Outpatient Hysteroscopic Treatment of Cervical Ectopic Pregnancy in a Primigravida Using the Ho:YAG Laser: A Case Report and Operative Protocol Evaluation
Abstract
1. Introduction
Methodology of the Literature Review
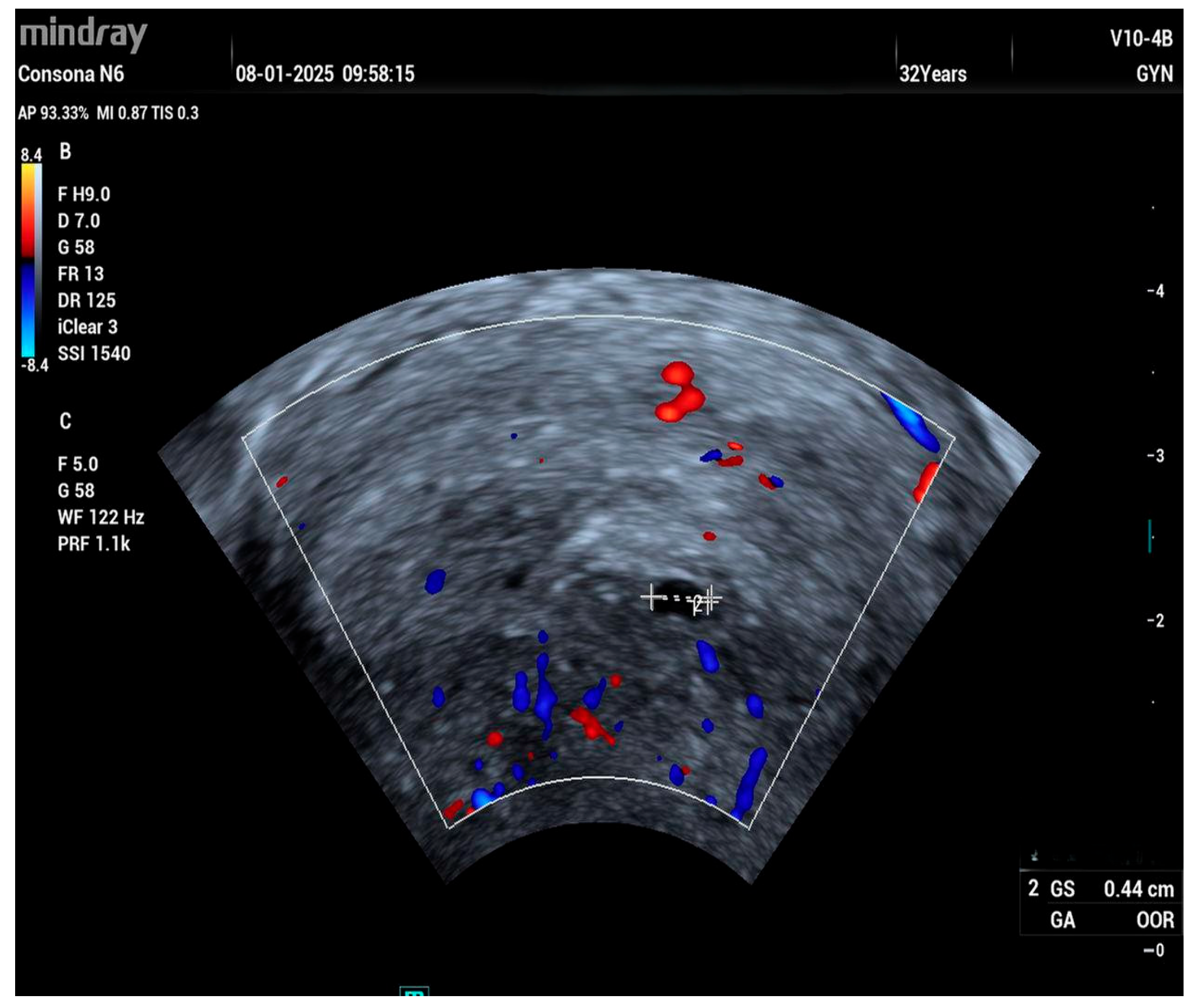
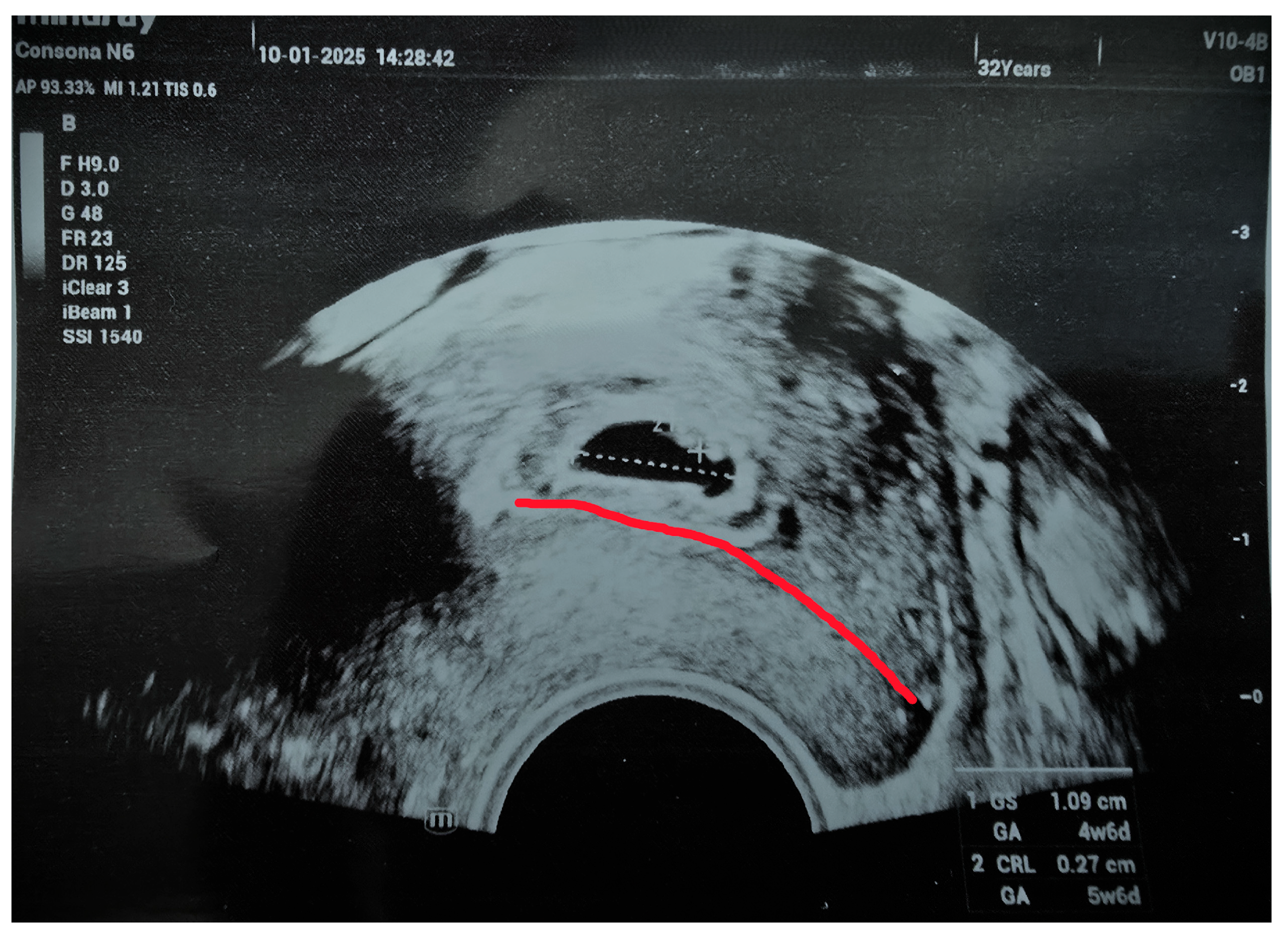
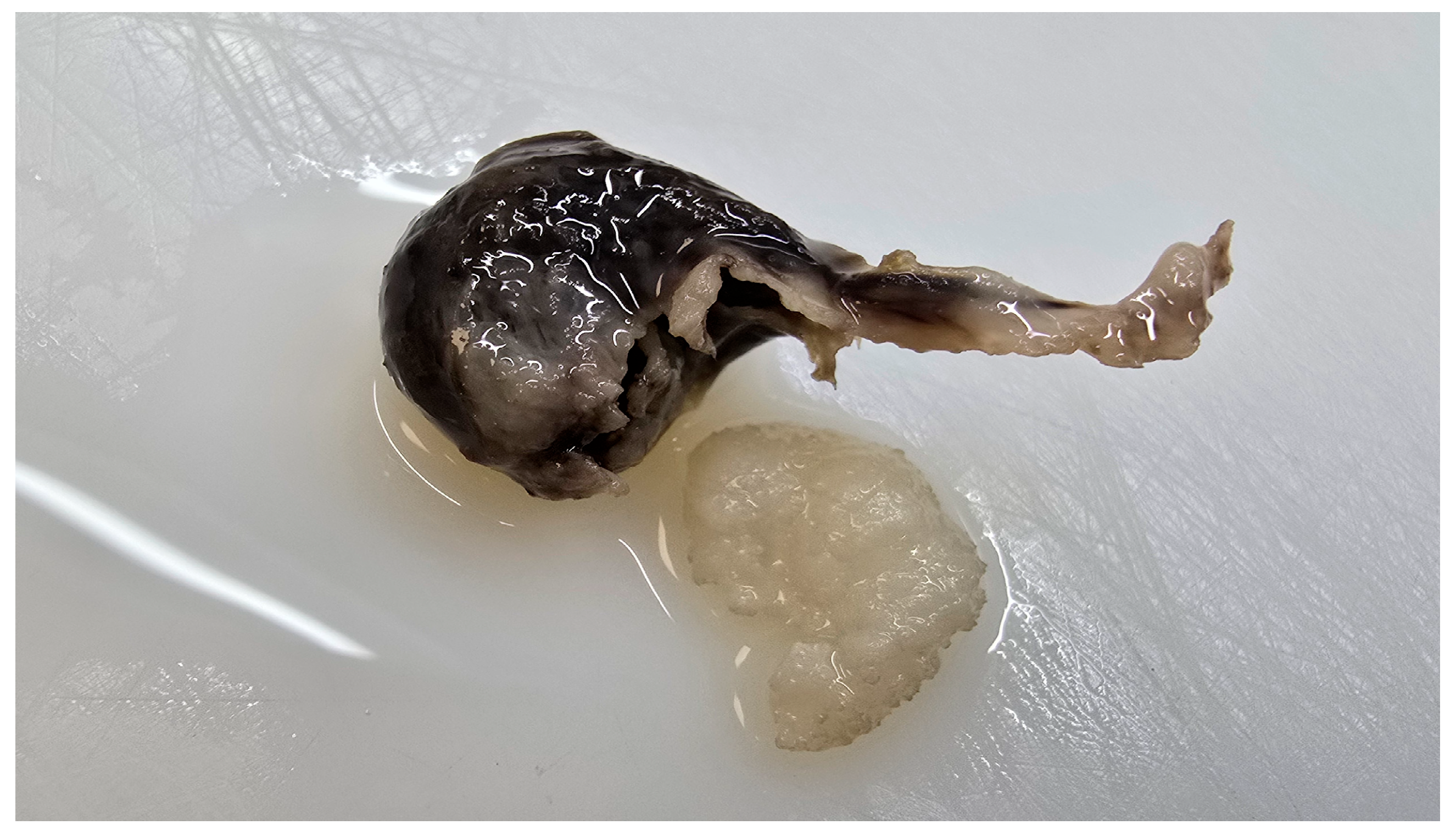
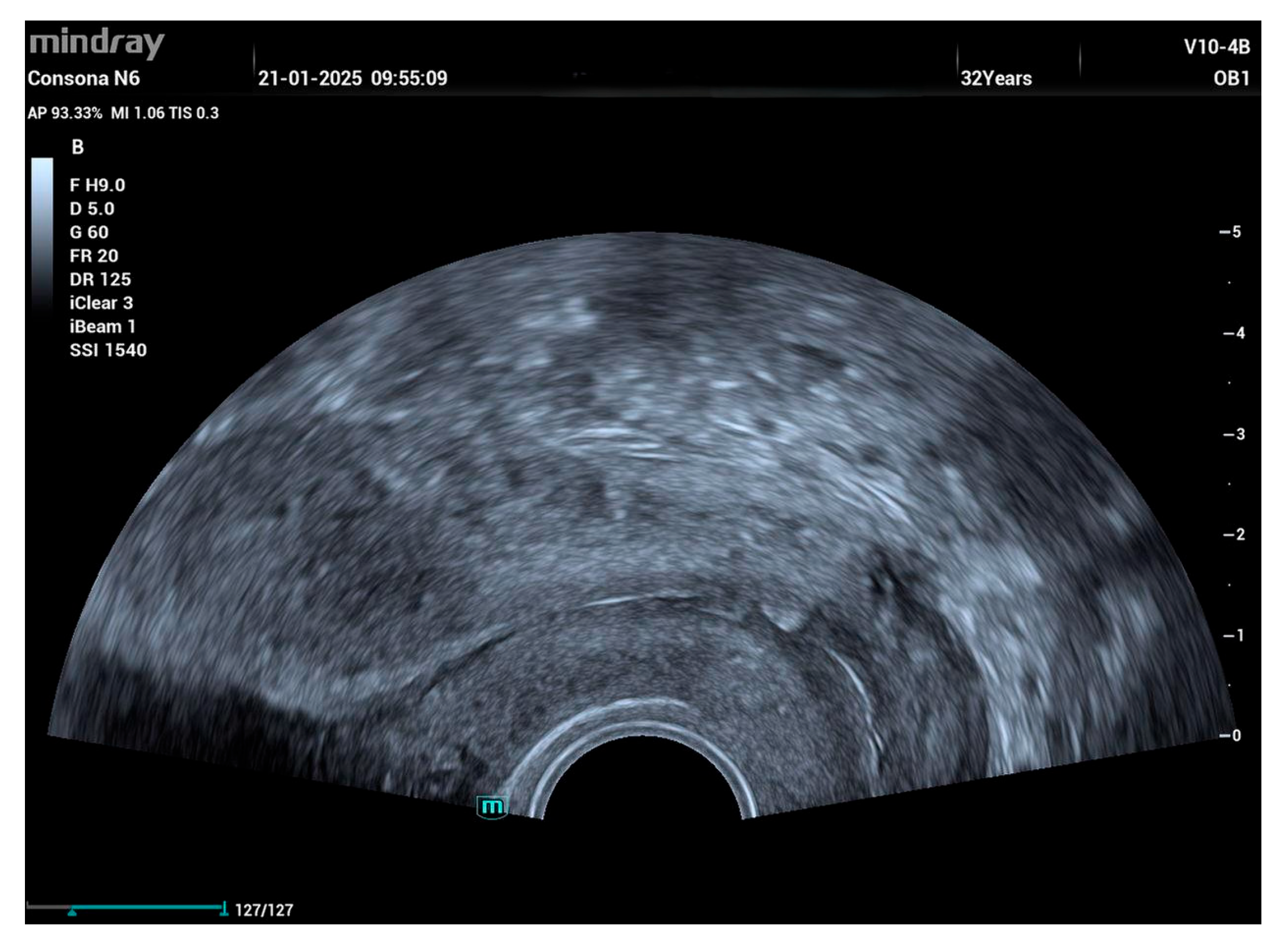
2. Case Report
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Panelli, D.M.; Phillips, C.H.; Brady, P.C. Incidence, diagnosis and management of tubal and nontubal ectopic pregnancies: A review. Fertil. Res. Pract. 2015, 1, 15. [Google Scholar] [CrossRef]
- Faschingbauer, F.; Mueller, A.; Voigt, F.; Beckmann, M.W.; Goecke, T.W. Treatment of heterotopic cervical pregnancies. Fertil. Steril. 2011, 95, 1787.e9–1787.e13. [Google Scholar] [CrossRef]
- Long, Y.; Zhu, H.; Hu, Y.; Shen, L.; Fu, J.; Huang, W. Interventions for non-tubal ectopic pregnancy. Cochrane Database Syst. Rev. 2020, 7, CD011174. [Google Scholar] [CrossRef]
