Focused Ultrasound as Targeted Therapy for Colorectal Cancer: A Comprehensive Review
Abstract
1. Introduction
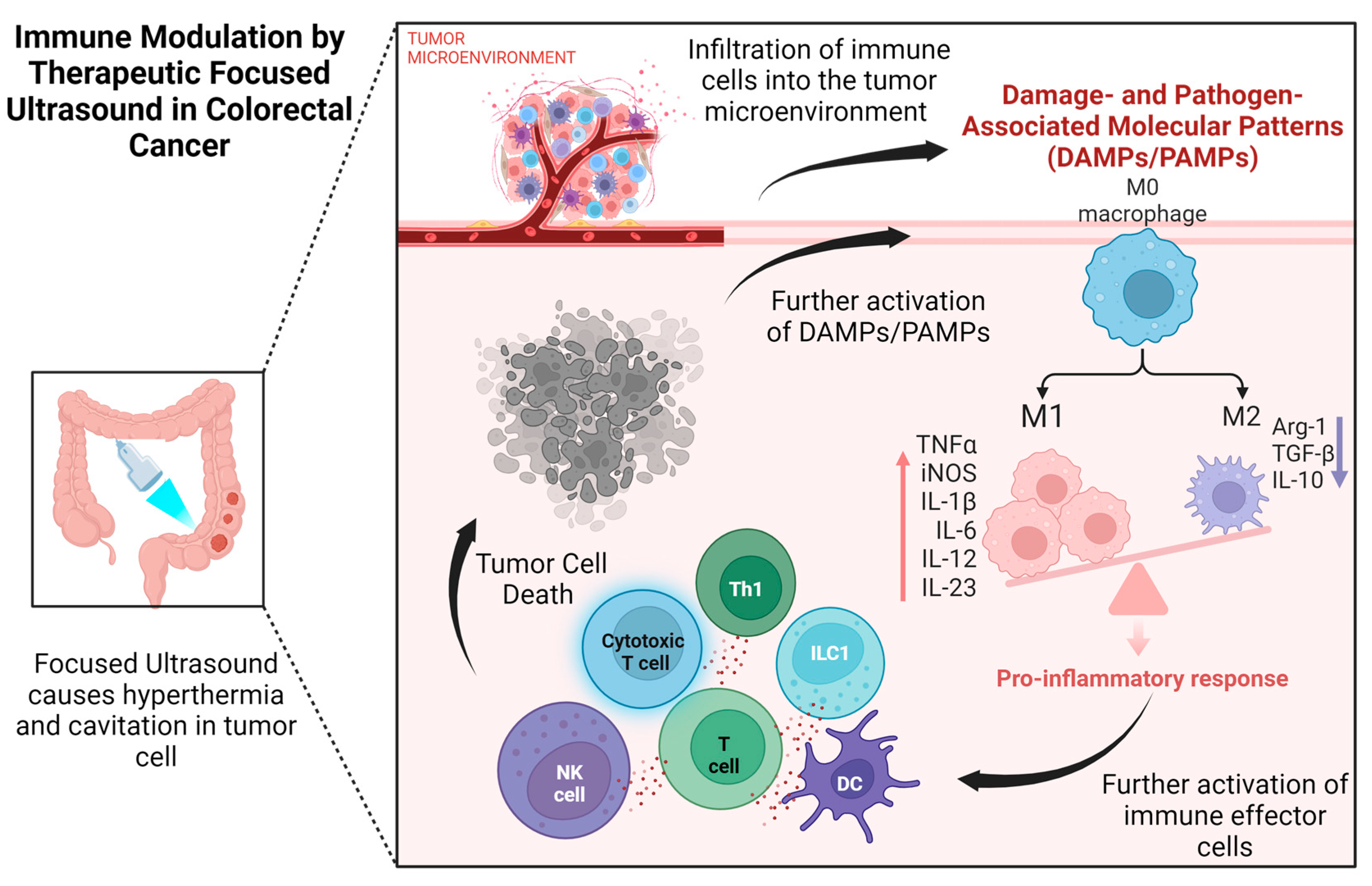
2. Immune Modulation Using Therapeutic Focused Ultrasound in Colorectal Cancer
3. Utilizing Therapeutic Focused Ultrasound for Colorectal Cancer Treatment
4. Investigating the Therapeutic Effects of Focused Ultrasound in Colorectal Cancer
5. Emerging Trends in High-Intensity Focused Ultrasound Research for Colon Cancer Treatment
6. Conclusions and Future Directions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Phenix, C.P.; Togtema, M.; Pichardo, S.; Zehbe, I.; Curiel, L. High Intensity Focused Ultrasound Technology, Its Scope and Applications in Therapy and Drug Delivery. J. Pharm. Pharm. Sci. 2014, 17, 136–153. [Google Scholar] [CrossRef]
- Cai, Y.; Sun, Y.; Xu, F.; Wu, Y.; Ren, C.; Hao, X.; Gao, B.; Cao, Q. Effects of High-Intensity Focused Ultrasound Combined with Levonorgestrel-Releasing Intrauterine System on Patients with Adenomyosis. Sci. Rep. 2023, 13, 9903. [Google Scholar] [CrossRef]
- Chen, J.F.; Wu, S.W.; Shi, Z.M.; Hu, B. Traditional Chinese Medicine for Colorectal Cancer Treatment: Potential Targets and Mechanisms of Action. Chin. Med. 2023, 18, 14. [Google Scholar] [CrossRef]
- Dupré, A.; Melodelima, D.; Pérol, D.; Chen, Y.; Vincenot, J.; Chapelon, J.Y.; Rivoire, M. First Clinical Experience of Intra-Operative High Intensity Focused Ultrasound in Patients with Colorectal Liver Metastases: A Phase i-Iia Study. PLoS ONE 2015, 10, 123751. [Google Scholar] [CrossRef]
- Nowak, S.; Kloth, C.; Theis, M.; Marinova, M.; Attenberger, U.I.; Sprinkart, A.M.; Luetkens, J.A. Deep Learning–Based Assessment of CT Markers of Sarcopenia and Myosteatosis for Outcome Assessment in Patients with Advanced Pancreatic Cancer after High-Intensity Focused Ultrasound Treatment. Eur. Radiol. 2023, 34, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Yin, Z.; Yao, C.; Zhang, L.; Qi, S. Application of Artificial Intelligence in Diagnosis and Treatment of Colorectal Cancer: A Novel Prospect. Front. Med. 2023, 10, 1128084. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Lau, H.C.H.; Cheng, W.Y.; Yu, J. Gut Microbiome in Colorectal Cancer: Clinical Diagnosis and Treatment. Genom. Proteom. Bioinforma. 2023, 21, 84–96. [Google Scholar] [CrossRef]
- Zorob, T.; Farooqi, M.A.; Ahsan, A.; Zaki, A.; Rathore, M.A.; Farooqi, H.M.U. Prevalence and Trends in Hepatitis B&C Virus among Blood Donors in Pakistan: A Regional Transfusion Center Study. Livers 2023, 3, 271–281. [Google Scholar] [CrossRef]
- Hossain, M.S.; Karuniawati, H.; Jairoun, A.A.; Urbi, Z.; Ooi, D.J.; John, A.; Lim, Y.C.; Kibria, K.M.K.; Mohiuddin, A.K.M.; Ming, L.C.; et al. Colorectal Cancer: A Review of Carcinogenesis, Global. Cancer 2022, 14, 1732. [Google Scholar] [CrossRef]
- Worlikar, T.; Hall, T.; Zhang, M.; Mendiratta-Lala, M.; Green, M.; Cho, C.; Xu, Z. Insights from in Vivo Preclinical Studies Cancer Studies with Hisotripsy. Int. J. Hyperth. 2023, 41, 2297650. [Google Scholar] [CrossRef]
- Yin, L.; Li, H.; Shi, L.; Chen, K.; Pan, H.; Han, W. Research Advances in Nanomedicine Applied to the Systemic Treatment of Colorectal Cancer. Int. J. Cancer 2023, 152, 807–821. [Google Scholar] [CrossRef] [PubMed]
- Ter Haar, G.; Shaw, A. Requirements for Measurement Standards in High Intensity Ultrasound (HIFU) Fields. NPL Rep. 2006, 15, DQL-AC 015. [Google Scholar]
