Olfactory Disorders in Post-Acute COVID-19 Syndrome
Abstract
:1. Introduction
2. Epidemiology
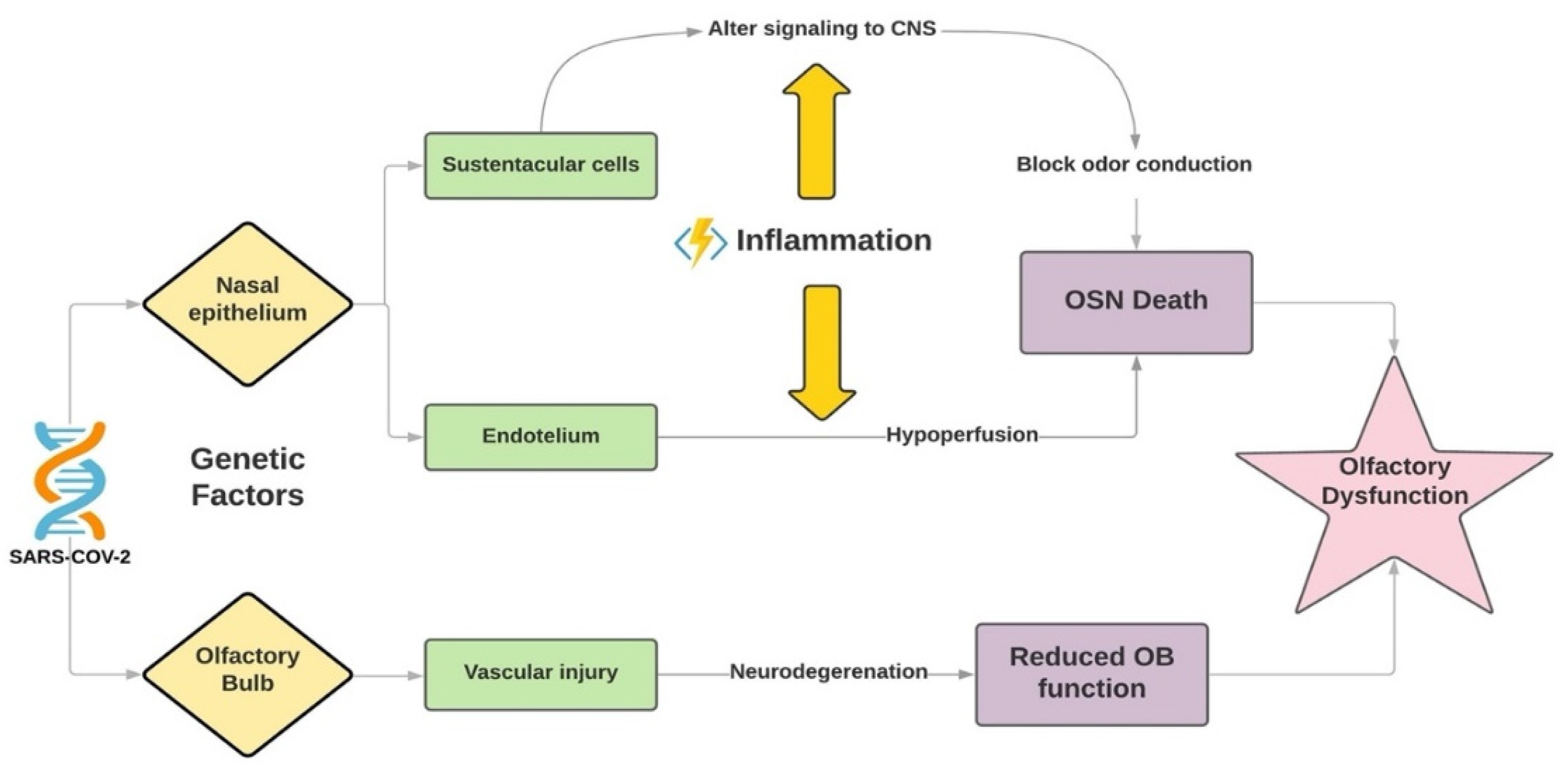
3. Pathophysiogenesis of Olfactory Dysfunction
4. Smell Dysfunction in PACS
5. Clinical Management Considerations
| Author | Country | Setting | Time (Days) | Population | n | Prevalence of Olfactory/Gustatory Dysfunction |
|---|---|---|---|---|---|---|
| Garrigues 2020 [13] | France | Cross sectional, single center | 110.9 | Hospitalized | 120 | Anosmia (13.3%) |
| Chopra 2020 [14] | United States | Prospective cohort, multicenter | 60 | Hospitalized | 488 | Loss of taste and/or smell (28%) |
| Rosales-Castillo 2020 [15] | Spain | Retrospective cohort, single center | 50.8 | Hospitalized | 118 | Anosmia (1.7%) |
| Jacobs 2020 [16] | United States | Prospective cohort, single center | 35 | Hospitalized | 183 | Lack of smell (9.3%) |
| Daher 2020 [37] | Germany | Prospective cohort, single center | 42 | Hospitalized | 33 | Loss of smell (12%) |
| Klein 2020 [38] | Israel | Prospective cohort, single center | 180 | Hospitalized (5.5%) and home-isolated | 112 | Smell changes (9.8%) |
| Moreno-Pérez 2021 [39] | Spain | Prospective cohort, multicenter | 112–126 | Hospitalized (58.2%) and home-isolated | 277 | Anosmia-dysgeusia (21%) |
| Seessle 2021 [40] | Germany | Prospective cohort, single center | 360 | Hospitalized (32.3%) and home-isolated | 96 | Anosmia (20.8%) |
| Tenford 2020 [41] | United States | Cross sectional, multicenter | 14–21 | Home-isolated | 270 | Loss of smell (27%) |
| Boscolo-Rizzo 2020 [42] | Italy | Cross sectional, single center | 28 | Home-isolated | 187 | Altered sense of smell or taste (51.3%) |
| Paderno 2020 [43] | Italy | Prospective cohort, multicenter | 30 | Home-isolated | 151 | Olfactory dysfunction (17.7%) |
| Valiente-De Santis 2020 [44] | Spain | Prospective cohort, single center | 84 | Home-isolated | 108 | Anosmia (9.3%) |
| Otte 2020 [45] | Germany | Cross sectional, single center | 56 | Home-isolated | 80 | Hyposmia (45.1%) |
| Blomberg 2021 [17] | Norway | Prospective cohort, multicenter | 168 | Home-isolated | 247 | Disturbed taste/smell (27%) |
Author Contributions
Funding
Conflicts of Interest
References
- Escandón, K.; Rasmussen, A.L.; Bogoch, I.I.; Murray, E.J.; Escandón, K.; Popescu, S.V.; Kindrachuk, J. COVID-19 false dichotomies and a comprehensive review of the evidence regarding public health, COVID-19 symptomatology, SARS-CoV-2 transmission, mask wearing, and reinfection. BMC Infect. Dis. 2021, 21, 1–47. [Google Scholar] [CrossRef]
- Cevik, M.; Kuppalli, K.; Kindrachuk, J.; Peiris, M. Virology, transmission, and pathogenesis of SARS-CoV-2. BMJ 2020, 371, 1–6. [Google Scholar]
- Centers for Disease Control and Prevention. Interim Clinical Guidance for Management of Patients with Confirmed Coronavirus Disease (COVID-19). Available online: https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-guidance-management-patients.html (accessed on 21 August 2021).
