Lymphatic Filariasis in Mainland Southeast Asia: A Systematic Review and Meta-Analysis of Prevalence and Disease Burden
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol
2.2. Information Sources
2.3. Search Strategy
2.4. Study Selection and Inclusion Criteria
2.5. Data Collection Process
2.6. Data Items
2.7. Risk of Bias Assessment
2.8. Summary Measures and Synthesis of Results
3. Results
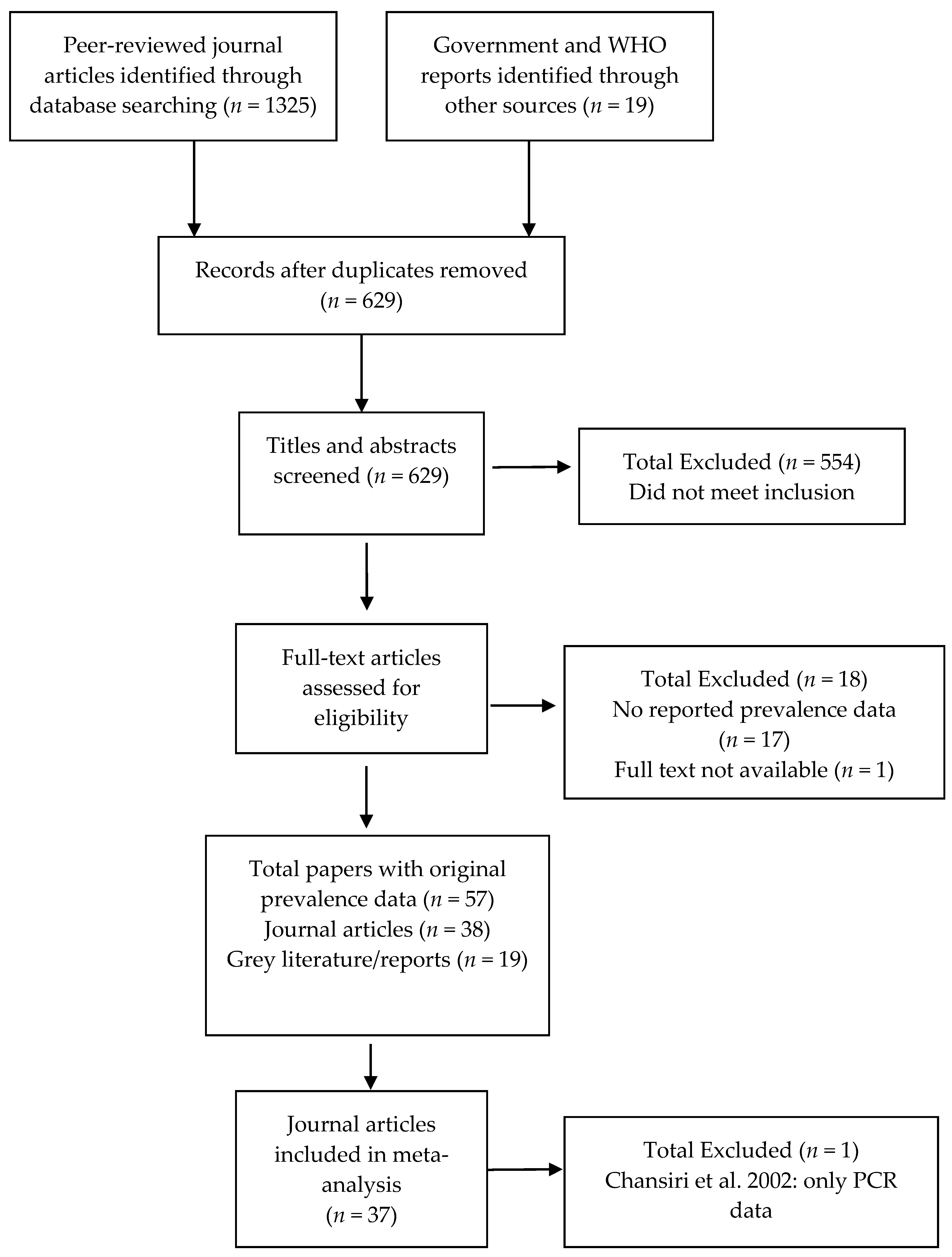
3.1. Study Selection
3.2. Study Characteristics
3.3. Risk of Bias within Studies
4. Prevalence Results and Discussion by Country
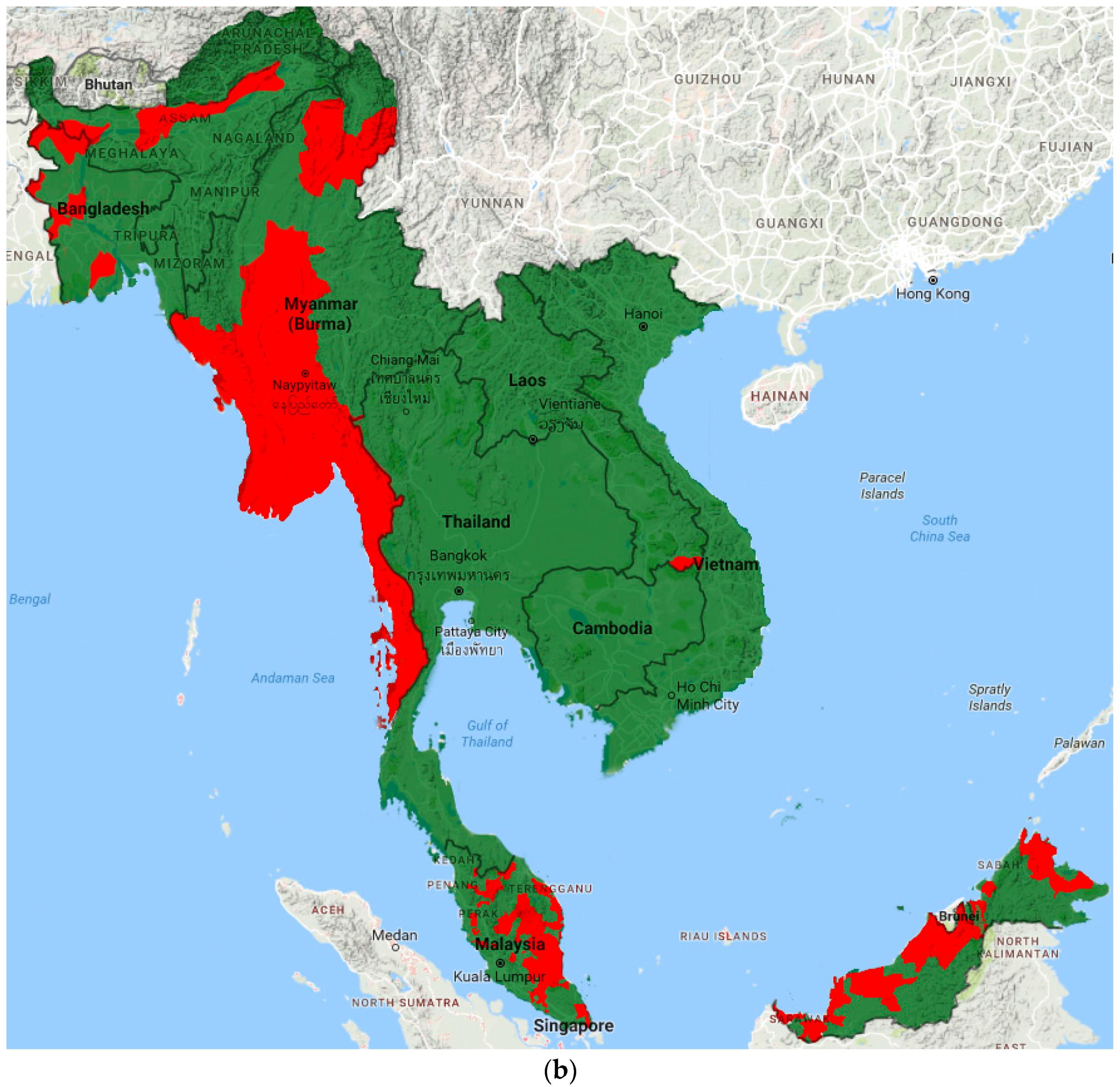
4.1. Overview
4.2. Bangladesh
4.2.1. Results
4.2.2. Discussion
4.3. Cambodia
4.3.1. Results
4.3.2. Discussion
4.4. Northeast India
4.4.1. Results
4.4.2. Discussion
4.5. Lao PDR
4.5.1. Results
4.5.2. Discussion
4.6. Malaysia
4.6.1. Results
4.6.2. Discussion
4.7. Myanmar
4.7.1. Results
4.7.2. Discussion
4.8. Thailand
4.8.1. Results
4.8.2. Discussion
4.9. Vietnam
4.9.1. Results
4.9.2. Discussion
4.10. Overall Prevalence Estimates for Mainland Southeast Asia
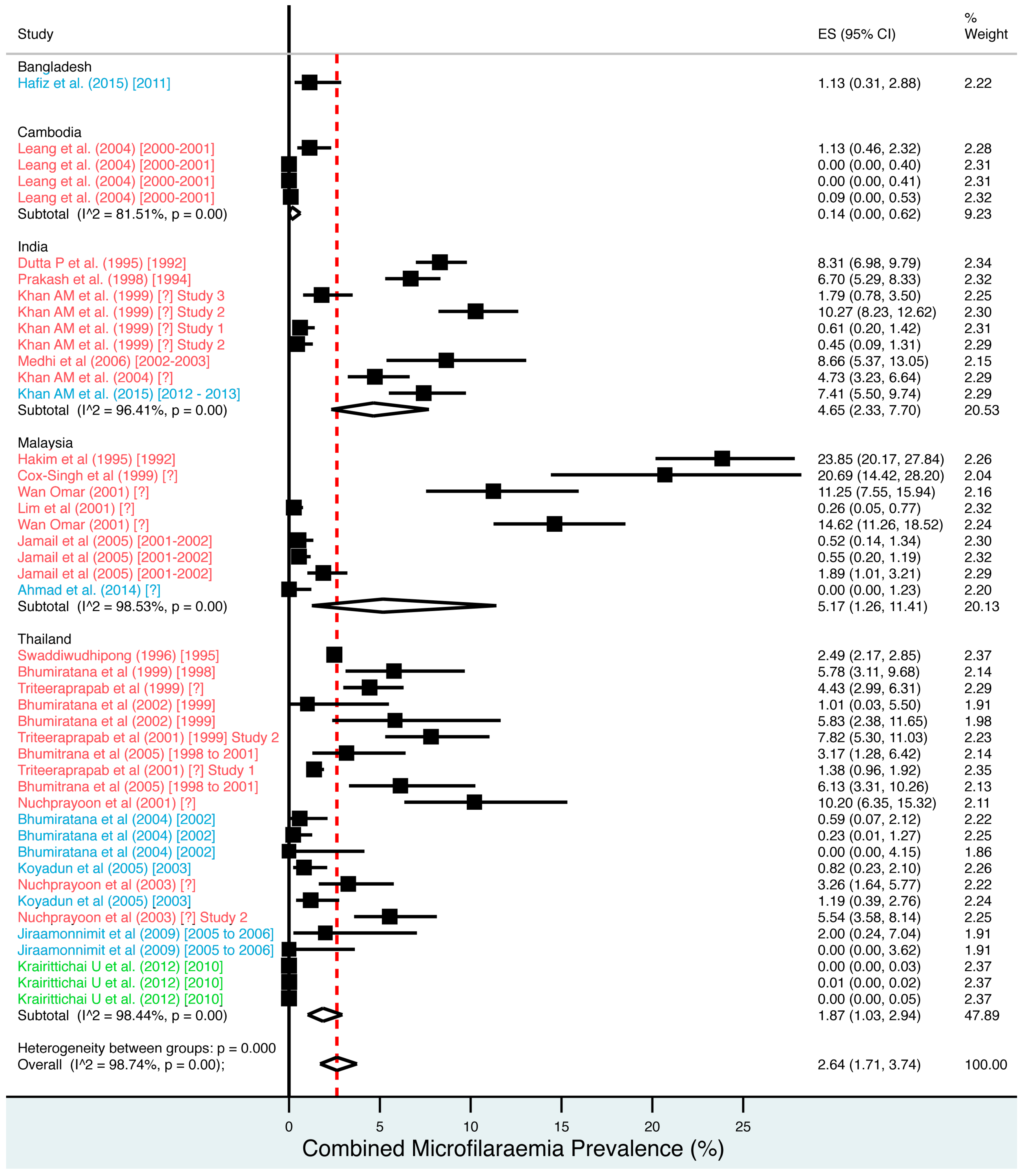
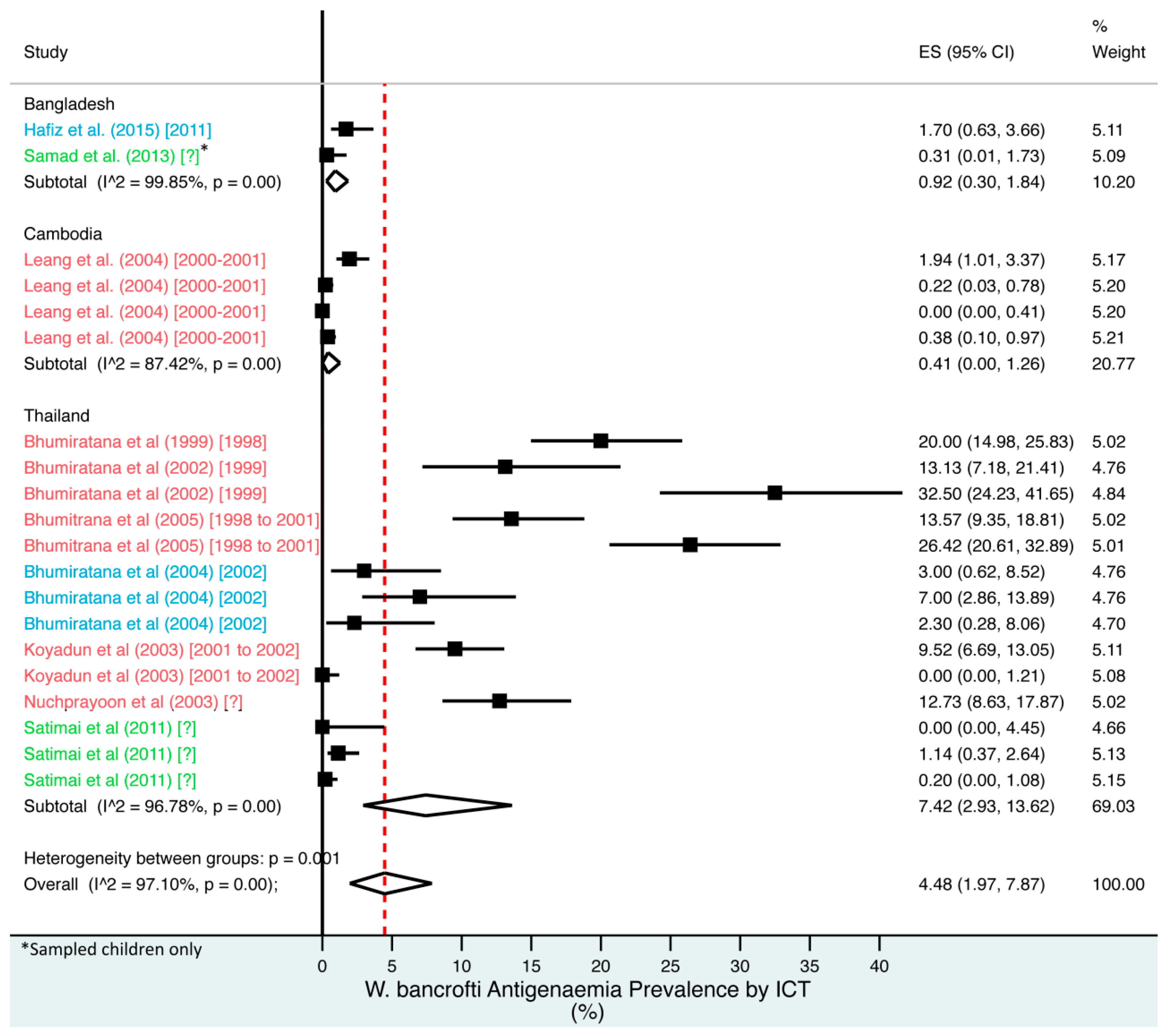
4.10.1. Meta-Analysis Results
4.10.2. Discussion
4.11. Limitations
5. Conclusions
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization. WHO Global Programme to Eliminate Lymphatic Filariasis: Progress Report for 2000–2009 and Strategic Plan 2010–2020; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- World Health Organization. Global programme to eliminate lymphatic filariasis: Progress report, 2015. Wkly. Epidemiol. Record 2016, 91, 441–460. [Google Scholar]
- Ramaiah, K.; Ottesen, E.A. Progress and impact of 13 years of the global programme to eliminate lymphatic filariasis on reducing the burden of filarial disease. PLoS Negl. Trop. Dis. 2014, 8, e3319. [Google Scholar] [CrossRef] [PubMed]