- Ye, A.; Liu, X. Clinical Value of High-Intensity Focused Ultrasound in Fetal Reduction. Eur. J. Obstet. Gynecol. Reprod. Biol. 2024, 294, 206–209. [Google Scholar] [CrossRef] [PubMed]
- Farooqi, M.A.; Kang, C.U.; Choi, K.H. Organ-on-Chip: Advancing Nutraceutical Testing for Improved Health Outcomes. ACS Omega 2023, 8, 31632–31647. [Google Scholar] [CrossRef] [PubMed]
- Evans, K.D.; McClure, A. Using High-Intensity Focused Ultrasound as a Means to Provide Targeted Drug Delivery. J. Diagnostic Med. Sonogr. 2016, 32, 343–350. [Google Scholar] [CrossRef]
- Arulpragasam, A.R.; van ’t Wout-Frank, M.; Barredo, J.; Faucher, C.R.; Greenberg, B.D.; Philip, N.S. Low Intensity Focused Ultrasound for Non-Invasive and Reversible Deep Brain Neuromodulation—A Paradigm Shift in Psychiatric Research. Front. Psychiatry 2022, 13, 825802. [Google Scholar] [CrossRef] [PubMed]
- ter Haar, G.; Coussios, C. High Intensity Focused Ultrasound: Physical Principles and Devices. Int. J. Hyperth. 2007, 23, 89–104. [Google Scholar] [CrossRef] [PubMed]
- Mattay, R.R.; Kim, K.; Shah, L.; Shah, B.; Sugrue, L.; Safoora, F.; Ozhinsky, E.; Narsinh, K.H. MR Thermometry during Transcranial MR Imaging-Guided Focused Ultrasound Procedures: A Review. Am. J. Neuroradiol. 2023, 44, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Zhu, H.; Zhang, L.; Kou, F.; Zhao, J.; Lei, J.; He, J. Targeted Therapeutic Effects of Oral Magnetically Driven Pectin Nanoparticles Containing Chlorogenic Acid on Colon Cancer. Particuology 2024, 84, 53–59. [Google Scholar] [CrossRef]
- Banerjee, A.; Pathak, S.; Subramanium, V.D.; Dharanivasan, G.; Murugesan, R.; Verma, R.S. Strategies for Targeted Drug Delivery in Treatment of Colon Cancer: Current Trends and Future Perspectives. Drug Discov. Today 2017, 22, 1224–1232. [Google Scholar] [CrossRef]
- Ebrahimi, N.; Afshinpour, M.; Fakhr, S.S.; Kalkhoran, P.G.; Shadman-Manesh, V.; Adelian, S.; Beiranvand, S.; Rezaei-Tazangi, F.; Khorram, R.; Hamblin, M.R.; et al. Cancer Stem Cells in Colorectal Cancer: Signaling Pathways Involved in Stemness and Therapy Resistance. Crit. Rev. Oncol. Hematol. 2023, 182, 103920. [Google Scholar] [CrossRef] [PubMed]
- Rastin, F.; Javid, H.; Oryani, M.A.; Rezagholinejad, N.; Afshari, A.R.; Karimi-Shahri, M. Immunotherapy for Colorectal Cancer: Rational Strategies and Novel Therapeutic Progress. Int. Immunopharmacol. 2024, 126, 111055. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Qiao, L.; Zhang, M.; Xue, Y.; Zhang, X.; Gao, X. Comparison of Prognosis among Patients with Colorectal Cancer Liver Metastases Treated by Surgical Resection, Radiofrequency Ablation and HIFU: A Protocol for Network Meta-Analysis. Medicine 2022, 101, E27915. [Google Scholar] [CrossRef] [PubMed]
- Sang, R.; Stratton, B.; Engel, A.; Deng, W. Liposome Technologies towards Colorectal Cancer Therapeutics. Acta Biomater. 2021, 127, 24–40. [Google Scholar] [CrossRef] [PubMed]
- Sengupta, S.; Balla, V.K. A Review on the Use of Magnetic Fields and Ultrasound for Non-Invasive Cancer Treatment. J. Adv. Res. 2018, 14, 97–111. [Google Scholar] [CrossRef]
- Hani, U.; Honnavalli, Y.K.; Begum, M.Y.; Yasmin, S.; Osmani, R.A.M.; Ansari, M.Y. Colorectal Cancer: A Comprehensive Review Based on the Novel Drug Delivery Systems Approach and Its Management. J. Drug Deliv. Sci. Technol. 2021, 63, 102532. [Google Scholar] [CrossRef]
