Mycetoma: Development of Diagnosis and Treatment
Abstract
1. Introduction
2. Epidemiology
3. Etiology
4. Pathogenesis
5. Clinical Presentation
6. Diagnosis
7. Direct Microscopic Examination
8. Histopathological Examination
9. Grain Culture
10. Molecular Profiling
11. Serodiagnostic Test
12. Radiography
13. Differential Diagnosis
14. Treatment
15. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ananthanarayan, B.A.; Jayaram, C.K.; Paniker, M.D. Textbook of Microbiology, 7th ed.; Orient Longman Private Ltd.: Hyderabad, India, 2006. [Google Scholar]
- Patton, L. Veda and Upanishad; Thursby, S.M.A.G., Ed.; Routledge: London, UK, 2004; p. 38. [Google Scholar]
- van de Sande, W.W. Global burden of human mycetoma: A systematic review and meta-analysis. PLoS Negl. Trop. Dis. 2013, 7, e2550. [Google Scholar] [CrossRef] [PubMed]
- Nenoff, P.; van de Sande, W.W.; Fahal, A.H.; Reinel, D.; Schöfer, H. Eumycetoma and actinomycetoma—An update on causative agents, epidemiology, pathogenesis, diagnostics and therapy. J. Eur. Acad. Dermatol. Venereol. 2015, 29, 1873–1883. [Google Scholar] [CrossRef] [PubMed]
- Carter, H. On a New and Striking form of Fungus Disease Principally Affecting the Foot and Prevailing Endemically in Many Parts of India. Trans. Med. Phys. Soc. Bombay 1860, 6, 104–142. [Google Scholar]
- Pinoy, E. Actinomycoses and mycetomas. Bull. Inst. Past 1913, 11, 929–938. [Google Scholar]
- Fahal, A.H.; Suliman, S.H.; Hay, R. Mycetoma: The Spectrum of Clinical Presentation. Trop. Med. Infect. Dis. 2018, 3, 97. [Google Scholar] [CrossRef]
- Agarwal, P.; Jagati, A.; Rathod, S.P.; Kalra, K.; Patel, S.; Chaudhari, M. Clinical Features of Mycetoma and the Appropriate Treatment Options. Res. Rep. Trop. Med. 2021, 12, 173–179. [Google Scholar] [CrossRef]
- Abbas, M.; Scolding, P.S.; Yosif, A.A.; El Rahman, R.F.; El-Amin, M.O.; Elbashir, M.K.; Groce, N.; Fahal, A.H. The disabling consequences of Mycetoma. PLoS Negl. Trop. Dis. 2018, 12, e0007019. [Google Scholar] [CrossRef]
- Fahal, A.H. Mycetoma: A global medical and socio-economic dilemma. PLoS Negl. Trop. Dis. 2017, 11, e0005509. [Google Scholar] [CrossRef]
- Emery, D.; Denning, D.W. The global distribution of actinomycetoma and eumycetoma. PLoS Negl. Trop. Dis. 2020, 14, e0008397. [Google Scholar] [CrossRef]
- Tritto, M.; Procop, G.W.; Billings, S.T.; Mirkin, G.; Hao, X. Eumycetoma, A Neglected Tropical Disease in the United States. J. Am. Podiatr. Med. Assoc. 2021, 111. [Google Scholar] [CrossRef]
- Bonifaz, A.; Tirado-Sánchez, A.; Calderón, L.; Saúl, A.; Araiza, J.; Hernández, M.; González, G.M.; Ponce, R.M. Mycetoma: Experience of 482 cases in a single center in Mexico. PLoS Negl. Trop. Dis. 2014, 8, e3102. [Google Scholar] [CrossRef]
- van de Sande, W.; Fahal, A.; Ahmed, S.A.; Serrano, J.A.; Bonifaz, A.; Zijlstra, E. Closing the mycetoma knowledge gap. Med. Mycol. 2018, 56 (Suppl. 1), 153–164. [Google Scholar] [CrossRef] [PubMed]
- Zijlstra, E.E.; van de Sande, W.W.J.; Welsh, O.; Mahgoub, E.S.; Goodfellow, M.; Fahal, A.H. Mycetoma: A unique neglected tropical disease. Lancet. Infect. Dis. 2016, 16, 100–112. [Google Scholar] [CrossRef]
- Zijlstra, E.E.; van de Sande, W.W.; Fahal, A.H. Mycetoma: A Long Journey from Neglect. PLoS Negl. Trop. Dis. 2016, 10, e0004244. [Google Scholar] [CrossRef] [PubMed]
