Newborn Sickle Cell and Thalassaemia Screening Programme: Automating and Enhancing the System to Evaluate the Screening Programme
Abstract
:1. Introduction
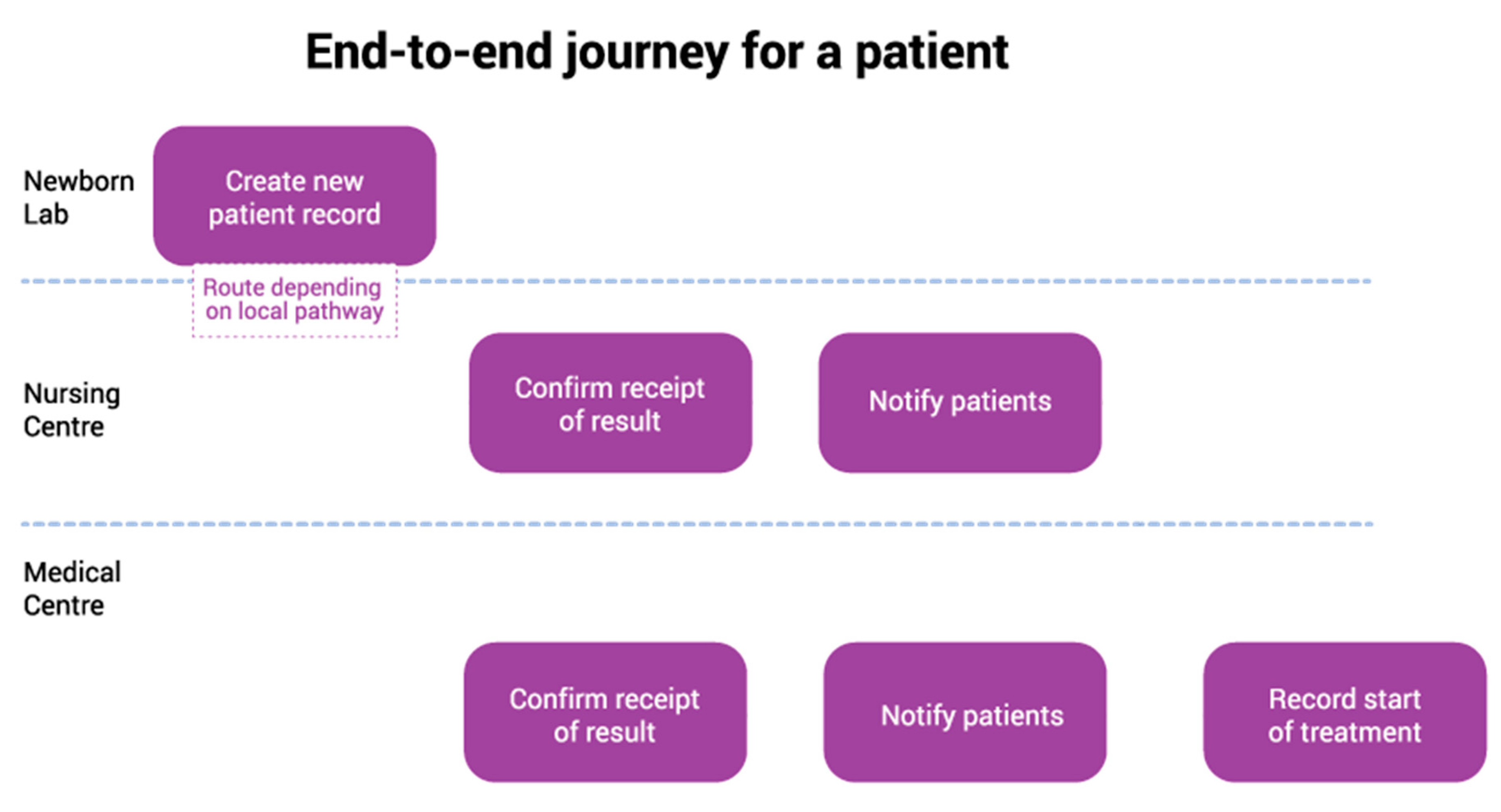
- records of babies already in the system that require follow up;
- babies identified by newborn screening as screen positive for sickle cell disease or thalassaemia;
- babies with sickle cell disease or thalassaemia presenting clinically.
