Identifying User Requirements for an Integrated E-Health Unit for Diabetes Mellitus
Abstract
1. Introduction
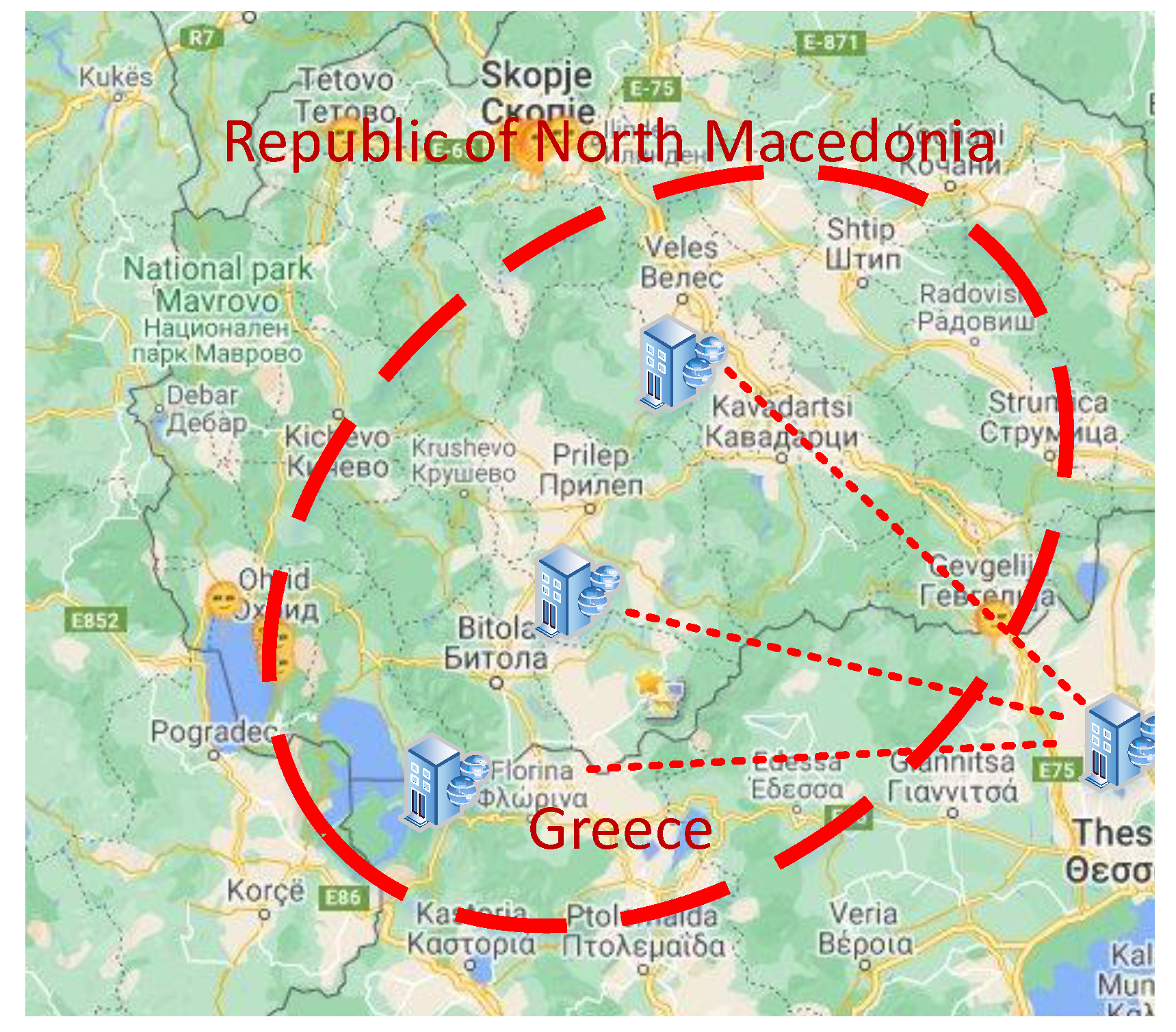
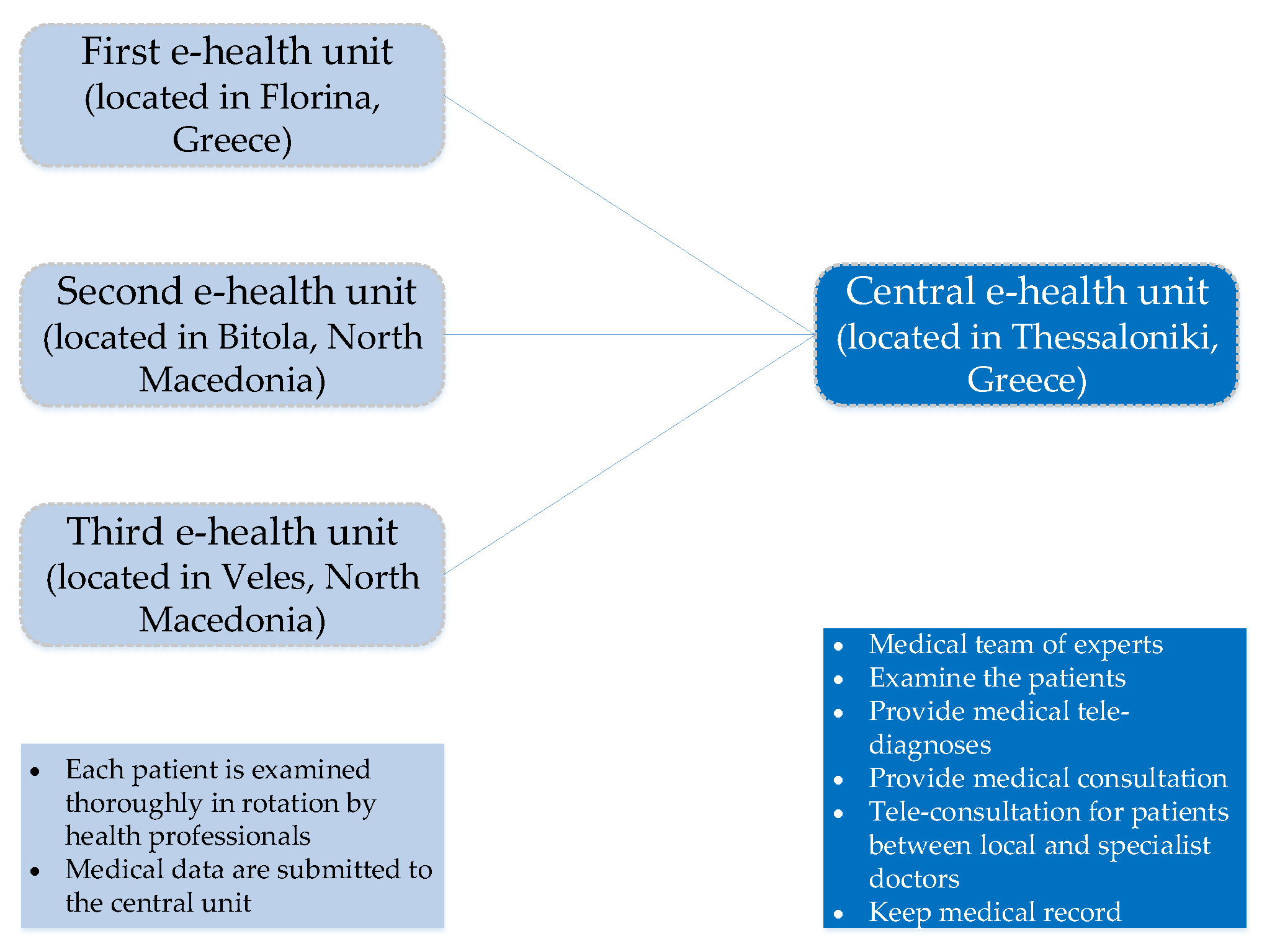
2. Telehealth Research Project Overview
- To support collaboration between research teams from the Republic of North Macedonia and Greece of scientists from different scientific fields (such as doctors, biologists, etc.) and closer cooperation among the two national health care systems to develop a common strategy for prevention, early diagnosis and treatment of obesity, DM and cardio-vascular disease (CVD).
- To raise awareness of the local and national authorities regarding the above health issues.
- To inform the regional population on the prevention, diagnosis, and treatment of DM, obesity and CVD.