- Bitan, O.; Wiener-Well, Y.; Segal, R.; Schwartz, E. Mycetoma (Madura Foot) in Israel: Recent Cases and a Systematic Review of the Literature. Am. J. Trop. Med. Hyg. 2017, 96, 1355–1361. [Google Scholar] [CrossRef][Green Version]
- Buonfrate, D.; Gobbi, F.; Angheben, A.; Marocco, S.; Farina, C.; Van Den Ende, J.; Bisoffi, Z. Autochthonous cases of mycetoma in Europe: Report of two cases and review of literature. PLoS ONE 2014, 9, e100590. [Google Scholar] [CrossRef] [PubMed]
- Green, W.O., Jr.; Adams, T.E. Mycetoma in the United States; A Review and Report of Seven Additional Cases. Am. J. Clin. Pathol. 1964, 42, 75–91. [Google Scholar] [CrossRef]
- Warintarawej, A.; Winter, W.G., Jr.; Goodman, N.L. Maduromycosis (Madura foot) in Kentucky. South. Med. J. 1975, 68, 1570–1575. [Google Scholar] [CrossRef]
- Das, L.; Dahiya, D.; Gupta, K.; Prakash, M.; Malhotra, B.; Rastogi, A.; Choudhary, H.; Rudramurthy, S.M.; Dutta, P. Eumycetoma of the Foot due to Fusarium solani in a Person with Diabetes Mellitus: Report of a Case and Review of Literature. Mycopathologia 2021, 186, 277–288. [Google Scholar] [CrossRef]
- Abushouk, A.; Nasr, A.; Masuadi, E.; Allam, G.; Siddig, E.E.; Fahal, A.H. The Role of Interleukin-1 cytokine family (IL-1β, IL-37) and interleukin-12 cytokine family (IL-12, IL-35) in eumycetoma infection pathogenesis. PLoS Negl. Trop. Dis. 2019, 13, e0007098. [Google Scholar] [CrossRef]
- Nasr, A.; Abushouk, A.; Hamza, A.; Siddig, E.; Fahal, A.H. Th-1, Th-2 Cytokines Profile among Madurella mycetomatis Eumycetoma Patients. PLoS Negl. Trop. Dis. 2016, 10, e0004862. [Google Scholar] [CrossRef]
- Grover, A.; Nagaraj, P.; Joseph, V.M.; Gadi, D. Unusual Presentation of Mycetoma of the Foot: A Rare Case Report. J. Orthop. Case Rep. 2017, 7, 12–15. [Google Scholar] [CrossRef] [PubMed]
- Abbott, P. Mycetoma in the Sudan. R. Soc. Trop. Med. Hyg. 1956, 50, 11–24. [Google Scholar] [CrossRef]
- Lopez Martinez, R.; Tovar, L.J.M.; Lavalle, P.; Welsh, O.; Saul, A.; Macotela Ruíz, A. Epidemiology of mycetoma in Mexico: Study of 2105 cases. Gac. Med. Mex. 1992, 128, 477–481. [Google Scholar] [PubMed]
- McGinnis, M.R. Mycetoma. Dermatol. Clin. 1996, 14, 97–104. [Google Scholar] [CrossRef]
- Ahmed, A.O.; van Leeuwen, W.; Fahal, A.; van de Sande, W.; Verbrugh, H.; van Belkum, A. Mycetoma caused by madurella mycetomatis: A neglected infectious burden. Lancet Infect. Dis. 2004, 4, 566–574. [Google Scholar] [CrossRef]
- Guerra-Leal, J.D.; Medrano-Danes, L.A.; Montemayor-Martinez, A.; Perez-Rodriguez, E.; Luna-Gurrola, C.E.; Arenas-Guzman, R.; Salas-Alanis, J.C. The importance of diagnostic imaging of mycetoma in the foot. Int. J. Dermatol. 2019, 58, 600–604. [Google Scholar] [CrossRef]
- Laohawiriyakamol, T.; Tanutit, P.; Kanjanapradit, K.; Hongsakul, K.; Ehara, S. The “dot-in-circle” sign in musculoskeletal mycetoma on magnetic resonance imaging and ultrasonography. SpringerPlus 2014, 3, 671. [Google Scholar] [CrossRef]
- Lichon, V.; Khachemoune, A. Mycetoma: A review. Am. J. Clin. Dermatol. 2006, 7, 315–321. [Google Scholar] [CrossRef]
- Queiroz-Telles, F.; Nucci, M.; Colombo, A.L.; Tobón, A.; Restrepo, A. Mycoses of implantation in Latin America: An overview of epidemiology, clinical manifestations, diagnosis and treatment. Med. Mycol. 2011, 49, 225–236. [Google Scholar] [CrossRef]
