Epidemiological Trends of Candidemia and the Impact of Adherence to the Candidemia Guideline: Six-Year Single-Center Experience
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Definition
2.3. Statistical Analysis
3. Results
3.1. Patient Population and Clinical Characteristics Stratified by Study Periods
3.2. Analysis of Risk Factors for Mortality
3.3. Candidemia and Candida Species with Resistance Patterns
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Pappas, P.G.; Kauffman, C.A.; Andes, D.R.; Clancy, C.J.; Marr, K.A.; Ostrosky-Zeichner, L.; Reboli, A.C.; Schuster, M.G.; Vazquez, J.A.; Walsh, T.J.; et al. Clinical Practice Guideline for the Management of Candidiasis: 2016 Update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2016, 62, e1–e50. [Google Scholar] [CrossRef] [PubMed]
- Horn, D.L.; Neofytos, D.; Anaissie, E.J.; Fishman, J.A.; Steinbach, W.J.; Olyaei, A.J.; Marr, K.A.; Pfaller, M.A.; Chang, C.H.; Webster, K.M. Epidemiology and outcomes of candidemia in 2019 patients: Data from the prospective antifungal therapy alliance registry. Clin. Infect. Dis. 2009, 48, 1695–1703. [Google Scholar] [CrossRef]
- Antinori, S.; Milazzo, L.; Sollima, S.; Galli, M.; Corbellino, M. Candidemia and invasive candidiasis in adults: A narrative review. Eur. J. Intern Med. 2016, 34, 21–28. [Google Scholar] [CrossRef] [PubMed]
- Guinea, J. Global trends in the distribution of Candida species causing candidemia. Clin. Microbiol. Infect. 2014, 20 (Suppl. 6), 5–10. [Google Scholar] [CrossRef] [PubMed]
- Morii, D.; Seki, M.; Binongo, J.N.; Ban, R.; Kobayashi, A.; Sata, M.; Hashimoto, S.; Shimizu, J.; Morita, S.; Tomono, K. Distribution of Candida species isolated from blood cultures in hospitals in Osaka, Japan. J. Infect. Chemother. 2014, 20, 558–562. [Google Scholar] [CrossRef]
- Jung, S.I.; Shin, J.H.; Song, J.H.; Peck, K.R.; Lee, K.; Kim, M.N.; Chang, H.H.; Moon, C.S.; Korean Study Group for Candidemia. Multicenter surveillance of species distribution and antifungal susceptibilities of Candida bloodstream isolates in South Korea. Med. Mycol. 2010, 48, 669–674. [Google Scholar]
- Yoo, J.I.; Choi, C.W.; Lee, K.M.; Kim, Y.K.; Kim, T.U.; Kim, E.C.; Joo, S.I.; Yun, S.H.; Lee, Y.S.; Kim, B.S. National surveillance of antifungal susceptibility of Candida species in South Korean hospitals. Med. Mycol. 2009, 47, 554–558. [Google Scholar] [CrossRef] [PubMed]
- Woo, E.K.; Han, C.; Jo, S.A.; Park, M.K.; Kim, S.; Kim, E.; Park, M.H.; Lee, J.; Jo, I. Morbidity and related factors among elderly people in South Korea: Results from the AnsanGeriatric (AGE) cohort study. BMC Public Health 2007, 7, 10. [Google Scholar] [CrossRef]
