Parallel Outbreaks of Deadly Pathogens (SARS-CoV-2, H5N8, EVD, Black Fungi) around East Africa and Asia in 2021: Priorities for Outbreak Management with Socio-Economic and Public Health Impact
Abstract
:1. Introduction
2. Methodology of the Review and Its Rationale
3. Results and Discussion
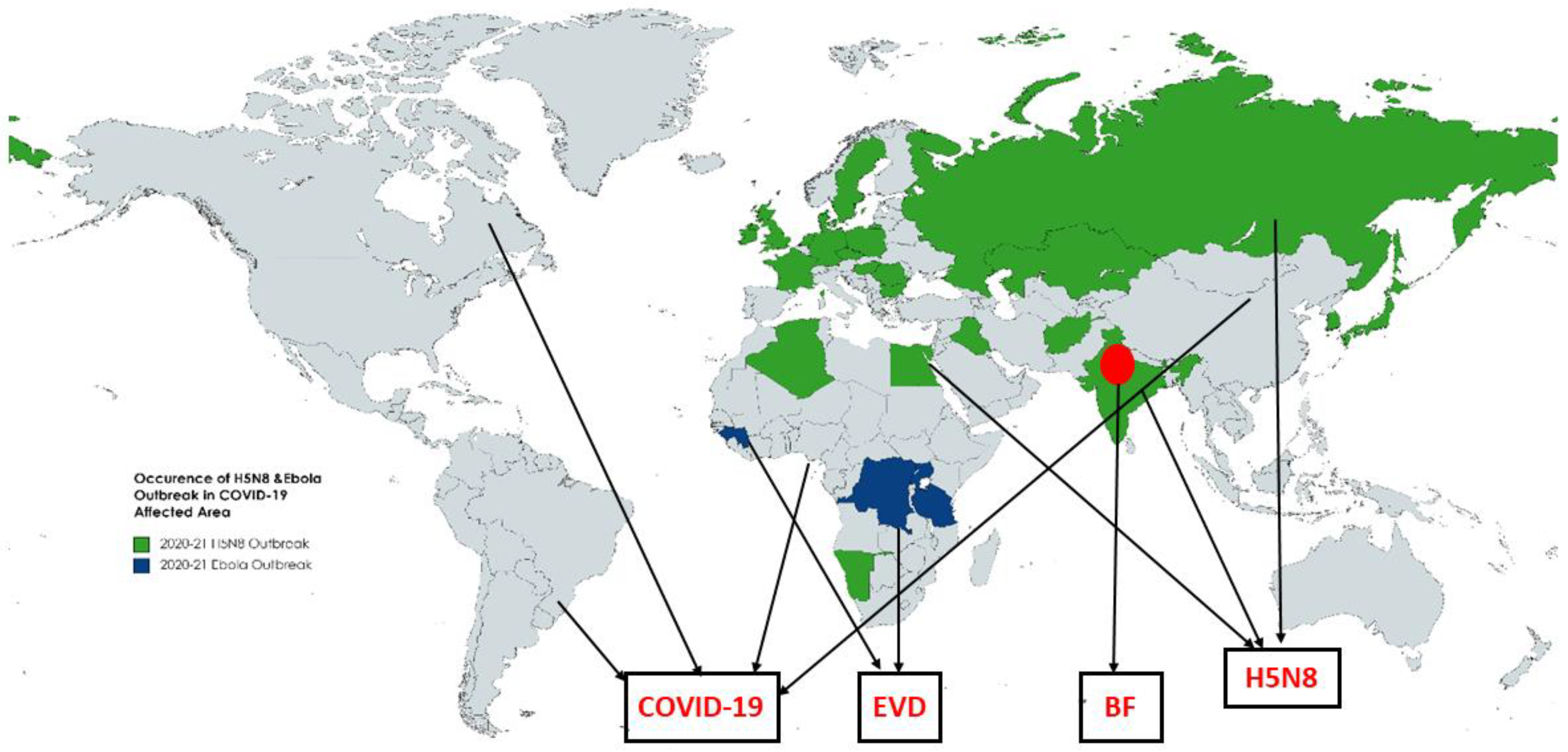
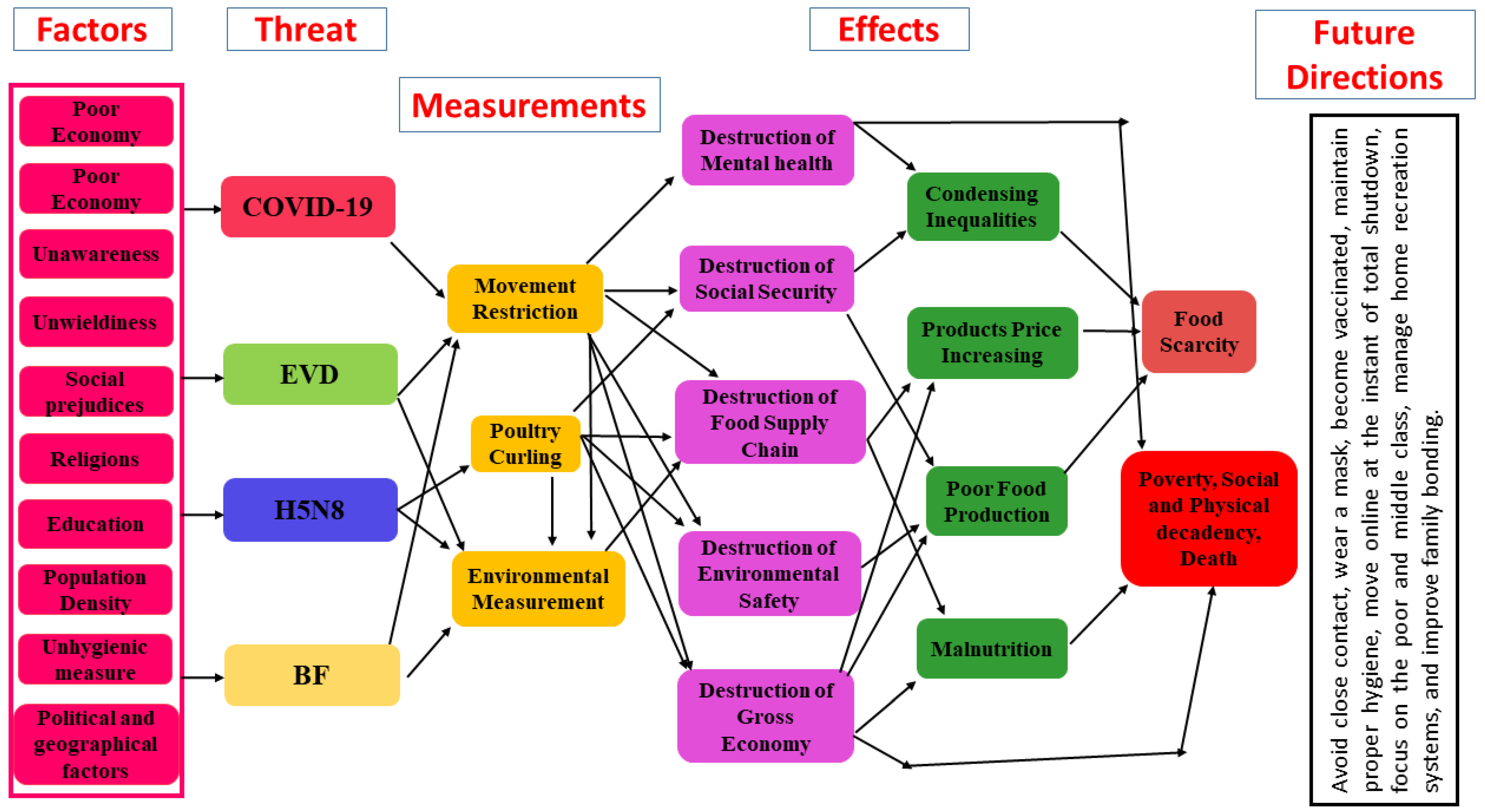
3.1. Possible Social Complications of Outbreaks in the Near Future
3.2. Impact of Each Outbreak on Public Health
3.3. Present Containment Strategies of All Outbreaks
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Rahman, M.S.; Hoque, M.N.; Islam, M.R.; Akter, S.; Alam, A.R.; Siddique, M.A.; Saha, O.; Rahaman, M.M.; Sultana, M.; Crandall, K.A.; et al. Epitope-based chimeric peptide vaccine de-sign against S, M and E proteins of SARS-CoV-2, the etiologic agent of COVID-19 pan-demic: An in silico approach. PeerJ. 2020, 8, e9572. [Google Scholar] [CrossRef]
- Islam, A.; Sayeed, A.; Rahman, K.; Zamil, S.; Abedin, J.; Saha, O.; Hassan, M.M. Assessment of basic reproduction number (R0), spatial and temporal epidemiological determinants, and genetic characterization of SARS-CoV-2 in Bangladesh. Infect. Genet. Evol. 2021, 92, 104884. [Google Scholar] [CrossRef]
- Nicola, M.; Alsafi, Z.; Sohrabi, C.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, M.; Agha, R. The so-cio-economic implications of the coronavirus and COVID-19 pandemic: A review. Int. J. Surg. 2020, 78, 185–193. [Google Scholar] [CrossRef] [PubMed]
- Rahaman, M.M.; Saha, O.; Rakhi, N.N.; Chowdhury, M.M.; Sammonds, P.; Kamal, A.M. Overlap-ping of locust swarms with COVID-19 pandemic: A cascading disaster for Africa. Pathog. Glob. Health 2020, 114, 285–286. [Google Scholar] [CrossRef] [PubMed]