- Murray, C.J.; Barber, R.M.; Foreman, K.J.; Ozgoren, A.A.; Abd-Allah, F.; Abera, S.F.; Aboyans, V.; Abraham, J.P.; Abubakar, I.; Abu-Raddad, L.J. Global, regional, and national disability-adjusted life years (DALYs) for 306 diseases and injuries and healthy life expectancy (HALE) for 188 countries, 1990–2013: Quantifying the epidemiological transition. Lancet 2015, 386, 2145–2191. [Google Scholar] [CrossRef]
- World Health Organization: Regional Office for South-East Asia. Towards Eliminating Lymphatic Filariasis: Progress in the South-East.Region. (2001–2011); World Health Organization Regional Office for South-East Asia: New Delhi, India, 2013. [Google Scholar]
- Weil, G.J.; Jain, D.C.; Santhanam, S.; Malhotra, A.; Kumar, H.; Sethumadhavan, K.V.P.; Liftis, F.; Ghosh, T.K. A monoclonal antibody-based enzyme immunoassay for detecting parasite antigenemia in bancroftian filariasis. J. Infect. Dis. 1987, 156, 350–355. [Google Scholar] [CrossRef] [PubMed]
- Weil, G.J.; Lammie, P.J.; Weiss, N. The ICT filariasis test: A rapid-format antigen test for diagnosis of bancroftian filariasis. Parasitol. Today 1997, 13, 401–404. [Google Scholar] [CrossRef]
- Gass, K.; de Rochars, M.V.B.; Boakye, D.; Bradley, M.; Fischer, P.U.; Gyapong, J.; Itoh, M.; Ituaso-Conway, N.; Joseph, H.; Kyelem, D. A multicenter evaluation of diagnostic tools to define endpoints for programs to eliminate bancroftian filariasis. PLoS Negl. Trop. Dis. 2012, 6, e1479. [Google Scholar] [CrossRef] [PubMed]
