Biomimetic Whitening Effect of Polyphosphate-Bleaching Agents on Dental Enamel
Abstract
1. Introduction
2. Materials and Methods
2.1. Specimen Preparation
2.2. Color Measurement
2.3. Color Change
2.4. Data Analysis
3. Results
3.1. L*, a*, b* Parameters
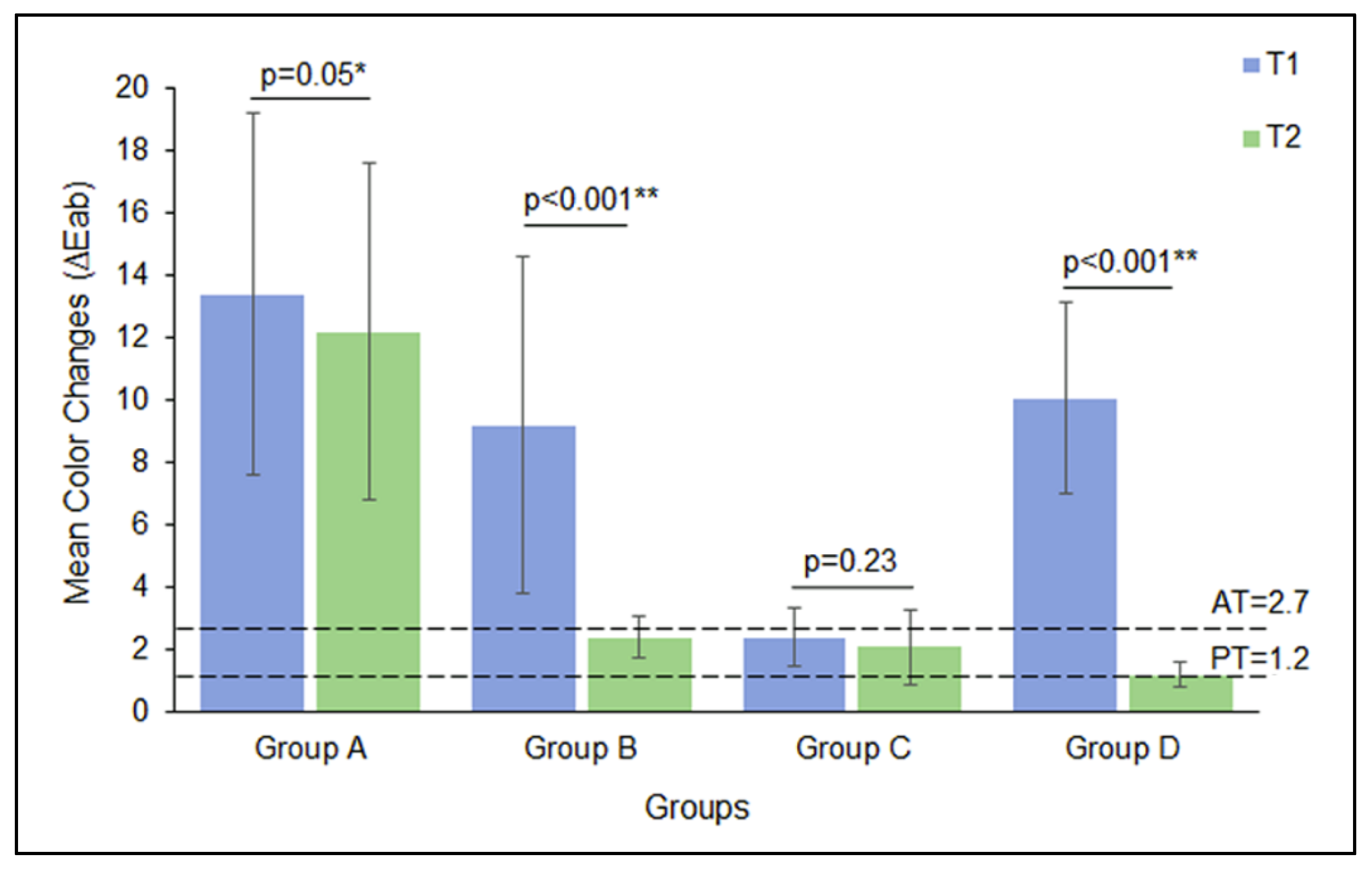
3.2. Color Difference
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Afrashtehfar, K.I.; Assery, M.K. Five considerations in cosmetic and esthetic dentistry. J. N. J. Dent. Assoc. 2014, 85, 14–15. [Google Scholar] [PubMed]
- Greenwall-Cohen, J.; Francois, P.; Silikas, N.; Greenwall, L.; Le Goff, S.; Attal, J.P. The safety and efficacy of ‘over the counter’ bleaching products in the UK. Br. Dent. J. 2019, 226, 271–276. [Google Scholar] [CrossRef] [PubMed]
- De Geus, J.L.; Wambier, L.M.; Kossatz, S.; Loguercio, A.D.; Reis, A. At-home vs. In-office Bleaching: A Systematic Review and Meta-analysis. Oper. Dent. 2016, 41, 341–356. [Google Scholar] [CrossRef] [PubMed]
- Dahl, J.E.; Pallesen, U. Tooth bleaching—A critical review of the biological aspects. Crit. Rev. Oral Biol. Med. 2003, 14, 292–304. [Google Scholar] [CrossRef]
- Alikhasi, M.; Yousefi, P.; Afrashtehfar, K.I. Smile design: Mechanical considerations. Dent. Clin. N. Am. 2022, 66, 477–487. [Google Scholar] [CrossRef]
- Li, Y. Safety controversies in tooth bleaching. Dent. Clin. N. Am. 2011, 55, 255–263. [Google Scholar] [CrossRef]
- Goldberg, M.; Grootveld, M.; Lynch, E. Undesirable and adverse effects of tooth-whitening products: A review. Clin. Oral Investig. 2010, 14, 1–10. [Google Scholar] [CrossRef]
- Torres, C.R.; Crastechini, E.; Feitosa, F.A.; Pucci, C.R.; Borges, A.B. Influence of pH on the effectiveness of hydrogen peroxide whitening. Oper. Dent. 2014, 39, E261–E268. [Google Scholar] [CrossRef]