- Ahmed, S.A.; Kloezen, W.; Duncanson, F.; Zijlstra, E.E.; de Hoog, G.S.; Fahal, A.H.; van de Sande, W.W. Madurella mycetomatis is highly susceptible to ravuconazole. PLoS Negl. Trop. Dis. 2014, 8, e2942. [Google Scholar] [CrossRef]
- Alam, K.; Maheshwari, V.; Bhargava, S.; Jain, A.; Fatima, U.; Haq, E.U. Histological diagnosis of madura foot (mycetoma): A must for definitive treatment. J. Glob. Infect. Dis. 2009, 1, 64–67. [Google Scholar] [CrossRef] [PubMed]
- Traynor, T.R.; Huffnagle, G.B. Role of chemokines in fungal infections. Med. Mycol. 2001, 39, 41–50. [Google Scholar] [CrossRef] [PubMed]
- Bellocchio, S.; Bozza, S.; Montagnoli, C.; Perruccio, K.; Gaziano, R.; Pitzurra, L.; Romani, L. Immunity to Aspergillus fumigatus: The basis for immunotherapy and vaccination. Med. Mycol. 2005, 43 (Suppl. 1), S181–S188. [Google Scholar] [CrossRef] [PubMed]
- Crameri, R.; Blaser, K. Allergy and immunity to fungal infections and colonization. Eur. Respir. J. 2002, 19, 151–157. [Google Scholar] [CrossRef]
- van de Sande, W.W.; Fahal, A.; Verbrugh, H.; van Belkum, A. Polymorphisms in genes involved in innate immunity predispose toward mycetoma susceptibility. J. Immunol. 2007, 179, 3065–3074. [Google Scholar] [CrossRef]
- Mhmoud, N.A.; Fahal, A.H.; van de Sande, W.W. The association between the interleukin-10 cytokine and CC chemokine ligand 5 polymorphisms and mycetoma granuloma formation. Med. Mycol. 2013, 51, 527–533. [Google Scholar] [CrossRef]
- Quain, A.M.; Khardori, N.M. Nutrition in Wound Care Management: A Comprehensive Overview. Wounds 2015, 27, 327–335. [Google Scholar]
- Stechmiller, J.K. Understanding the role of nutrition and wound healing. Nutr. Clin. Pract. 2010, 25, 61–68. [Google Scholar] [CrossRef]
- Fahal, A.H.; el Hassan, A.M.; Abdelalla, A.O.; Sheik, H.E. Cystic mycetoma: An unusual clinical presentation of Madurella mycetomatis infection. Trans. R. Soc. Trop. Med. Hyg. 1998, 92, 66–67. [Google Scholar] [CrossRef]
- Ponka, D.; Baddar, F. Microscopic potassium hydroxide preparation. Can. Fam. Physician Med. Fam. Can. 2014, 60, 57. [Google Scholar]
- Ahmed, A.A.; van de Sande, W.; Fahal, A.H. Mycetoma laboratory diagnosis: Review article. PLoS Negl. Trop. Dis. 2017, 11, e0005638. [Google Scholar] [CrossRef] [PubMed]
- Kitisin, T.; Muangkaew, W.; Ampawong, S.; Chutoam, P.; Thanomsridetchai, N.; Tangwattanachuleeporn, M.; Sukphopetch, P. Isolation of fungal communities and identification of Scedosporium species complex with pathogenic potentials from a pigsty in Phra Nakhon Si Ayutthaya, Thailand. New Microbiol. 2021, 44, 33–41. [Google Scholar] [PubMed]
- Ramsperger, M.; Duan, S.; Sorrell, T.C.; Meyer, W.; Chen, S.C.A. The Genus Scedosporium and Pseudallescheria: Current Challenges in Laboratory Diagnosis. Curr. Clin. Microbiol. Rep. 2014, 1, 27–36. [Google Scholar] [CrossRef]
- Arenas, R.; Fernandez Martinez, R.F.; Torres-Guerrero, E.; Garcia, C. Actinomycetoma: An update on diagnosis and treatment. Cutis 2017, 99, E11–E15. [Google Scholar]
- Lackner, M.; Najafzadeh, M.J.; Sun, J.; Lu, Q.; Hoog, G.S. Rapid identification of Pseudallescheria and Scedosporium strains by using rolling circle amplification. Appl. Environ. Microbiol. 2012, 78, 126–133. [Google Scholar] [CrossRef]
- Desnos-Ollivier, M.; Bretagne, S.; Dromer, F.; Lortholary, O.; Dannaoui, E. Molecular identification of black-grain mycetoma agents. J. Clin. Microbiol. 2006, 44, 3517–3523. [Google Scholar] [CrossRef]