- Ceylan, R.F.; Ozkan, B.; Mulazimogullari, E. Historical evidence for economic effects of COVID-19. Eur. J. Health Econ. 2020, 21, 817–823. [Google Scholar] [CrossRef]
- Saha, O.; Rakhi, N.N.; Sultana, A.; Rahman, M.M.; Rahaman, M.M. SARS-CoV-2 and COVID-19: A Threat to Global Health. Discov. Rep. 2020, 3, e13. [Google Scholar] [CrossRef]
- Baker, H.A.; Safavynia, S.A.; Evered, L.A. The ‘third wave’: Impending cognitive and function-al decline in COVID-19 survivors. Br. J. Anaesth. 2021, 126, 44–47. [Google Scholar] [CrossRef]
- Towhid, S.T.; Rakhi, N.N.; Arefin, A.S.; Saha, O.; Mamun, S.; Moniruzzaman, M.; Rahaman, M.M. COVID-19 and the Cardiovascular System: How the First Post-Modern Pandemic ‘Weak-ened’our Hearts. Discov. Rep. 2020, 3, e15. [Google Scholar] [CrossRef]
- Lewis, N.S.; Banyard, A.C.; Whittard, E.; Karibayev, T.; Al Kafagi, T.; Chvala, I.; Byrne, A.; Akberovna, S.M.; King, J.; Harder, T.; et al. Emergence and spread of novel H5N8, H5N5 and H5N1 clade 2.3.4.4 highly pathogenic avian influenza in 2020. Emerg. Microbes Infect. 2021, 10, 148–151. [Google Scholar] [CrossRef]
- Aborode, A.T.; Tsagkaris, C.; Jain, S.; Ahmad, S.; Essar, M.Y.; Fajemisin, E.A.; Adanur, I.; Uwishema, O. Ebola Outbreak amid COVID-19 in the Republic of Guinea: Priorities for Achieving Control. Am. J. Trop. Med. Hyg. 2021, 104, 1966–1969. [Google Scholar] [CrossRef]
- Dyer, O. Covid-19: India sees record deaths as “black fungus” spreads fear. BMJ 2021, 373, n1238. [Google Scholar] [CrossRef] [PubMed]
- Mucormycosis: The ’Black Fungus’ Maiming Covid Patients in India. Available online: https://www.bbc.com/news/world-asia-india-57027829 (accessed on 18 July 2021).