- the health of affected babies or children;
- timeliness of entry into care and start of their treatment;
- what can be learned from babies that die.
- improve patient safety by allowing users to view the status of patients along the care pathway;
- alert clinicians when important milestones (timely results to parents and entry into paediatric care) are breached;
- improve the quality and completeness of data to evaluate the programme;
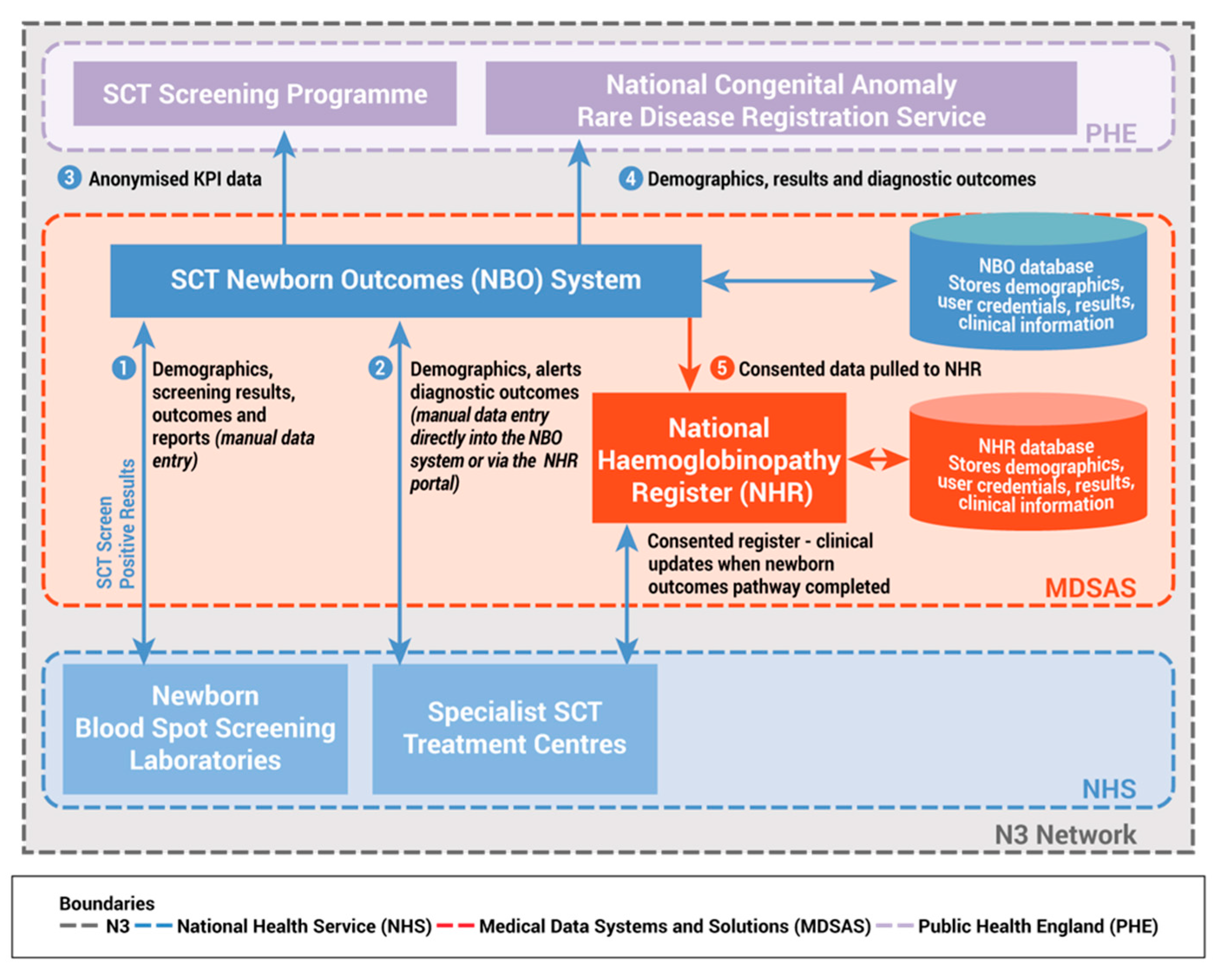
- reduce duplication of data entry by integrating with the National Haemoglobinopathy Register (NHR), a database of patients with haemoglobinopathies living in the UK and NCARDRS;
- reduce manual chasing through automated prompts;
- improve reporting so that users can monitor local performance and return annual data to PHE.