- Keller, A.; Malaspina, D. Hidden consequences of olfactory dysfunction: A patient report series. BMC Ear Nose Throat Disord. 2013, 13. [Google Scholar] [CrossRef] [Green Version]
- Bourgonje, A.R.; Abdulle, A.E.; Timens, W.; Hillebrands, J.L.; Navis, G.J.; Gordijn, S.J.; Bolling, M.C.; Dijkstra, G.; Voors, A.A.; Osterhaus, A.D.; et al. Angiotensin-converting enzyme 2 (ACE2), SARS-CoV-2 and the pathophysiology of coronavirus disease 2019 (COVID-19). J. Pathol. 2020, 251, 228–248. [Google Scholar] [CrossRef]
- Hamming, I.; Timens, W.; Bulthuis, M.L.C.; Lely, A.T.; Navis, G.J.; van Goor, H. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J. Pathol. 2004, 203, 631–637. [Google Scholar] [CrossRef] [PubMed]
- Wu, Z.; McGoogan, J.M. Characteristics of and Important Lessons from the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72314 Cases from the Chinese Center for Disease Control and Prevention. JAMA J. Am. Med. Assoc. 2020, 323, 1239–1242. [Google Scholar] [CrossRef] [PubMed]
- Shah, W.; Hillman, T.; Playford, E.D.; Hishmeh, L. Managing the long term effects of covid-19: Summary of NICE, SIGN, and RCGP rapid guideline. BMJ 2021, 372, n136. [Google Scholar] [CrossRef] [PubMed]
- Tsuchiya, H. Oral symptoms associated with COVID-19 and their pathogenic mechanisms: A literature review. Dent. J. 2021, 9, 32. [Google Scholar] [CrossRef] [PubMed]
- Greenhalgh, T.; Knight, M.; A’Court, C.; Buxton, M.; Husain, L. Management of post-acute covid-19 in primary care. BMJ 2020, 370, m3026. [Google Scholar] [CrossRef]
- Printza, A.; Katotomichelakis, M.; Valsamidis, K.; Metallidis, S.; Panagopoulos, P.; Panopoulou, M.; Petrakis, V.; Constantinidis, J. Smell and Taste Loss Recovery Time in COVID-19 Patients and Disease Severity. J. Clin. Med. 2021, 10, 966. [Google Scholar] [CrossRef]
- Parma, V.; Ohla, K.; Veldhuizen, M.G.; Niv, M.Y.; Kelly, C.E.; Bakke, A.J.; Cooper, K.W.; Bouysset, C.; Pirastu, N.; Dibattista, M. More than smell—COVID-19 is associated with severe impairment of smell, taste, and chemesthesis. Chem. Senses 2020, 45, 609–622. [Google Scholar] [CrossRef]
- Garrigues, E.; Janvier, P.; Kherabi, Y.; Le Bot, A.; Hamon, A.; Gouze, H.; Doucet, L.; Berkani, S.; Oliosi, E.; Mallart, E.; et al. Post-discharge persistent symptoms and health-related quality of life after hospitalization for COVID-19. J. Infect. 2020, 81, e4–e6. [Google Scholar] [CrossRef] [PubMed]
- Chopra, V.; Flanders, S.A.; O’Malley, M.; Malani, A.N.; Prescott, H.C. Sixty-day outcomes among patients hospitalized wed. Am. J. Physiol. Cell Physiol. 2020, 319, 945. [Google Scholar]
- Rosales-Castillo, A.; García de los Ríos, C.; Mediavilla García, J.D. Persistent symptoms after acute COVID-19 infection: Importance of follow-up. Med. Clínica Engl. Ed. 2021, 156, 35–36. [Google Scholar]