- Karadas, M.; Duymus, Z.Y. In Vitro Evaluation of the Efficacy of Different Over-the-Counter Products on Tooth Whitening. Braz. Dent. J. 2015, 26, 373–377. [Google Scholar] [CrossRef]
- Naidu, A.S.; Bennani, V.; Brunton, J.; Brunton, P. Over-the-Counter Tooth Whitening Agents: A Review of Literature. Braz. Dent. J. 2020, 31, 221–235. [Google Scholar] [CrossRef]
- Jurema, A.L.; Claudino, E.S.; Torres, C.R.; Bresciani, E.; Caneppele, T.M. Effect of Over-the-counter Whitening Products associated or Not with 10% Carbamide Peroxide on Color Change and Microhardness: In vitro Study. J. Contemp. Dent. Pract 2018, 19, 359–366. [Google Scholar] [PubMed]
- Jaime, I.M.; França, F.M.; Basting, R.T.; Turssi, C.P.; Amaral, F.L. Efficacy of hydrogen-peroxide-based mouthwash in altering enamel color. Am. J. Dent. 2014, 27, 47–50. [Google Scholar] [PubMed]
- Dantas, A.A.; Bortolatto, J.F.; Roncolato, Á.; Merchan, H.; Floros, M.C.; Kuga, M.C.; Junior, O.B.O. Can a bleaching toothpaste containing Blue Covarine demonstrate the same bleaching as conventional techniques? An in vitro, randomized and blinded study. J. Appl. Oral Sci. 2015, 23, 609–613. [Google Scholar] [CrossRef] [PubMed]
- Auschill, T.M.; Hellwig, E.; Schmidale, S.; Sculean, A.; Arweiler, N.B. Efficacy, side-effects and patients’ acceptance of different bleaching techniques (OTC, in-office, at-home). Oper. Dent. 2005, 30, 156–163. [Google Scholar] [CrossRef]
- Kim, Y.M.; Ha, A.N.; Kim, J.W.; Kim, S.J. Double-blind Randomized Study to Evaluate the Safety and Efficacy of Over-the-counter Tooth-whitening Agents Containing 2.9% Hydrogen Peroxide. Oper. Dent. 2018, 43, 272–281. [Google Scholar] [CrossRef]
- ADA. ADA Current Policies, Adopted 1954–2020. 2021. Available online: https://www.ada.org/-/media/project/ada-organization/ada/ada-org/files/about/current-policies-and-historical-publications/current_policies.pdf (accessed on 20 September 2022).