- Black Fungus Epidemic Triggers New Challenge in India. Available online: https://www.aa.com.tr/en/asia-pacific/black-fungus-epidemic-triggers-new-challenge-in-india/2253074 (accessed on 18 July 2021).
- Rocha, I.C.N.; Hasan, M.M.; Goyal, S.; Patel, T.; Jain, S.; Ghosh, A.; Cedeño, T.D.D. COVID-19 and Mucormycosis Syndemic: Double Health Threat to a Collapsing Healthcare System in India. Trop. Med. Int. Health 2021, 1–3. [Google Scholar] [CrossRef]
- About Mucormycosis|Mucormycosis|CDC. Available online: https://www.cdc.gov/fungal/diseases/mucormycosis/definition.html (accessed on 24 May 2021).
- Over 28,200 “Black Fungus” Cases Recorded in India. Available online: https://www.aa.com.tr/en/asia-pacific/over-28-200-black-fungus-cases-recorded-in-india/2266396 (accessed on 9 June 2021).
- Josephson, A.; Kilic, T.; Michler, J.D. Socioeconomic impacts of COVID-19 in low-income countries. Nat. Hum. Behav. 2021, 5, 557–565. [Google Scholar] [CrossRef] [PubMed]
- Shammi, M.; Doza, B.-D.; Islam, A.R.M.T.; Rahman, M. Strategic assessment of COVID-19 pandemic in Bangladesh: Comparative lockdown scenario analysis, public perception, and management for sustainability. Environ. Dev. Sustain. 2021, 23, 6148–6191. [Google Scholar] [CrossRef]
- Singh, K.; Kondal, D.; Mohan, S.; Jaganathan, S.; Deepa, M.; Venkateshmurthy, N.S.; Jarhyan, P.; Anjana, R.M.; Narayan, K.V.; Mohan, V.; et al. Health, psychosocial, and economic im-pacts of the COVID-19 pandemic on people with chronic conditions in India: A mixed methods study. BMC Public Health 2021, 21, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Kassegn, A.; Endris, E. Review on socio-economic impacts of ‘Triple Threats’ of COVID-19, desert locusts, and floods in East Africa: Evidence from Ethiopia. Cogent Soc. Sci. 2021, 7, 1885122. [Google Scholar] [CrossRef]
- Nagy, A.; Černíková, L.; Kunteová, K.; Dirbáková, Z.; Thomas, S.S.; Slomka, M.J.; Dán, Á.; Varga, T.; Máté, M.; Jiřincová, H.; et al. A universal RT-qPCR assay for “One Health” detection of influenza A viruses. PLoS ONE 2021, 16, e0244669. [Google Scholar] [CrossRef]
- Adlhoch, C.; Dabrera, G.; Penttinen, P.; Pebody, R.; On Behalf of Country Experts. Protective Measures for Humans against Avian Influenza A(H5N8) Outbreaks in 22 European Union/European Economic Area Countries and Israel, 2016–2017. Emerg. Infect. Dis. 2018, 24, e180269. [Google Scholar] [CrossRef] [Green Version]
- Kwon, J.H.; Lee, D.H.; Swayne, D.E.; Noh, J.Y.; Yuk, S.S.; Erdene-Ochir, T.O.; Hong, W.T.; Jeong, J.H.; Jeong, S.; Gwon, G.B.; et al. Highly pathogenic avian influenza A (H5N8) viruses rein-troduced into South Korea by migratory waterfowl, 2014–2015. Emerg. Infect. Dis. 2016, 22, 507. [Google Scholar] [CrossRef]
- Ku, K.B.; Park, E.H.; Yum, J.; Kim, J.A.; Oh, S.K.; Seo, S.H. Highly pathogenic avian influenza A (H5N8) virus from waterfowl, South Korea, 2014. Emerg. Infect. Dis. 2014, 20, 1587. [Google Scholar] [CrossRef]
- Briand, F.X.; Niqueux, E.; Schmitz, A.; Martenot, C.; Cherbonnel, M.; Massin, P.; Kerbrat, F.; Chatel, M.; Guillemoto, C.; Guillou-Cloarec, C.; et al. Highly Pathogenic Avian Influenza A (H5N8) Virus Spread by Short-and Long-Range Transmission, France, 2016–17. Emerg. Infect. Dis. 2021, 27, 508. [Google Scholar] [CrossRef]
