Ocular Fungal Infections
1. Introduction
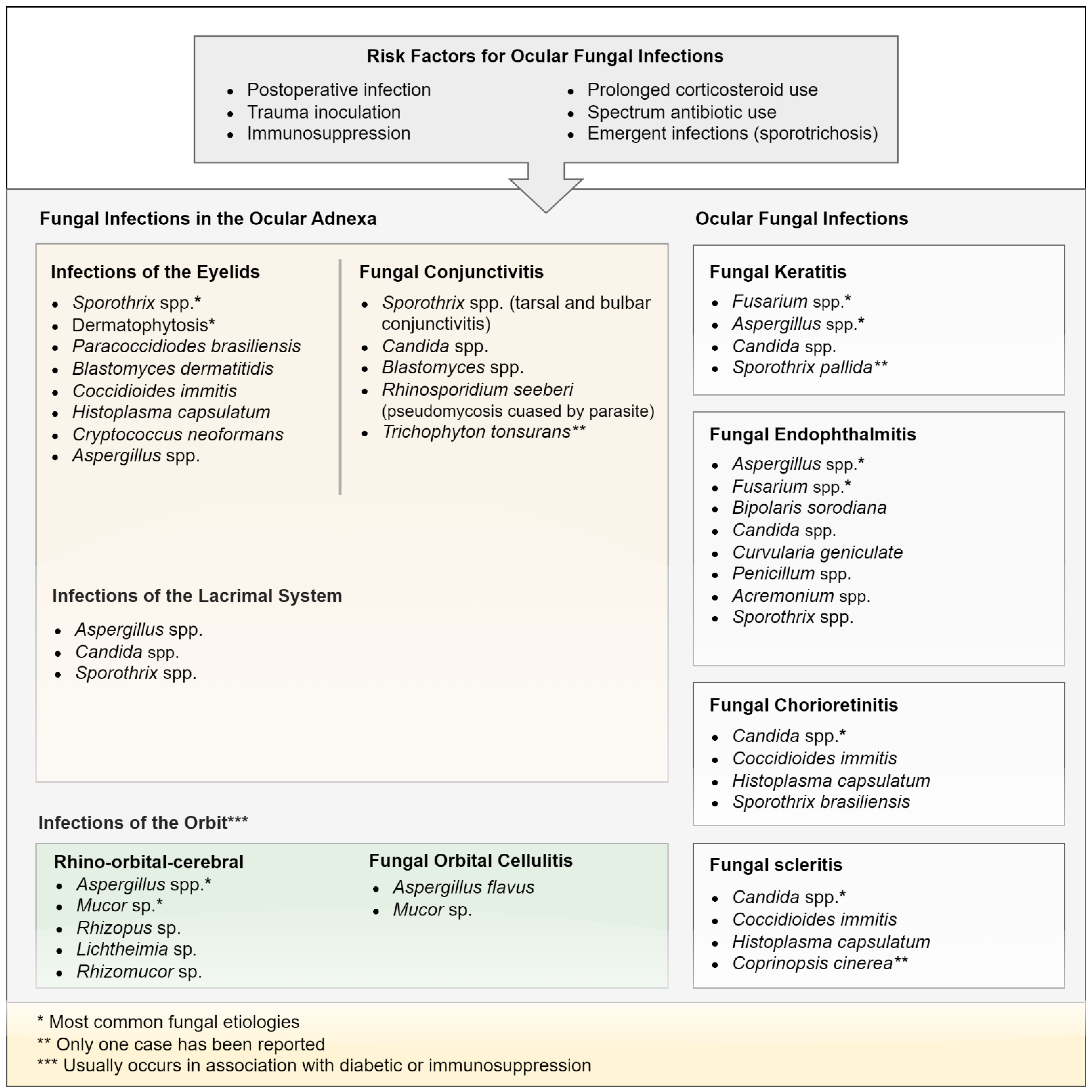
2. Fungal Infections in the Ocular Adnexa
3. Fungal Eye Infections
4. Conclusions
Funding
Conflicts of Interest
References
- Kalkanci, A.; Ozdek, S. Ocular Fungal Infections. Curr. Eye Res. 2011, 36, 179–189. [Google Scholar] [CrossRef] [PubMed]
- Tabbara, K.F. Infections of the Lacrimal System. In Ocular Infections; Essentials in Ophthalmology Book Series; Tabbara, K., El-Asrar, A., Khairallah, M., Eds.; Springer: Berlin/Heidelberg, Germany, 2014. [Google Scholar] [CrossRef]
- Sodhi, G.; Liu, E.; Renz, J.; Heher, K.; Kapadia, M. Infections of the Eyelids, Orbit, and Ocular Adnexa. In The Infected Eye; Laver, N., Specht, C., Eds.; Springer: Cham, Switzerland, 2016. [Google Scholar] [CrossRef]
- Khairallah, M.; Attia, S. Infections of the Orbit. In Ocular Infections; Essentials in Ophthalmology Book Series; Tabbara, K., El-Asrar, A., Khairallah, M., Eds.; Springer: Berlin/Heidelberg, Germany, 2014. [Google Scholar] [CrossRef]
- Moussa, K.; Ramanathan, S. Periocular Infections. In Emergency Management of Infectious Diseases; Chin, R., Frazee, B., Coralic, Z., Eds.; Cambridge University Press: Cambridge, UK, 2018; pp. 265–273. [Google Scholar] [CrossRef]
- Ramírez Soto, M.C. Sporotrichosis in the Ocular Adnexa: 21 Cases in an Endemic Area in Peru and Review of the Literature. Am. J. Ophthalmol. 2016, 162, 173–179.e3. [Google Scholar] [CrossRef] [PubMed]
- Gervini, R.L.; Vettorato, G.; Lecompte, S.M.; Biasi, T.B.; Ruthner, F.G.; Kronbauer, F.L. Ocular paracoccidioidomycosis: Report of two cases and review of literature. An. Bras. Dermatol. 2004, 79, 69–78. [Google Scholar] [CrossRef]
- Cruz, A.A.; Zenha, F.; Silva, J.T., Jr.; Martinez, R. Eyelid involvement in paracoccidioidomycosis. Ophthalmic Plast. Reconstr. Surg. 2004, 20, 212–216. [Google Scholar] [CrossRef]
- Fierro-Arias, L.; Araiza, J.; Cortés, D.; Hernández, M.A.; Ponce, R.M.; Bonifaz, A. Blepharitis associated to opportunistic fungi. Dermatol. Rev. Mex. 2014, 58, 134–141. [Google Scholar]