- Chetty, M.; Elson, J. Treating non-tubal ectopic pregnancy. Best Pract. Res. Clin. Obstet. Gynaecol. 2009, 23, 529538. [Google Scholar] [CrossRef] [PubMed]
- Nikolettos, K.; Oikonomou, E.; Kotanidou, S.; Kritsotaki, N.; Kyriakou, D.; Tsikouras, P.; Kontomanolis, E.; Gerede, A.; Nikolettos, N. A Systematic Review about Cervical Pregnancy and our Experience. Acta. Med. Litu. 2024, 31, 92–101. [Google Scholar] [CrossRef] [PubMed]
- Sharma, A.; Ojha, R.; Mondal, S.; Chattopadhyay, S.; Sengupta, P. Cervical intramural pregnancy: Report of a rare case. Niger. Med. J. 2013, 54, 271–273. [Google Scholar] [CrossRef]
- Parker, V.L.; Srinivas, M. Non-tubal ectopic pregnancy. Arch. Gynecol. Obstet. 2016, 294, 19–27. [Google Scholar] [CrossRef] [PubMed]
- Khachani, I.; Alami, M.; Bezad, R. Grossesse cervicale à 7 semaines d’aménorrhée: Défis de la prise en charge. Pan Afr. Med. J. 2017, 26, 11055. [Google Scholar] [CrossRef]
