Variant Sciatic Nerve Anatomy in Relation to the Piriformis Muscle on Magnetic Resonance Neurography: A Potential Etiology for Extraspinal Sciatica
Abstract
1. Introduction
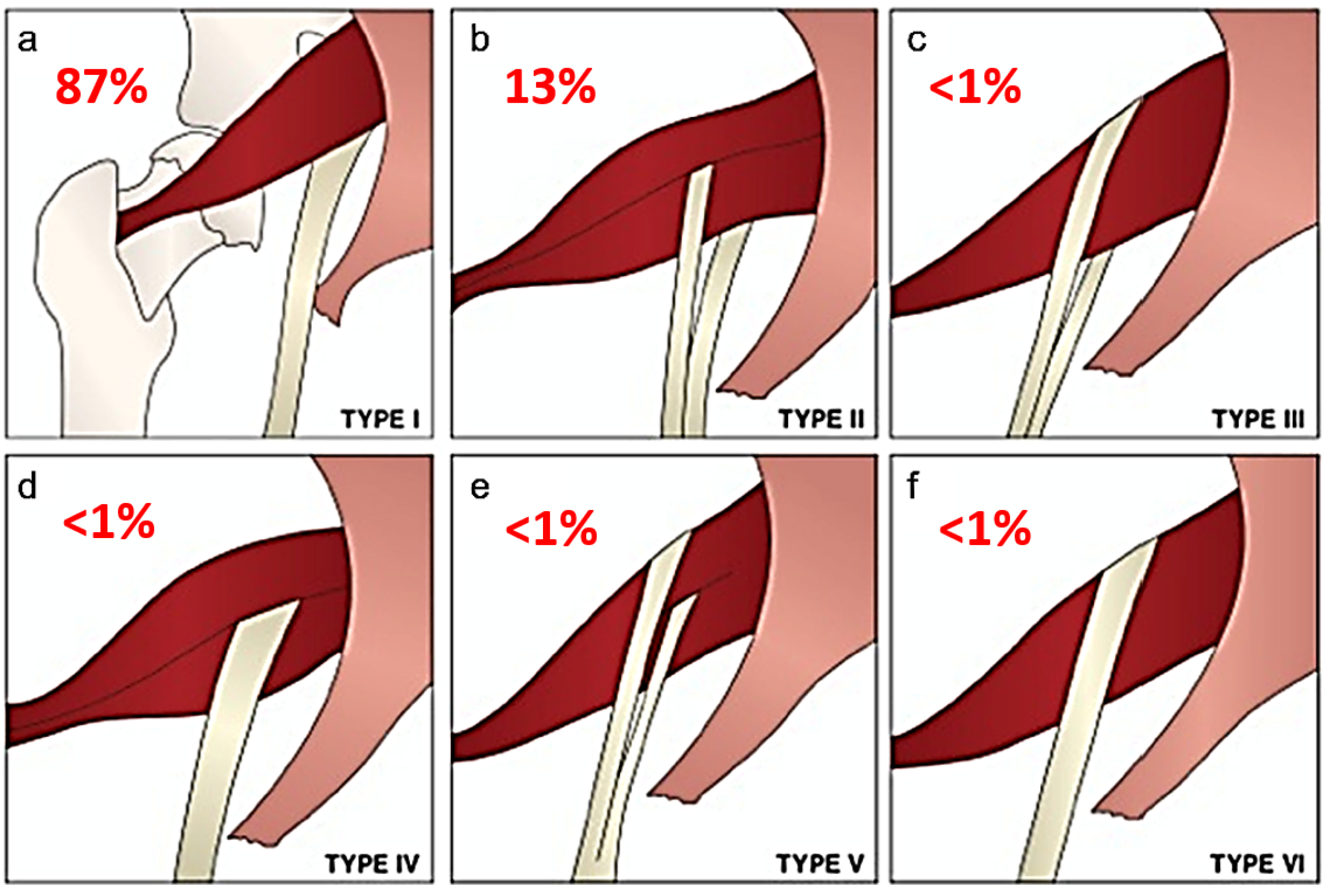
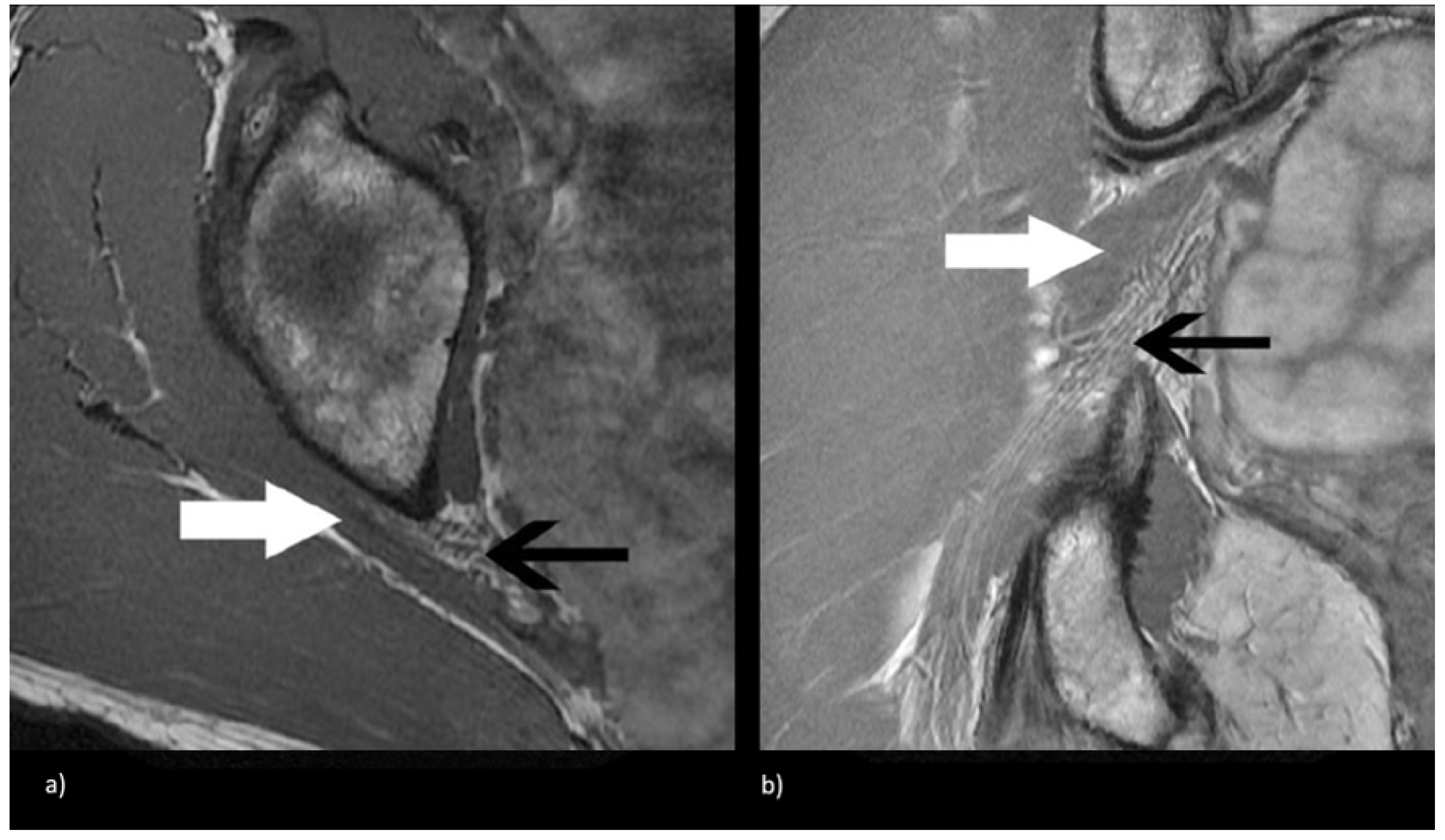
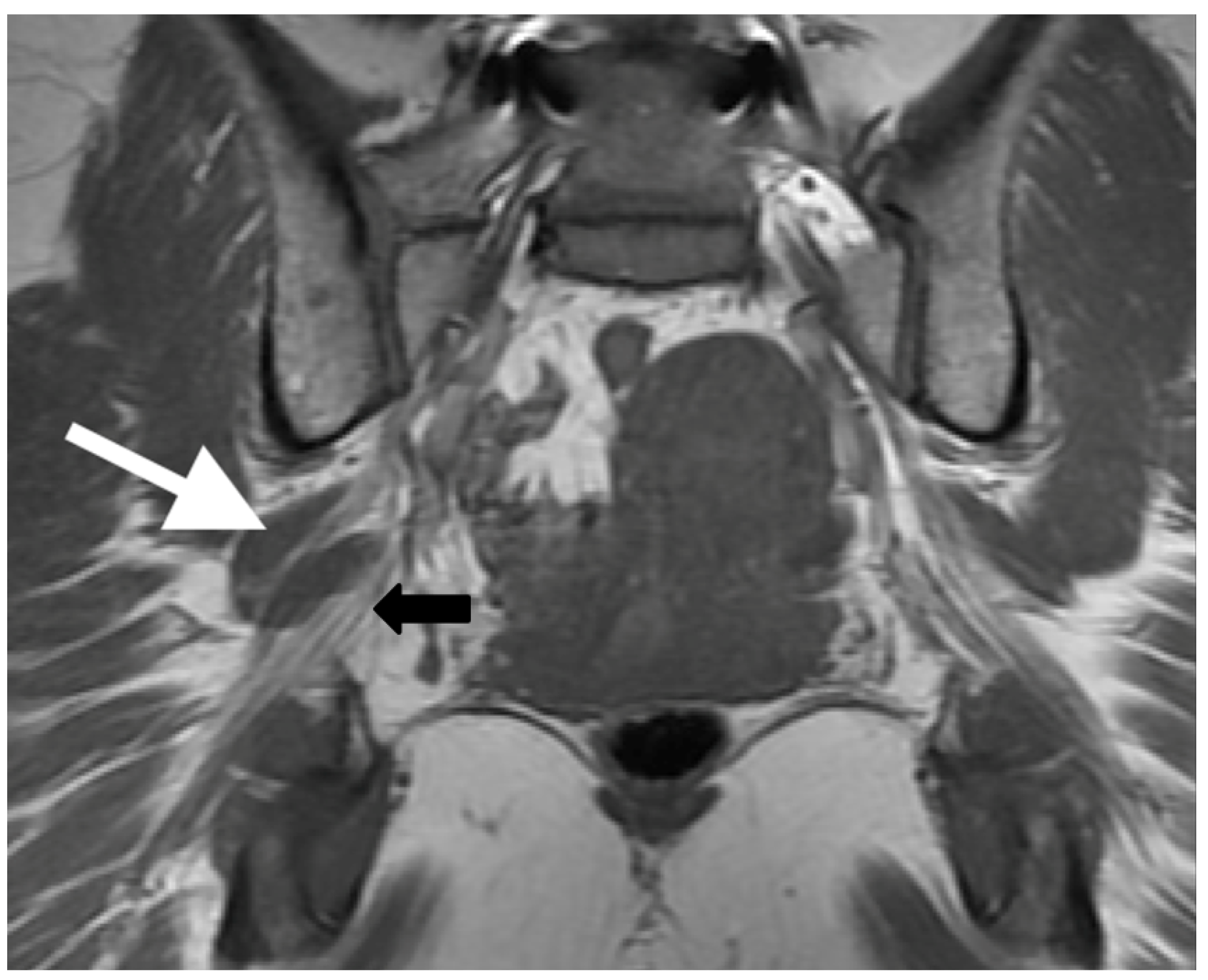
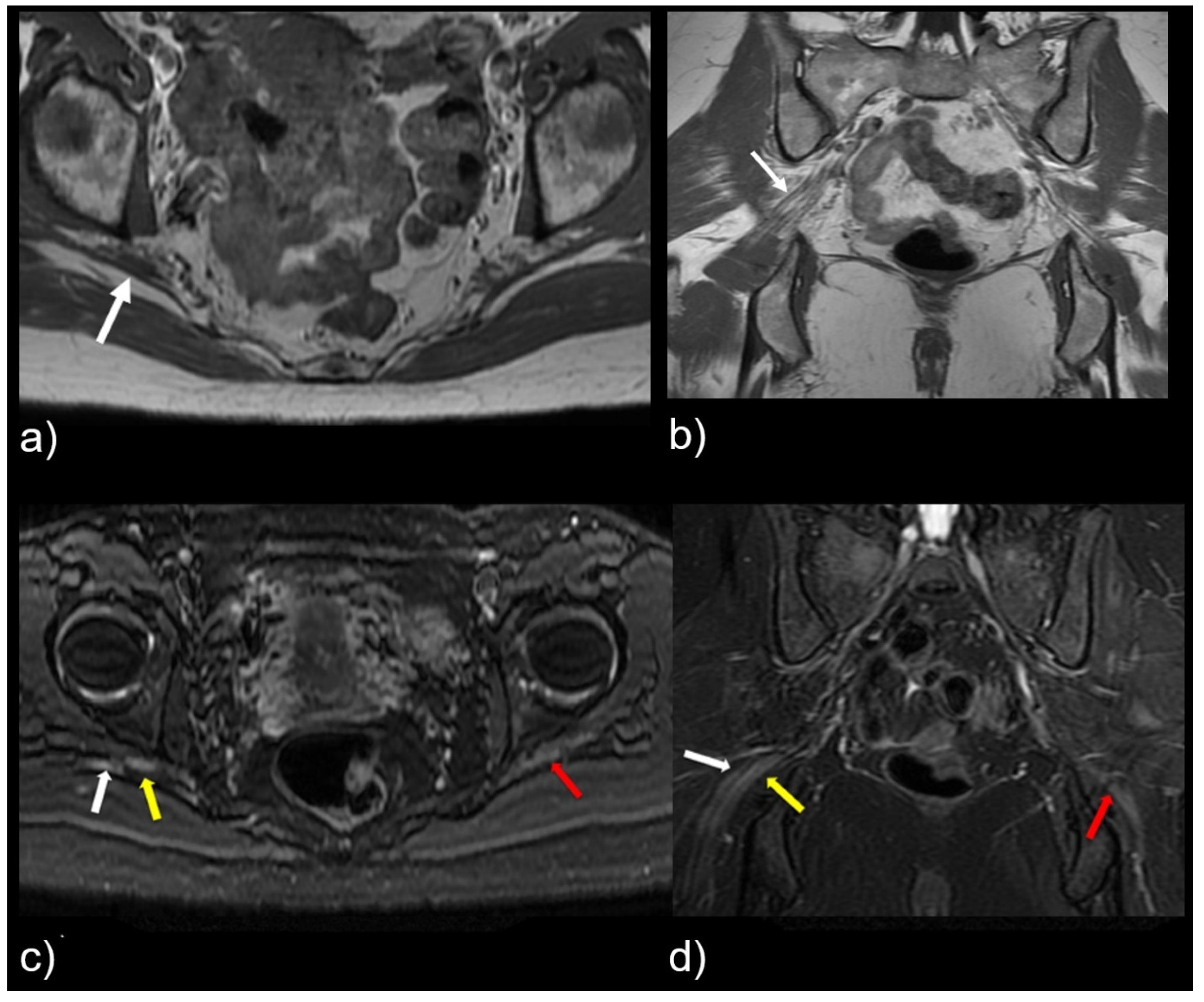
2. Materials and Methods
2.1. Patient Cohort
2.2. Image Acquisition
2.3. Image Evaluation
2.4. Statistical Analysis
3. Results
3.1. Patient Demographics
3.2. MR Neurography of the Sciatic Nerves
3.3. Sciatic Nerve Correlation with Findings at MR Neurography
3.4. Sciatic Nerve Correlation with Clinical Presentation and Outcomes
3.5. Statistical Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Konstantinou, K.; Dunn, K.M. Sciatica: Review of epidemiological studies and prevalence estimates. Spine 2008, 33, 2464–2472. [Google Scholar] [CrossRef]
- Ropper, A.H.; Zafonte, R.D. Sciatica. N. Engl. J. Med. 2015, 372, 1240–1248. [Google Scholar] [CrossRef] [PubMed]
- Hallin, R.P. Sciatic pain and the piriformis muscle. Postgrad. Med. 1983, 74, 69–72. [Google Scholar] [CrossRef]
- Kosukegawa, I.; Yoshimoto, M.; Isogai, S.; Nonaka, S.; Yamashita, T. Piriformis syndrome resulting from a rare anatomic variation. Spine 2006, 31, E664–E666. [Google Scholar] [CrossRef]