- Huang, P.; You, X.; Pan, M.; Li, S.; Zhang, Y.; Zhao, Y.; Wang, M.; Hong, Y.; Pu, Z.; Chen, L.; et al. A Novel Therapeutic Strategy Using Ultrasound Mediated Microbubbles Destruction to Treat Colon Cancer in a Mouse Model. Cancer Lett. 2013, 335, 183–190. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Huang, P.; Zhang, Y.; Chen, J.; Shentu, W.; Sun, Y.; Yang, Z.; Chen, S. Anti-Tumor Efficacy of Ultrasonic Cavitation Is Potentiated by Concurrent Delivery of Anti-Angiogenic Drug in Colon Cancer. Cancer Lett. 2014, 347, 105–113. [Google Scholar] [CrossRef] [PubMed]
- Haram, M.; Hansen, R.; Bouget, D.; Myhre, O.F.; Davies, C.d.L.; Hofsli, E. Treatment of Liver Metastases With Focused Ultrasound and Microbubbles in Patients With Colorectal Cancer Receiving Chemotherapy. Ultrasound Med. Biol. 2023, 49, 2081–2088. [Google Scholar] [CrossRef]
- Cambronero, S.; Dupré, A.; Mastier, C.; Melodelima, D. Non-Invasive High-Intensity Focused Ultrasound Treatment of Liver Tissues in an In Vivo Porcine Model: Fast, Large and Safe Ablations Using a Toroidal Transducer. Ultrasound Med. Biol. 2023, 49, 212–224. [Google Scholar] [CrossRef]
- Van Cutsem, E.; Borràs, J.M.; Castells, A.; Ciardiello, F.; Ducreux, M.; Haq, A.; Schmoll, H.J.; Tabernero, J. Improving Outcomes in Colorectal Cancer: Where Do We Go from Here? Eur. J. Cancer 2013, 49, 2476–2485. [Google Scholar] [CrossRef]
- Macharia, J.M.; Kaposztas, Z.; Varjas, T.; Budán, F.; Zand, A.; Bodnar, I.; Bence, R.L. Targeted Lactate Dehydrogenase Genes Silencing in Probiotic Lactic Acid Bacteria: A Possible Paradigm Shift in Colorectal Cancer Treatment? Biomed. Pharmacother. 2023, 160, 114371. [Google Scholar] [CrossRef]
- Doghish, A.S.; Zaki, M.B.; Eldeib, M.G.; Radwan, A.F.; Moussa, R.; Abdel-Wahab, M.M.; Kizilaslan, E.Z.; Alhamshry, N.A.A.; Ashour, A.E.; Elimam, H. The Potential Relevance of Long Non-Coding RNAs in Colorectal Cancer Pathogenesis and Treatment: A Review Focus on Signaling Pathways. Pathol. Res. Pract. 2024, 253, 155044. [Google Scholar] [CrossRef]
- Farooqi, M.A.; Ahsan, A.; Yousuf, S.; Shakoor, N.; Farooqi, H.M.U. Seroprevalence of Hepatitis E Virus Antibodies (IgG) in the Community of Rawalpindi. Livers 2022, 2, 108–115. [Google Scholar] [CrossRef]
- Al-Bataineh, O.; Jenne, J.; Huber, P. Clinical and Future Applications of High Intensity Focused Ultrasound in Cancer. Cancer Treat. Rev. 2012, 38, 346–353. [Google Scholar] [CrossRef] [PubMed]
- De, S.; Paul, S.; Manna, A.; Majumder, C.; Pal, K.; Casarcia, N.; Mondal, A.; Banerjee, S.; Nelson, V.K.; Ghosh, S.; et al. Phenolic Phytochemicals for Prevention and Treatment of Colorectal Cancer: A Critical Evaluation of In Vivo Studies. Cancers 2023, 15, 993. [Google Scholar] [CrossRef] [PubMed]
- Freitas, S.C.; Sanderson, D.; Caspani, S.; Magalhães, R.; Cortés-Llanos, B.; Granja, A.; Reis, S.; Belo, J.H.; Azevedo, J.; Gómez-Gaviro, M.V.; et al. New Frontiers in Colorectal Cancer Treatment Combining Nanotechnology with Photo- and Radiotherapy. Cancers 2023, 15, 383. [Google Scholar] [CrossRef]
- Mouratidis, P.X.E.; Ter Haar, G. Latest Advances in the Use of Therapeutic Focused Ultrasound in the Treatment of Pancreatic Cancer. Cancers 2022, 14, 638. [Google Scholar] [CrossRef]