- To identify the environmental and other risk factors that are involved in the development of DM, obesity, and CVD in the population that participate in the project.
- To facilitate access for doctors on both sides of the border to their patients’ data through telehealth.
- To support the life-long education of the COMETECH involved population and medical practitioners by using their telehealth interaction with experts as the means for training.
3. User Requirements
3.1. Medical Device Requirements
- Column scale (height scale, stadiometer). The column scale used in the COMETECH project is an electronic height measurement device with high accuracy. It is battery supplied and features a mechanism on the headpiece to ensure that the patient is in the right position and thereby contribute to obtaining accurate measurements.
- Blood Glucose (blood sugar) Monitoring System Device. The procedure is very easy and typical for this important test. After completion of the examination, the result is transferred and recorded in the software application platform.
- A hemoglobin A1c (HbA1c) test measures the amount of glucose attached to hemoglobin with a color touch display and easy handling device.
- Electronic Stethoscope is a wireless device in which the sounds are transmitted electronically, provides noise reduction, signal enhancement, and both visual and audio output. In the project, this device also combines ambient noise reduction technology and frictional noise dampening features with amplification, Bluetooth technology, and a friendly user interface.
- The electrocardiogram (ECG) test is applied using a battery-powered portable device that records the heart’s electrical activity. It can collect ECG signals simultaneously and print ECG waveform with a thermal printing system.
- The spirometer test (spirogram) is made by a spirometer device, for measuring the volume of air inspired and expired by the lungs. Once again, after completion of the examination, the results are automatically transferred and recorded in the software application platform.
- The blood pressure monitor, with ankle brachial index (ABI) device, includes four blood pressure cuffs for both arms and both legs, which measure electronically the blood pressure simultaneously at the above four points and automatically calculates the ABI index.
- The foot scanner is a lightweight, portable plantar pressure measurement device that records all the relevant information needed to analyze the foot’s behavior. The device automatically measures the plantar pressures and analyzes them. A straightforward interpretation of the foot’s function is displayed via detailed images and statistical graphs. After completion of the examination, the results are automatically transferred and recorded in the application.
- The advanced glycated end product monitoring device is a portable non-invasive monitoring device that uses ultra-violet light to excite auto fluorescence in human skin tissue. The AGE Reader has a light source that illuminates the tissue of interest (usually the arm).
- The non-mydriatic retinal camera (fundus camera) is a specially crafted low-power microscope fitted with a high-definition camera. It produces true color fundus photos of excellent quality. Additionally, it guarantees fully automated alignment, autofocus and auto shoot. The photographs taken can also be kept on file, resulting in a far more detailed and accurate optical history to be built up of the eye health over time.
- The pulse oximeter finger pulse blood oxygen SPO2 monitor is a small, portable clip-like battery-operated device for monitoring blood oxygen saturation and detecting the pulse rate non-invasively.
- The ECG Holter Monitoring system is a type of ambulatory electrocardiography device, a portable device for cardiac monitoring (the monitoring of the electrical activity of the cardiovascular system) for at least 24 to 48 h.
- The wireless weight scale measures BMI, lean, bone, muscle, water mass body fat, and visceral fat. It also estimates daily caloric intake, displays room temperature and humidity, tracks data, graphs, history, etc. As above, after completion of the examination, the results are automatically transferred and recorded in the software application platform.
3.2. E-Health Unit Requirements
- Security. Firstly, the telehealth equipment/medical devices should be locked in secure locked cabinets, especially those with a high price (e.g., digital cameras, electrocardiogram devices, etc.). Secondly, additional security sensors are required for monitoring the place and parameters such as heat, humidity, movements, etc.
- Privacy. The telehealth room must provide speech and visual privacy from external observers with adjacent spaces based on the telehealth room’s clinical function.
- Confidentiality. The room must ensure patient confidentiality.
- Connectivity. The room should be equipped with an Internet connection for the software application.