- Beaton, L.E.; Anson, B.J. The relation of the sciatic nerve and of its subdivisions to the piriformis muscle. Anat. Rec. 1937, 70, 1–5. [Google Scholar] [CrossRef]
- Natsis, K.; Totlis, T.; Konstantinidis, G.A.; Paraskevas, G.; Piagkou, M.; Koebke, J. Anatomical variations between the sciatic nerve and the piriformis muscle: A contribution to surgical anatomy in piriformis syndrome. Surg. Radiol. Anat. 2014, 36, 273–280. [Google Scholar] [CrossRef] [PubMed]
- Polesello, G.C.; Queiroz, M.C.; Linhares, J.P.T.; Amaral, D.T.; Ono, N.K. Anatomical variation of piriformis muscle as a cause of deep gluteal pain: Diagnosis using MR neurography and treatment. Rev. Bras. Ortop. 2013, 48, 114–117. [Google Scholar] [CrossRef][Green Version]
- Maravilla, K.R.; Bowen, B.C. Imaging of the peripheral nervous system: Evaluation of peripheral neuropathy and plexopathy. AJNR Am. J. Neuroradiol. 1998, 19, 1011–1023. [Google Scholar]
- Moore, K.R.; Tsuruda, J.S.; Dailey, A.T. The Value of MR Neurography for Evaluating Extraspinal Neuropathic Leg Pain: A Pictorial Essay. AJNR Am. J. Neuroradiol. 2001, 22, 786–794. [Google Scholar]
- Şirvanci, M.; Kara, B.; Duran, C.; Ozturk, E.; Karatoprak, O.; Onat, L.; Ulusoy, O.L.; Mutlu, A. Value of perineural edema/inflammation detected by fat saturation sequences in lumbar magnetic resonance imaging of patients with unilateral sciatica. Acta Radiol. 2009, 50, 205–211. [Google Scholar] [CrossRef] [PubMed]
