvant chemotherapy use after surgery for stage III colon cancer. J. Natl. Cancer Inst. 2001, 93, 850–857. [Google Scholar] [CrossRef]
- Kutner, J.S.; Vu, K.O.; Prindiville, S.A.; Byers, T.E. Patient age and cancer treatment decisions. Patient and physician views. Cancer Pract. 2000, 8, 114–119. [Google Scholar] [CrossRef]
- Newcomb, P.A.; Carbone, P.P. Cancer treatment and age: Patient perspectives. J. Natl. Cancer Inst. 1993, 85, 1580–1584. [Google Scholar] [CrossRef]
- El Shayeb, M.; Scarfe, A.; Yasui, Y.; Winget, M. Reasons physicians do not recommend, and patients refuse adjuvant chemotherapy for stage III colon cancer: A population-based chart review. BMC Res. Notes 2012, 5, 269. [Google Scholar] [CrossRef]
- Fortin, M.; Dionne, J.; Pinho, G.; Gignac, J.; Almirall, J.; Lapointe, L. Randomized controlled trials: Do they have external validity for patients with multiple comorbidities? Ann. Fam. Med. 2006, 4, 104–108. [Google Scholar] [CrossRef]
- Lewis, J.H.; Kilgore, M.L.; Goldman, D.P.; Trimble, E.L.; Kaplan, R.; Montello, M.J.; Housman, M.G.; Escarce, J.J. Participation of patients 65 years of age or older in cancer clinical trials. J. Clin. Oncol. 2003, 21, 1383–1389. [Google Scholar] [CrossRef]
- Meyerhardt, J.A.; Catalano, P.J.; Haller, D.G.; Mayer, R.J.; Macdonald, J.S.; 3rd Benson, A.B.; Fuchs, C.S. Impact of diabetes mellitus on outcomes in patients with colon cancer. J. Clin. Oncol. 2003, 21, 433–440. [Google Scholar] [CrossRef]
- Gronberg, B.H.; Sundstrom, S.; Kaasa, S.; Bremnes, R.M.; Fløtten, Ø.; Amundsen, T.; Hjelde, H.H.; von Plessen, C.; Jordhøy, M. Influence of comorbidity on survival, toxicity and health-related quality of life in patients with advanced non-small-cell lung cancer receiving platinum-doublet chemotherapy. Eur. J. Cancer 2010, 46, 2225–2234. [Google Scholar] [CrossRef]
- Lemmens, V.E.; Janssen-Heijnen, M.L.; Houterman, S.; Verheij, K.D.G.W.; Martijn, H.; van de Poll-Franse, L.; Coebergh, J.W. Which comorbid conditions predict complications after surgery for colorectal cancer? World J. Surg. 2007, 31, 192–199. [Google Scholar] [CrossRef]
- Peters, T.T.; Van der Laan, B.F.; Plaat, B.E.; Wedman, J.; Langendijk, J.A.; Halmos, G.B. The impact of comorbidity on treatment-related side effects in older patients with laryngeal cancer. Oral Oncol. 2011, 47, 56–61. [Google Scholar] [CrossRef] [PubMed]
- Seymour, M.T.; Thompson, L.C.; Wasan, H.S.; Middleton, G.; Brewster, A.E.; Shepherd, S.F.; O’Mahony, M.S.; Maughan, T.S.; Parmar, M.; Langley, R.E. Chemotherapy options in elderly and frail patients with metastatic colorectal cancer (MRC FOCUS2): An open- label, randomised factorial trial. Lancet 2011, 377, 1749–1759. [Google Scholar] [CrossRef]
- Lo Conte, N.K.; Smith, M.; Alberti, D.; Bozeman, J.; Cleary, J.F.; Setala, A.N.; Wodtke, G.; Wilding, G.; Holen, K.D. Amongst eligible patients, age and comorbidity do not predict for dose-limiting toxicity from phase I chemotherapy. Cancer Chemother. Pharmacol. 2010, 65, 775–780. [Google Scholar] [CrossRef] [PubMed]
- Yusuf, S.W. Chemotherapy for older patients with colorectal cancer. Lancet 2011, 378, 765, author reply 765–766. [Google Scholar] [CrossRef]
