The Digital Integrated Workflow in the Aesthetic Management of the Smile: A Case Report
Abstract
1. Introduction
2. Materials and Methods
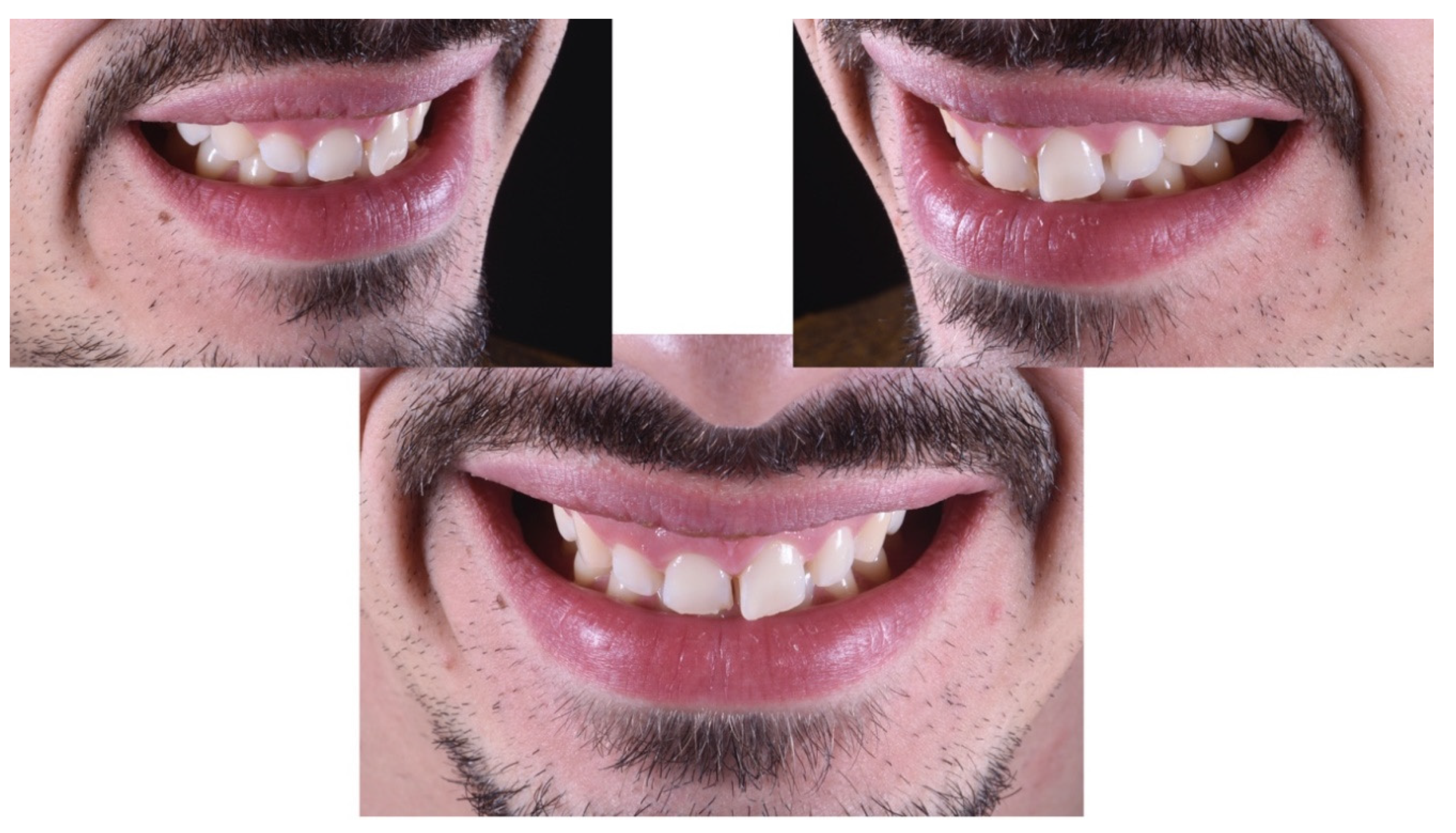
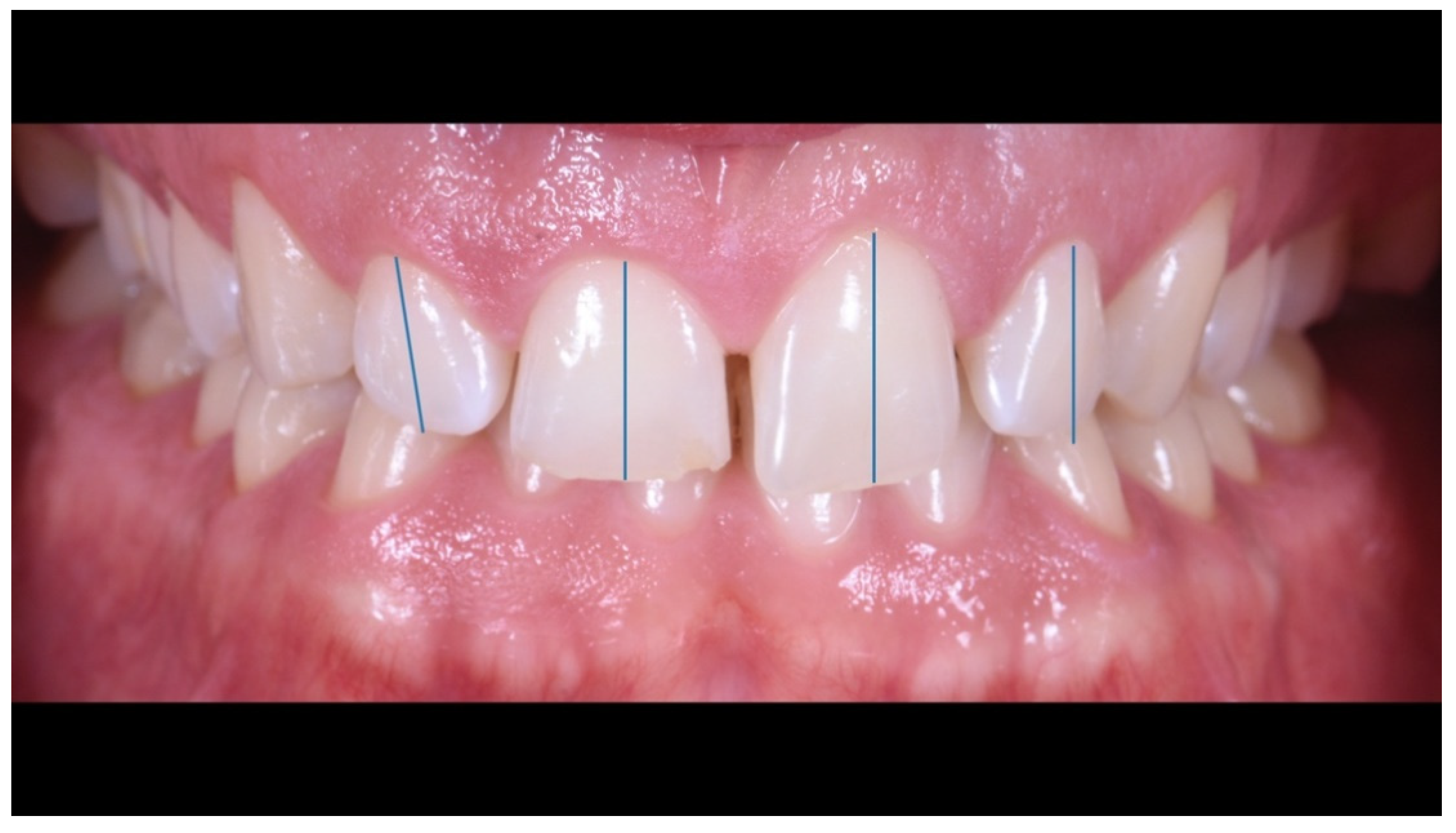
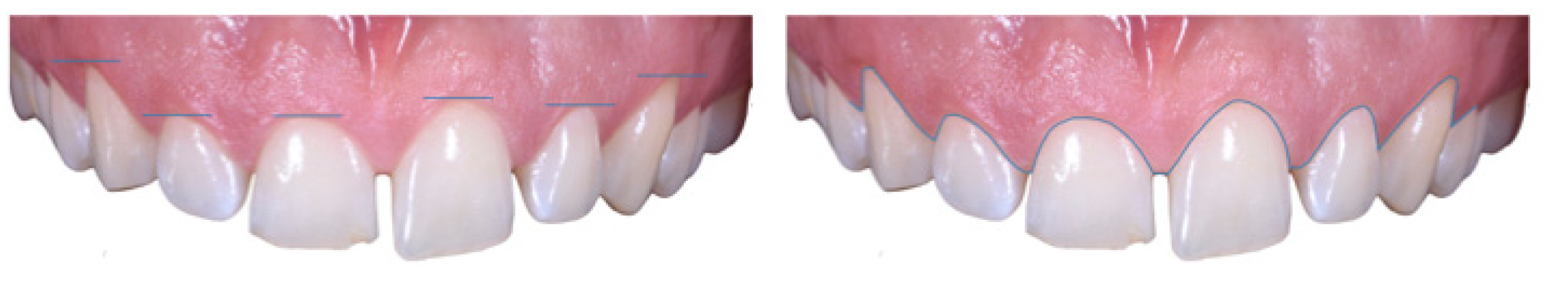
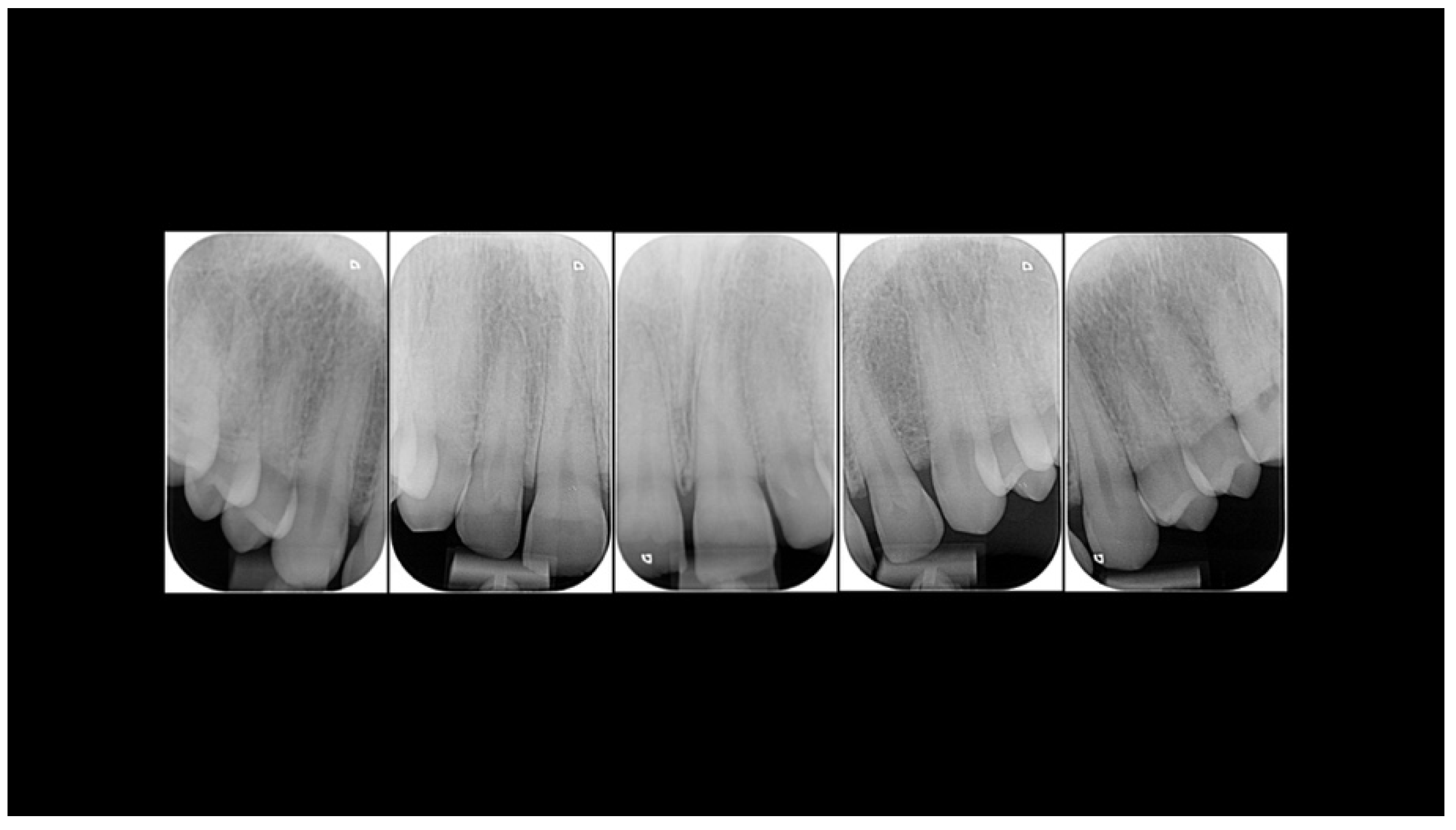
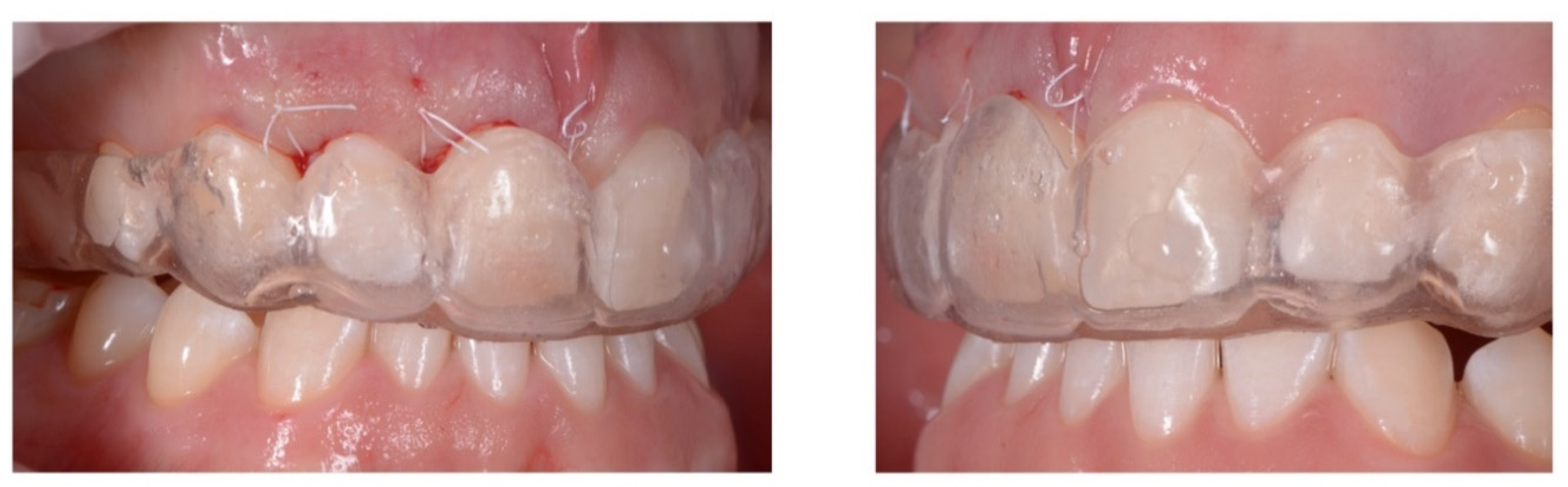
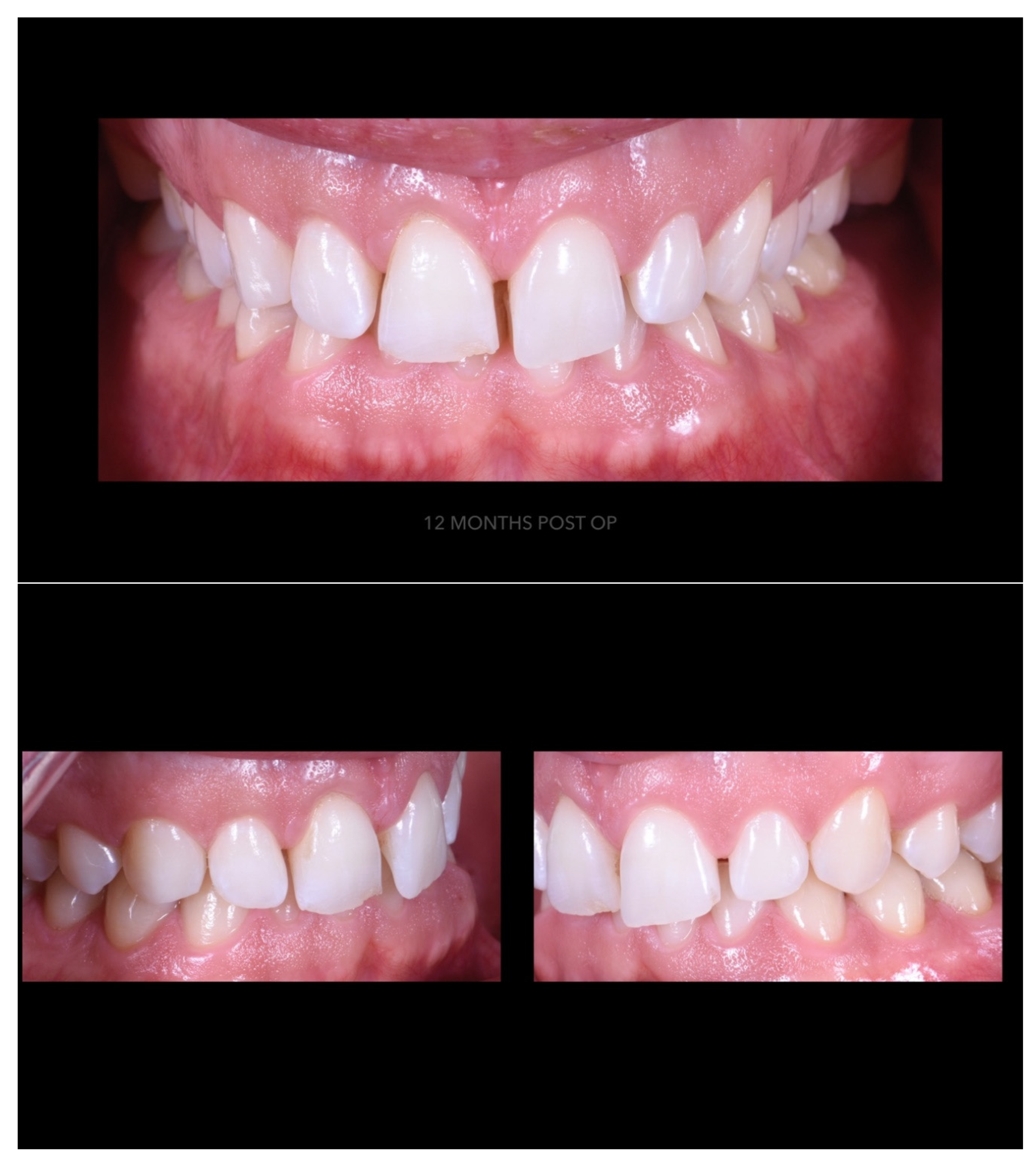
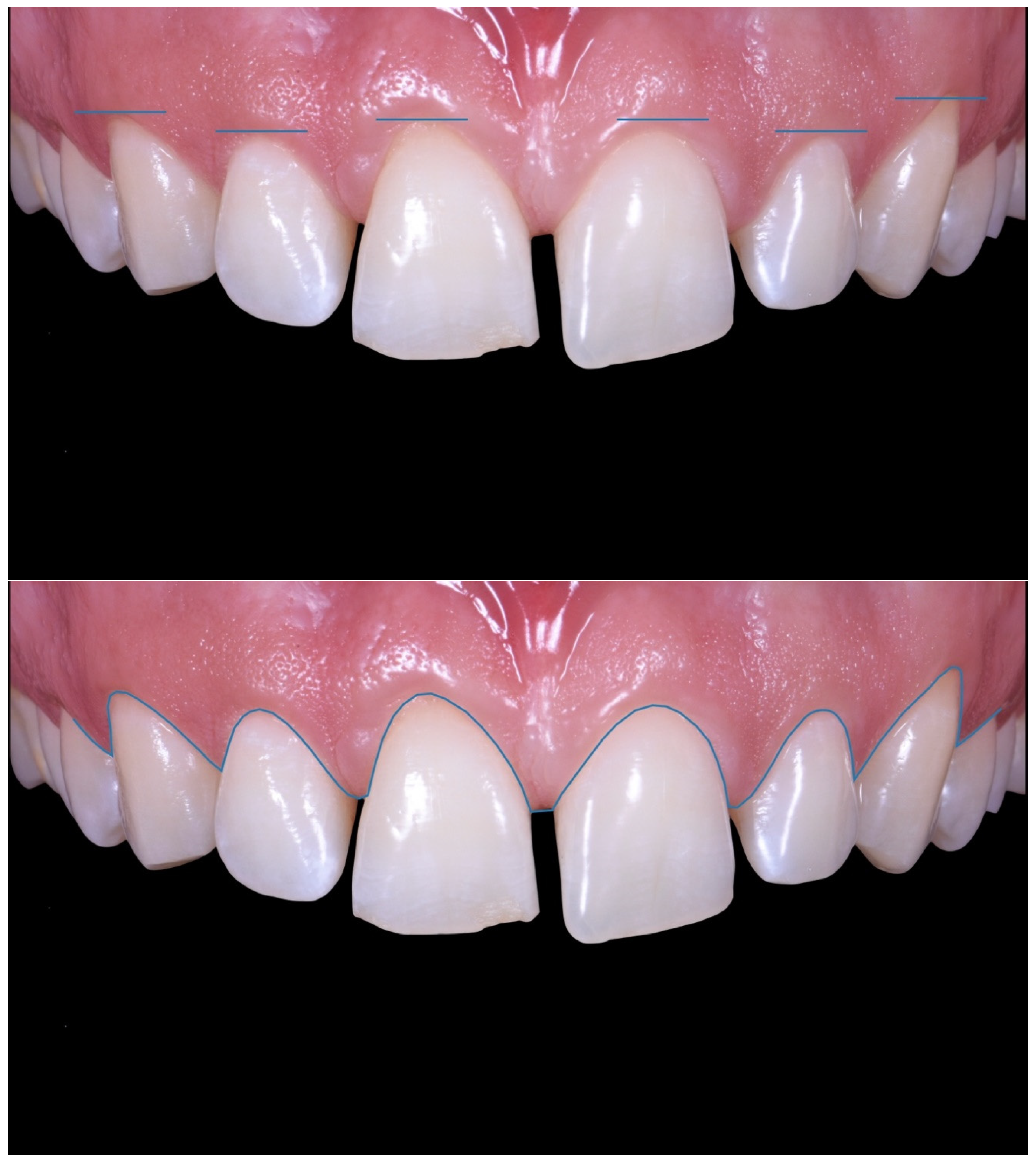
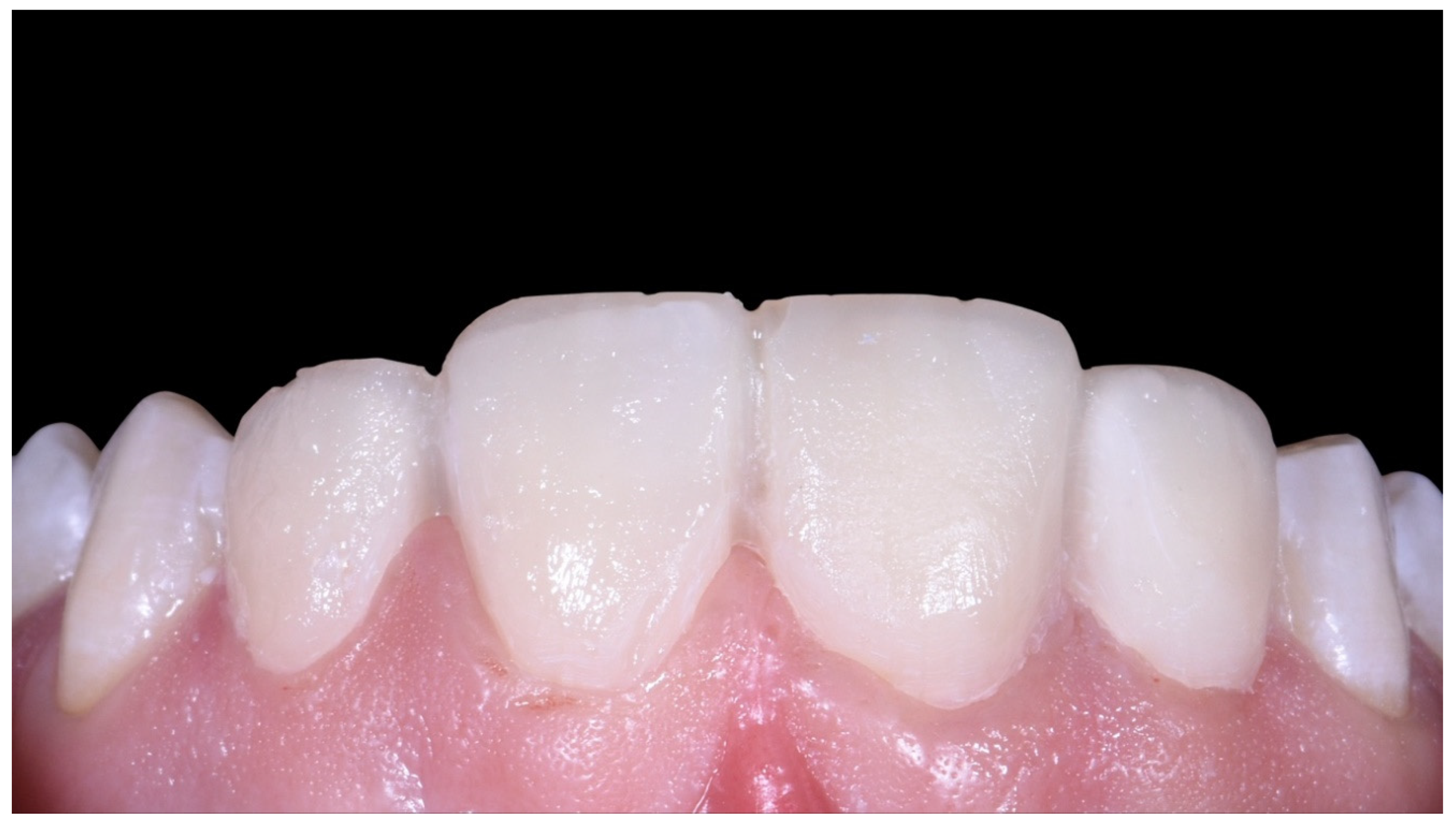
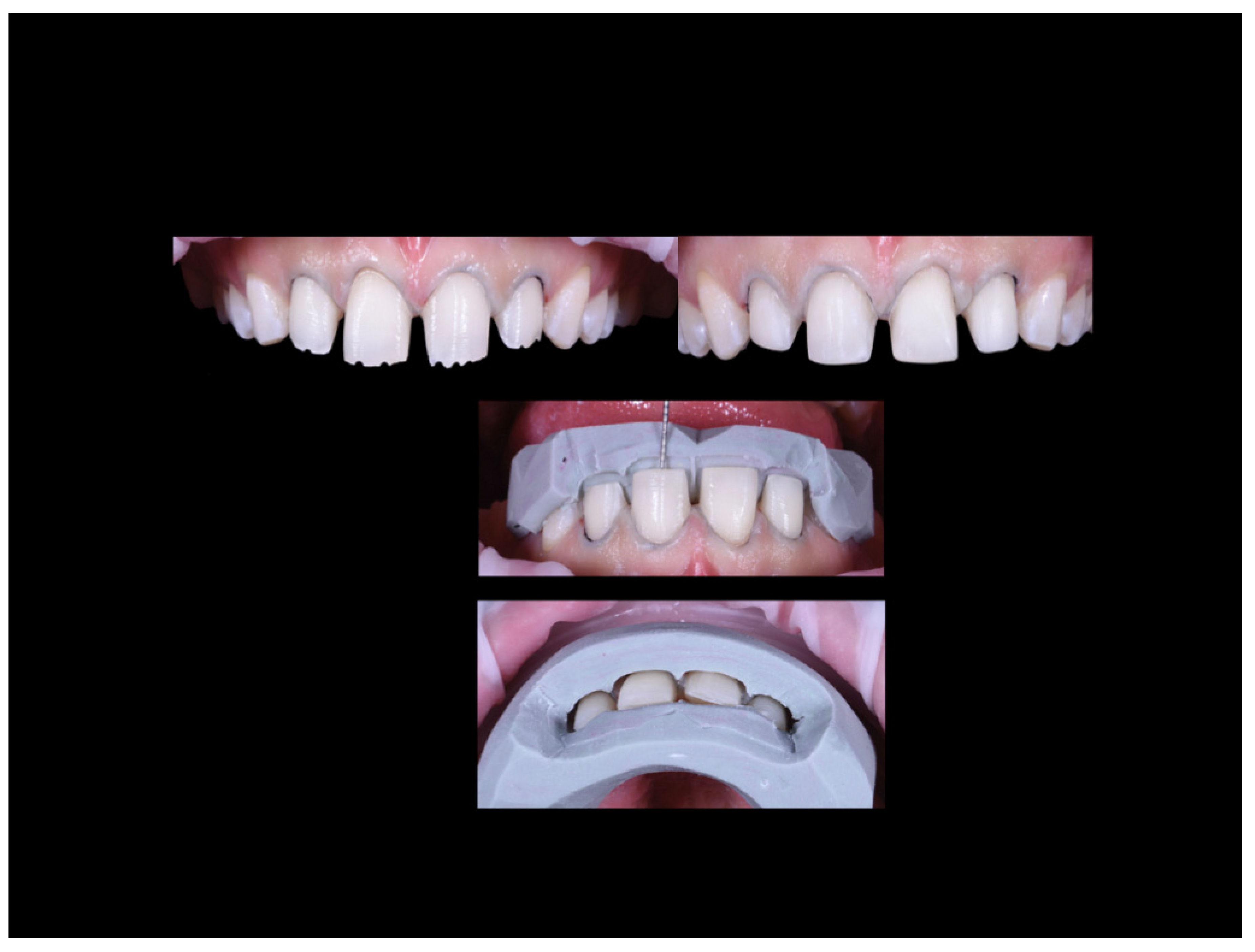
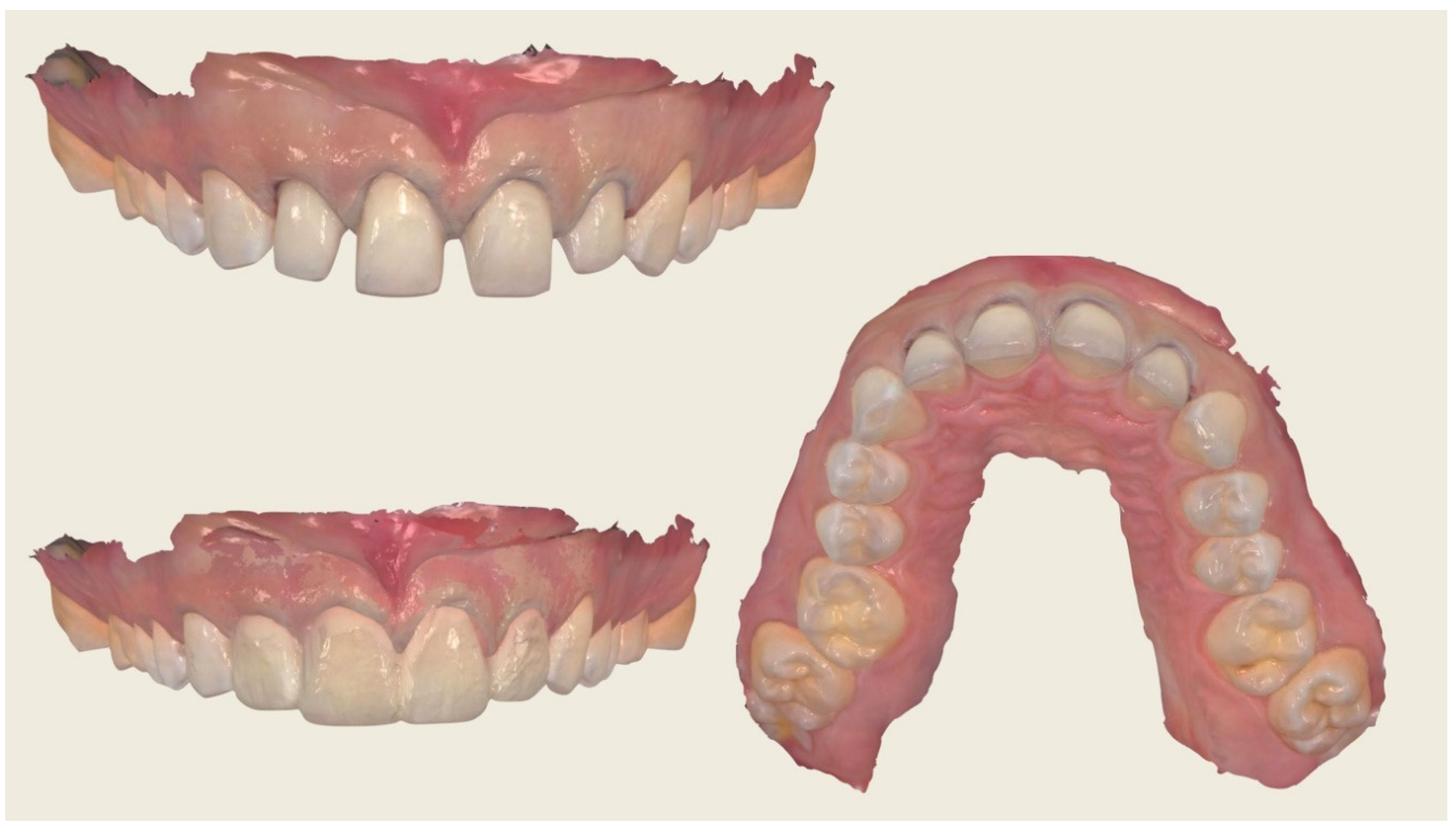
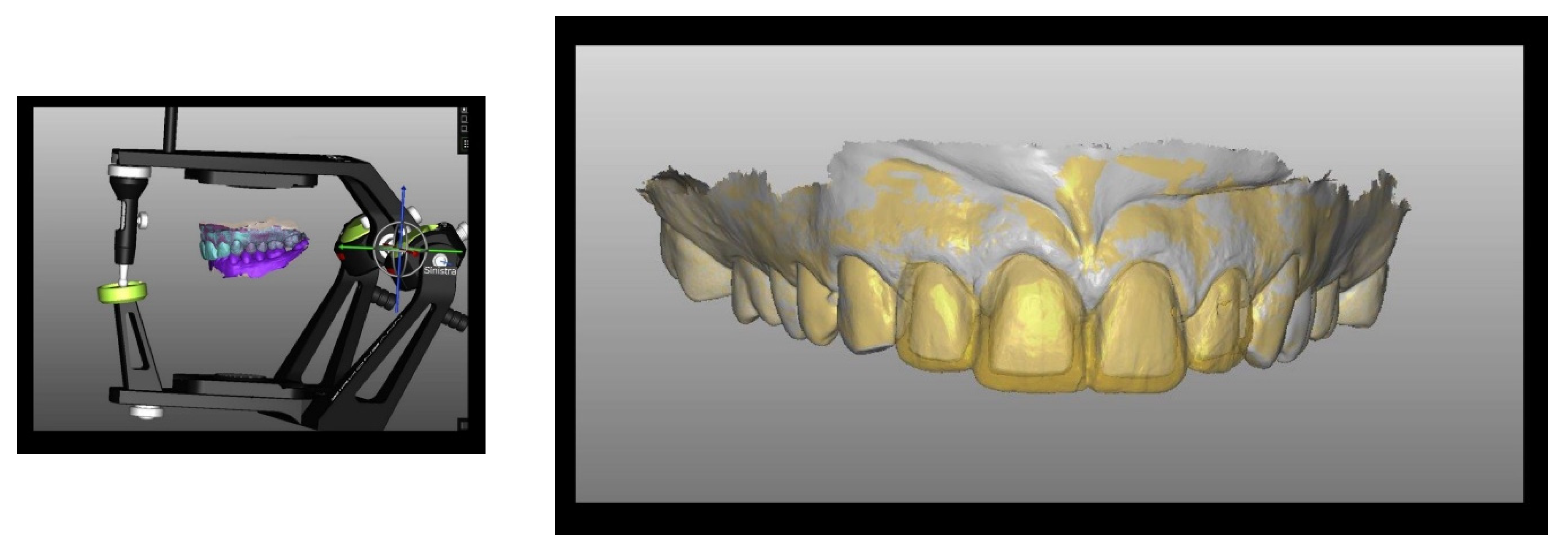
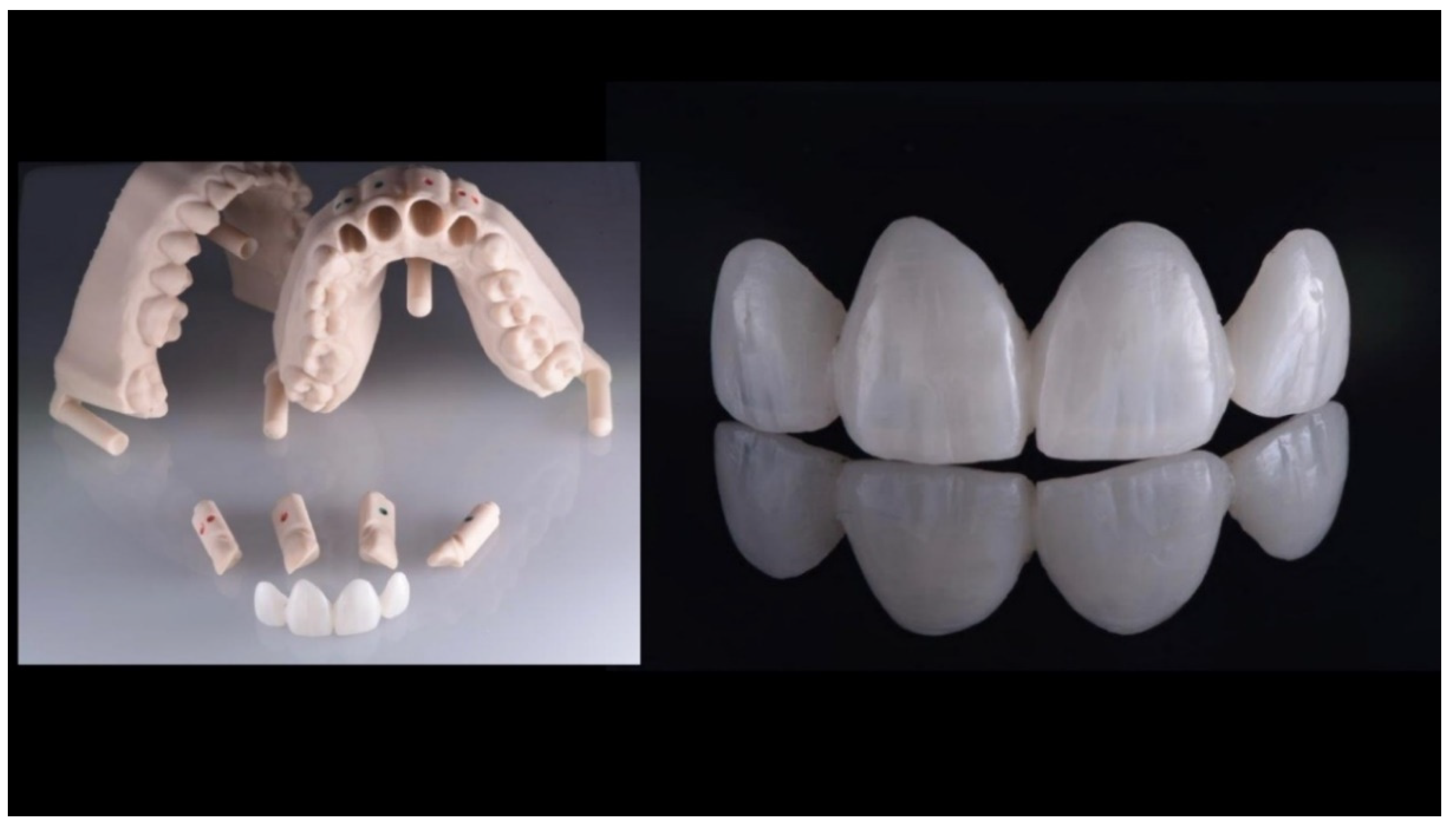
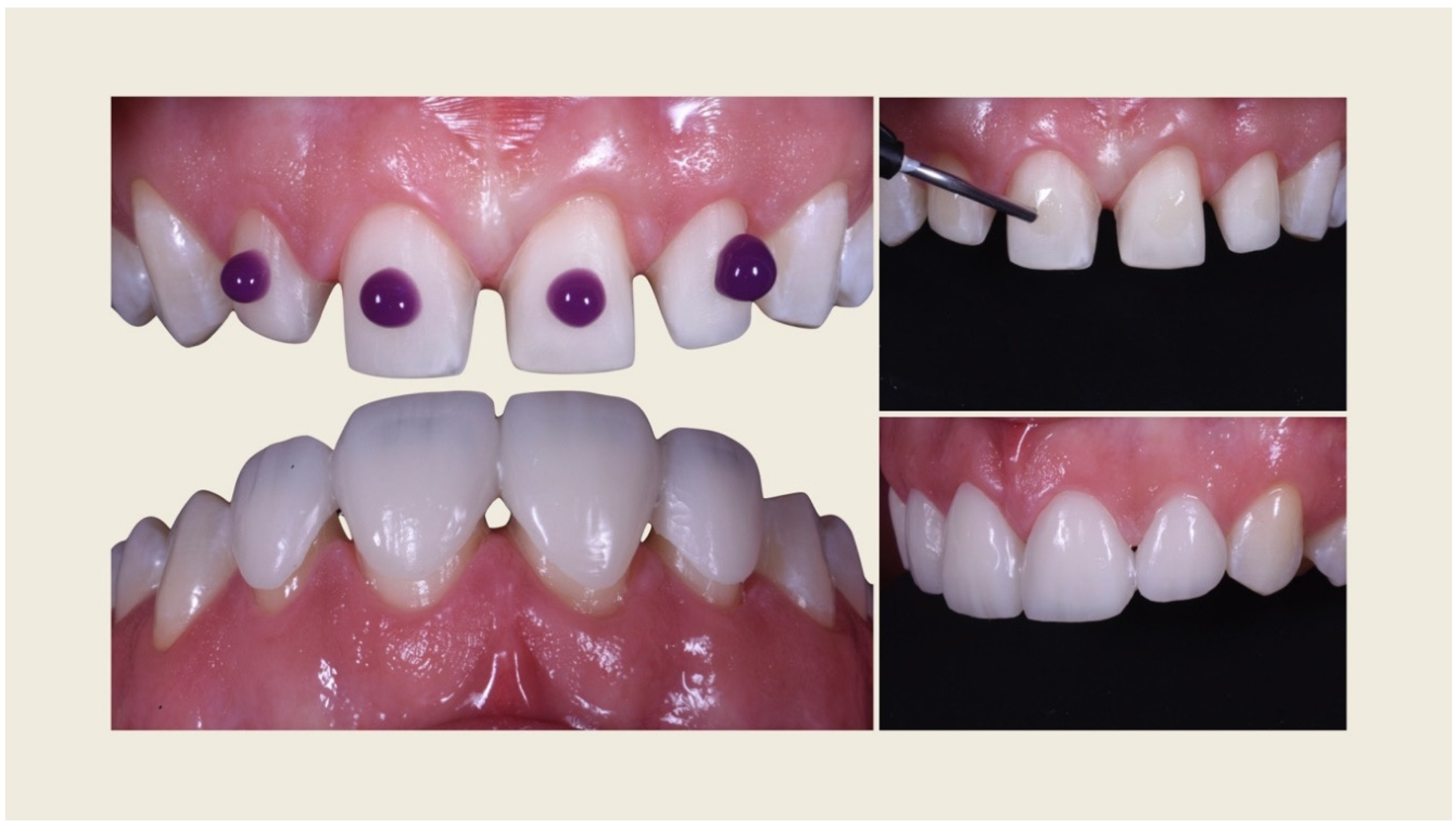