- Lewis, A.M.; Layzer, R.; Engstrom, J.W.; Barbaro, N.M.; Chin, C.T. Magnetic resonance neurography in extraspinal sciatica. Arch. Neurol. 2006, 63, 1469–1472. [Google Scholar] [CrossRef] [PubMed]
- Lee, E.Y.; Margherita, A.J.; Gierada, D.S.; Narra, V.R. MRI of piriformis syndrome. Am. J. Roentgenol. 2004, 183, 63–64. [Google Scholar] [CrossRef]
- Filler, A.G.; Haynes, J.; Jordan, S.E.; Prager, J.; Villablanca, J.P.; Farahani, K.; Mcbride, D.Q.; Tsuruda, J.S.; Morisoli, B.; Batzdorf, U.; et al. Sciatica of nondisc origin and piriformis syndrome: Diagnosis by magnetic resonance neurography and interventional magnetic resonance imaging with outcome study of resulting treatment. J. Neurosurg. Spine 2005, 2, 99–115. [Google Scholar] [CrossRef]
- Ro, T.H.; Edmonds, L. Diagnosis and Management of Piriformis Syndrome: A Rare Anatomic Variant Analyzed by Magnetic Resonance Imaging. J. Clin. Imaging Sci. 2018, 8, 6. [Google Scholar] [CrossRef] [PubMed]
- Eastlack, J.; Tenorio, L.; Wadhwa, V.; Scott, K.; Starr, A.; Chhabra, A. Sciatic neuromuscular variants on MR neurography: Frequency study and interobserver performance. Br. J. Radiol. 2017, 90, 20170116. [Google Scholar] [CrossRef]
- Chhabra, A.; Chalian, M.; Soldatos, T.; Andreisek, G.; Faridian-Aragh, N.; Williams, E.; Belzberg, A.J.; Carrino, J.A. 3-T High-Resolution MR Neurography of Sciatic Neuropathy. Am. J. Roentgenol. 2012, 198, W357–W364. [Google Scholar] [CrossRef] [PubMed]