- Guinat, C.; Nicolas, G.; Vergne, T.; Bronner, A.; Durand, B.; Courcoul, A.; Gilbert, M.; Guérin, J.-L.; Paul, M.C. Spatio-temporal patterns of highly pathogenic avian influenza virus subtype H5N8 spread, France, 2016 to 2017. Eurosurveillance 2018, 23, 1700791. [Google Scholar] [CrossRef] [PubMed]
- Redding, D.W.; Atkinson, P.M.; Cunningham, A.A.; Iacono, G.L.; Moses, L.M.; Wood, J.L.; Jones, K.E. Impacts of environmental and socio-economic factors on emergence and epidemic poten-tial of Ebola in Africa. Nat. Commun. 2019, 10, 4531. [Google Scholar] [CrossRef]
- Baseler, L.; Chertow, D.S.; Johnson, K.M.; Feldmann, H.; Morens, D.M. The pathogenesis of Ebo-la virus disease. Annu. Rev. Pathol. Mech. Dis. 2017, 12, 387–418. [Google Scholar] [CrossRef]
- Coltart, C.E.M.; Lindsey, B.; Ghinai, I.; Johnson, A.M.; Heymann, D.L. The Ebola outbreak, 2013–2016: Old lessons for new epidemics. Philos. Trans. R. Soc. B Biol. Sci. 2017, 372, 20160297. [Google Scholar] [CrossRef]
- Furuyama, W.; Marzi, A. Ebola Virus: Pathogenesis and Countermeasure Development. Annu. Rev. Virol. 2019, 6, 435–458. [Google Scholar] [CrossRef] [PubMed]
- Huber, C.; Finelli, L.; Stevens, W. The Economic and Social Burden of the 2014 Ebola Outbreak in West Africa. J. Infect. Dis. 2018, 218, S698–S704. [Google Scholar] [CrossRef] [PubMed]
- Ali, Z.; Green, R.; Zougmoré, R.B.; Mkuhlani, S.; Palazzo, A.; Prentice, A.M.; Haines, A.; Dangour, A.D.; Scheelbeek, P.F. Long-term impact of West African food system responses to COVID-19. Nat. Food 2020, 1, 768–770. [Google Scholar] [CrossRef]
- Stoop, N.; Desbureaux, S.; Kaota, A.; Lunanga, E.; Verpoorten, M. Covid-19 vs. Ebola: Impact on households and small businesses in North Kivu, Democratic Republic of Congo. World Dev. 2021, 140, 105352. [Google Scholar] [CrossRef]
- Islam, M.; Rakhi, N.N.; Islam, O.K.; Saha, O.; Rahaman, M. Challenges to be considered to evaluate the COVID-19 preparedness and outcome in Bangladesh. Int. J. Health Manag. 2020, 13, 263–264. [Google Scholar] [CrossRef]
- Nachega, J.B.; Mbala-Kingebeni, P.; Otshudiema, J.; Mobula, L.M.; Preiser, W.; Kallay, O.; Michaels-Strasser, S.; Breman, J.G.; Rimoin, A.W.; Nsio, J.; et al. Responding to the Challenge of the Dual COVID-19 and Ebola Epidemics in the Democratic Republic of Congo—Priorities for Achieving Control. Am. J. Trop. Med. Hyg. 2020, 103, 597–602. [Google Scholar] [CrossRef]
- Moona, A.A.; Islam, M.R. Mucormycosis or black fungus is a new fright in India during covid-19 pandemic: Associated risk factors and actionable items. Public Health Pract. (Oxf. Engl.) 2021, 2, 100153. [Google Scholar] [CrossRef]
- Black Fungus Detected in Covid-19 Survivors, 8 Lose Eyesight in Surat. India Today. 2021. Available online: www.indiatoday.in/coronavirus-outbreak/story/black-fungus-mucormycosis-detected-covid19-survivors-8-lose-eyesight-surat-fungal-infection-symptoms-1799971-2021-05-07 (accessed on 5 June 2021).
- Bangladesh Reports 1st Death by Black Fungus. Available online: https://www.aa.com.tr/en/asia-pacific/bangladesh-reports-1st-death-by-black-fungus/2253604 (accessed on 18 July 2021).