- Ahmed, S.A.; van de Sande, W.W.; Desnos-Ollivier, M.; Fahal, A.H.; Mhmoud, N.A.; de Hoog, G.S. Application of Isothermal Amplification Techniques for Identification of Madurella mycetomatis, the Prevalent Agent of Human Mycetoma. J. Clin. Microbiol. 2015, 53, 3280–3285. [Google Scholar] [CrossRef]
- Ahmed, S.A.; van den Ende, B.H.; Fahal, A.H.; van de Sande, W.W.; de Hoog, G.S. Rapid identification of black grain eumycetoma causative agents using rolling circle amplification. PLoS Negl. Trop. Dis. 2014, 8, e3368. [Google Scholar] [CrossRef]
- Fraser, M.; Borman, A.M.; Johnson, E.M. Rapid and Robust Identification of the Agents of Black-Grain Mycetoma by Matrix-Assisted Laser Desorption Ionization-Time of Flight Mass Spectrometry. J. Clin. Microbiol. 2017, 55, 2521–2528. [Google Scholar] [CrossRef]
- Salinas-Carmona, M.C.; Welsh, O.; Casillas, S.M. Enzyme-linked immunosorbent assay for serological diagnosis of Nocardia brasiliensis and clinical correlation with mycetoma infections. J. Clin. Microbiol. 1993, 31, 2901–2906. [Google Scholar] [CrossRef] [PubMed]
- Gumaa, S.A.; Mahgoub, E.S. Counterimmunoelectrophoresis in the diagnosis of mycetoma and its sensitivity as compared to immunodiffusion. Sabouraudia 1975, 13, 309–315. [Google Scholar] [CrossRef] [PubMed]
- McLaren, M.L.; Mahgoub, E.S.; Georgakopoulos, E. Preliminary investigation of the use of the enzyme linked immunosorbent assay (ELISA) in the serodiagnosis of mycetoma. Sabouraudia 1978, 16, 225–228. [Google Scholar] [CrossRef] [PubMed]
- van de Sande, W.W.; Janse, D.J.; Hira, V.; Goedhart, H.; van der Zee, R.; Ahmed, A.O.; Ott, A.; Verbrugh, H.; van Belkum, A. Translationally controlled tumor protein from Madurella mycetomatis, a marker for tumorous mycetoma progression. J. Immunol. 2006, 177, 1997–2005. [Google Scholar] [CrossRef] [PubMed]
- Elbadawi, H.S.; Mahgoub, E.; Mahmoud, N.; Fahal, A.H. Use of immunoblotting in testing Madurella mycetomatis specific antigen. Trans. R. Soc. Trop. Med. Hyg. 2016, 110, 312–316. [Google Scholar] [CrossRef]
- Fahal, A.H.; Finkelman, M.A.; Zhang, Y.; van de Sande, W.W. Detection of (1→3)-β-d-Glucan in Eumycetoma Patients. J. Clin. Microbiol. 2016, 54, 2614–2617. [Google Scholar] [CrossRef]
- El Shamy, M.E.; Fahal, A.H.; Shakir, M.Y.; Homeida, M.M. New MRI grading system for the diagnosis and management of mycetoma. Trans. R. Soc. Trop. Med. Hyg. 2012, 106, 738–742. [Google Scholar] [CrossRef]
- Hao, X.; Freedman, D.; Yim, J.; Le, M.; Baglio, R.; Levine, D.; Saffo, G.; Parthasarathy, P.; Mirkin, G. Dermatofibromas on the Foot and Ankle: A Clinicopathological Characterization of 31 Cases. JAPMA 2022, in press.
- Hao, X.; Billings, S.D.; Wu, F.; Stultz, T.W.; Procop, G.W.; Mirkin, G.; Vidimos, A.T. Dermatofibrosarcoma Protuberans: Update on the Diagnosis and Treatment. J. Clin. Med. 2020, 9, 1752. [Google Scholar] [CrossRef]
- Madden, C.; Spector, A.; Siddiqui, S.; Mirkin, G.; Yim, J.; Hao, X. Dermatofibrosarcoma Protuberans on Adult Toes: A Case Report and Review of the Literature. Anticancer. Res. 2019, 39, 2105–2111. [Google Scholar] [CrossRef]
- Hao, X.; Yim, J.; Robles-Sherman, E.; Firestone, L.; Bannerjee, A.; Vieweger, D.; Daughtry, E.; Le, M.; Mirkin, G.; Rubenstein, S. Clinicopathological characterization of the Kaposi sarcoma on the foot and ankle: Analysis of 11 Pptients seen in our clinics. JAPMA 2022, in press.