- Joiner, A. The bleaching of teeth: A review of the literature. J. Dent. 2006, 34, 412–419. [Google Scholar] [CrossRef]
- Kwon, S.R.; Meharry, M.; Oyoyo, U.; Li, Y. Efficacy of do-it-yourself whitening as compared to conventional tooth whitening modalities: An in vitro study. Oper. Dent. 2015, 40, E21–E27. [Google Scholar] [CrossRef]
- Rezende, M.; Coppla, F.M.; Chemin, K.; Chibinski, A.C.; Loguercio, A.D.; Reis, A. Tooth Sensitivity After Dental Bleaching With a Desensitizer-containing and a Desensitizer-free Bleaching Gel: A Systematic Review and Meta-analysis. Oper. Dent. 2019, 44, E58–E74. [Google Scholar] [CrossRef]
- Lee, J.-H.; Kim, S.-H.; Han, J.-S.; Yeo, I.-S.L.; Yoon, H.-I. Optical and Surface Properties of Monolithic Zirconia after Simulated Toothbrushing. Materials 2019, 12, 1158. [Google Scholar] [CrossRef]
- Bizhang, M.; Schmidt, I.; Chun, Y.P.; Arnold, W.H.; Zimmer, S. Toothbrush abrasivity in a long-term simulation on human dentin depends on brushing mode and bristle arrangement. PLoS ONE 2017, 12, e0172060. [Google Scholar] [CrossRef]
- Alfouzan, A.F.; Alotiabi, H.M.; Labban, N.; Al-Otaibi, H.N.; Al Taweel, S.M.; AlShehri, H.A. Color stability of 3D-printed denture resins: Effect of aging, mechanical brushing and immersion in staining medium. J. Adv. Prosthodont. 2021, 13, 160–171. [Google Scholar] [CrossRef] [PubMed]
- ISO/TR-28642:2016(E); Technical Report: Dentistry-Guidance on Colour Measurments. International Organization for Standardization: Geneva, Switzerland, 2016.
- CIE. Colorimtry-Technical Report, 3rd ed.; Report No.15.; Central Burea of CIE: Vienna, Austria, 2004. [Google Scholar]
- Paravina, R.D.; Ghinea, R.; Herrera, L.J.; Bona, A.D.; Igiel, C.; Linninger, M.; Sakai, M.; Takahashi, H.; Tashkandi, E.; Perez, M.D.M. Color difference thresholds in dentistry. J. Esthet. Restor. Dent. 2015, 27 (Suppl. 1), S1–S9. [Google Scholar] [CrossRef]
- Paravina, R.D.; Pérez, M.M.; Ghinea, R. Acceptability and perceptibility thresholds in dentistry: A comprehensive review of clinical and research applications. J. Esthet. Restor. Dent. 2019, 31, 103–112. [Google Scholar] [CrossRef] [PubMed]
- Matis, B.A.; Cochran, M.A.; Eckert, G. Review of the effectiveness of various tooth whitening systems. Oper. Dent. 2009, 34, 230–235. [Google Scholar] [CrossRef] [PubMed]
- Bizhang, M.; Chun, Y.H.; Damerau, K.; Singh, P.; Raab, W.H.; Zimmer, S. Comparative clinical study of the effectiveness of three different bleaching methods. Oper. Dent. 2008, 34, 635–641. [Google Scholar] [CrossRef] [PubMed]
- Sulieman, M. An overview of bleaching techniques: I. History, chemistry, safety and legal aspects. Dent. Update 2004, 31, 608–616. [Google Scholar] [CrossRef]
- Worschech, C.C.; Rodrigues, J.A.; Martins, L.R.; Ambrosano, G.M. In vitro evaluation of human dental enamel surface roughness bleached with 35% carbamide peroxide and submitted to abrasive dentifrice brushing. Pesqui. Odontol. Bras. 2003, 17, 342–348. [Google Scholar] [CrossRef]
- Türkun, M.; Sevgican, F.; Pehlivan, Y.; Aktener, B.O. Effects of 10% carbamide peroxide on the enamel surface morphology: A scanning electron microscopy study. J. Esthet. Restor. Dent. 2002, 14, 238–244. [Google Scholar] [CrossRef]
- Gökay, O.; Tunçbilek, M.; Ertan, R. Penetration of the pulp chamber by carbamide peroxide bleaching agents on teeth restored with a composite resin. J. Oral Rehabil. 2000, 27, 428–431. [Google Scholar] [CrossRef]