- Pemberton, J.D.; Vidor, I.; Sivak-Callcott, J.A.; Bailey, N.G.; Sarwari, A.R. North American blastomycosis of the eyelid. Ophthalmic Plast. Reconstr. Surg. 2009, 25, 230–232. [Google Scholar] [CrossRef]
- Dworak, D.P.; Kapustiak, J.; Ehklassi, T.A.; Patrianakos, T.D. Primary Cutaneous Coccidioidomycosis of the Eyelid: A Case Report. Ophthalmic Plast. Reconstr. Surg. 2016, 32, e40–e41. [Google Scholar] [CrossRef]
- Gupta, H.; Tankhiwale, S.S. A case of bilateral eyelid histoplasmosis mistaken as basal cell carcinoma. Can. J. Ophthalmol. 2017, 52, e45–e46. [Google Scholar] [CrossRef][Green Version]
- Deutsch, A.; Guzman, A.K.; Hossain, C.; Balagula, Y. Persistent eyelid ulceration in an immunocompromised host: A cutaneous sign with the potential for early diagnosis and intervention in disseminated cryptococcosis. JAAD Case Rep. 2020, 6, 388–389. [Google Scholar] [CrossRef]
- Das, D.; Modaboyina, S.; Bhandari, A.; Agrawal, S. Lower eyelid aspergillosis infection mimicking a pyogenic granuloma in a pregnant lady. BMJ Case Rep. 2020, 13, e238732. [Google Scholar] [CrossRef]
- Roy, A.; Srinivasan, M.; Das, S. Fungal Keratitis. In Infections of the Cornea and Conjunctiva; Das, S., Jhanji, V., Eds.; Springer: Singapore, 2021. [Google Scholar] [CrossRef]
- Klotz, S.A.; Penn, C.C.; Negvesky, G.J.; Butrus, S.I. Fungal and parasitic infections of the eye. Clin. Microbiol. Rev. 2000, 13, 662–685. [Google Scholar] [CrossRef]
- Arinelli, A.; Aleixo, A.L.Q.C.; Freitas, D.F.S.; do Valle, A.C.F.; Almeida-Paes, R.; Nobre Guimarães, A.L.; Oliveira, R.V.C.; Gutierrez-Galhardo, M.C.; Curi, A.L.L. Ocular Manifestations of Sporotrichosis in a Hyperendemic Region in Brazil: Description of a Series of 120 Cases. Ocul. Immunol. Inflamm. 2022, 2022, 1–9. [Google Scholar] [CrossRef]
- Ramírez-Soto, M.C.; Tirado-Sánchez, A.; Bonifaz, A. Ocular Sporotrichosis. J. Fungi 2021, 7, 951. [Google Scholar] [CrossRef]
- Garg, P.; Roy, A.; Roy, S. Update on fungal keratitis. Curr. Opin. Ophthalmol. 2016, 27, 333–339. [Google Scholar] [CrossRef]
- Mills, B.; Radhakrishnan, N.; Karthikeyan Rajapandian, S.G.; Rameshkumar, G.; Lalitha, P.; Prajna, N.V. The role of fungi in fungal keratitis. Exp. Eye Res. 2021, 202, 108372. [Google Scholar] [CrossRef]