- Vickers, M.M.; Powell, E.D.; Asmis, T.R.; Jonker, D.J.; Hilton, J.F.; O’Callaghan, C.J.; Tu, D.; Parulekar, W.; Jonker, M.J.M.D.J.; Hilton, J.F.; et al. Comorbidity, age and overall survival in patients with advanced pancreatic cancer—Results from NCIC CTG PA.3, a phase III trial of gemcitabine plus erlotinib or placebo. Eur. J. Cancer 2012, 48, 1434–1442. [Google Scholar] [CrossRef]
- Rieker, R.J.; Hammer, E.; Eisele, R.; Schmid, E.; Högel, J. The impact of comorbidity on the overall survival and the cause of death in patients after colorectal cancer resection. Langenbeck’s Arch. Surg. 2002, 387, 72–76. [Google Scholar] [CrossRef]
- Dehal, A.; Abbas, A.; Johna, S. Comorbidity and outcomes after surgery among women with breast cancer: Analysis of nationwide in-patient sample database. Breast Cancer Res. Treat. 2013, 139, 469–476. [Google Scholar] [CrossRef]
- Van Gestel, Y.R.; Lemmens, V.E.; de Hingh, I.H.; Steevens, J.; Rutten, H.J.T.; Nieuwenhuijzen, G.A.P.; van Dam, R.M.; Siersema, P.D. Influence of comorbidity and age on 1-, 2-and 3-month postoperative mortality rates in gastrointestinal cancer patients. Ann. Surg. Oncol. 2013, 20, 371–380. [Google Scholar] [CrossRef]
- Tomaszewski, J.J.; Uzzo, R.G.; Kutikov, A.; Hrebinko, K.; Mehrazin, R.; Corcoran, A.; Ginzburg, S.; Viterbo, R.; Chen, D.Y.T.; Greenberg, R.E.; et al. Assessing the burden of complications after surgery for clinically localized kidney cancer by age and comorbidity status. Urology 2014, 83, 843–849. [Google Scholar] [CrossRef]
- Jehn, C.F.; Boning, L.; Kroning, H.; Pezzutto, A.; Lüftner, D. Influence of co- morbidity, age and performance status on treatment efficacy and safety of cetuximab plus irinotecan in irinotecan-refractory elderly patients with metastatic colorectal cancer. Eur. J. Cancer 2014, 50, 1269–1275. [Google Scholar] [CrossRef]
- Abdollah, F.; Sun, M.; Schmitges, J.; Thuret, R.; Bianchi, M.; Shariat, S.F.; Briganti, A.; Jeldres, C.; Perrotte, P.; Montorsi, F.; et al. Survival benefit of radical prostatectomy in patients with localized prostate cancer: Estimations of the number needed to treat according to tumour and patient characteristics. J. Urol. 2012, 188, 73–83. [Google Scholar] [CrossRef]
- Earle, C.C.; Tsai, J.S.; Gelber, R.D.; Weinstein, M.C.; Neumann, P.J.; Weeks, J.C. Effectiveness of chemotherapy for advanced lung cancer in the elderly: Instrumental variable and propensity analysis. J. Clin. Oncol. 2001, 19, 1064–1070. [Google Scholar] [CrossRef]
- Rosenbaum, P.; Rubin, D. Reducing bias in observational studies using subclassification on the propensity score. J. Am. Stat. Assoc. 1984, 79, 516–524. [Google Scholar] [CrossRef]
- Riechelmann, R.P.; Del Giglio, A. Drug interactions in oncology: How common are they? Ann. Oncol. 2009, 20, 1907–1912. [Google Scholar] [CrossRef]
- Beijnen, J.H.; Schellens, J.H. Drug interactions in oncology. Lancet Oncol. 2004, 5, 489–496. [Google Scholar] [CrossRef]
- Blower, P.; de Wit, R.; Goodin, S.; Aapro, M. Drug-drug interactions in oncology: Why are they important and can they be minimized? Crit. Rev. Oncol. Hematol. 2005, 55, 117–142. [Google Scholar] [CrossRef]
- Riechelmann, R.P.; Tannock, I.F.; Wang, L.; Saad, E.D.; Taback, N.A.; Krzyzanowska, M.K. Potential drug interactions and duplicate prescriptions among cancer patients. J. Natl. Cancer Inst. 2007, 99, 592–600. [Google Scholar] [CrossRef]