- Flaitz, C.M.; Hicks, M.J. Effects of carbamide peroxide whitening agents on enamel surfaces and caries-like lesion formation: An SEM and polarized light microscopic in vitro study. ASDC J. Dent. Child 1996, 63, 249–256. [Google Scholar]
- Nathoo, S.A.; Chmielewski, M.B.; Kirkup, R.E. Effects of Colgate Platinum Professional Toothwhitening System on microhardness of enamel, dentin, and composite resins. Compend. Suppl. 1994, 17, S627–S630. [Google Scholar]
- Oltu, U.; Gürgan, S. Effects of three concentrations of carbamide peroxide on the structure of enamel. J. Oral Rehabil. 2000, 27, 332–340. [Google Scholar] [CrossRef] [PubMed]
- Leonard, R.H., Jr.; Haywood, V.B.; Phillips, C. Risk factors for developing tooth sensitivity and gingival irritation associated with nightguard vital bleaching. Quintessence Int. 1997, 28, 527–534. [Google Scholar] [PubMed]
- Calatayud, J.O.; de la Varga, P.M.; Calatayud, C.O.; Box, M.J.C. Comparative clinical study of two tooth bleaching protocols with 6% hydrogen peroxide. Int. J. Dent. 2009, 2009, 928306. [Google Scholar] [CrossRef]
- McGuckin, R.S.; Babin, J.F.; Meyer, B.J. Alterations in human enamel surface morphology following vital bleaching. J. Prosthet. Dent. 1992, 68, 754–760. [Google Scholar] [CrossRef]
- Haywood, V.B. Current status of nightguard vital bleaching. Compend. Contin. Educ. Dent. Suppl. 2000, 28, S10–S17, quiz S48. [Google Scholar]
- Kugel, G.; Kastali, S. Tooth-whitening efficacy and safety: A randomized and controlled clinical trial. Compend. Contin. Educ. Dent. Suppl. 2000, 29, S16–S21, quiz S42. [Google Scholar]
- Hegedüs, C.; Bistey, T.; Flóra-Nagy, E.; Keszthelyi, G.; Jenei, A. An atomic force microscopy study on the effect of bleaching agents on enamel surface. J. Dent. 1999, 27, 509–515. [Google Scholar] [CrossRef]
- Afrashtehfar, K.I. Increased predictability in tooth shade-matching. Oral Health 2013, 15, 44–50. [Google Scholar]
- Eimar, H.; Siciliano, R.; Abdallah, M.N.; Nader, S.A.; Amin, W.M.; Martinez, P.P.; Celemin, A.; Cerruti, M.; Tamimi, F. Hydrogen peroxide whitens teeth by oxidizing the organic structure. J. Dent. 2012, 40 (Suppl. 2), e25–e33. [Google Scholar] [CrossRef]
- Abdallah, M.N.; Eimar, H.; Bassett, D.C.; Schnabel, M.; Ciobanu, O.; Nelea, V.; McKee, M.D.; Cerruti, M.; Tamimi, F. Diagenesis-inspired reaction of magnesium ions with surface enamel mineral modifies properties of human teeth. Acta Biomater. 2016, 37, 174–183. [Google Scholar] [CrossRef] [PubMed]
- Matsumoto, H.; Yamamoto, T.; Hayakawa, T. Color changes of dental zirconia immersed in food and beverage containing water-soluble/lipid-soluble pigments. Dent. Mater. J. 2022. [Google Scholar] [CrossRef] [PubMed]
- Lee, E.H.; Ahn, J.S.; Lim, Y.J.; Kwon, H.B.; Kim, M.J. Effect of layer thickness and printing orientation on the color stability and stainability of a 3D-printed resin material. J. Prosthet. Dent. 2022, 127, 784.e1–784.e7. [Google Scholar] [CrossRef] [PubMed]
| Group Code/ Tooth Whitening Agents/Manufacturers | Composition | Delivery Method/ Duration of Use |
|---|---|---|
| Group A Opalescence™ PF/ Ultradent, South Jordan, UT, USA | 10% Carbamide Peroxide, 0.5% Potassium Nitrate, and 0.11% Fluoride Ions | Custom-made trays/ Eight hours per day for 10 days |