- Hao, X.; Yim, J.; Chang, S.; Schwartz, E.; Rubenstein, S.; Friske, C.; Shamim, S.; Masternick, E.; Mirkin, G. Acral Lentiginous Melanoma of Foot and Ankle: A Clinicopathological Study of 7 Cases. Anticancer Res. 2019, 39, 6175–6181. [Google Scholar] [CrossRef] [PubMed]
- Lacroix, C.; de Kerviler, E.; Morel, P.; Derouin, F.; Feuilhade de Chavin, M. Madurella mycetomatis mycetoma treated successfully with oral voriconazole. Br. J. Dermatol. 2005, 152, 1067–1068. [Google Scholar] [CrossRef] [PubMed]
- Loulergue, P.; Hot, A.; Dannaoui, E.; Dallot, A.; Poirée, S.; Dupont, B.; Lortholary, O. Successful treatment of black-grain mycetoma with voriconazole. Am. J. Trop. Med. Hyg. 2006, 75, 1106–1107. [Google Scholar] [CrossRef][Green Version]
- Negroni, R.; Tobón, A.; Bustamante, B.; Shikanai-Yasuda, M.A.; Patino, H.; Restrepo, A. Posaconazole treatment of refractory eumycetoma and chromoblastomycosis. Rev. Inst. Med. Trop. Sao Paulo 2005, 47, 339–346. [Google Scholar] [CrossRef]
- Karrakchou, B.; Boubnane, I.; Senouci, K.; Hassam, B. Madurella mycetomatis infection of the foot: A case report of a neglected tropical disease in a non-endemic region. BMC Dermatol. 2020, 20, 1. [Google Scholar] [CrossRef]
- Noguchi, H.; Matsumoto, T.; Kimura, U.; Hiruma, M.; Kano, R.; Kubo, M.; Fukushima, S.; Ihn, H. Fosravuconazole to treat severe onychomycosis in the elderly. J. Dermatol. 2021, 48, 228–231. [Google Scholar] [CrossRef]
- Shimoyama, H.; Yo, A.; Sei, Y.; Kuwano, Y. Treatment Outcome with Fosravuconazole for Onychomycosis. Mycopathologia 2021, 186, 259–267. [Google Scholar] [CrossRef]
- Cárdenas-de la Garza, J.A.; Welsh, O.; Cuéllar-Barboza, A.; Suarez-Sánchez, K.P.; De la Cruz-Valadez, E.; Cruz-Gómez, L.G.; Gallardo-Rocha, A.; Ocampo-Candiani, J.; Vera-Cabrera, L. Clinical characteristics and treatment of actinomycetoma in northeast Mexico: A case series. PLoS Negl. Trop. Dis. 2020, 14, e0008123. [Google Scholar] [CrossRef]