- Mottaleb, K.A.; Mainuddin, M.; Sonobe, T. COVID-19 induced economic loss and ensur-ing food security for vulnerable groups: Policy implications from Bangladesh. PLoS ONE 2020, 15, e0240709. [Google Scholar] [CrossRef] [PubMed]
- Organisation for Economic Cooperation and Development. Social Economy and the COVID-19 Crisis: Current and Future Roles; OECD Publishing: Paris, France, 2020. [Google Scholar]
- Uğur, N.G.; Akbıyık, A. Impacts of COVID-19 on global tourism industry: A cross-regional comparison. Tour. Manag. Perspect. 2020, 36, 100744. [Google Scholar] [CrossRef] [PubMed]
- Hossain, M.S.; Hami, I.; Sawrav, M.S.; Rabbi, M.F.; Saha, O.; Bahadur, N.M.; Rahaman, M.M. Drug Repurposing for Prevention and Treatment of COVID-19: A Clinical Landscape. Discoveries 2020, 8, e121. [Google Scholar] [CrossRef] [PubMed]
- Saha, O.; Hossain, M.S.; Rahaman, M.M. Genomic exploration light on multiple origin with potential parsimony-informative sites of the severe acute respiratory syndrome corona-virus 2 in Bangladesh. Gene Rep. 2020, 21, 100951. [Google Scholar] [CrossRef]
- Singh, S.; Roy, M.D.; Sinha, C.P.; Parveen, C.P.; Sharma, C.P.; Joshi, C.P. Impact of COVID-19 and lockdown on mental health of children and adolescents: A narrative review with recommendations. Psychiatry Res. 2020, 293, 113429. [Google Scholar] [CrossRef]
- Posel, D.; Oyenubi, A.; Kollamparambil, U. Job loss and mental health during the COVID-19 lockdown: Evidence from South Africa. PLoS ONE 2021, 16, e0249352. [Google Scholar] [CrossRef]
- Fana, M.; Pérez, S.T.; Fernandez-Macias, E. Employment impact of Covid-19 crisis: From short term effects to long terms prospects. J. Ind. Bus. Econ. 2020, 47, 1–20. [Google Scholar] [CrossRef]
- Nivette, A.E.; Zahnow, R.; Aguilar, R.; Ahven, A.; Amram, S.; Ariel, B.; Eisner, M.P. A global analysis of the impact of COVID-19 stay-at-home restrictions on crime. Nat. Hum. Behav. 2021, 5, 868–877. [Google Scholar] [CrossRef]
- Ahamed Mim, M.; Naznin Rakhi, N.; Saha, O.; Rahaman, M.M. Recommendation of fecal specimen for routine molecular detection of SARS-CoV-2 and for COVID-19 discharge criteria. Pathog Glob. Health 2020, 114, 168–169. [Google Scholar] [CrossRef] [PubMed]
- Ong, C.W.M.; Goletti, D. Impact of the global COVID-19 outbreak on the management of other communicable diseases. Int. J. Tuberc. Lung Dis. 2020, 24, 547–548. [Google Scholar] [CrossRef] [PubMed]
- WHO|Human Infection with Avian Influenza A (H5N8)—The Russian Federation. WHO. Available online: http://www.who.int/csr/don/26-feb-2021-influenza-a-russian-federation/en/ (accessed on 5 June 2021).
- Glynn, J.R. Age-specific incidence of Ebola virus disease. Lancet 2015, 386, 432. [Google Scholar] [CrossRef]
- Bower, H.; Johnson, S.; Bangura, M.S.; Kamara, A.J.; Kamara, O.; Mansaray, S.H.; Sesay, D.; Turay, C.; Checchi, F.; Glynn, J.R. Exposure-specific and age-specific attack rates for Ebola virus dis-ease in Ebola-affected households, Sierra Leone. Emerg. Infect. Dis. 2016, 22, 1403. [Google Scholar] [CrossRef] [Green Version]
- Yang, J.; Li, H. The impact of aging and COVID-19 on our immune system: A high-resolution map from single cell analysis. Protein Cell 2020, 11, 703–706. [Google Scholar] [CrossRef]
- Davies, N.G.; Klepac, P.; Liu, Y.; Prem, K.; Jit, M.; Eggo, R.M. Age-dependent effects in the trans-mission and control of COVID-19 epidemics. Nat. Med. 2020, 26, 1205–1211. [Google Scholar] [CrossRef]
- Dong, Y.; Mo, X.; Hu, Y.; Qi, X.; Jiang, F.; Jiang, Z.; Tong, S. Epidemiology of COVID-19 Among Children in China. Pediatrics 2020, 145, e20200702. [Google Scholar] [CrossRef] [Green Version]
- Abbasi, J. Younger Adults Caught in COVID-19 Crosshairs as Demographics Shift. JAMA 2020, 324, 2141. [Google Scholar] [CrossRef]
- Salvatore, P.P.; Sula, E.; Coyle, J.P.; Caruso, E.; Smith, A.R.; Levine, R.S.; Baack, B.N.; Mir, R.; Lockhart, E.R.; Tiwari, T.S.; et al. Recent increase in COVID-19 cases reported among adults aged 18–22 years—United States, 31 May–5 September 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 1419. [Google Scholar] [CrossRef]
- Liu, Y.; Mao, B.; Liang, S.; Yang, J.-W.; Lu, H.-W.; Chai, Y.-H.; Wang, L.; Zhang, L.; Li, Q.-H.; Zhao, L.; et al. Association between age and clinical characteristics and outcomes of COVID-19. Eur. Respir. J. 2020, 55, 2001112. [Google Scholar] [CrossRef] [Green Version]
- Foeller, E.M.; Valle, C.C.R.D.; Foeller, T.M.; Oladapo, O.T.; Roos, E.; Thorson, E.A. Pregnancy and breastfeeding in the context of Ebola: A systematic review. Lancet Infect. Dis. 2020, 20, e149–e158. [Google Scholar] [CrossRef]
- Bebell, L.M.; Oduyebo, T.; Riley, L.E. Ebola virus disease and pregnancy: A review of the current knowledge of Ebola virus pathogenesis, maternal, and neonatal outcomes. Birth Defects Res. 2017, 109, 353–362. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wastnedge, E.A.; Reynolds, R.M.; van Boeckel, S.R.; Stock, S.J.; Denison, F.C.; Maybin, J.A.; Critchley, H.O. Pregnancy and COVID-19. Physiol. Rev. 2021, 101, 303–318. [Google Scholar] [CrossRef]
- Dos Santos, W.G. Impact of virus genetic variability and host immunity for the success of COVID-19 vaccines. Biomed. Pharmacother. 2021, 136, 111272. [Google Scholar] [CrossRef]
- Zhou, P.; Liu, Z.; Chen, Y.; Xiao, Y.; Huang, X.; Fan, X.-G. Bacterial and fungal infections in COVID-19 patients: A matter of concern. Infect. Control. Hosp. Epidemiol. 2020, 41, 1124–1125. [Google Scholar] [CrossRef] [Green Version]
- Menon, B.S. Black Fungus: Is Diabetes Behind India’s High Number of Cases? BBC News. Updated 6 June 2021. Available online: https://www.bbc.com/news/world-asia-india-57252077 (accessed on 7 June 2021).