- Brady, J.; Corrie, P.; Chau, I.; Digumarti, R.; Adams, L.M.; Botbyl, J.; Laubscher, K.H.; Midgley, R.S.; Mallath, M. An Open-Label Study of the Safety and Tolerability of Pazopanib in Combination with FOLFOX6 or CapeOx in Patients with Colorectal Cancer. Investig. New Drugs 2013, 31, 1228–1235. [Google Scholar] [CrossRef]
- Calik, J.; Zawada, T.; Bove, T.; Dzi, P.; Pogorzelska-antkowiak, A. Healing Process after High-Intensity Focused Ultrasound Treatment of Benign Skin Lesions: Dermoscopic Analysis and Treatment Guidelines. J. Clin. Med. 2024, 13, 931. [Google Scholar] [CrossRef]
- Chen, M.; Liang, X.; Gao, C.; Zhao, R.; Zhang, N.; Wang, S.; Chen, W.; Zhao, B.; Wang, J.; Dai, Z. Ultrasound Triggered Conversion of Porphyrin/Camptothecin-Fluoroxyuridine Triad Microbubbles into Nanoparticles Overcomes Multidrug Resistance in Colorectal Cancer. ACS Nano 2018, 12, 7312–7326. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.S.; Rhim, H.; Min, J.C.; Hyo, K.L.; Choi, D. High-Intensity Focused Ultrasound Therapy: An Overview for Radiologists. Korean J. Radiol. 2008, 9, 291–302. [Google Scholar] [CrossRef] [PubMed]
- Xu, S.; Li, X.; Hu, Q.; Zhang, J.; Li, R.; Meng, L.; Zhu, X. Focused Ultrasound-Responsive Nanocomposite with Near-Infrared II Mechanoluminescence for Spatiotemporally Selective Immune Activation in Lymph Nodes. Chem. A Eur. J. 2024, 30, e202304066. [Google Scholar] [CrossRef] [PubMed]
- Wasielewska, J.M.; White, A.R. “Focused Ultrasound-Mediated Drug Delivery in Humans—A Path Towards Translation in Neurodegenerative Diseases”. Pharm. Res. 2022, 39, 427–439. [Google Scholar] [CrossRef] [PubMed]
- Hernandez Dominguez, O.; Yilmaz, S.; Steele, S.R. Stage IV Colorectal Cancer Management and Treatment. J. Clin. Med. 2023, 12, 2072. [Google Scholar] [CrossRef] [PubMed]
- Couture, O.; Foley, J.; Kassell, N.F.; Larrat, B.; Aubry, J.F. Review of Ultrasound Mediated Drug Delivery for Cancer Treatment: Updates from Pre-Clinical Studies. Transl. Cancer Res. 2014, 3, 494–511. [Google Scholar] [CrossRef]
- Rapoport, N.; Payne, A.; Dillon, C.; Shea, J.; Scaife, C.; Gupta, R. Focused Ultrasound-Mediated Drug Delivery to Pancreatic Cancer in a Mouse Model. J. Ther. Ultrasound 2013, 1, 2–12. [Google Scholar] [CrossRef]
- Dahan, M.; Cortet, M.; Lafon, C.; Padilla, F. Combination of Focused Ultrasound, Immunotherapy, and Chemotherapy: New Perspectives in Breast Cancer Therapy. J. Ultrasound Med. 2023, 42, 559–573. [Google Scholar] [CrossRef] [PubMed]
- Joel, E.; Richter, J.H.R. HHS Public Access Author Manuscript Gastroenterology. Physiol. Behav. 2017, 176, 139–148. [Google Scholar]
- van ’t Erve, I.; Medina, J.E.; Leal, A.; Papp, E.; Phallen, J.; Adleff, V.; Chiao, E.J.; Arun, A.S.; Bolhuis, K.; Simmons, J.K.; et al. Metastatic Colorectal Cancer Treatment Response Evaluation by Ultra-Deep Sequencing of Cell-Free DNA and Matched White Blood Cells. Clin. Cancer Res. 2023, 29, 899–909. [Google Scholar] [CrossRef]
- Al Sawaftah, N.M.; Husseini, G.A. Ultrasound-Mediated Drug Delivery in Cancer Therapy: A Review. J. Nanosci. Nanotechnol. 2020, 20, 7211–7230. [Google Scholar] [CrossRef]
- Ng, G.S.N.; Chow, I.S.W. Colorectal Cancer Presenting as Sacral Pain at a Chiropractic Clinic. Cureus 2023, 15, e39277. [Google Scholar] [CrossRef] [PubMed]
- Prager, G.W.; Taieb, J.; Fakih, M.; Ciardiello, F.; Van Cutsem, E.; Elez, E.; Cruz, F.M.; Wyrwicz, L.; Stroyakovskiy, D.; Pápai, Z.; et al. Trifluridine–Tipiracil and Bevacizumab in Refractory Metastatic Colorectal Cancer. N. Engl. J. Med. 2023, 388, 1657–1667. [Google Scholar] [CrossRef] [PubMed]