- Lammie, P.J.; Weil, G.; Noordin, R.; Kaliraj, P.; Steel, C.; Goodman, D.; Lakshmikanthan, V.B.; Ottesen, E. Recombinant antigen-based antibody assays for the diagnosis and surveillance of lymphatic filariasis—A multicenter trial. Filaria J. 2004, 3, 9. [Google Scholar] [CrossRef] [PubMed]
- Rebollo, M.P.; Bockarie, M.J. Shrinking the lymphatic filariasis map: Update on diagnostic tools for mapping and transmission monitoring. Parasitology 2014, 141, 1912–1917. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Global Programme to Eliminate Lymphatic Filariasis: Practical Entomology; World Health Organization: Geneva, Switzerland, 2013. [Google Scholar]
- World Health Organization. Validation of Elimination of Lymphatic Filariasis as A Public Health Problem; World Health Organization: Geneva, Switzerland, 2017. [Google Scholar]
- World Health Organization. Transmission Assessment Surveys in the Global Programme to Eliminate Lymphatic Filariasis: WHO Position Statement; World Health Organization: Geneva, Switzerland, 2012. [Google Scholar]
- Sudomo, M.; Chayabejara, S.; Duong, S.; Hernandez, L.; Wu, W.P.; Bergquist, R. Elimination of lymphatic filariasis in Southeast Asia. Adv. Parasitol. 2010, 72, 205–233. [Google Scholar] [PubMed]
- Michael, E.; Bundy, D.A.P.; Grenfell, B.T. Re-assessing the global prevalence and distribution of lymphatic filariasis. Parasitology 1996, 112, 409–428. [Google Scholar] [CrossRef] [PubMed]
- Meyrowitsch, D.W.; Nguyen, D.T.; Hoang, T.H.; Nguyen, T.D.; Michael, E. A review of the present status of lymphatic filariasis in Vietnam. Acta Trop. 1998, 70, 335–347. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269. [Google Scholar] [CrossRef] [PubMed]
- PROSPERO Registered Study Protocol. Available online: http://www.crd.york.ac.uk/PROSPERO/display_record.asp?ID=CRD42014013070#.VAihrWSSxBA (accessed on 11 December 2016).