- Hsu, L.Y.; Lee, D.G.; Yeh, S.P.; Bhurani, D.; Khanh, B.Q.; Low, C.Y.; Norasetthada, L.; Chan, T.; Kwong, Y.L.; Vaid, A.K.; et al. Epidemiology of invasive fungal diseases among patients with haematological disorders in the Asia-Pacific: A prospective observational study. Clin. Microbiol. Infect. 2015, 21, e7–e11. [Google Scholar] [CrossRef][Green Version]
- Choi, H.; Kim, J.H.; Seong, H.; Lee, W.; Jeong, W.; Ahn, J.Y.; Jeong, S.J.; Ku, N.S.; Yeom, J.S.; Kim, Y.K.; et al. Changes in the utilization patterns of antifungal agents, medical cost and clinical outcomes of candidemia from the health-care benefit expansion to include newer antifungal agents. Int. J. Infect. Dis. 2019, 83, 49–55. [Google Scholar] [CrossRef]
- Huang, H.Y.; Lu, P.L.; Wang, Y.L.; Chen, T.C.; Chang, K.; Lin, S.Y. Usefulness of EQUAL Candida scores for predicting outcomes in patients with candidemia: A retrospective cohort study. Clin. Microbiol. Infect. 2020, 26, 1501–1506. [Google Scholar] [CrossRef]
- Singer, M.; Deutschman, C.S.; Seymour, C.W.; Shankar-Hari, M.; Annane, D.; Bauer, M.; Bellomo, R.; Bernard, G.R.; Chiche, J.D.; Coopersmith, C.M.; et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). JAMA 2016, 315, 801–810. [Google Scholar] [CrossRef]
- Mellinghoff, S.C.; Hoenigl, M.; Koehler, P.; Kumar, A.; Lagrou, K.; Lass-Flörl, C.; Meis, J.F.; Menon, V.; Rautemaa-Richardson, R.; Cornely, O.A. EQUAL Candida Score: An ECMM score derived from current guidelines to measure QUAlity of Clinical Candidaemia Management. Mycoses 2018, 61, 326–330. [Google Scholar] [CrossRef] [PubMed]
- Bassetti, M.; Vena, A.; Meroi, M.; Cardozo, C.; Cuervo, G.; Giacobbe, D.R.; Salavert, M.; Merino, P.; Gioia, F.; Fernández-Ruiz, M.; et al. Factors associated with the development of septic shock in patients with candidemia: A post hoc analysis from two prospective cohorts. Crit. Care 2020, 24, 117. [Google Scholar] [CrossRef] [PubMed]
- Park, J.S.; Cho, S.H.; Youn, S.K.; Bak, Y.S.; Yu, Y.B.; Kim, Y.K. Epidemiological Characterization of Opportunistic Mycoses between the Years 2006 and 2010 in Korea. J. Microbiol. Biotechnol. 2016, 26, 145–150. [Google Scholar] [CrossRef] [PubMed]
- Conde-Rosa, A.; Amador, R.; Pérez-Torres, D.; Colón, E.; Sánchez-Rivera, C.; Nieves-Plaza, M.; González-Ramos, M.; Bertrán-Pasarell, J. Candidemia distribution, associated risk factors, and attributed mortality at a university-based medical center. Puerto Rico Health Sci. J. 2010, 29, 26–29. [Google Scholar]