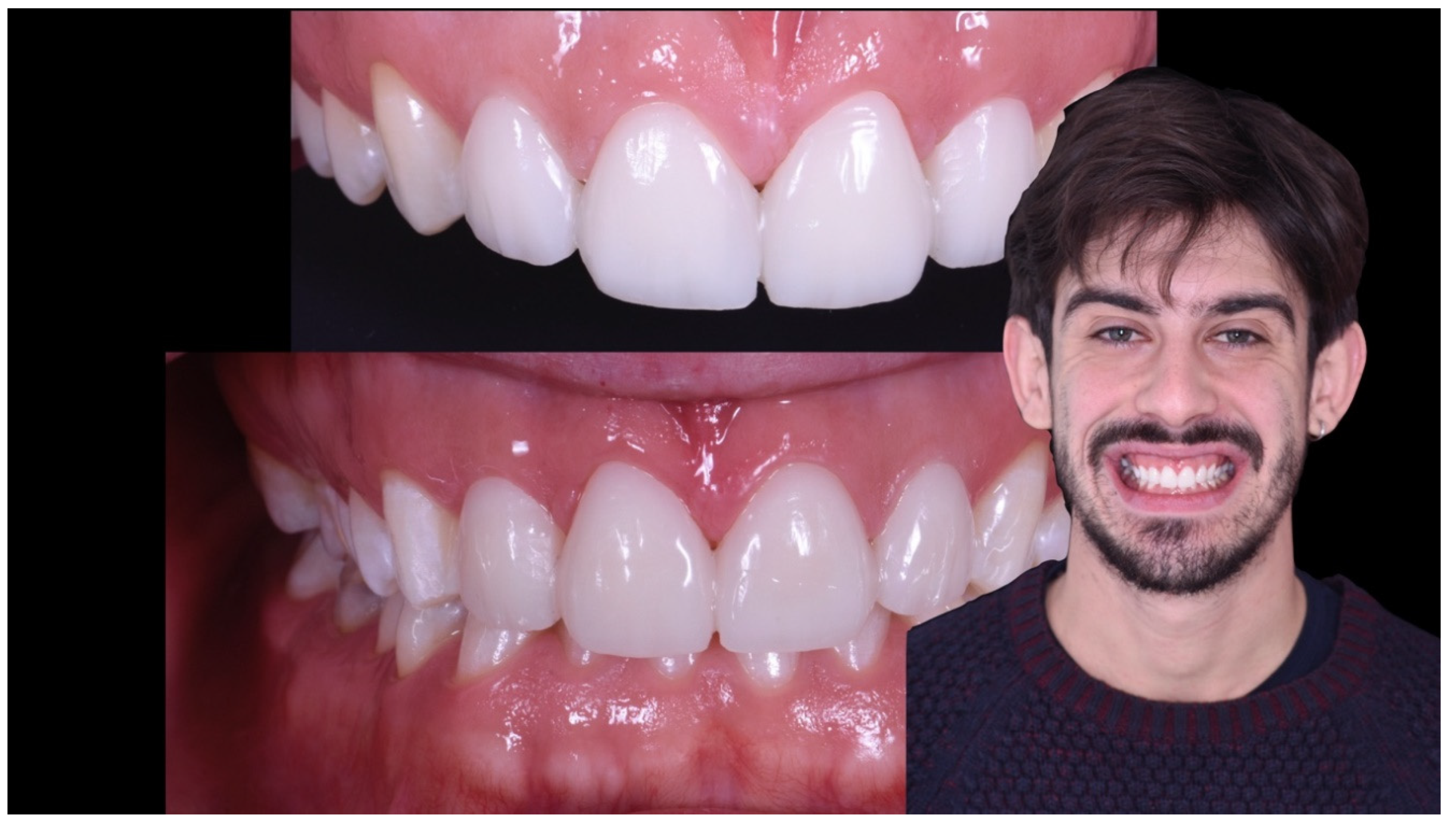
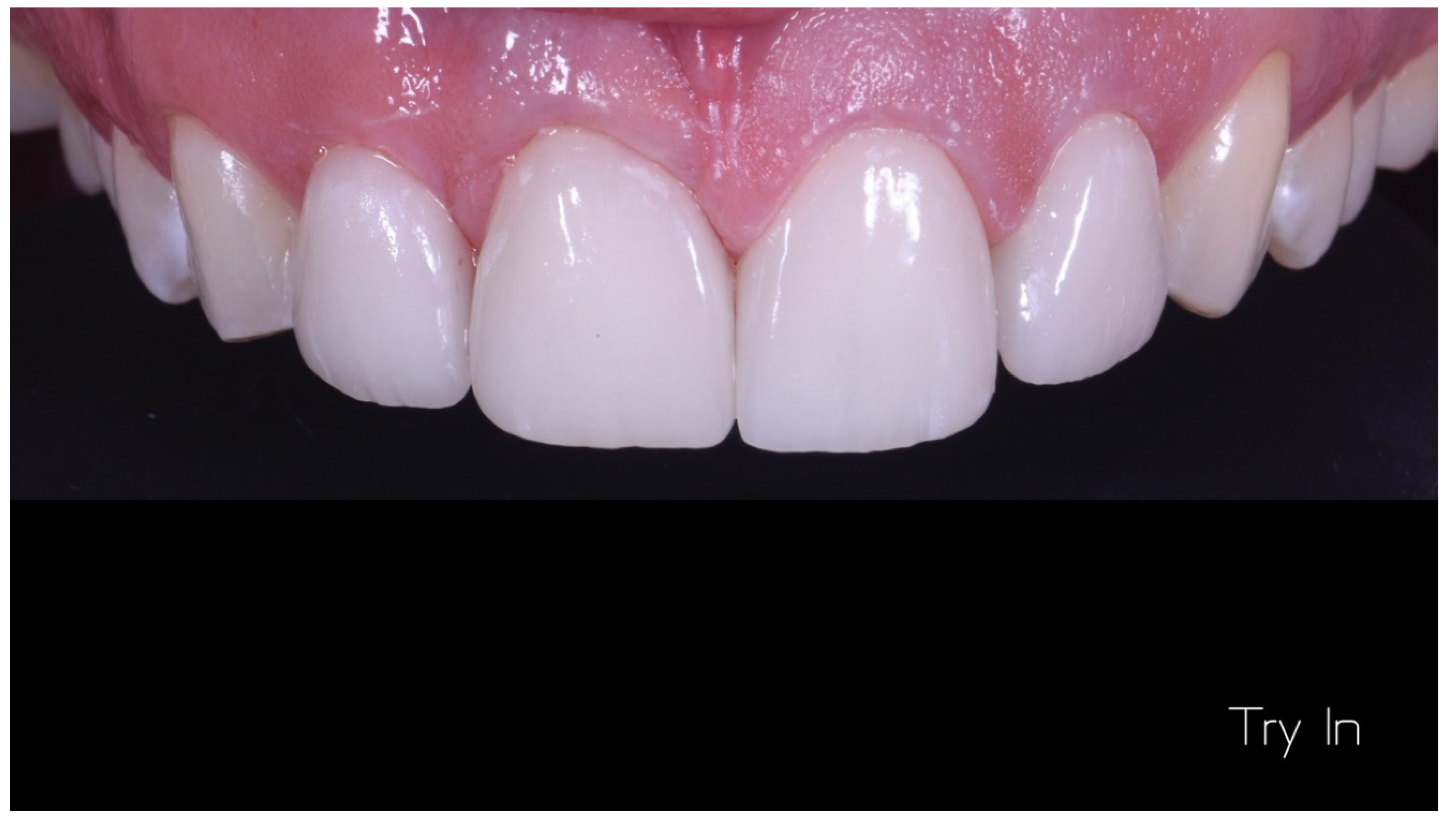
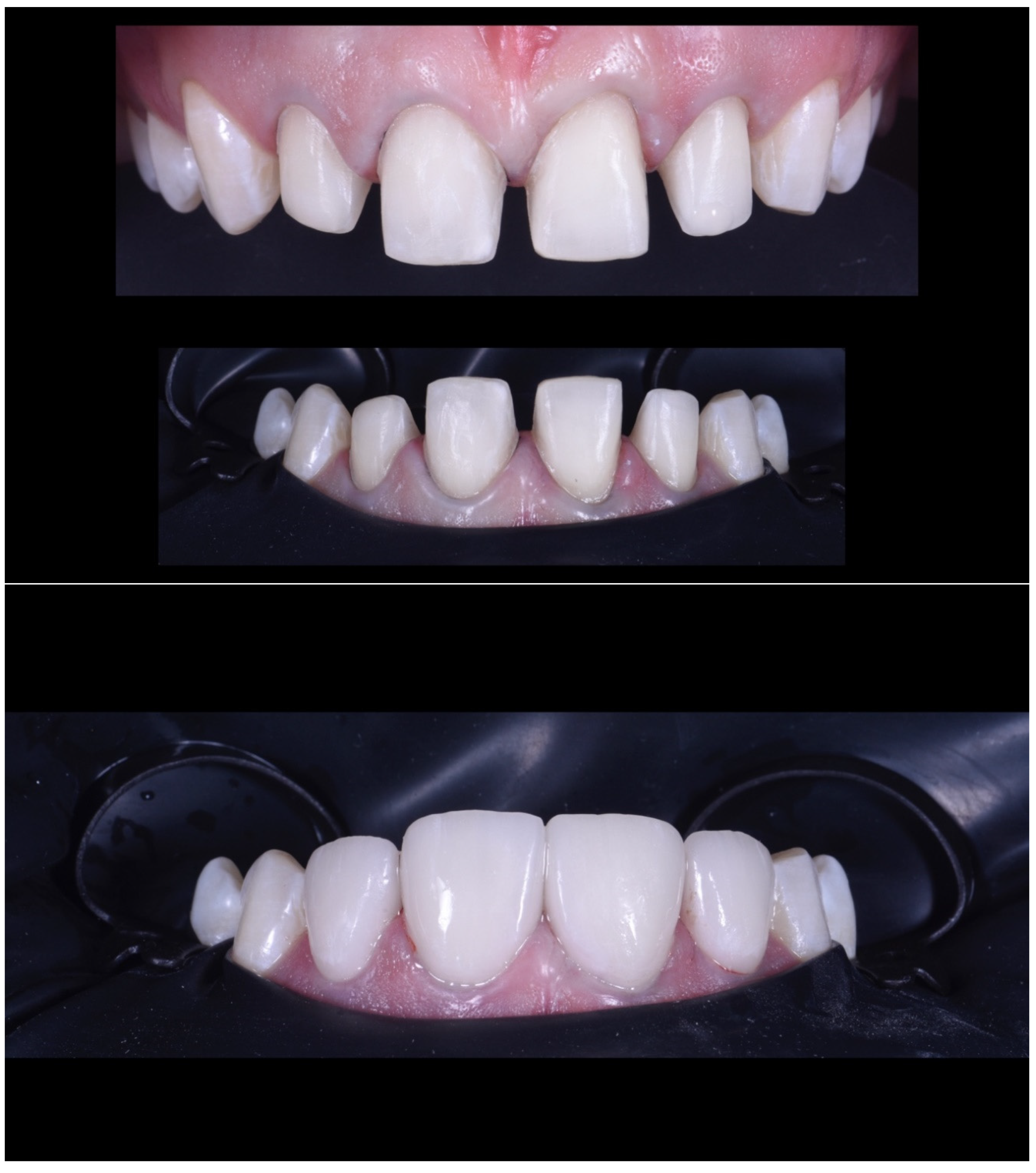
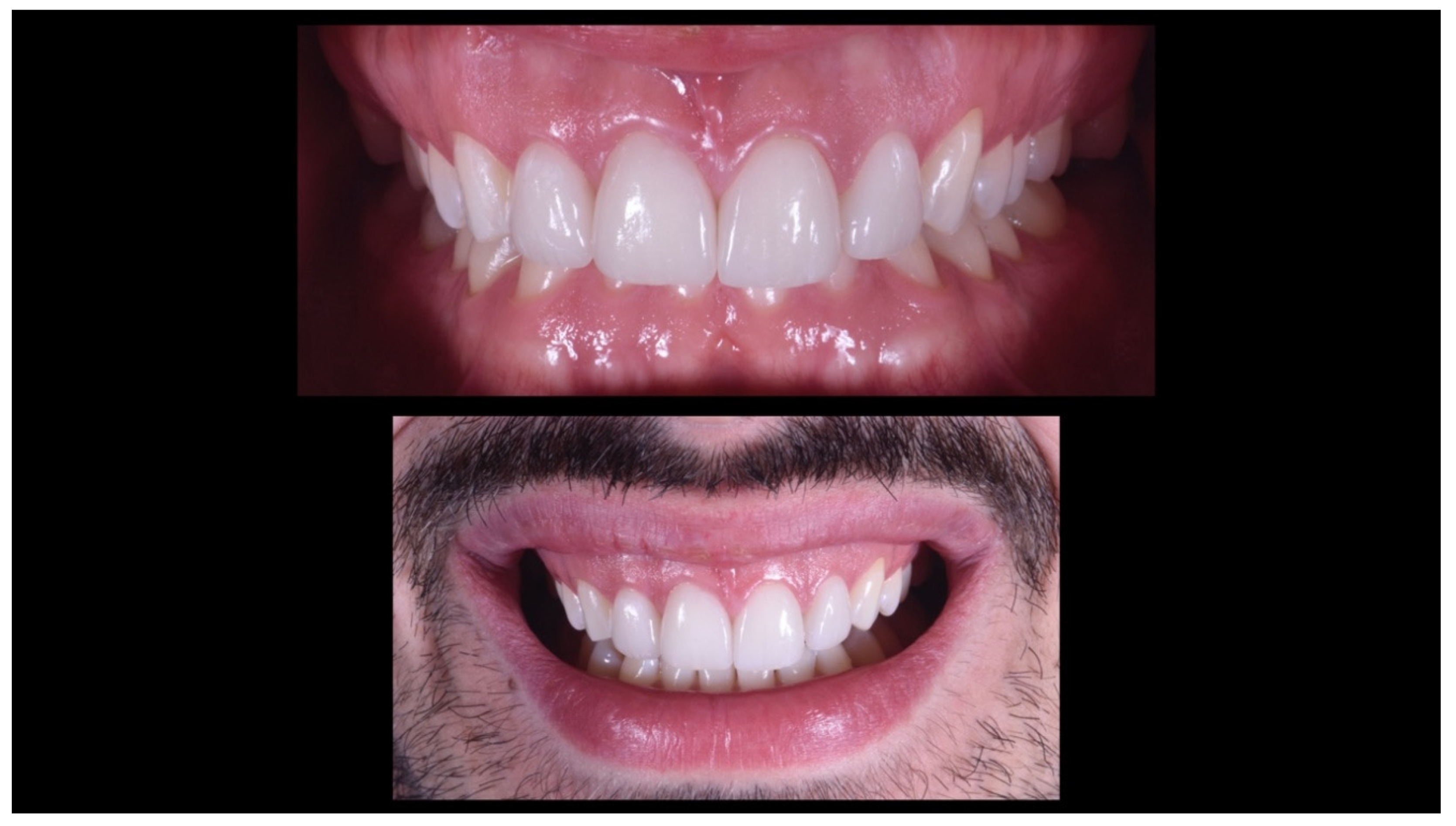
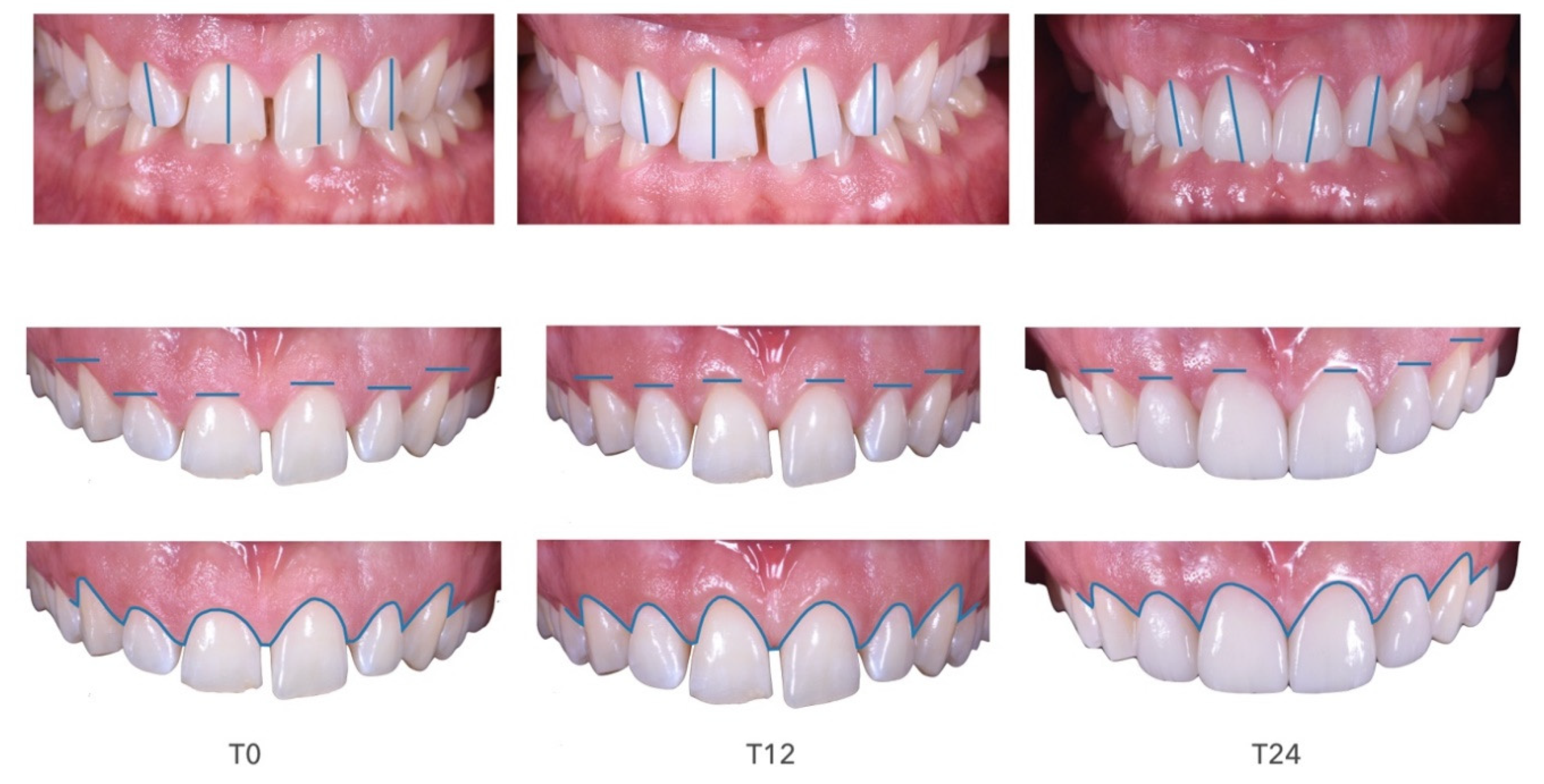
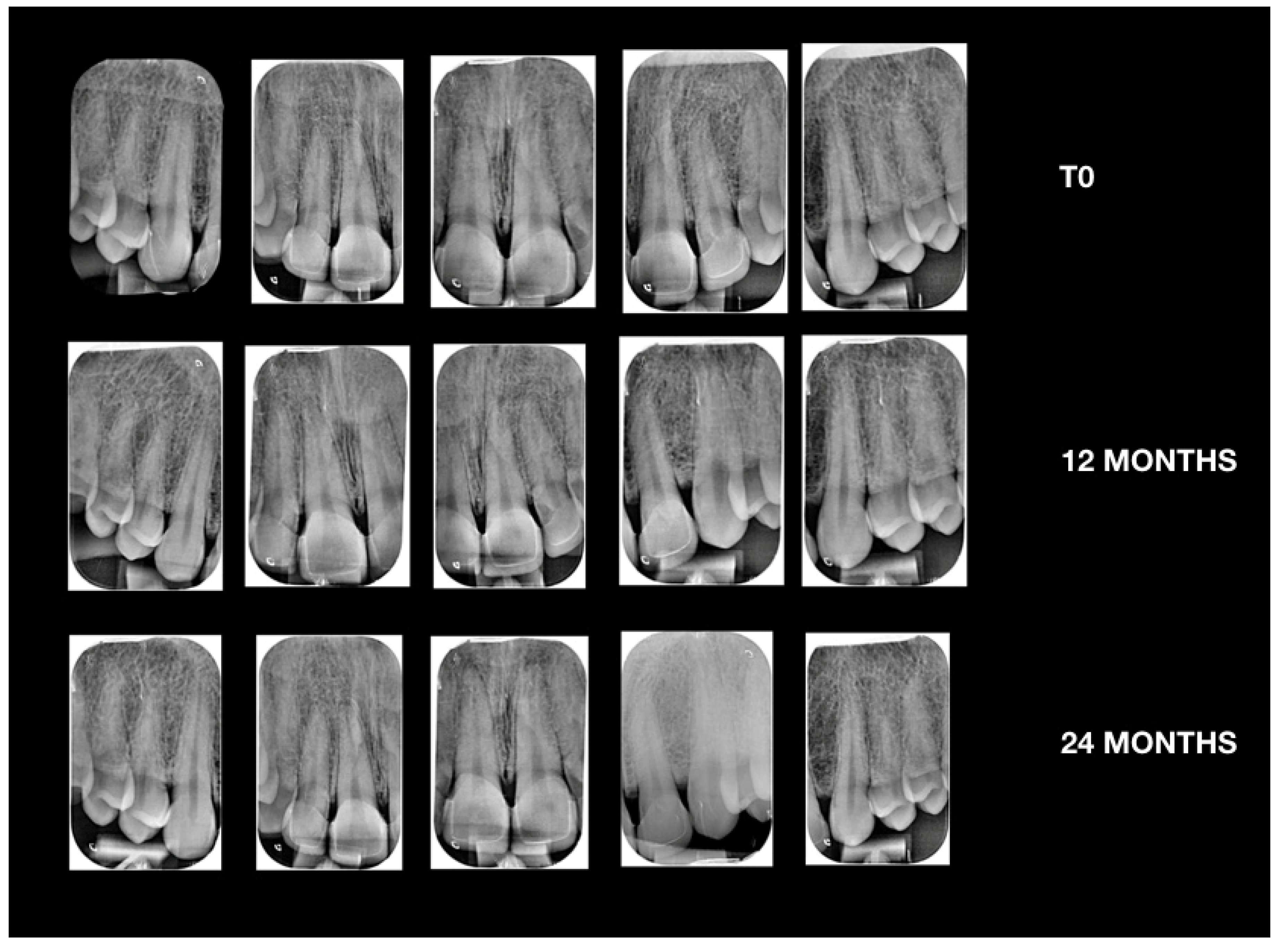
Case Report
3. Discussion
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Cervino, G.; Fiorillo, L.; Arzukanyan, A.V.; Spagnuolo, G.; Cicciù, M. Dental Restorative Digital Workflow: Digital Smile Design from Aesthetic to Function. Dent. J. (Basel) 2019, 7, 30. [Google Scholar] [CrossRef] [PubMed]
- Jokstad, A. Computer-assisted technologies used in oral rehabilitation and the clinical documentation of alleged advantages—A systematic review. J. Oral. Rehabil. 2017, 44, 261–290. [Google Scholar] [CrossRef] [PubMed]