- Quintero, E.; Hassan, C.; Senore, C.; Saito, Y. Progress and Challenges in Colorectal Cancer Screening. Gastroenterol. Res. Pract. 2012, 2012, 846985. [Google Scholar] [CrossRef] [PubMed]
- Sitta, J.; Howard, C.M. Applications of Ultrasound-Mediated Drug Delivery and Gene Therapy. Int. J. Mol. Sci. 2021, 22, 11491. [Google Scholar] [CrossRef] [PubMed]
- Moradi Kashkooli, F.; Hornsby, T.K.; Kolios, M.C.; Tavakkoli, J. Ultrasound-Mediated Nano-Sized Drug Delivery Systems for Cancer Treatment: Multi-Scale and Multi-Physics Computational Modeling. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnology 2023, 16, e1913. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Wan, L.; Huang, G.; Chen, C.; Wu, Y. Comparison of High-Intensity Focused Ultrasound and Microwave Ablation for the Treatment of Small Liver Metastatic Tumors. J. Int. Med. Res. 2023, 51. [Google Scholar] [CrossRef] [PubMed]
- Chowdhury, S.M.; Lee, T.; Willmann, J.K. Ultrasound-Guided Drug Delivery in Cancer. Ultrasonography 2017, 36, 171–184. [Google Scholar] [CrossRef]
- Teke, M.E.; Emuakhagbon, V.S. Trends in Colorectal Cancer Surveillance: Current Strategies and Future Innovations-. Curr. Colorectal Cancer Rep. 2019, 15, 79–89. [Google Scholar] [CrossRef]
- Olguin, J.E.; Mendoza-Rodriguez, M.G.; Sanchez-Barrera, C.A.; Terrazas, L.I. Is the Combination of Immunotherapy with Conventional Chemotherapy the Key to Increase the Efficacy of Colorectal Cancer Treatment? World J. Gastrointest. Oncol. 2023, 15, 251–267. [Google Scholar] [CrossRef]
- Cervantes, A.; Adam, R.; Roselló, S.; Arnold, D.; Normanno, N.; Taïeb, J.; Seligmann, J.; De Baere, T.; Osterlund, P.; Yoshino, T.; et al. Metastatic Colorectal Cancer: ESMO Clinical Practice Guideline for Diagnosis, Treatment and Follow-up☆. Ann. Oncol. 2023, 34, 10–32. [Google Scholar] [CrossRef]
- Wu, S.K.; Tsai, C.L.; Huang, Y.; Hynynen, K. Focused Ultrasound and Microbubbles-Mediated Drug Delivery to Brain Tumor. Pharmaceutics 2021, 13, 15. [Google Scholar] [CrossRef] [PubMed]
- Park, M.J.; Kim, Y.S.; Yang, J.; Sun, W.C.; Park, H.; Chae, S.Y.; Namgung, M.S.; Choi, K.S. Pulsed High-Intensity Focused Ultrasound Therapy Enhances Targeted Delivery of Cetuximab to Colon Cancer Xenograft Model in Mice. Ultrasound Med. Biol. 2013, 39, 292–299. [Google Scholar] [CrossRef]
- Hu, Z.; Yang, X.Y.; Liu, Y.; Sankin, G.N.; Pua, E.C.; Morse, M.A.; Lyerly, H.K.; Clay, T.M.; Zhong, P. Investigation of HIFU-Induced Anti-Tumor Immunity in a Murine Tumor Model. J. Transl. Med. 2007, 5, 34. [Google Scholar] [CrossRef]
- Mo, W.; Yu, Q.; Kuang, X.; He, T.; Lou, J.; Tang, R.; Zhang, K.; Li, L.; Zhao, L. Focused Ultrasound Restrains the Growth of Orthotopic Colon Cancer via Promoting Pyroptosis. Folia Histochem. Cytobiol. 2023, 61, 47–55. [Google Scholar] [CrossRef] [PubMed]
- Mouratidis, P.X.E.; Rivens, I.; Ter Haar, G. A Study of Thermal Dose-Induced Autophagy, Apoptosis and Necroptosis in Colon Cancer Cells. Int. J. Hyperth. 2015, 31, 476–488. [Google Scholar] [CrossRef] [PubMed]
- Liu, C. Characterization of the Colorectal Cancer by Combining High-Frequency Endoscopic Ultrasound and Quantitative Ultrasound. Available online: https://theses.lib.polyu.edu.hk/handle/200/7380 (accessed on 20 January 2024).