- World Health Organization. Institutional Repository of Information Sharing. Available online: http://apps.who.int/iris/ (accessed on 11 December 2016).
- Crowe, M. Crowe Critical Appraisal Tool (CCAT) User Guide; Conchra House: Scotland, UK, 2013. [Google Scholar]
- Jackson, R.; Ameratunga, S.; Broad, J.; Connor, J.; Lethaby, A.; Robb, G.; Wells, S.; Glasziou, P.; Heneghan, C. The GATE frame: Critical appraisal with pictures. Evid. Based Nurs. 2006, 9, 68–71. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Monitoring and Epidemiological Assessment of the Programme to Eliminate Lymphatic Filariasis at Implementation Unit Level; World Health Organization: Geneva, Switzerland, 2005. [Google Scholar]
- DerSimonian, R.; Laird, N. Meta-analysis in clinical trials. Controll. Clin. Trials 1986, 7, 177–188. [Google Scholar] [CrossRef]
- Higgins, J.; Thompson, S.G.; Deeks, J.J.; Altman, D.G. Measuring inconsistency in meta-analyses. BMJ 2003, 327, 557–560. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, A.F.; Ngui, R.; Muhammad Aidil, R.; Lim, Y.A.; Rohela, M. Current status of parasitic infections among Pangkor Island community in Peninsular Malaysia. Trop. Biomed. 2014, 31, 836–843. [Google Scholar] [PubMed]
- Bhumiratana, A.; Koyadun, S.; Srisuphanunt, M.; Satitvipawee, P.; Limpairojn, N.; Gaewchaiyo, G. Border and imported bancroftian filariases: Baseline seroprevalence in sentinel populations exposed to infections with Wuchereria bancrofti and concomitant HIV at the start of diethylcarbamazine mass treatment in Thailand. Southeast Asian J. Trop. Med. Public Health 2005, 36, 390–407. [Google Scholar] [PubMed]
- Bhumiratana, A.; Koyadun, S.; Suvannadabba, S.; Karnjanopas, K.; Rojanapremsuk, J.; Buddhirakkul, P.; Tantiwattanasup, W. Field trial of the ICT filariasis for diagnosis of Wuchereria bancrofti infections in an endemic population of Thailand. Southeast Asian J. Trop. Med. Public Health 1999, 30, 562–568. [Google Scholar] [PubMed]
- Bhumiratana, A.; Siriaut, C.; Koyadun, S.; Satitvipawee, P. Evaluation of a single oral dose of diethylcarbamazine 300 mg as provocative test and simultaneous treatment in Myanmar migrant workers with Wuchereria bancrofti infection in Thailand. Southeast Asian J. Trop. Med. Public Health 2004, 35, 591–598. [Google Scholar] [PubMed]
- Bhumiratana, A.; Wattanakull, B.; Koyadun, S.; Suvannadabba, S.; Rojanapremsuk, J.; Tantiwattanasup, W. Relationship between male hydrocele and infection prevalences in clustered communities with uncertain transmission of Wuchereria bancrofti on the Thailand-Myanmar border. Southeast Asian J. Trop. Med. Public Health 2002, 33, 7–17. [Google Scholar] [PubMed]
- Chansiri, K.; Phantana, S. A polymerase chain reaction assay for the survey of bancroftian filariasis. Southeast Asian J. Trop. Med. Public Health 2002, 33, 504–508. [Google Scholar] [PubMed]
- Cox-Singh, J.; Pomrehn, A.S.; Rahman, H.A.; Zakaria, R.; Miller, A.O.; Singh, B. Simple blood-spot sampling with nested polymerase chain reaction detection for epidemiology studies on Brugia malayi. Int. J. Parasitol. 1999, 29, 717–721. [Google Scholar] [CrossRef]
- Dutta, P.; Gogoi, B.K.; Chelleng, P.K.; Bhattacharyya, D.R.; Khan, S.A.; Goswami, B.K.; Mahanta, J. Filariasis in the labour population of a tea estate in Upper Assam. Indian J. Med. Res. 1995, 101, 245–246. [Google Scholar] [PubMed]
- Hafiz, I.; Graves, P.; Haq, R.; Flora, M.S.; Kelly-Hope, L.A. Clinical case estimates of lymphatic filariasis in an endemic district of Bangladesh after a decade of mass drug administration. Trans. R. Soc. Trop. Med. Hyg. 2015, 109, 700–709. [Google Scholar] [CrossRef] [PubMed]
- Hakim, S.L.; Vythilingam, I.; Marzukhi, M.I.; Mak, J.W. Single-dose diethylcarbamazine in the control of periodic brugian filariasis in Peninsular Malaysia. Trans. R. Soc. Trop. Med. Hyg. 1995, 89, 686–689. [Google Scholar] [CrossRef]
- Jamail, M.; Andrew, K.; Junaidi, D.; Krishnan, A.K.; Faizal, M.; Rahmah, N. Field validation of sensitivity and specificity of rapid test for detection of Brugia malayi infection. Trop. Med. Int. Health 2005, 10, 99–104. [Google Scholar] [CrossRef] [PubMed]
- Jiraamonnimit, C.; Wongkamchai, S.; Boitano, J.; Nochot, H.; Loymek, S.; Chujun, S.; Yodmek, S. A cohort study on anti-filarial IgG4 and its assessment in good and uncertain MDA-compliant subjects in brugian filariasis endemic areas in southern Thailand. J. Helminthol. 2009, 83, 351–360. [Google Scholar] [CrossRef] [PubMed]
- Khan, A.M.; Dutta, P.; Khan, S.A.; Baruah, N.K.; Sarma, C.K.; Mahanta, J. Prevalence of bancroftian filariasis in a foot-hill tea garden of upper Assam. J. Commun. Dis. 1999, 31, 145–146. [Google Scholar] [PubMed]
- Khan, A.M.; Dutta, P.; Khan, S.A.; Baruah, N.K.; Sharma, C.K.; Mahanta, J. Bancroftian filariasis in a weaving community of lower Assam. J. Commun. Dis. 1999, 31, 61–62. [Google Scholar] [PubMed]
- Khan, A.M.; Dutta, P.; Khan, S.A.; Mahanta, J. A focus of lymphatic filariasis in a tea garden worker community of central Assam. J. Environ. Biol. 2004, 25, 437–440. [Google Scholar] [PubMed]