- Agnini, A.; Agnini, A.; Coachman, C. La Rivoluzione Digitale; Quintessenza: Fiorano Modenese, Italy, 2014. [Google Scholar]
- Omar, D.; Duarte, C. The application of parameters for comprehensive smile esthetics by digital smile design programs: A review of literature. Saudi Dent. J. 2018, 30, 7–12. [Google Scholar] [CrossRef] [PubMed]
- Vandenberghe, B. The crucial role of imaging in digital dentistry. Dent Mater. 2020, 36, 581–591. [Google Scholar] [CrossRef] [PubMed]
- Kois, D.E.; Schmidt, K.K.; Raigrodski, A.J. Esthetic templates for complex restorative cases: Rationale and management. J. Esthet. Restor. Dent. 2008, 20, 48–239. [Google Scholar] [CrossRef] [PubMed]
- Mele, M.; Felice, P.; Sharma, P.; Mazzotti, C.; Bellone, P.; Zucchelli, G. Esthetic treatment of altered passive eruption. Periodontol. 2000 2018, 77, 65–83. [Google Scholar] [CrossRef] [PubMed]
- Garcia, P.P.; da Costa, R.G.; Calgaro, M.; Ritter, A.V.; Correr, G.M.; da Cunha, L.F.; Gonzaga, C.C. Digital smile design and mock-up technique for esthetic treatment planning with porcelain laminate veneers. J. Conserv. Dent. 2018, 21, 455–458. [Google Scholar] [PubMed]
- Levi, Y.L.A.S.; Cota, L.V.S.; Maia, L.P. Digital smile design for gummy smile correction. Indian J. Dent. Res. 2019, 30, 803–806. [Google Scholar] [PubMed]