- Riechelmann, R.P.; Zimmermann, C.; Chin, S.N.; Wang, L.; O’Carroll, A.; Zarinehbaf, S.; Krzyzanowska, M.K. Potential drug interactions in cancer patients receiving supportive care exclusively. J. Pain Symptom Manag. 2008, 35, 535–543. [Google Scholar] [CrossRef]
- Miranda, V.; Fede, A.; Nobuo, M.; Ayres, V.; Giglio, A.; Miranda, M.; Riechelmann, R.P. Adverse drug re- actions and drug interactions as causes of hospital ad- mission in oncology. J. Pain Symptom Manag. 2011, 42, 342–353. [Google Scholar] [CrossRef]
- Sasaki, T.; Fujita, K.; Sunakawa, Y.; Ishida, H.; Yamashita, K.; Miwa, K.; Saji, S.; Kato, Y.; Sasaki, Y. Concomitant polypharmacy is associated with irinotecan-related ad- verse drug reactions in patients with cancer. Int. J. Clin. Oncol. 2013, 18, 735–742. [Google Scholar] [CrossRef]
- Boulos, D.L.; Groome, P.A.; Brundage, M.D.; Siemens, D.R.; Mackillop, W.J.; Heaton, J.P.W.; Schulze, K.M.; Rohland, S.L. Predictive validity of five comorbidity indices in prostate carcinoma patients treated with curative intent. Cancer 2006, 106, 1804–1814. [Google Scholar] [CrossRef]
- Kendal, W.S. Dying with cancer: The influence of age, comorbidity, and cancer site. Cancer 2008, 112, 1354–1362. [Google Scholar] [CrossRef]
- Piccirillo, J.F.; Costas, I.; Claybour, P.; Siemens, D.R.; Mackillop, W.J.; Heaton, J.P.W.; Schulze, K.M.; Siemens, S.L.R.D.R.; Mackillop, W.J.; Heaton, J.P.W.; et al. The measurement of comorbidity by cancer registries. J. Regist. Manag. 2003, 30, 8–14. [Google Scholar]
- Piccirillo, J.F.; Tierney, R.M.; Costas, I.; Grove, L.; Jr, E.L.S. Prognostic importance of comorbidity in a hospital-based cancer registry. JAMA 2004, 291, 2441–2447. [Google Scholar] [CrossRef]
- Read, W.L.; Tierney, R.M.; Page, N.C.; Costas, I.; Govindan, R.; Spitznagel, E.L.J.; Piccirillo, J.F. Differential prognostic impact of comorbidity. J. Clin. Oncol. 2004, 22, 3099–3103. [Google Scholar] [CrossRef]
- Sarfati, D.; Blakely, T.; Pearce, N. Measuring cancer survival in populations: Relative survival versus cancer specific survival. Int. J. Epidemiol. 2010, 39, 598–610. [Google Scholar] [CrossRef]
- Kiderlen, M.; de Glas, N.A.; Bastiaannet, E.; Engels, C.C.; van de Water, W.; de Craen, A.J.M.; Portielje, J.E.A.; van de Velde, C.J.H.; Liefers, G.J. Diabetes in relation to breast cancer relapse and all-cause mortality in elderly breast cancer patients: A FOCUS study analysis. Ann. Oncol. 2013, 24, 3011–3016. [Google Scholar] [CrossRef]
- Fortin, M.; Bravo, G.; Hudon, C.; Lapointe, L.; Almirall, J.; Dubois, M.-F.; Vanass, A. Relationship between multimorbidity and health-related quality of life of patients in primary care. Qual. Life Res. 2006, 15, 83–91. [Google Scholar] [PubMed]
- Fortin, M.; Lapointe, L.; Hudon, C.; Vanasse, A.; Ntetu, A.L.; Maltais, D. Multimorbidity and quality of life in primary care: A systematic review. Health Qual. Life Outcomes 2004, 2, 51. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, B.; Ou, H.; Wang, F.; Erickson, S. A new co- morbidity index: The health-related quality of life comorbidity index. J. Clin. Epidemiol. 2011, 64, 309–319. [Google Scholar] [PubMed]