- Li, D.; Xia, R.; Zhang, Q.; Bai, C.; Li, Z.; Zhang, P. Evaluation of candidemia in epidemiology and risk factors among cancer patients in a cancer center of China: An 8-year case-control study. BMC Infect. Dis. 2017, 17, 536. [Google Scholar] [CrossRef][Green Version]
- Karabinis, A.; Hill, C.; Leclercq, B.; Tancrède, C.; Baume, D.; Andremont, A. Risk factors for candidemia in cancer patients: A case-control study. J. Clin. Microbiol. 1988, 26, 429–432. [Google Scholar] [CrossRef]
- Ortíz Ruiz, G.; Osorio, J.; Valderrama, S.; Álvarez, D.; Elías Díaz, R.; Calderón, J.; Ballesteros, D.; Franco, A. Risk factors for candidemia in non-neutropenic critical patients in Colombia. Med. Intensiva. 2016, 40, 139–144. [Google Scholar] [CrossRef] [PubMed]
- Finnerty, C.C.; Mabvuure, N.T.; Ali, A.; Kozar, R.A.; Herndon, D.N. The surgically induced stress response. JPEN J. Parenter. Enter. Nutr. 2013, 37 (Suppl. 5), 21S–29S. [Google Scholar] [CrossRef]
- Deitch, E.A.; Bridges, R.M. Effect of stress and trauma on bacterial translocation from the gut. J. Surg. Res. 1987, 42, 536–542. [Google Scholar] [CrossRef]
- Storfer, S.P.; Medoff, G.; Fraser, V.J.; Powderly, W.G.; Dunagan, W.C. Candiduria: Retrospective Review in Hospitalized Patients. Infect. Dis. Clin. Pract. 2014, 3, 23–29. [Google Scholar] [CrossRef]
- Ishikane, M.; Hayakawa, K.; Kutsuna, S.; Takeshita, N.; Ohmagari, N. The impact of infectious disease consultation in candidemia in a tertiary care hospital in Japan over 12 years. PLoS ONE 2019, 14, e0215996. [Google Scholar] [CrossRef] [PubMed]
- Vaquero-Herrero, M.P.; Ragozzino, S.; Castaño-Romero, F.; Siller-Ruiz, M.; Sánchez González, R.; García-Sánchez, J.E.; García-García, I.; Marcos, M.; Ternavasio-de la Vega, H.G. The Pitt Bacteremia Score, Charlson Comorbidity Index and Chronic Disease Score are useful tools for the prediction of mortality in patients with Candida bloodstream infection. Mycoses 2017, 60, 676–685. [Google Scholar] [CrossRef] [PubMed]
- Kang, S.J.; Kim, S.E.; Kim, U.J.; Jang, H.C.; Park, K.H.; Shin, J.H.; Jung, S.I. Clinical characteristics and risk factors for mortality in adult patients with persistent candidemia. J. Infect. 2017, 75, 246–253. [Google Scholar] [CrossRef]
- Schroeder, M.; Weber, T.; Denker, T.; Winterland, S.; Wichmann, D.; Rohde, H.; Ozga, A.K.; Fischer, M.; Kluge, S. Epidemiology, clinical characteristics, and outcome of candidemia in critically ill patients in Germany: A single-center retrospective 10-year analysis. Ann. Intensive Care 2020, 10, 142. [Google Scholar] [CrossRef] [PubMed]
- Morrell, M.; Fraser, V.J.; Kollef, M.H. Delaying the empiric treatment of candida bloodstream infection until positive blood culture results are obtained: A potential risk factor for hospital mortality. Antimicrob. Agents Chemother. 2005, 49, 3640–3645. [Google Scholar] [CrossRef] [PubMed]