- Rambabu, T.; Gayatri, C.; Sajjan, G.S.; Varma, P.V.K.; Srikanth, V. Correlation between Dentofacial Esthetics and Mental Temperament: A Clinical Photographic Analysis Using Visagism. Contemp. Clin. Dent. 2018, 9, 83–87. [Google Scholar] [PubMed]
- Nagy, Z.; Simon, B.; Mennito, A.; Evans, Z.; Renne, W.; Vág, J. Comparing the trueness of seven intraoral scanners and a physical impression on dentate human maxilla by a novel method. BMC Oral Health 2020, 20, 97. [Google Scholar] [CrossRef] [PubMed]
- Chaturvedi, S.; Alqahtani, N.M.; Addas, M.K.; Alfarsi, M.A. Marginal and internal fit of provisional crowns fabricated using 3D printing technology. Technol. Health Care. 2020, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Koralakunte, P.R.; Aljanakh, M. The role of virtual articulator in prosthetic and restorative dentistry. J. Clin. Diagn. Res. 2014, 8, ZE25-8. [Google Scholar] [CrossRef] [PubMed]
- Hsu, P.; Ramos, V., Jr.; Sadr, A. Microcomputed tomography evaluation of cement shrinkage under zirconia versus lithium disilicate veneers. J. Prosthet. Dent. 2020. [Google Scholar] [CrossRef] [PubMed]
- Cosenza, H.; Pamato, S.; Vermudt, A.; Pereira, J.R. Interdisciplinary approach using composite resin and ceramic veneers to manage an esthetic challenge. Prosthet. Dent. 2020. [Google Scholar] [CrossRef] [PubMed]