- McDaid, O.; Hanly, M.J.; Richardson, K.; Kee, F.; Kenny, R.A.; Savva, G.M. The effect of multiple chronic conditions on self-rated health, disability and quality of life among the older populations of Northern Ireland and the republic of Ireland: A comparison of two nationally representative cross-sectional surveys. BMJ Open 2013, 3, e002571. [Google Scholar] [CrossRef]
- Daskivich, T.J.; van de Poll-Franse, L.V.; Kwan, L.; Sadetsky, N.; Stein, D.M.; Litwin, M.S. From bad to worse: Comorbidity severity and quality of life after treatment for early-stage prostate cancer. Prostate Cancer Prostatic Dis. 2010, 13, 320–327. [Google Scholar] [CrossRef][Green Version]
- Litwin, M.S.; Greenfield, S.; Elkin, E.P.; Lubeck, D.P.; Broering, J.M.; Kaplan, S.H. Assessment of prognosis with the total illness burden index for prostate cancer: Aiding clinicians in treatment choice. Cancer 2007, 109, 1777–1783. [Google Scholar] [CrossRef]
- Osthus, A.A.; Aarstad, A.K.; Olofsson, J.; Aarstad, H.J. Co- morbidity is an independent predictor of health-related quality of life in a longitudinal cohort of head and neck cancer patients. Eur. Arch. Otorhinolaryngol. 2013, 270, 1721–1728. [Google Scholar] [CrossRef]
- Schubert-Fritschle, G.; Schlesinger-Raab, A.; Hein, R.; Stolz, W.; Volkenandt, M.; Hölzel, D.; Engel, J. Quality of life and comorbidity in localized malignant melanoma: Results of a German population-based cohort study. Int. J. Dermatol. 2013, 52, 693–704. [Google Scholar] [CrossRef]
- Schafer, I.; Hansen, H.; Schon, G.; Höfels, S.; Altiner, A.; Dahlhaus, A.; Gensichen, J.; Riedel-Heller, S.; Weyerer, S.; Blank, W.A. The influence of age, gender and socio-economic status on multimorbidity patterns in primary care. First results from the Multicare Cohort Study. BMC Health Serv. Res. 2012, 12, 89. [Google Scholar] [CrossRef]
- Haugnes, H.S.; Aass, N.; Fossa, S.D.; Dahl, O.; Klepp, O.; Wist, E.A.; Svartberg, J.; Wilsgaard, T.; Bremnes, R.M. Components of the metabolic syndrome in long-term survivors of testicular cancer. Ann. Oncol. 2007, 18, 241–248. [Google Scholar] [CrossRef]
- Smith, L.A.; Cornelius, V.R.; Plummer, C.J.; Levitt, G.; Verrill, M.; Canney, P.; Jones, A. Cardiotoxicity of anthracycline agents for the treatment of cancer: Systematic review and meta-analysis of randomised controlled trials. BMC Cancer 2010, 10, 337. [Google Scholar] [CrossRef]
- Carver, J.R.; Shapiro, C.L.; Ng, A.; Jacobs, L.; Schwartz, C.; Virgo, K.S.; Hagerty, K.L.; Somerfield, M.R.; Vaughn, D.J. American Society of Clinical Oncology clinical evidence review on the on- going care of adult cancer survivors: Cardiac and pulmonary late effects. J. Clin. Oncol. 2007, 25, 3991–4008. [Google Scholar] [CrossRef]
- Patnaik, J.L.; Byers, T.; Di Giuseppi, C.; Dabelea, D.; Denberg, T.D. Cardiovascular disease competes with breast cancer as the leading cause of death for older females diagnosed with breast cancer: A retrospective cohort study. Breast Cancer Res. 2011, 13, R64. [Google Scholar] [CrossRef]
- Lustberg, M.B.; Reinbolt, R.E.; Shapiro, C.L. Bone health in adult cancer survivorship. J. Clin. Oncol. 2012, 30, 3665–3674. [Google Scholar] [CrossRef]
- Wickham, R. Osteoporosis related to disease or therapy in patients with cancer. Clin. J. Oncol. Nurs. 2011, 15, E90–E104. [Google Scholar] [CrossRef]