- Andes, D.R.; Safdar, N.; Baddley, J.W.; Playford, G.; Reboli, A.C.; Rex, J.H.; Sobel, J.D.; Pappas, P.G.; Kullberg, B.J.; Mycoses Study Group. Impact of treatment strategy on outcomes in patients with candidemia and other forms of invasive candidiasis: A patient-level quantitative review of randomized trials. Clin. Infect. Dis. 2012, 54, 1110–1122. [Google Scholar] [CrossRef]
- Ko, J.H.; Jung, D.S.; Lee, J.Y.; Kim, H.A.; Ryu, S.Y.; Jung, S.I.; Joo, E.J.; Cheon, S.; Kim, Y.S.; Kim, S.W.; et al. Poor prognosis of Candida tropicalis among non-albicans candidemia: A retrospective multicenter cohort study, Korea. Diagn. Microbiol. Infect. Dis. 2019, 95, 195–200. [Google Scholar] [CrossRef]
- Negri, M.; Silva, S.; Henriques, M.; Oliveira, R. Insights into Candida tropicalis nosocomial infections and virulence factors. Eur. J. Clin. Microbiol. Infect. Dis. 2012, 31, 1399–1412. [Google Scholar] [CrossRef] [PubMed]
- Thomaz, D.Y.; de Almeida, J.N., Jr.; Lima, G.M.E.; Nunes, M.O.; Camargo, C.H.; Grenfell, R.C.; Benard, G.; Del Negro, G.M.B. An Azole-Resistant Candida parapsilosis Outbreak: Clonal Persistence in the Intensive Care Unit of a Brazilian Teaching Hospital. Front. Microbiol. 2018, 9, 2997. [Google Scholar] [CrossRef] [PubMed]
- Pinhati, H.M.; Casulari, L.A.; Souza, A.C.; Siqueira, R.A.; Damasceno, C.M.; Colombo, A.L. Outbreak of candidemia caused by fluconazole resistant Candida parapsilosis strains in an intensive care unit. BMC Infect. Dis. 2016, 16, 433. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.J.; Kim, Y.J.; Yong, D.; Byun, J.H.; Kim, T.S.; Chang, Y.S.; Choi, M.J.; Byeon, S.A.; Won, E.J.; Kim, S.H.; et al. Fluconazole-Resistant Candida parapsilosis Bloodstream Isolates with Y132F Mutation in ERG11 Gene, South Korea. Emerg. Infect. Dis. 2018, 24, 1768–1770. [Google Scholar] [CrossRef] [PubMed]
- Fan, X.; Xiao, M.; Zhang, D.; Huang, J.J.; Wang, H.; Hou, X.; Zhang, L.; Kong, F.; Chen, S.C.; Tong, Z.H.; et al. Molecular mechanisms of azole resistance in Candida tropicalis isolates causing invasive candidiasis in China. Clin. Microbiol. Infect. 2019, 25, 885–891. [Google Scholar] [CrossRef]
- Paul, S.; Kannan, I.; Mohanram, K. Extensive ERG11 mutations associated with fluconazole-resistant Candida albicans isolated from HIV-infected patients. Curr. Med. Mycol. 2019, 5, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Zheng, S.; Ng, T.Y.; Li, H.; Tan, A.L.; Tan, T.T.; Tan, B.H. A dedicated fungal culture medium is useful in the diagnosis of fungemia: A retrospective cross-sectional study. PLoS ONE 2016, 11, e0164668. [Google Scholar] [CrossRef]