- Location
- Space/size
- Layout
- Acoustics
- Lighting
- Equipment
4. Discussion and Conclusions
Author Contributions
Funding

Disclaimer
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Ekeland, G.; Bowes, A.; Flottorp, S. Effectiveness of telemedicine: A systematic review of reviews. Int. J. Med. Inform. 2010, 79, 736–771. [Google Scholar] [CrossRef]
- ASHE FGI. Lays Out Telehealth Guidelines. 2018. Available online: https://www.hfmmagazine.com/articles/3337-fgi-lays-out-telehealth-guidelines?utm_medium=email&utm_source=newsletter&utm_campaign=pdcnews&utm_content=20180509&eid=371822167&bid=2095993 (accessed on 30 January 2021).
- Caffery, L.J. Telehealth interventions for reducing waiting lists and waiting times for specialist outpatient services: A scoping review. J. Telemed. Telecare 2016, 22, 504–512. [Google Scholar] [CrossRef]
- Moffatt, J.; Diann, E. The reported benefits of telehealth for rural Australians. Aust. Health Rev. 2010, 34, 276–281. [Google Scholar] [CrossRef] [PubMed]
- Smith, A.; Thomas, E.; Snoswell, C.; Haydon, H.; Mehrotra, A.; Clemensen, J.; Caffery, L. Telehealth for global emergencies: Implications for coronavirus disease 2019 (COVID-19). J. Telemed. Telecare 2020, 26, 309–313. [Google Scholar] [CrossRef] [PubMed]
- Doarn, R.; Merrell, C. Telemedicine and e-health in disaster response. Telemed. e-Health 2014, 20, 605–607. [Google Scholar] [CrossRef] [PubMed]
- Zhou, X.; Snoswell, C.; Harding, L.; Bambling, M.; Edirippulige, S.; Bai, X.; Smith, A. The Role of Telehealth in Reducing the Mental Health Burden from COVID-19. Telemed. e-Health 2020, 26, 377–379. [Google Scholar] [CrossRef] [PubMed]
- Carter, L.; Nunlee-Bland, G.; Callender, C. A patient-centric, provider-assisted diabetes telehealth self-management intervention for urban minorities. Perspect. Health Inf. Manag. 2011, 8, 1b. [Google Scholar] [PubMed]
- Kaufman, R.; Starren, J.; Patel, L.; Morin, C.; Hilliman, C.; Pevzner, J. A cognitive framework for understanding barriers to the productive use of a diabetes home telemedicine system. In American Medical Informatics Association Symposium; Musen, M.A., Friedman, C.P., Teich, J.M., Eds.; American Medical Informatics Association: Bethesda, MD, USA, 2003; pp. 356–360. [Google Scholar]
- Odom, J.; Stancil, M.; Nelson, B.; Russ-Sellers, R.; Schwecke, N.; Dawson, J.; Reulbach, L.; Burns, A.; Lindholm, M.; Bruch, J. Improving Diabetes Control through Remote Glucose Monitoring in a Diabetes Self-Management Program for Employees of a Health System. Clin. Diabetes 2019, 37, 203–210. [Google Scholar] [CrossRef]
- Tang, P.; Overhage, J.; Chan, A.; Brown, N.; Aghighi, B.; Entwistle, M.; LuiHui, S.; Hyde, S.; Klieman, L.; Mitchell, C.; et al. Online disease management of diabetes: Engaging and Motivating Patients Online With Enhanced Resources-Diabetes (EMPOWER-D), a randomized controlled trial. J. Am. Med. Inform. Assoc. 2013, 20, 526–534. [Google Scholar] [CrossRef]
- Hanlon, P.; Daines, L.; Campbell, C.; McKinstry, B.; Weller, D.; Pinnock, H. Telehealth Interventions to Support Self-Management of Long-Term Conditions: A Systematic Metareview of Diabetes, Heart Failure, Asthma, Chronic Obstructive Pulmonary Disease, and Cancer. J. Med. Internet Res. 2017, 19, 172–181. [Google Scholar] [CrossRef] [PubMed]
- Crossen, S.; Raymond, J.; Neinstein, A. Top 10 Tips for Successfully Implementing a Diabetes Telehealth Program. Diabetes Technol. Ther. 2020, 22, 920–928. [Google Scholar] [CrossRef]
- Krupinski, E. Telemedicine Workplace Environments: Designing for Success. Healthcare 2014, 2, 139–146. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization, Regional Office for Europe. Diabetes: Data and Statistics. 2021. Available online: https://www.euro.who.int/en/health-topics/noncommunicable-diseases/diabetes/data-and-statistics (accessed on 30 January 2021).