- Liu, H.L.; Hsieh, H.Y.; Lu, L.A.; Kang, C.W.; Wu, M.F.; Lin, C.Y. Low-Pressure Pulsed Focused Ultrasound with Microbubbles Promotes an Anticancer Immunological Response. J. Transl. Med. 2012, 10, 221. [Google Scholar] [CrossRef]
- Çetin, E.; Karaböce, B.; Kilinç, O.; Orun, O. Biological Effects of HIFU on HT-29 Colon Cancer Cell Lines. In Proceedings of the 2018 IEEE International Symposium on Medical Measurements and Applications (MeMeA), Rome, Italy, 11–13 June 2018. [Google Scholar] [CrossRef]
- Tang, F.; Zhong, Q.; Ni, T.; Xue, Y.; Wu, J.; Deng, R.; Zhang, Q.; Li, Y.; He, X.; Yang, Z.; et al. High-Intensity Focused Ultrasound Ablation Combined with Systemic Therapy for Unresectable Colorectal Cancer Liver Metastasis: A Propensity Score-Matched Analysis. Cancer Med. 2023, 12, 21985–21995. [Google Scholar] [CrossRef]
- Yang, T.; Chen, Q.; Kuang, L.; Fu, Z.; Wang, Y.; Chen, Y.; Yang, L.; Xu, Y. Effectiveness and Safety of Ultrasound-Guided High-Intensity Focused Ultrasound Ablation for the Treatment of Colorectal Cancer Liver Metastases. Int. J. Hyperth. 2022, 39, 829–834. [Google Scholar] [CrossRef]
- Zhang, X.; Yang, G.; Zhang, Y.; Huang, P.; Qiu, J.; Sun, Y.; Shen, Z.; Liao, X.; Xia, H.; Shao, S.; et al. An Experimental Research into Endostatin Microbubble Combined with Focused Ultrasound for Anti-Tumor Angiogenesis in Colon Cancer. Gastroenterol. Rep. 2014, 2, 44–53. [Google Scholar] [CrossRef]
- Diana, M.; Schiraldi, L.; Liu, Y.-Y.; Memeo, R.; Mutter, D.; Pessaux, P.; Marescaux, J. High Intensity Focused Ultrasound (HIFU) Applied to Hepato-Bilio-Pancreatic and the Digestive System—Current State of the Art and Future Perspectives. HepatoBiliary Surg. Nutr. 2016, 5, 329–344. [Google Scholar] [CrossRef] [PubMed]
- Hubert, P.; David, M.; Apoutou, N.; Sabrina, C.; Yves, C.J.; Michel, R. High-Intensity Focused Ultrasound Ablation for the Treatment of Colorectal Liver Metastases during an Open Procedure: Study on the Pig. Ann. Surg. 2009, 249, 129–136. [Google Scholar] [CrossRef] [PubMed]
- Prachee, I.; Wu, F.; Cranston, D. Oxford’s Clinical Experience in the Development of High Intensity Focused Ultrasound Therapy. Int. J. Hyperth. 2021, 38, 81–88. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.; Lee, S.S.; Moon, H.; Park, S.Y.; Lee, H.J. Pd-L1 Targeting Immune-Microbubble Complex Enhances Therapeutic Index in Murine Colon Cancer Models. Pharmaceuticals 2021, 14, 6. [Google Scholar] [CrossRef] [PubMed]
- Ektate, K.; Munteanu, M.C.; Ashar, H.; Malayer, J.; Ranjan, A. Chemo-Immunotherapy of Colon Cancer with Focused Ultrasound and Salmonella-Laden Temperature Sensitive Liposomes (Thermobots). Sci. Rep. 2018, 8, 26–30. [Google Scholar] [CrossRef] [PubMed]
- Mouratidis, P.X.E.; ter Haar, G. HSP90 Inhibition Acts Synergistically with Heat to Induce a Pro-Immunogenic Form of Cell Death in Colon Cancer Cells. Int. J. Hyperth. 2021, 38, 1443–1456. [Google Scholar] [CrossRef] [PubMed]
- Hong, L.; Guo, Z.; Yu, H.; Li, B.; Si, T.; Liu, C. [Efficacy and safety of low-dose high intensity focused ultrasound combined with S-1 and oxaliplatin in metastatic colorectal patients with pelvic masses]. Zhonghua Yi Xue Za Zhi 2014, 94, 1929–1932. [Google Scholar] [PubMed]
- Moradi Kashkooli, F.; Jakhmola, A.; Hornsby, T.K.; Tavakkoli, J.; Kolios, M.C. Ultrasound-Mediated Nano Drug Delivery for Treating Cancer: Fundamental Physics to Future Directions. J. Control. Release 2023, 355, 552–578. [Google Scholar] [CrossRef] [PubMed]
- Imtiaz, C.; Farooqi, M.A.; Bhatti, T.; Lee, J.; Moin, R.; Kang, C.U.; Farooqi, H.M.U. Focused Ultrasound, an Emerging Tool for Atherosclerosis Treatment: A Comprehensive Review. Life 2023, 13, 1783. [Google Scholar] [CrossRef]
- Boissenot, T.; Bordat, A.; Larrat, B.; Varna, M.; Chacun, H.; Paci, A.; Poinsignon, V.; Fattal, E.; Tsapis, N. Ultrasound-Induced Mild Hyperthermia Improves the Anticancer Efficacy of Both Taxol® and Paclitaxel-Loaded Nanocapsules. J. Control. Release 2017, 264, 219–227. [Google Scholar] [CrossRef]
- Boissenot, T.; Bordat, A.; Fattal, E.; Tsapis, N. Ultrasound-Triggered Drug Delivery for Cancer Treatment Using Drug Delivery Systems: From Theoretical Considerations to Practical Applications. J. Control. Release 2016, 241, 144–163. [Google Scholar] [CrossRef] [PubMed]
- Ashar, H.; Ranjan, A. Immunomodulation and Targeted Drug Delivery with High Intensity Focused Ultrasound (HIFU): Principles and Mechanisms. Pharmacol. Ther. 2023, 244, 108393. [Google Scholar] [CrossRef] [PubMed]
- Jeong, H.S.; Hwang, H.; Oh, P.S.; Kim, E.M.; Lee, T.K.; Kim, M.; Kim, H.S.; Lim, S.T.; Sohn, M.H.; Jeong, H.J. Effect of High-Intensity Focused Ultrasound on Drug Release from Doxorubicin-Loaded PEGylated Liposomes and Therapeutic Effect in Colorectal Cancer Murine Models. Ultrasound Med. Biol. 2016, 42, 947–955. [Google Scholar] [CrossRef] [PubMed]
- Yusefi, M.; Shameli, K.; Lee-Kiun, M.S.; Teow, S.Y.; Moeini, H.; Ali, R.R.; Kia, P.; Jie, C.J.; Abdullah, N.H. Chitosan Coated Magnetic Cellulose Nanowhisker as a Drug Delivery System for Potential Colorectal Cancer Treatment. Int. J. Biol. Macromol. 2023, 233, 123388. [Google Scholar] [CrossRef]
- Zhu, H.; Chen, W.; Wu, F.; Li, K.; Zou, J.; Wang, Z. High-Intensity Focused Ultrasound in the Treatment of Hepatic Metastases from Colorectal Cancer of 18 Patients. Chinese J. Clin. Oncol. 2004, 1, 101–105. [Google Scholar] [CrossRef]