- Raj, N.; Vanathi, M.; Ahmed, N.H.; Gupta, N.; Lomi, N.; Tandon, R. Recent Perspectives in the Management of Fungal Keratitis. J. Fungi 2021, 7, 907. [Google Scholar] [CrossRef]
- Mayya, V.; Kamath Shevgoor, S.; Kulkarni, U.; Hazarika, M.; Barua, P.D.; Acharya, U.R. Multi-Scale Convolutional Neural Network for Accurate Corneal Segmentation in Early Detection of Fungal Keratitis. J. Fungi 2021, 7, 850. [Google Scholar] [CrossRef]
- Chongkae, S.; Youngchim, S.; Nosanchuk, J.D.; Laliam, A.; Tangmonkongvoragul, C.; Pruksaphon, K. Fungal Keratitis in Northern Thailand: Spectrum of Agents, Risk Factors and Putative Virulence Factors. J. Fungi 2021, 7, 475. [Google Scholar] [CrossRef]
- Huang, T.-E.; Ou, J.-H.; Hung, N.; Yeh, L.-K.; Ma, D.H.-K.; Tan, H.-Y.; Chen, H.-C.; Hung, K.-H.; Fan, Y.-C.; Sun, P.-L.; et al. Fusarium Keratitis in Taiwan: Molecular Identification, Antifungal Susceptibilities, and Clinical Features. J. Fungi 2022, 8, 476. [Google Scholar] [CrossRef]
- Durand, M.L. Bacterial and Fungal Endophthalmitis. Clin. Microbiol. Rev. 2017, 30, 597–613. [Google Scholar] [CrossRef]
- Haseeb, A.A.; Elhusseiny, A.M.; Siddiqui, M.Z.; Ahmad, K.T.; Sallam, A.B. Fungal Endophthalmitis: A Comprehensive Review. J. Fungi 2021, 7, 996. [Google Scholar] [CrossRef]
- Sakamoto, T.; Gotoh, K.; Hashimoto, K.; Tanamachi, C.; Watanabe, H. Risk Factors and Clinical Characteristics of Patients with Ocular Candidiasis. J. Fungi 2022, 8, 497. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ramírez-Soto, M.C.; Bonifaz, A. Ocular Fungal Infections. J. Fungi 2022, 8, 1078. https://doi.org/10.3390/jof8101078
Ramírez-Soto MC, Bonifaz A. Ocular Fungal Infections. Journal of Fungi. 2022; 8(10):1078. https://doi.org/10.3390/jof8101078
Chicago/Turabian StyleRamírez-Soto, Max Carlos, and Alexandro Bonifaz. 2022. "Ocular Fungal Infections" Journal of Fungi 8, no. 10: 1078. https://doi.org/10.3390/jof8101078
APA StyleRamírez-Soto, M. C., & Bonifaz, A. (2022). Ocular Fungal Infections. Journal of Fungi, 8(10), 1078. https://doi.org/10.3390/jof8101078