- James, W. World Health Organization recognition of the global obesity epidemic. Int. J. Obes. 2008, 32 (Suppl. 7), S120–S126. [Google Scholar] [CrossRef] [PubMed]
- Eurostat Statistics Overweight and Obesity-BMI Statistics. 2014. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php/Overweight_and_obesity_-_BMI_statistics (accessed on 30 January 2021).
- World Health Organization, Regional Office for Europe Nutrition. Physical Activity and Obesity Greece. 2013. Available online: https://www.euro.who.int/__data/assets/pdf_file/0013/243301/Greece-WHO-Country-Profile.pdf (accessed on 30 January 2021).
- European Commission, OECD. Health at a Glance: Europe State of Health in the EU Cycle. 2018. Available online: https://ec.europa.eu/health/sites/health/files/state/docs/2018_healthatglance_rep_en.pdf (accessed on 30 January 2021).
- European Commission, OECD. Health at a Glance: Europe State of Health in the EU Cycle. 2020. Available online: https://ec.europa.eu/health/sites/health/files/state/docs/2020_healthatglance_rep_en.pdf (accessed on 30 January 2021).
- World Health Organization. Investing in Health for Economic Development. 2004. Available online: https://www.who.int/macrohealth/action/sintesis15novingles.pdf (accessed on 30 January 2021).
- Hume, R.; Looney, J. Designing for Telehealth Spaces, Planning for the Next Generation of Health Care Delivery. 2016. Available online: https://www.hfmmagazine.com/articles/1889-designing-for-telehealth-spaces (accessed on 30 January 2021).
- Facility Guidelines Institute Guidelines for Design and Construction. 2018. Available online: https://fgiguidelines.org/guidelines/2018-fgi-guidelines/ (accessed on 22 August 2020).
- California Telehealth and eHEALTH Center (CTEC). Telehealth Room Design, Program Guide; CTRC: Augusta, GA, USA, 2011. [Google Scholar]
- PHSA. Guidelines for Telehealth Rooms Used by the Provincial Health Services Authority in Canada. 2015. Available online: http://www.phsa.ca/Documents/Telehealth/TH_Clinical_Guidelines_Sept2015.pdf (accessed on 12 August 2020).
- Krupinski, E.; Burdick, A.; Pak, H.; Bocachica, J.; Earles, L.; Edison, K.; Goldyne, M.; Hirota, T.; Kvedar, J.; McKoy, K. American Telemedicine Association’s Practice Guidelines for Teledermatology. Telemed. e Health 2008, 14, 289–302. [Google Scholar] [CrossRef] [PubMed]
- Krupinski, E.A. Medical grade vs. off-the-shelf color displays: Influence on observer performance and visual search. J. Digit. Imaging 2009, 22, 363–368. [Google Scholar] [CrossRef] [PubMed]
- Turvey, C.; Coleman, M.; Dennison, O.; Drude, K.; Goldenson, M.; Hirsch, P.; Jueneman, R.; Kramer, G.M.; Luxton, D.D.; Maheu, M.M. ATA Practice Guidelines for Video-Based Online Mental health Services. Telemed. e Health 2013, 19, 722–730. [Google Scholar] [CrossRef] [PubMed]
- Ontario Telehealth Network (OTN). Telehealth Space Location and Preparation Guidelines. Telehealth Space Location and Preparation. 2013. Available online: https://support.otn.ca/sites/default/files/space_and_location_guideline.pdf (accessed on 30 January 2021).
- Major, J. Telehealth room design. J. Telehealth Telecare 2005, 11, 10–14. Available online: https://telehealth.arizona.edu/sites/telehealth.arizona.edu/files/Fundamental_TelehealthRoomDesign.pdf (accessed on 30 January 2021). [CrossRef] [PubMed]
- Collins, J. Lighting design & layout of a telemedicine conference room. Telemed. Today 1996, 4, 26–28. [Google Scholar]
- First Nations of Quebec and Labrador Health and Social Services Commission. Teleconsultation Room Design. 2016. Available online: http://www.cssspnql.com/docs/default-source/centre-de-documentation/doc_telesante_salle_eng_web.pdf?sfvrsn=2 (accessed on 30 January 2021).