| Research Topic | Focused Ultrasound Setup | Model | Treatment Parameters | Results | Reference |
|---|---|---|---|---|---|
| Improving cetuximab delivery to colon cancer xenografts in mice through pulsed HIFU therapy | Therapy Imaging Probe System, Philips Research, Briarcliff Manor, NY, USA | Pre-clinical mice model | Acoustic intensity: 191 W cm−2 Ultrasound frequency during sonication: 1.3 MHz Pulse repetition frequency: Set at 1 Hz Duty cycle: 5%, with 50 ms on and 950 ms off periods | HIFU therapy amplifies the antitumor efficacy of cetuximab against human colon cancer xenograft models in mice. | [63] |
| Using FUS and microbubbles to treat liver metastases in colorectal cancer patients undergoing chemotherapy | Ultrasound scanner, Vivid E9 (VE96975, GE Vingmed Ultrasound AS, Horten, Norway) | Clinical model | FUS was applied at a frequency of 1.67 MHz, with a mechanical index of 0.5, a pulse repetition frequency of 0.33 Hz, 33 oscillations, and a duty cycle ranging from 0.2% to 0.4%. Microbubbles (MBs) of SonoVue were administered for 35 min. | Combining FUS and MBs is a safe and feasible approach to enhance chemotherapy effectiveness in cancer patients. | [29] |
| Investigating the antitumor immune response triggered by HIFU in a murine cancer model | HIFU transducer (Model H-102, Sonic Concepts, Seattle, WA, USA) | Pre-clinical Mice model bearing MC-38 colon adenocarcinoma tumors | The focal length of 63 mm, operating at 3.3 MHz (3rd Harmonic) with sinusoidal signals, using a portable ultrasound imaging system (Terason 2000, Terason, Inc., Burlington, MA, USA) with a 5/10 MHz probe for tumor alignment | Thermal and mechanical HIFU resulted in a 3.1-fold rise in CD11c+ cells, while a 4-fold increase was observed with mechanical HIFU. In comparison, DC injection alone resulted in a 1.5-fold increase. | [64] |
| FUS application in colon cancer tumor suppression | FUS transducer (V3330) supplied by Olympus (Houston, TX, USA) | A pre-clinical orthotopic colorectal cancer (CC) mouse model was established by injecting CT26-Luc cells into BALB/c mice | Irradiation intensity: 9.3 MHz Power: 4.5 W Treatment technique: FUS treatment is initiated from the tumor center, expanding gradually to edges with 1.0 mm point spacing. Exposure time: 10 s per treatment point | FUS treatment alleviated intestinal tissue injury in CC mice, as indicated by morphological changes. | [65] |
| Investigation of thermal dose-induced cell death pathways in colon cancer cells | T-type thermocouples (catalog number 6212164, RS Instruments, Corby, UK) | Pre-clinical in vitro models using human HCT116 and HT29 colon cancer cell lines | The thermocouples were configured to measure temperatures within a range of −50 °C to +200 °C, featuring a wire thickness of 0.2 mm, a probe diameter of 0.57 mm, and an accuracy of ±0.5 °C up to 125 °C | Treatment with ablative thermal doses resulted in the reduced viability of colon cancer cells. | [66] |
| Characterization of colorectal cancer | High-Frequency Endoscopic Ultrasound (EUS) System | Pre-clinical rabbit model of colorectal cancer | Cut-off frequency of 10 MHz in high pass and 63 MHz in low pass | High-frequency EUS system suitable for routine colonoscopy and potential functional tools. | [67] |
| Using high-intensity focused ultrasound to treat colorectal cancer liver metastases | JC FUS Tumor Treatment System Developed by Chongqing Haifu (HIFU) Technology Co., Ltd., Chongqing, China | Clinical model of patients with liver metastases from colorectal cancer after undergoing colectomy |
Frequency: 0.8 MHz Focal length: 135 mm Physical focus region: 2 mm × 2 mm × 8 mm Treatment duration: 3800–12,000 s | HIFU demonstrates safety, effectiveness, and non-invasiveness in treating hepatic metastases from colorectal cancer. | [68] |
| Examining the biological impact of HIFUS on HT-29 colon cancer cell lines | HIFU (H-102 model) transducer from Sonic Concepts | Pre-clinical in vitro model using HT-29 human colorectal adenocarcinoma cell line | Fundamental frequency of H-102: 1.10 MHz Focal point: 62.6 mm from the transducer face HIFU was applied to the focused well for 30 s | A notable decrease in viability rates was observed with increasing thermal doses. | [69] |
| Enhancing the efficacy of systemic therapy for unresectable liver metastasis from colorectal cancer through HIFU ablation | HIFU (model-2001, Shanghai Jiao Tong University’s Xindi Industrial Company, Shanghai, China) | Clinical model involving colorectal cancer liver metastasis patients | Ultrasonic frequency: 50 Hz Output power: 1 kW Effective treatment Depth: 30–150 mm Effect focus: 6 mm × 6 mm × 10 mm Focal Volume: 3 mm × 3 mm × 8 mm | HIFU ablation with systemic therapy controls the progression of colorectal cancer liver metastases. | [70] |
| Efficacy and safety of HIFU ablation for managing liver metastases from colorectal cancer | JC HIFU-200 system by Chongqing Haifu Medical Technology Co., Ltd., Chongqing, China | Clinical model (colorectal cancer liver metastasis patients) | The transducer, operating at 1.0 MHz, generates ultrasound energy with a focal region of 3 mm × 3 mm × 8 mm. It can smoothly move in six directions (X, Y, and Z axes) via computer control | HIFU ablation emerges as a safe and efficient treatment choice for patients with colorectal cancer liver metastases. | [71] |