- Astvad, K.M.T.; Johansen, H.K.; Røder, B.L.; Rosenvinge, F.S.; Knudsen, J.D.; Lemming, L.; Schønheyder, H.C.; Hare, R.K.; Kristensen, L.; Nielsen, L.; et al. Update from a 12-Year Nationwide Fungemia Surveillance: Increasing Intrinsic and Acquired Resistance Causes Concern. J. Clin. Microbiol. 2018, 56, e01564-17. [Google Scholar] [CrossRef]
| Total | Period 1 | Period 2 | p-Value | |
|---|---|---|---|---|
| N = 223 (%) | (2013–2015) | (2016–2018) | ||
| N = 69, (%) | N = 154, (%) | |||
| Age, median (IQR 1) | 71 (60–79) | 67 (57–76) | 72 (64–80) | 0.027 |
| Age ≥ 75 years | 85 (38.1) | 18 (26.1) | 67 (43.5) | 0.013 |
| Male | 127 (57.0) | 46 (66.7) | 81 (52.6) | 0.05 |
| Female | 96 (43.0) | 23 (33.3) | 73 (47.4) | |
| Main comorbidities | ||||
| Charlson comorbidity index, median (IQR) | 3 (1–6) | 3 (2–6) | 3 (1–6) | 0.97 |
| Diabetes mellitus | 83 (37.2) | 24 (34.8) | 59 (38.3) | 0.614 |
| Malignancy | 113 (50.7) | 39 (56.5) | 74 (48.1) | 0.242 |
| Chronic central nervous system disease | 64 (28.7) | 16 (23.2) | 48 (31.2) | 0.223 |
| Chronic kidney disease | 72 (32.3) | 19 (27.5) | 53 (34.4) | 0.31 |
| Chronic liver disease | 28 (12.6) | 11 (15.9) | 17 (11.0) | 0.307 |
| Chronic pulmonary disease | 30 (13.5) | 9 (13.0) | 21 (13.6) | 0.905 |
| Chronic heart disease | 103 (46.2) | 36 (52.2) | 67 (43.5) | 0.23 |
| Clinical conditions | ||||
| Mechanical ventilation | 66 (29.6) | 13 (18.8) | 53 (34.4) | 0.019 |
| Urinary catheter | 166 (74.4) | 41 (59.4) | 125 (81.2) | 0.001 |
| Central venous catheter | 160 (71.7) | 47 (68.1) | 113 (73.4) | 0.42 |
| Parenteral nutrition | 207 (92.8) | 60 (87.0) | 147 (95.5) | 0.045 |
| Hemodialysis | 46 (20.6) | 11 (15.9) | 35 (22.7) | 0.247 |
| Steroid use | 98 (43.9) | 40 (58.0) | 58 (37.7) | 0.005 |
| Neutropenia | 19 (8.5) | 10 (14.5) | 9 (5.8) | 0.032 |
| Chemotherapy | 60 (26.9) | 18 (26.1) | 42 (27.3) | 0.854 |
| Duration of hospital stay before candidemia diagnosis median days, (IQR) | 20 (8–41) | 13 (6–33) | 21 (9–45) | 0.046 |
| Recent surgery in the current admission | 61 (27.4) | 32 (46.4) | 29 (18.8) | <0.001 |
| Previous admission to intensive care unit within 3 months | 84 (37.7) | 21 (30.4) | 63 (40.9) | 0.136 |
| Previous use of antibiotics within 1 month | 200 (89.7) | 64 (92.8) | 136 (88.3) | 0.313 |
| Source of candidemia | ||||
| Gastrointestinal tract | 26 (11.7) | 6 (8.7) | 20 (13.0) | 0.356 |
| Central venous catheter | 130 (58.3) | 35 (50.7) | 95 (61.7) | 0.125 |
| Urinary tract | 12 (5.4) | 0 (0.0) | 12 (7.8) | 0.02 |