- Sugar, A.M. Mucormycosis. Clin. Infect. Dis. 1992, 14, S126–S129. [Google Scholar] [CrossRef]
- Singh, A.K.; Singh, R.; Joshi, S.R.; Misra, A. Mucormycosis in COVID-19: A systematic review of cases reported worldwide and in India. Diabetes Metab. Syndr. Clin. Res. Rev. 2021, 15, 102146. [Google Scholar] [CrossRef] [PubMed]
- Reddy, B.L.; Milton, H., Jr. The Causal Relationship between Eating Animals and Viral Epidemics. Microb. Physiol. 2020, 30, 2–8. [Google Scholar] [CrossRef] [PubMed]
- Tong, Y.; Shi, W.-F.; Liu, D.; Qian, J.; Liang, L.; Bo, X.-C.; Liu, J.; Ren, H.-G.; Fan, H.; Li, M.; et al. China Mobile Laboratory Testing Team in Sierra The China Mobile Laboratory Testing Team in Sierra Leone; Genetic diversity and evolutionary dynamics of Ebola virus in Sierra Leone. Nat. Cell Biol. 2015, 524, 93–96. [Google Scholar] [CrossRef]
- Boni, M.F.; Lemey, P.; Jiang, X.; Lam, T.T.Y.; Perry, B.W.; Castoe, T.A.; Robertson, D.L. Evolutionary origins of the SARS-CoV-2 sarbecovirus lineage responsible for the COVID-19 pandemic. Nat. Microbiol. 2020, 5, 1408–1417. [Google Scholar] [CrossRef]
- Saha, O.; Islam, I.; Shatadru, R.N.; Rakhi, N.N.; Hossain, M.S.; Rahaman, M.M. Temporal landscape of mutational frequencies in SARS-CoV-2 genomes of Bangladesh: Possible implications from the ongoing outbreak in Bangladesh. Virus Genes 2021, 1, 1–13. [Google Scholar]
- Lycett, S.J.; Duchatel, F.; Digard, P. A brief history of bird flu. Philos. Trans. R. Soc. B Biol. Sci. 2019, 374, 20180257. [Google Scholar] [CrossRef] [PubMed]
- Lycett, S.J.; Pohlmann, A.; Staubach, C.; Caliendo, V.; Woolhouse, M.; Beer, M.; Kuiken, T. Genesis and spread of multiple reassortants during the 2016/2017 H5 avian influenza epidemic in Eurasia. Proc. Natl. Acad. Sci. USA 2020, 117, 20814–20825. [Google Scholar] [CrossRef] [PubMed]
- France to Cull 600,000 Poultry to Stem Bird Flu. Reuters. Available online: https://www.reuters.com/business/healthcare-pharmaceuticals/france-cull-600000-poultry-stem-bird-flu-2021-01-05/ (accessed on 9 June 2021).
- Scoizec, A.; Niqueux, E.; Thomas, R.; Daniel, P.; Schmitz, A.; Le Bouquin, S. Airborne detection of H5N8 highly pathogenic avian influenza virus genome in poultry farms, France. Front. Vet. Sci. 2018, 5, 15. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- European Food Safety Authority. European Centre for Disease Prevention and Control and European Union Reference Laboratory for Avian Influenza, Adlhoch, C., Fusaro, A., Gonzales, J.L., Kuiken, T., Marangon, S., Niqueux, É., Staubach, C., Terregino, C., Muñoz Guajar-do I. Avian influenza overview December 2020–February 2021. EFSA J. 2021, 19, e06497. [Google Scholar]
- Govorkova, E.A.; McCullers, J.A. Therapeutics Against Influenza. Curr. Top. Microbiol. Immunol. 2011, 370, 273–300. [Google Scholar] [CrossRef]
- Nabi, G.; Wang, Y.; Lü, L.; Jiang, C.; Ahmad, S.; Wu, Y.; Li, D. Bats and birds as viral reservoirs: A physiological and ecological perspective. Sci. Total Environ. 2021, 754, 142372. [Google Scholar] [CrossRef]
- de Vries, R.D.; De Gruyter, H.L.; Bestebroer, T.M.; Pronk, M.; Fouchier, R.A.; Osterhaus, A.D.; Sutter, G.; Kreijtz, J.H.; Rimmelzwaan, G.F. Induction of influenza (H5N8) antibodies by modified vaccinia virus Ankara H5N1 vaccine. Emerg. Infect. Dis. 2015, 21, 1086. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ibrahim, M.; Zakaria, S.; Bazid, A.H.; Kilany, W.H.; El-Abideen, M.A.; Ali, A. A single dose of in-activated oil-emulsion bivalent H5N8/H5N1 vaccine protects chickens against the lethal challenge of both highly pathogenic avian influenza viruses. Comp. Immunol. Microbiol. Infect. Dis. 2021, 74, 101601. [Google Scholar] [CrossRef]
- Ren, H.; Wang, G.; Wang, S.; Chen, H.; Chen, Z.; Hu, H.; Cheng, G.; Zhou, P. Cross-protection of newly emerging HPAI H5 viruses by neutralizing human monoclonal antibodies: A viable alternative to oseltamivir. Platf. Dev. Expr. Purif. Stable Isot. labeled Monoclon. Antibodies Escherichia Coli 2016, 8, 1156–1166. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Baek, Y.G.; Lee, Y.N.; Lee, D.H.; Shin, J.I.; Lee, J.H.; Chung, D.H.; Lee, E.K.; Heo, G.B.; Sagong, M.; Kye, S.J.; et al. Multiple Reassortants of H5N8 Clade 2.3. 4.4 b Highly Pathogenic Avian Influ-enza Viruses Detected in South Korea during the Winter of 2020–2021. Viruses 2021, 13, 490. [Google Scholar] [CrossRef]
- Chan, M. Ebola Virus Disease in West Africa—No Early End to the Outbreak. N. Engl. J. Med. 2014, 371, 1183–1185. [Google Scholar] [CrossRef] [PubMed]
- Saeed, S.; Hasan, S.; Ahmad, S.A.; Masood, R. Ebola virus: A global public health menace: A narrative review. J. Fam. Med. Prim. Care 2019, 8, 2189–2201. [Google Scholar] [CrossRef] [PubMed]