- Muther, R.; Hales, L. Systematic Layout Planning, 4th ed.; Management and Industrial Research Publication: Marietta, GA, USA, 2015. [Google Scholar]
- Muther, R. Systematic Layout Planning; Cahners Books: Boston, MA, USA, 1973. [Google Scholar]
- Jain, S.; Yadav, K. Systematic Layout Planning: A Review of Improvement in Approach to Pulse Processing Mills. Int. Res. J. Eng. Technol. 2017, 4, 503–507. [Google Scholar]
- Dlaplus.com. Telemedicine Design: The Future of Healthcare Design. 2019. Available online: https://dlaplus.com/pages/telemedicine-design-the-future-of-healthcare-design (accessed on 30 January 2021).
- University of Colorado Denver. Telehealth Health Guide, Room Setup and Equipment Issues. Available online: http://www.tmhguide.org/site/epage/94034_871.htm (accessed on 12 May 2016).
- Jaana, M.; Paré, G. Home telemonItoring of Patients with Diabetes: A Systematic Assessment of Observed Effects. J. Eval. Clin. Pract. 2007, 13, 242–253. [Google Scholar] [CrossRef]
- Klonoff, D. Using Telemedicine to Improve Outcomes in Diabetes—An Emerging Technology. J. Diabetes Sci. Technol. 2009, 3, 624–628. [Google Scholar] [CrossRef] [PubMed]

| Devices | Space Area (m2) |
|---|---|
| 1. Desktop | 1 |
| 2. Non-mydriatic fundus camera | 2.5 |
| 3. Spirometer | 1 |
| 4. Glucometer | 1 |
| 5. Glycated Hemoglobin (HbA1c) | 1 |
| 6. Pulse oxymeter | 1 |
| 7. Electronic weight scale | 1 |
| 8. Height measuring | 1 |
| 9. Foot pressure measuring | 1 |
| 10. AGEs (Advanced Glycation End products) | 1 |
| 11. Blood Pressure and ABI measurement | 6 |
| 12. Electrocardiogram (ECG) | 6 |
| 13. Electronic stethoscope | 1 |
| Total area | 24.5 m2 |
| Devices | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Desktop | |||||||||||||
| 2. Non-mydriatic fundus camera | A | ||||||||||||
| 3. Spirometer | I | A | |||||||||||
| 4. Glucometer | I | O | A | ||||||||||
| 5. Glycated hemoglobin (HbA1c) | I | O | O | A | |||||||||
| 6. Pulse oxymeter | I | O | O | O | A | ||||||||
| 7. Electronic weight scale | I | O | O | O | O | A | |||||||
| 8. Height measuring | I | O | O | O | O | O | E | ||||||
| 9. Foot pressure measuring | I | O | O | O | O | O | O | E | |||||
| 10. AGEs (advanced glycation end products) | I | O | O | O | O | O | O | O | E | ||||
| 11. Blood pressure and ABI measurement | I | O | O | O | O | O | O | O | O | A | |||
| 12. Electrocardiogram (ECG) | I | O | O | O | O | O | O | O | O | O | A | ||
| 13. Electronic stethoscope | I | O | O | O | O | O | O | O | O | O | O | A |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tzilini, M.; Folinas, D.; Kazakos, K. Identifying User Requirements for an Integrated E-Health Unit for Diabetes Mellitus. Diabetology 2021, 2, 65-76. https://doi.org/10.3390/diabetology2020006
Tzilini M, Folinas D, Kazakos K. Identifying User Requirements for an Integrated E-Health Unit for Diabetes Mellitus. Diabetology. 2021; 2(2):65-76. https://doi.org/10.3390/diabetology2020006
Chicago/Turabian StyleTzilini, Maria, Dimitris Folinas, and Kyriakos Kazakos. 2021. "Identifying User Requirements for an Integrated E-Health Unit for Diabetes Mellitus" Diabetology 2, no. 2: 65-76. https://doi.org/10.3390/diabetology2020006
APA StyleTzilini, M., Folinas, D., & Kazakos, K. (2021). Identifying User Requirements for an Integrated E-Health Unit for Diabetes Mellitus. Diabetology, 2(2), 65-76. https://doi.org/10.3390/diabetology2020006