| Abscess | 3 (1.3) | 0 (0.0) | 3 (1.9) | 0.554 |
| Others or unknown | 52 (23.3) | 28 (40.6) | 24 (15.6) | <0.001 |
| Antifungal treatment | ||||
| No antifungal treatment | 41 (18.4) | 17 (24.6) | 24 (15.6) | 0.107 |
| Antifungal treatment | 182 (81.6) | 52 (75.4) | 130 (84.4) | |
| Fluconazole | 60/182 (33.0) | 29/52 (55.8) | 31/130 (23.8) | <0.001 |
| Voriconazole | 1/182 (0.5) | 1/52 (1.9) | 0/130 (0.0) | 0.286 |
| Amphotericin B | 5/182 (2.7) | 4/52 (7.7) | 1/130 (0.8) | 0.024 |
| Echinocandins 2 | 116/182 (63.7) | 18/52 (34.6) | 98/130 (75.4) | <0.001 |
| Antifungal treatment duration, median days (IQR) | 13 (5–16) | 11 (6–16) | 13 (5–16) | 0.885 |
| Length of hospital stay after diagnosis of candidemia, median days (IQR) | 19 (7–34) | 13 (6–33) | 19 (7–35) | 0.734 |
| EQUAL Candida score 3 | ||||
| For overall patients, median (IQR) | 15 (14–17) | 14 (12–17) | 16 (14–18) | <0.001 |
| For patients with central venous catheter 4 (IQR) | 17 (14–18) | 15 (14–17) | 17 (14–18) | 0.001 |
| For patients without central venous catheter 5 (IQR) | 14 (12–15) | 12 (11–14) | 14 (12–15) | 0.04 |
| Mortality day 30 after diagnosis of candidemia | 104 (46.6) | 30 (43.5) | 74 (48.1) | 0.527 |
| Total N = 223 (%) | Survivor N = 119, (%) | Non-Survivor N = 104, (%) | p-Value | |
|---|---|---|---|---|
| Age, median (IQR 1) | 71 (60–79) | 71 (60–79) | 72 (59–79) | 0.725 |
| Age ≥ 75 years | 85 (38.1) | 46 (38.7) | 39 (37.5) | 0.859 |
| Male Female | 127 (57.0) 96 (43.0) | 68 (57.1) 51 (42.9) | 59 (56.7) 45 (43.3) | 0.951 |
| Main comorbidities | ||||
| Charlson comorbidity index, median (IQR) | 3 (1–6) | 3 (1–5) | 3 (1–6) | 0.078 |
| Charlson comorbidity index ≥ 4 | 91 (40.8) | 42 (35.3) | 49 (47.1) | 0.073 |
| Diabetes mellitus | 83 (37.2) | 45 (37.8) | 38 (36.5) | 0.844 |
| Malignancy | 113 (50.7) | 55 (46.2) | 58 (55.8) | 0.155 |
| Chronic central nervous system disease | 64 (28.7) | 36 (30.3) | 28 (26.9) | 0.584 |
| Chronic kidney disease | 72 (32.3) | 34 (28.6) | 38 (36.5) | 0.204 |
| Chronic liver disease | 28 (12.6) | 12 (10.1) | 16 (15.4) | 0.233 |
| Chronic pulmonary disease | 30 (13.5) | 15 (12.6) | 15 (14.4) | 0.691 |
| Chronic heart disease | 103 (46.2) | 59 (49.6) | 44 (42.3) | 0.277 |
| Clinical conditions | ||||
| Mechanical ventilation | 66 (29.6) | 24 (20.2) | 42 (40.4) | 0.001 |
| Urinary catheter | 166 (74.4) | 83 (69.7) | 83 (79.8) | 0.086 |
| Central venous catheter | 160 (71.7) | 78 (65.5) | 82 (78.8) | 0.028 |
| Parenteral nutrition | 207 (92.8) | 108 (90.8) | 99 (95.2) | 0.200 |
| Hemodialysis | 46 (20.6) | 15 (12.6) | 31 (29.8) | 0.002 |