- Hu, J.; Tao, X.; Yin, L.; Shi, Y. Successful conservative treatment of cervical pregnancy with uterine artery embolization followed by curettage: A report of 19 cases. BJOG Int. J. Obstet. Gynaecol. 2016, 123 (Suppl. 3), 97–102. [Google Scholar] [CrossRef]
- Kamwendo, F.; Forslin, L.; Bodin, L.; Danielsson, D. Epidemiology of ectopic pregnancy during a 28 year period and the role of pelvic inflammatory disease. Sex. Transm. Infect. 2000, 76, 28–32. [Google Scholar] [CrossRef]
- Aroche Gutierrez, L.L.; Bunn, J.; Duvernois, G.; Baker, C. Cervical Ectopic Pregnancy: Combination Treatment With Multi-Dose Methotrexate Regimen, Uterine Artery Embolization, and Suction Curettage. Cureus. 2024, 16, e52125. [Google Scholar] [CrossRef]
- Surampudi, K. A case of cervical ectopic pregnancy: Successful therapy with methotrexate. J. Obstet. Gynaecol. India. 2012, 62 (Suppl. 1), 1–3. [Google Scholar] [CrossRef]
- Kirk, E.; Condous, G.; Haider, Z.; Syed, A.; Ojha, K.; Bourne, T. The conservative management of cervical ectopic pregnancies. Ultrasound Obstet. Gynecol. 2006, 27, 430–437. [Google Scholar] [CrossRef]