- Borzabadi-Farahani, A. The Adjunctive Soft-Tissue Diode Laser in Orthodontics. Compend. Contin. Educ. Dent. 2017, 38, e18–e31. [Google Scholar] [PubMed]
- Maiorana, C.; Speroni, S.; Herford, A.S.; Cicciù, M. Slow Orthodontic Teeth Extrusion to Enhance Hard and Soft Periodontal Tissue Quality before Implant Positioning in Aesthetic Area. Open Dent. J. 2012, 6, 137–142. [Google Scholar] [CrossRef] [PubMed]



© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scattarelli, P.; Smaniotto, P.; Leuci, S.; Cervino, G.; Gisotti, M. The Digital Integrated Workflow in the Aesthetic Management of the Smile: A Case Report. Prosthesis 2020, 2, 196-210. https://doi.org/10.3390/prosthesis2030017
Scattarelli P, Smaniotto P, Leuci S, Cervino G, Gisotti M. The Digital Integrated Workflow in the Aesthetic Management of the Smile: A Case Report. Prosthesis. 2020; 2(3):196-210. https://doi.org/10.3390/prosthesis2030017
Chicago/Turabian StyleScattarelli, Paolo, Paolo Smaniotto, Serena Leuci, Gabriele Cervino, and Mario Gisotti. 2020. "The Digital Integrated Workflow in the Aesthetic Management of the Smile: A Case Report" Prosthesis 2, no. 3: 196-210. https://doi.org/10.3390/prosthesis2030017
APA StyleScattarelli, P., Smaniotto, P., Leuci, S., Cervino, G., & Gisotti, M. (2020). The Digital Integrated Workflow in the Aesthetic Management of the Smile: A Case Report. Prosthesis, 2(3), 196-210. https://doi.org/10.3390/prosthesis2030017