- Khan, A.M.; Dutta, P.; Khan, S.A.; Mohapatra, P.K.; Baruah, N.K.; Sharma, C.K.; Mahanta, A.J. Lymphatic filariasis in two distinct communities of upper Assam. J. Commun. Dis. 1999, 31, 101–106. [Google Scholar] [PubMed]
- Khan, A.M.; Dutta, P.; Sarmah, C.K.; Baruah, N.K.; Das, S.; Pathak, A.K.; Sarmah, P.; Hussain, M.E.; Mahanta, J. Prevalence of lymphatic filariasis in a tea garden worker population of Dibrugarh (Assam), India after six rounds of mass drug administration. J. Vector Borne Dis. 2015, 52, 314–320. [Google Scholar] [PubMed]
- Koyadun, S.; Bhumiratana, A. Surveillance of imported bancroftian filariasis after two-year multiple-dose diethylcarbamazine treatment. Southeast Asian J. Trop. Med. Public Health 2005, 36, 822–831. [Google Scholar] [PubMed]
- Koyadun, S.; Bhumiratana, A.; Prikchu, P. Wuchereria bancrofti antigenemia clearance among Myanmar migrants after biannual mass treatments with diethylcarbamazine, 300 mg oral-dose FILADEC tablet, in Southern Thailand. Southeast Asian J. Trop. Med. Public Health 2003, 34, 758–767. [Google Scholar] [PubMed]
- Krairittichai, U.; Pungprakiet, D.; Boonthongtho, K.; Arsayot, K. Prevalence of infectious diseases of immigrant workers receiving health examinations at Rajavithi Hospital. J. Med. Assoc. Thail. 2012, 95 (Suppl. 3), S1–S6. [Google Scholar]
- Leang, R.; Socheat, D.; Bin, B.; Bunkea, T.; Odermatt, P. Assessment of disease and infection of lymphatic filariasis in Northeastern Cambodia. Trop. Med. Int. Health 2004, 9, 1115–1120. [Google Scholar] [CrossRef] [PubMed]
- Lim, B.H.; Rahmah, N.; Afifi, S.A.; Ramli, A.; Mehdi, R. Comparison of Brugia-ELISA and thick blood smear examination in a prevalence study of brugian filariasis in Setiu, Terengganu, Malaysia. Med. J. Malays. 2001, 56, 491–496. [Google Scholar]
- Medhi, G.K.; Hazarika, N.C.; Shah, B.; Mahanta, J. Study of health problems and nutritional status of tea garden population of Assam. Indian J. Med. Sci. 2006, 60, 496–505. [Google Scholar] [PubMed]
- Nuchprayoon, S.; Porksakorn, C.; Junpee, A.; Sanprasert, V.; Poovorawan, Y. Comparative assessment of an Og4C3 ELISA and an ICT filariasis test: A study of Myanmar migrants in Thailand. Asian Pac. J. Allergy Immunol. 2003, 21, 253–257. [Google Scholar] [PubMed]
- Nuchprayoon, S.; Sanprasert, V.; Porksakorn, C.; Nuchprayoon, I. Prevalence of bancroftian filariasis on the Thai-Myanmar border. Asian Pac. J. Allergy Immunol. 2003, 21, 179–188. [Google Scholar] [PubMed]
- Nuchprayoon, S.; Yentakam, S.; Sangprakarn, S.; Junpee, A. Endemic bancroftian filariasis in Thailand: detection by Og4C3 antigen capture ELISA and the polymerase chain reaction. J. Med. Assoc. Thail. 2001, 84, 1300–1307. [Google Scholar]
- Prakash, A.; Mohapatra, P.K.; Das, H.K.; Sharma, R.K.; Mahanta, J. Bancroftian filariasis in Namrup tea estate, district Dibrugarh, Assam. Indian J. Public Health 1998, 42, 103–107. [Google Scholar] [PubMed]
- Priest, J.W.; Jenks, M.H.; Moss, D.M.; Mao, B.; Buth, S.; Wannemuehler, K.; Soeung, S.C.; Lucchi, N.W.; Udhayakumar, V.; Gregory, C.J. Integration of multiplex bead assays for parasitic diseases into a national, population-based serosurvey of women 15–39 years of age in Cambodia. PLoS Negl. Trop. Dis. 2016, 10, e0004699. [Google Scholar] [CrossRef] [PubMed]
- Rahmah, N.; Lim, B.H.; Azian, H.; Ramelah, T.S.; Rohana, A.R. Short communication: Use of a recombinant antigen-based ELISA to determine prevalence of brugian filariasis among Malaysian schoolchildren near Pasir Mas, Kelantan-Thailand border. Trop. Med. Int. Health 2003, 8, 158–163. [Google Scholar] [CrossRef] [PubMed]
- Rahmah, N.; Nurulhasanah, O.; Norhayati, S.; Zulkarnain, I.; Norizan, M. Comparison of conventional versus real-time PCR detection of Brugia malayi DNA from dried blood spots from school children in a low endemic area. Trop. Biomed. 2010, 27, 54–59. [Google Scholar] [PubMed]
- Saha, A.K.; Mohanta, M.K. Bancroftian elephantiasis in Nilphamari, Bangladesh. Mymensingh Med. J. MMJ 2011, 20, 40–44. [Google Scholar] [PubMed]
- Samad, M.S.; Itoh, M.; Moji, K.; Hossain, M.; Mondal, D.; Alam, M.S.; Kimura, E. Enzyme-linked immunosorbent assay for the diagnosis of Wuchereria bancrofti infection using urine samples and its application in Bangladesh. J. Parasitol. Res. 2013, 62, 564–567. [Google Scholar] [CrossRef] [PubMed]
- Satimai, W.; Jiraamonnimit, C.; Thammapalo, S.; Choochote, W.; Luenee, P.; Boitano, J.J.; Wongkamchai, S. The impact of a national program to eliminate lymphatic filariasis in selected Myanmar immigrant communities in Bangkok and Ranong Province, Thailand. Southeast Asian J. Trop. Med. Public Health 2011, 42, 1054–1064. [Google Scholar] [PubMed]
- Swaddiwudhipong, W.; Tatip, Y.; Meethong, M.; Preecha, P.; Kobasa, T. Potential transmission of bancroftian filariasis in urban Thailand. Southeast Asian J. Trop. Med. Public Health 1996, 27, 847–849. [Google Scholar] [PubMed]
- Triteeraprapab, S.; Karnjanopas, K.; Porksakorn, C.; Sai-Ngam, A.; Yentakam, S.; Loymak, S. Lymphatic filariasis caused by Brugia malayi in an endemic area of Narathiwat Province, southern of Thailand. J. Med. Assoc. Thail. 2001, 84 (Suppl. S1), S182–S188. [Google Scholar]