- Varenika, V.; Lutz, A.M.; Beaulieu, C.F.; Bucknor, M.D. Detection and prevalence of variant sciatic nerve anatomy in relation to the piriformis muscle on MRI. Skelet. Radiol. 2017, 46, 751–757. [Google Scholar] [CrossRef]
- Virtanen, P.; Gommers, R.; Oliphant, T.E.; Haberland, M.; Reddy, T.; Cournapeau, D.; Burovski, E.; Peterson, P.; Weckesser, W.; Bright, J.; et al. SciPy 1.0: Fundamental Algorithms for Scientific Computing in Python. Nat. Methods 2020, 17, 261–272. [Google Scholar] [CrossRef]
- Heliövaara, M.; Mäkelä, M.; Knekt, P.; Impivaara, O.; Aromaa, A. Determinants of sciatica and low-back pain. Spine 1991, 16, 608–614. [Google Scholar] [CrossRef]
- Nakamura, H.; Seki, M.; Konishi, S.; Yamano, Y.; Takaoka, K. Piriformis syndrome diagnosed by cauda equina action potentials: Report of two cases. Spine 2003, 28, E37–E40. [Google Scholar] [CrossRef]
- Fishman, L.M.; Schaefer, M.P. The piriformis syndrome is underdiagnosed. Muscle Nerve 2003, 28, 646–649. [Google Scholar] [CrossRef] [PubMed]
- Foti, G.; Lombardo, F.; Fighera, A.; Giaretta, A.; Catania, M.; Serra, G.; Carbognin, G. Role of diffusion tensor imaging of sciatic nerve in symptomatic patients with inconclusive lumbar MRI. Eur. J. Radiol. 2020, 131, 109249. [Google Scholar] [CrossRef]