- Dai, M.; Liu, D.; Liu, M.; Zhou, F.; Li, G.; Chen, Z.; Zhou, F.; Li, G.; Chen, Z.; Zhang, Z.; et al. Patients with Cancer Appear More Vulnerable to SARS-CoV-2: A Multicenter Study during the COVID-19 Outbreak. Cancer Discov. 2020, 10, 783–791. [Google Scholar] [CrossRef]
- Rogado, J.; Pangua, C.; Serrano-Montero, G.; Obispo, B.; Marino, A.M.; Perez-Perez, M.; López-Alfonso, A.; Gullón, M.; Lara, M.Á. COIVD-19 and lung cancer: A greater fatality rate? Lung Cancer 2020, 146, 19–22. [Google Scholar] [CrossRef]
- Kuderer, N.M.; Choueiri, T.K.; Shah, D.P.; Shyr, Y.; Rubinstein, S.M.; Rivera, D.R.; Shete, S.; Hsu, C.-Y.; Desai, A.; de Lima Lopes, G.; et al. Clinical impact of COVID-19 on patients with cancer (CCC19): A cohort study. Lancet 2020, 395, 1907–1918. [Google Scholar] [CrossRef]
- Liang, W.; Guan, W.; Chen, R.; Wang, W.; Li, J.; Xu, K.; Li, C.; Ai, Q.; Lu, W.; Liang, H. Cancer patients in SARS-CoV-2 infection: A nationwide analysis in China. Lancet Oncol. 2020, 21, 335–337. [Google Scholar] [CrossRef]
- Mehta, V.; Goel, S.; Kabarriti, R.; Cole, D.; Goldfinger, M.; Acuna-Villaorduna, A.; Pradhan, K.; Thota, R.; Reissman, S.; Sparano, J.A. Case Fatality Rate of Cancer Patients with COVID-19 in a New York Hospital System. Cancer Discov. 2020, 10, 935–941. [Google Scholar] [CrossRef] [PubMed]
- Lara Alvarez, M.A.; Rogado Revuelta, J.; Obispo Portero, B.; Pangua Mendez, C.; Serrano Montero, G.; Lopez Alfonso, A. COVID-19 mortality in cancer patients in a Madrid hospital during the first 3 weeks of the epidemic. Med. Clin. 2020, 155, 202–204. [Google Scholar] [CrossRef] [PubMed]
- Rugge, M.; Zorzi, M.; Guzzinati, S. SARS-CoV-2 infection in the Italian Veneto region: Adverse outcomes in patients with cancer. Nat. Cancer 2020, 1, 784–788. [Google Scholar] [CrossRef] [PubMed]
- Luo, J.; Rizvi, H.; Preeshagul, I.R.; Egger, J.V.; Hoyos, D.; Bandlamudi, C.; McCarthy, C.G.; Falcon, C.J.; Schoenfeld, A.J.; Arbour, K.C.; et al. COVID-19 in patients with lung cancer. Ann. Oncol. Off. J. Eur. Soc. Med. Oncol. 2020, 31, 1386–1396. [Google Scholar] [CrossRef] [PubMed]
- Garassino, M.C.; Whisenant, J.G.; Huang, L.C.; Trama, A.; Torri, V.; Agustoni, F.; Baena, J.; Banna, G.; Berardi, R.; Bettini, A.C. COVID-19 in patients with thoracic malignancies (TERAVOLT): First results of an international, registry-based, cohort study. Lancet Oncol. 2020, 21, 914–922. [Google Scholar] [CrossRef]
- Passamonti, F.; Cattaneo, C.; Arcaini, L.; Bruna, R.; Cavo, M.; Merli, F.; Angelucci, E.; Krampera, M.; Cairoli, R.; Della Porta, M.G.; et al. Clinical characteristics and risk factors associated with COVID-19 severity in patients with haematological malignancies in Italy: A retrospective, multicentre, cohort study. Lancet Haematol. 2020, 7, e737–e745. [Google Scholar] [CrossRef]
- Sanchez-Pina, J.M.; Rodriguez Rodriguez, M.; Castro Quismondo, N.; Manso, G.; Colmenares, R.; Alos, D.G.; Paciello, M.L.; Zafra, D.; Garcia-Sanchez, C.; Villegas, C. Clinical course and risk factors for mortality from COVID-19 in patients with haematological malignancies. Eur. J. Haematol. 2020, 105, 597–607. [Google Scholar] [CrossRef]