| Inhibiting tumor angiogenesis in colon cancer through combined application of endostatin microbubbles and FUS | FUS (Sea Eagle Electronic Medical System Co. Ltd., Changzhou, China) | Pre-clinical in vivo model using BALB/c nude mice | Frequency: 238 kHz Output voltage: 400 Mv Focus incentive sound pressure: 1.4 MPa, irradiation sessions: 10 Time: 10 s | Targeted microbubbles, combined with FUS, effectively disrupt tumor microvasculature in subcutaneous colon cancer xenografts. | [72] |
| HIFU for hepato-biliopancreatic and digestive system | HIFU devices JC Model by Chongqing | Clinical model involving patients with colon, liver, and pancreas cancer | Acoustic power of 300 W, focal peak intensity of 20 KW/cm2, applied for 30 min | HIFU consistently alleviates cancer-related pain. | [73] |
| HIFU ablation for colorectal liver metastases during open surgery | HIFU device with 7.5 MHz ultrasound imaging probe (Vermon, Tours, France) | Pre-clinical model using pigs with colorectal liver metastases | Ultrasound fields generated by eight emitters operating at 3 MHz, distributed in a toroidal geometry with a 70 mm diameter | HIFU enables treatment with real-time ultrasound guidance. | [74] |
| Clinical experience with HIFU therapy development at Oxford | HIFU device | Clinical study involving patients with colon, liver, kidney, prostate, and pancreas cancer | N/A | HIFU targets both benign and malignant tissues. | [75] |
| Enhanced therapeutic index of PD-L1 targeting immune-microbubble complex in murine colon cancer models | Utilized FUS system (VIFU 2000®, Alpinion Medical Systems, Seoul, Republic of Korea) | Pre-clinical colorectal liver metastasis mice model (BALB/c nude mice) | Applied 1.1 MHz frequency, 100 Watts power, 100 Hz pulse repetition frequency, 5% duty cycle, 5 s ultrasound exposure per spot, with 2 mm spot distance | Demonstrated improvement in the therapeutic index for PD-L1 antibodies. | [76] |
| Utilizing FUS for chemo-immunotherapy of colon cancer | Utilized integrated ultrasound-HIFUS Alpinion platform with specific specifications | Pre-clinical on Balb/c mice as an in vivo model of colon cancer | The parameters for HIFU treatment included a 35% duty cycle, a pulse repetition frequency of 5 Hz, and a power of 6 W, aiming to reach a mean target temperature of 40–42.5 °C within the heated focus for 60 s | Combinatorial therapy has the potential for the treatment of colorectal cancer. | [77] |
| Exploring the effects of HIFU on anti-tumor immune response in a murine tumor model | HIFU transducer (H-102, Sonic Concepts, Seattle, WA, USA) Thermocouple (Custom designed IT-23, Physitemp Inc., Clifton, NJ, USA) | Pre-clinical in vitro model (mice bearing MC-38 colon adenocarcinoma tumors) | Transducer focal length: 63 mm; frequency: 3.3 MHz | FUS treatment can trigger a systemic antitumor immune response. | [78] |
| Enhancing anticancer immune response with low-pressure pulsed FUS and microbubbles | The sonogram-guided MB-FUS exposure system (Sonic Concepts, Seattle, WA, USA) | Pre-clinical in vitro model (tumor-bearing BALB/mice) | FUS exposure was administered at power levels of 5 and 30 W, corresponding to acoustic negative-peak pressures measured at 0.6 and 1.4 MPa, respectively | Exposure to low-pressure FUS stimulates an anticancer immune response. | [68] |
| HIFU combined therapy with S-1 and oxaliplatin in metastatic colorectal cancer patients | HIFU developed by Jingyuande Medical Equipment Co., Ltd., Xuzhou, China. Treatment System (FEP-BY02 type) | Clinical model (patient with colorectal cancer) | D Input electric power level Control range 300–500 W Element emission time (t1) 1–2 s, the number of times per point (T) 5–10 time | The combination therapy involving HIFUS and SOX proves to be efficacious and well tolerated in late-stage colorectal cancer patients with pelvic masses. | [79] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Farooqi, M.A.; Mahnoor, M.; Delgado, K.M.; Dahlgren, W.T.-T.; Kang, C.-U.; Farooqi, H.M.U. Focused Ultrasound as Targeted Therapy for Colorectal Cancer: A Comprehensive Review. Gastrointest. Disord. 2024, 6, 380-401. https://doi.org/10.3390/gidisord6020026
Farooqi MA, Mahnoor M, Delgado KM, Dahlgren WT-T, Kang C-U, Farooqi HMU. Focused Ultrasound as Targeted Therapy for Colorectal Cancer: A Comprehensive Review. Gastrointestinal Disorders. 2024; 6(2):380-401. https://doi.org/10.3390/gidisord6020026
Chicago/Turabian StyleFarooqi, Muhammad Awais, Mahnoor Mahnoor, Kaylee Marie Delgado, Wylie Thien-Tam Dahlgren, Chul-Ung Kang, and Hafiz Muhammad Umer Farooqi. 2024. "Focused Ultrasound as Targeted Therapy for Colorectal Cancer: A Comprehensive Review" Gastrointestinal Disorders 6, no. 2: 380-401. https://doi.org/10.3390/gidisord6020026
APA StyleFarooqi, M. A., Mahnoor, M., Delgado, K. M., Dahlgren, W. T.-T., Kang, C.-U., & Farooqi, H. M. U. (2024). Focused Ultrasound as Targeted Therapy for Colorectal Cancer: A Comprehensive Review. Gastrointestinal Disorders, 6(2), 380-401. https://doi.org/10.3390/gidisord6020026