- Jacobs, L.G.; Paleoudis, E.G.; Di Bari, D.L.; Nyirenda, T.; Friedman, T.; Gupta, A.; Rasouli, L.; Zetkulic, M.; Balani, B.; Ogedegbe, C.; et al. Persistence of symptoms and quality of life at 35 days after hospitalization for COVID-19 infection. PLoS ONE 2020, 15, e0243882. [Google Scholar] [CrossRef] [PubMed]
- Blomberg, B.; Mohn, K.G.I.; Brokstad, K.A.; Zhou, F.; Linchausen, D.W.; Hansen, B.A.; Lartey, S.; Onyango, T.B.; Kuwelker, K.; Sævik, M.; et al. Long COVID in a prospective cohort of home-isolated patients. Nat. Med. 2021, 23, 1–7. [Google Scholar]
- Makaronidis, J.; Firman, C.; Magee, C.G.; Mok, J.; Balogun, N.; Lechner, M.; Carnemolla, A.; Batterham, R.L. Distorted chemosensory perception and female sex associate with persistent smell and/or taste loss in people with SARS-CoV-2 antibodies: A community based cohort study investigating clinical course and resolution of acute smell and/or taste loss in people. BMC Infect. Dis. 2021, 21, 221. [Google Scholar] [CrossRef] [PubMed]
- Okada, Y.; Yoshimura, K.; Toya, S.; Tsuchimochi, M. Pathogenesis of taste impairment and salivary dysfunction in COVID-19 patients. Jpn. Dent. Sci. Rev. 2021, 57, 111–122. [Google Scholar] [CrossRef]
- Brann, D.H.; Tsukahara, T.; Weinreb, C.; Lipovsek, M.; Van Den Berge, K.; Gong, B.; Chance, R.; Macaulay, I.C.; Chou, H.J.; Fletcher, R.B.; et al. Non-neuronal expression of SARS-CoV-2 entry genes in the olfactory system suggests mechanisms underlying COVID-19-associated anosmia. Sci. Adv. 2020, 6, eabc5801. [Google Scholar] [CrossRef]
- Wang, F.; Kream, R.M.; Stefano, G.B. Long-term respiratory and neurological sequelae of COVID-19. Med. Sci. Monit. 2020, 26, e928996. [Google Scholar] [PubMed]
- Kapoor, D.; Verma, N.; Gupta, N.; Goyal, A. Post Viral Olfactory Dysfunction After SARS-CoV-2 Infection: Anticipated Post-pandemic Clinical Challenge. Indian J. Otolaryngol. Head Neck Surg. 2021, 1–8. [Google Scholar] [CrossRef]
- Doty, R.L. The olfactory system and Its disorders. Semin Neurol. 2009, 29, 74–81. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rashid, R.A.; Alaqeedy, A.A.; Al-Ani, R.M. Parosmia Due to COVID-19 Disease: A 268 Case Series. Indian J. Otolaryngol. Head Neck Surg. 2021, 1–8. [Google Scholar] [CrossRef]
- Marchese-Ragona, R.; Ottaviano, G.; Piero, N.; Vianello, A.; Miryam, C. Sudden hyposmia as a prevalent symptom of COVID-19 infection. medRxiv 2020. [Google Scholar] [CrossRef] [Green Version]
- Guedj, E.; Campion, J.Y.; Dudouet, P.; Kaphan, E.; Bregeon, F.; Tissot-Dupont, H.; Guis, S.; Barthelemy, F.; Habert, P.; Ceccaldi, M.; et al. 18F-FDG brain PET hypometabolism in patients with long COVID. Eur. J. Nucl. Med. Mol. Imaging 2021, 48, 2823–2833. [Google Scholar] [CrossRef] [PubMed]