- Chappell, K.E.; Robson, M.D.; Stonebridge-Foster, A.; Glover, A.; Allsop, J.M.; Williams, A.D.; Herlihy, A.H.; Moss, J.; Gishen, P.; Bydder, G.M. Magic angle effects in MR neurography. AJNR Am. J. Neuroradiol. 2004, 25, 431–440. [Google Scholar] [PubMed]
- Agnollitto, P.M.; Chu, M.W.K.; Simão, M.N.; Nogueira-Barbosa, M.H. Sciatic neuropathy: Findings on magnetic resonance neurography. Radiol. Bras. 2017, 50, 190–196. [Google Scholar] [CrossRef] [PubMed]
| MR Sequence | Orientation | Fat Saturation | FOV (cm) | Slice Thickness (mm) | TR (ms) | TE (ms) | Matrix (Pixels) | NEX |
|---|---|---|---|---|---|---|---|---|
| T1-weighted | Axial | No | 24 | 3 | 600 | min | 384 × 192 | 3.5 × 4 |
| T1-weighted | Coronal | No | 24 | 3 | 700 | min | 384 × 224 | 5 × 4 |
| T2-weighted IDEAL | Axial | Yes | 24 | 3 | 3700 | 70 | 256 × 160 | 6.5 × 2 |
| T2-weighted IDEAL | Coronal | Yes | 24 | 3 | 3000 | 70 | 288 × 192 | 5 × 2 |
| Attribute | Age | Gender | Symptoms | Surgery | Sciatic Nerve Variant | Increased Nerve T2 Signal | Split Sciatic at Ischial Tuberosity | Asymmetric Piriformis Size | Increased Nerve Caliber |
|---|---|---|---|---|---|---|---|---|---|
| p-value | 0.79 | 0.48 | 0.62 | 0.63 | 0.72 | 0.1 | 0.94 | 0.07 | 0.93 |
| Variant (n = 64) | Normal (n = 190) | p-Value | |
|---|---|---|---|
| Symptomatic | 41/64 (64%) | 87/190 (46%) | 0.01 |
| Increased nerve T2 signal | 40/64 (63%) | 82/190 (43%) | 0.01 |