| Group B iWhite Dark Stains Whitening Kit/ Sylphar, Deurle, Belgium | Hydrated Silica, Sodium Hexametaphosphate, Mannitol, Chondrus Crispus Powder, Charcoal Powder. | Ready to use trays/ 20 min per day for 5 days |
| Group C iWhite Dark Stains Toothpaste/ Sylphar, Deurle, Belgium | Hydrated Silica, Sodium Hexametaphosphate, Mannitol, Chondrus Crispus Powder, Charcoal Powder, Sodium Fluoride, Sodium Saccharin. | Toothbrush/ Two brushing cycles per day for 60 days |
| Group D 24 K White Charcoal Teeth Whitening Pen/ Active Wow, Tallahassee, FL, USA | Sodium Bicarbonate, Carbomer, Polysorbate 20, Sodium Hydroxide, Potassium Sorbate, Organic Coconut Charcoal. | Whitening Pen/One application per day for two days |
| Color Parameters | Mean ± SD | |||
|---|---|---|---|---|
| Group A | Group B | Group C | Group D | |
| T0 | ||||
| ΔL* | 66 ± 3.7 | 71.5 ± 5.52 | 68.9 ± 4.36 | 70.2 ± 5.7 |
| Δa* | −2.8 ± 1.41 | −3.2 ± 0.80 | −3.5 ± 0.67 | −3.6 ± 0.85 |
| Δb* | 4.4 ± 4.21 | 4.1 ± 4.48 | 3.9 ± 4.1 | 4.2 ± 4.79 |
| T1 | ||||
| ΔL* | 78.6 ± 7.17 | 80 ± 5 | 70 ± 4.26 | 80.6 ± 5 |
| Δa* | −1.6 ± 0.93 | −3.5 ± 0.82 | −3.7 ± 0.66 | −4 ± 0.62 |
| Δb* | 4.3 ± 2.93 | 4.2 ± 4.69 | 3.3 ± 4.59 | 3.6 ± 4.93 |
| T2 | ||||
| ΔL* | 77.4 ± 6.6 | 73.7 ± 5.31 | 69.3 ± 3.85 | 70.9 ± 5.43 |
| Δa* | −1.4 ± 0.84 | −3.5 ± 0.73 | −3.4 ± 0.74 | −3–3 ± 0.87 |
| Δb* | 5.2 ± 3.12 | 4.8 ± 4.65 | 4.4 ± 4.78 | 5.7 ± 4.92 |
| Color Parameters | T1-T0 | p Value | T2-T0 | p Value |
|---|---|---|---|---|
| Group A | ||||
| ΔL* | 12.6 ± 5.9 | 0.0001 * | 11.4 ± 5.51 | 0.0001 * |
| Δa* | 3.7 ± 1.16 | 0.0001 * | −3.5 ± 1.20 | 0.001 * |
| Δb* | −0.1 ± 1.89 | 0.61 | 0.8 ± 1.9 | 0.04 * |
| Group B | ||||
| ΔL* | 8.6 ± 5.81 | 0.0001 * | 2.2 ± 0.70 | 0.004 * |
| Δa* | −0.4 ± 0.52 | 0.003 * | −0.3 ± 0.19 | 0.003 * |
| Δb* | 0.0 ± 2.80 | 1.0 | 0.7 ± 0.56 | 0.013 * |
| Group C | ||||
| ΔL* | 1.2 ± 1.08 | 0.05 * | 0.4 ± 1.38 | 1.0 |
| Δa* | −0.3 ± 0.2 | 0.05 * | 0.1 ± 0.39 | 0.46 |
| Δb* | −0.6 ± 1.9 | 0.06 | 0.5 ± 1.90 | 0.34 |
| Group D | ||||
| ΔL* | 10.3 ± 3.06 | 0.0001 * | 0.7 ± 0.79 | 0.08 |
| Δa* | −0.4 ± 0.38 | 0.08 | 0.3 ± 0.23 | 0.05 * |
| Δb* | −0.6 ± 1.26 | 0.058 | 1.5 ± 0.45 | 0.04 * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alshehri, A.; Almutairi, B.; Jurado, C.A.; Afrashtehfar, K.I.; Albarrak, S.; Alharbi, A.; Alenazi, A.; Nurrohman, H.; Alshabib, A. Biomimetic Whitening Effect of Polyphosphate-Bleaching Agents on Dental Enamel. Biomimetics 2022, 7, 183. https://doi.org/10.3390/biomimetics7040183
Alshehri A, Almutairi B, Jurado CA, Afrashtehfar KI, Albarrak S, Alharbi A, Alenazi A, Nurrohman H, Alshabib A. Biomimetic Whitening Effect of Polyphosphate-Bleaching Agents on Dental Enamel. Biomimetics. 2022; 7(4):183. https://doi.org/10.3390/biomimetics7040183
Chicago/Turabian StyleAlshehri, Abdullah, Basil Almutairi, Carlos A. Jurado, Kelvin I. Afrashtehfar, Shug Albarrak, Asma Alharbi, Alanoud Alenazi, Hamid Nurrohman, and Abdulrahman Alshabib. 2022. "Biomimetic Whitening Effect of Polyphosphate-Bleaching Agents on Dental Enamel" Biomimetics 7, no. 4: 183. https://doi.org/10.3390/biomimetics7040183
APA StyleAlshehri, A., Almutairi, B., Jurado, C. A., Afrashtehfar, K. I., Albarrak, S., Alharbi, A., Alenazi, A., Nurrohman, H., & Alshabib, A. (2022). Biomimetic Whitening Effect of Polyphosphate-Bleaching Agents on Dental Enamel. Biomimetics, 7(4), 183. https://doi.org/10.3390/biomimetics7040183