- Zhang, L.; Zhu, F.; Xie, L.; Wang, C.; Chen, R.; Guan, H.Q.; Peng, L.; Chen, Y. Clinical characteristics of COVID-19-infected cancer patients: A retrospective case study in three hospitals within Wuhan, China. Ann. Oncol. Off. J. Eur. Soc. Med. Oncol. 2020, 31, 894–901. [Google Scholar] [CrossRef]
- Wang, H.; Zhang, L. Risk of COVID-19 for patients with cancer. Lancet Oncol. 2020, 21, E181. [Google Scholar] [CrossRef]
- Ueda, M.; Martins, R.; Hendrie, P.C.; McDonnell, T.; Crews, J.R.; Wong, T.L.; McCreery, B.; Jagels, B.; Crane, A. Managing cancer care during the COVID-19 pandemic: Agility and collaboration toward a common goal. J. Natl. Compr. Cancer Netw. 2020, 18, 366–369. [Google Scholar] [CrossRef]
- Sarfati, D. review of methods to measure comorbidity in cancer populations: No gold standard exists. J. Clin. Epidemiol. 2012, 65, 924–933. [Google Scholar] [CrossRef]
- Hall, S.F. A user’s guide to selecting a comorbidity index for clinical research. J. Clin. Epidemiol. 2006, 59, 849–855. [Google Scholar] [CrossRef]
- Walsh, J.; Harrison, J.D.; Young, J.M.; Butow, P.N.; Solomon, M.J.; Masya, L. What are the current barriers to effective cancer care coordination? A qualitative study. BMC Health Serv. Res. 2010, 10, 132. [Google Scholar] [CrossRef]
- US Department of Health and Human Services. Multiple Chronic Conditions—A Strategic Framework: Optimum Health and Quality of Life for Individuals with Multiple Chronic Conditions; US Department of Health and Human Services: Washington, DC, USA, 2010.
- Institute of Medicine. Living Well with Chronic Illness: A Call for Public Health Action; The National Academies Press: Washington, DC, USA, 2012. [Google Scholar]
- Caillet, P.; Canoui-Poitrine, F.; Vouriot, J.; Berle, M.; Reinald, N.; Krypciak, S.; Bastuji-Garin, S.; Culine, S.; Paillaud, E. Comprehensive geriatric assessment in the decision-making process in elderly patients with cancer: ELCAPA study. J. Clin. Oncol. 2011, 29, 3636–3642. [Google Scholar] [CrossRef]
- Extermann, M.; Hurria, A. Comprehensive geriatric assessment for older patients with cancer. J. Clin. Oncol. 2007, 25, 1824–1831. [Google Scholar] [CrossRef]
- Freyer, G.; Geay, J.F.; Touzet, S.; Provencal, J.; Weber, B.; Jacquin, J.-P.; Ganem, G.; Tubiana-Mathieu, N.; Gisserot, O.; Pujade-Lauraine, E. Comprehensive geriatric assessment predicts tolerance to chemotherapy and survival in elderly patients with advanced ovarian carcinoma: A GINECO study. Ann. Oncol. 2005, 16, 1795–1800. [Google Scholar] [CrossRef]
- Girre, V.; Falcou, M.C.; Gisselbrecht, M.; Gridel, G.; Mosseri, V.; Bouleuc, C.; Poinsot, R.; Vedrine, L.; Ollivier, L.; Garabige, V.; et al. Does a geriatric oncology consultation modify the cancer treatment plan for elderly patients? J. Gerontol. A Biol. Sci. Med. Sci. 2008, 63, 724–730. [Google Scholar] [CrossRef]
- Puts, M.T.; Hardt, J.; Monette, J.; Girre, V.; Springall, E.; Alibhai, S.M.H. Use of geriatric assessment for older adults in the oncology setting: A systematic review. J. Natl. Cancer Inst. 2012, 104, 1133–1163. [Google Scholar] [CrossRef]
- Puts, M.T.; Santos, B.; Hardt, J.; Monette, J.; Girre, V.; Atenafu, E.G.; Springall, E.; Alibhai, S.M.H. An update on a systematic review of the use of geriatric assessment for older adults in oncology. Ann. Oncol. 2014, 25, 307–315. [Google Scholar] [CrossRef]