| Steroid use | 98 (43.9) | 43 (36.1) | 55 (52.9) | 0.012 |
| Neutropenia | 19 (8.5) | 3 (2.5) | 16 (15.4) | 0.001 |
| Chemotherapy | 60 (26.9) | 26 (21.8) | 34 (32.7) | 0.069 |
| Duration of hospital stay before candidemia diagnosis median days, (IQR) | 20 (8–41) | 12 (5–28) | 29 (15–49) | <0.001 |
| Duration of hospital stay before candidemia diagnosis ≥ 21 days | 111 (49.8) | 44 (37.0) | 67 (64.4) | <0.001 |
| Recent surgery in the current admission | 61 (27.4) | 36 (30.3) | 25 (24.0) | 0.299 |
| Previous admission to intensive care unit within 3 months | 84 (37.7) | 36 (30.3) | 48 (46.2) | 0.014 |
| Previous use of antibiotics within 1 month | 200 (89.7) | 106 (89.1) | 94 (90.4) | 0.748 |
| Source of candidemia | ||||
| Gastrointestinal tract | 26 (11.7) | 15 (12.6) | 11 (10.6) | 0.638 |
| Central venous catheter | 130 (58.3) | 62 (52.1) | 68 (65.4) | 0.045 |
| Urinary tract | 12 (5.4) | 7 (5.9) | 5 (4.8) | 0.723 |
| Abscess | 3 (1.3) | 2 (1.7) | 1 (1.0) | 1.000 |
| Others or unknown | 52 (23.3) | 33 (27.7) | 19 (18.3) | 0.096 |
| Candida species of candidemia C. albicans C. parapsilosis C. tropicalis C. glabrata C. krusei C. guilliermondii C. utilis Other Candida species 2 | 93 (41.7) 46 (20.6) 52 (23.3) 21 (9.4) 2 (0.9) 4 (1.8) 2 (0.9) 3 (1.3) | 49 (41.2) 32 (26.9) 20 (16.8) 14 (11.8) 2 (1.7) 0 (0.0) 2 (1.7) 0 (0.0) | 44 (42.3) 14 (13.5) 32 (30.8) 7 (6.7) 0 (0.0) 4 (3.8) 0 (0.0) 3 (2.9) | 0.864 0.013 0.014 0.199 0.500 0.046 0.500 1.000 |
| Antifungal treatment No antifungal treatment Antifungal treatment | 41 (18.4) 182 (81.6) | 11 (9.2) 108 (90.8) | 30 (28.8) 74 (71.2) | <0.001 |
| Fluconazole Voriconazole Amphotericin B Echinocandins 3 | 60/182 (33.0) 1/182 (0.5) 5/182 (2.7) 116/182 (63.7) | 44/108 (40.7) 1/108 (0.8) 3/108 (2.8) 60/108 (50.4) | 16/74 (21.6) 0/74 (0.0) 2/74 (2.7) 56/74 (75.7) | 0.007 1.000 1.000 0.006 |
| Septic shock Mycological failure | 86 (38.6) 85 (38.5) | 23 (19.3) 10 (8.5) | 63 (60.6) 75 (72.1) | <0.001 <0.001 |
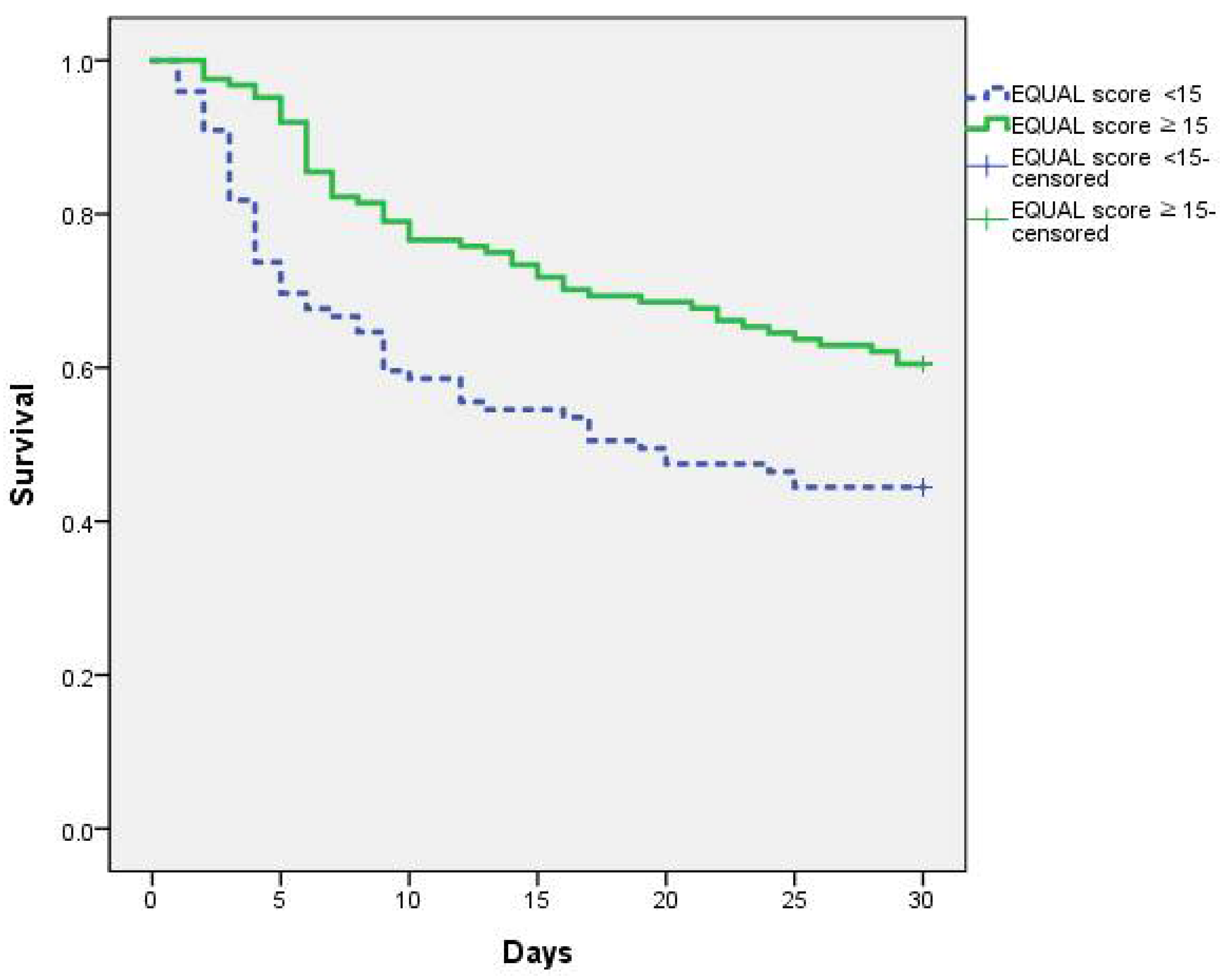
| EQUAL Candida score 4 For overall patients, median (IQR) EQUAL score < 15 for overall patients | 15 (14–17) 99 (44.4) | 15 (14–18) 44 (37.0) | 14 (14–17) 55 (52.9) | 0.222 0.017 |
| For patients with central venous catheter 5 (IQR) | 17 (14–18) | 17 (14–18) | 16 (14–17) | 0.052 |
| EQUAL score < 15 for patients with central venous catheter 5 | 58 (36.0) | 21 (26.9) | 37 (44.6) | 0.020 |
| For patients without central venous catheter 6 (IQR) | 14 (12–15) | 14 (12–15) | 14 (11–14) | 0.074 |
| EQUAL score < 12 for patients without central venous catheter 6 | 14 (22.6) | 6 (14.6) | 8 (38.1) | 0.054 |
| Odds Ratio | 95% Confidence Interval | p-Value | |