- Suleiman, S.H.; Wadaella el, S.; Fahal, A.H. The Surgical Treatment of Mycetoma. PLoS Negl. Trop. Dis. 2016, 10, e0004690. [Google Scholar] [CrossRef]
- Wadal, A.; Elhassan, T.A.; Zein, H.A.; Abdel-Rahman, M.E.; Fahal, A.H. Predictors of Post-operative Mycetoma Recurrence Using Machine-Learning Algorithms: The Mycetoma Research Center Experience. PLoS Negl. Trop. Dis. 2016, 10, e0005007. [Google Scholar] [CrossRef] [PubMed]
- Welsh, O.; Al-Abdely, H.M.; Salinas-Carmona, M.C.; Fahal, A.H. Mycetoma medical therapy. PLoS Negl. Trop. Dis. 2014, 8, e3218. [Google Scholar] [CrossRef] [PubMed]
- Al-Kathiri, L.; Al-Najjar, T.; Al-Asmaili, A. Successful Treatment of Recalcitrant Actinomycetoma of Gluteal Area with Combined Medical Treatment and Surgical Excision with Graft Reconstruction. Oman Med. J. 2020, 35, e111. [Google Scholar] [CrossRef] [PubMed]

| Eumycetoma | Actinomycetoma | |
|---|---|---|
| Pathogen | Fungi | Bacteria |
| Pathogenesis | Slow | Rapid |
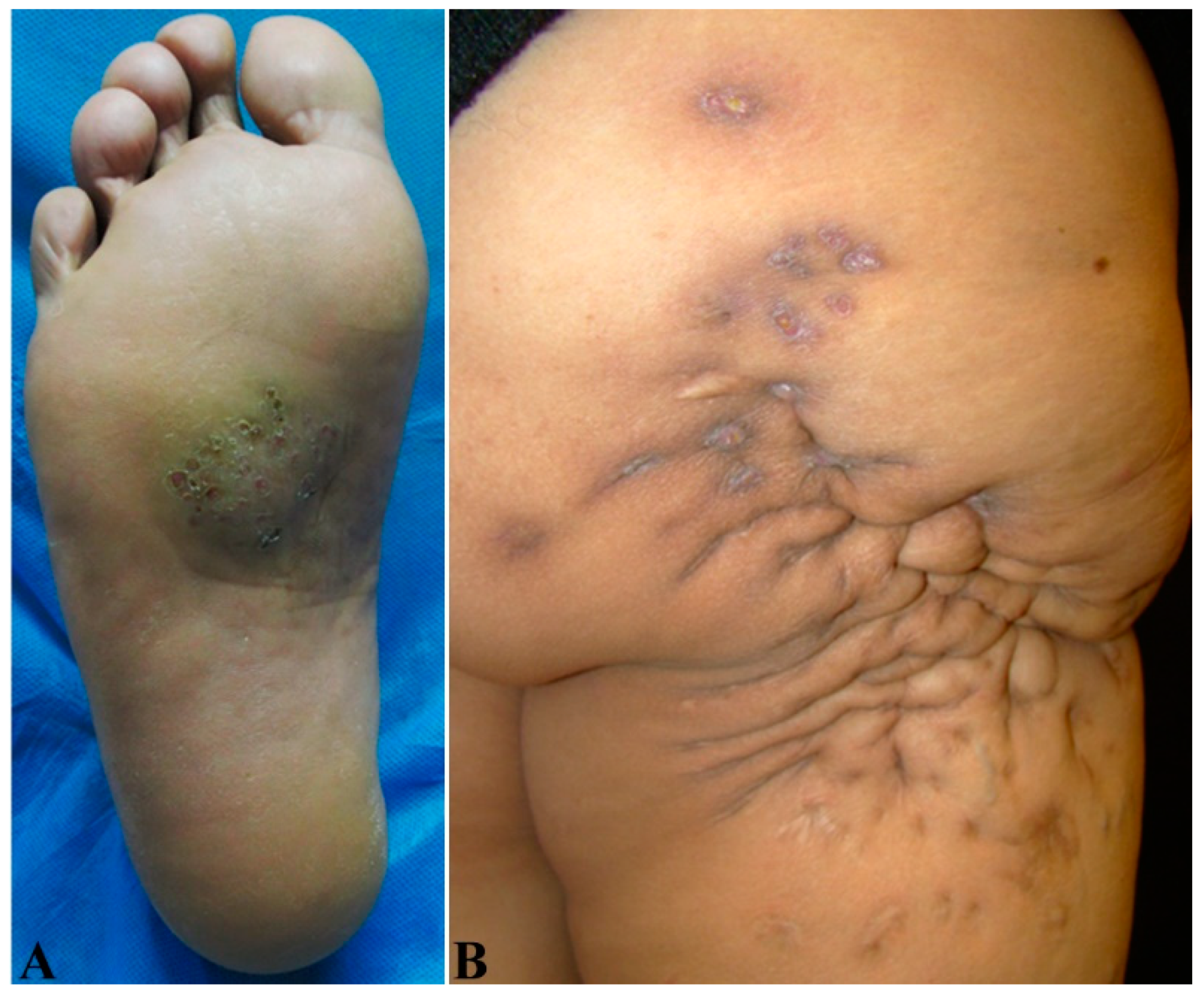
| Gross appearance | Single or multiple nodules with clear margin with rare or a few sinuses (Figure 3A,B) | Diffuse lesions without clear margin and with multiple sinuses and discharge of grains (Figure 2A,B) |
| Body region involved | The majority on the foot (70%; Figure 2A and Figure 3A,B) and hand (10%) [15]; the remaining in other parts of the body | Most on the foot (60%), followed by the trunk (back and chest), arms, forearms, legs, knees, thighs (Figure 2B), hands, shoulders, and abdominal wall [27] |
| Colors of grains [28] | Black: Madurella mycetomatis, Trematosphaeria grisea (formerly Madurella grisea), Leptospheria senegalensis, Leptosphaeria thompkinsii, Exophiala jeanselmei, Medicopsis romeroi (formerly P.romeroi), Curvularia lunata, Phytophthora parasitica, Plenodomus avramii, Corynespora