- Ramjaun, A.; Nassif, M.O.; Krotneva, S.; Huang, A.R.; Meguerditchian, A.N. Improved targeting of cancer care for older patients: A systematic review of the utility of comprehensive geriatric assessment. J. Geriatr. Oncol. 2013, 4, 271–281. [Google Scholar] [CrossRef]
- Wildiers, H.; Heeren, P.; Puts, M.; Topinkova, E.; Janssen-Heijnen, M.L.G.; Extermann, M.; Falandry, C.; Artz, A.; Brain, E.; Colloca, G. International Society of Geriatric Oncology consensus on geriatric assessment in older patients with cancer. J. Clin. Oncol. 2014, 32, 2595–2603. [Google Scholar] [CrossRef]
- McCorkle, R.; Ercolano, E.; Lazenby, M.; Schulman-Green, D.; Schilling, L.S.; Lorig, K.; Wagner, E.H. Self-management: Enabling and empowering patients living with cancer as a chronic illness. CA Cancer J. Clin. 2011, 61, 50–62. [Google Scholar] [CrossRef] [PubMed]
- Snyder, C.F.; Frick, K.D.; Herbert, R.J.; Blackford, A.L.; Neville, B.A.; Wolff, A.C.; Carducci, M.A.; Earle, C.C. Quality of care for comorbid conditions during the transition to survivorship: Differences between cancer survivors and noncancer controls. J. Clin. Oncol. 2013, 31, 1140–1148. [Google Scholar] [CrossRef] [PubMed]
- Earle, C.C.; Neville, B.A. Under use of necessary care among cancer survivors. Cancer 2004, 101, 1712–1719. [Google Scholar] [CrossRef] [PubMed]
- Popa, M.A.; Wallace, K.J.; Brunello, A.; Extermann, M.; Balducci, L. Potential drug interactions and chemotoxicity in older patients with cancer receiving chemotherapy. J. Geriatr. Oncol. 2014, 5, 307–314. [Google Scholar] [CrossRef]
- Neefan Leeuwen, R.W.; Brundel, D.H.; Neef, C.; van Gelder, T.; Mathijssen, R.H.J.; Burger, D.M.; Jansman, F.G.A. Prevalence of potential drug-drug interactions in cancer patients treated with oral anticancer drugs. Br. J. Cancer 2013, 108, 1071–1078. [Google Scholar] [CrossRef]
- Van Leeuwen, R.W.; Swart, E.L.; Boven, E.; Boom, F.A.; Schuitenmaker, M.G.; Hugtenburg, J.G. Potential drug interactions in cancer therapy: A prevalence study using an advanced screening method. Ann. Oncol. 2011, 22, 2334–2341. [Google Scholar] [CrossRef]
- Girre, V.; Arkoub, H.; Puts, M.T.; Vantelon, C.; Blanchard, F.; Droz, J.P.; Mignot, L. Potential drug interactions in elderly cancer patients. Crit. Rev. Oncol. Hematol. 2011, 78, 220–226. [Google Scholar] [CrossRef]
- Feuer, E.J.; Lee, M.; Mariotto, A.B.; Cronin, K.A.; Scoppa, S.; Penson, D.F.; Hachey, M.; Cynkin, L.; Carter, G.A.; Campbell, D. The Cancer Survival Query System: Making survival estimates from the Surveillance, Epidemiology, and End results program timelier and more relevant for recently diagnosed patients. Cancer 2012, 118, 5652–5662. [Google Scholar] [CrossRef]
- Daskivich, T.J.; Fan, K.H.; Koyama, T.; Albertsen, P.C.; Goodman, M.; Hamilton, A.S.; Hoffman, R.M.; Stanford, J.L.; Stroup, A.M.; Litwin, M.S. Effect of age, tumour risk, and comorbidity on competing risks for survival in a US population-based cohort of men with prostate cancer. Ann. Intern. Med. 2013, 158, 709–717. [Google Scholar] [CrossRef]
- US Department of Health and Human Services. Multiple Chronic Conditions: A Framework for Education and Training; US Department of Health and Human Services: Washington, DC, USA, 2015.
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).