|---|---|---|---|
| Charlson comorbidity index ≥ 4 | 3.302 | 1.276–8.546 | 0.014 |
| Neutropenia | 7.855 | 1.669–36.963 | 0.009 |
| Duration of hospital stay before candidemia diagnosis ≥ 21 days | 2.475 | 1.067–5.746 | 0.035 |
| Septic shock | 4.242 | 1.710–10.524 | 0.002 |
| Mycological failure | 29.519 | 11.175–77.970 | <0.001 |
| EQUAL Candida score 1 < 15 | 3.501 | 1.380–8.881 | 0.008 |
| Mechanical ventilation | 3.028 | 0.999–9.177 | 0.050 |
| Total N = 223 (%) | Period 1 (2013–2015) N = 69, (%) | Period 2 (2016–2018) N = 154, (%) | p-Value | |
|---|---|---|---|---|
| C. albicans Fluconazole susceptibility | 93 (41.7) 87/93 (93.5) | 27 (39.1) 27/27 (100.0) | 66 (42.9) 6/60 (90.9) | 0.602 0.176 |
| C. parapsilosis Fluconazole susceptibility | 46 (20.6) 34/46 (73.9) | 12 (17.4) 12/12 (100.0) | 34 (22.1) 22/34 (64.7) | 0.424 0.020 |
| C. tropicalis Fluconazole susceptibility | 52 (23.3) 51/52 (98.1) | 15 (21.7) 15/15 (100.0) | 37 (24.0) 36/37 (97.3) | 0.709 1.000 |
| C. glabrata Fluconazole susceptibility 1 | 21 (9.4) 19/20 (95.0) | 12 (17.4) 11/11 (100.0) | 9 (5.8) 8/9 (88.9) | 0.006 0.450 |
| C. krusei Fluconazole susceptibility | 2 (0.9) 0/2 (0.0) | 0 (0.0) NA 2 | 2 (1.3) 0/2 (0.0) | 1.000 NA |
| C. guilliermondii Fluconazole susceptibility | 4 (1.8) 4/4 (100.0) | 1 (1.4) 1/1 (100.0) | 3 (1.9) 3/3 (100.0) | 1.000 NA |
| C. utilis Fluconazole susceptibility | 2 (0.9) 2/2 (100.0) | 0 (0.0) NA | 2 (1.3) 2/2 (100.0) | 1.000 NA |
| Other Candida species 3 Fluconazole susceptibility 4 | 3 (1.3) 2/2 (100.0) | 2 (2.9) 1/1 (100.0) | 1 (0.6) 1/1 (100.0) | 0.227 NA |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, J.H.; Suh, J.W.; Kim, M.J. Epidemiological Trends of Candidemia and the Impact of Adherence to the Candidemia Guideline: Six-Year Single-Center Experience. J. Fungi 2021, 7, 275. https://doi.org/10.3390/jof7040275
Kim JH, Suh JW, Kim MJ. Epidemiological Trends of Candidemia and the Impact of Adherence to the Candidemia Guideline: Six-Year Single-Center Experience. Journal of Fungi. 2021; 7(4):275. https://doi.org/10.3390/jof7040275
Chicago/Turabian StyleKim, Jong Hun, Jin Woong Suh, and Min Ja Kim. 2021. "Epidemiological Trends of Candidemia and the Impact of Adherence to the Candidemia Guideline: Six-Year Single-Center Experience" Journal of Fungi 7, no. 4: 275. https://doi.org/10.3390/jof7040275
APA StyleKim, J. H., Suh, J. W., & Kim, M. J. (2021). Epidemiological Trends of Candidemia and the Impact of Adherence to the Candidemia Guideline: Six-Year Single-Center Experience. Journal of Fungi, 7(4), 275. https://doi.org/10.3390/jof7040275