- Dixit, N.; Venkatesan, S. Cervical Pregnancy: An Uncommon Ectopic Pregnancy. Med. J. Armed. Forces India. 2008, 64, 183–184. [Google Scholar] [CrossRef]
- Rusnell, L.; Lo, K.; Kaderali, S. Hysteroscopic resection of a cervical ectopic pregnancy. J. Obstet. Gynaecol. Can. 2025, 47, 102756. [Google Scholar] [CrossRef]
- Maglic, R.; Rakic, A.; Nikolic, B.; Maglic, D.; Jokanovic, P.; Mihajlovic, S. Management of Cervical Ectopic Pregnancy with Small-Caliber Hysteroscopy. JSLS J. Soc. Laparosc. Robot. Surg. 2021, 25, e2021.00016. [Google Scholar] [CrossRef] [PubMed]
- Di Lorenzo, G.; Mirenda, G.; Springer, S.; Mirandola, M.T.; Mangino, F.P.; Romano, F.; Ricci, G. Hysteroscopic Treatment of Cervical Pregnancy: A Scoping Review of the Literature. J. Minim. Invasive Gynecol. 2022, 29, 345–354.e1. [Google Scholar] [CrossRef] [PubMed]
- Sepúlveda González, G.; Villagómez Martínez, G.E.; Basurto Diaz, D.; Guerra de la Garza Evia, Á.R.; Rosales de León, J.C.; Arroyo Lemarroy, T.; Soria López, J.A. Successful Management of Heterotopic Cervical Pregnancy with Ultrasonographic-guided Laser Ablation. J. Minim. Invasive Gynecol. 2020, 27, 977–980. [Google Scholar] [CrossRef]
- Hosni, M.M.; Herath, R.P.; Mumtaz, R. Diagnostic and therapeutic dilemmas of cervical ectopic pregnancy. Obstet. Gynecol. Surv. 2014, 69, 261–276. [Google Scholar] [CrossRef] [PubMed]
- Choe, J.K.; Baggish, M.S. Hysteroscopic treatment of septate uterus with Neodymium: YAG laser. Fertil. Steril. 1992, 57, 81–84. [Google Scholar] [CrossRef]
- Donnez, J.; Nisolle, M. Endoscopic laser treatment of uterine malformations. Hum. Reprod. 1997, 12, 1381–1387. [Google Scholar] [CrossRef]
- Daniell, J.F.; Osher, S.; Miller, W. Hysteroscopic resection of uterine septi with visible light laser energy. J. Gynecol. Surg. 1987, 3, 217–220. [Google Scholar] [CrossRef]
- Nappi, L.; Pontis, A.; Sorrentino f Greco, P.; Angioni, S. Hysteroscopic Metroplasty for the Septate Uterus with Diode Laser: A pilot study. Eur. J. Obstet. Gynecol. Reprod. Biol. 2016, 206, 32–35. [Google Scholar] [CrossRef]
- Vitale, S.G.; Mikuš, M.; De Angelis, M.C.; Carugno, J.; Riemma, G.; Franušić, L.; Cerovac, A.; D’alterio, M.N.; Nappi, L.; Angioni, S. Diode laser use in hysteroscopic surgery: Current status and future perspectives. Minim. Invasive Ther. Allied. Technol. 2023, 32, 275–284. [Google Scholar] [CrossRef]
- Etrusco, A.; Buzzaccarini, G.; Laganà, A.S.; Chiantera, V.; Vitale, S.G.; Angioni, S.; D’Alterio, M.N.; Nappi, L.; Sorrentino, F.; Vitagliano, A.; et al. Use of Diode Laser in Hysteroscopy for the Management of Intrauterine Pathology: A Systematic Review. Diagnostics 2024, 14, 327. [Google Scholar] [CrossRef]
- Kulkarni, A.V.; Kulkarni, V.M.; Alahabade, R.; Ruikar, P.D.; Kulkarni, A.V. Holmium:YAG laser: A better tool for hysteroscopic septal transection. J. South Asian Fed. Obstet. Gynaecol. 2021, 13, 114–117. [Google Scholar] [CrossRef]
- Holmium: YAG surgical lasers. Health Devices 1995, 24, 92–122.