- Quaglio, G.; Goerens, C.; Putoto, G.; Rübig, P.; Lafaye, P.; Karapiperis, T.; Dario, C.; Delaunois, P.; Zachariah, R. Ebola: Lessons learned and future challenges for Europe. Lancet Infect. Dis. 2015, 16, 259–263. [Google Scholar] [CrossRef]
- Gupta, S.; Gupta, N.; Yadav, P.; Patil, D. Ebola virus outbreak preparedness plan for develop-ing Nations: Lessons learnt from affected countries. J. Infect. Public Health 2021, 14, 293–305. [Google Scholar] [CrossRef] [PubMed]
- Aruna, A.; Mbala, P.; Minikulu, L.; Mukadi, D.; Bulemfu, D.; Edidi, F.; Bulabula, J.; Tshapenda, G.; Nsio, J.; Kitenge, R.; et al. Ebola Virus Disease Outbreak—Democratic Republic of the Congo, August 2018–November 2019. Morb. Mortal. Wkly. Report 2019, 68, 1162. [Google Scholar] [CrossRef] [Green Version]
- Adepoju, P. Ebola and COVID-19 in DR Congo and Guinea. Lancet Infect. Dis. 2021, 21, 461. [Google Scholar] [CrossRef]
- Rojas, M.; Monsalve, D.M.; Pacheco, Y.; Acosta-Ampudia, Y.; Ramírez-Santana, C.; Ansari, A.A.; Gershwin, M.E.; Anaya, J.-M. Ebola virus disease: An emerging and re-emerging viral threat. J. Autoimmun. 2020, 106, 102375. [Google Scholar] [CrossRef]
- Wolf, J.; Jannat, R.; Dubey, S.; Troth, S.; Onorato, M.T.; Coller, B.A.; Hanson, M.E.; Simon, J.K. Development of Pandemic Vaccines: ERVEBO Case Study. Vaccines 2021, 9, 190. [Google Scholar] [CrossRef]
- Ullah, M.A.; Sarkar, B.; Islam, S.S. Exploiting the reverse vaccinology approach to design novel subunit vaccines against Ebola virus. Immunobiology 2020, 225, 151949. [Google Scholar] [CrossRef]
- Yazdanpanah, Y.; Arribas, J.R.; Malvy, D. Treatment of Ebola virus disease. Intensive Care Med. 2015, 41, 115–117. [Google Scholar] [CrossRef]
- Bishop, B.M. Potential and Emerging Treatment Options for Ebola Virus Disease. Ann. Pharmacother. 2014, 49, 196–206. [Google Scholar] [CrossRef]
- Kiiza, P.; Mullin, S.; Teo, K.; Adhikari, N.K.; Fowler, R.A. Treatment of Ebola-related critical illness. Intensive Care Med. 2020, 46, 285–297. [Google Scholar] [CrossRef] [PubMed]
- Markham, A. REGN-EB3: First Approval. Drugs 2021, 81, 175–178. [Google Scholar] [CrossRef] [PubMed]
- Joe, P.; Ashutosh, M.S.; Gajapathiraju, C.; Asmita, G. The Journey of Remdesivir: From Ebola to COVID-19. Drugs Context. 2020, 9, 1–9. [Google Scholar]
- Uyeki, T.M.; Mehta, A.K.; Davey, R.T., Jr.; Liddell, A.M.; Wolf, T.; Vetter, P.; Schmiedel, S.; Grünewald, T.; Jacobs, M.; Arribas, J.R.; et al. Clinical management of Ebola virus disease in the Unit-ed States and Europe. N. Engl. J. Med. 2016, 374, 636–646. [Google Scholar] [CrossRef] [Green Version]
- Chakraborty, I.; Maity, P. COVID-19 outbreak: Migration, effects on society, global envi-ronment and prevention. Sci. Total. Environ. 2020, 728, 138882. [Google Scholar] [CrossRef]
- Douglas, M.; Katikireddi, S.V.; Taulbut, M.; McKee, M.; McCartney, G. Mitigating the wider health effects of covid-19 pandemic response. BMJ 2020, 369, m1557. [Google Scholar] [CrossRef]
- Islam, N.; Sharp, S.J.; Chowell, G.; Shabnam, S.; Kawachi, I.; Lacey, B.; Massaro, J.M.; Sr, R.B.D.; White, M. Physical distancing interventions and incidence of coronavirus disease 2019: Natural experiment in 149 countries. BMJ 2020, 370, m2743. [Google Scholar] [CrossRef] [PubMed]
- Nussbaumer-Streit, B.; Mayr, V.; Dobrescu, A.I.; Chapman, A.; Persad, E.; Klerings, I.; Gartlehner, G. Quarantine alone or in combination with other public health measures to control COVID-19: A rapid review. Cochrane Database Syst. Rev. 2020, 4, CD013574. [Google Scholar]
- Heinz, F.X.; Stiasny, K. Profiles of current COVID-19 vaccines. Wien. Klin. Wochenschr. 2021, 133, 271–283. [Google Scholar] [CrossRef] [PubMed]
- Gómez, C.E.; Perdiguero, B.; Esteban, M. Emerging sars-cov-2 variants and impact in global vaccination programs against sars-cov-2/covid-19. Vaccines 2021, 9, 243. [Google Scholar] [CrossRef] [PubMed]
- Stasi, C.; Fallani, S.; Voller, F.; Silvestri, C. Treatment for COVID-19: An overview. Eur. J. Pharmacol. 2020, 889, 173644. [Google Scholar] [CrossRef]
- Chibber, P.; Haq, S.A.; Ahmed, I.; Andrabi, N.I.; Singh, G. Advances in the possible treatment of COVID-19: A review. Eur. J. Pharmacol. 2020, 883, 173372. [Google Scholar] [CrossRef]
- Rabby, M.I. Current drugs with potential for treatment of COVID-19: A literature review. J. Pharm. Pharm. Sci. 2020, 23, 58–64. [Google Scholar] [CrossRef]
- WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19-22 June 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---22-june-2020 (accessed on 10 June 2021).