- Yousefi-Koma, A.; Haseli, S.; Bakhshayeshkaram, M.; Raad, N.; Karimi-Galougahi, M. Multimodality Imaging With PET/CT and MRI Reveals Hypometabolism in Tertiary Olfactory Cortex in Parosmia of COVID-19. Acad. Radiol. 2021, 28, 749–751. [Google Scholar] [CrossRef] [PubMed]
- Xydakis, M.S.; Albers, M.W.; Holbrook, E.H.; Lyon, D.M.; Shih, R.Y.; Frasnelli, J.A.; Pagenstecher, A.; Kupke, A.; Enquist, L.W.; Perlman, S. Post-viral effects of COVID-19 in the olfactory system and their implications. Lancet Neurol. 2021, 20, 753–761. [Google Scholar] [CrossRef]
- Mehraeen, E.; Behnezhad, F.; Salehi, M.A.; Noori, T.; Harandi, H.; SeyedAlinaghi, S.A. Olfactory and gustatory dysfunctions due to the coronavirus disease (COVID-19): A review of current evidence. Eur. Arch. Oto-Rhino-Laryngol. 2021, 278, 307–312. [Google Scholar] [CrossRef]
- Crook, H.; Raza, S.; Nowell, J.; Young, M.; Edison, P. Long covid—Mechanisms, risk factors, and management. BMJ 2021, 374. [Google Scholar] [CrossRef]
- Whitcroft, K.L.; Hummel, T. Olfactory Dysfunction in COVID-19: Diagnosis and Management. JAMA J. Am. Med. Assoc. 2020, 323, 2512–2514. [Google Scholar] [CrossRef]
- Hummel, T.; Reden, K.R.J.; Hähner, A.; Weidenbecher, M.; Hüttenbrink, K.B. Effects of olfactory Training in patients with olfactory loss. Laryngoscope 2009, 119, 496–499. [Google Scholar] [CrossRef]
- Oleszkiewicz, A.; Heyne, L.; Sienkiewicz-Oleszkiewicz, B.; Cuevas, M.; Haehner, A.; Hummel, T. Odours count: Human olfactory ecology appears to be helpful in the improvement of the sense of smell. Sci. Rep. 2021, 11, 16888. [Google Scholar] [CrossRef] [PubMed]
- Liu, D.T.; Sabha, M.; Damm, M.; Philpott, C.; Oleszkiewicz, A.; Hähner, A.; Hummel, T. Parosmia is Associated with Relevant Olfactory Recovery After Olfactory Training. Laryngoscope 2021, 131, 618–623. [Google Scholar] [CrossRef] [PubMed]
- Abdelalim, A.A.; Mohamady, A.A.; Elsayed, R.A.; Elawady, M.A.; Ghallab, A.F. Corticosteroid nasal spray for recovery of smell sensation in COVID-19 patients: A randomized controlled trial. Am. J. Otolaryngol. 2021, 42, 102884. [Google Scholar] [CrossRef] [PubMed]
- Bousquet, J.; Akdis, C.A.; Jutel, M.; Bachert, C.; Klimek, L.; Agache, I.; Ansotegui, I.J.; Bedbrook, A.; Bosnic-Anticevich, S.; Canonica, G.W.; et al. Intranasal corticosteroids in allergic rhinitis in COVID-19 infected patients: An ARIA-EAACI statement. Allergy Eur. J. Allergy Clin. Immunol. 2020, 75, 2440–2444. [Google Scholar] [CrossRef] [PubMed]
- Daher, A.; Balfanz, P.; Cornelissen, C.; Müller, A.; Bergs, I.; Marx, N.; Müller-Wieland, D.; Hartmann, B.; Dreher, M.; Müller, T. Follow up of patients with severe coronavirus disease 2019 (COVID-19): Pulmonary and extrapulmonary disease sequelae. Respir. Med. 2020, 174, 106197. [Google Scholar] [CrossRef]
- Hadar, K.; Kim, A.; Noam, K.; Yuval, B.; Ran, N.P.; Mordechai, M.; Sarah, I.; Masha, Y.N. Onset, duration, and persistence of taste and smell changes and other COVID-19 symptoms: Longitudinal study in Israeli patients. MedRxiv 2020. [Google Scholar] [CrossRef]