- Triteeraprapab, S.; Nuchprayoon, I.; Porksakorn, C.; Poovorawan, Y.; Scott, A.L. High prevalence of Wuchereria bancrofti infection among Myanmar migrants in Thailand. Ann. Trop. Med. Parasitol. 2001, 95, 535–538. [Google Scholar] [CrossRef] [PubMed]
- Triteeraprapab, S.; Songtrus, J. High prevalence of bancroftian filariasis in Myanmar-migrant workers: A study in Mae Sot district, Tak province, Thailand. J. Med. Assoc. Thail. 1999, 82, 735–739. [Google Scholar]
- Wan Omar, A.; Sulaiman, O.; Yusof, S.; Ismail, G.; Fatmah, M.S.; Rahmah, N.; Khairul, A.A. Epidemiological screening of lymphatic filariasis among immigrants using dipstick colloidal dye immunoassay. Malays. J. Med. Sci. 2001, 8, 19–24. [Google Scholar] [PubMed]
- World Health Organization: Regional Office for South-East Asia. Elimination of Lymphatic Filariasis in the South-East Asia Region: Report of the Eighth Meeting of National National Programme Managers; WHO Regional Office for South-East Asia: New Delhi, India, 2011. [Google Scholar]
- World Health Organization: Regional Office for South-East Asia. Elimination of Lymphatic Filariasis in the South-East Asia Region: Report of the Fifth Meeting of National National Programme Managers; WHO Regional Office for South-East Asia: New Delhi, India, 2006. [Google Scholar]
- United States Agency for International Development. FHI360/USAID. End Neglected Tropical Diseases in Asia: Final Report; USAID: Washington, DC, USA, 2015.
- World Health Organization: Regional Office for the Western Pacific. First Mekong-Plus Programme Managers Workshop on Lymphatic Filariasis and Other Helminthiasis, Phnom Penh, Cambodia, 23–26 March 2009; WHO Regional Office for the Western Pacific: Manila, Philippines, 2009. [Google Scholar]
- World Health Organization: Regional Office for the Western Pacific. Malaysia: Country Cooperation Strategy 2009–2013; WHO Regional Office for the Western Pacific: Manila, Philippines, 2010. [Google Scholar]
- Myanmar Ministry of Health. Myanmar National Programme to Eliminate Lymphatic Filariasis: Annual Report (2005); Myanmar Ministry of Health: Naypyitaw, Myanmar, 2005.
- Myanmar Ministry of Health. Myanmar National Programme to Eliminate Lymphatic Filariasis: Annual Report (2011); Myanmar Ministry of Health: Naypyitaw, Myanmar, 2011.
- Myanmar Ministry of Health. Myanmar National Programme to Eliminate Lymphatic Filariasis: Annual Report (2012); Myanmar Ministry of Health: Naypyitaw, Myanmar, 2012.
- World Health Organization: Regional Office for South-East Asia. Regional Stategic Plan. for Elimination of Lymphatic Filariasis (2004–2007); WHO Regional Office for South-East Asia: New Delhi, India, 2004. [Google Scholar]
- World Health Organization: Regional Office for the Western Pacific. Report of the Thirteenth Meeting of the Western Pacific Regional Programme Review Group on Neglected Tropical Diseases; WHO Regional Office for the Western Pacific: Manila, Philippines, 2013. [Google Scholar]
- World Health Organization. UNDP-World Bank-WHO Special Programme for Research and Training in Tropical Diseases WHO-UNICEF Joint Programme for Health Mapping World Health Organization: Division of Tropical Diseases. Research on Rapid Geographical Assessment of Bancroftian Filariasis; World Health Organization: Geneva, Switzerland, 1998. [Google Scholar]
- World Health Organization: Regional Office for South-East Asia. South-East Asia Regional Programme Review Group of Elimination of Lymphatic Filariasis: Report of the Eight Meeting; WHO Regional Office for South-East Asia: New Delhi, India, 2011. [Google Scholar]
- World Health Organization: Regional Office for South-East Asia. South.-East. Asia Regional Programme Review Group of Elimination of Lymphatic Filariasis: Report of the First Meeting; WHO Regional Office for South-East Asia: New Delhi, India, 2005. [Google Scholar]
- World Health Organization: Regional Office for South-East Asia. South.-East. Asia Regional Programme Review Group of Elimination of Lymphatic Filariasis: Report of the Ninth Meeting; WHO Regional Office for South-East Asia: New Delhi, India, 2012. [Google Scholar]
- World Health Organization: Regional Office for South-East Asia. South.-East. Asia Regional Programme Review Group of Elimination of Lymphatic Filariasis: Report of the Seventh Meeting; WHO Regional Office for South-East Asia: New Delhi, India, 2010. [Google Scholar]
- World Health Organization: Regional Office for South-East Asia. South.-East. Asia Regional Programme Review Group of Elimination of Lymphatic Filariasis: Report of the Tenth Meeting; WHO Regional Office for South-East Asia: New Delhi, India, 2013. [Google Scholar]
- World Health Organization: Regional Office for the Western Pacific. Report of the Fourteenth Meeting of the Western Pacific Regional Programme Review Group on Neglected Tropical Diseases; WHO Regional Office for the Western Pacific: Manila, Philippines, 2014. [Google Scholar]
- World Health Organization. Strengthening the Assessment of Lymphatic Filariasis Transmission and Documenting the Achievement of Elimination; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- Cambodia Ministry of Planning. General Population Census of Cambodia 1998: Final Results, 2nd ed.; Cambodia Ministry of Planning: Phnom Penh, Cambodia, 2002.