- Xu, X.; Han, M.; Li, T.; Sun, W.; Wang, D.; Fu, B.; Zhou, Y.; Zheng, X.; Yang, Y.; Li, X.; et al. Effective treatment of severe COVID-19 patients with tocilizumab. Proc. Natl. Acad. Sci. USA 2020, 117, 10970–10975. [Google Scholar] [CrossRef] [PubMed]
- Lokugamage, K.G.; Hage, A.; Schindewolf, C.; Rajsbaum, R.; Menachery, V.D. SARS-CoV-2 sensitive to type I interferon pretreatment. BioRxiv 2020. [Google Scholar] [CrossRef] [Green Version]
- Walz, L.; Cohen, A.J.; Rebaza, A.P.; Vanchieri, J.; Slade, M.D.; Cruz, C.S.D.; Sharma, L. JAK-inhibitor and type I interferon ability to produce favorable clinical outcomes in COVID-19 patients: A systematic review and meta-analysis. BMC Infect. Dis. 2021, 21, 1–10. [Google Scholar] [CrossRef]
- Rajendran, K.; Krishnasamy, N.; Rangarajan, J.; Rathinam, J.; Natarajan, M.; Ramachandran, A. Convalescent plasma transfusion for the treatment of COVID-19: Systematic review. J. Med. Virol. 2020, 92, 1475–1483. [Google Scholar] [CrossRef]
- Sarkar, S.; Soni, K.D.; Khanna, P. Convalescent plasma is a clutch at straws in COVID-19 management! A systematic review and meta-analysis. J. Med Virol. 2021, 93, 1111–1118. [Google Scholar] [CrossRef] [PubMed]
| Outbreak | 1st Line Effects | 2nd Line Effects | Adverse Effect |
|---|---|---|---|
| Social | Destruction of social execution Vulnerable groups become helpless Loss of lives Education system collapse | Community imbalance Imbalance of all social activities Unethical activity by vulnerable groups Insecurity on future generation educations | Vulnerable groups victimized Insectary in community Political crisis Destruction of total education systems |
| Economic | Scarcity of basic materials including oxygen, medicine, etc. Rise of product prices Country GDP decrease Trading with neighboring country will be disturbed Loss of jobs Unemployment problems increase | Loss of livelihoods Destructions of local supply capacity Country’s economy fall | Increased poverty Higher scarcity of foods Breakdown of financial chain |
| Public Health | Health service insecurity Impairment of basic needs of life Health destruction of children and pregnant women Development of prejudice Loss of vision ability | Crisis in health sectors Development of abnormal children Environmental crisis Disruption of working ability | Loss of valuable lives Increase in abnormal mental health Malnutrition Loss of total working ability |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Khan, A.; Ema, N.T.; Rakhi, N.N.; Saha, O.; Ahamed, T.; Rahaman, M.M. Parallel Outbreaks of Deadly Pathogens (SARS-CoV-2, H5N8, EVD, Black Fungi) around East Africa and Asia in 2021: Priorities for Outbreak Management with Socio-Economic and Public Health Impact. COVID 2021, 1, 203-217. https://doi.org/10.3390/covid1010017
Khan A, Ema NT, Rakhi NN, Saha O, Ahamed T, Rahaman MM. Parallel Outbreaks of Deadly Pathogens (SARS-CoV-2, H5N8, EVD, Black Fungi) around East Africa and Asia in 2021: Priorities for Outbreak Management with Socio-Economic and Public Health Impact. COVID. 2021; 1(1):203-217. https://doi.org/10.3390/covid1010017
Chicago/Turabian StyleKhan, Afroza, Nayeema Talukder Ema, Nadira Naznin Rakhi, Otun Saha, Tamer Ahamed, and Md. Mizanur Rahaman. 2021. "Parallel Outbreaks of Deadly Pathogens (SARS-CoV-2, H5N8, EVD, Black Fungi) around East Africa and Asia in 2021: Priorities for Outbreak Management with Socio-Economic and Public Health Impact" COVID 1, no. 1: 203-217. https://doi.org/10.3390/covid1010017