2. Materials and Methods
2.1. Discovery
2.2. Alpha Phase
- build prototypes of your service;
- test your prototypes with users;
- demonstrate that the service you want to build is technically possible;
- find the problems with the design of your service and decide how you will solve them;
- make some estimates about how much your service will cost;
- identify the biggest risks for the Beta stage as early as possible.
- a Scrum Master (MDSAS Project Manager);
- a Scrum Team (MDSAS IT Business Analyst, Development, Operational and Implementation Team, PHE Project Lead, Programme Manager and Screening Technical Projects Manager);
- MDSAS and PHE Information and Clinical Governance Specialists and Clinical Safety Officers.
- user engagement,
- daily stand-up,
- backlog refinement.
2.3. Beta Phase
2.4. Initial Development
2.5. Private Beta
2.6. Public Beta
3. Results
4. Discussion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- PHE Sickle Cell and Thalassaemia Screening Standards. Available online: https://www.gov.uk/government/publications/sickle-cell-and-thalassaemia-screening-programme-standards/sickle-cell-and-thalassaemia-screening-standards-valid-for-data-collected-from-1-april-2019 (accessed on 21 July 2019).
- PHE. Sickle Cell and Thalassaemia Screening: Outcome Data Collection Template. Available online: https://www.gov.uk/government/publications/sickle-cell-and-thalassaemia-screening-outcome-data-collection-template (accessed on 9 July 2019).
- Streetly, A.; Sisodia, R.; Dick, M.; Latinovic, R.; Hounsell, K.; Dormandy, E. Evaluation of newborn sickle cell screening programme in England: 2010–2016. Arch. Dis. Child. 2017. Available online: https://adc.bmj.com/content/archdischild/early/2017/11/02/archdischild-2017-313213.full.pdf (accessed on 9 July 2019).
- Government Digital Service. Service Manual. Available online: https://www.gov.uk/service-manual (accessed on 24 July 2019).
- MDSAS and PHE. SCT Newborn Outcomes Alpha Phase Report; MDSAS and PHE: London, UK, March 2018. [Google Scholar]
- NHS Digital. General Data Protection Regulation. Available online: https://digital.nhs.uk/data-and-information/looking-after-information/data-security-and-information-governance/information-governance-alliance-iga/general-data-protection-regulation-gdpr-guidance (accessed on 21 July 2019).
- NHS Digital. Clinical Risk Management Standards. Available online: https://digital.nhs.uk/services/solution-assurance/the-clinical-safety-team/clinical-risk-management-standards (accessed on 21 July 2019).
- PHE. Guidance on Using the Sickle Cell and Thalassaemia Newborn Outcomes System, March 2019. Available online: https://www.gov.uk/government/publications/sickle-cell-and-thalassaemia-screening-newborn-outcomes-system (accessed on 21 July 2019).