| Split sciatic at ischial tuberosity | 56/64 (88%) | 20/190 (11%) | <0.0001 |
| Asymmetric piriformis size | 11/64 (17%) | 25/190 (13%) | 0.41 |
| Increased nerve caliber | 10/64 (16%) | 33/190 (17%) | 0.85 |
| Odds Ratio | 95% Confidence Interval | p-Value | |
|---|---|---|---|
| Symptomatic | 1.74 | [0.29, 10.10] | 0.54 |
| Increased nerve T2 signal | 2.75 | [1.45, 5.24] | 0.02 |
| Split sciatic at ischial tuberosity | 131.41 | [40.01, 431.56] | 0.001 |
| Asymmetric piriformis size | 1.54 | [0.70, 3.39] | 0.38 |
| Increased nerve caliber | 0.70 | [0.37, 1.30] | 0.72 |
| Variant (n = 64) | Normal (n = 190) | p-Value | |
|---|---|---|---|
| Symptomatic | 64% | 46% | 0.01 |
| Median symptom duration | 1.50 years | 1.75 years | 0.23 |
| Abnormal EMG | 23% | 33% | 0.70 |
| Need for surgery (neurolysis) | 10% | 8% | 0.75 |
| Eventual clinical improvement | 63% | 56% | 0.82 |
| Odds Ratio | 95% Confidence Interval | p-Value | |
|---|---|---|---|
| Anatomical variant | 1.74 | [0.29, 10.10] | 0.54 |
| T2 hyperintense signal | 1321.53 | [150.96, 11,569.27] | <0.0001 |
| Nerve caliber size | 0.57 | [0.03, 9.66] | 0.69 |
| Asymmetric piriformis | 57.64 | [4.35, 763.03] | 0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bharadwaj, U.U.; Varenika, V.; Carson, W.; Villanueva-Meyer, J.; Ammanuel, S.; Bucknor, M.; Robbins, N.M.; Douglas, V.; Chin, C.T. Variant