- Moreno-Pérez, O.; Merino, E.; Leon-Ramirez, J.M.; Andres, M.; Ramos, J.M.; Arenas-Jiménez, J.; Asensio, S.; Sanchez, R.; Ruiz-Torregrosa, P.; Galan, I.; et al. Post-acute COVID-19 syndrome. Incidence and risk factors: A Mediterranean cohort study. J. Infect. 2021, 82, 378–383. [Google Scholar] [CrossRef]
- Seeßle, J.; Waterboer, T.; Hippchen, T.; Simon, J.; Kirchner, M.; Lim, A.; Müller, B.; Merle, U. Persistent symptoms in adult patients one year after COVID-19: A prospective cohort study. Clin. Infect. Dis. 2021. [Google Scholar] [CrossRef]
- Tenforde, M.W.; Kim, S.S.; Lindsell, C.J.; Erica, B.R.; Nathan, I.S.; Clark, F.D.; Kevin, W.G.; Heidi, L.E.; Jay, S.S.; Howard, A.S.; et al. Symptom duration and risk factors for delayed return to usual health among outpatients with COVID-19 in a multistate health care systems network—United States, March-June 2020. MMWR Morb. Mortal Wkly. Rep. 2020, 69, 993–998. [Google Scholar] [CrossRef]
- Boscolo-Rizzo, P.; Borsetto, D.; Fabbris, C.; Spinato, G.; Frezza, D.; Menegaldo, A.; Mularoni, F.; Gaudioso, P.; Cazzador, D.; Marciani, S.; et al. Evolution of Altered Sense of Smell or Taste in Patients With Mildly Symptomatic COVID-19. JAMA Otolaryngol. Head Neck Surg. 2020, 146, 729–732. [Google Scholar] [CrossRef]
- Paderno, A.; Mattavelli, D.; Rampinelli, V.; Grammatica, A.; Raffetti, E.; Tomasoni, M.; Gualtieri, T.; Taboni, S.; Zorzi, S.; Del Bon, F.; et al. Olfactor and gustatory outcomes in COVID-19: A prospective evaluation in nonhospitalized subjects. Otolaryngol.–Head Neck Surg. 2020, 163, 1144–1149. [Google Scholar] [CrossRef] [PubMed]
- Lucía, V.D.S.; Inés, P.C.; Beatriz, S.; Gracia, E.G.; Juan, D.R.M.; Antonio, P.; Ignacio, M.G.; Marcial, D.F.; Manuel, C.; Francisco, O.; et al. Clinical and immunoserological status 12 weeks after infection with COVID-19: Prospective observational study. MedRxiv 2020. [Google Scholar] [CrossRef]
- Otte, M.S.; Eckel, H.N.C.; Poluschkin, L.; Klussmann, J.P.; Luers, J.C. Olfactory dysfunction in patients after recovering from COVID-19. Acta Otolaryngol. 2020, 140, 1032–1035. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Araújo, L.; Arata, V.; Figueiredo, R.G. Olfactory Disorders in Post-Acute COVID-19 Syndrome. Sinusitis 2021, 5, 116-122. https://doi.org/10.3390/sinusitis5020012
Araújo L, Arata V, Figueiredo RG. Olfactory Disorders in Post-Acute COVID-19 Syndrome. Sinusitis. 2021; 5(2):116-122. https://doi.org/10.3390/sinusitis5020012
Chicago/Turabian StyleAraújo, Laura, Vanessa Arata, and Ricardo G. Figueiredo. 2021. "Olfactory Disorders in Post-Acute COVID-19 Syndrome" Sinusitis 5, no. 2: 116-122. https://doi.org/10.3390/sinusitis5020012
APA StyleAraújo, L., Arata, V., & Figueiredo, R. G. (2021). Olfactory Disorders in Post-Acute COVID-19 Syndrome. Sinusitis, 5(2), 116-122. https://doi.org/10.3390/sinusitis5020012