- Service Specification No 170126S. Specialist Haemoglobinopathy Services (All Ages) Specialist Haemoglobinopathy Teams. Available online: https://www.england.nhs.uk/wp-content/uploads/2019/07/Specialist-Haemoglobinopathy-Teams-Service-Specification.pdf (accessed on 21 August 2019).
| Laboratory scientists/directors | 5 |
| Haematologists/paediatricians | 5 |
| SCT specialist nurse/counsellors | 2 |
| Patients societies/parent representatives | 4 |
| PHE information & governance leads/programme manager | 3 |
| NHR CEO | 1 |
| Newborn outcomes team at KCL administrator/analyst/paediatrician | 3 |
| Findings | Recommendations |
|---|---|
| There is currently no consolidated list of patients that people have submitted data on and are under their care, which means that relevant individuals have no visibility of the patient’s care beyond their step in the pathway. Without this access they rely on other departments for this information, and the process of requesting this data can be manual and time consuming. | A future solution should allow people who submit data to the programme to be able to view and export a consolidated list of all relevant patients. |
| There is duplication of effort inputting and submitting data. With no integration between systems, users are required to input the same data multiple times. For example, when haematologists receive a new patient, commonly they will need to input the same information on the NHR. | A future solution needs to, where possible, reduce the amount of duplicated effort. Thus, how a future solution could interact with existing systems to avoid the need to enter data more than once needs to be explored. |
| There is a lack of feedback from the newborn outcomes team when users have submitted the data. Many people interviewed felt they would benefit from a feedback mechanism and reports to improve their overall performance. | The future solution should include automatic confirmation when data has been received or uploaded. There should be functionality to allow reports to be created centrally. The ability for users outside of the central team to pull their own reports from a predefined reporting list should also be considered. |
| Poor quality data is submitted when users do not use the prescribed templates for submitting data, this requires a lot of manual effort to cleanse and reformat the data. It also makes it difficult to produce accurate reports if there is data missing. | There needs to be a clearly defined dataset. The future solution will need to have data validation rules to limit individuals from entering data that shouldn’t be on there and ensuring data quality and completeness. |
| The current process requires a lot of manual chasing of individuals for data. Eliciting information from haematologists/sickle cell counsellors can be challenging. | The future process will need to make sure that there are incentives to drive user adoption and ensure that data is submitted to the programme. For example, reducing their overall work effort. The new solution will also need to be user-friendly so that individuals are not put off submitting data. |
| Must | A key requirement, without which the system has no value |
| Should | An important requirement that must be delivered, but, where time is short, could be delayed for a future delivery. This should be a short-term delay. |
| Could | A requirement that would be beneficial to include if it does not cost too much or take too long to deliver, but that is not central to the project objectives. |
| Would | A requirement that will be needed in the future, but that is not required for this delivery. |
| “As a lab user I need diagnostic results so that I can QA the service and I need access to performance reports so that I can return data to PHE” |
| “As a paediatric haematologist I need to be able to pull data from the NBO system onto the NHR when parents’ consent so that I can avoid duplication of effort”. |
| “As a specialist nurse I need to be able to refer babies into treatment services so that I can ensure care is provided at the right centre”. |
| “As any user I need to visualise the patient’s progress along the pathway so that I am assured of safe handover from screening into treatment services” |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Coppinger, C.; O’Loughlin, R. Newborn Sickle Cell and Thalassaemia Screening Programme: Automating and Enhancing the System to Evaluate the Screening Programme. Int. J. Neonatal Screen. 2019, 5, 30. https://doi.org/10.3390/ijns5030030
Coppinger C, O’Loughlin R. Newborn Sickle Cell and Thalassaemia Screening Programme: Automating and Enhancing the System to Evaluate the Screening Programme. International Journal of Neonatal Screening. 2019; 5(3):30. https://doi.org/10.3390/ijns5030030
Chicago/Turabian StyleCoppinger, Catherine, and Robyn O’Loughlin. 2019. "Newborn Sickle Cell and Thalassaemia Screening Programme: Automating and Enhancing the System to Evaluate the Screening Programme" International Journal of Neonatal Screening 5, no. 3: 30. https://doi.org/10.3390/ijns5030030
APA StyleCoppinger, C., & O’Loughlin, R. (2019). Newborn Sickle Cell and Thalassaemia Screening Programme: Automating and Enhancing the System to Evaluate the Screening Programme. International Journal of Neonatal Screening, 5(3), 30. https://doi.org/10.3390/ijns5030030