- Beng, T.S.; Ahmad, R.; Hisam, R.S.R.; Heng, S.K.; Leaburi, J.; Ismail, Z.; Sulaiman, L.H.; Soyoti, R.F.H.M.; Lim, L.H. Molecular xenomonitoring of filarial infection in Malaysian mosquitoes under the National Program for Elimination of Lymphatic Filariasis. Southeast Asian J. Trop. Med. Public Health 2016, 47, 617–624. [Google Scholar]
- Mathieu, E.; Amann, J.; Eigege, A.; Richards, F.; Sodahlon, Y. Collecting baseline information for national morbidity alleviation programs: Different methods to estimate lymphatic filariasis morbidity prevalence. Am. J. Trop. Med. Hyg. 2008, 78, 153–158. [Google Scholar] [PubMed]
- Triteeraprapab, S.; Kanjanopas, K.; Suwannadabba, S.; Sangprakarn, S.; Poovorawan, Y.; Scott, A.L. Transmission of the nocturnal periodic strain of Wuchereria bancrofti by Culex quinquefasciatus: Establishing the potential for urban filariasis in Thailand. Epidemiol. Infect. 2000, 125, 207–212. [Google Scholar] [CrossRef] [PubMed]
- Bhumiratana, A.; Intarapuk, A.; Koyadun, S.; Maneekan, P.; Sorosjinda-Nunthawarasilp, P. Current bancroftian filariasis elimination on Thailand-Myanmar border: Public Health Challenges toward Postgenomic MDA Evaluation. ISRN Trop. Med. 2013, 2013. [Google Scholar] [CrossRef]
- Toothong, T.; Tipayamongkholgul, M.; Suwannapong, N.; Suvannadabba, S. Evaluation of mass drug administration in the program to control imported lymphatic filariasis in Thailand. BMC Public Health 2015, 15, 975. [Google Scholar] [CrossRef] [PubMed]


| Study (Publication Date) [Study Period] [Ref.] | Study Design | Sampling Population/Unit (Age of Participants) | Sample Size | Diagnostic Method | |
|---|---|---|---|---|---|
| Infection | Morbidity | ||||
| Bangladesh | |||||
| Hafiz et al. (2015) (2011) [33] | CSS b | Households in 30 villages (≥10) | 1242 | Mf, ICT | Hyd./Lymph. h |
| Saha et al. (2011) [NS g] [55] | CSS | Households in 19 unions (≥1) | 232,005 | - | Lymph. |
| Samad et al. (2013) [NS] [56] | FDE a | School children (5–10) | 319 | ICT, IgG4 e | - |
| Cambodia | |||||
| Leang et al. (2004) (2000–2001) [45] | CSS | 83 villages (≥1) | 3468 | Mf, ICT | Hyd./Lymph. |
| Priest et al. (2016) (2012) [52] | CSS | 2200 households (women 15–39) | 2150 | IgG4 | - |
| Northeast India | |||||
| Dutta et al. (1995) (1992) [32] | CSS | Individuals in 1 tea estate (≥1) | 1553 | Mf | NS |
| Khan et al. (1999) [NS] Study 1 [37] | CSS | Individuals in 1 tea estate (≥1) | 821 | Mf | Hyd./Lymph. |
| Khan et al. (1999) [NS] Study 2 [40] | CSS | 2 communities: tea workers and non-tea workers (≥1) | 1446 | Mf | NS |
| Khan et al. (1999) [NS] Study 3 [38] | CSS | 1 weaving community (≥1) | 446 | Mf | - |
| Khan et al. (2004) [NS] [39] | CSS | Individuals in 1 tea estate (≥1) | 656 | Mf | Hyd./Lymph. |
| Khan et al. (2015) (2012–2013) [41] | CSS | Individuals in 1 tea estate (infection ≥2, morbidity ≥18) | 634 | Mf | Hyd./Lymph. |
| Medhi et al. (2006) (2002–2003) [47] | CSS | Households in 8 tea estates (≥1) | 4016 | Mf | Hyd./Lymph. |
| Prakash et al. (1998) (1994) [51] | CSS | Households in 1 tea estate (≥1) | 1105 | Mf | Hyd./Lymph. |
| Malaysia | |||||
| Ahmad et al. (2014) [NS] [25] | CSS | Households/schools on 1 island (≥1) | 298 | Mf | - |
| Cox-Singh et al. (1999) [NS] [31] | CSS | 2 districts (NS) | 145 | Mf, PCR | - |
| Hakim et al. (1995) (1992) [34] | FDT c | 2 villages (≥6 months old) | 499 | Mf | - |
| Jamail et al. (2005) (2001–2002) [35] | FDE | 7 districts(≥1) | 2545 | Mf, IgG4 | - |
| Lim et al (2001) [NS] [46] | FDE | 5 villages and 2 schools (≥1) | 1134 | Mf, IgG4 | - |
| Rahmah et al. (2003) [NS] [53] | FDE | 16 schools (7–12) | 5138 | IgG4 | - |
| Rahmah et al. (2010) [NS] [54] | FDE | School children (6–10) | 973 | IgG4 | - |
| Wan Omar et al. (2001) [NS] [62] | FDE | Migrant workers in palm oil estates (WA i) | 630 | Mf | Lymph. |
| Thailand | |||||
| Bhumiratana et al. (2004) (2002) [28] | FDT | Myanmar workers (WA i) | 860 | Mf, ICT, Og4C3 | - |
| Bhumiratana et al. (2005) (1998–2001) [26] | CSS | Myanmars and Thais in multiple villages (≥1) | 433 | Mf, ICT, Og4C3 | - |
| Bhumiratana et al. (1999) (1998) [27] | FDE | Multiple villages (≥1) | 225 | Mf, ICT | Hyd. |
| Bhumiratana et al (2002) (1999) [29] | CSS | 1 village (≥1) | 219 | Mf, ICT | Hyd. |
| Chansiri et al. (2002) (1997–2001) [30] | CSS | Migrant workers in 4 provinces (WA i) | 1299 | PCR | - |
| Jiraamonnimit et al. (2009) (2005 to 2006] [36] | LO d | 3 provinces (≥7) | 500 | Mf, IgG4 | Lymph. |
| Koyadun et al. (2003) (2001–2002) [43] | FDT | Myanmar migrants and Thais in 3 districts (≥15) | 660 | ICT | - |