cassiicola, Phialophora verrucosa, Pseudochaetosphaeronema larense White: Neotestudina rosatii, Acremonium falciforme, Acremonium kiliense, Acremonium recifei, Cylindrocarpon cyanescens, Cylindrocarpon destructans, Scedosporium apiospermum (formerly Pseudallescheria boydii), Fusarium oxysoprum, Fusarium solani, Fusarium moniliforme, Cladosporium cladosporioides, Polycytella hominis White or pale: Aspergillus nidulans Green or pale: Aspergillus flavus | White–yellow or pink: Actinomadura madurae Yellow–brown: Streptomyces somaliensis Red: Actinomadura pellitieri White–yellow: Actinomyces israelii, Nocardia caviae, Nocardia farcinica White: Nocardia asteroides, Nocardia brasiliensis, Nocardia transvalensis Cream: Nocardia dassonvillei |
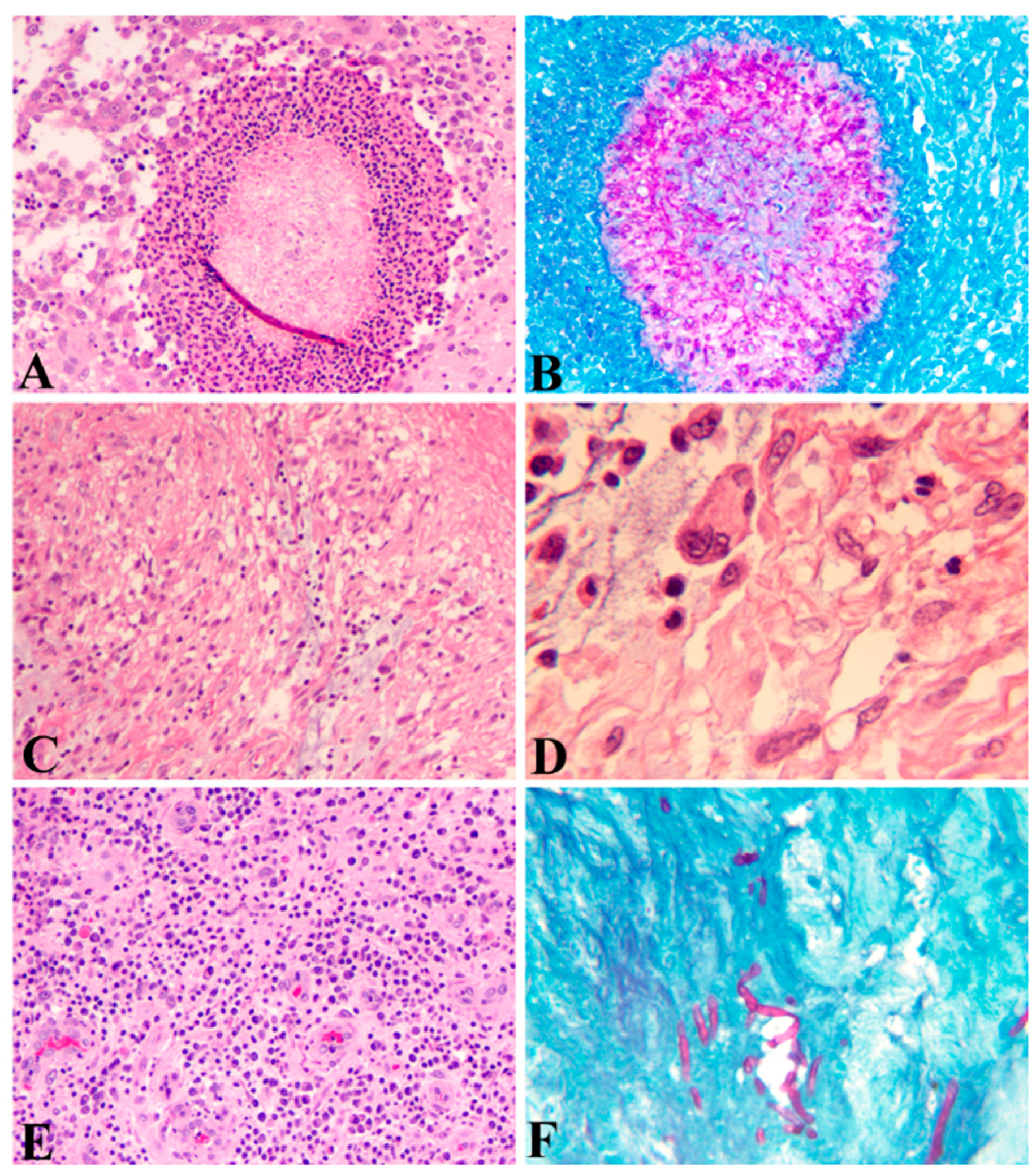
| Grain morphology | Madurella mycetomatis: Large granules (up to 1–2 mm or more) with interlacing hyphae embedded in interstitial brownish matrix; hyphae at periphery arranged radially with numerous chlamydospores Scedosporium apiospermum (formerly Pseudallescheria boydii): Eosinophilic, lighter in the center; numerous vesicles or swollen hyphae; peripheral eosinophilic fringe | Actinomadura madurae: Large (1–5 mm) and multilobulate; peripherally basophilic and centrally eosinophilic or pale-stained; filaments grow from the peripheral zone Streptomyces somaliensis: Large 0.5–2 mm or more) with dense thin filaments; often homogenously stained; transverse fracture lines Actinomyces israelii: Small grains (approximately 1 mm); central purple zone; loose clumps of filaments; Gram-positive delicate branching filaments breaking up into bacillary and coccal forms; Gram-negative amorphous matrix |
| Direct microscopy | KOH mount: Fungal hyphae and spores | Lugol’s iodine stain: filaments with a width of 0.5–1 μm |