Sciatic Nerve Anatomy in Relation to the Piriformis Muscle on Magnetic Resonance Neurography: A Potential Etiology for Extraspinal Sciatica. Tomography 2023, 9, 475-484. https://doi.org/10.3390/tomography9020039
Bharadwaj UU, Varenika V, Carson W, Villanueva-Meyer J, Ammanuel S, Bucknor M, Robbins NM, Douglas V, Chin CT. Variant Sciatic Nerve Anatomy in Relation to the Piriformis Muscle on Magnetic Resonance Neurography: A Potential Etiology for Extraspinal Sciatica. Tomography. 2023; 9(2):475-484. https://doi.org/10.3390/tomography9020039
Chicago/Turabian StyleBharadwaj, Upasana Upadhyay, Vanja Varenika, William Carson, Javier Villanueva-Meyer, Simon Ammanuel, Matthew Bucknor, Nathaniel M. Robbins, Vanja Douglas, and Cynthia T. Chin. 2023. "Variant Sciatic Nerve Anatomy in Relation to the Piriformis Muscle on Magnetic Resonance Neurography: A Potential Etiology for Extraspinal Sciatica" Tomography 9, no. 2: 475-484. https://doi.org/10.3390/tomography9020039
APA StyleBharadwaj, U. U., Varenika, V., Carson, W., Villanueva-Meyer, J., Ammanuel, S., Bucknor, M., Robbins, N. M., Douglas, V., & Chin, C. T. (2023). Variant Sciatic Nerve Anatomy in Relation to the Piriformis Muscle on Magnetic Resonance Neurography: A Potential Etiology for Extraspinal Sciatica. Tomography, 9(2), 475-484. https://doi.org/10.3390/tomography9020039