| Koyadun et al. (2005) (2003) [42] | CSS | Myanmar workers (≥10) | 904 | Mf | - |
| Krairittichai et al. (2012) (2010) [44] | RCS f | Migrant workers at 1 hospital (WA i) | 102,090 | Mf | - |
| Nuchprayoon et al. (2003) [NS] Study 1 [48] | FDE | Myanmar workers at 2 factories (WA i) | 337 | Mf, ICT, Og4C3 | Hyd. |
| Nuchprayoon et al. (2003) [NS] Study 2 [49] | CSS | 2 villages (≥1) | 433 | Mf, Og4C3, IgG4 | - |
| Nuchprayoon et al. (2001) [NS] [50] | CSS | 1 sub-district (≥1) | 196 | Mf, Og4C3, PCR | - |
| Satimai et al. (2011) [NS] [57] | CSS | Myanmar migrants and Thais in 2 provinces (≥1) | 1031 | ICT, IgG4 | - |
| Swaddiwudhipong et al. (1996) (1995) [58] | CSS | Myanmar workers and their families (≥1) | 8377 | Mf | NS |
| Triteeraprapab et al. (1999) [NS] [61] | CSS | Myanmar workers in 6 industrial plants (WA i) | 654 | Mf | - |
| Triteeraprapab et al. (2001) [NS] Study 1 [59] | CSS | 4 districts in 1 province (≥1) | 2462 | Mf | - |
| Triteeraprapab et al. (2001) (1999) Study 2 [60] | CSS | Myanmar migrants in 1 community (≥2) | 371 | Mf, Og4C3, IgG4 | - |
| Reports [Ref.] | Year | Sample Size | Diagnostic Method | |
|---|---|---|---|---|
| Infection | Morbidity | |||
| Annual Reports | ||||
| Myanmar Ministry of Health. National Program to Eliminate LF: Annual Reports [68,69,70] | 2004 | 23,668 | Mf | - |
| 2011 | 10,845 | Mf | - | |
| 2012 | 14,649 | Mf | Hyd./Lymph. c | |
| World Health Organization Reports | ||||
| WHO SEARO: Elimination of lymphatic filariasis in the Southeast Asia Region. Reports of the 1st, 7th, 8th, 9th, 10th Meeting of the Regional Program Review Group. [74,75,76,77,78] | 2005 | NS b | Mf (ICT) a | Hyd./Lymph. |
| 2010 | ||||
| 2011 | ||||
| 2012 | ||||
| 2013 | ||||
| WHO Regional Office for Southeast Asia: Elimination of lymphatic filariasis in the Southeast Asia Region. Reports of the 5th and 8th Meeting of the Regional Program Managers. [63,64] | 2006 | NS | Mf (ICT) a | Hyd./Lymph. |
| 2011 | ||||
| WHO Regional Office for Southeast Asia: Towards eliminating lymphatic filariasis: Progress in the Southeast Asia Region (2001–2011). [5] | 2013 | NS | Mf | Hyd./Lymph. |
| WHO Regional Office for Southeast Asia: Regional Strategic Plan for Elimination of Lymphatic Filariasis (2004–2007). [71] | 2004 | NS | Mf | Hyd./Lymph. |
| WHO Western Pacific Region: First Mekong-Plus Program Managers Workshop on Lymphatic Filariasis and Other Helminthiasis. [66] | 2009 | Cambodia: 23,705 Lao PDR: 9286 Vietnam: 18,302 | Mf/ICT | Hyd./Lymph. |
| WHO Regional Office for the Western Pacific. Reports of the 13th and 14th Meeting of the Western Pacific Regional Program Review Group on Neglected Tropical Diseases. [72,79] | 2013 | NS | Mf/ICT | Hyd./Lymph. |
| 2014 | ||||
| WHO Malaysia Office. Country Cooperation Strategy 2009–2013. [67] | 2010 | NS | Mf | - |
| WHO: Meeting of the Neglected Tropical Disease Strategic and Technical Advisory Group’s Monitoring and Evaluation Subgroup on Disease Specific Indicators. [80] | 2014 | NS | Mf | - |
| UNDP/World Bank/WHO/UNICEF. Research on rapid geographical assessment of Bancroftian filariasis. [73] | 1997 | 7000 | ICT | - |
| Non-Governmental Organization Reports | ||||
| Family Health International 360 and USAID: End Neglected Tropical Diseases in Asia Final Report. [65] | 2015 | Cambodia: 18,809 Lao PDR:3472 Vietnam: NS | Mf/ICT | Hyd./Lymph. |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dickson, B.F.R.; Graves, P.M.; McBride, W.J. Lymphatic Filariasis in Mainland Southeast Asia: A Systematic Review and Meta-Analysis of Prevalence and Disease Burden. Trop. Med. Infect. Dis. 2017, 2, 32. https://doi.org/10.3390/tropicalmed2030032
Dickson BFR, Graves PM, McBride WJ. Lymphatic Filariasis in Mainland Southeast Asia: A Systematic Review and Meta-Analysis of Prevalence and Disease Burden. Tropical Medicine and Infectious Disease. 2017; 2(3):32. https://doi.org/10.3390/tropicalmed2030032
Chicago/Turabian StyleDickson, Benjamin F. R., Patricia M. Graves, and William J. McBride. 2017. "Lymphatic Filariasis in Mainland Southeast Asia: A Systematic Review and Meta-Analysis of Prevalence and Disease Burden" Tropical Medicine and Infectious Disease 2, no. 3: 32. https://doi.org/10.3390/tropicalmed2030032
APA StyleDickson, B. F. R., Graves, P. M., & McBride, W. J. (2017). Lymphatic Filariasis in Mainland Southeast Asia: A Systematic Review and Meta-Analysis of Prevalence and Disease Burden. Tropical Medicine and Infectious Disease, 2(3), 32. https://doi.org/10.3390/tropicalmed2030032