| Histospecial staining | Periodic Acid–Schiff (PAS) (Figure 1B,F), Gomori Methanamine Silver (GMS) 2–5 µm wide hyphae | Gram, Acid-Fast Bacillus (AFB) Actinomadura grains are Gram positive, with 0.5–1 µm wide branching filaments and are AFB negative Nocardia species are Gram positive, and nearly all are weakly acid fast HE: the small grains of Nocardia are eosinophilic with a blue center and pink filaments |
| Bone invasion | Rare or involved after a long time | Rapid |
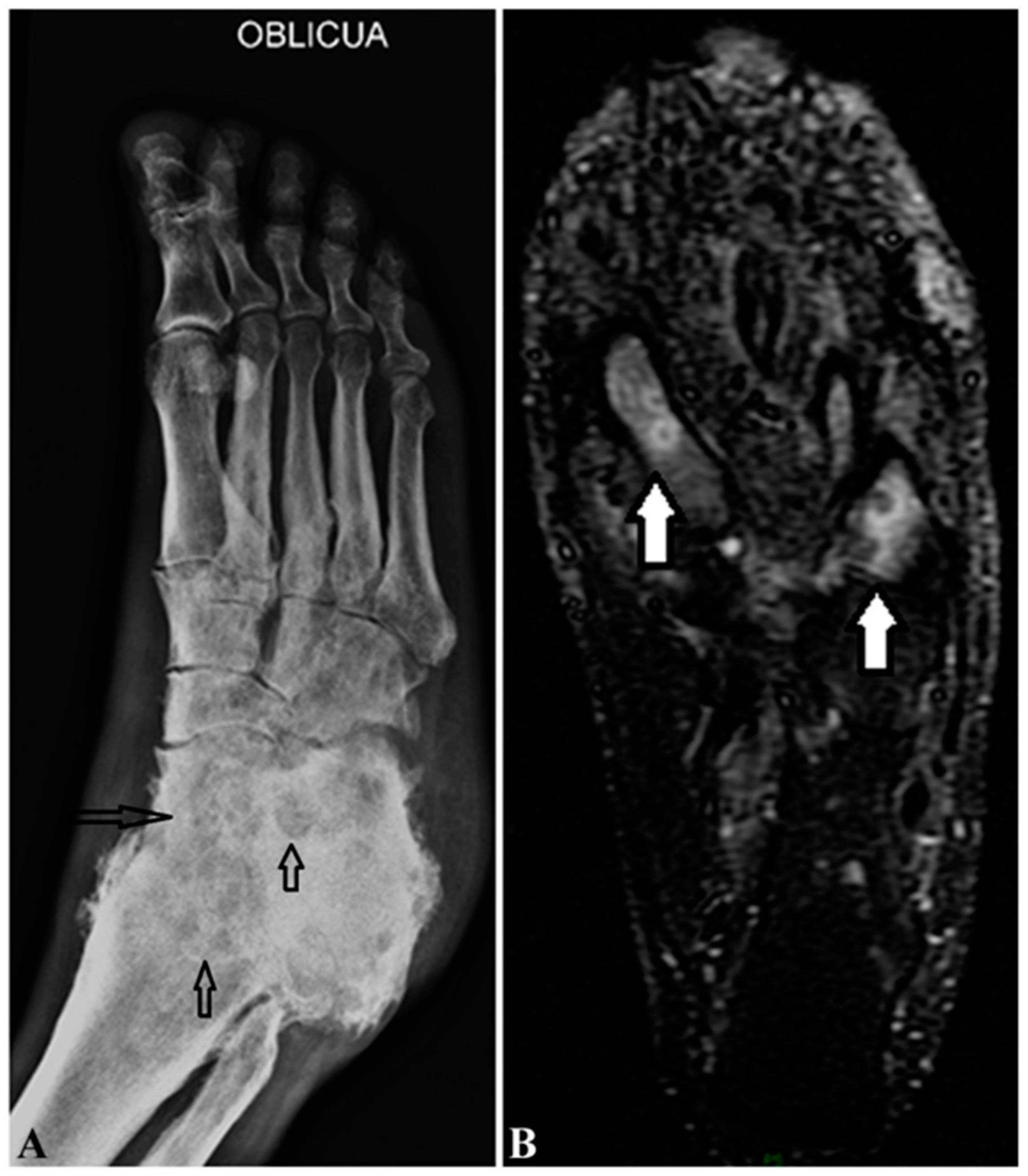
| Radiograph | Normal density and structure of the bone if not involved, “punched out” sign on the bone if involved [29] | “punched out” sign on the bones if involved (Figure 4A) [29] |
| Magnetic Resonance Imaging (MRI) and ultrasonography | “Dot in Circle” [12,29,30] Discrete small round hyperintense circles with central hypointense dots in the hypointense matrix of mass | “Dot in Circle” [29,30] Multiple small round hyperintense circles with central hypointense dots in the hypointense matrix of mass (Figure 4B) |
| Treatment | Surgical excision plus antifungal therapy | Antibiotics |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hao, X.; Cognetti, M.; Burch-Smith, R.; Mejia, E.O.; Mirkin, G. Mycetoma: Development of Diagnosis and Treatment. J. Fungi 2022, 8, 743. https://doi.org/10.3390/jof8070743
Hao X, Cognetti M, Burch-Smith R, Mejia EO, Mirkin G. Mycetoma: Development of Diagnosis and Treatment. Journal of Fungi. 2022; 8(7):743. https://doi.org/10.3390/jof8070743
Chicago/Turabian StyleHao, Xingpei, Marcus Cognetti, Rhonda Burch-Smith, Emerald O’Sullivan Mejia, and Gene Mirkin. 2022. "Mycetoma: Development of Diagnosis and Treatment" Journal of Fungi 8, no. 7: 743. https://doi.org/10.3390/jof8070743
APA StyleHao, X., Cognetti, M., Burch-Smith, R., Mejia, E. O., & Mirkin, G. (2022). Mycetoma: Development of Diagnosis and Treatment. Journal of Fungi, 8(7), 743. https://doi.org/10.3390/jof8070743