- Dequesne, J.; Sumner, D. Use of holmium laser in gynecological endoscopic surgery. In Lasers in Gynecology; Bastert, G., Wallwiener, D., Eds.; Springer: Berlin/Heidelberg, Germany, 1992. [Google Scholar]
- Tulikangas, P.K.; Smith, T.; Falcone, T.; Boparai, N.; Walters, M.D. Gross and histologic characteristics of laparoscopic injuries with four different energy sources. Fertil. Steril. 2001, 75, 806–810. [Google Scholar] [CrossRef]
- ESGE Special Interest Group “Innovations” Working Group. Laser in gynaecology−are they still obsolete? Review of past, present and future applications. Facts Views Vis. Obgyn 2020, 12, 63–66. [Google Scholar]
- Kulkarni, A.V.; Kulkarni, V.M.; Alahabade, R.; Ruikar, P.D.; Mahajan, R.; Kulkarni, T.; Giri, D.; Nandana, N. Hysteroscopic Metroplasty Using Holmium: YAG Laser for Treatment of Septate Uterus. J. Minim. Invasive Gynecol. 2024, 31, 271–272. [Google Scholar] [CrossRef] [PubMed]
- Sardana, K.; Garg, V.; Bansal, S.; Sandhu, J.; Daulaguphu, T. Basic of laser-tissue interactions. In Lasers in Dermatological Practice, 1st ed.; Sardana, K., Garg, V., Eds.; Jaypee: New Delhi, India, 2014. [Google Scholar]
- Bhatta, N.; Isaacson, K.; Bhatta, K.M.; Anderson, R.R. Comparative study of different laser systems. Fertil. Steril. 1994, 61, 581–591. [Google Scholar] [CrossRef] [PubMed]
- Stabile, G.; Mangino, F.P.; Romano, F.; Zinicola, G.; Ricci, G. Ectopic Cervical Pregnancy: Treatment Route. Medicina 2020, 56, 293. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cvetkov, D.; Lukanovic, D.; Yordanov, A. Outpatient Hysteroscopic Treatment of Cervical Ectopic Pregnancy in a Primigravida Using the Ho:YAG Laser: A Case Report and Operative Protocol Evaluation. Reprod. Med. 2025, 6, 21. https://doi.org/10.3390/reprodmed6030021
Cvetkov D, Lukanovic D, Yordanov A. Outpatient Hysteroscopic Treatment of Cervical Ectopic Pregnancy in a Primigravida Using the Ho:YAG Laser: A Case Report and Operative Protocol Evaluation. Reproductive Medicine. 2025; 6(3):21. https://doi.org/10.3390/reprodmed6030021
Chicago/Turabian StyleCvetkov, Dimitar, David Lukanovic, and Angel Yordanov. 2025. "Outpatient Hysteroscopic Treatment of Cervical Ectopic Pregnancy in a Primigravida Using the Ho:YAG Laser: A Case Report and Operative Protocol Evaluation" Reproductive Medicine 6, no. 3: 21. https://doi.org/10.3390/reprodmed6030021
APA StyleCvetkov, D., Lukanovic, D., & Yordanov, A. (2025). Outpatient Hysteroscopic Treatment of Cervical Ectopic Pregnancy in a Primigravida Using the Ho:YAG Laser: A Case Report and Operative Protocol Evaluation. Reproductive Medicine, 6(3), 21. https://doi.org/10.3390/reprodmed6030021







